Contents
- What is a cervix
- What is short cervix ?
- What is incompetent cervix ?
- Pregnant cervix
- What is low cervix soft closed cervix ?
- What is effaced cervix ?
- What is cervix dilation
- What is Tilted cervix
- What Is Cancer of the Cervix ?
- Types of cancer of the cervix
- Risk Factors for cancer of the cervix ?
- What Causes cancer of the cervix ?
- Cervix Cancer Prevention
- Things to do to prevent pre-cancers
- Tests for cervix cancer
- Tests for women with symptoms of cervix cancer or abnormal Pap results
- Cervix cancer Prevention and Early Detection
- General treatment information for cancer of the cervix
- Considering complementary and alternative methods
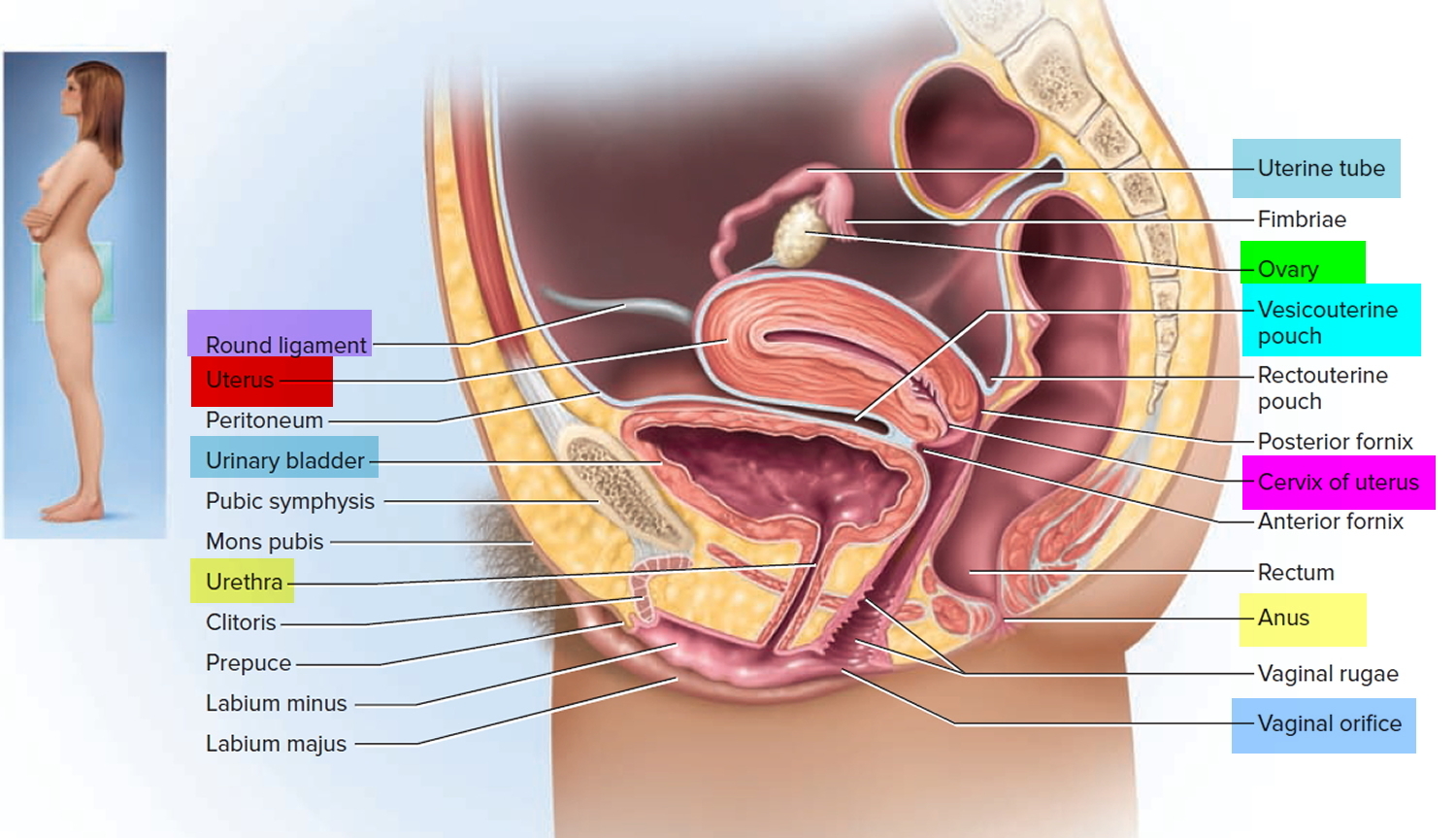
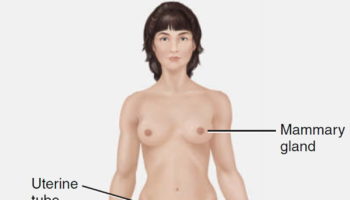
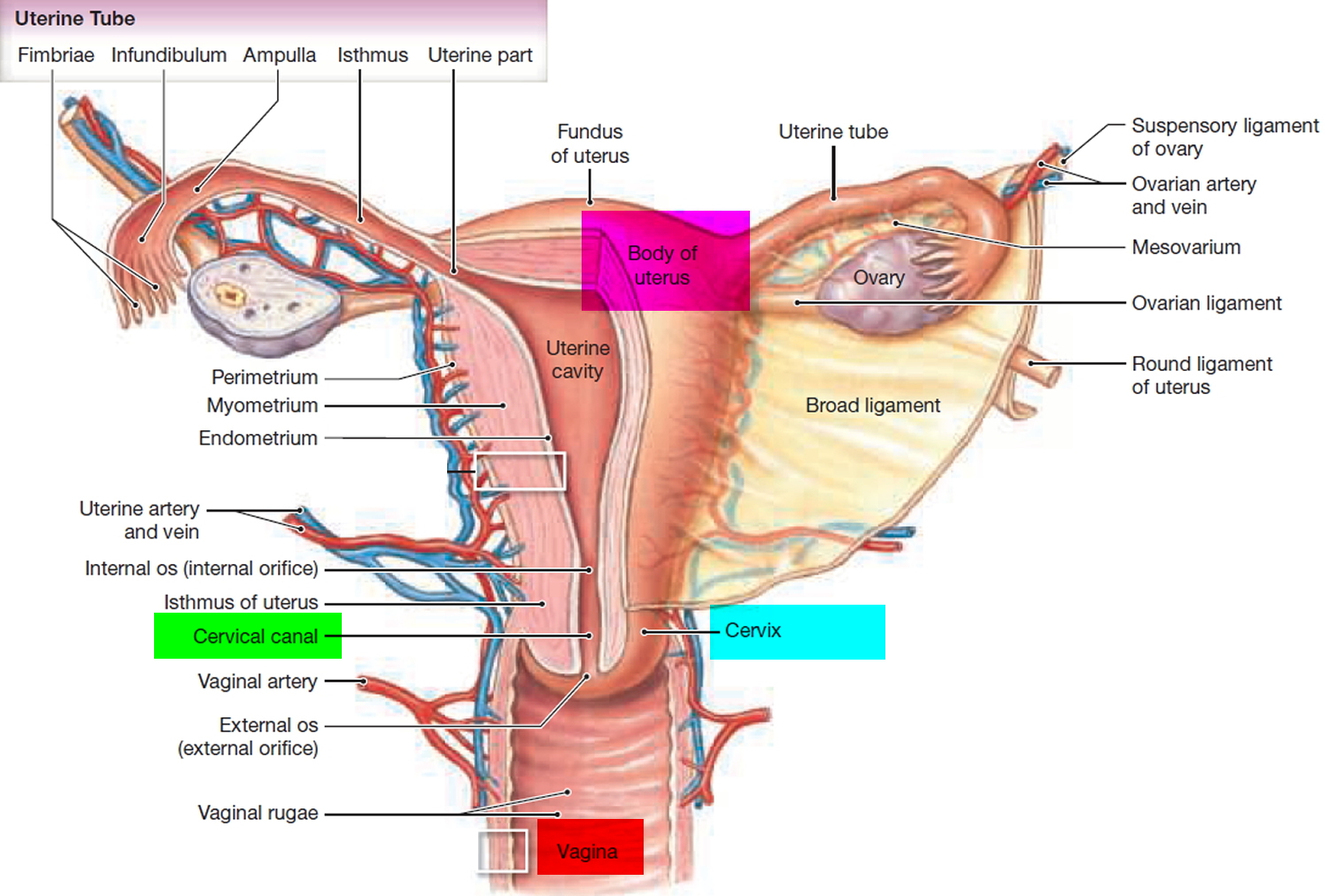
What is a cervix
The cervix is part of the lower end of the uterus. The lumen (internal cavity) of the uterus communicates with the vagina by way of a narrow passage through the cervix called the cervical canal.
Cervix function
The cervical canal contains cervical glands that secrete mucus, thought to prevent the spread of microorganisms from the vagina into the uterus. Near the time of ovulation, the mucus becomes thinner than usual and allows easier passage for sperm.
