Contents
What is an abscess
An abscess is a painful collection of pus, usually caused by a bacterial infection. Abscesses can develop anywhere in your body – under the skin, in an organ or between your organs. An abscess is often painful. If it is under the skin, abscess can also be called a boil.
Most abscesses are caused by a bacterial infection. When bacteria enter your body, your immune system sends infection-fighting white blood cells to the affected area.
As the white blood cells attack the bacteria, some nearby tissue dies, creating a hole which then fills with pus to form an abscess. The pus contains a mixture of dead tissue, white blood cells and bacteria.
Infective abscesses may affect healthy people, but they are more common in the following circumstances.
- Metabolic syndrome and obesity
- Smoking
- Diabetes
- Immune compromise
- IV drug users
Internal abscesses often develop as a complication of an existing condition, such as an infection elsewhere in your body. For example, if your appendix bursts as a result of appendicitis, bacteria can spread inside your tummy (abdomen) and cause an abscess to form.
See your doctor if you think you may have an abscess. They can examine a skin abscess or refer you to hospital if you may have an internal abscess.
There are several tests available to help diagnose an abscess, depending on where it’s located.
Treating an abscess
A small skin abscess may drain naturally, or simply shrink, dry up and disappear without any treatment.
However, larger abscesses may need to be treated with antibiotics to clear the infection, and the pus may need to be drained. This will usually be done either by inserting a needle through your skin or by making a small incision in the skin over the abscess.
Types of abscesses
Abscesses can also develop in other parts of the body, such as the brain, kidney, or other organs, usually as a complication of an existing medical condition.
There are many different types of abscesses, including:
