Contents
- What is cognitive behavioral therapy
- What are harmful thoughts and behavioral patterns, which are not?
- How is cognitive behavioral therapy different from other psychotherapies?
- What are advantages and disadvantages of CBT?
- Is CBT different when used in Children vs. Adults?
- How long does CBT take to work?
- When can CBT be combined with medications?
- What are potential limitations of CBT?
- When doesn’t CBT work?
- How does cognitive behavioral therapy (CBT) work?
- What can CBT help with?
- What are the stages of CBT?
- Who can provide CBT?
- What can I expect from CBT?
- What are risks of cognitive behavioral therapy (CBT)?
- How effective is cognitive behavioral therapy (CBT)?
What is cognitive behavioral therapy
Cognitive behavioral therapy also known as cognitive therapy or CBT, is a common type of psychotherapy (psychological treatment) or “talking therapy” that is based on the idea that how you think and behave affects how you feel 1. CBT (cognitive behavioral therapy) can help you manage your problems — with both mental and physical health problems. If you are thinking negatively about yourself or a situation and that is causing you problems, CBT might be able to help. You work with a therapist (psychotherapist, psychologists or psychiatrists) in a structured way, attending a limited number of sessions. CBT helps you become aware of your inaccurate or negative thinking so you can view challenging situations more clearly and respond to them in a more effective way. Cognitive behavioral therapy (CBT) has been demonstrated to be effective ― either alone or in combination with other therapies ― for a range of problems including depression, anxiety disorders, alcohol and drug use problems, marital problems, post-traumatic stress disorder (PTSD), eating disorders, and severe mental illness. But not everyone who benefits from CBT has a mental health condition. CBT can also be an effective tool to help anyone learn how to better manage stressful life situations. In some cases, CBT is most effective when it’s combined with other treatments, such as antidepressants or other medications.
The term cognitive comes from the Latin “cognoscere”, meaning “to recognize” 2. The point of cognitive behavioral therapy is to form a clear idea of your own thoughts, attitudes and expectations. The goal is to reveal and change false and distressing beliefs, because it is often not only the things and situations themselves that cause problems, but the importance that you attach to them too (see Figures 1 and 2 below). For example, a dangerous thought pattern might be when somebody immediately draws negative conclusions from an occurrence, generalizes them and applies them to similar situations. In psychology, this generalized way of thinking is called “over-generalizing.” For example, imagine you are driving on your way to an important meeting and maybe even running a little late and been stopped by a red light only to say something like, “Why do I always hit every red light?” If so, you are like many people who use words like “always” and “every” when you evaluate events even though those words probably are not entirely accurate. In other words, while you might be stopped by a lot of red lights, you probably do not always get stopped by every single one of them. This is an example of overgeneralizing, which is when you use overly broad language in our evaluations of events or people. You can really hear overgeneralizing in the language people use when they talk about provocations. They use words like “always,” “never,” “everybody,” and “nobody.” This type of thinking and language matters because once you say something always happens to you, you start responding to the pattern of events instead of just the one event that has just happened.
Another distressing error in reasoning is “catastrophizing”. Catastrophizing is a cognitive distortion that prompts people to jump to the worst possible conclusion, usually with very limited information or objective reason to despair. When a situation is upsetting, but not necessarily catastrophic, they still feel like they are in the midst of a crisis. This pattern of thinking can itself be destructive because unnecessary and persistent worry can lead to heightened anxiety and depression. But through learning to identify and reframe initially exaggerated conclusions, along with other techniques, people with a tendency to make a proverbial mountain out of a molehill can get a better hold on their negative thoughts.
Such thought patterns can sometimes develop into self-fulfilling prophecies and make life difficult for the people affected. Research demonstrates that problematic patterns of thinking and behavior underlie most forms of psychopathology 3. Behavioral change has been shown to lead to cognitive changes, and vice versa; these changes lead to reductions in psychopathology 4, 5.
Cognitive behavioral therapy (CBT) helps people learn to replace these thought patterns with more realistic and less harmful thoughts. Cognitive behavioral therapy (CBT) also helps people to think more clearly and to control their own thoughts better.
Numerous research studies suggest that CBT (cognitive behavioral therapy) leads to significant improvement in functioning and quality of life. In many studies, cognitive behavioral therapy has been demonstrated to be as effective as, or more effective than, other forms of psychological therapy or psychiatric medications 2.
It is important to emphasize that advances in CBT have been made on the basis of both research and clinical practice. Indeed, CBT is an approach for which there is ample scientific evidence that the methods that have been developed actually produce change. In this manner, CBT differs from many other forms of psychological treatment.
CBT has been around for many years. It’s the basis of other therapies such as acceptance and commitment therapy, mindfulness-based cognitive therapy, schema therapy and dialectical behavior therapy (DBT).
CBT is based on several core principles, including:
- Psychological problems are based, in part, on faulty or unhelpful ways of thinking.
- Psychological problems are based, in part, on learned patterns of unhelpful behavior.
- People suffering from psychological problems can learn better ways of coping with them, thereby relieving their symptoms and becoming more effective in their lives.
Core components and characteristics of Cognitive Behavior Therapy
- Cognitive behavioral therapy is offered in psychotherapy practices, hospitals and rehabilitation clinics. It is sometimes also offered as group therapy.
- Typical CBT treatments involve approximately 60- to 90-minute sessions per week for 8 to 12 weeks 6. But there is also no standard length of cognitive behavioral therapy. Some people already feel much better after a few sessions, while others need treatment for several months. This depends on the kind and severity of the problems, among other things.
- Symptom measures are collected frequently
- Treatment is goal-oriented and collaborative; patient is expected to be an active participant
- Treatment is focused on changing current problematic or maladaptive thoughts or behaviors
- Weekly homework assignments
CBT treatment usually involves efforts to change thinking patterns. These strategies might include:
- Learning to recognize one’s distortions in thinking that are creating problems, and then to reevaluate them in light of reality.
- Gaining a better understanding of the behavior and motivation of others.
- Using problem-solving skills to cope with difficult situations.
- Learning to develop a greater sense of confidence in one’s own abilities.
CBT treatment also usually involves efforts to change behavioral patterns. These strategies might include:
- Facing one’s fears instead of avoiding them.
- Using role playing to prepare for potentially problematic interactions with others.
- Learning to calm one’s mind and relax one’s body.
Not all CBT will use all of these strategies. Rather, the psychologist and patient/client work together, in a collaborative fashion, to develop an understanding of the problem and to develop a treatment strategy.
CBT places an emphasis on helping individuals learn to be their own therapists. Through exercises in the session as well as “homework” exercises outside of sessions, patients/clients are helped to develop coping skills, whereby they can learn to change their own thinking, problematic emotions, and behavior.
CBT therapists emphasize what is going on in the person’s current life, rather than what has led up to their difficulties. A certain amount of information about one’s history is needed, but the focus is primarily on moving forward in time to develop more effective ways of coping with life.
