Contents
What is an insulin pump
An insulin pump is a small battery-operated electronic device (computerized syringe) about the size of a mobile phone that delivers tiny amounts of fast acting insulin into the blood throughout the day and night. An insulin pump is worn 24 hours a day. Research has shown that insulin pump therapy can reduce the frequency of severe hypoglycaemia as well as improve quality of life. Using an insulin pump may also improve suboptimal blood glucose control. Only fast acting insulin is used in the insulin pump. Whenever food is eaten the insulin pump is programmed to deliver a surge of insulin into the body similar to the way the pancreas does in people without diabetes. Between meals a small and steady rate of insulin is delivered.
Insulin pumps can deliver insulin in two ways:
- In a steady measured and continuous dose (the “basal” insulin)
- As a surge (“bolus”) dose, at your direction, around mealtime.
The insulin pump is not an artificial pancreas (because you still have to monitor your blood glucose level), but pumps can help some people achieve better control, and many people prefer this continuous system of insulin delivery over injections.
Insulin pump therapy may especially be of assistance if any of the following applies to you:
- hypoglycemia unawareness (inability to detect ‘hypos’)
- severe and frequent hypoglycemia
- frequent night time hypoglycemia
- gastroparesis (delayed emptying of the stomach)
- an unpredictable lifestyle or daily routine (e.g. working nightshifts)
- extreme insulin sensitivity
- dawn phenomenon (rising blood glucose early in the morning)
- planning for, and during, pregnancy.
Pumps can be programmed to releases small doses of insulin continuously (basal), or a bolus dose close to mealtime to control the rise in blood glucose after a meal. This delivery system most closely mimics the body’s normal release of insulin.
Using an insulin pump may:
- reduce large fluctuations in blood glucose levels
- improve blood glucose (diabetes) levels
- increase your flexibility in the quantity and timing of meals
- decrease your risk of hypoglycemia during exercise while maintaining optimal blood glucose levels
- improve your quality of life.
You attach the insulin pump to your skin. Insulin flows into your body through a tiny flexible plastic tube called a catheter under your skin. With the aid of a small needle, the catheter is inserted through the skin into the fatty tissue and is taped in place. The tube (catheter) is replaced every 2 to 3 days and the insulin pump moved to another part of your body.
An insulin pump delivers a set amount of background insulin. You then add your extra mealtime insulin using the pump.
An insulin pump can give you more flexibility with what you eat and help you have more stable blood glucose levels. However, a pump might not suit everyone.
You’ll want to check with your insurance carrier before you buy a pump and supplies. Most carriers cover these, but some don’t.
Disadvantages of using a diabetes insulin pump
Although there are many good reasons as to why using an insulin pump can be an advantage, there are some disadvantages.
The disadvantages of using an insulin pump are that it:
- Can cause weight gain
- Can cause diabetic ketoacidosis (DKA) if your catheter comes out and you don’t get insulin for hours
- Can be expensive
- Can be bothersome since you are attached to the pump most of the time
- Can require a hospital stay or maybe a full day in the outpatient center to be trained
There are pluses and minuses to using an insulin pump. Even though using an insulin pump has disadvantages, most pump users agree the advantages outweigh the disadvantages.
Advantages of using a diabetes insulin pump
Some advantages of using an insulin pump instead of insulin injections are:
- Using an insulin pump means eliminating individual insulin injections
- Insulin pumps deliver insulin more accurately than injections
- Insulin pumps often improve HbA1C. HbA1c is a measure of long-term blood glucose levels. Research investigating the efficacy of insulin pump therapy in relation to blood glucose levels suggests that it can improve HbA1c, especially in those with an elevated HbA1c and in those who have been unable to reduce their HbA1c with multiple daily injections.
- Using an insulin pump usually results in fewer large swings in your blood glucose levels
- Using an insulin pump makes delivery of bolus insulin easier
- Insulin pumps allow you to be flexible about when and what you eat
- Using an insulin pump reduces severe low blood glucose episodes
- Using an insulin pump eliminates unpredictable effects of intermediate- or long-acting insulin
- Insulin pumps allow you to exercise without having to eat large amounts of carbohydrate
It is important that you have realistic expectations about insulin pump therapy. It is not a cure for people who require insulin to manage their diabetes but a way of delivering insulin that may offer increased flexibility, improved glucose levels and improved quality of life.
Insulin pump therapy requires motivation, regular blood glucose checking, the ability to learn insulin pump technology and the willingness to keep in regular contact with your diabetes educator or endocrinologist for review and adjustment of pump rates.
What does an insulin pump look like
If you have been diagnosed with diabetes, you may feel overwhelmed by all the new information you have learned and will continue to learn about managing your diabetes.
You already know your main goal should be to get your blood glucose (sugar) levels under control in order to increase your chances of a complication-free life. Many people know this, but need to know how to achieve good diabetes management, while balancing the day-to-day demands of diabetes with other life demands.
An insulin pump can help you manage your diabetes. By using an insulin pump, you can match your insulin to your lifestyle, rather than getting an insulin injection and matching your life to how the insulin is working.
