Contents
What is aquagenic urticaria
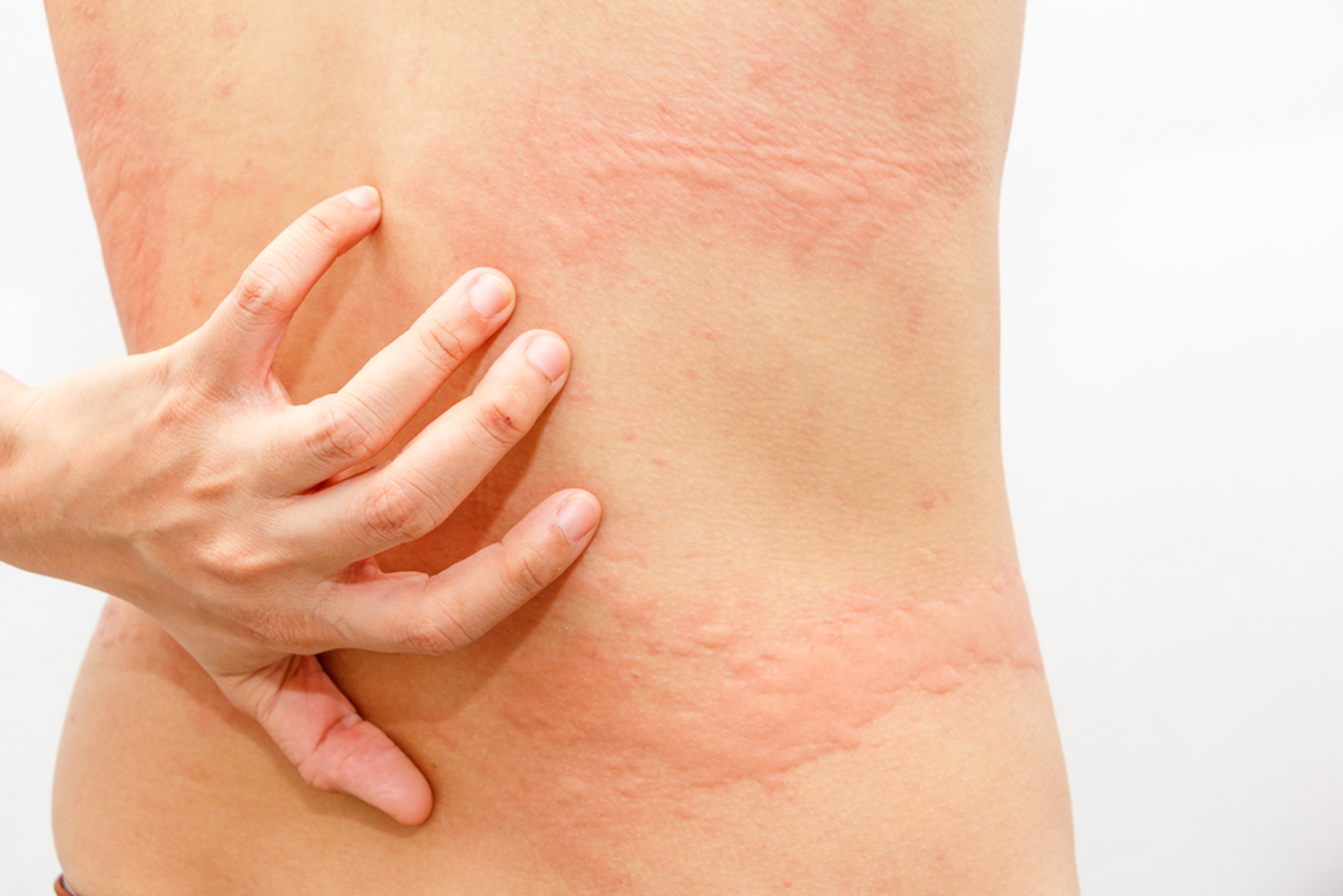
Aquagenic urticaria is a rare condition in which urticaria (hives) develop rapidly after the skin comes in contact with water, regardless of its temperature 1. Aquagenic urticaria was first described in 1964 by Shelly and Rawnsley 2.
