Contents
- What foods cause inflammation in the body
What foods cause inflammation in the body
Inflammation is the common link among the leading causes of death. Together, cardiovascular disease, cancer, and diabetes account for almost 70% of all deaths in the United States; these diseases share inflammation as a common link 1, 2. Dietary strategies clearly influence inflammation, as documented through both prospective observational studies as well as randomized controlled feeding trials in which participants agree to eat only the food provided to them 1, 3. Studies have shown how various dietary components can modulate key pathways to inflammation including sympathetic activity, oxidative stress, transcription factor nuclear factor kappa B (NF-κB) activation, and proinflammatory cytokine production 4. Circulating markers of inflammation, such as C-reactive protein (CRP), tumor necrosis factor (TNF)-alpha, and some interleukins (IL-6, IL-18), correlate with propensity to develop coronary heart disease and heart attacks 5, 6, 7. Previous studies have also shown that depression is associated with upregulated inflammatory response, characterized by increased levels of pro-inflammatory cytokines and other acute-phase proteins 8.
Diets that promote inflammation are 1:
- High in Refined Starches or Refined Carbs,
- High in Sugar,
- High in Saturated and Trans-fats,
- High in Salt (sodium),
- Alcohol,
- Food Additives,
- Low in omega-3 fatty acids,
- Low in natural antioxidants,
- Low in fiber from fruits,
- Low in vegetables, and
- Low in whole grains.
Since the above list of diets cause inflammation, therefore the main dietary strategy to reduce inflammation should include adequate omega-3 fatty acids intake, reduction of saturated and trans-fats, and consumption of a diet high in fruits, vegetables, nuts, and whole grains and low in refined grains. The whole diet approach seems particularly promising to reduce the inflammation associated with the metabolic syndrome (e.g. high “bad” triglyceride, low “good” HDL cholesterol, belly fat, high blood pressure, high blood sugar/insulin resistance). The choice of healthy sources of carbohydrate, fat, and protein, associated with regular physical activity and avoidance of smoking, is critical to fighting the war against chronic disease. Western dietary patterns warm up inflammation, while healthy dietary patterns cool it down.
A low-fat diet (≤30% of total calories) is still considered by many physicians to be a healthy choice for both primary and secondary prevention of cardiovascular disease (coronary heart disease) 9. An unintended consequence of emphasizing low-fat diets may have been to promote unrestricted carbohydrate intake, which reduces high-density lipoprotein cholesterol (HDL “good” cholesterol) and raises triglyceride levels, exacerbating the metabolic manifestations of the insulin resistance syndrome, also known as the metabolic syndrome 10.
Three dietary strategies may help prevent coronary heart disease (coronary artery disease) 11:
- Increase consumption of omega-3 fatty acids from fish or plant sources;
- Substitute nonhydrogenated unsaturated fats for saturated and trans-fats; and
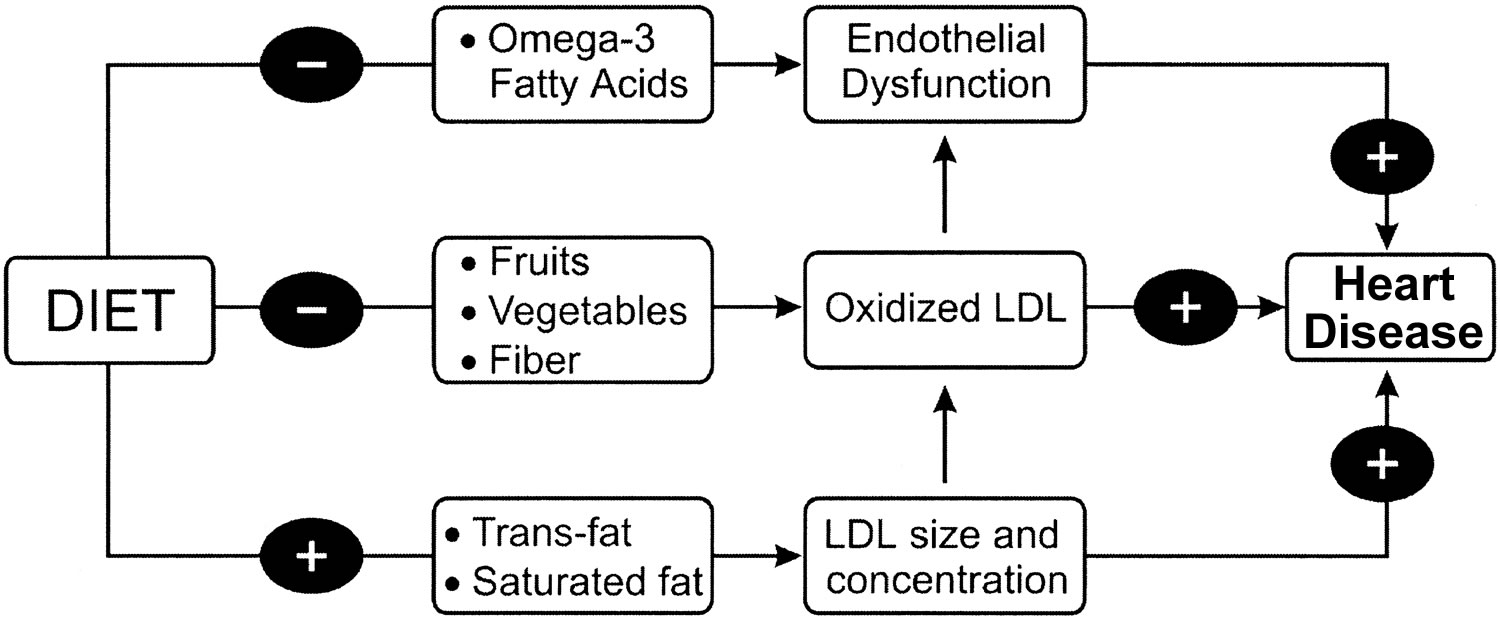
- Consume a diet high in fruits, vegetables, nuts, and whole grains and low in refined grains (see Figure 1).