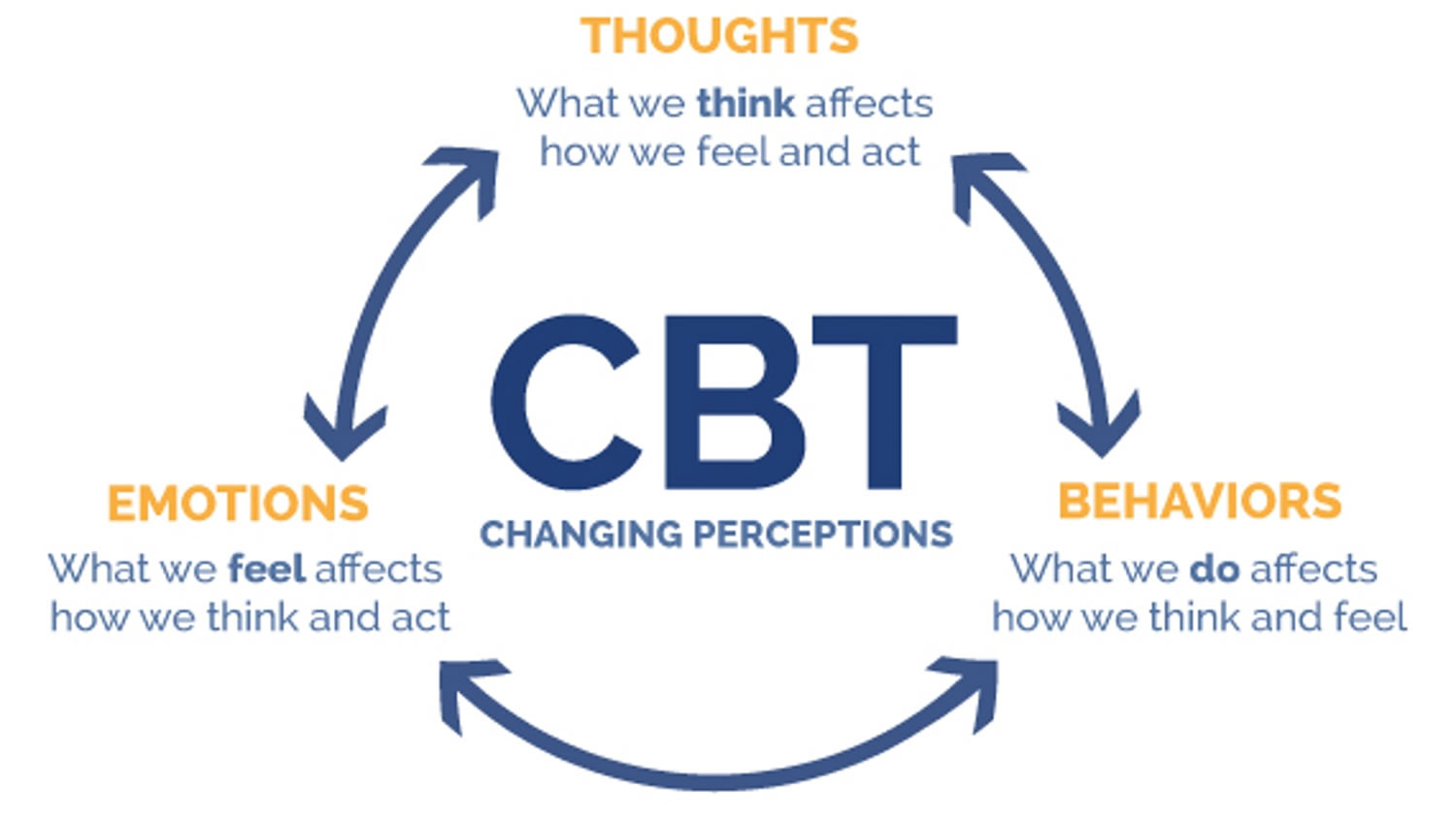
Figure 1. Principle of cognitive behavioral therapy
Footnote: Which methods of cognitive behavioral therapy are applied depends on your illness or problem to be treated. The basic principle behind CBT therapy is however always the same: What you think, how you feel and how you behave are all closely connected – and all of these factors have a decisive influence on your well-being.
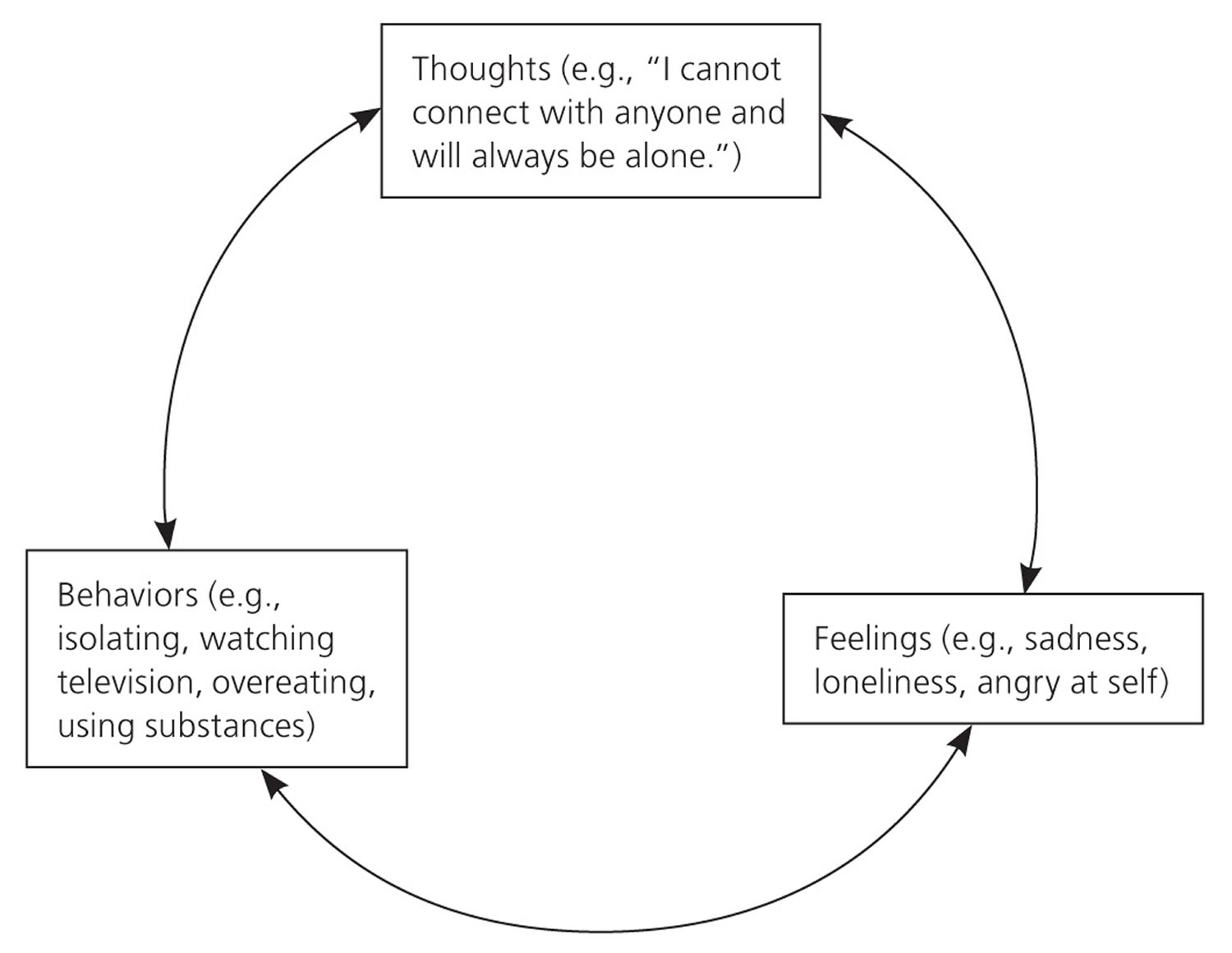
Figure 2. Cognitive Behavioral Model
Footnote: The cognitive behavioral model illustrates problematic patterns in thoughts and behaviors that lead to emotional difficulties and functional impairments.
