Contents
- What is pancreatic cancer
- What is the Pancreas
- Types of pancreatic cancer
- Pancreatic cancer life expectancy and survival
- Signs and symptoms of pancreatic cancer
- Pancreatic cancer causes
- Complications of pancreatic cancer
- Prevention of pancreatic cancer
- Pancreatic cancer diagnosis
- Pancreatic cancer stages
- Pancreatic cancer treatment
What is pancreatic cancer
Pancreatic cancer begins in the tissues of your pancreas — an organ in your abdomen that lies horizontally behind the lower part of your stomach. Your pancreas releases enzymes that aid digestion and hormones that help manage your blood sugar.
Around half of all new cases of pancreatic cancer are diagnosed in people aged 75 or over. It’s uncommon in people under 40 years of age.
Pancreatic cancer is hard to find early. The pancreas is deep inside the body, so early tumors can’t be seen or felt by health care providers during routine physical exams. People usually have no symptoms until the cancer has already spread to other organs.
Screening tests or exams are used to look for a disease in people who have no symptoms (and who have not had that disease before). At this time, no major professional groups recommend routine screening for pancreatic cancer in people who are at average risk. This is because no screening test has been shown to lower the risk of dying from this cancer.
The American Cancer Society’s estimates for pancreatic cancer in the United States for 2017 are:
- About 53,670 people (27,970 men and 25,700 women) will be diagnosed with pancreatic cancer.
- About 43,090 people (22,300 men and 20,790 women) will die of pancreatic cancer.
