Contents
What is calcinosis cutis
Calcinosis cutis or cutaneous calcification is a condition in which calcium salts are deposited in the skin and subcutaneous tissue 1.
Calcinosis cutis is classified into five main types:
- Dystrophic,
- Metastatic,
- Idiopathic,
- Iatrogenic, and
- Calciphylaxis.
Dystrophic calcinosis cutis
Dystrophic calcification is the most common cause of calcinosis cutis and is associated with normal laboratory serum values of calcium and phosphorus (phosphate). Dystrophic calcinosis cutis occurs in an area where there is damaged, inflamed, neoplastic or necrotic skin. Tissue damage may be from mechanical, chemical, infectious or other factors. There is an underlying disease, systemic sclerosis, dermatomyositis, mixed connective tissue disease, or lupus, that induces tissue damage and creates a nidus for calcification 1.
Conditions that can cause dystrophic calcinosis cutis include:
- Trauma
- Acne
- Varicose veins
- Infections
- Tumors (pilomatrixoma, cysts, basal cell carcinomas and others)
- Connective tissue disease (dermatomyositis, systemic sclerosis, cutaneous lupus erythematosus)
- Panniculitis
- Inherited diseases of connective tissue (Ehlers-Danlos syndrome, Werner syndrome, Pseudoxanthoma elasticum, Rothmund-Thomson syndrome)
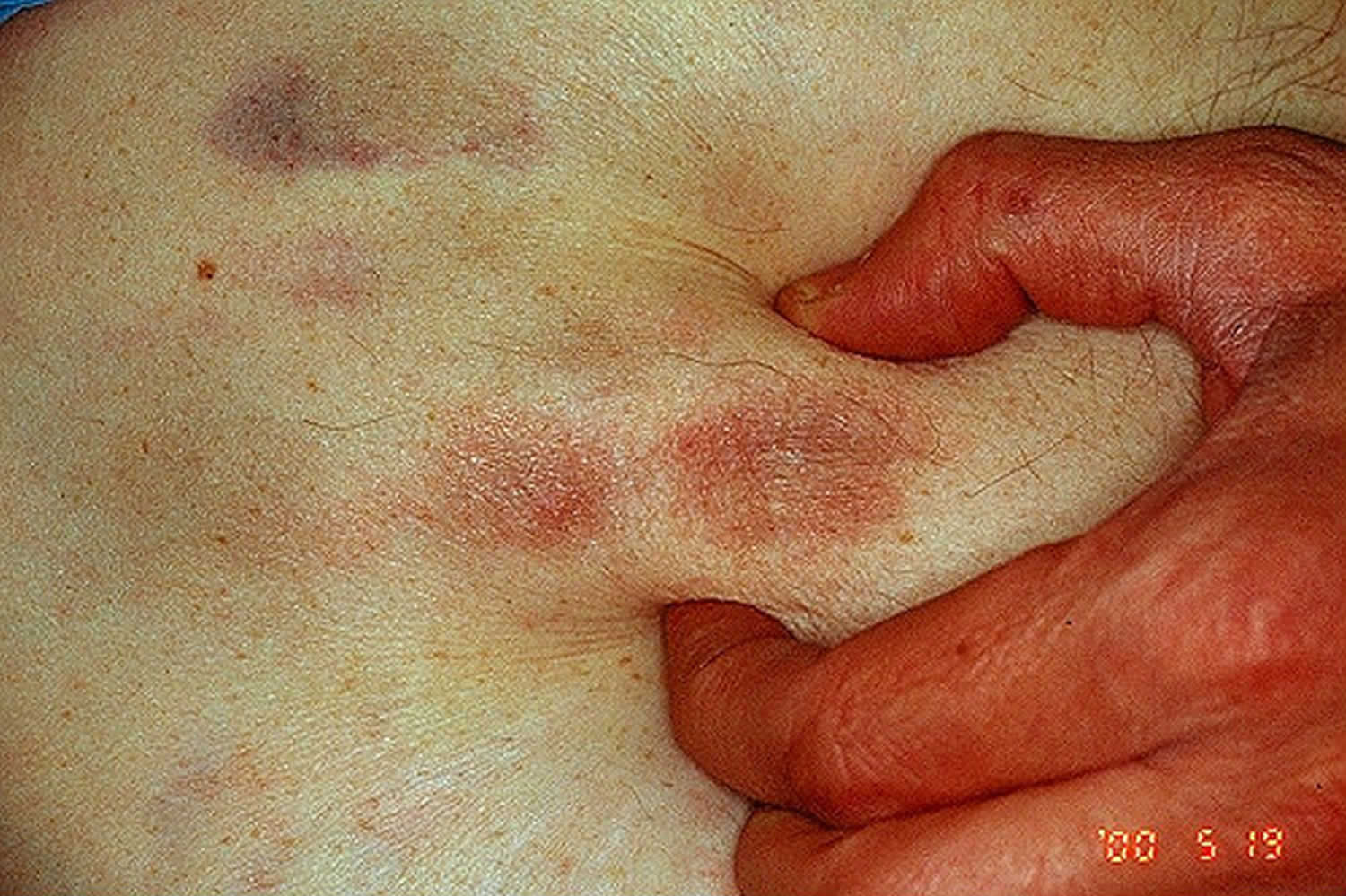
Dermatomyositis and scleroderma (especially the CREST syndrome – calcinosis, Raynaud’s phenomenon, esophageal dysfunction, sclerodactyly and telangiectasia) are the best recognized and most troublesome.
