Contents
What is Borrelia burgdorferi
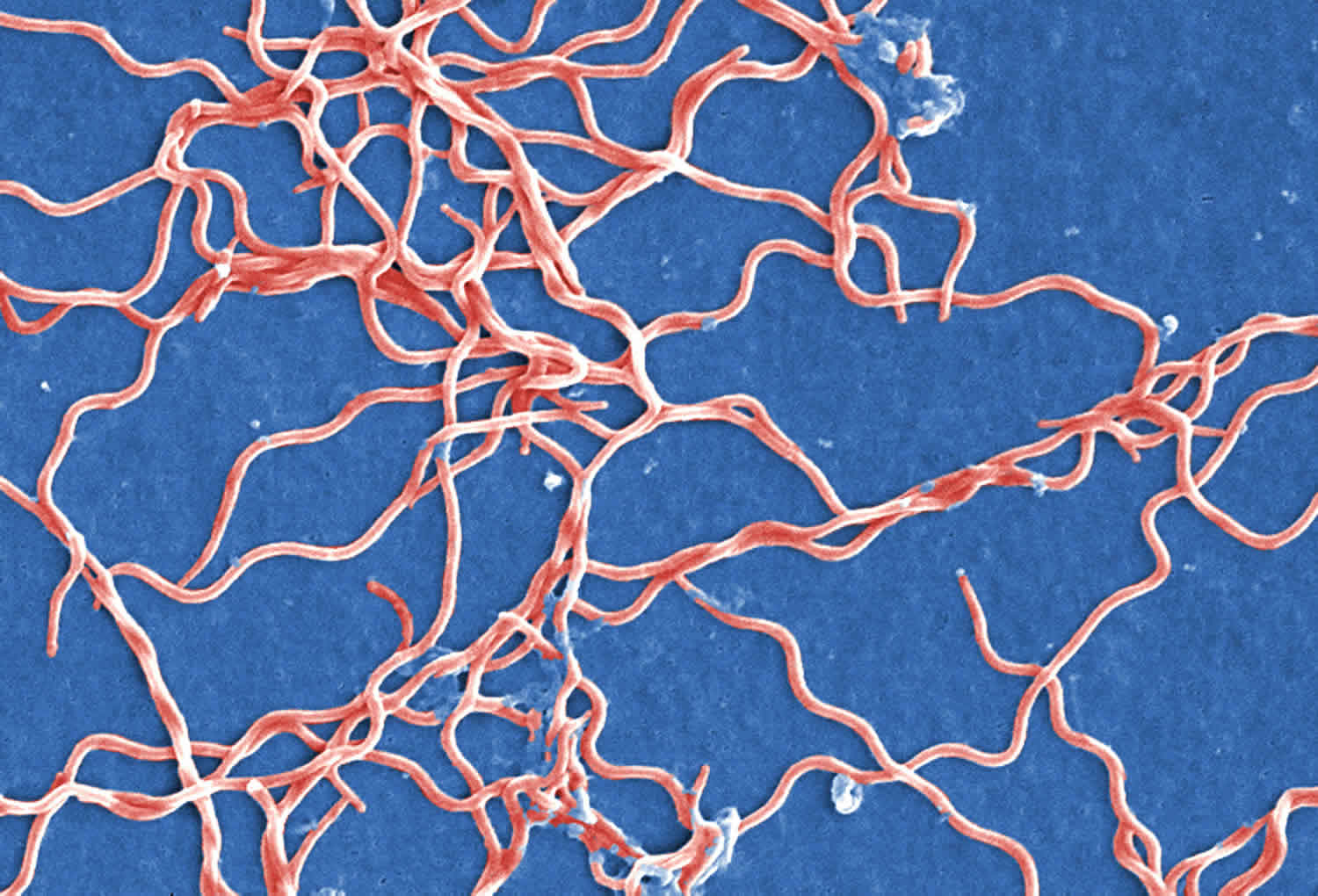
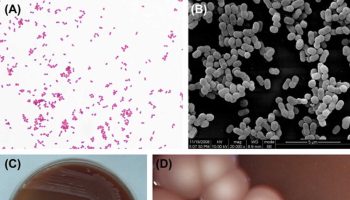
Borrelia burgdorferi is a bacterial spirochete responsible for Lyme disease and is transmitted by the bite of an infected Ixodes genus tick, mostly commonly Ixodes scapularis (also called deer tick or blacklegged tick). Borrelia burgdorferi is a member of the eubacterial phylum Spirochaetes. Members of this group of organisms share a distinctive morphology that includes a spiral or wavelike body and flagella (organs of motility) enclosed between the outer and inner membranes. Borrelia burgdorferi shape is long, twisted, and spindly, resembling pieces of noodle.
Borrelia burgdorferi causes a characteristic annular rash, arthritis, carditis, and in late stages, encephalopathy 1. In Eurasia, Lyme disease is caused by Borrelia burgdorferi, Borrelia afzelii, and Borrelia garinii 2.
Typical Borrelia burgdorferi (Lyme disease) symptoms include fever, headache, fatigue, and a characteristic skin rash called erythema migrans. If left untreated, infection can spread to joints, the heart, and the nervous system. Lyme disease is diagnosed based on symptoms, physical findings (e.g., rash), and the possibility of exposure to infected ticks. Laboratory testing is helpful if used correctly and performed with validated methods. Most cases of Lyme disease can be treated successfully with a few weeks of antibiotics. Steps to prevent Lyme disease include using insect repellent, removing ticks promptly, applying pesticides, and reducing tick habitat. The ticks that transmit Lyme disease can occasionally transmit other tickborne diseases as well.
Lyme disease, is the most common tick-borne illness in the United States. Many types of ticks bite people in the U.S., but only blacklegged ticks transmit the bacteria that cause Lyme disease 3. Furthermore, only blacklegged ticks in the highly endemic areas of the northeastern and north central U.S. are commonly infected 3. Finally, blacklegged ticks need to be attached for at least 24 hours before they can transmit Lyme disease, but in most cases, the tick must be attached for 36 to 48 hours or more before the Lyme disease bacterium can be transmitted 4. This is why it’s so important to remove them promptly and to check your body daily for ticks if you live in an endemic area.
Figure 1. Blacklegged tick (Ixodes scapularis)

The Lyme disease ticks can attach to any part of the human body but are often found in hard-to-see areas such as the groin, armpits, and scalp. Most humans are infected through the bites of immature ticks called nymphs. Nymphs are tiny (less than 2 mm) and difficult to see; they feed during the spring and summer months. Adult ticks can also transmit Lyme disease bacteria, but they are much larger and are more likely to be discovered and removed before they have had time to transmit the bacteria. Adult Ixodes ticks are most active during the cooler months of the year. In general, adult ticks are approximately the size of a sesame seed and nymphal ticks are approximately the size of a poppy seed.
Figure 2. Relative sizes of blacklegged ticks at different life stages

Each year, approximately 30,000 cases of Lyme disease are reported to CDC by state health departments and the District of Columbia and around 300,000 in the United States 5. However, this number does not reflect every case of Lyme disease that is diagnosed in the United States every year.
These ticks are typically about the size of a sesame seed. They live only in certain areas of the country:
- Northeast and mid-Atlantic (northeast Virginia to Maine)
- North central states (mostly Wisconsin and Minnesota)
- West Coast (mostly northern California)
Lyme disease can also be found in other parts of the United States. But it is rare to get it outside of where the black-legged tick lives. The disease is also found in Europe, Asia, and Australia.
Is it true that you can get Lyme disease anywhere in the U.S. ?
No. Lyme disease is spread through the bite of a blacklegged tick (Ixodes scapularis or Ixodes pacificus) that is infected with Borrelia burgdorferi. In the United States, most infections occur in the following endemic areas:
- Northeast and mid-Atlantic, from northeastern Virginia to Maine
- North central states, mostly in Wisconsin and Minnesota
- West Coast, particularly northern California
Maps showing the distribution of human cases are based on where people live, which because of travel, is not necessarily where they became infected. Cases are sometimes diagnosed and reported from an area where Lyme disease is not expected, but they are almost always travel-related.
Most people with Lyme disease develop a characteristic skin rash around the area of the bite. The rash may feel hot to touch and vary in size, shape, and color, but it will often have a “bull’s eye” appearance (a red ring with a clear center) 6. However, there are those who will not develop the rash, which can make Lyme disease hard to diagnose because its symptoms and signs mimic those of many other diseases 6.
