Contents
What is a cystoscopy
A cystoscopy is a medical procedure that involves a doctor using a small telescope with a camera called a cystoscope to look inside the lining of your bladder, the openings to the ureters and urethra, the tube that carries urine from the bladder to the outside of the body. A cystoscopy is important in diagnosing conditions that affect the bladder and urinary tract system. This may include early signs of cancer, infection, narrowing, blockage, or bleeding. Cystoscopy can be performed in a number of settings, including a doctor’s office or an operating room, with either topical pain medicine (a numbing jelly in the urethra) or under an anesthetic (general or sedation). A cystoscopy can be uncomfortable, but it is usually not painful.
A cystoscopy is usually a very safe procedure and serious complications are rare. Speak to your doctor or nurse about the possible risks of the procedure before having it.
To do this procedure, the doctor performing the cystoscopy uses a cystoscope—a long, thin instrument with an eyepiece on the external end and a tiny lens and a light on the end that is inserted into the bladder. Here, the healthcare provider can look closely at the inside of the urethra and bladder. The doctor inserts the cystoscope into the patient’s urethra, and the small lens magnifies the inner lining of the urethra and bladder, allowing the doctor to see inside the hollow bladder. Many cystoscopes have extra channels within the sheath to insert other small instruments that can be used to treat, wash the bladder or diagnose urinary problems.
There are two types of cystoscopy: a flexible cystoscopy and a rigid cystoscopy:
- A flexible cystoscope will be used if the specialist only needs to look inside your bladder. You will probably receive a local anesthetic gel or spray to numb the area.
- A rigid cystoscope will be used to take a sample of bladder tissue or treat the area by passing small surgical instruments down the tube. In this case you will probably have a general anesthetic or an epidural (spinal anesthetic).
Both involve passing a thin viewing tube called a cystoscope along the urethra (the tube that carries pee out of the body) and into the bladder, but they’re done in slightly different ways.
Men and women can have either type of cystoscopy. Ask your doctor or nurse which type you’re going to have if you’re not sure.
During a cystoscopy, the doctor may also remove tissue for further exam (called a biopsy). Some problems can be treated during the procedure.
Cystoscopy is most often done as an outpatient procedure. Before the procedure you will empty your bladder. Then you will be placed on an exam table. A liquid or gel local anesthetic may be used on your urethra. The average cystoscopy takes about 5 to 10 minutes.
Results
Your doctor might be able to discuss the results immediately after your procedure. Or, your doctor might need to wait to discuss the results at a follow-up appointment. If your cystoscopy involved collecting a biopsy to test for bladder cancer, that sample will be sent to a lab. When the tests are complete, your doctor will let you know the results.
cystoscopy
How long does a cystoscopy take?
The average cystoscopy takes about 5 to 10 minutes. The rigid cystoscopy procedure can last up to 15-30 minutes.
Does a cystoscopy hurt?
A numbing medicine in the form of a gel will be put into your urethra. This may be mildly uncomfortable until the area is numb. Once the urethra is numb and/or the anesthesia has taken effect, the healthcare provider will put the cystoscope into the urethra. You may have some discomfort when this is done.
During the cystoscopy procedure the bladder is slowly filled with sterile water or saline to better visualize the entire lining. As the fluid fills the bladder, the bladder wall is stretched so the urologist can see clearly. This will mimic the feeling of having a full bladder; however, patients who are awake during the cystoscopy procedure generally do not experience pain or feel mild discomfort.
However, after the cystoscope is removed, your urethra may be sore and you may have a burning feeling for up to 48 hours. You may find some blood in your urine at first, but this should go away within 12 to 24 hours. If you still have pain, or if you get a fever or your urine is bright red, tell your health care provider.
Reasons for Cystoscopy
A doctor may recommend a cystoscopy for a number of reasons, including either visible or microscopic blood in the urine (hematuria), bothersome urinary symptoms, recurrent urinary tract infections (UTIs), as a surveillance method after bladder or certain types of kidney cancer, or as part of a biopsy (diagnostic) or tumor destruction (therapeutic) procedure. No other tests are able to accurately evaluate the inner lining of the bladder to avoid cystoscopy.
Cystoscopy may also be used after gynecologic surgery near the bladder to check for proper placement of sutures and support devices.
Your doctor might conduct a second procedure called ureteroscopy at the same time as your cystoscopy. Ureteroscopy uses a smaller scope to examine the tubes that carry urine from your kidneys to your bladder (ureters).
A doctor may perform a cystoscopy to find the cause of many urinary conditions, including:
- frequent urinary tract infections
- blood in the urine, which is called hematuria
- frequent and urgent need to urinate
- unusual cells found in a urine sample
- painful urination, chronic pelvic pain, or interstitial cystitis (bladder inflammation)/painful bladder syndrome
- urinary blockage caused by prostate enlargement or some other abnormal narrowing of the urinary tract
- a stone in the urinary tract, such as bladder stones or a kidney stone
- an unusual growth, polyp, tumor, or cancer in the urinary tract
Some medical problems of the urinary tract that may be found during cystoscopy include:
- Cancer or tumor of the bladder
- Polyps or overgrowths of normal tissue
- Bladder stones, which are calcium crystals that can lead to infection, inflammation, bleeding, and blockages in the urinary tract.
- Scarring and damage caused by frequent urinary tract infections (UTIs)
- Abnormalities of the urinary tract that may be present at birth and may lead to a backflow of urine or kidney problems
- Injury of the urinary tract
There may be other reasons for your healthcare provider to recommend a cystoscopy.
