Contents
What is arthralgia
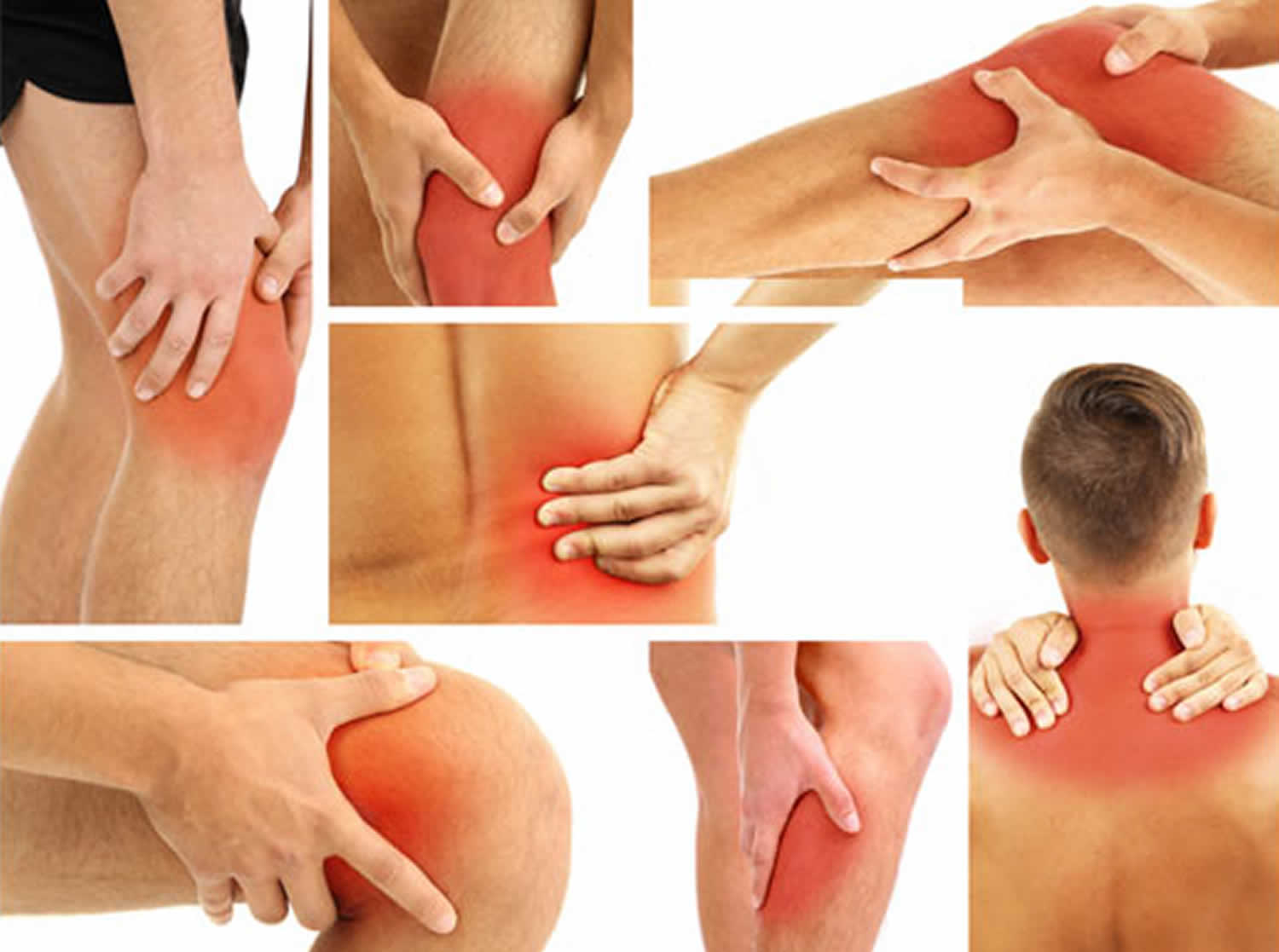
Arthralgia means joint pain or pain in the joint. Polyarthralgia means pain in several joints (two or more for the purposes of this discussion). Arthralgia can be discomfort, pain or inflammation arising from any part of a joint — including cartilage, bone, ligaments, tendons or muscles. Most commonly, however, joint pain refers to arthritis, which is inflammation or pain from within the joint itself.
