Contents
What is pulse oximeter
Pulse oximeter is a noninvasive method for monitoring a person’s oxygen saturation in arterial blood (SaO2) that is frequently used in hospital but are rarely used at home 1). Pulse oximetry is universally used for monitoring respiratory status of patients in the ICU (intensive care unit). Studies have shown that the presence of pulse oximetry may reduce the number of arterial blood gas samples obtained in the ICU and in the emergency department 2). The pulse oximeter has revolutionized modern medicine with its ability to continuously and transcutaneously monitor the functional oxygen saturation of hemoglobin in arterial blood (SaO2). However, the lack of incorporating explicit guidelines for the appropriate use of pulse oximetry may lessen the cost-effectiveness of pulse oximetry in the ICU 3). Though its reading of SpO2 (peripheral oxygen saturation) is not always identical to the more desirable reading of SaO2 (arterial blood oxygen saturation) from arterial blood gas analysis (taken directly via arterial blood), the two are correlated well enough that the safe, convenient, noninvasive, inexpensive pulse oximetry method is valuable for measuring oxygen saturation in clinical use.
Arterial blood gas analysis is a common investigation in emergency departments and intensive care units for monitoring patients with acute respiratory failure. It also has some applications in general practice, such as assessing the need for domiciliary oxygen therapy in patients with chronic obstructive pulmonary disease (COPD). An arterial blood gas result can help in the assessment of a patient’s gas exchange, ventilatory control and acid–base balance. Nurses are usually involved in taking and analyzing the person’s oxygen saturation (SO2) and normally they report these results to the doctors or anesthesiologists. Out of these results the anesthesiologists will then prescribe further treatment for the critically ill patient. Hence, it is important you are familiar with the information obtained to be able to detect the disturbances in ventilation, oxygen delivery and acid–base balance.
The conventional pulse oximeters use transmission sensors in which the light emitter and detector are on opposing surfaces of the tissue bed 4). These sensors are suitable for use on the finger, toe, or earlobe; when tested under conditions of low perfusion, finger probes performed better than other probes 5). Recently, pulse oximeter probes that use reflectance technology have been developed for placement on the forehead 6). The reflectance sensor has emitter and detector components adjacent to one another, so oxygen saturation is estimated from back-scattered light rather than transmitted light. In critically ill patients with low perfusion, the bias and precision between SpO2 and SaO2 were lower for the forehead reflectance probe than for the finger probe 7). The superiority of forehead reflectance probes over conventional digital probes, however, was not observed in patients with acute respiratory distress syndrome (ARDS) during a positive end-expiratory pressure (PEEP) recruitment maneuver 8).
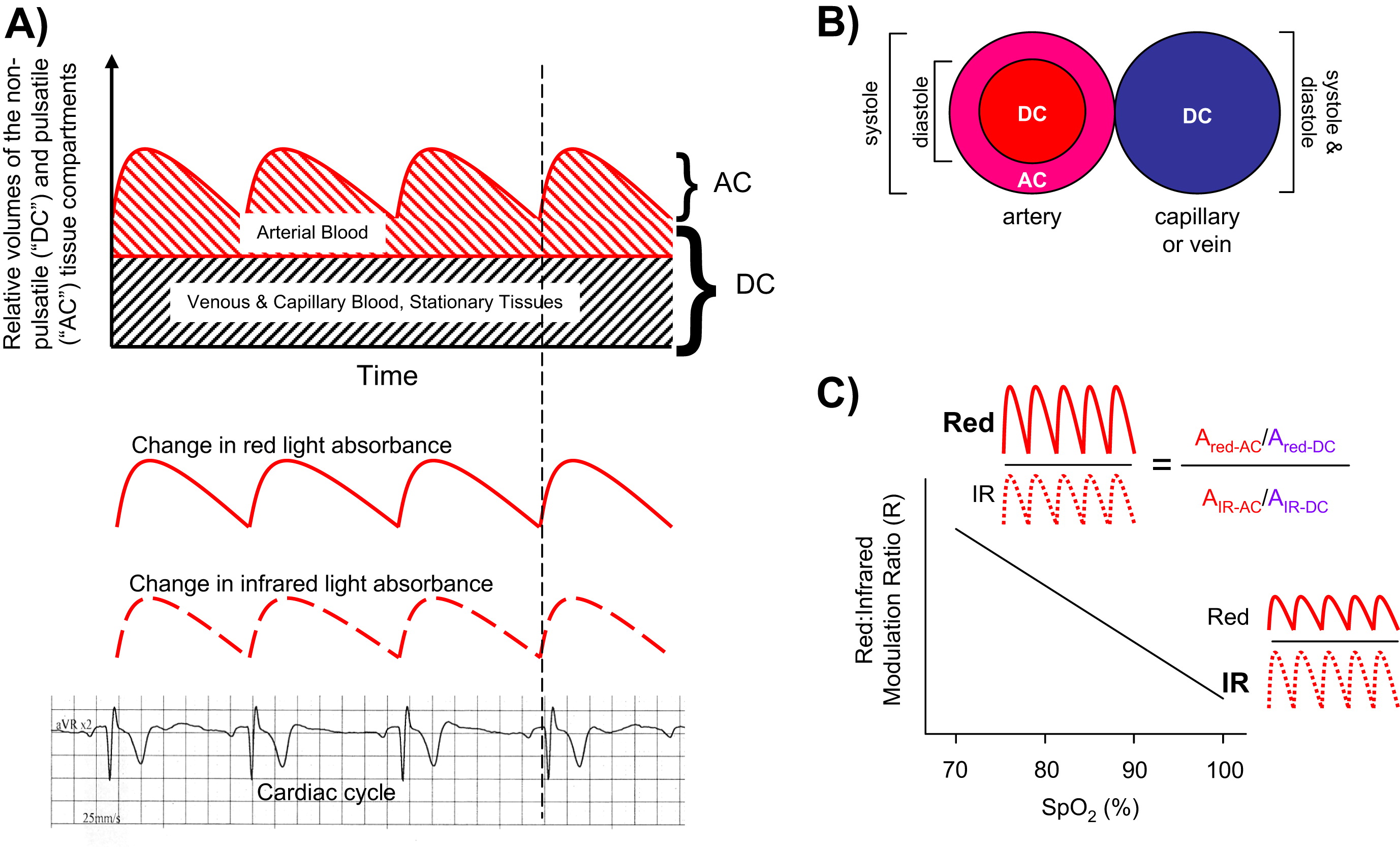
- Pulse oximetry is based on the principle that oxyhemoglobin (O2Hb) absorbs more near-infrared light than deoxyhemoglobin (HHb), and deoxyhemoglobin (HHb) absorbs more red light than oxyhemoglobin (O2Hb). Under optimal conditions, pulse oximeters do not calculate SpO2 of venous blood (and other stationary tissues) but rather only arterial SpO2 by determining changes in absorbance of the light transmitted over time; i.e., arterial blood volume changes with the cardiac cycle whereas the volumes of light absorbers in non-arterial tissues are relatively constant.
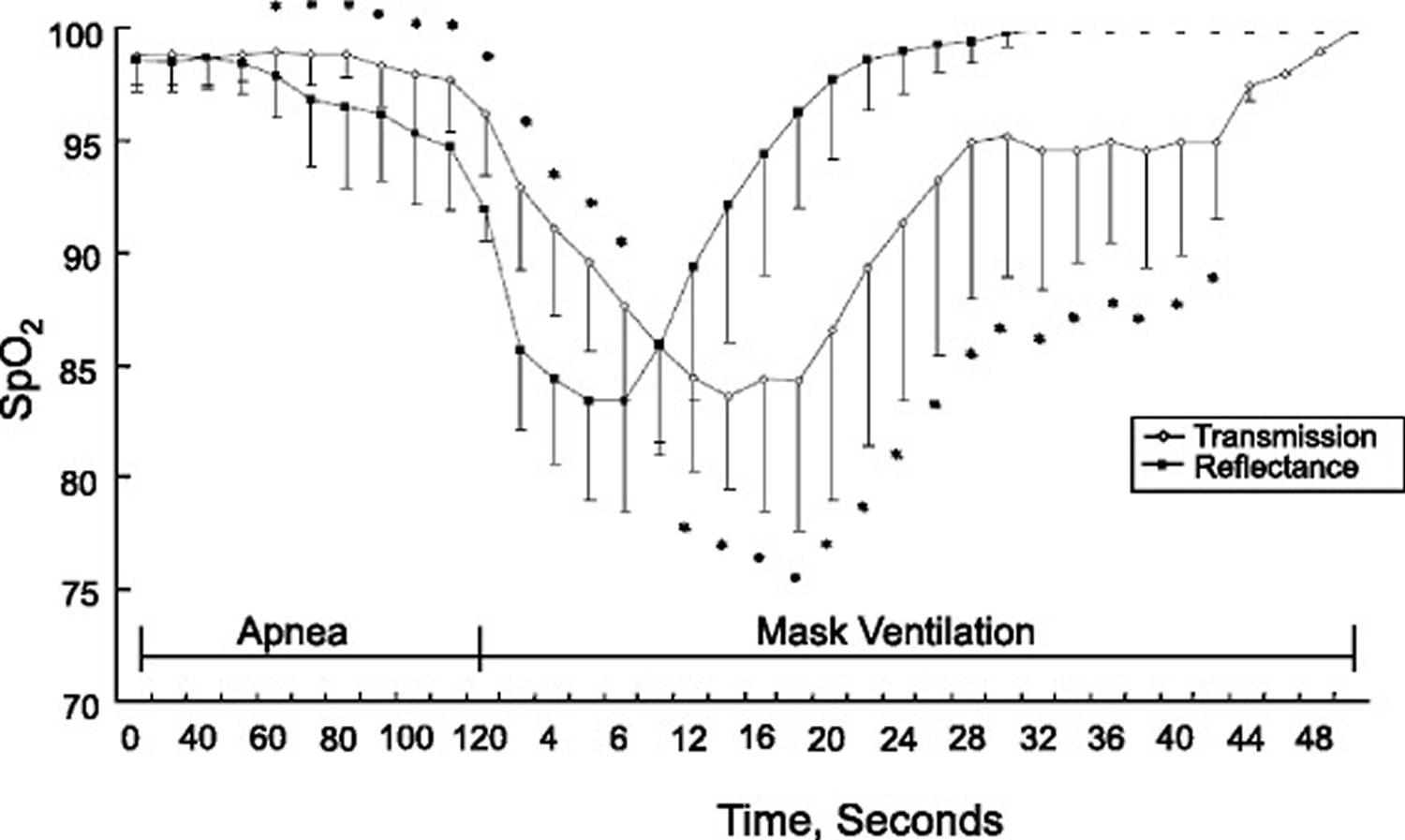
The response time of conventional oximeter probes varies; ear probes respond quicker to a change in O2 saturation than finger probes 9). A recent study compared the response time of the conventional finger probe with the reflectance forehead probe in patients undergoing general anesthesia [see Figure 7 below] 10). The lengths of time it took to detect a decrease in SpO2 to 90 % after apnea was induced (desaturation response time) were 94 seconds for the forehead probe and 100 seconds for the finger probe. After mask ventilation was started, the lengths of time it took to detect an increase in SpO2 to 100 % (re-saturation response time) were 23.2 seconds for the forehead probe and 28.9 seconds for the finger probes. The investigators speculated that the shorter response time with the reflectance forehead probe was most likely due to the location of the probe rather than to the workings of the reflectance technology. The forehead probe monitors O2 saturation from the supraorbital artery in which blood flow is abundant and is less likely to be affected by vasoconstriction than is a peripheral artery 11).
Oxygen saturation is the fraction of oxygen-saturated hemoglobin relative to total hemoglobin (unsaturated + saturated) in the blood. The human body requires and regulates a very precise and specific balance of oxygen in the blood. Normal blood oxygen levels in humans are considered 95–100 percent. If the level is below 90 percent, it is considered low resulting in hypoxemia. Blood oxygen levels below 80 percent may compromise organ function, such as the brain and heart, and should be promptly addressed. Continued low oxygen levels may lead to respiratory or cardiac arrest. Oxygen therapy may be used to assist in raising blood oxygen levels. Oxygenation occurs when oxygen molecules (O2) enter the tissues of the body. For example, blood is oxygenated in the lungs, where oxygen molecules travel from the air and into the blood. Oxygenation is commonly used to refer to medical oxygen saturation.
