Contents
What is cervical ectropion
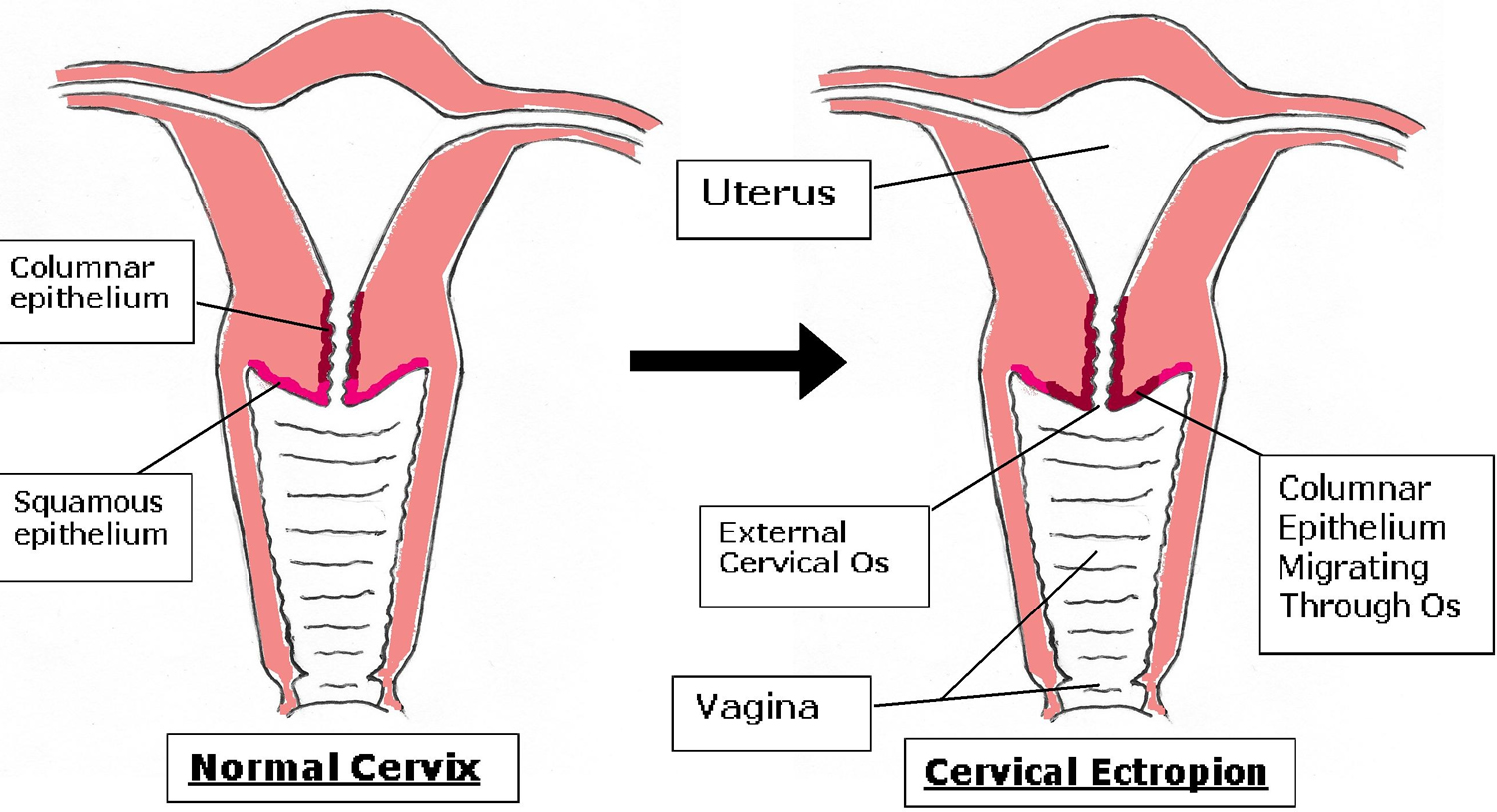
Cervical ectropion (also known as cervical erosion) is the presence of columnar cells on the ectocervix, which is normally composed of a squamous epithelium 1). Cervical ectropion is also sometimes referred to as the transformation zone of the cervix. A cervical ectropion occurs when, due to hormonal changes, the columnar epithelium moves onto the vaginal portion of the cervix (see Figures 3 to 6). A cervical ectropion appears red and may have an inflamed appearance due to the columnar epithelium being thinner than squamous epithelium. This makes the underlying blood vessels more apparent. Along with the red appearance, the columnar epithelium may also secrete mucus which, if abundant, causes a vaginal discharge 2). In western countries, cervical ectropion is considered as a physiological process not requiring treatment. Potential causes of cervical ectropion include adolescent age, pregnancy and hormonal contraceptives 3). Some clinicians believe cervical ectropion could be a normal asymptomatic variant, whereas others believe it to be correlated with chronic cervicitis 4). The decision to treat or not remains controversial 5). According to studies in support of routine treatment of cervical erosion, there is a possible relationship between squamous metaplasia and squamous cell carcinoma of the cervix (cervical cancer).
In China, however, cervical ectropion is considered as one of the most common types of chronic cervicitis (inflammation of the cervix) and it is thought that severe cervical ectropion may cause infertility 6). As a result, treatment for cervical ectropion is widely practiced in hospitals in China. It is reported that 20% to 50% of Chinese women of reproductive age have cervical ectropion 7).