Arthralgia can be mild, causing soreness only after certain activities, or it can be severe, making even limited movement, particularly bearing weight, extremely painful.
Arthralgia and swelling can affect any joint in the body, and is often accompanied by stiffness, aches and a feeling of heat or warmth.
Arthralgia and swelling can be either acute or chronic.
Acute arthralgia usually comes on quickly and lasts a short while. Some frequent causes of acute joint pain include:
- injury, such as sprains and strains
- overuse of the joint
- infection
- other illnesses, such as the flu.
Chronic conditions come on slowly and cause long-term problems. Some types of arthralgia and swelling may be caused by a rheumatic (or other) underlying condition.
The word ‘rheumatic’ refers to aches and pains affecting your joints, bones and muscles. While there are more than 200 different kinds of rheumatic conditions (including gout and lupus, the most common is arthritis, which means inflammation (swelling) of the joints. Arthritis can affect people of any age, not just elderly people. However, it’s important to remember that having arthralgia and swelling doesn’t always mean that you have arthritis.
Anyone who experiences pain and swelling in one or more joints should discuss this with their doctor. If you have chronic joint pain and swelling, your doctor will be able to assess your situation.
Arthralgia can be caused by many types of injuries or conditions. Arthralgia may be linked to arthritis, bursitis, and muscle pain. No matter what causes it, joint pain can be very bothersome. Some things that can cause joint pain are:
- Autoimmune diseases such as rheumatoid arthritis and lupus
- Bursitis
- Chondromalacia patellae
- Crystals in the joint — gout (especially found in the big toe) and CPPD arthritis (pseudogout)
- Infections caused by a virus
- Injury, such as a fracture
- Osteoarthritis
- Osteomyelitis (bone infection)
- Septic arthritis (joint infection)
- Tendinitis
- Unusual exertion or overuse, including strains or sprains
Signs of joint inflammation include:
- Swelling
- Warmth
- Tenderness
- Redness
- Pain with movement
Contact your doctor if:
- You have fever that is not associated with flu symptoms.
- You have lost 10 pounds (4.5 kilograms) or more without trying (unintended weight loss).
- Your joint pain lasts for more than several days.
- You have severe, unexplained joint pain and swelling, particularly if you have other unexplained symptoms.
Arthralgia vs Arthritis
Arthritis is inflammation of one or more of your joints. Arthritis is very common cause of arthralgia or joint disease. Arthritis is not a single disease, there are more than 100 different types of arthritis and related conditions. The most common types of arthritis are osteoarthritis and rheumatoid arthritis. People of all ages, sexes and races can and do have arthritis, and it is the leading cause of disability in America. More than 50 million adults and 300,000 children have some type of arthritis. Arthritis is most common among women and occurs more frequently as people get older.
The main symptoms of arthritis are joint pain, stiffness, swelling and decreased range of motion. Symptoms may come and go. They can be mild, moderate or severe. They may stay about the same for years, but may progress or get worse over time. Severe arthritis can result in chronic pain, inability to do daily activities and make it difficult to walk or climb stairs. Arthritis can cause permanent joint changes. These changes may be visible, such as knobby finger joints, but often the damage can only be seen on X-ray. Some types of arthritis also affect the heart, eyes, lungs, kidneys and skin as well as the joints.
Diagnosing arthritis
Arthritis diagnosis often begins with a primary care physician, who performs a physical exam and may do blood tests and imaging scans to help determine the type of arthritis. An arthritis specialist, or rheumatologist, should be involved if the diagnosis is uncertain or if the arthritis may be inflammatory. Rheumatologists typically manage ongoing treatment for inflammatory arthritis, gout and other complicated cases. Orthopaedic surgeons do joint surgery, including joint replacements. When the arthritis affects other body systems or parts, other specialists, such as ophthalmologists, dermatologists or dentists, may also be included in the health care team.
