Contents
- What is genital herpes
- Genital herpes cause
- How is genital herpes spread?
- Genital herpes complications
- How can you reduce your risk of getting genital herpes?
- Sexually Transmitted Disease (STD) Risk and Oral Sex
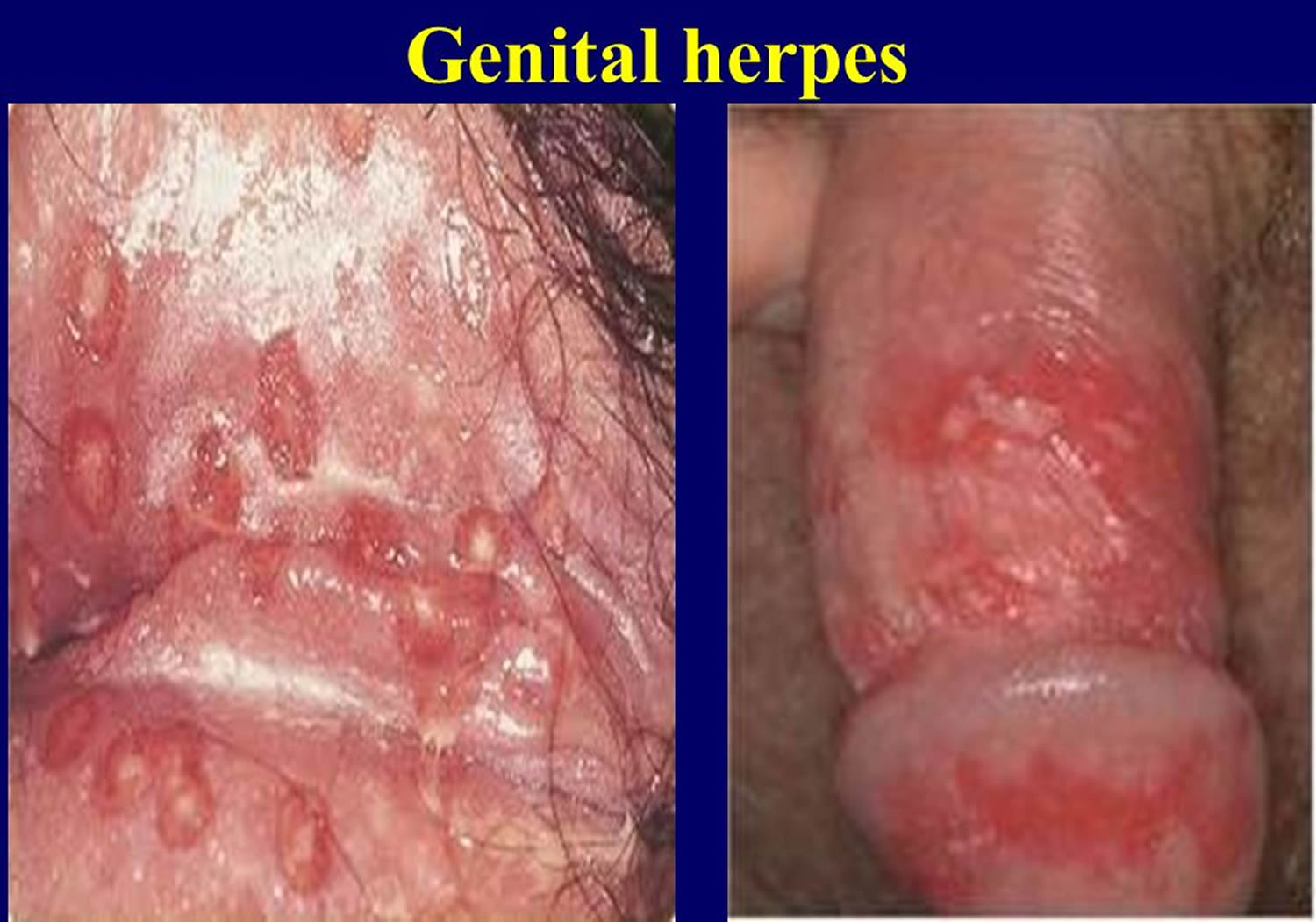
- What does genital herpes look like?
- Genital herpes signs and symptoms
- Genital herpes stages
- Genital herpes and pregnancy
- Genital herpes diagnosis
- Genital herpes test
- Genital herpes treatments
- Genital herpes prognosis
What is genital herpes
Genital herpes is a sexually transmitted disease (STD) caused by two types of herpes viruses – herpes simplex virus type 1 (HSV-1) and herpes simplex virus type 2 (HSV-2) 1, 2. Genital herpes is a chronic, lifelong viral infection that causes recurrent genital ulcers and on rare occasions, disseminated and visceral disease 3. Most people with genital herpes do not know they have it or may have very mild symptoms. Other people have pain, itching and sores around their genitals, anus or mouth. People with genital herpes are able to spread the virus despite having very mild symptoms or no symptoms. Genital herpes can often be spread by skin-to-skin contact during vaginal, anal and oral sex.
Genital herpes is common in the United States. At least 50 million people in the United States—about one in six adults—are infected with HSV. More than one out of every six people aged 14 to 49 years have genital herpes. Genital herpes is more common in women than in men.
Genital herpes can cause outbreaks of blisters or sores on the genitals and anus. Once infected, you can continue to have recurrent episodes of symptoms throughout your life.
There are 2 types of herpes simplex virus (HSV), both viruses can affect either the lips, mouth, genital or anal areas, however:
- Herpes simplex virus type 1 (HSV1) commonly causes cold sores on the lips, mouth or face. However, most people do not have any symptoms. Most people with oral herpes were infected during childhood or young adulthood from non-sexual contact with saliva. Oral herpes caused by HSV-1 can be spread from the mouth to the genitals through oral sex. This is why some cases of genital herpes are caused by HSV-1.
- Herpes simplex virus type 2 (HSV2) causes most genital herpes in the United States 4.
Genital herpes is most easily spread when there are blisters or sores, but can still be passed even if a person has no current blisters or sores or other symptoms. Herpes simplex virus (HSV) also can be present on the skin even if there are no sores. If a person comes into contact with the herpes simplex virus (HSV) on an infected person’s skin, he or she can become infected.
In 2018, there were an estimated 18.6 million people age 18-49 years living with genital herpes caused by herpes simplex virus type 2 (HSV-2), plus several additional million persons living with genital herpes caused by herpes simplex virus type 1 (HSV-1) 5. In 2018 alone, approximately 572,000 persons 18-49 years of age newly acquired HSV-2 in the United States 5. Since genital herpes is not a nationally notifiable condition, the true prevalence (persons living with genital herpes) and incidence (new cases of genital herpes) are difficult to accurately determine.
There is no cure for genital herpes, once you’re infected, you have the virus for the rest of your life. Symptoms often show up again after the first outbreak. Medicine can ease symptoms. It also lowers the risk of infecting others. Condoms can help prevent the spread of a genital herpes infection.
Treatment the first time you have genital herpes
- You may be prescribed antiviral medicine to stop the symptoms getting worse, you need to start taking this within 5 days of the symptoms appearing. You doctor may also give you cream for the pain.
Treatment if the blisters come back
- Go to your doctor or STD clinic if you have been diagnosed with genital herpes and need treatment for an outbreak. Antiviral medicine may help shorten an outbreak by 1 or 2 days if you start taking it as soon as symptoms appear. But outbreaks usually settle by themselves, so you may not need treatment. Recurrent outbreaks are usually milder than the first episode of genital herpes. Over time, outbreaks tend to happen less often and be less severe. Some people never have outbreaks.
- Some people who have more than 6 outbreaks in a year may benefit from taking antiviral medicine for 6 to 12 months. If you still have outbreaks of genital herpes during this time, you may be referred to a specialist.
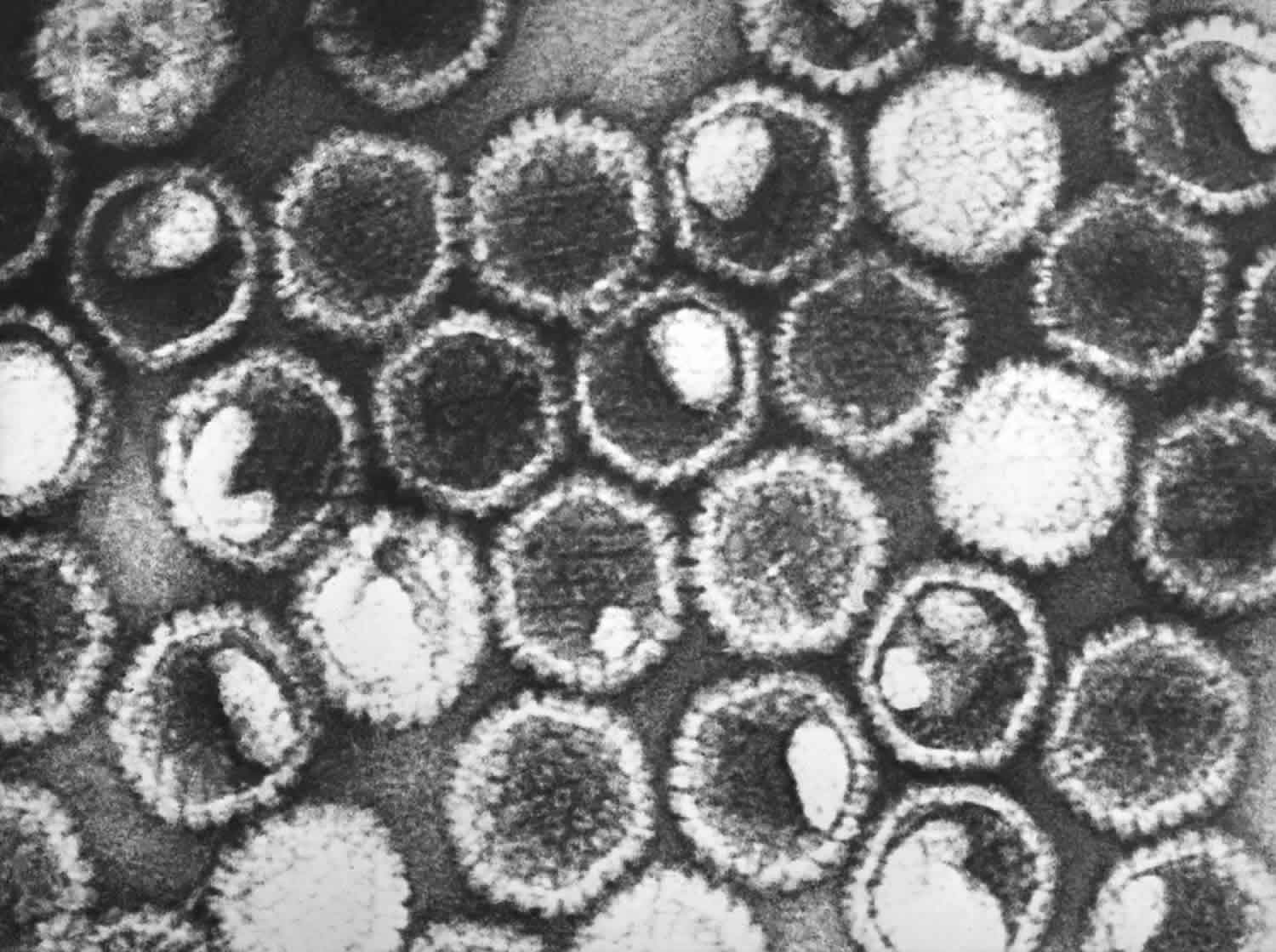
Figure 1. Herpes simplex virus (HSV)
Footnote: This negatively stained transmission electron microscopic image revealed the presence of numerous herpes simplex virions. At the core of its icosahedral proteinaceous capsid, the HSV contains a double-stranded DNA linear genome.
[Source 6 ]- If you think you have genital herpes, it is important to see a doctor as soon as possible. Your doctor can confirm the diagnosis with testing and start treatment. Anti-viral medication may help to prevent transmission. Talk to your doctor about this in more detail.
- If you have genital herpes, it is important to always use condoms and dental dams when having sex, even when you have no symptoms. A dental dam is a square of thin latex that can be placed over the vulva or anal area during oral sex. It is safest to avoid sex when you have blisters, sores or symptoms.