Pancreatic cancer accounts for about 3% of all cancers in the US and about 7% of all cancer deaths.
The average lifetime risk of pancreatic cancer for both men and women is about 1 in 65 (1.5%). But each person’s chances of getting this cancer can be affected by certain risk factors.
The symptoms of pancreatic cancer vary depending on where the cancer is in the pancreas – in the head, body or tail. The most common type of pancreatic cancer starts in the cells that produce digestive juices and is called an exocrine tumor. Endocrine pancreatic tumors are uncommon. They are also called neuroendocrine tumours. Most pancreatic neuroendocrine tumors don’t produce hormones so don’t cause specific symptoms. Pancreatic neuroendocrine tumours that produce hormones are called functional tumors. The symptoms are different for each type, depending on the hormone the tumor produces.
Pancreatic cancer typically spreads rapidly to nearby organs. It is seldom detected in its early stages. But for people with pancreatic cysts or a family history of pancreatic cancer, some screening steps might help detect a problem early. One sign of pancreatic cancer is diabetes, especially when it occurs with weight loss, jaundice or pain in the upper abdomen that spreads to the back.
Treatment may include surgery, chemotherapy, radiation therapy or a combination of these.
What is the Pancreas
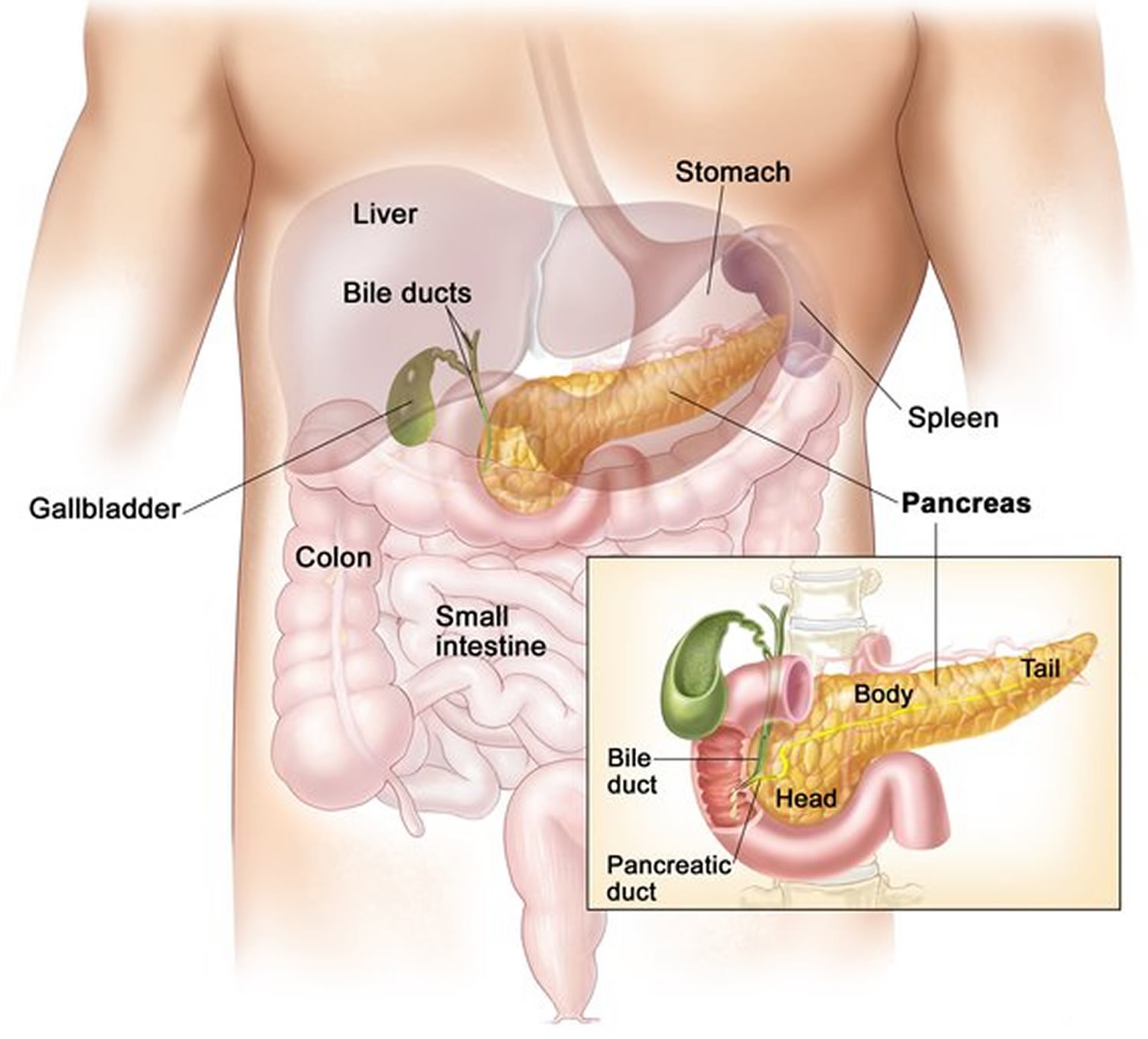
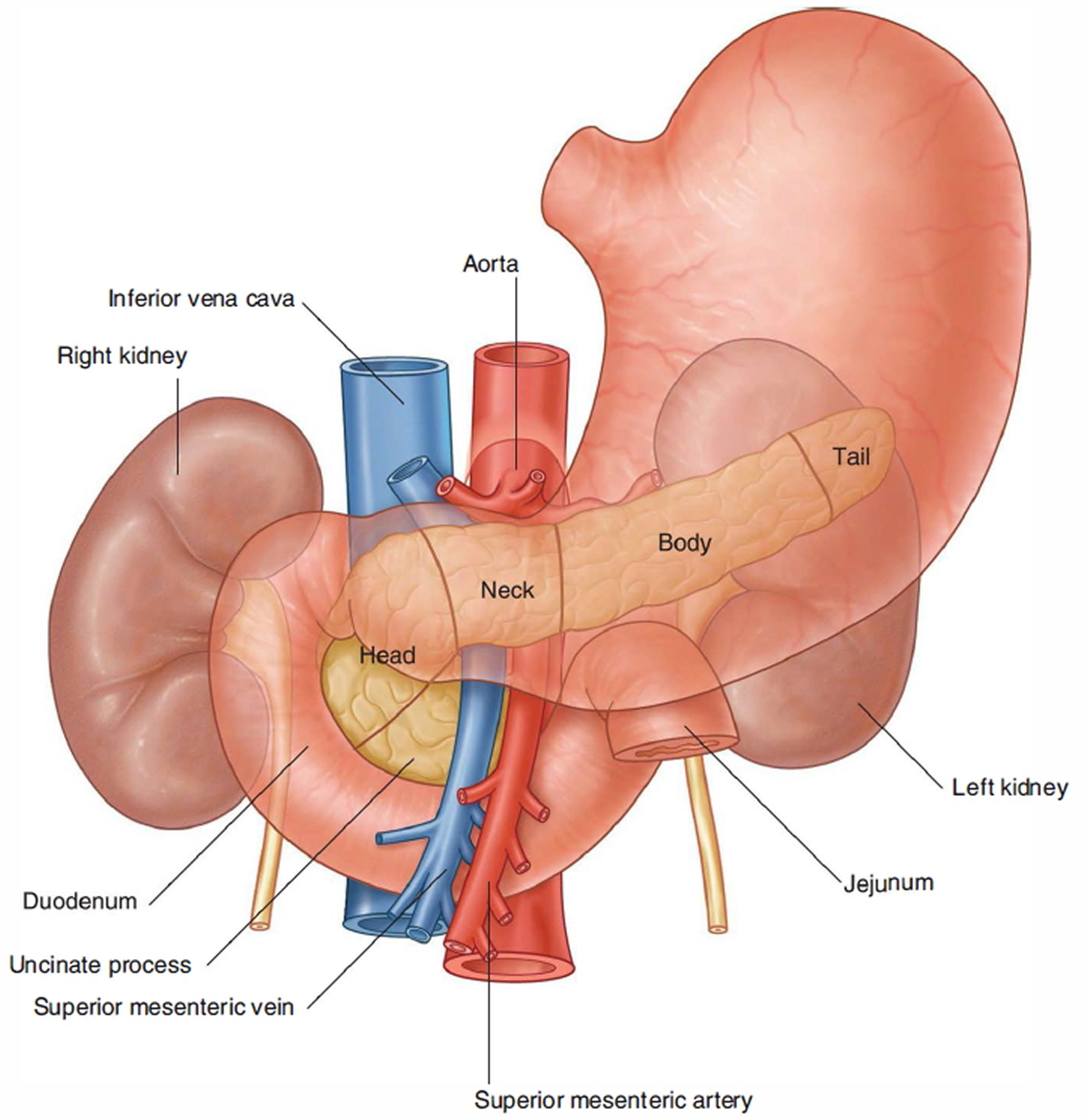
