Contents
What is genetic mosaicism
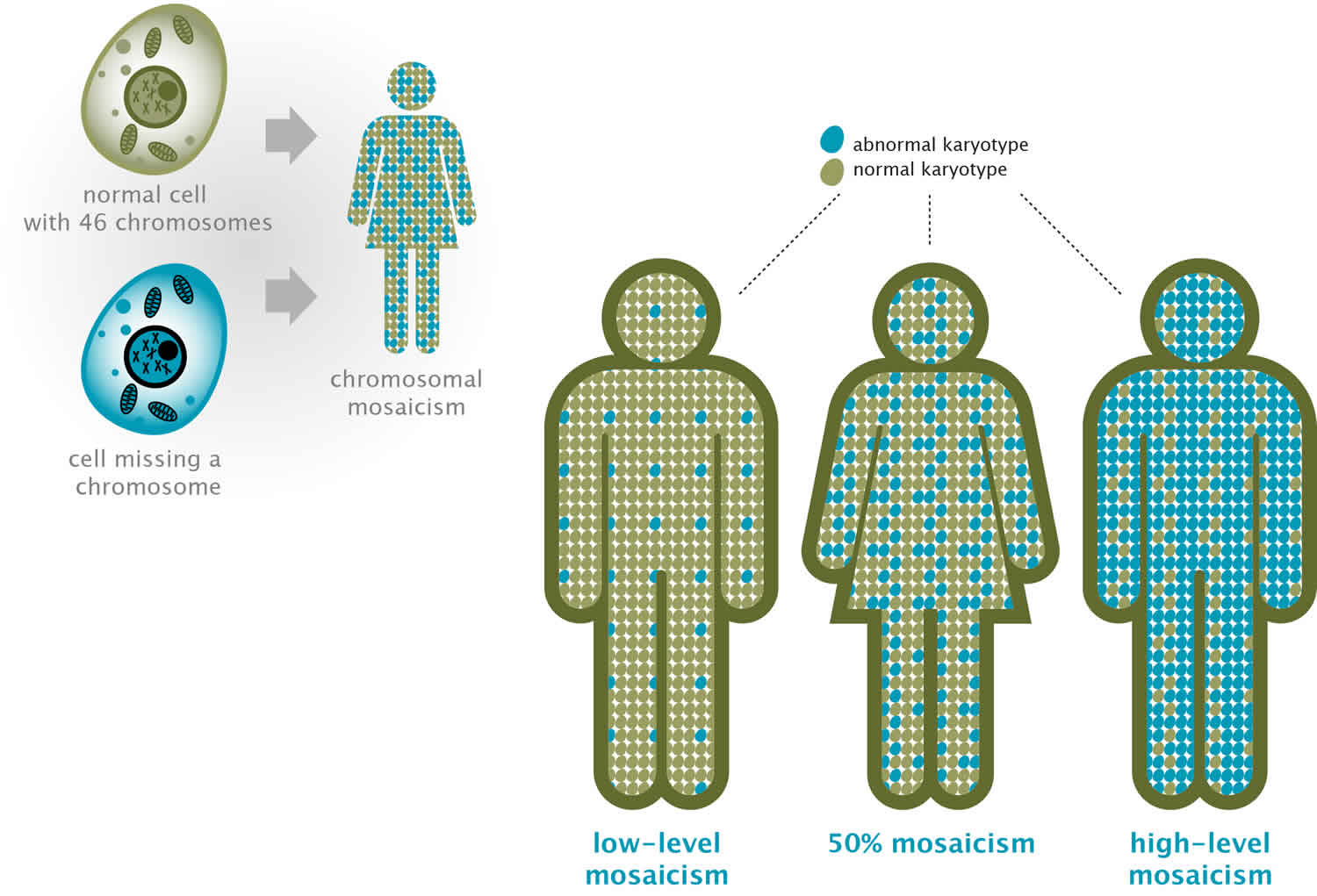
Mosaicism or chromosomal mosaicism, is an abnormal chromosome division resulting in two or more kinds of cells, each containing different numbers of chromosomes. Mosaicism is a condition in which cells within the same person have a different genetic makeup. A person with a genetic disorder may have both normal and abnormal cells. Scientists call this phenomenon mosaicism and it is the result of an error in cell division affecting a number of cells during early development of an embryo or fetus. Mosaicism is seen mainly at the chromosomal level, particularly in numerical disorders such as Down’s syndrome (trisomy 21), Klinefelter’s syndrome (47,XXY or XXY) or Turner’s syndrome (45X).
Mosaicism also occurs at the DNA level, e.g. in Fragile X syndrome, due to the (variable in the case of mosaicism) expansion of a trinucleotide repeat. Depending on the percentage of cells affected, the genetic disorder will be expressed more or less severely. In people with one of these symptoms doctors may also be able to see this visually and medically (more or fewer external characteristics and symptoms).
