Contents
Dry hands causes
Dry hands refers to skin that feels dry to touch (xerosis), is a condition of rough, dry skin with fine scaling of skin and, occasionally, with small cracks in the skin. Dry hands is lacking moisture in the outer horny cell layer (stratum corneum) and this results in cracks in the skin surface. Dry skin is also called xerosis or xeroderma or winter itch or asteatosis (lack of fat). Xerosis can affect the skin on any part of the body but commonly occurs on the lower legs, arms, scalp and hands. Constant scratching and rubbing can cause the skin to become thick and leathery. Xerosis can look like dry, rough patches of skin with cracks, flaking and peeling. The skin can be red and itchy.
Dry hands is a common condition which occurs when the outer layer of the skin becomes dehydrated. The skin loses its suppleness and small splits and/or cracks appear, followed by flaking or scales. The skin can become red and itchy. Dry hands affects males and females equally and tends to occur in older people more frequently. There is some racial variability in water and lipid content of the skin.
Often itchy, dry hands is caused by environmental factors, such as cold weather and frequent bathing, and by medical conditions, such as atopic dermatitis and malnutrition. Dry hands develops due to a decrease in the natural oils in the outer layer of skin, which makes the skin lose water.
Extremely dry skin can be a warning sign of a skin problem called dermatitis. Dermatitis means inflammation of the skin. It can cause an itchy rash or patches of dry irritated skin. The earlier dermatitis is diagnosed and treated the better. Without treatment, dermatitis often gets worse.
Atopic dermatitis (eczema) is a disorder associated with dry skin, which begins with intense itching that is aggravated by scratching. The exact cause of atopic dermatitis (eczema) is unknown, and there is no known cure.
- Atopic dermatitis (eczema) is a condition primarily affecting allergy-prone people.