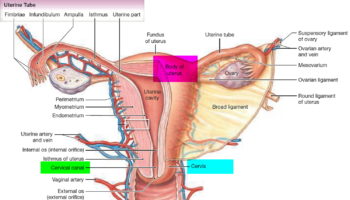
The cervix has two different parts and is covered with two different types of cells.
- The part of the cervix closest to the body of the uterus is called the endocervix and is covered with glandular cells.
- The part next to the vagina is the exocervix (or ectocervix) and is covered in squamous cells.
These two cell types meet at a place called the transformation zone. The exact location of the transformation zone changes as you get older and if you give birth.
The cervix and superior part of the vagina are supported by cardinal (lateral cervical) ligaments extending to the pelvic wall.
Figure 1. Cervix position
Figure 2. Cervix location
What is short cervix ?
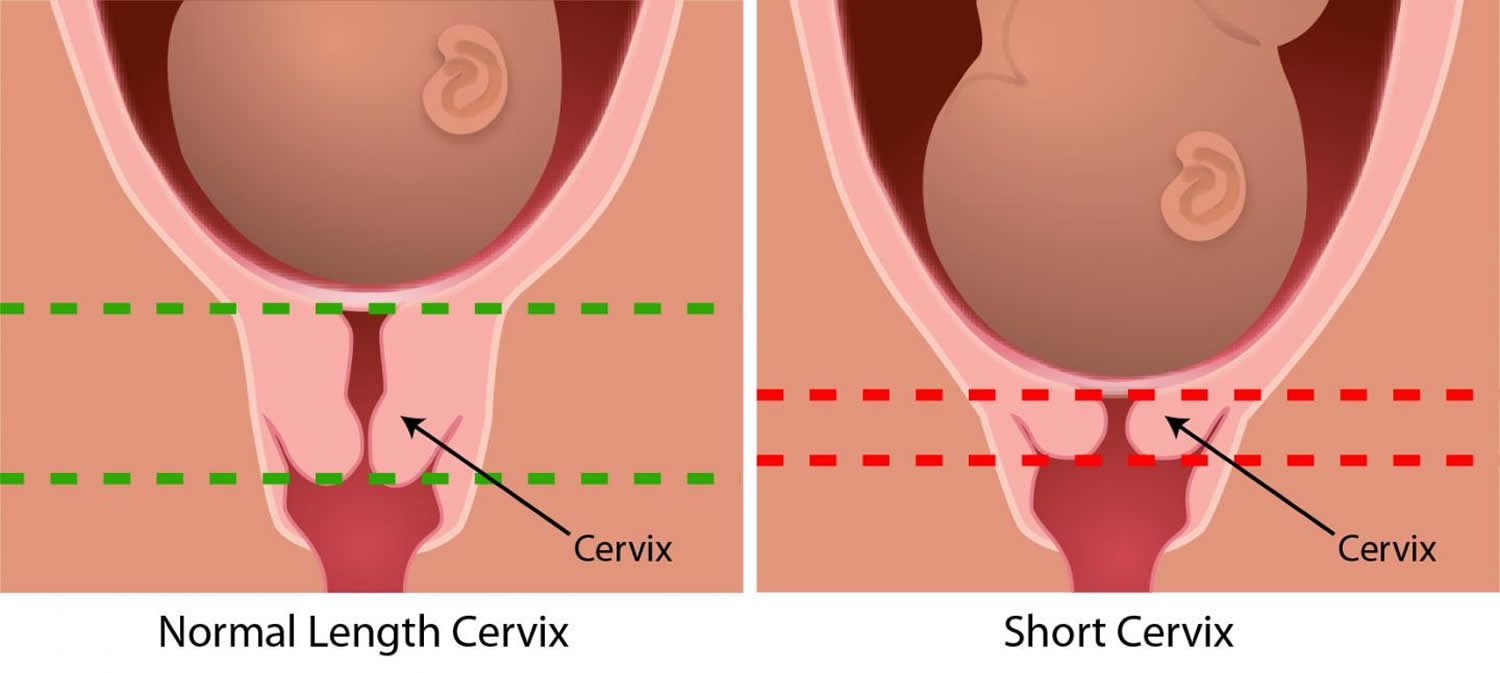
The cervix is the opening to the uterus (womb) that sits at the top of the vagina (birth canal). It opens, shortens and gets thinner and softer so your baby can pass through the birth canal during labor and birth.
In some women, the cervix opens too early during pregnancy or is shorter than normal. These conditions can cause problems during pregnancy.
A short cervix means the length of your cervix (also called cervical length) is shorter than normal. You may find out that you have a short cervix during an ultrasound that you get as part of your regular prenatal care. Prenatal care is medical care you get during pregnancy.
Checking for a short cervix is not a routine prenatal test. Your healthcare provider probably doesn’t check your cervical length unless:
- She has a reason to think it may be short.
- You have signs of preterm labor. This is labor that begins too soon, before 37 weeks of pregnancy.
- You have risk factors for premature birth, like you had a premature birth in the past or you have a family history of premature birth (premature birth runs in your family).
If your healthcare provider thinks you have a short cervix, she may check you regularly with ultrasound.
If you have a short cervix, you have a 1-in-2 chance (50 percent) of having a premature birth 1. If you have a short cervix and you’re pregnant with just one baby, your health care provider may recommend these treatments to help you stay pregnant longer:
- Cerclage: cervical cerclage is a procedure in which stitches are used to close the cervix during pregnancy to help prevent pregnancy loss or premature birth.
- Vaginal progesterone. Progesterone is a hormone that helps prepare your body for pregnancy. It may help prevent premature birth only if you have a short cervix and you’re pregnant with just one baby. You insert it in your vagina every day starting before or up to 24 weeks of pregnancy, and you stop taking it just before 37 weeks.
Many things can affect the length of your cervix, including:
- Having an overdistended (stretched or enlarged) uterus
- Problems caused by bleeding during pregnancy or inflammation (irritation) of the uterus
- Infection
- Cervical insufficiency
Figure 3. Short cervix
What is incompetent cervix ?
When you are told that you have an incompetent cervix, it simply means that your cervix begins to open up (dilates) too early during pregnancy, when you are between four and six weeks of your pregnancy. In case you do not know, the cervix mostly remains closed during the 9 months of pregnancy. An incompetent cervix can be thin and widen without any contractions or pain. This causes the amniotic fluid sac to bulge downwards into the cervix opening until it breaks. This leads to premature delivery or miscarriage. Contractions are when the muscles of your uterus get tight and then relax. They help push your baby out of your uterus during labor and birth.
Incompetent cervix can cause premature birth and miscarriage. Premature birth is when your baby is born too early, before 37 weeks of pregnancy. Miscarriage is when a baby dies in the womb before 20 weeks of pregnancy.
An incompetent or weakened cervix happens in about 1-2% of pregnancies. Almost 25% of babies miscarried in the second trimester are due to incompetent cervix.
Doctors don’t always know why incompetent cervix happens. You’re more likely than other women to have it if:
- You have defects in your uterus, like if it’s split into two sections.
- You’ve had surgery on your cervix.
- You have a short cervix. The shorter the cervix, the more likely you are to have cervical insufficiency.
- You’ve had injuries to your uterus that happened during a previous birth.
What Are the Symptoms of an Incompetent Cervix ?
If your have an incompetent cervix, you may not develop any symptoms or signs. Your cervix simply begins to open before 9 months are over without pain or contractions. You may feel very mild discomfort for a few days, but this is only possible if you are between 15 to 20 weeks of pregnancy.
However, look out for the following signs and symptoms, because they may indicate you’ve got an incompetent cervix:
- Backaches
- Pelvic pressure sensation
- Mild abdominal cramps
- Changes in your vaginal discharge
- Mild vaginal bleeding.
How is an Incompetent Cervix Diagnosed ?
The diagnosis of this condition can be challenging and is mostly based on a painless dilation of the cervix common after the first trimester. Some care provider can assess the length of the cervix from the vaginal opening during your second trimester to check for any cervical shortening through ultrasound. Other tests that are used to determine cervical incompetence include radiograph imaging and hysterosalpingography of cervix balloon tractions.
What Are the Risk Factors for Incompetent Cervix ?
You are at a higher risk of having this condition if:
- You have had a 2nd trimester miscarriage without known cause or if you have had an early spontaneous preterm delivery which was not caused by a placenta abruption or preterm labor.
- You have undergone a procedure like loop electrosurgical excision procedure (LEEP) or a cone biopsy on your cervix.
- Your mother used DES drugs while pregnant with you. This is a drug that was prescribed to expectant mothers to prevent miscarriage. Later it was found to be ineffective and it caused abnormalities in the reproductive tract of the fetus.
- You underwent a previous dilation and curettage or birth where your cervix was damaged or you have terminated several pregnancies.
- Your cervix is unusually shorter.
- You have undergone cervical insufficiency in previous pregnancies.
How Can an Incompetent Cervix Be Treated ?
