Contents
How to stop bleeding gums
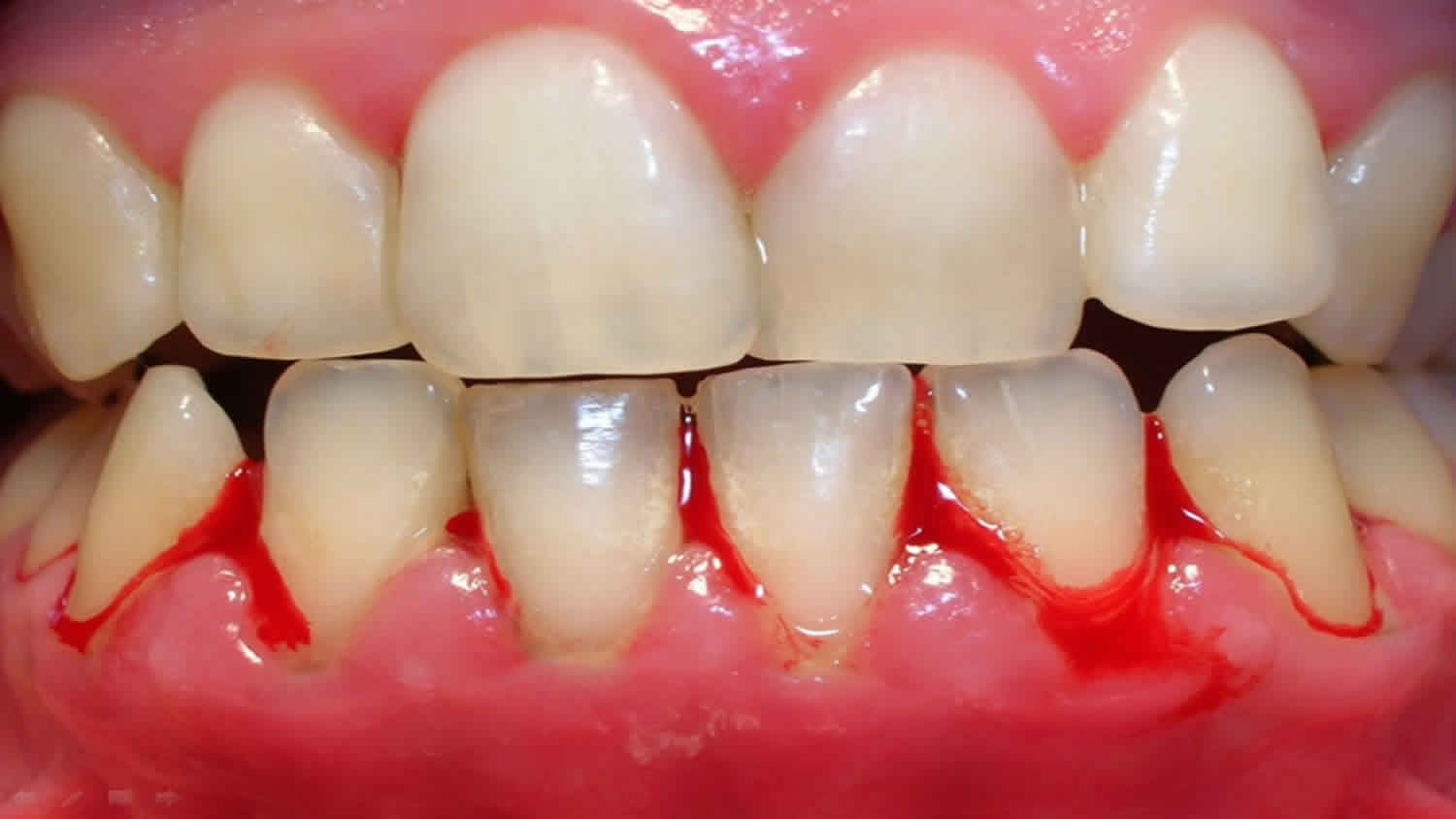
Bleeding gums can be a symptom of gingivitis, a mild form of gum disease, or more serious gum disease known as periodontitis. If your gums are bleeding after you have brushed or flossed your teeth, it could be a sign of gum diseases and you might need to pay more attention to your dental care. Gum disease occurs when the tissue that surrounds and supports your teeth becomes infected. The symptoms of gum disease include inflammation, redness, bleeding, bad breath and sponginess of the gums. Brushing your teeth and gums twice daily can help prevent gum disease. Healthy gums are firm and pale pink and fitted tightly around the teeth.
Other things can cause bleeding from the gums. It is quite common in people taking aspirin or other drugs, such as warfarin (a blood thinner), which ‘thin’ the blood. Other medicines may indirectly cause bleeding gums.
Some viral or bacterial infections may cause bleeding gums and also some systemic conditions like lupus erythematosus.