- Skin abscesses or boils – which develop under the skin often affecting the face, throat, armpits or groin
- Dental abscesses – a build-up of pus under a tooth or in the supporting gum and bone
- Pilonidal abscesses or cysts – a build-up of pus in the skin of the cleft of the buttocks (where the buttocks separate)
- Anal or anorectal abscesses – a build-up of pus in the rectum and anus
- Breast abscesses – can develop if mastitis is not treated quickly
- Vaginal abscesses also called Bartholin’s abscess – a build-up of pus inside one of the Bartholin’s glands, which are found on each side of the opening of the vagina
- A brain abscess – a rare but potentially life-threatening build-up of pus inside the skull
- A quinsy (peritonsillar abscess) – a build-up of pus between one of your tonsils and the wall of your throat
- A spinal cord abscess – a build-up of pus around the spinal cord
- Internal abscesses – which develop inside the body, in an organ or in the spaces between organs
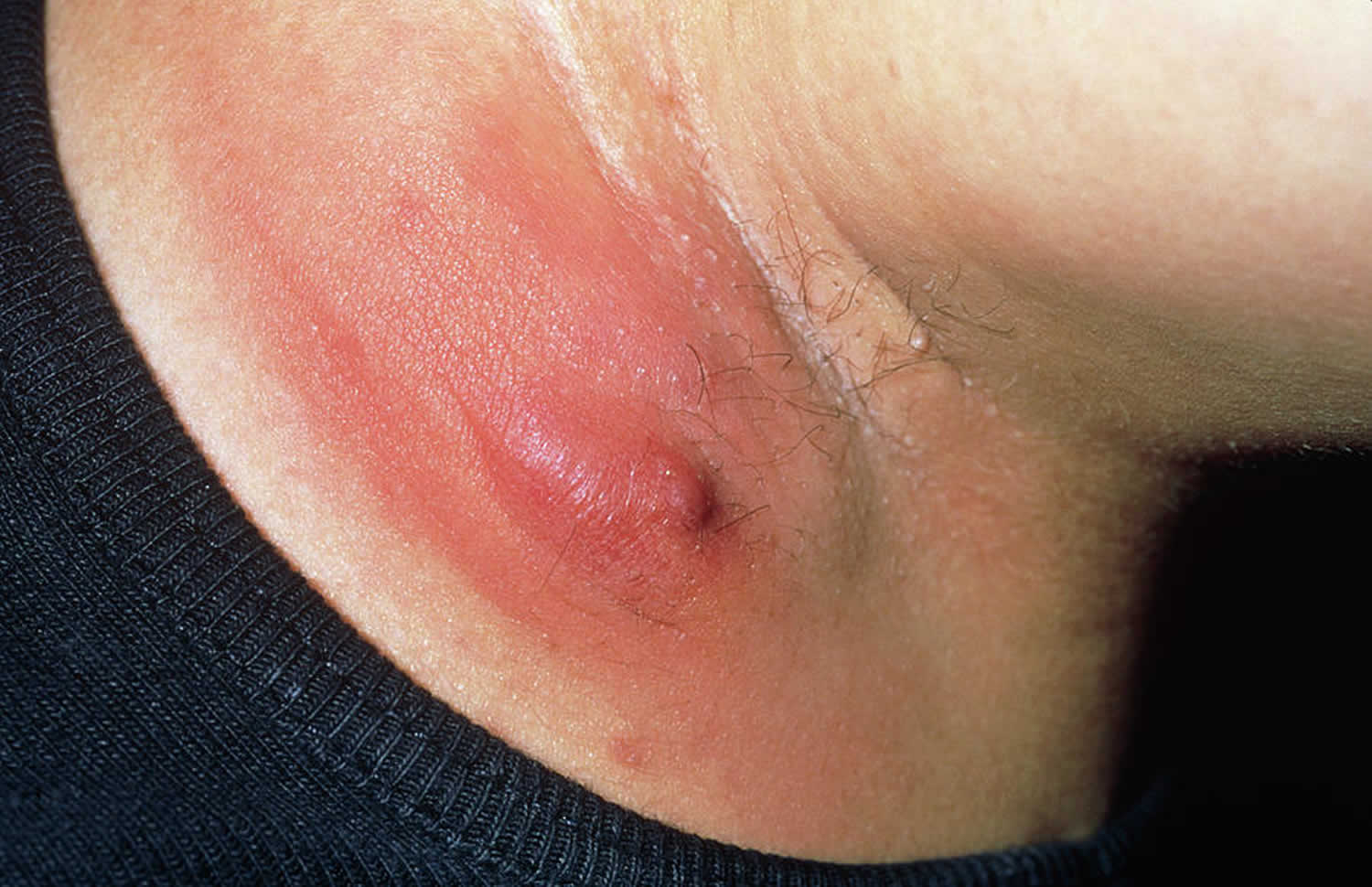
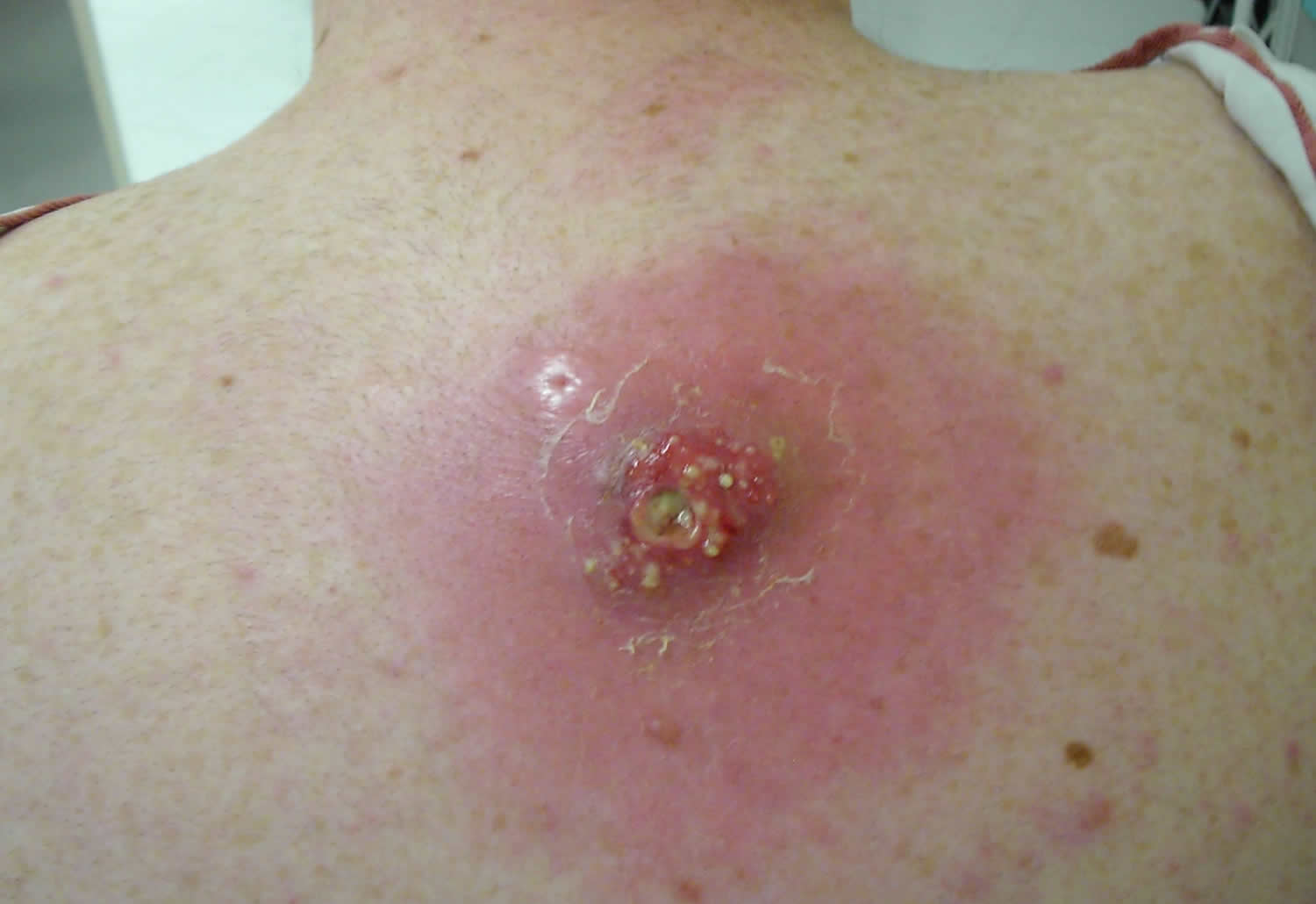
Skin abscess
A skin abscess is a buildup of pus in or on the skin. A skin abscess often appears as a swollen, pus-filled lump under the surface of the skin. You may also have other symptoms of an infection, such as a high temperature (fever) and chills.
A boil is a common example of a skin abscess.
When bacteria gets under the surface of your skin, an abscess can form. This can occur anywhere on the body, although skin abscesses tend to be more common in the:
- armpit or underarms
- hands, legs and feet
- face
- trunk
- genitals
- groin
- buttocks
Bacteria can get into your skin and cause an abscess if you have a minor skin wound, such as a small cut or graze, or if a sebaceous gland (oil gland) or sweat gland in your skin becomes blocked.
When to see a medical professional
See your doctor if you have any signs of skin infection, including:
- Drainage of any kind
- Fever
- Pain
- Redness
- Swelling
See your provider right away if you develop new symptoms during or after treatment of a skin abscess.