If your health care provider thinks you may have cervical insufficiency, she may check you regularly during pregnancy with transvaginal ultrasound starting at 16 to 20 weeks of pregnancy. Transvaginal ultrasound is an ultrasound in the vagina, not on the outside of your belly. An ultrasound is a prenatal test that uses sound waves and a computer screen to show a picture of your baby in the womb.
Medication
Progesterone supplementation can be recommended if you have had a history of premature births. Your doctor will recommend weekly shots of progesterone hormone on your 2nd trimester. However, further research is required to prove that progesterone can help women with the risk of cervix incompetence.
Cerclage is also recommended as a form of treatment. This is especially if you suffered preterm labor when you were between sixteen and thirty four weeks of pregnancy. This procedure can be done on an outpatient basis. You’re required to relax after the treatment.
Steroids are also prescribed together with other drugs to prevent preterm labor. However, this can only be done after the 24 weeks mark where the child has a chance of survival. Steroids also help the baby’s lungs to develop quicker, which helps if the baby is to be born prematurely.
Serial Ultrasounds
If you suffer from premature births, your doctor may recommend ultrasounds after every two weeks to monitor the cervix. This is done from the 15th week to the 26th week. If the cervix is seen to become weaker or open, your doctor may recommend cervical cerclage.
Cerclage
If your pregnancy has not reached the 26th week mark and you have a history of early births, cerclage can prevent a premature birth. This procedure involves the stitching of the cervix to close it. The stiches can be removed during labor or the last month of your pregnancy. Your doctor can also recommend this procedure even before your cervix opens. This is mostly done before 14 weeks.
However, this procedure is not ideal for every woman at risk of premature labor. It is important to talk to your doctor concerning the benefits and risks of cerclage.
You can get a cerclage as early as 13 to 14 weeks of pregnancy, and your provider removes the stitch at about 37 weeks of pregnancy. Cerclage may be right for you if you’re pregnant now with just one baby and:
- You had a cerclage in a past pregnancy.
- You’ve had one or more pregnancy losses in the second trimester.
- You had a spontaneous premature birth before 34 weeks in a past pregnancy with a cervix shorter than 25 millimeters (about 1 inch) before 24 weeks of pregnancy. Spontaneous means that labor began on its own.
- In this pregnancy, your cervix is opening in the second trimester.
A cerclage is not recommended if you’re pregnant with twins, even if your cervix is shorter than 25 millimeters.
A woman would not be eligible for a cerclage if:
- There is increased irritation of the cervix
- The cervix has dilated 4cm
- Membranes have ruptured
Possible complications of cervical cerclage include uterine rupture, maternal hemorrhage, bladder rupture, cervical laceration, preterm labor and premature rupture of the membranes. The likelihood of these risks is very minimal, and most health care providers feel that a cerclage is a life saving procedure that is worth the possible risks involved.
Bed Rest
Instead of the cerclage, some doctors will recommend bed rest. Also, bed rest can be recommended together with the different medical options. Even so, there is no substantial evidence to prove that bed rest works to prevent preterm labor, it works with the theory that relieving the cervix of the pressure can help.
Pregnant cervix
When a woman becomes pregnant, the narrow opening of the cervix is sealed with a mucus plug, which forms a protective barrier for the cervical canal. During pregnancy, a lot of changes occur in the cervix, as it softens, becomes longer, then shortens, dilates and becomes thinner as pregnancy progresses. Why do these things happen, and what is the role of the cervix during pregnancy ? Here is some information to answer this question about your reproductive anatomy.
During pregnancy, the position of your cervix will change, but this happens at various times for different women.
The cervix rises a little bit and becomes softer as early as the 12th day after ovulation or a bit later, when your home pregnancy test becomes positive. For some women, this occurs just before they are expecting their period, while for others it happens just when their pregnancy is confirmed by a doctor.
Thickening of the cervix is usually the first change observed, since it produces more glandular cells that form the mucus plug. It may also become inflamed, appearing red on examination, and sometimes allowing some bleeding (spotting).
Thickening of the cervix serves to protect the uterus, but when your date of delivery is near, it starts to prepare for childbirth. Your cervix will slowly dilate, which causes the mucus plug to be lost. This may occur a few weeks before your expected date of delivery, but in other women, it may happen just as labor commences. However, physical examination alone cannot provide information if you are close to delivery.
The cervix is rigid and closed before pregnancy, but it softens and elongates during pregnancy. However, during labor, the cervix shortens and dilates to allow the passage of your baby.
Cervical shortening before 37 weeks of pregnancy increases your risk of giving birth to a premature baby. A baby is usually born about 38 weeks after conception. Although the cervix gradually softens and effaces (decreases in length) as the baby grows bigger in the uterus, it does not open or dilate until you are ready to give birth. If your cervix is short before the 37th week, you may go into preterm labor. If premature birth occurs even earlier, your baby may have greater health risks.
Factors that influence the length of your cervix during pregnancy include:
- Biological differences among women
- Uterine activity of unknown origin
- Overdistended or overstretched uterus
- Complications related to bleeding during your pregnancy
- Inflammation
- Infection
- Weak cervix (incompetent cervix)
Signs and symptoms that you are experiencing preterm labor include frequent or regular uterine contractions, vaginal spotting, pelvic pressure, or constant low back ache. Consult your health care provider to determine by pelvic examination, if your cervix is beginning to open. An ultrasound examination may be done to measure the length of your cervix.
The health care provider will explain the risks and benefits of treatments to try to stop your preterm labor. However, if you are not in active labor but you are still in early pregnancy and in danger of premature labor, your doctor may suggest that you have a cervical cerclage. This surgical procedure closes the cervix by stitching it with strong sutures. This is usually done in women who have a history of giving birth prematurely and has an ultrasound showing the cervix beginning to open.
Other forms of treatment involve the use of a hormone (progesterone) or a pessary (a silicone device), which is placed around your cervix to prevent premature birth.
If you have a history of premature birth and are concerned about the length of your cervix during pregnancy, consult your doctor to know more about promoting healthy pregnancy.
What is low cervix soft closed cervix ?
If you find your cervix low and soft, it could mean many different things. The most common explanation is that you are pregnant. A cervix that is softening, otherwise known as “ripening”, tends to happenafter a successful ovulation. You might also be at the end of your ovulation cycle.
During ovulation, a low soft cervix is very common. In addition, you might notice more vaginal discharge at that point, which will help the sperm move toward the egg. Also, the cervix will open just slightly. If you feel your cervix low and soft, it means you might be ready to get pregnant, while high and hard means you are at the start of ovulation, and not yet ready to release the egg.
However, checking your cervix is very important, as each woman is different. Some women can tell when they have a low soft closed cervix that they are definitely pregnant. For others, the cervix doesn’t do that at all. You may need several months to test out yourself.
Table 1 below shows the cervical positions for many women and what they mean. Use this as a rough guide until you figure out your own cervical position schedule throughout your cycle.
Table 1. Cervix position and what they mean
| Position | Firmness | Openness | Meaning |
| Low | Firm | Slightly open | During menstrual bleeding |
| Low | Hard | Closed | Right after your period ends |
| High | Soft | Closed | At the beginning of ovulation |
| High | Very Soft | Open | During the height of ovulation |
| Low | Firm | Closed | Right after ovulation |
| High | Soft | Closed | When pregnancy has occurred |
How to Check Your Cervical Position
Always wash your hands before checking your cervix. Try to find a comfortable position for yourself, either sitting on the toilet or standing near the bathtub with one leg on the edge. Slide your middle finger inside your vagina slowly and gently. The cervix is usually three to six inches inside the vagina. You might also notice some clear mucus on your fingers after you check it – this is entirely normal.
Tips: To get the best idea of where and how your cervix lies, check it once a day after your period has stopped. Check your cervix at the same time every day, and always empty your bladder first. Use the same position to check it each time, as changing position can affect the height of your cervix.
Other Ways to Tell Your Ovulation
When you are trying to get pregnant, there is much more than a low soft closed cervix position to help you determine ovulation. Be aware that your fertility takes many forms. Track your menstrual cycle to find the most fertile days. Check your cervical mucus for thickness. Monitor your hormones with at-home kits. Tracking your basal body temperature to find the days when hormones make it go up and down. Look for physical symptoms, such as mood swings and breast changes which indicate that ovulation is on the way. Many women choose to use all these methods together to ensure pregnancy.