- It is also important to tell your sexual partners that you have genital herpes. Your doctor can help you decide who to tell and how to tell them.
- If you’re pregnant: It’s important to tell your obstetrician that you or a partner have had genital herpes, so that they can monitor you for symptoms and manage your pregnancy safely. There is a risk you can pass the virus on to your baby if you have a vaginal delivery during a first attack of genital herpes. If this happens you may be recommended to have a caesarean delivery.
I’m pregnant. How could genital herpes affect my baby?
If you are pregnant and have genital herpes, it is very important for you to go to prenatal care visits. Tell your doctor if you have ever had symptoms of, or have been diagnosed with, genital herpes. Also tell your doctor if you have ever been exposed to genital herpes. There is some research that suggests that genital herpes infection may lead to miscarriage, or could make it more likely for you to deliver your baby too early.
Herpes infection can be passed from you to your unborn child before birth but is more commonly passed to your infant during delivery. This can lead to a potentially deadly infection in your baby (called neonatal herpes). It is important that you avoid getting herpes during pregnancy. If you are pregnant and have genital herpes, you may be offered anti-herpes medicine towards the end of your pregnancy. This medicine may reduce your risk of having signs or symptoms of genital herpes at the time of delivery. At the time of delivery, your doctor should carefully examine you for herpes sores. If you have herpes symptoms at delivery, a cesarean section or ‘C-section’ is usually performed.
Genital herpes cause
Genital herpes is a sexually transmitted disease (STD) caused by two types of herpes viruses – herpes simplex virus type 1 (HSV-1) and herpes simplex virus type 2 (HSV-2) 2. People with HSV infections can pass along the virus even when they have no visible symptoms.
First-episode genital herpes caused by HSV-1 has been identified with increased frequency among young women, college students, and men who have sex with men 7, 8, 9, 10, 11. Acquisition of genital HSV-1 can occur through genital-genital contact or via receptive oral sex 12, 13. In some settings, such as university campuses, HSV-1 has now replaced HSV-2 as the leading cause of first-episode genital herpes 8. One proposed reason for this shift is decreasing HSV-1 orolabial infection in childhood and early adolescence 10, with first exposure to HSV-1 occurring later in life with sexual activity. Changing sex practices in young adults, namely an increase in oral-genital sex, may also contribute to the changing epidemiology of genital herpes 10. General HSV-1 seroprevalence data, such as reported in the National Health and Nutrition Examination Survey (NHANES) studies, do not provide accurate information on genital herpes infections, since it is not possible to determine whether infection is oral or genital with a positive HSV-1 serologic test. Nevertheless, HSV-1 does contribute significantly to the burden of genital HSV, and there are likely at least several million prevalent genital HSV-1 infections in the United States 5.
Herpes simplex 1
Herpes simplex virus type 1 (HSV-1) is a version of the virus that causes cold sores or fever blisters. People may be exposed to HSV-1 as children due to close skin-to-skin contact with someone infected.
A person with HSV-1 in tissues of the mouth can pass the virus to the genitals of a sexual partner during oral sex. The newly caught infection is a genital herpes infection.
Recurrent outbreaks of genital herpes caused by HSV-1 are often less frequent than outbreaks caused by HSV-2.
Neither HSV-1 nor HSV-2 survives well at room temperature. So the virus is not likely to spread through surfaces, such as a faucet handle or a towel. But kissing or sharing a drinking glass or silverware might spread the virus.
Herpes simplex 2
Herpes simplex virus type 2 (HSV-2) is the most common cause of genital herpes. The virus can be present:
- On blisters and ulcers or the fluid from ulcers
- The moist lining or fluids of the mouth
- The moist lining or fluids of the vagina or rectum
The virus moves from one person to another during sexual activity.
How is genital herpes spread?
You can get genital herpes by having vaginal, anal, or oral sex with someone who has the disease, often he/she is unaware that he/she has HSV infection 14, 15, 16.
If you do not have herpes, you can get infected if you come into contact with the herpes virus in 17:
- A herpes sore;
- Saliva (if your partner has an oral herpes infection) or genital secretions (if your partner has a genital herpes infection);
- Skin in the oral area if your partner has an oral herpes infection, or skin in the genital area if your partner has a genital herpes infection.
You can get herpes from a sex partner who does not have a visible sore or who may not know he or she is infected. It is also possible to get genital herpes if you receive oral sex from a sex partner who has oral herpes.
- You will not get herpes from toilet seats, bedding, or swimming pools, or from touching objects around you such as silverware, soap, or towels. If you have additional questions about how herpes is spread, consider discussing your concerns with a healthcare provider.
Risk factors for genital herpes
A higher risk of getting genital herpes is linked to:
- Contact with genitals through oral, vaginal or anal sex. Having sexual contact without using a barrier increases your risk of genital herpes. Barriers include condoms and condom-like protectors called dental dams used during oral sex. Women are at higher risk of getting genital herpes. The virus can spread more easily from men to women than from women to men.
- Having sex with multiple partners. The number of people you have sex with is a strong risk factor. Contact with genitals through sex or sexual activity puts you at higher risk. Most people with genital herpes do not know they have it. Each additional sexual partner raises your risk of being exposed to the virus that causes genital herpes.
- Having a partner who has genital herpes but is not taking medicine to treat it. There is no cure for genital herpes, but medicine can help limit outbreaks.
- Certain groups within the population. Women, people with a history of sexually transmitted diseases, older people, Black people in in the United States and men who have sex with men diagnosed with genital herpes at a higher than average rate. Women are more likely to have genital herpes than are men. The virus is sexually transmitted more easily from men to women than it is from women to men. People in groups at higher risk may choose to talk to a health care provider about their personal risk.
Genital herpes complications
Complications associated with genital herpes may include:
- Other sexually transmitted infections. Having genital sores increases your risk of transmitting or contracting other sexually transmitted infections, including HIV and AIDS.
- Newborn infection. Babies born to infected mothers can be exposed to the virus during the birthing process. Less often, the virus is passed during pregnancy or by close contact after delivery. Even with treatment, these newborns have a high risk of brain damage, blindness or death for the newborn.
- Bladder problems. In some cases, the sores associated with genital herpes can cause inflammation around the tube that delivers urine from your bladder to the outside world (urethra). The swelling can close the urethra for several days, requiring the insertion of a catheter to drain your bladder.
- Internal inflammatory disease. HSV infection can cause swelling and inflammation within the organs associated with sexual activity and urination. These include the ureter, rectum, vagina, cervix and uterus.
- Meningitis. In rare instances, HSV infection leads to inflammation of the membranes and cerebrospinal fluid surrounding your brain and spinal cord.
- Rectal inflammation (proctitis). Genital herpes can lead to inflammation of the lining of the rectum, particularly in men who have sex with men.
- Finger infection. An HSV infection can spread to a finger through a break in the skin causing discoloration, swelling and sores. The infections are called herpetic whitlow.
- Eye infection. HSV infection of the eye can cause pain, sores, blurred vision and blindness.
- Swelling of the brain. Rarely, HSV infection leads to inflammation and swelling of the brain, also called encephalitis.
- Infection of internal organs. Rarely, HSV in the bloodstream can cause infections of internal organs.
Persons with HSV-2 infection have a threefold increase in the risk of acquiring human immunodeficiency virus (HIV) infection 18. This may be related to open ulcers, or lymphocytes at the site of eruptions, facilitating HIV invasion during sexual contact 19.
Concurrent infection with HSV-2 and HIV increases the severity of HSV episodes and the likelihood of atypical presentations 20. The relationship between genital HSV-1 and HIV infections has not been well studied 21.
How can you reduce your risk of getting genital herpes?
The only way to avoid sexually transmitted diseases (STDs) is to not have vaginal, anal, or oral sex.
If you are sexually active, you can do the following things to lower your chances of getting genital herpes:
- Be in a long-term mutually monogamous relationship with a partner who is not infected with an STD (e.g., a partner who has been tested and has negative STD test results);
- Using latex condoms the right way every time you have sex.
Be aware that not all herpes sores occur in areas that are covered by a latex condom. Also, herpes virus can be released (shed) from areas of the skin that do not have a visible herpes sore. For these reasons, condoms may not fully protect you from getting herpes.
If you are in a relationship with a person known to have genital herpes, you can lower your risk of getting genital herpes if:
- Your partner takes an anti-herpes medication every day. This is something your partner should discuss with his or her doctor.
- You avoid having vaginal, anal, or oral sex when your partner has herpes symptoms (i.e., when your partner is having an outbreak).
Sexually Transmitted Disease (STD) Risk and Oral Sex
Oral sex involves using the mouth, lips, or tongue to stimulate the penis (fellatio), vagina (cunnilingus), or anus (anilingus) of a sex partner. The penis and testicles and the vagina and area around the vagina are also called the genitals or genital area.
Facts:
- The only way to avoid STDs is to not have vaginal, anal, or oral sex.
- Many sexually transmitted diseases (STDs) can be spread through oral sex.
- Using a condom, dental dam or other barrier method each and every time you have oral sex can reduce the risk of giving or getting an STD.
- Although oral sex may carry a lower risk for spreading HIV than other forms of sex, repeated unprotected exposures may increase risk of transmission.
Many STDs, as well as other infections, can be spread through oral sex. Anyone exposed to an infected partner can get an STD in the mouth, throat, genitals, or rectum. The risk of getting an STD from oral sex, or spreading an STD to others through oral sex, depends on a number of things, including:
- The particular STD.
- The sex acts practiced.
- How common the STD is in the population to which the sex partners belong.
- The number of specific sex acts performed.
Oral sex is commonly practiced by sexually active adults. Oral sex can happen between heterosexual (straight) and same-sex (gay or lesbian) couples. More than 85% of sexually active adults aged 18-44 years reported having had oral sex at least once with a partner of the opposite sex. A separate survey conducted during 2007-2010 found that 33% of teenage girls and boys aged 15-17 years reported having had oral sex with a partner of the opposite sex.
In general:
- It may be possible to get some STDs in the mouth or throat from giving oral sex to a partner with a genital or anal/rectal infection, particularly from giving oral sex to a partner with an infected penis.
- It also may be possible to get certain STDs on the penis (and possibly the vagina, anus or rectum) from getting oral sex from a partner with a mouth or throat infection.
- It’s possible to have an STD in more than one area at the same time, for example in the throat and the genitals.
- Several STDs that may be transmitted by oral sex can then spread throughout the body of an infected person.
- STDs can be spread to a sex partner even when the infected partner has no signs or symptoms. If you are infected with an STD, you might not know it because many STDs may have no symptoms.
Which Sexually Transmitted Diseases (STDs) Can Be Passed On from Oral Sex?
- Herpes (herpes simplex virus types 1 and 2)
- Syphilis (Treponema pallidum)
- Human papillomavirus (HPV)
- Human immunodeficiency virus (HIV)
- Trichomoniasis (Trichomonas vaginalis)
- Chlamydia (Chlamydia trachomatis)
- Gonorrhea (Neisseria gonorrhoeae)
- Hepatitis A virus, Shigella and intestinal parasites (amebiasis) can be spread through giving oral sex on the anus.
Is Oral Sex Safer than Vaginal or Anal Sex?
Many STDs can be spread through oral sex. However, it is difficult to compare the exact risks of getting specific STDs from specific types of sexual activity. This is partly because most people who have oral sex also have vaginal or anal sex. Also, few studies have looked at the risks of getting STDs other than HIV from giving oral sex on the vagina or anus, compared to giving oral sex on the penis.
Studies have shown that the risk of getting HIV from having oral sex with an infected partner (either giving or getting oral sex) is much lower than the risk of getting HIV from anal or vaginal sex with an infected partner. This may not be true for other STDs – in one study of gay men with syphilis, 1 out of 5 reported having only oral sex.
- Getting HIV from oral sex may be less likely than vaginal or anal sex, but it still carries risk. If you are having oral sex you should still protect yourself. Repeated unprotected oral sex exposure to HIV may represent a considerable risk for spread of HIV, as well as other STDs for which the risk of spread through oral sex has not been as well studied.
It is possible that getting certain STDs, such as chlamydia or gonorrhea, in the throat may not pose as great a threat to an infected person’s health as getting an STD in the genital area or rectum. Having these infections in the throat might increase the risk of getting HIV. Having gonorrhea in the throat also may lead to spread of the disease throughout the body. In addition:
- Having infections of chlamydia and gonorrhea in the throat may make it easier to spread these infections to others through oral sex. This is especially important for gonorrhea, since throat infections are harder to treat than urinary, genital or rectal infections.