What are harmful thoughts and behavioral patterns, which are not?
Harmful thoughts or behavioral habits can make people feel bad about themselves. There are helpful and unhelpful ways of reacting to a situation, often determined by how you think about them. For example: You see somebody you know on the street and say hello, but they do not say hello back. Your own reaction to that very much depends on how you assess the situation.
Another example is if your marriage has ended in divorce, you might think you’ve failed and that you’re not capable of having another meaningful relationship. This could lead to you feeling hopeless, lonely, depressed and tired, so you stop going out and meeting new people. You become trapped in a negative cycle, sitting at home alone and feeling bad about yourself. But rather than accepting this way of thinking you could accept that many marriages end, learn from your mistakes and move on, and feel optimistic about the future. This optimism could result in you becoming more socially active and you may start evening classes and develop a new circle of friends. This is a simplified example, but it illustrates how certain thoughts, feelings, physical sensations and actions can trap you in a negative cycle and even create new situations that make you feel worse about yourself.
CBT aims to stop negative cycles such as these by breaking down things that make you feel bad, anxious or scared. By making your problems more manageable, CBT can help you change your negative thought patterns and improve the way you feel.
CBT can help you get to a point where you can achieve this on your own and tackle problems without the help of a therapist.
| Reaction | Harmful | Neutral |
|---|---|---|
| Thoughts | “He ignored me – he doesn’t like me anymore.” | “He didn’t notice me – maybe he doesn’t feel well. I should give him a call and find out how he is doing.” |
| Feelings | Someone who thinks like this feels down, sad and rejected. | These thought patterns do not cause any negative feelings. |
| Behavior | The consequence of this thought is to avoid this person in the future, although the assumption could be completely false. | This thought is a prompt to get back in touch with the person to find out if everything is all right. |
How is cognitive behavioral therapy different from other psychotherapies?
Cognitive behavioral therapy is a problem-oriented strategy. CBT focuses on current problems and finding solutions for them. Unlike psychoanalysis, for example, it does not deal primarily with the past. Cognitive behavioral therapy is much more concerned with dealing with current problems. The most important thing is helping people to help themselves: They should be able to cope with their lives again without therapy as soon as possible. This does not mean that cognitive behavioral therapy completely ignores the influence of past events. But it mainly deals with identifying and changing current distressing thought and behavioral patterns.
Analytic psychotherapy, which has its origin in classic Freudian psychoanalysis, uses different methods. Here the therapist tries to help the patient discover and understand problems and their deeper causes.
CBT differs from many other psychotherapies because it is:
- pragmatic – it helps identify specific problems and tries to solve them
- highly structured – rather than talking freely about your life, you and your therapist discuss specific problems and set goals for you to achieve
- focused on current problems – it’s mainly concerned with how you think and act now rather than attempting to resolve past issues
- collaborative – your therapist will not tell you what to do; they’ll work with you to find solutions to your current difficulties
What are advantages and disadvantages of CBT?
Cognitive behavioral therapy (CBT) can be as effective as medicine in treating some mental health problems, but it may not be successful or suitable for everyone.
Some of the advantages of CBT include:
- CBT may be helpful in cases where medicine alone has not worked
- CBT can be completed in a relatively short period of time compared with other talking therapies
- The highly structured nature of CBT means it can be provided in different formats, including in groups, self-help books and online
- CBT teaches you useful and practical strategies that can be used in everyday life, even after the treatment has finished
Some of the disadvantages of CBT to consider include:
- You need to commit yourself to the process to get the most from it – a therapist can help and advise you, but they need your co-operation
- Attending regular CBT sessions and carrying out any extra work between sessions can take up a lot of your time
- CBT may not be suitable for people with more complex mental health needs or learning difficulties, as it requires structured sessions
- CBT involves confronting your emotions and anxieties – you may experience initial periods where you’re anxious or emotionally uncomfortable
- CBT focuses on the person’s capacity to change themselves (their thoughts, feelings and behaviours) – this does not address any wider problems in systems or families that often have a significant impact on someone’s health and wellbeing
Some critics also argue that because CBT only addresses current problems and focuses on specific issues, it does not address the possible underlying causes of mental health conditions, such as an unhappy childhood.
Is CBT different when used in Children vs. Adults?
Parental involvement in therapy is necessary when children receive CBT. Parents can ensure that their child engages in behavioral exercises between therapy sessions (e.g., in vivo exposures, pleasant activities), can change the child’s environment to promote more effective behaviors, and can help the child target changes in maladaptive thoughts. In general, CBT for children focuses more on behavior changes and less on cognitive changes. Cognitive behavioral therapy (CBT) is the only effective treatment for autism 7 and is an important adjunctive treatment for ADHD 8. In addition, CBT provides substantial benefits for children with depression or anxiety 9, 10.
How long does CBT take to work?
Your CBT program could be anywhere between 5 and 20 weeks, depending on your problem and the treatment program you and your therapist agree on.
When can CBT be combined with medications?
CBT can be used alone or in combination with medications for a variety of psychiatric disorders. Medications can be used to stabilize patients and promote recovery, whereas CBT can be used to encourage long-term changes in thoughts and behaviors.
CBT generally produces equivalent outcomes or provides additional benefits compared with the use of psychiatric medications alone 6. Moreover, CBT is often more cost-effective, has more enduring effects 11 and lacks the side effects associated with many psychiatric medications. The effects of CBT are reduced in patients who are receiving benzodiazepines 12; therefore, these medications should be avoided in patients with anxiety and trauma-related disorders. Although a combination of CBT and benzodiazepines may initially seem beneficial (e.g., reduced arousal, improved sleep), this approach may actually limit the gains made with CBT (e.g., patients may not be able to engage in exposure exercises when arousal is reduced as a result of medication use) 13, 14.
What are potential limitations of CBT?
CBT is most effective when patients complete therapeutic exercises outside of the treatment session; therefore, it requires a significant commitment from patients. Some of the therapeutic strategies may involve anxiety-eliciting stimuli, which can be distressing—although short-lived—for some patients. The structured nature of CBT is not a good fit for patients who are seeking insight into the underlying causes of their distress. Lastly, CBT is not a substitute for pharmacotherapy for some disorders. For example, CBT should be considered an adjunctive treatment in the management of bipolar disorder, psychotic disorders, and depression with psychotic features.
When doesn’t CBT work?
CBT may be difficult for people with learning difficulties and for those with complex mental health problems.
Also, CBT does not explore the underlying reasons for a person’s negative thoughts and unhelpful thought patterns — it focusses on improving the present problem.
How does cognitive behavioral therapy (CBT) work?
According to the cognitive behavioral model, psychopathology occurs because of problematic patterns in thinking and behavior that lead to difficult emotions and functional impairments (Figures 1 and 2). In CBT, you work with a therapist to recognize your patterns of thinking (cognition) and behavior that cause you problems. Then cognitive behavioral therapy teaches you practical ways to learn or re-learn more helpful and healthy habits. Basically, the aim of CBT is to help you adopt more adaptive patterns of thinking by challenging and breaking the habit of your negative thinking and behavior to improve your function and quality of your life.