In the Chinese medical literature, the occurrence of cervical ectropion is not considered to be caused solely by estrogenic hormonal changes; inflammation and trauma have also been implicated in its etiology 8). Inflammatory ectropion presents as a defect or degeneration and necrosis of cervical squamous epithelium combined with infiltration of large numbers of inflammatory cells as evidenced using histopathology. On a smear, superficial, intermediate and basement cells can be found with degenerated and necrotic cells, mild dyskaryotic cells and large numbers of neutrophils; small numbers of monocytes, lymphocytes, plasmocytes and macrophages can also be seen 9).
Cervical ectropion has been associated with both the combined oral contraceptive pill and chlamydia trachomatis 10). Changing the method of contraception may be considered for those women who are unable to accept the increase in physiological discharge associated with cervical ectropion. Screening for chlamydia and other sexually transmitted infections should be considered for those women who are at risk. Cervical ectropion has also been found in 5% to 25% of women presenting with postcoital bleeding (bleeding after sex) 11). The presence of the metaplastic columnar epithelium can also manifest a myriad of other symptoms including increased vaginal discharge, leukorrhea (a whitish or yellowish discharge of mucus from the vagina), pelvic pain, recurrent cervicitis (inflammation of the cervix), and dyspareunia (painful sex) 12). These women need appropriate follow up with a cervical smear and colposcopy.
Clinical macroscopic examination describes three grades (I, II and III) of cervical ectropion based on size, the severity of the lesion and the rate of growth of columnar epithelium. These are described as simple pattern, granular pattern and mammilla pattern 13). Macroscopically it may be difficult to distinguish cervical ectropion from cervical intraepithelial neoplasia (CIN), cancer in situ. Thus a cervical smear for cytological examination should be routinely performed to exclude dysplasia. In addition, colposcopy and a biopsy may also be needed for histopathologic examination.