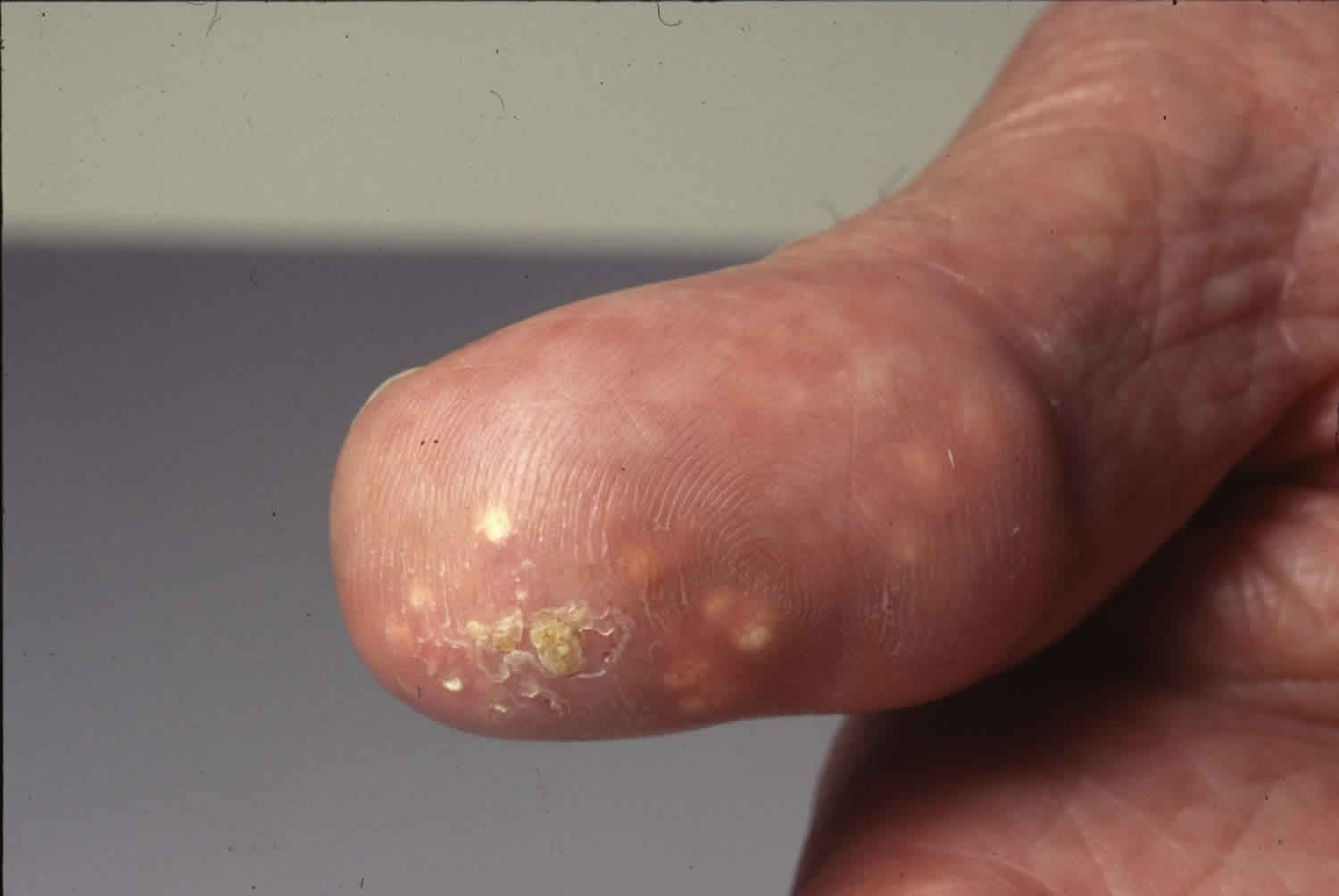
Figure 1. Dystrophic calcinosis cutis
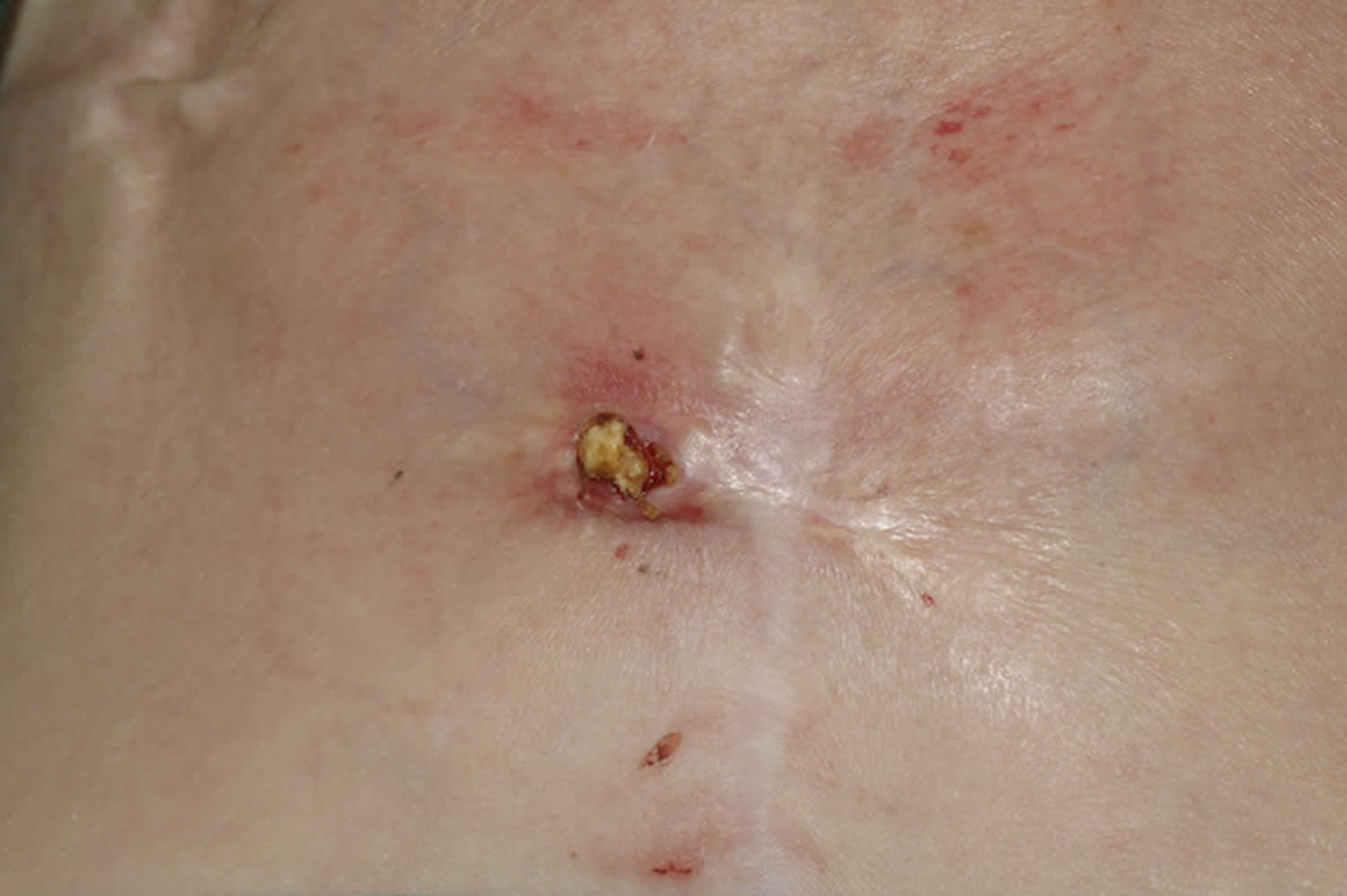
Figure 2. CREST syndrome
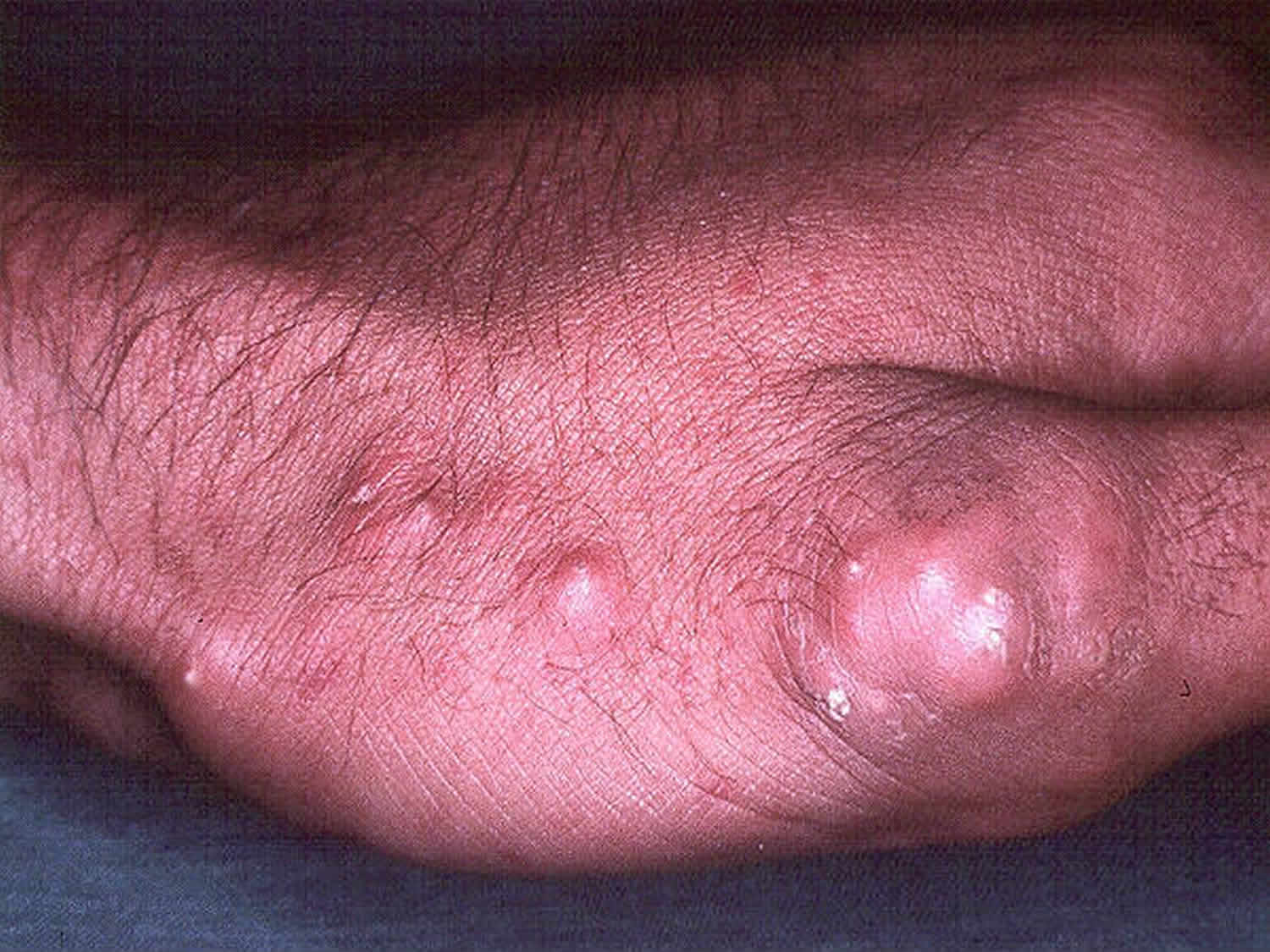
Figure 3. Calcinosis cutis scleroderma
Metastatic calcinosis cutis
Metastatic calcinosis cutis occurs in the setting of abnormal calcium and phosphate (phosphorus) metabolism and is often associated with hypercalcemia and/or hyperphosphatemia. Conditions that can cause metastatic calcinosis cutis include:
- Primary or secondary hyperparathyroidism
- Bone metastases
- Paraneoplastic hypercalcemia
