Contents
What is milia
Milia are multiple small skin cysts or tiny white bumps containing keratin (skin protein that forms hair, nail and dead skin cells). Milia are formed when flakes of keratin get trapped just below the skin’s surface. Milia are harmless cysts present as tiny pearly-white bumps just under the surface of the skin. Milia appear as 1–2 mm white-to-yellow, dome-shaped bumps that are not painful or itchy.
Milia are almost always seen in newborn babies, especially on the nose and are sometimes called “baby acne”, but that is incorrect since milia are NOT a true from of acne. Milia can also affect children and adults, with one type of milia causing pearly bumps around the eyes.
Milia are common in all ages and both sexes. They most often arise on the face, and are particularly prominent on the eyelids and cheeks, but they may occur elsewhere.
Milia usually don’t need treatment as they are harmless and usually go away by themselves.
There is no known prevention for milia.
Who’s at risk of developing milia
Milia can occur in people of all ages, of any ethnicity, and of either sex.
Milia can be categorized as either primary or secondary. Primary milia are formed directly from entrapped keratin and are usually found on the faces of infants and adults. Milia are so common in newborn babies (occurring in up to 50% of them) that they are considered normal.
Secondary milia are also tiny cysts and look similar, but these develop after something clogs the ducts leading to the skin surface, such as after an injury, burn, or blistering of the skin. Secondary milia may appear in affected skin of people with the following:
- Blistering skin conditions, such as bullous pemphigoid, epidermolysis bullosa, and porphyria cutanea tarda