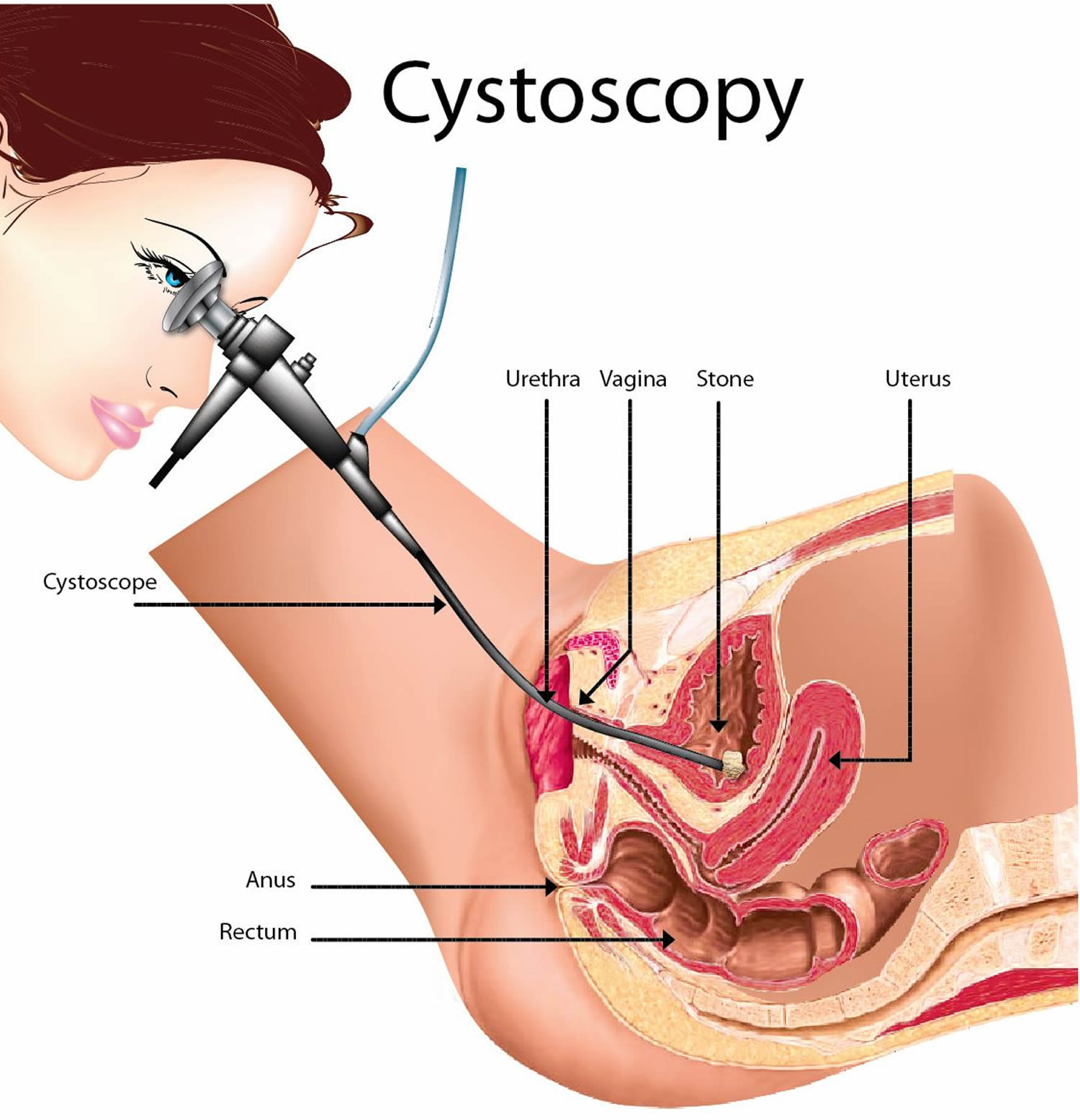
Figure 1. Cystoscopy procedure
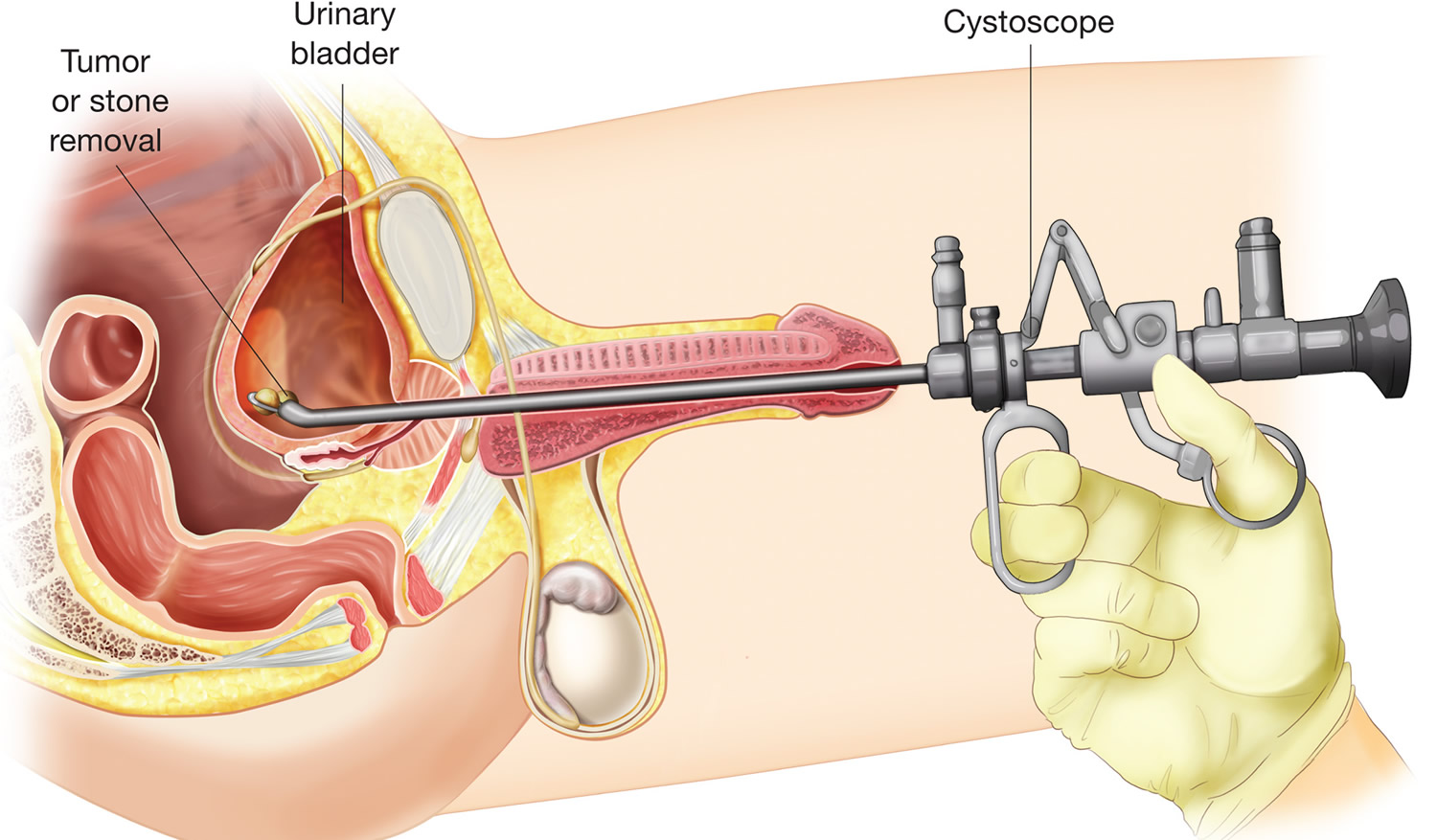
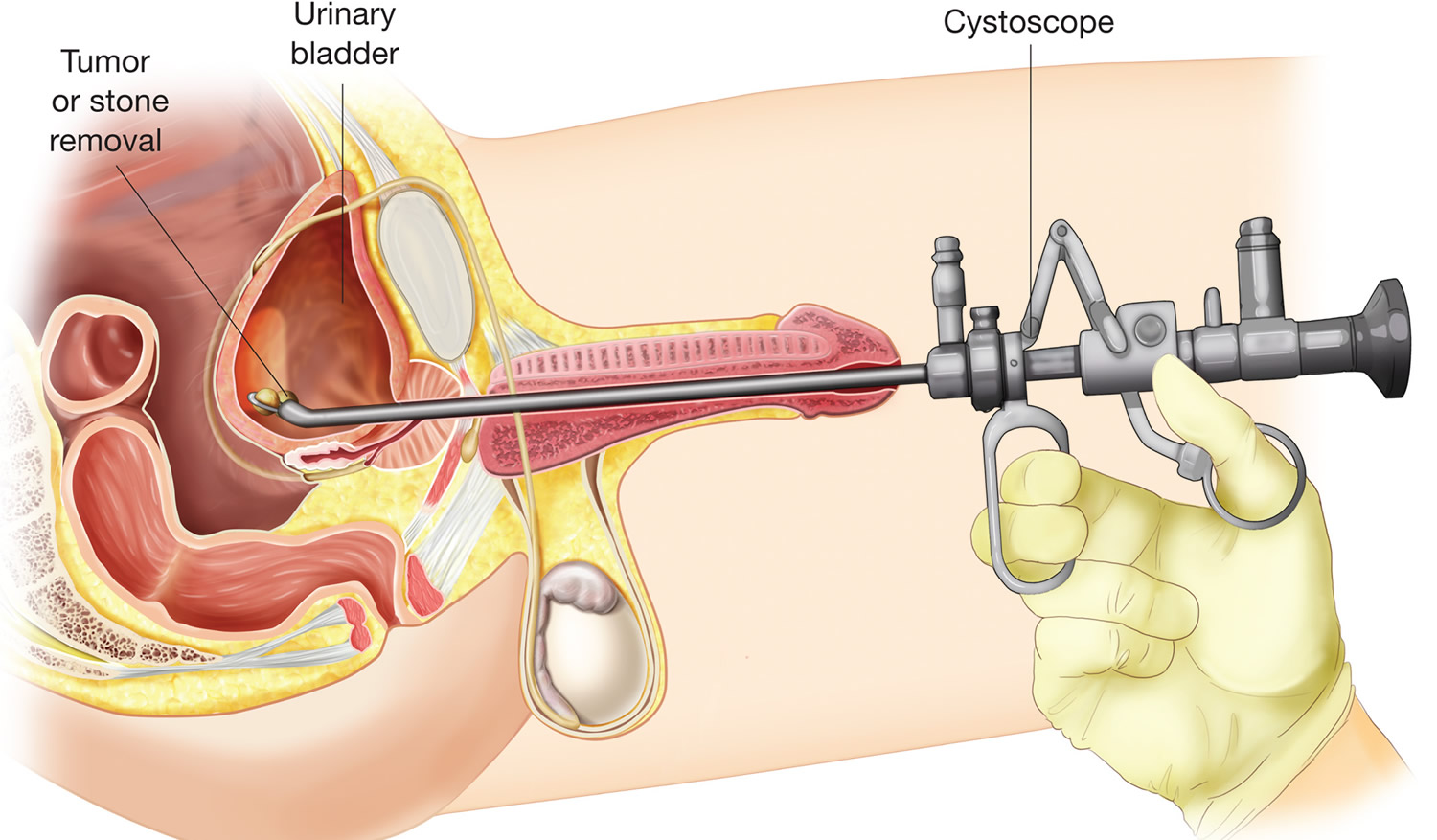
Figure 2. Cystoscopy male (rigid cystoscope)
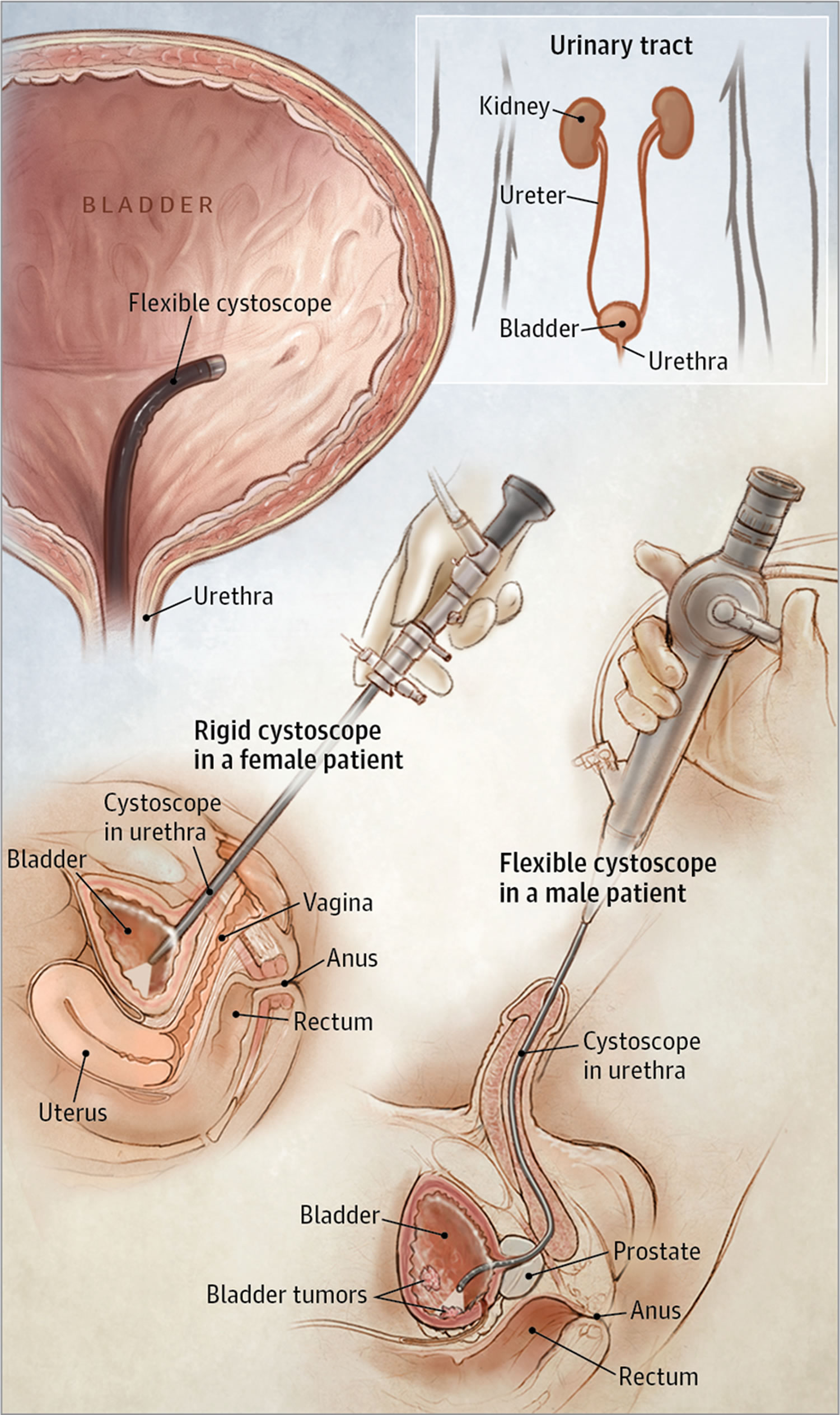
