Contents
- What is a Pap smear
- Importance of being screened for cervical cancer
- Pap smear procedure
- How Pap smear test results are reported
- Abnormal Pap smear results
- The HPV DNA Test
- Cancers linked to HPV infection
- Can HPV infection be prevented?
- Can a vaccine help prevent HPV?
- Who should be vaccinated against HPV and when?
- Why should the vaccines be given to pre-teens?
- What about men and women older than 26? Should they get one of the vaccines?
- Who should not get one of the HPV vaccines or who should wait?
- Is HPV testing needed before getting the vaccine?
- How long will the vaccines prevent HPV infection?
- Are HPV vaccines safe?
- Do women who have been vaccinated against HPV still need Pap smear tests?
- Will HPV affect my pregnancy or my baby?
- What is a cervix
- Pap smear guidelines
- Abnormal pap smear causes
- Types of cervical cancer
- Risk Factors for Cervical Cancer
- Human papillomavirus (HPV) infection
- Smoking
- Having a weakened immune system
- Chlamydia infection
- A diet low in fruits and vegetables
- Being overweight
- Long-term use of oral contraceptives (birth control pills)
- Intrauterine device (IUD) use
- Having multiple full-term pregnancies
- Being younger than 17 at your first full-term pregnancy
- Economic status
- Diethylstilbestrol (DES)
- Having a family history of cervical cancer
- Can HPV infection be prevented?
What is a Pap smear
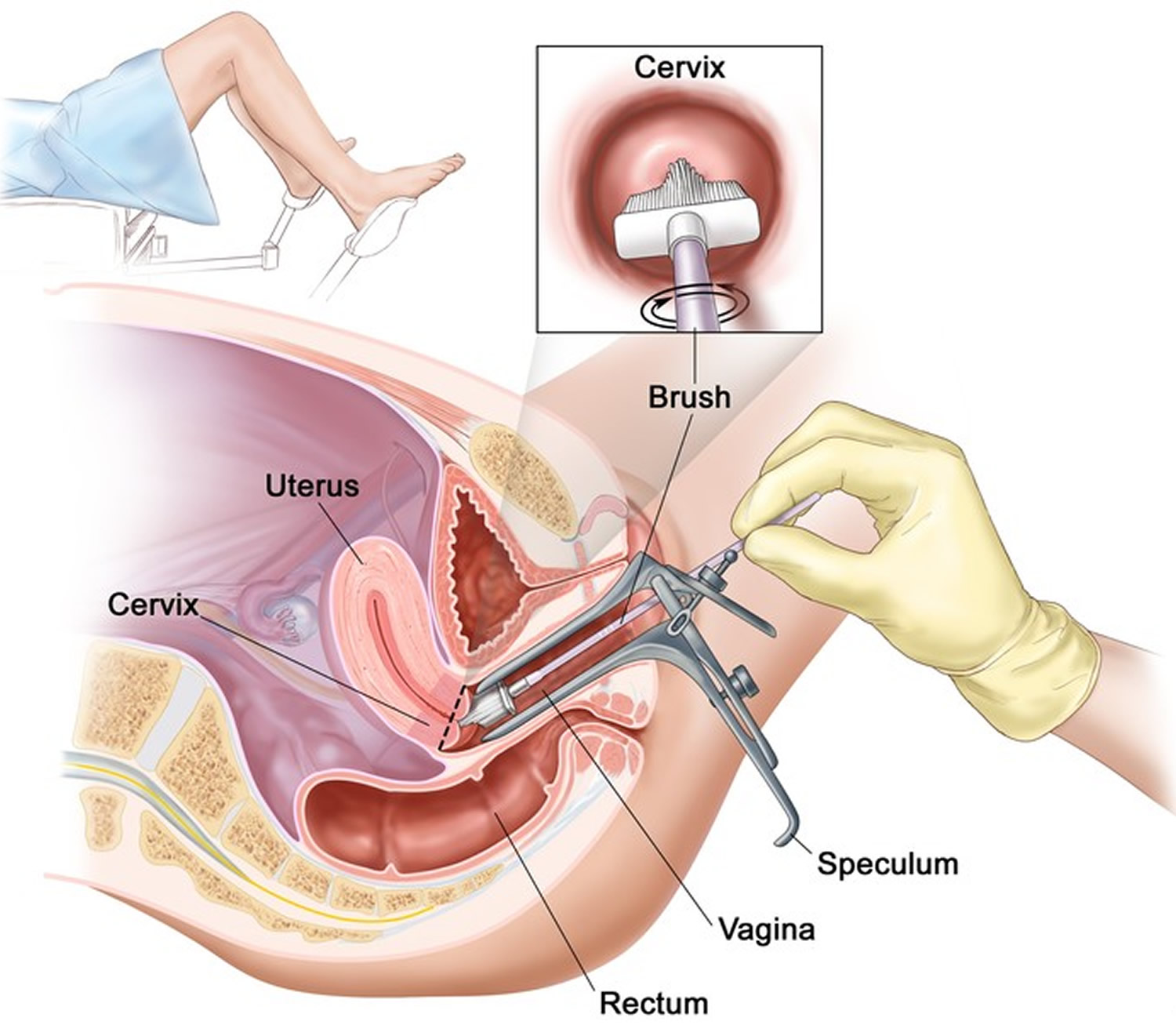
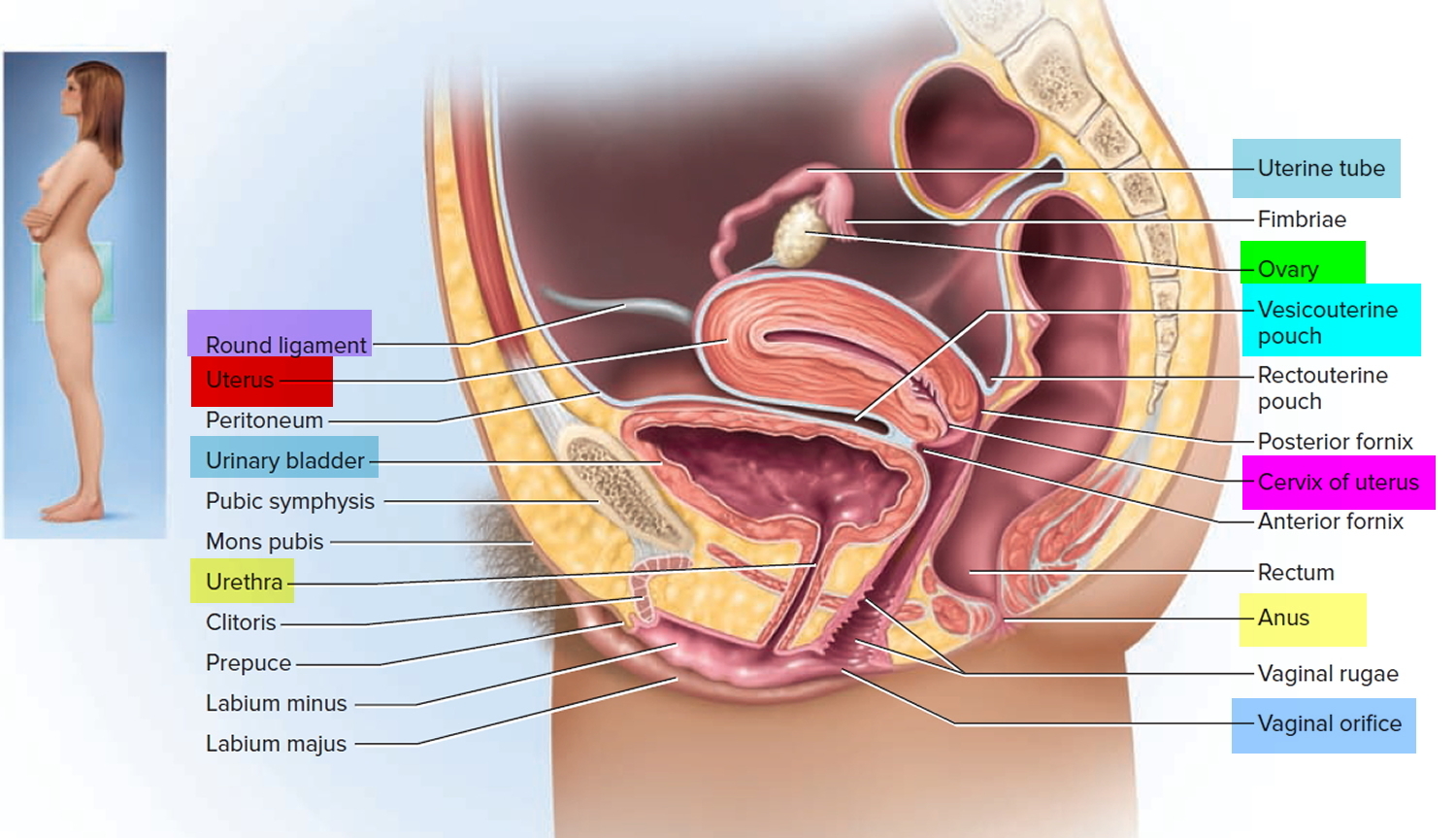
A Pap smear test is a routine screening test for early diagnosis of cervical cancer. Pap smear checks the cervix for abnormal cell changes. The cervix is the lower part of the uterus (womb), which opens into the vagina (see Figures 1 to 6). Cell changes can develop on the cervix that, if not found and treated, can lead to cervical cancer. Cervical cancer can almost always be prevented and having regular Pap smear tests is the key. The purpose of a Pap smear is to collect cells from your cervix, which is the lower end of your uterus. The cells collected in a Pap smear can detect if you have cervical cancer or suspicious cells that indicate you may develop cervical cancer.
The most common form of cervical cancer starts with pre-cancerous changes and there are ways to stop this disease from developing. The first way is to find and treat pre-cancers before they become true cancers, and the second is to prevent the pre-cancers.
Most women ages 21 to 65 should get regular Pap smear tests every 3 years as part of routine health care. Even if you are not currently sexually active, you should still have a Pap smear test. Women who have gone through menopause (when a woman’s periods stop) and are younger than 65 still need regular Pap smear tests.
Women who do not have a cervix (usually because of a hysterectomy), and who also do not have a history of cervical cancer or abnormal Pap smear results, do not need Pap smear tests. Women ages 65 and older who have had three normal Pap smear tests in a row and no abnormal test results in the last 10 years do not need Pap smear tests.
Your doctor can do a Pap smear test during a pelvic exam. It is a simple and quick test. You will lie down on an exam table. Your doctor will put an instrument called a speculum into your vagina and will open it to see your cervix (see Figure 1). He or she will then use a special stick or brush to take a few cells from the surface of and inside the cervix. The cells are placed on a glass slide and sent to a lab for testing. A Pap smear test may be mildly uncomfortable but should not be painful. You may have some spotting afterwards.
What does a pap smear test check for?
The Pap smear test is a procedure used to collect cells from the cervix so that they can be looked at under the microscope to find cancer and pre-cancer cells.
Importance of being screened for cervical cancer
Screening tests offer the best chance to have cervical cancer found early when successful treatment is likely. Screening can also actually prevent most cervical cancers by finding abnormal cervical cell changes (pre-cancers) so that they can be treated before they have a chance to turn into a cervical cancer.
If it’s found early, cervical cancer is one of the most successfully treatable cancers. In the United States, the cervical cancer death rate declined by more than 50% over the last 30 years. This is thought to be mainly due to the effectiveness of screening with the Pap smear test. Cervical cancer deaths in the United States have decreased dramatically since the implementation of widespread cervical cancer screening, and continue to decline, from 2.8 deaths per 100,000 women in 2000 to 2.3 deaths per 100,000 women in 2014 1). Most cases of cervical cancer occur in women who have not been adequately screened 2). Strategies that aim to ensure that all women are appropriately screened and receive adequate followup are most likely to be successful in further reducing cervical cancer incidence and mortality in the United States.