Although some clinicians claim that cervical ectropion is a spontaneous process of metaplasia and does not need treatment, there are several arguments that support treatment for cervical ectropion. The most popular argument supporting the treatment is cervical cancer protection. It is well known that there is a relationship between squamous metaplasia and induction of squamous cell carcinoma of the cervix and that the cells undergoing metaplasia are more susceptible to carcinogens 14), 15). Thus, theoretically, the risk of squamous cell carcinoma of the cervix may be lower if treatment of the cervical ectropion begins without delay. As proof of this theory, among all of the subjects included in a study involving 124 women with symptomatic cervical ectropion 16), there were 2 (1.8%) abnormal smear results after 1 year of follow-up. This high abnormality rate may be due to the inadequate mucosal barriers against sexually transmitted infections such as HPV (human papilloma virus) on cervical ectropion areas 17). Monroy et al. 18) also reported that the prevalence of HPV was higher in cervical ectropion and that HPV infection in cervical ectropion patients was accompanied by a mucosal IgA antibody response. Their results emphasized that cervical ectropion is a risk factor for infection with high-risk HPV genotypes, in particular HPV 18 19). Furthermore, cervical ectropion also makes the epithelium more sensitive to sexually transmitted infections such as Chlamydia trachomatis and Neisseria gonorrhoeae 20), 21) and this condition may explain the higher rates of recurrent cervicitis in these patients. Recurrent cervicitis may also be a reason for pelvic inflammatory disease, which causes pelvic pain.
Make an appointment with your doctor if you have any signs or symptoms that concern you.
What is a cervix
The cervix is part of the lower end of the uterus. The lumen (internal cavity) of the uterus communicates with the vagina by way of a narrow passage through the cervix called the cervical canal.
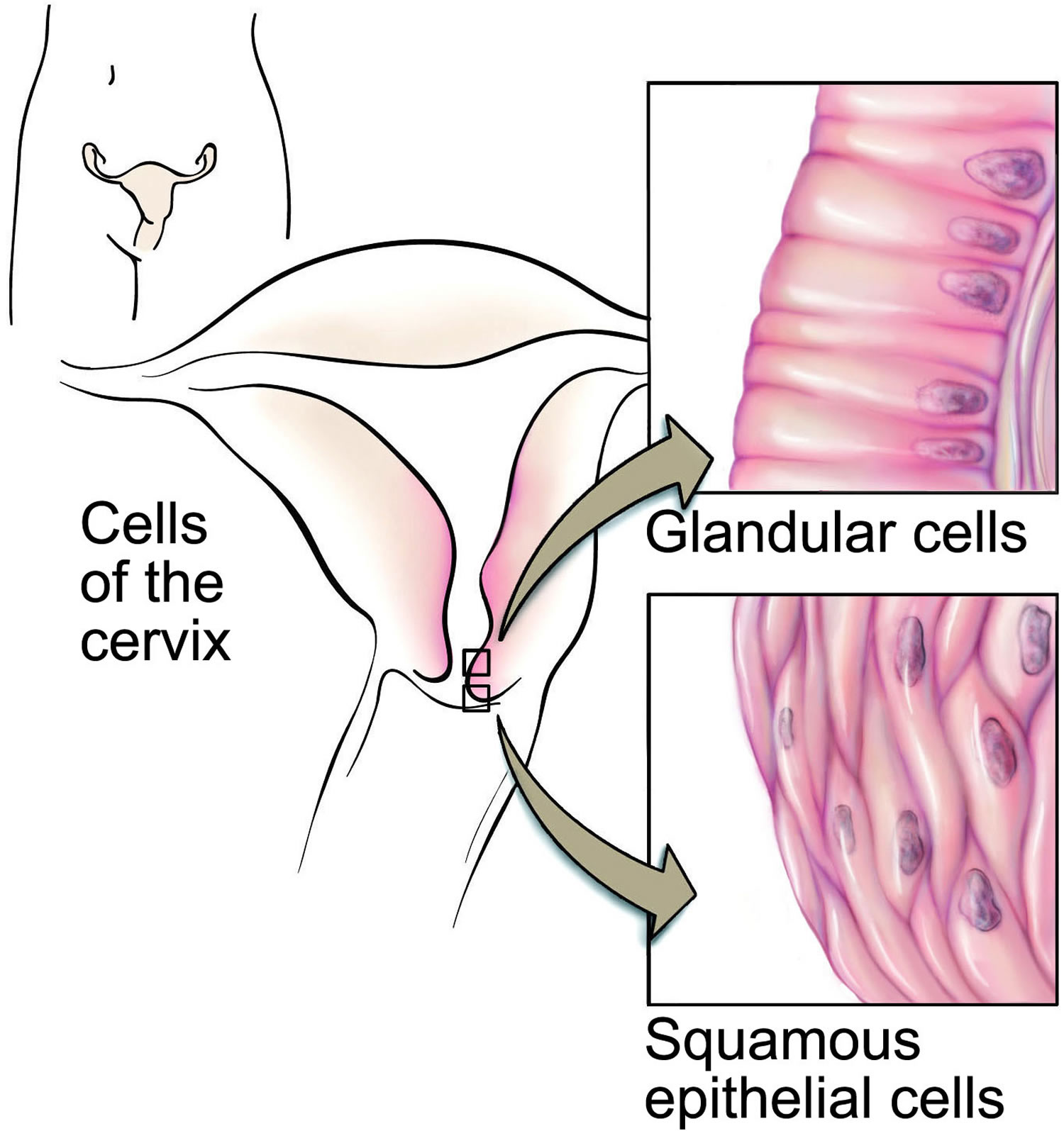
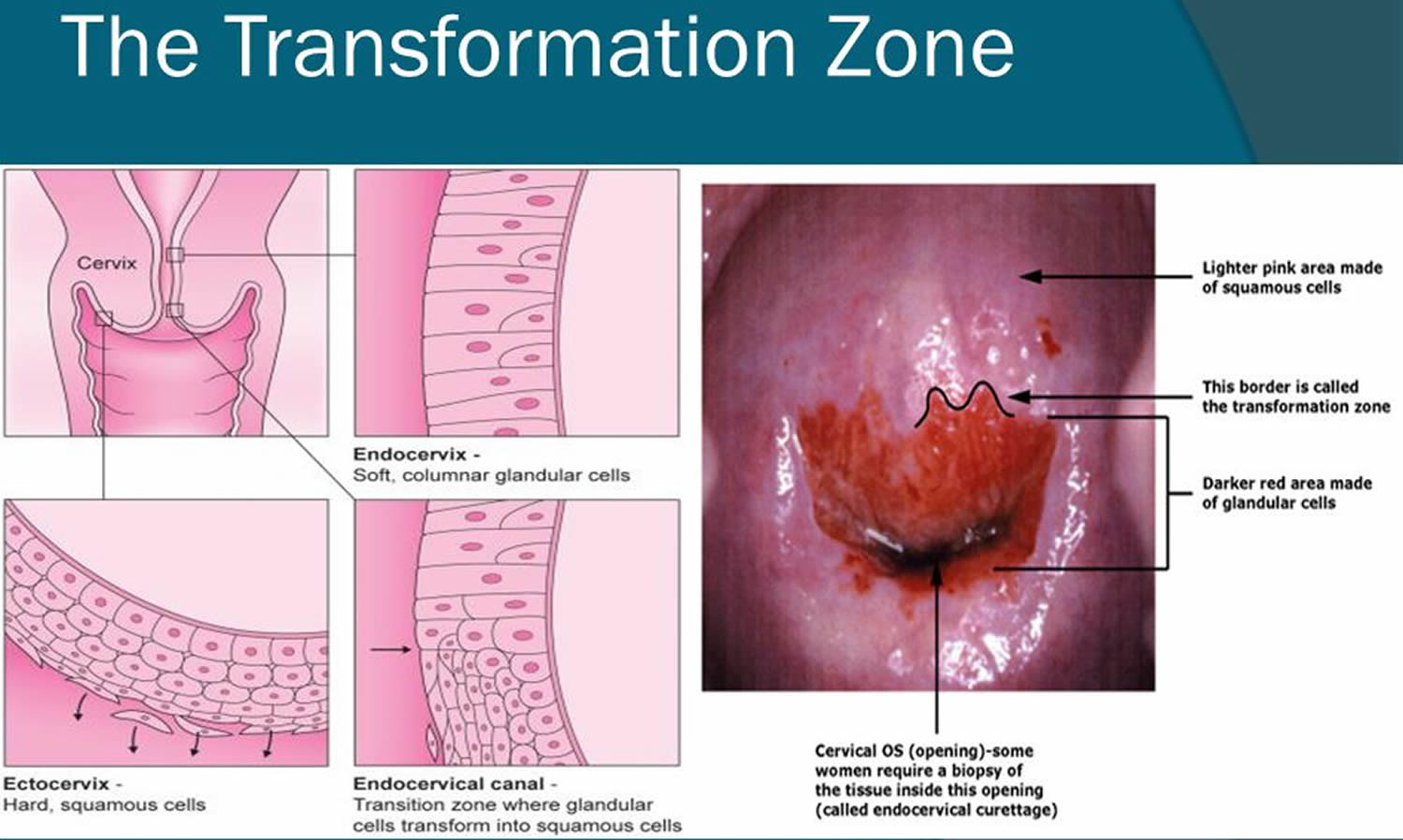
The cervix has two different parts and is covered with two different types of cells.
