Contents
What is curry powder
Curry powder is a spice mix of (most curry powder recipes include) curry leaves, coriander, turmeric, cumin, fenugreek, and chili peppers in their blends. Depending on the recipe, additional ingredients such as ginger, garlic, asafoetida, fennel seed, caraway, cinnamon, clove, mustard seed, green cardamom, black cardamom, nutmeg, white turmeric, curry leaf, long pepper, and black pepper may also be included 1. There is little agreement about what actually constitutes a curry. Curry powders and curry pastes produced and consumed in India are extremely diverse; some red, some yellow, some brown; some with five spices and some with as many as 20 or more. Besides the previously mentioned spices, other commonly found spices in different curry powders in India are allspice, white pepper, ground mustard, ground ginger, cinnamon, roasted cumin, cloves, nutmeg, mace, green cardamom seeds or black cardamom pods, bay leaves and coriander seeds.
The term curry likely derives from kari, the word for “sauce” in Tamil, a South-Indian language. Perplexed by that region’s wide variety of savory dishes, 17th-century British traders lumped them all under the term curry. But the original curry predates Europeans’ presence in India by about 4,000 years. Villagers living at the height of the Indus civilization used three key curry ingredients—ginger, garlic, and turmeric—in their cooking. This proto-curry, in fact, was eaten long before Arab, Chinese, Indian, and European traders plied the oceans in the past thousand years.
Curry leaves (Murraya koenigii) [see Figure 2], popularly known in India as kariveppilai, karivepaaku or kari patta. Curry leaves were originally cultivated in India for its aromatic leaves and for ornament is normally used for natural flavoring in curries and sauces. Originated in Tarai regions of Uttar Pradesh, India. It is now widely found in all parts of India and it adorns every house yard of southern India and also it is now cultivated and distributes throughout the world. The curry leaves plant is used in Indian system of medicine to treat various ailments 2. Parts of the plant have been used as raw material for the traditional medicine formulation in India. This plant is known to be the richest source of carbazole alkaloids. It has been reported by authors that carbazole alkaloids present in curry leaves and display various biological activities such as anti-tumor, anti-oxidative, anti-mutagenic and anti-inflammatory activities 3. Curry leaves and roots can be used to cure piles and allay heat of the body, thirst, inflammation and itching 4.
The aromatic curry leaves, which retains their flavor and other qualities even after drying, are slightly bitter, acrid, cooling, weakly acidic in tastes and are considered as a tonic, anthelmintic, analgesic, digestive, appetizing and are widely used in Indian cookery for flavoring food stuffs 5. The phytoconstituents isolated so far from the leaves are alkaloids viz., mahanine, koenine, koenigine, koenidine, girinimbiol, girinimibine, koenimbine, O-methyl murrayamine A, O-methyl mahanine, isomahanine, bismahanine, bispyrayafoline and other phytoconstituents such as coumarin glycoside viz., scopotin, murrayanine, calcium, phosphorus, iron, thiamine, riboflavin, niacin, vitamin C, carotene and oxalic acid 6. It also reported for anti-microbial, antioxidant 7. Essential oil composition of curry leaves has been studied by various workers 8. The essential oil from curry leaves yielded di-α-phellandrene, D-sabinene, D-α-pinene, dipentene, D-α-terpinol and caryophyllene 9. This essential oil from M. koenigii leaves is reported to possess antioxiant, antibacterial, antifungal, larvicidal, anticarcinogenic, hypoglycemic, anti-lipid peroxidative, hypolipidemic and antihypertensive activity 10.
Curry leaves have been reported to be effective in many diseased conditions 11, 12. Curry leaves may be medicinally useful for the treatment or prevention of diabetes, cancer and cardiovascular disease. Ingestion of curry leaves improved the plasma lipid profile in the rat feeding model 13. Curry leaves have also been promoted to treat both hypocholesterolemic effects and improved glycaemic status in obese mouse model 14. There are reports suggesting that the curry leaves possess anti-oxidative and anti-lipid per-oxidative actions 15. Thus, the leaves of the curry plant have the potential to provide protection against oxidative stress.
