Contents
What is whipworm
Human whipworm is also called Trichuris trichiura, is a roundworm that live in the large intestine and whipworm eggs are passed in the feces of infected persons. If the infected person defecates outside (near bushes, in a garden, or field) or if human feces as used as fertilizer, whipworm eggs (Trichuris trichiura) are deposited on soil. They can then mature into a form that is infective. Whipworm infection (trichuriasis) is caused by ingesting whipworm eggs. This can happen when hands or fingers that have contaminated dirt on them are put in the mouth or by consuming vegetables or fruits that have not been carefully cooked, washed or peeled. The larvae and adult worms live in the intestine of humans and can cause intestinal disease. The name is derived from the worm’s distinctive whip-like shape.
Whipworm is the third most common round worm of humans. Worldwide, with infections more frequent in areas with tropical weather and poor sanitation practices, and among children. It is estimated that 1 billion people in the world are infected with whipworm. Whipworm infection (trichuriasis) occurs in the southern United States. Whipworm, hookworm, and Ascaris are known as soil-transmitted helminths (parasitic worms). Together, they account for a major burden of disease worldwide.
People infected with whipworm can suffer light or heavy infections. Most people with light whipworm infections usually have no symptoms. People with heavy whipworm infections can experience frequent, painful passage of stool that contains a mixture of mucus, water, and blood. Rectal prolapse can also occur. Heavy infections, especially in small children, can cause gastrointestinal problems (abdominal pain, diarrhea, rectal prolapse), become severely anemic and possibly growth retardation. Whipworm infections are treatable with medication prescribed by your health care provider. Whipworm medications are albendazole, mebendazole or ivermectin. Each drug needs to be taken for 3 days. The drugs are effective and appear to have few side effects.
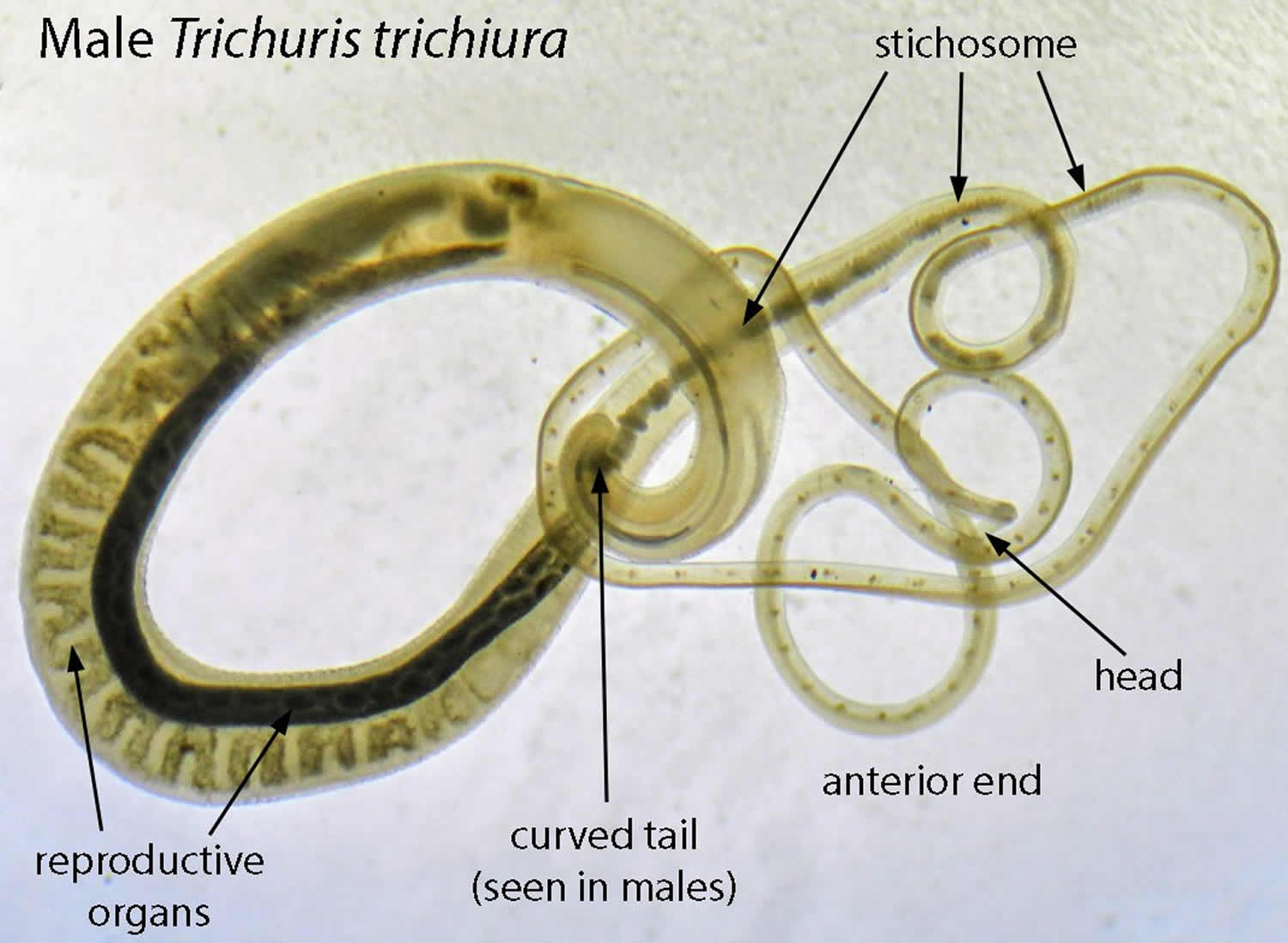
Figure 1. Human whipworm
Whipworm life cycle
