Contents
- What is electroconvulsive therapy
- What tests and assessments are required pre-electroconvulsive therapy?
- When is electroconvulsive therapy is most useful?
- Will I experience any pain?
- Do I have to remain in hospital whilst having electroconvulsive therapy?
- What are the number and frequency of treatments?
- What will happen towards the end of my acute course of electroconvulsive therapy?
- What is maintenance electroconvulsive therapy and will I be offered this option?
- What if I relapse?
- Are there alternatives to electroconvulsive therapy?
- Electroconvulsive therapy preparation
- How is electroconvulsive therapy given?
- Important information following electroconvulsive therapy
- Electroconvulsive therapy side effects
- Electroconvulsive therapy risks
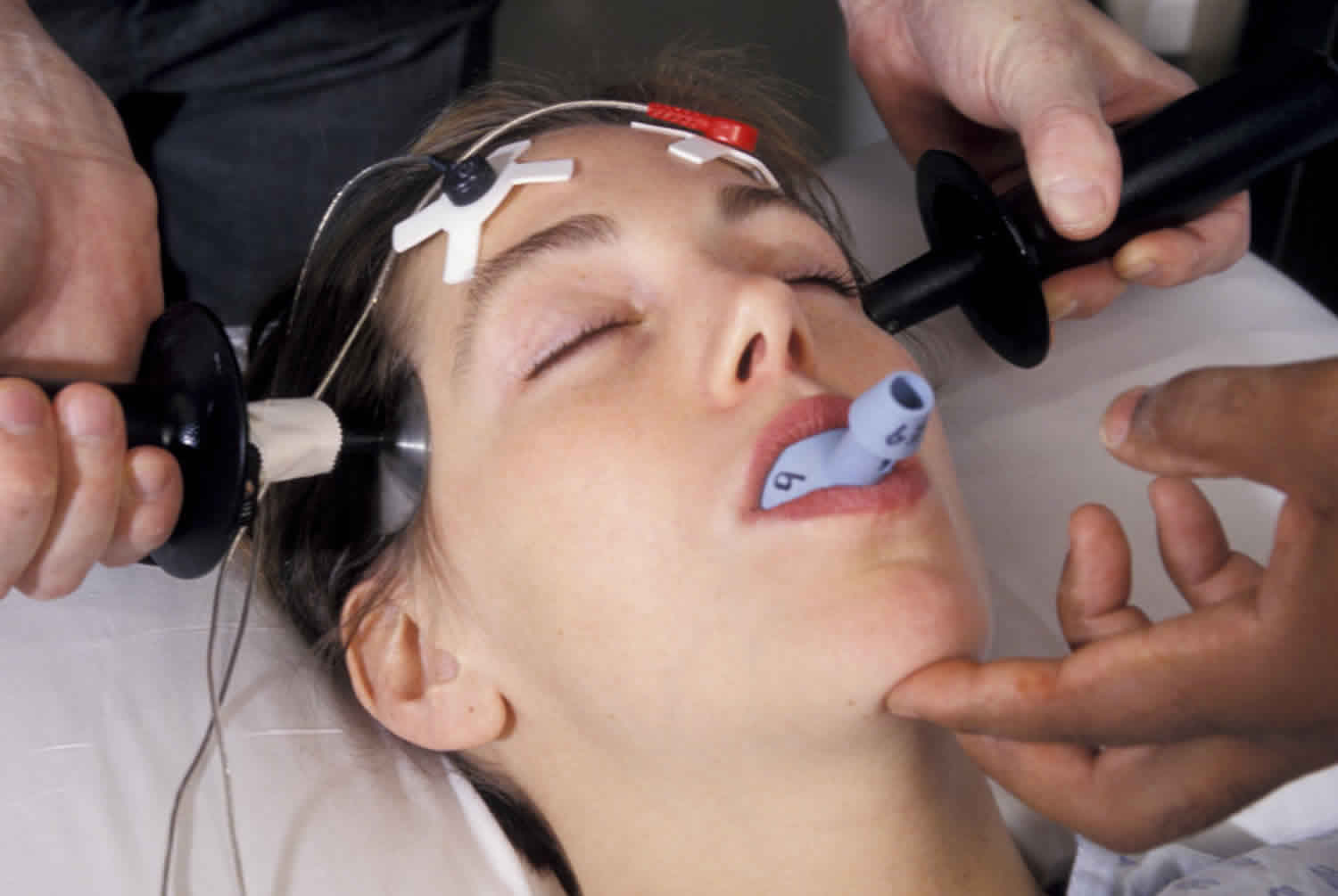
What is electroconvulsive therapy
Electroconvulsive therapy (ECT) involves passing brief, carefully-controlled electric currents through the brain 1. The electric currents affects the brain’s electrical activity in a way which can lessen depressive and psychotic symptoms. Electroconvulsive therapy is a relatively safe and effective treatment for some severe mental health conditions that are considered life threatening. Electroconvulsive therapy is used to treat certain psychiatric disorders such as severe depression, bipolar disorder and psychotic illnesses such as schizophrenia.