- Burns
- Blistering injury to skin, such as poison ivy
- Following skin resurfacing procedures such as dermabrasion or laser resurfacing
- Following long-term use of steroid creams
- Chronic sun damage
The most common locations for secondary milia include:
- Anywhere on the body where another skin condition exists, particularly on the backs of the hands
- On the faces of people who have had a lot of damage from sun exposure
Symptoms may include:
- Whitish, pearly bump in the skin of newborns
- Bumps that appear across the cheeks, nose, and chin
- Whitish, pearly bump on gums or roof of mouth (they may look like teeth coming through the gums)
In children, no treatment is needed. Skin changes on the face or cysts in the mouth often go away after the first few weeks of life without treatment. There are no lasting effects.
Adults may have milia removed to improve their appearance.
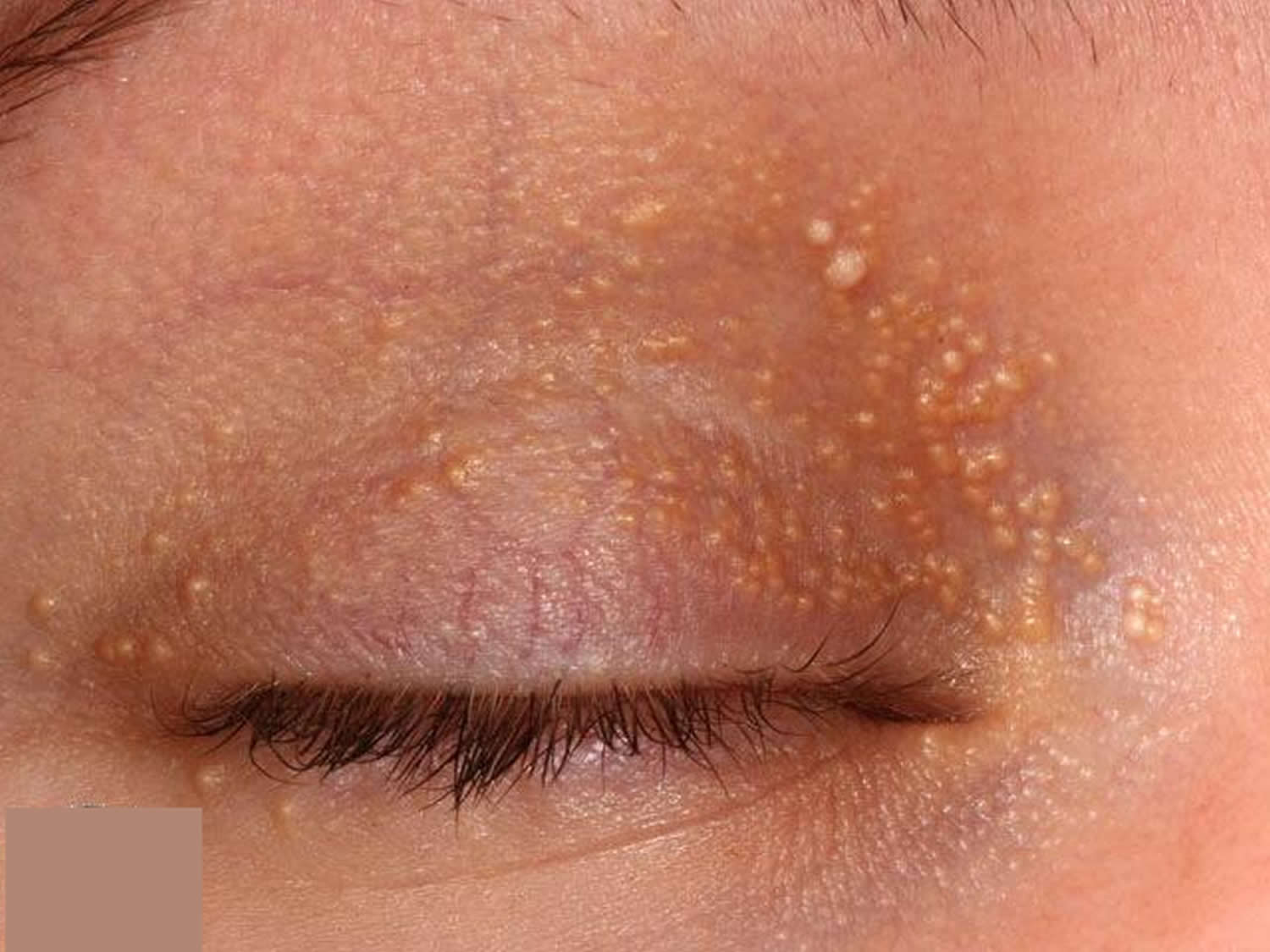
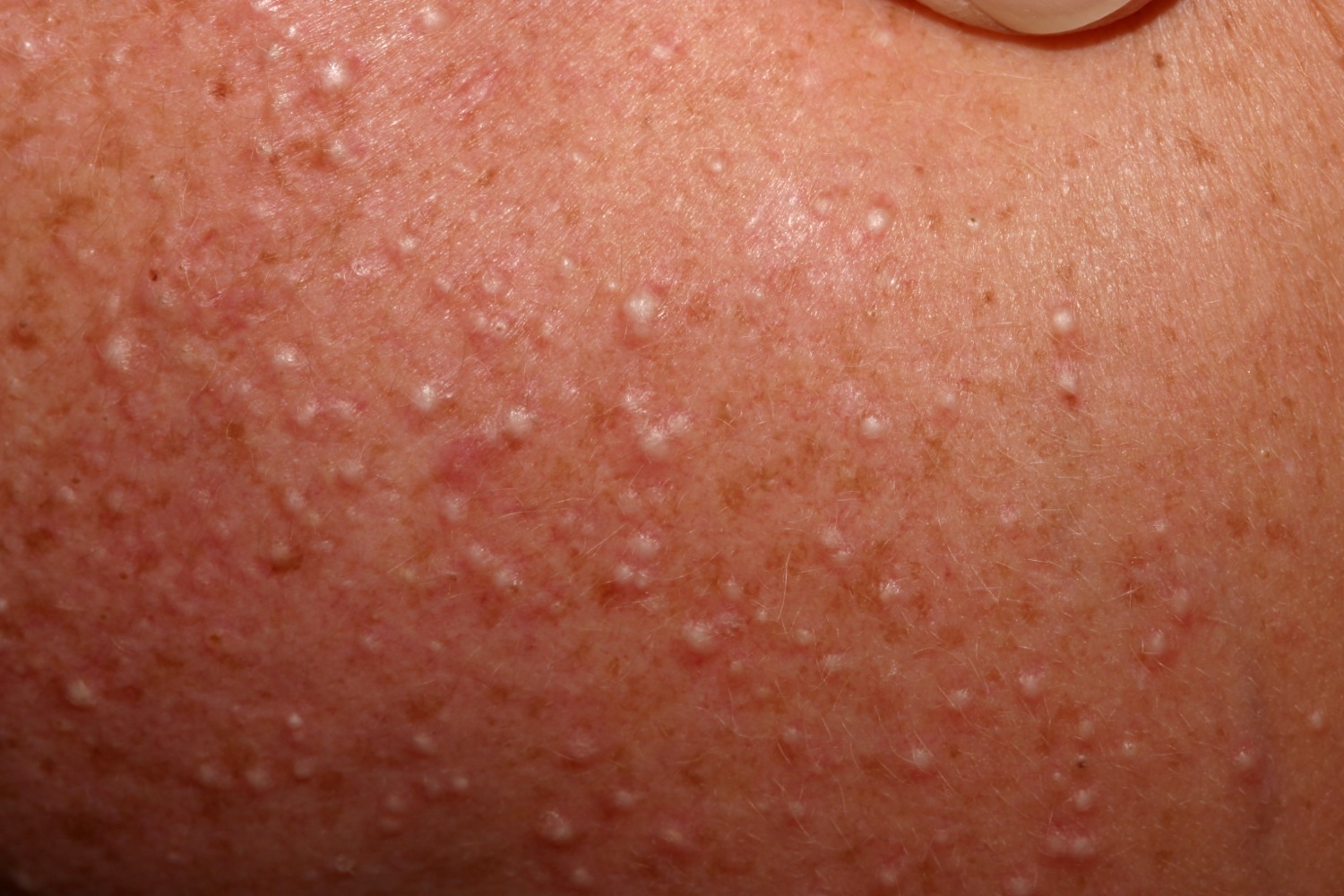
Figure 1. Milia skin
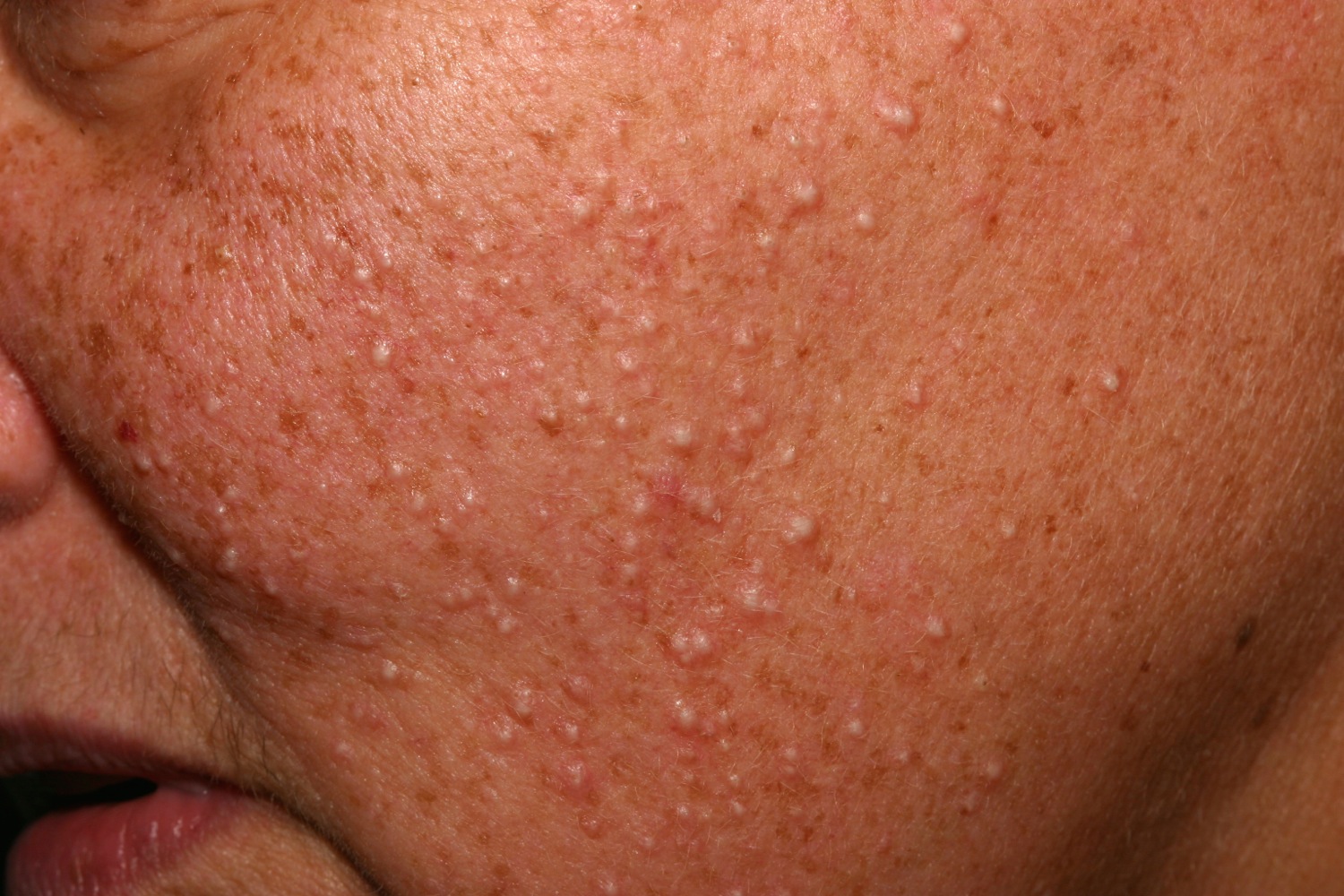
Figure 2. Milia on face
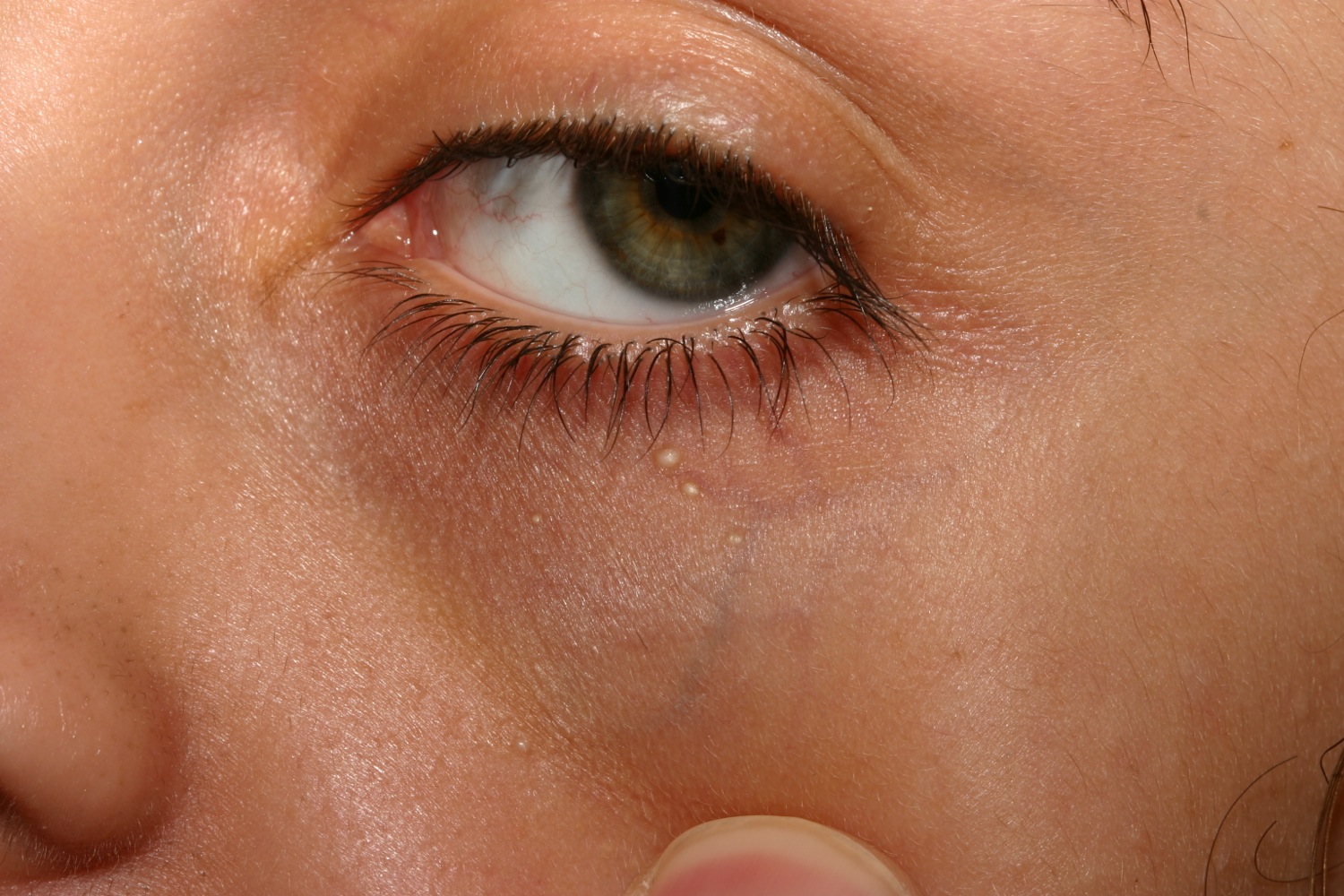
Figure 3. Milia under eyes
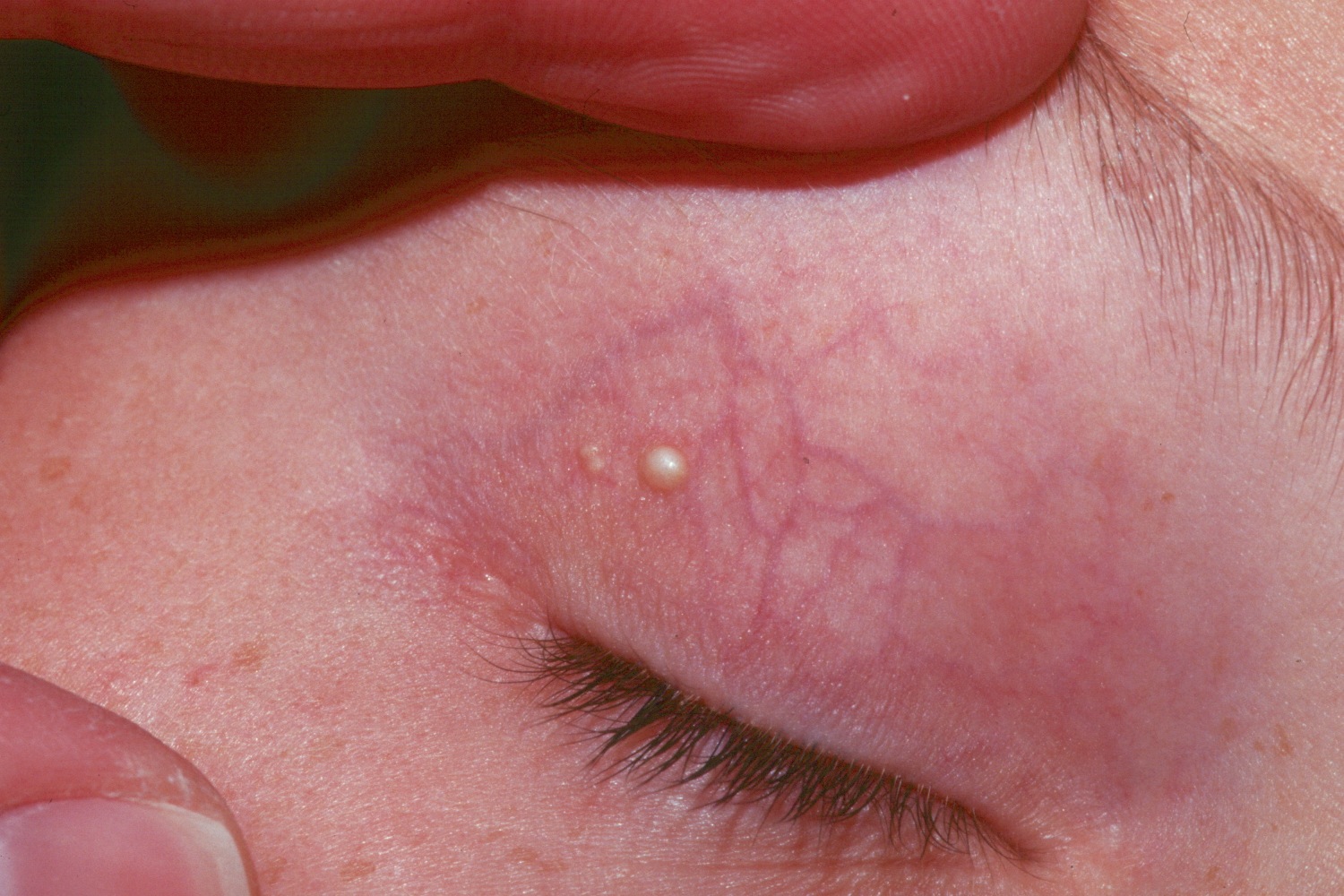
Figure 4. Milia on eyelid
Figure 5. Milia baby
Types of milia
There are many types of milia – here are the most common.
- Benign primary milia are usually clustered on the cheeks, eyelids, forehead and genitals of children or adults. These usually clear up naturally.
- Neonatal or congenital milia affects 40-50% of newborn babies and usually disappears in a few weeks or months without treatment.
- Secondary milia is a form of milia that may result from a rare disease, a medication or trauma. This form of milia may resolve spontaneously but tends to persist.