When you work closely with your diabetes care team, insulin pumps can help you keep your blood glucose levels within your target ranges.
People of all ages with type 1 diabetes use insulin pumps and people with type 2 diabetes have started to use them as well.
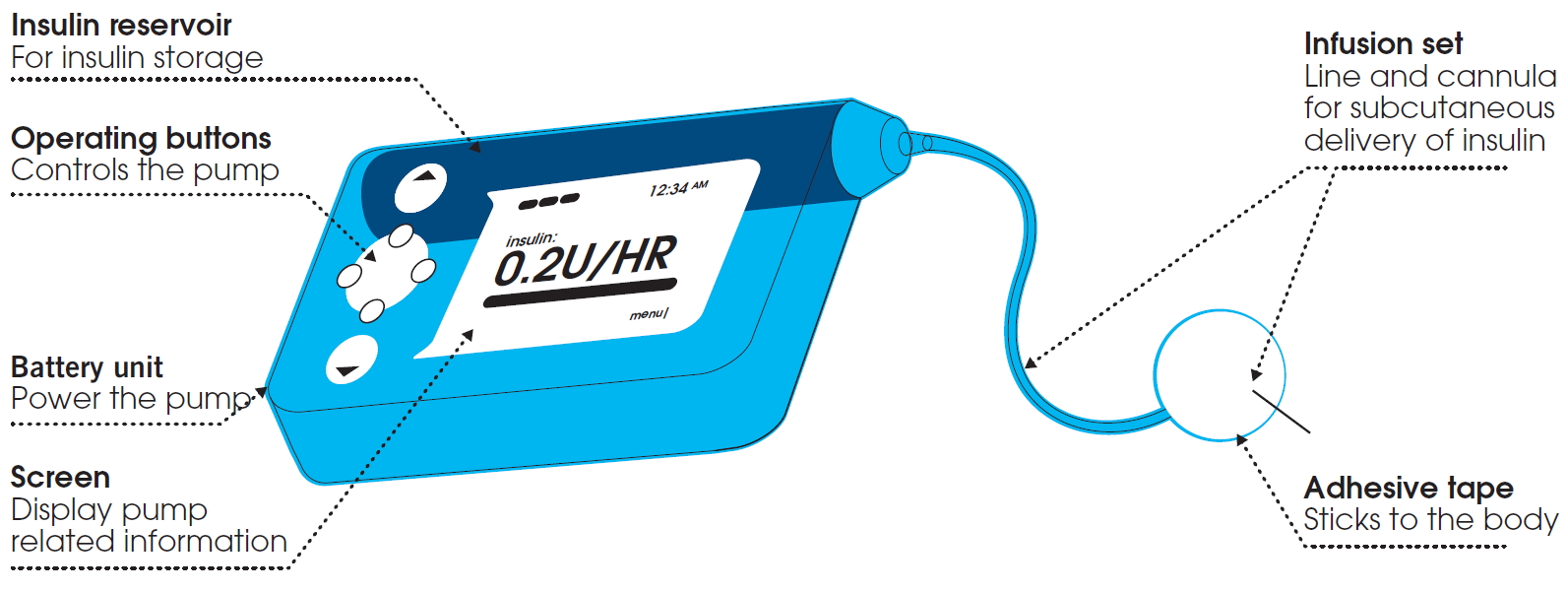
Figure 1. Insulin pump
How does an insulin pump work
An insulin pump can provide all the insulin requirements of a person with type 1 diabetes.
The pump contains a reservoir or cartridge filled with insulin. A microcomputer built into the pump allows you to program the pump to deliver a dose of insulin according to your needs. A small motor inside the pump controls the delivery of insulin. Insulin is delivered from the reservoir/cartridge through flexible tubing fitted with a small Teflon® (or metal) cannula that is inserted subcutaneously (under the skin) and held in place with special adhesive tape. Together, the tubing and cannula are called an infusion set. The cannula is easily inserted and removed by you; it is not surgically implanted. An introducer needle allows the cannula to be inserted under the skin. The needle is then removed leaving behind the cannula only. For those who do not want to insert the needles manually, there are disposable and reusable devices to assist with cannula insertion.
The cannula must be changed every two to three days. Metal cannulas may need to be changed every one to two days. The most common site to place infusion sets is in the abdomen (easy to access) but they can also be placed in the upper buttock, upper outer thigh, hip or upper arm.
Insulin pumps deliver rapid- or short-acting insulin 24 hours a day through a catheter placed under the skin. Your insulin doses are separated into:
- Basal rates
- Bolus doses to cover carbohydrate in meals
- Correction or supplemental doses
Basal insulin is delivered continuously over 24 hours, and keeps your blood glucose levels in range between meals and overnight. It delivers the insulin in two ways (basal and bolus), therefore replacing the need for long-acting insulin. Often, you program different amounts of insulin at different times of the day and night. An insulin pump delivers rapid-acting insulin such as NovoRapid® and Humalog®. This insulin starts working within 10 to 15 minutes of delivery, peaks within one to three hours and ceases working after three to five hours. A lack of insulin can lead to the rapid development of ketones and diabetic ketoacidosis (DKA) which is a life-threatening condition. For this reason, it is important to never disconnect from the pump for more than two hours without using an alternative method of insulin delivery (e.g. insulin injections) and to regularly check that the pump is delivering insulin. Prompt attention to rising blood glucose levels is essential in order to prevent diabetic ketoacidosis (DKA).