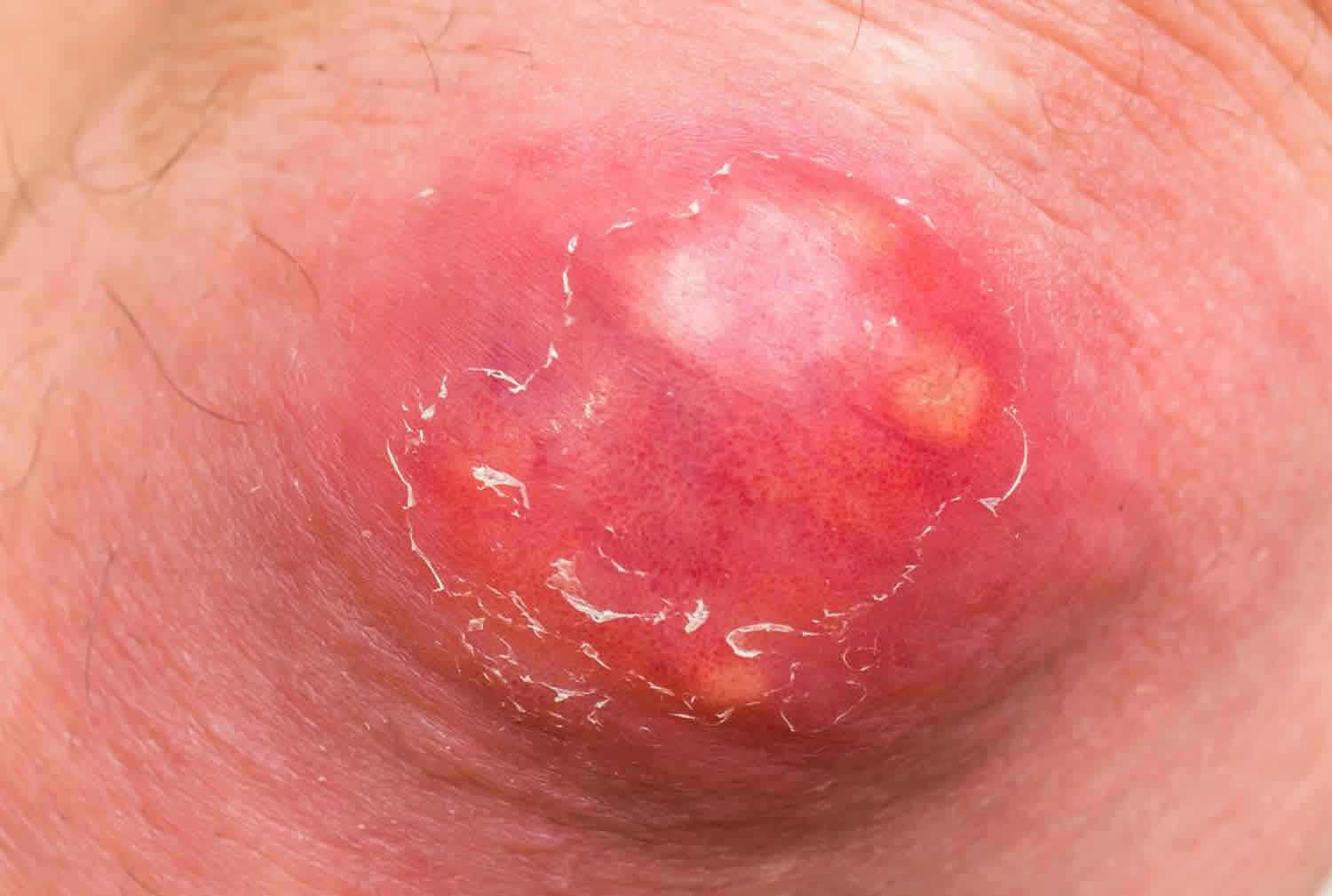
Figure 1. Skin abscess
Skin abscess causes
Skin abscesses are common and affect people of all ages. Skin abscesses occur when an infection causes pus to collect in the skin.
Skin abscesses may occur after developing:
- A bacterial infection (often staphylococcus)
- A minor wound or injury
- Boils
- Folliculitis (infection in a hair follicle)
A skin abscess may occur anywhere on the body.
Skin abscess prevention
Most skin abscesses are caused by bacteria getting into a minor wound, the root of a hair or a blocked oil or sweat gland.
Ensuring that your skin is clean, healthy and largely free of bacteria can help reduce the risk of skin abscesses developing.
You can reduce the risk of bacteria spreading by:
- washing your hands regularly
- encouraging people in your family to wash their hands regularly
- using separate towels and not sharing baths
- waiting until your skin abscess is fully treated and healed before using any communal equipment, such as gym equipment, saunas or swimming pools
Don’t squeeze the pus out of the abscess yourself, because this can easily spread the bacteria to other areas of your skin. If you use tissues to wipe any pus away from your abscess, dispose of them straight away to avoid germs spreading. Wash your hands after you’ve disposed of the tissues.
Take care when shaving your face, legs, underarm areas or bikini area to avoid nicking your skin. Clean any wounds immediately and visit your doctor if you think there may be something trapped in your skin. Don’t share razors or toothbrushes.
It may also help to reduce your risk of skin abscesses by:
- maintaining a healthy, balanced diet
- losing weight if you’re overweight or obese
- stopping smoking
Skin abscess symptoms
Skin abscesses symptoms may include:
- A high temperature (fever) or chills, in some cases
- Local swelling around the infected spot
- Warmth and redness in the affected area
- Hardened skin tissue
- A smooth swelling under your skin that can feel hard or firm
- Skin lesion that may be an open or closed sore, or a raised area
- Tenderness, pain and warmth in the affected area
- A visible build-up of white or yellow pus under the skin in the affected area
- Fluid or pus drainage
Possible complications
Complications that can occur from an abscess include:
- Spread of the infection in the same area
- Spread of the infection into the blood and throughout the body
- Tissue death (gangrene)
Skin abscess diagnosis
Your health care provider can diagnose the problem by looking at the affected area. A sample of pus may be taken from your abscess and sent for testing. This allows the specific bacteria causing the abscess to be identified, which can help determine the best way of treating it.
If you’ve had more than one skin abscess, you may be asked to give a urine sample. This will be tested for glucose, which is a sign of diabetes. People with diabetes have an increased risk of developing skin abscesses.
If you have recurring boils and abscesses, your doctor may ask the laboratory to test the bacteria further to see if it’s producing Panton-Valentine leukocidin (PVL) toxin. Additional treatments may be recommended, such as a body wash or an antibiotic cream, to stop these bacteria living on the body.
Skin abscess treatment
You can apply moist heat (such as warm compresses) to help the abscess drain and heal faster. DO NOT push and squeeze on the abscess.
Some small skin abscesses may drain naturally and get better without the need for treatment.
For larger or persistent skin abscesses, your doctor may prescribe a course of antibiotics to help clear the infection and prevent it from spreading. However, antibiotics alone may not be enough to clear a skin abscess, and the pus may need to be drained to clear the infection. If a skin abscess isn’t drained, it may continue to grow and fill with pus until it bursts, which can be very painful and can cause the infection to spread or recur.
If you have methicillin-resistant Staphylococcus aureus (MRSA) or another staph infection, follow instructions for self-care at home.
