Contents
What is tooth enamel
Tooth enamel is outermost layer of the tooth structure, and the hardest substance in your body. As the hardest substance in the human body, tooth enamel serves the important function of keeping your teeth protected, when you are biting and chewing food. Tooth enamel also keeps the sensitive pulp of your teeth sheltered from painful temperatures and chemicals. Even though tooth enamel is a strong substance, that does not mean that it can withstand all the pressure human’s put it through. Tooth enamel, like other bones in your body, is still prone to chips, cracks, and erosion.
Tooth enamel is a translucent structure, that covers the crown, which is the area of the tooth that is visible above the gumline. The structure underneath tooth enamel, known as dentin, is the area of the tooth that gives it its off-white color. However, due to its translucent nature, tooth enamel is prone to staining. Having frequent sugary snacks and drinks can increase the risk of tooth enamel erosion and decay, because your teeth come under constant attack and do not have time to recover. Coffee, tea, soda, wine, juices, and cigarettes are some common causes of teeth enamel staining. When tooth enamel becomes decayed, it reveals the inner-layer of the tooth, which can give your teeth a dark yellow color.
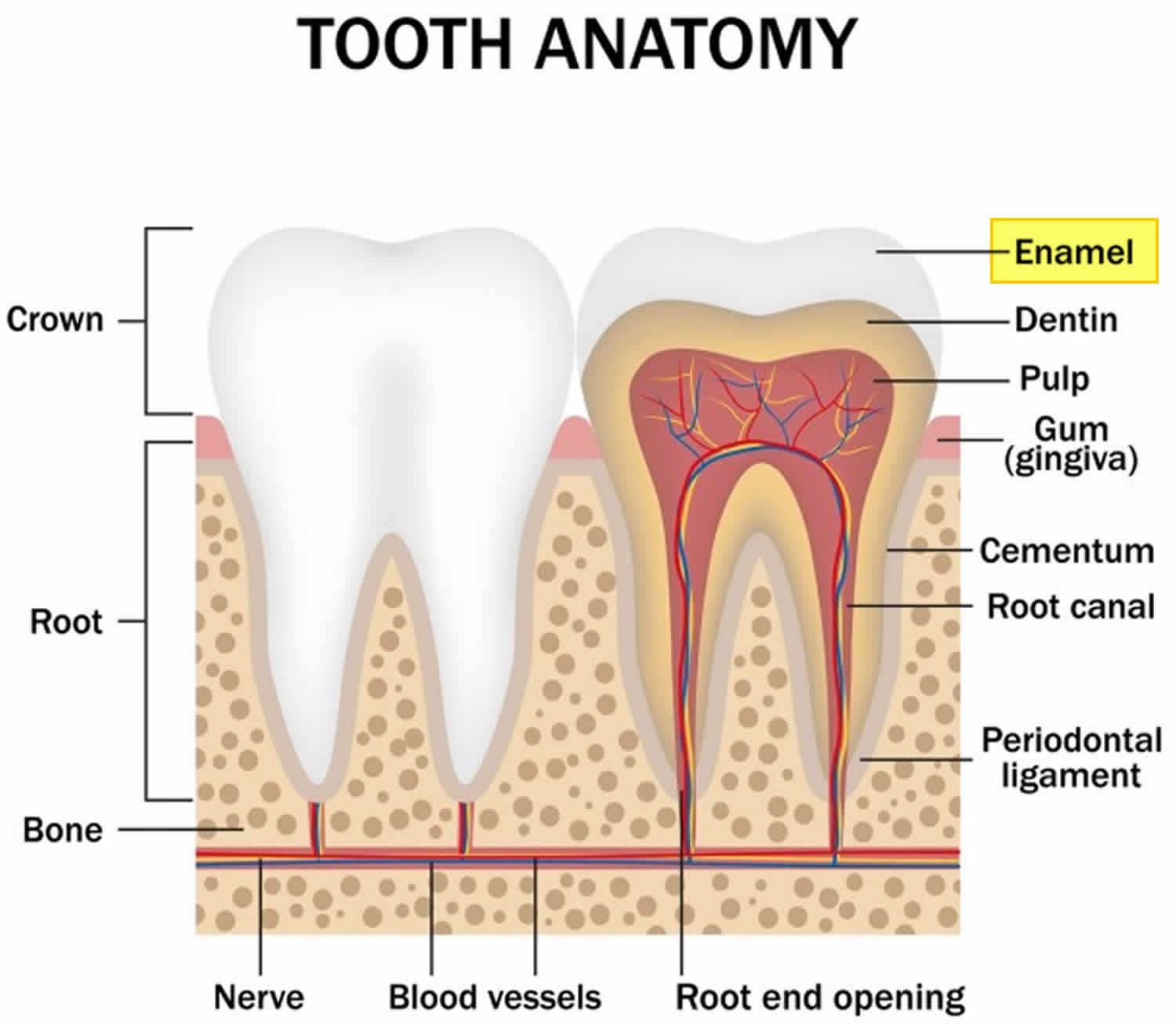
Your teeth are composed of four dental tissues. Three of them—enamel, dentin and cementum—are hard tissues. The fourth tissue—pulp, or the center of the tooth that contains nerves, blood vessels and connective tissue—is a soft, or non-calcified, tissue.