It most commonly affects women and symptoms often start around the onset of puberty 3. Some patients report itching too.
Most cases of aquagenic urticaria are sporadic, but several familial cases have been reported 4. Symptoms develop within 30 minutes after contact with water regardless of its temperature or source. The pruritic small wheals surrounded by erythema usually last less than 1 hour. Some patients report additional, systemic symptoms such as headache, lightheadedness, respiratory distress, and palpitations, but these are usually rare 4.
Two criteria are important for a correct diagnosis of this disease: excluding other causes of physical urticaria, and a positive water challenge test 5. This test is done by applying a water-drenched compress at 37 ºC to skin, preferably on the thorax, for 20 minutes. In patients with aquagenic urticaria, the test is positive when urticariform lesions appear, confirming the diagnosis 6.
The exact underlying cause of aquagenic urticaria is currently still unknown, but the interaction of water with unknown components in the epidermis or dermis might cause histamine release from sensitized dermal mast cells, which in turn leads to wheal formation 7, 8, 9. It has been suggested that water interacting with sebum or sebaceous glands can produce a toxin causing degranulation of mast cells, leading to histamine release and wheal formation. An alternative explanation has been that water-soluble antigens in the epidermis diffuse into the dermis and cause a histamine mediated reaction. Other mediators, such as acetylcholine, serotonin, and bradikynin may also be involved in the pathogenesis of aquagenic urticaria 10, 11, 12.
Although almost all cases of aquagenic urticaria are sporadic, there are a small number of familial cases in the medical literature 13. Some of these cases have been reported in association with other conditions, a few of which are genetically linked. For example, Pitarch et al. 13 published a case of three affected female siblings all with co-existent. Bernard-Soulier