Contents
- What is PSA test
- The risks of prostate screening
- How are researchers trying to improve the PSA test?
- PSA levels
- What does the PSA test result mean?
- What is a normal PSA test result?
- What if a screening test shows an elevated PSA level?
- What happens if Prostate Cancer Screening Test Results Aren’t Normal
- What is prostate gland
- What does the prostate gland do
- What is Prostate Cancer
- Benefits of Early Detection and Treatment
- Harms of Early Detection and Treatment
- United States Preventive Services Task Force Assessment
- Prostate Cancer Prevention
- Prostate Cancer Risk Factors
- How is the PSA test used in men who have been treated for prostate cancer?
- What does an increase in PSA level mean for a man who has been treated for prostate cancer?
What is PSA test
The PSA test also known as prostate-specific antigen (PSA), is a blood test used primarily to screen for prostate cancer and to help monitor prostate cancer in men. PSA (prostate-specific antigen) is a protein produced by both cancerous and noncancerous cells in the prostate, a small gland that sits below a man’s bladder. PSA is mostly found in semen, which also is produced in the prostate. Small amounts of PSA ordinarily circulate in the blood. The PSA test measures the level of PSA in a man’s blood. To determine your PSA level, a blood sample is taken from a vein in your arm at the doctor’s practice and sent to a laboratory. It can take a few days to get the test results back. The amount of PSA in the blood are usually reported as nanograms of PSA per milliliter (ng/mL) of blood. But anyone looking into the topic of PSA tests as a form of prostate cancer screening will come across conflicting information and advice. That’s because neither the pros nor the cons of the PSA test clearly outweigh each other. So the decision about whether or not to have the PSA test is a personal decision.
PSA tests for prostate cancer screening is designed to detect prostate cancer before it starts causing symptoms. Early diagnosis and treatment can improve the chances of recovery and lower the risk of the cancer spreading to other parts of the body (metastasis).
But screening has clear disadvantages: It also finds small tumors that don’t cause any problems. This is because in most men, prostate cancer grows so slowly that it doesn’t cause any problems for the rest of their lives. Men who have prostate cancer that is detected by screening are then subjected to the burdens and side effects of the diagnosis and treatment. The diagnosis of a medical condition that would never have caused any symptoms or problems is called overdiagnosis.
PSA exists in two main forms in the blood: complexed (cPSA, bound to other proteins) and free (not bound). The most frequently used PSA test is the total PSA, which measures the sum of complexed and the free PSA in the blood.
The free PSA test is sometimes used to help to determine whether a biopsy should be done when the total PSA is only slightly elevated. PSA is an enzyme (protein that helps different chemical reactions to occur) and when it is released into the blood, some circulating proteins inactivate PSA by binding to it. Benign prostate cells in benign prostatic hyperplasia (BPH) tend to release PSA that is not active (and, therefore, less likely to be bound by circulating proteins) and cancerous prostate cells tend to release PSA that is already protein-bound.
Therefore, men with benign prostatic hyperplasia (BPH) tend to have higher levels of free PSA and men with prostate cancer tend to have lower amounts of free PSA. A relatively low level of free PSA increases the chances that a cancer is present, even if the total PSA is not significantly elevated.
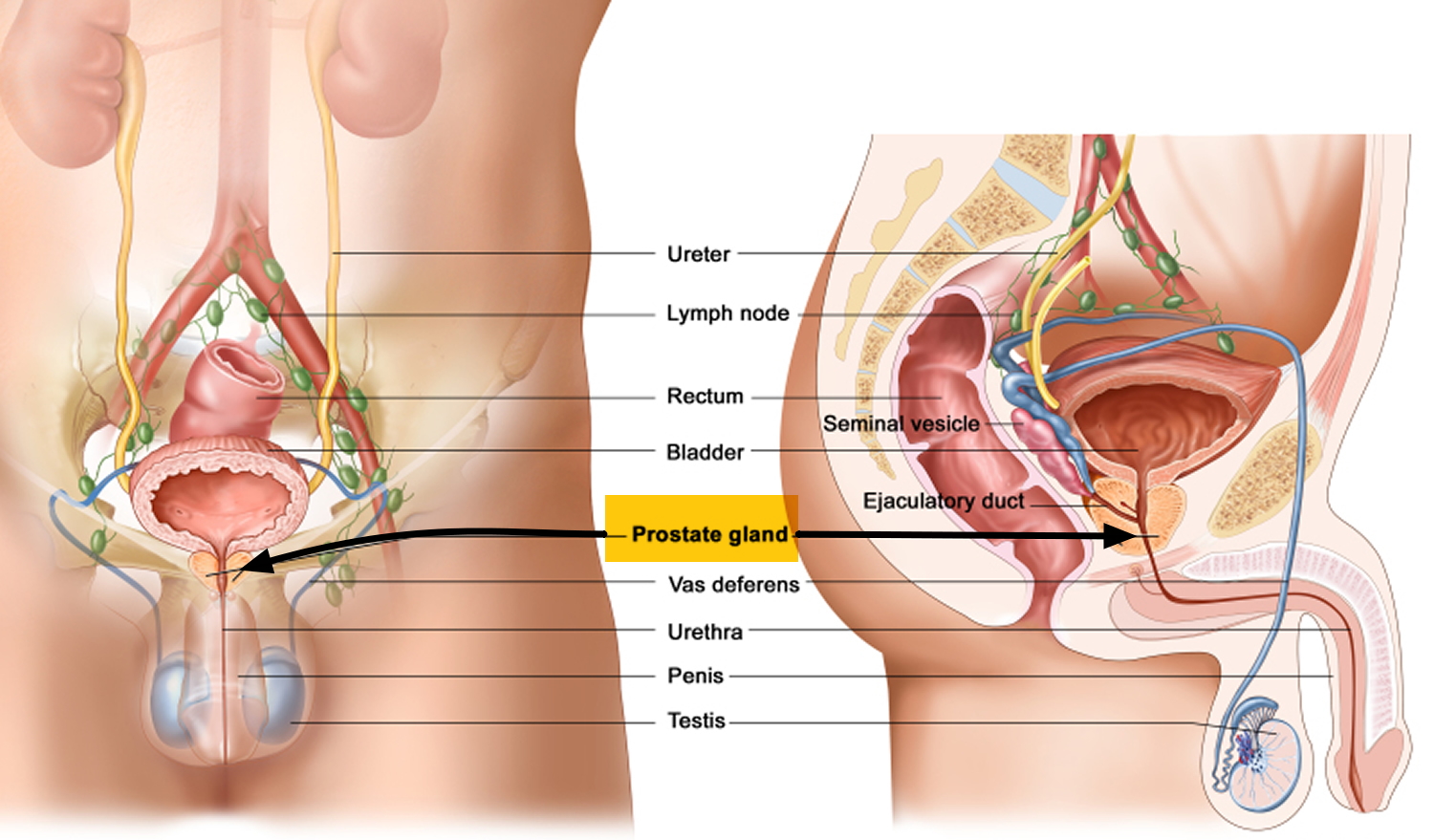
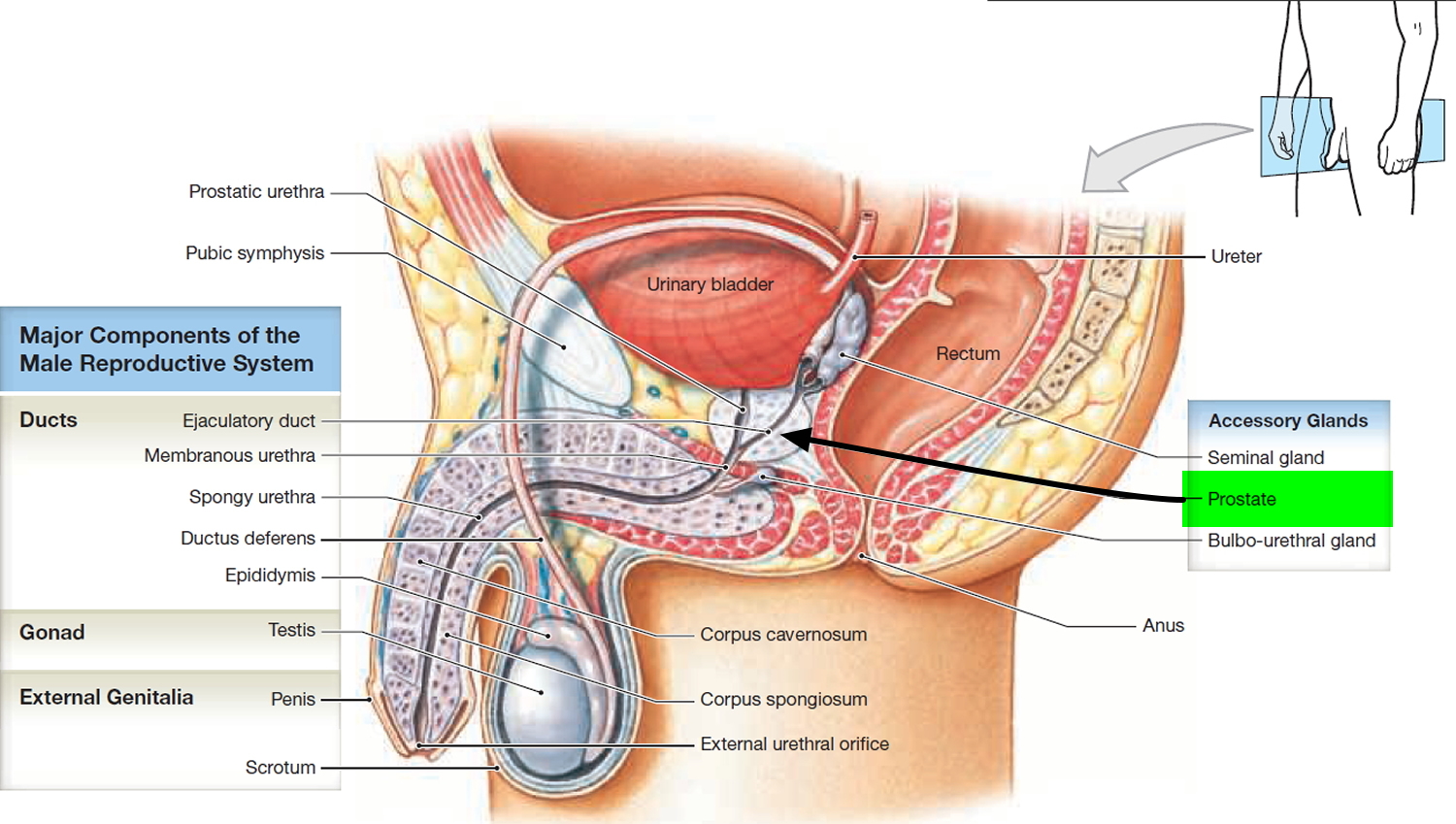
Figure 1. Prostate gland
What does the PSA level tell us?