- Infections from certain STDs, such as syphilis and HIV, spread throughout the body. Therefore, infections that are acquired in the throat may lead to the same health problems as infections acquired in the genitals or rectum.
- Mouth and throat infections by certain types of HPV may develop into oral or neck cancer.
What May Increase the Chances of Giving or Getting an STD through Oral Sex?
It is possible that certain factors may increase a person’s chances of getting HIV or other STDs during oral sex if exposed to an infected partner, such as:
- Having poor oral health which can include tooth decay, gum disease or bleeding gums, and oral cancer.
- Having sores in the mouth or on the genitals.
- Being exposed to the “pre-cum” or “cum” (also known as pre-ejaculate or ejaculate) of an infected partner.
However, no scientific studies have been done to show whether or not these factors actually do increase the risk of getting HIV or STDs from oral sex.
What Can You Do to Prevent STD Transmission During Oral Sex?
You can lower your chances of giving or getting STDs during oral sex by using a condom, dental dam or other barrier method each and every time you have oral sex.
For oral sex on the penis:
- Cover the penis with a non-lubricated latex condom.
- Use plastic (polyurethane) condoms if you or your partner is allergic to latex.
For oral sex on the vagina or anus:
- Use a dental dam.
- Cut open a condom to make a square, and put it between the mouth and the partner’s vagina or anus.
The only way to avoid STDs is to not have vaginal, anal, or oral sex.
If you are sexually active, you can do the following things to lower your chances of getting an STD:
- Being in a long-term mutually monogamous relationship with a partner who is not infected with an STD (e.g., a partner who has been tested and has negative STD test results).
- Using latex condoms the right way every time you have sex.
It’s important to remember that many infected individuals may be unaware of their infection because STDs often have no symptoms and are unrecognized.
If you are sexually active, you should get tested regularly for STDs and HIV and talk to your partner(s) about STDs. If you think you might have an STD, stop having sex and visit your doctor or clinic to get tested. There are free and low-cost options for testing in your area. It is important that you talk openly with your health care provider about any activities that might put you at risk for an STD, including oral sex.
What does genital herpes look like?
Most people who have genital herpes have no symptoms, or have very mild symptoms. You may not notice mild symptoms or you may mistake them for another skin condition, such as a pimple or ingrown hair. Because of this, most people who have herpes do not know it.
Herpes sores usually appear as one or more blisters on or around the genitals, rectum or mouth. The blisters break and leave painful sores that may take a week or more to heal. These symptoms are sometimes called “having an outbreak.” The first time someone has an outbreak they may also have flu-like symptoms such as fever, body aches, or swollen glands.
People who experience an initial outbreak of herpes can have repeated outbreaks, especially if they are infected with HSV-2. Repeat outbreaks are usually shorter and less severe than the first outbreak. Although the infection stays in the body for the rest of your life, the number of outbreaks may decrease over time.
You should be examined by your doctor if you notice any of these symptoms or if your partner has an STD or symptoms of an STD. STD symptoms can include an unusual sore, a smelly genital discharge, burning when urinating, or (for women) bleeding between periods.
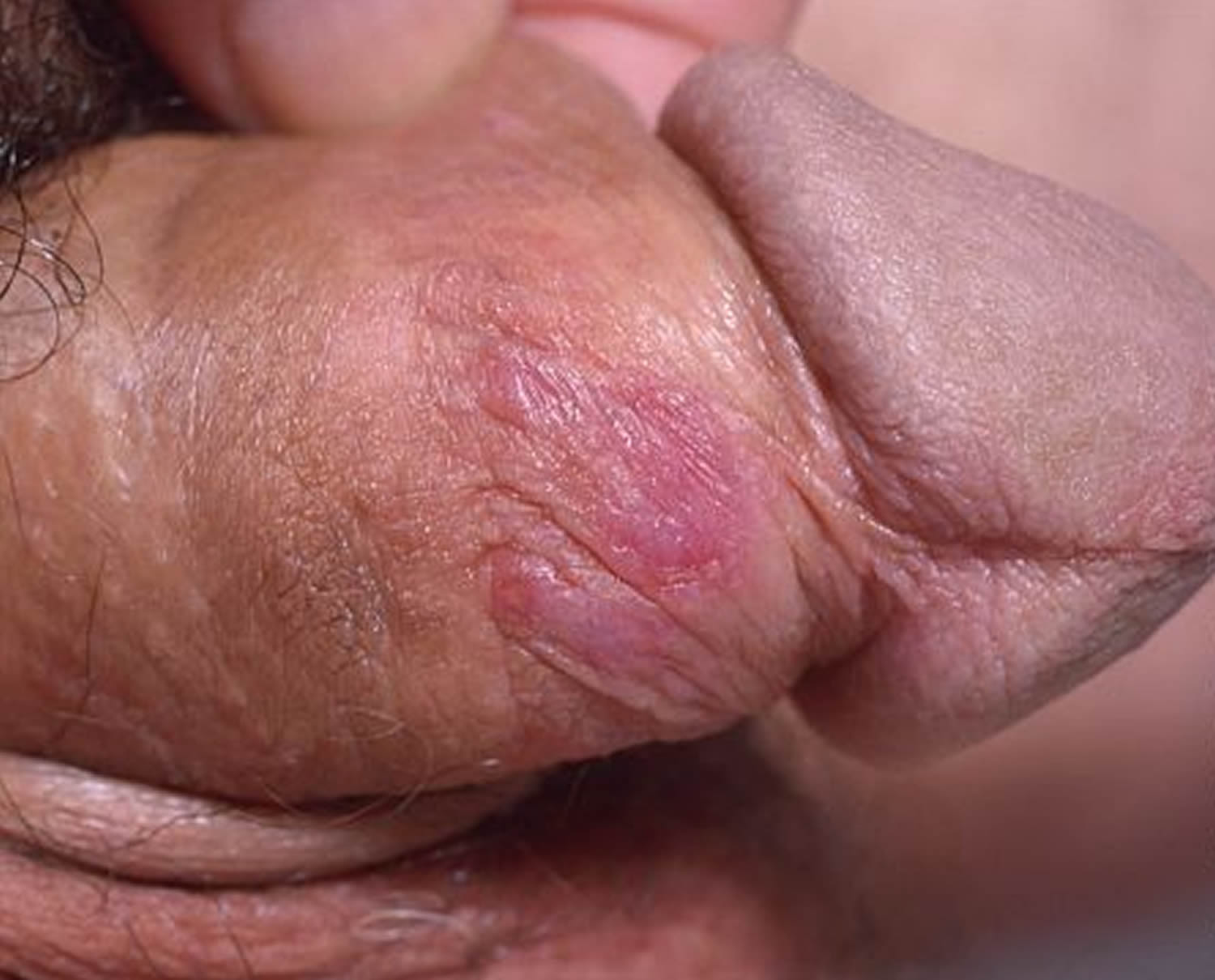
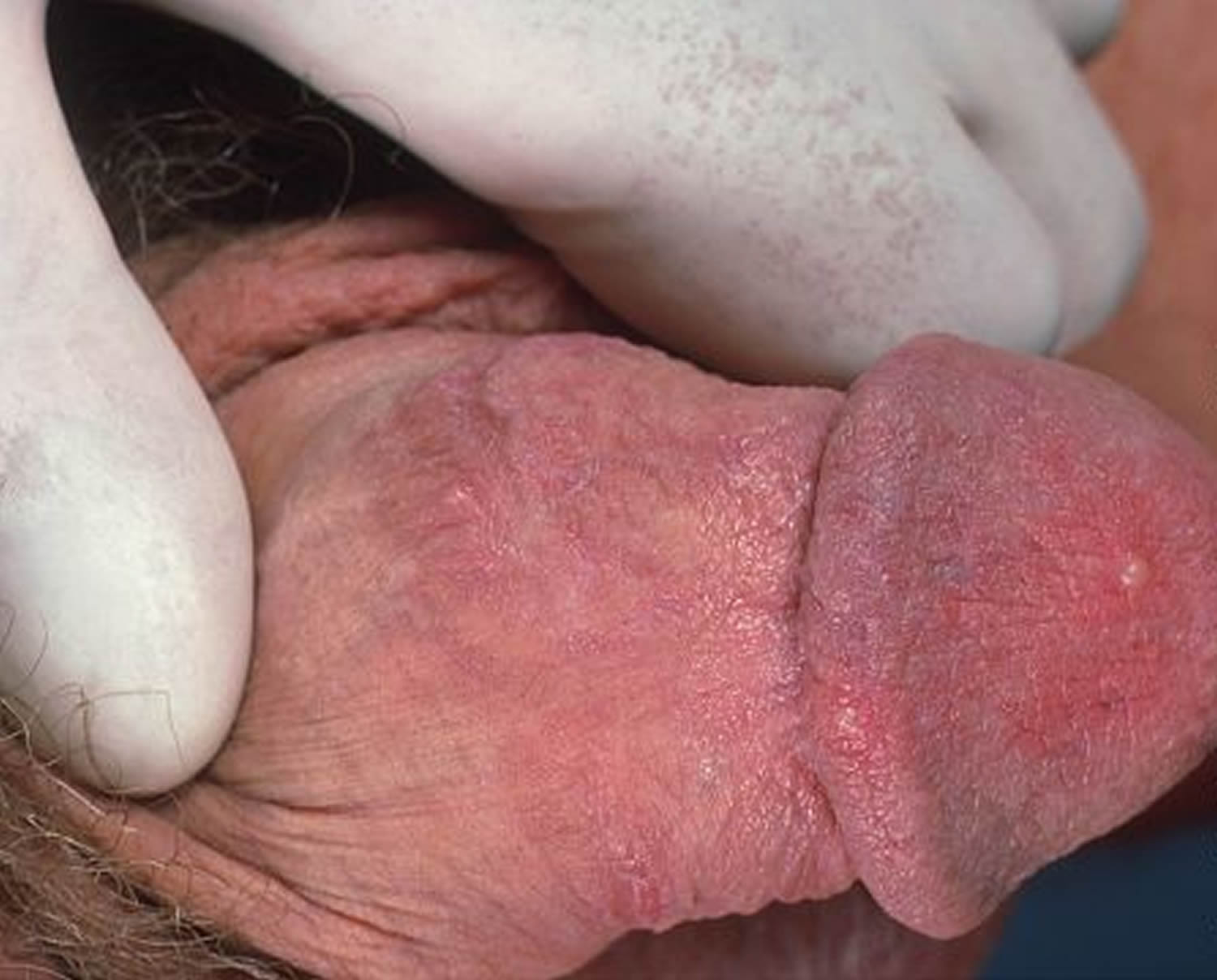
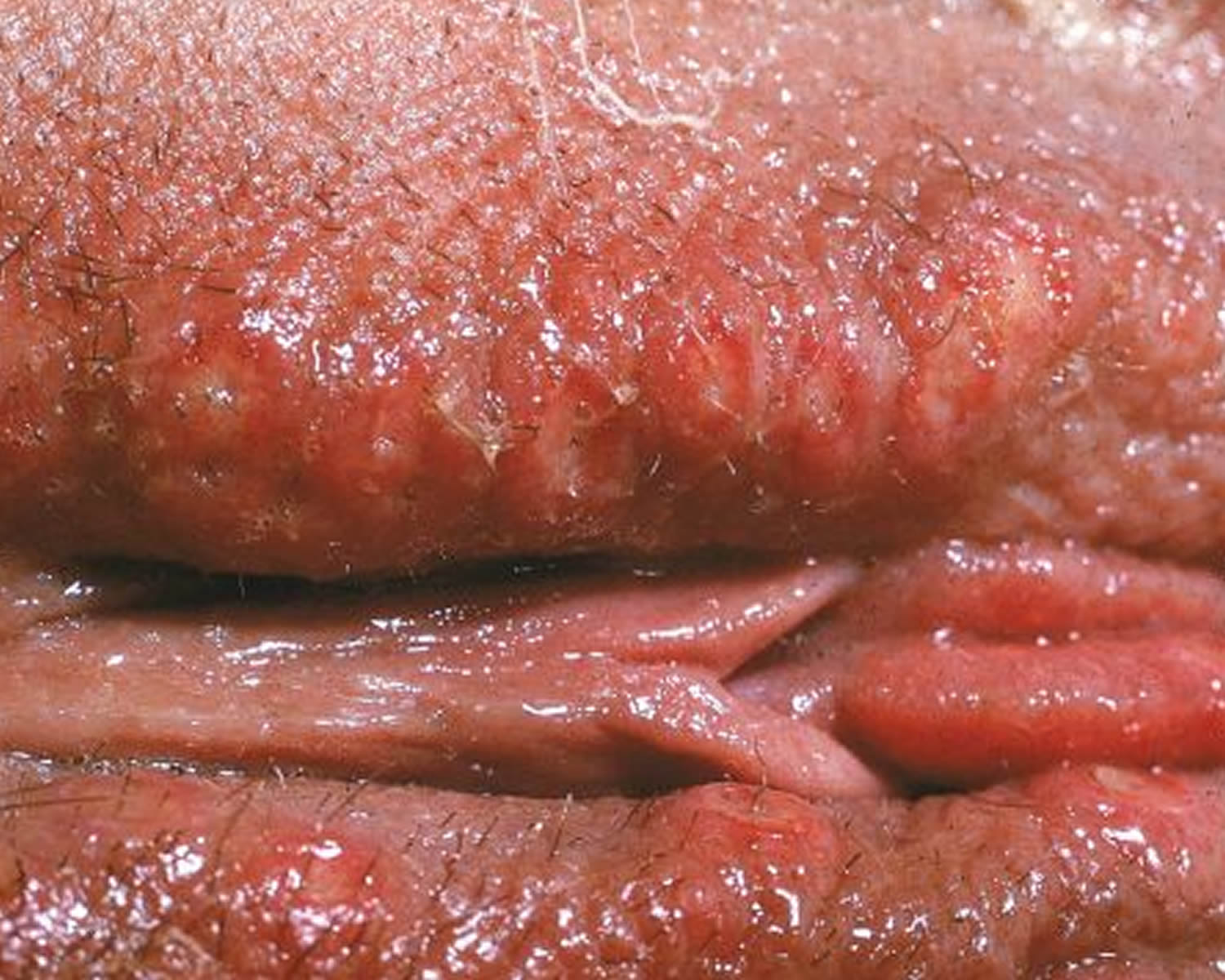
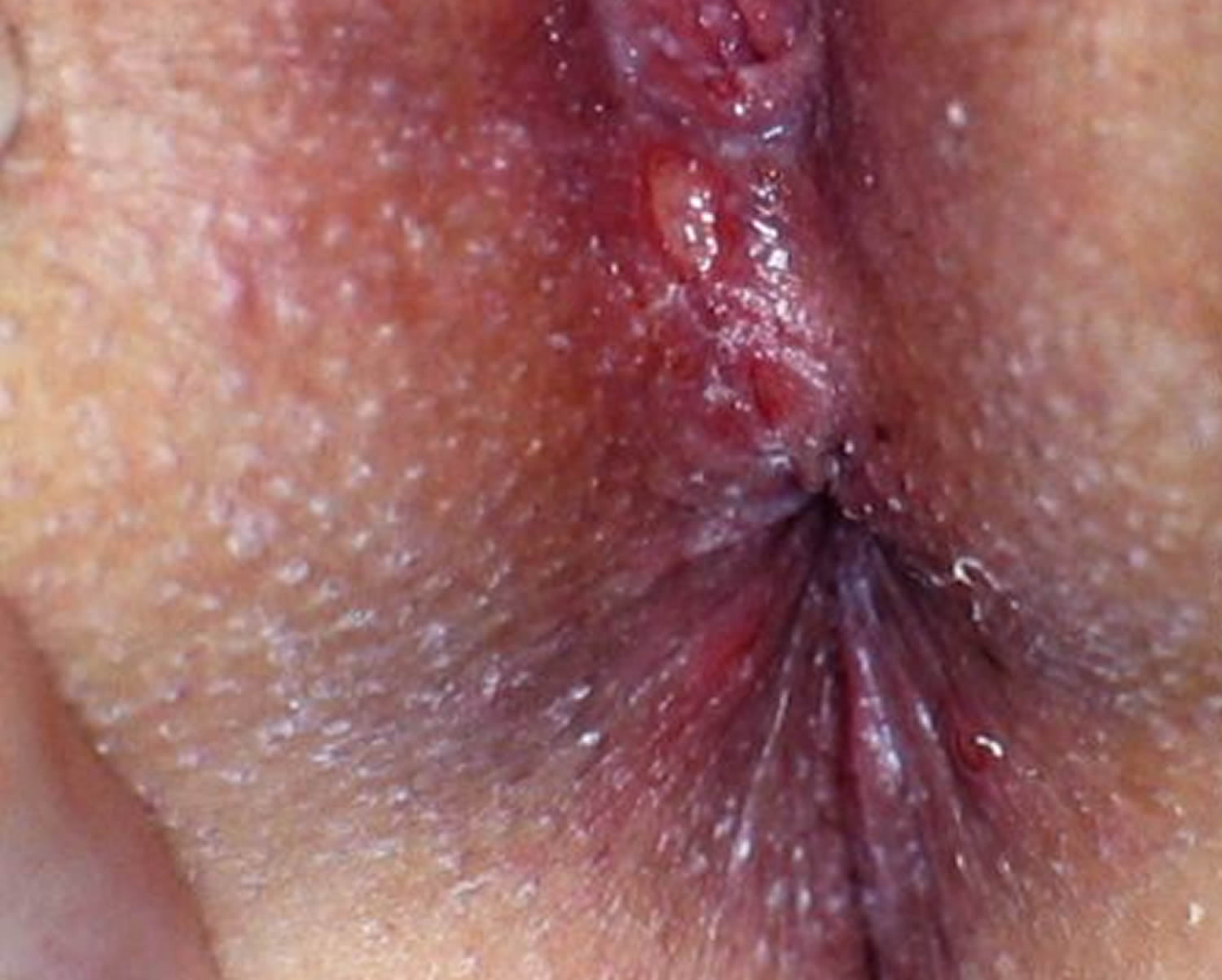
Figure 2. Male genital herpes
Figure 2. Female genital herpes
Genital herpes signs and symptoms
The symptoms of genital herpes can vary widely, depending upon whether you are having an initial or recurrent episode. However, many people infected with genital herpes never experience symptoms.
The first time a person has noticeable signs or symptoms of herpes may not be the initial episode. For example, it is possible to be infected for the first time, have few or no symptoms, and then have a recurrent outbreak with noticeable symptoms several years later. For this reason, it is often difficult to determine when the initial infection occurred, especially if a person has had more than one sexual partner. Thus, a current sexual partner may not be the source of the infection.
- Most people infected with HSV don’t know they have it because they don’t have any signs or symptoms or because their signs and symptoms are so mild.
When present, symptoms may begin about two to 12 days after exposure to the virus. If you experience symptoms of genital herpes, they may include:
- Pain or itching. You may experience pain and tenderness in your genital area until the infection clears.
- Small red bumps or tiny white blisters. These may appear a few days to a few weeks after infection.
- Ulcers. These may form when blisters rupture and ooze or bleed. Ulcers may make it painful to urinate.
- Scabs. Skin will crust over and form scabs as ulcers heal.
During an initial outbreak, you may have flu-like signs and symptoms such as swollen lymph nodes in your groin, headache, muscle aches and fever.
Differences in symptom location
Sores appear where the infection entered your body. You can spread the infection by touching a sore and then rubbing or scratching another area of your body, including your eyes.