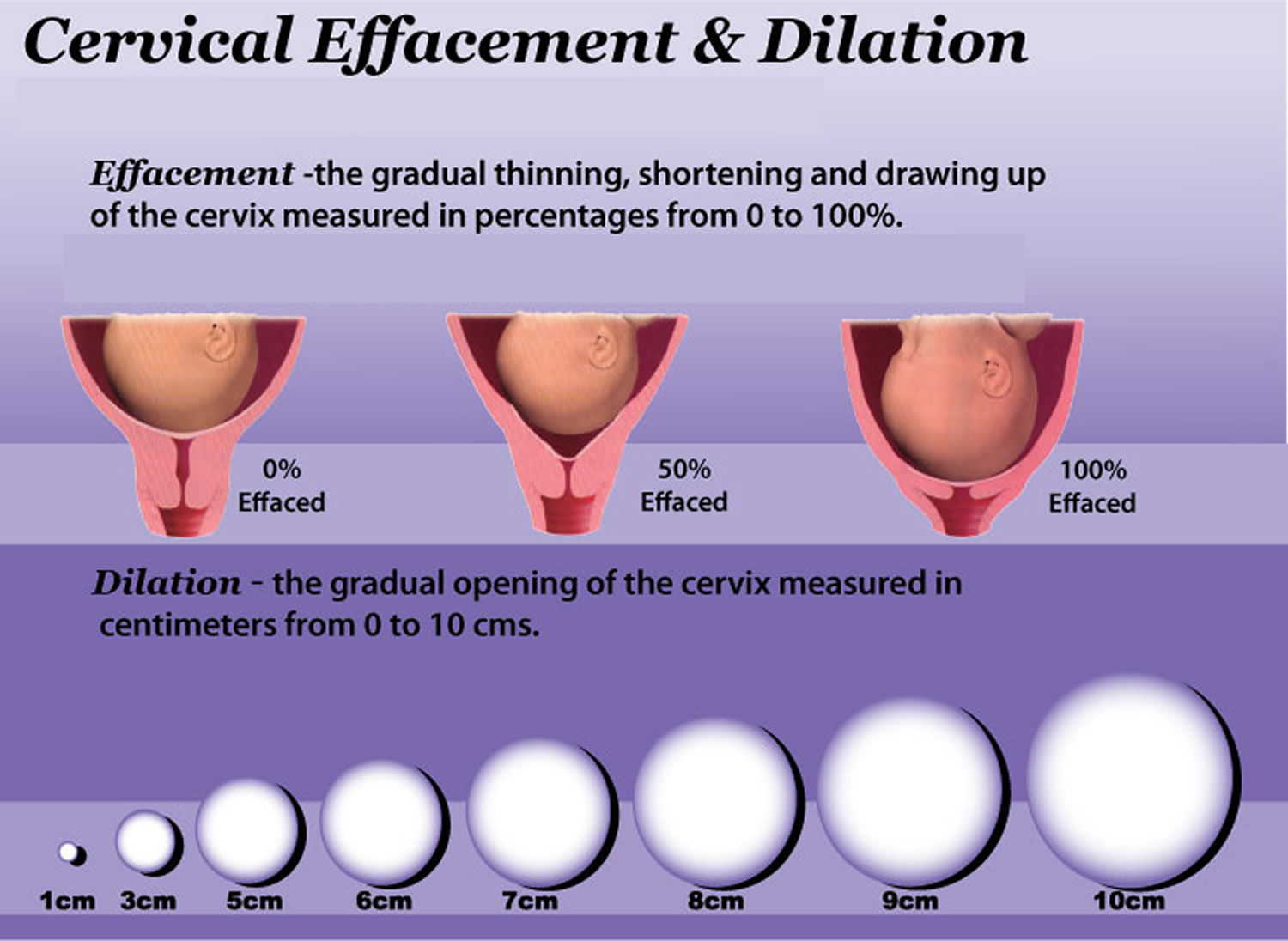
What is effaced cervix ?
The words effacement, being effaced and effacing are terms that you will hear often as you approach your last trimester of your pregnancy. These terms are used to describe the process that the cervix prepares itself for delivery and it is measured by percentage. If you are told that you are 50% effaced, this means that you are half way from complete effacement. 100% effacement or complete effacement tells you that your cervix is quite thin and you are about to get into labor.
Cervical effacement is the “ripened” or thinned stage of the cervix 3. Normally, the cervix of a woman who isn’t pregnant is thick and long. A normal cervix will measure between 3 to 5 centimeters in length. However, when you are pregnant and near the end of your pregnancy, the cervix will begin thinning out and becoming shorter. This process is what is referred to as effacement. The cervix naturally starts to become shorter and it begins to pull up to a point where it seems to disappear, becoming a part of the lower uterus.
Labor progression is described by the stretching and opening of the cervix. Throughout your pregnancy, your cervix will remain as normal before starting to thin out as labor nears. The cervix is estimated to dilate by a centimeter during each hour of labor. However, this should not be generalized because different women will dilate differently. A dilation of 0 – 4 centimeters is regarded to as early labor and this will progress as the woman nears child birth. It is rare for a woman to be dilated by up to 2 centimeter several weeks to giving birth. When cervix dilation measures between 4 and 7 centimeters, the woman is in active labor. At 7 to 10 centimeters, the woman is at the transition stage which is the final stage of labor. When the cervix is at 10 centimeters, this is considered full dilation and the woman is ready to give birth. 10 centimeters is about the size of the head of the newborn child.
As the expectant mother’s due date approaches, the baby’s head will drop down causing the uterus to contract. This contraction combined with the effacement going on and dilation will lead to cramping. These cramp pains and contraction may feel like active labor and this is actually described as false labor. It is also called Braxton Hicks contraction and these are merely signs of the labor process. This process will take a few weeks before the cervix is effaced fully. In first time pregnancies, the cervix can become effaced even before it is dilated but in subsequent pregnancies, dilation will occur before effacement.
In the last weeks of pregnancy, your doctor will examine your cervix to identify any changes that are occurring in preparation for birth. The cervical effacement will be measured to identify how ready the body is for delivery. 0% effacement would mean that your cervix has had no changes, while 50% effacement would mean that your cervix is half its ordinary thickness. When you are 100% effaced, your cervix is thinned out completely leaving only the uterus opening for delivery. At this stage, you will be going into labor in no time.
Figure 4. Cervix effacement
How to Efface the Cervix Naturally
The American Pregnancy Association makes it clear that complete effacement occurs when the baby is engaged to the mother’s pelvis. When 100% effaced, the cervix will soon start to push outward. Though this occurs naturally, effacement can also be induced medically when labor appears to have stalled using the methods below.
- Evening primrose oil
Evening primrose oil is recommended by a lot of midwives as a herbal treatment. The oil acts as prostaglandin which helps ripen the cervix. These oil capsules can be taken orally or rubbed on the cervix in the final weeks of pregnancies. These capsules can also be placed inside the woman’s vagina at bedtime. Evening primrose oil is not recommended for women who have had vaginal infections, placenta previa and other pregnancy complications.
- Sex
Sex in the last trimester can boost dilation in the cervix. Sperms have prostaglandins which can help thin out the cervix. However, this dilation encouragement method should not be practiced by women who have already lost their mucus plug. The mucus plug protects the cervix from infections caused by harmful bacteria which could affect the baby.
- Keep in a good position
The weight of the baby also could encourage dilation. Dilation will occur naturally when the baby drops down in preparation for birth. There are positions that also could encourage dilation and these include sitting on an exercise ball or sitting with your legs spread wide apart. Walking also could encourage dilation. Another technique you can use is getting on your hands and knees as this shifts the baby’s weight forward. In a nut shell, all positions that include opening up the pelvis or shifting the weight of the baby forward should help encourage dilation.
How do you know if and when your cervix is effaced ?
As mentioned above, first time pregnancies become effaced before the cervix is dilated. However, the reverse occurs for subsequent pregnancies. Towards the end of the pregnancy, your effacement progress will be checked by your doctor through routine prenatal visits and the doctor may have to take an internal examination to identify the extent of dilation. Based on the results, your doctor should be able to guess when you will deliver. However, this doesn’t mean that you should race to the delivery room because the prediction is as good as a guess meaning it may be much sooner that your actual due date. Chances that your doctors educated guess is accurate are quite rare and hundreds of women give birth weeks after the guess, so don’t be impatient.
The cervix will continue to dilate even when on labor and full dilation will occur towards the end of the transitional phase when dilation will be at 10 centimeters. There are three labor phases and the third stage is when the cervix completely opens up meaning your body is ready for delivery.
What is cervix dilation
When you are getting closer to your due date, you will notice your cervix dilating and softening to prepare for giving birth and this happens even before labor pains begin. The cervical dilation will happen during labor and is crucial in letting your baby pass out via the birth canal. Both cervical dilation and the other necessary changes for birth will be encouraged by your baby’s head putting pressure against your cervix and uterine contractions. You may be stressing when you are only, let’s say, 1 cm dilated. Whether you are a first time mom or have given birth before, you should know how you can dilate faster to fasten labor.
How to Dilate Your Cervix Faster
Notes and Precautions: You should always talk with your midwife or doctor ahead of time so they know what procedures you would be fine with and which ones you want to avoid. Each labor happens differently and in some cases you will need flexibility, but having a plan can still help.
You should always go with the natural method first, allowing your cervix to naturally dilate. Every mechanical or medical intervention will have a small risk and may even increase the risk of a cesarean section. Because of this, most doctors will only encourage you to speed up the dilation process or induce labor when they feel it is necessary.
Walk
When you are in labor you should try to walk as much as you can. The combination of body movement and gravity will help your baby descend down into your birth canal. In addition, the pressure that the baby’s head exerts on the cervix may help with dilation and even effacement (thinning) of your cervix. It can also help encourage contractions which in turn further help with dilation. You should ask someone to walk next to you and provide support and keep walking for as long as it is tolerable.