There are different types of arthritis:
- Adult-onset Still’s disease
- Ankylosing Spondylitis: Ankylosing spondylitis is a condition that mainly affects the spine. The joints of the neck, back and pelvis become inflamed, causing pain and stiffness. Other joints, such as the hips and shoulders, and other areas of the body such as the eyes, skin, bowel and lungs, can also be involved. Symptoms of ankylosing spondylitis usually begin between the ages of 15 and 45 years.
- Back Pain
- Behçet’s Disease
- Bursitis
- Calcium Pyrophosphate Deposition Disease (CPPD)
- Carpal Tunnel Syndrome
- Chondromalacia Patella
- Chronic Fatigue Syndrome
- Complex Regional Pain Syndrome
- Chronic recurrent multifocal osteomyelitis: Chronic recurrent multifocal osteomyelitis is a disease affecting the bones. Inflammation is normally one of the body’s protective responses to infection or injury, but in diseases such as chronic recurrent multifocal osteomyelitis, uncontrolled inflammation can cause damage. In chronic recurrent multifocal osteomyelitis, inflammation targets the bone and can occur throughout the body.
- Cryopyrin-Associated Periodic Syndromes (CAPS)
- Degenerative Disc Disease
- Developmental-Dysplasia of Hip
- Diffuse Idiopathic Skeletal Hyperostosis
- Ehlers-Danlos
- Familial Mediterranean Fever: Familial Mediterranean fever is a disease that results in episodes of fever, abdominal pain, chest pain, joint pain and rashes. Familial Mediterranean fever is most common in people of Mediterranean and Middle Eastern ancestry, but can occur in people of any ethnicity.
- Fibromyalgia: Fibromyalgia is a name given to a common group of symptoms marked by generalized pain and muscle stiffness, as well as extreme fatigue.These may range from very mild to severe, and may last for many years or come and go at different times. With the right advice most people find they learn to manage the pain and tiredness over time.
- Fifth Disease
- Giant Cell Arteritis
- Gout: Gout is a common and painful condition that affects the joints. Small crystals form in and around the joint, causing inflammation, pain and swelling. An attack of gout usually comes on very quickly, often overnight. The joint becomes very red, swollen and extremely painful. Gout normally affects one joint at a time, often the joint of the big toe.
- Granulomatosis with Polyangiitis
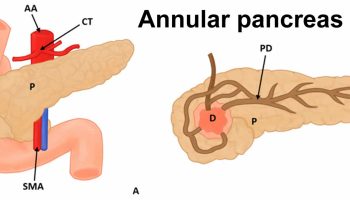
- Hemochromatosis: Haemochromatosis is a condition caused by a build-up of iron in your body. People with haemochromatosis absorb too much iron from food (iron overload) and the extra iron can damage organs, particularly the liver, heart, pancreas, bones and joints.
- Infectious Arthritis
- Inflammatory Arthritis
- Inflammatory Bowel Disease
- Juvenile Arthritis
- Juvenile Dermatomyositis (JD): Juvenile dermatomyositis is a rare condition that causes inflammation of the skin and muscle. Inflammation is one of the body’s protective responses to infection or injury, but in diseases such as juvenile dermatomyositis, uncontrolled inflammation can cause damage. Other parts of the body may also be affected such as the lung and intestines.
- Juvenile Idiopathic Arthritis (JIA): Juvenile idiopathic arthritis (JIA) is the name given to a number of types of arthritis that occur in children. Scientists do know that juvenile idiopathic arthritis (JIA) is an autoimmune condition. This means the body’s immune system (its protective mechanism against infection) starts to mistakenly attack healthy cells of the body.
- Juvenile Scleroderma
- Kawasaki Disease
- Lupus
- Lupus in Children & Teens
- Lyme Disease
- Mixed Connective Tissue Disease
- Myositis (include Polymyositis and Dermatomyositis)
- Non-radiographic Axial Spondyloarthritis: Non-radiographic Axial Spondyloarthritis is an autoimmune disease which causes arthritis in the spine and pelvis. While ‘non-radiographic Axial Spondyloarthritis’ is a very complicated name, it can be understood as: Non-radiographic: the inflammation will not show up on an x-ray (radiograph) but may show up on an MRI (magnetic resonance imaging).