Sometimes, especially with recurrent infections, you may need to wash off all the bacteria from your body to prevent re-infection (decolonisation). This can be done using antiseptic soap for most of your body and an antibiotic cream for the inside of your nose.
Incision and drainage
If your skin abscess needs draining, you’ll probably have a small operation carried out under anaesthetic – usually a local anaesthetic, where you remain awake and the area around the abscess is numbed.
Your doctor may cut open the abscess and drain it. If this is done:
- Numbing medicine will be put on your skin.
- Packing material may be left in the wound to help it heal.
You may need to take antibiotics by mouth to control the infection. A recent study 1 suggested that, for small uncomplicated skin abscesses, antibiotics after incision and drainage improve the chance of short term cure compared with placebo. an expert panel makes a weak recommendation in favour of trimethoprim-sulfamethoxazole (TMP-SMX, co-trimoxazole) or clindamycin in addition to incision and drainage over incision and drainage alone. For patients who have chosen to initiate antibiotics, the panel issues a strong recommendation for trimethoprim-sulfamethoxazole or clindamycin rather than a cephalosporin and a weak recommendation for trimethoprim-sulfamethoxazole rather than clindamycin 2. Clindamycin has a substantially higher risk of diarrhea than trimethoprim-sulfamethoxazole. Cephalosporins are probably not effective 1.
During the procedure, the surgeon makes a cut (incision) in the abscess, to allow the pus to drain out. They may also take a sample of pus for testing.
Once all of the pus has been removed, the surgeon will clean the hole that is left by the abscess using sterile saline (a salt solution).
The abscess will be left open but covered with a wound dressing, so if any more pus is produced it can drain away easily. If the abscess is deep, an antiseptic dressing (gauze wick) may be placed inside the wound to keep it open.
The procedure may leave a small scar.
Skin abscess prognosis
Most skin abscesses can be cured with proper treatment. Infections caused by MRSA respond to specific antibiotics.
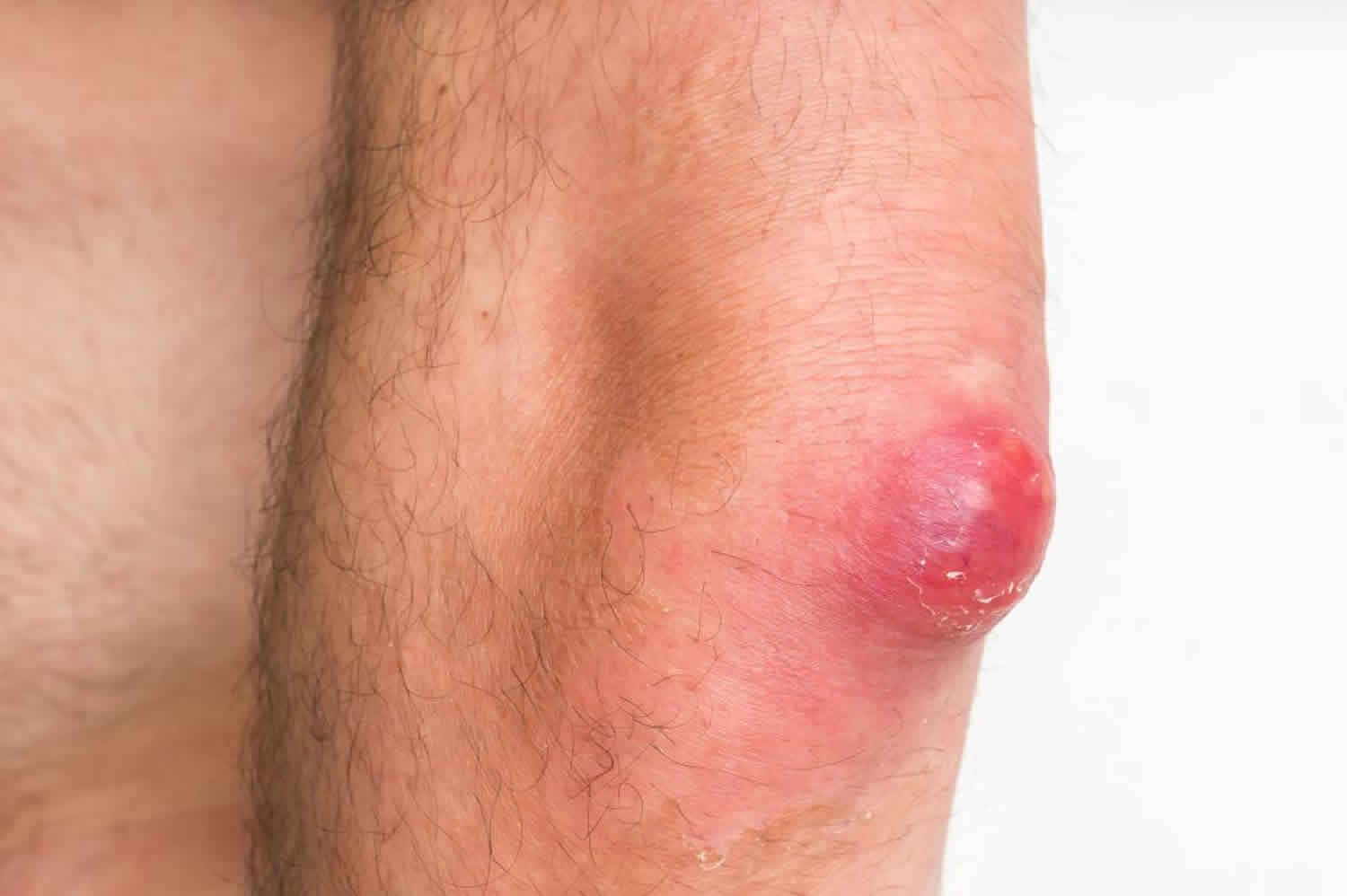
Figure 2. Abscess on leg
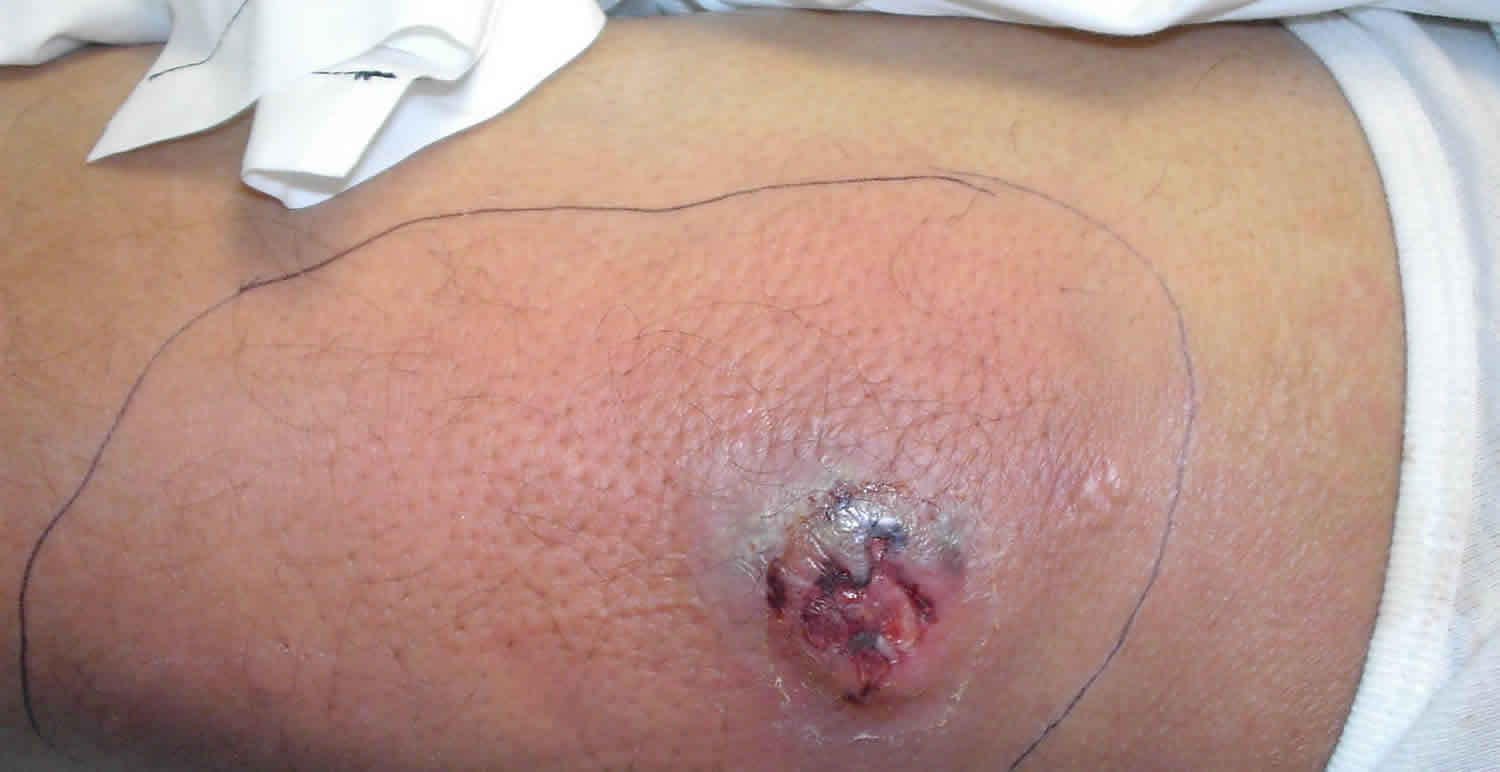
Figure 3. Abscess on face
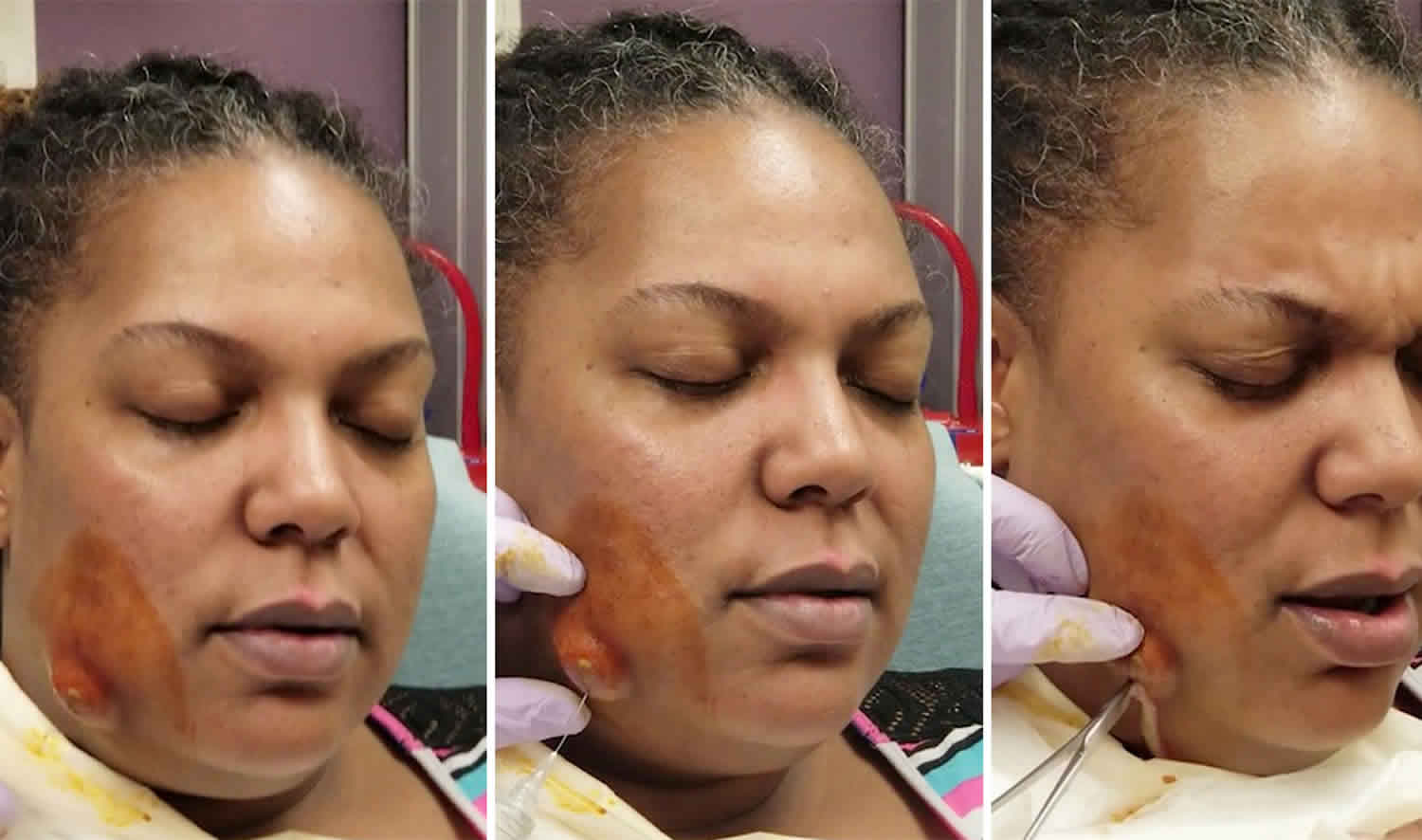
Figure 4. Armpit abscess
What is MRSA?