Figure 3. Bull’s eye rash of Lyme disease (Erythema migrans rash)
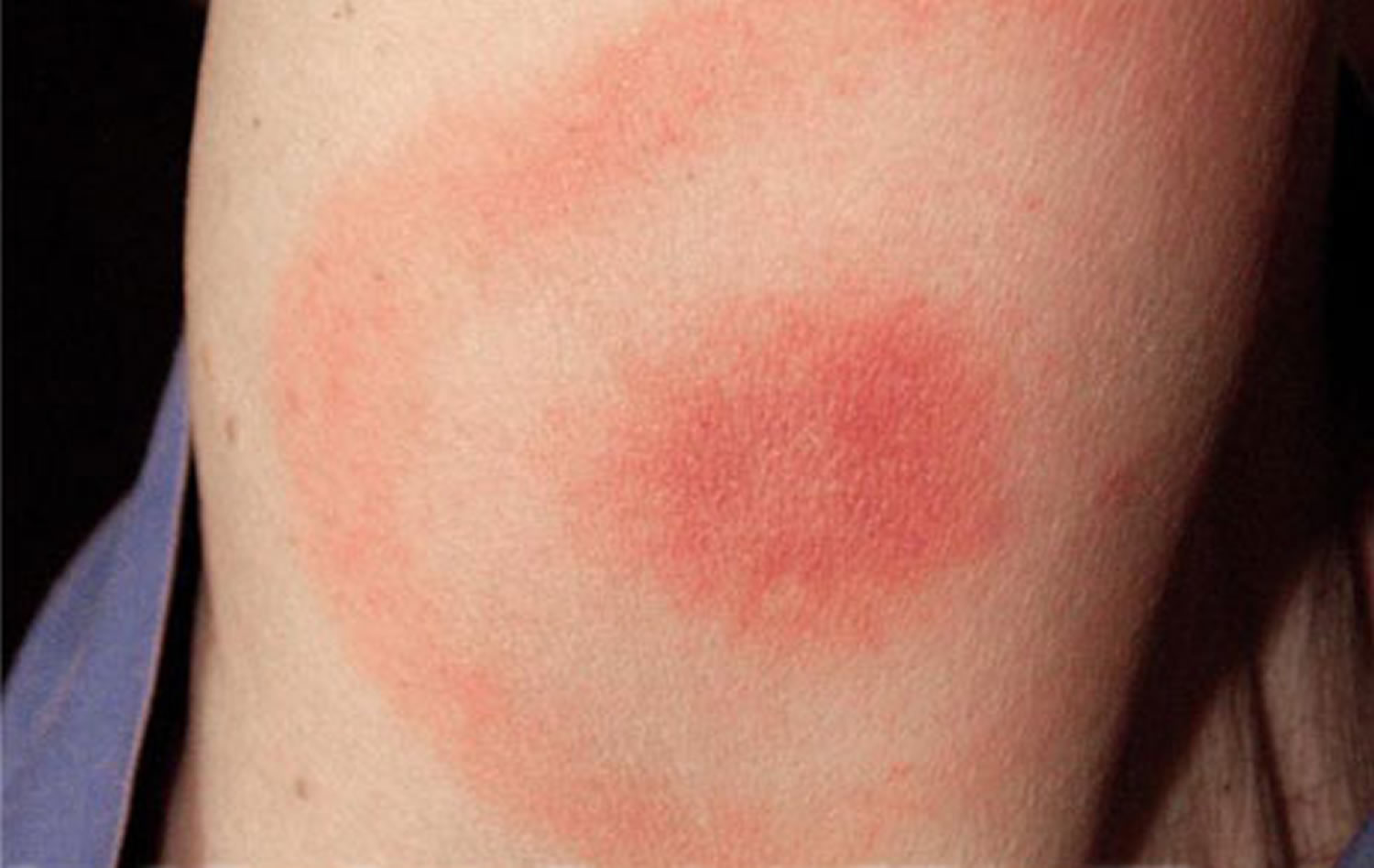
Figure 4. Expanding Lyme disease rash with central crust
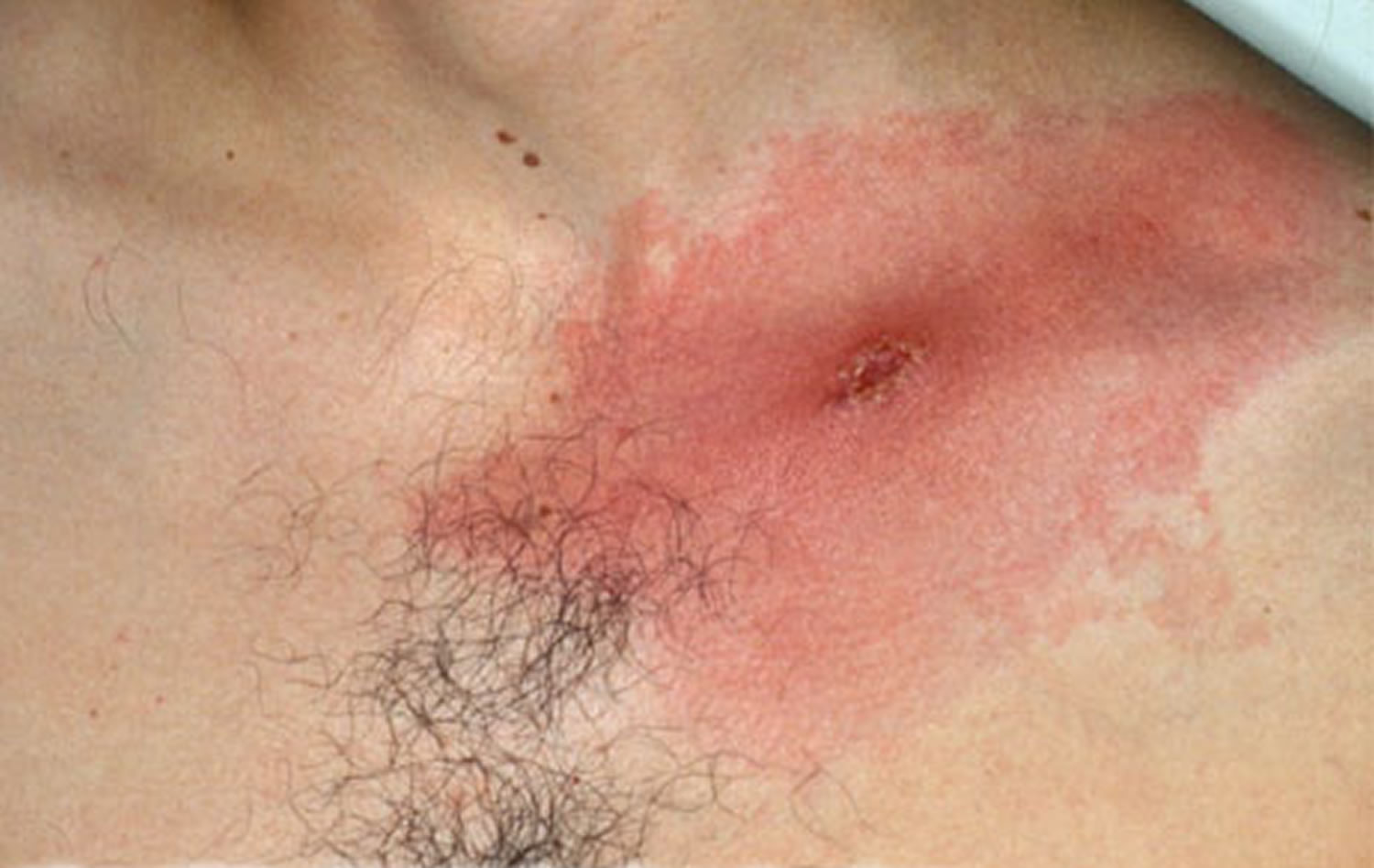
Figure 5. Multiple rashes of Lyme disease
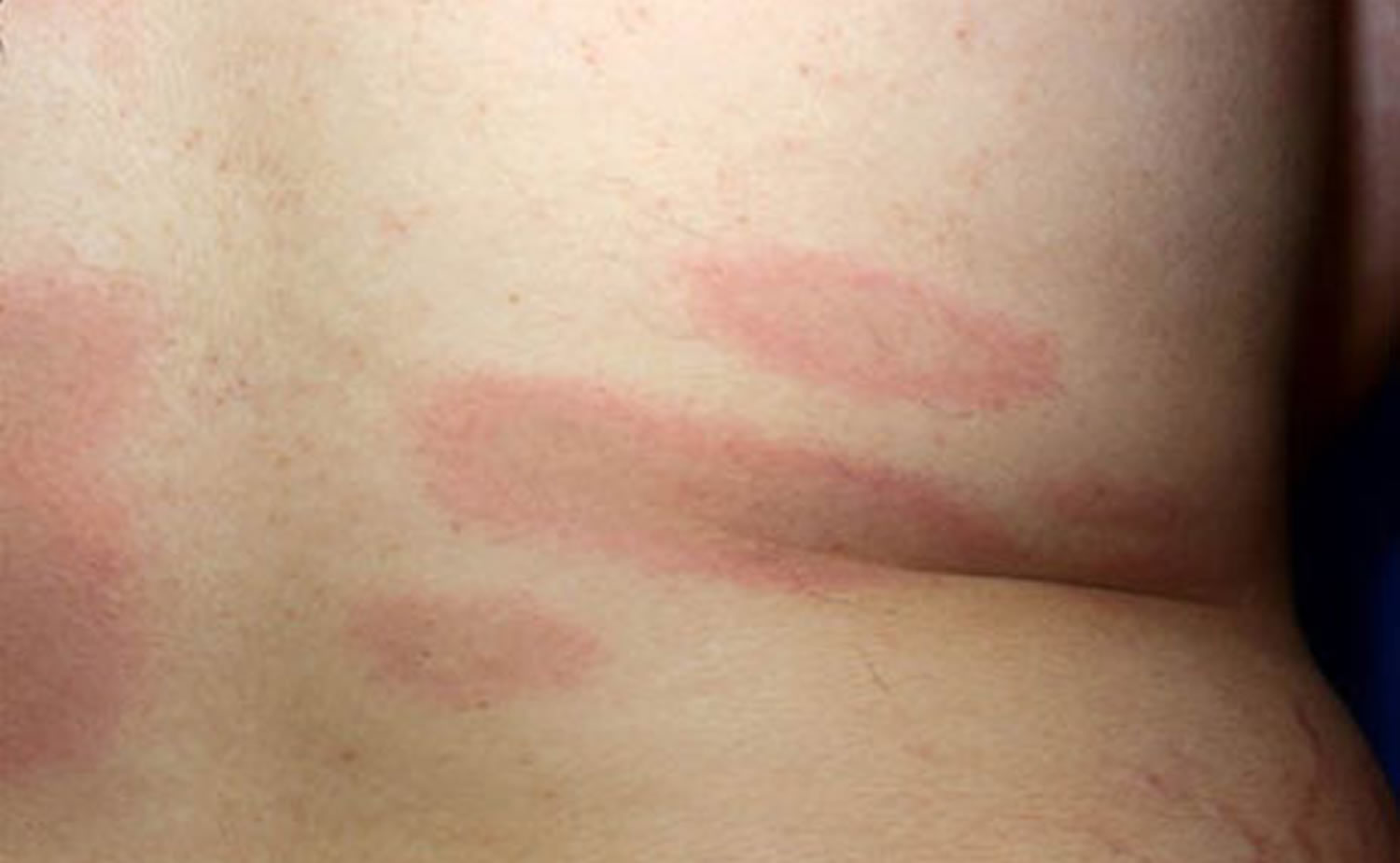
Figure 6. Lyme disease rash – bluish rash with no central clearing
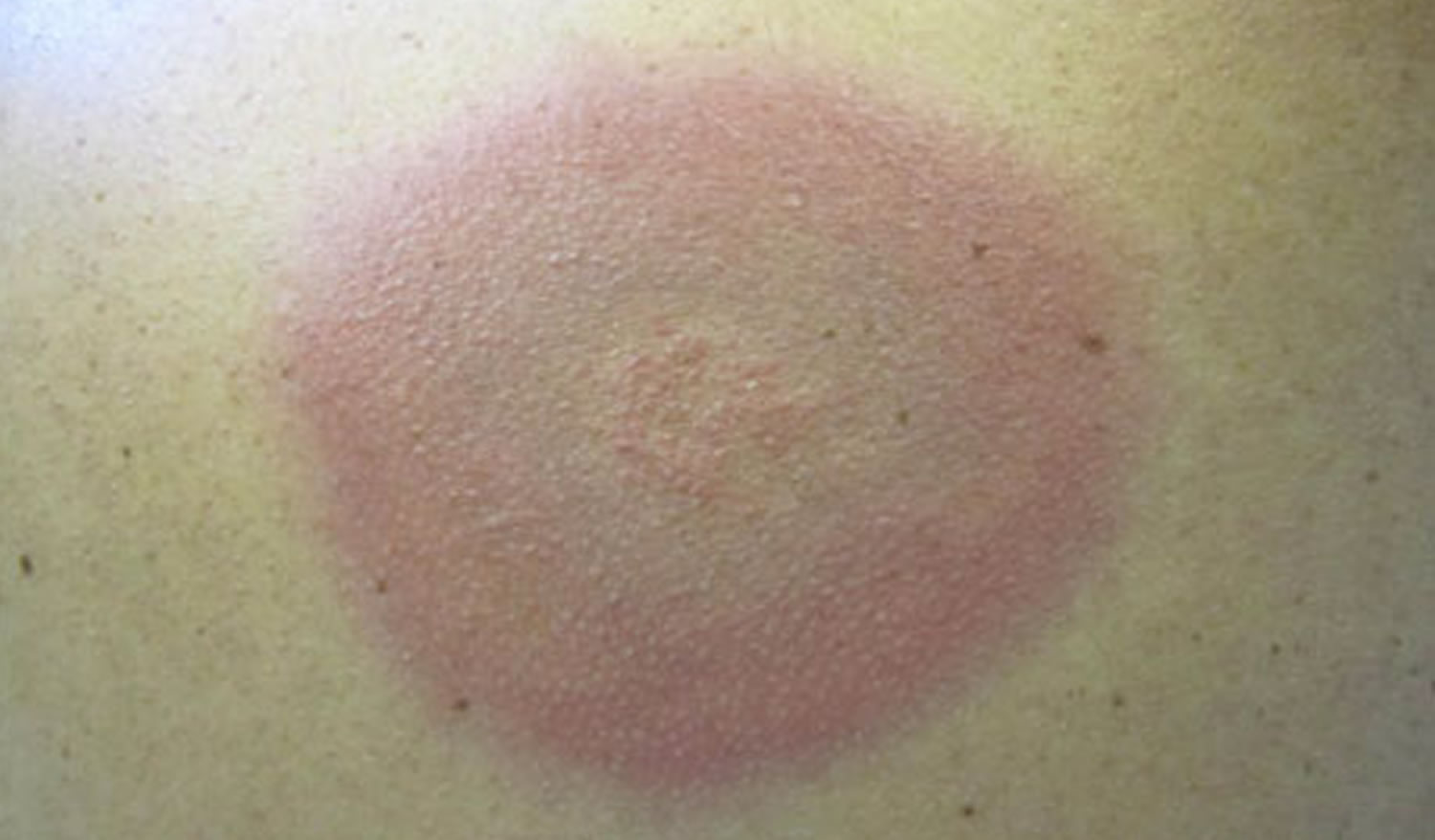
Figure 7. Lyme disease red-blue rash with central clearing
Anywhere from 7 to 14 days (or in some cases, 30 days) following an infected tick’s bite, the first stage of Lyme disease may begin with flu-like symptoms such as fever, chills, swollen lymph nodes, headaches, fatigue, muscle aches, and joint pain.
Neurological complications most often occur in the second stage of Lyme disease, with numbness, pain, weakness, Bell’s palsy (paralysis of the facial muscles), visual disturbances, and meningitis symptoms such as fever, stiff neck, and severe headache. Other problems, which may not appear until weeks, months, or years after a tick bite, include decreased concentration, irritability, memory and sleep disorders, and nerve damage in the arms and legs.
Most individuals with Lyme disease respond well to antibiotics and have full recovery. Early-stage Lyme disease responds very well to treatment. In most cases, taking an antibiotic for 2 to 4 weeks kills the bacteria and clears up the infection. Your doctor will tell you how long to take the antibiotic. It’s important to take all the medicine your doctor prescribes. This will prevent the spread of Lyme disease to your joints, nervous system, or heart. If you have problems with the medicine, do not quit taking it. See your doctor and talk to him or her about your side effects.
In a small percentage of individuals, symptoms may continue or recur, requiring additional antibiotic treatment. Varying degrees of permanent joint or nervous system damage may develop in individuals with late-stage Lyme disease.
Late-stage Lyme disease is also treated with antibiotics 7. It may be necessary to give the antibiotics intravenously (through an IV) at this stage. Medicine that reduces swelling and pain can ease arthritis associated with late-stage Lyme disease. If necessary, excess fluid can be drained from any affected joints.
Is Borrelia burgdorferi contagious
- There is no evidence that Lyme disease is transmitted from person-to-person. For example, a person cannot get infected from touching, kissing, or having sex with a person who has Lyme disease.
- Lyme disease acquired during pregnancy may lead to infection of the placenta and possible stillbirth; however, no negative effects on the fetus have been found when the mother receives appropriate antibiotic treatment. There are no reports of Lyme disease transmission from breast milk.
