Contents
What is oropharynx
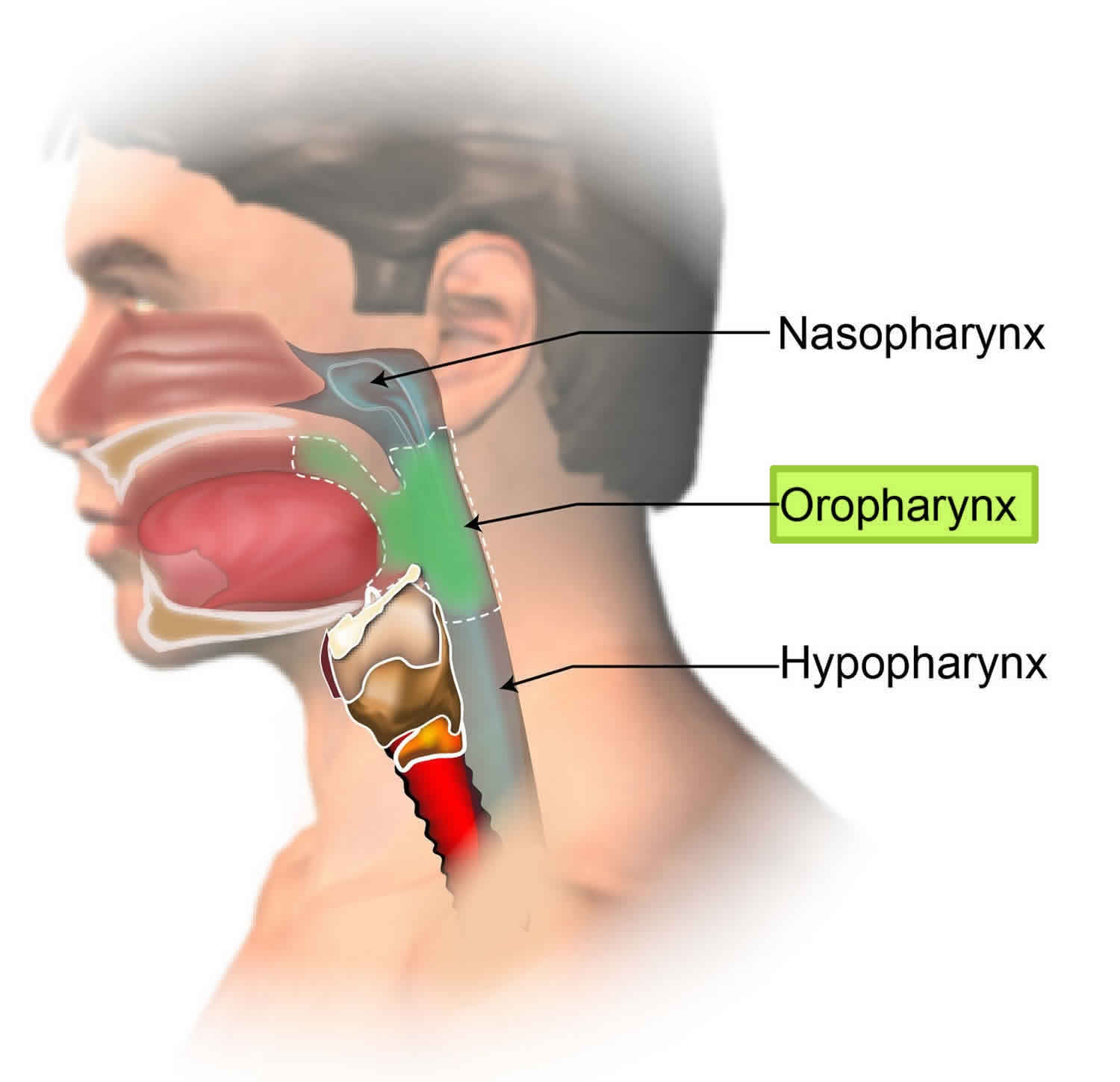
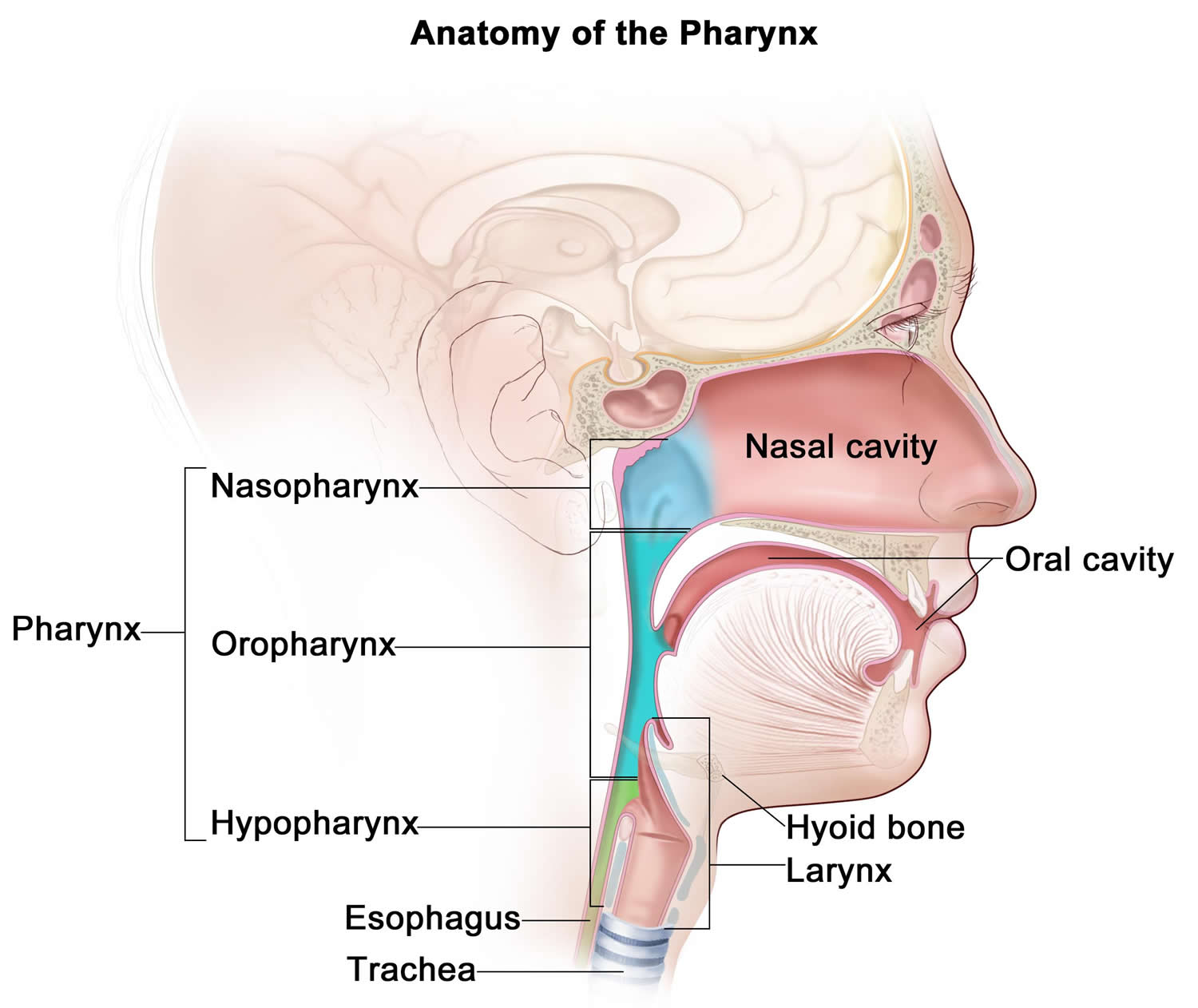
The oropharynx is the middle section of the pharynx (throat), behind the mouth. The oropharynx includes the base of the tongue (back 1/3), the soft palate at the back of the roof of the mouth, the tonsils, and the back of the throat. The oropharynx is behind the oral cavity, below the soft palate and above the epiglottis. The pharynx is a hollow tube about 5 inches long that starts behind the nose and ends where the trachea (windpipe) and esophagus (tube from the throat to the stomach) begin. Air and food pass through the pharynx on the way to the trachea or the esophagus. The three parts of the pharynx are the nasopharynx, oropharynx, and hypopharynx.