The effects of diet on coronary heart disease (coronary artery disease) can be mediated through multiple biologic pathways other than serum lipids, including oxidative stress, subclinical inflammation, endothelial dysfunction, insulin sensitivity, blood pressure, and thrombotic tendency 12.
Figure 1. Mechanisms through which unhealthy dietary patterns may lead to coronary heart disease
LDL = low-density lipoprotein (“bad” cholesterol).
[Source 13]Various dietary components including long chain omega-3 fatty acids, antioxidant vitamins, plant flavonoids, prebiotics and probiotics have the potential to modulate predisposition to chronic inflammatory conditions. These components act through a variety of mechanisms including decreasing inflammatory mediator production through effects on cell signaling and gene expression (omega-3 fatty acids, vitamin E, plant flavonoids), reducing the production of damaging oxidants (vitamin E and other antioxidants), and promoting gut barrier function and anti-inflammatory responses (prebiotics and probiotics) 14. In a large Danish study 15 involving over 7000 men and women who were followed over 15 years (1982-1998). What that study found was that in both men and women who frequently consume wholemeal bread, vegetables, fruits, and fish, was associated with a better overall survival rate as well as better cardiovascular survival 15.
Endothelial dysfunction is one of the mechanisms linking diet and the risk of cardiovascular disease 16, 17. This study 18 suggests a mechanism for the role of dietary patterns in the pathogenesis of cardiovascular disease. For example, women in the Nurses’ Health Study who ate a “American” diet (high in red and processed meats, sweets, desserts, French fries, and refined grains) had higher proinflammatory cytokines (C-reactive protein, Interleukin-6, E-selectin, soluble vascular cell adhesion molecule 1 and soluble intercellular adhesion molecule 1) than those with the “healthier” pattern, characterized by higher intakes of fruit, vegetables, legumes, fish, poultry, and whole grains 18. The levels of these mediators amplify the inflammatory response, are destructive and contribute to the clinical symptoms 14.
Arachidonic acid (AA) derived (omega-6) eicosanoids (primarily from refined vegetable oils such as corn, sunflower, and safflower) increase the production of proinflammatory cytokines IL-1, TNF-α, and IL-6, operating as precursors of the proinflammatory eicosanoids of the prostaglandin (PG)2-series 19. In contrast, the omega-3 (n-3) polyunsaturated fatty acids (PUFAs), found in fish, fish oil, walnuts, wheat germ, and some dietary supplements such as flax seed products can curb the production of Arachidonic acid (AA)-derived eicosanoids 20. The Omega-6 and Omega-3 polyunsaturated fatty acids (PUFAs) compete for the same metabolic pathways, and thus their balance is important 21. Accordingly, it is not surprising that both higher levels of Omega-3 polyunsaturated fatty acids (PUFAs) as well as lower Omega-6:Omega-3 ratios are associated with lower proinflammatory cytokine production 22.
Furthermore, in another study a healthy dietary pattern rich in fruit, vegetables and olive oil, such as the Mediterranean diet, is associated with lower levels of inflammatory markers, perhaps because of the anti-inflammatory properties of antioxidants 1.
The antioxidant properties of vegetables and fruits are thought to be one of the fundamental mechanisms underlying their anti-inflammatory dietary contributions 1. Oxidants such as superoxide radicals or hydrogen peroxide that are produced during the metabolism of food can activate the NF-κB pathway, promoting inflammation 23. Higher fruit and vegetable intakes are associated with lower oxidative stress and inflammation 23. In fact, some evidence suggests that the addition of antioxidants or vegetables may limit or even reverse proinflammatory responses to meals high in saturated fat 24.
Whole grains are healthier than refined grains because the process of refining carbohydrates results in the elimination of much of the fiber, vitamins, minerals, phytonutrients, and essential fatty acids 1. Furthermore, refined starches and sugars can rapidly alter blood glucose and insulin levels 1 and postprandial hyperglycemia can increase production of free radicals as well as proinflammatory cytokines 25.
List of foods that cause inflammation
Dietary patterns high in refined starches, sugar, and saturated and trans-fatty acids, poor in natural antioxidants and fiber from fruits, vegetables, and whole grains, and poor in omega-3 fatty acids – aka the Average American Diet – may cause an activation of the innate immune system, most likely by an excessive production of proinflammatory cytokines associated with a reduced production of anti-inflammatory cytokines 13.
An Americanization of food habits has been recognized throughout the world, characterized by a high-energy diet, with increasing consumption of industrially processed foods. These foods usually contain large amounts of salt, simple sugars, saturated and trans fats, which food industries offer in response to consumers’ demands. Consequently, the intake of complex carbohydrates, fibres, fruits and vegetables has decreased. The energy and animal proteins consumed largely exceed World Health Organization recommendations, while, generally, a smaller variety of foods is being consumed.