- Although no cases of Lyme disease have been linked to blood transfusion, scientists have found that the Lyme disease bacteria can live in blood that is stored for donation. Individuals being treated for Lyme disease with an antibiotic should not donate blood. Individuals who have completed antibiotic treatment for Lyme disease may be considered as potential blood donors.
- Although dogs and cats can get Lyme disease, there is no evidence that they spread the disease directly to their owners. However, pets can bring infected ticks into your home or yard. Consider protecting your pet, and possibly yourself, through the use of tick control products for animals.
- You will not get Lyme disease from eating venison or squirrel meat, but in keeping with general food safety principles, always cook meat thoroughly. Note that hunting and dressing deer or squirrels may bring you into close contact with infected ticks.
- There is no credible evidence that Lyme disease can be transmitted through air, food, water, or from the bites of mosquitoes, flies, fleas, or lice.
- Ticks not known to transmit Lyme disease include Lone star ticks (Amblyomma americanum), the American dog tick (Dermacentor variabilis), the Rocky Mountain wood tick (Dermacentor andersoni), and the brown dog tick (Rhipicephalus sanguineus).
Can Borrelia burgdorferi be transmitted sexually ?
There is no credible scientific evidence that Lyme disease is spread through sexual contact. Published studies in animals do not support sexual transmission 8, and the biology of the Lyme disease spirochete is not compatible this route of exposure 9. The ticks that transmit Lyme disease are very small and easily overlooked. Consequently, it is possible for sexual partners living in the same household to both become infected through tick bites, even if one or both partners doesn’t remember being bitten.
Can Borrelia burgdorferi be transmitted through breast milk ?
There are no reports of Lyme disease being spread to infants through breast milk. If you are diagnosed with Lyme disease and are also breastfeeding, make sure that your doctor knows this so that he or she can prescribe an antibiotic that’s safe for use when breastfeeding.
Can Borrelia burgdorferi be transmitted during a blood transfusion ?
Although no cases of Lyme disease have been linked to blood transfusion, scientists have found that the Lyme disease bacteria can live in blood from a person with an active infection that is stored for donation. Individuals being treated for Lyme disease with an antibiotic should not donate blood. Individuals who have completed antibiotic treatment for Lyme disease may be considered as potential blood donors. The Red Cross 10 provides additional information on the most recent criteria for blood donation.
Borrelia burgdorferi characteristics
Borrelia burgdorferi is member of the eubacterial phylum Spirochaetes 11. Members of this group of organisms share a distinctive morphology that includes a spiral or wavelike body and flagella (organs of motility) enclosed between the outer and inner membranes. Borrelia burgdorferi is a tick-borne obligate parasite whose normal reservoir is a variety of small mammals 12. Whereas infection of these natural hosts does not lead to disease, infection of humans can result in Lyme disease, as a consequence of the human immunopathological response to Borrelia burgdorferi 13.
Borrelia burgdorferi life cycle
Borrelia burgdorferi infects a wide range of vertebrate animals including small mammals, lizards, and birds 14. Ticks of the genus Ixodes transmit Borrelia burgdorferi between hosts and are the only natural agents through which humans have been shown to become infected 15. Worldwide geographic distribution of Lyme disease correlates to the overlapping ranges of both a competent reservoir host for Borrelia burgdorferi and the tick vector. In the northeastern and midwestern United States, the primary tick species for human disease is Ixodes scapularis (the black-legged tick) and in the western states Ixodes pacificus (the western black-legged tick) is the main agent of dissemination 16. European and Asian Lyme disease agents are primarily transmitted by Ixodes ricinus (the European sheep tick) and Ixodes persulcatus (the taiga tick), respectively 17.
Ticks most frequently acquire spirochetes from infected rodents during their larval feeding 18. After molting to the nymphal stage, infected ticks feed on a broad range of animals, including rodents, which become a new reservoir perpetuating the cycle 19. After the nymphs molt to the adult stage, they exclusively feed on larger mammals, which are often not competent hosts for Borrelia burgdorferi 19. The spirochetes are rarely, if ever, transmitted trans-ovarially 20, so the larval and nymphal feedings are crucial to maintaining the spirochete. Both nymphs and adults occasionally feed on humans, but the small size of the nymphs makes them difficult to detect and, hence, more likely to feed long enough to transmit the spirochete and cause Lyme disease.
The tick and mammalian hosts provide contrasting environments for bacterial growth. Notably, mammals regulate their body temperatures at about 37–39°C, whereas ticks vary with the ambient temperature, except when feeding on a mammal. Also, the pH of mammalian tissue and blood is neutral, whereas the tick midgut is a more basic environment 21. In order to cycle between two very different hosts, Borrelia burgdorferi varies its gene expression, leading to different protein components and enabling physiological adaptation to these environments 22. A number of studies have begun to delineate those changes.
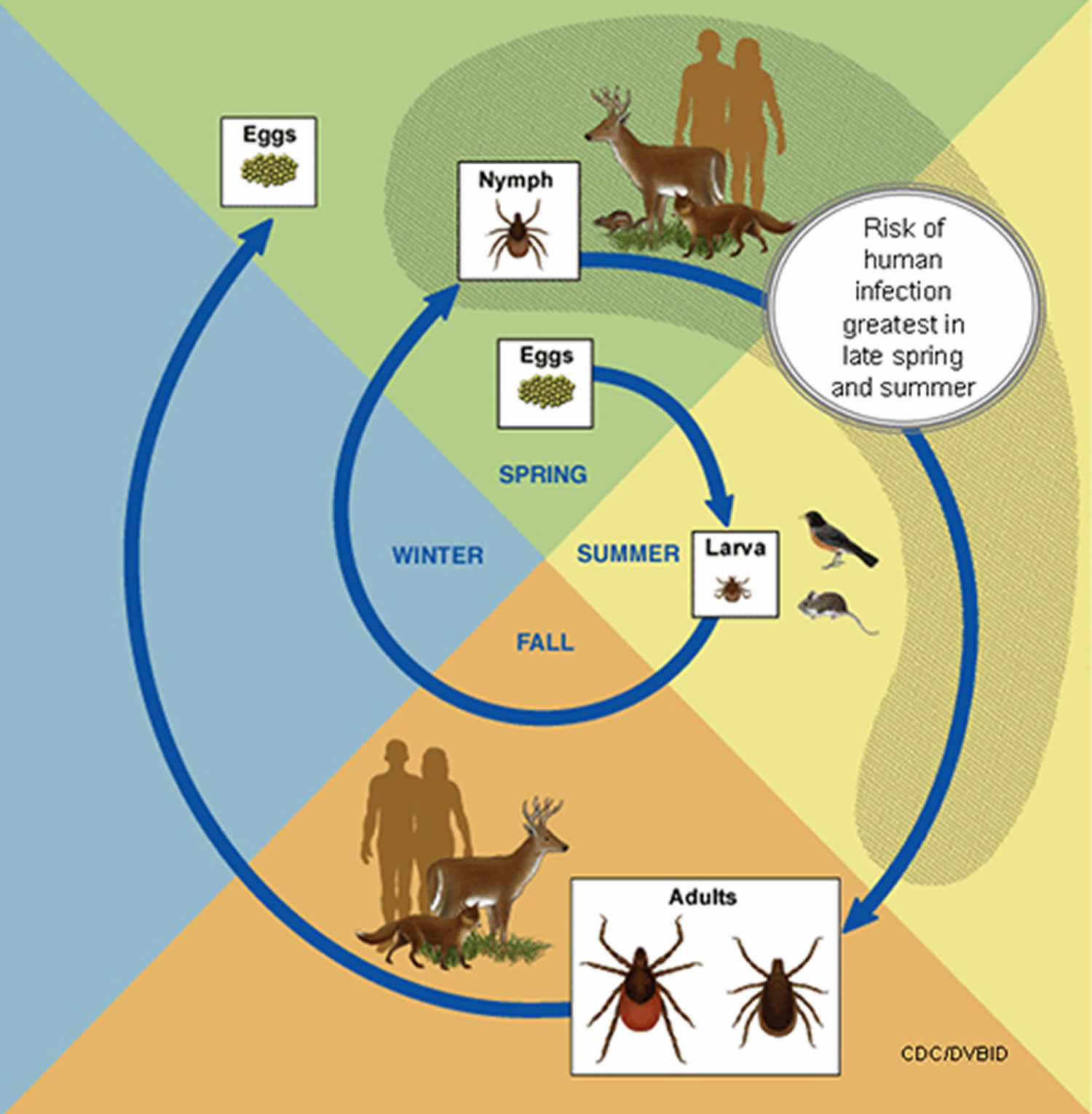
The lifecycle of blacklegged ticks (Ixodes scapularis and Ixodes pacificus) generally lasts two years. During this time, they go through four life stages: egg, six-legged larva, eight-legged nymph, and adult. After the eggs hatch, the ticks must have a blood meal at every stage to survive.
