Contents
What is Belly Fat
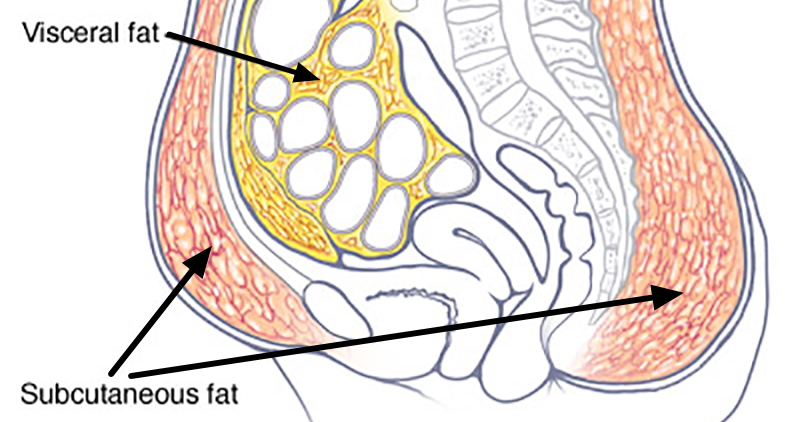
Belly fat is both the Visceral fat and Subcutaneous fat. Subcutaneous fat is the belly fat you can feel if you pinch excess skin and tissue around your middle – also commonly known as a “spare tire” or “love handle”. Visceral fat is belly fat that accumulates in your abdomen in the spaces between your organs – fat that build up in the spaces between and around your internal organs like around your heart, lungs, liver, pancreas, kidneys, stomach and intestines. Too much visceral fat is strongly linked with a greater risk of serious health problems 1.
A 6 year follow up study supported by the National Heart, Lung and Blood Institute published in the American Heart Association journal, Circulation, linked regular consumption of sugar-sweetened drinks (such as sodas, alcohol and fruit drinks) to increased visceral fat, a type of body fat that may contribute to a higher risk of diabetes and heart disease 2, 3.
More than 78 million adults in the United States were obese in 2009–2010 4. Current estimates are that 69 percent of adults are either overweight or obese (overweight is defined as a BMI of 25 to 29.9 kg/m2 and obesity as a BMI of ≥30 kg/m2), with approximately 35 percent obese 5. Perhaps of greatest concern is the shift in the obese BMI distribution to a higher prevalence of ‘extreme obesity’ with BMI ≥40 kg/m2, which was 6.6 percent in years 2009–2010 6 and the latest available rates 4 indicate no decline in obesity rates. These latest data from the National Health and Nutrition Examination Survey (NHANES) report that for both men and women obesity estimates for 2009–2010 did not differ significantly from estimates for 2003–2008. Yet, overweight and obesity continue to be highly prevalent, especially in some racial and ethnic minority groups as well as in those with lower incomes and less education.
When compared with normal weight individuals, obese patients incur 46 percent increased inpatient costs, 27 percent more physician visits and outpatient costs, and 80 percent increased spending on prescription drugs. The medical care costs of obesity in the United States are staggering. In 2008 dollars, these costs totaled about $147 billion 7.
Obesity raises the risk for morbidity from hypertension, dyslipidemia, type 2 diabetes, coronary heart disease, stroke, gallbladder disease, osteoarthritis, sleep apnea and respiratory problems, and some cancers 1. Obesity is also associated with increased risk in all-cause and cardiovascular mortality. The biomedical, psychosocial, and economic consequences of obesity have substantial implications for the health and well-being of the U.S. population.
Belly fat is a more dangerous fat
The panel 8 identified excess abdominal fat as associated with greater health risks (abnormal lipid, prothrombotic, and proinflammatory risk factors as well as organ infiltration by fat) than that in peripheral regions. Waist circumference is the most practical measure of abdominal fat. The panel identified waist circumference cutpoints of 40 inches for men and 35 inches for women to aid in individual risk assessment.
The trouble with belly fat is that it’s not limited to the extra layer of padding located just below the skin (subcutaneous fat). It also includes visceral fat — which lies deep inside your abdomen, surrounding your internal organs.