- Most Americans exceed the recommendations for added sugars, saturated fats, and sodium. Most people say that if there is a healthy choice on a menu they will take it. But observations and research show this is generally not the case. Instead, people tend to make choices based on how food tastes. Typically, the more sugar, salt and fat in the food, the more we will like it.
- About three-fourths of the population has an eating pattern that is low in vegetables, fruits, dairy, and oils.
- More than half of the population is meeting or exceeding total grain and total protein foods recommendations, but, are not meeting the recommendations for the subgroups within each of these food groups.
The typical eating patterns currently consumed by many in the United States do not align with the Healthy Dietary Guidelines. As shown in Figure 2, when compared to the healthy eating pattern:
- About three-fourths of the population has an eating pattern that is low in vegetables, fruits, dairy, and oils.
- Most Americans exceed the recommendations for added sugars, saturated fats, and sodium.
Figure 2. The Average American Diet containing foods that can cause inflammation
In addition, the eating patterns of many are too high in calories. Calorie intake over time, in comparison to calorie needs, is best evaluated by measuring body weight status. The high percentage of the population that is overweight or obese suggests that many in the United States over consume calories. More than two-thirds of all adults and nearly one-third of all children and youth in the United States are either overweight or obese.
The typical American diet is about 50% carbohydrate, 15% protein, and 35% fat. The Standard American Diet or “Western-style” dietary patterns with more red meat or processed meat, sugared drinks, sweets, refined carbohydrates, or potatoes-have been linked to obesity 26, 27, 28, 29. The Average American (Western-style) dietary pattern is also linked to increased risk of heart disease, diabetes, and other chronic conditions.
Meal frequency and snacking have increased over the past 30 years in the U.S. 30 on average, children get 27 percent of their daily calories from snacks, primarily from desserts and sugary drinks, and increasingly from salty snacks and candy.
What Americans Eat: Top 10 sources of calories in the U.S. diet
- Grain-based desserts (cakes, cookies, donuts, pies, crisps, cobblers, and granola bars)
- Yeast breads
- Chicken and chicken-mixed dishes
- Soda, energy drinks, and sports drinks
- Pizza
- Alcoholic beverages
- Pasta and pasta dishes
- Mexican mixed dishes
- Beef and beef-mixed dishes
- Dairy desserts(Source: Report of the 2010 Dietary Guidelines Advisory Committee)
For the 20-30 year old the top sources of “Nutrition” are:
- Regular soft drinks 8.8% of total energy
- Pizza 5.1% of total energy
- Beer 3.9%
- Hamburgers and meat loaf 3.4%
- White bread 3.3%
- Cake, doughnuts and pastries 3.3%
- French fries and fried potatos 3.0%
- Potato chips, corn chips and popcorn 2.7%
- Rice 2.6%
- Cheese and cheese spread 2.5%
Vitamins and Micronutrients Deficiency (Americans):
- Vitamin D – 70% of Americans of deficient (food source: oil fish – salmon, trout, mackerel, sardines)
- Vitamin E – 60% of Americans of deficient
- Magnesium – 45% of Americans of deficient (food source: green vegetables)
- Vitamin K – 35% of Americans of deficient (food source: dark green vegetables)
- Calcium – 35% of Americans of deficient (food source: fortified ready-to-eat cereals, cheese)
- Vitamin A – 34% of Americans of deficient (food source: red or orange vegetables)
- Vitamin C – 25% of Americans of deficient
- Omega 3 – very high % of Americans of deficient (food source: oily fish)
- Zinc – 8% of Americans of deficient
The low intake of micronutrients result in insidious increased DNA damage, that over time leads to the acceleration of aged-associated diseases e.g. increased cancer.
Fast food is known for its large portions, low prices, high palatability, and high sugar content, and there’s evidence from studies in teens and adults that frequent fast-food consumption contributes to overeating and weight gain 31, 32, 33, 34, 35, 36. A study on the effect of fast-food consumption on risk of obesity and type 2 diabetes, for example, followed 3,000 young adults for 13 years. People who had higher fast-food-intake levels at the start of the study weighed an average of about 13 pounds more than people who had the lowest fast-food-intake levels. They also had larger waist circumferences and greater increases in triglycercides, and double the odds of developing metabolic syndrome 32.
Refined Starches or Refined Carbs
The process of refining a food not only removes the fiber, but it also removes much of the food’s nutritional value, including B-complex vitamins, healthy oils and fat-soluble vitamins. Refined carbohydrates are plant-based foods that have the whole grain extracted during processing, where the fibers, starches, vitamins and minerals have been removed, leaving behind refined carbohydrates. Refined carbohydrates sources include bottled fruit juices, juice concentrates, white bread, pastries, sodas, donuts, cakes, cookies, sweets, chips and other highly processed or refined foods. These items contain easily digested carbohydrates that may contribute to weight gain, interfere with weight loss, and promote diabetes and heart disease 37.
Refined carbohydrates are composed of sugars (such as fructose and glucose) which have simple chemical structures composed of only one sugar (monosaccharides) or two sugars (disaccharides). Simple carbohydrates are easily and quickly utilized for energy by the body because of their simple chemical structure, often leading to a faster rise in blood sugar and insulin secretion from the pancreas – which can have negative health effects.
When it comes to carbohydrates, what’s most important is the type of carbohydrate you choose to eat because some sources are healthier than others. The amount of carbohydrate in the diet – high or low – is less important than the type of carbohydrate in the diet. For example, healthy, whole grains such as whole wheat bread, rye, barley and quinoa are better choices than highly refined white bread or French fries. For example, whole grain whole wheat flour.