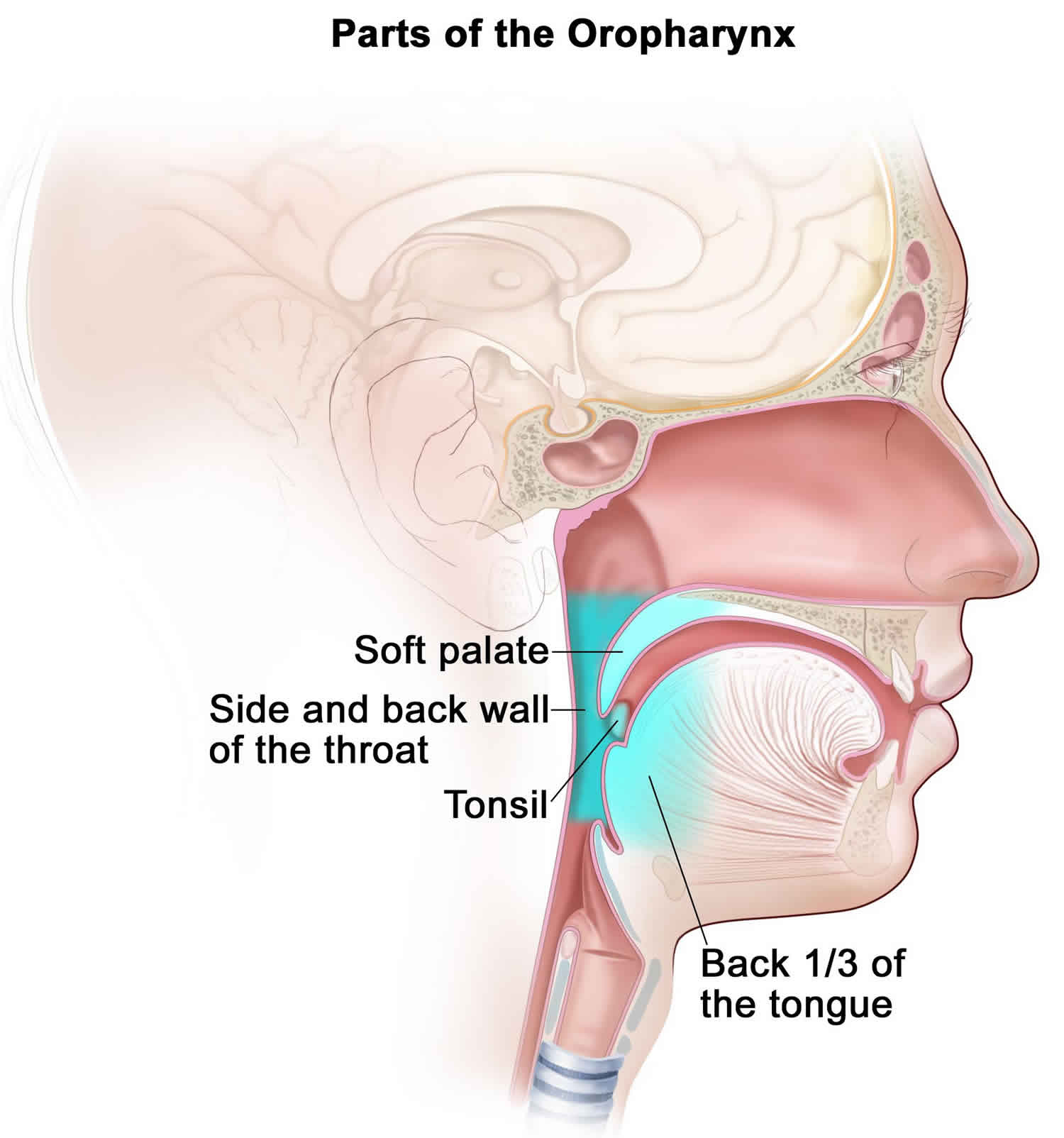
The oropharynx includes the following:
- Soft palate.