Despite the recognized benefits of cervical cancer screening, not all American women get screened. Most cervical cancers are found in women who have never had a Pap smear test or who have not had one recently. Women without health insurance and women who have recently immigrated are less likely to have cervical cancer screening.
Why do I need a Pap smear test?
A Pap smear test can save your life. It can find early signs of cervical cancer. If caught early, the chance of successful treatment of cervical cancer is very high. Pap smear tests can also find abnormal cervical cells before they turn into cancer cells. Treating these abnormal cells can help prevent most cases of cervical cancer from developing. Getting a Pap smear test is one of the best things you can do to prevent cervical cancer.
Benefits of early cervical cancer detection and treatment
The draft U.S. Preventive Services Task Force report 3) found convincing evidence that screening women ages 21 to 65 years substantially reduces cervical cancer incidence and mortality. In women ages 21 to 29 years, screening every 3 years with cytology alone substantially reduces cervical cancer incidence and mortality. In women ages 30 to 65 years, screening every 3 years with cytology alone or every 5 years with high-risk human papillomavirus (hrHPV) testing alone substantially reduces cervical cancer incidence and mortality.
The draft U.S. Preventive Services Task Force report 4) found adequate evidence that screening women older than age 65 years who have had adequate prior screening and are not otherwise at high risk for cervical cancer provides little benefit.
The draft U.S. Preventive Services Task Force report 5) found adequate evidence that screening women younger than age 21 years does not reduce cervical cancer incidence and mortality compared with beginning screening at age 21 years.
The draft U.S. Preventive Services Task Force report 6) found convincing evidence that screening women who have had a hysterectomy with removal of the cervix for indications other than a high-grade precancerous lesion or cervical cancer provides no benefit.
Harms of Pap smear screening
Screening with cervical cytology or high-risk human papillomavirus (hrHPV) testing can lead to harms, including more frequent followup testing and invasive diagnostic procedures (e.g., colposcopy and cervical biopsy), as well as unnecessary treatment in women with false-positive results. Evidence from randomized, controlled trials (RCTs) and observational studies indicate that harms from diagnostic procedures include vaginal bleeding, pain, infection, and failure to diagnose (due to inadequate sampling). Abnormal screening test results are also associated with psychological harms. In particular, women who received positive high-risk human papillomavirus (hrHPV) results reported greater distress and lower satisfaction with past and current sexual partners than women who received abnormal cytology results.
Harms of Treatment
The harms of treatment include risks from the treatment procedure and the potential downstream consequences of treatment. Evidence from observational studies indicates that certain treatments for precancerous lesions (e.g., cold-knife conization and loop excision) are associated with subsequent adverse pregnancy outcomes, such as preterm delivery and related complications 7). The draft U.S. Preventive Services Task Force report 8) found convincing evidence that many precancerous cervical lesions will regress, and that other lesions are indolent and slow-growing and will not become clinically important over a woman’s lifetime; identification and treatment of these lesions constitute overdiagnosis. Estimating the precise magnitude of overdiagnosis associated with any screening or treatment strategy is difficult, but it is of concern because it confers no benefit and leads to unnecessary surveillance, diagnostic tests, and treatments, with associated harms.
The draft U.S. Preventive Services Task Force report 9) found adequate evidence that the harms of screening for cervical cancer with cytology alone or high-risk human papillomavirus (hrHPV) testing alone in women ages 30 to 65 years are moderate. Screening strategies that include high-risk human papillomavirus (hrHPV) testing are slightly more sensitive than those that include cytology alone but also yield more false-positive results.
The draft U.S. Preventive Services Task Force report 10) found adequate evidence that the harms of screening for cervical cancer in women older than age 65 years who have had adequate prior screening and are not otherwise at high risk are at least small.
The draft U.S. Preventive Services Task Force report 11) found adequate evidence that the harms of screening for cervical cancer in women younger than age 21 years are moderate.
The draft U.S. Preventive Services Task Force report 12) found adequate evidence that screening for cervical cancer in women who have had a hysterectomy and do not have a history of a high-grade precancerous lesion or cervical cancer is associated with harms.
U.S. Preventive Services Task Force Assessment
The draft U.S. Preventive Services Task Force report 13) concludes with high certainty that the benefits of screening every 3 years with cytology alone substantially outweigh the harms in women ages 21 to 29 years. The draft U.S. Preventive Services Task Force report 14) concludes with high certainty that the benefits of screening every 3 years with cytology alone or every 5 years with hrHPV testing alone outweigh the harms in women ages 30 to 65 years.
The draft U.S. Preventive Services Task Force report 15) concludes with moderate certainty that the benefits of screening do not outweigh the potential harms in women older than age 65 years who have had adequate prior screening and are not otherwise at high risk for cervical cancer.
The draft U.S. Preventive Services Task Force report 16) concludes with moderate certainty that the harms of screening outweigh the benefits in women younger than age 21 years.
The draft U.S. Preventive Services Task Force report 17) concludes with high certainty that the harms of screening outweigh the benefits in women who have had a hysterectomy with removal of the cervix for indications other than a high-grade precancerous lesion or cervical cancer.
How often do I need to get a Pap test?
It depends on your age and health history. Talk with your doctor about what is best for you. Most women can follow these guidelines:
- If you are between ages 21 and 29, you should get a Pap smear test every 3 years.
- If you are between ages 30 and 64, you should get a Pap smear test and human papillomavirus (HPV) test together every 5 years or a Pap smear test alone every 3 years.
- If you are 65 or older, ask your doctor if you can stop having Pap smear tests.
Some women may need more frequent Pap smear tests. You should talk to your doctor about getting a Pap smear test more often if:
- You have a weakened immune system because of organ transplant, chemotherapy, or steroid use.
- Your mother was exposed to diethylstilbestrol (DES) while pregnant.
- You have had treatment for abnormal Pap smear results or cervical cancer in the past.
- You are HIV-positive. Women who are living with HIV, the virus that causes AIDS, are at a higher risk of cervical cancer and other cervical diseases. The U.S. Centers for Disease Control and Prevention (CDC) recommends that all HIV-positive women get an initial Pap smear test, and get re-tested 6 months later. If both Pap smear tests are normal, HIV-positive women can get yearly Pap smear tests in the future.
How can I reduce my chances of getting cervical cancer?
A well-proven way to prevent cervical cancer is to have testing (screening) to find pre-cancers before they can turn into invasive cancer. The Pap smear test (or Pap smear) and the human papillomavirus (HPV) test are used for this. If a pre-cancer is found it can be treated, stopping cervical cancer before it really starts. Most invasive cervical cancers are found in women who have not had regular Pap smear tests.
The Pap smear test is a procedure used to collect cells from the cervix so that they can be looked at under a microscope to find cancer and pre-cancer. These cells can also be used for HPV testing. An HPV test can be done on the same sample of cells collected from the Pap test. A Pap smear test can be done during a pelvic exam, but not all pelvic exams include a Pap smear test.
You can reduce your chances of getting cervical cancer in several ways:
- Get regular Pap smear tests. Regular Pap smear tests help your doctor find and treat any abnormal cells before they turn into cancer.
- Get an HPV vaccine (if you are 26 or younger). Most cases of cervical cancer are caused by a type of HPV that is passed from person to person through genital contact. Most women never know they have HPV. It usually stays hidden. While it sometimes goes away on its own, it can cause changes in the cells of the cervix. Pap smear tests usually find these changes. To learn more, read this fact sheet on HPV vaccines and young women.
- Be monogamous. Having sex with just one partner can also lower your risk. Be faithful to each other. That means that you only have sex with each other and no one else.
- Use condoms. The best way to prevent any sexually transmitted infection (STI), including HPV, the cause of most cases of cervical cancer, is to not have vaginal, oral, or anal sex. If you do have sex, use condoms. Condoms lower your risk of getting HPV and other STIs. Although HPV can also occur in female and male genital areas that are not protected by condoms, research shows that condom use is linked to lower cervical cancer rates. Protect yourself with a condom every time you have vaginal, anal, or oral sex.
- Not smoking.
The American Cancer Society recommendations for HPV vaccine use are similar to those from the federal Advisory Committee on Immunization Practices (ACIP), and include the following:
- Routine HPV vaccination for girls and boys should be started at age 11 or 12. The vaccination series can be started as early as age 9.
- HPV vaccination is also recommended for females 13 to 26 years old and for males 13 to 21 years old who have not started the vaccines, or who have started but not completed the series. Males 22 to 26 years old may also be vaccinated.*
- HPV vaccination is also recommended through age 26 for men who have sex with men and for people with weakened immune systems (including people with HIV infection), if they have not previously been vaccinated.
*For people 22 to 26 years old who have not started the vaccines, or who have started but not completed the series, it’s important to know that vaccination at older ages is less effective in lowering cancer risk.
It’s important to realize that no vaccine provides complete protection against all cancer-causing types of HPV, so routine cervical cancer screening with Pap smear is still necessary.
How can I get a free or low-cost Pap smear test?
Pap smear tests are covered under the Affordable Care Act, the health care law passed in 2010. Most insurance plans now cover Pap smear tests at no cost to you.
- If you have insurance, check with your insurance provider to find out what’s included in your plan.
- If you don’t have insurance, find a program near you that offers free or low-cost Pap smear tests (https://www.cdc.gov/cancer/nbccedp/screenings.htm).
- If you have Medicare, find out how often Medicare covers Pap smear tests and pelvic exams (https://www.medicare.gov/coverage/cervical-vaginal-cancer-screenings.html).
- If you have Medicaid, the benefits covered are different in each state, but certain benefits must be covered by every Medicaid program. Check with your state’s program to find out what’s covered (https://www.medicaid.gov/).
For information about other services covered by the Affordable Care Act, visit HealthCare.gov (http://www.healthcare.gov).
Do virgins need Pap smears?
Most health care organizations recommend women begin regular Pap smear testing at age 21. If you’re a virgin — meaning you haven’t had sexual (vaginal) intercourse — you may have a low risk of cervical cancer, but you can still consider Pap smear testing.
The purpose of a Pap smear is to collect cells from your cervix, which is the lower end of your uterus. The cells collected in a Pap smear can detect if you have cervical cancer or suspicious cells that indicate you may develop cervical cancer.
In most cases, cervical cancer is caused by a sexually transmitted infection called human papillomavirus (HPV). If you’ve never had any type of sexual intercourse, you’re unlikely to have HPV. However, there are other risk factors for developing cervical cancer, such as family history and smoking, so talk to your doctor if you have concerns.
For effective cervical cancer screening, many organizations recommend an initial Pap smear at age 21. Discuss when to begin cervical cancer screening with your doctor. Together you can decide what’s best for your particular situation.
Are Pap tests still needed after removal of the uterus (hysterectomy)?
It depends on the type of hysterectomy (surgery to remove the uterus) you had and your health history. If you’re unsure whether you still need Pap smear tests, discuss with your doctor what’s best for you.
If you had a partial hysterectomy — when the uterus is removed but the lower end of the uterus (cervix) remains — your health care provider will likely recommend continued Pap smear tests.
Similarly, if you had a partial hysterectomy or a total hysterectomy — when both the uterus and cervix are removed — for a cancerous or precancerous condition, regular Pap smear tests are still recommended as an early detection tool to monitor for a new cancer or precancerous change.
You can stop having Pap smear tests, however, if you had a total hysterectomy for a noncancerous condition.
Your age matters, too.
- If you no longer have a cervix because you had a hysterectomy for reasons other than cancer, you do not need Pap smear tests.
- If you had a hysterectomy because of abnormal cervical cells or cervical cancer, you should have a yearly Pap smear test until you have three normal tests.
- If you had your uterus removed but you still have a cervix (this type of hysterectomy is not common), you need regular Pap smear tests until you are 65 and have had three normal Pap smear tests in a row with no abnormal results in the last 10 years.
Who does not need a regular Pap smear test?