Figure 1. Curry powder
Figure 2. Curry leaves
Table 1. Curry powder nutrition facts
| Nutrient | Unit | Value per 100 g | |||||||||
| Approximates | |||||||||||
| Water | g | 8.8 | |||||||||
| Energy | kcal | 325 | |||||||||
| Energy | kJ | 1359 | |||||||||
| Protein | g | 14.29 | |||||||||
| Total lipid (fat) | g | 14.01 | |||||||||
| Ash | g | 7.07 | |||||||||
| Carbohydrate, by difference | g | 55.83 | |||||||||
| Fiber, total dietary | g | 53.2 | |||||||||
| Sugars, total | g | 2.76 | |||||||||
| Sucrose | g | 0.62 | |||||||||
| Glucose (dextrose) | g | 1.14 | |||||||||
| Fructose | g | 0.79 | |||||||||
| Lactose | g | 0 | |||||||||
| Maltose | g | 0 | |||||||||
| Galactose | g | 0.21 | |||||||||
| Minerals | |||||||||||
| Calcium, Ca | mg | 525 | |||||||||
| Iron, Fe | mg | 19.1 | |||||||||
| Magnesium, Mg | mg | 255 | |||||||||
| Phosphorus, P | mg | 367 | |||||||||
| Potassium, K | mg | 1170 | |||||||||
| Sodium, Na | mg | 52 | |||||||||
| Zinc, Zn | mg | 4.7 | |||||||||
| Copper, Cu | mg | 1.2 | |||||||||
| Manganese, Mn | mg | 8.3 | |||||||||
| Selenium, Se | µg | 40.3 | |||||||||
| Vitamins | |||||||||||
| Vitamin C, total ascorbic acid | mg | 0.7 | |||||||||
| Thiamin | mg | 0.176 | |||||||||
| Riboflavin | mg | 0.2 | |||||||||
| Niacin | mg | 3.26 | |||||||||
| Pantothenic acid | mg | 1.07 | |||||||||
| Vitamin B-6 | mg | 0.105 | |||||||||
| Folate, total | µg | 56 | |||||||||
| Folic acid | µg | 0 | |||||||||
| Folate, food | µg | 56 | |||||||||
| Folate, DFE | µg | 56 | |||||||||
| Choline, total | mg | 64.2 | |||||||||
| Betaine | mg | 28.8 | |||||||||
| Vitamin B-12 | µg | 0 | |||||||||
| Vitamin B-12, added | µg | 0 | |||||||||
| Vitamin A, RAE | µg | 1 | |||||||||
| Retinol | µg | 0 | |||||||||
| Carotene, beta | µg | 11 | |||||||||
| Carotene, alpha | µg | 0 | |||||||||
| Cryptoxanthin, beta | µg | 0 | |||||||||
| Vitamin A, IU | IU | 19 | |||||||||
| Lycopene | µg | 0 | |||||||||
| Lutein + zeaxanthin | µg | 0 | |||||||||
| Vitamin E (alpha-tocopherol) | mg | 25.24 | |||||||||
| Vitamin E, added | mg | 0 | |||||||||
| Tocopherol, beta | mg | 0 | |||||||||
| Tocopherol, gamma | mg | 1.15 | |||||||||
| Tocopherol, delta | mg | 0 | |||||||||
| Vitamin D (D2 + D3) | µg | 0 | |||||||||
| Vitamin D | IU | 0 | |||||||||
| Vitamin K (phylloquinone) | µg | 99.8 | |||||||||
| Lipids | |||||||||||
| Fatty acids, total saturated | g | 1.648 | |||||||||
| 4:0 | g | 0.012 | |||||||||
| 6:0 | g | 0.038 | |||||||||
| 8:0 | g | 0.013 | |||||||||
| 10:0 | g | 0.013 | |||||||||
| 12:0 | g | 0 | |||||||||
| 13:0 | g | 0.079 | |||||||||
| 14:0 | g | 0.637 | |||||||||
| 15:0 | g | 0 | |||||||||
| 16:0 | g | 0.681 | |||||||||
| 17:0 | g | 0 | |||||||||
| 18:0 | g | 0.174 | |||||||||
| 20:0 | g | 0 | |||||||||
| 22:0 | g | 0 | |||||||||
| 24:0 | g | 0 | |||||||||
| Fatty acids, total monounsaturated | g | 8.782 | |||||||||
| 14:1 | g | 0 | |||||||||
| 15:1 | g | 0 | |||||||||
| 16:1 undifferentiated | g | 0.013 | |||||||||
| 17:1 | g | 0 | |||||||||
| 18:1 undifferentiated | g | 8.742 | |||||||||
| 18:1 c | g | 8.742 | |||||||||
| 18:1 t | g | 0 | |||||||||
| 20:1 | g | 0.013 | |||||||||
| 22:1 undifferentiated | g | 0.014 | |||||||||
| 24:1 c | g | 0 | |||||||||
| Fatty acids, total polyunsaturated | g | 3.056 | |||||||||
| 18:2 undifferentiated | g | 2.788 | |||||||||
| 18:3 undifferentiated | g | 0.268 | |||||||||
| 18:3 n-3 c,c,c (ALA) | g | 0.255 | |||||||||
| 18:3 n-6 c,c,c | g | 0.013 | |||||||||
| 18:04:00 | g | 0 | |||||||||
| 20:2 n-6 c,c | g | 0 | |||||||||
| 20:3 undifferentiated | g | 0 | |||||||||
| 20:4 undifferentiated | g | 0 | |||||||||
| 20:5 n-3 (EPA) | g | 0 | |||||||||
| 22:5 n-3 (DPA) | g | 0 | |||||||||
| 22:6 n-3 (DHA) | g | 0 | |||||||||
| Fatty acids, total trans | g | 0 | |||||||||
| Fatty acids, total trans-monoenoic | g | 0 | |||||||||
| Cholesterol | mg | 0 | |||||||||
| Amino Acids | |||||||||||
| Tryptophan | g | 0.11 | |||||||||
| Threonine | g | 0.35 | |||||||||
| Isoleucine | g | 0.63 | |||||||||
| Leucine | g | 0.89 | |||||||||
| Lysine | g | 0.7 | |||||||||
| Methionine | g | 0.19 | |||||||||