Because the prostate gland has a very good blood supply, small amounts of PSA constantly pass into the bloodstream. PSA levels under 3 nanograms per milliliter (ng/mL) are considered to be normal, but there is a big gray area. High PSA levels can be a sign of prostate cancer, but may also be caused by many other conditions. The reason: If the prostate gland changes or is irritated, a little more PSA is automatically released into the bloodstream. For instance, high PSA levels may result from:
- an inflammation of the prostate gland (prostatitis),
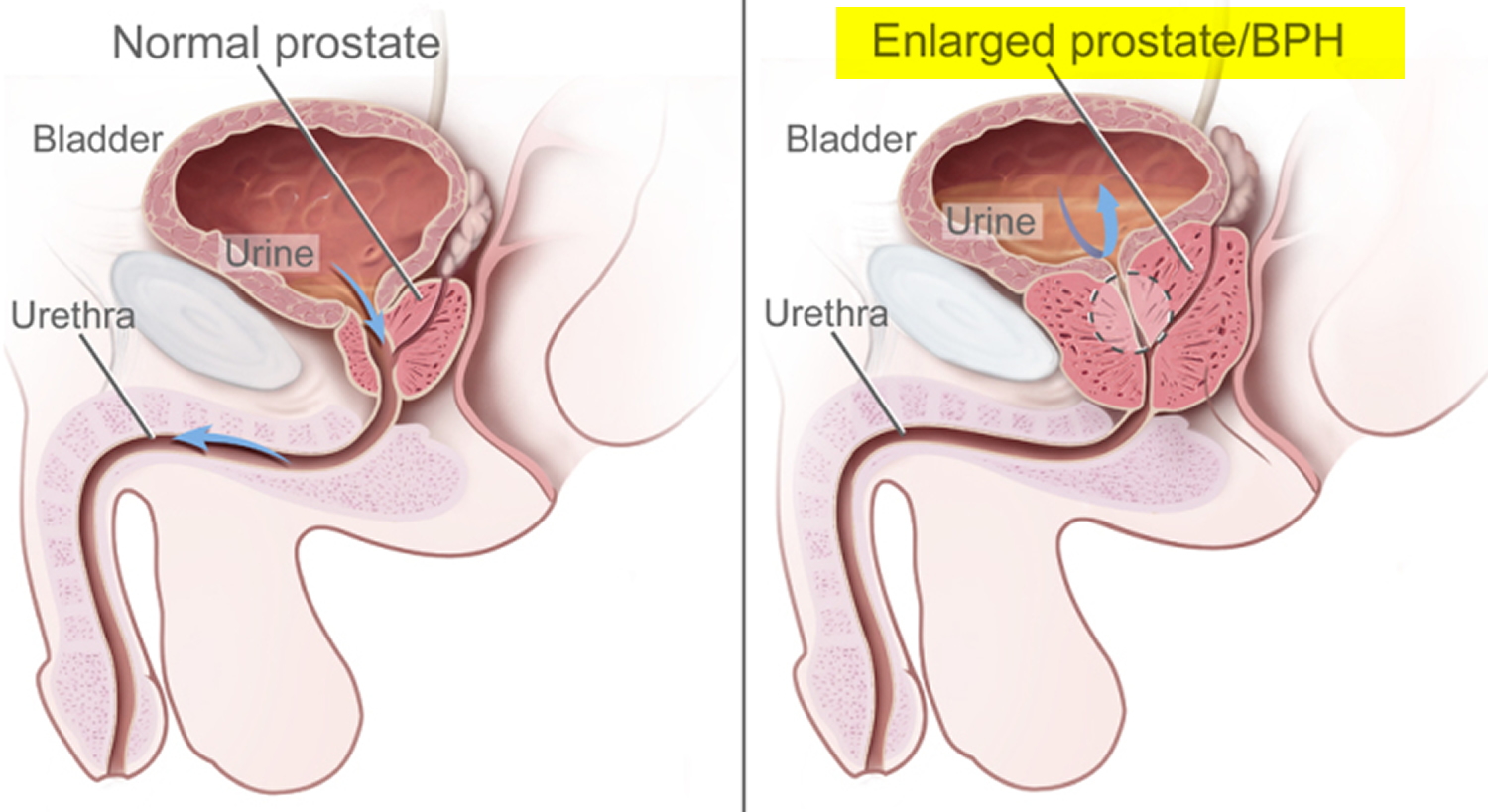
- a benign enlarged prostate (benign prostatic hyperplasia),
- a urinary tract infection (UTI),
- pressure exerted on the prostate, for example after riding a bicycle, or after examining the prostate gland by feeling it with a finger (palpation) or doing an
- ultrasound scan, or
- ejaculation.
It is a good idea to let the doctor know if any of the above have occurred so that the test results can be interpreted correctly or the test can be postponed.
But normal PSA levels do not definitely rule out cancer, either. In rare cases, men have normal PSA levels despite having cancer.
But if the PSA level is very high, for example over 10 ng/mL, it is probably due to prostate cancer. PSA levels are rarely that high, though.
What problems can arise when a tissue sample is taken?
High PSA levels can be caused by many things, so abnormal test results do not mean that you have cancer. To find out whether the high PSA levels are caused by cancer or something else, tissue samples (biopsy) are usually taken from the prostate.
This involves inserting a tube about the width of a finger into the rectum (the end part of the bowel) through the anus (bottom). From there, a fine, hollow needle is pushed into the prostate through the wall of the bowel to take several tissue samples. Ultrasound is used to check that the needle is moved to the right place. Ten to twelve samples are usually taken. Men are given antibiotics before having the procedure to prevent infections. A local anesthetic helps to prevent pain. Men often have visible blood in their urine or sperm for several days after the biopsy. About 40 out of 1,000 men have a fever for a while. About 10 out of 1,000 men end up going to the hospital to get treatment for an infection with a fever following a biopsy.
The PSA test is a good tool but not a perfect one, and most experts agree that screening should be done on asymptomatic men only after thorough discussions with their healthcare providers on the benefits and risks and after informed decisions are made to undergo screening. Elevated levels of PSA are associated with prostate cancer, but they may also be seen with prostatitis and benign prostatic hyperplasia (BPH). PSA levels tend to increase in all men as they age, and men of African American heritage may have levels that are higher than other men, even at earlier ages. Therefore, determining what a high PSA score means can be complicated.
The PSA test in numbers: What results can be expected?
The data from the major European study 1 can be used to get a rough idea of what can be expected from PSA screening.
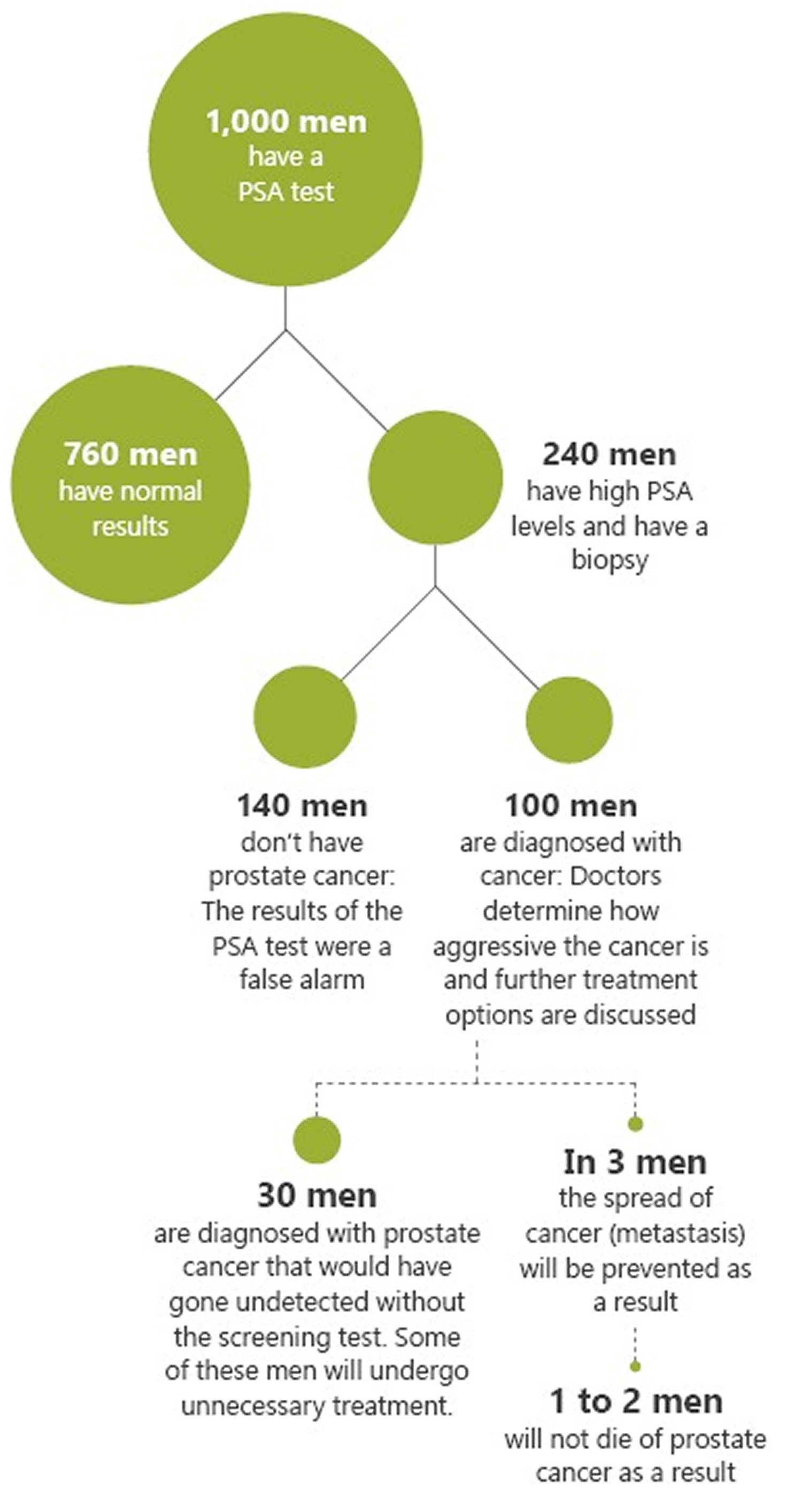
If 1,000 men between the ages of 55 and 69 regularly have PSA screening tests over a time period of 13 years, the following results can be expected:
- About 760 men will have normal results.
- About 240 men will have a high PSA level. Most of these men will then have tissue samples taken from their prostate to check the organ for cancer cells.
- In about 140 of these men, the biopsy will not find any prostate cancer. The PSA test will have been a false alarm.
- In about 100 men with abnormal PSA levels, cancerous cells will be found. Depending on how large and aggressive the cancer is, various treatments may be considered: common ones include “active surveillance,” radiotherapy or surgery.
How great are the benefits and risks of PSA screening?
- If 1,000 men participate in the PSA screening program, about 1 to 2 deaths from prostate cancer will be prevented.
- The spread of the cancer to other parts of the body (metastasis) will be prevented in about 3 out of 1,000 men.
- But the test will also detect tumors and cell changes that would never have caused any problems. This kind of “overdiagnosis” is estimated to occur in about 30 out of 1,000 men who take part in this screening program, and they may receive unnecessary treatment as a result.
Figure 3 shows the pros and cons of PSA screening at a glance. These numbers are estimates. On the one hand, different PSA cut-off levels are recommended in Germany. Also, the men in the study were observed for only 13 years on average afterwards. A longer observation period could lead to different results.
Whether a man finds that the possible advantages of PSA screening tests outweigh the possible drawbacks will depend on his personal situation and preferences. You can take your time when deciding whether or not to have the test. There are good reasons both for and against having PSA screening tests, so no man should feel pressured into having the PSA test.
Figure 3. PSA screening test pros and cons
Some organizations, such as the U.S. Preventive Services Task Force 2, feel that the harms associated with over-diagnosis and over-treatment outweigh the potential benefits and advise against using PSA to screen for prostate cancer in healthy men of any age. The American Cancer Society 3 and the American Urological Association 4 recommend that men discuss the advantages and disadvantages of PSA-based screening for prostate cancer with their healthcare provider before making an informed decision about whether to be screened or not.