Primary milia in children and adults
- Found around eyelids, cheeks, forehead and genitalia
- In young children, a row of milia may appear along the nasal crease
- May clear in a few weeks or persist for months or longer
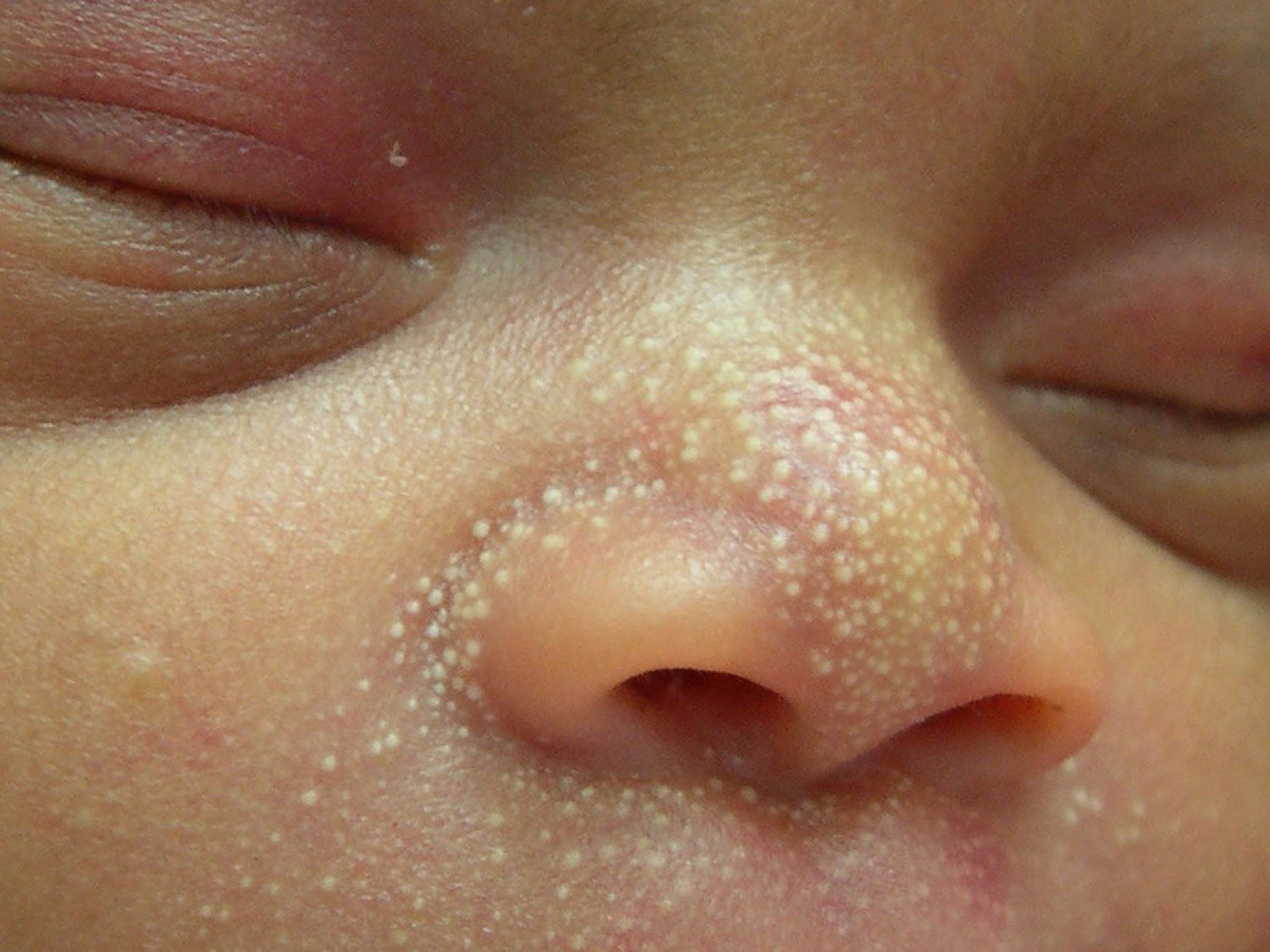
Milia newborn
- Affect 40–50% of newborn babies
- Few to numerous lesions
- Often seen on the nose, but may also arise inside the mouth on the mucosa (Epstein pearls) or palate (Bohn nodules) or more widely on scalp, face and upper trunk – they occur in up to 85% of infants
- Heal spontaneously within a few weeks of birth.