| Cystine | g | 0.2 | |||||||||
| Phenylalanine | g | 0.58 | |||||||||
| Tyrosine | g | 0.4 | |||||||||
| Valine | g | 0.75 | |||||||||
| Arginine | g | 0.89 | |||||||||
| Histidine | g | 0.29 | |||||||||
| Alanine | g | 0.55 | |||||||||
| Aspartic acid | g | 1.79 | |||||||||
| Glutamic acid | g | 2.27 | |||||||||
| Glycine | g | 0.79 | |||||||||
| Proline | g | 1.24 | |||||||||
| Serine | g | 0.39 | |||||||||
| Hydroxyproline | g | 0 | |||||||||
| Other | |||||||||||
| Alcohol, ethyl | g | 0 | |||||||||
| Caffeine | mg | 0 | |||||||||
| Theobromine | mg | 0 | |||||||||
| Proanthocyanidin | |||||||||||
| Proanthocyanidin dimers | mg | 9.5 | |||||||||
| Proanthocyanidin trimers | mg | 22.9 | |||||||||
| Proanthocyanidin 4-6mers | mg | 41.8 | |||||||||
| Proanthocyanidin 7-10mers | mg | 0 | |||||||||
| Proanthocyanidin polymers (>10mers) | mg | 0 | |||||||||
Table 2. Chemical composition (%) of the essential oil of curry leaves from south region of Tamilnadu, India
| Compound | Oil (%) | KI |
|---|---|---|
| Α- Eudesmol | 0.2 | 1657 |
| β-Pinene | 0.3 | 974 |
| Myrcene | 6.12 | 991 |
| p-Cymene | 0.23 | 1023 |
| Limonene | 0.61 | 1027 |
| 1,8-Cineole | 1.56 | 1030 |
| (Z)-β-Ocimene | 0.36 | 1036 |
| (E)-β-Ocimene | 3.68 | 1047 |
| γ-Terpinene | 0.21 | 1057 |
| α-Terpinolene | 0.3 | 1087 |
| Linalool | 32.83 | 1104 |
| 1-Octen-3 yl acetate | 0.24 | 1108 |
| 3-Octanyl acetate | 0.26 | 1112 |
| Allo-Ocimene | 5.02 | 1129 |
| α-Terpineol | 4.9 | 1191 |
| Nerol | 1.32 | 1228 |
| Carvone | 0.16 | 1244 |
| Linalyl acetate | 16 | 1258 |
| Lavandulyl acetate | 0.23 | 1293 |
| Myrtenyl acetate | 0.1 | 1325 |
| Neryl acetate | 3.45 | 1359 |
| Geranyl acetate | 6.18 | 1383 |
| Β-Elemene | 0.26 | 1393 |
| Z-Jasmone | 0.3 | 1402 |
| α-Gurjunene | 0.1 | 1411 |
| β-Caryophyllene | 1.3 | 1422 |
| Germacrene D | 0.2 | 1479 |
| α-Amorphene | 0.7 | 1483 |
| δ-Cadinene | 0.26 | 1522 |
| Elemol | 7.44 | 1552 |
| Viridiflorol | 0.92 | 1595 |
| γ-Eudesmol | 0.77 | 1635 |
| Β- Eudesmol | 1.15 | 1654 |
Monoterpene Hydrocarbons 11.81 %
Oxygenated Monoterpenes 72.15 %
Sesquiterpene hydrocarbons 03.12 %
Oxygenated Sesquiterpenes 10.48 %
Table 3. Curry leaves essential oil antibacterial activity compared with selected antibiotics tested on ten strains of bacterial pathogens
| Sl.No. | Tested Bacteria | Zone of inhibition (mm) | ||
|---|---|---|---|---|
| Curry leaves essential oil | Negative Control | Positive Control | ||
| 1 | Corynebacterium psedotuberculosis | 15 | 5 | 20 (GEN10) |
| 2 | Streptococcus pyogenes | 10 | 6 | 24 (P10) |
| 3 | Klebsiella pneumoniae | 15 | 5 | 24 (GEN10) |
| 4 | Pseudomonas aeruginosa | 14 | 5 | 12 (CLR15) |
| 5 | Enterobacter aerogenes | 13 | 6 | 20(GEN10) |
| 6 | Salmonella enterica | 11 | 6 | 22 (GEN10) |
| 7 | Proteus mirabilis | 24 | 6 | 23 (AMX10) |
| 8 | Staphylococcus aureus | 16 | 5 | 20 (GEN10) |
Note: AMX10 = Amoxicillin (10mg/disc); CLR15 = Clarithromycin (15mg/disc); GEN10 = Gentamicin (10mg/disc); P10 = Penicillin (10mg/disc)
[Source 4]From the results outlined in table 3 above, the undiluted curry leaves essential oil exhibited strong antibacterial activity when tested with microorganisms. In comparison with the antibiotics as positive control they are expressing the remarkable antibacterial activities against Proteus mirabilis compared with Amoxicillin (10mg/disc), Staphylococcus aureus compared in Gentamicin (10mg/disc), Corynebacterium pseudotuberculosis compared in Gentamicin (10mg/disc), Klebsiella pneumonia compared in Gentamicin (10mg/disc), Pseudomonas aeruginosa compared in Clarithromycin (15mg/disc), Enterobacter aerogenes compared in Gentamicin (10mg/disc) and the moderate level zone of inhibition observed against in Salmonella enterica compared in Gentamicin (10mg/disc), Streptococcus pyogenes compared in Penicillin (10mg/disc). And based on this research 17, it was concluded that the chemical composition and antioxidative properties of the essential leaf oil of curry leaves from South Tamilnadu, India, that linalool, elemol, geranyl acetate, myrcene, allo-Ocimene and α-terpinene are the main components with such capacity.