Figure 3. Male cystoscopy (Flexible cystoscopy)
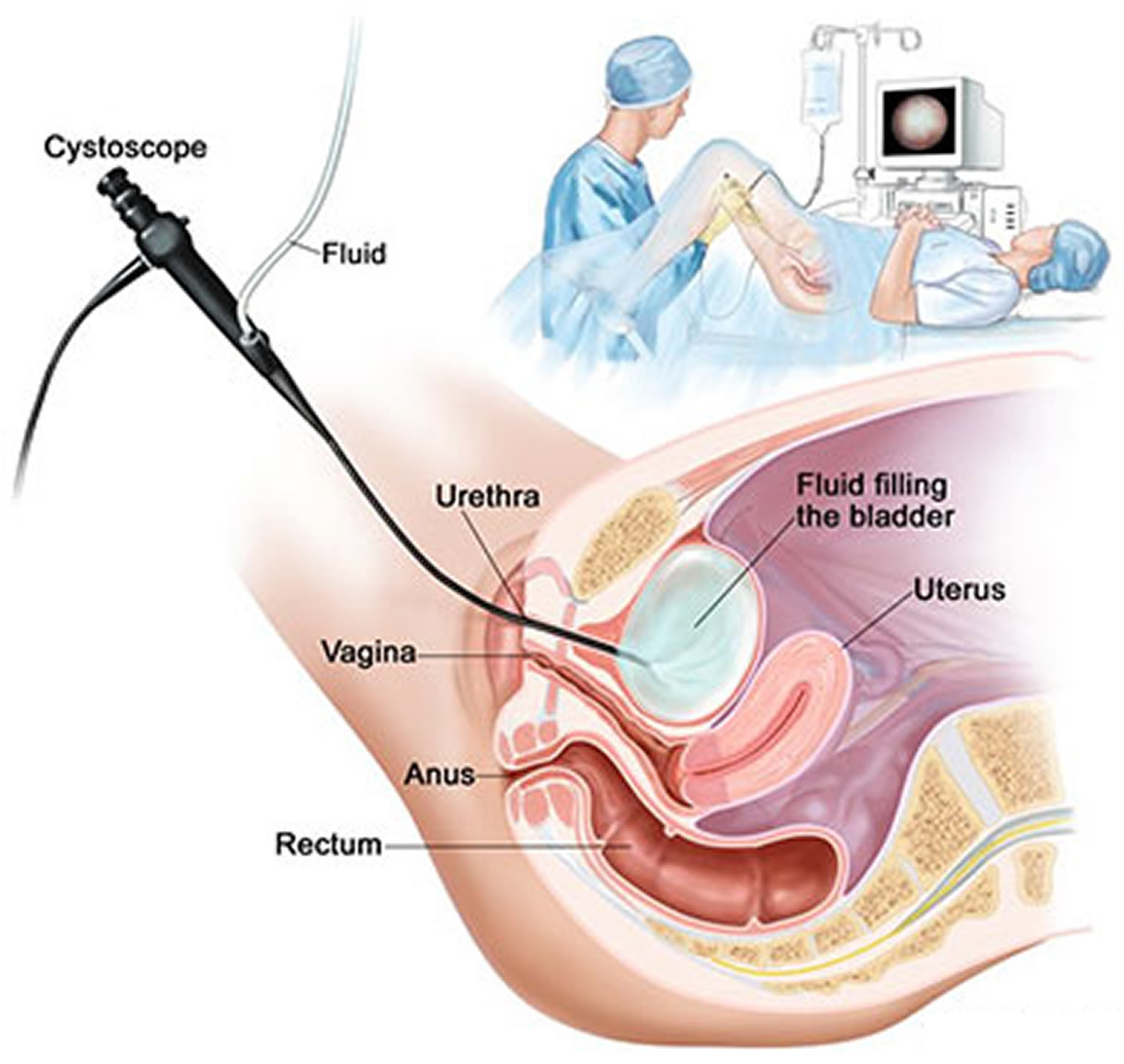
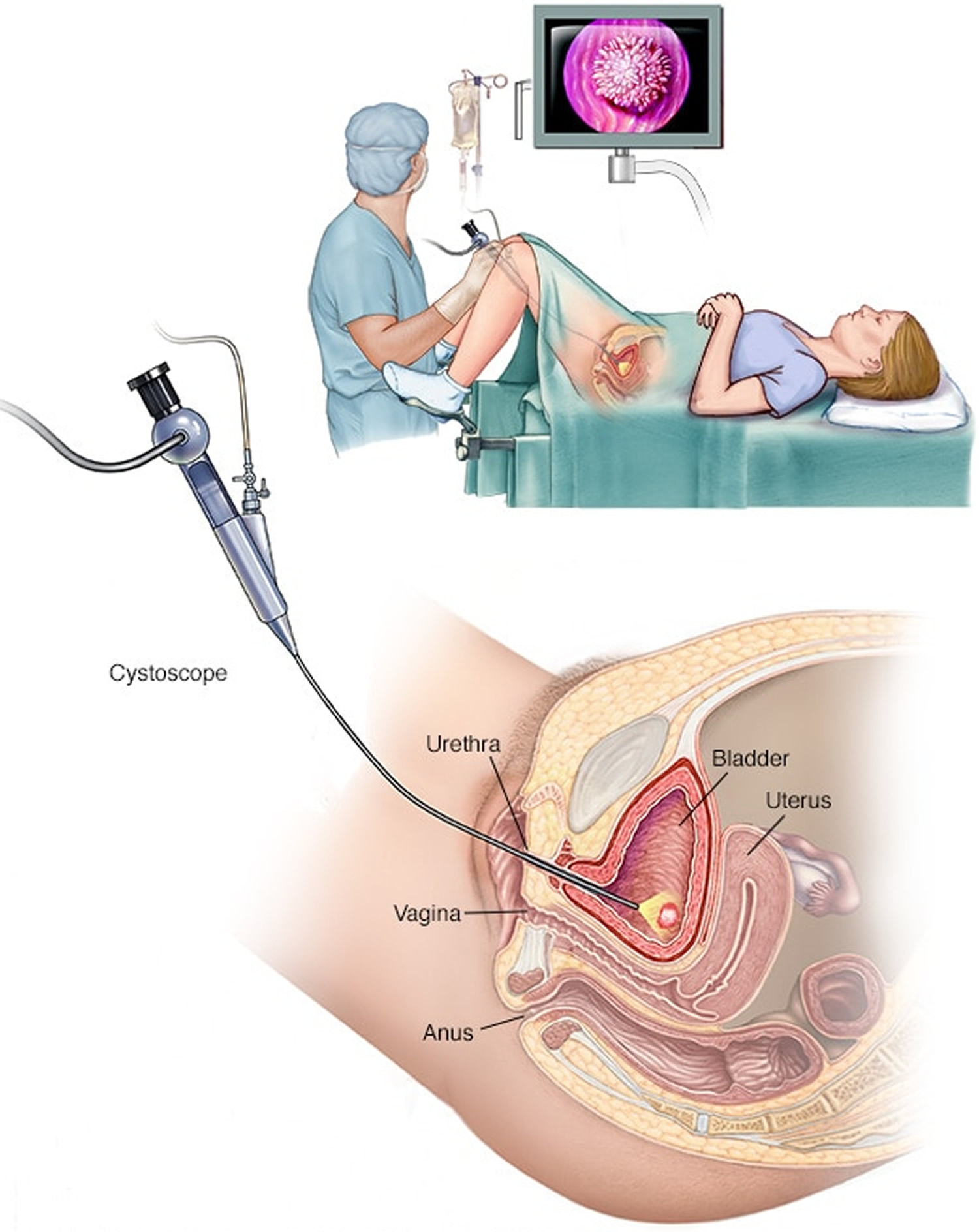
Figure 4. Cystoscopy female (flexible cystoscope)
Urinary bladder
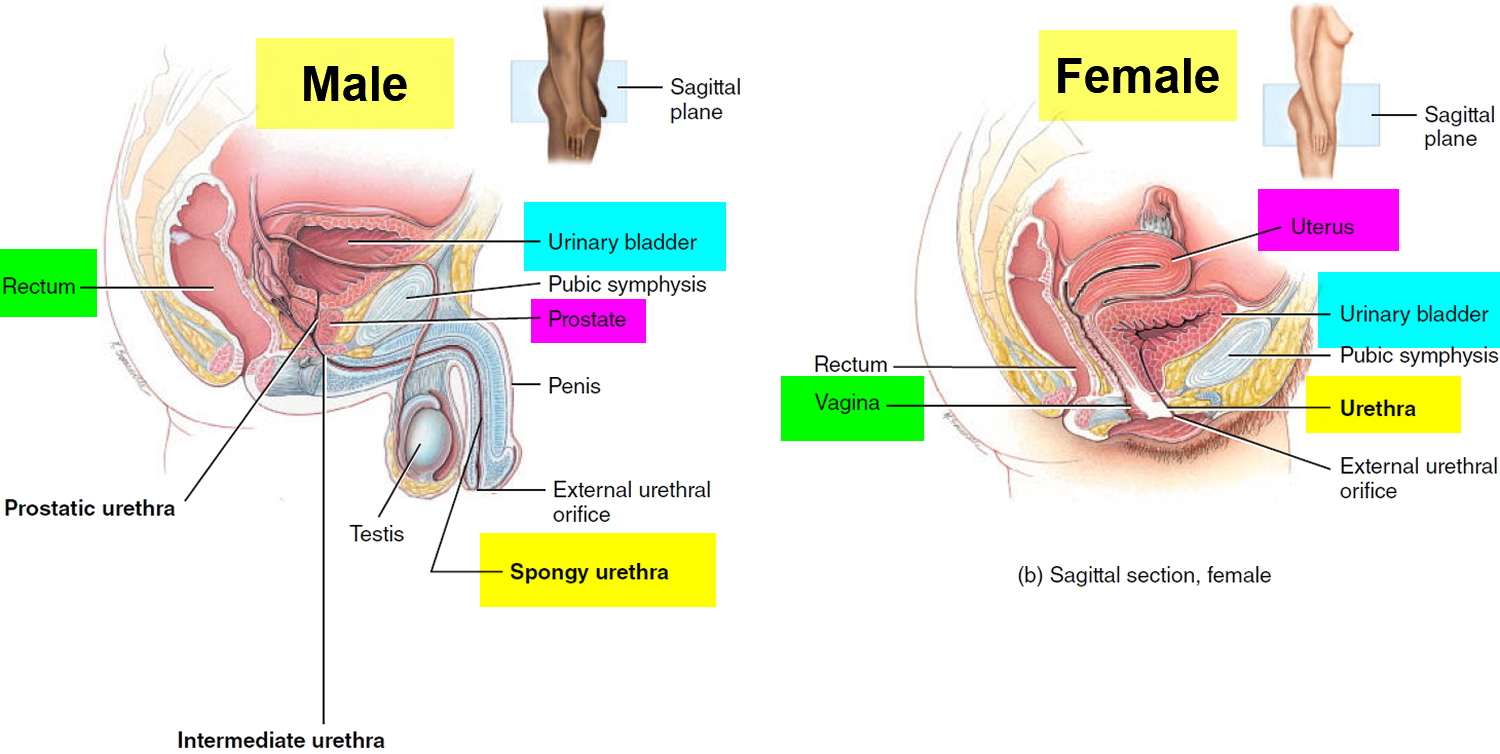
The urinary bladder is a hollow, collapsible muscular sac that stores and expels urine situated in the pelvic cavity posterior to the pubic symphysis. In males, it is
directly anterior to the rectum; in females, it is anterior to the vagina and inferior to the uterus (see Figure 5). Folds of the peritoneum hold the urinary bladder in position. When slightly distended due to the accumulation of urine, the urinary bladder is spherical. When it is empty, it collapses. As urine volume increases, it becomes pear shaped and rises into the abdominal cavity.