- Osteoarthritis
- Osteoporosis
- Pagets disease of bone
- Palindromic Rheumatism
- Patellofemoral Pain Syndrome
- Pediatric Rheumatic Diseases
- Pediatric SLE
- Polymyalgia Rheumatica: Polymyalgia rheumatica means ‘pain in many muscles’. It is a condition that causes inflammation of the joints and tissues around the joints. This causes muscles to feel painful and stiff, especially in the shoulder, neck and hip areas. Polymyalgia rheumatica is different to fibromyalgia, a condition that does not cause inflammation.
- Pseudogout
- Psoriatic Arthritis: Psoriatic arthritis is a condition that causes inflammation of the joints. This causes the joints to become painful, stiff and often swollen. Usually only people who have a skin disease called psoriasis are affected by psoriatic arthritis.
- Raynaud’s Phenomenon
- Reactive Arthritis: Reactive arthritis is a condition that causes inflammation, pain and swelling of the joints. It usually develops after an infection, often in the bowel or genital areas. The infection causes activity in the immune system.
- Reflex Sympathetic Dystrophy
- Reiter’s Sydrome
- Rheumatic Fever
- Rheumatism
- Rheumatoid Arthritis: Rheumatoid arthritis is a common inflammatory form of arthritis, is an autoimmune disease that causes pain and swelling of the joints. In an autoimmune disease, your immune system starts attacking your own healthy tissues. In rheumatoid arthritis, the immune system targets the lining of the joints, causing inflammation and joint damage.
- Ross River virus and Barmah Forest virus are infections that are spread to humans through mosquito bites. They cause similar illnesses, including joint inflammation and pain. People of all ages are at risk of developing these infections. Ross River virus is the most common and widespread of mosquito borne diseases that infect humans in Australia.
- Scleroderma: The word ‘scleroderma’ means ‘hard skin’. Scleroderma affects the connective tissues of the body (tissues that hold together joints, muscles, blood vessels and internal organs). Symptoms vary greatly from person to person and also depend on what part of the body is involved.
- Sjögren’s Disease: Sjögren’s syndrome is an autoimmune condition. The normal role of your body’s immune system is to fight off infections and diseases to keep you healthy. In an autoimmune disease like Sjögren’s syndrome, your immune system starts attacking your own healthy tissues.
- Spinal Stenosis
- Spondyloarthritis: Spondyloarthritis (sometimes called spondyloarthropathy or seronegative arthritis) is a name for types of arthritis that commonly affect the spine.
- Systemic Juvenile Idiopathic Arthritis
- Systemic Lupus Erythematosus: Systemic lupus erythematosus (also called SLE or lupus) is an autoimmune condition. The normal role of your body’s immune system is to fight off infections and diseases to keep you healthy. In an autoimmune disease like lupus, your immune system starts attacking your own healthy tissues.
- Systemic Lupus Erythematosus in Children & Teens
- Systemic Sclerosis
- Temporal Arteritis
- Tendinitis
- Vasculitis
Degenerative arthritis
Osteoarthritis is the most common type of arthritis. Osteoarthritis affects the whole joint including bone, cartilage, ligaments and muscles. When the cartilage – the slick, cushioning surface on the ends of bones – wears away, bone rubs against bone, causing pain, swelling and stiffness. Over time, joints can lose strength and pain may become chronic. Risk factors for osteoarthritis include excess weight, family history, age and previous injury (an anterior cruciate ligament, or ACL, tear, for example). Although often described as ‘wear and tear’, this is not an accurate description of osteoarthritis. Osteoarthritis is now thought to be the result of a joint working extra hard to repair itself.
When the joint symptoms of osteoarthritis are mild or moderate, they can be managed by:
- balancing activity with rest
- using hot and cold therapies
- regular physical activity
- maintaining a healthy weight
- strengthening the muscles around the joint for added support
- using assistive devices
- taking over-the-counter (OTC) pain relievers or anti-inflammatory medicines
- avoiding excessive repetitive movements
If joint symptoms are severe, causing limited mobility and affecting quality of life, some of the above management strategies may be helpful, but joint replacement may be necessary.