Use Birth Balls
Another option is to sit on a birth ball with your legs spread apart. Use a bed or chair to rest your upper body and then squat on the ball as this will relax your pelvic muscles and widen your pelvis. You can also gently rock and use gravity to bring your baby’s head down to your cervix to encourage dilation.
Do Gentle Exercises
Sometimes doing gentle exercises like walking a short distance, as mentioned above, can help with dilation. Another great idea is to go up then down stairs but be sure to do so in long and slow strides. This will help stretch and dilate your cervix. Walking wider and slower than normal increases the stretch of the cervix, encouraging dilation.
Relax with Warm Shower
Try either standing or sitting in a warm shower to help yourself relax. By relaxing, you prevent tense muscles which would make the physical work harder. Using a warm shower can ease tension while helping with cervical dilation and contractions. You can also lie in warm water, but make sure someone helps you get in and out.
If you are looking for other ways to relax, try listening to some soothing music. You can also ask someone to give you a gentle massage. No matter the way you relax, it will produce the same beneficial effects in terms of cervical dilation.
Empty Your Bladder
When your bladder is full, this inhibits contractions so there will be less pressure on your cervix, resulting in a slower dilation. Instead, be sure to urinate regularly.
Stimulate Your Nipples or Have Sex
Stimulation is one of the effective methods to dilate your cervix. It varies from woman to woman and sometimes simply rubbing your nipples will help, while other women find having sexual intercourse works best. This is considered a low-risk and safe option. The hormones found in semen (prostaglandins) will help your cervix efface and dilate. In fact, doctors will sometimes administer these hormones to encourage labor. After you orgasm, your body will release oxytocin which is another hormone capable of encouraging cervical dilation. You can also release this hormone by stimulating your nipples.
Try Acupressure
Acupressure is related to acupuncture but instead of applying needles to the pressure points, you simply apply pressure. You only need to understand anatomy and don’t need any special training to perform it. The most important pressure point for dilation is located on your hand, specifically the webbing between your forefinger and thumb. It should feel slightly tender when pressed. Apply the pressure for a minute or less then give it a break for two minutes and repeat on the other hand.
Medical Methods
You can also consider using a medication that is applied to your cervix by your doctor to dilate and soften your cervix.
- Misoprostol is a prostaglandin and can soften the cervix when placed within the vagina. It is safe, relatively inexpensive, and commonly used by doctors.
- Dinoprostone is similar and also a prostaglandin. You can either have it squirted into the cervical opening or inserted into your vagina in the form of a suppository.
- The enzyme hyaluronidase is produced from bovine testes. It can be injected into your cervix to help soften and dilate it. It will sometimes be used in cases when a woman’s cervix hasn’t dilated or ripened at all.
What is Tilted cervix
A tilted uterus, also called a tipped uterus, retroverted uterus or retroflexed uterus, is a normal uterus anatomical variation 4. It shouldn’t interfere with your ability to fall pregnant and have a baby.
In most women, the uterus tips forward at the cervix. About 1 in 4 women, however, has a uterus that leans backward, or tilts, at the cervix. In the past, doctors thought that a tilted uterus might have contributed to infertility. But experts now know that the position of the uterus doesn’t affect the ability of sperm to reach an egg.
Occasionally, a sharply tilted uterus may happen when scar tissues (adhesions) form due to conditions such as endometriosis, infection or prior surgery. Although this may make it more challenging for sperm to reach an egg, conception can still occur. However, in these cases, you may benefit from seeing a fertility specialist.
Figure 5. Tipped (tilted) uterus
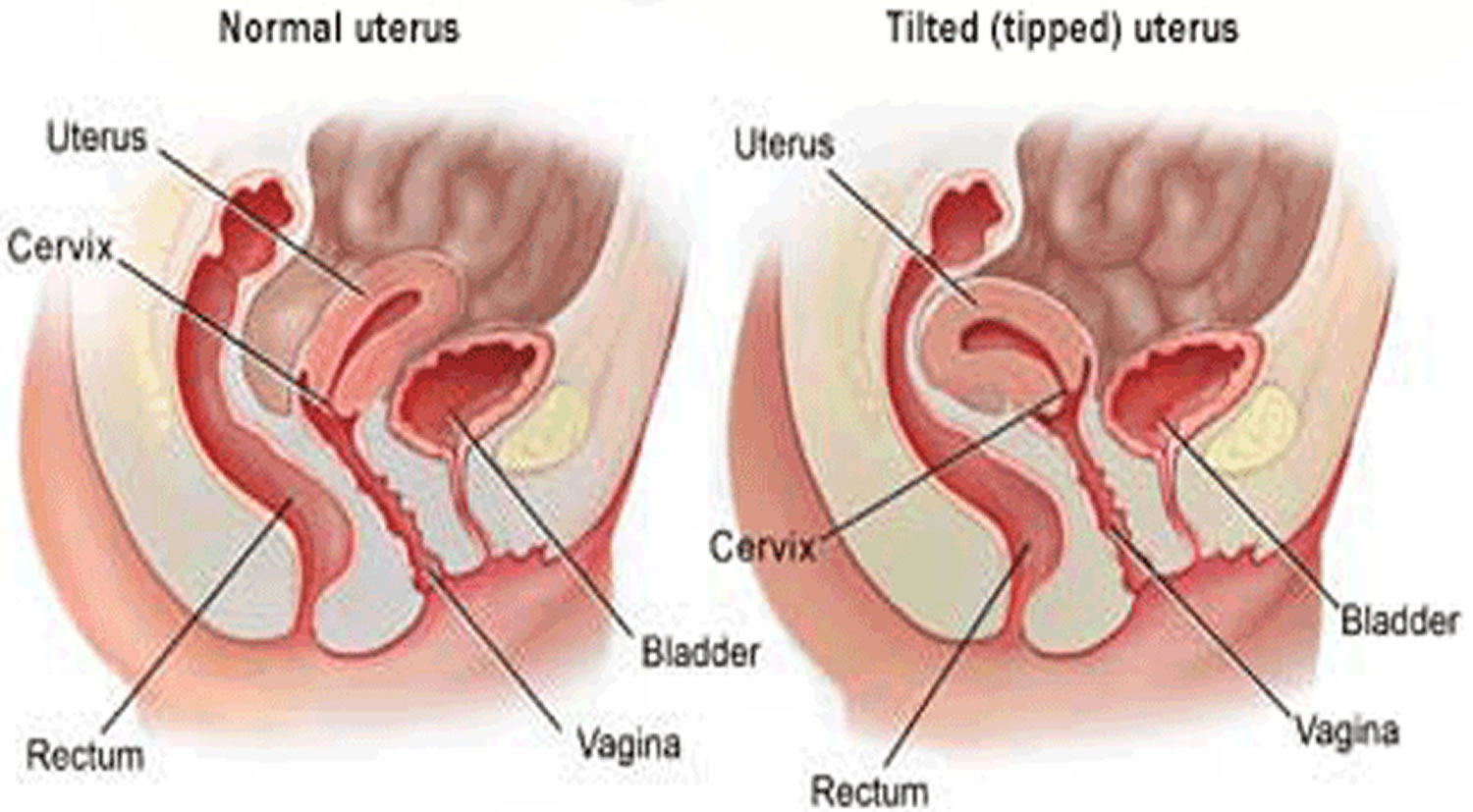
Causes of tilted uterus
Tilted uterus or retroversion of the uterus is common 5. One in 4 women has this condition. The problem may also occur due to weakening of the pelvic ligaments at the time of menopause. An enlarged uterus can also be caused by pregnancy or a tumor.
Scar tissue in the pelvis (pelvic adhesions) can also hold the uterus in a retroverted position. Scarring may come from 5:
- Endometriosis
- Infection in uterus or tubes
- Pelvic surgery
Symptoms of tilted uterus
Tilted uterus almost never causes any symptoms.
Rarely, it may cause pain or discomfort.
How is tilted uterus diagnosed ?
A pelvic exam will show the position of the uterus. However, a tilted uterus can sometimes be mistaken for a pelvic mass or a growing fibroid. A rectovaginal exam may be used to distinguish between a mass and a tilted uterus.
An ultrasound test can be used to see the exact position of the uterus.
Treatment for tilted uterus
Treatment is not needed most of the time. Underlying disorders, such as endometriosis or adhesions, should be treated as needed.
Outlook (Prognosis) for tilted uterus
In most cases, the condition does not cause problems.
Possible Complications of tilted uterus
Atypical positioning of the uterus may be caused by endometriosis, salpingitis, or pressure from a growing tumor.
When to Contact a Medical Professional
Call your health care provider if you have ongoing pelvic pain or discomfort.
Prevention of tilted uterus
There is no way to prevent the problem. Early treatment of uterine infections or endometriosis may reduce the chances of a change in the position of the uterus.
Tilted uterus and getting pregnant
Tilted uterus shouldn’t interfere with your ability to conceive 4.
What Is Cancer of the Cervix ?
Cancer starts when cells in the body begin to grow out of control. Cells in nearly any part of the body can become cancer, and can spread to other areas of the body.