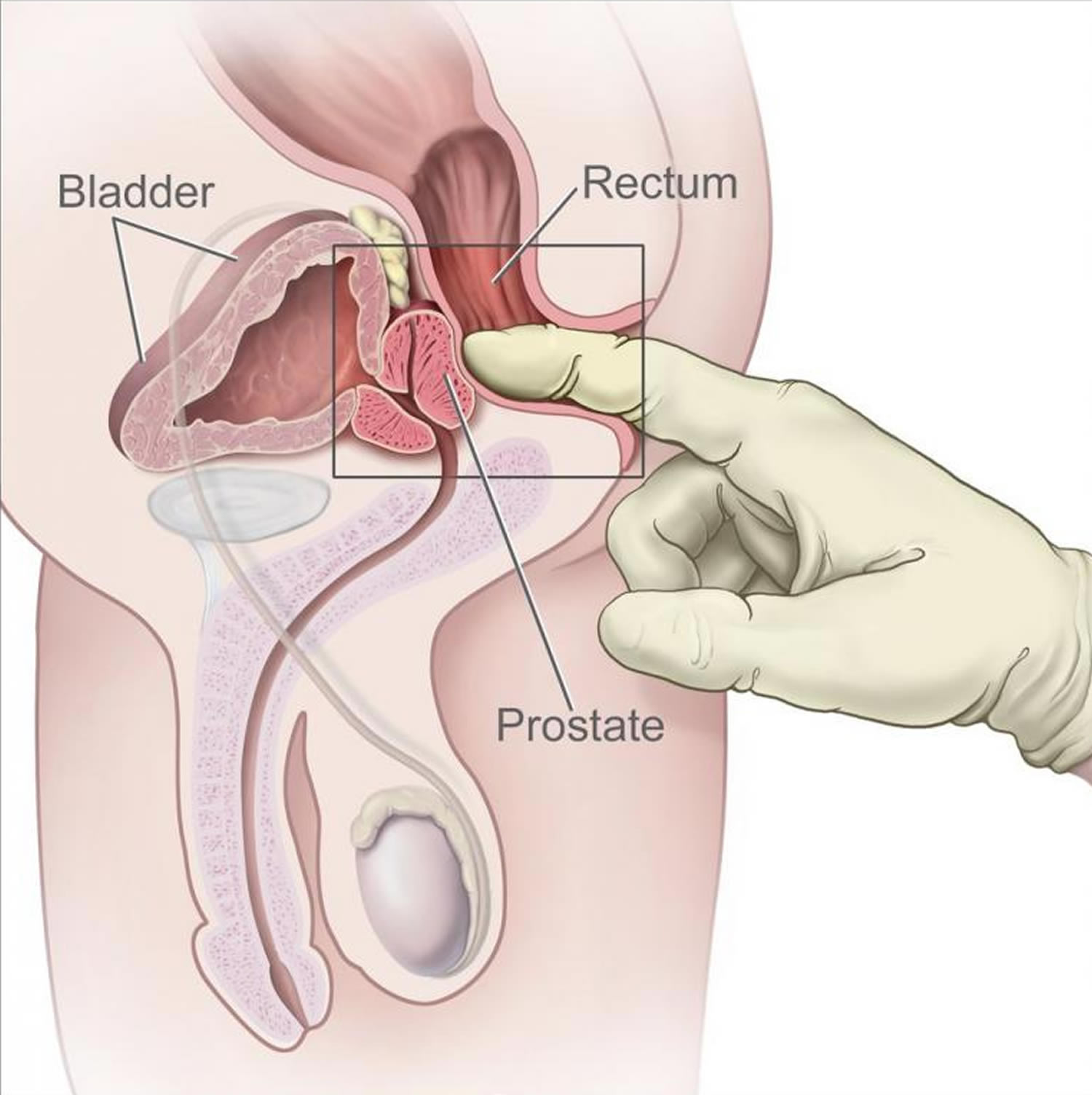
Prostate cancer can often be found early by testing for prostate-specific antigen (PSA) levels in a man’s blood. Another way to find prostate cancer early is the digital rectal exam (DRE), in which the doctor puts a gloved, lubricated finger into the rectum to feel the prostate gland. Digital rectal exam is less effective than the PSA blood test in finding prostate cancer, but it can sometimes find cancers in men with normal PSA levels. For this reason, it may be included as a part of prostate cancer screening.
- PSA is not diagnostic of cancer. The gold standard for identifying prostate cancer is the prostate biopsy, collecting small samples of prostate tissue and identifying abnormal cells under the microscope. Prostate biopsy involves inserting a tube about the width of a finger into the rectum (the end part of the bowel) through the anus (bottom). From there, a fine, hollow needle is pushed into the prostate through the wall of the bowel to take several tissue samples. Ultrasound is used to check that the needle is moved to the right place. Ten to twelve samples are usually taken. Men are given antibiotics before having the procedure to prevent infections. A local anesthetic helps to prevent pain. Men often have visible blood in their urine or sperm for several days after the biopsy. About 40 out of 1,000 men have a fever for a while. About 10 out of 1,000 men end up going to the hospital to get treatment for an infection with a fever following a biopsy.
- When is a biopsy recommended? Opinions vary about which PSA levels mean that a biopsy should be recommended. The medical societies in Germany agree that a prostate biopsy is a good idea if:
- the PSA levels are higher than 4 nanograms per milliliter (ng/mL) and a second test shows the same results, or
- the PSA levels increase considerably over several measurements.
- When is a biopsy recommended? Opinions vary about which PSA levels mean that a biopsy should be recommended. The medical societies in Germany agree that a prostate biopsy is a good idea if:
- Although prostate cancer is a relatively common type of cancer in men and the number two cause of death, many prostate cancers are slow-growing. These slow-growing types may never cause symptoms or become life-threatening. Yet prostate cancer found through screening may be treated with surgery or radiation therapy, which can have serious side effects, such as incontinence or erectile dysfunction.
- The total PSA test can be elevated temporarily for a variety of reasons, so if an initial PSA is elevated, another PSA may be done a few weeks after the first to determine if the PSA is still elevated. If the repeat test is elevated, a healthcare provider may recommend that series of PSAs be done over time to determine whether the level goes down, stays elevated, or continues to increase. In cases where the cancer appears to be slow-growing, the healthcare provider and patient may decide to monitor its progress rather than pursue immediate treatment (called “watchful waiting”).
- If the digital rectal exam (DRE) is normal but the PSA is moderately elevated, a free PSA test may be used to look at the ratio of free to total PSA. This can help to distinguish between prostate cancer and other non-cancer causes of elevated PSA.
- Other tests may also be recommended if either the PSA or the digital rectal exam (DRE) is found to be abnormal. A urinalysis may be done, for example, to check for urinary tract infection and imaging tests, such as an ultrasound, may be done to examine the prostate.
- A prostate cancer gene 3 (PCA3) RNA test may be used for certain patients. If a man had a high PSA level and a biopsy of the prostate did not show cancer and the PSA level remains high after the biopsy, a prostate cancer gene 3 (PCA3) RNA test may be done. This test measures the amount of PCA3 RNA in the urine after a DRE. If the PCA3 RNA level is higher than normal, another biopsy may help diagnose prostate cancer.
- If prostate cancer is diagnosed, the total PSA test may be used as a monitoring tool to help determine the effectiveness of treatment. It may also be ordered at regular intervals after treatment to detect recurrence of the cancer.
There is no unanimous opinion in the medical community regarding the benefits of prostate cancer screening using PSA testing.
- Those who advocate regular screening believe that finding prostate cancer early offers men a better chance to cure the disease if your cancer warrants treatment. It also may inform you that you don’t need your prostate cancer treated.
- Those who recommend against regular screening note that because most prostate cancers grow very slowly, the side effects of diagnosis (a prostate biopsy) and treatment would likely outweigh any benefit that might be derived from detecting the cancer at a stage when it is unlikely to cause problems.
Prostate cancer can often be found early using a simple PSA blood test, but it’s not clear if the benefits of PSA testing for all men for prostate cancer outweigh the risks, such as finding (and treating) cancers that probably never would have caused any problems. Because of this, it’s important to talk to a health care provider about the uncertainties, risks, and potential benefits of prostate cancer screening before deciding whether or not to be tested. To decide whether to have a PSA test, you have to discuss this issue with your doctor, considering your risk factors and weighing your personal preferences.
Recent studies of screening in large U.S. and European populations have suggested that the benefits of screening may not occur for 10 or more years after screening, given the long natural history of prostate cancer. These studies also suggest that a large number of men will need to be screened (over 1,000) and treated (nearly 50) to save one life from prostate cancer. PSA screening increased the number of prostate cancer cases diagnoses each year in the USA, and most of these new cases are non-aggressive or low risk prostate cancer. Very few men will die of these less aggressive forms of prostate cancer in the first decade after diagnosis.
Several randomized trials of prostate cancer screening have been carried out. One of the largest is the Prostate, Lung, Colorectal, and Ovarian Cancer Screening Trial, which the National Cancer Institute conducted to determine whether certain screening tests can help reduce the numbers of deaths from several common cancers. In the prostate portion of the trial, the PSA test and digital rectal exam (DRE) were evaluated for their ability to decrease a man’s chances of dying from prostate cancer.
The Prostate, Lung, Colorectal, and Ovarian investigators 5 found that men who underwent annual prostate cancer screening had a higher incidence of prostate cancer than men in the control group but the same rate of deaths from the disease. Overall, the results suggest that many men were treated for prostate cancers that would not have been detected in their lifetime without screening. Consequently, these men were exposed unnecessarily to the potential harms of treatment.
A second large trial, the European Randomized Study of Screening for Prostate Cancer 6, 7, compared prostate cancer deaths in men randomly assigned to PSA-based screening or no screening. As in the Prostate, Lung, Colorectal, and Ovarian, men in European Randomized Study of Screening for Prostate Cancer who were screened for prostate cancer had a higher incidence of the disease than control men. In contrast to the Prostate, Lung, Colorectal, and Ovarian, however, men who were screened had a lower rate of death from prostate cancer 7, 6.
A recent paper analyzed data from the Prostate, Lung, Colorectal, and Ovarian Trial using a complicated statistical model to account for the fact that some men in the Prostate, Lung, Colorectal, and Ovarian trial who were assigned to the control group had nevertheless undergone PSA screening. This analysis suggested that the level of benefit in the Prostate, Lung, Colorectal, and Ovarian and European Randomized Study of Screening for Prostate Cancer trials were similar and that both trials were consistent with some reduction in prostate cancer death in association with prostate cancer screening 8. Such statistical modeling studies have important limitations and rely on unverified assumptions that can render their findings questionable (or more suitable for further study than to serve as a basis for screening guidelines). More importantly, the model could not provide an assessment of the balance of benefits versus harms from screening.
The United States Preventive Services Task Force has analyzed the data from all reported prostate cancer screening trials, principally from the Prostate, Lung, Colorectal, and Ovarian and European Randomized Study of Screening for Prostate Cancer trials, and estimated that, for every 1,000 men ages 55 to 69 years who are screened every 1 to 4 years for 10 to 15 years 9:
- About 1 death from prostate cancer would be avoided
- 120 men would have a false-positive test result that leads to a biopsy, and some men who get a biopsy would experience at least moderately bothersome symptoms from the biopsy
- 100 men would be diagnosed with prostate cancer. Of those, 80 would be treated (either immediately or after a period of active surveillance) with surgery or radiation. At least 60 of these men would have a serious complication from treatment, such as erectile dysfunction and/or urinary incontinence.
Figure 4. Digital rectal exam
The U.S. Preventative Task Force Final Recommendation regarding Prostate Cancer Screening 2:
Men aged 55 to 69 years
For men aged 55 to 69 years, the decision to undergo periodic prostate-specific antigen (PSA)–based screening for prostate cancer should be an individual one. Before deciding whether to be screened, men should have an opportunity to discuss the potential benefits and harms of screening with their clinician and to incorporate their values and preferences in the decision. Screening offers a small potential benefit of reducing the chance of death from prostate cancer in some men. However, many men will experience potential harms of screening, including false-positive results that require additional testing and possible prostate biopsy; overdiagnosis and overtreatment; and treatment complications, such as incontinence and erectile dysfunction. In determining whether this service is appropriate in individual cases, patients and clinicians should consider the balance of benefits and harms on the basis of family history, race/ethnicity, comorbid medical conditions, patient values about the benefits and harms of screening and treatment-specific outcomes, and other health needs. Clinicians should not screen men who do not express a preference for screening.
Men 70 years and older
The U.S. Preventative Task Force recommends against PSA-based screening for prostate cancer in men 70 years and older.
The American Academy of Family Physicians 10 and the Canadian Task Force on Preventive Health Care 11 recommend against PSA-based screening for prostate cancer. The American College of Physicians 12 recommends that clinicians discuss the benefits and harms of screening with men aged 50 to 69 years and only recommends screening for men who prioritize screening and have a life expectancy of more than 10 to 15 years. The American Urological Association 4 recommends that men aged 55 to 69 years with a life expectancy of more than 10 to 15 years be informed of the benefits and harms of screening and engage in shared decision making with their clinicians, taking into account each man’s values and preferences. It notes that to reduce the harms of screening, the screening interval should be 2 or more years. The American Urological Association also notes that decisions about screening, including potentially starting screening before age 55 years, should be individual ones for African American men and men with a family history of prostate cancer. The American Cancer Society 3 recommends that men thinking about getting screened for prostate cancer should make informed decisions based on available information, discussion with their doctor, and their own views on the possible benefits, risks, and limits of prostate cancer screening. The American Cancer Society also adopted detailed screening recommendations in 2016 that highlight the importance of shared decision making and the need for informed discussion of the uncertainties, risks, and potential benefits of screening. It recommends conversations about screening beginning at age 50 years and earlier for African American men and men with a father or brother with a history of prostate cancer before age 65 years.
- It should be noted that these recommendations apply to screening only, i.e. testing of healthy men without symptoms. Once the diagnosis of prostate cancer is confirmed by biopsy, PSA is still routinely recommended and used for risk-assessment and post-treatment monitoring.
- Most experts agree that there is no role for PSA screening for men expected to live less than 10 years. Ultimately, decisions about screening should be individualized based on a man’s level of risk, overall health, and life expectancy, as well as his desire for eventual treatment if he is diagnosed with prostate cancer.
American Cancer Society Recommendations for Prostate Cancer Early Detection
The American Cancer Society recommends that men have a chance to make an informed decision with their health care provider about whether to be screened for prostate cancer. The decision should be made after getting information about the uncertainties, risks, and potential benefits of prostate cancer screening. Men should not be screened unless they have received this information. The discussion about screening should take place at:
- Age 50 for men who are at average risk of prostate cancer and are expected to live at least 10 more years.