Your body maintains a stable level of oxygen saturation for the most part by chemical processes of aerobic metabolism associated with breathing. Using the respiratory system, red blood cells, specifically the hemoglobin, gather oxygen in the lungs and distribute it to the rest of the body. The needs of your body’s blood oxygen may fluctuate such as during exercise when more oxygen is required or when living at higher altitudes. A blood cell is said to be “saturated” when carrying a normal amount of oxygen. Both too high and too low arterial oxygen saturation levels can have adverse effects on your body.
Healthy individuals at sea level usually exhibit oxygen saturation values between 96% and 99%, and should be above 94%. At 1,600 meters’ altitude (about one mile high) oxygen saturation should be above 92%.
An SaO2 (arterial oxygen saturation) value below 90% causes hypoxia (which can also be caused by anemia). Hypoxia due to low SaO2 is indicated by cyanosis, but oxygen saturation does not directly reflect tissue oxygenation. The affinity of hemoglobin to oxygen may impair or enhance oxygen release at the tissue level. Oxygen is more readily released to the tissues (i.e., hemoglobin has a lower affinity for oxygen) when pH is decreased, body temperature is increased, arterial partial pressure of carbon dioxide (PaCO2) is increased, and 2,3-DPG levels (a byproduct of glucose metabolism also found in stored blood products) are increased. When the hemoglobin has greater affinity for oxygen, less is available to the tissues. Conditions such as increased pH, decreased temperature, decreased PaCO2, and decreased 2,3-DPG will increase oxygen binding to the hemoglobin and limit its release to the tissue.
Pros and cons of different types of pulse oximeter probes
The reason pulse oximeter probes interrogate the finger, nose, ear lobe, and forehead is because the skin in these areas have a much higher vascular density than, for example, the skin of the chest wall 12). Reusable clip probes (finger, nasal, ear) and single-patient adhesive probes (finger, forehead) are the two main types of pulse oximeter probes. Advantages of the reusable clip probes are the rapidity in which they can be employed, the ease in which different body sites can sampled in the event of low amplitude waves, and cost-effectiveness in outpatient settings where multiple patients can be measured sequentially with one probe because only a single reading of SpO2 is required. Advantages of the single-patient adhesive probes are potentially less transmission of nosocomial infections, more secure placement when there is excessive patient movement, and ability to monitor sites other than the acral regions since the latter areas are more vulnerable to vasoconstriction. Thus, for continuous monitoring of SpO2, one particular type of probe may be more appropriate than others depending on the clinical circumstance; i.e., some “trial-and-error” may be necessary to find the optimal probe. For example, in hypotensive, vasoconstricted patients, ear and forehead probes may be more reliable as these areas are less likely to vasoconstrict than the fingers in response to endogenous and exogenous catecholamines 13). In hypothermia, where there is secondary vasoconstriction, the forehead probe has been shown to be more reliable than the finger probe 14).
Even after optimizing the type of probe, false readings of SpO2 may occur in various settings and medical conditions, summarized in Table 1.
Table 1. Causes and mechanisms of unreliable pulse oximetry SpO2 readings
| 1. Causes of intermittent drop-outs or inability to read SpO2 |
| • Poor perfusion due to a number of causes, e.g., hypovolemia, vasoconstriction, etc |
| 2. Causes of falsely normal or elevated SpO2 |
| • Carbon monoxide poisoning |
| • Sickle cell anemia vasoocclusive crises (overestimation of FO2Hb and underestimation of SaO2) |
| 3. Causes of falsely low SpO2 |
| • Venous pulsations |
| • Excessive movement |
| • Intravenous pigmented dyes |
| • Inherited forms of abnormal hemoglobin |
| • Fingernail polish |
| • Severe anemia (with concomitant hypoxemia) |
| 4. Causes of falsely low or high SpO2 |
| • Methemoglobinemia |
| • Sulfhemoglobinemia |
| • Poor probe positioning |
| • Sepsis and septic shock |
| 5. Causes of falsely low FO2Hb as measured by a co-oximeter |
| • Severe hyperbilirubinemia |
| • Fetal Hb (HbF) |
Causes of intermittent drop-outs or inability to read pulse oximeter SpO2
It is common knowledge that an attenuated and/or inconsistent wave tracing generated by pulse oximeters displayed on intensive care unit monitors is an indication that the SpO2 reading is unreliable or may become so, i.e., increased drop outs or false transient SpO2 changes. The amplitude of such a pulse oximeter waveform reflects the amount of cardiac-induced light modulation, as noted by the near simultaneous onset of the QRS complex on the electrocardiogram with the onset of the positive deflection of the pulse oximetry wave tracing (Figure 4A below). Although portable pulse oximeters do not typically have such wave tracings, they often have a pulse signal bar that shows the level of change in light absorbance (and thus strength of the pulse) to indicate the possibility of a suboptimal reading.
Low-amplitude pulse oximetry wave tracings may be due to poor finger perfusion resulting from vasoconstriction and/or hypotension from a number of causes including distributive or hypovolemic shock, hypothermia, use of vasoconstrictor agents, and poor cardiac output due to pump failure or dysrhythmia. Arterial compression (e.g., pumped-up sphygmomanometer) or arterial blockage proximal to probe placement (e.g., peripheral vascular disease) can also result in poor pulse oximetry wave tracings. Decreased pulse amplitude in the arterial blood signal additionally decreases the pulse oximeter’s signal to noise ratio and potentially result in the inability to post values, intermittent drop-outs and alarms, and unstable SpO2 readings. Knowing that the aforementioned conditions can result in false SpO2 readings is the single best deterrent to accepting falsely low SpO2 readings. While clinical assessment can help differentiate spurious from true SpO2 readings, uncertain cases should be corroborated by arterial blood gas analysis taken directly from arterial blood sample.
Pulse oximetry normal range
Normal pulse oximetry value is generally considered to be in the 95-98%. Values under 90 percent are considered low. However, as you will soon see, 90% or greater can be considered acceptable.
Why is a normal oxygen saturation 98% and not 100%?
After the diffusion of oxygen from the alveoli to the capillary occurs, this oxygenated blood moves to the pulmonary vein to the left atrium. This blood contains a PaO2 of 104 mmHg [partial pressure of arterial blood (PaO2)], on average. This blood constitutes 98% of cardiac output. Another 2% of the cardiac output comes from the bronchial veins, and this blood has a PvO2 of 40 mmHg [partial pressure of capillary venous blood (PvO2)]. This unoxygenated blood is shunted into the pulmonary vein, and mixes with arterial blood. It is because of this natural shunt that a normal saturation is 98% and not 100%.
The saturation of arterial hemoglobin (SaO2), as measured by arterial blood gas, is normally about 98%. The saturation of arterial hemoglobin, as measured by pulse oximeter (SpO2) is also about 98%.
Causes of falsely normal or elevated SpO2 pulse oximetry value
Carbon monoxide poisoning
Carbon monoxide (CO) is an odorless, colorless, tasteless, and non-irritating gas. Since patients with CO poisoning may present with signs and symptoms that are non-specific (e.g., headaches), mimics of other disorders (e.g., food poisoning, alcohol intoxication, acute psychiatric decompensation, or “flu-like symptoms”), or with genuine disorders that are precipitated by CO toxicity (e.g., angina, syncope), the diagnosis is often missed with occult exposure. CO toxicity may be due to exposure from a variety of sources including propane-powered engine, natural gas, automobile exhaust, portable generators, gas log fireplaces, kerosene heaters, fire smoke, and paint strippers and spray paints as dichloromethane in these products gets metabolized to CO. The principal pathogenic mechanism of CO poisoning is the strong avidity of CO for Hb (240× greater than O2), forming carboxy-Hb (COHb), reducing the O2 carrying capacity of Hb and precipitating tissue hypoxemia. CO can also impair myoglobin and mitochondrial function; increase guanylate cyclase activation which can lead to vasodilation and hypotension; and augment lipid peroxidation causing microvascular impairment and reperfusion injury.
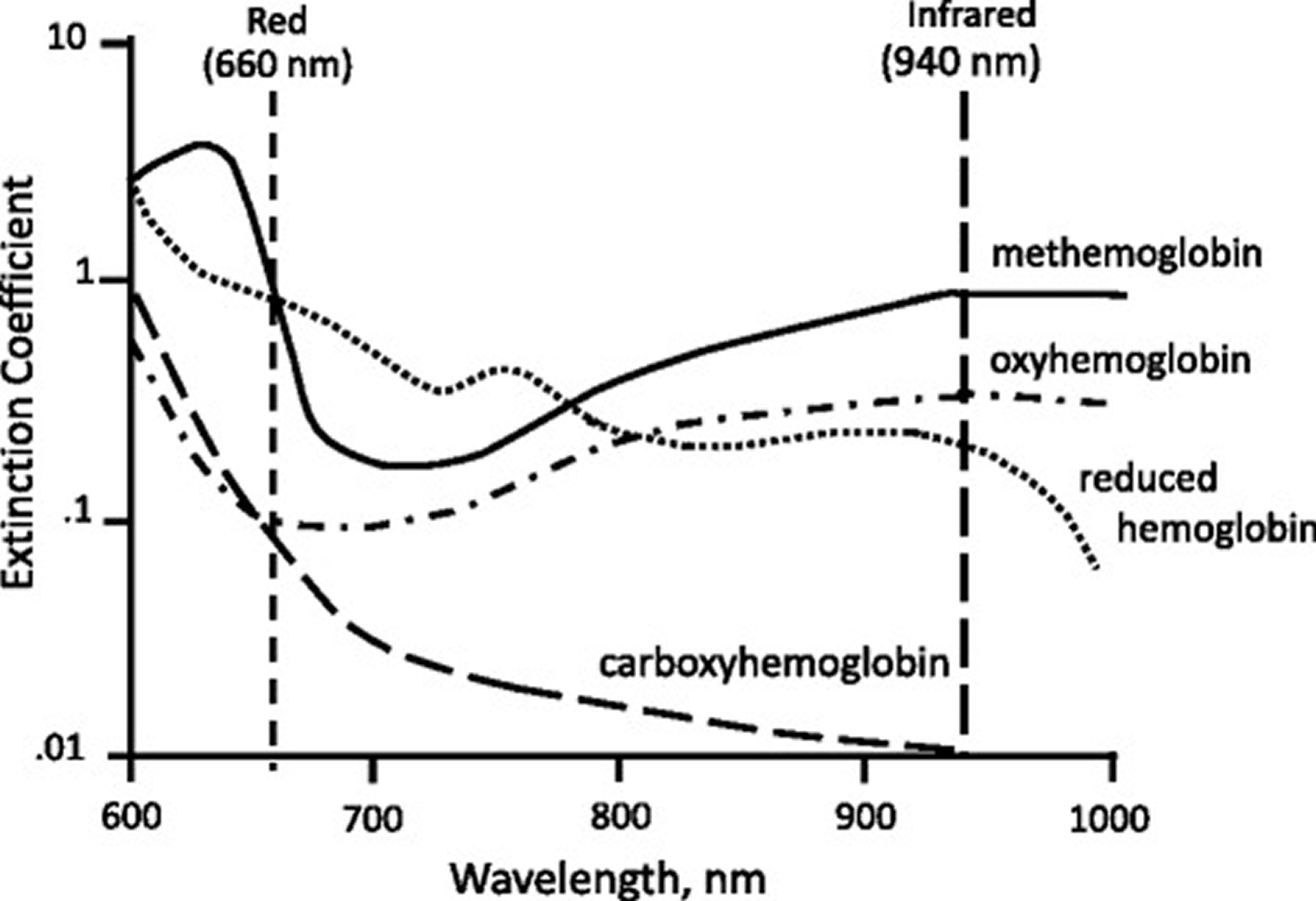
While considering the possibility of CO poisoning in the differential diagnosis is a linchpin in recognizing its presence in an ill patient, the diagnosis must be made objectively. Because oxyhemoglobin (O2Hb) and carboxy-Hb (COHb) absorb red light (660 nm) similarly and carboxy-Hb (COHb) absorbs very little near-infrared light (940 nm) (see Figure 5 below), the photodiode of standard pulse oximeters – that only emit red and near-infrared light – cannot differentiate between oxyhemoglobin (O2Hb) and carboxy-Hb (COHb). The similar absorptive property of oxyhemoglobin (O2Hb) and carboxy-Hb (COHb) for red light is consistent with the clinical observation that patients with carboxyhemoglobinemia can appear bright red and not cyanotic.10 In the context of R, because carboxy-Hb (COHb) will decrease both deoxyhemoglobin (HHb) and O2Hb concentrations, the normally greater red light absorption by deoxyhemoglobin (HHb) will be decreased but the red light absorption of the combined oxyhemoglobin (O2Hb) and carboxy-Hb (COHb) species will be maintained or slightly increased. However, because deoxyhemoglobin (HHb) still absorbs red light better than either carboxy-Hb (COHb) or O2Hb, the reduction in deoxyhemoglobin (HHb) in the presence of carboxyhemoglobinemia results in a net effect of decreased red light absorption and R that is reduced more than predicted (see Figure 4C), resulting in SpO2 that overestimates the fractional oxyhemoglobin (O2Hb) content (FO2Hb), which is also measured by co-oximeters but in contrast to SaO2, takes into account COHb concentrations. Thus, in significant carboxyhemoglobinemia, standard pulse oximeters can give a false normal (or elevated) SpO2 when in fact the fractional O2Hb content (FO2Hb) is low. Semantically, it is important to emphasize that it is the fractional O2Hb content (FO2Hb) content and not the SaO2 that is decreased by carboxy-Hb (COHb). For pulse oximeters to be able to detect carboxy-Hb (COHb) as well as oxyhemoglobin (O2Hb) and deoxyhemoglobin (HHb), an instrument with at least three light beams of different wavelengths would have to be employed10; while they exist, they are not widely available.