Blacklegged ticks can feed from mammals, birds, reptiles, and amphibians. The ticks need to have a new host at each stage of their life, as shown below.
Tick infection occurs when larval ticks feed on small rodents infected by Borrelia burgdorferi. When ticks reach the nymphal stage, they feed on, infect a wide range of mammals, and perpetuate the infectious cycle. In the nymphal stage, infection is more likely to spread to humans due to: the small size of the nymphal tick, the ticks increased numbers, and increased seasonal human activity in woodland areas (late spring and summer). Borrelia burgdorferi infects the skin after a tick attaches for at least 24 hours. From the skin, the spirochete spreads hematogenously or lymphatically to other organs. The human host mounts an adaptive and innate immune response resulting in macrophage, and antibody-mediated control and eradication of Borrelia burgdorferi. Several weeks or months may pass before the host immune system gains control of the infection, which will occur despite the presence of antibiotics. If not treated, the spirochete can survive in localized recesses of the body for several years causing arthritis or neurologic sequelae 23.
Figure 8. Borrelia burgdorferi life cycle
Borrelia burgdorferi prevention
The best way to prevent Borrelia burgdorferi (Lyme disease) is to avoid being bitten by ticks. When you are outdoors, follow these guidelines:
- Avoid areas that are wooded, brushy, or have tall grass.
- Walk in the center of trails.
- Use an insect repellent with at least 20% DEET. It can be put on clothing or sparingly on the skin. Don’t apply it to the face or hands of children.
- Treat clothing, tents, or other gear with repellents containing 0.5% permethrin.
- Wear light-colored clothing. This makes it easier to see and remove ticks from your clothes.
- Wear a long-sleeved shirt and long pants. Tuck your pant legs into your socks or boots for added protection.
After you get home, check everything and everyone for ticks.
- Bathe or shower as soon as you can to wash off any ticks that have not attached to you.
- Check your entire body for ticks. Use a mirror for places you can’t see. Check your children and your pets. Common tick locations include the back of the knees, groin area, underarms, ears, scalp, and the back of the neck.
- Check any gear you used, including coats, backpacks, or tents.
- Tumble dry clothes or blankets on high heat in the dryer for 10 to 15 minutes. This should kill any ticks. If clothes are dirty, wash them in hot water and dry on high heat for 60 minutes.
How to remove a tick
If you find a tick attached to your skin, there’s no need to panic—the key is to remove the tick as soon as possible. There are several tick removal devices on the market, but a plain set of fine-tipped tweezers work very well.
To remove a tick, follow these steps:
- Using a pair of fine-tipped or pointy tweezers, grasp the tick by the head or mouth-parts right where they enter the skin. DO NOT grasp the tick by the body.
- Without jerking, pull firmly and steadily directly outward. DO NOT twist the tick out or apply petroleum jelly, a hot match, alcohol, nail polish or any other irritant to the tick in an attempt to get it to back out. Your goal is to remove the tick as quickly as possible–not waiting for it to detach. If the mouth-parts to break off and remain in the skin, remove the mouth-parts with tweezers. If you are unable to remove the mouth easily with clean tweezers, leave it alone and let the skin heal.
- Never crush a tick with your fingers. Dispose of a live tick by putting it in alcohol, placing it in a sealed bag/container, wrapping it tightly in tape, or flushing it down the toilet.
- Clean the bite wound with with rubbing alcohol or soap and water. Keep in mind that certain types of fine-pointed tweezers, especially those that are etched, or rasped, at the tips, may not be effective in removing nymphal deer ticks. Choose unrasped fine-pointed tweezers whose tips align tightly when pressed firmly together.
Then, monitor the site of the bite for the appearance of a rash beginning 3 to 30 days after the bite. At the same time, learn about the other early symptoms of Lyme disease and watch to see if they appear in about the same timeframe. If a rash or other early symptoms develop, see a physician immediately. Be sure to tell the doctor about your recent tick bite, when the bite occurred, and where you most likely acquired the tick.
Figure 9. How to remove a tick

Borrelia burgdorferi symptoms
Untreated Borrelia burgdorferi infection (Lyme disease) can produce a wide range of symptoms, depending on the stage of infection. These include fever, rash, facial paralysis, and arthritis. Seek medical attention if you observe any of these symptoms and have had a tick bite, live in an area known for Lyme disease, or have recently traveled to an area where Lyme disease occurs.
Lyme disease may present in one of 3 stages:
Early Localized Disease
This stage presents days to weeks after a tick bite that many do not remember due to the small size of the nymphal tick. Erythema migrans initially appears as a small red papule or macule that enlarges to form an annular lesion. The lesion may or may not exhibit central clearing. This presentation is due to the outward spread of the spirochete through the skin tissues. Common locations for this rash include thigh, groin, and axilla.
Early Disseminated Disease
After hematogenous or lymphatic dissemination of the disease, patients may exhibit secondary annular lesions accompanied by headaches, neck stiffness, fever, chills, arthralgias, muscle aches, and profound malaise. After several weeks to months, neurologic abnormalities present as meningitis, subtle encephalitis, cranial neuritis, neuropathy, ataxia, or myelitis. Rarely, cardiac complications occur and present as atrioventricular blocks of varying degrees, myopericarditis, or cardiomegaly.
Late Disease
This stage occurs months after infection by Borrelia burgdorferi. At this point, sporadic episodes of arthritis affecting large joints (i.e. knees) can present and last weeks to months in a single joint. Chronic neurologic sequelae may occur as another manifestation of late-stage disease. A subtle encephalopathy affecting memory, mood, or sleep settles in months to years after the onset of infection 24.
Early Signs and Symptoms (3 to 30 days after tick bite)
- Fever, chills, headache, fatigue, muscle and joint aches, and swollen lymph nodes
Erythema migrans rash:
- Occurs in approximately 70 to 80 percent of infected persons
- Begins at the site of a tick bite after a delay of 3 to 30 days (average is about 7 days)
- Expands gradually over a period of days reaching up to 12 inches or more (30 cm) across
- May feel warm to the touch but is rarely itchy or painful
- Sometimes clears as it enlarges, resulting in a target or “bull’s-eye” appearance
- May appear on any area of the body.
Later Signs and Symptoms (days to months after tick bite)
- Severe headaches and neck stiffness
- Additional erythema migrans rashes on other areas of the body
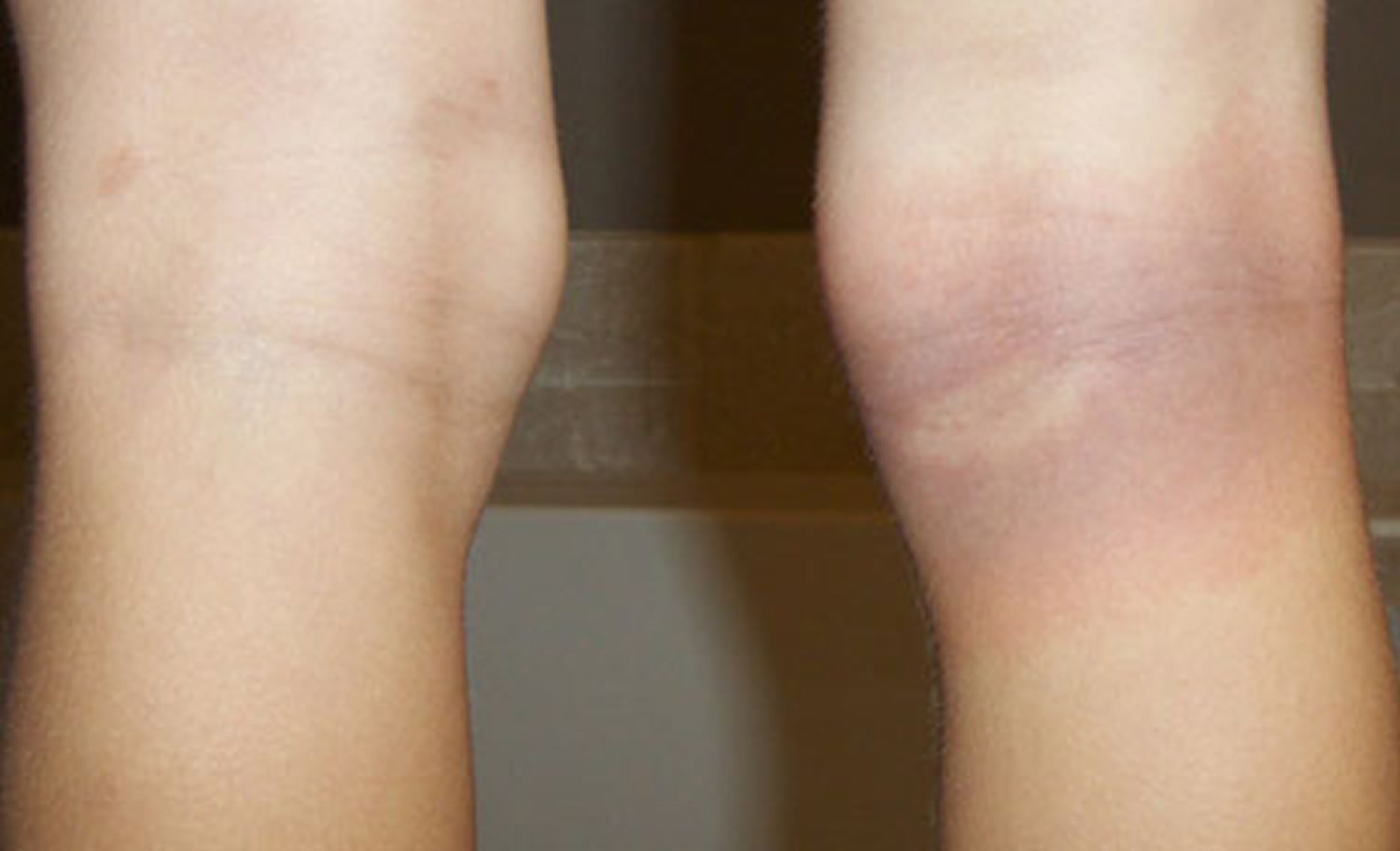
- Arthritis with severe joint pain and swelling, particularly the knees and other large joints.