- Anatomical Crown. The visible part of your tooth. It is normally covered by enamel.
- Gums also called gingiva. Soft tissues that cover and protect the roots of your teeth and cover teeth that have not yet erupted.
- Pulp chamber. The space occupied by the pulp—the soft tissue at the center of your teeth containing nerves, blood vessels and connective tissue.
- Neck. The area where the crown joins the root.
- Dentin. That part of the tooth that is beneath enamel and cementum. It contains microscopic tubules (small hollow tubes or canals). When dentin loses its protective covering (enamel), the tubules allow heat and cold or acidic or sticky foods to stimulate the nerves and cells inside the tooth, causing sensitivity.
- Bone (alveolar bone). The part of the jaw that surrounds the roots of the teeth.
- Root Canal. The portion of the pulp cavity inside the root of a tooth; the chamber within the root of the tooth that contains the pulp.
- Cementum. Hard connective tissue covering the tooth root, giving attachment to the periodontal ligament.
- Periodontal Ligament. A system of collagenous connective tissue fibers that connect the root of a tooth to its socket.
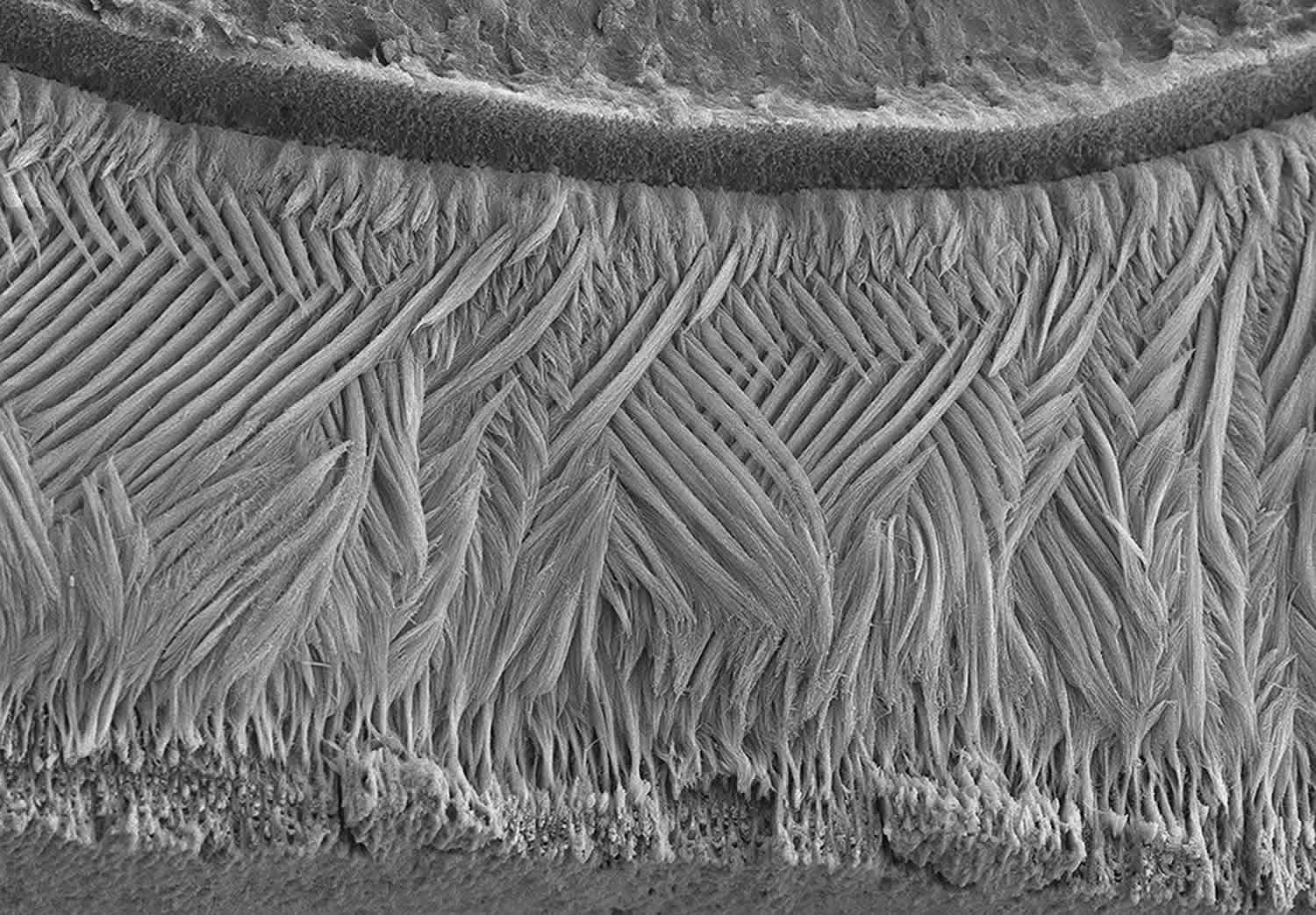
Figure 2 below shows a scanning electron microscopy image of tooth enamel showing the lattice pattern formed by enamel rods, an arrangement that confers strength and flexibility. Genetic mutations affecting enamel formation can result in defects in the thickness, mineralization, and/or lattice pattern of the enamel. This can produce weak teeth prone to decay, which in turn can increase other health risks such as systemic infections and heart disease.
Unfortunately, once your teeth’s enamel is eroded, there are no ways to regenerate the enamel. However, there are some lifestyle choices you can make to help strengthen your enamel. For one, maintaining healthy oral hygiene can help ensure that you do not lose excess enamel from acid erosion caused by bacteria.
Other routes you can take to protect your enamel, include taking vitamin D and calcium supplements. Vitamin D and calcium naturally promote bone growth and strengthen your teeth. Lastly, you can try brushing your teeth with a fluoride toothpaste or using a fluoride rinse to strengthen your enamel. Fluoride is known to protect your teeth from demineralization caused by acid erosion from bacteria and sugar.