The pancreas is an organ that sits behind the stomach. It’s shaped a bit like a fish with a wide head, a tapering body, and a narrow, pointed tail. In adults it’s about 6 inches long but less than 2 inches wide. The head of the pancreas is on the right side of the abdomen (belly), behind where the stomach meets the duodenum (the first part of the small intestine). The body of the pancreas is behind the stomach, and the tail of the pancreas is on the left side of the abdomen next to the spleen.
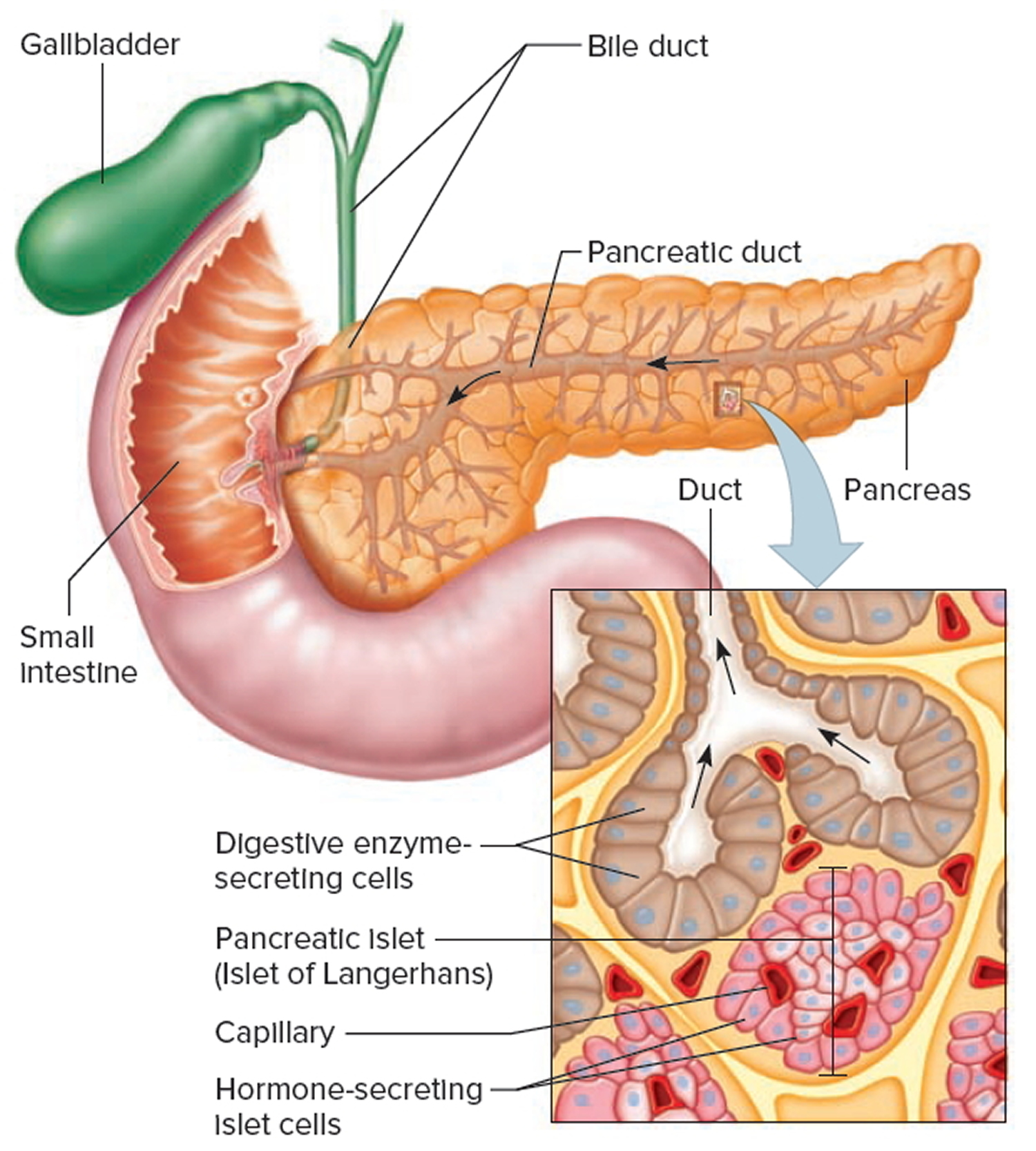
The pancreas is both an endocrine and exocrine gland (see Figure 4). The endocrine part of the pancreas consists of groups of cells that are closely associated with blood vessels. These groups form “islands” of cells called pancreatic islets (islets of Langerhans). The pancreatic islets include two distinct types of cells—alpha cells, which secrete the hormone glucagon, and beta cells, which secrete the hormone insulin. Both insulin and glucagon are important hormones which help control blood sugar levels and are released directly into the blood.
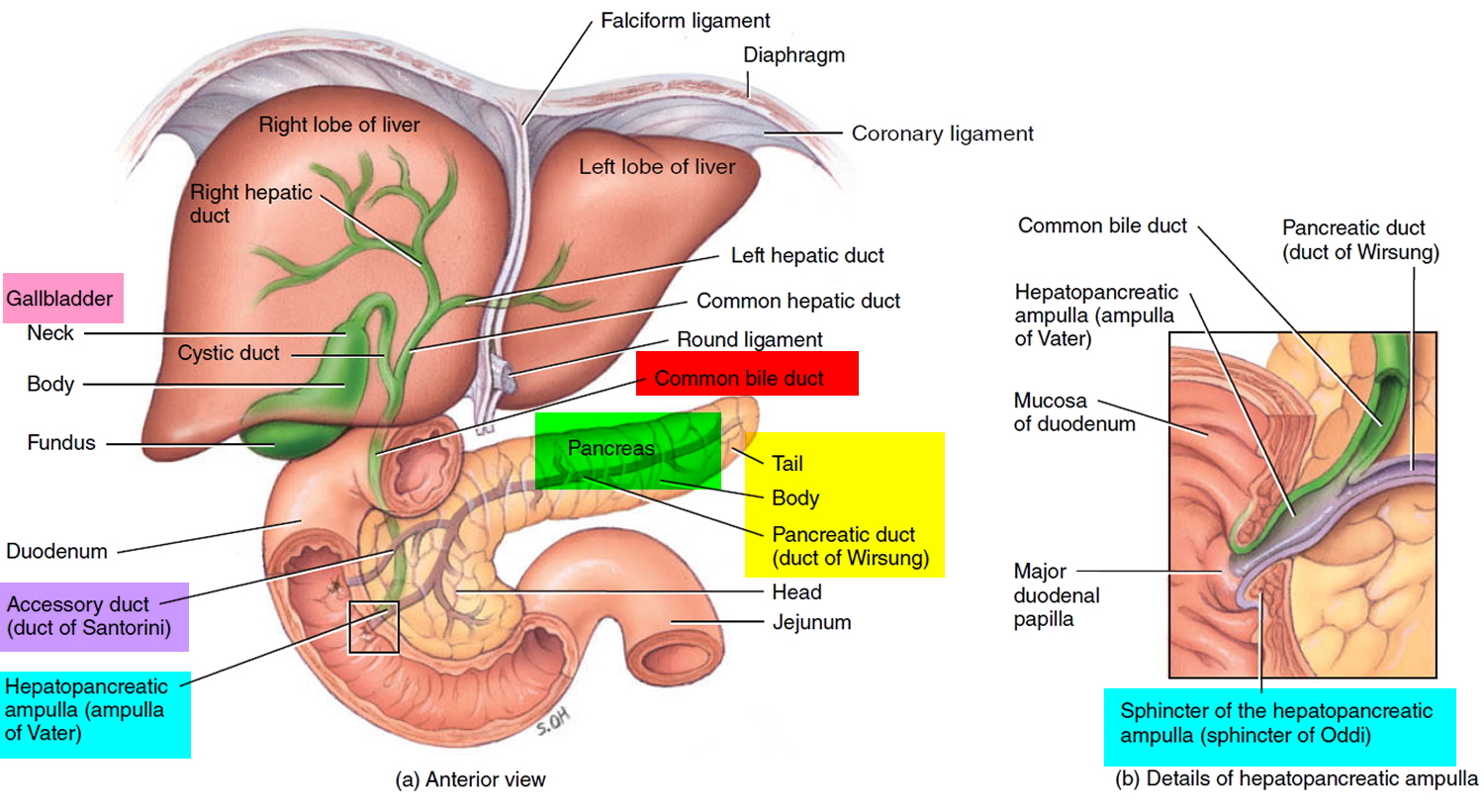
About 99% of the pancreas is exocrine tissue, which secretes 1,200 to 1,500 mL of pancreatic juice per day – that are released into the small intestines to help you digest foods (especially fats). The enzymes are first released into tiny tubes called ducts. These merge to form larger ducts, which empty into the pancreatic duct. The pancreatic duct merges with the common bile duct (the duct that carries bile from the liver), and empties into the duodenum (the first part of the small intestine) at the ampulla of Vater. Pancreatic islets are relatively concentrated in the tail of the pancreas, whereas the head is more exocrine. Over 90% of pancreatic cancers arise from the ducts of the exocrine portion (ductal carcinomas), so cancer is most common in the head of the gland.