Cervical cancer starts in the cells lining the cervix — the lower part of the uterus (womb). This is sometimes called the uterine cervix. The fetus grows in the body of the uterus (the upper part). The cervix connects the body of the uterus to the vagina (birth canal).
Most cancer of the cervix begin in the cells in the transformation zone 6. These cells do not suddenly change into cancer. Instead, the normal cells of the cervix first gradually develop pre-cancerous changes that turn into cancer. Doctors use several terms to describe these pre-cancerous changes, including cervical intraepithelial neoplasia (CIN), squamous intraepithelial lesion (SIL), and dysplasia 6. These changes can be detected by the Pap test and treated to prevent cancer from developing.
Although cervical cancers start from cells with pre-cancerous changes (pre-cancers), only some of the women with pre-cancers of the cervix will develop cancer 6. It usually takes several years for cervical pre-cancer to change to cervical cancer, but it also can happen in less than a year. For most women, pre-cancerous cells will go away without any treatment. Still, in some women pre-cancers turn into true (invasive) cancers. Treating all cervical pre-cancers can prevent almost all cervical cancers.
Types of cancer of the cervix
Cervical cancers and cervical pre-cancers are classified by how they look under a microscope. The main types of cervical cancers are squamous cell carcinoma and adenocarcinoma.
- Most (up to 9 out of 10) cervical cancers are squamous cell carcinomas. These cancers develop from cells in the exocervix and the cancer cells have features of squamous cells under the microscope. Squamous cell carcinomas most often begin in the transformation zone (where the exocervix joins the endocervix).
- Most of the other cervical cancers are adenocarcinomas. Adenocarcinomas are cancers that develop from gland cells. Cervical adenocarcinoma develops from the mucus-producing gland cells of the endocervix. Cervical adenocarcinomas seem to have become more common in the past 20 to 30 years.
- Less commonly, cervical cancers have features of both squamous cell carcinomas and adenocarcinomas. These are called adenosquamous carcinomas or mixed carcinomas.
Although almost all cervical cancers are either squamous cell carcinomas or adenocarcinomas, other types of cancer also can develop in the cervix. These other types, such as melanoma, sarcoma, and lymphoma, occur more commonly in other parts of the body.
Risk Factors for cancer of the cervix ?
A risk factor is anything that changes your chance of getting a disease such as cancer. Different cancers have different risk factors. For example, exposing skin to strong sunlight is a risk factor for skin cancer. Smoking is a risk factor for many cancers. But having a risk factor, or even several, does not mean that you will get the disease.
Several risk factors increase your chance of developing cervical cancer. Women without any of these risk factors rarely develop cervical cancer. Although these risk factors increase the odds of developing cervical cancer, many women with these risks do not develop this disease. When a woman develops cervical cancer or pre-cancerous changes, it might not be possible to say that a particular risk factor was the cause.
In thinking about risk factors, it helps to focus on those you can change or avoid (like smoking or human papilloma virus infection), rather than those you cannot (such as your age and family history). However, it is still important to know about risk factors that cannot be changed, because it’s even more important for women who have these factors to get regular Pap tests to detect cervical cancer early.
Cancer of the cervix risk factors include:
Human papilloma virus (HPV) infection
Infection by the human papilloma virus (HPV) is the most important risk factor for cervical cancer. HPV is a group of more than 150 related viruses. Some of them cause a type of growth called papillomas, which are more commonly known as warts.
- HPV can infect cells on the surface of the skin, and those lining the genitals, anus, mouth and throat, but not the blood or internal organs such as the heart or lungs.
- HPV can spread from one person to another during skin-to-skin contact. One way HPV spreads is through sex, including vaginal, anal, and even oral sex.
- Different types of HPV cause warts on different parts of the body. Some cause common warts on the hands and feet; others tend to cause warts on the lips or tongue.
Certain types of HPV may cause warts on or around the female and male genital organs and in the anal area. These are called low-risk types of HPV because they are seldom linked to cancer.
Other types of HPV are called high-risk types because they are strongly linked to cancers, including cancer of the cervix, vulva, and vagina in women, penile cancer in men, and cancers of the anus, mouth, and throat in both men and women.
Doctors believe that a woman must be infected with HPV in order to develop cervical cancer. Although this can mean infection with any of the high-risk types, about two-thirds of all cervical cancers are caused by HPV 16 and 18.
Infection with HPV is common, and in most people the body can clear the infection by itself. Sometimes, however, the infection does not go away and becomes chronic. Chronic infection, especially when it is caused by certain high-risk HPV types, can eventually cause certain cancers, such as cervical cancer.
Although there is currently no cure for HPV infection, there are ways to treat the warts and abnormal cell growth that HPV causes.
Smoking
When someone smokes, they and those around them are exposed to many cancer-causing chemicals that affect organs other than the lungs. These harmful substances are absorbed through the lungs and carried in the bloodstream throughout the body.
Women who smoke are about twice as likely as non-smokers to get cervical cancer. Tobacco by-products have been found in the cervical mucus of women who smoke. Researchers believe that these substances damage the DNA of cervix cells and may contribute to the development of cervical cancer. Smoking also makes the immune system less effective in fighting HPV infections.
Having a weakened immune system
Human immunodeficiency virus (HIV), the virus that causes AIDS, damages a woman’s immune system and puts them at higher risk for HPV infections. This might explain why women with AIDS have a higher risk for cervical cancer.
The immune system is important in destroying cancer cells and slowing their growth and spread. In women with HIV, a cervical pre-cancer might develop into an invasive cancer faster than it normally would.
Another group of women at risk for cervical cancer are those taking drugs to suppress their immune response, such as those being treated for an autoimmune disease (in which the immune system sees the body’s own tissues as foreign and attacks them, as it would a germ) or those who have had an organ transplant.
Chlamydia infection
Chlamydia is a relatively common kind of bacteria that can infect the reproductive system. It is spread by sexual contact. Chlamydia infection can cause pelvic inflammation, leading to infertility.
Some studies have seen a higher risk of cervical cancer in women whose blood tests and cervical mucus showed evidence of past or current chlamydia infection. Women who are infected with chlamydia often have no symptoms. In fact, they may not know that they are infected at all unless they are tested for chlamydia during a pelvic exam.
A diet low in fruits and vegetables
Women whose diets don’t include enough fruits and vegetables may be at increased risk for cervical cancer.
Being overweight
Overweight women are more likely to develop adenocarcinoma of the cervix.
Long-term use of oral contraceptives (birth control pills)
There is evidence that taking oral contraceptives (OCs) for a long time increases the risk of cancer of the cervix. Research suggests that the risk of cervical cancer goes up the longer a woman takes OCs, but the risk goes back down again after the OCs are stopped, and returns to normal about 10 years after stopping.
The American Cancer Society believes that a woman and her doctor should discuss whether the benefits of using OCs outweigh the potential risks.
Intrauterine device ( IUD) use
Some research suggests that women who had ever used an intrauterine device (IUD) had a lower risk of cervical cancer. The effect on risk was seen even in women who had an IUD for less than a year, and the protective effect remained after the IUDs were removed.
Using an IUD might also lower the risk of endometrial (uterine) cancer. However, IUDs do have some risks. A woman interested in using an IUD should first discuss the possible risks and benefits with her doctor. Also, a woman with multiple sexual partners should use condoms to lower her risk of sexually transmitted illnesses no matter what other form of contraception she uses.
Having multiple full-term pregnancies
Women who have had 3 or more full-term pregnancies have an increased risk of developing cervical cancer. No one really knows why this is true. One theory is that these women had to have had unprotected intercourse to get pregnant, so they may have had more exposure to HPV. Also, studies have pointed to hormonal changes during pregnancy as possibly making women more susceptible to HPV infection or cancer growth. Another thought is that pregnant women might have weaker immune systems, allowing for HPV infection and cancer growth.
Being younger than 17 at your first full-term pregnancy
Women who were younger than 17 years when they had their first full-term pregnancy are almost 2 times more likely to get cervical cancer later in life than women who waited to get pregnant until they were 25 years or older.
Economic status
Many low-income women do not have easy access to adequate health care services, including Pap tests. This means they may not get screened or treated for cervical pre-cancers.
Diethylstilbestrol
Diethylstilbestrol is a hormonal drug that was given to some women between 1940 and 1971 to prevent miscarriage. Women whose mothers took diethylstilbestrol (when pregnant with them) develop clear-cell adenocarcinoma of the vagina or cervix more often than would normally be expected. These types of cancer are extremely rare in women who haven’t been exposed to diethylstilbestrol. There is about 1 case of vaginal or cervical clear-cell adenocarcinoma in every 1,000 women whose mothers took diethylstilbestrol during pregnancy. This means that about 99.9% of “diethylstilbestrol daughters” do not develop these cancers.
Diethylstilbestrol-related clear cell adenocarcinoma is more common in the vagina than the cervix. The risk appears to be greatest in women whose mothers took the drug during their first 16 weeks of pregnancy. The average age of women diagnosed with diethylstilbestrol-related clear-cell adenocarcinoma is 19 years. Since the use of diethylstilbestrol during pregnancy was stopped by the FDA in 1971, even the youngest diethylstilbestrol daughters are older than 40 − past the age of highest risk. Still, there is no age cut-off when these women are felt to be safe from diethylstilbestrol-related cancer. Doctors do not know exactly how long these women will remain at risk.