- Destructive bone disease, e.g. Paget disease
- Milk-alkali syndrome
- Excessive vitamin D intake
- Sarcoidosis
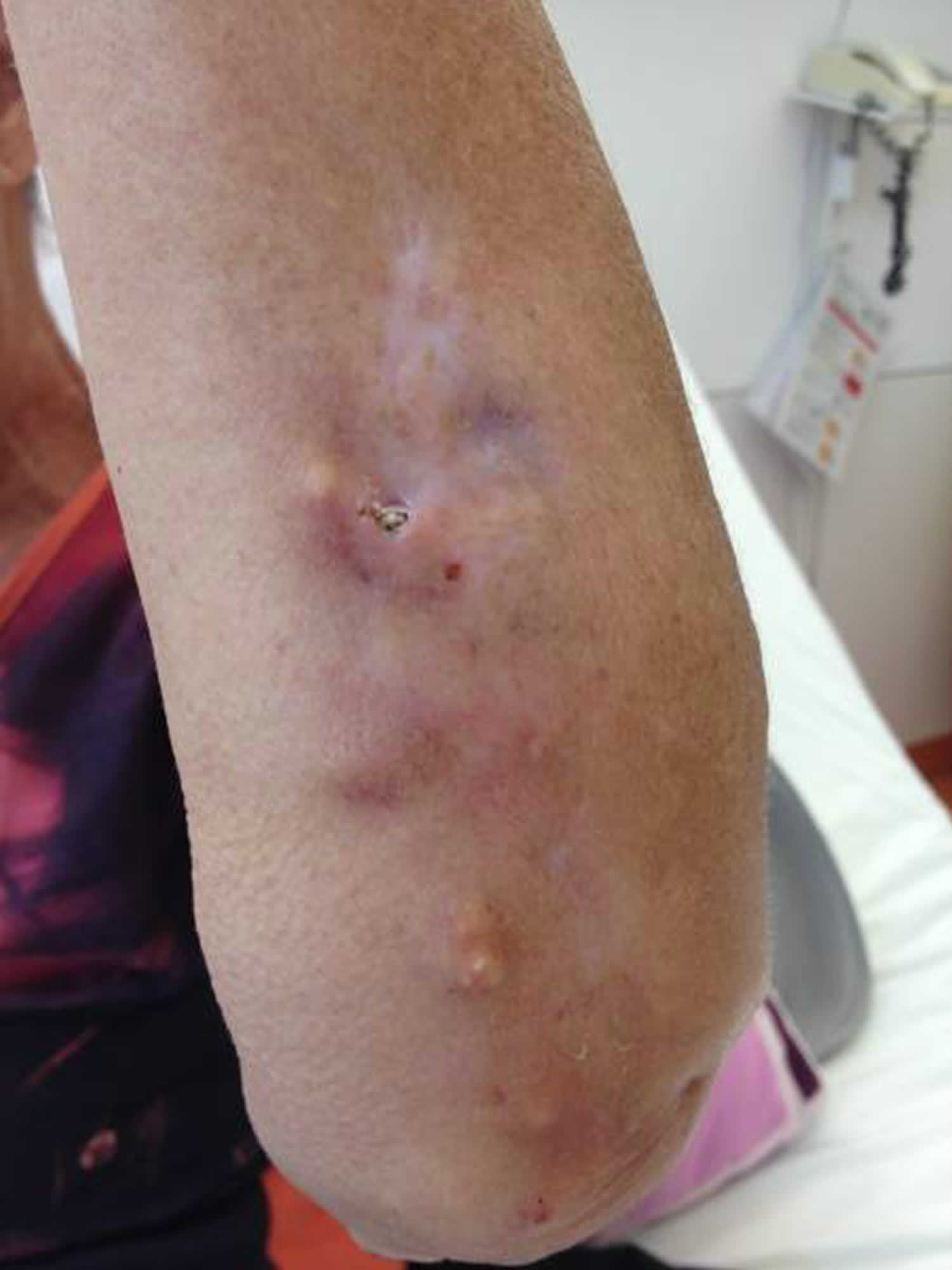
Metastatic calcification presents with predominantly periarticular calcification in addition to signs and symptoms of hypercalcemia (e.g. abdominal pain, renal failure, cardiac arrhythmias and depression).
Figure 4. Metastatic calcinosis cutis
Idiopathic calcinosis cutis
Idiopathic calicnosis cutis (unknown) generally occurs in the absence of any known tissue injury or abnormal laboratory values. Calcification is usually localized to one general