Contents
What is gastroschisis
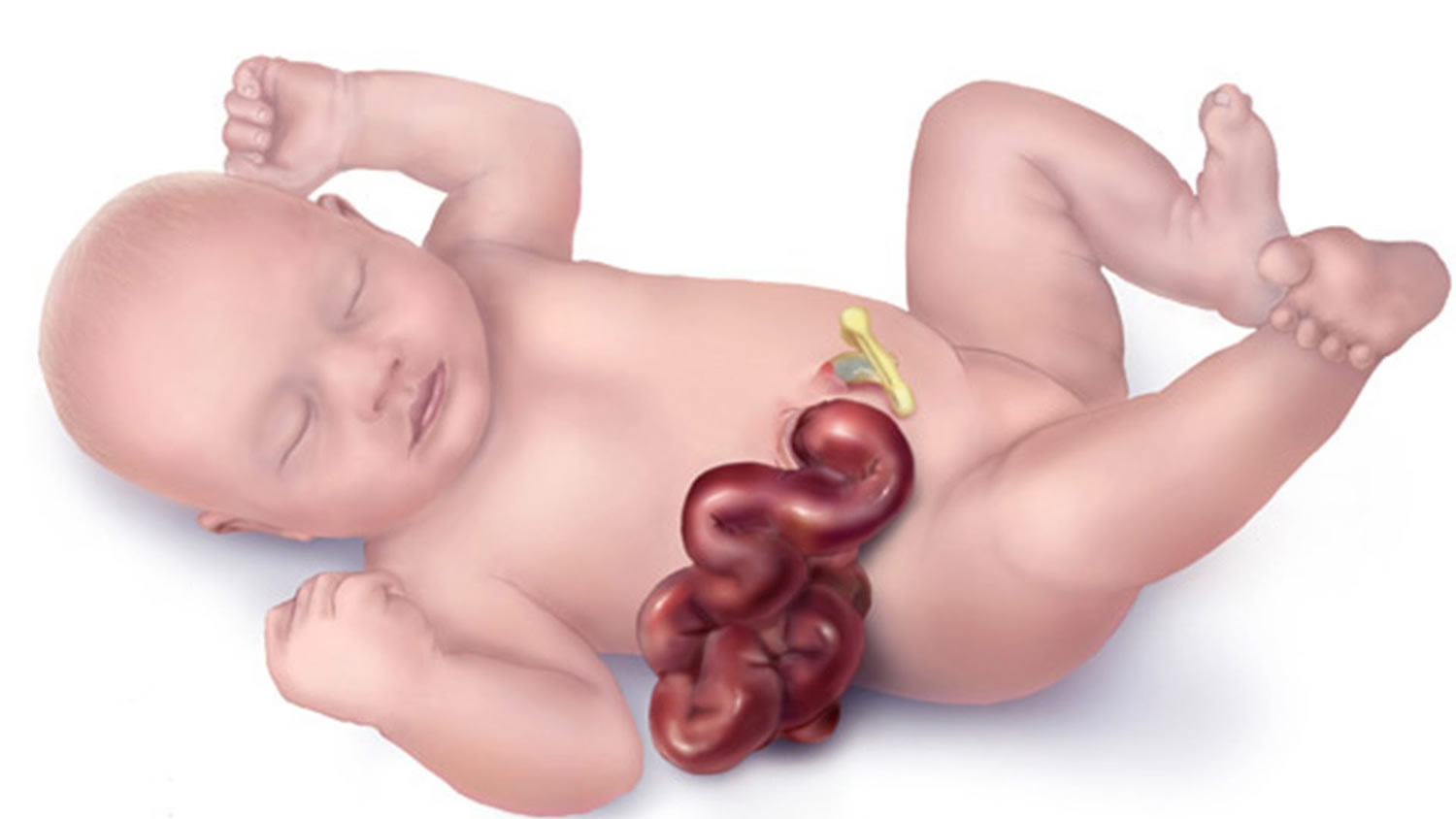
Gastroschisis is an uncommon birth defect of the anterior abdominal wall where the baby’s intestines are found outside of the baby’s body, exiting through a hole beside the belly button. The hole can be small or large and sometimes other organs, such as the stomach and liver, can also be found outside of the baby’s body.
