Contents
What is gallbladder sludge
Gallbladder sludge also known as biliary sand, biliary sediment, or thick bile, has been defined as a mixture of precipitated crystals, glycoproteins, cellular debris and mucin 1. Although gallbladder sludge composition varies, cholesterol monohydrate crystals, calcium bilirubinate granules and other calcium salts are the main constituents 2. Gallbladder sludge has often been considered an incidental finding by radiologists 3 and can occur secondarily to stagnant biliary flow and gallbladder dysmotility 4. Gallbladder sludge is usually detected on transabdominal ultrasonography seen as a liquid-liquid level in the gallbladder 5. On ultrasound, gallbladder sludge appears as a low amplitude homogeneous echoes, layering on the posterior wall. It moves slowly with changes in patient position. Small amounts of gallbladder sludge may mimic gallstones (so called “tumefactive sludge”) but sludge does not cause shadowing, unless associated with gallstones 6. Large amounts of tumefactive sludge may mimic a mass. Gallbladder sludge is associated with pregnancy; with rapid weight loss, particularly in the obese; with critical illness involving low or absent oral intake and the use of total parenteral nutrition (TPN); and following gastric surgery 7. Gallbladder sludge is also associated with biliary stones with common bile duct obstruction; with certain drugs, such as ceftriaxone and octreotide; and with bone marrow or solid organ transplantation 7.
The presence of gallbladder sludge on the gallbladder ultrasound suggests the presence of gallstones and is associated with a high rate of recurrence of pancreatitis in nonoperated patients 8.
The clinical course of gallbladder sludge varies. Gallbladder sludge often vanishes, particularly if the causative event disappears; other cases wax and wane, and some go on to gallstones 7. Complications caused by gallbladder sludge include biliary colic, acute cholangitis, and acute pancreatitis. Asymptomatic patients with gallbladder sludge or microlithiasis require no therapy. When patients are symptomatic or if complications arise, cholecystectomy is indicated. For the elderly or those at risk from the surgery, endoscopic sphincterotomy can prevent recurrent episodes of pancreatitis. Medical therapy is limited, although some approaches may show promise in the future.
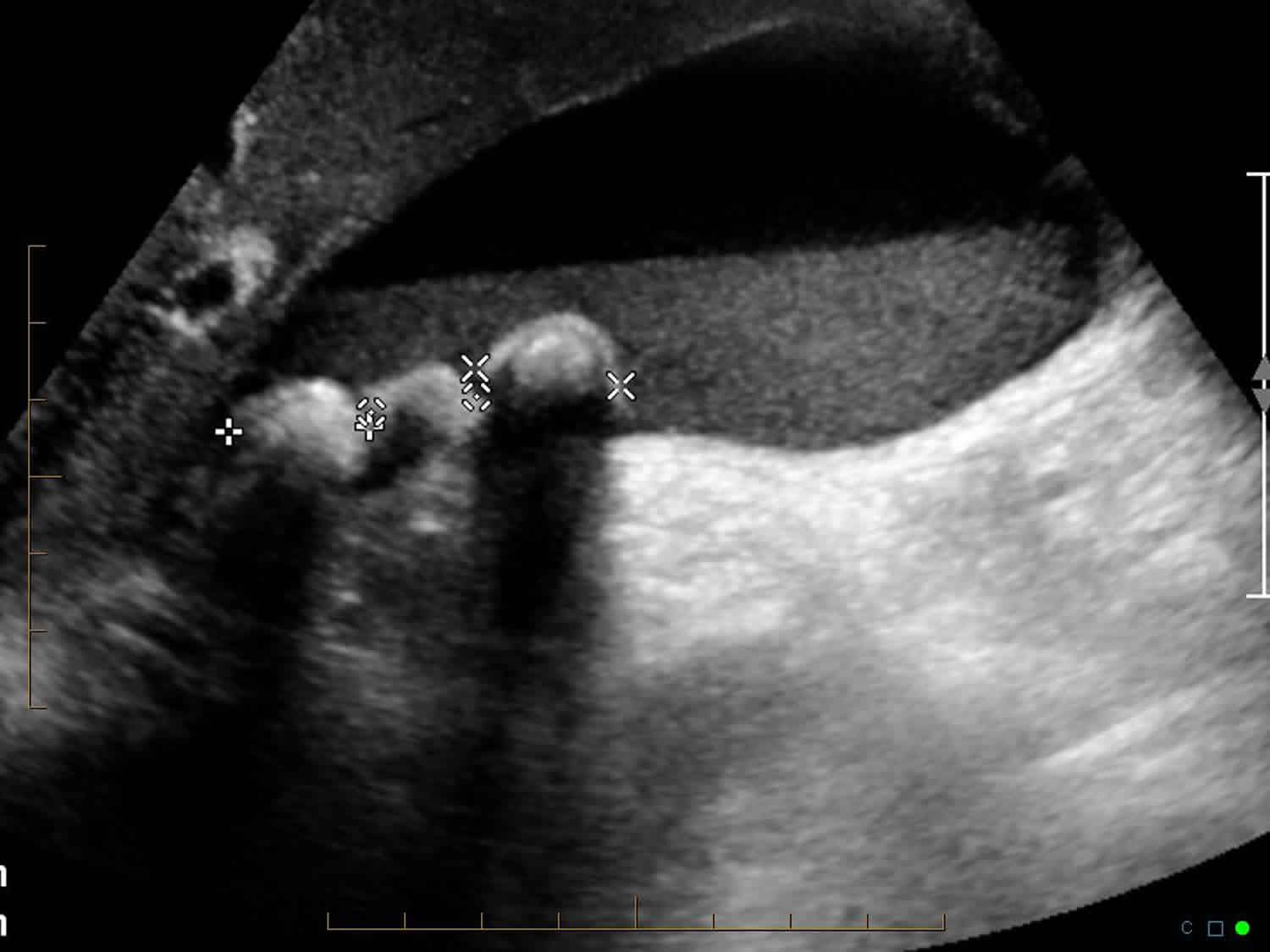
Figure 1. Gallbladder sludge ultrasound
Footnote: Distended gall bladder containing echogenic, gravity dependent, mobile, biliary sludge with calculi. No specific features of cholecystitis ie no wall thickening or surrounding edema (nor pain on ultrasound probing of the fundus).
Can gallbladder sludge go away?
The clinical course of gallbladder sludge varies. Gallbladder sludge often vanishes, particularly if the causative event disappears; other cases wax and wane, and some go on to gallstones 7. Complications caused by gallbladder sludge include biliary colic, acute cholangitis, and acute pancreatitis. Asymptomatic patients with gallbladder sludge or microlithiasis require no therapy. When patients are symptomatic or if complications arise, cholecystectomy is indicated. For the elderly or those at risk from the surgery, endoscopic sphincterotomy can prevent recurrent episodes of pancreatitis. Medical therapy is limited, although some approaches may show promise in the future.