- Age 45 for men at high risk of developing prostate cancer. This includes African Americans and men who have a first-degree relative (father, brother, or son) diagnosed with prostate cancer at an early age (younger than age 65).
- Age 40 for men at even higher risk (those with more than one first-degree relative who had prostate cancer at an early age).
After this discussion, men who want to be screened should be tested with the prostate-specific antigen (PSA) blood test. The digital rectal exam (DRE) may also be done as a part of screening.
If, after this discussion, a man is unable to decide if testing is right for him, the screening decision can be made by the health care provider, who should take into account the man’s general health preferences and values.
If no prostate cancer is found as a result of screening, the time between future screenings depends on the results of the PSA blood test:
- Men who choose to be tested who have a PSA of less than 2.5 ng/mL may only need to be retested every 2 years.
- Screening should be done yearly for men whose PSA level is 2.5 ng/mL or higher.
Because prostate cancer often grows slowly, men without symptoms of prostate cancer who do not have a 10-year life expectancy should not be offered testing since they are not likely to benefit. Overall health status, and not age alone, is important when making decisions about screening.
Even after a decision about testing has been made, the discussion about the pros and cons of testing should be repeated as new information about the benefits and risks of testing becomes available. Further discussions are also needed to take into account changes in a man’s health, values, and preferences.
The risks of prostate screening
The risks of prostate screening include the following:
- Finding prostate cancer may not improve health or help a man live longer.
Screening may not improve your health or help you live longer if you have cancer that has already spread to the area outside of the prostate or to other places in your body.
Some cancers never cause symptoms or become life-threatening, but if found by a screening test, the cancer may be treated. Finding these cancers is called overdiagnosis. It is not known if treatment of these cancers would help you live longer than if no treatment were given.
Treatments for prostate cancer, such as radical prostatectomy and radiation therapy, may have long-term side effects in many men. The most common side effects are erectile dysfunction and urinary incontinence.
Some studies of patients with newly diagnosed prostate cancer showed these patients had a higher risk of death from cardiovascular (heart and blood vessel) disease or suicide. The risk was greatest in the first weeks or months after diagnosis.
Follow-up tests, such as a biopsy, may be done to diagnose cancer.
If a PSA test is higher than normal, a biopsy of the prostate may be done. Complications from a biopsy of the prostate may include fever, pain, blood in the urine or semen, and urinary tract infection. Even if a biopsy shows that a patient does not have prostate cancer, he may worry more about developing prostate cancer in the future.
False-negative test results can occur.
Screening test results may appear to be normal even though prostate cancer is present. A man who receives a false-negative test result (one that shows there is no cancer when there really is) may delay seeking medical care even if he has symptoms.
False-positive test results can occur.
Screening test results may appear to be abnormal even though no cancer is present. A false-positive test result (one that shows there is cancer when there really isn’t) can cause anxiety and is usually followed by more tests, (such as biopsy) which also have risks.
Your doctor can advise you about your risk for prostate cancer and your need for screening tests.
Is any PSA test preparation needed to ensure the quality of the sample?
Ejaculation should be avoided for 24 hours before sample collection, as it has been associated with elevated PSA levels. The sample should also be collected prior to the health practitioner performing a digital rectal exam (DRE) and prior to (or several weeks after) a prostate biopsy, as both of these can also elevate PSA levels.
Since the DRE can cause a temporary elevation in PSA, the blood sample is usually collected prior to performing the DRE.
Prostate manipulation by biopsy or resection of the prostate will significantly elevate PSA levels. The blood test should be done before surgery or six weeks after manipulation.
Rigorous physical activity affecting the prostate, such as bicycle riding, may cause a temporary rise in PSA level. Ejaculation within 24 hours of testing can be associated with elevated PSA levels and should be avoided.
Large doses of some chemotherapeutic drugs, such as cyclophosphamide and methotrexate, may increase or decrease PSA levels.
In some men, PSA may rise temporarily due to other prostate conditions, especially infection. A study found that in about half of men with a high PSA, values later return to normal. Some authorities recommend that a high PSA should be repeated, between 6 weeks and 3 months after the high PSA, before taking any further action. Some health practitioners will prescribe a course of antibiotics if there is evidence that there is infection of the prostate.
Fasting time and serum PSA levels
The results of this study 13 indicate that fasting time has a statistically significant effect on serum PSA levels, and an increased fasting time is generally associated with a modest increase in the number of patients with abnormal PSA values, particularly at the extremes. The peak PSA levels were observed at 4 hour of fasting, which may be due to diurnal variation. Simulating the changes that would occur in PSA values if fasting times were altered revealed that the percentage change in the number of abnormal PSA values can range from −1.07% to 1.63%, which would translate into minimal clinical effect. Lau rt al. 14 recommend that the optimal time to obtain an accurate PSA level is fasting for 7–9 hours, which avoids the increased PSA levels observed with fasting extremes as well as possible diurnal rhythm variations that may exist in shorter fasting times.
When is PSA test ordered?
For men who wish to be screened for prostate cancer, the American Cancer Society recommends that healthy men of average risk consider waiting to get tested until age 50, while the American Urological Association recommends screening for men between the ages of 55 and 69 with no routine screening after age 70.
For those at high risk, such as American men of African descent and men with a family history of the disease, the recommendation is to consider beginning testing at age 40 or 45. (See Screening Tests for Adults (30-49): Prostate cancer and Screening Tests for Adults (50 and Up): Prostate cancer for details on screening recommendations.)
The total PSA test and digital rectal exam (DRE) may also be ordered when a man has symptoms that could be due to prostate cancer, such as difficult, painful, and/or frequent urination, back pain, and/or pelvic pain.
If a total PSA level is elevated, a healthcare provider may order a repeat test a few weeks later to determine whether the PSA concentrations have returned to normal.
A free PSA is primarily ordered when a man has a moderately elevated total PSA. The results give the healthcare provider additional information about whether the person is at an increased risk of having prostate cancer and help with the decision of whether to biopsy the prostate.
The total PSA may be ordered at regular intervals during treatment of men who have been diagnosed with prostate cancer and when a man with cancer is participating in “watchful waiting” and not currently treating his prostate cancer.
What are some of the limitations and potential harms of the PSA test for prostate cancer screening?
Detecting prostate cancer early may not reduce the chance of dying from prostate cancer. When used in screening, the PSA test can help detect small tumors that do not cause symptoms. Finding a small tumor, however, may not necessarily reduce a man’s chance of dying from prostate cancer. Many tumors found through PSA testing grow so slowly that they are unlikely to threaten a man’s life. Detecting tumors that are not life threatening is called “overdiagnosis,” and treating these tumors is called “overtreatment.”
Overtreatment exposes men unnecessarily to the potential complications and harmful side effects of treatments for early prostate cancer, including surgery and radiation therapy. The side effects of these treatments include urinary incontinence (inability to control urine flow), problems with bowel function, erectile dysfunction (loss of erections, or having erections that are inadequate for sexual intercourse), and infection.
In addition, finding cancer early may not help a man who has a fast-growing or aggressive tumor that may have spread to other parts of the body before being detected.
The PSA test may give false-positive or false-negative results. A false-positive test result occurs when a man’s PSA level is elevated but no cancer is actually present. A false-positive test result may create anxiety for a man and his family and lead to additional medical procedures, such as a prostate biopsy, that can be harmful. Possible side effects of biopsies include serious infections, pain, and bleeding.
Most men with an elevated PSA level turn out not to have prostate cancer; only about 25% of men who have a prostate biopsy due to an elevated PSA level actually are found to have prostate cancer when a biopsy is done 15.
A false-negative test result occurs when a man’s PSA level is low even though he actually has prostate cancer. False-negative test results may give a man, his family, and his doctor false assurance that he does not have cancer, when he may in fact have a cancer that requires treatment.
How are researchers trying to improve the PSA test?
Scientists are investigating ways to improve the PSA test to give doctors the ability to better distinguish cancerous from benign conditions and slow-growing cancers from fast-growing, potentially lethal cancers. Some doctors might consider using different types of PSA tests to help decide if you need a prostate biopsy, but not all doctors agree on how to use these other PSA tests. If your PSA test result isn’t normal, ask your doctor to discuss your cancer risk and your need for further tests. None has been proven to decrease the risk of death from prostate cancer. Some of the methods being studied include:
Percent-free PSA
PSA occurs in 2 major forms in the blood. One form is attached to blood proteins, while the other circulates free (unattached). The percent-free PSA (fPSA) is the ratio of how much PSA circulates free compared to the total PSA level. The percentage of free PSA is lower in men who have prostate cancer than in men who do not.
This test is sometimes used to help decide if you should have a prostate biopsy if your PSA results are in the borderline range (like between 4 and 10). A lower percent-free PSA means that your chance of having prostate cancer is higher and you should probably have a biopsy.
Many doctors recommend biopsies for men whose percent-free PSA is 10% or less, and advise that men consider a biopsy if it is between 10% and 25%. Using these cutoffs detects most cancers and helps some men avoid unnecessary prostate biopsies. This test is widely used, but not all doctors agree that 25% is the best cutoff point to decide on a biopsy, and the cutoff may change depending on the overall PSA level.
Complexed PSA
This test directly measures the amount of PSA that is attached to other proteins (the portion of PSA that is not “free”). This test could be done instead of checking the total and free PSA, and it could give the same amount of information as the other tests done separately. This test is being studied to see if it provides the same level of accuracy.
Tests that combine different types of PSA
Some newer tests, such as the prostate health index (phi) and the 4Kscore test, combine the results of different types of PSA to get an overall score that reflects the chance a man has prostate cancer. These tests might be useful in men with a slightly elevated PSA, to help determine if they should have a prostate biopsy. Some tests might be used to help determine if a man who has already had a prostate biopsy that didn’t find cancer should have another biopsy.
PSA velocity
The PSA velocity is not a separate test. It is a measure of how fast the PSA rises over time. Normally, PSA levels go up slowly with age. Some research has found that these levels go up faster if a man has cancer, but studies have not shown that the PSA velocity is more helpful than the PSA level itself in finding prostate cancer. For this reason, the American Cancer Society guidelines do not recommend using the PSA velocity as part of screening for prostate cancer.
PSA density
PSA levels are higher in men with larger prostate glands. The PSA density is sometimes used for men with large prostate glands to try to adjust for this. The doctor measures the volume (size) of the prostate gland with transrectal ultrasound and divides the PSA number by the prostate volume. A higher PSA density indicates a greater likelihood of cancer. PSA density has not been shown to be as useful as the percent-free PSA test.
Age-specific PSA ranges
PSA levels are normally higher in older men than in younger men, even when there is no cancer. A PSA result within the borderline range might be very worrisome in a 50-year-old man but cause less concern in an 80-year-old man. For this reason, some doctors have suggested comparing PSA results with results from other men of the same age.
But because the usefulness of age-specific PSA ranges is not well proven, most doctors and professional organizations (as well as the makers of the PSA tests) do not recommend their use at this time.
Pro-PSA
Pro-PSA refers to several different inactive precursors of PSA. There is some evidence that pro-PSA is more strongly associated with prostate cancer than with BPH. One recently approved test combines measurement of a form of pro-PSA called [-2]proPSA with measurements of PSA and free PSA. The resulting “prostate health index” can be used to help a man with a PSA level of between 4 and 10 ng/mL decide whether he should have a biopsy.
IsoPSA
PSA exists in different structural forms (called isoforms) in the blood. The IsoPSA test, which measures the entire spectrum of PSA isoforms rather than the concentration of PSA in the blood, may improve the selection of men with prostate cancer for biopsy 16.
PSA in combination with other protein biomarkers
Tests that combine measurements of PSA in blood with measurements of other biomarkers linked to prostate cancer in blood or urine are being studied for their ability to distinguish high-risk disease. These other biomarkers include kallikrein-related peptidase 2, prostate cancer antigen 3 (PCA3), and the TMPRSS2-ERG gene fusion.
PSA levels
Most men without prostate cancer have PSA levels under 4 nanograms per milliliter (ng/mL) of blood. The chance of having prostate cancer goes up as the PSA level goes up.
When prostate cancer develops, the PSA level usually goes above 4. Still, a level below 4 does not guarantee that a man doesn’t have cancer. About 15% of men with a PSA below 4 will have prostate cancer on a biopsy.
Men with a PSA level between 4 and 10 have about a 1 in 4 chance of having prostate cancer. If the PSA is more than 10, the chance of having prostate cancer is over 50%.