Gastroschisis affects about one in 5000 babies 1. The Centers for Disease Control and Prevention (CDC) estimates that about 1,871 babies are born each year in the United States with gastroschisis, but several studies show that recently this birth defect has become more common, particularly among younger mothers 2. Gastroschisis occurs early during pregnancy when the muscles that make up the baby’s abdominal wall do not form correctly. A hole occurs which allows the intestines and other organs to extend outside of the body, usually to the right side of belly button. Because the intestines are not covered in a protective sac and are exposed to the amniotic fluid, the intestines can become irritated, causing them to shorten, twist, or swell. Generally, affected infants undergo corrective surgery within hours of birth. Though long-term outcomes for babies born with simple gastroschisis are generally good, some children may have problems with digestion later in life 3.
Mothers with the following may be at higher risk of having babies with gastrochisis:
- Younger age
- Fewer resources
- Poor nutrition during pregnancy
- Use illegal substances
Gastroschisis can be detected on prenatal ultrasound scans. Gastroschisis is usually diagnosed antenatally on routine ultrasound scanning. Unlike other congenital anomalies, gastroschisis is rarely associated with other major congenital abnormalities 4. The rate of spontaneous preterm birth in pregnancies complicated by fetal gastroschisis is over 50% 5. Anecdotally, many specialists recommend planned birth before term to minimize the risk of bowel damage, although there are no reliable data on how commonly this intervention is performed.
Although gastroschisis is usually surgically treatable with good results, many neonates require prolonged intensive care and parenteral nutrition. The costs of treatment may therefore be considerable. In addition, gastroschisis is often associated with intestinal injury such as necrosis or atresia (absence or closure of a natural passage of the body), leading to further complications, for example malabsorption, dysmotility or sepsis 6, and a high proportion of gastroschisis pregnancies are complicated by some degree of intrauterine growth restriction 7.
The defect is usually repaired surgically within a few hours of birth, to place the abdominal organs inside the baby’s body and repair the hole in the abdominal wall and most babies eventually do well. If the abdominal cavity is too small, a mesh sack is stitched around the borders of the defect and the edges of the defect are pulled up. The sack is called a silo. Over 5 to 7 days, the intestine returns into the abdominal cavity and the defect can be closed. More than one surgical procedure may be required to correct the defect. And many gastroschisis babies require prolonged intensive care support and artificial feeding, and some babies die. Some have long‐term bowel problems with eating, digestion of food, absorption of nutrients or malabsorption. Before the baby is born, the exposed bowel can be injured, and early birth may prevent this. However, early birth may also cause complications due to prematurity for the baby and possibly longer labor for the mother. There is currently no clear guidance. In one small randomized controlled trial 8, involving 42 women, there were no significant differences in outcomes for mother or baby when pre‐term birth at 36 weeks was planned, compared with later birth. However, it was such a small trial that it does not rule out important benefits or harms from early birth. There was also small overall difference in gestational age at birth between the two groups in the trial, possibly because of the high rate of spontaneous preterm birth with this condition. Currently, there is insufficient evidence to guide practice. Further trials are needed.
Gastroschisis life expectancy
The baby has a good chance of recovering if there are no other problems and if the abdominal cavity is large enough. A very small abdominal cavity may result in complications that require more surgeries.
Gastroschisis life expectancy depends primarily on the degree of injury to the bowel, and on the presence of other birth defects. Babies with gastroschisis generally do well, but there remains a mortality rate of 5% to 10% and some require prolonged parenteral nutrition and intensive care 9. Significant injury to the exposed bowel may occur in utero, and earlier birth may reduce this, improve long‐term outcomes and reduce complications, such as necrotising enterocolitis. However, it may also increase complications related to prematurity. There is a lack of published data in this area 9. Although most babies with gastroschisis have an excellent long‐term outcome, a small proportion require repeated surgery and some have malabsorption problems from bowel atresia. The long‐term effects on health outcomes remain uncertain, with little information in the literature.
Gastroschisis complications
A small number of babies with gastroschisis (about 10%) may have parts of the intestines that did not develop normally in the womb. With these babies, their intestines may not work normally even after the organs are put back inside the abdominal cavity.
The increased pressure from the misplaced abdominal contents can decrease blood flow to the intestines and kidneys. It can also make it difficult for the baby to expand the lungs, leading to breathing problems.
Another complication is bowel death necrosis. This occurs when intestinal tissue dies due to low blood flow or infection.