Figure 1. Pancreas location
Figure 2. Pancreas
Figure 3. Relationship of the pancreas to the liver, gallbladder, and duodenum
Figure 4. Pancreas cell types
Types of pancreatic cancer
The exocrine cells and endocrine cells of the pancreas form different types of tumors. It’s very important to know if the cancer in the pancreas is an exocrine or endocrine cancer. They have distinct risk factors and causes, have different signs and symptoms, are diagnosed with different tests, are treated in different ways, and have different outlooks.
Exocrine pancreatic cancers
Exocrine cancers are by far the most common type of pancreas cancer. If you are told you have pancreatic cancer, it’s most likely an exocrine pancreatic cancer.
Pancreatic adenocarcinoma: About 95% of cancers of the exocrine pancreas are adenocarcinomas. These cancers usually start in the ducts of the pancreas. Less often, they develop from the cells that make the pancreatic enzymes, in which case they are called acinar cell carcinomas.
Less common types of exocrine cancer: Other, less common exocrine cancers include adenosquamous carcinomas, squamous cell carcinomas, signet ring cell carcinomas, undifferentiated carcinomas, and undifferentiated carcinomas with giant cells.
Ampullary cancer (carcinoma of the ampulla of Vater): This cancer starts in the ampulla of Vater, which is where the bile duct and pancreatic duct come together and empty into the small intestine. Ampullary cancers aren’t technically pancreatic cancers, but they are included here because they are treated much the same.
Ampullary cancers often block the bile duct while they’re still small and have not spread far. This blockage causes bile to build up in the body, which leads to yellowing of the skin and eyes (jaundice). Because of this, these cancers are usually found earlier than most pancreatic cancers, and they usually have a better prognosis (outlook).
Pancreatic endocrine tumors (neuroendocrine tumors)
Tumors of the endocrine pancreas are uncommon, making up less than 5% of all pancreatic cancers. As a group, they are often called pancreatic neuroendocrine tumors (NETs) or islet cell tumors.
Pancreatic neuroendocrine tumors (NETs) can be benign (not cancer) or malignant (cancer). Benign and malignant tumors can look alike under a microscope, so it isn’t always clear if a pancreatic neuroendocrine tumor (NET) is really cancer. Sometimes it only becomes clear that an neuroendocrine tumor (NET) is cancer when it spreads outside the pancreas.
There are many types of pancreatic neuroendocrine tumors (NETs).
Functioning neuroendocrine tumors (NETs): About half of pancreatic NETs make hormones that are released into the blood and cause symptoms. These are called functioning tumors. Each one is named for the type of hormone the tumor cells make.
- Gastrinomas come from cells that make gastrin. About half of gastrinomas are cancers.
- Insulinomas come from cells that make insulin. Most insulinomas are benign (not cancer).
- Glucagonomas come from cells that make glucagon. Most glucagonomas are cancers.
- Somatostatinomas come from cells that make somatostatin. Most somatostatinomas are cancers.
- VIPomas come from cells that make vasoactive intestinal peptide (VIP). Most VIPomas are cancers.
- PPomas come from cells that make pancreatic polypeptide. Most PPomas are cancers.
Most functioning NETs are gastrinomas or insulinomas. The other types are rare.
Non-functioning NETs: These tumors don’t make enough excess hormones to cause symptoms. They are more likely to be cancer than are functioning tumors. Because they don’t make excess hormones that cause symptoms, they can often grow quite large before they’re found.
Carcinoid tumors: These NETs are much more common in other parts of the digestive system, although rarely they can start in the pancreas. These tumors often make serotonin (also called 5-HT) or its precursor, 5-HTP.
The treatment and outlook for pancreatic NETs depend on the specific tumor type and the stage (extent) of the tumor, but the outlook is generally better than that of pancreatic exocrine cancers.
Benign and precancerous growths in the pancreas
Some growths in the pancreas are simply benign (not cancer), while others might become cancer over time if left untreated (known as precancers). Because people are getting imaging tests such as CT scans more often than in the past (for a number of reasons), these types of pancreatic growths are now being found more often.
Serous cystic neoplasms (SCNs) (also known as serous cystadenomas) are tumors that have sacs (cysts) filled with watery fluid. Serous cystic neoplasms (serous cystadenomas) are almost always benign, and most don’t need to be treated unless they grow large or cause symptoms.
Mucinous cystic neoplasms (MCNs) (also known as mucinous cystadenomas) are slow-growing tumors that have cysts filled with a jelly-like substance called mucin. These tumors almost always occur in women. While they are not cancer, some of them can progress to cancer over time if not treated, so these tumors are typically removed with surgery.
Intraductal papillary mucinous neoplasms (IPMNs) are benign tumors that grow in the pancreatic ducts. Like mucinous cystic neoplasms (mucinous cystadenomas), these tumors make mucin, and over time they sometimes become cancer if not treated. Some intraductal papillary mucinous neoplasms can just be followed closely over time, but some might need to be removed with surgery if they have certain features, such as if they are in the main pancreatic duct.
Solid pseudopapillary neoplasms (SPNs) are rare, slow-growing tumors that almost always develop in young women. Even though these tumors tend to grow slowly, they can sometimes spread to other parts of the body, so they are best treated with surgery. The outlook for people with these tumors is usually very good.
Pancreatic cancer life expectancy and survival
Survival rates tell you what portion of people with the same type and stage of cancer are still alive a certain amount of time (usually 5 years) after they were diagnosed. They can’t tell you how long you will live, but they may help give you a better understanding about how likely it is that your treatment will be successful. Some people will want to know the survival rates for their cancer, and some people won’t. If you don’t want to know, you don’t have to.
What is a 5-year survival rate?
Statistics on the outlook for a certain type and stage of cancer are often given as 5-year survival rates, but many people live longer – often much longer – than 5 years. The 5-year survival rate is the percentage of people who live at least 5 years after being diagnosed with cancer. For example, a 5-year survival rate of 70% means that an estimated 70 out of 100 people who have that cancer are still alive 5 years after being diagnosed. Keep in mind, however, that many of these people live much longer than 5 years after diagnosis.
But remember, the 5-year relative survival rates are estimates – your outlook can vary based on a number of factors specific to you.
Cancer survival rates don’t tell the whole story
Survival rates are often based on previous outcomes of large numbers of people who had the disease, but they can’t predict what will happen in any particular person’s case. There are a number of limitations to remember:
- The numbers below are among the most current available. But to get 5-year survival rates, doctors have to look at people who were treated at least 5 years ago. As treatments are improving over time, people who are now being diagnosed with pancreatic cancer may have a better outlook than these statistics show.