- Side and back walls of the throat.
- Tonsils.
- Back one-third of the tongue.
Figure 1. Oropharynx anatomy
Figure 2. Oropharynx parts
Oropharynx function
Muscles of the oropharynx play necessary roles in swallowing and speech.
Where is the oropharynx located?
The oropharynx is the middle section of the pharynx (throat), behind the mouth. The oropharynx includes the base of the tongue (back 1/3), the soft palate at the back of the roof of the mouth, the tonsils, and the back of the throat. The oropharynx is behind the oral cavity, below the soft palate and above the epiglottis.
The oropharynx includes the following:
- Soft palate.
- Side and back walls of the throat.
- Tonsils.
- Back one-third of the tongue.
Oropharynx infection
Pharyngitis
Pharyngitis or sore throat, is discomfort, pain, or scratchiness in the throat. It often makes it painful to swallow.
Call your doctor if:
- You develop a sore throat that does not go away after several days
- You have a high fever, swollen lymph nodes in your neck, or a rash
Seek medical care right away if you have a sore throat and trouble breathing.
Pharyngitis causes
Pharyngitis is caused by swelling in the back of the throat (pharynx) between the tonsils and the voice box (larynx).
Most sore throats are caused by colds, the flu, coxsackie virus or mono (mononucleosis).
Bacteria that can cause pharyngitis in some cases:
- Strep throat is caused by group A streptococcus.
- Less commonly, bacterial diseases such as gonorrhea and chlamydia can cause sore throat.
Most cases of pharyngitis occur during the colder months. The illness often spreads among family members and close contacts.
Pharyngitis symptoms
The main symptom is a sore throat.
Other symptoms may include:
- Fever
- Headache
- Joint pain and muscle aches
- Skin rashes
- Swollen lymph nodes (glands) in the neck
Pharyngitis possible complications
Pharyngitis complications may include:
- Ear infection
- Sinusitis
- Abscess near the tonsils
Pharyngitis diagnosis
Your health care provider will perform a physical exam and look at your throat.
A rapid Strep test or throat culture to test for strep throat may be done. Other laboratory tests may be done, depending on the suspected cause.
Pharyngitis treatment
Most sore throats are caused by viruses. Antibiotics do not help viral sore throats. Using these medicines when they are not needed leads to antibiotics not working as well when they are needed.
Sore throat is treated with antibiotics if:
- A strep test or culture is positive. Your provider cannot diagnose strep throat by symptoms or a physical exam alone.
- A culture for chlamydia or gonorrhea is positive.
Sore throat caused by the flu (influenza) may be helped by antiviral medicines.
The following tips may help your sore throat feel better:
- Drink soothing liquids. You can either drink warm liquids, such as lemon tea with honey, or cold liquids, such as ice water. You could also suck on a fruit-flavored ice pop.
- Gargle several times a day with warm salt water (1/2 tsp or 3 grams of salt in 1 cup or 240 milliliters of water).
- Suck on hard candies or throat lozenges. Young children should not be given these products because they can choke on them.
- Use of a cool-mist vaporizer or humidifier can moisten the air and soothe a dry and painful throat.