If your PSA level is high, your doctor may advise either waiting a while and repeating the test, or getting a prostate biopsy to find out if you have cancer. When considering whether to do a prostate biopsy to look for cancer, not all doctors use the same PSA cutoff point. Some may advise it if the PSA is 4 or higher, while others might recommend it starting at a lower level, such as 2.5 or 3. Other factors, such as your age, race, and family history, may affect this decision.
Factors that might affect PSA levels
A number of factors other than prostate cancer can also raise PSA levels:
- An enlarged prostate: Conditions such as benign prostatic hyperplasia (BPH), a non-cancerous enlargement of the prostate that affects many men as they grow older, can raise PSA levels.
- Older age: PSA levels normally go up slowly as you get older, even if you have no prostate abnormality.
- Prostatitis: This term refers to infection or inflammation of the prostate gland, which can raise PSA levels.
- Ejaculation: This can make the PSA go up for a short time, and then go down again. This is why some doctors suggest that men abstain from ejaculation for a day or two before testing.
- Riding a bicycle: Some studies have suggested that cycling may raise PSA levels (possibly because the seat puts pressure on the prostate), although not all studies have found this.
- Certain urologic procedures: Some procedures done in a doctor’s office that affect the prostate, such as a prostate biopsy or cystoscopy, can result in higher PSA levels for a short time. Some studies have suggested that a digital rectal exam might raise PSA levels slightly, although other studies have not found this. Still, if both a PSA test and a digital rectal exam are being done during a doctor visit, some doctors advise having the blood drawn for the PSA before having the digital rectal exam, just in case.
- Certain medicines: Taking male hormones like testosterone (or other medicines that raise testosterone levels) may cause a rise in PSA.
Some things might cause PSA levels to go down (even if a man has prostate cancer):
- 5-alpha reductase inhibitors: Certain drugs used to treat benign prostatic hyperplasia (BPH) or urinary symptoms, such as finasteride (Proscar or Propecia) or dutasteride (Avodart), may lower PSA levels. These drugs can also affect prostate cancer risk. Tell your doctor if you are taking these medicines because they may lower PSA levels, so the doctor might need to adjust the reading.
- Herbal mixtures: Some mixtures that are sold as dietary supplements may also mask a high PSA level. This is why it’s important to let your doctor know if you are taking any type of supplement, even ones that are not necessarily meant for prostate health. Saw palmetto (an herb used by some men to treat BPH) does not seem to affect PSA.
- Obesity: Obese (very overweight) men tend to have lower PSA levels.
- Aspirin: Some research has suggested that men taking aspirin regularly may have lower PSA levels. This effect may be greater in non-smokers. More research is needed to confirm this finding. If you take aspirin regularly (for example, to help prevent heart disease), talk to your doctor before you stop taking it for any reason.
- Statins: Some studies have linked the long-term use of cholesterol-lowering drugs known as statins, such as atorvastatin (Lipitor), rosuvastatin (Crestor), and simvastatin (Zocor), with lower PSA levels.
- Thiazide diuretics: Thiazide diuretics, such as hydrochlorothiazide, are a type of water pill often used to treat high blood pressure. Taking a thiazide diuretic for years is linked to lower PSA levels.
For men not known to have prostate cancer, it’s not always clear if lowering the PSA is helpful. In some cases the factor that lowers the PSA may also lower a man’s risk of prostate cancer. But in other cases, it might lower the PSA level without affecting a man’s risk of cancer. This could actually be harmful, if it were to lower the PSA from an abnormal level to a normal one, as it might result in not detecting a cancer. This is why it’s important to talk to your doctor about anything that might affect your PSA level.
Why should I avoid sexual activity before a PSA test?
Before having a PSA test to test for prostate cancer, men should not have ejaculated during the previous 48 hours.
Semen released during sexual activity can cause PSA (prostate-specific antigen) levels to rise temporarily, which may affect the test results.
For the same reason, before having a PSA test, men should not have:
- exercised vigorously in the previous 48 hours
- an active urinary infection (PSA may remain raised for many months)
- had a prostate biopsy in the previous six weeks
What does the PSA test result mean?
PSA test results can be interpreted a number of different ways and there may be differences in cutoff values between different laboratories.
- The value for total PSA below which the presence of prostate cancer is considered to be unlikely is 4.0 ng/ml (nanograms per milliliter of blood). There are some that feel that this level should be lowered to 2.5 ng/ml in order to detect more cases of prostate cancer. Others argue that this would lead to more over-diagnosing and over-treating cancers that are not clinically significant.
- There is agreement that men with a total PSA level greater than 10.0 ng/ml are at an increased risk for prostate cancer (more than a 50% chance, according to the American Cancer Society).
- Total PSA levels between 4.0 ng/ml and 10.0 ng/ml may indicate prostate cancer (about a 25% chance, according to the American Cancer Society), benign prostate hyperplasia (BPH), or inflammation of the prostate. These conditions are more common in the elderly, as is a general increase in PSA levels. Total PSA between 4.0 ng/ml and 10.0 ng/ml is often referred to as the “gray zone.” It is in this range that the free PSA may be useful.
- Free PSA—prostate tumors typically produce mostly complexed PSA (cPSA), not free PSA. Benign prostate cells tend to produce more free PSA, which will not complex with proteins. Thus, when men in the gray zone have decreased levels of free PSA, it means that they have increased cPSA and a higher probability of prostate cancer. Conversely, when they have elevated levels of free PSA and low cPSA, the risk is diminished. The ratio of free to total PSA can help the individual and his healthcare provider decide whether or not a prostate biopsy should be performed.
Additional evaluations of the PSA test results are sometimes used in an effort to increase the usefulness of the total PSA as a screening tool. They include:
- PSA velocity—the change in PSA concentrations over time; if the PSA continues to rise significantly over time (at least 3 samples at least 18 months apart), then it is more likely that prostate cancer is present. If it climbs rapidly, then the affected person may have a more aggressive form of cancer.
- PSA doubling time—another version of the PSA velocity; it measures how rapidly the PSA concentration doubles.
- PSA density—a comparison of the PSA concentration and the volume of the prostate (as measured by ultrasound); if the PSA level is greater than what one would expect given the size of the prostate, the chance that a cancer is present may be higher.
- Age-specific PSA ranges—since PSA levels naturally increase as a man ages, it has been proposed that normal ranges be tailored to a man’s age.
During treatment for prostate cancer, the PSA level should begin to fall. At the end of treatment, it should be at very low or undetectable levels in the blood. If concentrations do not fall to very low levels, then the treatment has not been fully effective. Following treatment, the PSA test is performed at regular intervals to monitor the person for cancer recurrence. Since even tiny increases can be significant, those affected may want to have their monitoring PSA tests done by the same laboratory each time so that testing variation is kept to a minimum.
A test called “ultrasensitive PSA” (USPSA) may be useful in monitoring for persistence or recurrence of cancer after treatment. This test detects PSA at much lower levels than the traditional test. It has been suggested that increases in PSA due to the persistence or return of cancer can be identified much sooner with this test. However, results of this test must be interpreted with caution. Because the test is very sensitive, there can be small increases in PSA levels from one time to the next even when no cancer is present (false positive).
What is a normal PSA test result?
There is no specific normal or abnormal level of PSA in the blood, and levels may vary over time in the same man. In the past, most doctors considered PSA levels of 4.0 ng/mL and lower as normal. Therefore, if a man had a PSA level above 4.0 ng/mL, doctors would often recommend a prostate biopsy to determine whether prostate cancer was present.
However, more recent studies have shown that some men with PSA levels below 4.0 ng/mL have prostate cancer and that many men with higher levels do not have prostate cancer 17. In addition, various factors can cause a man’s PSA level to fluctuate. For example, a man’s PSA level often rises if he has prostatitis or a urinary tract infection. Prostate biopsies and prostate surgery also increase PSA level. Conversely, some drugs—including finasteride and dutasteride, which are used to treat benign prostatic hyperplasia (BPH)—lower a man’s PSA level. PSA level may also vary somewhat across testing laboratories.
Another complicating factor is that studies to establish the normal range of PSA levels have been conducted primarily in populations of white men. Although expert opinions vary, there is no clear consensus regarding the optimal PSA threshold for recommending a prostate biopsy for men of any racial or ethnic group.
In general, however, the higher a man’s PSA level, the more likely it is that he has prostate cancer. Moreover, a continuous rise in a man’s PSA level over time may also be a sign of prostate cancer.
What if a screening test shows an elevated PSA level?
If a man who has no symptoms of prostate cancer chooses to undergo prostate cancer screening and is found to have an elevated PSA level, the doctor may recommend another PSA test to confirm the original finding. If the PSA level is still high, the doctor may recommend that the man continue with PSA tests and DREs at regular intervals to watch for any changes over time.
If a man’s PSA level continues to rise or if a suspicious lump is detected during a digital rectal exam (DRE), the doctor may recommend additional tests to determine the nature of the problem. A urine test may be recommended to check for a urinary tract infection. The doctor may also recommend imaging tests, such as a transrectal ultrasound, x-rays, or cystoscopy.
If prostate cancer is suspected, the doctor will recommend a prostate biopsy. During this procedure, multiple samples of prostate tissue are collected by inserting hollow needles into the prostate and then withdrawing them. Most often, the needles are inserted through the wall of the rectum (transrectal biopsy). A pathologist then examines the collected tissue under a microscope. The doctor may use ultrasound to view the prostate during the biopsy, but ultrasound cannot be used alone to diagnose prostate cancer.
What happens if Prostate Cancer Screening Test Results Aren’t Normal
If the results of early detection tests – the prostate-specific antigen (PSA) blood test and/or digital rectal exam (DRE) – suggest that you might have prostate cancer, your doctor will do other tests, such as a transrectal ultrasound (TRUS) and a prostate biopsy to find out.
Transrectal ultrasound
For this test, a small probe about the width of a finger is lubricated and placed in your rectum. The probe gives off sound waves that enter the prostate and create echoes. The probe picks up the echoes, and a computer turns them into a black and white image of the prostate.
This procedure often takes less than 10 minutes and is done in a doctor’s office or outpatient clinic. You will feel some pressure when the transrectal ultrasound (TRUS) probe is placed in your rectum, but it is usually not painful. The area may be numbed before the procedure.
Transrectal ultrasound (TRUS) is not used as a screening test for prostate cancer because it can’t always tell the difference between normal tissue and cancer. Instead, it is most often used to look for prostate cancer when a man has symptoms or has an abnormal PSA level or digital rectal exam (DRE). It is also used during a prostate biopsy to guide the biopsy needles into the correct area of the prostate.
Transrectal ultrasound is useful in other situations as well. It can be used to measure the size of the prostate gland, which can help determine the PSA density and may also affect which treatment options a man has. Transrectal ultrasound is also used as a guide during some forms of prostate cancer treatment.
Prostate biopsy
A biopsy is a procedure in which small samples of the prostate are removed and then looked at under a microscope. A core needle biopsy is the main method used to diagnose prostate cancer. It is usually done by a urologist, a surgeon who treats cancers of the genital and urinary tract, which includes the prostate gland.
Using transrectal ultrasound to “see” the prostate gland, the doctor quickly inserts a thin, hollow needle through the wall of the rectum and into the prostate. When the needle is pulled out, it removes a small cylinder (core) of prostate tissue. This is repeated several times. Most urologists will take about 12 core samples from different parts of the prostate.
Though the procedure sounds painful, each biopsy usually causes only a brief uncomfortable sensation because it is done with a special spring-loaded biopsy instrument. The device inserts and removes the needle in a fraction of a second. Most doctors who do the biopsy will numb the area first with local anesthetic. You might want to ask your doctor if he or she plans to do this.
The biopsy itself takes about 10 minutes and is usually done in the doctor’s office. You will probably be given antibiotics to take before the biopsy and possibly for a day or 2 after to reduce the risk of infection.
For a few days after the procedure, you may feel some soreness in the area and will probably notice blood in your urine. You may also have some light bleeding from your rectum, especially if you have hemorrhoids. Many men notice blood in their semen or have rust-colored semen. This can last for several weeks after the biopsy, depending on how often you ejaculate.
Your biopsy samples will be sent to a lab, where they will be looked at with a microscope to see if they contain cancer cells. If cancer is seen, it will also be assigned a grade. This is often expressed as a Gleason score (or Gleason sum). Most Gleason scores range from 6 to 10 (although they can be lower). The higher your Gleason score, the more likely it is that your cancer will grow and spread quickly.
Getting the biopsy results (in the form of a pathology report) usually takes at least 1 to 3 days, but it can sometimes take longer.