Gallbladder sludge diet
There is increasing evidence to support a connection between dietary intake and gallstone disease. In studies of non-pregnant women, high intake of dietary carbohydrates has been linked to gallstone disease and cholecystectomy 9, although not all studies support this conclusion 10, 11. Since many of these studies evaluated symptomatic gallstone disease, further clarification on whether carbohydrate intake affects the incidence of gallstones or the risk of developing symptoms from pre-existing gallstones is needed. If carbohydrate intake is indeed associated with gallstone formation, dietary modification might be an effective method of prevention. Presently, the effect of carbohydrate intake on gallstone disease is unclear and needs further investigation.
In this prospective study 12, the researchers found high total carbohydrate and fructose intake to be associated with increased risk of incident gallbladder sludge and stones during pregnancy. These associations persisted despite adjustment for numerous potential confounding factors, such as pre-pregnancy BMI (body mass index), weight gain during pregnancy, and serum lipid and glucose levels. The strength of the association for high carbohydrate or fructose intake was greater than the effect of race or ethnicity, which were not significant risk factors for gallbladder sludge or gallstones in their previous studies, but is less than the association they have previously seen for obesity 13.
Among the individual carbohydrates examined in the prospective study 12, fructose was found to be uniquely associated with incident gallbladder disease independent of total carbohydrate intake. The mechanism by which fructose promotes gallbladder disease is unclear, although excessive fructose intake has been shown to produce conditions that favor gallstone formation. Fructose promotes hepatic insulin resistance in humans 14, a condition that enhances cholesterol gallstone formation in mice 15. Fructose bypasses phosphofructokinase, the rate limiting enzymatic step imposed on glucose, and its metabolites are funneled into fatty acid synthesis, resulting in hepatic lipogenesis, hypertriglyceridemia, and visceral fat deposition 16. Prolonged consumption of a fructose rich diet results in elevation of serum leptin20, a satiety hormone that has been associated with gallbladder disease during pregnancy 17. Excessive fructose intake might contribute to the metabolic syndrome 18 and gallstones, in turn, are linked to the metabolic syndrome 19. Thus, insulin resistance and the metabolic syndrome are potential pathways connecting fructose intake to gallstone formation. It is unclear why other individual carbohydrates were not associated with gallstone formation, although scientists hypothesize that they have differing effects upon glucose or lipid metabolism and insulin sensitivity.