Electroconvulsive therapy is used for the fast treatment of severe depression, mania or psychosis. Electroconvulsive therapy may be used when symptoms are severe, when a situation is life-threatening, or when other forms of treatment have been ineffective.
Despite the controversial history of electroconvulsive therapy, there is now a clear body of scientific evidence that electroconvulsive therapy is effective in improving depressive and psychotic symptoms in the short term. For uncomplicated, severe depression, evidence suggests at least an 80% improvement. However, as with all forms of medical treatment, not all patients improve at the same rate. It is important to note that it will generally take around 4 to 5 treatments before you may feel an improvement in your symptoms.
To make the return of symptoms less likely, doctors may prescribe medication and psychotherapy. Some people may require several courses of the treatment over their lifetime.
Electroconvulsive therapy should only be used with the informed consent of the person being treated. Before electroconvulsive therapy can be used, the person being treated must give informed consent to show that they understand the treatment, as well as the risks and benefits. If they are unable to give consent because of their mental health, their psychiatrist will seek a decision from the state’s mental health authority.
A person who gives consent can withdraw it at any time.
If at any time you feel concerned or wish to discuss your progress, or have any questions regarding treatment do not hesitate to discuss these with the electroconvulsive therapy staff and your doctor.
Before your first electroconvulsive therapy treatment, you will have a thorough psychiatric evaluation as well as a complete physical health examination to ensure that electroconvulsive therapy is indicated for your health condition.
Electroconvulsive therapy is most useful in the treatment of:
- Severe forms of depression
- Severe manic symptoms, including bipolar disorder
Electroconvulsive therapy is useful because it works more quickly than other treatments such as medicines or therapy. Electroconvulsive therapy is used cautiously because it is more intrusive than other treatments and may cause memory problems. Since the effects are short-lived, long-term treatment with antidepressant or mood-stabilizing medicine is usually needed.
Like any procedure involving anesthesia, electroconvulsive therapy carries a small degree of risk. The most common side effects are headache, stomach upsets, aching muscles and short-term memory loss.
Studies have shown that electroconvulsive therapy does not harm the brain or change its anatomy in any way, as the strength of the electrical current is too low to cause damage.
Electroconvulsive therapy key facts
- Electroconvulsive therapy was developed in 1938, and was an unregulated treatment during the 40s and 50s. This led to many misconceptions about shock therapy and electroconvulsive therapy.
- Electroconvulsive therapy is used in many countries, and its safety and effectiveness is well documented.
- Approximately eight out of 10 people who undergo electroconvulsive therapy will experience dramatic improvement in symptoms.
Electroconvulsive therapy myths and misconceptions
- Myth: Electroconvulsive therapy is ‘shock therapy’ that leaves a patient brain damaged and writhing in pain.
- Reality: Electroconvulsive therapy does induce seizures, but patients are first given a muscle relaxant and general anaesthetic. There is no evidence that Electroconvulsive therapy causes brain damage. Media depictions of Electroconvulsive therapy, such as in the film One Flew Over the Cuckoo’s Nest, are inaccurate and further stigmatise a safe and effective treatment.
- Myth: Electroconvulsive therapy is given without your consent.
- Reality: If your psychiatrist suggests that electroconvulsive therapy might be helpful for you, you can refuse the treatment. Where a patient is not able to provide consent – for example, if they are unresponsive or severely delusional – their family and carers help the psychiatrist to make a decision in their best interests and in these instances, approval from the mental health authority is usually required.
- Myth: Electroconvulsive therapy erases memory.
- Reality: Most patients experience some short-term memory loss, which often improves with time. It is rare to experience long-term memory loss from Electroconvulsive therapy
- Myth: Electroconvulsive therapy is only used for depression.
- Reality: Electroconvulsive therapy most commonly used for people with severe depression that has not responded to other treatments. It is also used to treat people with bipolar disorder, schizophrenia and psychosis.
What tests and assessments are required pre-electroconvulsive therapy?
Prior to your first electroconvulsive therapy treatment any tests/reviews will be discussed with you.
- Blood tests, ECG and chest x-ray may be ordered by your treating psychiatrist.
- Medications will be reviewed and may be adjusted by your treating psychiatrist.
- Anesthetic review will be conducted by the electroconvulsive therapy anesthetist.
When is electroconvulsive therapy is most useful?
Electroconvulsive therapy has been shown to be the most effective antidepressant treatment available for severe depression, with a response rate of over 70%. However, further treatment either through continued electroconvulsive therapy or antidepressant pharmacotherapy is beneficial in the prevention relapse in depressive symptoms after an effective acute electroconvulsive therapy course.