- Facial palsy (loss of muscle tone or droop on one or both sides of the face) – Bell’s palsy
- Intermittent pain in tendons, muscles, joints, and bones
- Heart palpitations or an irregular heart beat (Lyme carditis)
- Episodes of dizziness or shortness of breath
- Inflammation of the brain and spinal cord
- Nerve pain
- Shooting pains, numbness, or tingling in the hands or feet
- Problems with short-term memory.
Lyme disease can progress to a late stage months to years after the initial tick bite, which may result in substantial morbidity, primarily from chronic arthritis 25. These complications are distinct from what have recently been named “post–Lyme disease syndrome,” which refers to the nonspecific symptoms (e.g., fatigue) that may persist after successful treatment, and “chronic Lyme disease,” which refers more broadly to chronic symptoms occurring in patients who may or may not have Lyme disease 26.
What is Lyme carditis ?
Lyme carditis occurs when Lyme disease bacteria enter the tissues of the heart 27. This can interfere with the normal movement of electrical signals from the heart’s upper to lower chambers, a process that coordinates the beating of the heart. The result is something physicians call “heart block,” which can be mild, moderate, or severe. Heart block from Lyme carditis can progress rapidly.
Cardiac involvement usually occurs within one to two months after infection (range of less than one week to seven months) 28. Lyme carditis is a less common complication of systemic disease, occurring in approximately 4 to 10 percent of patients 29. It may present as chest pain, light-headedness, fainting, shortness of breath on exertion, heart palpitations, fatigue, heart palpitations or syncope, and often includes some form of atrioventricular block. A study of 105 patients with Lyme carditis reported that 49 percent had third-degree atrioventricular block, 28 percent had some form of second- or first-degree atrioventricular block, and 23 percent had no conduction abnormalities 30. Other less common manifestations include myopericarditis, bundle branch block, and heart failure 28.
Patients with Lyme carditis usually have other symptoms such as fever and body aches, and they may have more specific symptoms of Lyme disease, such as the erythema migrans rash.
How is Lyme carditis treated ?
Lyme carditis can be treated with oral or intravenous (IV) antibiotics, depending on how severe it is. Some patients might need a temporary pacemaker.
Can Lyme carditis be fatal ?
Yes. Between 1985 and 2008, medical journals reported four deaths, worldwide, as a result of Lyme carditis 27.
What is a Heart Block ?
Heart block is a problem in the electrical signals in the heart 31.
Normally, the heart beat starts in an area in the top chambers of the heart (atria). This area is the heart’s pacemaker. The electrical signals travel to the lower chambers of the heart (ventricles). This keeps the heart beat steady and regular.
Heart block occurs when the electrical signal is slowed down or does not reach the bottom chambers of the heart. Your heart may beat slowly, or it may skip beats. Heart block may resolve on its own, or it may be permanent and require treatment.
The symptoms and severity of heart block depend on which type you have. First-degree heart block may not cause any severe symptoms.
Second-degree heart block may result in the heart skipping a beat or beats. This type of heart block also can make you feel dizzy or faint.
Third-degree heart block limits the heart’s ability to pump blood to the rest of the body. This type of heart block may cause fatigue (tiredness), dizziness, and fainting. Third-degree heart block requires prompt treatment because it can be fatal.
A medical device called a pacemaker is used to treat third-degree heart block and some cases of second-degree heart block. This device uses electrical pulses to prompt the heart to beat at a normal rate. Pacemakers typically are not used to treat first-degree heart block.
All types of heart block may increase your risk for other arrhythmias, such as atrial fibrillation. Talk with your doctor to learn more about the signs and symptoms of a heart block.
How long does it take for a person to recover from Lyme carditis ?
Typically the patient receives antibiotic treatment for 14-21 days. Most symptoms are gone within 1-6 weeks.
Post-Lyme disease syndrome and chronic Lyme disease
Post-Lyme disease syndrome and chronic Lyme disease are areas of uncertainty due to fluctuating definitions and lack of research on incidence, prevalence, and pathogenesis 32. Post-Lyme disease syndrome is tentatively defined by the Infectious Disease Society of America (IDSA) as “a term to describe patients who have had well-documented Lyme disease and who remain symptomatic for many months to years after completion of appropriate antibiotic therapy.” IDSA’s recommendations have inclusion criteria to elucidate this syndrome further. These criteria include the onset of any of the following symptoms within 6 months of definitively diagnosed Lyme disease and persistence of symptoms for 6 months after completion of appropriate antibiotic therapy:
- Fatigue
- Widespread musculoskeletal pain
- Complaints of cognitive difficulties
Chronic Lyme disease is a term inclusive of post-Lyme disease syndrome and other clinical symptoms for which there is no convincing biologic evidence in relationship to B. burgdorferi infection. These patients may have persistent pain, neurocognitive symptoms, and/or fatigue with or without evidence (clinical or serologic) of previous Lyme disease. Experts do not recommend any prolonged or repeated antibiotic courses for chronic Lyme disease or post-Lyme disease syndrome as evidence is lacking that doing so has any therapeutic advantages 24.
Borrelia burgdorferi diagnosis
Lyme disease is diagnosed based on:
- Signs and symptoms
- A history of possible exposure to infected blacklegged ticks
Laboratory blood tests are helpful if used correctly and performed with validated methods. Laboratory tests are not recommended for patients who do not have symptoms typical of Lyme disease. Just as it is important to correctly diagnose Lyme disease when a patient has it, it is important to avoid misdiagnosis and treatment of Lyme disease when the true cause of the illness is something else.
Two-step Laboratory Testing Process for Borrelia burgdorferi
The Centers for Disease Control and Prevention (CDC) currently recommends a two-step process when testing blood for evidence of antibodies against the Borrelia burgdorferi. Both steps can be done using the same blood sample.
The first step uses a testing procedure called “EIA” (enzyme immunoassay) or rarely, an “IFA” (indirect immunofluorescence assay). If this first step is negative, no further testing of the specimen is recommended. If the first step is positive or indeterminate (sometimes called “equivocal”), the second step should be performed. The second step uses a test called an immunoblot test, commonly, a “Western blot” test. Results are considered positive only if the EIA/IFA and the immunoblot are both positive.
The two steps of Lyme disease testing are designed to be done together. The Centers for Disease Control and Prevention does not recommend skipping the first test and just doing the Western blot. Doing so will increase the frequency of false positive results and may lead to misdiagnosis and improper treatment.
New tests may be developed as alternatives to one or both steps of the two-step process. Before CDC will recommend new tests, their performance must be demonstrated to be equal to or better than the results of the existing procedure, and they must be FDA approved.