CBT involves three core strategies applied alone or in combination, depending on the patients’ needs 3:
- Identifying and challenging problematic thoughts and beliefs, with the goal of helping patients develop more realistic and adaptive thoughts and beliefs,
- Scheduling pleasant activities to increase environmental reinforcement, and
- Extended exposure to unpleasant thoughts, situations, or physiologic sensations to decrease avoidance and arousal associated with anxiety-eliciting stimuli.
Negative and unhelpful thinking can show itself in different ways. Some examples are catastrophizing, where you always assume the worst possible outcome, and personalization, where you take everything personally.
CBT is a structured, didactic (intended to teach) and goal-oriented form of therapy — it focuses on goals and is specific to an individual. Cognitive behavioral therapy doesn’t look back over your past, it centers on solving your current problems. Most psychotherapists who practice CBT personalize and customize the therapy to the specific needs of each patient.
CBT often includes:
- Learning about your mental health condition
- Learning and practicing techniques such as relaxation, coping, resilience, stress management and assertiveness
In the 1960s, Aaron Beck developed cognitive behavior therapy (CBT) or cognitive therapy 15, 16, 17. Aaron Beck began to notice that his patients with depression often verbalized thoughts that were lacking in validity and noted characteristic “cognitive distortions” in their thinking. His empirical observations led him to start viewing depression not so much as a mood disorder but as a cognitive disorder. Based on his clinical observations and empirical findings, Beck outlined a new cognitive theory of depression. He published Cognitive Therapy for Depression 18 after having published a study that evaluated and demonstrated the efficacy of cognitive therapy. The combination of a detailed treatment protocol manual with outcome research was an innovation in psychotherapy practice that had only previously been attempted by behavior therapists in treating discrete behavioral problems. By accomplishing the same feat with a more complex set of clinical interventions that included cognitive, emotional, and behavioral components, Beck pioneered a model for what psychologists many years later defined as an “empirically validated psychological treatment.”
Other clinicians and researchers became interested and began developing CBT treatment protocols and evaluating their efficacy. Specific treatment protocols were developed for some psychiatric disorders. As behavioral strategies were incorporated, the term cognitive therapy changed to cognitive behavior therapy. Today CBT is the most extensively researched of all psychotherapies with several evidence-based treatment protocols.
Cognitive‐behavioral therapy (CBT) is founded in behavioral analysis and operant theory 19, cognitive theory 20 and social learning theory 21. Associations between cognitions, emotions, and behaviors are emphasized and are believed to interact to influence desired outcomes. Thus, cognitive‐behavioral therapy (CBT) is focused on altering maladaptive social/environmental, behavioral, and cognitive factors in order to reduce symptoms and prevent relapse.
Cognitive behavioral therapy (CBT) can help you make sense of overwhelming problems by breaking them down into smaller parts.
In CBT, problems are broken down into 5 main areas:
- Situations
- Thoughts
- Emotions
- Physical feelings
- Actions
CBT is based on the concept of these 5 areas being interconnected and affecting each other. For example, your thoughts about a certain situation can often affect how you feel both physically and emotionally, as well as how you act in response.
Cognitive Model
CBT is based on a straightforward, common-sense model of the relationships among cognition, emotion, and behavior 22, 23.
Three aspects of cognition are emphasized:
- Automatic thoughts
- Cognitive distortions
- Underlying beliefs or schemas
Automatic Thoughts
An individual’s immediate, unpremeditated interpretations of events are referred to as automatic thoughts. Automatic thoughts shape both the individual’s emotions and their actions in response to events. For example, a friend may cross you in the hallway and not say hello to you. If you were to have an automatic thought of “he hates me,” or “I have done something to anger him,” it is likely to impact your mood and cause you to feel upset and also to behave in an avoidant manner when you see him next. On the other hand, if you had the automatic thought, “he is in a hurry,” you would not be too concerned, and you would not be avoidant when you were to see him next.
CBT is based on the observation that dysfunctional automatic thoughts that are exaggerated, distorted, mistaken, or unrealistic in other ways, play a significant role in psychopathology.
Cognitive Distortions
Errors in logic are quite prevalent in patients with psychological disorders. They lead individuals to erroneous conclusions. Below are some cognitive distortions that are commonly seen in individuals with psychopathology:
- Dichotomous thinking: Things are seen regarding two mutually exclusive categories with no shades of gray in between.
- Overgeneralization: Taking isolated cases and using them to make wide generalizations.
- Selective abstraction: Focusing exclusively on certain, usually negative or upsetting, aspects of something while ignoring the rest.
- Disqualifying the positive: Positive experiences that conflict with the individual’s negative views are discounted.
- Mind reading: Assuming the thoughts and intentions of others.
- Fortune telling: Predicting how things will turn out before they happen.
- Minimization: Positive characteristics or experiences are treated as real but insignificant.
- Catastrophizing: Focusing on the worst possible outcome, however unlikely, or thinking that a situation is unbearable or impossible when it is just uncomfortable.
- Emotional reasoning: Making decisions and arguments based on how you feel rather than objective reality.
- “Should” statements: Concentrating on what you think “should” or “ought to be” rather than the actual situation you are faced with or having rigid rules which you always apply no matter the circumstances.
- Personalization, blame, or attribution: Assuming you are completely or directly responsible for a negative outcome. When applied to others consistently, the blame is the distortion.
Underlying Beliefs
Underlying beliefs shape the perception and interpretation of events. Belief systems or schemas take shape as we go through life experiences. They are defined as templates or rules for information processing that underlie the most superficial layer of automatic thoughts. Beliefs are understood at two levels in CBT:
Core Beliefs
- The central ideas about self and the world
- The most fundamental level of belief
- They are global, rigid, and overgeneralized
Examples of dysfunctional core beliefs:
- “I am unlovable”
- “I am inadequate”
- “The world is a hostile and dangerous place”
Intermediate Beliefs
- Consist of assumptions, attitudes, and rules
- Influenced in their development by the core beliefs
Examples of dysfunctional intermediate beliefs:
- “To be accepted, I should always please others.”
- “I should be excellent at everything I do to be considered adequate.”
- “It is best to have as little as possible to do with people.”
Common CBT Strategies
There are numerous techniques used in CBT, so the list below is by no means exhaustive. Depending on the needs of the particular client, cognitive behavioral therapy is likely to involve some of the following:
Responses to unhealthy thinking
- ‘Cognitive restructuring’ involves trying to re-evaluate the negative thinking patterns that maintain distorted beliefs about oneself, the world, and relating to others. For instance, a person with social phobia could be taught to challenge his or her assumption that social rejection is inevitable.
- Strategies to promote more effective problem solving and decision making are emphasized.
- ‘Mindfulness’ techniques help clients gain some distance from their negative thinking so they can recognize that thoughts do not have to determine behaviors.
Responses to unhealthy behaviors
- Clients are taught how to gradually start to re-enter situations they have been avoiding (e.g., because of fear in anxiety disorders, or low motivation in depression). This is not done in a coercive way; instead, clients learn how to gain a sense of control and predictability in situations that previously seemed overwhelming.
- Activities that provide a sense of pleasure or mastery are planned to promote a more enjoyable and fulfilling life.
- Training in new skills may be provided, such as how to communicate more effectively, be assertive, or enhance social interactions.
Responses to painful feelings
- Clients are sometimes taught how to work on accepting or tolerating painful emotions, and sometimes taught how to try to change those emotions in the moment.
- Relaxation exercises are often included to help reduce overall stress.
- Strategies to manage extreme emotional reactions are taught, such as ways to deal with intense anger or urges to harm oneself.
What can CBT help with?