Sickle cell anemia vasoocclusive crises
Complications of sickle cell disease, such as vasoocclusive crisis and acute chest syndrome, are often precipitated or exacerbated by hypoxemia, and can result in a vicious cycle of additional sickling and vasoocclusive crises 16). Thus, accurate detection of hypoxemia in these patients plays an important role in mitigating further red blood cell sickling. The accuracy of pulse oximetry in monitoring oxygenation in sickle cell disease has been debated. In a study of 17 patients with sickle cell disease, SpO2 was found to overestimate fractional O2Hb content (FO2Hb) content by an average of 3.4% and to underestimate SaO2 by an average of 1.1% 17). However, these minor biases in pulse oximeter readings did not lead to a misdiagnosis of either normoxemia or hypoxemia. Similarly, a study of 24 patients with sickle cell disease determined that SpO2 underestimated SaO2 readings by 1.6%; this difference was clinically insignificant 18). However, the authors note that while SpO2 may be used as an accurate representation of SaO2 in sickle cell disease, the fractional O2Hb content (FO2Hb) may be a more useful measurement, as some individuals with sickle cell disease may have elevated carboxy-Hb (COHb) (due to the metabolism of heme to bilirubin and carbon monoxide); in these instances, SpO2 overestimates the FO2Hb. Other studies additionally suggest that SpO2 overestimation of fractional O2Hb content (FO2Hb) and underestimation of SaO2 become more significant during vasoocclusive crises 19).
Another important caveat with oxygen saturation determination in sickle cell patients is that under normoxic conditions, where there is little HbS (sickle cell Hb) polymerization, HbS affinity for oxygen is similar to the normal HbA. However, in the presence of conditions that precipitates sickling, including hypoxemia, HbS has less affinity for oxygen and the oxygen-Hb dissociation curve is shifted to the right, i.e., for any given PaO2, the SaO2 is lower 20). Teleologically, this shift is advantageous to increase oxygen unloading to tissues.
Hypoxemia
Normal pulse oximeter readings usually range from 95 to 100 percent. Values under 90 percent are considered low. Hypoxemia is a below-normal level of oxygen in your blood, specifically in the arteries. Hypoxemia is a sign of a problem related to breathing or circulation, and may result in various symptoms, such as shortness of breath.
Hypoxemia is determined by measuring the oxygen level in a blood sample taken from an artery (arterial blood gas). It can also be estimated by measuring the oxygen saturation of your blood using a pulse oximeter — a small device that clips to your finger.
Normal arterial oxygen is approximately 75 to 100 millimeters of mercury (mm Hg). Values under 60 mm Hg usually indicate the need for supplemental oxygen.
Causes of hypoxemia
Several factors are needed to continuously supply the cells and tissues in your body with oxygen:
- There must be enough oxygen in the air you are breathing
- Your lungs must be able to inhale the oxygen-containing air — and exhale carbon dioxide
- Your bloodstream must be able to circulate blood to your lungs, take up the oxygen and carry it throughout your body
A problem with any of these factors — for example, high altitude, asthma or heart disease — might result in hypoxemia, particularly under more extreme conditions, such as exercise or illness. When your blood oxygen falls below a certain level, you might experience shortness of breath, headache, and confusion or restlessness.
Common causes of hypoxemia include:
- Anemia
- ARDS (Acute respiratory distress syndrome)
- Asthma
- Congenital heart defects in children
- Congenital heart disease in adults
- COPD (chronic obstructive pulmonary disease)
- Emphysema
- Interstitial lung disease
- Medications, such as certain narcotics and anesthetics, that depress breathing
- Pneumonia
- Pneumothorax (collapsed lung)
- Pulmonary edema (excess fluid in the lungs)
- Pulmonary embolism (blood clot in an artery in the lung)
- Pulmonary fibrosis (scarred and damaged lungs)
- Sleep apnea
When to see a doctor
Seek emergency care if you have:
- Severe shortness of breath that comes on suddenly and affects your ability to function.
- Severe shortness of breath with a cough, rapid heartbeat and fluid retention at high elevations (above 8,000 feet, or about 2,400 meters). These are signs and symptoms of fluid leaking from blood vessels into your lungs (high-altitude pulmonary edema), which can be fatal.
See your doctor as soon as possible if you have:
- Shortness of breath after slight exertion or when you’re at rest
- Shortness of breath that gets worse when you exercise or are physically active
- Abrupt awakenings with shortness of breath or a feeling that you’re choking — these may be symptoms of sleep apnea
Self-care
To cope with chronic shortness of breath, try to:
- Stop smoking. If you’ve been diagnosed with COPD or another lung disease, the single most important thing you can do is to quit smoking.
- Avoid passive smoke. Avoid places where others smoke. Secondhand smoke can cause further lung damage.
- Get regular exercise. It may seem difficult to exercise when you have trouble breathing, but regular exercise can improve your overall strength and endurance.
Causes of falsely low pulse oximeter readings
Venous pulsations
Venous pulsations, causing a significant change in venous volume with each cardiac cycle, can contribute to a falsely low SpO2 reading because venous O2Hb saturation (SvO2) is now also measured by the pulse oximeter, artificially lowering the arterial saturation. Venous pulsations can occur when adhesive fingerprobes are placed too tightly around the finger, in severe tricuspid regurgitation, when the location of the probes are in dependent positions (e.g., probe on the forehead with the patient in a Trendelenburg position), and possibly in distributive shock where widespread vasodilation results in physiologic arteriovenous shunting 21). When venous pulsations is considered to be occurring with a forehead sensor in a patient requiring the supine or Trendelenburg position, an elastic-tensioned headband applied to the forehead sensor can significantly reduce the occurrence of falsely low SpO2 readings 22).
Excessive movement
Excessive movement such as tremor or convulsions has been documented to cause spuriously low SpO2, with desaturations below 50% sometimes observed 23), though less commonly SpO2 overestimations can also occur. In theory, motion can cause the normally static tissues in relation to the sensor position to change over the time frame of the arterial pulses. At times, this motion can augment or mimic the cardiac-induced signals as the blood in the veins (and other previously stationary tissues) are now moving, further modulating the red and infrared light attenuation in the probed tissue. However, many newer generation pulse oximeters have improved processing algorithms that reduce the occurrence of false SpO2 readings due to excessive patient movements 24).
Intravenous pigmented dyes
Pigmented dyes are used medically or as agents in various medical diagnostic tests; e.g., the principal medicinal use of methylene blue is in methemoglobinemia where it serves as a reducing agent. Methylene blue has also been used as a dye in endoscopic polypectomy where it is injected into the submucosa around the polyp to be removed, marking the site in the event additional tissues need to be excised. Indigo carmine (FD&C Blue#2)-based dye is infrequently used to detect amniotic fluid leaks as well as to detect leaks in the urinary system during surgery since intravenous indigo carmine is cleared rapidly by the kidneys. Iodocyanine green is used for various medical diagnostic tests such as determination of hepatic function and liver blood flow, and for ophthalmic angiography.
Peak light absorption of methylene blue is 668 nm, very close to the strong red light absorption by deoxyhemoglobin (HHb), resulting in a higher R value and mimicking deoxyhemoglobin (HHb) 25). Hence, administration of methylene blue into the blood stream can falsely reduce SpO2 readings. In human volunteers with normal baseline SpO2 (≥97%), a profound drop in SpO2 occurred following intravenous administration of 5 mL of 1% methylene blue with a median nadir SpO2 of 65% although there was a wide range in SpO2 reduction among the subjects 26). Indocyanine green and indigo carmine do not have as great absorption for red light. This is consistent with the finding that intravenous injection of indocyanine green had only a minor decrease of ∼3–4% in SpO2 using a finger probe and intravenous injection of indigo carmine resulted in little or no change in SpO2 27).
Inherited forms of abnormal hemoglobin
Uncommon Hb variants have been reported to cause spuriously decreased SpO2 readings, including Hb Lansing 28), Hb Bonn 29), Hb Koln 30), Hb Hammersmith 31), and Hb Cheverly 32). Sarikonda et al. 33) reported a father and daughter with SpO2 readings that were more than 10% lower than SaO2 measurements due to an abnormal Hb variant (Hb Lansing) which accounted for ∼11% of their total Hb. Assessment of oxygen affinity was normal, suggesting that interference of absorbance of red and/or near-infrared light by the abnormal Hb accounted for the spurious reduction in SpO2 34). A father and son were reported to have falsely low SpO2 due to mutation of the ALPHA-Hb gene in which resulted in a histidine-to-aspartatic acid substitution (Hb Bonn) 35). Hb Bonn was found to have a peak absorption at 668 nm (same as methylene blue), very close to the red light wavelength of 660 nm 36). Hence, in the context of R, Hb Bonn causes an enhanced red light absorption, resulting in an elevated R value and lower SpO2 measurement; in other words, Hb Bonn behaves like deoxyhemoglobin (HHb) and methylene blue. Similarly, Hb Cheverly spectra showed that the red light absorbance for this abnormal Hb was greater than for HbA 37). Absorption spectra for both O2Hb and HHb for a patient with 5.4% Hb Koln found red light absorbance was greater for Hb Koln than for HbA, indicating that R would be biased positively, falsely lowering SpO2 38).
Fingernail polish
Earlier reports of pulse oximeters noted that fingernail polish, particularly black, blue, and green color, can lower SpO2 by up to 10% 39). More recent studies with newer models of pulse oximeters found that fingernail polish has only a minor effect on SpO2 readings; i.e., black and brown fingernail polish displayed the greatest reduction in the SpO2 reading but by an average decrease of ≤2% 40).
Severe anemia (with concomitant hypoxemia)
Theoretically, anemia should not have much effect on SpO2 readings since both oxyhemoglobin (O2Hb) and deoxyhemoglobin (HHb) would be proportionately affected. However, it has been observed that severe anemia can spuriously affect SpO2 41). Mechanistically, this is because scatter of visible and near-infrared light by human tissues is not accounted for by the simplified Beer–Lambert equation, which assumes a single, well-defined light path 42). This light scatter would be affected by the number of red blood cells; i.e., in anemia, there would be less light scatter whereas calibration curves are derived from healthy individuals without anemia. Thus, with change in Hb content, the pathlength for the transmitted red and near-infrared light would be altered, creating a bias in R and SpO2 readings.