Curry powder health benefits
The most active component of turmeric is curcumin 18. Curcumin [1,7-bis(4-hydroxy-3-methoxyphenyl)-1,6-heptadien-3,5-dione] is an orange–yellow crystalline powder – that gives a strong yellow color to the spice turmeric, is practically insoluble in water.
Turmeric is the powdered rhizome of Curcuma longa, a member of the ginger family and has been commonly used for flavor and color in food preparation in South Asia 19. In addition, it has been traditionally used as an herbal medicine to treat inflammatory and other disease conditions 19.
Turmeric is an ingredient of spice blends, mainly curry powder, which generally consists of turmeric, clove, paprika, ginger, cardamom, coriander, cumin, mace, pepper and cinnamon. Turmeric is commonly used as natural pigment (yellow 3) in the cosmetic and textile production but it is widely used in food industry. Indeed, turmeric is classified as an additive in E100 category and is used as food color additive in mustard, pastries, daily products and canned fish 20. Furthermore, according to the Joint FAO/WHO Expert Committee on Food Additives 21 the admissible daily intake is 0–3 mg/kg body weight and it was established at the 61st JECFA in 2003.
Curcumin’s use for various disease indications is primarily due to its active biological functions, i.e., anti-inflammatory, anti-oxidant, anti-microbial, anti-Alzheimer, anti-tumor, anti-diabetic, and anti-rheumatic activities 22. In addition, curcumin has been proven as a hypoglycemic, hepato-, nephron-, cardio-, and neuro-protective molecule 23. More importantly, this molecule also suppresses thrombosis and protects against myocardial infarction. It is, by far, the most prominent polyphenol, widely consumed on a daily basis along with food (in India, Eastern Asia, and some African countries), which leads to better compliance. Curcumin usage began in ancient days; however, in 1949, the first scientific evidence of its anti-bacterial activity at very low concentrations was reported in the journal “Nature” and extensive research began only after 1994.
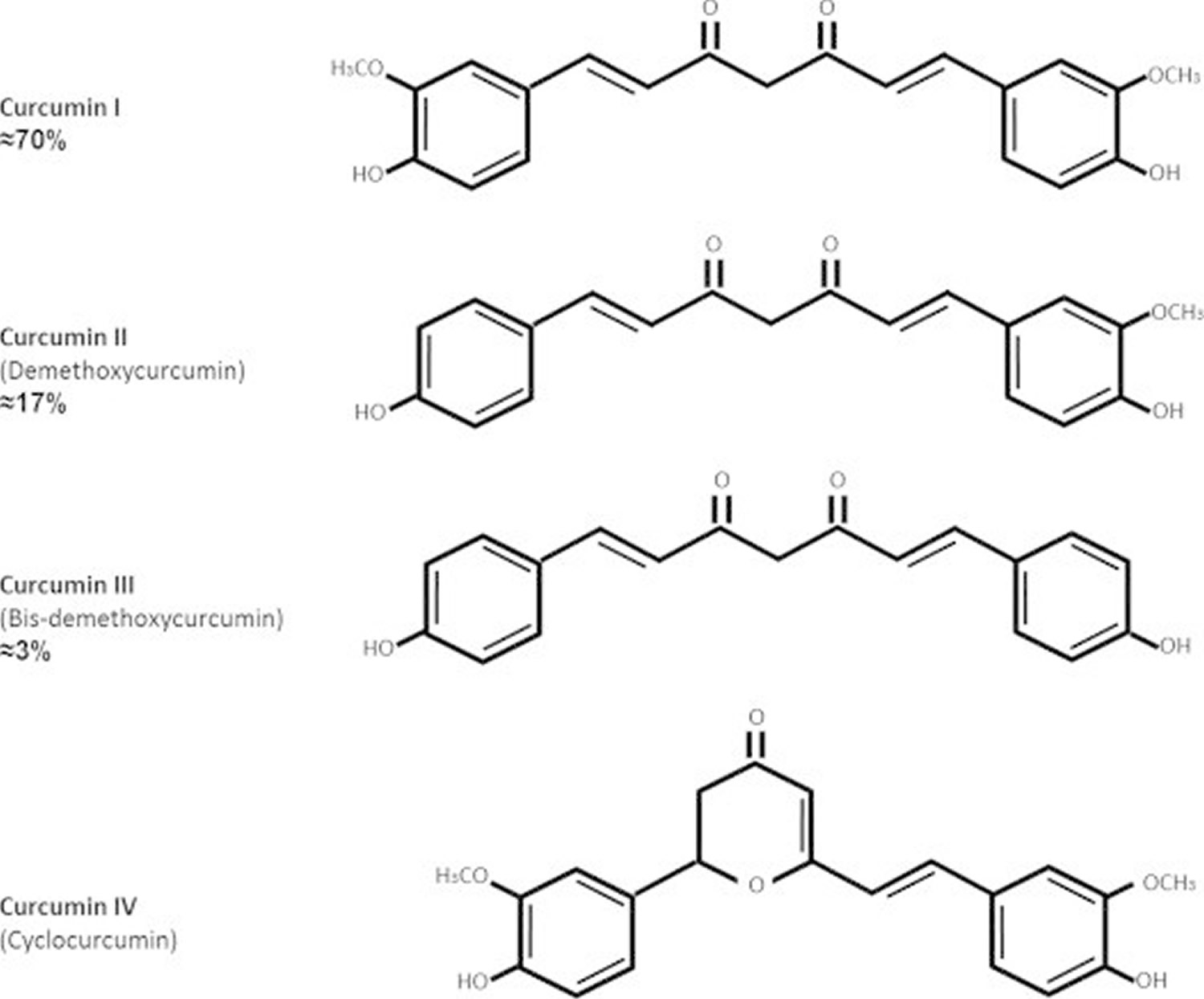
The biological activities of curcumin have been studied extensively 24. Curcumin is considered “generally recognized as safe (GRAS)” by the US Food Drug Administration 25, 26. Curcuma contains 60–70% carbohydrate, 8.6% protein, 5–10% fat, 2–7% fiber, 3–5% curcuminoids (50–70% curcumin) and up to 5% essential oils and resins 27. The curcuminoid content in turmeric may vary between 2 and 9%, depending on geographical conditions 28. The composition of curcuminoids is approximately 70% curcumin (curcumin I), 17% demethoxycurcumin (curcumin II), 3% bis-demethoxycurcumin (curcumin III) and the rest (10%) is called cyclocurcumin (curcumin IV) 29 (Figure 3). However, the last compound has been associated with poor or non-biological activity 30. The structure of curcumin (Figure 3) was first described in 1910 by Lampe and Milobedeska and proved to be diferuloylmethane 28. Studies indicate that functional groups associated to curcumin chemical structure including bis-α, β−unsaturated β-diketone, two methoxy groups, two phenolic hydroxy groups and two double-conjugated bonds might play an essential role in antiproliferative and anti-inflammatory activities assigned to curcumin 31. Curcumin has keto-enol tautomers, of which keto form predominates in acid and neutral solutions and enol form in alkaline solutions.
Figure 3. Chemical structures and abundance of curcuminoids in turmeric that have therapeutic effects
Curcumin traditional uses in folk medicine and biological properties
