What is osmotic diuresis
Osmotic diuresis is increased urination due to the presence of certain substances in the filtered fluid by the kidneys. This fluid eventually becomes urine. These substances cause additional water to come into the urine, increasing its amount. The excretion occurs when substances such as glucose enter the kidney tubules and cannot be reabsorbed (due to a pathological state or the normal nature of the substance). The substances cause an increase in the osmotic pressure within the tubule, causing retention of water within the lumen, and thus reduces the reabsorption of water, increasing urine output (i.e. diuresis). The same effect can be seen in therapeutics such as mannitol, which is used to increase urine output and decrease extracellular fluid volume. Uncontrolled diabetes can induce hypovolemic-hyponatremia due to osmotic diuresis 1. Osmotic diuresis results in dehydration from polyuria and the classic polydipsia (excessive thirst) associated with diabetes mellitus. Moreover, in diabetic ketoacidosis ketone bodies (b-hydroxybutyrate and acetoacetate) obligate urinary electrolyte losses and aggravate the renal sodium wasting 2.
Osmotic diuresis can be caused by:
- Hyperglycemia or high blood sugar (glucose) 3
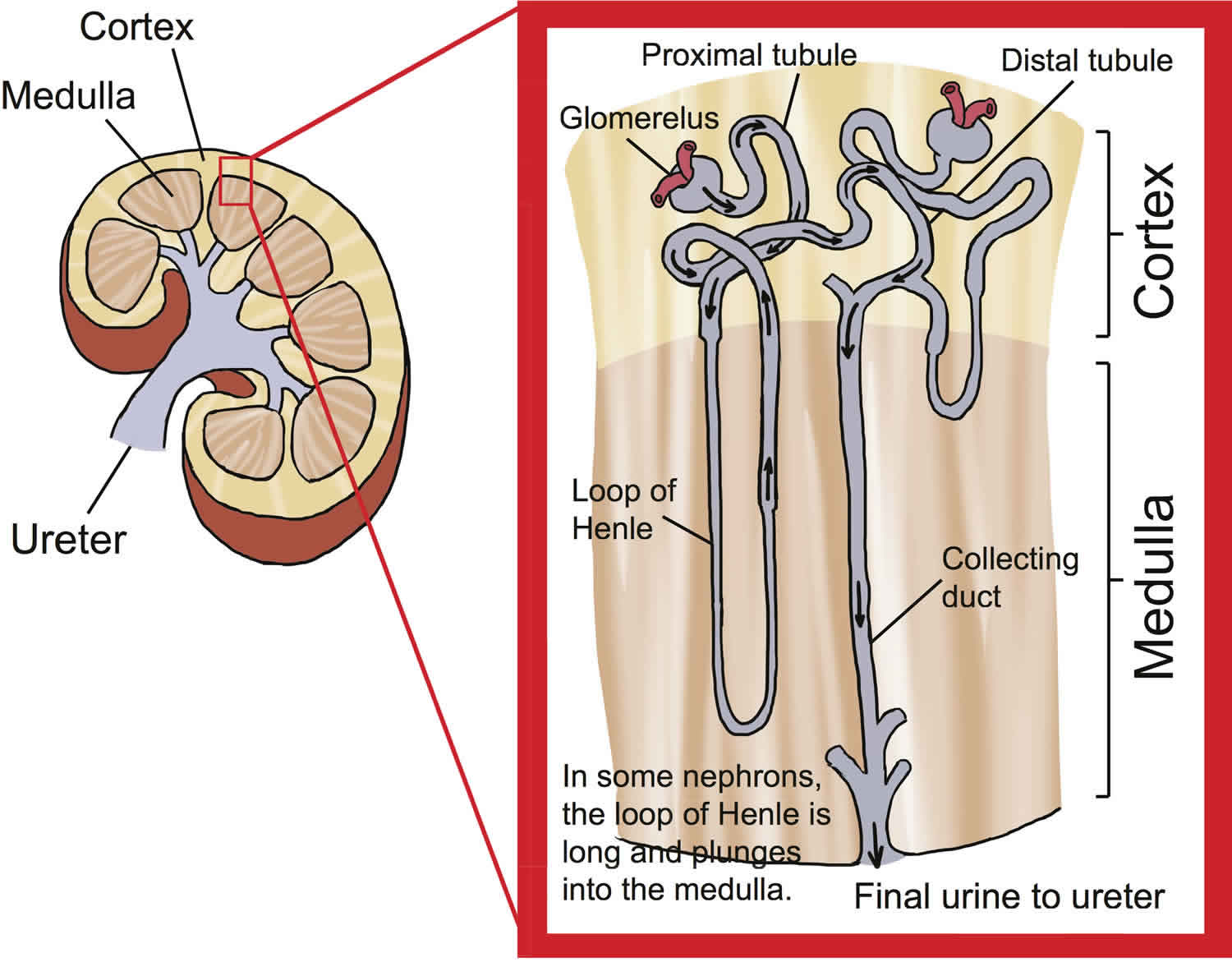
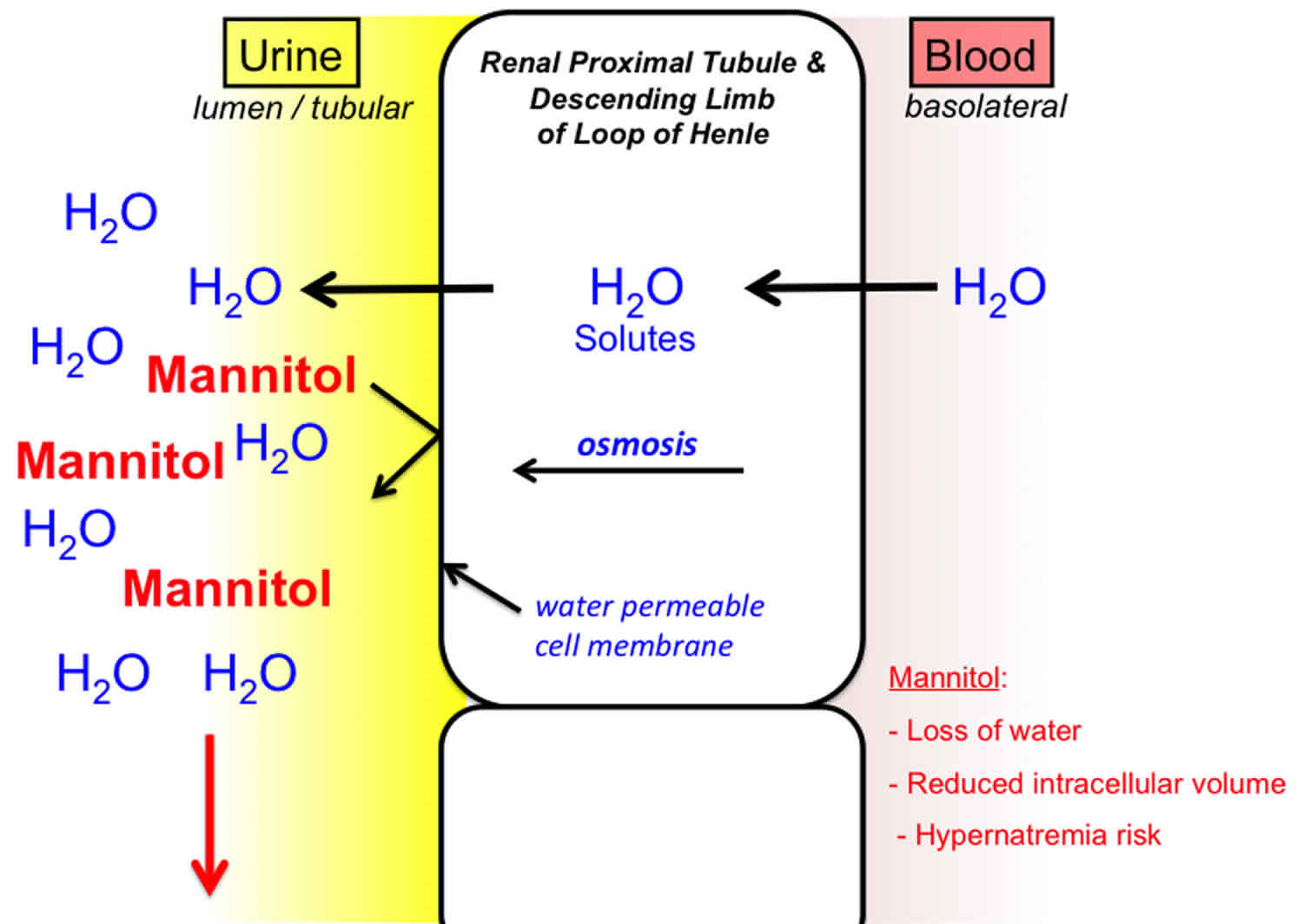
- Use of certain medicines, such as Mannitol. Mannitol is a sugar alcohol that does not cross cell membranes, and acts as an osmotic diuretic that inhibits sodium and water reabsorption in the proximal tubule, as well as the loop of Henle. Mannitol produces a greater loss of water compared to sodium and potassium. The increase in urine flow also decreases the contact time between fluid and the tubular epithelium, which reduces sodium (Na) reabsorption as well as water reabsorption. This resulting loss of sodium (Na) is of lesser magnitude than the loss of water, resulting in excessive water loss and hypernatremia.
- An osmotic diuresis may also result from excessive urea production owing to excessive protein administration.