Urinary bladder capacity averages 700–800 mL. It is smaller in females because the uterus occupies the space just superior to the urinary bladder.
Anatomy of the Urinary Bladder
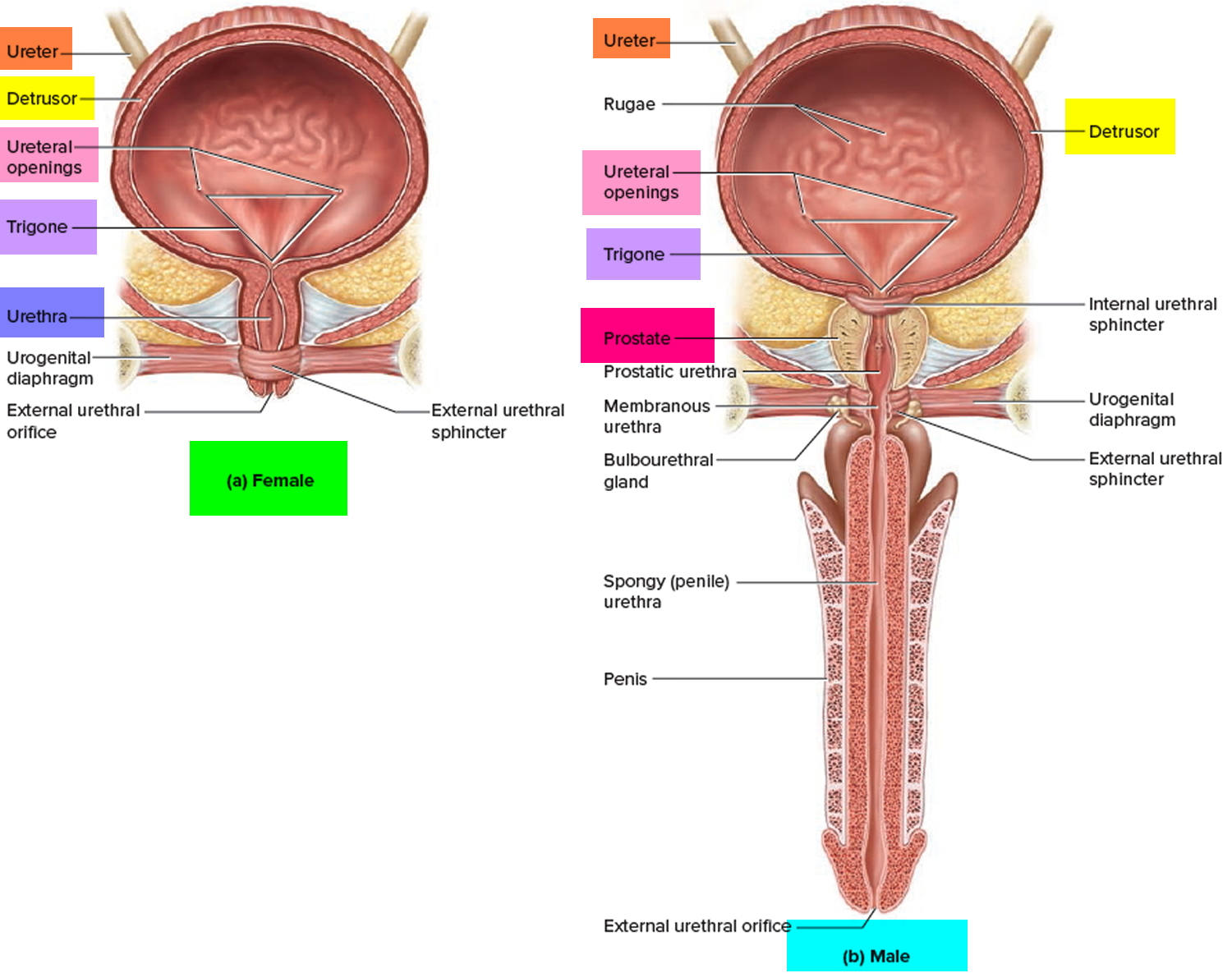
In the floor of the urinary bladder is a small triangular area called the trigone. The two posterior corners of the trigone contain the two ureteral openings; the opening into the urethra, the internal urethral orifice, lies in the anterior corner (see Figure 6). Because its mucosa is firmly bound to the muscularis, the trigone has a smooth appearance. Three coats make up the wall of the urinary bladder. The deepest is the mucosa, a mucous membrane composed of transitional epithelium and an underlying lamina propria similar to that of the ureters. The transitional epithelium permits stretching. Rugae (the folds in the mucosa) are also present to permit expansion of the urinary bladder. Surrounding the mucosa is the intermediate muscularis, also called the detrusor muscle (to push down),
which consists of three layers of smooth muscle fibers: the inner longitudinal, middle circular, and outer longitudinal layers. Around the opening to the urethra the circular fibers form an internal urethral sphincter; inferior to it is the external urethral sphincter, which is composed of skeletal muscle and is a modification of the deep muscles of the perineum. The most superficial coat of the urinary bladder on the posterior and inferior surfaces is the adventitia, a layer of areolar connective tissue that is continuous with that of the ureters. Over the superior surface of the urinary bladder is the serosa, a layer of visceral peritoneum.
Figure 5. Urinary bladder location
Figure 6. Urinary bladder anatomy
Flexible cystoscopy
A flexible cystoscopy is where a thin (about the width of a pencil) and bendy cystoscope is used. You stay awake while it’s carried out.
Flexible cystoscopy preparation
You’ll be sent instructions to follow before your appointment. This will include advice about eating, drinking, and what to do about any medicines you’re taking.
You can usually eat and drink as normal before a flexible cystoscopy.
Before the procedure starts, you’ll be asked to undress from the waist down and put on a hospital gown.
You may be asked to pee into a container so it can be checked for an infection. The procedure may be delayed if a urine infection is found.