Men and women can develop sores on the:
- Buttocks and thighs
- Anus
- Mouth
- Urethra (the tube that allows urine to drain from the bladder to the outside)
Women can also develop sores in or on the:
- Vaginal area
- External genitals
- Cervix
Men can also develop sores in or on the:
- Penis
- Scrotum
Genital herpes stages
The clinical manifestations of genital herpes vary significantly when comparing first clinical episode and recurrent outbreaks. The severity and frequency of clinical manifestations, and the recurrence rate, are influenced by viral type (HSV-1 versus HSV-2) and immune status of the host. Investigators have shown that strong HSV-specific T-cell responses during primary genital infection correlate with lower numbers of recurrences in subsequent years 22. Women tend to have more severe disease characterized by more systemic symptoms when compared with men 23, 24. The incubation period between HSV acquisition and onset of symptoms is, on average, 4 days (range 2 to 12 days). Reactivation induces viral replication and is precipitated by multiple known factors (trauma, fever, ultraviolet light, physical or emotional stress, immunosuppression, fatigue, menses, sexual intercourse) as well as unknown factors 23, 25. Herpes simplex virus causes a wide spectrum of disease depending on whether the infection is a primary, nonprimary (infection with HSV-1 or HSV-2 in an individual with preexisting antibodies to the other virus), or a recurrent episode.
First clinical episode
The first clinical episode refers to the initial symptomatic occurrence of genital herpes. The first clinical episode with HSV-1 or HSV-2 can occur (1) at the time of primary infection (absence of antibody to HSV-1 and HSV-2), (2) at the time of nonprimary infection (presence of HSV-1 or HSV-2 antibody with acquisition of the other viral type), or (3) with a symptomatic outbreak of HSV in a person with prior asymptomatic acquisition of the same viral type. Approximately 25% of patients who present with a first clinical episode of HSV-2 have a positive HSV-2 antibody test, consistent with previous unrecognized or asymptomatic acquisition of HSV-2 24.
Primary genital infection
Primary infection is defined as the first infection with either HSV-1 or HSV-2 with absence of antibodies to either HSV type. Primary genital infection is often symptomatic, but patients may have unrecognized or subclinical infection. For most people, the first herpes outbreak is the most severe, and symptoms tend to be more severe in women than men. The first outbreak usually occurs within a few weeks after infection with the virus. When a person is first infected with HSV, symptoms appear about 2–10 days after the virus enters the body. Symptoms tend to resolve within two to three weeks in the absence of antiviral therapy. Serum antibodies appear within 12 weeks of the primary infection in most persons 26. The following summarizes key features that may occur with primary HSV-1 or HSV-2 genital infection:
- Severe multiple bilateral genital ulcers, blisters, pain, itching, painful urination (dysuria), vaginal or urethral discharge, and tender inguinal lymph node (lymphadenopathy).
- For women, the sites most frequently involved include the vagina, vulva, buttocks, anus, and thighs; for men, the penis, scrotum, anus, buttocks and thighs may be affected. Signs and symptoms typically include blisters that become painful ulcers. Blisters on the penis or outer labia may crust over and heal. New lesions may develop for up to five to seven days after the first group appears.
- Without antiviral therapy, lesions last 2 to 3 weeks, with evolution of the lesions from vesicle pustule to wet ulcers to dry crusts 27
- The median duration of viral shedding is about 10 to 12 days and correlates with the time from the onset of vesicles to crusting of lesions 1
- Systemic symptoms (fever, muscle ache [myalgias], headaches, aseptic meningitis, or symptoms of autonomic nervous system dysfunction such as urinary retention) peak within 3 to 5 days of onset of lesions and gradually recede over the next 3 to 4 days 28.
- In women, HSV shedding from the cervix occurs in 80 to 90% of primary HSV-1 and HSV-2 infections 24. Cervicitis may involve the ectocervix or endocervix, with or without clinical symptoms. In most cases, the cervix appears abnormal to inspection with ulcerative lesions, erythema, or friability.
- Common manifestations of herpes proctitis include fever, pain, discharge, tenesmus, and constipation; some individuals will have severe anal ulcerations visible on anoscopy. In addition, some will develop symptoms of autonomic dysfunction, including difficulty urinating 29.
- Infection of the urethra and/or penile meatus may cause a clear mucoid discharge that may be mistaken for chlamydial or gonococcal urethritis 30.
The first outbreak of genital herpes may last 2–4 weeks. During this time, the sores break open and release fluid. Over a period of days, the sores become crusted and then heal without leaving scars.
There may also be tender, swollen lymph nodes in the groin, flu-like symptoms, such as joint pain, fever, and headache, and it may be painful to urinate.
A small percentage of people can develop headache, nausea and vomiting, or difficulty urinating. These symptoms occur when the herpes infection affects the nervous system.
People who have pain when they try to defecate may have proctitis (inflammation of the rectum or anus). Men who have sex with men are more prone to this complication than other patients.