Even when taking many samples, biopsies can still sometimes miss a cancer if none of the biopsy needles pass through it. This is known as a false-negative result. If your doctor still strongly suspects you have prostate cancer (because your PSA level is very high, for example) a repeat biopsy may be needed to help be sure.
Prostate biopsy results are sometimes called suspicious. The pathologist may use terms such as prostatic intraepithelial neoplasia (PIN), atypical small acinar proliferation (ASAP, or just atypia), or proliferative inflammatory atrophy (PIA). Suspicious results mean that the cells don’t look like cancer, but they don’t look quite normal, either. If your biopsy results come back suspicious, your doctor may want to repeat the biopsy.
What is prostate gland
The prostate is a chestnut-shaped structure that surrounds the urethra and ejaculatory ducts immediately inferior to the urinary bladder. It measures about 2 × 4 × 3 cm and is an aggregate of 30 to 50 compound tubuloacinar glands enclosed in a single fibrous capsule. These glands empty through about 20 pores in the urethral wall. The stroma of the prostate consists of connective tissue and smooth muscle, like that of the seminal vesicles. The thin, milky secretion of the prostate constitutes about 30% of the semen.
The prostate slowly increases in size from birth to puberty. It then expands rapidly until about age 30, after which time its size typically remains stable until about age 45, when further enlargement may occur, constricting the urethra and interfering with urine flow.
In addition to its susceptibility to prostate cancer and tumors, the prostate is also subject to infection in sexually transmitted diseases (STDs). Prostatitis, inflammation of the prostate, is the single most common reason that men consult a urologist.
Figure 5. Prostate gland
What does the prostate gland do
The fluid expelled during orgasm is called semen (seminal fluid). A typical ejaculation discharges 2 to 5 mL of semen, composed of about 10% sperm and spermatic duct secretions, 30% prostatic fluid, 60% seminal vesicle fluid, and a trace of bulbourethral fluid. Most of the sperm emerge in the first one or two jets of semen. The semen usually has a sperm count of 50 to 120 million sperm/mL. A sperm count any lower than 20 to 25 million sperm/mL is usually associated with infertility (sterility), the inability to fertilize an egg.
The prostate and seminal vesicles contribute the following constituents to the semen:
- The prostate produces a thin, milky, slightly acidic (pH about 6.5) white fluid containing calcium, citrate, and phosphate ions, which is a nutrient for the sperm,; a clotting enzyme; and a protein-hydrolyzing enzyme called serine protease (prostate-specific antigen, PSA), which is an enzyme that helps liquefy semen. Measuring the levels of PSA (prostate-specific antigen) in a man’s blood is the most important method of screening for prostate cancer. The citric acid in prostatic fluid is used by sperm for ATP production via the Krebs cycle. Several proteolytic enzymes, such as prostate-specific antigen (PSA), pepsinogen, lysozyme, amylase, and hyaluronidase, eventually break down the clotting proteins from the seminal vesicles. The function of the acid phosphatase secreted by the prostate is unknown. Seminalplasmin in prostatic fluid is an antibiotic that can destroy bacteria. Seminalplasmin may help decrease the number of naturally occurring bacteria in semen and in the lower female reproductive tract. Secretions of the prostate enter the prostatic urethra through many prostatic ducts. Prostatic secretions make up about 30% of the volume of semen and contribute to sperm motility and viability.
- The seminal vesicles contribute a viscous yellowish fluid, the last component of the semen to emerge. It contains fructose and other carbohydrates, citrate, prostaglandins and a clotting protein called prosemenogelin.
What is Prostate Cancer
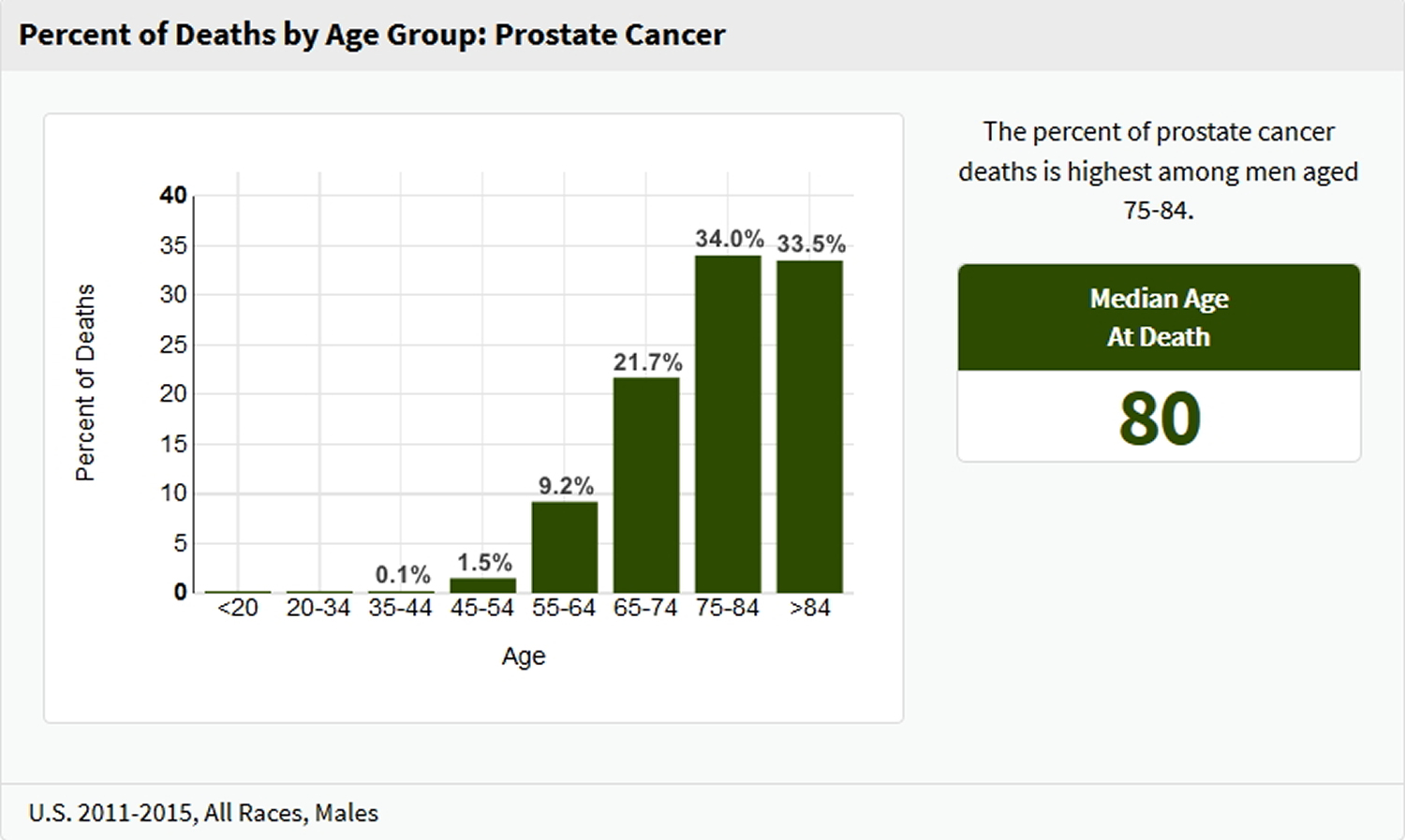
Prostate cancer is one of the most common types of cancer that affects men and prostate cancer is found mainly in older men. Prostate cancer occurs more often in African-American men than in white men. African-American men with prostate cancer are more likely to die from the disease than white men with prostate cancer. In the United States, the lifetime risk of being diagnosed with prostate cancer is approximately 11%, and the lifetime risk of dying of prostate cancer is 2.5% 18. Although the number of men with prostate cancer is large, most men diagnosed with this disease do not die from it. In 2013, the most recent year for which data are available, approximately 172,000 men in the United States were diagnosed with prostate cancer and almost 28,000 died of prostate cancer 19. Prostate cancer causes more deaths in men than any other cancer except lung cancer. From 2003 to 2012, the prostate cancer mortality rate among US men decreased significantly by 3.4% per year (3.3% and 3.9% per year in white and black men, respectively) 20. Most cases of prostate cancer found in autopsy studies are microscopic, well-differentiated lesions that did not affect men’s health during their lifetime. Data from screening trials suggest that many cases of low-risk cancer detected by screening would never have caused symptoms or affected men’s health had they never been identified through screening. Many men with prostate cancer never experience symptoms and, without screening, would never know they have the disease. In autopsy studies of men who died of other causes, more than 20% of men aged 50 to 59 years and more than 33% of men aged 70 to 79 years were found to have prostate cancer 21. In some men, the cancer is more aggressive and leads to death. The median age of death from prostate cancer is 80 years, and more than two-thirds of all men who die of prostate cancer are older than 75 years 18. African American men have an increased lifetime risk of prostate cancer death compared with those of other races/ethnicities (4.2% for African American men, 2.9% for Hispanic men, 2.3% for white men, and 2.1% for Asian and Pacific Islander men) 18.
Screening for prostate cancer begins with a test that measures the amount of PSA protein in the blood. An elevated PSA level may be caused by prostate cancer but can also be caused by other conditions, including an enlarged prostate (benign prostatic hyperplasia) and inflammation of the prostate (prostatitis). Some men without prostate cancer may therefore have positive screening results (ie, “false-positive” results). Men with a positive PSA test result may undergo a transrectal ultrasound-guided core-needle biopsy of the prostate to diagnose prostate cancer.
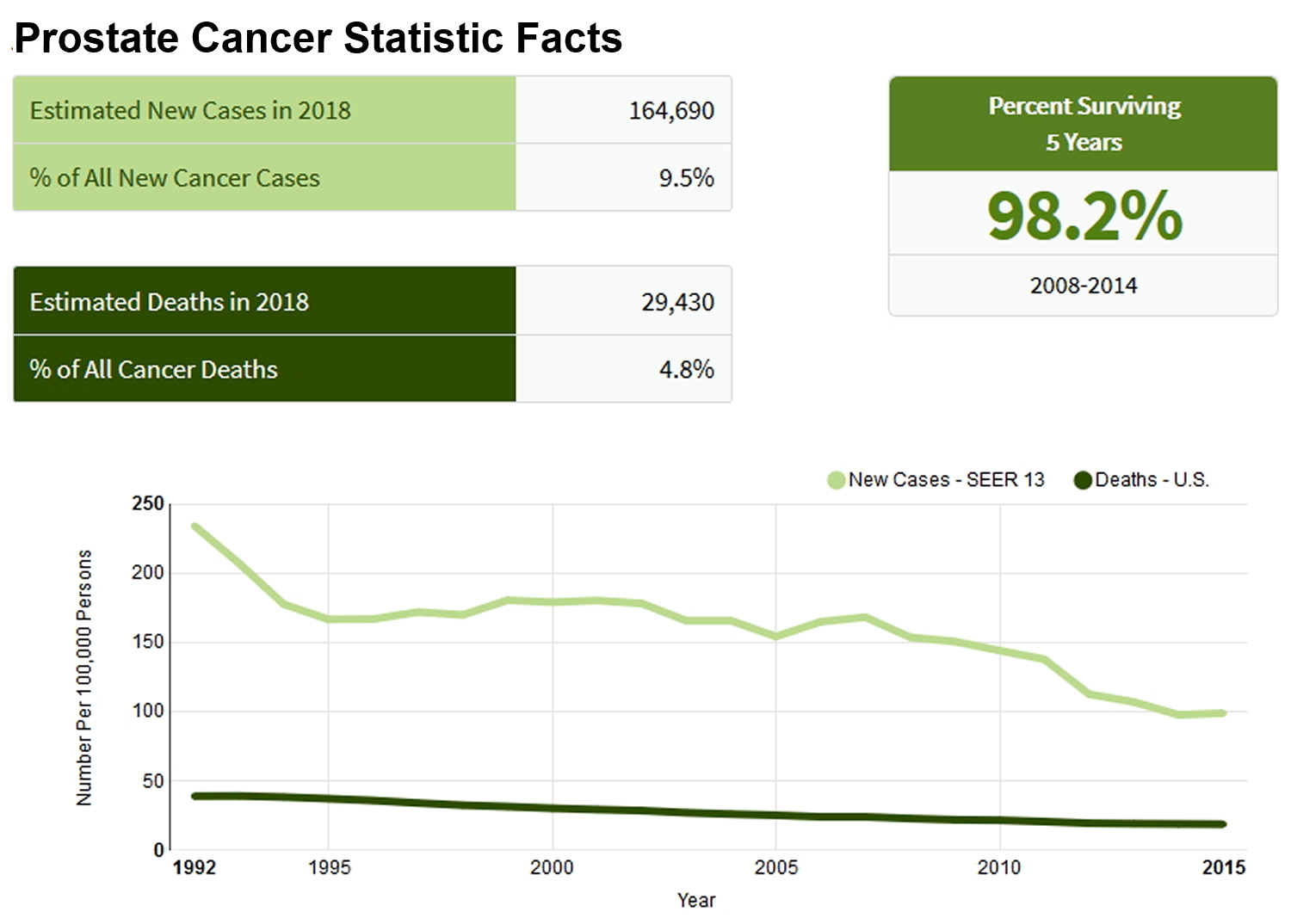
Prostate Cancer Stats 22
- Number of New Cases and Deaths per 100,000: The number of new cases of prostate cancer was 112.6 per 100,000 men per year. The number of deaths was 19.5 per 100,000 men per year. These rates are age-adjusted and based on 2011-2015 cases and deaths.