Typically, foods with highly processed refined carbohydrates (eg, white bread) are digested at a much faster rate and have higher glycemic index (high GI) values than do more compact granules (low-starch gelatinization) and high amounts of viscose soluble fiber (eg, barley, oats, and rye) foods. These refined carbohydrates are more rapidly attacked by digestive enzymes due to grinding or milling that reduces particle size and removes most of the bran and the germ. Numerous epidemiologic studies have found that higher intake of refined carbohydrates (reflected by increased dietary Glycemic Load) is associated with greater risk of type 2 diabetes and heart disease, whereas higher consumption of whole grains protects against these conditions 38.
Table 1. List of refined carbs for more than 100 common foods with their glycemic index and glycemic load, per serving.
| FOOD | Glycemic index (glucose = 100) | Serving size (grams) | Glycemic load per serving |
| BAKERY PRODUCTS AND BREADS | |||
| Banana cake, made with sugar | 47 | 60 | 14 |
| Banana cake, made without sugar | 55 | 60 | 12 |
| Sponge cake, plain | 46 | 63 | 17 |
| Vanilla cake made from packet mix with vanilla frosting (Betty Crocker) | 42 | 111 | 24 |
| Apple muffin, made with rolled oats and sugar | 44 | 60 | 13 |
| Apple muffin, made with rolled oats and without sugar | 48 | 60 | 9 |
| Waffles, Aunt Jemima® | 76 | 35 | 10 |
| Bagel, white, frozen | 72 | 70 | 25 |
| Baguette, white, plain | 95 | 30 | 14 |
| Coarse barley bread, 80% kernels | 34 | 30 | 7 |
| Hamburger bun | 61 | 30 | 9 |
| Kaiser roll | 73 | 30 | 12 |
| Pumpernickel bread | 56 | 30 | 7 |
| 50% cracked wheat kernel bread | 58 | 30 | 12 |
| White wheat flour bread, average | 75 | 30 | 11 |
| Wonder® bread, average | 73 | 30 | 10 |
| Whole wheat bread, average | 69 | 30 | 9 |
| 100% Whole Grain® bread (Natural Ovens) | 51 | 30 | 7 |
| Pita bread, white | 68 | 30 | 10 |
| Corn tortilla | 52 | 50 | 12 |
| Wheat tortilla | 30 | 50 | 8 |
| BEVERAGES | |||
| Coca Cola® (US formula) | 63 | 250 mL | 16 |
| Fanta®, orange soft drink | 68 | 250 mL | 23 |
| Lucozade®, original (sparkling glucose drink) | 95 | 250 mL | 40 |
| Apple juice, unsweetened | 41 | 250 mL | 12 |
| Cranberry juice cocktail (Ocean Spray®) | 68 | 250 mL | 24 |
| Gatorade, orange flavor (US formula) | 89 | 250 mL | 13 |
| Orange juice, unsweetened, average | 50 | 250 mL | 12 |
| Tomato juice, canned, no sugar added | 38 | 250 mL | 4 |
| BREAKFAST CEREALS AND RELATED PRODUCTS | |||
| All-Bran®, average | 44 | 30 | 9 |
| Coco Pops®, average | 77 | 30 | 20 |
| Cornflakes®, average | 81 | 30 | 20 |
| Cream of Wheat® | 66 | 250 | 17 |
| Cream of Wheat®, Instant | 74 | 250 | 22 |
| Grape-Nuts® | 75 | 30 | 16 |
| Muesli, average | 56 | 30 | 10 |
| Oatmeal, average | 55 | 250 | 13 |
| Instant oatmeal, average | 79 | 250 | 21 |
| Puffed wheat cereal | 80 | 30 | 17 |
| Raisin Bran® | 61 | 30 | 12 |
| Special K® (US formula) | 69 | 30 | 14 |
| GRAINS | |||
| Pearled barley, average | 25 | 150 | 11 |
| Sweet corn on the cob | 48 | 60 | 14 |
| Couscous | 65 | 150 | 9 |
| Quinoa | 53 | 150 | 13 |
| White rice, boiled, type non-specified | 72 | 150 | 29 |
| Quick cooking white basmati | 63 | 150 | 26 |
| Brown rice, steamed | 50 | 150 | 16 |
| Parboiled Converted white rice (Uncle Ben’s®) | 38 | 150 | 14 |
| Whole wheat kernels, average | 45 | 50 | 15 |
| Bulgur, average | 47 | 150 | 12 |
| COOKIES AND CRACKERS | |||
| Graham crackers | 74 | 25 | 13 |
| Vanilla wafers | 77 | 25 | 14 |
| Shortbread | 64 | 25 | 10 |
| Rice cakes, average | 82 | 25 | 17 |
| Rye crisps, average | 64 | 25 | 11 |
| Soda crackers | 74 | 25 | 12 |
| DAIRY PRODUCTS AND ALTERNATIVES | |||
| Ice cream, regular, average | 62 | 50 | 8 |
| Ice cream, premium (Sara Lee®) | 38 | 50 | 3 |
| Milk, full-fat, average | 31 | 250 mL | 4 |
| Milk, skim, average | 31 | 250 mL | 4 |
| Reduced-fat yogurt with fruit, average | 33 | 200 | 11 |
| FRUITS | |||
| Apple, average | 36 | 120 | 5 |
| Banana, raw, average | 48 | 120 | 11 |
| Dates, dried, average | 42 | 60 | 18 |
| Grapefruit | 25 | 120 | 3 |
| Grapes, black | 59 | 120 | 11 |
| Oranges, raw, average | 45 | 120 | 5 |
| Peach, average | 42 | 120 | 5 |
| Peach, canned in light syrup | 52 | 120 | 9 |
| Pear, raw, average | 38 | 120 | 4 |
| Pear, canned in pear juice | 44 | 120 | 5 |
| Prunes, pitted | 29 | 60 | 10 |
| Raisins | 64 | 60 | 28 |