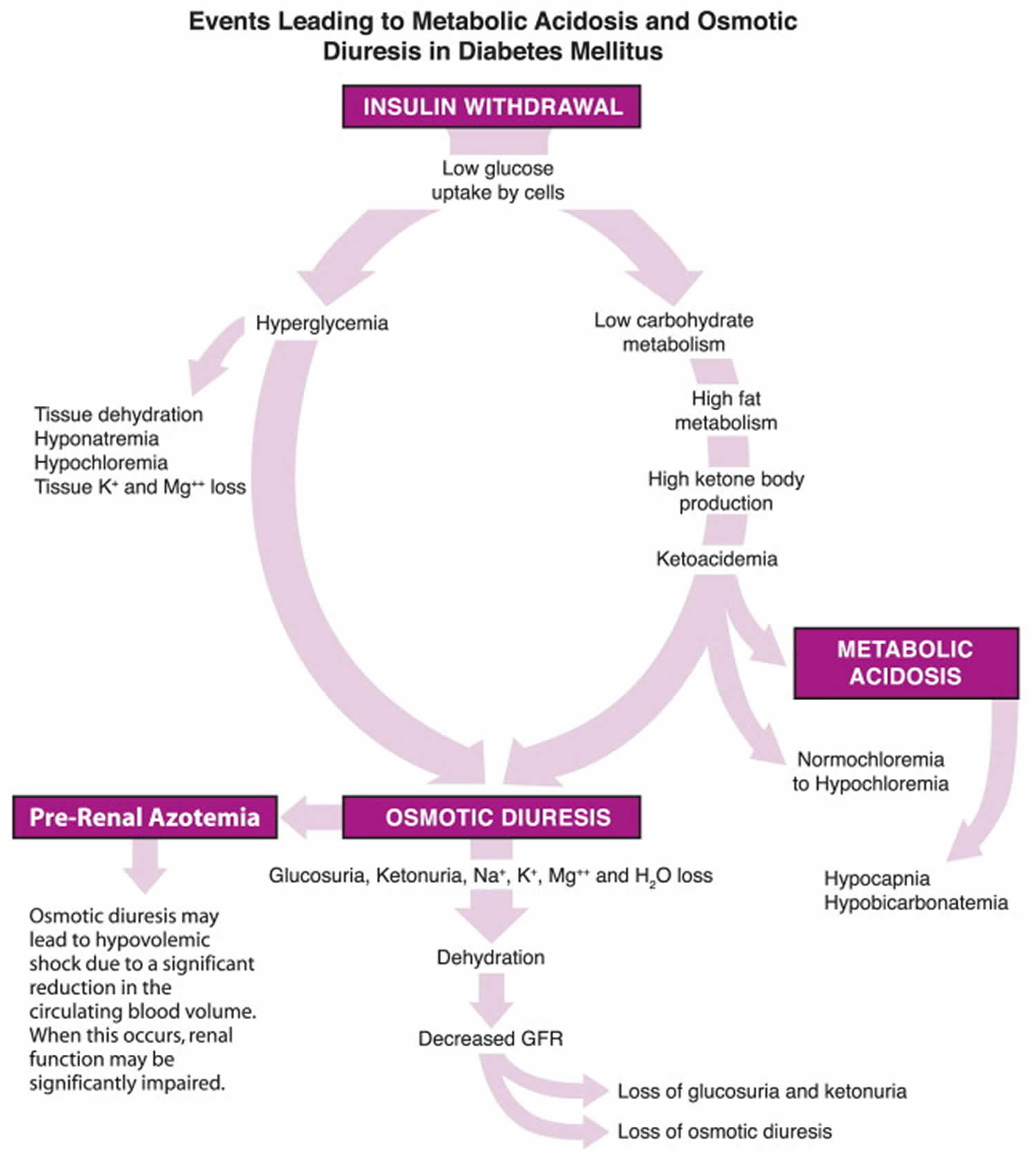
Figure 1. Osmotic diuresis in diabetes
Figure 2. Osmotic diuresis due to mannitol
Osmotic diuresis in hyperglycemia
Hyperglycemia causes osmotic diuresis that leads to hypovolemia, hyponatremia, decreased glomerular filtration rate (GFR), and worsening hyperglycemia 4. At the cellular level, increased blood glucose levels result in mitochondrial injury by generating reactive oxygen species, and endothelial dysfunction by inhibiting nitric oxide production. Hyperglycemia increases levels of pro-inflammatory cytokines such as TNF-α and IL-6 leading to immune system dysfunction. These changes can eventually lead to increased risk of infection, impaired wound healing, multiple organ failure, prolonged hospital stay and death.
- Liamis G, Liberopoulos E, Barkas F, Elisaf M. Diabetes mellitus and electrolyte disorders. World J Clin Cases. 2014;2(10):488-96. https://www.ncbi.nlm.nih.gov/pmc/articles/PMC4198400/[↩]
- Liamis G, Milionis HJ, Elisaf M. Hyponatremia in patients with infectious diseases. J Infect. 2011;63:327–335[↩]
- Waldhausl W, Kleinberger G, Korn A, Dudczak R, Bratusch-Marrain P, Nowotny P. Severe hyperglycemia: effects of rehydration on endocrine derangements and blood glucose concentration. Diabetes 1979; 28:577-584[↩]
- Corsino L, Dhatariya K, Umpierrez G. Management of Diabetes and Hyperglycemia in Hospitalized Patients. [Updated 2017 Oct 1]. In: Feingold KR, Anawalt B, Boyce A, et al., editors. Endotext [Internet]. South Dartmouth (MA): MDText.com, Inc.; 2000-. Available from: https://www.ncbi.nlm.nih.gov/books/NBK279093[↩]