- It is vital that people using insulin pumps monitor their blood glucose at least four times a day, preferably six times a day.
- Check your blood glucose level at least 8–10 times a day when you start using a pump. When blood glucose levels are stabilized, a minimum of four checks a day (before each meal) are needed so that you can program your pump to deliver the appropriate amount of insulin you need according to your blood glucose levels.
- Learn to:
- count carbohydrates and get lots of practice, preferably well before you start on a pump
- adjust your insulin rates according to blood glucose level patterns and trends
- adjust your insulin doses or rates according to activity levels, ketones or sick days.
- Respond quickly when blood glucose levels show hyperglycaemia (high blood glucose level) and/or if ketones are present in the blood. Long acting insulin is not used in a pump so if there are any technical problems with the pump or the
infusion set, blood glucose levels can rise very quickly, increasing your risk of diabetic ketoacidosis. - In the future, it is hoped that blood glucose sensors will ‘talk’ to the pump and automatically adjust insulin doses as required.
When you eat, you use buttons on the insulin pump to give additional insulin called a bolus. You take a bolus to cover the carbohydrate in each meal or snack. If you eat more than you planned, you can simply program a larger bolus of insulin to cover it.
You also take a bolus to treat high blood glucose levels. If you have high blood glucose levels before you eat, you give a correction or supplemental bolus of insulin to bring it back to your target range.
Approximately half of your daily dose of insulin is spread across 24 hours (basal rate), so the hourly rate of insulin given is very small. The remainder of your daily dose is given as bolus doses at meal and snack times and to correct high blood glucose levels. These bolus doses can be smaller than those given with injections because the insulin is more reliably absorbed.
Most insulin pump will calculate the insulin dose for each meal or snack based on the insulin to carbohydrate ratio programmed into the pump. This ratio is calculated with your diabetes educator or endocrinologist. You need to know the carbohydrate content of the meal or snack you intend to eat so that you can enter the amount of carbohydrate into the pump. The insulin pump will calculate the insulin dose required for the meal. ‘Smart pumps’ can also add a correctional bolus of insulin at this time if your pre-meal blood glucose level is out of the target range.
Although it is possible to rely on a ‘smart pump’ to calculate the insulin dose required, it is important that the insulin pump user understands the basis of the calculation so that the dose recommended by the insulin pump can be verified.
Insulin pumps and continuous glucose monitoring systems
There have been significant advances in the development of continuous glucose monitoring systems in recent times. Continuous glucose monitoring systems is a means of measuring glucose levels continuously in order to gain insight into patterns and trends in glucose levels throughout the day and night. A continuous glucose monitoring systems sensor is worn separately to the pump, inserted under the skin, and measures the level of glucose in the interstitial fluid (fluid in the tissue). The sensor is disposable and changed according to manufacturer recommendations.
Whilst continuous glucose monitoring systems sensor readings provide excellent information regarding glucose trends and patterns, they are an indication only and should never be used to calculate a dose of insulin. Normal blood glucose checks must still be done, both to calibrate the device and prior to administering a dose of insulin. The blood check results are used to calibrate the sensor to help maintain accuracy. Sensors need to be changed every five to seven days.
Basal Insulin
Insulin pumps provide a constant infusion of rapid-acting insulin (called a basal rate) to control blood glucose levels throughout the day.
The basal insulin is the insulin that your body needs continuously for normal metabolism. It maintains stable blood glucose in the absence of food. The diabetes insulin pump delivers insulin automatically and continuously (at individually-set intervals; commonly this is every three minutes), 24 hours a day. The rate of delivery (basal rate) is programmed in units per hour and adjusted according to your needs. This rate is initially calculated by your diabetes educator or endocrinologist. In time, with the support of your diabetes care team, you will learn to make adjustments to your own rates according to the patterns and trends
of your blood glucose levels.
Multiple Basal Programs
Make your pump work with your lifestyle and blood glucose trends by programming more than one basal rate to run throughout the day. For instance, you may want to program a higher rate (that’s more insulin) for the early morning, when wake-up hormone levels (known as the dawn phenomenon) might raise your blood glucose. But you may also program a lower basal rate (for less insulin) for afternoons, when you’re more sensitive to insulin. Work with your diabetes care team to adjust your basal rates to reflect your lifestyle and glucose trends throughout the day.
Temporary Basal Rates
There are a host of factors that affect your blood glucose, including food and drink, exercise, medication, and illness. To prevent high and/or low blood glucose in the face of short-term changes, your insulin dosing needs to be adjusted. That’s where a temporary basal rate comes in: You can increase or decrease your basal rate by a certain percentage for a programmed number of hours.