| Watermelon | 72 | 120 | 4 |
| BEANS AND NUTS | |||
| Baked beans | 40 | 150 | 6 |
| Black-eyed peas | 50 | 150 | 15 |
| Black beans | 30 | 150 | 7 |
| Chickpeas | 10 | 150 | 3 |
| Chickpeas, canned in brine | 42 | 150 | 9 |
| Navy beans, average | 39 | 150 | 12 |
| Kidney beans, average | 34 | 150 | 9 |
| Lentils | 28 | 150 | 5 |
| Soy beans, average | 15 | 150 | 1 |
| Cashews, salted | 22 | 50 | 3 |
| Peanuts | 13 | 50 | 1 |
| PASTA and NOODLES | |||
| Fettucini | 32 | 180 | 15 |
| Macaroni, average | 50 | 180 | 24 |
| Macaroni and Cheese (Kraft®) | 64 | 180 | 33 |
| Spaghetti, white, boiled, average | 46 | 180 | 22 |
| Spaghetti, white, boiled 20 min | 58 | 180 | 26 |
| Spaghetti, whole-grain, boiled | 42 | 180 | 17 |
| SNACK FOODS | |||
| Corn chips, plain, salted | 42 | 50 | 11 |
| Fruit Roll-Ups® | 99 | 30 | 24 |
| M & M’s®, peanut | 33 | 30 | 6 |
| Microwave popcorn, plain, average | 65 | 20 | 7 |
| Potato chips, average | 56 | 50 | 12 |
| Pretzels, oven-baked | 83 | 30 | 16 |
| Snickers Bar®, average | 51 | 60 | 18 |
| VEGETABLES | |||
| Green peas | 54 | 80 | 4 |
| Carrots, average | 39 | 80 | 2 |
| Parsnips | 52 | 80 | 4 |
| Baked russet potato | 111 | 150 | 33 |
| Boiled white potato, average | 82 | 150 | 21 |
| Instant mashed potato, average | 87 | 150 | 17 |
| Sweet potato, average | 70 | 150 | 22 |
| Yam, average | 54 | 150 | 20 |
| MISCELLANEOUS | |||
| Hummus (chickpea salad dip) | 6 | 30 | 0 |
| Chicken nuggets, frozen, reheated in microwave oven 5 min | 46 | 100 | 7 |
| Pizza, plain baked dough, served with parmesan cheese and tomato sauce | 80 | 100 | 22 |
| Pizza, Super Supreme (Pizza Hut®) | 36 | 100 | 9 |
| Honey, average | 61 | 25 | 12 |
The complete list of the glycemic index and glycemic load for more than 1,000 foods can be found in the article “International tables of glycemic index and glycemic load values: 2008” by Fiona S. Atkinson, Kaye Foster-Powell, and Jennie C. Brand-Miller in the December 2008 issue of Diabetes Care, Vol. 31, number 12, pages 2281-2283 39.
Examples of refined carbs
Refined Breads
Many of the breads found on grocery store shelves are considered refined carbohydrates. These breads are often made from enriched and bleached flours, and these flours are typically listed as the first or second ingredient on the nutrition label. In addition, the list of ingredients will often include vitamins and minerals that are added during the post-refining, enrichment process. Sourdough, white and plain wheat bread are excellent examples of refined breads, whereas 100 percent whole-wheat or whole-grain breads are not refined.
Refined Rice
Like bread, some forms of rice are considered to be refined grains. White rice and most of the quick-cook rices are refined and, as a result, do not contain an intact grain. They may be enriched to enhance their nutritional profile, but they typically lack the fiber found in the non-refined brown rice. One cup of white rice counts as 2 ounces of refined grains.
Refined Cereals
Many of the sugary, cold cereals found in grocery stores are considered to be refined grains. They are typically made from enriched flour due to the refining of their original wheat, corn or oat grain. Refined cereals typically have 2 or fewer grams of fiber per serving, and one cup of a refined cereal, such as corn flakes, counts as 1 ounce of refined grains.
Refined Pasta
Unlike whole wheat or whole grain pasta, refined pasta lacks much of the fiber and the B-complex vitamins found in the unprocessed version. Like other processed starches, refined pasta may be enriched with nutrients such as folate, thiamin and riboflavin, and some versions of refined pasta may even have omega 3 fatty acids added during processing. Thus, if you prefer the less grainy taste of refined pasta, make sure that it has been fully enriched with the aforementioned nutrients.
Refined Snack Foods
Snack foods are typically made with refined carbs such as bleached flours and sugar in order to increase palatability. These snack foods have little nutritional value and, as a result, provide empty calories in the diet. Cakes, cookies, pie, candy and chips are all examples of refined snack foods, and according to the U.S. Department of Agriculture, these foods should not constitute more than 120 to 330 calories per day.
List of refined carbs
Any foods that have been processed for quick consumption.