Although subcutaneous fat poses cosmetic concerns, visceral fat is linked with far more dangerous health problems. Regardless of your overall weight, having a large amount of belly fat increases your risk of:
- Cardiovascular disease and heart disease
- Insulin resistance and type 2 diabetes
- Colorectal cancer and breast cancer
- Sleep apnea
- Raised levels of triglycerides and abnormal cholesterol
- Premature death from any cause
- High blood pressure
- Alzheimer’s Disease and Dementia
Obesity and Dementia
Dementia is also a major public health problem that will continue to increase rapidly as people live to older ages. By age 85 years, the incidence of dementia approaches 10% 9 and its prevalence is approximately 30% 10. The most common form of dementia is Alzheimer disease, a degenerative dementia. Vascular dementia, the second most common dementia, is a direct consequence of cerebrovascular disorders. Recently, however, several studies suggest that there may be an association between Alzheimer’s disease and vascular disorders, such as atherosclerosis 11, hypertension, coronary heart disease, and diabetes mellitus 12. Since overweight and obesity increase risk of vascular disorders 13, overweight and obesity may be risk factors for both Alzheimer disease and Vascular dementia.
Dr. Deborah Gustafson, Associate Professor, Neuropsychiatric Epidemiology Unit, University of Gothenburg, Sweden, and her colleagues analyzed data on dementia incidence in 290 Swedish women who were age 70 at the beginning of the study. Women who developed dementia in their 80s had an average BMI at age 70 that was 2 units (kg/m2) higher than that of women in their 80s who did not develop dementia. Imaging studies of women in another population study in Gothenburg showed that those with atrophy in their brains’ temporal lobes were likely to have higher BMIs. Her data suggested that overweight at high ages is a risk factor for dementia, particularly Alzheimer’s Disease, in women 14. This study may have profound implications for dementia prevention.
Research also has associated belly fat with an increased risk of premature death — regardless of overall weight. In fact, some studies have found that even when people were considered a normal weight based on standard body mass index (BMI) measurements, a large waistline increased the risk of dying of cardiovascular disease.
This visceral fat in surrounding your internal organs makes toxins that affect the way your body works, among them are chemicals called cytokines that boost your chances of heart disease and make your body less sensitive to insulin, which can bring on diabetes. Cytokines also cause inflammation, which can lead to certain cancers, says a researcher at the American Cancer Society. In recent years, scientists have uncovered links between belly fat and cancers of the colon, esophagus, and pancreas. Carrying too much belly fat puts you at risk of developing high blood pressure, Type 2 diabetes, heart disease, stroke, migraines, and dementia.
Your waist size is a clue to whether you’re at high risk for type 2 diabetes, high blood pressure, high cholesterol, and heart disease. To measure your waist circumference, use a tape measure and visit waist-hip-ratio measurement page.
Belly fat is sneaky. Because it’s tucked away inside your body, giving you a false sense of security about how healthy you actually are. You may not be seriously overweight, but that doesn’t mean you don’t have a problem.
How can you tell if your belly fat is putting your health at risk ? That part is easy. No special blood tests or scans are required. All you need is a tape measure. The size of your waist says it all – visit waist-hip-ratio measurement page.
The higher the number, the greater the danger your tummy poses to your health.
- For women, a waist measurement of 35 inches or more is cause for concern.
- For men, a waist measurement of 40 inches or more could spell trouble.
If you have to move to a bigger pants size, even if your weight is considered normal for your height, or even if you haven’t noticed much weight gain, that’s an important sign it’s time to start eating better and exercising more.
Thin People Have It, Too – Even if you’re thin, you can still have too much visceral fat. How much you have is partly about your genes, and partly about your lifestyle, especially how active you are. Visceral fat likes inactivity. In one study, thin people who watched their diets but didn’t exercise were more likely to have too much visceral fat.
The key is to be active, no matter what size you are.
Your weight is largely determined by how you balance the calories you eat with the energy you burn. If you eat too much and exercise too little, you’re likely to carry excess weight — including belly fat.
Alcohol’s calories contribute to beer belly
Drinking excess alcohol can cause you to gain belly fat — the beer belly. However, beer alone isn’t to blame. Drinking too much alcohol of any kind can increase belly fat, because alcohol contains calories.
For men age 65 and younger, moderation means up to two drinks a day. For men older than age 65, it means up to one drink a day. The less you drink, the fewer calories you’ll consume and the less likely you’ll be to gain belly fat.