Bleeding when brushing your teeth should never be regarded as normal, any more than bleeding from the scalp with hair brushing should be.
Facts on gum disease:
- Gum disease affects gums, bone and the tissues supporting your teeth.
- If plaque is not brushed from your teeth and gums and is allowed to build up, signs of gum disease may appear.
- Plaque is a sticky colorless film of bacteria that builds up on teeth, mainly near the gum line and between the teeth where it’s difficult to clean. If plaque is not brushed off, the bacteria combines with food to produce acids. This acid starts the decay process and irritates gums.
- The longer plaque is allowed to build up, the more gums become irritated.
- Avoiding brushing in these areas makes the condition worse.
- Gentle brushing to remove plaque also massages gums and helps with the healing process.
- The mildest form of gum disease is called gingivitis. Symptoms include inflammation of the gums, redness, swelling and some bleeding. Bad breath, a bad taste in your mouth and gums that feel soft or spongy are also signs of gum disease.
- Gingivitis is reversible and can heal, leaving no permanent damage.
- If plaque is allowed to build up, it eventually hardens and calcifies. This is called calculus or tartar and results in further irritation to gums.
- Calculus can only be removed by a dental professional.
There are 2 main types of gum disease:
- Gingivitis and
- Periodontitis.
Gingivitis
Gingivitis is a common and mild form of gum disease (periodontal disease) that causes irritation, redness and swelling (inflammation) of your gingiva, the part of your gum around the base of your teeth. The gums may also bleed easily when they are brushed. Bad breath is another sign of gum disease.
The most common cause of gingivitis is poor oral hygiene. Good oral health habits, such as brushing at least twice a day, flossing daily and getting regular dental checkups, can help prevent and reverse gingivitis.
It’s important to take gingivitis seriously and treat it promptly. Gingivitis can lead to much more serious gum disease called periodontitis and tooth loss.
If gingivitis is not treated, the inflammation may spread to the bone supporting the teeth to cause a more severe form of gum disease called periodontitis. Periodontitis may cause the area of the gum closest to the tooth to become weak. Spaces may form between the tooth and the gum, and these may trap germs, leading to even more swelling. Over time, the bone supporting the teeth can be lost, causing the teeth to become loose and possibly fall out.
Four different types of chronic gingivitis are described, depending on the predisposing factors:
- Plaque-induced gingivitis. This gingivitis occurs as a result of infection caused by the presence of dental plaque.
- Gingivitis modified by systemic factors. These would include puberty-associated gingivitis, menstrual cycle-associated gingivitis, pregnancy-associated gingivitis, diabetes-associated gingivitis and gingivitis associated with leukemia.
- Gingivitis modified by medications. These include drug-influenced gingival enlargement and drug-induced gingivitis, like oral contraceptive-associated gingivitis and drug-induced gingival overgrowth due to phenytoin or cyclosporin.
- Gingivitis modified by malnutrition. These include gingivitis due to vitamin C deficiency (scurvy) or protein deficiency. Acute necrotisinig ulcerative gingivitis is also known as Vincent’s gingivitis, Vincent’s gingivostomatitis, ulceromembraneous gingivitis, or trench mouth.
Signs and symptoms of gingivitis include:
- Swollen or puffy gums
- Dusky red or dark red gums
- Gums that bleed easily when you brush or floss
- Bad breath
- Receding gums
- Tender gums
The good news is that gingivitis can be reversed. You might think it is best to stop brushing if your gums are red or puffy. Try to keep brushing, as this will get rid of the bacteria and plaque that are causing the problem. Soon the gums should look and feel better. If not, see your dentist or oral health professional.
To prevent gum disease, gently brush your teeth and gums twice a day with a fluoridated toothpaste. Even if it causes bleeding, brush twice a day.
You should also visit your dentist regularly for a check-up and cleaning.
Periodontitis
Periodontitis is an advanced stage of gum disease that may occur if gingivitis is not treated.
The periodontium is the name given to the group of structures that surround and support the teeth, keeping them in place. Periodontitis is the inflammation of the periodontium, caused by the bacteria in plaque and the body’s immune response to it.
The structures affected by periodontitis include the covering of the tooth root (cementum), the bone and the fibres that connect the tooth root to the bone (periodontal ligament).
When the gum is weakened by gum disease, spaces can form between the tooth root and the gum. These spaces are called ‘periodontal pockets’. Bacteria get trapped in these pockets and cause even more damage to the periodontium. Over time, bone is damaged and lost, and larger spaces begin to form between the tooth and the gum.
If periodontitis is not treated, the structures that hold the tooth firmly into the gum can become so damaged that teeth become loose and may need to be removed.
Smoking and poorly managed diabetes are risk factors for periodontitis.