- These statistics are based on the stage of the cancer when it was first diagnosed. They do not apply to cancers that later come back or spread, for example.
- The outlook for people with pancreatic cancer varies by the stage (extent) of the cancer – in general, the survival rates are higher for people with earlier stage cancers. But many other factors can affect a person’s outlook, such as age and overall health, and how well the cancer responds to treatment. The outlook for each person is specific to their circumstances.
Your doctor can tell you how these numbers may apply to you, as he or she is familiar with your particular situation.
Survival rates for exocrine pancreatic cancer
The numbers below come from the National Cancer Data Base and are based on people diagnosed with exocrine pancreatic cancer between 1992 and 1998 1. In general, people who can be treated with surgery tend to live longer than those not treated with surgery.
- The 5-year survival rate for people with stage IA pancreatic cancer is about 14%. For stage IB cancer, the 5-year survival rate is about 12%.
- For stage IIA pancreatic cancer, the 5-year survival rate is about 7%. For stage IIB cancer, the 5-year survival rate is about 5%.
- The 5-year survival rate for stage III pancreatic cancer is about 3%.
- Stage IV pancreatic cancer has a 5-year survival rate of about 1%. Still, there are often treatment options available for people with this stage of cancer.
According to Surveillance, Epidemiology, and End Results Program (SEER 18) 2007-2013, All Races, Both Sexes ~ 8.2 Percent Surviving 5 Years 2.
Survival by Stage 2
Cancer stage at diagnosis, which refers to extent of a cancer in the body, determines treatment options and has a strong influence on the length of survival. In general, if the cancer is found only in the part of the body where it started it is localized (sometimes referred to as stage 1). If it has spread to a different part of the body, the stage is regional or distant. The earlier pancreatic cancer is caught, the better chance a person has of surviving five years after being diagnosed. For pancreatic cancer, 9.7% are diagnosed at the local stage. The 5-year survival for localized pancreatic cancer is 31.5%.
Remember, these survival rates are only estimates – they can’t predict what will happen to any individual person. We understand that these statistics can be confusing and may lead you to have more questions. Talk to your doctor to better understand your specific situation.
Survival rates for neuroendocrine pancreatic tumors (treated with surgery)
For pancreatic neuroendocrine tumors (NETs), survival statistics by stage are only available for patients treated with surgery. These numbers come from the National Cancer Data Base and are based on patients diagnosed between 1985 and 2004.
- The 5-year survival rate for people with stage I pancreatic NETs is about 61%.
- For stage II pancreatic NETs, the 5-year survival rate is about 52%.
- The 5-year relative survival rate for stage III pancreatic NETs is about 41%.
- Stage IV pancreatic NETs have a 5-year survival rate of about 16%. Still, there are often treatment options available for people with these cancers.
In this database, the overall 5-year survival rate for people who did not have their tumors removed by surgery was 16%.
Signs and symptoms of pancreatic cancer
In the early stages, pancreatic cancer doesn’t usually cause any symptoms, which can make it difficult to diagnose.
It’s important to remember that these symptoms can be caused by many different conditions, and aren’t usually the result of cancer. But you should see your doctor if you’re concerned, or if these symptoms start suddenly.
Early pancreatic cancer symptoms are:
- Pain in the back or stomach area that radiates to your back– which may come and go at first and is often worse when you lie down or after you’ve eaten. Some people may only have back pain. This is often felt in the middle of the back, and is persistent. Almost 7 out of 10 people (70%) with pancreatic cancer go to their doctors because they have pain. Pain is more common in cancers of the body and tail of the pancreas. People describe it as a dull pain that feels as if it is boring into you. It can begin in the stomach area and spread around to the back. The pain is worse when you lie down and is better if you sit forward. It can be worse after meals.
- Loss of appetite or unintended weight loss. People diagnosed with pancreatic cancer might have recently lost a lot of weight (at least 10% of their total body weight) for no apparent reason. This symptom is more common in cancers of the head of the pancreas.
- Jaundice – the most obvious sign is yellowing of the skin and whites of the eyes; it also causes your urine to be dark yellow or orange and your stools (feces) to be pale-colored. Many people with pancreatic cancer have jaundice when they first go to their doctors. Most of these people will have pain as well. Around 1 in 10 people (10%) have painless jaundice. Jaundice is more common with cancer of the head of the pancreas because the tumour blocks the bile duct. This tube carries bile into the duodenum. If it is blocked the bile ends up in your bloodstream. It is passed out in your urine rather than through the bowel. Bile contains a lot of yellow pigments so it turns the skin yellow. Jaundice is a common symptom of many liver and gallbladder diseases. It is often easier to spot in the whites of the eyes rather than the skin.
Signs and symptoms of pancreatic cancer often don’t occur until the disease is advanced. Other symptoms may include:
- Depression
- New-onset diabetes
- Blood clots
- Fatigue
- Itching. You might have itching if you have bad jaundice. The increased bile salts in the bloodstream cause itching in the skin.
- Sickness. You may feel or be sick because you have jaundice or an inflamed pancreas. Both these conditions upset the delicate chemical balance of the body. You might also be sick if the cancer, or inflammation around it, starts to block food from passing out of the stomach and into the first part of the bowel. Due to sickness, you might have a loss of appetite which can cause weight loss.
- Nausea and vomiting
- Bowel changes. If your pancreatic duct blocks, you might develop a symptom called steatorrhoea. This means fatty stools (poo). You may pass frequent, large bowel motions that are pale colored and smelly, and are difficult to flush away. These bowel disturbances can mean that you are not absorbing your food properly. This can also cause weight loss.
- Fever and shivering. You might have a temperature from time to time because you have jaundice or an inflamed pancreas. When your temperature is high you may feel cold and shivery.
- Indigestion. Indigestion causes heartburn, bloating and sickness. It is a common problem in the general population, and for most people it isn’t a sign of cancer. If it is persistent or isn’t getting better with medicines, you should go back to see your doctor.
You may also develop symptoms of diabetes if you have pancreatic cancer, because it can produce chemicals that interfere with the normal effect of insulin.
Diabetes: Some people diagnosed with cancer of the pancreas are found to be newly diabetic. Some have been diagnosed with diabetes within the previous year. If you have diabetes you are not producing enough insulin. So there is too much sugar in your blood. The sugar passes out of the body in the urine and takes some water with it.
This causes:
- thirst
- passing a lot of urine
- weakness
- weight loss and hunger
Blood clots
Occasionally, pancreatic cancer is linked to blood clots. They may form in the deep veins in the legs for example, or in smaller veins anywhere on the body. Sometimes the clots will disappear and then develop somewhere else in the body.