Latent stage
After the initial outbreak, the virus travels to a bundle of nerves at the base of the spine, where it remains inactive for a period of time. This is called the latent stage. There are no symptoms during this stage.
Recurrent symptomatic infection
After a person is first infected, HSV stays in the body. It travels to nerve cells near the spine and stays there until something triggers it to become active again. When this happens, the virus then travels along the nerves, back to where it first entered the body, and causes a new outbreak of sores and blisters. This is called a recurrence. The virus can be passed to others during a recurrence.
Many people experience recurrent episodes of genital herpes, which occur when the virus travels through nerves to the skin’s surface, causing an outbreak of ulcers. These recurrent episodes tend to be milder than the initial outbreak symptoms that typically resolves within 3 to 5 days after onset. The time for lesions to heal is usually more rapid than with initial infection. The signs and symptoms of genital herpes may recur, off and on, for years. Some people experience numerous episodes each year. For many people, however, the outbreaks are less frequent as time passes.
The number of subsequent episodes of symptomatic infection is higher in women than in men and in persons who experience prolonged symptoms associated with primary infection 31, 32
Ulcers may develop in the same area as those of the first outbreak, or may appear in other areas. It is possible to develop lesions in areas where there was no direct contact; for example, it is possible to have lesions around the anus without having had anal sex.
Genital herpes recurs frequently in many patients, especially in those with HSV type 2. Over time, recurrences generally become less frequent and less severe. However, it is also possible to have a recurrence a few years after the initial HSV infection was acquired. This type of delayed herpes outbreak can be especially distressing if you never had symptoms during the initial infection, leading you to worry about the sexual activities of your past or present sexual partner(s).
Prodrome — As many as 50 percent of people with a recurrent outbreak experience mild symptoms before ulcers develop. These are called prodromal symptoms, and may include burning, itching, tingling, or pain in the buttocks, lower back, legs, or hips. Recurrences tend to become less frequent and less severe after the first year.
Triggers for recurrence — Illness, stress, sunlight, and fatigue can trigger recurrent herpes outbreaks. In women, menstrual periods may trigger an outbreak.
Genital herpes and pregnancy
Newborn infants can become infected with herpes virus during pregnancy, during labor or delivery, or after birth during the first 28 days after birth 33. Herpes type 2 virus (genital herpes) is the most common cause of herpes infection in newborn babies. But herpes type 1 virus (oral herpes) can also occur. Neonatal HSV infrequently occurs, with an estimated incidence of 1 in 3,000 deliveries 33, 34. In the United States, however, HSV-related neonatal deaths increased significantly between 1995 and 2017 35.
Newborn infants can become infected with herpes virus:
- In the uterus (this is unusual)
- Passing through the birth canal (birth-acquired herpes, the most common method of infection) also called intrapartum infection
- Right after birth (postpartum) from being kissed or having other contact with someone who has herpes mouth sores
The following five factors have been identified as the major influence for risk of transmission 36:
- Whether the HSV infection is primary or recurrent
- HSV antibody status of the pregnant person
- Duration of membrane rupture
- Integrity of mucocutaneous barrier (e.g. use of fetal scalp electrodes)
- Mode of the delivery (vaginal versus cesarean)
Approximately 85% of neonatal HSV infections result from intrapartum infection (a period from the onset of labor through delivery of the placenta), with the remaining cases involving HSV exposure and transmission during the intrauterine (in utero) or postpartum (postnatal) periods 36. The risk of intrapartum HSV transmission is highest among pregnant persons who newly acquire genital HSV-2 (or HSV-1) late in pregnancy when compared to women who have reactivation of genital HSV during pregnancy 33.
If the mother has an active outbreak of genital herpes at the time of delivery, the baby is more likely to become infected during birth. Some mothers may not know they have herpes sores inside their vagina.
The highest HSV transmission risk occurs when a pregnant person acquires HSV near the time of delivery 37, 38, 39. If a pregnant woman has primary genital HSV infection and is shedding HSV at the time of delivery, the risk of HSV transmission to the neonate is 10 to 30 times higher than if they are shedding HSV during a recurrent episode of genital herpes 36.
Some women have had herpes infections in the past, but are not aware of it, and may pass the virus to their baby.
If your baby has any symptoms of birth-acquired herpes, including skin blisters with no other symptoms, have the baby seen by your doctor right away.
It’s important to avoid getting herpes during pregnancy. If your partner has herpes and you don’t have it, be sure to always use condoms during sexual intercourse. Your partner could pass the infection to you even if they are not currently experiencing an outbreak. If there are visible sores, avoid having sex completely until the sores have healed.
If you’re pregnant and have genital herpes, or if you have ever had sex with someone who had it, tell her doctor. Your doctor will give you an antiviral medicine to start taking toward the end of your pregnancy. This will make it less likely that you will have an outbreak at or near the time you deliver your baby.
If you have an active genital herpes infection at or near the time of delivery, you can pass it to your baby. When the baby passes through the birth canal, it may come in contact with sores and become infected with the virus. This can cause brain damage, blindness, or even death in newborns.
If you do have an outbreak of genital herpes at the time of delivery, the American Academy of Obstetricians and Gynecologists and the American Academy of Pediatrics recommend performing a cesarean section or C-sectionr; ideally, the cesarean section should be performed before rupture of membranes 36, 40. With a C-section, the baby won’t go through the birth canal and be exposed to the virus. This lessens the risk of giving herpes to your baby.
The recommendation to perform cesarean section in this setting should be followed regardless of whether the HSV lesions are a result of recent HSV acquisition or reactivation of established HSV infection 41, 27. In addition, if possible, use of invasive monitoring during labor should be limited 41, 39. However, delivery by cesarean section does not completely eliminate the risk for HSV transmission to the infant 40, 42. Pregnant women with a history of recurrent HSV, but no symptoms or signs of genital herpes or prodromal symptoms, can give birth vaginally, regardless of whether they are taking prophylactic suppressive antiviral therapy.
Women with active genital herpes lesions near or at delivery
Women can have active HSV lesions at the time of delivery either through acquisition of HSV infection near delivery or reactivation of established HSV infection. The American Academy of Obstetricians and Gynecologists recommends cesarean section (ideally, before rupture of membranes) for any pregnant woman with active genital herpes lesions or prodromal symptoms at the time of delivery 40, 42. In addition, if possible, use of invasive monitors during delivery should be limited 39. Delivery by cesarean section does not completely eliminate the risk for HSV transmission to the infant 40. Most experts recommend that women with first-episode genital HSV infection near term should be managed in consultation with maternal-fetal medicine and infectious diseases specialists; for those women who acquire HSV in the third trimester, cesarean section may be offered 43. The initial management should include prompt antiviral treatment of the genital HSV infection.
Management of babies with herpes
Infants with HSV disease should be treated with parenteral acyclovir therapy in consultation with a pediatric infectious diseases specialist. Treatment duration is generally 14 days for SEM disease or 21 days for disseminated and central nervous system disease, and suppressive therapy after central nervous system disease may be indicated for up to 6 months; detailed guidelines are available for management of neonates who are delivered vaginally in the presence of maternal genital HSV lesions 41, 44. Despite improvement in outcomes with parenteral acyclovir and subsequent suppressive oral acyclovir therapy, neurodevelopmental outcomes remain poor in neonates with central nervous system herpes if present at birth 44, 45:
Recommended treatment regimen of neonatal herpes for infants with neonatal herpes limited to the skin and mucous membranes:
- Acyclovir 20 mg/kg body weight IV every 8 hours for 14 days
Recommended regimen for infants with neonatal herpes who have disseminated disease and disease involving the brain and spinal cord (CNS):
- Acyclovir 20 mg/kg body weight IV every 8 hours for 21 days
Genital herpes diagnosis
Your doctor usually can diagnose genital herpes based history of your sexual activity, a physical exam and the results of certain laboratory tests:
- Viral culture. This test involves taking a tissue sample or scraping of the sores for examination in the laboratory.
- Polymerase chain reaction (PCR) test also called nucleic acid amplification test (NAAT). PCR is used to copy your DNA from a sample of your blood, tissue from a sore or spinal fluid. The DNA can then be tested to establish the presence of HSV and determine which type of HSV you have.
- Antigen detection. The use of direct fluorescent antibody (DFA) testing offers lower sensitivity than viral culture or PCR and is not recommended 46.
- Cytologic examination: Cells infected with HSV will show characteristic changes, and these can be observed by obtaining a sample from the lesion and smearing it on a microscope slide (e.g. Tzanck smear). This test is not recommended due to low sensitivity (less than 80%) and lack of differentiation of HSV-1 from HSV-2.
- Blood test. This test analyzes a sample of your blood for the presence of HSV antibodies to detect a past herpes infection.
To confirm a diagnosis of genital herpes, your doctor will likely take a sample from an active sore. One or more tests of these samples are used to see if you have herpes simplex virus (HSV), infection and show whether the infection is HSV-1 or HSV-2.
Less often, a lab test of your blood may be used for confirming a diagnosis or ruling out other infections.
Your doctor will likely recommend that you get tested for other STDs. Your partner should also be tested for genital herpes and other STDs.
Genital herpes test
Because HSV-1 and HSV-2 infections are indistinguishable visually, suspected infection should be confirmed by type-specific testing to guide management 11, 3. In the presence of active lesions, nucleic acid amplification test (NAAT) is the preferred test, with sensitivity and specificity greater than 95% 3.
Two types of tests are recommended for detection of HSV in clinical samples: nucleic acid amplification test (NAAT) methods or viral culture. Among these tests, the nucleic acid amplification test (NAAT) is the preferred test for detecting HSV in clinical samples 41, 3. Regardless of which test is used, for all samples collected from a lesion, it is important to obtain an adequate quantity of cells by scraping the base of the lesion. Furthermore, if vesicles or pustules are present, they should be unroofed, and the base of the ulcer swabbed to obtain adequate cells for viral culture or polymerase chain reaction (PCR) 46. Using the fluid from a vesicular lesion for diagnostic purposes has low yield since HSV is an intracellular virus.
Nucleic Acid Amplification Tests (NAATs)
The nucleic acid amplification tests, such as polymerase chain reaction (PCR) test for HSV DNA, are the preferred methods of diagnosing HSV in clinical samples, primarily because of the very high sensitivity (90.9-100%) and high specificity with this technique 41, 47. When compared with culture, the sensitivity of HSV PCR is significantly higher. Most commercially available PCR assays can differentiate HSV-1 from HSV-2 infection 48, 49. For adults and children with suspected HSV central nervous system infection, PCR is the preferred test for detecting HSV in cerebrospinal fluid 50.
Viral culture
Prior to the availability of polymerase chain reaction (PCR) testing, viral culture was the gold standard for diagnosing HSV from a clinical specimen. Viral culture is highly specific, but sensitivity declines rapidly as lesions begin to heal. During primary infection, the yield for viral isolation is approximately 80% for early vesicles, 70% for ulcers, and 25% for crusted lesions 51. For recurrent HSV infection, HSV is isolated in only 25 to 50% of lesions 51. Isolates from culture can be typed as HSV-1 or HSV-2.
Type-specific serologic tests
Two types of HSV serologic tests are commercially available: type-common and type-specific 41. Type-specific serologic tests are based on antigens specific for HSV-1 (gG1) and HSV-2 (gG2), and these tests are preferred since they can distinguish antibodies to HSV-2 from antibodies to HSV-1 46. Type-common serologic tests do not distinguish HSV-2 from HSV-1. Because HSV-2 infections are usually sexually acquired, and HSV-2 only rarely causes oral disease, the presence of type-specific HSV-2 antibody nearly always indicates anogenital herpes infection 41. In contrast, the presence of HSV-1 antibody does not distinguish anogenital from orolabial HSV-1 infection. Antibodies to HSV develop during the first several weeks following infection and persist indefinitely. The type-specific assays commonly used in clinical practice are the enzyme-linked immunosorbent (ELISA) IgG assays and Western blot assays. The use of HSV IgM antibody assays is not recommended for the serodiagnosis of genital herpes since they have low sensitivity and specificity 41.