Regular checkups can identify cavities and other dental conditions before they cause troubling symptoms and lead to more-serious problems. The sooner you seek care, the better your chances of reversing the earliest stages of tooth decay and preventing its progression. If a cavity is treated before it starts causing pain, you probably won’t need extensive treatment.
To prevent tooth cavity, gently brush your teeth and gums twice a day with a fluoridated toothpaste. You should also visit your dentist regularly for a check-up and cleaning.
- Good oral hygiene. That means brushing your teeth for two minutes at least twice daily — in the morning and before going to bed — and flossing at least once a day. Better yet, brush after every meal or snack or as your dentist recommends. Flossing before you brush allows you to clean away the loosened food particles and bacteria.
- Regular dental visits. See your dentist or dental hygienist regularly for cleanings, usually every six to 12 months. If you have risk factors that increase your chance of developing periodontitis — such as having dry mouth, taking certain medications or smoking — you may need professional cleaning more often.
- Annual dental X-rays can help identify diseases that are not seen by a visual dental examination and monitor for changes in your dental health.
- Good health practices. Practices such as healthy eating and managing blood sugar if you have diabetes also are important to maintain gum health.
Figure 1. Tooth anatomy
Figure 2. Tooth enamel electron microscopy
Tooth enamel loss
Tooth enamel loss and tooth decay is caused by the things you eat and drink. Cavities are permanently damaged areas in your tooth enamel that develop into tiny openings or holes. Cavities, also called tooth decay or caries, are caused by a combination of factors, including bacteria in your mouth, frequent snacking, sipping sugary drinks and not cleaning your teeth well. Consumables such as chocolate, sweets, fizzy drinks and fruit juices all generate plaque acids that gradually dissolve away the tooth enamel and dentine of the tooth.