area. It includes tumoral calcinosis, subepidermal calcified nodules, and scrotal calcinosis cutis.
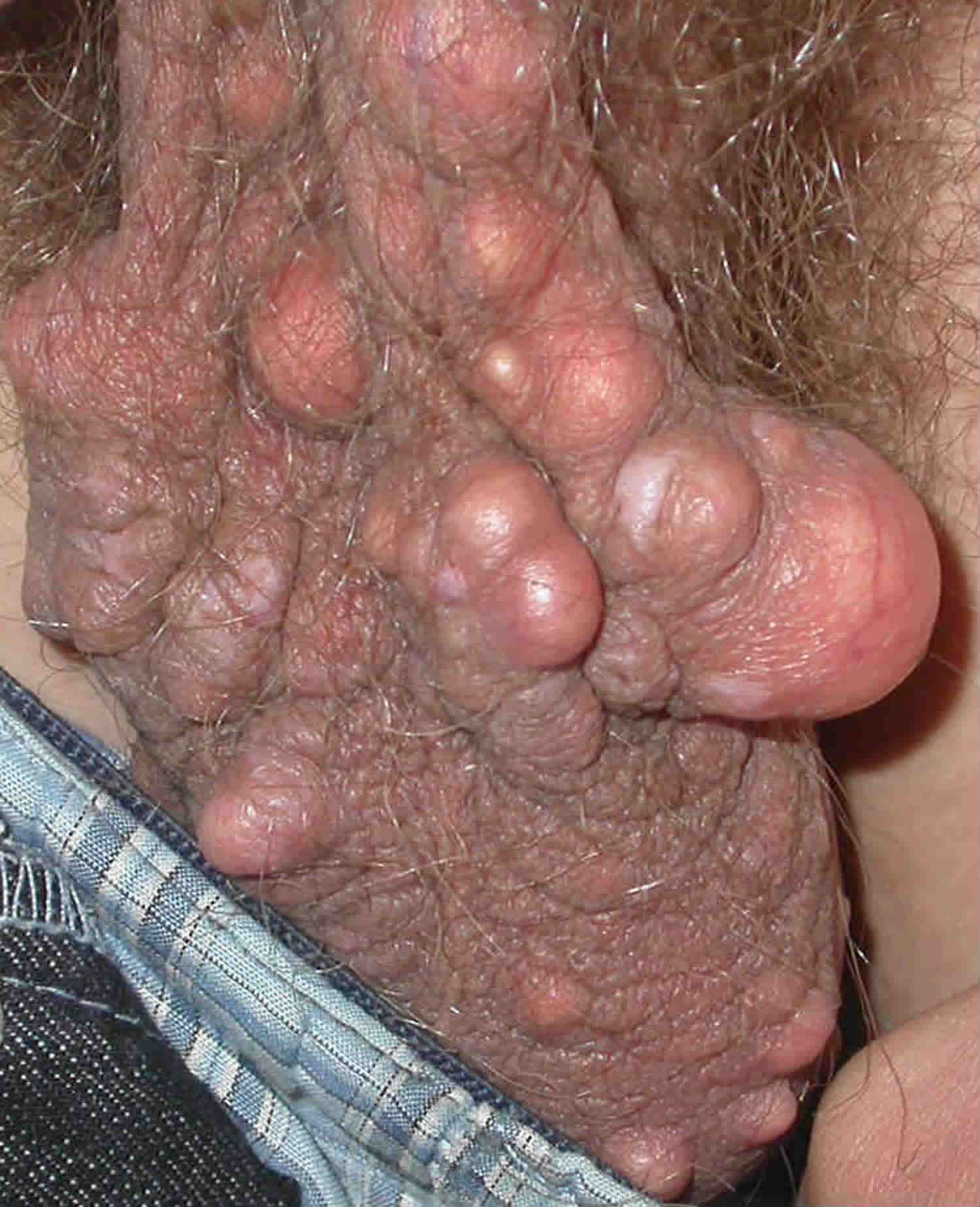
Scrotal calcinosis cutis is the best recognized of these conditions presenting in men aged 20-40 years, as multiple, white-yellow, firm, subcutaneous nodules, sitting within the scrotal skin
Other examples include subepidermal calcified nodules, tumoral calcinosis (large subcutaneous masses around the major joints, most usually seen in adolescents) and miliary calcinosis cutis
Figure 5. Scrotal calcinosis cutis
Iatrogenic calcinosis cutis