This condition is apparent at birth and will be detected in the hospital at delivery if it has not already been seen on routine fetal ultrasound exams during pregnancy. If you have given birth at home and your baby appears to have this defect, call the local emergency number right away.
Complications from gastroschisis can include intestinal problems, breathing difficulties, and infection 10. Some cases of gastroschisis may resolve in utero, with closure of the hole of the abdominal wall, resulting in strangulation and destruction of the herniated bowel (vanishing gastroschisis or vanishing gut syndrome), and very short-bowel syndrome 11. Other complications include incomplete bowel (atresia), destruction (necrosis), perforation or twisting (volvulos). The prognosis of these cases is poor, but detecting these problems during pregnancy (antenatal diagnosis) and having fetal intervention may improve the outcome in the future 12.
Can a baby die from gastroschisis?
Yes, overall, gastroschisis is associated with a mortality rate of 5% to 10% 13.
Gastroschisis ultrasound
Gastroschisis causes
The exact cause of a gastroschisis is usually not known, but gastroschisis is more common in babies born to young mothers 14 or to mothers who may have used alcohol or tobacco during their pregnancies 10, suggesting environmental factors may have a part to play. Some babies have gastroschisis because of a change in their genes or chromosomes. Gastroschisis might also be caused by a combination of genes and other factors, such as the things the mother comes in contact with in the environment or what the mother eats or drinks, or certain medicines she uses during pregnancy.
The incidence of gastroschisis is thought to be increasing, both in developed and in developing countries 15.
Recently, Centers for Disease Control and Prevention (CDC) researchers have reported important findings about some factors that affect the risk of having a baby with gastroschisis:
- Younger age: teenage mothers were more likely to have a baby with gastroschisis than older mothers 16
- Alcohol and tobacco: women who consumed alcohol or were a smoker were more likely to have a baby with gastroschisis 17
Centers for Disease Control and Prevention (CDC) continues to study birth defects like gastroschisis in order to learn how to prevent them. If you are pregnant or thinking about getting pregnant, talk with your doctor about ways to increase your chance of having a healthy baby.
Gastroschisis symptoms
A gastroschisis can be seen when the baby is born. There is a hole in the abdominal wall. The small intestine is often outside the abdomen near the umbilical cord. Other organs that may also be seen are the large intestine, stomach, or gallbladder.
If the intestine is damaged, the baby will have problems absorbing food.
- 80%-99% of babies have gastroschisis
- Lump in the abdomen
- Intestine sticks through the abdominal wall near the umbilical cord
- Problems with movement and absorption in the gut due to the unprotected intestine being exposed to irritating amniotic fluid
- 30%-79% of babies have intestinal atresia
- 5%-29% of babies have abnormality of mesentery morphology
Gastroschisis diagnosis
Gastroschisis can be diagnosed during pregnancy or after the baby is born. Gastroschisis is typically diagnosed on routine ultrasound examinations before a baby is born. These babies may need to be born in hospitals with specialists who are experienced in treating gastroschisis.
During Pregnancy
During pregnancy, there are screening tests (prenatal tests) to check for birth defects and other conditions. Gastroschisis might result in an abnormal result on a blood or serum screening test or it might be seen during an ultrasound (which creates pictures of the baby’s body while inside the womb).
After the Baby is Born
Gastroschisis is immediately seen at birth.
Gastroschisis treatment
- If identified before birth, mothers with gastroschisis need special monitoring to make sure the unborn baby remains and healthy. Plans should be made for careful delivery and immediate management of the problem after birth.
- The treatment for gastroschisis is surgery. A surgeon will put the bowel back into the abdomen and close the defect, if possible. If the abdominal cavity is too small, a mesh sack is stitched around the borders of the defect and the edges of the defect are pulled up. Over time, the herniated intestine falls back into the abdominal cavity, and the defect can be closed.
- Other treatments for the baby include nutrients by IV and antibiotics to prevent infection. The baby’s temperature must be carefully controlled, since the exposed intestine allows a lot of body heat to escape.
Soon after the baby is born, surgery will be needed to place the abdominal organs inside the baby’s body and repair the defect.