Syndrome, a rare autosomal recessive disorder causing a prolonged bleeding time for which more than 30 mutations of the GPIbα, GPIbβ and GPIX genes have been described 14. These genes map to chromosomes 17p12, 22q11.2 and 3q21 respectively. They postulated that although the association could be a coincidence, it might constitute an association of genetic loci.
Treudler er al 15 reported an association of familial aquagenic urticaria with familial lactose intolerance over three generations. They described a male patient with aquagenic urticaria whose grandmother, mother, aunt and cousin were all affected. The patient, mother and grandmother were also affected by familial lactose intolerance. Familial lactose intolerance is caused by a deficiency of the enzyme lactase which is encoded on chromosome 2, a different genetic locus to the mutations causing Bernard-Soulier syndrome (chromosomes 17, 22 and 3).
Due to the rarity of the condition, there is very limited data regarding the effectiveness of individual treatments; however, various medications and therapies have been used with variable success 16, 17.
It is characterized by small punctate wheals on the area of skin in contact with the water.
Figure 1. Aquagenic urticaria
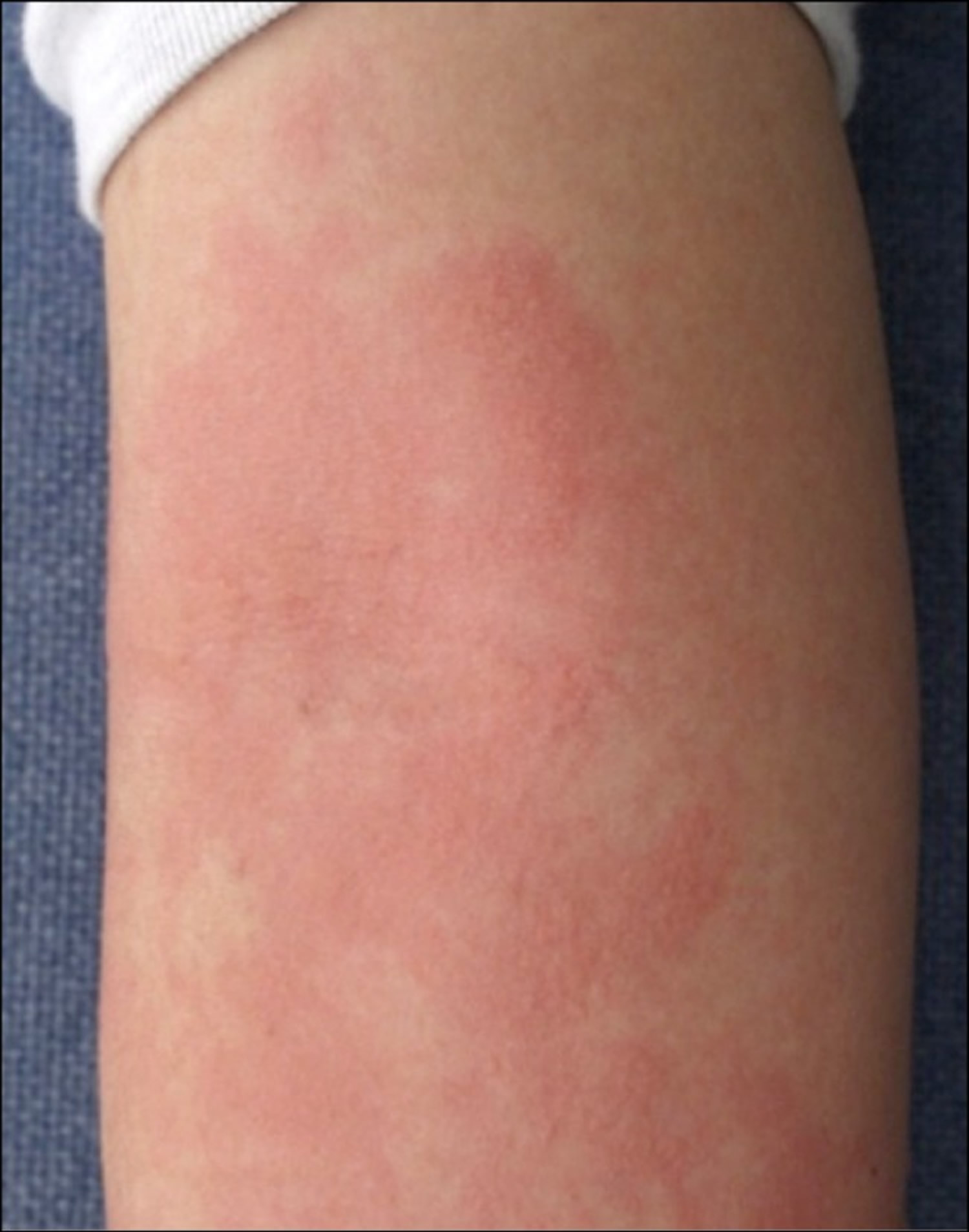
Note: Multiple small wheals with surrounding erythema were seen on the right forearm after applying a towel soaked in tap water at body temperature for 5 minutes.
Aquagenic urticaria facts
In addition to the patient’s history, the diagnosis relies on the results of the water provocation test. Magerl et al. 18 recommended applying a wet cloth at body temperature onto an area of the skin for 20 minutes. Because aquagenic urticaria may be associated with other types of physical urticaria, such as dermographism 19, cholinergic urticaria 20 and cold urticaria 21, 22, 23, 24, these condition should be excluded, especially cholinergic urticaria, in which the wheals are similar morphologically 4. Previously reported cases of aquagenic urticaria are described in Table 1.