Methicillin-resistant Staphylococcus aureus (MRSA), a type of staph bacteria that is resistant to several antibiotics. In the general community, MRSA most often causes skin infections. In some cases, it causes pneumonia (lung infection) and other issues. If left untreated, MRSA infections can become severe and cause sepsis – a life-threatening reaction to severe infection in the body.
- You can’t tell by looking at the skin if it is a staph infection (including MRSA).
- Contact your doctor if you think you have an infection. Finding infections early and getting care make it less likely that the infection will become severe.
- Do not try to treat the infection yourself by picking or popping the sore.
- Cover possible infections with clean, dry bandages until you can be seen by a doctor, nurse, or other health care provider.
In a healthcare setting, such as a hospital or nursing home, MRSA can cause severe problems such as bloodstream infections, pneumonia and surgical site infections.
Anyone can get MRSA on their body from contact with an infected wound or by sharing personal items, such as towels or razors, that have touched infected skin. MRSA infection risk can be increased when a person is in activities or places that involve crowding, skin-to-skin contact, and shared equipment or supplies. People including athletes, daycare and school students, military personnel in barracks, and those who recently received inpatient medical care are at higher risk.
Studies show that about one in three people carry staph in their nose, usually without any illness. Two in 100 people carry MRSA. There are not data showing the total number of people who get MRSA skin infections in the community.
The Centers for Disease Control and Prevention (CDC) encourages clinicians to consider MRSA (methicillin-resistant Staphylococcus aureus) in the differential diagnosis of skin and soft tissue infections compatible with Staphylococcus aureus infections, especially those that are purulent (fluctuant or palpable fluid-filled cavity, yellow or white center, central point or “head,” draining pus, or possible to aspirate pus with needle or syringe). A patient’s presenting complaint of “spider bite” should raise suspicion of an Staphylococcus aureus infection.
Recent data suggest that MRSA as a cause of skin infections in the general community remains at high probability. The spectrum of disease caused by MRSA appears to be similar to that of Staphylococcus aureus in the community. Skin and soft tissue infections, specifically furuncles (abscessed hair follicles or “boils”), carbuncles (coalesced masses of furuncles), and abscesses, are the most frequently reported clinical manifestations. The role of MRSA in cellulitis without abscess or purulent drainage is less clear since cultures are rarely obtained.
Can I prevent MRSA?
There are the steps you can take to reduce your risk of MRSA infection:
- Maintain good hand and body hygiene. Wash hands often, and clean your body regularly, especially after exercise.
- Keep cuts, scrapes and wounds clean and covered until healed.
- Avoid sharing personal items such as towels and razors.
- Get care early if you think you might have an infection.
What are MRSA Symptoms?
Sometimes, people with MRSA skin infections first think they have a spider bite. However, unless a spider is actually seen, the irritation is likely not a spider bite. Most staph skin infections, including MRSA, appear as a bump or infected area on the skin that might be:
- Red
- Swollen
- Painful
- Warm to the touch
- Full of pus or other drainage
- Accompanied by a fever
If you or someone in your family experiences these signs and symptoms, cover the area with a bandage, wash your hands, and contact your doctor. It is especially important to contact your doctor if signs and symptoms of an MRSA skin infection are accompanied by a fever.
Figure 5. MRSA skin infection
MRSA treament
In the community, incision and drainage remains the primary therapy for these purulent skin infections. Empiric antimicrobial coverage for MRSA may be warranted in addition to incision and drainage based on clinical assessment (e.g., presence of systemic symptoms, severe local symptoms, immune suppression, extremes of patient age, infections in a difficult to drain area, or lack of response to incision and drainage alone).
Antibiotic treatment, if indicated, should be guided by the susceptibility profile of the organism. Obtaining specimens for culture and susceptibility testing is useful to guide therapy, particularly for those with more severe infections and those who fail to respond adequately to initial management.
MRSA skin infections can develop into more serious infections. It is important to discuss a follow-up plan with your patients in case they develop systemic symptoms or worsening local symptoms, or if symptoms do not improve within 48 hours.
Skin and soft-tissue infections MRSA management guideline 3:
- For a cutaneous abscess, incision and drainage is the primary treatment. For simple abscesses or boils, incision and drainage alone is likely to be adequate, but additional data are needed to further define the role of antibiotics, if any, in this setting.
- Antibiotic therapy is recommended for abscesses associated with the following conditions: severe or extensive disease (e.g, involving multiple sites of infection) or rapid progression in presence of associated cellulitis, signs and symptoms of systemic illness, associated comorbidities or immunosuppression, extremes of age, abscess in an area difficult to drain (e.g, face, hand, and genitalia), associated septic phlebitis, and lack of response to incision and drainage alone.
- For outpatients with purulent cellulitis (e.g, cellulitis associated with purulent drainage or exudate in the absence of a drainable abscess), empirical therapy for community-associated MRSA is recommended pending culture results. Empirical therapy for infection due to β-hemolytic streptococci is likely to be unnecessary. Five to 10 days of therapy is recommended but should be individualized on the basis of the patient’s clinical response.