- Foods made with refined or “white” flour also contain less fiber and protein than whole-grain products.
- Snacks, such as crisps, sausage rolls, pies and pasties
- Granola bars
- Ice cream
- Donuts
- Cakes
- Twinkies
- Pastries
- Canned fruits with added sugar or syrup
- Sweets
- Fruit drinks
- Colas and carbonated sweetened beverages
- Energy drinks
- Sports drink
- Jams
- Crackers
- Dressings
- Sauces
- Cookies
- Fruit chews
- Pizzas
- Apple pies
- Anything with added sugar.
Sugar by Any Other Name
You don’t always see the word “sugar” on a food label. It sometimes goes by another name, like these:
- White sugar
- Brown sugar
- Raw sugar
- Agave nectar
- Brown rice syrup
- Corn syrup
- Corn syrup solids
- Coconut sugar
- Coconut palm sugar
- High-fructose corn syrup
- Invert sugar
- Dextrose
- Anhydrous dextrose
- Crystal dextrose
- Dextrin
- Evaporated cane juice
- Fructose sweetener
- Liquid fructose
- Glucose
- Lactose
- Honey
- Malt syrup
- Maple syrup
- Molasses
- Pancake syrup
- Sucrose
- Trehalose
- Turbinado sugar
Watch out for items that list any form of sugar in the first few ingredients.
Food Additives
“Food additive” is defined by the Food and Drug Administration (FDA) as “Everything Added to Food in the United States” 40. In its broadest sense, a food additive is any substance added to food. Legally, the term refers to “any substance the intended use of which results or may reasonably be expected to result — directly or indirectly — in its becoming a component or otherwise affecting the characteristics of any food” 40. This definition includes any substance used in the production, processing, treatment, packaging, transportation or storage of food 40. Therefore, this definition excludes ingredients whose use is generally recognized as safe (where government approval is not needed), those ingredients approved for use by FDA or the U.S. Department of Agriculture (USDA) prior to the food additives provisions of law, and color additives and pesticides where other legal premarket approval requirements apply. This definition includes any substance used in the production, processing, treatment, packaging, transportation or storage of food, many of which we use at home every day (e.g., sugar, baking soda, salt, vanilla, yeast, spices and colors). Additives are used to maintain or improve safety, freshness, nutritional value taste, texture and appearance. The use of food additives has become more prominent in recent years due to the increased production of prepared, processed, and convenience foods. Today more than 3000 substances are used as food additives 40. Salt, sugar, and corn syrup are by far the most widely used additives in food in this country.
According to the FDA, “Direct food additives are those that are added to a food for a specific purpose in that food” 40. For example, xanthan gum — used in salad dressings, chocolate milk, bakery fillings, puddings and other foods to add texture. Or using phosphates in meat and poultry products to retain moisture and protect the flavor. Most direct additives are identified on the ingredient label of foods.
“Indirect food additives are those that become part of the food in trace amounts due to its packaging, storage or other handling,” according to the FDA 40. For instance, minute amounts of packaging substances may find their way into foods during storage. Food packaging manufacturers must prove to the FDA that all materials coming in contact with food are safe before they are permitted for use in such a manner.
FDA defines a color additive as any dye, pigment, or substance which—when added or applied to a food, drug, or cosmetic, or to the human body—is capable (alone or through reactions with other substances) of imparting color. FDA is responsible for regulating all color additives to ensure that foods containing color additives are safe to eat, contain only approved ingredients, and are accurately labeled.
A color additive is any dye, pigment or substance which when added or applied to a food, drug or cosmetic, or to the human body, is capable (alone or through reactions with other substances) of imparting color 40. FDA is responsible for regulating all color additives to ensure that foods containing color additives are safe to eat, contain only approved ingredients and are accurately labeled.
Color additives are used in foods for many reasons: 1) to offset color loss due to exposure to light, air, temperature extremes, moisture and storage conditions; 2) to correct natural variations in color; 3) to enhance colors that occur naturally; and 4) to provide color to colorless and “fun” foods. Without color additives, colas wouldn’t be brown, margarine wouldn’t be yellow and mint ice cream wouldn’t be green. Color additives are now recognized as an important part of practically all processed foods we eat.
FDA’s permitted colors are classified as subject to certification or exempt from certification, both of which are subject to rigorous safety standards prior to their approval and listing for use in foods.
- Certified colors are synthetically produced (or human made) and used widely because they impart an intense, uniform color, are less expensive, and blend more easily to create a variety of hues. There are nine certified color additives approved for use in the United States (e.g., FD&C Yellow No. 6. See chart for complete list.). Certified food colors generally do not add undesirable flavors to foods.
- Colors that are exempt from certification include pigments derived from natural sources such as vegetables, minerals or animals. Nature derived color additives are typically more expensive than certified colors and may add unintended flavors to foods. Examples of exempt colors include annatto extract (yellow), dehydrated beets (bluish-red to brown), caramel (yellow to tan), beta-carotene (yellow to orange) and grape skin extract (red, green).