The primary cause of tooth enamel erosion occurs from bacteria creating acids that wear away the enamel. Enamel erosion can also result from the following factors:
- Drinking too many soft drinks. Soft drinks are high in phosphoric and citric acid, which seep through the pores in your enamel and cause corrosion.
- Drinking too many fruit drinks. Fruit drinks are high in citric acid, which can be as erosive as battery acids.
- Dry mouth. Your saliva plays an important role in washing away bacteria, and keeping your teeth protected from enamel-destroying acids. Dry mouth, also known as xerostomia, can lead to tooth decay, because your mouth is not having a healthy salivary flow to rinse away acids.
- Acid reflux. Acid reflux, also known as GERD (gastroesophageal reflux disease), along with other gastrointestinal problems can lead to premature enamel erosion from acid damage.
- Diets that are high in sugar and starches. Bacteria in your mouth feast on sugar and starches, creating an acid by-product that can eat away your enamel.
- Friction. Routine wear and tear, friction, and stress can all lead to enamel erosion. Physical wear and tear often occur from improper flossing, biting on hard objecting, or grinding your teeth at night.
Cavities and tooth decay are among the world’s most common health problems. They’re especially common in children, teenagers and older adults. But anyone who has teeth can get cavities, including infants.
If cavities aren’t treated, they get larger and affect deeper layers of your teeth. They can lead to a severe toothache, infection and tooth loss. Regular dental visits and good brushing and flossing habits are your best protection against cavities and tooth decay.
If plaque is allowed to build up, acid can begin to break down the surface of your tooth. This can cause holes known as cavities, as well as gum disease, and in severe cases abscesses and tooth loss.
Added and hidden sugars are commonly found in processed food and fruit, and are a threat to your teeth. The more sugar you consume, the likelier the chances of obtaining dental decay.
In the early stages of dental decay there are no symptoms, but your dental team can spot cavities in the early stages when they examine or x-ray your teeth.
The biting surfaces of the teeth and the surfaces between the teeth are most likely to decay. This is because food and plaque can become stuck in these areas. Any part of the tooth can be at risk.
Cavities are caused by tooth decay — a process that occurs over time. Here’s how tooth decay develops:
- Plaque forms. Dental plaque is a clear sticky film that coats your teeth. It’s due to eating a lot of sugars and starches and not cleaning your teeth well. When sugars and starches aren’t cleaned off your teeth, bacteria quickly begin feeding on them and form plaque. Plaque that stays on your teeth can harden under or above your gum line into tartar (calculus). Tartar makes plaque more difficult to remove and creates a shield for bacteria.
- Plaque attacks. The acids in plaque remove minerals in your tooth’s hard, outer enamel. This erosion causes tiny openings or holes in the enamel — the first stage of cavities. Once areas of enamel are worn away, the bacteria and acid can reach the next layer of your teeth, called dentin. This layer is softer than enamel and less resistant to acid. Dentin has tiny tubes that directly communicate with the nerve of the tooth causing sensitivity.
- Destruction continues. As tooth decay develops, the bacteria and acid continue their march through your teeth, moving next to the inner tooth material (pulp) that contains nerves and blood vessels. The pulp becomes swollen and irritated from the bacteria. Because there is no place for the swelling to expand inside of a tooth, the nerve becomes pressed, causing pain. Discomfort can even extend outside of the tooth root to the bone.
Risk factors for tooth cavities
Everyone who has teeth is at risk of getting cavities, but the following factors can increase risk:
- Tooth location. Decay most often occurs in your back teeth (molars and premolars). These teeth have lots of grooves, pits and crannies, and multiple roots that can collect food particles. As a result, they’re harder to keep clean than your smoother, easy-to-reach front teeth.
- Certain foods and drinks. Foods that cling to your teeth for a long time — such as milk, ice cream, honey, sugar, soda, dried fruit, cake, cookies, hard candy and mints, dry cereal, and chips — are more likely to cause decay than foods that are easily washed away by saliva.
- Frequent snacking or sipping. When you steadily snack or sip sugary drinks, you give mouth bacteria more fuel to produce acids that attack your teeth and wear them down. And sipping soda or other acidic drinks throughout the day helps create a continual acid bath over your teeth.
- Bedtime infant feeding. When babies are given bedtime bottles filled with milk, formula, juice or other sugar-containing liquids, these beverages remain on their teeth for hours while they sleep, feeding decay-causing bacteria. This damage is often called baby bottle tooth decay. Similar damage can occur when toddlers wander around drinking from a sippy cup filled with these beverages.