Table 1. Reported cases of aquagenic urticaria in the literature
| No. | Sex | Age (yr) | Visit time from onset | Atopy or urticaria history | Family history | Biopsy | Successful treatment (time to remission) |
|---|---|---|---|---|---|---|---|
| 1 | F | 27 | 18 yr | (−) | Brother | (−) | Avoidance (N/A) |
| 2 | F | 24 | 2 yr | (−) | (−) | (−) | Avoidance (N/A) |
| 3 | M | 49 | 3 yr | (−) | (−) | (−) | N/A |
| 44 | F | 30 | 1 yr | (−) | (−) | (−) | Promethazine, chlorpheniramine, hydroxyzine, petrolatum oint, scopolamine 9% sol (N/A) |
| 54 | F | 14 | 1.5 yr | (−) | (−) | (−) | Promethazine, chlorpheniramine, hydroxyzine, petrolatum oint, scopolamine 9% sol (N/A) |
| 63 | F | 29 | 15 yr | AC, AR, AU | Sisters | (−) | Terfenadine (N/A) |
| 73 | F | 17 | 2 yr | (−) | (−) | Terfenadine (N/A) | |
| 81 | F | 15 | N/A | (−) | (−) | (−) | Chlorpheniramine (N/A) |
| 91 | F | 17 | 4 yr | (−) | Father | (−) | N/A |
| 10 | M | 20 | 2.5 yr | Asthma, DG | (−) | (−) | N/A |
| 11 | F | 30 | 23 yr | DG | (−) | (−) | Clemastine 1 mg or tritoqualine 100 mg (N/A) |
| 12 | F | 40 | 33 yr | (−) | (−) | (−) | N/A |
| 13 | F | 30 | 5 yr | (−) | (−) | (−) | Hydroxyzine 10 mg, cyproheptadine 4 mg (N/A) |
| 14 | M | 55 | 1 yr | DG | (−) | (−) | Hydroxyzine 25 mg (N/A) |
| 15 | F | 33 | 4 yr | Father | (−) | PUVA (2 wk) | |
| 16 | M | 3 | <1 h | (−) | (−) | (−) | Dimetindene 15 drops (N/A) |
| 17 | F | 21 | 3 yr | (−) | (−) | (−) | Astemizole 10 mg/d (N/A) |
| 18 | M | 7 | 2 mo | Asthma, AR, DG | (−) | (−) | UVB (22 wk), cyproheptadine 6 mg/d+hydroxyzine 75 mg/d (N/A) |
| 19 | F | 11 | 6 mo | ChU | (−) | (−) | Hydroxyzine 25 mg (1 wk) |
| 20 | M | 29 | 6 mo | (−) | (−) | (−) | Hydroxyzine 20 mg (15 d) |
| 21 | M | 20 | 10 yr | (−) | (−) | (−) | Avoidance (N/A) |
| 22 | M | 17 | 10 mo | (−) | (−) | (−) | Desloratadine (9 mo) |
| 23 | M | 15 | 3 mo | (−) | (−) | (−) | Desloratadine (3 mo) |
| 24 | M | 11 | From baby | (−) | (−) | (−) | Hydroxyzine 50~75 mg/d (1 mo) |
| 25 | F | 40 | 7 mo | (−) | (−) | (−) | Fexofenadine 360~540 mg/d (N/A) |
| 2612 | M | 18 | 3 yr | (−) | Brother | (−) | Cetirizine 10 mg/d (N/A) |
| 27 | M | 18 | 3 yr | (−) | Brother | (−) | Cetirizine 10 mg/d (N/A) |
| 28 | M | 13 | 1 yr | (−) | (−) | (−) | Petrolatum cream (immediately) |
| 29 | F | 28 | 4 yr | (−) | Father, brother, sister, daughter | (−) | Refusal of treatment |
| 30* | F | 1 | From birth | (−) | See No. 29 | (−) | Refusal of treatment |
| 31 | M | 19 | 6 yr | (−) | (−) | (−) | Terfenadine 60 mg+mequitazine 6 mg+topical 1% diphenhidramine oint(partial improvement) (N/A) |
| 32 | F | 21 | 2 yr | (−) | (−) | (−) | Levocetirizine 5 mg (N/A) |
| 33 | F | 21 | 1 mo | (−) | (−) | (−) | N/A |
| 34 | F | 36 | 1 mo | CoU | (−) | (−) | Treatment failure (hydroxyzine, chloropheniramine, cimetidine, prednisolone, mequtazine, cyproheptadine, montelukast, fexofenadine, petrolatum oint) |
| 35 | M | 19 | 3 yr | (−) | (−) | (−) | Fexofenadine 180 mg (2 wk) |
| 36 | M | 4 | 1 yr | (−) | (−) | (−) | Ketotifen syrup 10 ml (4 wk) |
| Our case | M | 18 | 1 wk | (−) | (−) | Done | Bepotastine (5 mo) |
F: female, N/A: not available, M: male, AC: allergic conjunctivitis, AR: allergic rhinitis, AU: acute urticaria, DG: dermographism, PUVA: psoralen plus ultraviolet A, UVB: ultraviolet B, ChU: cholinergic urticaria, CoU: cold urticarial. *A daughter of case No. 29.