- Heat, humidity, detergents/soaps, abrasive clothing (e.g., very scratchy wools), chemicals, smoke, as well as stress may trigger eczema.
- Scratching increases the chances of developing a superimposed infection because it produces breaks in the skin.
What causes dry hands
Dry hands occurs when the skin loses moisture. Dry hands is common in winter when the cold air outside and the heated air inside creates a low relative humidity.
- Bathing or hand washing too frequently can contribute to dry hands especially if one uses harsh soaps.
- Dry hands that starts in early childhood may be one of about 20 types of ichthyosis (fish-scale skin). There is often a family history of dry skin.
- Dry skin is commonly seen in people with atopic dermatitis.
- Nearly everyone > 60 years has dry skin.
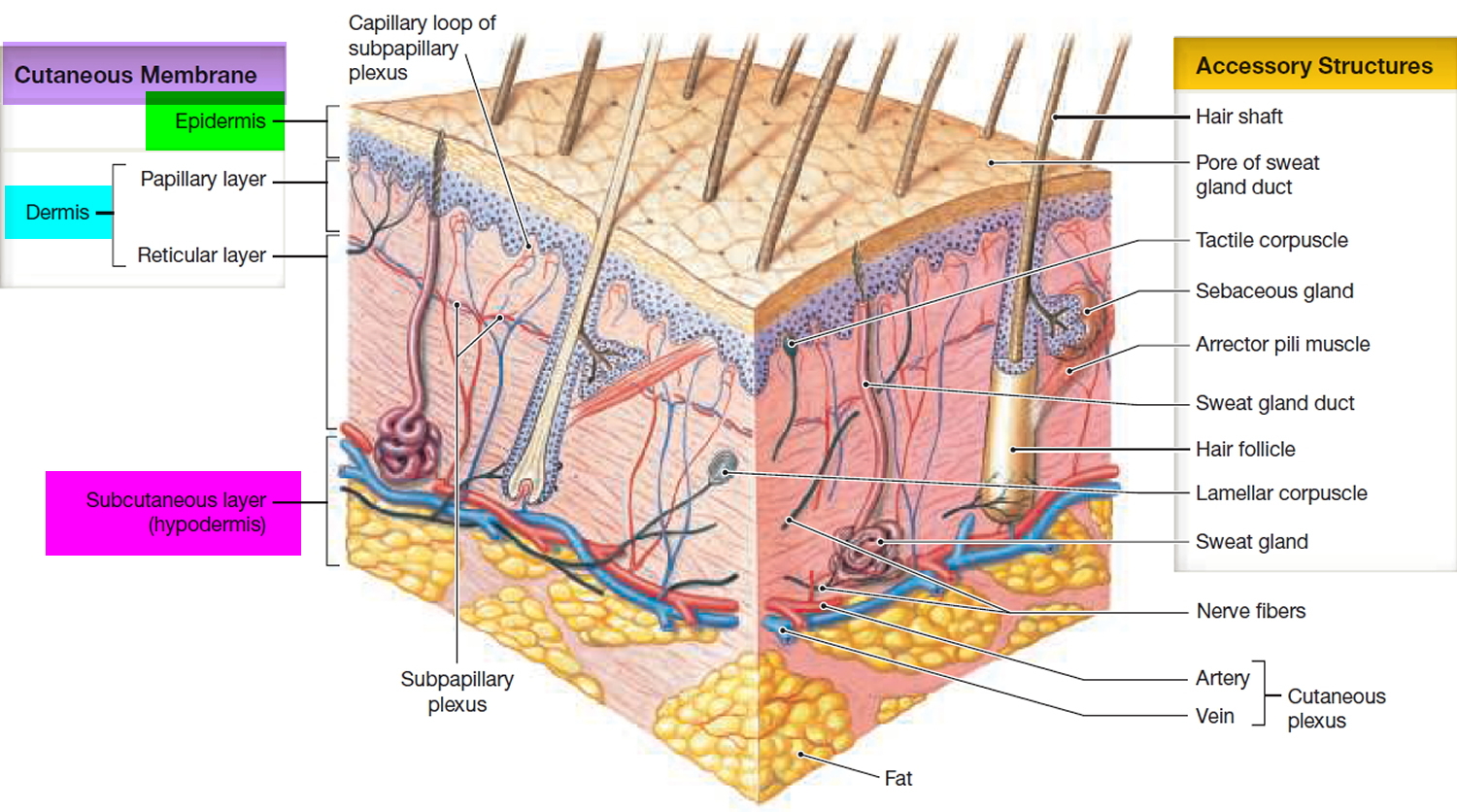
Figure 1. Skin structure
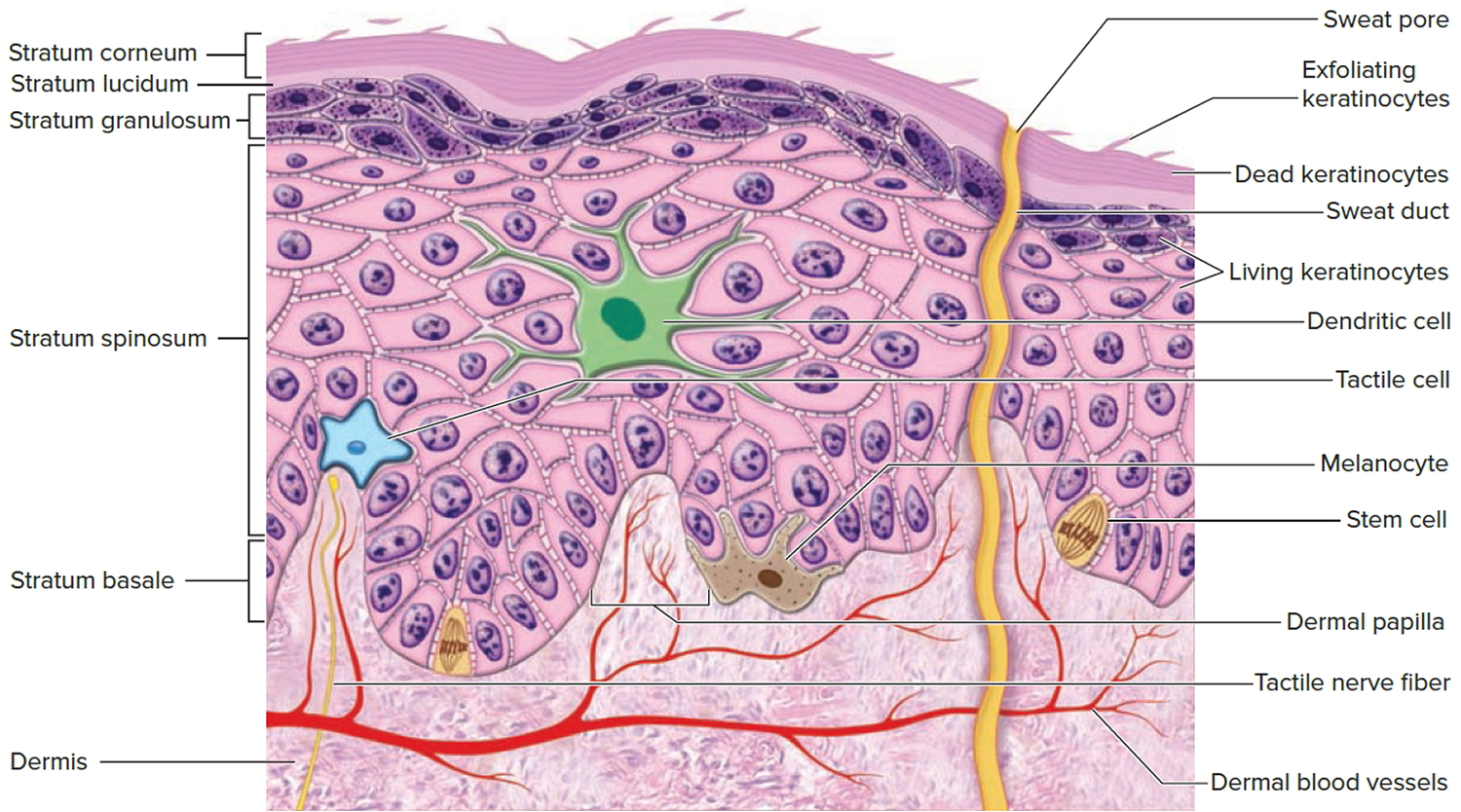
Figure 2. Structure and skin cells of the Epidermis
What factors contribute to skin dryness?
Dry skin can be seen in people of any age, of any race, and of either gender. However, the incidence of dry skin increases with age; nearly all individuals over the age of 60 have some degree of dry skin.
- Age: Increasing age and menopause can be associated with a natural reduction of skin moisture. As you age, your skin becomes thinner and drier. By your 40s, many people need to use a good moisturizer every day.
- Genetic factors: ichthyosis (fish-scale skin)
- Skin problems: atopic dermatitis (also called eczema) and psoriasis. People who had atopic dermatitis (eczema) as a child tend to have dry skin as adults.
- Medical conditions:
- Diabetes
- Hypothyroidism
- Down syndrome
- Liver or kidney disease
- Malnutrition
- HIV/AIDS
- Lymphoma
- Medications: diuretics, cholesterol lowering drugs, retinoids
- Environmental factors:
- Cold and windy weather, dry climate
- Long hot showers or baths
- Excessive hand washing
- Contact with harsh irritants such as harsh soaps or detergents
- Air-conditioning and heating
- Sun exposure and sun damage.