Flexible cystoscopy procedure
For a flexible cystoscopy:
- you lie down flat on a special couch
- your genitals are cleaned with an antiseptic and a sheet is placed over the surrounding area
- local anaesthetic gel is applied to your urethra to numb it and help the cystoscope move along it more easily
- the cystoscope is inserted into your urethra and gently moved down towards your bladder
- water may be pumped into your bladder so your doctor or nurse can see inside it more clearly – you may be able to see images sent to a monitor by a camera in the cystoscope
The flexible cystoscope is usually removed after a few minutes. A nurse will stay with you throughout to explain what’s happening.
Does flexible cystoscopy hurt?
People often fear that a cystoscopy will be painful, but it doesn’t usually hurt. Tell your doctor or nurse if you feel any pain during it.
It can be a bit uncomfortable and you may feel like you need to pee during the procedure, but this will only last a few minutes.
Flexible cystoscopy afterwards
After the cystoscope is removed, you may need to go straight to the toilet to empty your bladder before changing back into your clothes.
Your doctor or nurse may be able discuss the results of the cystoscopy shortly afterwards. But if a small tissue sample was removed for testing (biopsy), you may not get the results for two or three weeks.
You can usually go home shortly after a flexible cystoscopy.
Rigid cystoscopy
A rigid cystoscopy is where a cystoscope that doesn’t bend is used. You’re either put to sleep for the procedure or the lower half of your body is numbed while it’s carried out.
Rigid cystoscopy preparation
You’ll be sent instructions to follow before your appointment. This will include advice about eating, drinking, and what to do about any medicines you’re taking.
You’ll usually need to stop eating and drinking for a few hours before a rigid cystoscopy. You’ll also need to arrange for someone to give you a lift home, as you won’t be able to drive for 24 hours.
You’ll be asked to change into a hospital gown for the procedure.
You may be asked to pee into a container so it can be checked for an infection. The procedure may be delayed if a urine infection is found.
Rigid cystoscopy procedure
For a rigid cystoscopy:
- you lie down on a special couch with your legs in supports
- your genitals are cleaned with an antiseptic and a sheet is placed over the surrounding area
- you’re given an injection of general anaesthetic (which makes you fall asleep) into your hand, or a spinal anaesthetic (which numbs the lower half of your body) into your lower back
- the cystoscope is inserted into your urethra and gently moved down towards your bladder
- water may be pumped into your bladder so your doctor or nurse can see inside it more clearly
How long does a cystoscopy take?
The procedure can last up to 15-30 minutes.
Does cystoscopy hurt?
You may have a short, sharp pain as the injection of anesthetic is given, but you won’t have any pain or discomfort during the procedure because you’ll be asleep or your lower half will be numbed.
Rigid cystoscopy afterwards
When the procedure is finished, you’ll be taken to a room or ward to recover from the anesthetic.
Sometimes you may have a thin tube called a catheter placed into your bladder to help you pee. This will be taken out before you go home.
Your doctor or nurse may be able to discuss the results of the cystoscopy shortly afterwards. But if a small tissue sample was removed for testing (biopsy), you may not get the results for two or three weeks.
You can usually go home once the anesthetic has worn off and you’re able to empty your bladder.
Cystoscopy preparation
Your doctor may want you to provide a urine sample to ensure that there is no infection prior to the cystoscopy procedure. He or she may also prescribe a dose of an antibiotic pill to be taken on the day of the cystoscopy procedure. Additional preparation such as stopping blood thinning medications may be needed if a biopsy is planned. Your healthcare provider will give you specific instructions regarding how long to fast. You may be given other instructions about a special diet to follow for a day or two before the cystoscopy procedure.
The type of fasting (not eating or drinking anything) needed before the cystoscopy procedure will depend on the type of anesthetic being used.
If you are going to have a general anesthetic you must stop eating and drinking several hours before the procedure.
If you are going to have a spinal anesthetic (an epidural) you must stop eating and drinking several hours before the procedure.
If you are having a local anesthetic you can eat and drink as usual.
- If you are pregnant or think you might be, tell your healthcare provider.
- Tell your healthcare provider if you are sensitive to or are allergic to any medicines, latex, iodine, tape, or anesthetic agents (local and general).
- Make sure your healthcare provider has a list of all medicines (prescribed and over-the-counter), herbs, vitamins, and supplements that you are taking.
- Tell your healthcare provider if you have a history of bleeding disorders or if you are taking any anticoagulant (blood-thinning) medicines, aspirin, or other medicines that affect blood clotting. You may need to stop these medicines before the procedure.
- If local anesthesia is used, you will be awake during the procedure, but you may be given a sedative. You will need someone to drive you home afterwards.
- If you think you have a urinary tract infection, tell your healthcare provider, because cystoscopy should not be done. Your healthcare provider may check your urine for infection before doing the procedure. (Signs of infection include things like frequent urination, pain or burning when passing urine, fever, and urine that looks dark, cloudy, or reddish in color and smells bad.)
Based on your medical condition, your healthcare provider may request other specific preparation.
Cystoscopy procedure
A cystoscopy may be done on an outpatient basis or during a hospital stay. Cystoscopy procedures may vary, depending on your condition and your healthcare provider’s practices.
Generally, a cystoscopy follows this process:
- You will need to remove any clothing, jewelry, or other objects that may interfere with the procedure.
- If you are asked to remove your clothing, you will be given a gown to wear.
- An intravenous (IV) line may be started in your arm or hand.
- Often an antibiotic is given before the procedure.
- You may be given an IV sedative or anesthetic, depending on your situation and the type of scope that will be used. This will make you sleepy and not feel pain during the cystoscopy. If a sedative or anesthetic is given, your heart rate, blood pressure, breathing, and blood oxygen level will be monitored throughout the procedure.
- You will be positioned on an exam table on your back with your knees up and spread apart. Your feet will be placed in stirrups.
- The genital area is cleaned prior to beginning.
- A numbing medicine in the form of a gel will be put into your urethra. This may be mildly uncomfortable until the area is numb.
- Once the urethra is numb and/or the anesthesia has taken effect, the healthcare provider will guide the cystoscope into the bladder through the urethra. You may have some discomfort when this is done. The cystoscope is a thin, lighted tube with lenses. Most often the cystoscope is bendable (flexible cystoscope), but some models are rigid (rigid cystoscope).
- As the cystoscope is passed through the urethra, the healthcare provider will check the lining. The cystoscope will be moved up until it reaches the bladder.