- The part of the cervix closest to the body of the uterus is called the endocervix and is covered with glandular cells.
- The part next to the vagina is the exocervix (or ectocervix) and is covered in squamous cells.
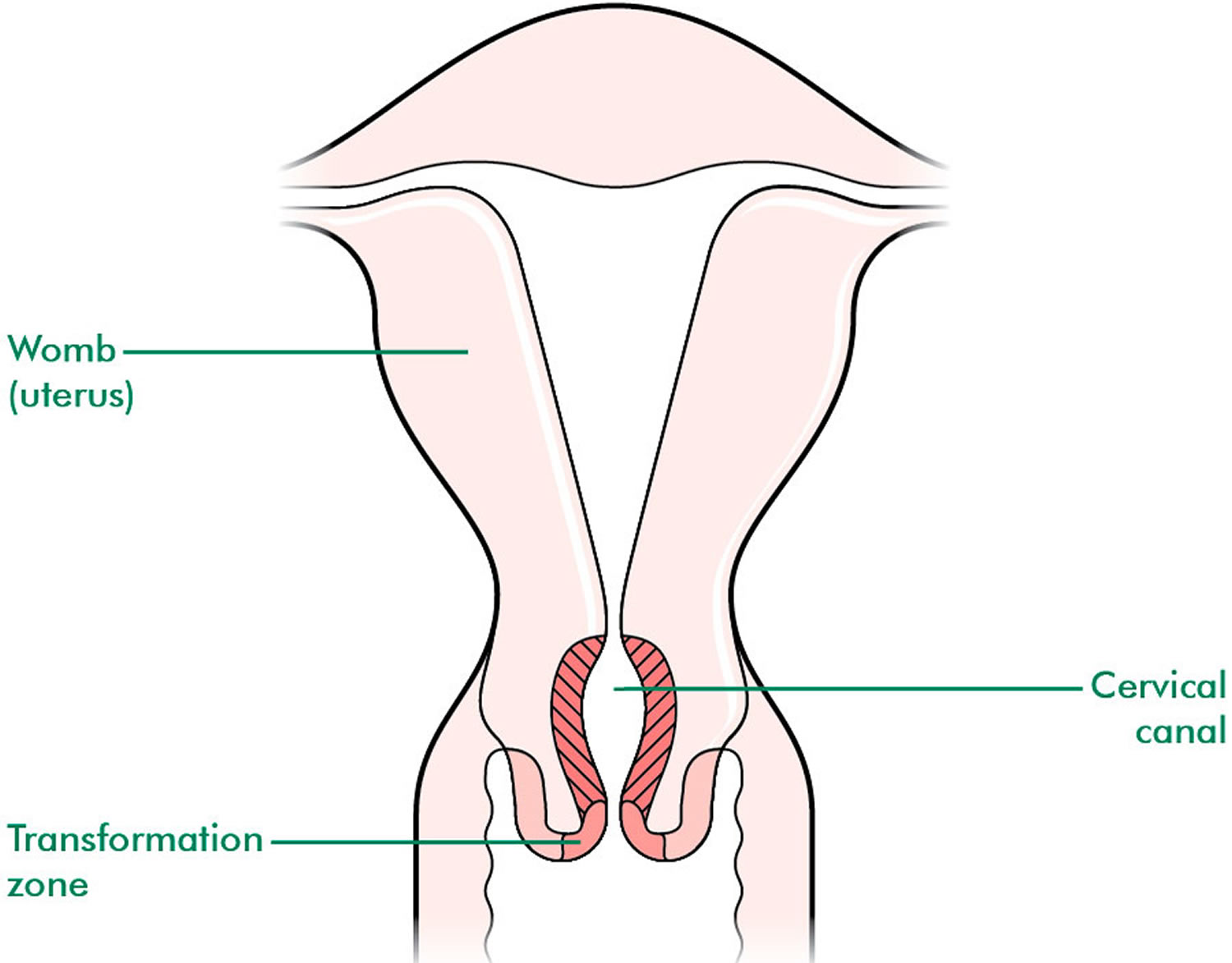
These two cell types meet at a place called the transformation zone. The exact location of the transformation zone changes as you get older and if you give birth.
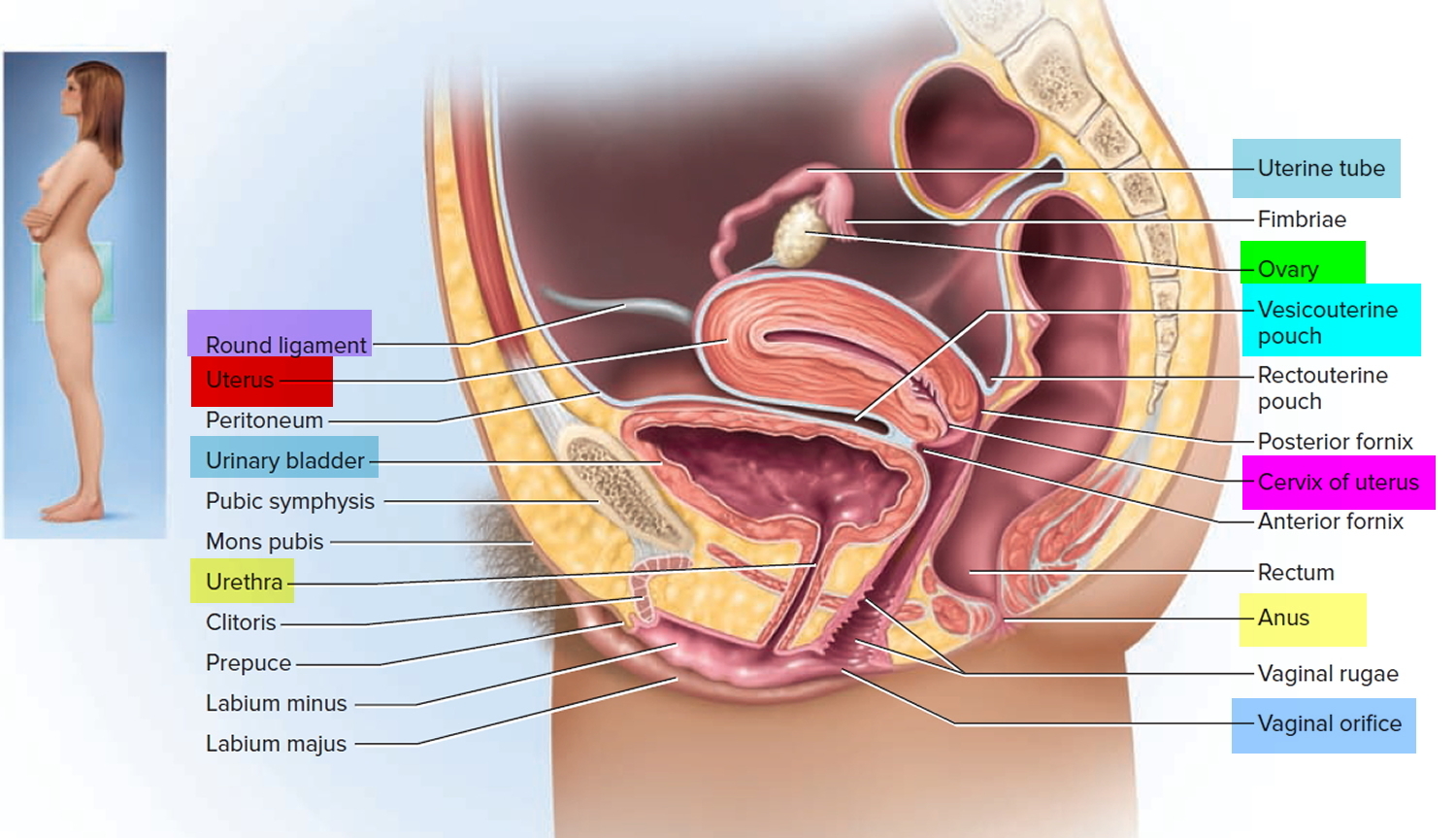
Figure 1. Cervix position
Figure 2. Cervix location
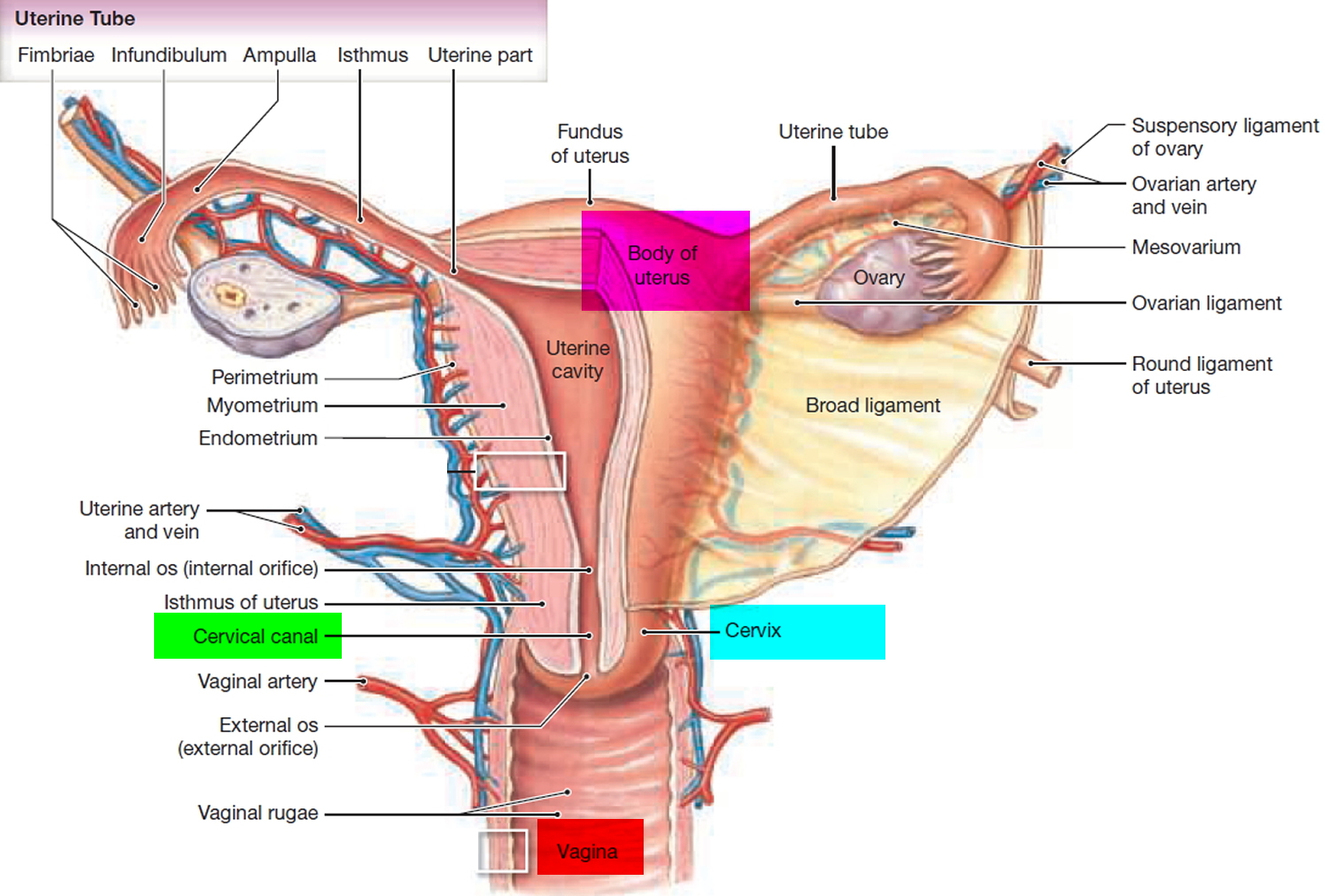
Figure 3. Cervical epithelium
Figure 5. Cervical Transformation Zone
Figure 6. Cervical Transformation Zone
Cervical ectropion causes