Cognitive behavioral therapy is used to treat a wide range of issues. Cognitive behavioral therapy can help children, teenagers and adults with physical, emotional, psychological and psychiatric issues such as depression, anxiety disorders, alcohol and drug use problems, marital problems, eating disorders, and severe mental illness.
CBT is often the preferred type of psychotherapy because it can quickly help you identify and cope with specific challenges. Cognitive behavioral therapy generally requires fewer sessions than other types of therapy and is done in a structured way.
CBT has also been shown to help people with 24, 25, 26, 27:
- Anxiety disorders like generalized anxiety disorder, panic disorder, social anxiety disorder, health anxiety and phobias
- Autism
- Obsessive-compulsive disorder (OCD)
- Post-traumatic stress disorder (PTSD)
- Depression 28
- Bipolar disorders 29
- Eating disorders
- Relationship issues
- Anger and stress
- Personality disorders 30
- Problem gambling
- Phobias
- Psychosis 11
- Sexual disorders
- Sleep disorders 31
- Substance abuse or substance use disorders
- Schizophrenia
- Tic disorders
CBT can also help people with physical problems, such as:
- Chronic pain 32
- Fibromyalgia
- Migraines
- Chronic fatigue syndrome
- Insomnia 31
- Irritable bowel syndrome (IBS)
- Tinnitus 33
CBT may help you:
- Manage symptoms of mental illness
- Prevent a relapse of mental illness symptoms
- Treat a mental illness when medications aren’t a good option
- Learn techniques for coping with stressful life situations
- Identify ways to manage emotions
- Resolve relationship conflicts and learn better ways to communicate
- Cope with grief or loss
- Overcome emotional trauma related to abuse or violence
- Cope with a medical illness
- Manage chronic physical symptoms
CBT effectively targets symptoms of anxiety 34, 9, 35, 36, depression 4, 5, 10, PTSD 37, 38, ADHD 8, 39, autism 7, 40, obsessive-compulsive disorder (OCD) and tic disorders 41, personality disorders 42, 30, eating disorders 43 and insomnia 31 in children, adolescents, and adults. Numerous meta-analyses and reviews have demonstrated that CBT reduces psychiatric symptoms and functional impairments, and improves quality of life 6. The American Psychological Association lists CBT as an effective treatment for numerous disorders 44. Moreover, CBT has been shown to be as effective as or more effective than medications for depression, anxiety, and trauma-related disorders 11 and it is a useful adjunctive therapy for disorders such as ADHD, schizophrenia, and bipolar disorder 11.
Cognitive behavioral therapy for ADHD
A recent review showed that behavioral parent training, behavioral classroom management, and behavioral peer interventions are well-established treatments for ADHD 39. Behavioral parent training and behavioral classroom management focus on strategies implemented by adults to help children with ADHD function more effectively, including creating structure and routines, setting clear rules and expectations, using effective commands, and rewarding or punishing the child based on his or her compliance. These techniques help reduce behavioral problems experienced by children with ADHD and decrease the need for polypharmacy to manage symptoms 39.
Cognitive behavioral therapy for autism
Early intensive behavioral interventions are the only evidence-based treatment that confers significant benefits in children with autism 7. These interventions should be initiated before three years of age and often consist of 12 to 40 hours of intensive treatment per week, for at least one year. Parents and therapists engage in intensive exercises focused on reinforcing and rewarding adaptive behaviors. Behavioral treatments for autism produce significant improvements in IQ and adaptive behaviors 40.
What are the stages of CBT?
- First you will work with your therapist to understand what are the most troubling problems for you.
- Then you work out what your thoughts, emotions and beliefs are about these situations.
- You will identify which of these thoughts, emotions and beliefs are negative or inaccurate.
- Working with your therapist, you find ways to challenge them. You might ask yourself: is that true? Or you might ask yourself: so what?
- You then also identify what behaviors are you doing based on these negative beliefs that you could change.
- Then you can find ways to think and act that are less harmful to you.
Who can provide CBT?
Psychologists, psychiatrists, some family doctors with training in mental health, mental health nurses, some counselors and other therapists may provide CBT.
- Psychologists. Psychologists have doctoral degrees (Ph.D., Ed.D., Psy.D.) from graduate programs approved by the American Psychological Association and the Canadian Psychological Association. Clinical psychologists also have a one-year clinical internship, and one to two years of supervised postdoctoral experience is generally required to receive a license. Licensing or certification procedures vary and are the responsibility of state or provincial governing bodies.
- Clinical Social Workers. A clinical social worker must have a college degree plus at least two years of graduate training in a program accredited by the Council on Social Work Education. Certified social workers have a master’s or doctoral degree in Social Work (MSW, DSW, or Ph.D.) from a program approved by the Council on Social Work Education, have had two years of post-degree experience in the practice of social work, and must have passed an examination given by the Academy of Certified Social Workers (ACSW). Licensing procedures vary from state to state and province to province.
- Psychiatrists. A Psychiatrist must have a medical degree. Although, technically, an individual can practice psychiatry having had four years of medical school and a one-year medical internship, most psychiatrists continue their training in a five-year residency program in psychiatry. Psychiatrists who have Board certification have had two years of post-residency experience practicing psychiatry and must have passed an examination given by the American Board of Psychiatry and Neurology. But please note that the board certification for psychiatrists does not include any specifics about their training in or knowledge of CBT.
- Professional Counselors. Professional counselors usually have master’s (M.E.D., M.A.E., M.A., or M.S.), specialist (Ed.S.), or doctoral (Ph.D. or Ed.D.) degrees from an accredited university. Certified counselors typically have graduate training in counseling, and must have passed an examination given by the National Board of Certified Counselors. Licensing procedures vary from state to state and province to province.
CBT can be conducted in private or group sessions — it may be in person or via telehealth or be an online course/ online (e-therapy). Your doctor can refer you to a CBT therapist, or help you find a counsellor or psychologist experienced in it.
There are several online CBT programs (some free) that you can access or that your doctor can refer you to, including Moodgym (https://moodgym.com.au). Moodgym is an online self-help program designed to help users prevent and manage symptoms of depression and anxiety. Moodgym is like an interactive, online self-help book which teaches skills based on cognitive behavior therapy (CBT). You can log back in to at any time to learn more skills or to add to your workbooks and diaries.
What can I expect from CBT?
CBT helps you to understand how your thinking affects your mood and behavior. You’ll learn skills that will help with your current problems and that you can apply to future problems. Cognitive behavioral therapy relies on a close professional relationship with your therapist. They will help you to recognize the difference between helpful and unhelpful thoughts, and teach you how to challenge and let go of the unhelpful thoughts.
Cognitive behavioral therapy may be done one-on-one or in groups with family members or with people who have similar issues. Online resources are available that may make participating in CBT possible, especially if you live in an area with few local mental health resources.
CBT is structured and usually has a set end point.
Therapy sessions tend to be relatively structured, meaning that an agenda is set to make sure that certain material is covered in each session. The session always starts with a brief update and check on mood. This is followed by bridging from the previous session to establish continuity. The agenda of what will be talked about in the session is set up collaboratively, and the homework the patient had to do between the sessions is reviewed before plunging into talking about any problem. Issues on the agenda are talked about punctuated with feedback and summaries. The session ends with setting up further homework and a final summary.
CBT usually involves a session lasting an hour once a week. In addition, there is usually some homework to do between sessions. You’ll work with your therapist to set some tasks to practise what you talk about. CBT can be used at the same time as relaxation techniques, breathing techniques, medication or supportive counseling.