- Somatic mosaicism: Somatic mosaicism refers to the occurrence of two genetically distinct populations of cells within an individual, derived from a postzygotic mutation. Somatic mosaicism is present in the genomes of cells that make up the body of the organism and do not contribute to gametes produced by the individual thus are not transmitted to offspring 1
- Gonadal mosaicism: Genetic variation that is present in the genomes of cells that specifically contribute to the gametes 1
- Gonosomal mosaicism: Genetic variation that is present in the genomes of both somatic cells and germline cells 1
- Pigmentary mosaicism is a term that describes varied patterns of pigmentation in the skin caused by genetic heterogeneity of the skin cells 2
Mosaicism can affect any type of cell, including:
- Blood cells
- Egg and sperm cells
- Skin cells
Some examples of single-gene diseases that are associated with somatic mosaicism are listed below 3:
- Metabolic disorders:
- Tyrosinemia type I
- Lesch-Nyhan
- Conradi-Hunermann-Happle
- Immune dysfunction
- Adenosine deaminase deficiency
- Wiskott-Aldrich syndrome
- Clotting disorders
- Hemophilia A
- Hemophilia B
- Skeletal Disorders
- Marfan syndrome
- Pseudoachondroplasia
- Muscle Disorders
- Duchenne musclar dystrophy
- Congenital myotonic dystrophy
- Chromosomal instability
- Bloom syndrome
- Fanconi anemia
- Tumor suppressor
- Neurofibromatosis type I
- Neurofibromatosis type II
- Tuberous sclerosis
- Skin disorders
- Bullous ichthysiform erythroderma
- Incontinentia pigmenti
- Endocrine disorders:
- Androgen insensitivity
- Nervous-system disorders:
- Friedreich ataxia
Figure 1. Chromosomal mosaicism
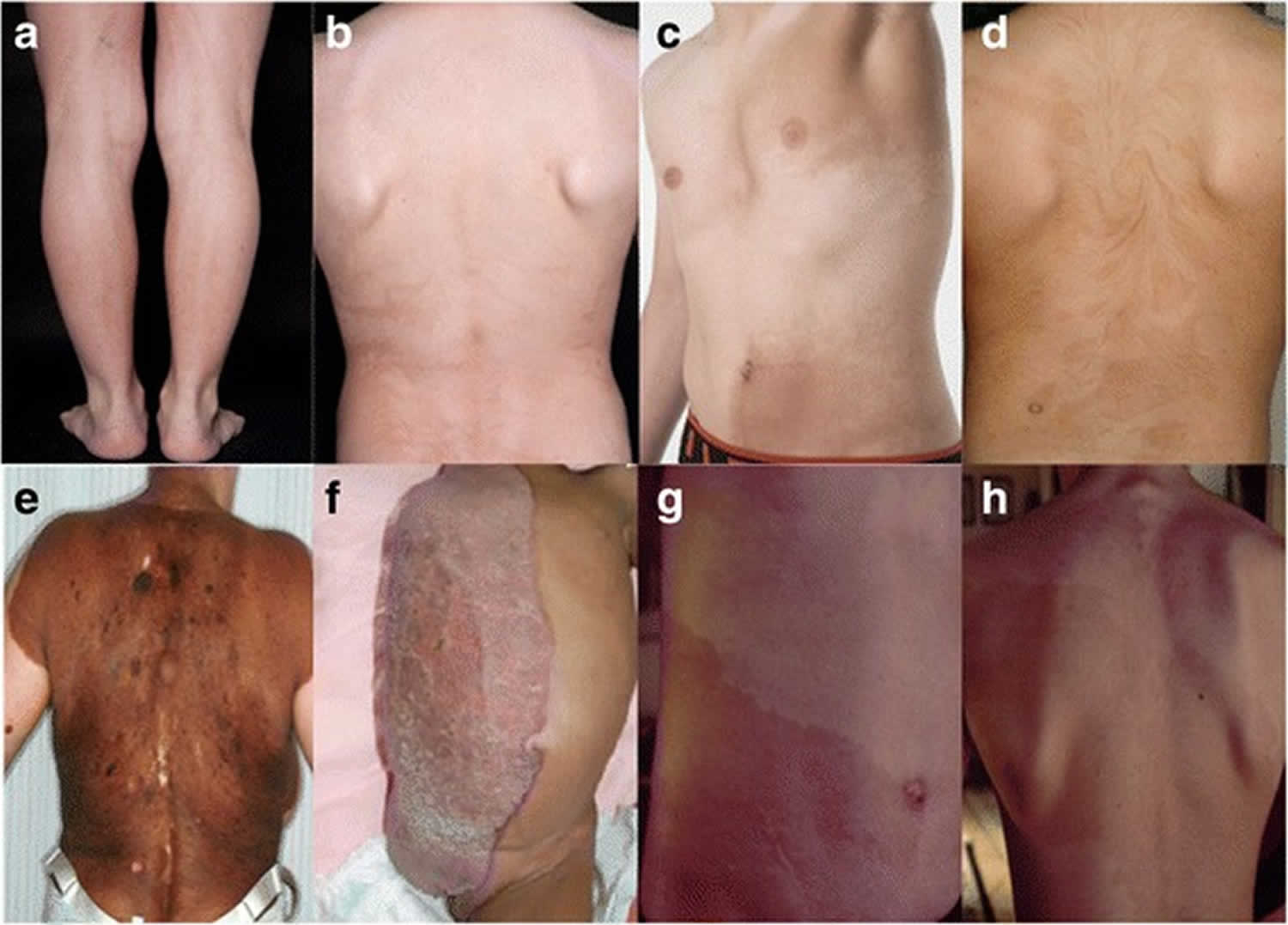
Figure 2. Pigmentary mosaicism
Footnote: Clinical examples of archetypical patterns of cutaneous mosaicism. (a) Hyperpigmentation following Blaschko lines in narrow bands, (b) hyperpigmentation following Blaschko lines in broad bands, (c) checkerboard pattern, (d) phylloid hyperpigmentation, (e) giant melanocytic nevus representing patchy pattern, (f) CHILD-syndrome representing lateralization pattern (g) and (h) cutis tricolor of the Ruggieri-Happle type
[Source 2 ]Confined placental mosaicism
Confined placental mosaicism in when the placenta have a different chromosome makeup from the baby that occurs in approximately 1-2% of all pregnancies 4. Normally the placenta and the baby come from the same cells, they have exactly the same amount of chromosomes most (98-99%) of the time.
When it comes to genetic testing, confined placental mosaicism is important to remember particularly when it comes to chorionic villus sampling (CVS) procedures. If someone has a CVS and the results show an extra or missing chromosome, scientists know that the most likely thing is that the pregnancy also has that extra or missing chromosome. However, 1-2% of the time, that extra or missing chromosome is only found in the placenta and not in the pregnancy.