Age and genetics may contribute to gaining belly fat
Aging does play a role too. As you age, you lose muscle — especially if you’re not physically active. Loss of muscle mass decreases the rate at which your body uses calories, which can make it more challenging to maintain a healthy weight. According to the 2015-2020 Dietary Guidelines for Americans, men in their 50s need about 200 fewer calories daily than they do in their 30s due to this muscle loss.
Your genes also can contribute to your chances of being overweight or obese, as well as play a role in where you store fat. However, balancing the calories you consume with activity can help prevent weight gain, despite your age and genetics.
Losing weight and exercising will shrink your belly fat
You can tone abdominal muscles with crunches or other targeted abdominal exercises, but just doing these exercises won’t get rid of belly fat. However, visceral fat responds to the same diet and exercise strategies that can help you shed excess pounds and lower your total body fat. To battle the bulge:
- Eat a healthy diet. Emphasize plant-based foods, such as fruits, vegetables and whole grains. Leafy greens, whole grains, nuts, fibers and beans are all good for keeping away the fat that stays deep in your belly. Choose lean sources of protein such as fish and low-fat dairy products. Limit saturated fat, found in meat and high-fat dairy products, such as cheese and butter. Also limit processed meats. Choose moderate amounts of monounsaturated and polyunsaturated fats — found in fish, nuts and certain vegetable oils — instead. Eat healthy for the long haul and avoid fad diets , crash diets and quick fixes.
- Swap fruits. Go for strawberries, blueberries, and raspberries instead of high-sugar bananas and grapes. They can quell your cravings just as well.
- Keep portion sizes in check. Even when you’re making healthy choices, calories add up. At home, slim down your portion sizes. In restaurants, share meals — or eat half your meal and take the rest home.
- Go natural. Processed foods are not your friends. When you’re in a rush, it’s easy to overlook the fact that packaged foods are often loaded with trans fats, sugar, and salt — all guaranteed to boost belly fat.
- Replace and skip sugary beverages like alcohol and fruit juice with water. Whether it’s a latte, a regular soda, a mug of beer or a glass of wine, it’s got calories. Drink water or beverages with artificial sweetener instead.
- Consider doing Intermittent Fasting or the Fast Diet (5:2 Diet Plan).
- Try a Mediterranean-style eating plan. The diet is good for your heart and can lower blood sugar. You’ll eat more fruits, grains, beans, and nuts, along with healthy fats like olive oil.
- Include physical activity in your daily routine. For most healthy adults, the Department of Health and Human Services recommends moderate aerobic activity, such as brisk walking, for at least 150 minutes a week or vigorous aerobic activity, such as jogging, for at least 75 minutes a week. If you use a step counter, remember that it takes an average of 10,000 steps per day to prevent weight gain. Some studies indicate it might take 15,000 steps per day to prevent the regain of weight after significant weight loss. In addition, strength training exercises like lifting weights are recommended at least twice a week. Muscle burns more calories than fat, so the more you have, the more pounds you’ll torch, even when you’re sitting still. Think about hitting the gym instead of the trail. In one study, healthy middle-aged men who did 20 minutes of daily weight training gained less abdominal fat than men who spent the same time doing aerobic exercises, such as biking. Strength training is also good for women and it won’t make you bulky. You still need to do some cardio, but make sure strength training is in the mix. If you want to lose weight or meet specific fitness goals, you’ll need to exercise more. Exercise also has the most immediate benefits, because it gets at both obesity and stress under control. You can add bursts of higher intensity to any workout. Research shows that a few quick bursts of high-intensity exercise — such as a 30-second sprint or intense pullup set — may be more effective, and easier to fit into your schedule.
- Don’t skimp on sleep. Lack of sleep can lead to weight gain, diabetes, and other health problems. Four or 5 hours a night just isn’t enough. Try to get between 7 and 8 hours of sleep. In one study, people who got 6 to 7 hours of sleep per night gained less visceral fat over 5 years compared to those who slept 5 or fewer hours per night or 8 or more hours per night.
- Manage your stress. The stress hormone cortisol can override your diet and workouts. When it goes through your body, fat deposits relocate to your belly area. Everyone has stress. How you handle it matters. The best things you can do include relaxing with friends and family, meditating, exercising to blow off steam, and getting counseling. That leaves you healthier and better prepared to make good choices for yourself. Exercise and meditation can both be great ways to dial down your stress to nontoxic levels.