Genital herpes treatments
There’s no cure for genital herpes. Treatment with prescription antiviral medications may:
- Help sores heal sooner during an initial outbreak
- Lessen the severity and duration of symptoms in recurrent outbreaks
- Reduce the frequency of recurrence
- Minimize the chance of transmitting the herpes virus to another
Genital herpes anti-viral medications include 41, 3:
- Acyclovir (Zovirax) 400 mg orally 3 times/day for 7–10 days
- OR
- Valacyclovir (Valtrex) 1 gm orally 2 times/day for 7–10 days
- OR
- Famciclovir 250 mg orally 3 times/day for 7–10 days
* Treatment can be extended if healing is incomplete after 10 days of therapy.
Despite some evidence from animal models that early treatment may impact the long-term natural history of the infection, human trials have shown that oral acyclovir treatment of primary genital herpes does not influence the frequency of subsequent genital recurrences 52, 53.
These antiviral drugs will stop the herpes simplex virus multiplying once it reaches the skin or mucous membranes but cannot eradicate the virus from its resting stage within the nerve cells. They can therefore shorten and prevent episodes while the drug is being taken, but a single course cannot prevent future episodes.
Your doctor may prescribe anti-viral medication to help reduce the severity of genital herpes symptoms. This is most effective when started within 72 hours of the first symptoms.
If you have frequent or severe recurrent episodes there are medications available to help control them.
Other treatments being studied include:
- Imiquimod cream, an immune enhancer
- Human leukocyte interferon alpha cream.
Both appear less beneficial than conventional antiviral drugs.
Your doctor may recommend that you take the medicine only when you have symptoms of an outbreak or that you take a certain medication daily, even when you have no signs of an outbreak. These medications are usually well-tolerated, with few side effects.
- Different formulations of topical antiviral creams are available. They are not generally recommended for genital herpes.
Genital herpes treatment regimen
The dose and length of treatment depends upon whether the outbreak is the first episode or is a recurrence.
Initial episode
The first episode of genital herpes is generally treated with 7 to 10 days of one antiviral medication, taken by mouth.
Genital herpes anti-viral medications include 41, 3:
- Acyclovir (Zovirax) 400 mg orally 3 times/day for 7–10 days
- OR
- Valacyclovir (Valtrex) 1 gm orally 2 times/day for 7–10 days
- OR
- Famciclovir 250 mg orally 3 times/day for 7–10 days
* Treatment can be extended if healing is incomplete after 10 days of therapy.
Treatment of severe disease
Intravenous (IV) acyclovir should be provided for persons with severe HSV disease or complications requiring hospitalization (e.g. disseminated infection, pneumonitis, or hepatitis) or complications of the central nervous system (e.g. meningitis or encephalitis) 41. The recommended regimen is acyclovir 5 to 10 mg/kg intravenously every 8 hours for 2 to 7 days or until clinical improvement is observed, followed by oral antiviral therapy to complete at least 10 days of total therapy. Treatment of HSV encephalitis requires 21 days of intravenous therapy. Acyclovir dose adjustment is recommended for individuals with impaired kidney function.
Episodic therapy
Episodic therapy is a treatment strategy of taking antiviral medicines only when outbreaks occur as soon as prodromal symptoms present or within one day of lesion onset. Episodic therapy may be recommended if you have fewer than six outbreaks each year. Unfortunately, episodic treatment does not reduce the frequency of outbreaks. Persons with recurrent herpes ideally receive an antiviral prescription with instructions to self-initiate treatment promptly with the onset of prodromal symptoms that are consistent with genital herpes.
The advantage of episodic therapy is that it can decrease the duration and severity of the illness by hours to a few days.
Treatment is most likely to be effective if it is started within 72 hours of the first symptoms. People with a history of recurrent genital herpes are often advised to keep a supply of antiviral medication in their home, which they can initiate at the first signs of a recurrence (eg, pain or tingling symptoms or at the sign of their first blister).
Acyclovir, famciclovir, and valacyclovir are effective for episodic treatment of genital herpes, and clinical trials have established efficacy with multiple different dosing options.
Recommended episodic therapy regimens 41, 3, 54, 55, 56, 57, 58, 59:
- Acyclovir 800 mg orally twice a day for 5 days
- OR
- Acyclovir 800 mg orally three times a day for 2 days
- OR
- Famciclovir 1 g orally twice daily for 1 day
- OR
- Famciclovir 500 mg orally once, followed by 250 mg orally twice daily for 2 days
- OR
- Famciclovir 125 mg orally twice daily for 5 days
- OR
- Valacyclovir 500 mg orally twice a day for 3 days
- OR
- Valacyclovir 1 g orally once a day for 5 days
Suppressive therapy
Suppressive therapy is low dose antiviral treatment that is taken every day to prevent outbreaks. The advantage of suppressive therapy is that it decreases the frequency and duration of recurrences, and can reduce the risk of transmitting HSV to an uninfected sex partner. Suppressive therapy may be recommended if you have six or more recurrences each year or have a weakened immune system due to the human immunodeficiency virus (HIV), use of immune-suppressing drugs, or other factors. Suppressive therapy may also be an option if you are in a sexual relationship with a partner who does not have a history of genital herpes or antibodies to HSV-1 or 2 (as determined by blood testing). One study of valacyclovir showed that taking suppressive therapy can reduce the chances of transmitting the virus by approximately one-half.
Recommended suppressive therapy regimens 41:
- Acyclovir 400 mg orally twice a day
- OR
- Valacyclovir 500 mg orally once a day
- Note: Valacyclovir 500 mg once a day might be less effective than other valacyclovir or acyclovir dosing regimens in persons who have very frequent recurrences (i.e., ≥10 episodes per year).
- OR
- Valacyclovir 1 g orally once a day
- OR
- Famciclovir 250 mg orally twice a day
Persons with 10 or more recurrences per year may benefit from increased doses of valacyclovir (1 gram daily) to suppress genital herpes recurrences 41, 60. There is no evidence that long-term suppressive therapy in immunocompetent persons leads to antiviral resistance. Since frequency of recurrences may diminish over time, clinicians should periodically reassess the need for continued suppressive therapy. Suppressive therapy with valacyclovir (500 mg daily) also reduces transmission of HSV-2 to partners who are HSV-seronegative 61.
It is not clear how long suppressive therapy should continue. Some experts recommend taking a break from treatment periodically (every few years) to determine if suppressive therapy is still needed. If recurrent outbreaks develop, suppressive therapy may be restarted.
No treatment
It is not necessary to treat a recurrent episode of genital herpes. No treatment may be appropriate for some patients, particularly those with infrequent outbreaks or minimal symptoms. It also may be appropriate if the patient is not currently sexually active, so transmission of HSV is not a consideration.
Which treatment regimen is right for me?
Many people with recurrent herpes are unsure which treatment regimen (episodic or daily suppression) is right for them. The factors you should consider include how often you have outbreaks, how severe your symptoms are, and the risk of passing the infection to a sexual partner.
- If you have frequent outbreaks, severe symptoms, or want to avoid infecting a sexual partner, suppressive treatment might be recommended.
- If you do not have frequent outbreaks, are not bothered by symptoms (pain) during an outbreak, and are not concerned about infecting a sexual partner (because you are not sexually active), episodic therapy or no therapy are reasonable options.
Genital HSV in people with HIV
Antiviral therapy has been found to be safe and effective for episodic and suppressive therapy of genital herpes in persons with HIV 62, 63, 64. Since individuals with HIV may have severe, prolonged cases of orolabial, genital, and perianal HSV infections, the recommended episodic therapy options utilize higher doses and longer courses of antiviral medications 41. In persons with HIV, suppressive therapy with acyclovir, valacyclovir, or famciclovir is effective in decreasing HSV outbreaks 41, 65, 66. Unlike in HSV-2 serodifferent couples without HIV, in whom antiviral treatment significantly reduces HSV-2 transmission to the susceptible partner, treatment of persons with HIV-1 and HSV-2 coinfection with daily suppressive antiviral therapy does not reduce the transmission of HSV-2 to susceptible partners 61, 67. Persons with HIV who have a CD4 count less than 250 cells/mm3 have a significant increase in genital herpes outbreaks in the first 6 months after starting antiretroviral therapy; to prevent these outbreaks, some experts recommend suppressive therapy during this 6-month period 41.
Episodic therapy for recurrent genital herpes among people with HIV* 41:
- Acyclovir 400 mg orally three times a day for 5–10 days
- OR
- Famciclovir 500 mg orally twice a day for 5–10 days
- OR
- Valacyclovir 1 g orally twice a day for 5–10 days
Note: *For severe HSV disease, initiating therapy with acyclovir 5–10 mg/kg IV every 8 hours might be necessary.
Daily suppressive therapy among people with HIV 41:
- Acyclovir 400–800 mg orally two to three times a day
- OR
- Famciclovir 500 mg orally twice a day
- OR
- Valacyclovir 500 mg orally twice a day
Development of antiviral-resistant HSV is rare among immunocompetent persons, even those who take long-term HSV suppressive therapy 68. Most cases of antiviral-resistant HSV have occurred in severely immunocompromised individuals 69. Antiviral-resistant HSV most often results from absent or decreased production of viral thymidine kinase (TK-negative mutants) 70. The oral antiviral agents used to treat genital HSV—acyclovir, famciclovir, and valacyclovir—all require activation by HSV thymidine kinase and therefore are ineffective against TK-negative mutants. Foscarnet bypasses the thymidine kinase cascade and directly inhibits the viral DNA polymerase; it is highly effective against antiviral-resistant HSV 71, 72. Cidofovir does not require activation by viral thymidine kinase, and both intravenous and topical forms of this drug have been successfully used to treat antiviral-resistant HSV 73, 74. Topical imiquimod has also been effective in persons with HIV who have antiviral-resistant HSV-2 infections, but experience is limited 75, 76. The following list includes the options for treatment of antiviral-resistant genital HSV, but management should involve consultation with an infectious diseases specialist 41:
- Foscarnet: The treatment of choice for antiviral-resistant HSV is foscarnet 40-80 mg/kg body weight IV every 8 hours, until clinical resolution is attained. Foscarnet can potentially cause severe adverse effects, including nephrotoxicity and electrolyte disturbances.
- Cidofovir: 5 mg/kg body weight IV once weekly until clinical resolution is attained. Note that cidofovir can cause severe renal abnormalities.
- Imiquimod 5% cream: Apply to lesions and leave on for 8 hours 3 times per week until clinical resolution.
- Cidofovir 1% gel: Apply to lesions 2-4 times daily until clinical resolution is attained. This preparation is not commercially available and must be compounded by a pharmacist.
Home remedies for genital herpes
The symptoms can also be helped by:
- gently bathing the area with a warm salt solution (also called a sitz bath) (1 teaspoon to 2 cups water, or 1 cup of salt in a bath)
- pain medication, such as paracetamol or ibuprofen may also help relieve the pain of genital ulcers.
- local anesthetic ointment
- urinating while sitting in a warm bath, if urination is painful
- soaps and bubble baths should be avoided. It is important to keep the genital area clean and dry, and to avoid tight or irritating underwear and clothing.
- over-the-counter creams and ointments are generally not recommended.
Genital herpes prognosis
There is no cure for genital herpes, once you’re infected, you have the virus for the rest of your life 77. Early identification of symptoms, and prompt institution of pharmacotherapy can lead to early suppression of viral replication. Abstinence during known viral shedding can decrease the risk of transmission to a seronegative partner. The herpes viruses as a family are responsible for significant neurological morbidity, and unfortunately, HSV-2 persists in the seropositive individual for a lifetime 77.