- Try over-the-counter pain medicines, such as acetaminophen.
Tonsillitis
Tonsillitis is a common childhood illness but teenagers and adults can get it too. It usually goes away on its own after a few days.
Tonsillitis can feel like a bad cold or flu. The tonsils at the back of your throat will be red and swollen.
The main symptoms of tonsillitis in children and adults are:
- a sore throat
- difficulty swallowing
- hoarse or no voice
- a high temperature of 38C or above
- coughing
- headache
- feeling sick
- earache
- feeling tired
Sometimes the symptoms can be more severe and include:
- swollen painful glands in your neck – feels like a lump on the side of your neck
- white pus-filled spots on your tonsils at the back of your throat
- bad breath (halitosis)
It’s important to get an accurate diagnosis if your child has symptoms that may indicate tonsillitis.
Call your doctor if your child is experiencing:
- A sore throat that doesn’t go away within 24 to 48 hours
- Painful or difficult swallowing
- Extreme weakness, fatigue or fussiness
Get immediate care if your child has any of these symptoms:
- Difficulty breathing
- Extreme difficulty swallowing
- Drooling
Tonsillitis causes
Tonsillitis is most often caused by common viruses, but bacterial infections can also be the cause.
The most common bacterium causing tonsillitis is Streptococcus pyogenes (group A streptococcus), the bacterium that causes strep throat. Other strains of strep and other bacteria also may cause tonsillitis.
Why do tonsils get infected?
The tonsils are the immune system’s first line of defense against bacteria and viruses that enter your mouth. This function may make the tonsils particularly vulnerable to infection and inflammation. However, the tonsil’s immune system function declines after puberty — a factor that may account for the rare cases of tonsillitis in adults.
Risk factors for tonsillitis
Risk factors for tonsillitis include:
- Young age. Tonsillitis most often occurs in children, but rarely in those younger than age 2. Tonsillitis caused by bacteria is most common in children ages 5 to 15, while viral tonsillitis is more common in younger children.
- Frequent exposure to germs. School-age children are in close contact with their peers and frequently exposed to viruses or bacteria that can cause tonsillitis.
Tonsillitis prevention
The germs that cause viral and bacterial tonsillitis are contagious. Therefore, the best prevention is to practice good hygiene. Teach your child to:
- Wash his or her hands thoroughly and frequently, especially after using the toilet and before eating
- Avoid sharing food, drinking glasses, water bottles or utensils
- Replace his or her toothbrush after being diagnosed with tonsillitis
To help your child prevent the spread of a bacterial or viral infection to others:
- Keep your child at home when he or she is ill
- Ask your doctor when it’s all right for your child to return to school
- Teach your child to cough or sneeze into a tissue or, when necessary, into his or her elbow
- Teach your child to wash his or her hands after sneezing or coughing
Tonsillitis symptoms
Tonsillitis most commonly affects children between preschool ages and the mid-teenage years. Common signs and symptoms of tonsillitis include:
- Red, swollen tonsils
- White or yellow coating or patches on the tonsils
- Sore throat
- Difficult or painful swallowing
- Fever
- Enlarged, tender glands (lymph nodes) in the neck
- A scratchy, muffled or throaty voice
- Bad breath
- Stomachache, particularly in younger children
- Stiff neck
- Headache
In young children who are unable to describe how they feel, signs of tonsillitis may include:
- Drooling due to difficult or painful swallowing
- Refusal to eat
- Unusual fussiness
Tonsillitis complications
Inflammation or swelling of the tonsils from frequent or ongoing (chronic) tonsillitis can cause complications such as:
- Difficulty breathing
- Disrupted breathing during sleep (obstructive sleep apnea)
- Infection that spreads deep into surrounding tissue (tonsillar cellulitis)
- Infection that results in a collection of pus behind a tonsil (peritonsillar abscess)
Strep infection
If tonsillitis caused by group A streptococcus or another strain of streptococcal bacteria isn’t treated, or if antibiotic treatment is incomplete, your child has an increased risk of rare disorders such as:
- Rheumatic fever, an inflammatory disorder that affects the heart, joints and other tissues
- Poststreptococcal glomerulonephritis, an inflammatory disorder of the kidneys that results in inadequate removal of waste and excess fluids from blood
Tonsillitis diagnosis
Your child’s doctor will start with a physical exam that will include:
- Using a lighted instrument to look at your child’s throat and likely his or her ears and nose, which may also be sites of infection
- Checking for a rash known as scarlatina, which is associated with some cases of strep throat
- Gently feeling (palpating) your child’s neck to check for swollen glands (lymph nodes)
- Listening to his or her breathing with a stethoscope
- Checking for enlargement of the spleen (for consideration of mononucleosis, which also inflames the tonsils)
Throat swab
With this simple test, the doctor rubs a sterile swab over the back of your child’s throat to get a sample of secretions. The sample will be checked in the clinic or in a lab for streptococcal bacteria.