Iatrogenic calcinosis cutis arises secondary to a treatment or procedure, for example parenteral administration of calcium or phosphate and in newborns from repeated heel sticks inducing precipitation of calcium salts.
Iatrogenic calcinosis cutis has been seen with intravenous calcium gluconate, calcium chloride, and para-aminosalicylic acid during the treatment of pulmonary tuberculosis. It is also seen after administration of electrodes with pastes containing calcium chloride for electroencephalography. Tumor lysis syndrome and calcinosis cutis after organ transplant fall under this category. Iatrogenic calcification can be prevented by diluting the calcium solution and lowering phosphorus levels before administration.
Calciphylaxis
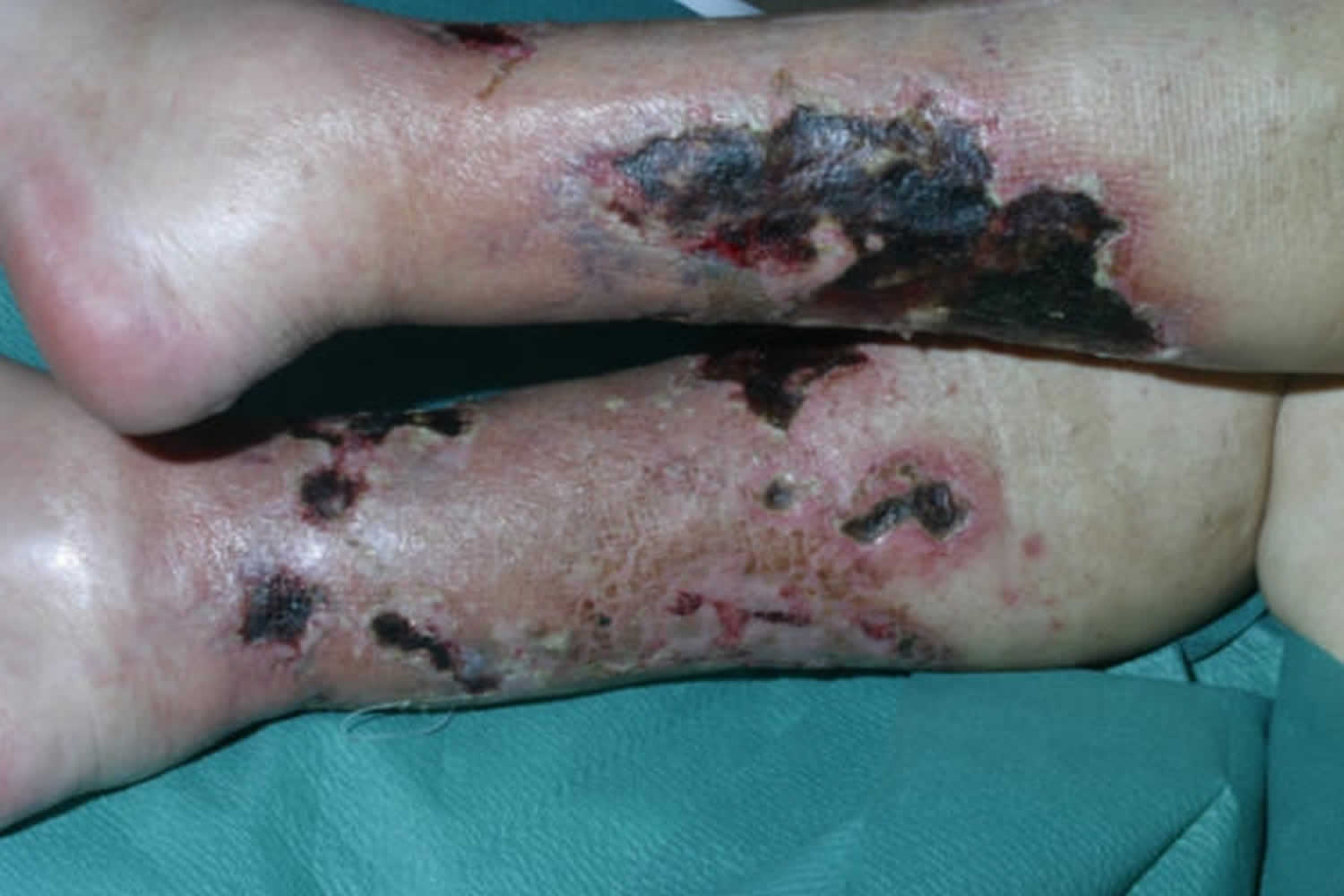
Calciphylaxis is a condition characterized by necrosis (cellular death) of the skin and fatty tissue. Calciphylaxis involves calcification of small and medium-sized blood vessels and is associated with chronic renal failure and dialysis. Calciphylaxis is seen mainly in patients with end-stage kidney disease. Calciphylaxis is also sometimes called calcific uremic arteriolopathy or calcific vasculopathy.