Many of these histopathologic findings are the same as those of acute urticaria, in which interstitial dermal edema, dilated venules, endothelial swelling, and sparse infiltration of inflammatory cells have been described 25. Mast cells are concentrated around the blood vessels of normal dermis, with one to three cells per cross-sectional vessel profile 26.
Aquagenic urticaria symptoms
Itchy wheals usually develop within 30 to 60 minutes of contact with water, irrespective of the temperature. The differential diagnosis should be made with cholinergic urticaria and cold urticaria 6. In cholinergic urticaria wheals develop in response to heat, exertion, sweating or emotional stress 27. Lesions form in cold urticaria when the patient is exposed to low temperatures 28. The challenge test with ice is negative in aquagenic urticaria, which excludes cold urticaria. Lesions do not arise only with increased temperatures, as occurs in cholinergic urticaria.
Aquagenic urticaria treatment
Antihistamines are the first line treatment for aquagenic urticaria 29. In recalcitrant cases, the dose can be increased by as much as four-fold the conventional dose 29. Phototherapy and barrier cream are alternative or additional treatments if antihistamines fail to prevent recurrence 30. The efficacy of phototherapy is related to its induction of both immunosuppression, including a decreased mast cell response, and epidermal thickening, which disturbs the penetration of water and thus also inhibits mast cell stimulation 31. Barrier cream prevents the penetration of water into the dermis. However, the various emollients and water-resistant creams investigated have not yielded conspicuous success 32, except in a few cases in which a petrolatum-containing ointment was applied before water exposure 32. Anticholinergics such as scopolamine may also offer relief 33. Most of the patients were successfully controlled with antihistamines, although some of them changed treatment modalities because of drowsiness.
Barrier methods involving application of oil-in-water emulsion creams on the skin for water protection are effective 34.
The most common medications for urticaria include 35:
- Sleep-causing (sedating) type-1 antihistamines such as diphenhydramine, hydroxyzine, or cetirizine
- Non-sleep-causing (non-sedating) type-1 antihistamines such as loratadine, fexofenadine, or desloratadine
- Type-2 antihistamines such as anitidine, cimetidine, or famotidine.
Refractory cases have been treated with ultraviolet (UV) radiation (both psoralen plus UVA therapy and UVB), either alone or in combination with antihistamines. It is hypothesized that the effect of ultraviolet therapy is mediated by thickening of the epidermis, which may prevent water penetration, interaction with dendritic cells, and immunosuppression or a decreased mast cell response 36, 37.
- Aquagenic urticaria. https://rarediseases.info.nih.gov/diseases/10901/aquagenic-urticaria[↩]
- AQUAGENIC URTICARIA. CONTACT SENSITIVITY REACTION TO WATER. SHELLEY WB, RAWNSLEY HM. JAMA. 1964 Sep 21; 189():895-8. https://jamanetwork.com/journals/jama/article-abstract/1164601). Aquagenic urticaria is a rare variant of physical urticaria induced by direct contact with water, regardless of its temperature or source ((Aquagenic urticaria in 2 adolescents. Yavuz ST, Sahiner UM, Tuncer A, Sackesen C. J Investig Allergol Clin Immunol. 2010; 20(7):624-5. http://www.jiaci.org/issues/vol20issue7/14-22.pdf[↩]