- Lifetime Risk of Developing Prostate Cancer: Approximately 11.2 percent of men will be diagnosed with prostate cancer at some point during their lifetime, based on 2013-2015 data.
- Prevalence of Prostate Cancer: In 2015, there were an estimated 3,120,176 men living with prostate cancer in the United States.
Benefits of Early Detection and Treatment
The goal of screening for prostate cancer is to identify high-risk, localized prostate cancer that can be successfully treated, thereby preventing the morbidity and mortality associated with advanced or metastatic prostate cancer.
Adequate evidence from randomized clinical trials shows that PSA-based screening programs in men aged 55 to 69 years may prevent approximately 1.3 deaths from prostate cancer over approximately 13 years per 1000 men screened 23, 24. Screening programs may also prevent approximately 3 cases of metastatic prostate cancer per 1000 men screened 23. Current results from screening trials show no reductions in all-cause mortality from screening. There is inadequate evidence to assess whether the benefits for African American men and men with a family history of prostate cancer aged 55 to 69 years are different than the benefits for the average-risk population. There is also inadequate evidence to assess whether there are benefits to starting screening in these high-risk groups before age 55 years.
Adequate evidence from randomized clinical trials is consistent with no benefit of PSA-based screening for prostate cancer on prostate cancer mortality in men 70 years and older.
Harms of Early Detection and Treatment
The harms of screening for prostate cancer include harms from the PSA screening test and subsequent harms from diagnosis and treatment. Potential harms of screening include frequent false-positive results and psychological harms. One major trial in men screened every 2 to 4 years concluded that, over 10 years, more than 15% of men experienced at least 1 false-positive test result 25. Harms of diagnostic procedures include complications of prostate biopsy, such as pain, hematospermia (blood in semen or ejaculate), and infection. Approximately 1% of prostate biopsies result in complications requiring hospitalization. The false-positive and complication rates from biopsy are higher in older men 23. Adequate evidence suggests that the harms of screening and diagnostic procedures are at least small.
PSA-based screening for prostate cancer leads to the diagnosis of prostate cancer in some men whose cancer would never have become symptomatic during their lifetime. Treatment of these men results in harms and provides them with no benefit. This is known as overdiagnosis, and follow-up of large randomized trials suggests that 20% to 50% of men diagnosed with prostate cancer through screening may be overdiagnosed 23. Overdiagnosis rates would be expected to increase with age and to be highest in men 70 years and older because older men have high risk of death from competing causes.
Harms of prostate cancer treatment include erectile dysfunction, urinary incontinence, and bothersome bowel symptoms. About 1 in 5 men who undergo radical prostatectomy develop long-term urinary incontinence requiring use of pads, and 2 in 3 men will experience long-term erectile dysfunction. More than half of men who receive radiation therapy experience long-term sexual erectile dysfunction and up to 1 in 6 men experience long-term bothersome bowel symptoms, including bowel urgency and fecal incontinence 23. Adequate evidence suggests that the harms of overdiagnosis and treatment are at least moderate.
Adequate evidence shows that the harms of screening in men older than 70 years are at least moderate and greater than in younger men because of increased risk of false-positive results, harms from diagnostic biopsy, and harms from treatment.
United States Preventive Services Task Force Assessment
PSA-based screening for prostate cancer has both potential benefits and harms. The United States Preventive Services Task Force does not recommend screening for prostate cancer unless men express a preference for screening after being informed of and understanding the benefits and risks. The decision about whether to be screened for prostate cancer requires that each man incorporate his own values about the potential benefits and harms. The potential harms of screening, diagnostic procedures, and treatment occur soon after screening takes place. Although the potential benefits may occur any time after screening, they generally occur years after treatment, because progression from asymptomatic, screen-detected cancer to symptomatic, metastasized cancer or death (if it occurs at all) may take years or decades to occur.
The United States Preventive Services Task Force concludes with moderate certainty that the net benefit of PSA-based screening for prostate cancer in men aged 55 to 69 years is small for some men. How each man weighs specific benefits and harms will determine whether the overall net benefit is small.
The United States Preventive Services Task Force concludes with moderate certainty that the potential benefits of PSA-based screening for prostate cancer in men 70 years and older do not outweigh the expected harms.
Prostate Cancer Prevention
There is no sure way to prevent prostate cancer. Many risk factors such as age, race, and family history can’t be controlled. But there are some things you can do that might lower your risk for this disease.
Body weight, physical activity, and diet
The effects of body weight, physical activity, and diet on prostate cancer risk are not clear, but there are things you can do that might lower your risk.
Some studies have found that men who are overweight may have a slightly lower risk of prostate cancer overall, but a higher risk of prostate cancers that are likely to be fatal.
Studies have found that men who are regularly physically active have a slightly lower risk of prostate cancer. Vigorous activity may have a greater effect, especially on the risk of advanced prostate cancer.
Several studies have suggested that diets high in certain vegetables (including tomatoes, cruciferous vegetables, soy, beans, and other legumes) or fish may be linked with a lower risk of prostate cancer, especially more advanced cancers. Examples of cruciferous vegetables include cabbage, broccoli, and cauliflower.
Although not all studies agree, several have found a higher risk of prostate cancer in men whose diets are high in calcium. There may also be an increased risk from consuming dairy foods.
For now, the best advice about diet and activity to possibly reduce the risk of prostate cancer is to:
- Eat at least 2½ cups of a wide variety of vegetables and fruits each day.
- Be physically active.
- Stay at a healthy weight.
It may also be sensible to limit calcium supplements and to not get too much calcium in the diet. This does not mean that men who are being treated for prostate cancer should not take calcium supplements if their doctor recommends them.
Vitamin, mineral, and other supplements
Vitamin E and selenium: Some earlier studies suggested that taking vitamin E or selenium supplements might lower prostate cancer risk.
But in a large study known as the Selenium and Vitamin E Cancer Prevention Trial (SELECT), neither vitamin E nor selenium supplements were found to lower prostate cancer risk. In fact, men in the study taking the vitamin E supplements were later found to have a slightly higher risk of prostate cancer. For selenium supplements, the risk of prostate cancer was unchanged in men who had lower selenium levels at the start of the study. Men who had higher baseline levels, though, had an increased risk of high-grade (fast-growing) prostate cancer.
Soy and isoflavones: Several studies are now looking at the possible effects of soy proteins (called isoflavones) on prostate cancer risk. The results of these studies are not yet available.
Taking any supplements can have both risks and benefits. Before starting vitamins or other supplements, talk with your doctor.
Medicines
Some drugs might help reduce the risk of prostate cancer.
5-alpha reductase inhibitors
5-alpha reductase is an enzyme in the body that changes testosterone into dihydrotestosterone (DHT), the main hormone that causes the prostate to grow. Drugs called 5-alpha reductase inhibitors, such as finasteride (Proscar) and dutasteride (Avodart), block this enzyme from making DHT. These drugs are used to treat benign prostatic hyperplasia (BPH), a non-cancerous growth of the prostate.
Large studies of both of these drugs have been done to see if they might also be useful in lowering prostate cancer risk. In these studies, men taking either drug were less likely to develop prostate cancer after several years than men getting an inactive placebo.
When the results were looked at more closely, the men who took these drugs had fewer low-grade prostate cancers, but slightly more higher-grade prostate cancers, which are more likely to grow and spread. Long term, though, this didn’t seem to affect death rates – both groups of men had similar survival.
These drugs can cause sexual side effects such as lowered sexual desire and erectile dysfunction (impotence). But they can help with urinary problems from benign prostatic hyperplasia (BPH) such as trouble urinating and leaking urine (incontinence).
Although these drugs are safe, they aren’t approved by the FDA to help prevent prostate cancer. Right now, it isn’t clear that taking one of these drugs just to lower prostate cancer risk is very helpful. Still, men who want to know more about these drugs should discuss them with their doctors.
Aspirin
Some research suggests that men who take aspirin daily for a long time might have a lower risk of getting and dying from prostate cancer. But more research is needed to show if the possible benefits outweigh the risks. Long-term aspirin use can have side effects, including an increased risk of bleeding in the digestive tract. While aspirin can also have other health benefits, at this time most doctors don’t recommend taking it solely to try to lower prostate cancer risk.
Other drugs
Other drugs and dietary supplements that might help lower prostate cancer risk are now being tested in clinical trials. But so far, no drug or supplement has been found to be helpful in studies large enough for experts to recommend them.
Prostate Cancer Risk Factors
A risk factor is anything that affects your chance of getting a disease such as cancer. Different cancers have different risk factors. Some risk factors, like smoking, can be changed. Others, like a person’s age or family history, can’t be changed.
But having a risk factor, or even several, does not mean that you will get the disease. Many people with one or more risk factors never get cancer, while others who get cancer may have had few or no known risk factors.
Researchers have found several factors that might affect a man’s risk of getting prostate cancer.
Age
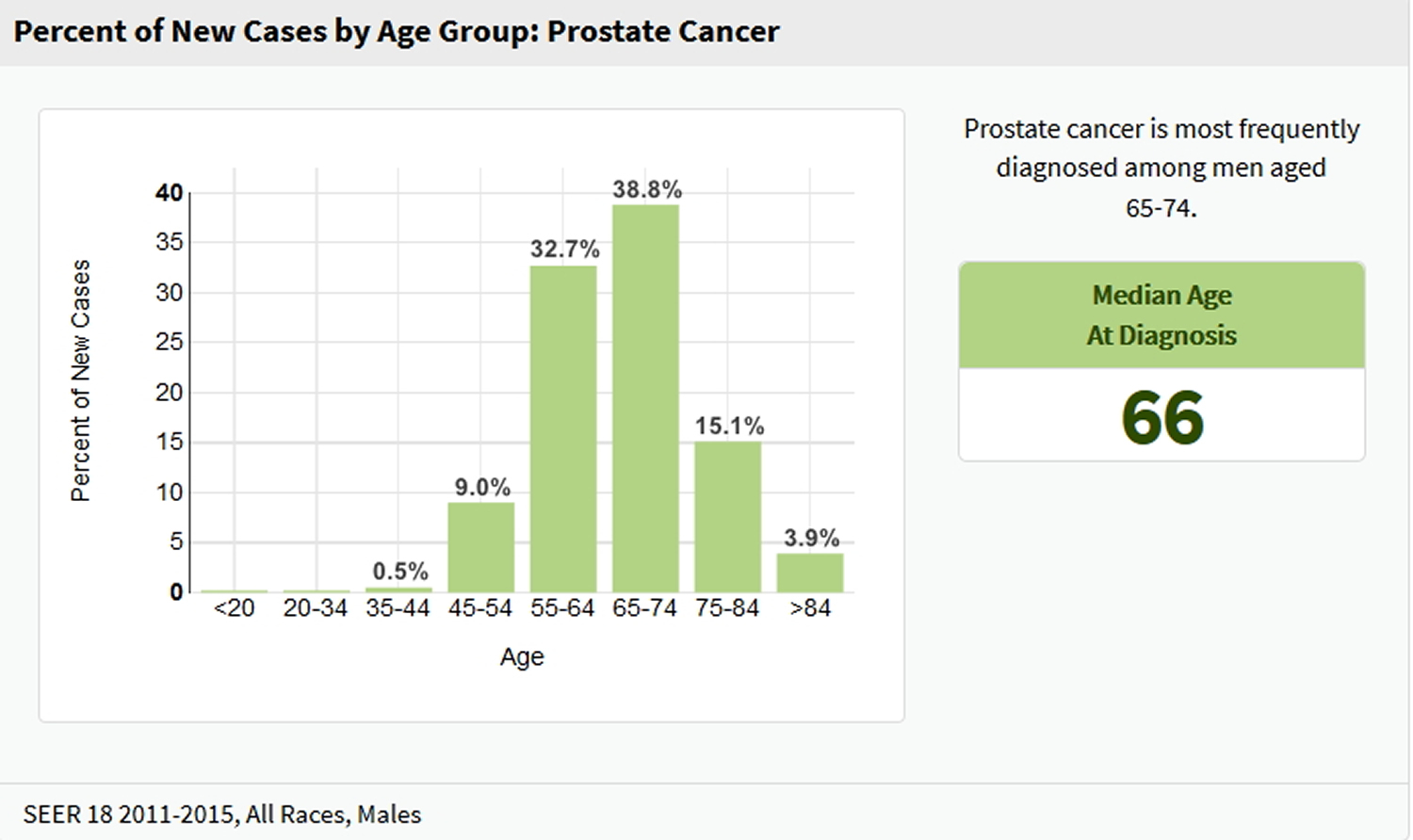
Prostate cancer is rare in men younger than 40, but the chance of having prostate cancer rises rapidly after age 50. About 6 in 10 prostate cancers are found in men older than 65.