Calciphylaxis is classified as calcinosis circumscripta if it is limited to an extremity or joint. Calcinosis universalis occurs when there is diffuse involvement of subcutaneous and fibrous structures of muscles and tendons. Clinically, nodules or plaques tend to progress quickly to livedo-like areas and then ulcerate. The thighs, abdomen and buttocks are the most commonly affected sites. Ulceration is associated with severe pain. In patients with renal failure, lesions on the trunk are associated with a much higher mortality rate than lesions on the legs.
In 1981, approximately 50 cases of calciphylaxis were reported in the world literature. Today, the incidence is estimated at 1 per cent per year in patients undergoing renal dialysis. The mortality is extremely high, up to 80%, often within several months of onset. The primary cause of death is from secondary infection of the ulcers, and sepsis.
Most patients with calciphylaxis have chronic kidney disease. Other conditions associated with accelerated calcium deposition in soft tissues and at risk of calciphylaxis include:
- Obesity
- Diabetes
- Caucasian race
- Female sex
- Hypoalbuminemia
- Warfarin (an anticoagulant)
- Multiple myeloma,
- Polyneuropathy,
- Organomegaly,
- Endocrinopathy,
- Cirrhosis, and
- Rheumatoid arthritis.
Figure 6. Calciphylaxis
Calcinosis cutis causes
Calcinosis may be caused by trauma, inflammation, varicose veins, tumors, infections, connective tissue disease, hyperphosphatemia, and hypercalcemia. Calcinosis cutis is associated with systemic sclerosis.
Calcinosis cutis commonly occurs in patients with systemic sclerosis, especially the limited form (CREST syndrome – calcinosis, Raynaud’s phenomenon, esophageal dysfunction, sclerodactyly and telangiectasia). Twenty-five percent to 40% of patients with limited systemic sclerosis will develop calcinosis cutis ten years after the onset of disease. Calcinosis cutis is seen in 30% of adults and up to 70% of children and adolescents with dermatomyositis. Patients with systemic lupus erythematosus can present with periarticular calcification in 33% of cases and soft tissue calcification in 17%.
Calcinosis cutis signs and symptoms
The signs and symptoms of calcinosis cutis vary according to the underlying cause. In many cases the lesions gradually develop and are often symptomless. The lesions usually appear as firm, whitish/yellowish papules, plaques or nodules on the surface of the skin. A solitary lesion may develop, although multiple lesions are more common. Lesions may become tender and ulcerate, discharging chalk-like creamy material consisting mainly of calcium phosphate with a small amount of calcium carbonate.
Fingertip lesions may be painful, while lesions at other sites may restrict joint mobility and limit movement due to stiffening of the skin. In severe cases cutaneous gangrene may occur.
The nodules can vary in shape and size and can be painful leading to functional impairment. The lesions in dystrophic calcification are localized based on the underlying disease. The areas most commonly affected in systemic sclerosis are the forearms, elbows, fingers, and knees. Calcification occurs in elbows and knees and areas of previous inflammatory lesions in dermatomyositis. The extremities, buttocks, underneath lupus lesions, and periarticular areas are affected in lupus erythematosus. Lesions are located periarticular in metastatic calcification. The lesions are located around joints in tumoral calcinosis and on children’s faces in subepidermal calcified nodules in idiopathic calcification. The calcification is located at sites of venipuncture in iatrogenic calcification.
Calcinosis cutis diagnosis
Laboratory tests are performed to determine any metabolic abnormalities that may give rise to elevated calcium and phosphate levels. Radiological examinations including plain film x-ray, CT scanning and bone scintigraphy are useful in demonstrating the extent of tissue calcification.