- Inadequate brushing. If you don’t clean your teeth soon after eating and drinking, plaque forms quickly and the first stages of decay can begin.
- Not getting enough fluoride. Fluoride, a naturally occurring mineral, helps prevent cavities and can even reverse the earliest stages of tooth damage. Because of its benefits for teeth, fluoride is added to many public water supplies. It’s also a common ingredient in toothpaste and mouth rinses. But bottled water usually does not contain fluoride.
- Younger or older age. In the United States, cavities are common in very young children and teenagers. Older adults also are at higher risk. Over time, teeth can wear down and gums may recede, making teeth more vulnerable to root decay. Older adults also may use more medications that reduce saliva flow, increasing the risk of tooth decay.
- Dry mouth. Dry mouth is caused by a lack of saliva, which helps prevent tooth decay by washing away food and plaque from your teeth. Substances found in saliva also help counter the acid produced by bacteria. Certain medications, some medical conditions, radiation to your head or neck, or certain chemotherapy drugs can increase your risk of cavities by reducing saliva production.
- Worn fillings or dental devices. Over the years, dental fillings can weaken, begin to break down or develop rough edges. This allows plaque to build up more easily and makes it harder to remove. Dental devices can stop fitting well, allowing decay to begin underneath them.
- Heartburn. Heartburn or gastroesophageal reflux disease (GERD) can cause stomach acid to flow into your mouth (reflux), wearing away the enamel of your teeth and causing significant tooth damage. This exposes more of the dentin to attack by bacteria, creating tooth decay. Your dentist may recommend that you consult your doctor to see if gastric reflux is the cause of your enamel loss.
- Eating disorders. Anorexia and bulimia can lead to significant tooth erosion and cavities. Stomach acid from repeated vomiting (purging) washes over the teeth and begins dissolving the enamel. Eating disorders also can interfere with saliva production.
Tips for preventing tooth decay
Though cavities can be repaired, try to avoid them by taking care of your teeth. Ask your dentist which tips are best for you.
Good oral and dental hygiene can help you avoid cavities and tooth decay. Here’s how:
- Floss your teeth at least once a day to remove plaque and food that’s stuck between your teeth after eating. Bedtime is an important time to floss.
- Brush your teeth with fluoride toothpaste after eating or drinking or at least twice a day. The American Dental Association recommends brushing your teeth twice a day with fluoride toothpaste. Bedtime is an important time to brush.
- Brush up and down in a circular motion. When you brush your teeth, you help remove food and plaque — a sticky white film that forms on your teeth and contains bacteria. After you eat a meal or snack that contains sugar, the bacteria in plaque produce acids that attack tooth enamel. Repeated attacks can break down tooth enamel and lead to cavities. Plaque that isn’t removed can also harden into tartar, making it harder to keep teeth clean.
- Gently brush your gums as well to keep them healthy.
- Limit or avoid sweets and sugary drinks, like soda or juice. Whenever you eat or drink beverages other than water, you help your mouth bacteria create acids that can destroy tooth enamel. If you snack or drink throughout the day, your teeth are under constant attack.
- Drink some tap water. Most public water supplies have added fluoride, which can help reduce tooth decay significantly. If you drink only bottled water that doesn’t contain fluoride, you’ll miss out on fluoride benefits.
- Consider dental sealants. A sealant is a protective plastic coating applied to the chewing surface of back teeth. It seals off grooves and crannies that tend to collect food, protecting tooth enamel from plaque and acid. The Centers for Disease Control and Prevention (CDC) recommends sealants for all school-age children. Sealants may last for several years before they need to be replaced, but they need to be checked regularly.
- Consider fluoride treatments. Your dentist may recommend periodic fluoride treatments, especially if you aren’t getting enough fluoride through fluoridated drinking water and other sources. He or she may also recommend custom trays that fit over your teeth for application of prescription fluoride if your risk of tooth decay is very high.
- See your dentist twice a year for regular checkups.
- Ask about antibacterial treatments. If you’re especially vulnerable to tooth decay — for example, because of a medical condition — your dentist may recommend special antibacterial mouth rinses or other treatments to help cut down on harmful bacteria in your mouth.
- Combined treatments. Chewing xylitol-based gum along with prescription fluoride and an antibacterial rinse can help reduce the risk of cavities.