The unembryonated eggs are passed with the stool (1). In the soil, the eggs develop into a 2-cell stage (2), an advanced cleavage stage (3) and then they embryonate (4); eggs become infective in 15 to 30 days. After ingestion (soil-contaminated hands or food), the eggs hatch in the small intestine, and release larvae (5), that mature and establish themselves as adults in the colon (6). The adult worms (approximately 4 cm in length) live in the cecum and ascending colon. The adult worms are fixed in that location, with the anterior portions threaded into the mucosa. The females begin to oviposit 60 to 70 days after infection. Female worms in the cecum shed between 3,000 and 20,000 eggs per day. The life span of the adults is about 1 year.
Figure 2. Whipworm life cycle
How is whipworm spread?
Whipworms live in the intestine and whipworm eggs are passed in the feces of infected persons. If the infected person defecates outside (near bushes, in a garden, or field), or if the feces of an infected person are used as fertilizer, then eggs are deposited on the soil. They can then mature into a form that is infective. Roundworm infection is caused by ingesting eggs. This can happen when hands or fingers that have contaminated dirt on them are put in the mouth, or by consuming vegetables or fruits that have not been carefully cooked, washed or peeled.
Who is at risk for whipworm infection?
Infection occurs worldwide in warm and humid climates where sanitation and hygiene are poor, including in temperate climates during warmer months. Persons in these areas are at risk if soil contaminated with human feces enters their mouths or if they eat vegetables or fruits that have not been carefully washed, peeled or cooked.
Whipworm symptoms
People infected with whipworm can suffer light or heavy infections. People with light infections usually have no symptoms. People with heavy symptoms can experience frequent, painful passage of stool that contains a mixture of mucus, water, and blood. Rectal prolapse can also occur. Heavy infection in children can lead to severe anemia, growth retardation, and impaired cognitive development.
Whipworm prevention
- Avoid contact with soil that may be contaminated with human feces, including with human fecal matter (“night soil”) used to fertilize crops.
- Wash your hands with soap and warm water before handling food.
- Teach children the importance of washing hands to prevent infection.
- Wash, peel, or cook all raw vegetables and fruits before eating, particularly those that have been grown in soil that has been fertilized with manure.
Transmission of infection to others can be prevented by:
- Not defecating outdoors,
- Effective sewage disposal systems.
When should you wash your hands?