For a complete discussion on food additives and food coloring go to our other posts:
- The effects of diet on inflammation: emphasis on the metabolic syndrome. Giugliano D, Ceriello A, Esposito K. J Am Coll Cardiol. 2006 Aug 15; 48(4):677-85. https://www.ncbi.nlm.nih.gov/pubmed/16904534/[↩][↩][↩][↩][↩][↩][↩]
- Inflammation and cancer: how hot is the link ? Aggarwal BB, Shishodia S, Sandur SK, Pandey MK, Sethi G. Biochem Pharmacol. 2006 Nov 30; 72(11):1605-21. https://www.ncbi.nlm.nih.gov/pubmed/16889756/[↩]
- Health effects of trans-fatty acids: experimental and observational evidence. Mozaffarian D, Aro A, Willett WC. Eur J Clin Nutr. 2009 May; 63 Suppl 2():S5-21. https://www.ncbi.nlm.nih.gov/pubmed/19424218/[↩]
- Kiecolt-Glaser JK. Stress, Food, and Inflammation: Psychoneuroimmunology and Nutrition at the Cutting Edge. Psychosomatic medicine. 2010;72(4):365-369. doi:10.1097/PSY.0b013e3181dbf489. https://www.ncbi.nlm.nih.gov/pmc/articles/PMC2868080/[↩]
- Plasma concentration of interleukin-6 and the risk of future myocardial infarction among apparently healthy men. Circulation, 101 (2000), pp. 1767-1772.[↩]
- Elevation of tumor necrosis factor-alpha and increased risk of recurrent coronary events after myocardial infarction. Circulation, 101 (2000), pp. 2149-2153.[↩]
- Interleukin-18 is a strong predictor of cardiovascular death in stable and unstable angina. Circulation, 106 (2002), pp. 24-30.[↩]
- Associations of depression with C-reactive protein, IL-1, and IL-6: a meta-analysis. Howren MB, Lamkin DM, Suls J. Psychosom Med. 2009 Feb; 71(2):171-86. https://www.ncbi.nlm.nih.gov/pubmed/19188531/[↩]
- Diets and cardiovascular disease. An evidence-based assessment. J Am Coll Cardiol, 45 (2005), pp. 1379-1387.[↩]
- The diet-heart hypothesis: a critique. J Am Coll Cardiol, 43 (2004), pp. 731-733.[↩]
- Optimal diets for prevention of coronary heart disease. JAMA, 288 (2002), pp. 2569-2578.[↩]
- Diet, nutrition, and coronary heart disease. P.S. Douglas (Ed.), Cardiovascular Health and Disease in Women (2nd edition.), WB Saunders, Philadelphia, PA (2002), pp. 71-92.[↩]
- The Effects of Diet on Inflammation: Emphasis on the Metabolic Syndrome. Journal of the American College of Cardiology Volume 48, Issue 4, 15 August 2006, Pages 677-685. http://www.sciencedirect.com/science/article/pii/S0735109706013350[↩][↩]
- Inflammatory disease processes and interactions with nutrition. Br J Nutr. 2009 May;101 Suppl 1:S1-45. doi: 10.1017/S0007114509377867. https://www.ncbi.nlm.nih.gov/pubmed/19586558/[↩][↩]
- Dietary patterns and mortality in Danish men and women: a prospective observational study. British Journal of Nutrition (2001), 85, 219-225. DOI: 10.1079/BJN2000240. https://www.cambridge.org/core/services/aop-cambridge-core/content/view/2C582B42A8FEC3F37A7EEE62875078B1/S0007114501000307a.pdf[↩][↩]
- Ross R. Atherosclerosis, an inflammatory disease. N Engl J Med 1999;340:115-26. https://www.ncbi.nlm.nih.gov/pubmed/9887164[↩]
- Brown AA, Hu FB. Dietary modulation of endothelial function: implications for cardiovascular disease. Am J Clin Nutr 2001;73:673-86. http://ajcn.nutrition.org/content/73/4/673.full[↩]
- Major dietary patterns are related to plasma concentrations of markers of inflammation and endothelial dysfunction. Lopez-Garcia E, Schulze MB, Fung TT, Meigs JB, Rifai N, Manson JE, Hu FB. Am J Clin Nutr. 2004 Oct; 80(4):1029-35. http://ajcn.nutrition.org/content/80/4/1029.long[↩][↩]
- In humans, serum polyunsaturated fatty acid levels predict the response of proinflammatory cytokines to psychologic stress. Maes M, Christophe A, Bosmans E, Lin A, Neels H. Biol Psychiatry. 2000 May 15; 47(10):910-20. https://www.ncbi.nlm.nih.gov/pubmed/10807964/[↩]
- Habitual dietary intake of n-3 and n-6 fatty acids in relation to inflammatory markers among US men and women. Pischon T, Hankinson SE, Hotamisligil GS, Rifai N, Willett WC, Rimm EB. Circulation. 2003 Jul 15; 108(2):155-60. http://circ.ahajournals.org/content/108/2/155.long[↩]
- Depressive symptoms, omega-6:omega-3 fatty acids, and inflammation in older adults. Kiecolt-Glaser JK, Belury MA, Porter K, Beversdorf DQ, Lemeshow S, Glaser R. Psychosom Med. 2007 Apr; 69(3):217-24. https://www.ncbi.nlm.nih.gov/pmc/articles/PMC2856352/[↩]
- Relationship of plasma polyunsaturated fatty acids to circulating inflammatory markers. Ferrucci L, Cherubini A, Bandinelli S, Bartali B, Corsi A, Lauretani F, Martin A, Andres-Lacueva C, Senin U, Guralnik JM. J Clin Endocrinol Metab. 2006 Feb; 91(2):439-46. https://www.ncbi.nlm.nih.gov/pubmed/16234304/[↩]