Consider setting a higher rate if you’re stressed out, menstruating, or receiving corticosteroids of any kind (injections, pills, etc.). You might need a lower rate if you’re exercising or sick and unable to eat much (your body will need some insulin, however).
Stopping Delivery
For hypoglycemia prevention, Medtronic’s MiniMed 530G and 630G pumps automatically stop insulin delivery for up to two hours when your glucose level reaches a preset low threshold and you don’t respond to an alert. It’s particularly valuable for those who experience hypoglycemia multiple times during the night and for those who have hypoglycemia unawareness—the inability to feel the symptoms of low blood glucose.
Bolus Insulin
In addition to enhancing diabetes management through basal insulin delivery, pumps also provide ways to optimize blood glucose levels related to mealtime and correction doses—referred to as bolus insulin delivery.
A bolus is a dose of insulin that is delivered on demand. Insulin pump users manually activate the pump to give a meal bolus to match the amount of carbohydrate in the food about to be eaten. The amount of insulin delivered as a meal bolus is calculated using an insulin-to-carbohydrate ratio initially set by your diabetes educator or endocrinologist based on your individual needs.
Insulin pump makes and models vary in how they are operated but you typically program into the pump the amount of carbohydrate you intend to eat and the pump calculates the amount of insulin you need based on the programmed insulin-to-carbohydrate ratio.
You can also manually enter a dose of insulin that you have calculated but this is not the ideal way to use an insulin pump.
Some insulin pumps come with a meter that allows you to set a fixed insulin dose to deliver at meal times. Again this is not the ideal way to give a bolus but in some cases it can be useful.
The right amount of insulin delivered as a bolus dose should return the blood glucose to the target range within two to three hours of eating.
Correction bolus: delivered to correct a high blood glucose reading. This is calculated according to your insulin sensitivity or correction factor set by your diabetes educator or endocrinologist.
Extended, or “Square Wave,” Bolus
Meals high in protein, fat, and fiber take longer to raise blood glucose. Deliver a standard bolus with such a meal, and the immediate insulin dose could cause low blood glucose. The most effective mealtime bolus for foods high in protein, fat, and/or fiber will begin lowering blood glucose an hour or more after eating. That’s where an extended bolus comes in. It’s also a good option for people with gastroparesis, a disorder that delays stomach emptying and causes foods to be absorbed slowly.
Dual Wave Bolus
A dual wave bolus combines the immediate and extended bolus. It’s helpful when eating foods that consist of high fat and/or protein paired with simple carbohydrates. Take, for instance, a hamburger: The early burst of insulin provides immediate coverage for the initial carb from the bun, and the delayed bolus covers any carb slowed down by the fat and protein in the burger.
Added features
Insulin Sensitivity Factor
The insulin sensitivity factor represents the number of points your glucose drops with 1 unit of insulin—essentially how sensitive you are to insulin. Your health care provider can help you calculate an insulin sensitivity factor, which you can enter into your pump. The pump uses the factor to calculate bolus insulin when you correct for high blood glucose.
Insulin Duration
Input insulin duration into your pump, and the device will use it to calculate how long bolused insulin will work to lower your blood glucose. This feature prevents insulin “stacking” due to correction doses that are given too frequently. Because rapid-acting insulin lasts three to four hours, the insulin duration setting limits additional correction doses given too soon after an initial correction bolus.
Insulin-to-Carb Ratio
The insulin-to-carb ratio describes how many grams of carbohydrate you expect to be covered by 1 unit of rapid-acting insulin. Your diabetes care team can help you calculate your initial insulin-to-carb ratio, which you’ll fine-tune together over time. Your pump can use your insulin-to-carb ratio to decide how many units of insulin you should take based on the amount of carbohydrate grams you tell the pump that you plan to eat.
Placing the insulin pump
Knowing how an insulin pump works is one thing. But you may be wondering where you are supposed to put it. You can buy a insulin pump case or it can be attached to a waistband, pocket, bra, garter belt, sock, or underwear. You can also tuck any excess tubing into the waistband of your underwear or pants.
When you sleep, you could try laying the insulin pump next to you on the bed. You could even try wearing it on a waistband, armband, legband, or clip it to the blanket, sheet, pajamas, stuffed toy, or pillow with a belt clip.
Showering and bathing are other instances when you should know where to put your insulin pump. Although insulin pumps are water resistant, they should not be set directly in the water. Instead, you can disconnect it. All insulin pumps have a disconnect port for activities, such as swimming, bathing, or showering. Some pumps can be placed on the side of the tub, in a shower caddy, or in a soap tray. There are also special cases you can buy. You can hang these cases from your neck or from a shower curtain hook.
No matter what you may think, you can still have fun when you are using an insulin pump. When you exercise or play sports, you can wear a strong elastic waist band with a pump case. You can also wear it on an armband where it is visible. Women can tape the insulin pump to the front of their sports bra.
Some coaches do not allow any devices to be worn because getting the pump knocked into you or falling on it can be painful. In this case, you may just need to take the insulin pump off.
When you have to disconnect insulin pump
When you disconnect your pump, you are stopping all delivery (basal and bolus) by the insulin pump.