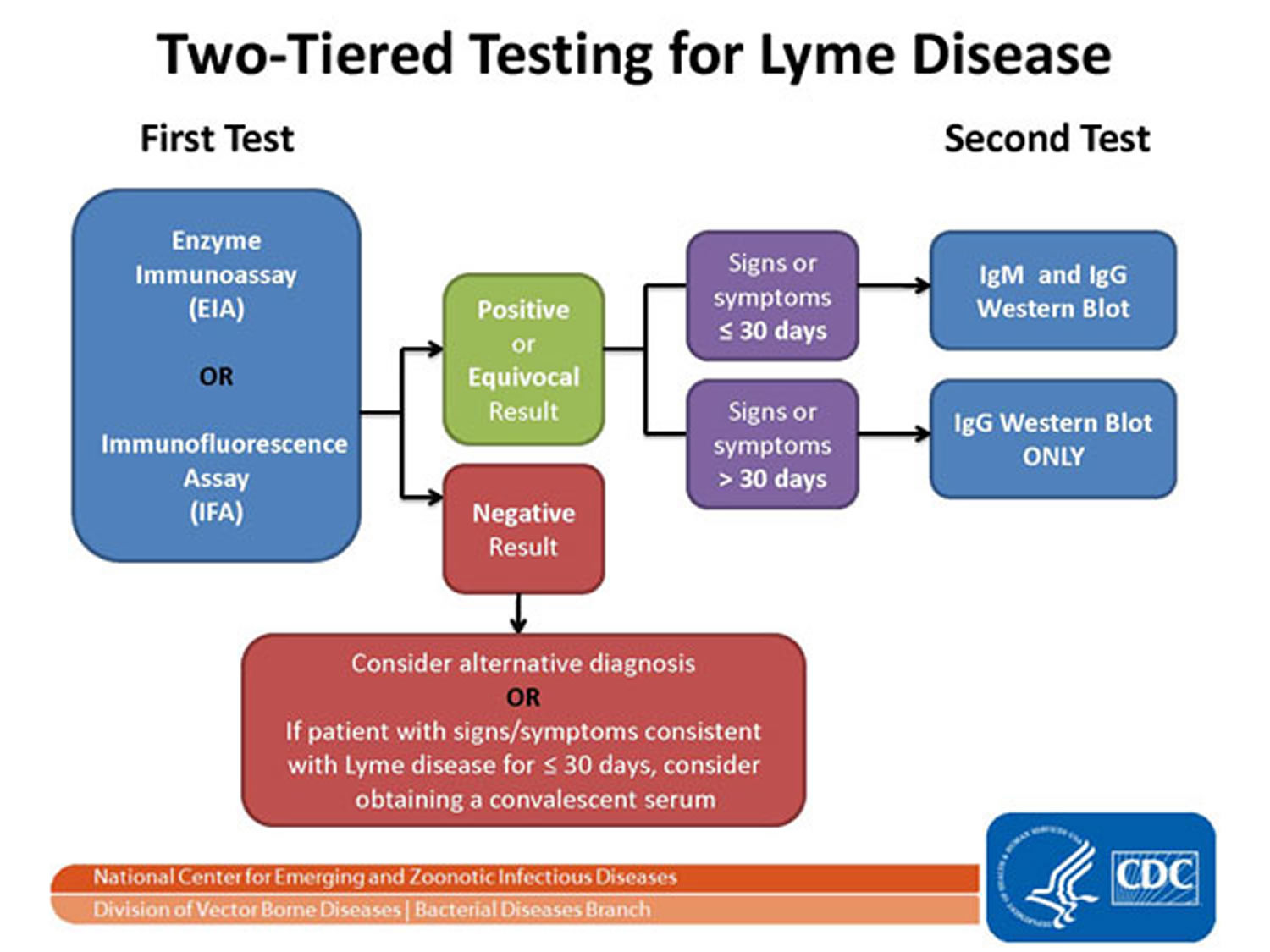
Figure 10. Two-Tiered Testing for Lyme Disease
Notes: The Two-tier Testing Decision Tree describes the steps required to properly test for Lyme disease. The first required test is the Enzyme Immunoassay (EIA) or Immunofluorescence Assay (IFA). If this test yields negative results, the provider should consider an alternative diagnosis. Or in cases where the patient has had symptoms for less than or equal to 30 days, the provider may treat the patient and follow up with a convalescent serum. If the first test yields positive or equivocal results, two options are available: 1) if the patient has had symptoms for less than or equal to 30 days, an IgM Western Blot is performed; 2) if the patient has had symptoms for more than 30 days, the IgG Western Blot is performed. The IgM should not be used if the patient has been ill for more than 30 days.
[Source 33]Understanding the EIA Test
Several types of EIA tests exist. Validated and FDA-approved EIAs include “ELISA” (enzyme-linked immunosorbent assay) and “ELFA” (enzyme-linked fluorescent immunoassay). Lyme disease testing measures a person’s antibody (or immune response) to the bacteria that cause Lyme disease. EIA tests are designed to be very “sensitive”, meaning that when they are used properly, almost everyone with Lyme disease will test positive. It is also possible, however, to test positive with an EIA test even when you do not have Lyme disease. This can occur because of other medical conditions, including:
- Tick-borne relapsing fever
- Syphilis
- Anaplasmosis (formerly known as granulocytic ehrlichiosis)
- Leptospirosis
- Some autoimmune disorders (e.g., lupus)
- Bacterial endocarditis
- Infection with Helicobacter pylori, Epstein Barr virus, or Treponema denticola (bacteria found in the mouth that can cause gum disease and/or infection after dental procedures)
For this reason, doctors want to verify any “positive” or “equivocal” (indeterminate) EIA results by performing an immunoblot test such as a Western blot. The Western blot or other FDA-approved type of immunoblot can help distinguish patients who have Lyme disease from those with other conditions.
Understanding the Immunoblot Test
The immunoblot is a laboratory test that looks for antibodies the body makes against different molecules, or “antigens,” that are part of the Borrelia burgdorferi bacteria. Western Blots were the first type of immunoblot developed for Lyme disease testing. Later, a striped type of immunoblot was approved by the FDA that does not require human interpretation of bands.
Practically speaking, the test produces something that looks like a bar code used on grocery items, with several lines or “bands”. Each line represents antibodies to a different component of the bacteria. As with bar codes, the presence of any one or two lines is not particularly meaningful. Instead, it is the combination of multiple, specific lines that identifies the infection as being due to Borrelia burgdorferi.
Immunoblot tests for Lyme disease testing can detect two different classes of antibodies: IgM and IgG. IgM antibodies are made sooner, so testing for them can be helpful for identifying patients during the first few weeks of infection. The downside of testing for IgM antibodies is that they are more likely to give false positive results. Tests for IgG antibodies are more reliable, but can take 4-6 weeks for the body to produce in large enough quantities for the test to detect them.
If this sounds complex, that’s because it is. Just remember the following:
- The immunoblot should not be run without first performing an EIA or IFA.
- The immunoblot should not be run if the EIA or IFA tests are negative.
- A positive IgM immunoblot is only meaningful during the first 4 weeks of illness
- If you’ve been ill for longer than 4-6 weeks and the IgG immunoblot test is negative, it is unlikely that you have Lyme disease, even if the IgM immunoblot is positive.
Note on test result interpretation: It is not correct to interpret a test result that has only some bands that are positive as being “mildly” or “somewhat” positive for Lyme disease. The criterion that requires at least 5 IgG bands reflects the fact that people with Lyme disease have at least 5 antigens (specific molecules) detectable.
Borrelia burgdorferi treatment
The treatment of Lyme disease is determined mainly by the clinical manifestations of the disease. In general, oral regimens are recommended for early localized disease. Intravenous regimens are reserved for patients with neurologic symptoms (e.g., meningitis), symptomatic cardiac disease, or, in a few cases, refractory Lyme arthritis. Many experts recommend doxycycline as the preferred agent for oral treatment because of its activity against other tick-borne illnesses (e.g., human granulocytic anaplasmosis), which can occur in up to 10 percent of patients with Lyme disease 26.
Patients treated with appropriate antibiotics in the early stages of Lyme disease usually recover rapidly and completely. Antibiotics commonly used for oral treatment include doxycycline, amoxicillin, or cefuroxime axetil. Patients with certain neurological or cardiac forms of illness may require intravenous treatment with drugs such as ceftriaxone or penicillin.