- Inflammatory disease processes and interactions with nutrition. Calder PC, Albers R, Antoine JM, Blum S, Bourdet-Sicard R, Ferns GA, Folkerts G, Friedmann PS, Frost GS, Guarner F, Løvik M, Macfarlane S, Meyer PD, M’Rabet L, Serafini M, van Eden W, van Loo J, Vas Dias W, Vidry S, Winklhofer-Roob BM, Zhao J. Br J Nutr. 2009 May; 101 Suppl 1():S1-45. https://www.ncbi.nlm.nih.gov/pubmed/19586558/[↩][↩]
- Effect of dietary antioxidants on postprandial endothelial dysfunction induced by a high-fat meal in healthy subjects. Esposito K, Nappo F, Giugliano F, Giugliano G, Marfella R, Giugliano D. Am J Clin Nutr. 2003 Jan; 77(1):139-43. http://ajcn.nutrition.org/content/77/1/139.long[↩]
- Inflammatory cytokine concentrations are acutely increased by hyperglycemia in humans: role of oxidative stress. Esposito K, Nappo F, Marfella R, Giugliano G, Giugliano F, Ciotola M, Quagliaro L, Ceriello A, Giugliano D. Circulation. 2002 Oct 15; 106(16):2067-72. http://circ.ahajournals.org/content/106/16/2067.long[↩]
- Schulze MB, Fung TT, Manson JE, Willett WC, Hu FB. Dietary patterns and changes in body weight in women. Obesity (Silver Spring). 2006;14:1444-53. https://www.ncbi.nlm.nih.gov/pubmed/16988088[↩]
- Newby PK, Muller D, Hallfrisch J, Andres R, Tucker KL. Food patterns measured by factor analysis and anthropometric changes in adults. Am J Clin Nutr. 2004;80:504-13. https://www.ncbi.nlm.nih.gov/pubmed/15277177[↩]
- Schulz M, Nothlings U, Hoffmann K, Bergmann MM, Boeing H. Identification of a food pattern characterized by high-fiber and low-fat food choices associated with low prospective weight change in the EPIC-Potsdam cohort. J Nutr. 2005;135:1183-9. https://www.ncbi.nlm.nih.gov/pubmed/15867301[↩]
- Newby PK, Muller D, Hallfrisch J, Qiao N, Andres R, Tucker KL. Dietary patterns and changes in body mass index and waist circumference in adults. Am J Clin Nutr. 2003;77:1417-25. https://www.ncbi.nlm.nih.gov/pubmed/12791618[↩]
- Popkin BM, Duffey KJ. Does hunger and satiety drive eating anymore? Increasing eating occasions and decreasing time between eating occasions in the United States. Am J Clin Nutr. 2010;91:1342-7. https://www.ncbi.nlm.nih.gov/pubmed/20237134[↩]
- Duffey KJ, Gordon-Larsen P, Jacobs DR, Jr., Williams OD, Popkin BM. Differential associations of fast food and restaurant food consumption with 3-y change in body mass index: the Coronary Artery Risk Development in Young Adults Study. Am J Clin Nutr. 2007;85:201-8. https://www.ncbi.nlm.nih.gov/pubmed/17209197[↩]
- Duffey KJ, Gordon-Larsen P, Steffen LM, Jacobs DR, Jr., Popkin BM. Regular consumption from fast food establishments relative to other restaurants is differentially associated with metabolic outcomes in young adults. J Nutr. 2009;139:2113-8. https://www.ncbi.nlm.nih.gov/pubmed/19776183[↩][↩]
- Taveras EM, Berkey CS, Rifas-Shiman SL, et al. Association of consumption of fried food away from home with body mass index and diet quality in older children and adolescents. Pediatrics. 2005;116:e518-24. https://www.ncbi.nlm.nih.gov/pubmed/16199680[↩]
- French SA, Harnack L, Jeffery RW. Fast food restaurant use among women in the Pound of Prevention study: dietary, behavioral and demographic correlates. Int J Obes Relat Metab Disord. 2000;24:1353-9. https://www.ncbi.nlm.nih.gov/pubmed/11093299[↩]
- Pereira MA, Kartashov AI, Ebbeling CB, et al. Fast-food habits, weight gain, and insulin resistance (the CARDIA study): 15-year prospective analysis. Lancet. 2005;365:36-42. www.ncbi.nlm.nih.gov/pubmed/15639678[↩]
- Rosenheck R. Fast food consumption and increased caloric intake: a systematic review of a trajectory towards weight gain and obesity risk. Obes Rev. 2008;9:535-47. https://www.ncbi.nlm.nih.gov/pubmed/18346099[↩]
- Harvard University, Harvard School of Public Health. Carbohydrates. https://www.hsph.harvard.edu/nutritionsource/carbohydrates/[↩]
- Optimal diets for prevention of coronary heart disease. Hu FB, Willett WC. JAMA. 2002 Nov 27; 288(20):2569-78. https://www.ncbi.nlm.nih.gov/pubmed/12444864/[↩]
- Diabetes Care 2008 Dec; 31(12): 2281-2283. https://doi.org/10.2337/dc08-1239. International Tables of Glycemic Index and Glycemic Load Values: 2008. http://care.diabetesjournals.org/content/31/12/2281.full[↩]
- Overview of Food Ingredients, Additives & Colors. U.S. Food and Drug Administration. https://www.fda.gov/Food/IngredientsPackagingLabeling/FoodAdditivesIngredients/ucm094211.htm[↩][↩][↩][↩][↩][↩][↩]