Potential causes of ectropion include adolescent age, pregnancy, and hormonal contraceptives. Some clinicians believe ectropion could be a normal asymptomatic variant, whereas others believe it to be correlated with chronic cervicitis.
Cervical ectropion symptoms
Cervical ectropion consists of secretion of epithelium and may increase mucus production, which may cause:
- Vaginal discharge is the most common symptom.
- Abnormal bleeding from the uterus
- Post-coital bleeding (vaginal bleeding after sex)
- Recurrent cervicitis
- Pelvic pain or pain during intercourse
Post-coital bleeding mainly comes from surface lesions of the genital tract to include cervical polyps, cervicitis, ectropion, cervical intra-epithelial lesion (CIN), or carcinoma 22). The prevalence of cervical cancer in women with postcoital bleeding is 3.0 to 5.5% and prevalence of CIN is 6.8% to 17.8% 23).Therefore, if you have any abnormal discharge, bleeding, pain in your pelvic area, you need to see a doctor in order to exclude cancer or other more serious gynecologic problems.
Cervical ectropion treatment
The treatment goal for symptomatic ectropion is to destroy the glandular columnar epithelium, thereby inducing squamous metaplasia, leading to the resolution of vulvovaginal pruritus, irritation, yellowish discharge, and dyspareunia. Reported treatment modalities include laser ablation, microwave ablationand cryosurgery.6, 7, 11, 12, 13 Most studies have reported very high cure rates, such as a case series of 50 patients by Mohanty et al7 who reported a cure rate of 98% in patients who were treated with cryotherapy.
The treatments currently available are electrocoagulation 24), cryocauterization 25), laser cauterization, focused ultrasound 26), platelet-rich plasma injections 27), herbal therapies 28) and drug treatment 29). Li et al. 30) investigated the therapeutic effect of focused ultrasound therapy in patients with symptomatic cervical ectopy. They reported that the rate of effectiveness of focused ultrasound was 99.8%, and the cure rate was 72.52% in patients with symptomatic cervical ectopy 31). Hua et al. 32) reported the effectiveness of autologous platelet-rich plasma applications for the treatment of benign cervical ectopy, with complete-cure rates of 93.7% 33). Although most of the treatment modalities address the efficacy of cervical ectropion regression, some symptoms may not totally end with treatment, including herbal therapies, cauterization and cryotherapy 34).
References [ + ]