Diethylstilbestrol daughters may also be at increased risk of developing squamous cell cancers and pre-cancers of the cervix linked to HPV.
Having a family history of cervical cancer
Cervical cancer may run in some families. If your mother or sister had cervical cancer, your chances of developing the disease are 2 to 3 times higher than if no one in the family had it. Some researchers suspect that some instances of this familial tendency are caused by an inherited condition that makes some women less able to fight off HPV infection than others. In other instances, women in the same family as a patient already diagnosed could be more likely to have one or more of the other non-genetic risk factors previously described in this section.
What Causes cancer of the cervix ?
In recent years, there has been a lot of progress in understanding what happens in cells of the cervix when cancer develops. In addition, several risk factors have been identified that increase the odds that a woman might develop cervical cancer.
The development of normal human cells mostly depends on the information contained in the cells’ DNA. DNA is the chemical in our cells that makes up our genes, which control how our cells work. We look like our parents because they are the source of our DNA. But DNA affects more than just how we look.
Some genes control when cells grow, divide, and die:·
- Genes that help cells grow, divide, and stay alive are called oncogenes.
- Genes that help keep cell growth under control or make cells die at the right time are called tumor suppressor genes.
Cancers can be caused by DNA mutations (gene defects) that turn on oncogenes or turn off tumor suppressor genes.
Human papilloma viruses (HPV) cause the production of two proteins known as E6 and E7 which turn off some tumor suppressor genes. This may allow the cervical lining cells to grow too much and to develop changes in additional genes, which in some cases will lead to cancer.
But HPV is not the only cause of cervical cancer. Most women with HPV don’t get cervical cancer, and certain other risk factors, like smoking and HIV infection, influence which women exposed to HPV are more likely to develop cervical cancer.
Cervix Cancer Prevention
The most common form of cervical cancer starts with pre-cancerous changes and there are ways to stop this disease from developing. The first way is to find and treat pre-cancers before they become true cancers, and the second is to prevent the pre-cancers.
Finding cervical pre-cancers
A well-proven way to prevent cervical cancer is to have testing (screening) to find pre-cancers before they can turn into invasive cancer. The Pap test (or Pap smear) and the human papilloma virus (HPV) test are used for this. If a pre-cancer is found it can be treated, stopping cervical cancer before it really starts. Most invasive cervical cancers are found in women who have not had regular Pap tests.
The Pap test is a procedure used to collect cells from the cervix so that they can be looked at under a microscope to find cancer and pre-cancer. These cells can also be used for HPV testing. A Pap test can be done during a pelvic exam, but not all pelvic exams include a Pap test.
An HPV test can be done on the same sample of cells collected from the Pap test.
The most important thing you can do to prevent cervical cancer is to be tested according to American Cancer Society guidelines.
The American Cancer Society recommends that women follow these guidelines to help find cervix cancer early 7. Following these guidelines can also find pre-cancers, which can be treated to keep cervical cancer from forming.
- All women should begin cervical cancer testing (screening) at age 21. Women aged 21 to 29, should have a Pap test every 3 years. HPV testing should not be used for screening in this age group (it may be used as a part of follow-up for an abnormal Pap test).
- Beginning at age 30, the preferred way to screen is with a Pap test combined with an HPV test every 5 years. This is called co-testing and should continue until age 65.
- Another reasonable option for women 30 to 65 is to get tested every 3 years with just the Pap test.
- Women who are at high risk of cervical cancer because of a suppressed immune system (for example from HIV infection, organ transplant, or long-term steroid use) or because they were exposed to diethylstilbestrol in utero may need to be screened more often. They should follow the recommendations of their health care team.
- Women over 65 years of age who have had regular screening in the previous 10 years should stop cervical cancer screening as long as they haven’t had any serious pre-cancers (like CIN2 or CIN3) found in the last 20 years (CIN stands for cervical intraepithelial neoplasia). Women with a history of CIN2 or CIN3 should continue to have testing for at least 20 years after the abnormality was found.
- Women who have had a total hysterectomy (removal of the uterus and cervix) should stop screening (such as Pap tests and HPV tests), unless the hysterectomy was done as a treatment for cervical pre-cancer (or cancer). Women who have had a hysterectomy without removal of the cervix (called a supra-cervical hysterectomy) should continue cervical cancer screening according to the guidelines above.
- Women of any age should NOT be screened every year by any screening method.
- Women who have been vaccinated against HPV should still follow these guidelines.
Some women believe that they can stop cervical cancer screening once they have stopped having children. This is not true. They should continue to follow American Cancer Society guidelines.
Although annual (every year) screening should not be done, women who have abnormal screening results may need to have a follow-up Pap test (sometimes with a HPV test) done in 6 months or a year.
The American Cancer Society guidelines for early detection of cervical cancer do not apply to women who have been diagnosed with cervical cancer, cervical pre-cancer, or HIV infection. These women should have follow-up testing and cervical cancer screening as recommended by their health care team.
Screening tests offer the best chance to have cervical cancer found early when successful treatment is likely. Screening can also actually prevent most cervical cancers by finding abnormal cervical cell changes (pre-cancers) so that they can be treated before they have a chance to turn into a cervical cancer.
If it’s found early, cervical cancer is one of the most successfully treatable cancers. In the United States, the cervical cancer death rate declined by more than 50% over the last 30 years. This is thought to be mainly due to the effectiveness of screening with the Pap test.
Despite the recognized benefits of cervical cancer screening, not all American women get screened. Most cervical cancers are found in women who have never had a Pap test or who have not had one recently. Women without health insurance and women who have recently immigrated are less likely to have cervical cancer screening.
Things to do to prevent pre-cancers
There are also some things you can do to prevent pre-cancers, such as:
- Avoiding exposure to HPV
- Getting an HPV vaccine
- Not smoking
Tests for cervix cancer
The first step in finding cervical cancer is often an abnormal Pap test result. This will lead to further tests which can diagnose cervical cancer.
Cervical cancer may also be suspected if you have symptoms like abnormal vaginal bleeding or pain during sex. Your primary doctor or gynecologist often can do the tests needed to diagnose pre-cancers and cancers and may also be able to treat a pre-cancer.
If there is a diagnosis of invasive cancer, your doctor should refer you to a gynecologic oncologist, a doctor who specializes in cancers of women’s reproductive systems.
Tests for women with symptoms of cervix cancer or abnormal Pap results
Medical history and physical exam
First, the doctor will ask you about your personal and family medical history. This includes information related to risk factors and symptoms of cervical cancer. A complete physical exam will help evaluate your general state of health. The doctor will do a pelvic exam and may do a Pap test if one has not already been done. In addition, your lymph nodes will be felt for evidence of metastasis (cancer spread).
The Pap test is a screening test, not a diagnostic test. It cannot tell for certain if you have cervical cancer. An abnormal Pap test result may mean more testing, sometimes including tests to see if a cancer or a pre-cancer is actually present. The tests that are used include colposcopy (with biopsy), endocervical scraping, and cone biopsies.
Colposcopy
If you have certain symptoms that are suggestive of cancer or if your Pap test result shows abnormal cells, you will need to have a test called colposcopy. You will lie on the exam table as you do with a pelvic exam. A speculum will be placed in the vagina to help the doctor see the cervix. The doctor will use a colposcope to examine the cervix. The colposcope is an instrument that stays outside the body and has magnifying lenses. It lets the doctor see the surface of the cervix closely and clearly. Colposcopy itself is usually no more uncomfortable than any other speculum exam. It can be done safely even if you are pregnant. Like the Pap test, it is better not to do it during your menstrual period.
The doctor will put a weak solution of acetic acid (similar to vinegar) on your cervix to make any abnormal areas easier to see. If an abnormal area is seen, a biopsy (removal of a small piece of tissue) will be done. The tissue is sent to a lab to be looked at under a microscope. A biopsy is the best way to tell for certain if an abnormal area is a pre-cancer, a true cancer, or neither. Although the colposcopy procedure is usually not painful, the cervical biopsy can cause discomfort, cramping, bleeding, or even pain in some women.
Cervical biopsies
Several types of biopsies can be used to diagnose cervical pre-cancers and cancers. If the biopsy can completely remove all of the abnormal tissue, it might be the only treatment needed.
Colposcopic biopsy
For this type of biopsy, first the cervix is examined with a colposcope to find the abnormal areas. Using a biopsy forceps, a small (about 1/8-inch) section of the abnormal area on the surface of the cervix is removed. The biopsy procedure may cause mild cramping, brief pain, and some slight bleeding afterward. A local anesthetic is sometimes used to numb the cervix before the biopsy.