Curcuminoids have been consumed as therapeutic infusions over the centuries worldwide. In Ayurvedic medicine, curcumin is a well-documented treatment for various respiratory conditions such as, asthma, bronchial hyperactivity and allergy, as well as for liver disorders, anorexia, rheumatism, diabetic wounds, runny nose, cough and sinusitis 32. In traditional Chinese medicine curcumin has been used to treat diseases associated with abdominal pain 33. In ancient Hindu medicine, it was used to treat sprains and swelling 32. In Oriental cultures, it has traditionally been used as good therapeutic alternative, particularly as an anti-inflammatory, antioxidant, anticarcinogenic and antimicrobial reagent. In fact, it has been scientifically proven that curcumin is indeed antioxidant 34, anti-inflammatory 35 and antibacterial 36. Moreover, it has also been used because of its hepatoprotective 37, thrombosuppressive, neuroprotective 38, cardioprotective 34, antineoplasic 39, antiproliferative 40, hypoglycemic and antiarthritic effect 33. Curcumin has also been used for the treatment of intestinal parasites and as a remedy for poisoning, snakebites and various other complaints 41.
Therapeutic Applications of Curcumin Nanoformulations
From the literature, it is evident that poor solubility, bioavailability, and pharmacokinetics are major barriers to the clinical translational use of curcumin. Various strategies have been developed to overcome these problems. In numerous in vitro (test tube) and in vivo (animal) studies, nanoformulations of curcumin exhibited superior therapeutic benefits over the free curcumin 42 in a side-by-side setting. Recent clinical trials demonstrate that curcumin nanoformulations exhibit improved bioavailability of curcumin and thus provide a strong rationale for future clinical use once additional important mechanistic perspectives are understood. In this section, we precisely discuss the use of various curcumin nanoformulations in a number of diseases. Although, there is no report out there demonstrating clinical benefit of curcumin nanoformulation, but since curcumin nanoformulation(s) have shown superior outcomes in both in vitro and in vivo studies, it is believed that greater effects can be expected from curcumin nanoformulations over free curcumin. Clinical trials confirm that curcumin nanoformulations improve curcumin bioavailability and are systemically safe 43. However, testing of these formulations as therapeutic modalities is required and is crucial for future clinical trials and before human therapeutic use.
Several in vitro investigations demonstrate that curcumin inhibits cancer cells growth at concentration of 5–30 μM 44, resembling cisplatin and gem-citabine (chemotherapeutic drug) concentrations. Because of its exceptional medicinal value, a total of 68 clinical trials have been registered with clinicaltrials.gov in which the majority of them are targeting cancer.
Curcumin Toxicity and Side Effects
Turmeric and its constituents play a vital role in the management of various diseases including cancer. Toxicity and lethal dose level of curcumin are important before using in health management. Several studies were performed to check the safe dose of curcumin in animal model studies. No significant toxicity was observed of turmeric and its constituent curcumin at various doses. An important study in which animals were fed curcumin with a dose of 1.8 gms/kg and 0.8 mg/kg in rat and monkey, respectively, for 90 days showed no adverse effects 45. An important study in which animals were fed curcumin with a dose of 1.8 gms/kg and 0.8 mg/kg in rat and monkey, respectively, for 90 days showed no adverse effects 45. Curcumin is remarkably well tolerated, but its bioavailability is poor. It does not show to be toxic to humans 46 even at high doses. Earlier studies concluded that combination therapy using 8 g oral curcumin daily with gemcitabine-based chemotherapy was safe and feasible in patients with pancreatic cancer 47 and other study concluded that oral curcumin is well tolerated and, despite its limited absorption, showed biological activity 48. An important study based on advanced pancreatic cancer patients showed that 5 patients out of 17 patients receiving curcumin with dose 8 gms/day with gemcitabine showed intractable abdominal pain after a few days to 2 weeks of curcumin intake 49.