Table 1. Treatment options for Lyme disease
| Clinical symptoms | Treatment | ||||||
|---|---|---|---|---|---|---|---|
| Adults | Children | Duration | Comments | ||||
Early localized | |||||||
| Doxycycline, 100 mg orally twice per day | Doxycycline, 4 mg per kg orally per day in two divided doses (maximum of 100 mg twice per day) in children eight years or older | 14 days (range of seven to 10 days for azithromycin; 10 to 21 days for doxycycline; and14 to 21 days for amoxicillin or cefuroxime axetil) |
| |||
or | or | ||||||
Amoxicillin, 500 mg orally three times per day | Amoxicillin, 50 mg per kg orally per day in three divided doses (maximum of 500 mg per dose) | ||||||
or | or | ||||||
Cefuroxime axetil (Ceftin), 500 mg orally twice per day | Cefuroxime axetil, 30 mg per kg orally per day in two divided doses (maximum of 500 mg per dose) | ||||||
or | or | ||||||
Azithromycin (Zithromax), 500 mg orally once per day | Azithromycin, 10 mg per kg orally per day (maximum of 500 mg per day) | ||||||
Early disseminated | |||||||
| Ceftriaxone (Rocephin), 2 g intravenously per day | Ceftriaxone, 50 to 75 mg per kg intravenously per day (maximum of 2 g per dose) | 14 days (range of 14 to 21 days for ceftriaxone or cefotaxime and 10 to 28 days for oral doxycycline) |
| |||
or | or | ||||||
Cefotaxime (Claforan), 2 g intravenously every eight hours | Cefotaxime, 150 to 200 mg per kg intravenously per day in three or four divided doses (maximum of 6 g per day) | ||||||
or | or | ||||||
Doxycycline, 200 to 400 mg orally in two divided doses per day | Doxycycline, 4 to 8 mg per kg intravenously in two divided doses per day in children eight years or older (maximum of 100 to200 mg per dose) | ||||||
Late | |||||||
| Same oral antibiotics as used for erythema migrans | Same oral antibiotics as used for erythema migrans | 28 days |
| |||
| Same intravenous antibiotics as used for neurologic symptoms of early disseminated disease | Same intravenous antibiotics as used for neurologic symptoms of early disseminated disease | 14 to 28 days | ||||
Note: Treatments are listed in order of most to least preferred.
Borrelia burgdorferi prognosis
The long-term prognosis for patients who are treated with antibiotics is excellent, regardless of symptoms or stage. No response to antibiotic therapy can best be explained by the probability that the patient was misdiagnosed with Lyme disease. Once treatment is started, the flu-like symptoms may persist for a few more weeks. Symptom persistence does not mean that treatment has to be repeated 34.
- Shapiro ED. Borrelia burgdorferi (Lyme disease). Pediatr Rev. 2014 Dec;35(12):500-9.[↩]
- Bernard Q, Thakur M, Smith AA, Kitsou C, Yang X, Pal U. Borrelia burgdorferi protein interactions critical for microbial persistence in mammals. Cell. Microbiol. 2019 Feb;21(2):e12885.[↩]
- Lyme Disease Frequently Asked Questions (FAQ). Centers for Disease Control and Prevention. https://www.cdc.gov/lyme/faq/[↩][↩]
- Lyme Disease. Centers for Disease Control and Prevention. https://www.cdc.gov/lyme/transmission/index.html[↩][↩]
- How many people get Lyme disease ? Centers for Disease Control and Prevention. https://www.cdc.gov/lyme/stats/index.html[↩]
- Lyme disease. National Institute of Allergy and Infectious Diseases. https://www.ninds.nih.gov/Disorders/All-Disorders/Neurological-Complications-Lyme-Disease-Information-Page[↩][↩]
- Lyme Disease. American Academy of Family Physicians. https://familydoctor.org/condition/lyme-disease/[↩]
- Woodrum JE, Oliver JH, Jr., 1999. Investigation of venereal, transplacental, and contact transmission of the Lyme disease spirochete, Borrelia burgdorferi, in Syrian hamsters. J Parasitol 85: 426-30. https://www.ncbi.nlm.nih.gov/pubmed/10386432[↩]
- Porcella SF, Schwan TG, 2001. Borrelia burgdorferi and Treponema pallidum: a comparison of functional genomics, environmental adaptations, and pathogenic mechanisms. J Clin Invest 107: 651-6. https://www.ncbi.nlm.nih.gov/pmc/articles/PMC208952/[↩]
- Eligibility Requirements. American National Red Cross. http://www.redcrossblood.org/donating-blood/eligibility-requirements[↩]
- Tilly K, Rosa PA, Stewart PE. Biology of infection with Borrelia burgdorferi. Infect Dis Clin North Am. 2008;22(2):217–v. doi:10.1016/j.idc.2007.12.013 https://www.ncbi.nlm.nih.gov/pmc/articles/PMC2440571[↩]
- Lyme disease-a tick-borne spirochetosis? Burgdorfer W, Barbour AG, Hayes SF, Benach JL, Grunwaldt E, Davis JP. Science. 1982 Jun 18; 216(4552):1317-9.[↩]
- Host-pathogen interactions promoting inflammatory Lyme arthritis: use of mouse models for dissection of disease processes. Wooten RM, Weis JJ. Curr Opin Microbiol. 2001 Jun; 4(3):274-9.[↩]
- Clark K, Hendricks A, Burge D. Molecular identification and analysis of Borrelia burgdorferi sensu lato in lizards in the southeastern United States. Appl Environ Microbiol. 2005;71(5):2616–2625.[↩]
- Steere AC. Lyme Disease. N Engl J Med. 2001;345(2):115–125.[↩]
- Burgdorfer W, Lane RS, Barbour AG, et al. The western black-legged tick, Ixodes pacificus, a vector of Borrelia burgdorferi. Am J Trop Med Hyg. 1985;34:925–930[↩]
- Gern L, Humair P-F. Ecology of Borrelia burgdorferi sensu lato in Europe. In: Gray JS, Kahl O, Lane RS, et al., editors. Lyme Borreliosis: Biology, Epidemiology and Control. Wallingford: CABI Publishing; 2002. pp. 149–174[↩]
- Donahue JG, Piesman J, Spielman A. Reservoir competence of white-footed mice for Lyme disease spirochetes. Am J Trop Med Hyg. 1987;36:92–96.[↩]
- Lane RS, Piesman J, Burgdorfer W. Lyme borreliosis: relation of its causative agent to its vectors and hosts in North America and Europe. Annu Rev Entomol. 1991;36:587–609[↩][↩]
- Patrican LA. Absence of Lyme disease spirochetes in larval progeny of naturally infected Ixodes scapularis (Acari:Ixodidae) fed on dogs. J Med Entomol. 1997;34(1):52–55.[↩]
- Ribeiro JMC. The midgut hemolysin of Ixodes dammini (Acari: Ixodidae) J Parasitol. 1988;74:532–537.[↩]
- Yang X, Goldberg MS, Popova TG, et al. Interdependence of environmental factors influencing reciprocal patterns of gene expression in virulent Borrelia burgdorferi. Mol Microbiol. 2000;37(6):1470–1479[↩]
- Tilly K, Rosa PA, Stewart PE. Biology of infection with Borrelia burgdorferi. Infect. Dis. Clin. North Am. 2008 Jun;22(2):217-34, v[↩]
- Wormser GP, Dattwyler RJ, Shapiro ED, Halperin JJ, Steere AC, Klempner MS, Krause PJ, Bakken JS, Strle F, Stanek G, Bockenstedt L, Fish D, Dumler JS, Nadelman RB. The clinical assessment, treatment, and prevention of lyme disease, human granulocytic anaplasmosis, and babesiosis: clinical practice guidelines by the Infectious Diseases Society of America. Clin. Infect. Dis. 2006 Nov 01;43(9):1089-134[↩][↩]
- Marques A. Chronic Lyme disease: a review. Infect Dis Clin North Am. 2008;22(2):341–360, viiviii.[↩]
- Wormser GP, Dattwyler RJ, Shapiro ED, et al. The clinical assessment, treatment, and prevention of lyme disease, human granulocytic anaplasmosis, and babesiosis: clinical practice guidelines by the Infectious Diseases Society of America [published correction appears in Clin Infect Dis. 2007;45(7):941]. Clin Infect Dis. 2006;43(9):1089–1134.[↩][↩][↩]
- What you need to know about Lyme carditis. Centers for Disease Control and Prevention. https://www.cdc.gov/lyme/signs_symptoms/lymecarditis.html[↩][↩]
- Steere AC. Lyme disease. N Engl J Med. 2001;345(2):115–125.[↩][↩]
- Sigal LH. Early disseminated Lyme disease: cardiac manifestations. Am J Med. 1995;98(4A):25S–28S, discussion 28S–29S.[↩]
- van der Linde MR. Lyme carditis: clinical characteristics of 105 cases. Scand J Infect Dis Suppl. 1991;77:81–84.[↩]
- Heart Block. National Heart, Lung and Blood Institute. https://www.nhlbi.nih.gov/health/health-topics/topics/hb/[↩]
- Tatum R, Pearson-Shaver AL. Borrelia Burgdorferi. [Updated 2018 Dec 2]. In: StatPearls [Internet]. Treasure Island (FL): StatPearls Publishing; 2019 Jan-. Available from: https://www.ncbi.nlm.nih.gov/books/NBK532894[↩]
- Two-step Laboratory Testing Process. Centers for Disease Control and Prevention. https://www.cdc.gov/lyme/diagnosistesting/labtest/twostep/index.html[↩]
- Stanek G, Gray J, Strle F, Wormser G. Lyme borreliosis. Lancet Infect Dis. 2004 Apr;4(4):197-8; discussion 198-9.[↩]