Here are some important tips to remember when disconnecting your insulin pump.
- It is important for you to remember that if you stop your pump while it is in the middle of delivering any bolus — it will NOT be resumed. You may need to program a new one.
- Be sure to bolus to cover the basal rate you will miss. If your blood glucose level is under 150, you can wait an hour to bolus.
- Do not go longer than one to two hours without any insulin.
- Monitor your blood glucose every three to four hours.
Now that you know how the insulin pump works and how to wear it, take a look at some of the facts to see if this is right for you.
Getting started with an insulin pump
Once you have talked with your diabetes care team and have become comfortable with all of the options on your insulin pump, you and your team will need to do the following in order to get you started.
- Determine how much insulin to use in the insulin pump by averaging the total units of insulin you use per day for several days. (You may start with about 20% less if you are switching to rapid-acting insulin.)
- Divide the total dosage into 40-50% for basal and 50-60% for bolus insulin.
- Divide the basal portion by 24 to determine a beginning hourly basal rate.
- Then, adjust the hourly basal rate up or down for patterns of highs and lows, such as more insulin for dawn phenomenon and less for daily activity.
- Determine a beginning carbohydrate dose (insulin:carb ratio) using the 450 (or 500) rule. Divide by the total units of insulin/day to get the number of grams of carbohydrate covered by one unit of insulin. This dose may be raised or lowered based on your history and how much fast-acting insulin you took in the past.
- Determine the dose of insulin to correct high blood glucose with the 1800 (or 1500) rule. Divide 1800 by the total units of insulin/day to see how much one unit of insulin lowers your blood glucose. This dose must be evaluated by your health care team. It is often too high for children or for people who have not had diabetes very long.
Good insulin pump habits
It may take several months to get comfortable with the insulin pump. During those first months is the time to adopt some good habits. Here are some tips to help you adjust:
- Take your insulin at a specific time, such as five minutes before you eat, so you don’t forget boluses
- When traveling anywhere, bring extra supplies or at least an insulin pen, in case you are unable to use your pump for some reason
- With an insulin pump, when you eat, what you eat, and how much you eat is up to you. You can eat more carbohydrate and still manage your blood glucose, but weight gain can happen. Talk to a dietitian about this when you start on the pump. It’s a lot easier to not to gain weight, than it is to lose it after you have already gained it
- When you take the insulin pump off or turn it off, figure out a system to remember to turn it back on. Listen to the alarms on the pump or set a timer
- Make a habit of recording blood glucose checks, carbohydrate amounts, carbohydrate doses, correction doses, and exercise when you do them. It really helps to sit down and look over your blood glucose record at the end of every week (or even every day) to see if you have any problem areas. Reviewing your records is the key to improving blood glucose control
- Your diabetes provider and insulin pump company have record forms, or you can make your own. Just be sure that you have enough room to record everything you need. Keeping daily records is best, but some people find keeping records for two weekdays and one weekend day gives enough information to see the patterns.
Places to wear the insulin pump
Some people are comfortable with wearing the insulin pump on their belt. The pump may come with a leather carry case or clip, which holds the device and gives the appearance of a pager or small mobile phone.
Others simply carry the pump in a pocket. Some women prefer to wear the pump in their bra or attached to a garter on the leg. Each of the pump suppliers has accessories and there are now also many websites selling pump accessories.
The cannula, which is inserted under the skin, is often placed in the abdominal area but can also be placed in the upper buttock, upper and outer thigh, hip or upper arm.
Swimming
Swimming is a very healthy activity for people with diabetes including those using a pump. Some pumps are waterproof and tested to an international standard while others are watertight. This means it is possible to swim, shower and surf without taking your pump off if you so choose. If you participate regularly in water sports it is advisable to check the individual product specifications regarding waterproof status before choosing your pump.
If you do swim with your waterproof pump you should check for any cracks or loose cartridge or battery covers and so on. If you do not check these things the pump may not be covered under the warranty, as they may be deemed ‘user error’. When wearing the pump during water-based activities you need to be sure it is attached securely. If a pump becomes disconnected in the water it might be difficult to recover and generally health funds will not cover a replacement pump during the warranty period.
Most infusion sets are fitted with a quick-release connection, which allows the pump to be disconnected without removing the cannula from under the skin. This means that it is possible to quickly disconnect from your pump to take a shower, bath or swim. Pump users can safely disconnect from their pump for up to two hours but should monitor blood glucose levels and replace missed basal insulin if necessary.
Diabetes specialists or diabetes educators can advise on the replacement of basal insulin during periods of not using the pump. An insulin pump should not be worn in a spa or sauna as the heat can affect the pump and the insulin.
Sleeping
One of the questions most commonly asked about pump therapy is ‘Where do I put the pump when I go to sleep?’
Some common places people leave their pumps are:
- under their pillow or in their bed
- clipped to their pyjamas or in a pyjama pocket
- specially designed waist bands.
Sex
Some people find that the pump can be worn during sexual activity without causing problems, but for many the pump may get in the way. Pumps can be easily disconnected using the quick-release connection whenever required (for no longer than two hours), but of course it is important to remember to reconnect. The pump can be put in ‘suspend’ or ‘stop’ mode and it will alarm regularly to remind you to reconnect.