- Once the cystoscope is in the bladder, the healthcare provider may put sterile water or saline into the bladder to help expand it and make the lining of the bladder easier to see. While the bladder is being filled, this will mimic the feeling of having a full bladder; however, patients who are awake during the cystoscopy procedure generally do not experience pain or feel mild discomfort. You may have the urge to urinate.
- The healthcare provider will check the bladder for any abnormalities.
- The bladder wall should appear smooth, and the bladder should be normal size, shape and position. There should not be any blockages. If any tissue appears abnormal, the cystoscope can be used to remove a small sample.
- A long, thin tool may be passed through the cystoscope to take out a piece of bladder tissue for testing. A urine sample may be taken from the bladder, too.
- The cystoscope will be carefully removed after the procedure has been completed.
The cystoscopy procedure is typically complete within a few minutes depending on the need for biopsy or other intervention.
Cystoscopy recovery
After the cystoscopy procedure, you may be taken to a recovery room for observation if sedation or anesthesia was used. Your recovery process will vary depending on the type of sedation that was given. How long it takes to recover depends if you had a flexible cystoscopy (using local anesthetic gel) or a rigid cystoscopy (under general anesthetic or spinal anesthetic).
Once your blood pressure, pulse, and breathing are stable and you are alert, you will be taken to your hospital room or discharged to your home. Cystoscopy is most often done on an outpatient basis.
You may go back to your usual diet and activities unless your healthcare provider tells you otherwise.
You will be encouraged to drink extra fluids, which dilutes the urine and reduces urinary discomfort, such as burning. Some burning with urination is normal after the procedure but should lessen over time. A warm sitz bath or tub bath may be urged to help ease urinary discomfort.
Some patients experience mild discomfort in their urethra and and you may have a burning feeling with urination, for up to 48 hours after cystoscopy. Pink or red discoloration of the urine with blood may be possible as well, but this should go away within 12 to 24 hours. You should report any fever, blood clots, or worsening pain after cystoscopy to your doctor. It is important to stay well hydrated after this procedure.
Take a pain reliever such as acetaminophen (paracetamol) for soreness or discomfort as advised by your healthcare provider. Aspirin or certain other pain medicines may increase the chance of bleeding. Be sure to take only recommended medicines.
You may be given an antibiotic to take after the procedure. This is to help prevent infection. Be sure to take the antibiotic exactly as instructed.
Tell your healthcare provider if you have any of the following:
- Fever and/or chills
- Urinary frequency or urgency
- Inability to urinate
- Lower back pain
- Continued burning with urination or blood in the urine
Your healthcare provider may give you other instructions after the procedure, depending on your situation.
Going home
After a flexible cystoscopy
You’ll be able to go home shortly after a flexible cystoscopy, once you’ve emptied your bladder.
There’s usually no need to wait in the hospital until the anesthetic has completely worn off.
After a rigid cystoscopy
If you have a rigid cystoscopy, you’ll probably need to stay in hospital for a few hours until the anesthetic starts to wear off.
You can go home once you’re feeling better and you’ve emptied your bladder. Most people leave hospital the same day, but sometimes an overnight stay might be needed.
You’ll need to arrange for someone to take you home as you won’t be able to drive for at least 24 hours.
Getting back to normal
After a flexible cystoscopy
You can return to your normal activities – including work, exercise and having sex – as soon as you feel able to after a flexible cystoscopy.
This will often be later the same day or possibly the day after.
After a rigid cystoscopy
After a rigid cystoscopy:
- rest at home for a day or two – you may need to take a couple of days off work
- make sure someone stays with you for the first 24 hours
- don’t drive or drink alcohol for at least 24 hours
You can usually return to your normal activities – including work, exercise and having sex – when you feel able to.
Contact your doctor for advice if:
- the pain or bleeding lasts more than a few days
- peeing is very painful
- your pee becomes so bloody that you can’t see through it
- you see red lumps (blood clots) in your pee
- you can’t empty your bladder
- your pee smells bad
- you get a high temperature (fever) of 38 °C (100.4 °F) or above
- you feel sick or vomit
- you have pain in your lower back or side
Go to your nearest accident and emergency (A&E) department if you feel really unwell.
These problems could be caused by complications of a cystoscopy, such as an infection.
Cystoscopy side effects
A cystoscopy is usually a very safe procedure and serious complications are rare.
For a few days after a flexible cystoscopy, you may see blood in your urine and feel mild discomfort when passing urine.
With a rigid cystoscopy, you may have some difficulty controlling your bladder (incontinence) for the first few hours after the procedure, but this will usually settle. You may also have some discomfort, need to pass urine urgently or have blood in your urine for a few days.
Bleeding persists very rarely. If it does, discuss with your doctor.
There is also a small risk of developing a urinary tract infection. This can affect your urethra, bladder or kidneys.
Complications of cystoscopy may include:
- Infection
- Bleeding
- Urinary retention due to irritation and swelling from the procedure
- Bladder perforation (poking a hole in the bladder with the cystoscope)
If you experience any side effects, such problems with bleeding or passing urine or develop a fever, it is important to see your doctor as soon as possible.
There may be other risks depending on your specific medical condition. Be sure to discuss any concerns with your healthcare provider before the cystoscopy procedure.
Urinary tract infection may interfere with a cystoscopy.
Urinary tract infections
Urinary tract infections (UTIs) are one of the most common complications of a cystoscopy. These are infections of the bladder, kidneys, or small tubes connected to them.
Symptoms of a UTI can include:
- a burning sensation when peeing that lasts longer than two days
- a high temperature (fever) of 38 °C (100.4 °F) or above
- pee that smells bad
- feeling sick and vomiting
- pain in your lower back or side
Contact your doctor if you have symptoms of a urinary tract infection (UTI). You may need to take antibiotics.
Being unable to empty your bladder
Some people find it difficult to pee after having a cystoscopy.
You’ll normally be asked to empty your bladder before leaving hospital to make sure you’re able to, but sometimes it can become difficult to pee after going home.
This can be a sign that your urethra (the tube that carries pee out of the body) or your prostate (a small gland found in men) is swollen.
Contact your doctor for advice if you’re unable to empty your bladder after a cystoscopy. A thin tube called a catheter may need to be temporarily placed in your bladder to help you pee.
Bleeding and bladder damage
It’s normal to have some blood in your pee for a few days after a cystoscopy. But in rare cases it can be a sign that your bladder has been damaged.
Contact your doctor if you have lots of blood in your pee – for example, you can’t see through your pee – or the bleeding doesn’t stop within a few days.
You may need to have a temporary catheter or surgery to repair any damage to your bladder.