Electroconvulsive therapy is often prescribed as a treatment for depression when other treatments (antidepressant medication and psychological therapy) have failed to produce an improvement in symptoms, when patients have experienced serious side effects from medications, or are unable to safely take particular medications due to a medical condition. Due to the fast acting antidepressant effects of electroconvulsive therapy it may also be prescribed when the risk of suicide is high or when a patient is too unwell to eat, drink or take medications.
Electroconvulsive therapy is also used in the treatment of acute mania, catatonia and schizophrenia. However, the National Institute for Health and Care Excellence 2 advises that electroconvulsive therapy should not be used for the general management of schizophrenia.
Will I experience any pain?
Electroconvulsive therapy is not painful as you are administered a general anesthetic and you will be asleep for the treatment. You may experience headache and/or muscle pain usually within the first few hours after electroconvulsive therapy. This is often more marked following the first treatment and less for subsequent treatments. This can be easily alleviated with analgesia e.g., acetaminophen (paracetamol).
Do I have to remain in hospital whilst having electroconvulsive therapy?
Whether you require an admission to hospital for electroconvulsive therapy or that you are to receive electroconvulsive therapy as a day patient depends on a number of factors. Patients that require an acute course are better treated initially as inpatients. Outpatient status may be considered for treatment in the latter stages of treatment or those considered for maintenance treatment. You will need to discuss these options with your psychiatrist.
What are the number and frequency of treatments?
Generally patients undergo an average of ten electroconvulsive therapy treatments. This depends on your individual progress and assessment. Treatments are usually given 2 -3 times per week for the initial treatment course.
What will happen towards the end of my acute course of electroconvulsive therapy?
To remain well after a course of electroconvulsive therapy, it is important to continue with a form of antidepressant treatment. An antidepressant or other drug may be introduced towards the end of the course to help prevent relapse. Outpatient day program, counseling and other supports may be introduced to assist your return to a normal life. For a few patients who do not remain well on medications, maintenance electroconvulsive therapy may be offered.
What is maintenance electroconvulsive therapy and will I be offered this option?
Your psychiatrist may discuss maintenance electroconvulsive therapy with you towards the end of your acute course of electroconvulsive therapy. This will be based on an individual clinical assessment as to whether this is a viable option for you. This is given on a gradually extended basis starting at weekly and progressing to monthly or even longer between treatments.
What if I relapse?
If there is a relapse in your illness, it is important to treat quickly. It may require changes to medications, or it may require a further course of electroconvulsive therapy. In either case it is essential to act promptly so you do not have to endure an extended period of illness.
Are there alternatives to electroconvulsive therapy?
Alternatives to electroconvulsive therapy are currently being researched include:
- Mild brain stimulation (MBS) – relevant parts of the brain are stimulated with very weak currents via two electrodes placed on the head
- Transcranial magnetic stimulation (TMS) – a coil that creates a magnetic field is held next to the head to stimulate the relevant parts of the brain
Unlike electroconvulsive therapy, neither treatment requires a general anesthetic.
Electroconvulsive therapy preparation
- Fast from midnight
- If medications have been prescribed prior to electroconvulsive therapy take with only a small sip of water.
- Ensure your hair is clean and dry
- Do not apply face creams, moisturizers or makeup. Remove nail polish and jewellery.
- Do not bring cigarettes, lighters and mobile phones into the treatment room.
- Dress in loose clothing to enable the easy application of the monitors
- If you wear contact lenses, glasses or dentures these can be removed in the treatment room and placed under your trolley. If you have worn contact lenses please ensure you bring a case.
How is electroconvulsive therapy given?
Electroconvulsive therapy is administered in a hospital, usually by the treating psychiatrist and an anesthetist. The person being treated is given a general anesthetic and a muscle relaxant, so is unconscious during the treatment.
Electrodes are placed on one (unilateral) or both (bilateral) sides of the scalp and a small electric current is passed between these in order to trigger a brief generalized seizure. The person does not feel anything due to the anesthetic and does not convulse due to the muscle relaxant. The seizure temporarily changes the chemistry in the brain and improves some symptoms quickly.
The person being treated doesn’t feel discomfort and usually wakes up 5 to 10 minutes after the procedure. They may feel groggy at first, but will be clear-headed within 30 minutes.
You will remain in the recovery room for an additional 30 minutes where you will be observed by experienced nursing staff for 30 minutes.
Treatment is typically repeated a number of times. While most people show some improvement after 3 to 4 sessions, some may need 20 to 25 sessions, depending on the nature of the illness and the response to treatment. Treatments are usually given 2 to 3 times a week.