Exercise
Regular physical activity is recommended as part of the diabetes management plan. Physical activity can be much easier with a pump because it is possible to temporarily reduce the basal rate of insulin before, during and after the period of exercise to help prevent hypos.
During a long bushwalk or bike ride, for example, it is possible to reduce the basal insulin to 30 per cent of normal in order to reduce the risk of hypos. After exercise, a recovery period with a reduced basal rate is usually needed. It is recommended that you remove the pump during vigorous contact sports. Missed basal insulin can be given as a small bolus if required. The pump should not be removed for longer than two hours or you will risk developing ketones and feeling unwell.
Pregnancy
Ideally, pump therapy should be initiated at least three months prior to conception. This allows time to optimize control and become proficient in the operation of the pump. Of course, if you are already pregnant it is still possible to commence pump therapy and you should discuss this with your diabetes care team. Some hospitals and pump companies may loan you a pump so that you may trial pump therapy before you commit to a purchase.
The advantages of using an insulin pump during pregnancy include:
- tighter diabetes control with less frequent hypoglycemia
- ability to fine-tune the changing insulin requirements that occur during pregnancy
- easier management of morning sickness
- lower likelihood of the baby developing macrosomia (large birthweight)
- more convenience and flexibility during labor because insulin delivery rates are able to be changed according to your needs
- variable rates allow more flexibility whilst breastfeeding.
Sick days
During periods of illness, your insulin requirements may change. A pump can make sick days easier to manage because there is greater flexibility with adjusting insulin doses and delivery rates. A sick day management plan should be prepared in advance with your diabetes educator or endocrinologist and put into action during illness. Your diabetes educator can support and guide you through sick day management so it is important to make contact if you do not have experience in managing sick days yourself.
School
It is important that all teachers and staff caring for the student be informed of the student’s insulin pump and that this detail be recorded in the student’s type 1 diabetes school management plan and kept on file.
Using a pump may make participating in school sports and managing blood glucose levels during times of sickness easier because basal rates can be adjusted to prevent hypos and hyperglycemia.
Travel
When going on trips it is important to remember to take extra supplies of:
- pump batteries
- pump consumables
- insulin (including long-acting) and insulin pens or syringes in case the pump fails
- glucose/ketone meter
- blood and ketone test strips.
You may consider carrying a spare pump. Pump companies will loan you a spare pump (it may carry a cost) but you will need to contact them a few weeks beforehand.
It is highly recommended that you carry a letter from your doctor in case you get inspected at airport security. Some pumps may be affected if scanned by a ‘wand’, but walking through metal detectors at airport security will not affect the pump.
When is insulin pump therapy not recommended
Insulin pump therapy is not recommended for people who:
- are not performing or are not willing to perform frequent blood glucose checks
- are not willing or able to calculate the amount of carbohydrate in meals and snacks
- are not able to detect air bubbles in the infusion line (vision impaired)
- are not able to hear the alarms (hearing impaired), although most modern pumps have a vibration alarm as well as an audible alarm
- are not able to press the buttons on a pump (e.g. severe arthritis)
- are not able to manage possible problems which may arise, including site infections and blocked lines
- are not willing or able to keep in regular contact with their diabetes educator or have regular reviews by their endocrinologist
- are in any way unable to manage the pump functions.
How do I choose an insulin pump?
There are a variety of insulin pumps by different manufacturers on the market. All insulin pumps work in the same basic manner but will vary in their specific functions and features. Your diabetes educator can support you in the process of choosing an insulin pump and help you to work out which one is best for you.
Diabetes insulin pump technology is constantly changing. Be sure to thoroughly research the various insulin pumps you are interested in and make an informed choice. If you have any questions about insulin pump functions speak to your diabetes educator, or the relevant insulin pump company representatives who will be able to help you.
Diabetes insulin pump features to consider
Calculating insulin
Insulin pumps calculate the amount of insulin required to cover the carbohydrate eaten (using rates set by your diabetes educator or
endocrinologist). Insulin pumps also calculate the insulin dose required to correct any high blood glucose level that you enter in the insulin pump that is outside your target range.
Tracking active insulin
Insulin pumps have a feature that prevents you from ‘stacking’ or giving too much insulin. When you enter your blood glucose level and carbohydrate intake, the pump will calculate the dose required after considering the insulin still active or ‘on board’ from a previous bolus. This may assist with avoiding hypos.
Bolus types
Insulin pumps can be programmed to deliver a meal bolus in different ways. A meal bolus may be delivered, for example, over a period of two hours rather than all at once. These different bolus types can make eating a variety of foods and eating out much easier.
Insulin delivery
Pumps vary in the increments of the basal rate and bolus dose that can be delivered. If you have a very small total daily dose of insulin or are very insulin sensitive (e.g. small children) then small delivery doses will be important.
Insulin reservoir/cartridge size
The reservoir/cartridge size varies between pumps, so depending on your daily dose of insulin some pumps will be more suitable than others.