See your doctor straight away if you have these symptoms:
- pain, redness and swelling around the area where the clot is
- the area around the clot might feel warm to touch
Signs and symptoms of pancreatic neuroendocrine tumors
Pancreatic neuroendocrine tumors (NETs) often release excess hormones into the bloodstream. Different types of tumors make different hormones, which can lead to different symptoms.
Gastrinomas
These tumors make gastrin, a hormone that tells the stomach to make more acid. Too much gastrin causes a condition known as Zollinger-Ellison syndrome, in which the stomach makes too much acid. This leads to stomach ulcers, which can cause pain, nausea, and loss of appetite. Severe ulcers can start bleeding. If the bleeding is mild, it can lead to anemia (too few red blood cells), which can cause symptoms like feeling tired and being short of breath. If the bleeding is more severe, it can make stool black and tarry. Severe bleeding can itself be life-threatening.
If the stomach acid reaches the small intestine, it can damage the cells of the intestinal lining and break down digestive enzymes before they have a chance to digest food. This can cause diarrhea and weight loss.
Glucagonomas
These tumors make glucagon, a hormone that increases glucose (sugar) levels in the blood. Most of the symptoms that can be caused by a glucagonoma are mild and are more often caused by something else.
Excess glucagon can raise blood sugar, sometimes leading to diabetes. This can cause symptoms such as feeling thirsty and hungry, and having to urinate often.
People with these tumors can also have problems with diarrhea, weight loss, and malnutrition. The nutrition problems can lead to symptoms like irritation of the tongue and the corners of the mouth.
The symptom that brings most people with glucagonomas to their doctor is a rash called necrolytic migratory erythema. This is a red rash with swelling and blisters that often travels from place to place on the skin.
Insulinomas
These tumors make insulin, which lowers blood glucose levels. Too much insulin leads to low blood sugar, which can cause symptoms like weakness, confusion, sweating, and rapid heartbeat. When blood sugar gets very low, it can lead to a person passing out or even going into a coma and having seizures.
Somatostatinomas
These tumors make somatostatin, which helps regulate other hormones. Symptoms of this type of tumor can include belly pain, nausea, poor appetite, weight loss, diarrhea, symptoms of diabetes (feeling thirsty and hungry, and having to urinate often), and jaundice (yellowing of the skin and eyes).
The early symptoms of a somatostatinoma tend to be mild and are more often caused by other things, so these tumors tend to be diagnosed at an advanced stage. Often, they are not found until they spread to the liver, when they cause problems like jaundice and pain.
VIPomas
These tumors make a substance called vasoactive intestinal peptide (VIP). Too much VIP can lead to problems with diarrhea. This may be mild at first, but gets worse over time. By the time they are diagnosed, most people have severe, watery diarrhea.
Other symptoms can include nausea, vomiting, muscle cramps, feeling weak or tired, and flushing (redness and warmth in the face or neck).
People with these tumors also tend to have low levels of acid in their stomachs, which can lead to problems digesting food.
PPomas
These tumors make pancreatic polypeptide (PP), which helps regulate both the exocrine and endocrine pancreas. They can cause problems such as belly pain and an enlarged liver. Some people also get watery diarrhea.
Carcinoid tumors
These tumors often make serotonin or its precursor, 5-HTP. When a pancreatic tumor makes these substances, they first travel to the liver. The liver breaks these substances down before they can reach the rest of the body and cause problems. Because of this, carcinoid tumors often don’t cause symptoms until they spread outside the pancreas.
When these tumors do spread, it is most often to the liver. There, the cancer cells can release hormones directly into the blood leaving the liver. This can cause the carcinoid syndrome, with symptoms including flushing (redness and warmth in the face or neck), diarrhea, wheezing, and a rapid heart rate. These symptoms often occur in episodes, between which the person may feel fine.
Over a long time, the hormone-like substances released by these tumors can damage heart valves, causing shortness of breath, weakness, and a heart murmur (an abnormal heart sound).
Non-functioning neuroendocrine tumors
These tumors don’t make excess hormones, so they don’t cause symptoms in early stages and often grow quite large before they are found. Most of these are cancers and start to cause problems as they get larger or spread outside the pancreas. Symptoms can be like those from exocrine pancreas cancers, including jaundice (yellowing of the eyes and skin), belly pain, and weight loss.
Symptoms caused by the cancer spreading
When pancreatic NETs spread, most often they go to the liver. This can enlarge the liver, which can cause pain and loss of appetite. It can also affect liver function, sometimes leading to jaundice (yellowing of the skin and eyes) and abnormal blood tests.
These cancers can also spread to other organs and tissues. The symptoms depend on where the cancer is growing. For example, cancer spread to the lungs can cause shortness of breath or a cough. Spread to bones can cause pain in those bones.
Pancreatic cancer causes
It’s not clear what causes pancreatic cancer in most cases. Doctors have identified factors, such as smoking, that increase your risk of developing the disease.
Pancreatic cancer occurs when cells in your pancreas develop mutations in their DNA. These mutations cause cells to grow uncontrollably and to continue living after normal cells would die. These accumulating cells can form a tumor. Untreated pancreatic cancer spreads to nearby organs and blood vessels.
Most pancreatic cancer begins in the cells that line the ducts of the pancreas. This type of cancer is called pancreatic adenocarcinoma or pancreatic exocrine cancer. Rarely, cancer can form in the hormone-producing cells or the neuroendocrine cells of the pancreas. These types of cancer are called islet cell tumors, pancreatic endocrine cancer and pancreatic neuroendocrine tumors.
Risk factors for pancreatic cancer
Factors that may increase your risk of pancreatic cancer include:
- Chronic inflammation of the pancreas (pancreatitis)
- Diabetes
- Family history of genetic syndromes that can increase cancer risk, including a BRCA2 gene mutation, Lynch syndrome and familial atypical mole-malignant melanoma (FAMMM) syndrome
- Family history of pancreatic cancer
- Smoking
- Obesity
- Older age, as most people are diagnosed after age 65
A large study demonstrated that the combination of smoking, long-standing diabetes and a poor diet increases the risk of pancreatic cancer beyond the risk of any one of these factors alone.
Complications of pancreatic cancer
As pancreatic cancer progresses, it can cause complications such as:
- Weight loss. A number of factors may cause weight loss in people with pancreatic cancer. The cancer itself may cause weight loss. Nausea and vomiting caused by cancer treatments or a tumor pressing on your stomach may make it difficult to eat. Or your body may have difficulty processing nutrients from food because your pancreas isn’t making enough digestive juices.