Examples of CBT in practice:
- CBT for Anxiety: CBT often focuses on replacing negative automatic thoughts that can occur in generalized anxiety disorder and may be used alone or in combination with medications such as selective serotonin reuptake inhibitors, which are typically first-line as benzodiazepines have a greater risk of adverse outcomes. In treating panic disorder, CBT may include desensitization to triggers that provoke anxiety; it is important to note, however, that a potential adverse effect of this technique is a temporary mild increase in anxiety 45.
- CBT for Depression: In patients with chronic depression, the combination of CBT and antidepressant medication is more effective than either intervention alone. In patients who are no longer taking part in activities that typically bring them pleasure, CBT may initially focus on reinitiating positive activities to overcome inertia 46.
- CBT for Attention Deficit Hyperactivity Disorder (ADHD): Cognitive behavioral therapy is the initial recommended treatment for children younger than 6 years old, while stimulant medications are the recommended initial intervention for ADHD in children 6 years and older. Behavioral treatments are also recommended for older children, especially if they have a poor response or adverse effects on medication. Cognitive behavioral therapy interventions include parent training and behavioral classroom management with a focus on setting clear rules and expectations for the child with appropriate rewards and punishments and daily feedback 47.
Typical CBT treatments involve approximately 60-minute sessions occurring weekly for 8 to 12 weeks 47.
CBT therapy preparation
You might decide on your own that you want to try cognitive behavioral therapy. Or a doctor or someone else may suggest CBT to you. Here’s how to get started:
- Find a therapist. You can get a referral from a doctor, health insurance plan, friend or other trusted source. Many employers offer counseling services or referrals through employee assistance programs. Or you can find a therapist on your own — for instance, through a local or state psychological association or by searching the internet.
- Association for Behavioral and Cognitive Therapies (https://www.abct.org)
- National Association of Cognitive-Behavioral Therapists (https://www.nacbt.org)
- Academy of Cognitive & Behavioral Therapies (https://www.academyofct.org)
- American Psychological Association – Therapist locator (https://locator.apa.org)
- Understand the costs. If you have health insurance, find out what coverage it offers for psychotherapy. Some health plans cover only a certain number of therapy sessions a year. Also, talk to your therapist about fees and payment options. You will want to know:
- How much does the therapist charge per session?
- Does the therapist charge according to income (sliding scale)?
- Does the therapist charge for the initial session? (Since many therapists do charge for the initial session, you should get this information before your first visit.)
- Is there a policy concerning vacations and missed or canceled sessions? Is there a charge?
- Will your health insurance cover you if you see this therapist?
- Will the therapist want you to pay after each session, or will you be billed periodically?
- Review your concerns. Before your first appointment, think about what issues you’d like to work on. While you can also sort this out with your therapist, having some sense in advance may provide a starting point.
Check your therapist qualifications
Psychotherapist is a general term, rather than a job title or indication of education, training or licensure. Examples of psychotherapists include psychiatrists, psychologists, licensed professional counselors, licensed social workers, licensed marriage and family therapists, psychiatric nurses, or other licensed professionals with mental health training.
Before seeing a psychotherapist, check his or her:
- Background and education. Trained psychotherapists can have a number of different job titles, depending on their education and role. Most have a master’s or doctoral degree with specific training in psychological counseling. Medical doctors who specialize in mental health (psychiatrists) can prescribe medications as well as provide psychotherapy.
- Certification and licensing. Make sure that the therapist you choose meets state certification and licensing requirements for his or her particular discipline.
- Area of expertise. Ask whether the therapist has expertise and experience treating your symptoms or your area of concern, such as eating disorders or PTSD.
The key is to find a skilled therapist who can match the type and intensity of therapy with your needs.
Your first CBT therapy session
At your first session, your therapist will typically gather information about you and ask what concerns you’d like to work on. The therapist will likely ask you about your current and past physical and emotional health to gain a deeper understanding of your situation. Your therapist may discuss whether you might benefit from other treatment as well, such as medications.
The first session is also an opportunity for you to interview your therapist to see if he or she will be a good match for you. Make sure you understand:
- His or her approach
- What type of therapy is appropriate for you
- The goals of your treatment
- The length of each session
- How many therapy sessions you may need
It might take a few sessions for your therapist to fully understand your situation and concerns, and to determine the best course of action. If you don’t feel comfortable with the first therapist you see, try someone else. Having a good “fit” with your therapist can help you get the most benefit from CBT.
Confidentiality
Except in very specific circumstances, conversations with your therapist are confidential. However, a therapist may break confidentiality if there is an immediate threat to safety or when required by state or federal law to report concerns to authorities. These situations include:
- Threatening to immediately or soon (imminently) harm yourself or take your own life
- Threatening to imminently harm or take the life of another person
- Abusing a child or a vulnerable adult ― someone over age 18 who is hospitalized or made vulnerable by a disability
- Being unable to safely care for yourself
During CBT therapy
Your therapist will encourage you to talk about your thoughts and feelings and what’s troubling you. Don’t worry if you find it hard to open up about your feelings. Your therapist can help you gain more confidence and comfort.
CBT generally focuses on specific problems, using a goal-oriented approach. As you go through the therapy process, your therapist may ask you to do homework — activities, reading or practices that build on what you learn during your regular therapy sessions — and encourage you to apply what you’re learning in your daily life.
Your therapist’s approach will depend on your particular situation and preferences. Your therapist may combine CBT with another therapeutic approach — for example, interpersonal therapy, which focuses on your relationships with other people.
Steps in CBT
CBT typically includes these steps:
- Identifying troubling situations or conditions in your life. These may include such issues as a medical condition, divorce, grief, anger or symptoms of a mental health disorder. You and your therapist may spend some time deciding what problems and goals you want to focus on.
- Becoming aware of your thoughts, emotions and beliefs about these problems. Once you’ve identified the problems to work on, your therapist will encourage you to share your thoughts about them. This may include observing what you tell yourself about an experience (self-talk), your interpretation of the meaning of a situation, and your beliefs about yourself, other people and events. Your therapist may suggest that you keep a journal of your thoughts.
- Identifying your negative or inaccurate thinking. To help you recognize patterns of thinking and behavior that may be contributing to your problem, your therapist may ask you to pay attention to your physical, emotional and behavioral responses in different situations.
- Reshaping your negative or inaccurate thinking. Your therapist will likely encourage you to ask yourself whether your view of a situation is based on fact or on an inaccurate perception of what’s going on. This step can be difficult. You may have long-standing ways of thinking about your life and yourself. With practice, helpful thinking and behavior patterns will become a habit and won’t take as much effort.
Duration of CBT therapy
CBT is generally considered short-term therapy — ranging from about five to 20 sessions. You and your therapist can discuss how many sessions may be right for you. Factors to consider include:
- Type of disorder or situation
- Severity of your symptoms
- How long you’ve had your symptoms or have been dealing with your situation
- How quickly you make progress
- How much stress you’re experiencing
- How much support you receive from family members and other people
What are risks of cognitive behavioral therapy (CBT)?
In general, there’s little risk or side effects in having cognitive behavioral therapy. But you may feel emotionally uncomfortable at times. This is because CBT can cause you to explore or confront painful feelings, emotions and experiences. You may cry, get upset or feel angry during a challenging session. You may also feel physically drained. It is crucial to speak openly with your psychotherapist if any difficulties come up during therapy.