The only women who do not need regular Pap smear tests are:
- Women ages 65 and older who have had three normal Pap smear tests in a row and no abnormal test results in the last 10 years, and have been told by their doctors that they don’t need to be tested anymore.
- Women who do not have a cervix (usually because of a hysterectomy) and who do not have a history of cervical cancer or abnormal Pap smear results.
All women should speak to a doctor before stopping regular Pap smear tests.
Pap smear procedure
Pap smear prep
You can do several things to make your Pap test as accurate as possible:
- Try not to schedule an appointment for a time during your menstrual period. The best time is at least 5 days after your menstrual period stops.
- Don’t use tampons, birth-control foams or jellies, other vaginal creams, moisturizers, suppositories, or lubricants, or vaginal medicines for 2 to 3 days before the Pap test.
- Don’t use vaginal deodorant sprays or powders
- Don’t douche for 2 to 3 days before the Pap test.
- Don’t have vaginal sex for 2 days before the Pap test.
How the Pap test is done
The Pap test is a procedure used to collect cells from the cervix so that they can be looked at under the microscope to find cancer and pre-cancer.
The health care professional first places a speculum inside the vagina. The speculum is a metal or plastic instrument that keeps the vagina open so that the cervix can be seen clearly. Next, using a small spatula, a sample of cells and mucus is lightly scraped from the exocervix. A small brush or a cotton-tipped swab is then inserted into the opening of the cervix to take a sample from the endocervix. If your cervix has been removed (because you had a trachelectomy or hysterectomy) as a part of the treatment for a cervical cancer or pre-cancer, the cells will be sampled from the upper part of the vagina (known as the vaginal cuff). The samples are then prepared so that they can be looked at under a microscope in the lab.
Although the Pap smear test has been more successful than any other screening test in preventing a cancer, it’s not perfect. One of the limitations of the Pap smear test is that the results need to be examined by the human eye, so an accurate analysis of the hundreds of thousands of cells in each sample is not always possible. Engineers, scientists, and doctors are working together to improve this test. Because some abnormalities may be missed (even when samples are looked at in the best labs), it’s not a good idea to have this test less often than American Cancer Society guidelines recommend (see guidelines below).
A pelvic exam is not the same as a Pap smear test
Many people confuse pelvic exams with Pap smear tests. The pelvic exam is part of a woman’s routine health care. During a pelvic exam, the doctor looks at and feels the reproductive organs, including the uterus and the ovaries and may do tests for sexually transmitted disease. Pelvic exams may help find other types of cancers and reproductive problems. Pap smear tests are often done during pelvic exams after the speculum is placed. Sometimes a pelvic exam is done without having a Pap smear test, but a Pap smear test is needed to find early cervical cancer or pre-cancers. Ask your doctor if you had a Pap smear test with your pelvic exam.
Should I get a Pap test when I have my period?
No. Doctors suggest you schedule a Pap test when you do not have your period. The best time to be tested is 10 to 20 days after the first day of your period.
When will I get the results of my Pap smear test?
Usually it takes one to three weeks to get Pap smear test results. Most of the time, test results are normal. If the test shows that something might be wrong, your doctor will contact you to schedule more tests. There are many reasons for abnormal Pap smear test results. Abnormal Pap smear test results do not always mean you have cancer.
How Pap smear test results are reported
The most widely used system for describing Pap smear test results is the Bethesda System. There are 3 main categories, some of which have sub-categories:
- Negative for intraepithelial lesion or malignancy
- Epithelial cell abnormalities
- Other malignant neoplasms.
You may need further testing if your Pap test showed any of the abnormalities below. See Work-up of abnormal Pap test results.
Negative for intraepithelial lesion or malignancy
This category means that no signs of cancer, pre-cancer, or other significant abnormalities were found. There may be findings that are unrelated to cervical cancer, such as signs of infection with yeast, herpes, or Trichomonas vaginalis (a microscopic parasite), for example. Specimens from some women may also show “reactive cellular changes”, which is the way cervical cells appear when infection or other irritation is around.
Epithelial cell abnormalities
This means that the cells lining the cervix or vagina show changes that might be cancer or a pre-cancer condition. This category is divided into several groups for squamous cells and glandular cells.
Squamous cell abnormalities
Atypical squamous cells (ASCs)
This category includes two types of abnormalities:
- Atypical squamous cells of uncertain significance (ASC-US) is a term used when there are cells that look abnormal, but it is not possible to tell if this is caused by infection, irritation, or a pre-cancer. Most of the time, cells labeled atypical squamous cells of uncertain significance (ASC-US) are not pre-cancer, but more testing is needed to be sure.
- Atypical squamous cells where high-grade squamous intraepithelial lesion (HSIL) can’t be excluded (ASC-H) is a term used when the cells look abnormal but are more concerning for a possible pre-cancer that needs more testing and may need treatment.
Squamous intraepithelial lesions (SILs)
These abnormalities are divided into two categories:
- In low-grade SIL (LSIL) the cells look mildly abnormal.
- In high-grade SIL (HSIL) the cells look severely abnormal and are less likely than the cells in LSIL to go away without treatment. They are also more likely to eventually develop into cancer if they are not treated.
Further tests are needed if squamous intraepithelial lesion (SIL) is seen on a Pap smear test. This is discussed in Work-up of abnormal Pap test results (see below). If treatment is needed, it can cure most squamous intraepithelial lesions (SILs) and prevent true cancer from developing.
Squamous cell carcinoma: This result means that the woman is likely to have an invasive cervical cancer. Further testing will be done to be sure of the diagnosis before treatment can be planned.
Glandular cell abnormalities
Atypical glandular cells
When the glandular cells do not look normal, but they have concerning features that could be cancerous, the term used is atypical glandular cells. In this case, the patient should have more testing done.
Adenocarcinoma
Cancers of the glandular cells are called adenocarcinomas. In some cases, the pathologist examining the cells can tell whether the adenocarcinoma started in the endocervix, in the uterus (endometrium), or elsewhere in the body.
Other malignant neoplasms
This category is for other types of cancer that hardly ever affect the cervix, such as malignant melanoma, sarcomas, and lymphoma.
Abnormal Pap smear results
It can be scary to hear that your Pap smear test results are “abnormal.” But abnormal Pap smear test results usually do not mean you have cancer. Most often there is a small problem with the cervix. If results of the Pap smear test are unclear or show a small change in the cells of the cervix, your doctor may repeat the Pap smear test immediately, in 6 months, or a year, or he or she may run more tests.
Some abnormal cells will turn into cancer. Treating abnormal cells that don’t go away on their own can prevent almost all cases of cervical cancer. If you have abnormal results, talk with your doctor about what they mean. Your doctor should answer any questions you have and explain anything you don’t understand. Treatment for abnormal cells is often done in a doctor’s office during a routine appointment.
If the test finds more serious changes in the cells of the cervix, the doctor will suggest more tests. Results of these tests will help your doctor decide on the best treatment.
Work-up of Abnormal Pap Smear Test Results
The first step in finding cervical cancer is often an abnormal Pap smear test result. This will lead to further tests, which can diagnose cervical cancer.
Cervical cancer may also be suspected if you have symptoms like abnormal vaginal bleeding or pain during sex. Your primary doctor or gynecologist often can do the tests needed to diagnose pre-cancers and cancers and may also be able to treat a pre-cancer.
If there is a diagnosis of invasive cancer, your doctor should refer you to a gynecologic oncologist, a doctor who specializes in cancers of women’s reproductive systems.
Tests for women with symptoms of cervical cancer or abnormal Pap smear test results
Medical history and physical exam
First, the doctor will ask you about your personal and family medical history. This includes information related to risk factors and symptoms of cervical cancer. A complete physical exam will help evaluate your general state of health. The doctor will do a pelvic exam and may do a Pap smear test if one has not already been done. In addition, your lymph nodes will be felt for evidence of metastasis (cancer spread).
The Pap smear test is a screening test, not a diagnostic test. It cannot tell for certain if you have cervical cancer. An abnormal Pap smear test result may mean more testing, sometimes including tests to see if a cancer or a pre-cancer is actually present. The tests that are used include colposcopy (with biopsy), endocervical scraping and cone biopsies.
Colposcopy
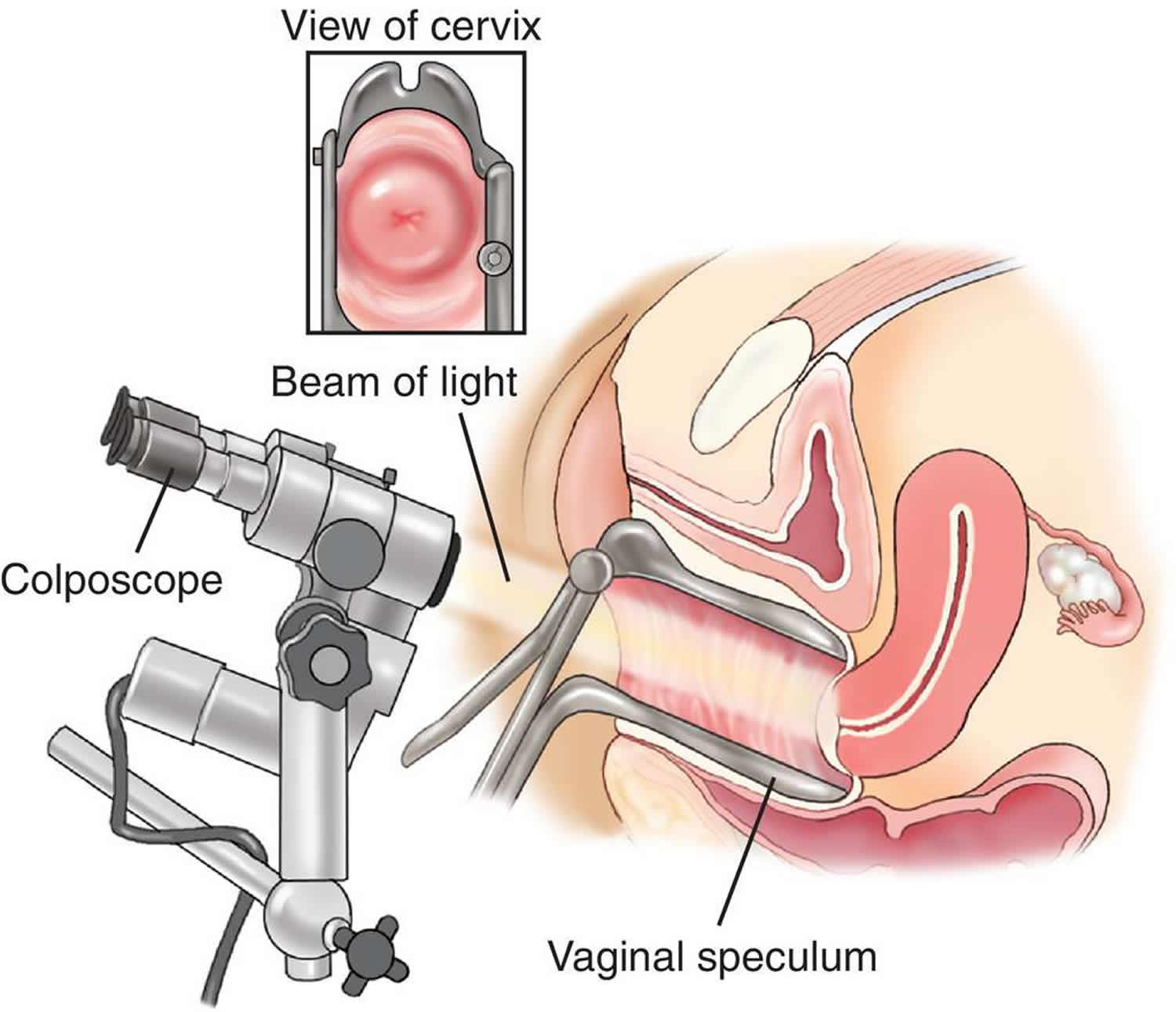
If you have certain symptoms that are worrisome for cancer or if your Pap smear test shows abnormal cells, you will need to have a test called colposcopy. You will lie on the exam table as you do with a pelvic exam. A speculum will be placed in the vagina to help the doctor see the cervix. The doctor will use a colposcope to examine the cervix. The colposcope is an instrument that stays outside the body and has magnifying lenses. It lets the doctor see the surface of the cervix closely and clearly. Colposcopy itself usually causes no more discomfort than any other speculum exam. It can be done safely even if you are pregnant. Like the Pap smear test, it is better not to have it during your menstrual period.