- Don’t Smoke. As if you need another reason to quit. Smoking makes you more likely to store fat in your belly, rather than your hips and thighs. And that’s bad. And it’s also a cause of diabetes. And cancer. And heart disease. And lung disease. And … you get the idea. If you’ve tried before, try again.
Losing belly fat takes effort and patience. To lose excess fat and keep it from coming back, aim for slow and steady weight loss — up to 2 pounds (1 kilogram) a week.
Forget cosmetic surgery, it isn’t the solution here. Liposuction doesn’t reach inside the abdominal wall. So it can’t get rid of visceral belly fat.
It comes down to personal choice. You have to decide that this is what you want to do. There’s no magic. You just have to make up your mind that you’re going to turn your health around.
In a study published in The New England Journal of Medicine in 2009, followed 811 overweight adults over 2 years 15, who were prescribed Low Calorie Diets (a deficit of 750 kcal per day from baseline, as calculated from the person’s resting energy expenditure and activity level) and all the low calorie diets should include 8% or less of saturated fat, at least 20 g of dietary fiber per day, and 150 mg or less of cholesterol per 1000 kcal). Carbohydrate-rich foods with a low glycemic index were recommended in each diet. Each participant’s caloric prescription represented one of the four diets:
- Fat 20%, Protein 15% and Carbohydrate 65% (Low-fat and Average-protein and High carb)
- Fat 20%, Protein 25% and Carbohydrate 55% (Low-fat and High-protein and Average carb)
- Fat 40%, Protein 15% and Carbohydrate 45% (High-fat and Average-protein and Average carb)
- Fat 40%, Protein 25% and Carbohydrate 35% (High-fat and High-protein and Low carb)
- All participants’ goal for physical activity was 90 minutes of moderate exercise per week. Participation in exercise was monitored by questionnaire and by the online self-monitoring tool.
Group sessions were held once a week, 3 of every 4 weeks during the first 6 months and 2 of every 4 weeks from 6 months to 2 years; individual sessions were held every 8 weeks for the entire 2 years. Daily meal plans in 2-week blocks were provided. Participants were instructed to record their food and beverage intake in a daily food diary and in a web-based self-monitoring tool that provided information on how closely their daily food intake met the goals for macronutrients and energy. Behavioral counseling was integrated into the group and individual sessions to promote adherence to the assigned diets. Contact among the groups was avoided.
At 6 months, participants assigned to each diet had lost an average of 6 kg, which represented 7% of their initial weight; they began to regain weight after 12 months.
- By 2 years, weight loss remained similar in those who were assigned to a diet with 15% protein and those assigned to a diet with 25% protein (3.0 and 3.6 kg, respectively); in those assigned to a diet with 20% fat and those assigned to a diet with 40% fat (3.3 kg for both groups); and in those assigned to a diet with 65% carbohydrates and those assigned to a diet with 35% carbohydrates (2.9 and 3.4 kg, respectively).
- Among the 80% of participants who completed the trial, the average weight loss was 4 kg; 14 to 15% of the participants had a reduction of at least 10% of their initial body weight. Satiety, hunger, satisfaction with the diet, and attendance at group sessions were similar for all diets; attendance was strongly associated with weight loss (0.2 kg per session attended). The diets improved lipid-related risk factors and fasting insulin levels.
Conclusions: Reduced-calorie diets result in clinically meaningful weight loss regardless of which macronutrients they emphasize. All of the diets resulted in meaningful weight loss, despite the differences in macronutrient composition 15.
The study also found that the more group counseling sessions participants attended, the more weight they lost, and the less weight they regained. This supports the idea that not only is what you eat important, but behavioral, psychological, and social factors are important for weight loss as well 15.
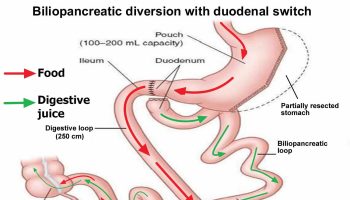
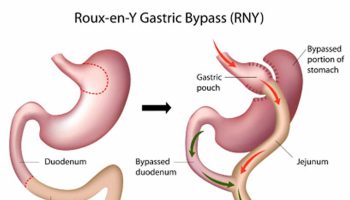
Bariatric Surgery: Belly Fat’s Last Resort
For many people, bariatric weight loss surgery maybe a good option as a last resort. These procedures can shrink the stomach’s volume so people feel full sooner and lose weight. Bariatric surgeries (also called gastric bypass) can also reduce the absorption of nutrients, causing weight loss.