- Before, during, and after preparing food
- Before eating food
- Before and after caring for someone who is sick
- Before and after treating a cut or wound
- After using the toilet
- After changing diapers or cleaning up a child who has used the toilet
- After blowing your nose, coughing, or sneezing
- After touching an animal, animal feed, or animal waste
- After handling pet food or pet treats
- After touching garbage
How should you wash your hands?
- Wet your hands with clean, running water (warm or cold), turn off the tap, and apply soap.
- Lather your hands by rubbing them together with the soap. Be sure to lather the backs of your hands, between your fingers, and under your nails.
- Scrub your hands for at least 20 seconds. Need a timer? Hum the “Happy Birthday” song from beginning to end twice.
- Rinse your hands well under clean, running water.
- Dry your hands using a clean towel or air dry them.
What should you do if you don’t have soap and clean, running water?
Washing hands with soap and water is the best way to reduce the number of germs on them in most situations. If soap and water are not available, use an alcohol-based hand sanitizer that contains at least 60% alcohol. Alcohol-based hand sanitizers can quickly reduce the number of germs on hands in some situations, but sanitizers do not eliminate all types of germs and might not remove harmful chemicals.
- Hand sanitizers are not as effective when hands are visibly dirty or greasy.
How do you use hand sanitizers?
- Apply the product to the palm of one hand (read the label to learn the correct amount).
- Rub your hands together.
- Rub the product over all surfaces of your hands and fingers until your hands are dry.
Caution: Swallowing alcohol-based hand sanitizers can cause alcohol poisoning. Keep it out of reach of young children.
Whipworm diagnosis
Health care providers can diagnose whipworm by taking a stool sample. By using a microscope, providers can look for the presence of whipworm eggs.
Laboratory Diagnosis
Microscopic identification of whipworm eggs in feces is evidence of infection. Because eggs may be difficult to find in light infections, a concentration procedure is recommended. Because the severity of symptoms depend on the worm burden, quantification of the latter (e.g. with the Kato-Katz technique) can prove useful.
Examination of the rectal mucosa by proctoscopy (or directly in case of prolapses) can occasionally demonstrate adult worms.
Whipworm treatment
Whipworm is effectively treated with albendazole, mebendazole or ivermectin. Each drug needs to be taken for 3 days. Dosage guidelines are the same for children as for adults. Albendazole should be taken with food. Ivermectin should be taken with water on an empty stomach and the safety of ivermectin for children weighing less than 15 kg has not been established. Neither albendazole nor ivermectin is FDA-approved for treating whipworm.
Whipworm medication
Oral albendazole is available for human use in the United States.
Mebendazole is available in the United States only through compounding pharmacies.
Oral ivermectin is available for human use in the United States.
| Drug | Dosage for adults and children |
|---|---|
| Albendazole | 400 mg orally for 3 days |
| Mebendazole | 100 mg orally twice a day for 3 days |
| Ivermectin | 200 mcg/kg/day orally for 3 days |
Albendazole
Treatment in Pregnancy
Albendazole is pregnancy category C.
- Pregnancy Category C: Either studies in animals have revealed adverse effects on the fetus (teratogenic or embryocidal, or other) and there are no controlled studies in women or studies in women and animals are not available. Drugs should be given only if the potential benefit justifies the potential risk to the fetus.
Data on the use of albendazole in pregnant women are limited, though the available evidence suggests no difference in congenital abnormalities in the children of women who were accidentally treated with albendazole during mass prevention campaigns compared with those who were not. In mass prevention campaigns for which the World Health Organization (WHO) has determined that the benefit of treatment outweighs the risk, WHO allows use of albendazole in the 2nd and 3rd trimesters of pregnancy. However, the risk of treatment in pregnant women who are known to have an infection needs to be balanced with the risk of disease progression in the absence of treatment.
Treatment During Breastfeeding
It is not known whether albendazole is excreted in human milk. Albendazole should be used with caution in breastfeeding women.