In an experimental study of dogs, SpO2 was found to be an accurate representation of SaO2 readings down to a hematocrit range of 10–14%. When the hematocrit dropped below 10%, the accuracy of the pulse oximeter deteriorated, underestimating co-oximeter readings by an average of 5.4% 43). These findings were corroborated in a human study where in hypoxemic patients, the presence of anemia caused the SpO2 to further underestimate the SaO2 44). In contrast, for normoxic individuals, severe anemia had minimal impact on SpO2 values 45). While the mechanistic explanation for this phenomenon is complicated and beyond the scope of this review, it is important to emphasize that anemia per se does not cause a spuriously low SpO2 but rather causes the SpO2 to underestimate the SaO2 in patients with true hypoxemia, but has little impact on SpO2 measurements in normoxic individuals. Since SpO2 is underestimated in those with bona fide hypoxemia in the presence of severe anemia, this direction of error is fortuitous since earlier warning of hypoxemia by SpO2 measurements will result in more timely administration of supplemental oxygen.
Pulse oximeter uses
Pulse oximetry can provide an early warning of hypoxemia 46). In the largest randomized trial involving more than 20,000 perioperative patients, rates of incidence of hypoxemia (SpO2 of less than 90 %) were 7.9 % in patients who were monitored with pulse oximetry and only 0.4 % in patients without an oximeter 47). The anesthesiologists reported that oximetry led to a change in therapy on at least one occasion in up to 17 % of the patients. Using 95,407 electronically recorded pulse oximetry measurements from patients who underwent non-cardiac surgery at two hospitals, Ehrenfeld and colleagues 48) reported that during the intraoperative period, 6.8 % of patients had a hypoxemic event (SpO2 of less than 90) and 3.5 % of patients had a severe hypoxemic event (SpO2 of not more than 85 %) lasting more than 2 minutes. Hypoxemic events occurred mostly during the induction or emergent phase of anesthesia; these time periods are consistent with the clinical view that anesthesia-transitional states are high-risk periods for hypoxemia 49). In patients undergoing gastric bypass surgery, continuous monitoring of SpO2 revealed that episodic hypoxemia (SpO2 of less than 90 % for at least 30 seconds) occurred in all patients. For each patient, desaturation lasted as long as 21 ± 15 minutes 50).
Pulse oximetry has been shown to be reliable in titrating the fractional inspired oxygen concentration (FIO2) in patients requiring mechanical ventilation; aiming for an SpO2 of 92 % is reasonable for ensuring satisfactory oxygenation in Caucasian patients 51). To determine whether the ratio of SpO2 to FIO2 (S/F) can be used as a surrogate for the ratio of PaO2 to FIO2 (P/F), SpO2 and PaO2 data from 1,074 patients with acute lung injury or acute respiratory distress syndrome (ARDS) who were enrolled in two large clinical trials were compared 52). An SpO2/FIO2 ratio of 235 predicted a PaO2/FIO2 ratio of 200 (oxygenation criterion for ARDS), a sensitivity of 0.85, and a specificity of 0.85. An SpO2/FIO2 ratio of 310 reflected a PaO2/FIO2 ratio of 300 (oxygenation criterion for acute lung injury), a sensitivity of 0.91, and a specificity of 0.56. In patients undergoing surgery, the S/F ratio was shown to be a reliable proxy for the PaO2/FIO2 ratio, especially in those patients requiring positive end-expiratory pressure (PEEP) levels of greater than 9 cm H2O and those patients with a PaO2/FIO2 ratio of 300 or less 53). In the ICU, the SpO2/FIO2 ratio can also be a surrogate measure for the PaO2/FIO2 ratio when calculating the sequential organ failure assessment score, which measures the severity of organ dysfunction in critically ill patients 54).
Causes of falsely low or high pulse oximeter SpO2
Poor probe positioning resulting in decrease absorption of red and/or infrared light
Poor probe positioning can result in light shunting wherein the emitted light bypasses tissues and strikes the photodetector. If both transmitted red and/or infrared light are largely unabsorbed, the R value can approach 1. As a result, similar to that seen with methemoglobinemia, the SpO2 may either overestimate or underestimate the SaO2.
In older models of pulse oximeters, ambient light complicated SpO2 measurements by directly hitting the photodetector and/or by increasing the amount light going through the tissues, making the SpO2 measurements unreliable. However, most modern pulse oximeters are able to “subtract” the ambient light signals. If effects of ambient light remain a concern, shielding the probe with an opaque material is a simple solution.
Methemoglobinemia
Methemoglobinemia should be considered in patients with cyanosis, particularly in the presence of a normal or near normal partial pressure of oxygen (PaO2) 55). Methemoglobin (MetHb) is formed when the iron (Fe) in the heme moiety is oxidized from Fe+2 to Fe+3. MetHb impairs oxygen delivery to tissues by two distinct mechanisms: (i) MetHb itself is less able to bind oxygen and (ii) MetHb causes the oxygen dissociation curve of normal Hb to shift to the left which impairs unloading of oxygen at the tissue level – causing profound tissue hypoxia.
Hereditary MetHb is rare and is due to subjects having abnormal Hb (HbM) or having cytochrome b5 reductase deficiency. Most cases of methemoglobinemia are usually due to oxidizing chemicals or drugs such as nitrites, nitrates, aniline dyes, aniline derivatives (phenacetin, dapsone), sulfonamides, and lidocaine. Only 1.5–2 gm MetHb/dL of blood (a 10–20% of total Hb) can cause cyanosis. In anemic patients, cyanosis is less apparent because the corresponding absolute level of MetHb will be lower. MetHb levels between 20 and 45% can produce headaches, weakness, breathlessness, and altered mental status. Metabolic acidosis, dysrhythmias, and myocardial ischemia due to tissue hypoxia can also occur. MetHb levels between 50 and 60% are often fatal, presenting with hemodynamic instability, generalized seizures, and coma.
MetHb absorbs more infrared than either oxyhemoglobin (O2Hb) or deoxyhemoglobin (HHb) (Figure 5). Since its absorbance of red light is similar to deoxyhemoglobin (HHb) (Figure 5), patients with significant methemoglobinemia can appear cyanotic and their blood very dark in color. Moreover, because MetHb absorbs both red and infrared light equally well (Figure 5), high MetHb levels result in an R value that approaches 1, which happens to be equivalent to a SpO2 of 80–85%.5, 10 Therefore, high MetHb levels will cause the SpO2 to trend toward 85%, resulting in an overestimation or underestimation of the SaO2, depending on whether there is true hypoxemia that is <85% or normoxia, respectively. MetHb level can be directly analyzed by a CO-oximeter. Treatment of methemoglobinemia includes stopping the offending agent, supportive care, and administration of a reducing agent such as methylene blue in severe cases, bearing in mind that methylene blue can cause spuriously low SpO2.
Sulfhemoglobinemia
Sulfhemoglobin (SulfHb) is formed by the irreversible oxidation of Fe+2 in the porphyrin ring of Hb to Fe+3 (similar to MetHb) but additionally has a sulfur atom incorporated into the porphyrin ring. It is most often caused by oxidizing drugs that may or may not contain sulfur; in the latter cases, it is thought that endogenous hydrogen sulfide (H2S) derived from gut bacteria is the source for the sulfur, particularly in severely constipated states 56). Hence, SulfHb may be formed by aniline dyes, acetanilid, phenacetin, phenozapyridine, nitrates, sulfonamides, metoclopramide (structurally similar to aniline dyes), flutamide, dapsone, dimethyl sulfoxide (DMSO) or by exposure to sulfurated chemicals such as hydroxylamine sulfate used in various cleaning solutions 57). Sulfhemoglobin (SulfHb) cannot carry oxygen 58).
The major clinical manifestation of sulfhemoglobinemia is the presence of cyanosis. A mean capillary concentration of only 0.5 gm/dL (5 gm/L) of sulfhemoglobin (SulfHb) is sufficient for detectable cyanosis [compared with 1.5 gm/dL for MetHb and 5 gm/dL for deoxyhemoglobin (HHb)]. While SulfHb markedly reduces oxygen transport, it also shifts the normal Hb oxygen dissociation curve to the right, facilitating oxygen unloading in tissues. Note that this rightward shift of the normal Hb oxygen dissociation curve by SulfHb is opposite to that seen with methemoglobinemia, where O2 unloading is impaired at the tissue level. Hence, sulfhemoglobinemia has fewer adverse clinical consequences than methemoglobinemia for the same level of concentration. Nevertheless, extremely high SulfHb levels will ultimately impair oxygen transport by reducing O2Hb.
SulfHb has greater red light (660 nm) absorbance than HHb or MetHb 59). Although it is not known precisely, SulfHb most likely has a similar degree of absorbance at red and near-infrared light because there have been several reports that the SpO2 of persons with severe sulfhemoglobinemia are ∼85%, a sign that absorbance of red and near-infrared light are similar with SulfHb, resulting in a R value that approaches 1 (as seen with methemoglobinemia) 60). While most co-oximeters have four wavelengths and are able to differentiate O2Hb, HHb, COHb, and MetHb, they cannot specifically identify SulfHb. Moreover, significantly high levels of SulfHb are often falsely reported as MetHb as many spectrophotometers cannot accurately differentiate MetHb from SulfHb. In these instruments, additional biochemical testing is required to differentiate between SulfHb and MetHb; e.g., SulfHb remains intact after addition of cyanide to the blood sample whereas MetHb disappears. However, newer generations of co-oximeters can differentiate between SulfHb and MetHb. In centers where determination of SulfHb levels are not available, unresponsiveness to methylene blue may be the only indication of sulfhemoglobinemia in patients initially presumed to have methemoglobinemia. There is no specific treatment for sulfhemoglobinemia (no known antidote available) other than eliminating exposure to the offending agent and supportive therapy. The concentration of SulfHb will decrease as erythrocytes are destroyed and replaced. For extremely symptomatic cases, exchange transfusion has been performed with success 61).
Sepsis and septic shock
There are conflicting studies on how SpO2 is biased in the setting of sepsis and septic shock. Secker and Spiers18 compared 80 paired SpO2 and SaO2 readings in patients with septic shock and showed that only in those with low systemic vascular resistance (as measured by a pulmonary artery catheter), the SpO2 underestimated the SaO2 by a mean of 1.4%, a level that was statistically significant but unlikely to be clinically important. These results are supported by a human study where induction of hyperemia in one arm of volunteers resulted in lower SpO2 than the control arm 62). A hypothesis to explain this phenomenon is that vasodilation from the sepsis resulted in creation of arteriovenous shunts that culminated in venous pulsations and spurious detection by the pulse oximeter of some venous blood as arterial 63).
By contrast, a retrospective review of 88 patients with severe sepsis and septic shock found that in those with hypoxemia (defined as SaO2 < 90%), SpO2 significantly overestimated SaO2 by nearly 5% 64). In several studies examining critically ill patients with various acute illnesses, some found SpO2 underestimated SaO2 while others found the opposite 65). Even in those studies that examined only septic patients, factors that may account for a difference in the direction in which SpO2 is biased include differences in: (i) the extent of fluid resuscitation and tissue perfusion, (ii) sepsis-induced cardiac dysfunction, (iii) sites interrogated by the pulse oximeter probe, (iv) types of pulse oximeters and probes used, (v) vasoconstrictor use, and (vi) the presence of other co-morbid conditions that may spuriously affect SpO2 values unpredictably. Thus, a number of variables that occur in patients with severe sepsis and septic shock make it difficult to predict which direction SpO2 may be biased. Until more definitive studies are performed, it appears prudent to at least determine how well SpO2 correlates with SaO2 and FO2Hb measurements in any unstable, critically ill, cardiopulmonary patient.