Your doctor may recommend pancreatic enzyme supplements to aid in digestion. Try to maintain your weight by adding extra calories where you can and making mealtime as pleasant and relaxed as possible.
- Jaundice. Pancreatic cancer that blocks the liver’s bile duct can cause jaundice. Signs include yellow skin and eyes, dark-colored urine, and pale-colored stools. Jaundice usually occurs without abdominal pain.
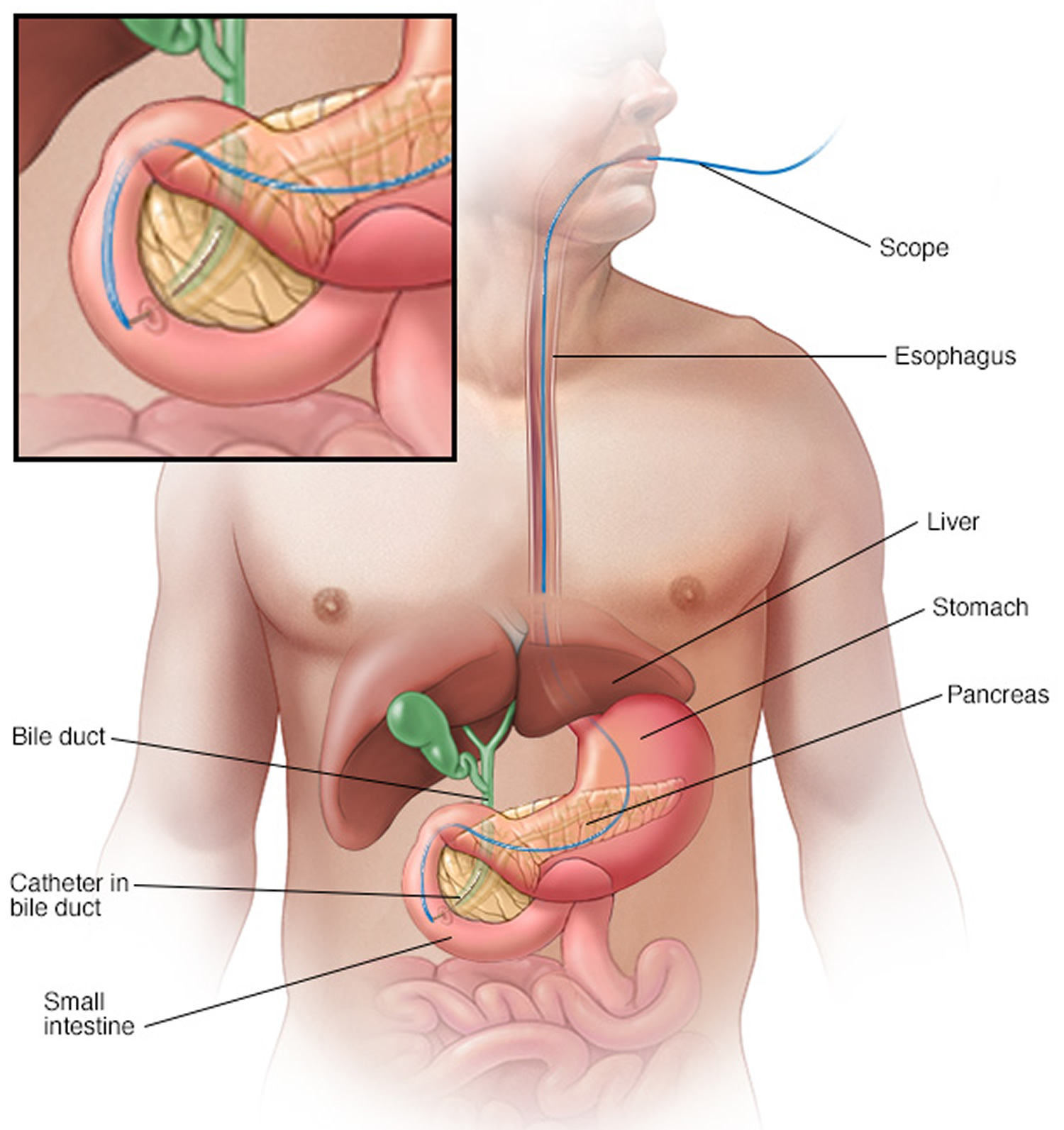
Your doctor may recommend that a plastic or metal tube (stent) be placed inside the bile duct to hold it open. This is done with the help of a procedure called endoscopic retrograde cholangiopancreatography (ERCP). During ERCP an endoscope is passed down your throat, through your stomach and into the upper part of your small intestine. A dye is then injected into the pancreatic and bile ducts through a small hollow tube (catheter) that’s passed through the endoscope.
Figure 5. Endoscopic retrograde cholangiopancreatography (ERCP)
Note: Endoscopic retrograde cholangiopancreatography (ERCP) uses a dye to highlight the bile ducts on X-ray images. A thin, flexible tube (endoscope) with a camera on the end is passed down your throat and into your small intestine. The dye enters the ducts through a small hollow tube (catheter) passed through the endoscope.
Finally, images are taken of the ducts.
- Pain. A growing tumor may press on nerves in your abdomen, causing pain that can become severe. Pain medications can help you feel more comfortable. Radiation therapy might help stop tumor growth temporarily to give you some relief.
In severe cases, your doctor might recommend a procedure to inject alcohol into the nerves that control pain in your abdomen (celiac plexus block). This procedure stops the nerves from sending pain signals to your brain.
- Bowel obstruction. Pancreatic cancer that grows into or presses on the first part of the small intestine (duodenum) can block the flow of digested food from your stomach into your intestines.
Your doctor may recommend a tube (stent) be placed in your small intestine to hold it open. Or surgery may be necessary to attach your stomach to a lower point in your intestines that isn’t blocked by cancer.
Prevention of pancreatic cancer
You may reduce your risk of pancreatic cancer if you:
- Stop smoking. If you smoke, try to stop. Talk to your doctor about strategies to help you stop, including support groups, medications and nicotine replacement therapy. If you don’t smoke, don’t start.
- Maintain a healthy weight. If you are at a healthy weight, work to maintain it. If you need to lose weight, aim for a slow, steady weight loss — 1 to 2 pounds (0.5 to 1 kilogram) a week. Combine daily exercise with a diet rich in vegetables, fruit and whole grains with smaller portions to help you lose weight.
- Choose a healthy diet. A diet full of colorful fruits and vegetables and whole grains may help reduce your risk of cancer.