- Schiffer JT, Corey L. New concepts in understanding genital herpes. Curr Infect Dis Rep. 2009 Nov;11(6):457-64. doi: 10.1007/s11908-009-0066-7[↩][↩]
- Genital Herpes – CDC Detailed Fact Sheet. https://www.cdc.gov/std/herpes/stdfact-herpes-detailed.htm[↩][↩]
- Genital Herpes. https://www.cdc.gov/std/treatment-guidelines/herpes.htm[↩][↩][↩][↩][↩][↩][↩]
- Gnann JW Jr, Whitley RJ. CLINICAL PRACTICE. Genital Herpes. N Engl J Med. 2016 Aug 18;375(7):666-74. doi: 10.1056/NEJMcp1603178[↩]
- Spicknall IH, Flagg EW, Torrone EA. Estimates of the Prevalence and Incidence of Genital Herpes, United States, 2018. Sex Transm Dis. 2021 Apr 1;48(4):260-265. doi: 10.1097/OLQ.0000000000001375[↩][↩][↩]
- Centers for Disease Control and Prevention Public Health Image Library. Dr. Fred Murphy & Sylvia Whitfield, 1975.[↩]
- Ryder N, Jin F, McNulty AM, Grulich AE, Donovan B. Increasing role of herpes simplex virus type 1 in first-episode anogenital herpes in heterosexual women and younger men who have sex with men, 1992-2006. Sex Transm Infect. 2009 Oct;85(6):416-9. doi: 10.1136/sti.2008.033902[↩]
- Roberts CM, Pfister JR, Spear SJ. Increasing proportion of herpes simplex virus type 1 as a cause of genital herpes infection in college students. Sex Transm Dis. 2003 Oct;30(10):797-800. doi: 10.1097/01.OLQ.0000092387.58746.C7[↩][↩]
- James M. Sizemore, Jr, Fred Lakeman, Richard Whitley, Annalee Hughes, Edward W. Hook III, The Spectrum of Genital Herpes Simplex Virus Infection in Men Attending a Sexually Transmitted Disease Clinic, The Journal of Infectious Diseases, Volume 193, Issue 7, 1 April 2006, Pages 905–911, https://doi.org/10.1086/500841[↩]
- Heather Bradley, Lauri E. Markowitz, Theda Gibson, Geraldine M. McQuillan, Seroprevalence of Herpes Simplex Virus Types 1 and 2—United States, 1999–2010, The Journal of Infectious Diseases, Volume 209, Issue 3, 1 February 2014, Pages 325–333, https://doi.org/10.1093/infdis/jit458[↩][↩][↩]
- Bernstein DI, Bellamy AR, Hook EW 3rd, Levin MJ, Wald A, Ewell MG, Wolff PA, Deal CD, Heineman TC, Dubin G, Belshe RB. Epidemiology, clinical presentation, and antibody response to primary infection with herpes simplex virus type 1 and type 2 in young women. Clin Infect Dis. 2013 Feb;56(3):344-51. doi: 10.1093/cid/cis891[↩][↩]
- Cherpes TL, Meyn LA, Hillier SL. Cunnilingus and vaginal intercourse are risk factors for herpes simplex virus type 1 acquisition in women. Sex Transm Dis. 2005 Feb;32(2):84-9. doi: 10.1097/01.olq.0000151414.64297.46[↩]
- William E. Lafferty, Lois Downey, Connie Celum, Anna Wald, Herpes Simplex Virus Type 1 as a Cause of Genital Herpes: Impact on Surveillance and Prevention, The Journal of Infectious Diseases, Volume 181, Issue 4, April 2000, Pages 1454–1457, https://doi.org/10.1086/315395[↩]
- Gregory J. Mertz, Asymptomatic Shedding of Herpes Simplex Virus 1 and 2: Implications for Prevention of Transmission, The Journal of Infectious Diseases, Volume 198, Issue 8, 15 October 2008, Pages 1098–1100, https://doi.org/10.1086/591914[↩]
- Mertz GJ, Benedetti J, Ashley R, Selke SA, Corey L. Risk factors for the sexual transmission of genital herpes. Ann Intern Med. 1992 Feb 1;116(3):197-202. doi: 10.7326/0003-4819-116-3-197[↩]
- Mertz GJ, Schmidt O, Jourden JL, Guinan ME, Remington ML, Fahnlander A, Winter C, Holmes KK, Corey L. Frequency of acquisition of first-episode genital infection with herpes simplex virus from symptomatic and asymptomatic source contacts. Sex Transm Dis. 1985 Jan-Mar;12(1):33-9. doi: 10.1097/00007435-198501000-00007[↩]
- Ribes JA, Steele AD, Seabolt JP, Baker DJ. Six-year study of the incidence of herpes in genital and nongenital cultures in a central Kentucky medical center patient population. J Clin Microbiol. 2001 Sep;39(9):3321-5. doi: 10.1128/JCM.39.9.3321-3325.2001[↩]
- Freeman EE, Weiss HA, Glynn JR, Cross PL, Whitworth JA, Hayes RJ. Herpes simplex virus 2 infection increases HIV acquisition in men and women: systematic review and meta-analysis of longitudinal studies. AIDS. 2006 Jan 2;20(1):73-83. doi: 10.1097/01.aids.0000198081.09337.a7[↩]
- Corey L. Synergistic copathogens–HIV-1 and HSV-2. N Engl J Med. 2007 Feb 22;356(8):854-6. doi: 10.1056/NEJMe068302. Erratum in: N Engl J Med. 2007 Apr 5;356(14):1487.[↩]
- Leeyaphan C, Surawan TM, Chirachanakul P, Prasertworonun N, Punyaratabandhu P, Omcharoen V, Jiamton S. Clinical characteristics of hypertrophic herpes simplex genitalis and treatment outcomes of imiquimod: a retrospective observational study. Int J Infect Dis. 2015 Apr;33:165-70. doi: 10.1016/j.ijid.2015.02.002[↩]
- Tan DH, Kaul R, Walsmley S. Left out but not forgotten: Should closer attention be paid to coinfection with herpes simplex virus type 1 and HIV? Can J Infect Dis Med Microbiol. 2009 Spring;20(1):e1-7. doi: 10.1155/2009/965263[↩]
- Franzen-Röhl E, Schepis D, Atterfelt F, Franck K, Wikström A, Liljeqvist JÅ, Bergström T, Aurelius E, Kärre K, Berg L, Gaines H. Herpes simplex virus specific T cell response in a cohort with primary genital infection correlates inversely with frequency of subsequent recurrences. Sex Transm Infect. 2017 May;93(3):169-174. doi: 10.1136/sextrans-2016-052811[↩]
- Genital Herpes: A Review. Am Fam Physician. 2016;93(11):928-934. https://www.aafp.org/pubs/afp/issues/2016/0601/p928.html[↩][↩]
- Corey L, Adams HG, Brown ZA, Holmes KK. Genital herpes simplex virus infections: clinical manifestations, course, and complications. Ann Intern Med. 1983 Jun;98(6):958-72. doi: 10.7326/0003-4819-98-6-958[↩][↩][↩]
- Erin E. Horn, MA, Eric Turkheimer, PhD, Eric Strachan, PhD, Psychological Distress, Emotional Stability, and Emotion Regulation Moderate Dynamics of Herpes Simplex Virus Type 2 Recurrence, Annals of Behavioral Medicine, Volume 49, Issue 2, April 2015, Pages 187–198, https://doi.org/10.1007/s12160-014-9640-9[↩]
- Ashley-Morrow R, Krantz E, Wald A. Time course of seroconversion by HerpeSelect ELISA after acquisition of genital herpes simplex virus type 1 (HSV-1) or HSV-2. Sex Transm Dis. 2003 Apr;30(4):310-4. doi: 10.1097/00007435-200304000-00007[↩]
- Kimberlin DW, Rouse DJ. Clinical practice. Genital herpes. N Engl J Med. 2004 May 6;350(19):1970-7. doi: 10.1056/NEJMcp023065[↩][↩]
- Christine Johnston, Amalia Magaret, Stacy Selke, Michael Remington, Lawrence Corey, Anna Wald, Herpes Simplex Virus Viremia during Primary Genital Infection, The Journal of Infectious Diseases, Volume 198, Issue 1, 1 July 2008, Pages 31–34, https://doi.org/10.1086/588676[↩]
- Goodell SE, Quinn TC, Mkrtichian E, Schuffler MD, Holmes KK, Corey L. Herpes simplex virus proctitis in homosexual men. Clinical, sigmoidoscopic, and histopathological features. N Engl J Med. 1983 Apr 14;308(15):868-71. doi: 10.1056/NEJM198304143081503[↩]
- Ong JJ, Morton AN, Henzell HR, Berzins K, Druce J, Fairley CK, Bradshaw CS, Read TR, Hocking JS, Chen MY. Clinical Characteristics of Herpes Simplex Virus Urethritis Compared With Chlamydial Urethritis Among Men. Sex Transm Dis. 2017 Feb;44(2):121-125. doi: 10.1097/OLQ.0000000000000547[↩]
- Engelberg R, Carrell D, Krantz E, Corey L, Wald A. Natural history of genital herpes simplex virus type 1 infection. Sex Transm Dis. 2003 Feb;30(2):174-7. doi: 10.1097/00007435-200302000-00015[↩]
- Benedetti J, Corey L, Ashley R. Recurrence rates in genital herpes after symptomatic first-episode infection. Ann Intern Med. 1994 Dec 1;121(11):847-54. doi: 10.7326/0003-4819-121-11-199412010-00004[↩]
- Corey L, Wald A. Maternal and neonatal herpes simplex virus infections. N Engl J Med. 2009 Oct 1;361(14):1376-85. doi: 10.1056/NEJMra0807633. Erratum in: N Engl J Med. 2009 Dec 31;361(27):2681. https://www.ncbi.nlm.nih.gov/pmc/articles/PMC2780322[↩][↩][↩]
- Matthias J, du Bernard S, Schillinger JA, Hong J, Pearson V, Peterman TA. Estimating Neonatal Herpes Simplex Virus Incidence and Mortality Using Capture-recapture, Florida. Clin Infect Dis. 2021 Aug 2;73(3):506-512. doi: 10.1093/cid/ciaa727[↩]
- Slutsker JS, Schillinger JA. Assessing the Burden of Infant Deaths Due to Herpes Simplex Virus, Human Immunodeficiency Virus, and Congenital Syphilis: United States, 1995 to 2017. Sex Transm Dis. 2021 Aug 1;48(8S):S4-S10. doi: 10.1097/OLQ.0000000000001458[↩]
- Kimberlin DW, Baley J; Committee on Infectious Diseases; Committee on Fetus and Newborn. Guidance on management of asymptomatic neonates born to women with active genital herpes lesions. Pediatrics. 2013 Feb;131(2):383-6. doi: 10.1542/peds.2012-3217[↩][↩][↩][↩]
- Pinninti SG, Kimberlin DW. Maternal and neonatal herpes simplex virus infections. Am J Perinatol. 2013 Feb;30(2):113-9. doi: 10.1055/s-0032-1332802[↩]
- Brown ZA, Selke S, Zeh J, Kopelman J, Maslow A, Ashley RL, Watts DH, Berry S, Herd M, Corey L. The acquisition of herpes simplex virus during pregnancy. N Engl J Med. 1997 Aug 21;337(8):509-15. doi: 10.1056/NEJM199708213370801[↩]
- Brown ZA, Wald A, Morrow RA, Selke S, Zeh J, Corey L. Effect of serologic status and cesarean delivery on transmission rates of herpes simplex virus from mother to infant. JAMA. 2003 Jan 8;289(2):203-9. doi: 10.1001/jama.289.2.203[↩][↩][↩]
- ACOG Committee on Practice Bulletins. ACOG Practice Bulletin. Clinical management guidelines for obstetrician-gynecologists. No. 82 June 2007. Management of herpes in pregnancy. Obstet Gynecol. 2007 Jun;109(6):1489-98. doi: 10.1097/01.aog.0000263902.31953.3e[↩][↩][↩][↩]
- Workowski KA, Bachmann LH, Chan PA, Johnston CM, Muzny CA, Park I, Reno H, Zenilman JM, Bolan GA. Sexually Transmitted Infections Treatment Guidelines, 2021. MMWR Recomm Rep. 2021 Jul 23;70(4):1-187. doi: 10.15585/mmwr.rr7004a1[↩][↩][↩][↩][↩][↩][↩][↩][↩][↩][↩][↩][↩][↩][↩][↩][↩][↩][↩][↩]
- Roberts SW, Cox SM, Dax J, Wendel GD Jr, Leveno KJ. Genital herpes during pregnancy: no lesions, no cesarean. Obstet Gynecol. 1995 Feb;85(2):261-4. doi: 10.1016/0029-7844(94)00346-F[↩][↩]
- Management of Genital Herpes in Pregnancy: ACOG Practice Bulletin Summary, Number 220. Obstet Gynecol. 2020 May;135(5):1236-1238. doi: 10.1097/AOG.0000000000003841[↩]