Pulse oximetry effect on clinical outcome
To date, the largest randomized controlled trial that has evaluated the impact of pulse oximetry on outcome was the study by Moller and colleagues 66) in 20,802 surgical patients. Although myocardial ischemia occurred less frequently in the oximetry than the control group, the numbers of post-operative complications and hospital deaths were similar in the two groups 67).
In a more recent randomized study in 1,219 post-operative patients, Ochroch and colleagues 68) assessed the impact of pulse oximetry on the rate of transfer to the ICU from a post-surgical care floor. Upon admission to the study floor, patients were randomly assigned to receive monitoring with a pulse oximeter either continuously (n = 589) (oximeter group) or intermittently (n = 630) according to clinical needs as judged by a nurse or a physician (control group). The percentages of patients transferred to the ICU were similar in the oximeter group and the control group (6.7 % versus 8.5 %). A lower rate of ICU transfers for pulmonary complications was noted in the oximeter group. For those patients who required ICU transfer, the estimated cost from enrollment to completion of the study was less in the oximeter group ($15,481) than in the control group ($18,713) despite the older age and higher comorbidity of the former. The authors speculate that reduction in pulmonary transfers to the ICU may be due to the earlier recognition and treatment of post-operative pulmonary complications.
The lack of demonstrable benefit of pulse oximetry on outcome in clinical trials may be due to the signal-to-noise ratio 69). Because the outcome under evaluation (readmission to the ICU, myocardial infarction, or death) is rare, a huge number of patients are needed to show a reduction in these events 70). To demonstrate a reduction in complications in the study by Moller and colleagues, for example, a 23-fold increase in enrollment would have been required 71).
The fact that randomized trials failed to demonstrate that routine monitoring with pulse oximetry improved patient outcome has not stopped anesthesiologists from using pulse oximeters 72). When surveyed, 94 % of the anesthesiologists in the study by Moller and colleagues 73) considered the pulse oximeters to be helpful in guiding clinical management. They believed that maintaining oxygenation within the physiologic limits with the help of pulse oximetry might help avert irreversible injury. It is this perspective that has made pulse oximetry a crucial part of standard of care despite the absence of proven efficacy 74).
Oxyhemoglobin Dissociation Curve
The Oxyhemoglobin Dissociation curve shows how blood carries oxygen through the body. It also shows the relationship between SpO2 and PaO2 as determined by hemoglobin’s affinity for oxygen.
Here is a simple way of understanding the Oxyhemoglobin Dissociation curve.
Because oxygen does not dissolve easily in water very little of it can actually be carried directly in the plasma, only about 1.5%. The rest of it has to be combined with the hemoglobin in the blood in order to be transported. The oxygen and the hemoglobin have to bind together, and there are four heme groups which can each combine with one molecule of oxygen. When combined it is then known as oxyhemoglobin (O2Hb). When the oxygen binds from the hemoglobin this is known dissociation and there are several factors to take into consideration when considering binding and dissociation.
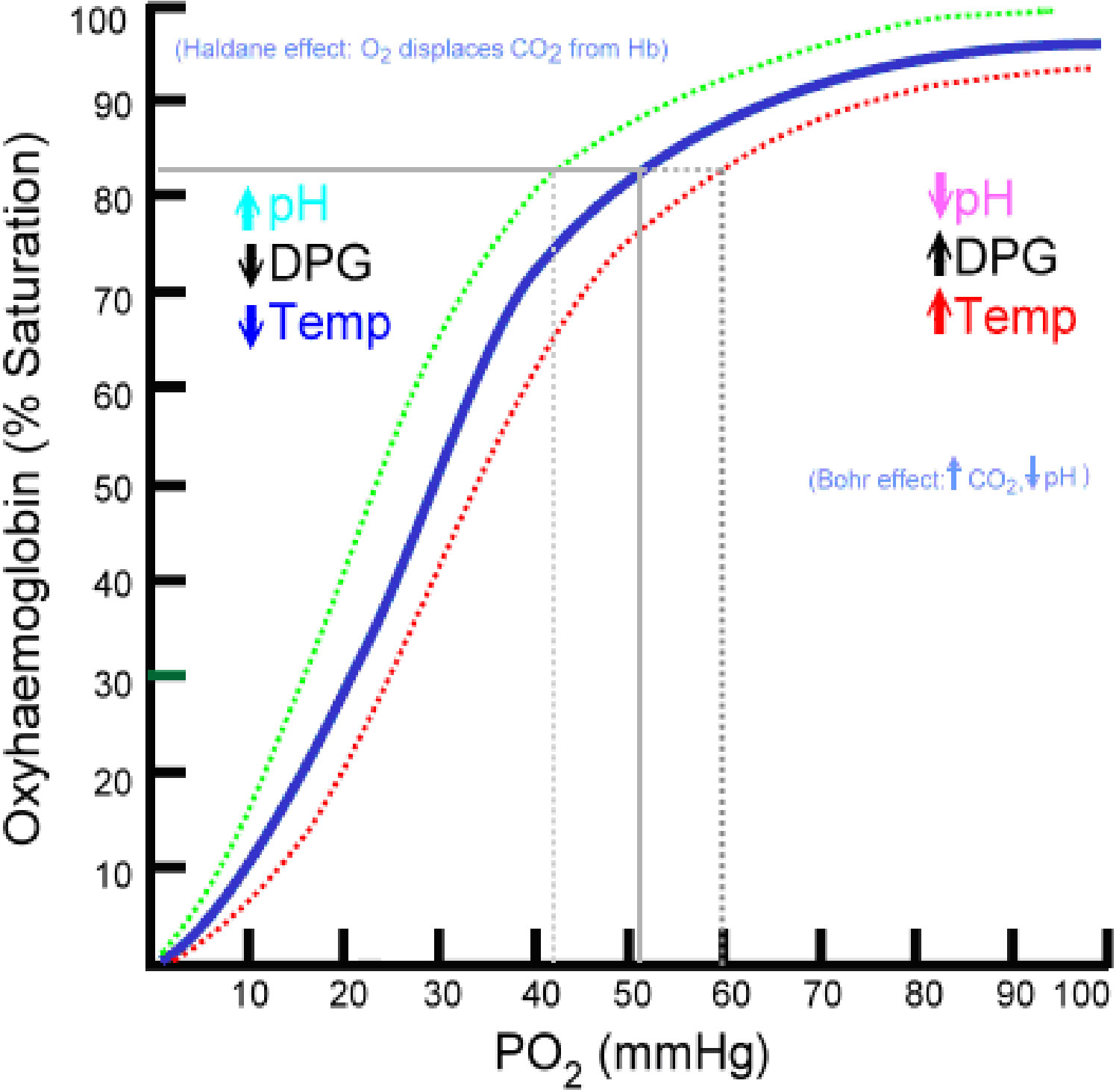
The partial pressure of oxygen (PO2) is the most important factor when considering how much oxygen combines with hemoglobin. When deoxyhemoglobin (HHb) is completely converted to oxyhemoglobin (O2Hb) it is said to be fully saturated, and when it contains a mixture of the two it is said to be only partially saturated. The relationship between the percentage saturation of hemoglobin and partial pressure of oxygen is illustrated in the Figure 1 below, this is usually known as the oxygen-hemoglobin dissociation curve.
Figure 1. Oxyhemoglobin Dissociation curve
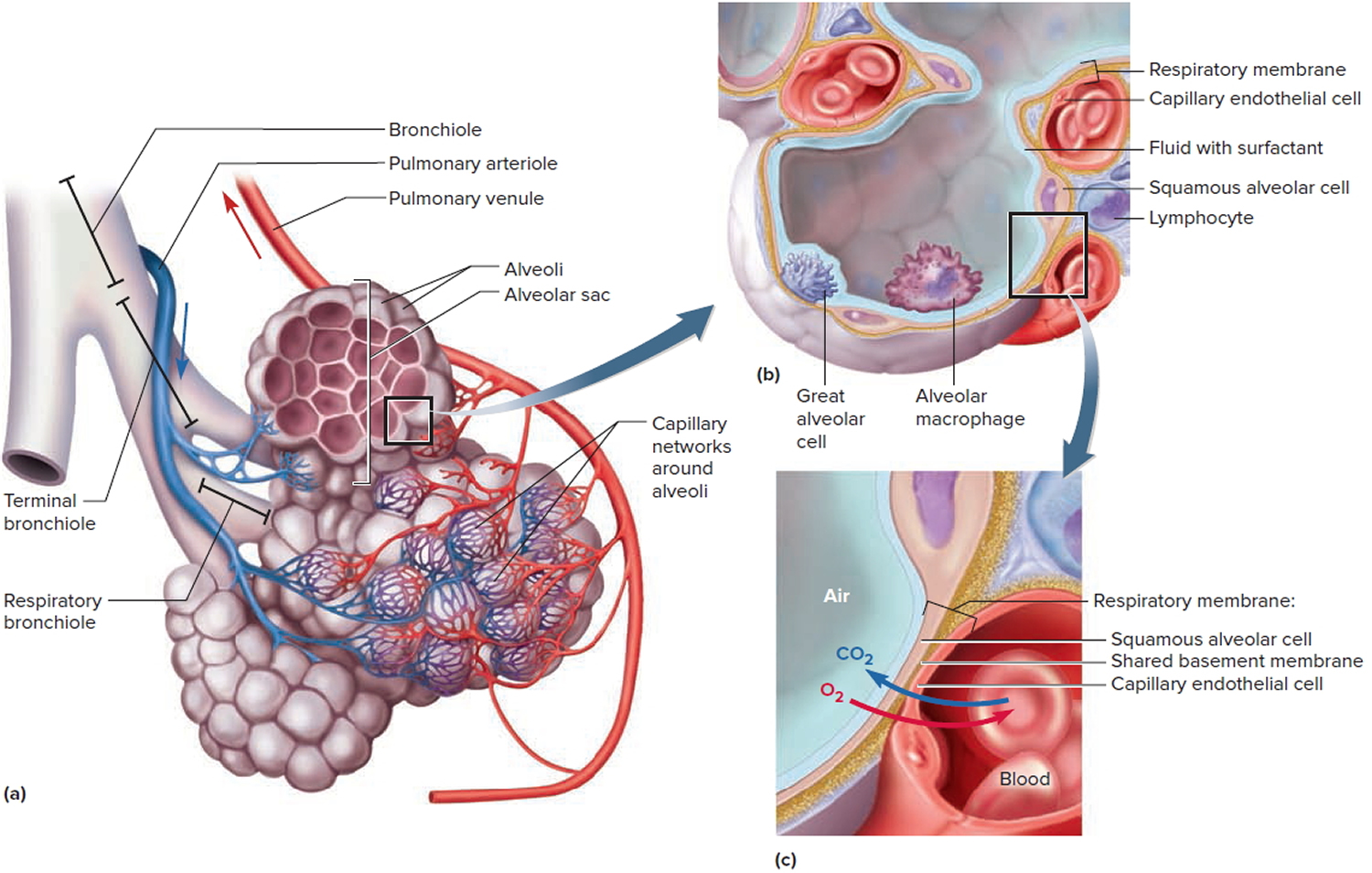
Figure 2. Lungs alveoli
Note: (a) Clusters of alveoli and their blood supply. (b) Structure of an alveolus. (c) Structure of the respiratory membrane.
You can see from the above that when the partial pressure of oxygen (PO2) is high, hemoglobin binds with large amounts of oxygen (O2) and is almost fully saturated. So the greater the partial pressure of oxygen the more oxygen will combine with hemoglobin.
You can also see from the above figure that the hemoglobin is still 90% or more saturated with oxygen even at partial pressures of between 60 to 100 mmHg. So the blood can still pick up nearly a full load of oxygen even when the alveoli partial pressure of oxygen (PAO2) is low.
As the partial pressure of oxygen becomes even lower, at 40 mmHg you can see that the percentage of hemoglobin saturated with oxygen drops off quite quickly. So large amounts of oxygen are released from hemoglobin at these partial pressures. This is important in some of the more active tissues where the partial pressure of oxygen can decrease well below 40 mmHg. The large amount of oxygen released as a consequence means that the tissues can continue to work.