Signs of periodontitis include:
- bleeding gums
- swollen gums
- receding gums (the gum line shrinks away from the tooth making teeth look longer)
- bad breath
- a bad taste in the mouth
- tenderness when biting
- loose teeth, or teeth that have moved
Make an appointment with your dentist or oral health professional if you think you have any of these signs. They can talk with you about how to care for your teeth. They can also professionally remove plaque and hardened plaque (calculus). Early treatment of periodontitis can save affected teeth.
You should see a dentist regularly for check-ups. See your dentist as soon as possible if you have swollen or bleeding gums, or if your teeth feel loose.
- If you notice any signs and symptoms of gingivitis, schedule an appointment with your dentist. The sooner you seek care, the better your chances of reversing damage from gingivitis and preventing its progression to periodontitis.
Home remedies for bleeding gums
The advice below may help for mild gum disease:
- Brush your teeth twice a day – once in the morning and once just before bedtime. Better yet, brush after every meal or snack or as your dentist recommends. Flossing before you brush allows you to clean away the loosened food particles and bacteria.
- Use dental floss regularly – your dentist or pharmacist will be able to advise you about this.
- Brush all the plaque away from your teeth, between your teeth and around your gum line.
- Use a small soft toothbrush and a pea size amount of adult fluoride toothpaste. Spit the toothpaste out but don’t rinse.
- Don’t avoid brushing areas, even if they bleed.
- If your gums are sore, use a soft toothbrush.
- Antibacterial mouthwashes (available from your pharmacist) may also help. Talk to your dentist or pharmacist first, as sometimes medical mouthwashes can cause side effects.
- Don’t smoke or chew tobacco.
- If you think you might have gum disease (gingivitis), it’s important to see a dentist, as getting treatment early can help protect your teeth.
Bleeding after dental treatment or injury
If you start to bleed after dental treatment, or injury to your mouth or teeth, the advice below may help:
- Apply pressure over the area with a pad made from a clean, rolled up, cotton handkerchief or other clean cloth that has been slightly dampened with clean water.
- Keep this pad in place for 15 minutes without removing it. Check to see if the bleeding has stopped. If not, repeat the process and keep the pad in place until you are seen by a dentist.
- If you are in pain, get advice on pain relief medicines you can take.
- Avoid strenuous activity.
- Avoid very hot food and drinks.
- If you smoke, try to cut down or quit as it may irritate your mouth.
Follow any advice you received from your dentist about rinsing your mouth and eating and drinking after dental procedures.
Can gum disease be cured?
Gingivitis can be cured without permanent damage. Try to keep brushing and flossing, as this will get rid of the bacteria and plaque that are causing the problem. Soon the gums should look and feel better. If not, see your dentist or oral health professional.
Periodontitis can’t be cured, but it can be controlled. The bone loss may be very slow or stopped.
Bleeding gums causes
Gum disease is usually caused by a build-up of plaque on teeth and along the gum line. Plaque is a sticky coating containing bacteria that builds up on teeth. Your immune system tries to get rid of plaque with an inflammation response. This is seen by the redness and swelling of the gum around the tooth. Plaque irritates the gums, causing them to bleed easily. If the plaque is not brushed off, it can become hard and further irritate the gums. Hardened plaque is called calculus or tartar. It can only be removed by a dental health professional.
Everybody has a range of bacteria in their mouth. Plaque is constantly being formed by some of these bacteria when they feed on the sugars in the foods and drinks you consume. Plaque provides the perfect environment for the bacteria that can cause gum disease to live and multiply.
Here’s how plaque can lead to gingivitis:
- Plaque forms on your teeth. Plaque is an invisible, sticky film composed mainly of bacteria that forms on your teeth when starches and sugars in food interact with bacteria normally found in your mouth. Plaque requires daily removal because it re-forms quickly.
- Plaque turns into tartar. Plaque that stays on your teeth can harden under your gumline into tartar (calculus), which collects bacteria. Tartar makes plaque more difficult to remove, creates a protective shield for bacteria and causes irritation along the gumline. You need professional dental cleaning to remove tartar.
- Gingiva become inflamed (gingivitis). The longer that plaque and tartar remain on your teeth, the more they irritate the gingiva, the part of your gum around the base of your teeth, causing inflammation. In time, your gums become swollen and bleed easily. Tooth decay (dental caries) also may result. If not treated, gingivitis can advance to periodontitis and eventual tooth loss.