Many clinics are equipped with a lab that can get a test result within a few minutes. However, a second more reliable test is usually sent out to a lab that can return results within 24 to 48 hours.
If the rapid Strep test in-clinic test comes back positive, then your child almost certainly has a bacterial infection. If the test comes back negative, then your child likely has a viral infection. Your doctor will wait, however, for the more reliable out-of-clinic lab test to determine the cause of the infection.
Complete blood cell count (CBC)
Your doctor may order a CBC with a small sample of your child’s blood. The result of this test, which can often be completed in a clinic, produces a count of the different types of blood cells. The profile of what’s elevated, what’s normal or what’s below normal can indicate whether an infection is more likely caused by a bacterial or viral agent. A CBC is not often needed to diagnose strep throat. However, if the strep throat lab test is negative, the CBC may be needed to help determine the cause of tonsillitis.
Tonsillitis treatment
At-home care
Whether tonsillitis is caused by a viral or bacterial infection, at-home care strategies can make your child more comfortable and promote better recovery.
If a virus is the expected cause of tonsillitis, these strategies are the only treatment. Your doctor won’t prescribe antibiotics. Your child will likely be better within seven to 10 days.
At-home care strategies to use during the recovery time include the following:
- Encourage rest. Encourage your child to get plenty of sleep.
- Provide adequate fluids. Give your child plenty of water to keep his or her throat moist and prevent dehydration.
- Provide comforting foods and beverage. Warm liquids — broth, caffeine-free tea or warm water with honey — and cold treats like ice pops can soothe a sore throat.
- Prepare a saltwater gargle. If your child can gargle, a saltwater gargle of 1 teaspoon (5 milliliters) of table salt to 8 ounces (237 milliliters) of warm water can help soothe a sore throat. Have your child gargle the solution and then spit it out.
- Humidify the air. Use a cool-air humidifier to eliminate dry air that may further irritate a sore throat, or sit with your child for several minutes in a steamy bathroom.
- Offer lozenges. Children older than age 4 can suck on lozenges to relieve a sore throat.
- Avoid irritants. Keep your home free from cigarette smoke and cleaning products that can irritate the throat.
- Treat pain and fever. Talk to your doctor about using ibuprofen (Advil, Children’s Motrin, others) or acetaminophen (Tylenol, others) to minimize throat pain and control a fever. Low fevers without pain do not require treatment.
Except for certain diseases, children and teenagers should not take aspirin because when used to treat symptoms of cold or flu-like illnesses, it has been linked to Reye’s syndrome, a rare but potentially life-threatening condition.
Antibiotics
If tonsillitis is caused by a bacterial infection, your doctor will prescribe a course of antibiotics. Penicillin taken by mouth for 10 days is the most common antibiotic treatment prescribed for tonsillitis caused by group A streptococcus. If your child is allergic to penicillin, your doctor will prescribe an alternative antibiotic.