- Kimberlin DW, Whitley RJ, Wan W, Powell DA, Storch G, Ahmed A, Palmer A, Sánchez PJ, Jacobs RF, Bradley JS, Robinson JL, Shelton M, Dennehy PH, Leach C, Rathore M, Abughali N, Wright P, Frenkel LM, Brady RC, Van Dyke R, Weiner LB, Guzman-Cottrill J, McCarthy CA, Griffin J, Jester P, Parker M, Lakeman FD, Kuo H, Lee CH, Cloud GA; National Institute of Allergy and Infectious Diseases Collaborative Antiviral Study Group. Oral acyclovir suppression and neurodevelopment after neonatal herpes. N Engl J Med. 2011 Oct 6;365(14):1284-92. doi: 10.1056/NEJMoa1003509[↩][↩]
- James SH, Kimberlin DW. Neonatal herpes simplex virus infection: epidemiology and treatment. Clin Perinatol. 2015 Mar;42(1):47-59, viii. doi: 10.1016/j.clp.2014.10.005[↩]
- Johnston C, Corey L. Current Concepts for Genital Herpes Simplex Virus Infection: Diagnostics and Pathogenesis of Genital Tract Shedding. Clin Microbiol Rev. 2016 Jan;29(1):149-61. doi: 10.1128/CMR.00043-15[↩][↩][↩]
- Teo JW, Chiang D, Jureen R, Lin RT. Clinical evaluation of a helicase-dependant amplification (HDA)-based commercial assay for the simultaneous detection of HSV-1 and HSV-2. Diagn Microbiol Infect Dis. 2015 Nov;83(3):261-2. doi: 10.1016/j.diagmicrobio.2015.07.018[↩]
- Van Der Pol B, Warren T, Taylor SN, Martens M, Jerome KR, Mena L, Lebed J, Ginde S, Fine P, Hook EW 3rd. Type-specific identification of anogenital herpes simplex virus infections by use of a commercially available nucleic acid amplification test. J Clin Microbiol. 2012 Nov;50(11):3466-71. doi: 10.1128/JCM.01685-12[↩]
- Anna Wald, Meei-Li Huang, David Carrell, Stacy Selke, Lawrence Corey, Polymerase Chain Reaction for Detection of Herpes Simplex Virus (HSV) DNA on Mucosal Surfaces: Comparison with HSV Isolation in Cell Culture, The Journal of Infectious Diseases, Volume 188, Issue 9, 1 November 2003, Pages 1345–1351, https://doi.org/10.1086/379043[↩]
- Tyler KL. Herpes simplex virus infections of the central nervous system: encephalitis and meningitis, including Mollaret’s. Herpes. 2004 Jun;11 Suppl 2:57A-64A.[↩]
- LeGoff J, Péré H, Bélec L. Diagnosis of genital herpes simplex virus infection in the clinical laboratory. Virol J. 2014 May 12;11:83. doi: 10.1186/1743-422X-11-83. Erratum in: Virol J. 2015;12:167.[↩][↩]
- Efstathiou S, Field HJ, Griffiths PD, Kern ER, Sacks SL, Sawtell NM, Stanberry LR. Herpes simplex virus latency and nucleoside analogues. Antiviral Res. 1999 Apr;41(3):85-100. doi: 10.1016/s0166-3542(99)00003-0[↩]
- Simmons A, Field HJ. Can HSV latency be conquered by current antiviral therapies? Sex Transm Infect. 1998 Feb;74(1):1-2.[↩]
- Fife KH, Barbarash RA, Rudolph T, Degregorio B, Roth R. Valaciclovir versus acyclovir in the treatment of first-episode genital herpes infection. Results of an international, multicenter, double-blind, randomized clinical trial. The Valaciclovir International Herpes Simplex Virus Study Group. Sex Transm Dis. 1997 Sep;24(8):481-6. doi: 10.1097/00007435-199709000-00007[↩]
- Wald Anna, Carrell David, Remington Michael, Kexel Elizabeth, Zeh Judy, Corey Lawrence, Two-Day Regimen of Acyclovir for Treatment of Recurrent Genital Herpes Simplex Virus Type 2 Infection, Clinical Infectious Diseases, Volume 34, Issue 7, 1 April 2002, Pages 944–948, https://doi.org/10.1086/339325[↩]
- Bartlett BL, Tyring SK, Fife K, Gnann JW Jr, Hadala JT, Kianifard F, Berber E. Famciclovir treatment options for patients with frequent outbreaks of recurrent genital herpes: the RELIEF trial. J Clin Virol. 2008 Oct;43(2):190-5. doi: 10.1016/j.jcv.2008.06.004. Epub 2008 Jul 14. Erratum in: J Clin Virol. 2009 Feb;44(2):183.[↩]
- Wald A, Carrell D, Remington M, Kexel E, Zeh J, Corey L. Two-day regimen of acyclovir for treatment of recurrent genital herpes simplex virus type 2 infection. Clin Infect Dis. 2002 Apr 1;34(7):944-8. doi: 10.1086/339325[↩]
- Bodsworth NJ, Crooks RJ, Borelli S, Vejlsgaard G, Paavonen J, Worm AM, Uexkull N, Esmann J, Strand A, Ingamells AJ, Gibb A. Valaciclovir versus aciclovir in patient initiated treatment of recurrent genital herpes: a randomised, double blind clinical trial. International Valaciclovir HSV Study Group. Genitourin Med. 1997 Apr;73(2):110-6. doi: 10.1136/sti.73.2.110[↩]
- Chosidow O, Drouault Y, Leconte-Veyriac F, Aymard M, Ortonne JP, Pouget F, Revuz J, Decazes JM, Malkin JE. Famciclovir vs. aciclovir in immunocompetent patients with recurrent genital herpes infections: a parallel-groups, randomized, double-blind clinical trial. Br J Dermatol. 2001 Apr;144(4):818-24. doi: 10.1046/j.1365-2133.2001.04139.x[↩]
- M. Reitano, S. Tyring, W. Lang, C. Thoming, A.-M. Worm, S. Borelli, L. O. Chambers, J. M. Robinson, L. Corey, Valaciclovir for the Suppression of Recurrent Genital Herpes Simplex Virus Infection: A Large-Scale Dose Range-Finding Study, The Journal of Infectious Diseases, Volume 178, Issue 3, September 1998, Pages 603–610, https://doi.org/10.1086/515385[↩]
- Corey L, Wald A, Patel R, Sacks SL, Tyring SK, Warren T, Douglas JM Jr, Paavonen J, Morrow RA, Beutner KR, Stratchounsky LS, Mertz G, Keene ON, Watson HA, Tait D, Vargas-Cortes M; Valacyclovir HSV Transmission Study Group. Once-daily valacyclovir to reduce the risk of transmission of genital herpes. N Engl J Med. 2004 Jan 1;350(1):11-20. doi: 10.1056/NEJMoa035144[↩][↩]
- Romanowski B, Aoki FY, Martel AY, Lavender EA, Parsons JE, Saltzman RL. Efficacy and safety of famciclovir for treating mucocutaneous herpes simplex infection in HIV-infected individuals. Collaborative Famciclovir HIV Study Group. AIDS. 2000 Jun 16;14(9):1211-7. doi: 10.1097/00002030-200006160-00019[↩]
- Lara B. Strick, Anna Wald, Connie Celum, Management of Herpes Simplex Virus Type 2 Infection in HIV Type 1–Infected Persons, Clinical Infectious Diseases, Volume 43, Issue 3, 1 August 2006, Pages 347–356, https://doi.org/10.1086/505496[↩]
- Conant MA, Schacker TW, Murphy RL, Gold J, Crutchfield LT, Crooks RJ; International Valaciclovir HSV Study Group. Valaciclovir versus aciclovir for herpes simplex virus infection in HIV-infected individuals: two randomized trials. Int J STD AIDS. 2002 Jan;13(1):12-21. doi: 10.1258/0956462021924550[↩]
- Schacker T, Hu HL, Koelle DM, Zeh J, Saltzman R, Boon R, Shaughnessy M, Barnum G, Corey L. Famciclovir for the suppression of symptomatic and asymptomatic herpes simplex virus reactivation in HIV-infected persons. A double-blind, placebo-controlled trial. Ann Intern Med. 1998 Jan 1;128(1):21-8. doi: 10.7326/0003-4819-128-1-199801010-00004[↩]
- Edwin DeJesus, Anna Wald, Terri Warren, Timothy W. Schacker, Sylvie Trottier, Mohsen Shahmanesh, Joanne L. Hill, for The Valacyclovir International HSV Study Group, Valacyclovir for the Suppression of Recurrent Genital Herpes in Human Immunodeficiency Virus–Infected Subjects, The Journal of Infectious Diseases, Volume 188, Issue 7, 1 October 2003, Pages 1009–1016, https://doi.org/10.1086[↩]
- Mujugira A, Magaret AS, Celum C, Baeten JM, Lingappa JR, Morrow RA, Fife KH, Delany-Moretlwe S, de Bruyn G, Bukusi EA, Karita E, Kapiga S, Corey L, Wald A; Partners in Prevention HSV/HIV Transmission Study Team. Daily acyclovir to decrease herpes simplex virus type 2 (HSV-2) transmission from HSV-2/HIV-1 coinfected persons: a randomized controlled trial. J Infect Dis. 2013 Nov 1;208(9):1366-74. doi: 10.1093/infdis/jit333[↩]
- Reyes M, Shaik NS, Graber JM, Nisenbaum R, Wetherall NT, Fukuda K, Reeves WC; Task Force on Herpes Simplex Virus Resistance. Acyclovir-resistant genital herpes among persons attending sexually transmitted disease and human immunodeficiency virus clinics. Arch Intern Med. 2003 Jan 13;163(1):76-80. doi: 10.1001/archinte.163.1.76[↩]
- Myron J. Levin, Teresa H. Bacon, Jeffry J. Leary, Resistance of Herpes Simplex Virus Infections to Nucleoside Analogues in HIV-Infected Patients, Clinical Infectious Diseases, Volume 39, Issue Supplement_5, November 2004, Pages S248–S257, https://doi.org/10.1086/422364[↩]
- Piret J, Boivin G. Resistance of herpes simplex viruses to nucleoside analogues: mechanisms, prevalence, and management. Antimicrob Agents Chemother. 2011 Feb;55(2):459-72. doi: 10.1128/AAC.00615-10[↩]
- Sauerbrei A, Deinhardt S, Zell R, Wutzler P. Phenotypic and genotypic characterization of acyclovir-resistant clinical isolates of herpes simplex virus. Antiviral Res. 2010 Jun;86(3):246-52. doi: 10.1016/j.antiviral.2010.03.002[↩]
- Sharon Safrin, Tania Assaykeen, Stephen Follansbee, John Mills, Foscarnet Therapy for Acyclovir-ResistantMucocutaneous Herpes Simplex Virus Infection in 26 AIDS Patients: Preliminary Data, The Journal of Infectious Diseases, Volume 161, Issue 6, June 1990, Pages 1078–1084, https://doi.org/10.1093/infdis/161.6.1078[↩]
- McElhiney LF Pharmd Rph. Topical cidofovir for treatment of resistant viral infections. Int J Pharm Compd. 2006 Sep-Oct;10(5):324-8.[↩]
- T. Kopp, A. Geusau, A. Rieger, G. Stingl, Successful treatment of an aciclovir‐resistant herpes simplex type 2 infection with cidofovir in an AIDS patient, British Journal of Dermatology, Volume 147, Issue 1, 1 July 2002, Pages 134–138, https://doi.org/10.1046/j.1365-2133.2002.04747.x[↩]
- Perkins N, Nisbet M, Thomas M. Topical imiquimod treatment of aciclovir-resistant herpes simplex disease: case series and literature review. Sex Transm Infect. 2011 Jun;87(4):292-5. doi: 10.1136/sti.2010.047431[↩]
- Lascaux, A.-S., Caumes, E., Deback, C., Melica, G., Challine, D., Agut, H. and Lévy, Y. (2012), Successful treatment of aciclovir and foscarnet resistant Herpes simplex virus lesions with topical imiquimod in patients infected with human immunodeficiency virus type 1. J. Med. Virol., 84: 194-197. https://doi.org/10.1002/jmv.23188[↩]
- Mathew Jr J, Sapra A. Herpes Simplex Type 2. [Updated 2022 Aug 8]. In: StatPearls [Internet]. Treasure Island (FL): StatPearls Publishing; 2023 Jan-. Available from: https://www.ncbi.nlm.nih.gov/books/NBK554427[↩][↩]