Whilst the partial pressure of oxygen is the most important factor when considering the binding and dissociation to hemoglobin there are also a number of other factors to take into account;
- The pH of an environment is directly related to the number of hydrogen ions. Hydrogen ions alter the structure of hemoglobin decreasing its oxygen carrying capacity. The lowered pH therefore means that more oxygen is available for tissue cells as the pH will be lower here.
- Carbon dioxide can also bind to hemoglobin and therefore as the partial pressure of carbon dioxide rises the hemoglobin releases oxygen more readily. Thus an increased partial pressure of carbon dioxide producer a more acid environment that helps to split oxygen from hemoglobin.
- A raised temperature also tends to result in an increased amount of oxygen released from hemoglobin. As heat is a by product of cellular activity, and more active cells will generate more heat this will further promote the release of oxygen from the oxyhemoglobin.
- 2,3-biphosphoglycerate (2.3 DPG) is formed in red blood cells when they break down glucose. When this combines with hemoglobin the hemoglobin binds oxygen less tightly. So the greater the level, the more oxygen is released from hemoglobin. Some hormones such as epinephrine, and norepinephrine increase the formation of 2,3-biphosphoglycerate (2.3 DPG).
Carbon dioxide is carried by the blood in three main ways. A small amount is dissolved in plasma. This diffuses into the alveoli upon reaching the lungs.
More of it combines with the globin in hemoglobin.
But the greatest percentage of carbon dioxide is transported in plasma is bicarbonate ions. The carbon dioxide in the tissue capillaries reacts with water to form carbonic acid. This carbonic acid then dissociates into hydrogen ions and bicarbonate ions.
The Oxyhemoglobin Dissociation Curve
Venous blood has a PO2 of 40 and is generally referred to as PvO2. As more oxygen molecules enter the capillary bloodstream, this increases the PO2, and therefore increases reduced hemoglobin’s affinity for oxygen. It is here where the capillary system converts from being part of the unoxygenated venous system to the oxygenated arterial system.
As the PO2 of capillary blood increases, more and more oxygen molecules bind with hemoglobin until a majority of hemoglobin becomes completely saturated. A normal SpO2 value here is about 98%, or a range of 95-98%. An acceptable range is 90%. The capillary then becomes part of the arterial system, with its PO2 now being referred to as PaO2.
So, the curve has an s-shape because, at lower PO2s, oxygen binds to hemoglobin at a high rate, and this slows down as hemoglobin become more saturated. At PO2s above 60 the curve is relatively flat, meaning that the oxygen content of the blood will not change much with subsequent increases in PO2. In other words, the only way to get more oxygen to tissues would require adding more hemoglobin molecules to the blood, which would require a blood transfusion. Or, another simpler method would be to add more oxygen to the plasma by increasing the fraction of inspired oxygen (FiO2).
4-5-6-7-8-9 Rule. It is because of the Oxyhemoglobin Dissociation Curve that you can use SpO2 to estimate PaO2.
- PO2 40 = SpO2 70%
- PO2 50 = SpO2 80%
- PO2 60 = SpO2 90%
Because of normal variations in PAO2 (as explained above), the PaO2 may likewise vary. So, that said, the following is generally considered as true of PaO2.
- Normal: 80-100 mm Hg
- Hypoxemia: 60-80 mm Hg
- Severe Hypoxemia: 40-60 mm Hg
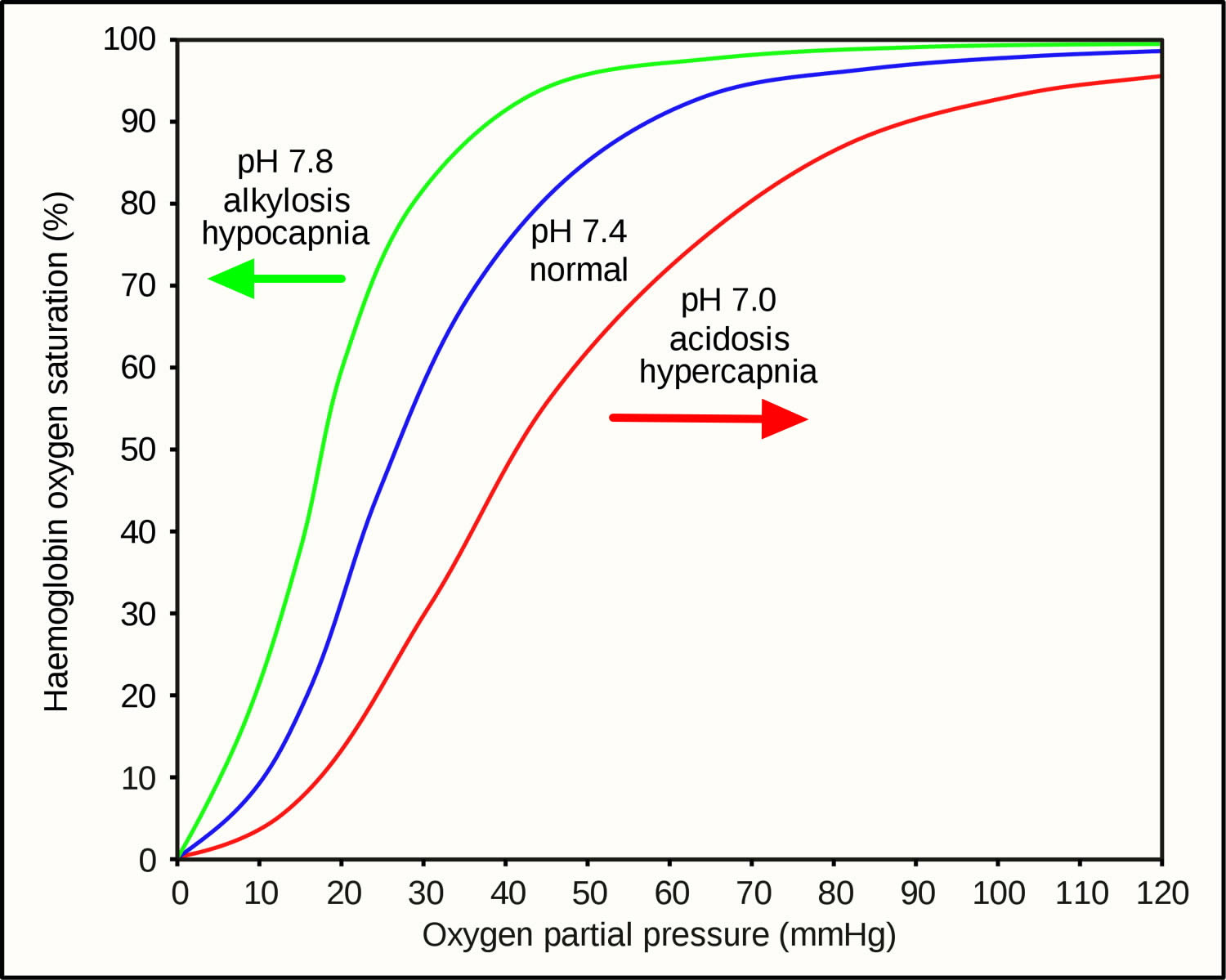
Shifting of the Oxyhemoglobin Dissociation Curve
Certain conditions cause hemoglobin to release more oxygen into the bloodstream, shifting the curve to the right; certain conditions cause hemoglobin to pick up more oxygen from the bloodstream, shifting the curve to the left. Both of these conditions will have a direct affect on SpO2 and PaO2
1) Shift to the right
The Oxyhemoglobin Dissociation Curve shifts to the right when hemoglobin has a decreased affinity for oxygen, and has a “harder” time making the bond with oxygen. This decreases hemoglobin’s affinity for oxygen, causing it to un-bond with hemoglobin and enter tissues.
- Lower SpO2 for a given PO2
- Requires a higher PO2 to achieve the desired SpO2
- Hemoglobin more likely to dump oxygen into tissues (active muscles need more oxygen)
- Heat. Anything that creates heat will move curve to right.
- Acidosis or low pH
- High CO2 causes Acidosis
- Exercise (heats up body)
- Increased 2,3-biphosphoglycerate (2.3 DPG)
2) Shift to the left
The curve shifts to the left when hemoglobin has an increased affinity for oxygen, and has an “easier” time making the bond with oxygen.
- Higher SpO2 for a given PO2
- Hemoglobin is more likely to cling to O2 and not let go (activity is minimal)
- Think Cold. The colder your body, the slower activity will be.
- Hypothermia (cold tissues)
- Rest (minimal exertion)
- Hypocarbia
- CO2 poisoning
- Alkalotic (tissues cold)
- Decreased 2,3-biphosphoglycerate (2.3 DPG)
- Fetal Hemoglobin (fetus needs less oxygen and can live off lower PO2s)
What is 2,3-biphosphoglycerate (2.3 DPG)?
It’s a substance in the blood that controls movement of oxygen from the blood to tissues.
Increasing 2.3 DPG: This is your bodies way of responding to lack of oxygen. It lowers hemoglobin’s affinity for oxygen, causing hemoglobin to release oxygen into the bloodstream for tissues to use. This moves the curve to the right. The following conditions cause the body to increase production of 2.3 DPG:
- Anemia (it may take 24 hours after transfusion to replenish supply, and return curve to normal)
- Chronic Obstructive Pulmonary Disease (COPD)
- Cystic Fibrosis
- Congenital heart diseases
- Anything that increases metabolism (heat), such as acidosis, exercise, fever, etc.
Decreasing 2.3 DPG: This results from lack of DPG enzymes to make 2.3 DPG. The body responds by increasing red blood cells (RBCs) that are weak and burst easy. This moves the curve to the left. When this happens your body will increase 2.3 DPG production to try to move it back to normal. The following conditions cause this:
- Erythrocytosis
- Anemia
- Large blood transfusion
The science behind Oxyhemoglobin Dissociation curve
Fick’s law: The rate of oxygen diffusion is proportionate to the concentration difference of oxygen and the surface area. In other words, it travels from areas of high pressure to areas of lower pressure. According to this law, a gas travels from areas of high pressure to areas of low pressure.
Since room air has a partial pressure of oxygen (PaO2) of 160, and alveoli have a PaO2 is 104, oxygen easily makes it’s way through the air passages to the alveoli. Similarly, venous capillary blood has a PaO2 of 40, so oxygen easily diffuses across the respiratory membrane to the capillary system. Capillary PaO2 now becomes 104, thus becoming part of the arterial circulation.
Henry’s Law: Gases dissolve in liquids in proportion to their partial pressures, depending also on how soluble they are in specific fluids and on the temperature. This is important because most oxygen inside the body is stored in fluid, such as blood. Inside the nose it is humidified, and the alveoli are saturated with water vapor which has its own partial pressure.
Total Pressure: This is the tension given off by a molecule of a gas if it were to be confined inside a container. The pressure is caused by movement of the molecules, and the pressure or tension they cause by constantly impacting the surface of the container. The total pressure of a gas is summed up by the total pressure of all the molecules contained in it.
Partial Pressure: This is the pressure exerted by a single gas component in a mixture. It is the pressure of an individual gas of a mixture. Partial Pressure of Oxygen is designated as PO2. PO2 after humidified and heated to normal body temperature (37°C): 149 mmHg. Partial Pressure of Alveolar Oxygen is designated as PAO2: 104 mmHg. Partial pressure of capillary venous blood (PvO2) is 40 mmHg.
So oxygen moves from the alveoli, across the respiratory membrane, to the capillary blood because of the pressure difference: 104-40 = 64 mmHg pressure difference.
This pressure difference, or pressure gradient, is perfect for oxygen diffusion to occur from the alveoli to the capillary system. So, oxygen molecules are released from the alveoli (PAO2 104 mmHg) into the venous capillary system (PvO2 O2 40 mmHg).
Dalton’s Law: The total pressure of a mixture of gases equals the sum of the partial pressures of the individual gases in that mixture.
Room Air contains about 79% nitrogen and 21% oxygen (There are other gases in the air, although they will be omitted here for to make this easier to understand). Usually, 21% is generally designated as the Fraction of Inspired Oxygen in Room Air.