At the time of the procedure, the doctor will apply a weak solution of acetic acid (similar to vinegar) to your cervix to make any abnormal areas easier to see. If an abnormal area is seen, a biopsy (removal of a small piece of tissue) will be done. The tissue is sent to a lab to be looked at under a microscope. A biopsy is the best way to tell for certain whether an abnormal area is a pre-cancer, a true cancer, or neither. Although the colposcopy procedure is usually not painful, the cervical biopsy can cause discomfort, cramping, bleeding, or even pain in some women.
Figure 2. Colposcopy
Cervical biopsies
Several types of biopsies can be used to diagnose cervical pre-cancers and cancers. After these procedures, patients may feel mild cramping or pain and may also have some light bleeding.
- Colposcopic biopsy
For this type of biopsy, the cervix is examined with a colposcope to find the abnormal areas. A local anesthetic may then be used to numb the cervix before the biopsy. Using biopsy forceps, a small section of the abnormal area is removed.
- Endocervical curettage (endocervical scraping)
Sometimes the transformation zone (the area at risk for HPV infection and pre-cancer) cannot be seen with the colposcope, so something else must be done to check that area for cancer. This means taking a scraping of the endocervix by inserting a narrow instrument (called a curette) into the endocervical canal (the part of the cervix closest to the uterus). The curette is used to scrape the inside of the canal to remove some of the tissue, which is then sent to the lab for examination.
- Cone biopsy
In this procedure, also known as conization, the doctor removes a cone-shaped piece of tissue from the cervix. The tissue removed in the cone includes the transformation zone where cervical pre-cancers and cancers are most likely to start.
A cone biopsy is not only used to diagnose pre-cancers and cancers. It can also be used as a treatment since it can sometimes completely remove pre-cancers and some very early cancers.
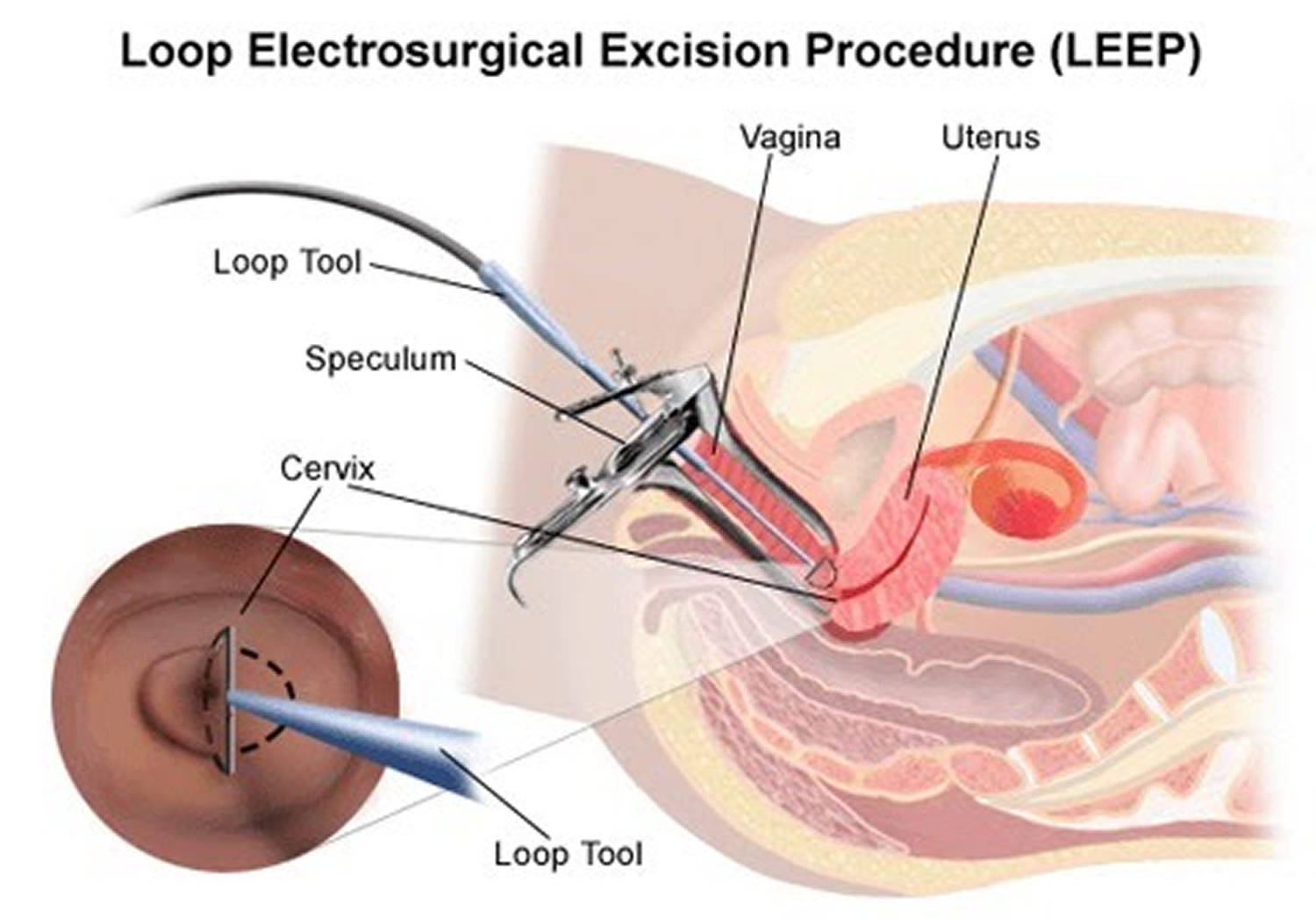
The methods commonly used for cone biopsies are the loop electrosurgical excision procedure (LEEP), also called the large loop excision of the transformation zone (LLETZ), and the cold knife cone biopsy. With both procedures, you might have mild cramping and some bleeding for a few weeks.
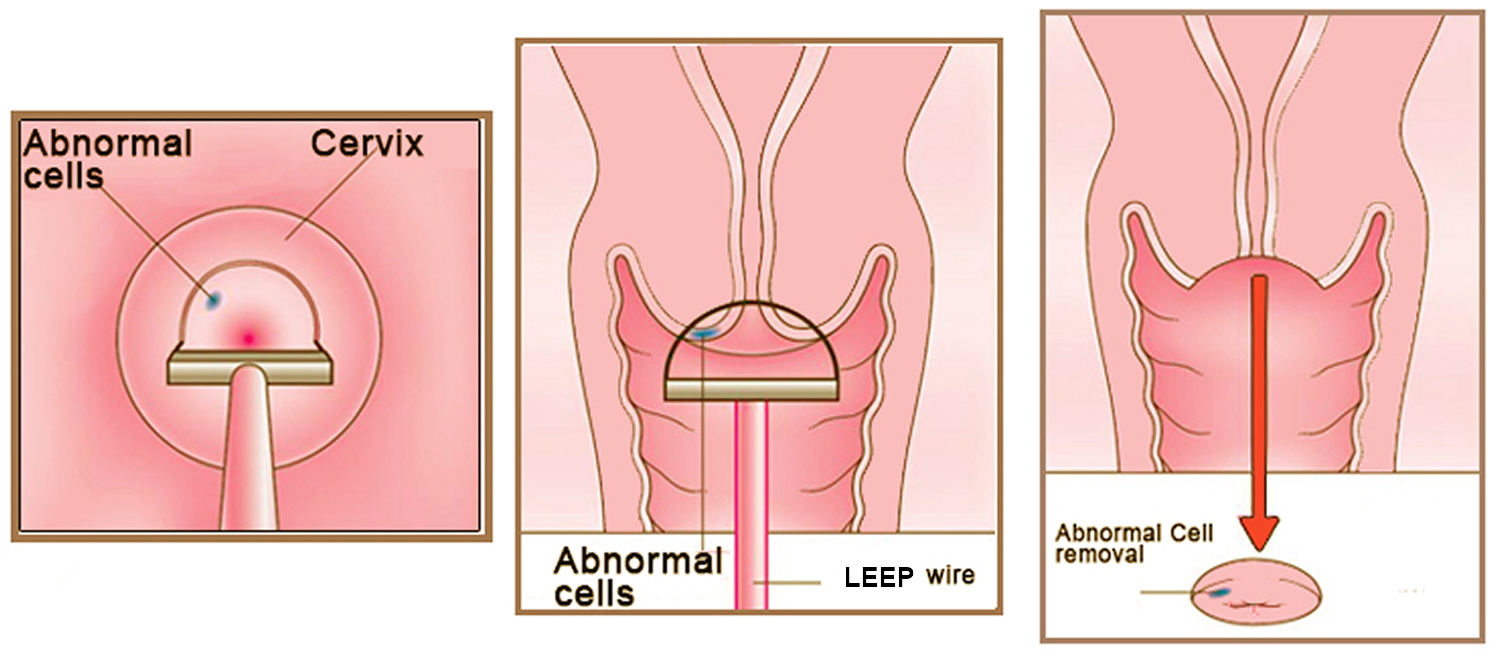
- Loop electrosurgical procedure (LEEP or LLETZ): In this method, the tissue is removed with a thin wire loop that is heated by electricity and acts as a small knife. For this procedure, a local anesthetic is used, and it can be done in your doctor’s office.
- Cold knife cone biopsy: This method uses a surgical scalpel or a laser instead of a heated wire to remove tissue. · You will receive anesthesia during the operation (either a general anesthesia, where you are asleep, or a spinal or epidural anesthesia, where an injection into the area around the spinal cord makes you numb below the waist) and it is done in a hospital.
Having any type of cone biopsy will not prevent most women from getting pregnant, but if a large amount of tissue has been removed, women may have a higher risk of giving birth prematurely and having a low birth weight baby. In rare cases, the cervix is narrowed after the procedure. This narrowing may cause problems with menstruation.
Some possible complications of LEEP procedure may include:
- Infection
- Bleeding
- Changes or scarring in the cervix from removal of tissue
- Trouble getting pregnant
- Potential for preterm birth or having a low birth weight baby
- Incomplete removal of the abnormal cells
Figure 3. LEEP procedure (LLETZ procedure)
Figure 4. LEEP cone biopsy
My Pap smear test result was a “false positive.” What does this mean?
Pap smear tests are not always perfect. False positive and false negative results can happen. This can be upsetting and confusing.
- False positive. A false positive Pap smear test occurs when a woman is told she has abnormal cervical cells, but the cells are not actually abnormal or cancerous. If your doctor says your Pap smear results were a false positive, there is no problem.
- False negative. A false negative Pap smear test is when a woman is told her cells are normal, but there is a problem with the cervical cells that was missed. False negatives delay the discovery and treatment of unhealthy cells of the cervix. But having regular Pap smear tests boosts your chances of finding any problems. Cervical cancers usually take many years to develop. If abnormal cells are missed at one time, they will probably be found on your next Pap smear test.
What tests will I need?
The tests (or treatment) you will need depend on the results of the Pap smear test.
The specific results of your Pap smear test, along with your age, will guide your doctor to the next step. It may involve a follow-up Pap smear test in a year, an HPV test, or one of the procedures above. Your doctor will most likely use the guidelines for abnormal Pap smear test results from the American Congress of Obstetricians and Gynecologists when deciding on what follow-up plan is best for you.