Several other studies have looked at dietary carbohydrates and gallstones in men and non-pregnant women, but they are heterogeneous in their definition of gallstone disease, method of dietary assessment, and results. In subset analyses including only women, an Australian case-control study 20 found high sugar intake to be associated with gallstones detected by ultrasound, cholecystography, or intraoperative visualization, while an Indian case-control study 21 found high intake of total and refined carbohydrates to be associated with gallstones detected intraoperatively or by radiological methods. In Italy, a large cross-sectional study 22 showed that high carbohydrate intake was associated with previously undiagnosed gallstones detected by ultrasound among females, while two other European studies 23, 11 had mixed results. Two prospective studies using data from the Nurses’ Health Study also had conflicting results. In the first study 10, intake of carbohydrate and sucrose was not associated with cholecystectomy or imaging-confirmed symptomatic gallstones that did not require cholecystectomy. In the second study 9, high consumption of carbohydrate, starch, sucrose, and fructose was positively associated with the risk of cholecystectomy. The opposing results from the Nurses’ Health Study based studies might be due to differences in statistical power as the latter study had longer patient follow-up duration and more identified cases (4 years, 612 cases vs. 16 years, 5771 cases).
In conclusion, scientsts have shown that a diet rich in total carbohydrates and fructose is associated with formation of biliary sludge and stones during pregnancy 12. These associations persisted despite adjustment for various potential confounding factors. Therefore, dietary intervention might be an effective strategy to reduce the incidence of biliary disease among pregnant women.
Gallbladder sludge causes
Gallbladder sludge is associated with pregnancy; with rapid weight loss, particularly in the obese; with critical illness involving low or absent oral intake and the use of total parenteral nutrition (TPN); and following gastric surgery 7. Previous studies indicate that gallbladder sludge forms in up to 31% of pregnant women 24. Gallbladder sludge is also associated with biliary stones with common bile duct obstruction; with certain drugs, such as ceftriaxone and octreotide; and with bone marrow or solid organ transplantation 7. Gallbladder sludge has also been reported with intensive insulin therapy 25.
Gallbladder sludge symptoms
Gallbladder sludge should be considered in any patient with vague abdominal symptoms and right-upper-quadrant pain and jaundice 26. Complications caused by gallbladder sludge include biliary colic, acute cholangitis, and acute pancreatitis.
Gallbladder sludge symptoms that may occur include:
- Pain in the right upper or middle upper abdomen for at least 30 minutes. The pain may be constant or cramping. It can feel sharp or dull.
- Fever
- Yellowing of skin and whites of the eyes (jaundice)
Other symptoms may include:
- Clay-colored stools
- Nausea and vomiting
Blockage by gallstones may cause swelling or infection in the:
- Gallbladder (cholecystitis)
- Tube that carries bile from the liver to the gallbladder and intestines (cholangitis)
- Pancreas (pancreatitis)
Gallbladder sludge diagnosis
Tests and procedures used to diagnose gallbladder sludge and gallstones include:
- Tests to create pictures of your gallbladder. Your doctor may recommend an abdominal ultrasound and a computerized tomography (CT) scan to create pictures of your gallbladder. These images can be analyzed to look for signs of gallstones.
- Tests to check your bile ducts for gallstones. A test that uses a special dye to highlight your bile ducts on images may help your doctor determine whether a gallstone is causing a blockage. Tests may include a hepatobiliary iminodiacetic acid (HIDA) scan, magnetic resonance imaging (MRI) or endoscopic retrograde cholangiopancreatography (ERCP). Gallstones discovered using ERCP can be removed during the procedure.
- Blood tests to look for complications. Blood tests may reveal an infection, jaundice, pancreatitis or other complications caused by gallstones.
Gallbladder sludge treatment
The clinical course of gallbladder sludge varies. Gallbladder sludge often vanishes, particularly if the causative event disappears; other cases wax and wane, and some go on to gallstones 7. Complications caused by gallbladder sludge include biliary colic, acute cholangitis, and acute pancreatitis.