Race/ethnicity
Prostate cancer occurs more often in African-American men and Caribbean men of African ancestry than in men of other races. African-American men are also more than twice as likely to die of prostate cancer than white men. Prostate cancer occurs less often in Asian-American and Hispanic/Latino men than in non-Hispanic whites. The reasons for these racial and ethnic differences are not clear.
Geography
Prostate cancer is most common in North America, northwestern Europe, Australia, and on Caribbean islands. It is less common in Asia, Africa, Central America, and South America.
The reasons for this are not clear. More intensive screening in some developed countries probably accounts for at least part of this difference, but other factors such as lifestyle differences (diet, etc.) are likely to be important as well. For example, Asian Americans have a lower risk of prostate cancer than white Americans, but their risk is higher than that of men of similar backgrounds living in Asia.
Family history
Prostate cancer seems to run in some families, which suggests that in some cases there may be an inherited or genetic factor. (Still, most prostate cancers occur in men without a family history of it.)
Having a father or brother with prostate cancer more than doubles a man’s risk of developing this disease. (The risk is higher for men who have a brother with the disease than for those who have a father with it.) The risk is much higher for men with several affected relatives, particularly if their relatives were young when the cancer was found.
Gene changes
Several inherited gene changes (mutations) seem to raise prostate cancer risk, but they probably account for only a small percentage of cases overall. For example:
- Inherited mutations of the BRCA1 or BRCA2 genes raise the risk of breast and ovarian cancers in some families. Mutations in these genes (especially in BRCA2) may also increase prostate cancer risk in some men.
- Men with Lynch syndrome (also known as hereditary non-polyposis colorectal cancer, or HNPCC), a condition caused by inherited gene changes, have an increased risk for a number of cancers, including prostate cancer.
Other inherited gene changes can also raise a man’s risk of prostate cancer.
Factors with less clear effect on prostate cancer risk
Diet
The exact role of diet in prostate cancer is not clear, but several factors have been studied.
Men who eat a lot of red meat or high-fat dairy products appear to have a slightly higher chance of getting prostate cancer. These men also tend to eat fewer fruits and vegetables. Doctors aren’t sure which of these factors is responsible for raising the risk.
Some studies have suggested that men who consume a lot of calcium (through food or supplements) may have a higher risk of developing prostate cancer. Dairy foods (which are often high in calcium) might also increase risk. But most studies have not found such a link with the levels of calcium found in the average diet, and it’s important to note that calcium has other important health benefits.
Obesity
Being obese (very overweight) does not seem to increase the overall risk of getting prostate cancer.
Some studies have found that obese men have a lower risk of getting a low-grade (less dangerous) form of the disease, but a higher risk of getting more aggressive prostate cancer. The reasons for this are not clear.
Some studies have also found that obese men may be at greater risk for having more advanced prostate cancer and of dying from prostate cancer, but not all studies have found this.
Smoking
Most studies have not found a link between smoking and getting prostate cancer. Some research has linked smoking to a possible small increased risk of dying from prostate cancer, but this finding needs to be confirmed by other studies.
Chemical exposures
There is some evidence that firefighters can be exposed to chemicals that may increase their risk of prostate cancer.
A few studies have suggested a possible link between exposure to Agent Orange, a chemical used widely during the Vietnam War, and prostate cancer, although not all studies have found such a link. The Institute of Medicine considers there to be “limited/suggestive evidence” of a link between Agent Orange exposure and prostate cancer.
Inflammation of the prostate
Some studies have suggested that prostatitis (inflammation of the prostate gland) may be linked to an increased risk of prostate cancer, but other studies have not found such a link. Inflammation is often seen in samples of prostate tissue that also contain cancer. The link between the two is not yet clear, and is an active area of research.
Sexually transmitted infections
Researchers have looked to see if sexually transmitted infections (like gonorrhea or chlamydia) might increase the risk of prostate cancer, because they can lead to inflammation of the prostate. So far, studies have not agreed, and no firm conclusions have been reached.
Vasectomy
Some studies have suggested that men who have a vasectomy (minor surgery to make men infertile) have a slightly increased risk for prostate cancer, but other studies have not found this. Research on this possible link is still being done.
How is the PSA test used in men who have been treated for prostate cancer?
The PSA test is often used to monitor patients who have a history of prostate cancer to see if their cancer has recurred (come back). If a man’s PSA level begins to rise after prostate cancer treatment, it may be the first sign of a recurrence. Such a “biochemical relapse” typically appears months or years before other clinical signs and symptoms of prostate cancer recurrence.
However, a single elevated PSA measurement in a patient who has a history of prostate cancer does not always mean that the cancer has come back. A man who has been treated for prostate cancer should discuss an elevated PSA level with his doctor. The doctor may recommend repeating the PSA test or performing other tests to check for evidence of a recurrence. The doctor may look for a trend of rising PSA level over time rather than a single elevated PSA level.
What does an increase in PSA level mean for a man who has been treated for prostate cancer?
If a man’s PSA level rises after prostate cancer treatment, his doctor will consider a number of factors before recommending further treatment. Additional treatment based on a single PSA test is not recommended. Instead, a rising trend in PSA level over time in combination with other findings, such as an abnormal result on imaging tests, may lead a man’s doctor to recommend further treatment.
- Schröder FH, Hugosson J, Roobol MJ, Tammela TL, Zappa M, Nelen V et al. Screening and prostate cancer mortality: results of the European Randomised Study of Screening for Prostate Cancer (ERSPC) at 13 years of follow-up. Lancet 2014; 384(9959): 2027-2035. https://www.ncbi.nlm.nih.gov/pmc/articles/PMC4427906/[↩]
- Final Recommendation Statement Prostate Cancer: Screening https://www.uspreventiveservicestaskforce.org/Page/Document/RecommendationStatementFinal/prostate-cancer-screening1[↩][↩]
- American Cancer Society Recommendations for Prostate Cancer Early Detection. https://www.cancer.org/cancer/prostate-cancer/early-detection/acs-recommendations.html[↩][↩]
- Carter HB, Albertsen PC, Barry MJ, et al. Early detection of prostate cancer: AUA Guideline. J Urol. 2013;190(2):419-426.[↩][↩]
- Pinsky PF, Prorok PC, Yu K, et al. Extended mortality results for prostate cancer screening in the PLCO trial with median follow-up of 15 years. Cancer 2017; 123(4):592-599. https://www.ncbi.nlm.nih.gov/pmc/articles/PMC5725951/[↩]
- Schröder FH, Hugosson J, Roobol MJ, et al. Screening and prostate cancer mortality: Results of the European Randomised Study of Screening for Prostate Cancer (ERSPC) at 13 years of follow-up. Lancet 2014; 384: 2027-2035. https://www.ncbi.nlm.nih.gov/pmc/articles/PMC4427906/[↩][↩]
- Schröder FH, Hugosson J, Roobol MJ, et al. Prostate-cancer mortality at 11 years of follow-up. New England Journal of Medicine 2012;366(11):981-990. https://www.nejm.org/doi/10.1056/NEJMoa1113135[↩][↩]
- Tsodikov A, Gulati R, Heijnsdijk EAM, et al. Reconciling the effects of screening on prostate cancer mortality in the ERSPC and PLCO trials. Annals of Internal Medicine 2017; 167(7):449-455. https://www.ncbi.nlm.nih.gov/pmc/articles/PMC5734053/[↩]
- U.S. Preventive Health Services Task Force. Prostate Cancer Screening Draft Recommendations https://www.uspreventiveservicestaskforce.org/Page/Document/RecommendationStatementFinal/prostate-cancer-screening1[↩]
- American Academy of Family Physicians. Clinical preventive service recommendation: prostate cancer. https://www.aafp.org/patient-care/clinical-recommendations/all/prostate-cancer.html[↩]
- Bell N, Connor Gorber S, Shane A, et al; Canadian Task Force on Preventive Health Care. Recommendations on screening for prostate cancer with the prostate-specific antigen test. CMAJ. 2014;186(16):1225-1234.[↩]
- Qaseem A, Barry MJ, Denberg TD, Owens DK, Shekelle P; Clinical Guidelines Committee of the American College of Physicians. Screening for prostate cancer: a guidance statement from the Clinical Guidelines Committee of the American College of Physicians. Ann Intern Med. 2013;158(10):761-769.[↩]
- Tuncel A, Aksut H, Agras K, Tekdogan U, Ener K, et al. Is serum prostate-specific antigen level affected by fasting and nonfasting? Urology. 2005;66:105–7. https://www.ncbi.nlm.nih.gov/pubmed/15992912[↩]
- Lau CK, Guo M, Viczko JA, Naugler CT. A population study of fasting time and serum Prostate-Specific Antigen (PSA) level. Asian J Androl. 2014;16:740–4. https://www.ncbi.nlm.nih.gov/pmc/articles/PMC4215671/[↩]
- Barry MJ. Clinical practice. Prostate-specific-antigen testing for early diagnosis of prostate cancer. New England Journal of Medicine 2001;344(18):1373-1377. https://www.nejm.org/doi/full/10.1056/NEJM200105033441806[↩]
- Klein EA, Chait A, Hafron JM, et al. The single-parameter, structure-based IsoPSA assay demonstrates improved diagnostic accuracy for detection of any prostate cancer and high-grade prostate cancer compared to a concentration-based assay of total prostate-specific antigen: A preliminary report. European Urology 2017; S0302-2838(17)30236-1. https://www.ncbi.nlm.nih.gov/pubmed/28396176[↩]
- Thompson IM, Pauler DK, Goodman PJ, et al. Prevalence of prostate cancer among men with a prostate-specific antigen level < or =4.0 ng per milliliter. New England Journal of Medicine 2004;350(22):2239-2246. https://www.nejm.org/doi/10.1056/NEJMoa031918[↩]
- National Cancer Institute. Cancer stat facts: prostate cancer. https://seer.cancer.gov/statfacts/html/prost.html[↩][↩][↩]
- Centers for Disease Control and Prevention. United States cancer statistics: 1999–2014 cancer incidence and mortality data. https://nccd.cdc.gov/uscs/[↩]
- Ryerson AB, Eheman CR, Altekruse SF, et al. Annual report to the nation on the status of cancer, 1975–2012, featuring the increasing incidence of liver cancer. Cancer. 2016;122(9):1312-1337.[↩]
- Jahn JL, Giovannucci EL, Stampfer MJ. The high prevalence of undiagnosed prostate cancer at autopsy: implications for epidemiology and treatment of prostate cancer in the prostate-specific antigen-era. Int J Cancer. 2015;137(12):2795-2802.[↩]
- Cancer Stat Facts: Prostate Cancer https://seer.cancer.gov/statfacts/html/prost.html[↩]
- Fenton JJ, Weyrich MS, Durbin S, Liu Y, Bang H, Melnikow J. Prostate-Specific Antigen–Based Screening for Prostate Cancer: A Systematic Evidence Review for the US Preventive Services Task Force. Evidence Synthesis No. 154. AHRQ Publication No. 17-05229-EF-1. Rockville, MD: Agency for Healthcare Research and Quality; 2018.[↩][↩][↩][↩][↩]
- Fenton JJ, Weyrich MS, Durbin S, Liu Y, Bang H, Melnikow J. Prostate-specific antigen-based screening for prostate cancer: evidence report and systematic review for the US Preventive Services Task Force. JAMA. 2018;319(18):1914-1931.[↩]
- Kilpeläinen TP, Tammela TL, Roobol M, et al. False-positive screening results in the European randomized study of screening for prostate cancer. Eur J Cancer. 2011;47(18):2698-2705.[↩]