Total Pressure of Atmospheric Air as sea level: 760 mmHg
- Partial Pressure of Nitrogen (PN2) in room air: 600 mmHg
- Partial Pressure of Oxygen (PO2) in room air: 160 mmHg
These pressures may vary depending on the temperature, humidity, and atmospheric pressure.
Affinity of Hemoglobin
Hemoglobin (Hb) is a protein present in red blood cells (erythrocytes). In the capillary system oxygen comes into contact with a reduced hemoglobin, or a hemoglobin that has no oxygen molecule on it. This makes it so the hemoglobin has a high attraction, or high affinity, for oxygen. Oxygen (O2) then binds with a hemoglobin
The amount of oxygen bound to hemoglobin at any time is based on the partial pressure of oxygen that it is exposed to. Since freshly oxygenated capillary blood has a PaO2 of 104 under normal conditions, reduced hemoglobin (hemoglobin that does not have oxygen) has a high affinity for it.
Some oxygen molecules will remain in the plasma, although a majority is picked up and transported by a hemoglobin molecule. The normal percentage of hemoglobin carrying oxygen is referred to as the oxygen saturation (SpO2), and a normal value is generally considered to be in the 95-98%. However, as you will soon see, 90% or greater can be considered acceptable.
Hemoglobin does not affect the partial pressure of oxygen, and so the PaO2 of arterial blood remains 104. The accepted range of PaO2 is generally considered to be in the 80-100 range. When a cell uses up it’s oxygen molecules, it has a PO2 that ranges somewhere around 22-35. As the hemoglobin approaches this cell with a lower PO2, it releases it’s hemoglobin. The cell on this end is said to have a high affinity for oxygen.
What does a pulse oximeter measure
Pulse oximetry is based on the principle that oxyhemoglobin (O2Hb) and deoxyhemoglobin (HHb) differentially absorb red and near-infrared light. It is fortuitous that oxyhemoglobin (O2Hb) and deoxyhemoglobin (HHb) have significant differences in absorption at red and near-infrared light because these two wavelengths penetrate tissues well whereas blue, green, yellow, and far-infrared light are significantly absorbed by non-vascular tissues and water 75). Oxyhemoglobin (O2Hb) absorbs greater amounts of infrared light and lower amounts of red light than does deoxyhemoglobin (HHb); this is consistent with experience – well-oxygenated blood with its higher concentrations of oxyhemoglobin (O2Hb) appears bright red to the eye because it scatters more red light than does deoxyhemoglobin (HHb). On the other hand, deoxyhemoglobin (HHb) absorb more red light and appears less red. Exploiting this difference in light absorption properties between oxyhemoglobin (O2Hb) and deoxyhemoglobin (HHb), pulse oximeters emit two wavelengths of light, red at 660 nm and near-infrared at 940 nm from a pair of small light-emitting diodes located in one arm of the finger probe. The light that is transmitted through the finger is then detected by a photodiode on the opposite arm of the probe; i.e., the relative amount of red and infrared light absorbed are used by the pulse oximeter to ultimately determine the proportion of hemoglobin (Hb) bound to oxygen.
The ability of pulse oximetry to detect SpO2 (peripheral oxygen saturation) of only arterial blood is based on the principle that the amount of red and infrared light absorbed fluctuates with the cardiac cycle, as the arterial blood volume increases during systole and decreases during diastole; in contrast, the blood volume in the veins and capillaries as well as the volumes of skin, fat, bone, etc, remain relatively constant. A portion of the light that passes through tissues without being absorbed strikes the probe’s photodetector and, accordingly, creates signals with a relatively stable and non-pulsatile “direct current” (DC) component and a pulsatile “alternating current” (AC) component (Figure 4A). A cross-sectional diagram of an artery and a vein during systole and diastole illustrates the non-pulsatile (DC) and pulsatile (AC) compartments of arteries and the relative absence of volume change in veins and capillaries (Figure 4B). Pulse oximeters use amplitude of the absorbances to calculate the Red:IR Modulation Ratio (R) 76); i.e., R = (Ared,AC/Ared,DC)/(AIR,AC/AIR,DC) where A = absorbance; in other words, R is a double-ratio of the pulsatile and non-pulsatile components of red light absorption to infrared light absorption. At low arterial oxygen saturations, where there is increased HHb, the relative change in amplitude of the red light absorbance due to the pulse is greater than the IR absorbance, i.e., Ared,AC > AIR,AC, resulting in a higher R value; conversely, at higher oxygen saturations, AIR,AC > Ared,AC and the R value is lower (Figure 4C). A microprocessor in pulse oximeters uses this ratio (calculated over a series of pulses) to determine the SpO2 based on a calibration curve that was generated empirically by measuring R in healthy volunteers whose saturations were altered from 100% to approximately 70%5 (Figure 4C). Thus, SpO2 readings below 70% should not be considered quantitatively reliable although it is unlikely any clinical decisions would be altered based on any differences in SpO2 measured below 70% 77).
How pulse oximeters exclude the influence of venous and capillary blood and other stationary tissues from the calculation of SpO2 can be conceptually understood by examining the Beer–Lambert Law of absorbance. According to the Beer–Lambert Law as applied to a modeled blood vessel, A = ɛbc where A = absorbance, ɛ = absorption (or extinction) coefficient of hemoglobin at a specified wavelength (a combination of the O2Hb and HHb coefficients), b = pathlength traveled by the emitted light through the blood vessel, and c = concentration of Hb. Simply measuring absolute absorbance would be an inaccurate estimate of arterial SpO2 since elevated levels of HHb in the venous blood would also contribute to the measured value. However, a pulse oximeter is able to determine only arterial SpO2 by measuring changes in absorbance over time. To illustrate this concept mathematically, the total absorbance (At) can be thought of as a linear combination of venous (Av) and arterial (Aa) absorbances (At = Av + Aa = ɛvbvcv + ɛabaca). Since pulse oximeters measure absorbance with respect to time, the derivative of the previous equation becomes dAt/dt = d(ɛvbvcv)/dt + d(ɛabaca)/dt. Since ɛ and c are constants (note that ɛ can vary depending on the wavelength of light, but is a constant for any particular wavelength and Hb species), the previous equation simplifies to dAt/dt = (dbv/dt)(ɛvcv) + (dba/dt)(ɛaca). Since arteries dilate and constrict much more than veins, i.e., the change in ba ≫ the change in bv (dba/dt ≫ dbv/dt), we can assume bv as a constant and dbv/dt = 0; hence, the previous equation simplifies to dAt/dt = (dba/dt)(ɛaca), or equivalently ΔAt = ΔAa; in other words, the change in At measured = change in absorbance due to the arterial blood content with little or no contribution by the venous blood. Therefore, an adequate pulse is necessary for pulse oximeters to work and is the basis for the well-known fact that attempting to measure SpO2 in regions with little or no blood perfusion will result in absent or inaccurate readings 78).
Figure 4. What a pulse oximeter measure
Footnotes:
Schematic diagram of light absorbance by a pulse oximeter. (A) In a person with good cardiac function, the onset of the cardiac systole, as denoted by the onset of the QRS complex coincides with the onset in the increase of the arterial blood volume. The amount of red and IR light absorbed in the arterial compartment also rises and fall with systole and diastole, respectively, due to the increase and decrease in blood volume. The volume that increases with systole is also known as the pulsatile or “alternating current” (AC) compartment and the compartment in which the blood volume does not change with the cardiac cycle is known as the non-pulsatile or “direct current” (DC) compartment. (B) A cross-sectional diagram of an artery and a vein displaying the pulsatile (AC) and non-pulsatile (DC) compartments of the blood vessels. Note that only the artery has a pulsatile (AC) component. (C) A diagram of a calibration (standard) curve of the Red:IR Modulation Ratio in relation to the SpO2. Increased red light absorbance (increased R) is associated with increased deoxyhemoglobin, i.e., lower SpO2.
How does a pulse oximeter work
Pulse oximetry is based on two physical principles:
- The presence of a pulsatile signal generated by arterial blood, which is relatively independent of non-pulsatile arterial blood, venous and capillary blood, and other tissues; and
- The fact that oxyhemoglobin (O2Hb) and deoxyhemoglobin (HHb) have different absorption spectra 79).
Currently available oximeters measures oxygen saturation by using two light-emitting diodes (LEDs) that emit light at the 660 nm (red) and the 940 nm (infrared) wavelengths by illuminating the skin 80). These two wavelengths are used because oxyhemoglobin (O2Hb) and deoxyhemoglobin (HHb) have different absorption spectra at these particular wavelengths (see Figure 4). In the red region, oxyhemoglobin (O2Hb) absorbs less light than reduced hemoglobin (Hb), while the reverse occurs in the infrared region. The ratio of absorbance at these wavelengths is calibrated empirically against direct measurements of arterial blood oxygen saturation (SaO2) in volunteers, and calibrated against direct measurements of arterial oxygen saturation (SaO2) to establish the pulse oximeter’s measure of arterial saturation (SpO2) and the resulting calibration algorithm is stored in a digital microprocessor within the pulse oximeter. During subsequent use, the calibration curve is used to generate the pulse oximeter’s estimate of arterial saturation SpO2 (peripheral oxygen saturation) 81). In addition to the digital readout of O2 saturation, most pulse oximeters display aplethysmographic waveform which can help clinicians distinguish an artifact from the true signal (Figure 5).
Figure 5. How pulse oximeter work – transmitted light absorbance spectra of four hemoglobin species: oxyhemoglobin, reduced hemoglobin, carboxyhemoglobin, and methemoglobin
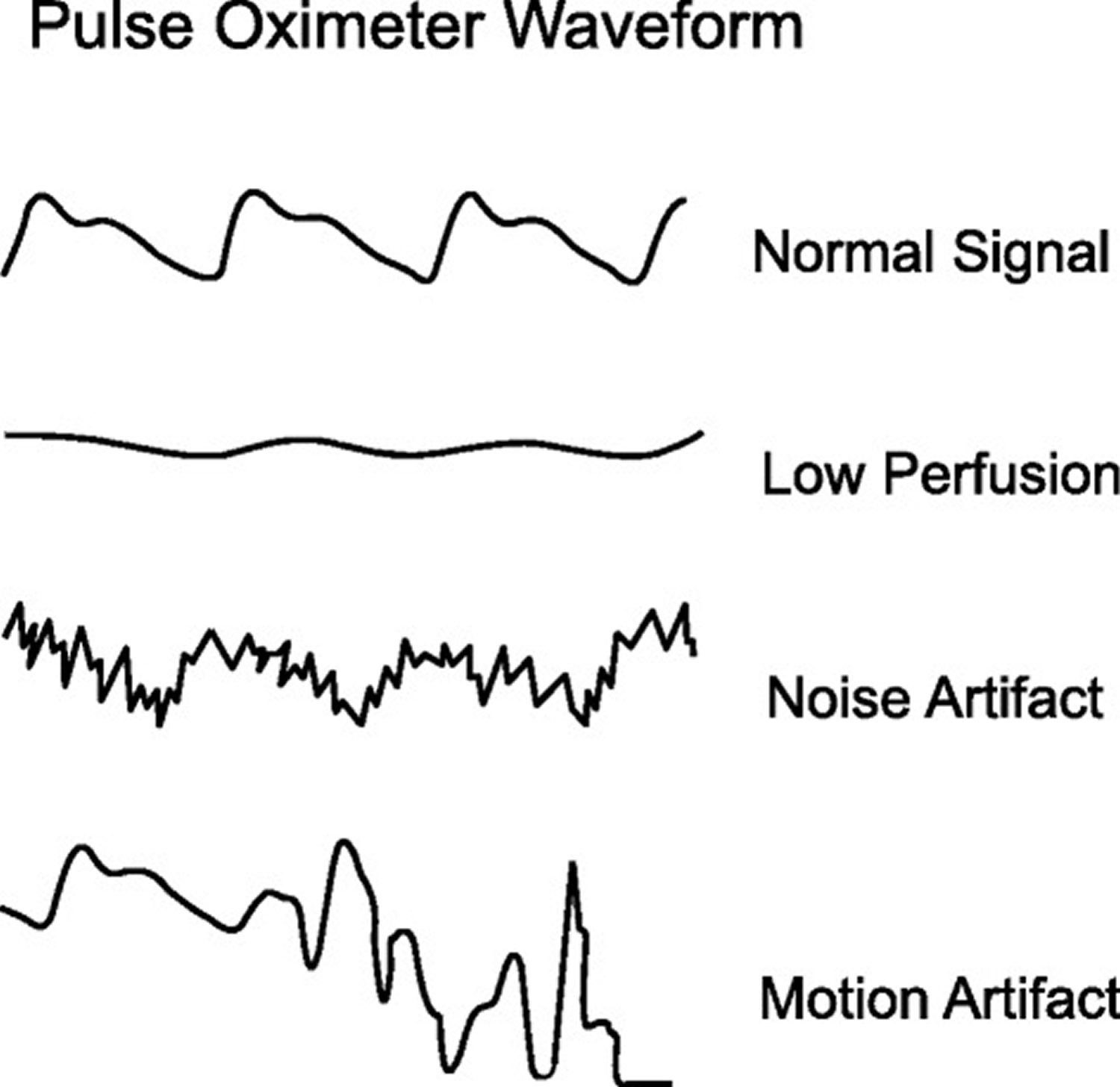
Figure 6. Common pulsatile signals on a pulse oximeter
Footnotes: (Top panel) Normal signal showing the sharp waveform with a clear dicrotic notch. (Second panel) Pulsatile signal during low perfusion showing a typical sine wave. (Third panel) Pulsatile signal with superimposed noise artifact giving a jagged appearance. (Bottom panel) Pulsatile signal during motion artifact showing an erratic waveform.