Important information following electroconvulsive therapy
Once you have recovered from the electroconvulsive therapy procedure the nursing staff will accompany you back to the ward. It is important that you remain on the ward until you have been reviewed by your psychiatrist.
Breakfast and any medications will be administered.
A post electroconvulsive therapy medical review will be conducted.
Refrain from smoking or participating in excessive exercise for at least 2 hours.
For 24 hours after electroconvulsive therapy:
- Avoid driving a motor vehicle or operating machinery, including domestic appliances.
- Avoid making any major personal decisions, sign contracts or enter into any business arrangements during an acute course of treatment.
Electroconvulsive therapy side effects
Despite its controversial history, the risks and side effects of modern electroconvulsive therapy are very low. The main side effect of electroconvulsive therapy is short-term memory loss 3. Electroconvulsive therapy can also cause varying degrees of memory problems, including long-term and even permanent memory loss 4.
People can also feel disorientated and confused straight after electroconvulsive therapy.
Patients with severe depression commonly experience impaired concentration and attention, which usually improves with electroconvulsive therapy. Most patients will have some memory impairment of the time surrounding the electroconvulsive therapy treatment and associated time in hospital. Some of this will be from the depression, as memories are not well formed when you are experiencing poor concentration.
Over the course of electroconvulsive therapy, it may be more difficult to remember newly learned information. This difficulty disappears following completion of the electroconvulsive therapy course.
Some patients also report a partial loss of memory for events that occurred during the time prior to electroconvulsive therapy. While many of these memories typically return after electroconvulsive therapy, rarely a few patients do report long lasting memory impairment.
The extent and duration of memory impairment can depend on type and frequency of electroconvulsive therapy. This is why it is important to report any perceived memory impairment as the treatment can be adjusted.
Other side effects include heart rhythm disturbances, low blood pressure, headaches, nausea and sore jaw muscles.
Electroconvulsive therapy risks
Electroconvulsive therapy carries the risks associated with having a general anesthetic. Overall the medical complication rate with electroconvulsive therapy is very low and is comparable to other minor medical procedures involving anesthesia (2.0-2.5 deaths per 100,000). Some patients with pre-existing medical conditions have an increased risk associated with electroconvulsive therapy. All patients undergo a medical review prior to electroconvulsive therapy.
A brief period of confusion following electroconvulsive therapy is relatively common 5. Some people may experience a headache or nausea and these side effects can be treated with medication if necessary. Muscle soreness or aching can also occur after electroconvulsive therapy as a result of the medications given to relax muscles during electroconvulsive therapy. These effects are transient, usually lasting only a few hours after the electroconvulsive therapy.
Electroconvulsive therapy can cause temporary memory loss. Specifically, some patients experience difficulties lying down new memories during the course of electroconvulsive therapy and may be unable to remember events which occurred during this period. Evidence from research suggests that if memory and thinking are affected by electroconvulsive therapy, the period of memory problems is relatively brief and test scores have usually returned to pre-electroconvulsive therapy levels one month after treatment.
Sometimes occasional memories from the past may be forgotten. It is also important to note that many patients suffering from depression already have problems with attention, concentration, thinking and memory prior to commencing electroconvulsive therapy. It is not uncommon for patients to report that their memory is better following electroconvulsive therapy. The safety of electroconvulsive therapy has also been examined with detailed brain scans done before and after electroconvulsive therapy. There is no evidence that electroconvulsive therapy causes brain damage 6.
- Loo, C. K., Katalinic, N., Martin, D., and Schweitzer, I. (2012). A review of ultrabrief pulse width electroconvulsive therapy. Therapeutic Advances in Chronic Disease, 3(2), 69-85.[↩]
- Guidance on the use of electroconvulsive therapy. https://www.nice.org.uk/guidance/ta59[↩]
- Semkovska, M., and McLoughlin, D.M. (2010). Objective cognitive performance associated with electroconvulsive therapy for depression: A system review and meta-analysis. Biological Psychiatry, 68(6), 568-577.[↩]
- Semkovska, M., Keane, D., Babalola, O., and McLoughlin, D. M. (2011). Unilateral brief-pulse electroconvulsive therapy and cognition: Effects of electrode placement, stimulus dosage and time. Journal of Psychiatric Research, 45(6), 770-780.[↩]
- Rose, D., Fleischmann, P., Wykes, T., Leese, M. and Bindman J.(2003). Patients’ perspectives on electroconvulsive therapy: Systematic review. British Medical Journal, 326, 1363.[↩]
- Baker, P. L., Trevino, K., McClintock, S. M., Wani, A., and Husain, M. M. (2012). Clinical applications of electroconvulsive therapy and transcranial magnetic stimulation for the treatment of major depressive disorder: A critical review. Neuropsychiatry, 2(5), 443-451.[↩]