- Seol JE, Kim DH, Park SH, Kang JN, Sung HS, Kim H. Aquagenic Urticaria Diagnosed by the Water Provocation Test and the Results of Histopathologic Examination. Annals of Dermatology. 2017;29(3):341-345. doi:10.5021/ad.2017.29.3.341. https://www.ncbi.nlm.nih.gov/pmc/articles/PMC5438944/[↩][↩]
- Yavuz ST, Sahiner UM, Tuncer A, Sackesen C. Aquagenic urticaria in 2 adolescents. J Investig Allergol Clin Immunol. 2010;20:624–625. http://www.jiaci.org/issues/vol20issue7/14-22.pdf[↩][↩][↩]
- Parker RK, Crowe MJ, Guin JD. Aquagenic urticaria. Cutis. 1992;50:283-4.[↩]
- Black AK, Lawlon F, Greaves MW. Consensus meeting on the definition of physical urticarias and urticarial vasculitis. Clin Exp Dermatol. 1996;21:424-6.[↩][↩]
- Shelly WB, Rawnsley HM. Aquagenic urticaria. Contact sensitivity reaction to water. JAMA. 1964;189:895–898. https://jamanetwork.com/journals/jama/article-abstract/1164601[↩]
- Czarnetzki BM, Breetholt KH, Traupe H. Evidence that water acts as a carrier for an epidermal antigen in aquagenic urticaria. J Am Acad Dermatol. 1986;15:623–627. https://www.ncbi.nlm.nih.gov/pubmed/2429997[↩]
- Sibbald RG, Black AK, Eady RA, James M, Greaves MW. Aquagenic urticaria: evidence of cholinergic and histaminergic basis. Br J Dermatol. 1981;105:297–302. https://www.ncbi.nlm.nih.gov/pubmed/7272209[↩]
- Frances AM, Fiorenza G, Frances RJ. Aquagenic urticária: report of a case. Allergy Asthma Proc. 2004;25:195-7.[↩]
- Medeiros M Jr. Aquegenic urticaria. J Investig Allergol Clin Immunol. 1996;6:63-4.[↩]
- Sibbad RG, Black AK, Eady RA, James M, Greaves MW. Aquagenic urticaria: evidence of cholinergic and histaminergic basis. Br J Dermatol. 1981;105:297-302.[↩]
- Pitarch G, Torrijos A, Martínez-Menchón T, Sánchez-Carazo JL, Fortea JM. Familial aquagenic urticaria and bernard-soulier syndrome. Dermatology. 2006;6(1):96–7. doi: 10.1159/000089035. https://www.karger.com/Article/Abstract/89035[↩][↩]
- Kunishima S, Kamiya T, Saito H. Genetic abnormalities of Bernard-Soulier syndrome. Int J Hematol. 2002;6(4):319–27. doi: 10.1007/BF02982690. https://www.ncbi.nlm.nih.gov/pubmed/12463594[↩]
- Treudler R, Tebbe B, Steinhoff M, Orfanos CE. Familial aquagenic urticaria associated with familial lactose intolerance. J Am Acad Dermatol. 2002;6(4):611–3. doi: 10.1067/mjd.2002.124599. https://www.ncbi.nlm.nih.gov/pubmed/12271310[↩]
- Dice JP & Gonzalez-Reyes E. Physical urticarias. UpToDate. March, 2016.[↩]
- Park H, Kim HS, Yoo DS, et al. Aquagenic Urticaria: A Report of Two Cases. Annals of Dermatology. 2011;23(Suppl 3):S371-S374. doi:10.5021/ad.2011.23.S3.S371. https://www.ncbi.nlm.nih.gov/pmc/articles/PMC3276800/[↩]
- Magerl M, Borzova E, Giménez-Arnau A, Grattan CE, Lawlor F, Mathelier-Fusade P, et al. The definition and diagnostic testing of physical and cholinergic urticarias–EAACI/GA2LEN/EDF/UNEV consensus panel recommendations. Allergy. 2009;64:1715–1721. https://www.ncbi.nlm.nih.gov/pubmed/19793059[↩]
- Bonnetblanc JM, Andrieu-Pfahl F, Meraud JP, Roux J. Familial aquagenic urticaria. Dermatologica. 1979;158:468–470. https://www.ncbi.nlm.nih.gov/pubmed/38152[↩]