Biopsy of cutaneous lesions is used to confirm diagnosis. On histology of calcinosis cutis, granules and deposits of calcium are seen in the dermis, often with a surrounding foreign-body giant cell reaction. Calcium deposits may also be found in subcutaneous tissue.
Laboratory studies
A complete blood count should be obtained for lupus erythematosus and possible malignant neoplasms. A basic metabolic panel with creatinine and urea can be obtained to evaluate for chronic kidney failure. A parathyroid hormone and vitamin D level to rule out hyperparathyroidism and hypervitaminosis D. Calcium, phosphate, total proteins, albumin, 24 hour urine excretion of calcium/inorganic phosphate levels should be obtained for metastatic calcification. Creatine Phosphokinase (CPK), lactate dehydrogenase (LDH), glutamic oxaloacetic transaminase (GOT), glutamic pyruvic transaminase (GPT), and aldolase levels should be obtained to evaluate for dermatomyositis. Antinuclear antibodies (ANA), anti-dsDNA, and anti-ENA for lupus and systemic sclerosis. Anti-ENA looks at Ro, La, Sm, RNP, Scl-70, Jo1. Bicarbonate and arterial pH can be obtained to rule out milk and alkali syndrome.
Calcinosis cutis treatment
The underlying cause of calcinosis cutis should be identified and treated accordingly. Steps can be taken to help facilitate treatment and increase blood flow to the extremities. These include avoiding trauma, smoking cessation, decrease stress and exposure to the cold.
Depending on the underlying cause, a multidisciplinary team of physicians including nephrologist, rheumatologist, and hematologist may be needed to manage the condition.
Medical therapy may be used to help relieve symptoms of the condition but are generally of limited and variable benefit. Medications that may be tried include corticosteroids, probenecid, colchicine, sodium etidronate, diphosphonates, diltiazem, and magnesium and aluminium antacids.
Smaller lesions have been reported to respond to warfarin, ceftriaxone, and intravenous immunoglobulin (IVIG).
Larger lesions respond to diltiazem, bisphosphonates, probenecid, aluminum hydroxide and surgical excision or curettage. Patients with small and localized lesions are good candidates for surgical treatment whereas more generalized disease will require medical management.
Diltiazem
Diltiazem is the most commonly used treatment for calcinosis cutis. It decreases the amount of calcium that enters cells and macrophages of the damaged tissues. High doses at 2 mg/kg/d to 4 mg/kg/d are necessary for therapeutic response.
Warfarin
Vitamin K levels have been measured to be high in some patients with calcinosis cutis, and the use of warfarin 1mg/d normalizes the levels and has some improvement for small lesions.
Bisphosphonates
Bisphosphonates work on macrophages which are active at the affected sites. It prevents the release of proinflammatory cytokines. It also reduces calcium turnover and resorption. Bisphosphonates show good response mainly in dermatomyositis and systemic sclerosis. Etidronate is used at 800 mg/d. Oral alendronate is used at 70 mg/wk, and pamidronate is used at 90 mg/wk. Their side effects include osteonecrosis of the jaw, fever, infusion site reaction, and low levels of calcium, phosphate, and magnesium.
Minocycline
Minocycline inhibits matrix metalloproteinases which reduce inflammation and ulceration and also chelates calcium. The drug is used at 50 mg to 100 mg/d and is seen to be effective in systemic sclerosis.
Ceftriaxone
Ceftriaxone effects matrix metalloproteinases, chelates calcium, and is anti-inflammatory. It is used at 2 g/d for 20 days and is best used in morphea profunda.
Aluminum Hydroxide
Aluminum hydroxide binds phosphorus and reduces the intestinal absorption of phosphorus. It is used at doses of 2.24 g/d, 2.4 g/d, and 1.8 g/d for calcinosis cutis in dermatomyositis and lupus.
Probenecid
Probenecid inhibits uric acid reuptake in the proximal tubule and increases renal phosphate excretion. It is used at 1.5 g/d and response is seen in juvenile dermatomyositis.
Topical Sodium Thiosulfate
Sodium thiosulfate is used because it increases calcium solubility. Topical sodium thiosulfate mixed with zinc oxide has been used successfully in ulcerated dystrophic calcification. Intralesional injections of sodium thiosulfate were shown to be successful in calcinosis cutis in a patient with lupus panniculitis. Intravenous sodium thiosulfate has been effective in treatment calciphylaxis and calcinosis cutis but is associated with more adverse side effects.
Other Treatments
Colchicine has been used due to its anti-inflammatory properties. IVIG at a dose of 2 g/kg has been shown to work in digital calcification in CREST syndrome and dermatomyositis. Intralesional corticosteroid injections have been used for limited systemic sclerosis. Extracorporeal shockwave lithotripsy has been used with good clinical response. Surgical excision is the most common method used. Carbon dioxide laser light has been effective in treating small lesions and lesions on the digits.
Surgical removal of lesions is indicated when they:
- become very painful
- ulcerate and recurrent infections occur
- cause functional impairment.
Because surgical trauma may stimulate further calcification, it may be best to excise a small site before going ahead with a large excision. Recurrence is common after excision.