Infusion sets
Not all infusion sets are suitable for everybody. Some people with very little subcutaneous fat will need a different type of infusion set to those with more. Some people have skin sensitivities so will require a set with little tape in contact with the skin.
Insertion devices
Some infusion sets have an insertion device that assists you to insert the cannula with its introducer needle. This can make infusion set changes much easier, especially for children.
Computer software
All insulin pumps have software that allows you to upload pump activity into a program that can analyze the data. The program can save the data in a format that makes it suitable for sharing electronically with diabetes health professionals.
Food database
Insulin pumps with a food database allow you to store the carbohydrate content of a large range of foods that you commonly eat for easy reference.
Water resistance
Some insulin pumps are splash resistant and others are waterproof to certain depth specifications. See the manufacturer’s website for individual water resistance specifications.
Continuous glucose monitoring systems
Some insulin pumps are continuous glucose monitoring systems–ready, and can display real-time glucose information on the monitor. Some can even automatically halt insulin delivery for a couple of hours if the system detects that your glucose level has fallen below a pre-set threshold and you do not respond. Continuous glucose monitoring systems can be useful especially at night when you are asleep.
Insulin pump cost
The cost of an insulin pump ranges from $6000 to $8000, depending on the brand.
Who pays?
In many cases private health insurance funds will rebate the full costs of the pump. However, the level of cover required will vary from fund to fund so it’s a good idea to shop around.
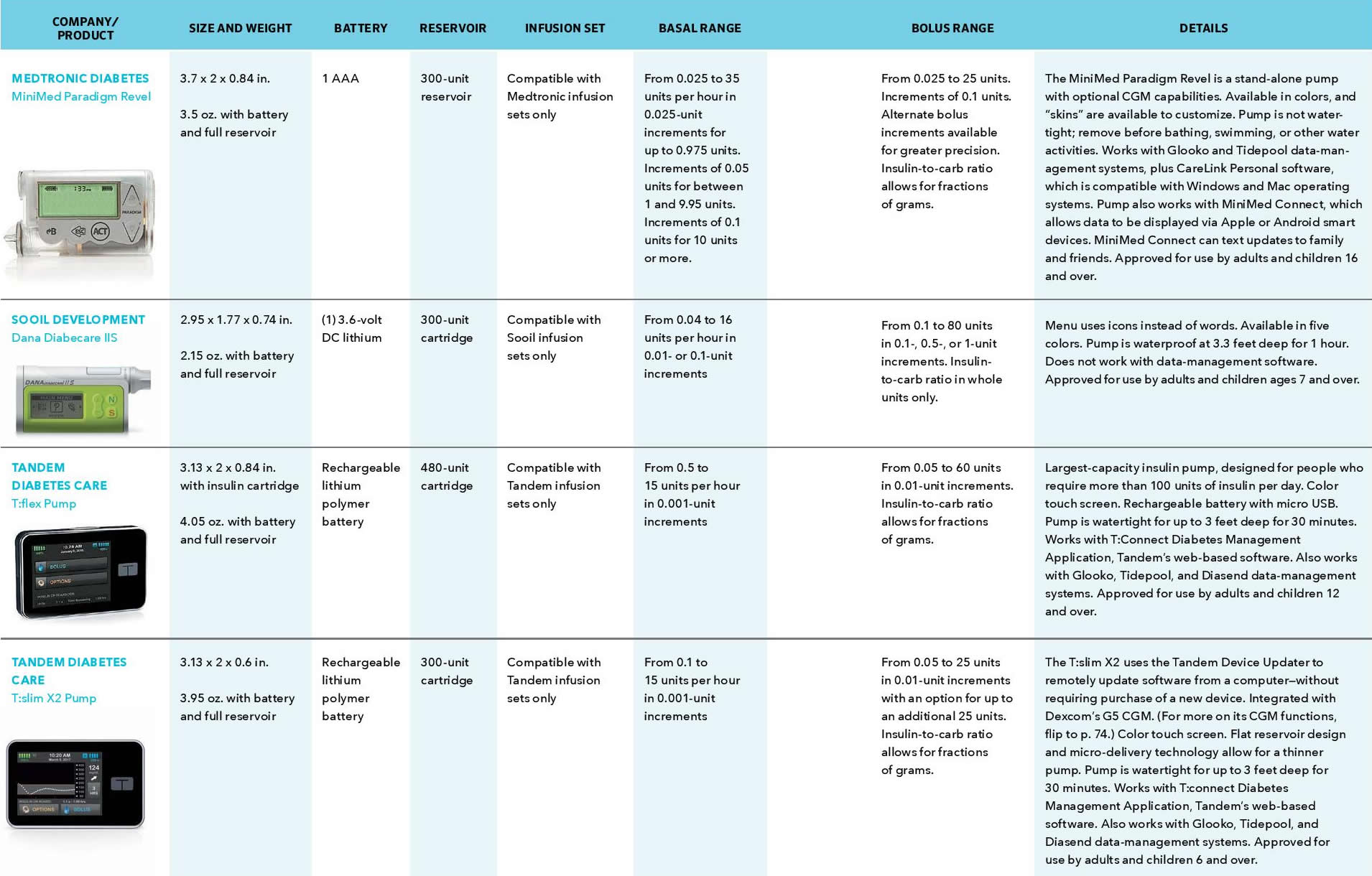
Diabetes insulin pump comparison chart
What are the challenges of insulin pump therapy?