A study reported that hepatotoxicity was seen in mice fed with whole turmeric (0.2%, 1%, 5%) or ethanolic turmeric extract (ETE; 0.05%, 0.25%) for 14 days 50. Earlier report based on curcumin has shown that curcumin doses ranging from 0.45 to 3.6 gms/day for 1 to 4 months showed nausea and diarrhea and also caused an increase in serum alkaline phosphatase and lactate dehydrogenase contents 51.
- https://www.mccormick.com/gourmet/spices-and-flavors/organic/organic-curry-powder[↩]
- The antimicrobial activity of essential oil from Dracocephalum foetidum against pathogenic microorganisms. Lee SB, Cha KH, Kim SN, Altantsetseg S, Shatar S, Sarangerel O, Nho CW. J Microbiol. 2007 Feb; 45(1):53-7. https://www.ncbi.nlm.nih.gov/pubmed/17342056/[↩]
- Stress repression in restrained rats by (R)-(-)-linalool inhalation and gene expression profiling of their whole blood cells. Nakamura A, Fujiwara S, Matsumoto I, Abe K. J Agric Food Chem. 2009 Jun 24; 57(12):5480-5. https://www.ncbi.nlm.nih.gov/pubmed/19456160/[↩]
- Rajendran MP, Pallaiyan BB, Selvaraj N. Chemical composition, antibacterial and antioxidant profile of essential oil from Murraya koenigii (L.) leaves. Avicenna Journal of Phytomedicine. 2014;4(3):200-214. https://www.ncbi.nlm.nih.gov/pmc/articles/PMC4104627/[↩][↩][↩]
- Mantle D, Anderton JG, Falkous G, Barnes M, Jones P, Perry EK. Comparison of methods for determination of total antioxidant status: application to analysis of medicinal plant essential oils. Biochem Physiol, part B. Biochem Molecul Biol. 1998;121B:385–391.[↩]
- Walde GS, Joythirmay T, Rao PGP, Shivaswamy R, Srinivas P. Flavour volatiles of leaves, fruits and seed cotyledons of Murraya koenigii L. Flav Frag J. 2005;20:169–172.[↩]
- Deshmukh SK, Jain PC, Agarwal SC. Antimicrobial activity of the essential oil of the leaves of Murraya koenigii (Linn) Spreng (Indian curry leaf) Fitoterapia. 1986;57:295.[↩]
- Romero A, Doval M, Stura M, Judis X. Antioxidant properties of polyphenol-containing extract from soybean fermented with Saccharomyces cerevisiae. Eur J Lipid Sci Technol. 2004;105:424–431.[↩]
- Gopalan C, Rama Shastri BV, Balasubramanian SC. Nutritive value of Indian Foods. Vol. 66. New Delhi: ICMR; 1984. p. 117.[↩]
- Jasim Uddin Chowdhury Md, Nazrul Islam Bhuiyan, Mohammed Yusuf. Chemical composition of the leaf essential oils of Murraya koenigii (L.) Spreng and Murraya paniculata (L.) Jack. Bangladesh J Pharmacol. 2008;3:59–63.[↩]
- Arulselvan P., Subramanian S.P. Beneficial effects of Murraya koenigii leaves on antioxidant defense system and ultrastructural changes of pancreatic β-cell in experimental diabetes. Chem. Biol. Interact. 2007;165:155–164. https://www.ncbi.nlm.nih.gov/pubmed/17188670[↩]
- Kesari A.N., Kesari S., Singh S.K., Gupta R.K., Watal G. Studies on the glycemic and lipidemic effect of Murraya koenigii in experimental animals. J. Ethnopharmacol. 2007;112:305–311.[↩]
- Firdaus SB, Ghosh D, Chattyopadhyay A, et al. Protective effect of antioxidant rich aqueous curry leaf (Murraya koenigii) extract against gastro-toxic effects of piroxicam in male Wistar rats. Toxicology Reports. 2014;1:987-1003. doi:10.1016/j.toxrep.2014.06.007. https://www.ncbi.nlm.nih.gov/pmc/articles/PMC5598401/[↩]
- Singh A.P., Wilson T., Vorsa V., Luthria D., Freeman M.R., Scott R.M., Bilenker D., Shah S., Somasundaram S., Vorsa N. LC–MS–MS characterization of curry leaf flavonols and antioxidant activity. Food Chem. 2011;127:80–85.[↩]
- Mitra E., Ghosh A.K., Ghosh D., Mukherjee D., Chattopadhyay A., Dutta S., Pattari S.K., Bandyopadhyay D. Protective effect of aqueous curry leaf (Murraya koenigii) extract against cadmium-induced oxidative stress in rat heart. Food Chem. Toxicol. 2012;50:340–353 https://www.ncbi.nlm.nih.gov/pubmed/22342528[↩]
- United States Department of Agriculture Agricultural Research Service. National Nutrient Database for Standard Reference Release 28. https://ndb.nal.usda.gov/ndb/search/list[↩]