Some forms of CBT, such as exposure therapy, may require you to confront situations you’d rather avoid — such as airplanes if you have a fear of flying. This can lead to temporary stress or anxiety.
Furthermore, hardly any research has been done on possible side effects of psychotherapy. However, working with a skilled therapist will minimize any risks. The coping skills you learn can help you manage and conquer negative feelings and fears.
How effective is cognitive behavioral therapy (CBT)?
Cognitive behavioral therapy may not cure your condition or make an unpleasant situation go away. But it can give you the power to cope with your situation in a healthy way and to feel better about yourself and your life.
Cognitive behavioral therapy requires the patient’s commitment and own initiative. CBT can only be successful if the patient actively takes part in the treatment and also works on their problems between sessions. This can be a considerable challenge, especially with severe conditions such as depression or anxiety disorders. That is why medication is sometimes used at first to quickly relieve the worst symptoms so that psychotherapy can be started.
It is also important that you and your psychotherapist have a close and trusting working relationship. It can sometimes take a while to find the right therapist.
Choosing a certain kind of psychotherapy also depends on your goals. If you feel the need for deep insight into the causes of your problems, cognitive behavioral therapy is probably not the right choice. It is particularly useful if you are mainly interested in tackling specific problems and are only secondarily concerned with the “why.”
CBT isn’t effective for everyone. But you can take steps to get the most out of your therapy and help make it a success.
- Approach therapy as a partnership. Therapy is most effective when you’re an active participant and share in decision-making. Make sure you and your therapist agree about the major issues and how to tackle them. Together, you can set goals and assess progress over time.
- Be open and honest. Success with therapy depends on your willingness to share your thoughts, feelings and experiences, and on being open to new insights and ways of doing things. If you’re reluctant to talk about certain things because of painful emotions, embarrassment or fears about your therapist’s reaction, let your therapist know about your reservations.
- Stick to your treatment plan. If you feel down or lack motivation, it may be tempting to skip therapy sessions. Doing so can disrupt your progress. Attend all sessions and give some thought to what you want to discuss.
- Don’t expect instant results. Working on emotional issues can be painful and often requires hard work. It’s not uncommon to feel worse during the initial part of therapy as you begin to confront past and current conflicts. You may need several sessions before you begin to see improvement.
- Do your homework between sessions. If your therapist asks you to read, keep a journal or do other activities outside of your regular therapy sessions, follow through. Doing these homework assignments will help you apply what you’ve learned in the therapy sessions.
- If CBT therapy isn’t helping, talk to your therapist. If you don’t feel that you’re benefiting from CBT after several sessions, talk to your therapist about it. You and your therapist may decide to make some changes or try a different approach.
What to do if you are dissatisfied with your therapist
- Talk with your therapist. People can feel angry or frustrated at times about their therapy. If you do, you should discuss these concerns, dissatisfactions, and questions with the therapist. A good therapist will be open to hearing them and discuss your dissatisfaction with you.
- Get a Second Opinion. If you feel that the issues and problems you have raised with your therapist are not being resolved, you may want to consider asking for a consultation with another professional. Usually the therapist you are seeing can suggest someone you can consult. If your therapist objects to your consulting another professional, you should change to another therapist who will not object.
- Consider changing therapists. Many people feel that it is never acceptable to change therapists once therapy has begun. This is simply not true. Good therapists realize that they might not be appropriate for every person.
The most important thing you need to ask yourself when deciding to continue with a particular therapist is, “Am I changing in the direction I want to change?” If you do not feel that you are improving, and if, after discussing this with your therapist, it does not appear likely to you that you will improve with this therapist, you should consult another therapist.
- What is Cognitive Behavioral Therapy? https://www.apa.org/ptsd-guideline/patients-and-families/cognitive-behavioral[↩]
- InformedHealth.org [Internet]. Cologne, Germany: Institute for Quality and Efficiency in Health Care (IQWiG); 2006-. Cognitive behavioral therapy. 2013 Aug 7 [Updated 2016 Sep 8]. Available from: https://www.ncbi.nlm.nih.gov/books/NBK279297[↩][↩]
- Beck JS. Cognitive Behavior Therapy: Basics and Beyond. 2nd ed. New York, NY: Guilford Press; 2011.[↩][↩]
- Dobson KS, Hollon SD, Dimidjian S, et al. Randomized trial of behavioral activation, cognitive therapy, and antidepressant medication in the prevention of relapse and recurrence in major depression. J Consult Clin Psychol. 2008;76(3):468–477.[↩][↩]
- Mazzucchelli T, Kane R, Rees C. Behavioral activation treatments for depression in adults: a meta-analysis and review. Clin Psychol Sci Pract. 2009;16(4):383–411.[↩][↩]
- Common Questions About Cognitive Behavior Therapy for Psychiatric Disorders. Am Fam Physician. 2015 Nov 1;92(9):807-812. https://www.aafp.org/afp/2015/1101/p807.html[↩][↩][↩]
- Eldevik S, Hastings RP, Hughes JC, Jahr E, Eikeseth S, Cross S. Meta-analysis of early intensive behavioral intervention for children with autism. J Clin Child Adolesc Psychol. 2009;38(3):439–450.[↩][↩][↩]
- Daley D, van der Oord S, Ferrin M, et al.; European ADHD Guidelines Group. Behavioral interventions in attention-deficit/hyperactivity disorder: a meta-analysis of randomized controlled trials across multiple outcome domains. J Am Acad Child Adolesc Psychiatry. 2014;53(8):835–847, 847.e1–847.e5.[↩][↩]
- Reynolds S, Wilson C, Austin J, Hooper L. Effects of psychotherapy for anxiety in children and adolescents: a meta-analytic review. Clin Psychol Rev. 2012;32(4):251–262.[↩][↩]
- Klein JB, Jacobs RH, Reinecke MA. Cognitive-behavioral therapy for adolescent depression: a meta-analytic investigation of changes in effect-size estimates. J Am Acad Child Adolesc Psychiatry. 2007;46(11):1403–1413.[↩][↩]
- Turner DT, van der Gaag M, Karyotaki E, Cuijpers P. Psychological interventions for psychosis: a meta-analysis of comparative outcome studies. Am J Psychiatry. 2014;171(5):523–538.[↩][↩][↩][↩]