Expense
Using an insulin pump with its disposable infusion sets, cartridges and batteries is more costly than using insulin pens or syringes. Private health insurance will cover the cost of the pump but the consumables must be purchased. This cost will vary according to the brand of pump and the supplies required but will probably amount to approximately $20–$30 a month if you qualify for subsidized pump consumables.
Insulin dose adjustment
Life on an insulin pump can take some getting used to. It may take some time to get your insulin dose regulated on the pump. Initially you can expect lots of ups and downs in your blood glucose levels while you and your diabetes care team intensively monitor and make the necessary adjustments. In the first week or so you need to contact your diabetes educator every one to two days to make adjustments to your rates. As your blood glucose levels stabilize, and you become more comfortable with your pump, the contact will be less frequent.
Being connected
Being connected to a piece of equipment 24 hours a day is probably the issue that most concerns people when they are considering insulin pump therapy. There is no doubt that life with a pump provides greater flexibility in day-to-day living, eating and exercising, but getting used to wearing it around the clock can take some time. Modern pumps are small and compact, which means that they are easy to disguise. You can conceal them in pockets, bras, on belts, clips or in carry cases. Many come in bright colors or have interchangeable covers like a mobile phone. Infusion sets have quick release connections so the pump can be easily detached from the cannula for showering or swimming. It does not take long before most pump users forget that they are attached.
Skills required
Although insulin pumps are quite user-friendly in terms of programming and daily use, they still require a certain level of skill to program and make changes to basal rates, set bolus doses, alarms and so on. You also have to learn to change cartridges and infusion sets.
You will have at least one intensive training session with your diabetes educator when you are fitted with your pump, but there is also a lot of ‘on-the-job training’ as you get to know your pump in the first few weeks.
You will need to keep records and stay in frequent contact with your diabetes educator in the beginning to safely adjust insulin rates and learn the skills needed.
A special note about kids and teens
For children and teenagers operating the pump themselves, emotional maturity is essential. Pumping requires a lot of motivation and diligence. The child or teenager needs to be able and prepared to:
- • check blood glucose levels eight to 10 times a day initially
- • check blood glucose levels at least four times a day once blood glucose levels stabilize
- • count the carbohydrate content of the foods they eat.
Body image is also an important consideration. A pump is worn 24 hours a day and is a visible sign of type 1 diabetes. Consider this when thinking about a pump at a time when body image is important, especially during adolescence.
If you are a parent of a child with type 1 diabetes, you also have the responsibility to ensure that you are committed to pump therapy. You need to understand that although the benefits of pump therapy are immense, the level of commitment is high.
You need to know as much about the pump as if it were your own and you need to be prepared to problem solve should an issue arise at school or at social activities.
Regular discussion and supervision of your child remains essential.
Technical problems
Even the most reliable equipment encounters technical problems at times. Insulin pumps and their in-built micro-computers are very reliable but problems can arise. Infusion sets can become blocked, computers can fail, screens and pump bodies can be damaged. Pumps do have some alarms and safety features to alert the user to possible problems. It’s a good idea to record your rates somewhere e.g. diary, iPhone. Regularly downloading your pump data allows easy access to the last programmed rates in case of pump failure.
Technical assistance is available from individual pump companies 24 hours a day. In case of any problems or pump failure it is important to have available insulin pens or syringes and a supply of in-date long-acting insulin in your refrigerator, as well as a written back-up plan.
Skin problems
One of the most common problems associated with insulin pump use is skin irritation. Infusion sets feature hypoallergenic adhesive tape that is designed to minimize skin irritation. Those with sensitive skin may still experience itching, rashes or minor inflammation. There are many different brands of infusion sets on the market and you may need to experiment to find a brand that suits your skin. You can also consider using a skin barrier to minimize contact between your skin and the tape of the infusion set.
Skin infections are another potential problem
Skin infections will not normally occur as long as you:
- wash your hands
- clean your skin appropriately
- use a proper technique when changing infusion sets
- change the set on a regular basis.
More rapid development of ketones
Ketones are chemicals produced when the body breaks down stored fat for energy because there is not enough insulin in the blood. Insulin pumps do not use long-acting insulin, so any interruption in insulin delivery for more than a few hours can lead to ketosis.
Ketosis is a state characterized by elevated levels of ketones in the blood. If not treated promptly, ketosis can lead to diabetic ketoacidosis (DKA); a life-threatening condition that requires emergency treatment in hospital. For this reason, pump users need to check their BGLs at least four times a day. Ketones must be checked when blood glucose levels are 15mmol/L or more at the first sign of illness.
If this situation should arise, always make urgent contact with your diabetes care team. Always have in-date ketone test strips (either blood or urine) available for use.