The HPV DNA Test
HPV is short for human papillomavirus. HPVs are a group of more than 150 related viruses. Each HPV virus is given a number, which is called an HPV type. HPVs are called papillomaviruses because some HPV types cause papillomas (warts), which are non-cancerous tumors. But some types of HPV are known to cause cancer, including cancers of the cervix (the base of the womb at the top of the vagina), vagina, vulva (the area around the outside of the vagina), penis, anus, and parts of the mouth and throat.
HPVs are attracted to and can live only in certain cells called squamous epithelial cells. These cells are found on the surface of the skin and on moist surfaces (called mucosal surfaces) like:
- The vagina, cervix, vulva (area around the outside of the vagina), and anus
- The inner foreskin and urethra of the penis
- The inner lining of the nose, mouth, and throat
- The trachea (windpipe) and bronchi (smaller breathing tubes branching off the trachea)
- The inner eyelids
About 75% of the HPV types cause warts on the skin – often on the arms, chest, hands, and feet. These are common warts.
The other 25% of HPV types are considered mucosal types of HPV. These can infect the moist surface layers that line organs and cavities of the body that open to the outside, like those listed above. The mucosal HPV types are also called genital (or anogenital) type HPVs because they often affect the anal and genital area.
Genital HPV (human papilloma virus) is not the same as HIV (human immunodeficiency virus, a virus that causes AIDS) or herpes (herpes simplex virus either HSV-1 or HSV-2). HPV (human papilloma virus) is divided into 2 main groups:
- Low-risk HPV types
Some types of HPV can cause warts (papillomas) on or around the genitals and anus of both men and women. Women may also have warts on the cervix and in the vagina. Because these HPV types rarely cause cancer, they are called “low-risk” viruses.
- High-risk HPV types
Other types of HPV are called “high-risk” because they can cause cancer in both men and women. Doctors worry more about the cell changes and pre-cancers linked to these types, because they’re more likely to grow into cancers over time. Common high-risk HPV types include HPV 16 and 18.
Infection with HPV is very common. In most people, the body is able to clear the infection on its own. But sometimes, the infection doesn’t go away. Chronic, or long-lasting infection, especially when it’s caused by certain high-risk HPV types, can cause cancer over time.
The most important risk factor for developing cervical cancer is infection with HPV (human papilloma virus). Doctors can now test for the HPV (high-risk or carcinogenic types) that are most likely to cause cervical cancer by looking for pieces of their DNA in cervical cells. The test can be done at the same time as the Pap smear test, with the same swab or a second swab. You won’t notice a difference in your exam if you have both tests.
The HPV test is most often used in 2 situations:
- The HPV gene test can be used in combination with the Pap smear test to screen for cervical cancer. The American Cancer Society recommends this combination for women 30 and older. The HPV DNA test is not recommended to screen for cervical cancer in women under 30. That is because women in their 20s who are sexually active are much more likely (than older women) to have an HPV infection that will go away on its own. For these younger women, results of this test are not as significant and may be more confusing. For more information, see the American Cancer Society document HPV and HPV Testing.
- The HPV DNA test can also be used in women who have slightly abnormal Pap smear test results – atypical squamous cells of uncertain significance (ASC-US) to find out if they might need more testing or treatment.
An HPV DNA test has been approved by the FDA to be used without a Pap smear test to screen for cervical cancer.
The HPV tests on the market are only approved to find cervical HPV infection in women. They can be used to help test women at certain ages and after certain Pap test findings to help look for cervical cancer.
- There’s no approved HPV test to find HPV on the penis or vulva, or in the anus, mouth, or throat.
- There’s no test for men or women to check one’s overall “HPV status.”
- For cervical cancer screening, the American Cancer Society recommends that women ages 30 to 65 get both an HPV test and Pap test every 5 years. (Another option for these women is just a Pap smear test every 3 years. While this can find the cell changes caused by HPV, it does not find HPV infection.)
Follow-up of HPV testing
If your Pap smear test result is normal, but you test positive for HPV, the main options are:
- Repeat co-testing (with a Pap smear test and an HPV test) in one year
- Testing for HPV types 16 or 18 (this can often be done on the sample in the lab). If the test is positive for HPV types 16 or 18, colposcopy would be recommended (colposcopy is discussed in the section above, work-up of abnormal Pap smear test results). If you test negative, you should get repeat co-testing in one year.
How do people get HPV?
HPV can be passed from one person to another by skin-to-skin contact, such as occurs with sexual activity. The main way HPV is spread is through sexual activity, including vaginal, anal, and oral sex. HPV can be spread even when an infected person has no visible signs or symptoms.
The virus can also be spread by genital contact without sex, although this is not common.
HPV infection is very common. Most men and women who have ever had sex get at least one type of genital HPV at some time in their lives. Anyone who has had sex can get HPV, even if it was only with only one person, but infections are more likely in people who have had many sex partners. Even if a person delays sexual activity until marriage, or only has one partner, they are still at risk of HPV infection if their partner has been exposed.
You cannot get HPV from:
- Toilet seats
- Hugging or holding hands
- Swimming pools or hot tubs
- Sharing food or utensils
- Being unclean
You can have HPV:
- Even if it has been years since you were sexually active
- Even if you do not have any signs or symptoms
Cancers linked to HPV infection
Cervical cancer
Cervical cancer is the most common cancer linked to HPV in women. Nearly all cervical cancers are caused by HPV.
Cervical cancer can be found early and even prevented with routine screening tests. The Pap smear test looks for changes in cervical cells caused by HPV infection. Whilst the HPV test looks for the infection itself.
Cervical cancer is preventable with vaccines and regular screening tests. More than half of the women in the United States who get cervical cancer have never had or rarely had a Pap smear test.
Vulvar cancer
HPV can also cause cancer of the vulva, which is the outer part of the female genital organs. This cancer is much less common than cervical cancer.
There’s no standard screening test for this cancer other than routine physical exams.
Vaginal cancer
Most vaginal cancers contain HPV.
Many vaginal pre-cancers also contain HPV, and these changes may be present for years before turning into cancer. These pre-cancers can sometimes be found with the same Pap test that’s used to test for cervical cancer and pre-cancer. If a pre-cancer is found, it can be treated, stopping cancer before it really starts.
Penile cancer
In men, HPV can cause cancer of the penis. It’s more common in men with HIV and those who have sex with other men.
There’s no standard screening test to find early signs of penile cancer. Because almost all penile cancers start under the foreskin of the penis, they may be noticed early in the course of the disease.
Anal cancer
HPV can cause cancer of the anus in both men and women. It’s more common in people with HIV and in men who have sex with other men.
Screening tests for anal cancer are not routinely recommended for all people. Still, some experts recommend anal cytology testing (also called an anal Pap test because it’s much like the Pap test used for cervical cancer) for people at higher risk of anal cancer. This includes men who have sex with men, women who have had cervical cancer or vulvar cancer, anyone who is HIV-positive, and anyone who has had an organ transplant.
Mouth and throat cancer
HPV is found in some mouth and throat cancers in men and women. Most cancers found in the back of the throat, including the base of the tongue and tonsils, are HPV-related. These are the most common HPV-related cancers in men.
There’s no standard screening test to find these cancers early. Still, many can be found early during routine exams by a dentist, doctor, dental hygienist, or by self-exam.
Can HPV infection be prevented?
There’s no sure way to prevent infection with all the different types of HPV. But there are things you can do to lower your chances of being infected. There are also vaccines that can be used to protect young people from the HPV types most closely linked to cancer and genital warts.
HPV is passed from one person to another during contact with an infected part of the body. Although HPV can be spread during sexual contact – including vaginal, anal, and oral sex – sex isn’t the only way for the infection to spread. All that’s needed is skin-to-skin contact with an area of the body infected with HPV. There may be other ways to become infected with HPV that aren’t yet clear.
HPV can be present for years without causing any symptoms. It doesn’t always cause warts or any other symptoms. Someone can have the virus and pass it on without knowing it.
- Condom use
Condoms (“rubbers”) provide some protection against HPV, but they do not completely prevent infection.
Condoms must be used correctly every time sex occurs. Even then, condoms can’t protect completely because they don’t cover every possible HPV-infected area of the body, such as the skin on the genital or anal area. Still, condoms do provide some protection against HPV, and they also help protect against some other sexually transmitted infections.
- Limiting sex partners
If you are sexually active, limiting the number of sex partners and avoiding sex with people who have had many other sex partners can help lower your risk of exposure to genital HPV. But again, HPV is very common, so having sex with even one other person can put you at risk.
- HPV vaccines
HPV vaccines can prevent infection with certain types of HPV, including types that are linked to HPV-related cancers, as well as types linked to anal and genital warts.
Vaccines are approved for use in males and females. They can only be used to prevent HPV infection – they don’t help treat an existing infection. To work best, the vaccines should be given at or before age 11 or 12.
Can a vaccine help prevent HPV?
Yes. Vaccines are available to help prevent infection by certain types of HPV and some of the cancers linked to those types. As of 2017, Gardasil 9® is the only HPV vaccine available in the United States. Other HPV vaccines are available outside the U.S.
All of these vaccines help prevent infection by HPV-16 and HPV-18. These 2 types cause about 70% of all cervical cancers and pre-cancers, as well as many cancers of the anus, penis, vulva, vagina, and throat.
Gardasil 9 helps prevent infection by 4 types of HPV (16, 18, 6 and 11), plus 5 other high risk types: 31, 33, 45, 52 and 58. Together these types cause about 90% of cervical cancers.
Who should be vaccinated against HPV and when?
HPV vaccine produces the strongest immune response in preteens. To work best, the HPV vaccines should be given at age 11 or 12. The vaccines are given in a series of shots.
The American Cancer Society’s recommendations for HPV vaccine use:
- Routine HPV vaccination for girls and boys should be started at age 11 or 12. The vaccination series can be started as early as age 9.
- HPV vaccination is also recommended for females 13 to 26 years old and for males 13 to 21 years old who have not started the vaccines, or who have started but not completed the series. Males 22 to 26 years old may also be vaccinated.*
- HPV vaccination is also recommended through age 26 for men who have sex with men and for people with weakened immune systems (including people with HIV infection), if they have not previously been vaccinated.
*For people 22 to 26 years old who have not started the vaccines, or who have started but not completed the series, it’s important to know that vaccination at older ages is less effective in lowering cancer risk.
Why should the vaccines be given to pre-teens?
The vaccines work best at this age. Research shows that younger people have a better immune response to the vaccine than those in their late teens and early 20s. And, the vaccines will prevent the covered types of HPV only if they are given before exposure to the virus.
This is also an age when other vaccinations are given, and when children are likely to still be getting regular medical check-ups.
What about men and women older than 26? Should they get one of the vaccines?
HPV vaccines are not approved nor recommended after age 26. While the vaccines are safe, they will not provide much, if any, benefit.
Who should not get one of the HPV vaccines or who should wait?
Pregnant women should NOT get any HPV vaccine at this time, even though they appear to be safe for both mother and the unborn baby. If a woman who is pregnant does get an HPV vaccine, it’s not a reason to consider ending the pregnancy. Women who started a vaccine series before they learned they were pregnant should complete the series after the pregnancy.
Make sure the health care provider knows about any severe allergies. The following should not get an HPV vaccine:
- Anyone with a severe allergy to latex should not get the Cervarix vaccine.
- Those with a severe allergy to yeast should not receive Gardasil or Gardasil 9.
- Anyone who has ever had a life-threatening allergic reaction to anything else contained in the vaccines
- Anyone who has had a serious reaction to an earlier dose of HPV vaccine
Is HPV testing needed before getting the vaccine?
No. In fact, testing is not recommended because it cannot show if the HPV vaccine will be effective or not. A positive HPV test result doesn’t always tell you which types of HPV you have. And even if you are infected with one type of HPV, the vaccine could still prevent other types of HPV infection. A negative test result cannot tell you if you’ve had HPV in the past.