- Job: Nurses, hair stylists, and people in other occupations often immerse their skin in water throughout the day. This can cause the skin to become dry, raw, and cracked.
- Swimming: Some pools have high levels of chlorine, which can dry the skin.
Signs and symptoms of dry skin
The most common locations for dry skin include:
- Legs, especially the fronts of the lower legs (shins)
- Arms
- Trunk, especially the side areas between the bottom rib and the hip (flanks)
- Backs of the hands
Symptoms of dry skin include:
- Scaling, flaking, or peeling skin
- Skin that feels rough
- Skin tightness, especially after bathing
- Itching
- Cracks in the skin that may bleed
Dry skin appears as dull, rough skin with fine scales that flake off easily. In more advanced stages of dry skin, the skin may have cracks that resemble a dry lake bed. When dry skin cracks, germs can get in through the skin. Once inside, germs can cause an infection. Red, sore spots on the skin may be an early sign of an infection. Inflammation of the areas may lead to pink or red patches.
Dry skin can be completely without symptoms (asymptomatic), though more inflamed skin tends to be mildly to severely itchy.
How is dry hands diagnosed?
- Xerosis can be diagnosed by your dermatologist examining the skin and taking a medical history. You may need certain investigations if your doctor suspects that your dry skin is caused by an underlying medical condition.
- If a rash is present a biopsy may be necessary to help diagnose and confirm various skin diseases associated with xerosis.
How to get rid of dry hands
- Identify and treat contributing factors (see list above).
- Reduce the frequency and length of baths or showers and use lukewarm water.
- Avoid soap and use soap-free, fragrance-free cleansers or bath oil.
- Pat your skin dry with a soft towel and do not rub too vigorously.
- Apply a bland emollient or moisturizer after hand washing or showering while the skin is still warm and damp. Repeat an application of moisturizer as often as necessary throughout the day. Your dermatologist can recommend a good emollient or moisturizer for you to use.