Your child must take the full course of antibiotics as prescribed even if the symptoms go away completely. Failure to take all of the medication as directed may result in the infection worsening or spreading to other parts of the body. Not completing the full course of antibiotics can, in particular, increase your child’s risk of rheumatic fever and serious kidney inflammation.
Talk to your doctor or pharmacist about what to do if you forget to give your child a dose.
Surgery
Surgery to remove tonsils (tonsillectomy) may be used to treat frequently recurring tonsillitis, chronic tonsillitis or bacterial tonsillitis that doesn’t respond to antibiotic treatment. Frequent tonsillitis is generally defined as:
- More than seven episodes in one year
- More than four to five episodes a year in each of the preceding two years
- More than three episodes a year in each of the preceding three years
A tonsillectomy may also be performed if tonsillitis results in difficult-to-manage complications, such as:
- Obstructive sleep apnea (OSA)
- Breathing difficulty
- Swallowing difficulty, especially meats and other chunky foods
- An abscess that doesn’t improve with antibiotic treatment
Tonsillectomy is usually done as an outpatient procedure, unless your child is very young, has a complex medical condition or if complications arise during surgery. That means your child should be able to go home the day of the surgery. A complete recovery usually takes seven to 14 days.
Oropharynx cancer
Oropharyngeal cancer is a type of head and neck cancer. Sometimes more than one cancer can occur in the oropharynx and in other parts of the oral cavity, nose, pharynx, larynx (voice box), trachea, or esophagus at the same time.
Most oropharyngeal cancers are squamous cell carcinomas (SCC) (~95 percent). Squamous cells are the thin, flat cells lining the inside of the oropharynx.
Oropharyngeal cancer causes
Smoking or being infected with human papillomavirus can increase the risk of oropharyngeal cancer.
Oropharyngeal cancer risk factors
Anything that increases your risk of getting a disease is called a risk factor. Having a risk factor does not mean that you will get cancer; not having risk factors doesn’t mean that you will not get cancer. Talk with your doctor if you think you may be at risk.
The most common risk factors for oropharyngeal cancer include the following:
- A history of smoking cigarettes for more than 10 pack years and other tobacco use.
- Personal history of head and neck cancer.
- Heavy alcohol use.
- Being infected with human papillomavirus (HPV), especially HPV type 16. The number of cases of oropharyngeal cancers linked to HPV infection is increasing.
- Chewing betel quid, a stimulant commonly used in parts of Asia.
Oropharyngeal cancer signs and symptoms
Signs and symptoms of oropharyngeal cancer include a lump in the neck and a sore throat.
These and other signs and symptoms may be caused by oropharyngeal cancer or by other conditions. Check with your doctor if you have any of the following:
- A sore throat that does not go away.
- Trouble swallowing.
- Trouble opening the mouth fully.
- Trouble moving the tongue.
- Weight loss for no known reason.
- Ear pain.
- A lump in the back of the mouth, throat, or neck.
- A white patch on the tongue or lining of the mouth that does not go away.
- Coughing up blood.
Sometimes oropharyngeal cancer does not cause early signs or symptoms.
Oropharyngeal cancer diagnosis
Tests that examine the mouth and throat are used to help detect (find), diagnose, and stage oropharyngeal cancer.
The following tests and procedures may be used:
- Physical exam and history: An exam of the body to check general signs of health, including checking for signs of disease, such as swollen lymph nodes in the neck or anything else that seems unusual. The medical doctor or dentist does a complete exam of the mouth and neck and looks under the tongue and down the throat with a small, long-handled mirror to check for abnormal areas. An exam of the eyes may be done to check for vision problems that are caused by nerves in the head and neck. A history of the patient’s health habits and past illnesses and treatments will also be taken.