How long will the vaccines prevent HPV infection?
How long a vaccine will protect people is never known when the vaccine is first introduced. Current research shows that the vaccines are effective, and there’s no sign that the protection decreases with time. Research will continue to look at how long protection against HPV lasts, and if booster shots will be needed.
Are HPV vaccines safe?
All of the HPV vaccines were tested in thousands of people around the world before they were approved. And they continue to be constantly monitored for safety. So far, all studies show no deaths have been linked to any HPV vaccine. Common, mild side effects include headache, fever, nausea, and dizziness. Sometimes pain and redness can happen where the shot was given.
As with any medication or injection, people may have an allergic reaction afterwards. Anyone who has a severe (life threatening) allergy to any ingredient in the HPV vaccine should not get the vaccine, including a severe allergy to yeast. Some people may faint after getting any vaccine, including HPV vaccines. Fainting after getting a shot is more common in teens than in young children or adults. To keep people from getting hurt from fainting, a 15-minute waiting period for people of all ages is recommended after any vaccination.
Monitoring for possible side effects
Like all vaccines, even “old” vaccines approved many years ago, the HPV vaccines are continuously monitored for side effects. The US Centers for Disease Control and Prevention (CDC) and the US Food and Drug Administration (FDA) review all serious side effects reported to the Vaccine Adverse Event Reporting System (VAERS) to watch for potential safety concerns that may need further study.
Do women who have been vaccinated against HPV still need Pap smear tests?
Yes. Women who have been vaccinated will still need regular testing for cervical cancer because the vaccines do not prevent all of the types of HPV that can cause cervical cancer.
If I have a positive HPV test, what does it mean?
If you have cervical HPV infection and an abnormal Pap test result, your health care provider will explain what other tests you might need.
If you have cervical HPV infection and a normal Pap test result, it means that you have genital HPV, but no cell changes were seen on your Pap test. There are 2 options:
- You’ll most likely be tested with an HPV test and a Pap test again in 12 months.
In most cases, re-testing in 12 months shows no sign of the virus.
If the virus does go away and your Pap test is normal you can go back to normal screening.
If the virus is still there or changes are seen on the Pap test, you’ll need more testing.
- As another option, the provider may suggest testing specifically for HPV-16 or both -16 and -18 (the 2 types that are most likely to cause cervical cancer).
If testing shows that you have HPV-16 and/or -18, more testing will be needed.
If the test doesn’t show infection with HPV-16 and/or -18, you should be retested in 12 months with both an HPV test and a Pap test.
Will HPV affect my pregnancy or my baby?
HPV infection does not directly affect the chances of getting pregnant.
If HPV infection leads to cervical changes that need to be treated, the treatment should not affect your chances of getting pregnant. But if you have many treatments and biopsies, which can happen with more frequent screening, the risk of pre-term labor and low birth weight babies can go up.
HPV is rarely passed from a mother to her baby. The rare cases where this has happened do not involve the types of HPV that can cause cancer. “How do you get HPV?” has more on HPV being transmitted from mother to baby during pregnancy.
What is a cervix
The cervix is part of the lower end of the uterus. The lumen (internal cavity) of the uterus communicates with the vagina by way of a narrow passage through the cervix called the cervical canal.
Cervix function
The cervical canal contains cervical glands that secrete mucus, thought to prevent the spread of microorganisms from the vagina into the uterus. Near the time of ovulation, the mucus becomes thinner than usual and allows easier passage for sperm.
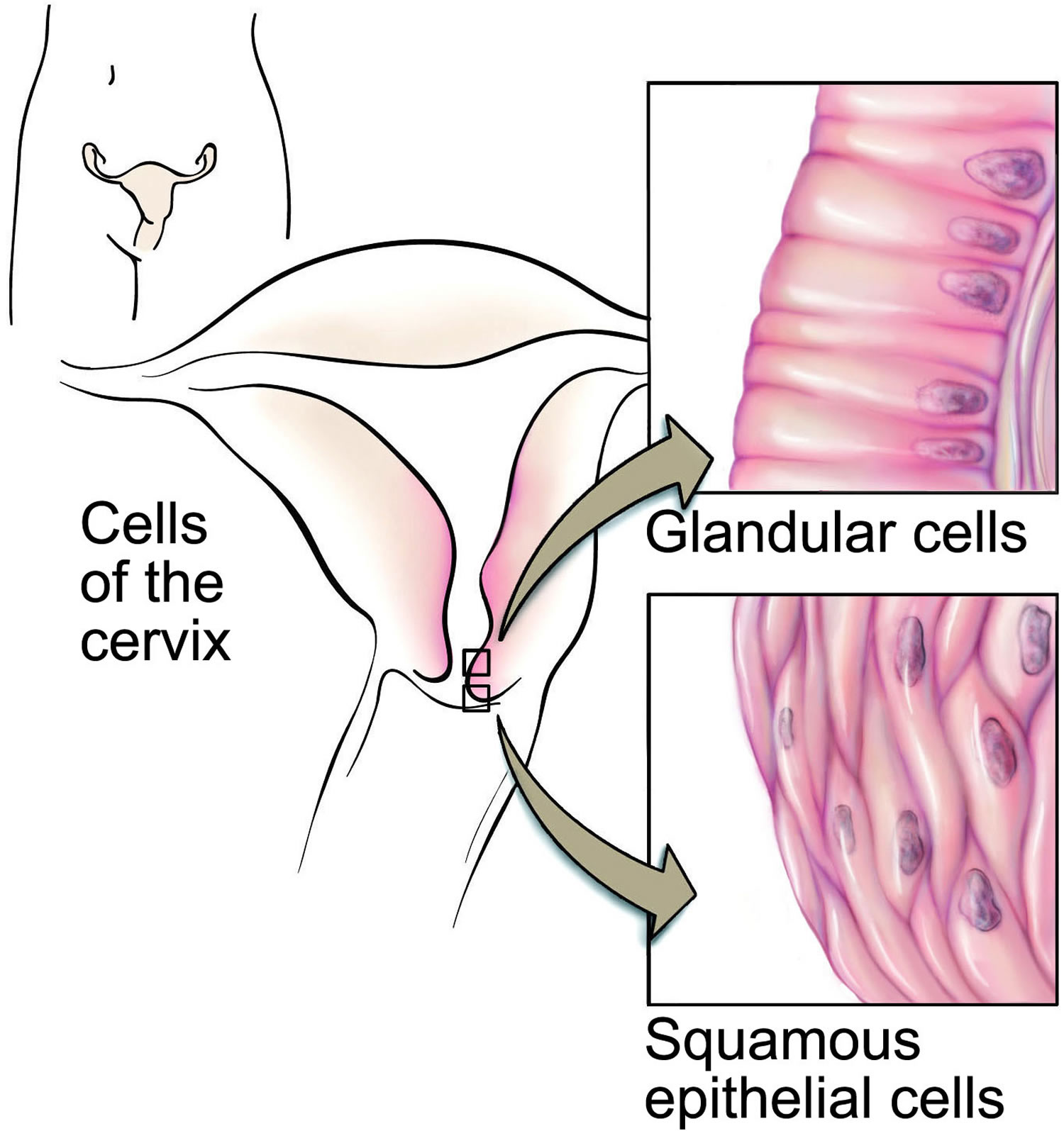
The cervix has two different parts and is covered with two different types of cells.
- The part of the cervix closest to the body of the uterus is called the endocervix and is covered with glandular cells.
- The part next to the vagina is the exocervix (or ectocervix) and is covered in squamous cells.
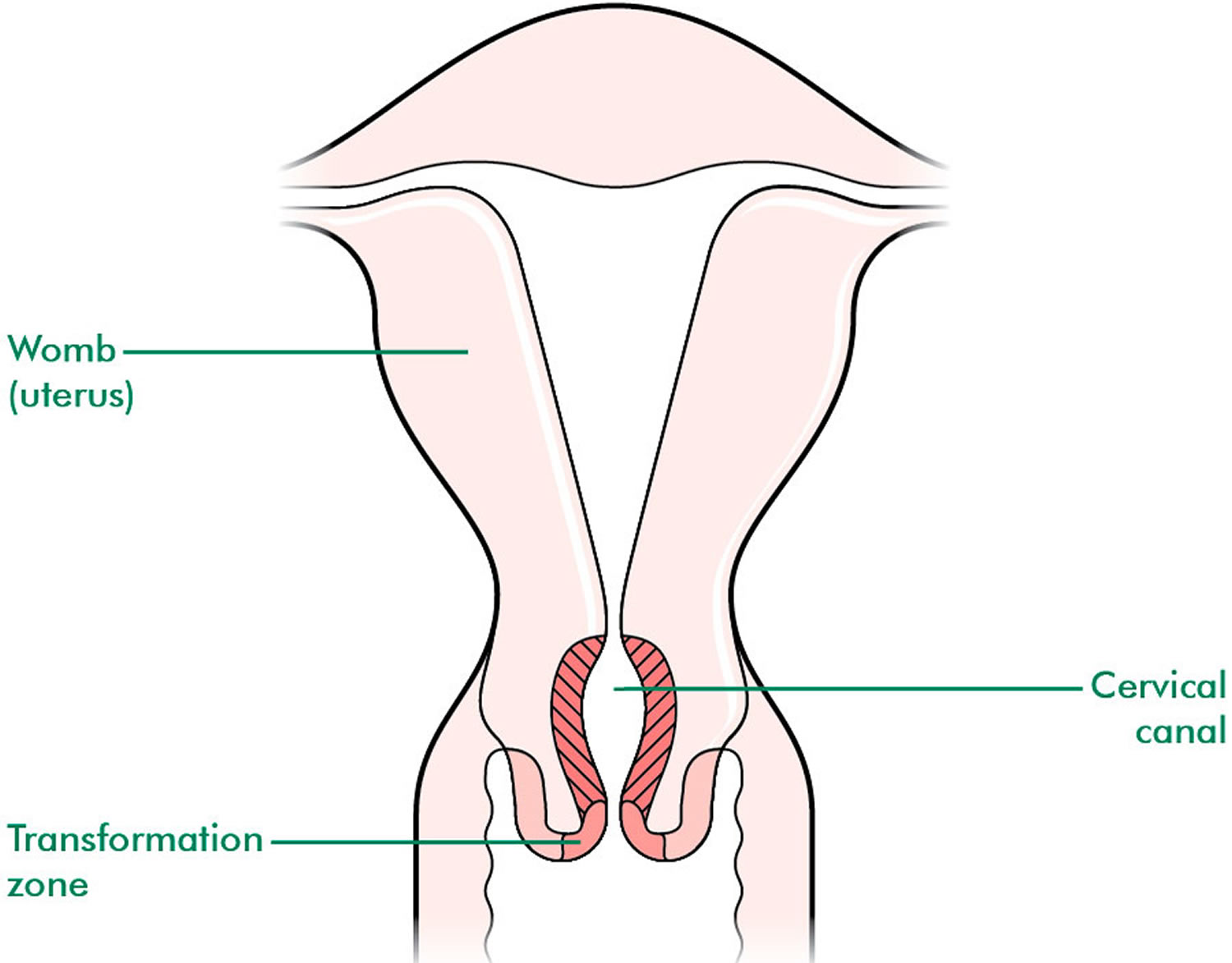
These two cell types meet at a place called the transformation zone. The exact location of the transformation zone changes as you get older and if you give birth.
The cervix and superior part of the vagina are supported by cardinal (lateral cervical) ligaments extending to the pelvic wall.