- Rajendran MP, Pallaiyan BB, Selvaraj N. Chemical composition, antibacterial and antioxidant profile of essential oil from Murraya koenigii (L.) leaves. Avicenna Journal of Phytomedicine. 2014;4(3):200-214. https://www.ncbi.nlm.nih.gov/pmc/articles/PMC4104627/ [↩]
- Sandur S.K., Pandey M.K., Sung B., Ahn K.S., Murakami A., Sethi G., Limtrakul P., Badmaev V., Aggarwal B.B. Curcumin, demethoxycurcumin, bisdemethoxycurcumin, tetrahydrocurcumin and turmerones differentially regulate anti-inflammatory and anti-proliferative responses through a ROS-independent mechanism. Carcinogenesis. 2007;28:1765–1773. https://www.ncbi.nlm.nih.gov/pubmed/17522064[↩]
- Pharmacology of Curcuma longa. Ammon HP, Wahl MA. Planta Med. 1991 Feb; 57(1):1-7. https://www.ncbi.nlm.nih.gov/pubmed/2062949/[↩][↩]
- Himesh S., Sharan P.S., Mishra K., Govind N., Singhai A. Qualitative and quantitative profile of curcumin from ethanolic extract of curcuma longa. International Research Journal of Pharmacy. 2011;2:180–184.[↩]
- Esatbeyoglu T., Huebbe P., Ernst I.M., Chin D., Wagner A.E., Rimbach G. Curcumin—from molecule to biological function. Angewandte Chemie International Edition (in English) 2012;51:5308–5332.[↩]
- Curcumin: the Indian solid gold. Aggarwal BB, Sundaram C, Malani N, Ichikawa H. Adv Exp Med Biol. 2007; 595():1-75. https://www.ncbi.nlm.nih.gov/pubmed/17569205/[↩]
- Renoprotective effect of the antioxidant curcumin: Recent findings. Trujillo J, Chirino YI, Molina-Jijón E, Andérica-Romero AC, Tapia E, Pedraza-Chaverrí J. Redox Biol. 2013 Sep 17; 1():448-56. https://www.ncbi.nlm.nih.gov/pmc/articles/PMC3814973/[↩]
- Multiple biological activities of curcumin: a short review. Maheshwari RK, Singh AK, Gaddipati J, Srimal RC. Life Sci. 2006 Mar 27; 78(18):2081-7. https://www.ncbi.nlm.nih.gov/pubmed/16413584/[↩]
- Curcumin from turmeric (Curcuma longa L.). https://www.accessdata.fda.gov/scripts/fdcc/?set=GRASNotices&id=686&sort=GRN_No&order=DESC&startrow=1&type=basic&search=Curcumin[↩]
- Curcuminoids purified from turmeric (Curcuma longa L.). https://www.accessdata.fda.gov/scripts/fdcc/?set=GRASNotices&id=460&sort=GRN_No&order=DESC&startrow=1&type=basic&search=Curcumin[↩]
- Trujillo J, Chirino YI, Molina-Jijón E, Andérica-Romero AC, Tapia E, Pedraza-Chaverrí J. Renoprotective effect of the antioxidant curcumin: Recent findings. Redox Biology. 2013;1(1):448-456. doi:10.1016/j.redox.2013.09.003. https://www.ncbi.nlm.nih.gov/pmc/articles/PMC3814973/[↩]
- Esatbeyoglu T., Huebbe P., Ernst I.M., Chin D., Wagner A.E., Rimbach G. Curcumin—from molecule to biological function. Angewandte Chemie International Edition (in English) 2012;51:5308–5332. https://www.ncbi.nlm.nih.gov/pubmed/22566109[↩][↩]
- Goel A., Aggarwal B.B. Curcumin, the golden spice from Indian saffron, is a chemosensitizer and radiosensitizer for tumors and chemoprotector and radioprotector for normal organs. Nutrition and Cancer. 2010;62:919–930. https://www.ncbi.nlm.nih.gov/pubmed/20924967[↩]
- Rahman I., Biswas S.K., Kirkham P.A. Regulation of inflammation and redox signaling by dietary polyphenols. Biochemical Pharmacology. 2006;72:1439–1452. https://www.ncbi.nlm.nih.gov/pubmed/16920072[↩]
- Aggarwal B.B., Sung B. Pharmacological basis for the role of curcumin in chronic diseases: an age-old spice with modern targets. Trends in Pharmacological Sciences. 2009;30:85–94. https://www.ncbi.nlm.nih.gov/pubmed/19110321[↩]
- Araújo C.C., Leon L.L. Biological activities of Curcuma longa L. Memorias do Instituto Oswaldo Cruz. 2001;96:723–728. https://www.ncbi.nlm.nih.gov/pubmed/11500779[↩][↩]
- Goel A., Kunnumakkara A.B., Aggarwal B.B. Curcumin as Curecumin: from kitchen to clinic. Biochemical Pharmacology. 2008;75:787–809. https://www.ncbi.nlm.nih.gov/pubmed/17900536[↩][↩]
- González-Salazar A., Molina-Jijón E., Correa F., Zarco-Márquez G., Calderón-Oliver M., Tapia E., Zazueta C., Pedraza-Chaverri J. Curcumin protects from cardiac reperfusion damage by attenuation of oxidant stress and mitochondrial dysfunction. Cardiovascular Toxicology. 2011;11:357–364. https://www.ncbi.nlm.nih.gov/pubmed/21769543[↩][↩]