Risk factors for gum disease
Gingivitis is common, and anyone can develop it. Factors that can increase your risk of gingivitis include:
- Poor oral care habits
- Smoking or chewing tobacco
- Older age
- Dry mouth
- Poor nutrition, including vitamin C deficiency
- Dental restorations that don’t fit properly or crooked teeth that are difficult to clean
- Conditions that decrease immunity such as leukemia, HIV/AIDS or cancer treatment
- Certain drugs, such as phenytoin (Dilantin, Phenytek) for epileptic seizures, and some calcium channel blockers, used for angina, high blood pressure and other conditions
- Hormonal changes, such as those related to pregnancy, menstrual cycle or use of birth control pills
- Genetics
- Medical conditions such as certain viral and fungal infections
Gum disease prevention
Regular tooth brushing helps to prevent gum disease by removing the plaque that causes it. Remember to:
- Brush your teeth and along the gum line twice a day – in the morning and before going to bed. Better yet, brush after every meal or snack or as your dentist recommends. Flossing before you brush allows you to clean away the loosened food particles and bacteria.
- Use a toothbrush with a small head and soft bristles and fluoride toothpaste
- Use floss, interdental brushes, or another tool recommended by an oral health professional to clean in between teeth.
- Have a dental check-up, see your dentist regularly. See your dentist or dental hygienist regularly for cleanings, usually every six to 12 months. If you have risk factors that increase your chance of developing periodontitis — such as having dry mouth, taking certain medications or smoking — you may need professional cleaning more often. Annual dental X-rays can help identify diseases that are not seen by a visual dental examination and monitor for changes in your dental health.
Plaque can easily build up on dentures, increasing the risk for tooth decay. Dentures need to be cleaned well twice a day with a soft toothbrush and mild liquid soap to keep gums healthy.
Other things that can help to prevent gum disease:
- Avoiding sugary foods and drinks, especially between meals
- Drinking plenty of water (fluoridated where possible)
- Quitting smoking
- For people with diabetes, keeping blood sugar levels well-controlled will help to reduce the risk of gum disease.
Gum disease complications
Untreated gingivitis can progress to gum disease that spreads to underlying tissue and bone (periodontitis), a much more serious condition that can lead to tooth loss.
Chronic gingiva inflammation has been thought to be associated with some systemic diseases such as respiratory disease, diabetes, coronary artery disease, stroke and rheumatoid arthritis. Some research suggests that the bacteria responsible for periodontitis can enter your bloodstream through gum tissue, possibly affecting your heart, lungs and other parts of your body. But more studies are needed to confirm a link.
Trench mouth, also known as necrotizing ulcerative gingivitis, is a severe form of gingivitis that causes painful, infected, bleeding gums and ulcerations. Trench mouth is rare today in developed nations, though it’s common in developing countries that have poor nutrition and poor living conditions.
Gum disease diagnosis
Your dentist will examine your teeth and may need to take x-rays. They will probably clean all the plaque and tartar from your teeth and advise you on how to clean your teeth well. You may also need the roots of your teeth treated to get rid of the germs.
Dentists usually diagnose gingivitis based on:
- Review of your dental and medical history and conditions that may contribute to your symptoms.
- Examination of your teeth, gums, mouth and tongue for signs of plaque and inflammation.
- Measuring the pocket depth of the groove between your gums and your teeth by inserting a dental probe beside your tooth beneath your gum line, usually at several sites throughout your mouth. In a healthy mouth, the pocket depth is usually between 1 and 3 millimeters (mm). Pockets deeper than 4 mm may indicate gum disease.
- Dental X-rays to check for bone loss in areas where your dentist sees deeper pockets.
- Other tests as needed. If it’s not clear what has caused your gingivitis, your dentist may recommend that you get a medical evaluation to check for underlying health conditions. If your gum disease is advanced, your dentist may refer you to a specialist in gum diseases (periodontist).
Bleeding gums treatment
Prompt treatment usually reverses symptoms of gingivitis and prevents its progression to more serious gum disease and tooth loss. You have the best chance for successful treatment when you also adopt a daily routine of good oral care and stop tobacco use.
Professional gingivitis care includes:
- Professional dental cleaning. Your initial professional cleaning will include removing all traces of plaque, tartar and bacterial products — a procedure known as scaling and root planing. Scaling removes tartar and bacteria from your tooth surfaces and beneath your gums. Root planning removes the bacterial products produced by inflammation, smooths the root surfaces, discouraging further buildup of tartar and bacteria, and allows proper healing. The procedure may be performed using instruments, a laser or an ultrasonic device.
- Dental restoration, if needed. Misaligned teeth or poorly fitting crowns, bridges or other dental restorations may irritate your gums and make it harder to remove plaque during daily oral care. If problems with your teeth or dental restorations contribute to your gingivitis, your dentist may recommend fixing these problems.
- Ongoing care. Gingivitis usually clears up after a thorough professional cleaning — as long as you continue good oral hygiene at home. Your dentist will help you plan an effective at-home program and a schedule of regular professional checkups and cleaning.
If you’re consistent with your home oral hygiene, you should see the return of pink, healthy gum tissue within days or weeks.