Your doctor will determine if treatment for gallbladder sludge is indicated based on your symptoms and the results of diagnostic testing. Asymptomatic patients with gallbladder sludge or microlithiasis require no therapy. When patients are symptomatic or if complications arise, cholecystectomy is indicated. For the elderly or those at risk from the surgery, endoscopic sphincterotomy can prevent recurrent episodes of pancreatitis. Medical therapy is limited, although some approaches may show promise in the future.
Gallbladder sludge surgery
In general, people who have symptoms will need surgery right away or soon after the stone is found.
- A technique called laparoscopic cholecystectomy is most commonly used. This procedure uses small surgical incisions, which allow for a faster recovery. A patient can often go home from the hospital within 1 day of surgery.
- In the past, open cholecystectomy (gallbladder removal) was most often done. However, this technique is less common now.
Endoscopic retrograde cholangiopancreatography (ERCP) and a procedure called a sphincterotomy may be done to find or treat gallstones in the common bile duct.
Medications to dissolve gallstones
Medicines may be given in pill form to dissolve cholesterol gallstones. However, these drugs may take 2 years or longer to work, and the gallstones may return after treatment ends.
Sometimes medications don’t work. Medications for gallstones aren’t commonly used and are reserved for people who can’t undergo surgery.
Rarely, chemicals are passed into the gallbladder through a catheter. The chemical rapidly dissolves cholesterol stones. This treatment is hard to perform, so it is not done very often. The chemicals used can be toxic, and the gallstones may return.
Shock wave lithotripsy
Shock wave lithotripsy (ESWL) of the gallbladder has also been used for people who cannot have surgery. This treatment is not used as often as it once was because gallstones often come back.
Gallbladder sludge flush
Gallbladder flush also called a gallbladder cleanse or a liver flush — is an alternative remedy for ridding the body of gallstones. However, no scientific evidence suggests that a gallbladder flush helps prevent or treat gallstones or any other disease.
In most cases, a gallbladder flush involves eating or drinking a combination of olive oil, herbs and some type of fruit juice over the course of two or more days — during which you may be advised to eat nothing else. There’s no standard formula for gallbladder flushing regimens and products. Different practitioners follow their own recipes.
Proponents of gallbladder cleansing claim that the treatment helps break up gallstones and stimulates the gallbladder to release them in stool. The large, repeated doses of olive oil in gallbladder flush preparations do have a laxative effect. And people who have taken a gallbladder flush report finding lumps that look like gallstones in their stool just after the procedure. When analyzed, though, these lumps turn out to be composed of oil, juice and other materials.
Gallbladder cleansing is not without risk. Some people have nausea, vomiting, diarrhea and abdominal pain during the flushing or cleansing period. Individual components of the herbal mixtures used in a gallbladder cleanse may present their own health hazards.
Gallstones that cause no symptoms typically require no treatment. If you have gallstones that require treatment, discuss proven treatment options with your doctor, such as surgical removal, bile salt tablets or sound wave therapy outlined above.
- Secchi P., Pöppl A.G., Ilha A., Kunert Filho H.C., Lima F.E.S., García A.B. Prevalence, risk factors, and biochemical markers in dogs with ultrasound-diagnosed biliary sludge. Res Vet Sci. 2012;93:1185–1189[↩]
- Ko C.W., Sekijima J.H., Lee S.P. Biliary sludge. Ann Intern Med. 1999;130:301–311[↩]
- Berent A.C. Acute biliary diseases of the dog and cat. In: Silverstein D., Hopper K., editors. Small animal critical care medicine. Saunders Elsevier; Missouri: 2008. pp. 542–546[↩]