Pulse oximeter accuracy
The accuracy of commercially available oximeters differ widely, probably because of the different algorithms employed in signal processing 82). These algorithms are limited by the range of saturations that can be safely obtained in volunteers, and also the accuracy of the measurement standard 83). Comparison of pulse oximetry with direct CO-oximeter measurements should be reported in terms of the mean difference between the two techniques (bias) and the standard deviation of the differences (precision).
In healthy volunteers, oximeters commonly have a mean difference (bias) of < 2% and a standard deviation (precision) of < 3% when SaO2 is 90% or above 84). Comparable results have also been obtained in critically ill patients with good arterial perfusion 85). Accuracy of pulse oximeters deteriorates when SaO2 falls to 80% or less. In healthy volunteers under hypoxic conditions, bias of pulse oximetry varies from -15.0 to 13.1 while the precision ranges from 1.0 to 16.0 86). In a study in critically ill patients, eight out of 13 oximeters had a bias ≥ ± 5% when SaO2 was < 80% 87). In a study of 54 ventilator-dependent patients, the accuracy of oximetry deteriorated significantly at low SaO2 values. Bias ± precision was 1.7 ± 1.2% for SaO2 values > 90%, and it increased to 5.1 ± 2.7% when SaO2 was ≤ 90% 88).
Different probes that are used with a pulse oximeter can also affect the accuracy of SpO2 (peripheral oxygen saturation) measurements. In patients with poor peripheral perfusion as a consequence of cardiopulmonary bypass surgery, finger probes had lower precision and more readings within 3% of the reference (CO-oximeter) than the other probes. Overall rankings were significantly better for the finger probes than probes on other sites 89). The response time of oximeter probes was assessed by Severinghaus and Naifeh 90) who induced 30-60s hypoxic plateaus between an SaO2 of 40 and 70% in healthy volunteers. Oximeter probes placed on the ear generally had a much faster response to a sudden decrease in fractional inspired oxygen concentration (FiO2) than did the finger probes (10-20 versus 24-35s, respectively). Employing hypobaric facility to induce hypoxia in normal volunteers, Young et al. 91) also observed that the response time of the finger probes were slower than the ear probes in response to either a decrease or increase in O2 saturation.
Figure 7. The response time of the conventional finger probe with the reflectance forehead probe in patients undergoing general anesthesia
Pulse oximeter limitations
Pulse oximeters have a number of limitations which may lead to inaccurate readings. Pulse oximeters measure SaO2 (arterial blood oxygen saturation) that is physiologically related to arterial oxygen tension (PaO2) according to the oxyhemoglobin (O2Hb) dissociation curve. Because the oxyhemoglobin (O2Hb) dissociation curve has a sigmoid shape, oximetry is relatively insensitive in detecting the development of hypoxemia in patients with high baseline levels of PaO2 92).
Limitations of pulse oximetry:
- Shape of oxygen dissociation curve
- Carboxyhemoglobin (COHb)
- Methemoglobin (MetHb)
- Anemia
- Dyes
- Nail polish
- Ambient light
- False alarms
- Motion artifact
- Skin pigmentation
- Low perfusion state
- Limited knowledge of the technique
Pulse oximeters employ only two wavelengths of light and, thus, can distinguish only two substances, deoxyhemoglobin (HHb) and oxyhemoglobin (O2Hb). When carboxyhemoglobin (COHb) and methemoglobin (MetHb) are also present, four wavelengths are required to determine the ‘fractional SaO2’: i.e., (O2Hb × 100)/(Hb + O2Hb + COHb + MetHb). In the presence of elevated carboxyhemoglobin (COHb) levels, oximetry consistently over- estimated the true SaO2 93) by the amount of COHb present. Elevated methemoglobin (MetHb) levels also may cause inaccurate oximetry readings 94). Accordingly, multiwavelength oximeters that are capable of estimating blood levels of COHb and MetHb have recently been designed 95). In healthy volunteers, the accuracy of a multiwavelength oximeter (Masimo Rainbow-SET Rad-57 Pulse CO-oximeter; Masimo Corporation, Irvine, CA, USA) in measuring dyshemoglobins was evaluated by inducing carboxyhemoglobinemia (levels range from 0 % to 15 %) and methemoglobinemia (levels range from 0 % to 12 %) 96). Bias between COHb levels measured with the pulse CO-oximeter and COHb levels measured with the laboratory CO-oximeter (standard method) was −1.22 %; the corresponding precision was 2.19 %. Bias ± precision of MetHB measured with the pulse CO-oximeter and MetHb measured with the laboratory CO-oximeter was 0.0 % ± 0.45 %. The accuracy of pulse CO-oximeters in measuring COHb levels was also assessed during hypoxia 97). In 12 healthy volunteers, the pulse CO-oximeter was accurate in measuring COHb at an SaO2 of less than 95 % (bias of −0.7 % and precision of 4.0 %); however, when the SaO2 dropped below 85%, the pulse CO-oximeter was unable to measure COHb levels. In patients evaluated in the emergency department with suspected carbon monoxide poisoning, the bias between pulse CO-oximetric measurement of COHb and laboratory CO-oximetric measurement of COHb was less than 3 % 98). The limits of agreement between the measurements, however, were large (−11.6 % to 14.14 %) 99), leading some authors to conclude that these new pulse CO-oximeters may not be used interchangeably with standard laboratory measurements of COHb 100).
Anemia does not appear to affect the accuracy of pulse oximetry: in non-hypoxemic patients with acute anemia (mean Hb, 5.2 ± 0.3 g/dl), pulse oximetry was accurate in measuring O2 saturation with a bias of only 0.53% 101). However, in patients with sickle cell anemia presenting with acute vasoocclusive crisis 102), mean bias of pulse oximetry was 4.5% (in some patients it was as high as 8%), which was significantly greater than in a control group of patients without sickle cell anemia. Severe hyperbilirubinemia (mean bilirubin, 30.6 mg/dl) does not effect the accuracy of pulse oximetry 103).
Intravenous dyes such as methylene blue, indocyaninegreen, and indigocarmine can cause falsely low SpO2 readings 104), an effect that persists for up to 20 min 105). Nail polish, if blue, green or black, causes inaccurate SpO2 readings 106),whereas acrylic nails do not interfere with pulse oximetry readings 107). Falsely low and high SpO2 readings occur with fluorescent and xenon arc surgical lamps 108).
Motion artifact continues to be a significant source of error and false alarms 109). In a recent, prospective study in an intensive care unit (ICU) setting, SpO2 signals accounted for almost 86% of a total 2,942 false alarms 110). In 123 patients recovering from general or spinal-epidural anesthesia, 77% of pulse oximeter alarms were false in nature, which the investigators attributed to sensor displacement,motion artifact, and a decrease in skin perfusion 111). In this study, the alarm threshold was set at an SpO2 of 90% and it is not clear if a minimum duration was specified. A recent study in 647 patients in the recovery room compared the influence of two pulse oximeter lower alarm limit settings (SpO2 90% = group 90 and SpO2 85% = group 85) on the incidence of hypoxemia 112). Although the number of audible alarms wa slower in group 85, hypoxic episodes (defined asSpO2 ≤ 90% lasting > 1 min) were more common in group 90 than in group 85 (11 versus 6%, respectively). The investigators concluded that decreasing the alarm limit to reduce false alarms may lead to increase in more relevant episodes of hypoxemia.
Various methods have been employed to reject motion artifact but have met with little success 113). An innovative technological approach, termed Masimo signal extraction technology (SET™;Masimo Corporation, Mission Viejo, California, USA), was recently introduced to extract the true signal from artifact due to noise and low perfusion 114). This technique incorporates new algorithms for processing the pulse oximeter’s red and infrared light signals that enable the noise component, which is common to the two wavelengths, to be measured and subtracted. When tested in healthy volunteers during standardized motion, Masimo SET™ exhibited much lower error rates (defined as percentage of time that the oximeter error exceeded 5%, 7%, and 10%) and dropout rates (defined as the percentage of time that the oximeter provided no SpO2 data) than did the Nellcor N-200 and Nellcor N-3000 oximeters (Nellcor Puritan Bennett, Pleasanton, California, USA)for all test conditions 115). The lowest performance index (defined as the percentage of time that the oximeter’s value was within 7% of the control SpO2 value) was 97% for Masimo SET™ compared with 47% for the N-3000 and 68% for the N-200. In 50 postoperative patients, Dumas et al 116) observed that a pulse oximeter’s alarm frequency was decreased two fold with a Masimo SET™ system versus a conventional oximeter (Nellcor N-200). Improved performance was particularly striking during conditions of gross (non-rhythmic) motion and tremor, when a 22-fold reduction in signal loss over time was observed.
Inaccurate oximetry readings have been observed in pigmented patients, but not by all investigators 117). In 33 healthy black subjects during normoxia and hypoxia, the correlation between SpO2 and SaO2 was inferior with a Biox IIA oximeter (Ohmeda, Boulder, Colorado, USA) than with the older Hewlett-Packard (Waltham, Massachusetts, USA) (non-pulse) oximeter 118). In critically ill patients 119), bias ± precision was greater in black patients, 3.3 ± 2.7%, than in white patients, 2.2 ±1.8%; also, a bias > 4% occurred more frequently in black patients (27%) than in white patients (11%).
Low perfusion states, such as low cardiac output, vasoconstriction and hypothermia, may impair peripheral perfusion and may make it difficult for a sensor to distinguish a true signal from background noise. In cardiac surgery patients experiencing hypothermia and poor perfusion, only two of 20 oximeters (Criticare CSI 503, Criticare Systems, Inc., Milwaukee, Wisconsin, USA; DatexSatlite, Datex Instrumentarium Corp., Helsinki, Finland) provided measurements within ± 4% of the CO-oximeter value 120). Measurements of SpO2 with a Biox 3700 oximeter had a bias > ± 4% in 37% of patients receiving vasoactive therapy 121).
An under-recognized and worrisome problem with pulse oximetry is that many users have a limited understanding of how it functions and the implications of its measurements. In a recent survey 122), 30% of physicians and 93%of nurses thought that the oximeter measured PaO2. Some clinicians also have a limited knowledge of the Oxyhemoglobin Dissociation curve and they do not recognize that SpO2 values in the high 80s represent seriously low values of PaO2. In the above survey, some doctors and nurses were not especially worried about patients with SpO2 values as low as 80% (equivalent to PaO2 ≤ 45 mmHg).
References [ + ]