If the gastroschisis defect is small (only some of the intestine is outside of the belly), it is usually treated with surgery soon after birth to put the organs back into the belly and close the opening. If the gastroschisis defect is large (many organs outside of the belly), the repair might done slowly, in stages. The exposed organs might be covered with a special material and slowly moved back into the belly. After all of the organs have been put back in the belly, the opening is closed.
Babies with gastroschisis often need other treatments as well, including receiving nutrients through an IV line, antibiotics to prevent infection, and careful attention to control their body temperature.
Gastroschisis surgery
Gastroschisis repair also called silo repair 3, is a procedure done on an infant to correct a birth defect that causes an opening in the skin and muscles covering the belly (abdominal wall). The opening allows the intestines and sometimes other organs to bulge outside the belly.
The goal of the procedure is to place the organs back into the baby’s belly and fix the defect. Repair may be done right after the baby is born. This is called primary repair. Or, the repair is done in stages. This is called staged repair. Surgery for primary repair is done in the following way:
- If possible, the surgery is performed the day your baby is born. This surgery is done when there is only a small amount of intestine outside the belly and the intestine isn’t very swollen.
- Right after birth, the intestine that is outside the belly is placed in a special bag or is covered with a plastic wrap to protect it.
- Your baby is then prepared for surgery.
- Your baby receives general anesthesia. This is medicine that allows your baby to sleep and be pain-free during the operation
- The surgeon examines your baby’s intestine (bowel) closely for signs of damage or other birth defects. Unhealthy parts are removed. The healthy edges are stitched together.
- The intestine is placed back into the belly.
- The opening in the wall of the belly is repaired.
Staged repair is done when your baby isn’t stable enough for primary repair. It may also be done if the baby’s intestine is very swollen or there is a large amount of intestine outside the body. Or, it is done when the baby’s belly isn’t large enough to contain all of the intestine. The repair is performed the following way:
- Right after birth, the baby’s intestine and any other organs that are outside the belly are placed in a long plastic pouch. This pouch is called a silo. The silo is then attached to the baby’s belly.
- The other end of the silo is hung above the baby. This allows gravity to help the intestine to slip into the belly. Each day, the health care provider also gently tightens the silo to push the intestine into the belly.
- It may take up to 2 weeks for all of the intestine and any other organs to be back inside the belly. The silo is then removed. The opening in the belly is repaired.
More surgery may be needed at a later time to repair the muscles in your baby’s belly.
Gastroschisis surgery risks
Risks for anesthesia and surgery in general are:
- Allergic reactions to medicines
- Breathing problems
- Bleeding
- Infection
Risks for gastroschisis repair are:
- Breathing problems if the baby’s belly area (abdominal space) is smaller than normal. The baby may need a breathing tube and breathing machine for a few days or weeks after surgery.
- Inflammation of tissues that line the wall of the abdomen and cover the abdominal organs.
- Organ injury.
- Problems with digestion and absorbing nutrients from food, if a baby has a lot of damage to the small bowel.
- Temporary paralysis (muscles stop moving) of the small bowel.
- Abdominal wall hernia.
After the gastroschisis surgery
After surgery, your baby will receive care in the NICU (neonatal intensive care unit). The baby will be placed in a special to keep your baby warm.
Your baby may need to be on a breathing machine until organ swelling has decreased and the size of the belly area has increased.
Other treatments your baby will probably need after surgery are:
- A nasogastric tube placed through the nose to drain the stomach and keep it empty.
- Antibiotics.
- Fluids and nutrients given through a vein.
- Oxygen.
- Pain medicines.
Feedings are started through the nasogastric tube as soon as your baby’s bowel starts functioning after surgery. Feedings by mouth will start very slowly. Your baby may eat slowly and may need feeding therapy, lots of encouragement, and time to recover after a feeding.
The average stay in the hospital is a few weeks up to a few months. You may be able to take your baby home once he or she is taking all foods by mouth and gaining weight.
Gastroschisis surgery prognosis
After you go home, your child may develop a blockage in the intestines (bowel obstruction) due to a kink or scar in the intestines. The doctor can tell you how this will be treated.
Most of the time, gastroschisis can be corrected with one or two surgeries. How well your baby does will depend on how much damage there was to the intestine.
After recovering from surgery, most children with gastroschisis do very well and live normal lives. Most babies who are born with gastroschisis do not have any other birth defects.