- Davis RS, Remigio LK, Schocket AL, Bock SA. Evaluation of a patient with both aquagenic and cholinergic urticaria. J Allergy Clin Immunol. 1981;68:479–483. https://www.ncbi.nlm.nih.gov/pubmed/7310013[↩]
- Kim CH, Ryu ST, Park SW, Lee JH, Oh WS, Chang SI, et al. A case of the coexistence of cold urticaria and aquagenic urticaria. Korean J Asthma Allergy Clin Immunol. 2004;24:350–352.[↩]
- Gimenez-Arnau A, Serra-Baldrich E, Camarasa JG. Chronic aquagenic urticaria. Acta Derm Venereol. 1992;72:389. https://www.ncbi.nlm.nih.gov/pubmed/1361294[↩]
- Luong KV, Nguyen LT. Aquagenic urticaria: report of a case and review of the literature. Ann Allergy Asthma Immunol. 1998;80:483–485. https://www.ncbi.nlm.nih.gov/pubmed/9647271[↩]
- Parker RK, Crowe MJ, Guin JD. Aquagenic urticaria. Cutis. 1992;50:283–284. https://www.ncbi.nlm.nih.gov/pubmed/1424795[↩]
- Mobini N, Toussaint S, Kamino H. Noninfectious erythematous, papular, and squamous diseases. In: Elder DE, Elenitsas R, Johnson BL Jr, Murphy GF, Xu X, editors. Lever’s histopathology of the skin. 10th ed. Philadelphia: Lippincott Williams & Wilkins; 2008. pp. 169–203.[↩]
- Velazquez EF, Murphy GF. Introduction to dermatopathologic diagnosis. In: Elder DE, Elenitsas R, Johnson BL Jr, Murphy GF, Xu X, editors. Lever’s histopathology of the skin. 10th ed. Philadelphia: Lippincott Williams & Wilkins; 2008. pp. 7–66.[↩]
- Tromovitch TA. Urticaria from contact with water. Calif Med. 1967;106:400-1.[↩]
- Shelley WB, Rawnsley HM. Aquagenic urticaria. JAMA. 1964;189:119-22[↩]
- Kai AC, Flohr C. Aquagenic urticaria in twins. The World Allergy Organization Journal. 2013;6(1):2. doi:10.1186/1939-4551-6-2. https://www.ncbi.nlm.nih.gov/pmc/articles/PMC3646536/[↩][↩]
- Juhlin L, Malmros-Enander I. Familial polymorphous light eruption with aquagenic urticaria: successful treatment with PUVA. Photodermatol. 1986;3:346–349. https://www.ncbi.nlm.nih.gov/pubmed/3588355[↩]
- Gollhausen R, Kaidbey K, Schechter N. UV suppression of mast cell-mediated wealing in human skin. Photodermatol. 1985;2:58–67. https://www.ncbi.nlm.nih.gov/pubmed/4041035[↩]
- McGee JS, Kirkorian AY, Pappert AS, Milgraum SS. An adolescent boy with urticaria to water: review of current treatments for aquagenic urticaria. Pediatr Dermatol. 2014;31:116–117. https://www.ncbi.nlm.nih.gov/pubmed/22994854[↩][↩]
- Seize MB, Ianhez M, de Souza PK, Rotta O, Cestari Sda C. Familial aquagenic urticaria: report of two cases and literature review. An Bras Dermatol. 2009;84:530–533. https://www.ncbi.nlm.nih.gov/pubmed/20098859[↩]
- Bayle P, Gadroy A, Messer L, Bazex J. Localized aquagenic urticaria: efficacy of a barrier cream. Contact Dermatitis. 2003;49:160–161. https://www.ncbi.nlm.nih.gov/pubmed/14678215/[↩]
- Hives (Urticaria). https://www.skinsight.com/skin-conditions/child/urticaria-hives[↩]
- Dice JP. Physical urticaria. Immunol Allergy Clin North Am. 2004;24:225–246. https://www.ncbi.nlm.nih.gov/pubmed/15120149[↩]
- Martínez-Escribano JA, Quecedo E, De la Cuadra J, Frías J, Sánchez-Pedreño P, Aliaga A. Treatment of aquagenic urticaria with PUVA and astemizole. J Am Acad Dermatol. 1997;36:118–119. https://www.ncbi.nlm.nih.gov/pubmed/8996279[↩]