Figure 5. Cervix position
Figure 6. Cervix location
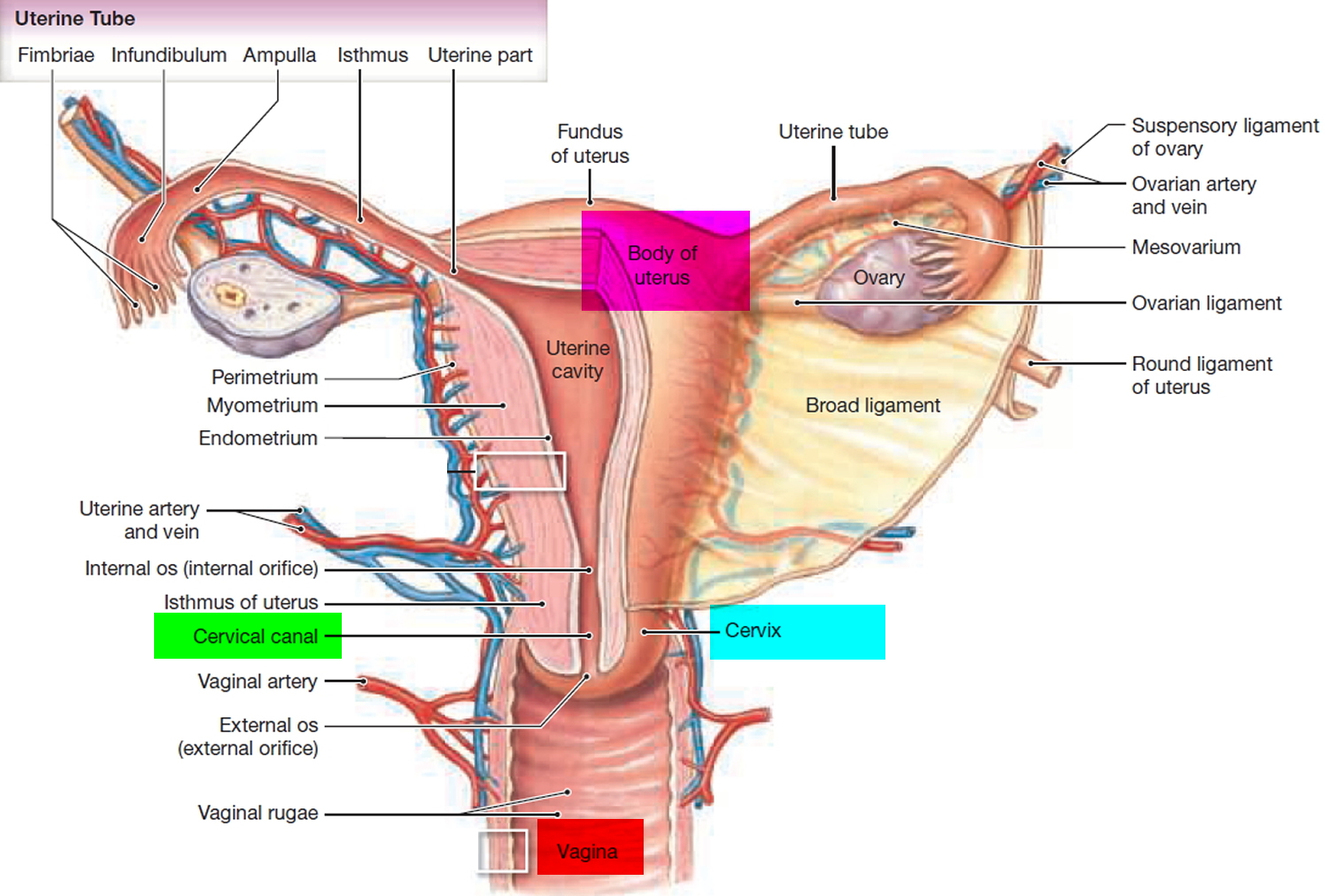
Figure 7. Cervical epithelium
Pap smear guidelines
The U.S. Preventive Services Task Force – Draft Guidelines for the Prevention and Early Detection of Cervical Cancer
Here is a draft 2017 Cervical Cancer: Screening Guideline by the U.S. Preventive Services Task Force 18)
Note:
The first three recommendations apply to asymptomatic women who have a cervix, regardless of their sexual history or HPV vaccination status. None of these recommendations apply to women who have been diagnosed with a high-grade precancerous cervical lesion or cervical cancer. These recommendations also do not apply to women with in utero exposure to diethylstilbestrol (DES) or women who have a compromised immune system (e.g., women living with HIV).
Women younger than age 21 years
The U.S. Preventive Services Task Force 19) recommends against screening for cervical cancer in women younger than age 21 years.
Women ages 21 to 65 years
The U.S. Preventive Services Task Force 20) recommends screening for cervical cancer every 3 years with cervical cytology alone in women ages 21 to 29 years. The U.S. Preventive Services Task Force 21) recommends either screening every 3 years with cervical cytology alone or every 5 years with high-risk human papillomavirus (hrHPV) testing alone in women ages 30 to 65 years.
Women older than age 65 years
The U.S. Preventive Services Task Force 22) recommends against screening for cervical cancer in women older than age 65 years who have had adequate prior screening and are not otherwise at high risk for cervical cancer.
Women who have had a hysterectomy
The U.S. Preventive Services Task Force 23) recommends against screening for cervical cancer in women who have had a hysterectomy with removal of the cervix and do not have a history of a high-grade precancerous lesion (i.e., cervical intraepithelial neoplasia [CIN] grade 2 or 3) or cervical cancer. As part of the clinical evaluation, clinicians should confirm through review of surgical records or direct examination that the cervix was removed.
The American Cancer Society Guidelines Guidelines for the Prevention and Early Detection of Cervical Cancer
The American Cancer Society recommends that women follow these guidelines to help find cervical cancer early 24). Following these guidelines can also find pre-cancers, which can be treated to keep cervical cancer from forming.
- All women should begin cervical cancer testing (screening) at age 21. Women aged 21 to 29, should have a Pap smear test every 3 years. HPV testing should not be used for screening in this age group (it may be used as a part of follow-up for an abnormal Pap smear test).
- Beginning at age 30, the preferred way to screen is with a Pap smear test combined with an HPV test every 5 years. This is called co-testing and should continue until age 65.
- Another reasonable option for women 30 to 65 is to get tested every 3 years with just the Pap smear test.
- Women who are at high risk of cervical cancer because of a suppressed immune system (for example from HIV infection, organ transplant, or long-term steroid use) or because they were exposed to diethylstilbestrol (DES) in utero may need to be screened more often. They should follow the recommendations of their health care team.
- Women over 65 years of age who have had regular screening in the previous 10 years should stop cervical cancer screening as long as they haven’t had any serious pre-cancers (like CIN2 or CIN3) found in the last 20 years (CIN stands for cervical intraepithelial neoplasia). Women with a history of CIN2 or CIN3 should continue to have testing for at least 20 years after the abnormality was found.
- Women who have had a total hysterectomy (removal of the uterus and cervix) should stop screening (such as Pap smear tests and HPV tests), unless the hysterectomy was done as a treatment for cervical pre-cancer (or cancer). Women who have had a hysterectomy without removal of the cervix (called a supra-cervical hysterectomy) should continue cervical cancer screening according to the guidelines above.
- Women of any age should NOT be screened every year by any screening method.
- Women who have been vaccinated against HPV should still follow these guidelines.
Some women believe that they can stop cervical cancer screening once they have stopped having children. This is not true. They should continue to follow American Cancer Society guidelines.
Although annual (every year) screening should not be done, women who have abnormal screening results may need to have a follow-up Pap smear test (sometimes with a HPV test) done in 6 months or a year.
The American Cancer Society guidelines for early detection of cervical cancer do not apply to women who have been diagnosed with cervical cancer, cervical pre-cancer, or HIV infection. These women should have follow-up testing and cervical cancer screening as recommended by their health care team.
Abnormal pap smear causes
Cervical cancer starts in the cells lining the cervix — the lower part of the uterus (womb) (see Figures 5 to 9). This is sometimes called the uterine cervix. The fetus grows in the body of the uterus (the upper part). The cervix connects the body of the uterus to the vagina (birth canal).
The cervix is made of two different parts and is covered with two different types of cells.
- The part of the cervix closest to the body of the uterus is called the endocervix and is covered with glandular cells.
- The part next to the vagina is the exocervix (or ectocervix) and is covered in squamous cells.
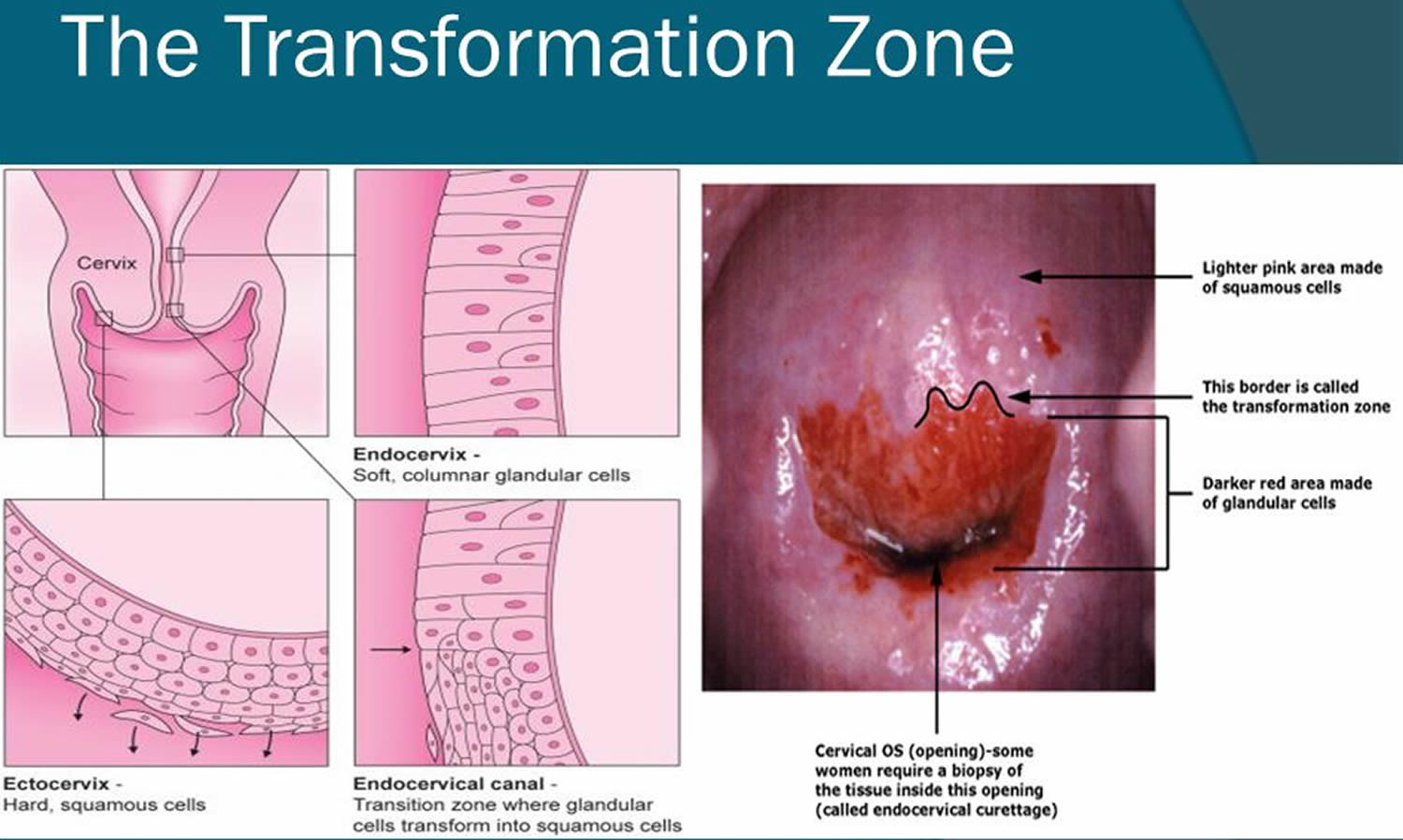
These two cell types meet at a place called the transformation zone (Figures 8 and 9). The exact location of the transformation zone changes as you age and if you give birth.