Osteoarthritis can prevented by staying active, maintaining a healthy weight, and avoiding injury and repetitive movements.
Inflammatory arthritis
A healthy immune system is protective. It generates internal inflammation to get rid of infection and prevent disease. But the immune system can go awry, mistakenly attacking your joints with uncontrolled inflammation, potentially causing joint erosion and may damage internal organs, eyes and other parts of the body. Rheumatoid arthritis and psoriatic arthritis are examples of inflammatory arthritis. Researchers believe that a combination of genetics and environmental factors can trigger autoimmunity. Smoking is an example of an environmental risk factor that can trigger rheumatoid arthritis in people with certain genes.
With autoimmune and inflammatory types of arthritis, early diagnosis and aggressive treatment is critical. Slowing disease activity can help minimize or even prevent permanent joint damage. Remission is the goal and may be achieved through the use of one or more medications known as disease-modifying antirheumatic drugs (DMARDs). The goal of treatment is to reduce pain, improve function, and prevent further joint damage.
Infectious arthritis
A bacterium, virus or fungus can enter the joint and trigger inflammation. Examples of organisms that can infect joints are salmonella and shigella (food poisoning or contamination), chlamydia and gonorrhea (sexually transmitted diseases) and hepatitis C (a blood-to-blood infection, often through shared needles or transfusions). In many cases, timely treatment with antibiotics may clear the joint infection, but sometimes the arthritis becomes chronic.
Metabolic arthritis
Uric acid is formed as the body breaks down purines, a substance found in human cells and in many foods. Some people have high levels of uric acid because they naturally produce more than is needed or the body can’t get rid of the uric acid quickly enough. In some people the uric acid builds up and forms needle-like crystals in the joint, resulting in sudden spikes of extreme joint pain, or a gout attack. Gout can come and go in episodes or, if uric acid levels aren’t reduced, it can become chronic, causing ongoing pain and disability.
Arthralgia symptoms
Arthralgia means joint pain.
Depending on the type of arthritis you have, your signs and symptoms may include:
- Pain
- Stiffness
- Swelling
- Redness
- Decreased range of motion
Arthralgia diagnosis
Your doctor will ask you questions about your medical history and symptoms, including:
- Which joint hurts? Is the pain on one side or both sides?
- What started the pain and how often have you had it? Have you had it before?
- Did this pain begin suddenly and severely, or slowly and mildly?
- Is the pain constant or does it come and go? Has the pain become more severe?
- Have you injured your joint?
- Have you had an illness, rash, or fever?
- Does resting or moving make the pain better or worse? Are certain positions more or less comfortable? Does keeping the joint elevated help?
- Do medicines, massage, or applying heat reduce the pain?
- What other symptoms do you have?
- Is there any numbness?
- Can you bend and straighten the joint? Does the joint feel stiff?
- Are your joints stiff in the morning? If so, for how long does the stiffness last?
- What makes the stiffness better?
A physical exam will be done, looking for signs of joint abnormality including:
- Swelling
- Tenderness
- Warmth
- Pain with motion
- Abnormal motion such as limitation, loosening of the joint, grating sensation
Tests that may be done include:
- Complete blood count (CBC) or blood differential
- C-reactive protein (CRP)
- Joint x-ray
- Sedimentation rate (ESR)
- Blood tests specific to various autoimmune disorders
- Joint aspiration to obtain joint fluid for culture, white cell count and examination for crystals
Arthralgia treatment
Arthralgia treatment involves treating the underlying cause. For non-arthritic joint pain, both rest and exercise are important. Warm baths, massage, and stretching exercises should be used as often as possible. Acetaminophen (Tylenol) may help the soreness feel better.
Nonsteroidal anti-inflammatory drugs (NSAIDs) such as ibuprofen, indomethacin or naproxen may help relieve pain and swelling. Talk to your doctor before giving aspirin or NSAIDs such as ibuprofen to children.
Other treatments may include:
- Injection of a corticosteroid medicine into the joint
- Antibiotics and often surgical drainage, in case of infection (usually require hospitalization)
- Physical therapy for muscle and joint rehabilitation