- Wang M.E., Chen Y.C., Chen I.S., Hsieh S.C., Chen S.S., Chiu C.H. Curcumin protects against thioacetamide-induced hepatic fibrosis by attenuating the inflammatory response and inducing apoptosis of damaged hepatocytes. The Journal of Nutritional Biochemistry. 2012;23:1352–1366. https://www.ncbi.nlm.nih.gov/pubmed/22221674[↩]
- Mun S.H., Joung D.K., Kim Y.S., Kang O.H., Kim S.B., Seo Y.S., Kim Y.C., Lee D.S., Shin D.W., Kweon K.T., Kwon D.Y. Synergistic antibacterial effect of curcumin against methicillin-resistant Staphylococcus aureus. Phytomedicine. 2013;20:714–718. https://www.ncbi.nlm.nih.gov/pubmed/23537748[↩]
- Osawa T. Nephroprotective and hepatoprotective effects of curcuminoids. Advances in Experimental Medicine and Biology. 2007;595:407–423. https://www.ncbi.nlm.nih.gov/pubmed/17569222[↩]
- Wang H.M., Zhao Y.X., Zhang S., Liu G.D., Kang W.Y., Tang H.D., Ding J.Q., Chen S.D. PPARgamma agonist curcumin reduces the amyloid-beta-stimulated inflammatory responses in primary astrocytes. Journal of Alzheimer’s Disease. 2010;20:1189–1199. https://www.ncbi.nlm.nih.gov/pubmed/20413894[↩]
- Aggarwal B.B., Kumar A., Bharti A.C. Anticancer potential of curcumin: preclinical and clinical studies. Anticancer Research. 2003;23:363–398. https://www.ncbi.nlm.nih.gov/pubmed/12680238[↩]
- Bachmeier B.E., Killian P., Pfeffer U., Nerlich A.G. Novel aspects for the application of curcumin in chemoprevention of various cancers. Frontiers in Bioscience (Scholar edition) 2010;S2:697–717. https://www.ncbi.nlm.nih.gov/pubmed/20036978[↩]
- Maheshwari R.K., Singh A.K., Gaddipati J., Srimal R.C. Multiple biological activities of curcumin: a short review. Life Sciences. 2006;78:2081–2087. https://www.ncbi.nlm.nih.gov/pubmed/16413584[↩]
- Curcumin nanoformulations: a future nanomedicine for cancer. Yallapu MM, Jaggi M, Chauhan SC. Drug Discov Today. 2012 Jan; 17(1-2):71-80. https://www.ncbi.nlm.nih.gov/pmc/articles/PMC3259195/[↩]
- Yallapu MM, Nagesh PKB, Jaggi M, Chauhan SC. Therapeutic Applications of Curcumin Nanoformulations. The AAPS Journal. 2015;17(6):1341-1356. doi:10.1208/s12248-015-9811-z. https://www.ncbi.nlm.nih.gov/pmc/articles/PMC4627456[↩]
- Treasure J. Herbal medicine and cancer: an introductory overview. Semin Oncol Nurs. 2005;21:177–83. https://www.ncbi.nlm.nih.gov/pubmed/16092805[↩]
- Majeed M, Badmaev V, Shivakumar U, Rajendran R. Curcuminoids. Antioxidant Phytonutrients. Piscataway, NJ, USA: Nutriscience; 1995.[↩][↩]
- Soni KB, Kuttan R. Effect of oral curcumin administration on serum peroxides and cholesterol levels in human volunteers. Indian Journal of Physiology and Pharmacology. 1992;36(4):273–275. https://www.ncbi.nlm.nih.gov/pubmed/1291482[↩]
- Kanai M, Yoshimura K, Asada M, et al. A phase I/II study of gemcitabine-based chemotherapy plus curcumin for patients with gemcitabine-resistant pancreatic cancer. Cancer Chemotherapy and Pharmacology. 2011;68(1):157–164. https://www.ncbi.nlm.nih.gov/pubmed/20859741[↩]
- Dhillon N, Aggarwal BB, Newman RA, et al. Phase II trial of curcumin in patients with advanced pancreatic cancer. Clinical Cancer Research. 2008;14(14):4491–4499. http://clincancerres.aacrjournals.org/content/14/14/4491.long[↩]
- Epelbaum R, Schaffer M, Vizel B, Badmaev V, Bar-Sela G. Curcumin and gemcitabine in patients with advanced pancreatic cancer. Nutrition and Cancer. 2010;62(8):1137–1141. https://www.ncbi.nlm.nih.gov/pubmed/21058202[↩]
- Kandarkar SV, Sawant SS, Ingle AD, Deshpande SS, Maru GB. Subchronic oral hepatotoxicity of turmeric in mice—histopathological and ultrastructural studies. Indian Journal of Experimental Biology. 1998;36(7):675–679. https://www.ncbi.nlm.nih.gov/pubmed/9782784[↩]
- Sharma RA, Euden SA, Platton SL, et al. Phase I clinical trial of oral curcumin: biomarkers of systemic activity and compliance. Clinical Cancer Research. 2004;10(20):6847–6854. http://clincancerres.aacrjournals.org/content/10/20/6847.long [↩]