Juvenile milia
- Associated with Rombo syndrome, basal cell naevus syndrome, Bazex-Dupre-Christol syndrome, pachyonychia congenita, Gardner syndrome and other genetic disorders
- May be congenital (present at birth) or appear later in life
Milia en plaque
- Multiple milia appear on within an inflamed plaque up to several centimeters in diamater
- Usually found on eyelid, behind ears, on cheeks or jaw
- Affect children and adults, especially middle-aged women
- Sometimes associated with other skin disease including pseudoxanthoma elasticum, discoid lupus erythematosus, lichen planus
Multiple eruptive milia
- Crops of numerous milia appear over a few weeks to months
- Lesions may be asymptomatic or itchy
- Most often affect face, upper arms and upper trunk
Traumatic milia
- Occur at site of injury as skin heals
- Arise from eccrine sweat ducts
- Examples include thermal burns, dermabrasion, blistering rashes such as bullous pemphigoid
- Often seen on back of hands and fingers in porphyria cutanea tarda
- Milia-like calcified nodule may develop after neonatal heel stick blood test
Milia associated with drugs
May rarely milia follow use of topical medication e.g., phenols, hydroquinone, 5-fluorouracil cream, corticosteroid creams.
What causes milia
Milia occur when dead skin becomes trapped in small pockets at the surface of the skin or mouth. They are common in newborn infants.
Similar cysts are seen in the mouths of newborn infants. They are called Epstein pearls. These cysts also go away on their own.
Adults may develop milia on the face. The bumps and cysts also occur on parts of the body that are swollen (inflamed) or injured. Rough sheets or clothing may irritate the skin and mild reddening around the bump. The middle of the bump will stay white.
Milia symptoms
Milia are most commonly seen on a baby’s nose, chin or cheeks, though they may also occur in other areas, such as on the upper trunk and limbs.
Sometimes similar bumps appear on a baby’s gums or the roof of the mouth. These are known as Epstein pearls. Some babies also develop baby acne, often characterized by small red bumps and pustules on the cheeks, chin and forehead, which can occur with or without milia.
Milia diagnosis
Milia are easy to identify and can be diagnosed by a doctor without any need for testing.
A similar condition to milia is neonatal or baby acne, which can also be diagnosed on sight.
However, on occasion, a skin biopsy may be performed. This shows a small epidermoid cyst coming from a vellus hair follicle.
Milia should be distinguished from other types of cyst, comedones, xanthelasma and syringomas. Colloid milia are golden coloured bumps on cheeks and temples associated with excessive exposure to sunlight.
They should also be distinguished from milia-like cysts noted on dermoscopy in seborrhoeic keratoses, papillomatous moles and some basal cell carcinomas.
Milia treatment
Milia usually go away naturally within weeks or months without any treatment. They don’t leave scars and trying to squeeze or burst them at home is not recommended.
While around half of newborn babies have milia, the bumps usually go away without treatment in several weeks to months. They are hard to prevent but it can help to gently wipe your baby’s face every day.
Milia affecting children and adults can be more persistent.
Home remedies
Try these tips to help your baby’s skin look its best:
- Keep your baby’s face clean. Wash your baby’s face daily with warm water and mild baby soap.
- Dry your baby’s face gently. Simply pat your baby’s skin dry.
- Don’t pinch or scrub the bumps. You may cause more irritation or an infection.
- Avoid using lotions or oils on your baby’s face.
How to get rid of milia
If milia continue to concern you, see a doctor, particularly if you notice any redness or swelling. Your doctor may recommend a suitable cream (e.g., topical retinoids). Topical retinoid cream such as tretinoin, tazarotene, or adapalene.
The lesion may also be de-roofed using a sterile needle or blade and the contents squeezed or pricked out. They may be simply removed by the use of a 19 gauge needle. After cleansing the area with alcohol, the needle is inserted just under the lesion, followed by removal of the cyst material with a tool called a comedone extractor. Aluminum chloride may then be applied to stop the bleeding.
Milia removal
In some cases, your doctor can remove milia by slicing off the top of individual cysts with a sterile blade or needle and squeezing them out. Milia may also be removed by your doctor by:
- Burning them off with diathermy (high frequency heat treatment)
- Freezing them with liquid nitrogen (cryotherapy)
- Milia may be destroyed using curettage
- Chemical peels, dermabrasion and laser ablation have been reported to be effective when used for very extensive milia.
- Milia en plaque may improve with minocycline (a tetracycline antibiotic).