- Lips and hands may need extra attention. Lip balms need to be applied multiple times throughout the day to the lips. Similarly, thicker moisturizers or balms should be applied to your hands frequently.
- Treat eczema, psoriasis and other skin conditions. Discuss this with your dermatologist.
- Wear cotton (or other natural fibers) next to your skin and under wool or synthetic clothing if these cause itching or irritation to the skin.
- Use a humidifier to add moisture to the air inside your home.
- If the condition becomes worse, please see your doctor or dermatologist.
Home remedies for dry cracked hands
If your dry skin is caused by something that you are doing, such as immersing your hands in water all day, you may need to stop doing this for a few days. When you start up again, you may need to wear gloves or apply a special moisturizer throughout the day.
Moisturizer
Moisturize your skin by applying a moisturizer ointment, cream, or lotion 2 to 3 times a day, or as often as needed throughout the day can help. It can make the skin softer, smoother, and less likely to crack. Body moisturizers come in a few forms — ointments, creams, lotions, and oils. Your doctor can tell you which is recommended for you. Moisturizers help lock in moisture, so they work best on damp skin. After you bathe, pat skin dry then apply your moisturizer.
For very dry skin, a moisturizer that contains urea or lactic acid may be helpful. These ingredients help the skin hold water. You can find these ingredients in both prescription moisturizers and those that you can buy without a prescription. A drawback is that these ingredients can sting if you have eczema or cracked skin.
Healthy hand washing and bathing habits can improve dry skin:
- Take a bath or shower only once daily. More frequent bathing can make the skin lose water (dehydrate).
- Use lukewarm (not hot) water. Hot water removes your natural skin oils more quickly. Warm water is best for bathing.
- Limit bath time to 5-10 minutes. A 5- to 10-minute bath or shower adds moisture to the skin. Spending more time in the water often leaves your skin less hydrated than before you started. Do not bathe more often than once a day.
- Avoid harsh deodorant soaps (or limit their use to armpits, groin, and feet).
- Use a gentle cleanser (non-soap cleansers). Soaps can strip oils from the skin. Stop using deodorant bars, antibacterial soaps, perfumed soaps, and skin care products containing alcohol, like hand sanitizers. Look for either a mild, fragrance-free soap or a soap substitute that moisturizes.
- Pat (don’t rub) the skin dry after bathing.
- Apply moisturizer immediately after bathing, while the skin is still moist. Moisturize right after baths and showers to lock in moisture from a bath or shower, apply a moisturizer while the skin is still damp.
- When choosing a moisturizer, look for oil-based creams and ointments, which work better than water-based lotions.
The following over-the-counter products may be helpful:
- Petrolatum or petroleum jelly (Vaseline®)
- Fragrance-free creams or ointments
- Preparations containing alpha-hydroxy acids such as glycolic acid or lactic acid
- Creams containing urea
- Over-the-counter cortisone cream (if the areas are itchy)
- Topical antibiotics applied immediately to any cracks in the skin to help prevent infection
Use a humidifier in the bedroom during the cold, dry seasons to help prevent dry skin.
- Apply cool cloths to itchy dry skin.
- Cover up outdoors in winter. In the cold, wear a scarf and gloves to help prevent chapped lips and hands.
See your doctor for an evaluation if the above self-care measures do not cure your dry skin and dry hands.
Treatments your doctor may prescribe
Sometimes people need a dermatologist’s help to get relief from dry skin.
Your doctor or dermatologist may prescribe:
When skin is extremely dry, your dermatologist may prescribe a medicine that you can apply to your skin. This may be a corticosteroid (cortisone-like) or an immune modulator (tacrolimus, pimecrolimus). These medicines tend to be quite good at relieving the itch, redness, and swelling. You also may need to use a moisturizer several times a day.
- Cream containing alpha- or beta-hydroxy acids (glycolic acid, lactic acid, salicylic acid)
- Urea-based cream
- Preparation containing high concentrations of propylene glycol
- Corticosteroid (cortisone) cream, if the skin is inflamed or very itchy
If your doctor suspects that a medical condition is causing your dry skin, then he or she may do blood tests or other diagnostic procedures. The best treatment for dry skin caused by a medical problem is to treat the medical problem.
What is the prognosis of dry hands?
Dry hands can be a long term and recurring problem, especially in winter. Using a non-soap cleanser and moisturizer should become part of your skin care routine.