- Pilling S, Mayo-Wilson E, Mavranezouli I, Kew K, Taylor C, Clark DM; Guideline Development Group. Recognition, assessment and treatment of social anxiety disorder: summary of NICE guidance. BMJ. 2013;346:f2541.[↩]
- Otto MW, Smits JA, Reese HE. Combined psychotherapy and pharmacotherapy for mood and anxiety disorders in adults: review and analysis. Clin Psychol Sci Pract. 2005;12(1):72–86.[↩]
- World Health Organization. Guidelines for the management of conditions specifically related to stress. http://apps.who.int/iris/bitstream/handle/10665/85119/9789241505406_eng.pdf[↩]
- BECK AT. THINKING AND DEPRESSION. I. IDIOSYNCRATIC CONTENT AND COGNITIVE DISTORTIONS. Arch Gen Psychiatry. 1963 Oct;9:324-33. doi: 10.1001/archpsyc.1963.01720160014002[↩]
- BECK AT. THINKING AND DEPRESSION. II. THEORY AND THERAPY. Arch Gen Psychiatry. 1964 Jun;10:561-71. doi: 10.1001/archpsyc.1964.01720240015003[↩]
- Beck AT. Cognitive therapy and the emotional disorders. New York, NY: International Universities Press; 1976.[↩]
- Beck AT, Rush AJ, Shaw BF, Emery G. Cognitive therapy of depression. New York, NY: Guilford Press; 1979.[↩]
- Bergin AE. Individual psychotherapy and behavior therapy. Annu Rev Psychol. 1975;26:509-56. doi: 10.1146/annurev.ps.26.020175.002453[↩]
- Beck AR, Rush AJ, Shaw B, Emery G. Cognitive Therapy of Depression. New York: Guilford Press, 1979.[↩]
- Bandura A. Social Learning Theory. New Jersey: Prentice-Hall, 1977.[↩]
- Heenan A, Pipe A, Lemay K, Davidson JR, Tulloch H. Cognitive-Behavioral Therapy for Insomnia Tailored to Patients With Cardiovascular Disease: A Pre-Post Study. Behav Sleep Med. 2020 May-Jun;18(3):372-385. doi: 10.1080/15402002.2019.1594815[↩]
- de Jonge M, Bockting CLH, Kikkert MJ, van Dijk MK, van Schaik DJF, Peen J, Hollon SD, Dekker JJM. Preventive cognitive therapy versus care as usual in cognitive behavioral therapy responders: A randomized controlled trial. J Consult Clin Psychol. 2019 Jun;87(6):521-529. doi: 10.1037/ccp0000395[↩]
- van den Berk Clark, C., Moore, R., Secrest, S., Tuerk, P., Norman, S., Myers, U., Lustman, P. J., Schneider, F. D., Barnes, J., Gallamore, R., Ovais, M., Plurad, J. A., & Scherrer, J. F. (2019). Factors Associated With Receipt of Cognitive-Behavioral Therapy or Prolonged Exposure Therapy Among Individuals With PTSD. Psychiatric services (Washington, D.C.), 70(8), 703–713. https://doi.org/10.1176/appi.ps.201800408[↩]
- Zilcha-Mano, S., Eubanks, C. F., & Muran, J. C. (2019). Sudden gains in the alliance in cognitive behavioral therapy versus brief relational therapy. Journal of consulting and clinical psychology, 87(6), 501–509. https://doi.org/10.1037/ccp0000397[↩]
- Keefe JR, Chambless DL, Barber JP, Milrod BL. Treatment of anxiety and mood comorbidities in cognitive-behavioral and psychodynamic therapies for panic disorder. J Psychiatr Res. 2019 Jul;114:34-40. doi: 10.1016/j.jpsychires.2019.04.009[↩]
- Fact Sheets of ABCT. https://www.abct.org/fact-sheets[↩]
- Dimidjian S, Hollon SD, Dobson KS, et al. Randomized trial of behavioral activation, cognitive therapy, and antidepressant medication in the acute treatment of adults with major depression. J Consult Clin Psychol. 2006;74(4):658–670.[↩]
- Miklowitz DJ, Scott J. Psychosocial treatments for bipolar disorder: cost-effectiveness, mediating mechanisms, and future directions. Bipolar Disord. 2009;11(suppl 2):110–122.[↩]
- Matusiewicz AK, Hopwood CJ, Banducci AN, Lejuez CW. The effectiveness of cognitive behavioral therapy for personality disorders. Psychiatr Clin North Am. 2010;33(3):657–685.[↩][↩]
- Okajima I, Komada Y, Inoue Y. A meta-analysis on the treatment effectiveness of cognitive behavioral therapy for primary insomnia. Sleep Biol Rhythms. 2011;9(1):24–34.[↩][↩][↩]
- Taguchi, K., Numata, N., Takanashi, R., Takemura, R., Yoshida, T., Kutsuzawa, K., Yoshimura, K., & Shimizu, E. (2021). Integrated cognitive behavioral therapy for chronic pain: An open-labeled prospective single-arm trial. Medicine, 100(6), e23859. https://doi.org/10.1097/MD.0000000000023859[↩]
- Fuller, T., Cima, R., Langguth, B., Mazurek, B., Vlaeyen, J. W., & Hoare, D. J. (2020). Cognitive behavioural therapy for tinnitus. The Cochrane database of systematic reviews, 1(1), CD012614. https://doi.org/10.1002/14651858.CD012614.pub2[↩]
- Cuijpers P, Sijbrandij M, Koole S, Huibers M, Berking M, Andersson G. Psychological treatment of generalized anxiety disorder: a meta-analysis. Clin Psychol Rev. 2014;34(2):130–140.[↩]
- Sánchez-Meca J, Rosa-Alcázar AI, Marín-Martínez F, Gómez-Conesa A. Psychological treatment of panic disorder with or without agoraphobia: a meta-analysis [published correction appears in Clin Psychol Rev. 2010;30(6):815–817]. Clin Psychol Rev. 2010;30(1):37–50.[↩]
- Hofmann SG, Smits JA. Cognitive-behavioral therapy for adult anxiety disorders: a meta-analysis of randomized placebo-controlled trials. J Clin Psychiatry. 2008;69(4):621–632.[↩]
- Powers MB, Halpern JM, Ferenschak MP, Gillihan SJ, Foa EB. A meta-analytic review of prolonged exposure for posttraumatic stress disorder. Clin Psychol Rev. 2010;30(6):635–641.[↩]
- Le QA, Doctor JN, Zoellner LA, Feeny NC. Cost-effectiveness of prolonged exposure therapy versus pharmacotherapy and treatment choice in posttraumatic stress disorder (the Optimizing PTSD Treatment Trial): a doubly randomized preference trial. J Clin Psychiatry. 2014;75(3):222–230.[↩]
- Evans SW, Owens JS, Bunford N. Evidence-based psychosocial treatments for children and adolescents with attention-deficit/hyperactivity disorder. J Clin Child Adolesc Psychol. 2014;43(4):527–551.[↩][↩][↩]
- Rogers SJ, Vismara LA. Evidence-based comprehensive treatments for early autism. J Clin Child Adolesc Psychol. 2008;37(1):8–38.[↩][↩]
- Rosa-Alcázar AI, Sánchez-Meca J, Gómez-Conesa A, Marín-Martínez F. Psychological treatment of obsessive-compulsive disorder: a meta-analysis. Clin Psychol Rev. 2008;28(8):1310–1325.[↩]
- Lynch TR, Trost WT, Salsman N, Linehan MM. Dialectical behavior therapy for borderline personality disorder. Annu Rev Clin Psychol. 2007;3:181–205.[↩]
- Keel PK, Haedt A. Evidence-based psychosocial treatments for eating problems and eating disorders. J Clin Child Adolesc Psychol. 2008;37(1):39–61.[↩]
- American Psychological Association, Society of Clinical Psychology. Psychological treatments. https://div12.org/psychological-treatments/treatments[↩]
- Locke AB, Kirst N, Shultz CG. Diagnosis and management of generalized anxiety disorder and panic disorder in adults. Am Fam Physician. 2015 May 1;91(9):617-24. https://www.aafp.org/afp/2015/0501/p617.html[↩]
- Rupke SJ, Blecke D, Renfrow M. Cognitive therapy for depression. Am Fam Physician. 2006 Jan 1;73(1):83-6. https://www.aafp.org/afp/2006/0101/p83.html[↩]
- Coffey SF, Banducci AN, Vinci C. Common Questions About Cognitive Behavior Therapy for Psychiatric Disorders. Am Fam Physician. 2015 Nov 1;92(9):807-12. https://www.aafp.org/afp/2015/1101/p807.html[↩][↩]