- PET-CT scan: A procedure that combines the pictures from a positron emission tomography (PET) scan and a computed tomography (CT) scan. The PET and CT scans are done at the same time with the same machine. The combined scans give more detailed pictures of areas inside the body than either scan gives by itself. A PET-CT scan may be used to help diagnose disease, such as cancer, plan treatment, or find out how well treatment is working.
- CT scan (CAT scan): A procedure that makes a series of detailed pictures of areas inside the body, such as the head and neck, taken from different angles. The pictures are made by a computer linked to an x-ray machine. A dye is injected into a vein or swallowed to help the organs or tissues show up more clearly. This procedure is also called computed tomography, computerized tomography, or computerized axial tomography.
- PET scan (positron emission tomography scan): A procedure to find malignant tumor cells in the body. A small amount of radioactive glucose (sugar) is injected into a vein. The PET scanner rotates around the body and makes a picture of where glucose is being used in the body. Malignant tumor cells show up brighter in the picture because they are more active and take up more glucose than normal cells do.
- MRI (magnetic resonance imaging): A procedure that uses a magnet, radio waves, and a computer to make a series of detailed pictures of areas inside the body. This procedure is also called nuclear magnetic resonance imaging (NMRI).
- Biopsy: The removal of cells or tissues so they can be viewed under a microscope by a pathologist to check for signs of cancer. A fine-needle biopsy is usually done to remove a sample of tissue using a thin needle.
The following procedures may be used to remove samples of cells or tissue:
- Endoscopy: A procedure to look at organs and tissues inside the body to check for abnormal areas. An endoscope is inserted through an incision (cut) in the skin or opening in the body, such as the mouth or nose. An endoscope is a thin, tube-like instrument with a light and a lens for viewing. It may also have a tool to remove abnormal tissue or lymph node samples, which are checked under a microscope for signs of disease. The nose, throat, back of the tongue, esophagus, stomach, larynx, windpipe, and large airways will be checked. The type of endoscopy is named for the part of the body that is being examined. For example, pharyngoscopy is an exam to check the pharynx.
- Laryngoscopy: A procedure in which the doctor checks the larynx (voice box) with a mirror or a laryngoscope to check for abnormal areas. A laryngoscope is a thin, tube-like instrument with a light and a lens for viewing the inside of the throat and voice box. It may also have a tool to remove tissue samples, which are checked under a microscope for signs of cancer.
If cancer is found, the following test may be done to study the cancer cells:
- HPV test (human papillomavirus test): A laboratory test used to check the sample of tissue for certain types of HPV infection. This test is done because oropharyngeal cancer can be caused by HPV.
Oropharyngeal cancer prognosis
The prognosis (chance of recovery) depends on the following:
- Whether the patient has HPV infection of the oropharynx.
- Whether the patient has a history of smoking cigarettes for ten or more pack years.
- The stage of the cancer.
- The number and size of lymph nodes with cancer.
Oropharyngeal tumors related to HPV infection have a better prognosis and are less likely to recur than tumors not linked to HPV infection.
Oropharyngeal cancer treatment
Oropharyngeal cancer treatment options
- There are different types of treatment for patients with oropharyngeal cancer.
- Patients with oropharyngeal cancer should have their treatment planned by a team of doctors with expertise in treating head and neck cancer.
- Four types of standard treatment are used:
- Surgery
- Radiation therapy
- Chemotherapy
- Targeted therapy
- New types of treatment are being tested in clinical trials.
- Treatment for oropharyngeal cancer may cause side effects.
- Patients may want to think about taking part in a clinical trial.
- Patients can enter clinical trials before, during, or after starting their cancer treatment.
- Follow-up tests may be needed.
Treatment options depend on the following:
- The stage of the cancer.
- Keeping the patient’s ability to speak and swallow as normal as possible.
- The patient’s general health.
Patients with oropharyngeal cancer have an increased risk of another cancer in the head or neck. This risk is increased in patients who continue to smoke or drink alcohol after treatment.