- Saunders H, Thornton LA, Burchell R. Medical and surgical management of gallbladder sludge and mucocoele development in a Miniature Schnauzer. Int J Vet Sci Med. 2017;5(1):75–80. Published 2017 Apr 20. doi:10.1016/j.ijvsm.2017.01.002[↩]
- Shaffer EA. Gallbladder sludge: what is its clinical significance?. Curr Gastroenterol Rep. 2003;3 (2): 166-73[↩]
- Ferreira, Adilson Cunha et al. Fatores de risco clínicos e ultra-sonográficos relacionados à litíase vesicular assintomática em mulheres. Radiol Bras [online]. 2004, vol.37, n.2, pp. 77-82 http://dx.doi.org/10.1590/S0100-39842004000200004[↩]
- Gallbladder sludge: what is its clinical significance? Curr Gastroenterol Rep. 2001 Apr;3(2):166-73. https://www.ncbi.nlm.nih.gov/pubmed/11276386[↩][↩][↩][↩][↩][↩][↩]
- Delaney K, Velez L. The significance of gallbladder sludge in the patient with acute pancreatitis. Crit Care. 2007;11(Suppl 2):P403. doi:10.1186/cc5563 https://www.ncbi.nlm.nih.gov/pmc/articles/PMC4095456/[↩]
- Tsai CJ, Leitzmann MF, Willett WC, Giovannucci EL. Glycemic load, glycemic index, and carbohydrate intake in relation to risk of cholecystectomy in women. Gastroenterology. 2005;129:105–12[↩][↩]
- Maclure KM, Hayes KC, Colditz GA, Stampfer MJ, Willett WC. Dietary predictors of symptom-associated gallstones in middle-aged women. Am J Clin Nutr. 1990;52:916–22[↩][↩]
- Jorgensen T, Jorgensen LM. Gallstones and diet in a Danish population. Scand J Gastroenterol. 1989;24:821–6[↩][↩]
- Wong AC, Ko CW. Carbohydrate intake as a risk factor for biliary sludge and stones during pregnancy. J Clin Gastroenterol. 2013;47(8):700–705. doi:10.1097/MCG.0b013e318286fdb0 https://www.ncbi.nlm.nih.gov/pmc/articles/PMC3681860[↩][↩][↩]
- Ko CW, Beresford SA, Schulte SJ, Matsumoto AM, Lee SP. Incidence, natural history, and risk factors for biliary sludge and stones during pregnancy. Hepatology. 2005;41:359–365[↩]
- Faeh D, Minehira K, Schwarz JM, Periasamy R, Park S, Tappy L. Effect of fructose overfeeding and fish oil administration on hepatic de novo lipogenesis and insulin sensitivity in healthy men. Diabetes. 2005;54:1907–13[↩]
- Biddinger SB, Haas JT, Yu BB, Bezy O, Jing E, Zhang W, et al. Hepatic insulin resistance directly promotes formation of cholesterol gallstones. Nat Med. 2008;14:778–82[↩]
- Stanhope KL, Bremer AA, Medici V, Nakajima K, Ito Y, Nakano T, et al. Consumption of fructose and high fructose corn syrup increase postprandial triglycerides, LDL-cholesterol, and apolipoprotein-B in young men and women. J Clin Endocrinol Metab. 2011;96:E1596–605[↩]
- Ko CW, Beresford SA, Schulte SJ, Matsumoto AM, Lee SP. Incidence, natural history, and risk factors for biliary sludge and stones during pregnancy. Hepatology. 2005;41:359–365.[↩]
- Dekker MJ, Su Q, Baker C, Rutledge AC, Adeli K. Fructose: a highly lipogenic nutrient implicated in insulin resistance, hepatic steatosis, and the metabolic syndrome. Am J Physiol Endocrinol Metab. 2010;299:E685–94[↩]
- Stokes CS, Krawczyk M, Lammert F. Gallstones: environment, lifestyle and genes. Dig Dis. 2011;29:191–201.[↩]
- Scragg RK, McMichael AJ, Baghurst PA. Diet, alcohol, and relative weight in gall stone disease: a case-control study. Br Med J (Clin Res Ed) 1984;288:1113–9[↩]
- Tandon RK, Saraya A, Paul S, Kapur BM. Dietary habits of gallstone patients in Northern India. J Clin Gastroenterol. 1996;22:23–7[↩]
- Attili AF, Scafato E, Marchioli R, Marfisi RM, Festi D. Diet and gallstones in Italy: the cross-sectional MICOL results. Hepatology. 1998;27:1492–8[↩]
- Misciagna G, Centonze S, Leoci C, Guerra V, Cisternino AM, Ceo R, et al. Diet, physical activity, and gallstones–a population-based, case-control study in southern Italy. Am J Clin Nutr. 1999;69:120–6[↩]
- Incidence, natural history, and risk factors for biliary sludge and stones during pregnancy. Ko CW, Beresford SA, Schulte SJ, Matsumoto AM, Lee SP. Hepatology. 2005 Feb; 41(2):359-65.[↩]
- Acalculous cholecystitis. Batey A, Khan MA. Clin Gastroenterol Hepatol. 2007 Mar; 5(3):e8.[↩]
- Kalra S, Kalra B, Thakur A, Sharma A. Biliary sludge and recurrent ketoacidosis: a case report. Diabetol Metab Syndr. 2009;1:28. Published 2009 Dec 22. doi:10.1186/1758-5996-1-28 https://www.ncbi.nlm.nih.gov/pmc/articles/PMC2804582[↩]