The exact reason for confined placental mosaicism is unknown, but it is thought that after the placenta and the baby separate, some sort of error happens during cell division in the placenta, which causes some of the cells to have an extra or missing chromosome.
If confined placental mosaicism is suspected on a chorionic villus sampling (CVS) result, it may be recommended to perform an amniocentesis procedure to confirm. Because the cells obtained from an amniocentesis are from directly around the baby, it is more accurate in determining whether the pregnancy actually has the extra or missing chromosome.
Mosaicism symptoms
Symptoms vary and are very difficult to predict. Symptoms may not be as severe if you have both normal and abnormal cells.
Mosaicism diagnosis
Genetic testing can diagnose mosaicism. Tests will likely need to be repeated to confirm the results, and to help determine the type and severity of the disorder.
A diagnosis of mosaicism may cause confusion and uncertainty. A genetic counselor may help answer any questions about diagnosis and testing.
Mosaicism treatment
Treatment will depend on the type and severity of the disorder. You may need less intense treatment if only some of the cells are abnormal.
Mosaicism prognosis
How well you do depends on which organs and tissues are affected (for example, the brain or heart). It is difficult to predict the effects of having two different cell lines in one person.
In general, people with a high number of abnormal cells have the same outlook as people with the typical form of the disease (those who have all abnormal cells). The typical form is also called non-mosaic.
People with a low number of abnormal cells may be only mildly affected. They may not discover that they have mosaicism until they give birth to a child who has the non-mosaic form of the disease. Sometimes a child born with the non-mosaic form will not survive, but a child born with mosaicism will.
- Campbell IM, Shaw CA, Stankiewicz P, Lupski JR. Somatic mosaicism: implications for disease and transmission genetics. Trends Genet. 2015;31(7):382-92. https://www.ncbi.nlm.nih.gov/pmc/articles/PMC4490042/[↩][↩][↩]
- Kromann AB, Ousager LB, Ali IKM, Aydemir N, Bygum A. Pigmentary mosaicism: a review of original literature and recommendations for future handling. Orphanet J Rare Dis. 2018;13(1):39. Published 2018 Mar 5. doi:10.1186/s13023-018-0778-6 https://www.ncbi.nlm.nih.gov/pmc/articles/PMC5839061[↩][↩]
- Chial, H. (2008) Somatic mosaicism and chromosomal disorders. Nature Education 1(1):69[↩]
- Confined Placental Mosaicism(CPM). https://geneticsupportfoundation.org/patientlibrary/cpm.pdf[↩]