Endocervical curettage (endocervical scraping)
Sometimes the transformation zone (the area at risk for HPV infection and pre-cancer) cannot be seen with the colposcope and something else must be done to check that area for cancer. This means taking a scraping of the endocervix by inserting a narrow instrument (called a curette) into the endocervical canal (the part of the cervix closest to the uterus). The curette is used to scrape the inside of the canal to remove some of the tissue, which is then sent to the laboratory for examination. After this procedure, patients may feel a cramping pain, and they may also have some light bleeding.
Cone biopsy
In this procedure, also known as conization, the doctor removes a cone-shaped piece of tissue from the cervix. The base of the cone is formed by the exocervix (outer part of the cervix), and the point or apex of the cone is from the endocervical canal. The tissue removed in the cone includes the transformation zone (the border between the exocervix and endocervix, where cervical pre-cancers and cancers are most likely to start).
A cone biopsy can also be used as a treatment to completely remove many pre-cancers and some very early cancers. Having had a cone biopsy will not prevent most women from getting pregnant, but if a large amount of tissue has been removed, women may have a higher risk of giving birth prematurely.
The methods commonly used for cone biopsies are the loop electrosurgical excision procedure (LEEP), also called the large loop excision of the transformation zone (LLETZ), and the cold knife cone biopsy.
Loop electrosurgical procedure (LEEP, LLETZ): In this method, the tissue is removed with a thin wire loop that is heated by electricity and acts as a small knife. For this procedure, a local anesthetic is used, and it can be done in your doctor’s office.
Cold knife cone biopsy: This method is done in a hospital. A surgical scalpel or a laser is used to remove the tissue instead of a heated wire. You will receive anesthesia during the operation (either a general anesthesia, where you are asleep, or a spinal or epidural anesthesia, where an injection into the area around the spinal cord makes you numb below the waist). Having any type of cone biopsy will not prevent most women from getting pregnant, but if a large amount of tissue has been removed, women may have a higher risk of giving birth prematurely.
Pre-cancerous changes in a biopsy are called cervical intraepithelial neoplasia (CIN). Sometimes the term dysplasia is used instead of CIN. CIN is graded on a scale of 1 to 3 based on how much of the cervical tissue looks abnormal when viewed under the microscope.
How biopsy results are reported
- In CIN1, not much of the tissue looks abnormal, and it is considered the least serious cervical pre-cancer (mild dysplasia).
- In CIN2 more of the tissue looks abnormal (moderate dysplasia)
- In CIN3 most of the tissue looks abnormal; CIN3 is the most serious pre-cancer (severe dysplasia) and includes carcinoma in situ).
If a biopsy shows a pre-cancer, doctors will take steps to keep an actual cancer from developing. Treatment of women with abnormal pap results is discussed in
Cervix cancer Prevention and Early Detection
Diagnostic tests for women with cervical cancer
If a biopsy shows that cancer is present, your doctor may order certain tests to see how far the cancer has spread. Many of the tests described below are not necessary for every patient. Decisions about using these tests are based on the results of the physical exam and biopsy.
Cystoscopy, proctoscopy, and examination under anesthesia
These are most often done in women who have large tumors. They are not necessary if the cancer is caught early.
In cystoscopy a slender tube with a lens and a light is placed into the bladder through the urethra. This lets the doctor check your bladder and urethra to see if cancer is growing into these areas. Biopsy samples can be removed during cystoscopy for pathologic (microscopic) testing. Cystoscopy can be done under a local anesthetic, but some patients may need general anesthesia. Your doctor will let you know what to expect before and after the procedure.
Proctoscopy is a visual inspection of the rectum through a lighted tube to check for spread of cervical cancer into your rectum.
Your doctor may also do a pelvic exam while you are under anesthesia to find out if the cancer has spread beyond the cervix.
Imaging studies
If your doctor finds that you have cervical cancer, certain imaging studies may be done to look inside the body. These tests can show if and where the cancer has spread, which will help you and your doctor decide on a treatment plan.
Chest x-ray
Your chest may be x-rayed to see if cancer has spread to your lungs. This is very unlikely unless the cancer is far advanced.
Computed tomography (CT)
CT scans are usually done if the tumor is larger or if there is concern about cancer spread. For more information, see CT Scan for Cancer.
Magnetic resonance imaging (MRI)
MRI looks at soft tissue parts of the body sometimes better than other imaging tests. Your doctor will decide which imaging test is best for your situation.
Intravenous urography
Intravenous urography (also known as intravenous pyelogram, or IVP) is an x-ray of the urinary system taken after a special dye is injected into a vein. This test can find abnormal areas in the urinary tract, caused by the spread of cervical cancer. The most common finding is a blockage of the ureters (tubes that connect the kidneys to the bladder) by the cancer. IVP is rarely used for patients with cervical cancer because CT and MRI are also good at finding abnormal areas in the urinary tract, as well as others not seen with an IVP.
Positron emission tomography (PET scan)
PET scans use glucose (a form of sugar) that contains a radioactive atom. Cancer cells in the body absorb large amounts of the radioactive sugar and a special camera can detect the radioactivity.
This test can help see if the cancer has spread to lymph nodes. PET scans can also be useful if your doctor thinks the cancer has spread but doesn’t know where, because they scan your whole body.
PET scans are often combined with CT scans using a machine that can do both at the same time. The combined PET/CT test is rarely used for patients with early cervical cancer, but may be used to look for more advanced cancer or if radiation treatment is a possibility.
General treatment information for cancer of the cervix
The options for treating each patient with cervical cancer depend on the stage of disease. The stage of a cervical cancer describes its size, depth of invasion (how far it has grown into the cervix), and how far it has spread.
After establishing the stage of your cervical cancer, your cancer care team will recommend your treatment options. Think about your options without feeling rushed. If there is anything you do not understand, ask for an explanation. Although the choice of treatment depends largely on the stage of the disease at the time of diagnosis, other factors that may influence your options are your age, your general health, your individual circumstances, and your preferences. Cervical cancer can affect your sex life and your ability to have children. These concerns should also be considered as you make treatment decisions.
Depending on the type and stage of your cancer, you may need more than one type of treatment. Doctors on your cancer treatment team may include:
- A gynecologist: a doctor who treats diseases of the female reproductive system
- A gynecologic oncologist: a doctor who specializes in cancers of the female reproductive system
- A radiation oncologist: a doctor who uses radiation to treat cancer
- A medical oncologist: a doctor who uses chemotherapy and other medicines to treat cancer
Many other specialists may be involved in your care as well, including nurse practitioners, nurses, psychologists, social workers, rehabilitation specialists, and other health professionals.
Common types of treatments for cervical cancer include:
- Surgery
- Radiation therapy
- Chemotherapy (chemo)
- Targeted therapy
For the earliest stages of cervical cancer, either surgery or radiation combined with chemo may be used. For later stages, radiation combined with chemo is usually the main treatment. Chemo (by itself) is often used to treat advanced cervical cancer.
It is often a good idea to get a second opinion, especially from doctors experienced in treating cervical cancer. A second opinion can give you more information and help you feel more confident about choosing a treatment plan. Some insurance companies require a second opinion before they will agree to pay for certain treatments. Almost all will pay for a second opinion. Still, you might want to check your coverage first, so you’ll know if you will have to pay for it.
It is important to discuss all of your treatment options, including their goals and possible side effects, with your doctors to help make the decisions that best fit your needs. It’s also very important to ask questions if there’s anything you’re not sure about.
Your recovery is the goal of your cancer care team. If a cure is not possible, the goal may be to remove or destroy as much of the cancer as possible to help you live longer and feel better. Sometimes treatment is aimed at relieving symptoms. This is called palliative treatment.
Considering complementary and alternative methods
You may hear about alternative or complementary methods that your doctor hasn’t mentioned to treat your cancer or relieve symptoms. These methods can include vitamins, herbs, and special diets, or other methods such as acupuncture or massage, to name a few.
Complementary methods refer to treatments that are used along with your regular medical care. Alternative treatments are used instead of a doctor’s medical treatment. Although some of these methods might be helpful in relieving symptoms or helping you feel better, many have not been proven to work. Some might even be dangerous.
- Cervical insufficiency and short cervix. March of Dimes Foundation. https://www.marchofdimes.org/complications/cervical-insufficiency-and-short-cervix.aspx[↩]
- Low Soft Closed Cervix http://www.newkidscenter.com/Low-Soft-Closed-Cervix.html[↩]
- What Does Effacement Mean? Newkids Center. http://www.newkidscenter.com/What-Does-Effacement-Mean.html[↩]
- Tilted uterus: Can it lead to infertility? Mayo Clinic. https://www.mayoclinic.org/tilted-uterus/expert-answers/faq-20058485[↩][↩]
- Retroversion of the uterus. Medline Plus. https://medlineplus.gov/ency/article/001506.htm[↩][↩]
- What Is Cervical Cancer ? American Cancer Society. https://www.cancer.org/cancer/cervical-cancer/about/what-is-cervical-cancer.html[↩][↩][↩]
- The American Cancer Society Guidelines for the Prevention and Early Detection of Cervical Cancer. American Cancer Society. https://www.cancer.org/cancer/cervical-cancer/prevention-and-early-detection/cervical-cancer-screening-guidelines.html[↩]