What type of toothpaste should I use?
It’s important to use a toothpaste with the right concentration of fluoride. Check the packaging to find out how much fluoride each brand contains.
- Adults should use a toothpaste that contains at least 1,350 parts per million (ppm) fluoride.
- Children don’t need to use special “children’s toothpaste”. Children of all ages can use family toothpaste, as long as it contains 1,350-1,500ppm fluoride.
- Children aged six and under who don’t have tooth decay can use a lower-strength children’s toothpaste, but make sure it contains at least 1,000ppm fluoride.
- Below the age of three, children should use just a smear of toothpaste. Children aged three to six years should use a pea-sized blob of toothpaste. Make sure children don’t lick or eat toothpaste from the tube.
Your dentist may advise you or your child to use a toothpaste with a higher concentration of fluoride, if you need it.
Tooth enamel erosion symptoms
Common symptoms of tooth enamel erosion include:
- Tooth sensitivity, especially to hot, cold or sweet food and drinks
- Chipped teeth or sharp tooth edges
- Tooth discoloration or darkening of the teeth
- Thinning or shortened teeth, may be recognized as changes in the bite
- Pain or irritation in the mouth
The signs and symptoms of tooth cavities vary, depending on their extent and location. When a cavity is just beginning, you may not have any symptoms at all. As the decay gets larger, it may cause signs and symptoms such as:
- Toothache, spontaneous pain or pain that occurs without any apparent cause
- Tooth sensitivity
- Mild to sharp pain when eating or drinking something sweet, hot or cold
- Visible holes or pits in your teeth
- Brown, black or white staining on any surface of a tooth
- Pain when you bite down
Tooth enamel erosion diagnosis
Your dentist can usually detect tooth decay by:
- Asking about tooth pain and sensitivity
- Examining your mouth and teeth
- Probing your teeth with dental instruments to check for soft areas
- Looking at dental X-rays, which can show the extent of cavities and decay
Your dentist will also be able to tell you which of the three types of cavities you have — smooth surface, pit and fissure, or root.
How to restore tooth enamel
Tooth enamel is a hard calcified tissue covering the dentin in the crown of your tooth. Because tooth enamel contains no living cells, tooth enamel cannot repair damage from decay or from wear. Only a dentist can correct these conditions.
Treatment of cavities depends on how severe they are and your particular situation. Treatment options include:
- Fluoride treatments. If your cavity just started, a fluoride treatment may help restore your tooth’s enamel and can sometimes reverse a cavity in the very early stages. Professional fluoride treatments contain more fluoride than the amount found in tap water, toothpaste and mouth rinses. Fluoride treatments may be liquid, gel, foam or varnish that’s brushed onto your teeth or placed in a small tray that fits over your teeth.
- Fillings. Fillings, also called restorations, are the main treatment option when decay has progressed beyond the earliest stage. Fillings are made of various materials, such as tooth-colored composite resins, porcelain or dental amalgam that is a combination of several materials.
- Crowns. For extensive decay or weakened teeth, you may need a crown — a custom-fitted covering that replaces your tooth’s entire natural crown. Your dentist drills away all the decayed area and enough of the rest of your tooth to ensure a good fit. Crowns may be made of gold, high strength porcelain, resin, porcelain fused to metal or other materials.
- Root canals. When decay reaches the inner material of your tooth (pulp), you may need a root canal. This is a treatment to repair and save a badly damaged or infected tooth instead of removing it. The diseased tooth pulp is removed. Medication is sometimes put into the root canal to clear any infection. Then the pulp is replaced with a filling.
- Tooth extractions. Some teeth become so severely decayed that they can’t be restored and must be removed. Having a tooth pulled can leave a gap that allows your other teeth to shift. If possible, consider getting a bridge or a dental implant to replace the missing tooth.
Restorative dentistry for tooth enamel
Depending on the level of your tooth enamel loss, there are a variety of cosmetic treatments your dentist can use to restore the function of tooth enamel. In less severe cases, dental bonding can be used to cover sensitive teeth, while also improving the color of the teeth.
For significant enamel loss, your dentist will most likely recommend porcelain veneers or porcelain crowns, for even more significant damage. Porcelain crowns restore the function and beauty of your teeth by completely encapsulating them with a tooth-like structure made from porcelain.
On the other hand, porcelain veneers only restore the front outer shell of the teeth for a more aesthetic restoration.