- For outpatients with nonpurulent cellulitis (e.g, cellulitis with no purulent drainage or exudate and no associated abscess), empirical therapy for infection due to β-hemolytic streptococci is recommended. The role of community-associated MRSA is unknown. Empirical coverage for community-associated MRSA is recommended in patients who do not respond to β-lactam therapy and may be considered in those with systemic toxicity. Five to 10 days of therapy is recommended but should be individualized on the basis of the patient’s clinical response.
- For empirical coverage of community-associated MRSA in outpatients with skin and soft-tissue infection, oral antibiotic options include the following: clindamycin, trimethoprim-sulfamethoxazole (TMP-SMX), a tetracycline (doxycycline or minocycline) and linezolid. If coverage for both β-hemolytic streptococci and community-associated MRSA is desired, options include the following: clindamycin alone or trimethoprim-sulfamethoxazole (TMP-SMX) or a tetracycline in combination with a β-lactam (e.g, amoxicillin) or linezolid alone.
- The use of rifampin as a single agent or as adjunctive therapy for the treatment of skin and soft-tissue infection is not recommended.
- For hospitalized patients with complicated skin and soft-tissue infection (complicated skin and soft-tissue infection; defined as patients with deeper soft-tissue infections, surgical/traumatic wound infection, major abscesses, cellulitis, and infected ulcers and burns), in addition to surgical debridement and broad-spectrum antibiotics, empirical therapy for MRSA should be considered pending culture data. Options include the following: intravenous (IV) vancomycin, oral (PO) or IV linezolid 600 mg twice daily, daptomycin 4 mg/kg/dose IV once daily, telavancin 10 mg/kg/dose IV once daily, and clindamycin 600 mg IV or PO 3 times a day. A β-lactam antibiotic (e.g, cefazolin) may be considered in hospitalized patients with nonpurulent cellulitis with modification to MRSA-active therapy if there is no clinical response. Seven to 14 days of therapy is recommended but should be individualized on the basis of the patient’s clinical response.
- Cultures from abscesses and other purulent skin and soft-tissue infections are recommended in patients treated with antibiotic therapy, patients with severe local infection or signs of systemic illness, patients who have not responded adequately to initial treatment, and if there is concern for a cluster or outbreak.
For children
- 9. For children with minor skin infections (such as impetigo) and secondarily infected skin lesions (such as eczema, ulcers, or lacerations), mupirocin 2% topical ointment can be used.
- 10. Tetracyclines should not be used in children <8 years of age.
- 11. In hospitalized children with complicated skin and soft-tissue infection, vancomycin is recommended. If the patient is stable without ongoing bacteremia or intravascular infection, empirical therapy with clindamycin 10–13 mg/kg/dose IV every 6–8 h (to administer 40 mg/kg/day) is an option if the clindamycin resistance rate is low (e.g, <10%) with transition to oral therapy if the strain is susceptible. Linezolid 600 mg PO/IV twice daily for children ≥12 years of age and 10 mg/kg/dose PO/IV every 8 h for children <12 years of age is an alternative.
Abscess symptoms
The symptoms of an abscess depend on where it develops in your body.
If you have an abscess under the skin or in the mouth, symptoms may include swelling and redness in the area. As pus builds up, it may cause pain. You may also have swollen glands (lymph nodes) and a fever.
It’s more difficult to identify an abscess inside the body (an internal abscess), but signs include:
- pain in the affected area
- a high temperature
- generally feeling unwell
Imaging tests such as ultrasound may be needed to find the problem.
Internal abscess symptoms
Abscesses that develop inside an organ or in the spaces between organs can be more difficult to identify than skin abscesses. The symptoms can be vague and there may be no obvious external signs of a problem.
The symptoms of an internal abscess can also vary depending on exactly where in the body the abscess develops. For example, a liver abscess may cause jaundice, whereas an abscess in or near the lungs may cause a cough or shortness of breath.
General symptoms of an internal abscess can include:
- discomfort in the area of the abscess
- fever
- increased sweating
- feeling sick
- vomiting
- chills
- pain or swelling in your tummy (abdomen)
- loss of appetite and weight loss
- extreme tiredness (fatigue)
- diarrhea or constipation
Abscess causes
Most abscesses are caused by an infection with staphylococcal bacteria. Abscesses usually develop when you have a bacterial infection that your immune system tries to contain. When bacteria enter the body, the immune system sends white blood cells to fight the infection. This causes swelling (inflammation) at the site of infection and the death of nearby tissue. In the process of fighting the infection, pus (a liquid or semi-liquid mixture of bacteria, white blood cells and dead cells) is produced. A cavity is created, which fills with pus to form an abscess. The abscess may get larger and more painful as the infection continues and more pus is produced.
Some types of staphylococcal bacteria produce a toxin called Panton-Valentine leukocidin (PVL) which kills white blood cells. This causes the body to make more cells to keep fighting the infection, and can lead to repeated skin infections.
In rare cases, an abscess may be caused by a virus, fungi or parasites.
Other causes include non-bacterial infections, ingrown hairs, or a blocked gland or duct.
Abscess may also develop around a foreign body, such as a splinter.
The most common causes of infective abscesses are:
- Staphylococcus aureus; the usual cause of boils (furuncles and carbuncles, the most common form of cutaneous abscess), wound infection or infected eczema.
- Methicillin resistant Staphylococcus aureus (MRSA), which may cause recurrent abscesses.
- Streptococcus pyogenes; the usual cause of cellulitis and erysipelas
- Mycobacterium tuberculosis (TB) and atypical mycobacterial infection
- Anaerobes, gram negative organisms, rare bacterial infections and mixed infections
- Fungal infection, e.g., kerion
- Severe viral infection e.g, herpes simplex
- Infestations or parasitic infections
A sterile abscess may persist after infection has been cleared, as it contains dead or necrotic tissue and inflammatory cells.
Sterile abscess may occur after corticosteroid injection. This is more likely when the medication has spilled into subcutaneous fat. A foreign-body or other hypersensitivity reaction to injected material such as bovine collagen may also result in abscess formation.