Treatment in Pediatric Patients
The safety of albendazole in children less than 6 years old is not certain. Studies of the use of albendazole in children as young as one year old suggest that its use is safe. According to WHO guidelines for mass prevention campaigns, albendazole can be used in children as young as 1 year old. Many children less than 6 years old have been treated in these campaigns with albendazole, albeit at a reduced dose.
Mebendazole
Treatment in Pregnancy
Mebendazole is in pregnancy category C.
- Pregnancy Category C: Either studies in animals have revealed adverse effects on the fetus (teratogenic or embryocidal, or other) and there are no controlled studies in women or studies in women and animals are not available. Drugs should be given only if the potential benefit justifies the potential risk to the fetus.
Data on the use of mebendazole in pregnant women are limited. The available evidence suggests no difference in congenital anomalies in the children of women who were treated with mebendazole during mass treatment programs compared with those who were not. In mass treatment programs for which the World Health Organization (WHO) has determined that the benefit of treatment outweighs the risk, WHO allows use of mebendazole in the 2nd and 3rd trimesters of pregnancy. The risk of treatment in pregnant women who are known to have an infection needs to be balanced with the risk of disease progression in the absence of treatment.
Treatment During Breastfeeding
It is not known whether mebendazole is excreted in breast milk. The WHO classifies mebendazole as compatible with breastfeeding and allows the use of mebendazole in lactating women.
Treatment in Pediatric Patients
The safety of mebendazole in children has not been established. There is limited data in children age 2 years and younger. Mebendazole is listed as an intestinal antihelminthic medicine on the WHO Model List of Essential Medicines for Children, intended for the use of children up to 12 years of age.
Ivermectin
Treatment in Pregnancy
Ivermectin is pregnancy category C.
- Pregnancy Category C: Either studies in animals have revealed adverse effects on the fetus (teratogenic or embryocidal, or other) and there are no controlled studies in women or studies in women and animals are not available. Drugs should be given only if the potential benefit justifies the potential risk to the fetus.
Data on the use of ivermectin in pregnant women are limited, though the available evidence suggests no difference in congenital abnormalities in the children of women who were accidentally treated during mass prevention campaigns with ivermectin compared with those who were not. The World Health Organization (WHO) excludes pregnant women from mass prevention campaigns that use ivermectin. However, the risk of treatment in pregnant women who are known to have an infection needs to be balanced with the risk of disease progression in the absence of treatment.
Treatment During Breastfeeding
Ivermectin is excreted in low concentrations in human milk. Ivermectin should be used in breast-feeding women only when the risk to the infant is outweighed by the risk of disease progress in the mother in the absence of treatment.
Treatment in Pediatric Patients
The safety of ivermectin in children who weigh less than 15kg has not been demonstrated. According to the WHO guidelines for mass prevention campaigns, children who are at least 90 cm tall can be treated safely with ivermectin. The WHO growth standard curves show that this height is reached by 50% of boys by the time they are 28 months old and by 50% of girls by the time they are 30 months old, many children less than 3 years old been safely treated with ivermectin in mass prevention campaigns, albeit at a reduced dose.
What is preventive treatment?
In developing countries, groups at higher risk for soil-transmitted helminth infections (hookworm, Ascaris, and whipworm) are often treated without a prior stool examination. Treating in this way is called preventive treatment (or “preventive chemotherapy”). The high-risk groups identified by the World Health Organization are preschool and school-age children, women of childbearing age (including pregnant women in the 2nd and 3rd trimesters and lactating women) and adults in occupations where there is a high risk of heavy infections. School-age children are often treated through school-health programs and preschool children and pregnant women at visits to health clinics.
What is mass drug administration?
The soil-transmitted helminths (hookworm, Ascaris, and whipworm) and four other “neglected tropical diseases” (river blindness, lymphatic filariasis, schistosomiasis and trachoma) are sometimes treated through mass drug administrations. Since the drugs used are safe and inexpensive or donated, entire risk groups are offered preventive treatment. Mass drug administrations are conducted periodically (often annually), commonly with drug distributors who go door-to-door. Multiple neglected tropical diseases are often treated simultaneously using mass drug administrations.