If your back is against the wall, you’re suffering from health problems, and your quality of life is significantly compromised, it’s an appropriate option. If you’re unable to achieve meaningful and lasting weight loss through nonsurgical measures, you may consider having a bariatric surgery.
- US Department of Health and Human Services, National Institutes of Health. Managing Overweight and Obesity in Adults: Systematic Evidence Review from the Expert Panel. https://www.nhlbi.nih.gov/sites/www.nhlbi.nih.gov/files/obesity-evidence-review.pdf[↩][↩]
- Circulation. 2016;CIRCULATION AHA.115.018704. Sugar-Sweetened Beverage Consumption is Associated With Change of Visceral Adipose Tissue Over 6 Years of Follow-Up. http://circ.ahajournals.org/content/early/2016/01/06/CIRCULATIONAHA.115.018704[↩]
- Stanhope KL, Schwarz JM, Keim NL, Griffen SC, Bremer AA, Graham JL, Hatcher B, Cox CL, Dyachenko A, Zhang W, McGahan JP, Seibert A, Krauss RM, Chiu S, Schaefer EJ, Ai M, Otokozawa S, Nakajima K, Nakano T, Beysen C, Hellerstein MK, Berglund L, Havel PJ. Consuming fructose-sweetened, not glucose-sweetened, beverages increases visceral adiposity and lipids and decreases insulin sensitivity in overweight/obese humans. J Clin Invest. 2009;119(5):1322–1334. https://www.ncbi.nlm.nih.gov/pmc/articles/PMC2673878/[↩]
- Ogden CL, Carroll MD, Kit BK, Flegal KM. Prevalence of Obesity in the United States, 2009–2010. NCHS Data Brief. 2012;Jan(82):1-8.[↩][↩]
- Flegal KM, Carroll MD, Kit BK, Ogden CL. Prevalence of obesity and trends in the distribution of body mass index among US adults, 1999-2010. JAMA. 2012;307(5):491-7. [↩]
- Ogden CL, Carroll MD. Prevalence of Overweight, Obesity, and Extreme Obesity Among Adults: United States, Trends 1960–1962 Through 2007–2008. Hyattsville, MD: National Center for Health Statistics, 2010.[↩]
- Finkelstein EA, Trogdon JG, Cohen JW, Dietz W. Annual medical spending attributable to obesity: payer-and service-specific estimates. Health Aff (Millwood). 2009;28(5):w822-31.[↩]
- US Department of Health and Human Services, National Insitutes of Health. National Heart, Lung and Blood Institute. Systematic Evidence Review From the Obesity Expert Panel, 2013. Managing Overweight and Obesity in Adults[↩]
- Aevarsson OSkoog I A population-based study on the incidence of dementia disorders between 85 and 88 years of age. J Am Geriatr Soc. 1996;441455- 1460.[↩]
- Skoog INilsson LPalmertz BAndreasson L-ASvanborg A A population-based study of dementia in 85-year-olds. N Engl J Med. 1993;328153- 158. http://www.nejm.org/doi/full/10.1056/NEJM199301213280301[↩]
- Hofman AOtt ABreteler MMB et al. Atherosclerosis, apolipoprotein E, and prevalence of dementia and Alzheimer’s disease in the Rotterdam Study. Lancet. 1997;349151- 154. http://www.thelancet.com/journals/lancet/article/PIIS0140-6736(96)09328-2/fulltext[↩]
- Skoog IKalaria RNBreteler MM Vascular factors and Alzheimer disease. Alzheimer Dis Assoc Disord. 1999;13 (Suppl 3) S106- S114.[↩]
- Kopelman PG Obesity as a medical problem. Nature. 2000;404635- 643[↩]
- Arch Intern Med. 2003;163(13):1524-1528. doi:10.1001/archinte.163.13.1524. – An 18-Year Follow-up of Overweight and Risk of Alzheimer Disease – http://jamanetwork.com/journals/jamainternalmedicine/fullarticle/215834[↩]
- N Engl J Med. 2009 Feb 26;360(9):859-73. doi: 10.1056/NEJMoa0804748. Comparison of weight-loss diets with different compositions of fat, protein, and carbohydrates. https://www.ncbi.nlm.nih.gov/pubmed/19246357[↩][↩][↩]