Certain inflammatory skin diseases may cause tissue destruction and abscess formation, in the absence of pathogens (infectious microbes). These include:
- Hidradenitis suppurativa
- Acne conglobata and acne fulminans
- Crohn skin disease
- Panniculitis (inflamed subcutaneous fat)
Internal abscesses
Internal abscesses often develop as a complication of an existing condition, such as an infection elsewhere in your body. For example, if your appendix bursts as a result of appendicitis, bacteria can spread inside your tummy (abdomen) and cause an abscess to form.
Abscesses that develop inside the tummy (abdomen) are caused by an infection reaching tissue deeper within the body. This can occur as a result of:
- an injury
- abdominal surgery
- an infection spreading from a nearby area
There are many ways an infection can spread into the abdomen and cause an abscess to develop.
For example, a lung abscess can form after a bacterial infection in your lungs, such as pneumonia, and a burst appendix can spread bacteria within your abdomen.
Risk factors for developing abscess
In addition to the specific causes mentioned above, things that increase the likelihood of an abscess developing can include:
- having a weakened immune system – this could be because of a medical condition such as HIV, or a treatment such as chemotherapy
- having diabetes
- having an underlying inflammatory condition, such as hidradenitis suppurativa
- being a carrier of staphylococcal bacteria
However, many abscesses develop in people who are otherwise generally healthy.
Abscess prevention
- Hygiene: wash hands frequently (or use hand rubs) and do not share towels, clothing, razors and tooth brushes.
- Avoid scratches or nicks to your skin
- Eat healthily — eat plenty of fresh fruit and vegetables to build your immune system and keep a healthy weight.
- Avoid smoking
- Reduce transmission to others: while infected, do not share equipment at a community gym or attend sauna or swimpool.
- Dispose of tissues and dressings in sealed bag or burn them.
- Take care not to nick skin while shaving
- Aim for normal weight
It’s difficult to prevent internal abscesses, as they’re often complications of other conditions.
Abscess diagnosis
For skin abscesses see skin abscess diagnosis above.
For internal abscesses
- Abscesses that develop inside your body are more difficult to diagnose than skin abscesses because they can’t be seen.
- Your doctor will ask you about your symptoms and any other health conditions you may have. If necessary, they’ll refer you to a specialist in hospital.
What tests should be done?
If the cause of an abscess is unknown, the following tests may be undertaken.
- Microscopy and Gram stain
- Bacterial culture (standard, anaerobic, and at low temperature)
- Biopsy of adjacent tissue
If a patient has had recurrent abscesses, consider nutritional deficiency, especially of iron; immune deficiency; immune suppression by medications such as systemic steroids; diabetes; or poor circulation.
Abscess treatment
Abscesses can be treated in a number of different ways, depending on the type of abscess and how large it is.
The main treatment options include:
- antibiotics
- a drainage procedure
- surgery
Small abscesses can sometimes burst and heal on their own. However, larger or internal abscesses need to be drained by a doctor (sometimes involving surgery). You may also need to take antibiotics.
An abscess should be explored to remove foreign bodies, and its contents should be removed. This requires making a surgical incision and draining the pus. The cavity is then thoroughly washed out with saline. It should be left open to allow further pus to drain away. Wicks are sometimes inserted if the abscess is deep, to help it drain.
Once an abscess has drained, it usually heals quickly and doesn’t cause long-term consequences.
Internal abscess treatment
The pus usually needs to be drained from an internal abscess, either by using a needle inserted through the skin (percutaneous abscess drainage) or with surgery.
The method used will depend on the size of your abscess and where it is in your body.
Antibiotics will usually be given at the same time, to help kill the infection and prevent it spreading. These may be given as tablets or directly into a vein (intravenously).
Percutaneous drainage
If the internal abscess is small, your surgeon may be able to drain it using a fine needle. Depending on the location of the abscess, this may be carried out using either a local or general anaesthetic.
The surgeon may use ultrasound scans or computerized tomography (CT) scans to help guide the needle into the right place.
Once the abscess has been located, the surgeon drains the pus using the needle. They may make a small incision in your skin over the abscess, then insert a thin plastic tube called a drainage catheter into it.
The catheter allows the pus to drain out into a bag and may have to be left in place for up to a week.
This procedure may be carried out as a day case procedure, which means you’ll be able to go home the same day, although some people will need to stay in hospital for a few days.
As with the incision and drainage procedure for skin abscesses, percutaneous drainage may leave a small scar.
Surgery
You may need to undergo surgery if:
- your internal abscess is too large to be drained with a needle
- a needle can’t get to the abscess safely
- needle drainage hasn’t been effective in removing all of the pus
The type of surgery you have will depend on the type of internal abscess you have and where it is in your body. Generally, it involves making a larger incision in your skin to allow the pus to be washed out.
Antibiotics for abscess
Antibiotics are often prescribed, chosen according to the organism causing the abscess and its sensitivities.
- Wang W, Chen W, Liu Y, et al. Antibiotics for uncomplicated skin abscesses: systematic review and network meta-analysis. BMJ Open 2018;8:e020991. doi: 10.1136/bmjopen-2017-020991 https://bmjopen.bmj.com/content/8/2/e020991[↩][↩]
- Vermandere M, Aertgeerts B, Agoritsas T, et al. Antibiotics after incision and drainage for uncomplicated skin abscesses: a clinical practice guideline. BMJ. 2018;360:k243. Published 2018 Feb 6. doi:10.1136/bmj.k243 https://www.ncbi.nlm.nih.gov/pmc/articles/PMC5799894/[↩]
- Catherine Liu, Arnold Bayer, Sara E. Cosgrove, Robert S. Daum, Scott K. Fridkin, Rachel J. Gorwitz, Sheldon L. Kaplan, Adolf W. Karchmer, Donald P. Levine, Barbara E. Murray, Michael J. Rybak, David A. Talan, Henry F. Chambers; Clinical Practice Guidelines by the Infectious Diseases Society of America for the Treatment of Methicillin-Resistant Staphylococcus aureus Infections in Adults and Children, Clinical Infectious Diseases, Volume 52, Issue 3, 1 February 2011, Pages e18–e55, https://doi.org/10.1093/cid/ciq146[↩]