- Loane M, Dolk H, Bradbury I, EUROCAT Working Group. Increasing prevalence of gastroschisis in Europe 1980‐2002: a phenomenon restricted to younger mothers?. Paediatric and Perinatal Epidemiology 2007;21(4):363‐9.[↩]
- Jones AM, Isenburg J, Salemi JL, et al.; for the National Birth Defects Prevention Network. Increasing prevalence of gastroschisis—14 States, 1995-2012. MMWR morb Mortal Wkly Rep. 2016 Jan 22;65(2):23-6[↩]
- Lepigeon K, Van Mieghem T, Vasseur Maurer S, Giannoni E, and Baud D. Gastroschisis – what should be told to parents. Prenatal Diagnosis. April 2014; 34(4):316-26. https://www.ncbi.nlm.nih.gov/pubmed/24375446[↩][↩]
- Fillingham A, Rankin J. Prevalence, prenatal diagnosis and survival of gastroschisis. Prenatal Diagnosis 2008;28(13):1232‐7.[↩]
- Huang J, Kurkchubasche J, Carr SR, Wesselhoeft CW, Tracy TF, Luks FI. Benefits of term delivery in infants with antenatally diagnosed gastroschisis. Obstetrics & Gynecology 2002;100(4):695‐9.[↩]
- Lund CH, Bauer K, Berrios M. Gastroschisis: incidence, complications, and clinical management in the neonatal intensive care unit. Perinatal and Neonatal Nursing 2007;21(1):63‐8.[↩]
- Juhasz‐Böss I, Goelz R, Solomayer EF, Fuchs J, Meyberg‐Solomayer G. Fetal and neonatal outcome in patients with anterior abdominal wall defects (gastroschisis and omphalocele). Journal of Perinatal Medicine 2011;40(1):85‐90.[↩]
- Logghe H, Mason G, Stringer M, Thornton J. Postnatal bowel function in fetuses with gastroschisis is not improved by elective preterm delivery: a prospective pilot study. American Journal of Obstetrics and Gynecology 2001;185(6):S242.[↩]
- Grant NH, Dorling J, Thornton JG. Elective preterm birth for fetal gastroschisis. Cochrane Database of Systematic Reviews 2013, Issue 6. Art. No.: CD009394. DOI: 10.1002/14651858.CD009394.pub2[↩][↩]
- Prefumo F and Izzi C. Fetal abdominal wall defects. Best Practice and Research Clinical Obstetrics and Gynaecology. April 2014; 28(3):391-402. https://www.ncbi.nlm.nih.gov/pubmed/24342556[↩][↩]
- Dennison FA. Closed gastroschisis, vanishing midgut and extreme short bowel syndrome: Case report and review of the literature. Ultrasound. August, 2016; 24(3):170-174. https://www.ncbi.nlm.nih.gov/pubmed/27867410[↩]
- Marinovic VM, Lukac M, Mikovic Z, Grujic B, Milickovic M, Samardzija G, Stojanovic A & Sabbagh D. Outcome differences between simple and complex gastroschisis. Ann Ital Chir. October 14, 2016; 87:pii: S0003469X16025926. https://www.ncbi.nlm.nih.gov/pubmed/27845942[↩]
- Bradnock TJ, Marven S, Owen A, Johnson P, Kurinczuk JJ, Spark P, et al. Gastroschisis: one year outcomes from national cohort study. BMJ 2011;15:343.[↩]
- Curry JI, McKinney P, Thornton JG, Stringer MD. The aetiology of gastroschisis. BJOG: an international journal of obstetrics and gynaecology 2000;107:1339‐6.[↩]
- Feldkamp ML, Carey JC, Sadler TW. Development of gastroschisis: review of hypotheses, a novel hypothesis, and implications for research. American Journal of Medical Genetics 2007;143A(7):639‐52.[↩]
- Jones AM, Isenburg J, Salemi JL, et al.; for the National Birth Defects Prevention Network. Increasing prevalence of gastroschisis—14 States, 1995-2012. MMWR morb Mortal Wkly Rep. 2016 Jan 22;65(2):23-6.[↩]
- Bird TM, Robbins JM, Druschel C, Cleves MA, Yang S, Hobbs CA, & the National Birth Defects Prevention Study. Demographic and environmental risk factors for gastroschisis and omphalocele in the National Birth Defects Prevention Study. J Pediatr Surg. 2009;44:1546-1551.[↩]