Most cervical cancers begin in the cells in the transformation zone. These cells do not suddenly change into cancer. Instead, the normal cells of the cervix first gradually develop pre-cancerous changes that turn into cancer. Doctors use several terms to describe these pre-cancerous changes, including cervical intraepithelial neoplasia (CIN), squamous intraepithelial lesion (SIL), and dysplasia. These changes can be detected by the Pap smear test.
Although cervical cancers start from cells with pre-cancerous changes (pre-cancers), only some of the women with pre-cancers of the cervix will develop cancer. It usually takes several years for cervical pre-cancer to change to cervical cancer, but it can happen in less than a year. For most women, pre-cancerous cells will go away without any treatment. Still, in some women pre-cancers turn into true (invasive) cancers. Treating all cervical pre-cancers can prevent almost all true cervical cancers.
Figure 8. Cervical Transformation Zone
Figure 9. Cervical Transformation Zone
Types of cervical cancer
Cervical cancers and cervical pre-cancers are classified by how they look under a microscope. The main types of cervical cancers are squamous cell carcinoma and adenocarcinoma.
- Most (up to 9 out of 10) cervical cancers are squamous cell carcinomas. These cancers form from cells in the exocervix and the cancer cells have features of squamous cells under the microscope. Squamous cell carcinomas most often begin in the transformation zone (where the exocervix joins the endocervix).
- Most of the other cervical cancers are adenocarcinomas. Adenocarcinomas are cancers that develop from gland cells. Cervical adenocarcinoma develops from the mucus-producing gland cells of the endocervix. Cervical adenocarcinomas seem to have become more common in the past 20 to 30 years.
- Less commonly, cervical cancers have features of both squamous cell carcinomas and adenocarcinomas. These are called adenosquamous carcinomas or mixed carcinomas.
Although almost all cervical cancers are either squamous cell carcinomas or adenocarcinomas, other types of cancer also can develop in the cervix. These other types, such as melanoma, sarcoma, and lymphoma, occur more commonly in other parts of the body.
Risk Factors for Cervical Cancer
A risk factor is anything that changes your chance of getting a disease such as cancer. Different cancers have different risk factors. For example, exposing skin to strong sunlight is a risk factor for skin cancer. Smoking is a risk factor for many cancers. But having a risk factor, or even several, does not mean that you will get the disease.
Several risk factors increase your chance of developing cervical cancer. Women without any of these risk factors rarely develop cervical cancer. Although these risk factors increase the odds of developing cervical cancer, many women with these risks do not develop this disease. When a woman develops cervical cancer or pre-cancerous changes, it may not be possible to say with certainty that a particular risk factor was the cause.
In thinking about risk factors, it helps to focus on those you can change or avoid (like smoking or human papillomavirus infection), rather than those you cannot (such as your age and family history). However, it is still important to know about risk factors that cannot be changed, because it’s even more important for women who have these factors to get regular Pap smear tests to detect cervical cancer early.
Cervical cancer risk factors include:
Human papillomavirus (HPV) infection
The most important risk factor for cervical cancer is infection by the human papillomavirus (HPV). HPV is a group of more than 150 related viruses, some of which cause a type of growth called papillomas, which are more commonly known as warts.
HPV can infect cells on the surface of the skin, and those lining the genitals, anus, mouth and throat, but not the blood or internal organs such as the heart or lungs.
HPV can be spread from one person to another during skin-to-skin contact. One way HPV is spread is through sexual activity, including vaginal, anal, and even oral sex.
Different types of HPV cause warts on different parts of the body. Some cause common warts on the hands and feet; others tend to cause warts on the lips or tongue.
Certain types of HPV may cause warts on or around the female and male genital organs and in the anal area. These are called low-risk types of HPV because they are seldom linked to cancer.
Other types of HPV are called high-risk types because they are strongly linked to cancers, including cancers of the cervix, vulva, and vagina in women, penile cancer in men, and cancers of the anus, mouth and throat in men and women. The high-risk types include HPV 16, HPV 18, HPV 31, HPV 33, and HPV 45, as well as some others. There might be no visible signs of infection with a high-risk HPV until pre-cancerous changes or cancer develops.
Doctors believe that a woman must be infected with HPV in order to develop cervical cancer. Although this can mean infection with any of the high-risk types, about two-thirds of all cervical cancers are caused by HPV 16 and 18.
Infection with HPV is common, and in most people the body can clear the infection by itself. Sometimes, however, the infection does not go away and becomes chronic. Chronic infection, especially when it is caused by certain high-risk HPV types, can eventually cause certain cancers, such as cervical cancer.
Although scientists believe that it’s necessary to have had HPV for cervical cancer to develop, most women with this virus do not develop cancer. Doctors believe that other factors must come into play for cancer to develop. Some of these known factors are listed below.
Smoking
When someone smokes, they and those around them are exposed to many cancer-causing chemicals that affect organs other than the lungs. These harmful substances are absorbed through the lungs and carried in the bloodstream throughout the body. Women who smoke are about twice as likely as non-smokers to get cervical cancer. Tobacco by-products have been found in the cervical mucus of women who smoke. Researchers believe that these substances damage the DNA of cervix cells and may contribute to the development of cervical cancer. Smoking also makes the immune system less effective in fighting HPV infections.
Having a weakened immune system
Human immunodeficiency virus (HIV), the virus that causes AIDS, damages the immune system and puts women at higher risk for HPV infections. This might explain why women with AIDS have a higher risk for cervical cancer. The immune system is important in destroying cancer cells and slowing their growth and spread. In women with HIV, a cervical pre-cancer might develop into an invasive cancer faster than it normally would.
Another group of women at risk of cervical cancer are those taking drugs to suppress their immune response, such as those being treated for an autoimmune disease (in which the immune system sees the body’s own tissues as foreign and attacks them, as it would a germ) or those who have had an organ transplant.
Chlamydia infection
Chlamydia is a relatively common kind of bacteria that can infect the reproductive system. It is spread by skin to skin contact. Chlamydia infection can cause pelvic inflammation, leading to infertility. Some studies have seen a higher risk of cervical cancer in women whose blood tests and cervical mucus showed evidence of past or current chlamydia infection. Women who are infected with chlamydia often have no symptoms. In fact, they may not know that they are infected at all unless they are tested for chlamydia during a pelvic exam.
A diet low in fruits and vegetables
Women whose diets don’t include enough fruits and vegetables may be at increased risk for cervical cancer.
Being overweight
Overweight women are more likely to develop adenocarcinoma of the cervix.
Long-term use of oral contraceptives (birth control pills)
There is evidence that taking oral contraceptives (OCs) for a long time increases the risk of cancer of the cervix. Research suggests that the risk of cervical cancer goes up the longer a woman takes OCs, but the risk goes back down again after the OCs are stopped and returns to normal about 10 years after stopping.
The American Cancer Society believes that a woman and her doctor should discuss whether the benefits of using OCs outweigh the potential risks.
Intrauterine device (IUD) use
Some research suggests that women who had ever used an intrauterine device (IUD) had a lower risk of cervical cancer. The effect on risk was seen even in women who had an IUD for less than a year, and the protective effect remained after the IUDs were removed.
Using an IUD might also lower the risk of endometrial (uterine) cancer. However, IUDs do have some risks. A woman interested in using an IUD should first discuss the potential risks and benefits with her doctor. Also, a woman with multiple sexual partners should use condoms to lower her risk of sexually transmitted illnesses no matter what other form of contraception she uses.
Having multiple full-term pregnancies
Women who have had 3 or more full-term pregnancies have an increased risk of developing cervical cancer. No one really knows why this is true. One theory is that these women had to have had unprotected intercourse to get pregnant, so they may have had more exposure to HPV. Also, studies have pointed to hormonal changes during pregnancy as possibly making women more susceptible to HPV infection or cancer growth. Another thought is that pregnant women might have weaker immune systems, allowing for HPV infection and cancer growth.
Being younger than 17 at your first full-term pregnancy
Women who were younger than 17 years when they had their first full-term pregnancy are almost twice as likely to get cervical cancer later in life than women who waited to get pregnant until they were 25 years or older.
Economic status
Many low-income women do not have easy access to adequate health care services, including Pap tests. This means they may not get screened or treated for cervical cancers pre-cancers.
Diethylstilbestrol (DES)
DES is a hormonal drug that was given to some women between 1940 and 1971 to prevent miscarriage. Women whose mothers took DES (when pregnant with them) develop clear cell adenocarcinoma of the vagina or cervix more often than would normally be expected. This type of cancer is extremely rare in women who haven’t been exposed to DES. There is about 1 case of this type of cancer in every 1,000 women whose mothers took DES during pregnancy. This means that about 99.9% of “DES daughters” do not develop these cancers.
DES-related clear cell adenocarcinoma is more common in the vagina than the cervix. The risk appears to be greatest in women whose mothers took the drug during their first 16 weeks of pregnancy. The average age of women diagnosed with DES-related clear-cell adenocarcinoma is 19 years. Since the use of DES during pregnancy was stopped by the FDA in 1971, even the youngest DES daughters are older than 40 − past the age of highest risk. Still, there is no age cut-off when these women are felt to be safe from DES-related cancer. Doctors do not know exactly how long women will remain at risk.
DES daughters may also be at increased risk of developing squamous cell cancers and pre-cancers of the cervix linked to HPV.
Having a family history of cervical cancer
Cervical cancer may run in some families. If your mother or sister had cervical cancer, your chances of developing the disease are 2 to 3 times higher than if no one in the family had it. Some researchers suspect some instances of this familial tendency are caused by an inherited condition that makes some women less able to fight off HPV infection than others. In other instances, women from the same family as a patient already diagnosed could be more likely to have one or more of the other non-genetic risk factors.
Can HPV infection be prevented?
There’s no sure way to prevent infection with all the different types of HPV. But there are things you can do to lower your chances of being infected. There are also vaccines that can be used to protect young people from the HPV types most closely linked to cancer and genital warts.
HPV is passed from one person to another during contact with an infected part of the body. Although HPV can be spread during sexual contact – including vaginal, anal, and oral sex – sex isn’t the only way for the infection to spread. All that’s needed is skin-to-skin contact with an area of the body infected with HPV. There may be other ways to become infected with HPV that aren’t yet clear.
HPV can be present for years without causing any symptoms. It doesn’t always cause warts or any other symptoms. Someone can have the virus and pass it on without knowing it.
- Condom use
Condoms (“rubbers”) provide some protection against HPV, but they do not completely prevent infection.
Condoms must be used correctly every time sex occurs. Even then, condoms can’t protect completely because they don’t cover every possible HPV-infected area of the body, such as the skin on the genital or anal area. Still, condoms do provide some protection against HPV, and they also help protect against some other sexually transmitted infections.
- Limiting sex partners
If you are sexually active, limiting the number of sex partners and avoiding sex with people who have had many other sex partners can help lower your risk of exposure to genital HPV. But again, HPV is very common, so having sex with even one other person can put you at risk.
- HPV vaccines
HPV vaccines can prevent infection with certain types of HPV, including types that are linked to HPV-related cancers, as well as types linked to anal and genital warts.
Vaccines are approved for use in males and females. They can only be used to prevent HPV infection – they don’t help treat an existing infection. To work best, the vaccines should be given at or before age 11 or 12.
Things to remember about HPV
- HPV is a very common virus. Most men and women who have ever had sexual contact will get HPV at some time in their lives.
- There is no treatment for HPV, but in most cases it goes away without treatment.
- Having HPV does not mean you will get cancer. Most of the time HPV goes away by itself.
- Certain people are at higher risk for HPV-related health problems. This includes gay and bisexual men and people with weak immune systems (including those who have HIV/AIDS).
- Most HPV infections that lead to cancer can be prevented with vaccines.
- Most cervical cancers can be prevented by regular screening.
References [ + ]