Consider meeting with a genetic counselor if you have a family history of pancreatic cancer. He or she can review your family health history with you and determine whether you might benefit from a genetic test to understand your risk of pancreatic cancer or other cancers.
Pancreatic cancer diagnosis
If your doctor suspects pancreatic cancer, he or she may have you undergo one or more of the following tests:
- Imaging tests that create pictures of your internal organs. These tests help your doctors visualize your internal organs, including the pancreas. Techniques used to diagnose pancreatic cancer include ultrasound, computerized tomography (CT) scans, magnetic resonance imaging (MRI) and, sometimes, positron emission tomography (PET) scans.
- Using a scope to create ultrasound pictures of your pancreas. An endoscopic ultrasound (EUS) uses an ultrasound device to make images of your pancreas from inside your abdomen. The device is passed through a thin, flexible tube (endoscope) down your esophagus and into your stomach in order to obtain the images.
- Removing a tissue sample for testing (biopsy). A biopsy is a procedure to remove a small sample of tissue for examination under a microscope. Your doctor may obtain a sample of tissue from the pancreas by inserting a needle through your skin and into your pancreas (fine-needle aspiration). Or he or she may remove a sample during EUS, guiding special tools into the pancreas.
- Blood test. Your doctor may test your blood for specific proteins (tumor markers) shed by pancreatic cancer cells. One tumor marker test used in pancreatic cancer is called CA19-9. But the test isn’t always reliable, and it isn’t clear how best to use the CA19-9 test results. Some doctors measure your levels before, during and after treatment.
Computed tomography (CT) scan
The CT scan makes detailed cross-sectional images of your body. CT scans are often used to diagnose pancreatic cancer because they can show the pancreas fairly clearly. They can also help show if cancer has spread to organs near the pancreas, as well as to lymph nodes and distant organs. A CT scan can help determine if surgery might be a good treatment option.
If your doctor thinks you might have pancreatic cancer, you might get a special type of CT known as a multiphase CT scan or a pancreatic protocol CT scan. During this test, different sets of CT scans are taken over several minutes after you get an injection of an intravenous (IV) contrast.
CT-guided needle biopsy: CT scans can also be used to guide a biopsy needle into a suspected pancreatic tumor. But if a needle biopsy is needed, most doctors prefer to use endoscopic ultrasound (described below) to guide the needle into place.
Magnetic resonance imaging (MRI)
MRI scans use radio waves and strong magnets instead of x-rays to create detailed images of parts of your body. Most doctors prefer to look at the pancreas with CT scans, but an MRI might also be done.
Special types of MRI scans can also be used in people who might have pancreatic cancer:
- MR cholangiopancreatography (MRCP), which can be used to look at the pancreatic and bile ducts, is described below in the section on cholangiopancreatography.
- MR angiography (MRA), which looks at blood vessels, is mentioned below in the section on angiography.
Ultrasound
Ultrasound tests use sound waves to create images of organs such as the pancreas.
Abdominal ultrasound: For this test, a wand-shaped probe is moved over the skin of the abdomen. It gives off sound waves and detects the echoes as they bounce off organs. If it’s not clear what might be causing a person’s abdominal symptoms, this might be the first test done because it is easy to do and it doesn’t expose a person to radiation. But if signs and symptoms are more likely to be caused by pancreatic cancer, a CT scan is often more useful.
Endoscopic ultrasound (EUS): This test is more accurate than abdominal ultrasound and can be very helpful in diagnosing pancreatic cancer. This test is done with a small ultrasound probe on the tip of an endoscope, which is a thin, flexible tube that doctors use to look inside the digestive tract.
For this test, you will first be sedated (given medicine to make you sleepy). The scope is then passed through your mouth or nose, down through the stomach, and into the first part of the small intestine. It is then pointed toward the pancreas, which is next to the small intestine. The probe on the tip of the endoscope can get very close to the pancreas, so this is a very good way to look at the pancreas. If a tumor is seen, a small, hollow needle can be passed down the endoscope to get biopsy samples of it.
Cholangiopancreatography
This is an imaging test that looks at the pancreatic ducts and bile ducts to see if they are blocked, narrowed, or dilated. These tests can help show if someone might have a pancreatic tumor that is blocking a duct. They can also be used to help plan surgery. The test can be done in different ways, each of which has pros and cons.
Endoscopic retrograde cholangiopancreatography (ERCP): For this test, an endoscope (a thin, flexible tube with a tiny video camera on the end) is passed down the throat, through the esophagus and stomach, and into the first part of the small intestine. This is usually done while you are sedated (given medicine to make you sleepy).
The doctor can see through the endoscope to find the ampulla of Vater (where the common bile duct empties into the small intestine). The doctor guides a catheter (a very small tube) through the tip of the endoscope and into the common bile duct. A small amount of dye (contrast material) is then injected into the common bile duct, and x-rays are taken. This dye outlines the bile and pancreatic ducts. The x-rays can show narrowing or blockage in these ducts that might be due to pancreatic cancer. The doctor doing this test can also put a small brush through the tube to remove cells for a biopsy (see below).
ERCP can also be used to place a stent (small tube) into a bile or pancreatic duct to keep it open if a nearby tumor is pressing on it. This is described in more detail in the section on palliative surgery in Surgery for pancreatic cancer.
Magnetic resonance cholangiopancreatography (MRCP): This is a non-invasive way to look at the pancreatic and bile ducts using the same type of machine used for standard MRI scans. Unlike ERCP, it does not require an infusion of a contrast dye. Because this test is non-invasive, doctors often use MRCP if the purpose is just to look at the pancreatic and bile ducts. But this test can’t be used to get biopsy samples of tumors or to place stents in ducts.
Percutaneous transhepatic cholangiography (PTC): In this procedure, the doctor puts a thin, hollow needle through the skin of the belly and into a bile duct within the liver. A contrast dye is then injected through the needle, and x-rays are taken as it passes through the bile and pancreatic ducts. As with ERCP, this approach can also be used to take fluid or tissue samples or to place a stent into a duct to help keep it open. Because it is more invasive (and might cause more pain), PTC is not usually used unless ERCP has already been tried or can’t be done for some reason.
Somatostatin receptor scintigraphy (SRS)
This test, also known as OctreoScan, can be very helpful in finding pancreatic neuroendocrine tumors (NETs). A hormone-like substance called octreotide that is bound to a radioactive substance is injected into a vein. Octreotide travels through the blood and attaches to the tumor cells of many types of NETs (although it is less helpful for insulinomas).
Several hours after the injection, a special camera can be used to show where the radioactivity is in the body. More scans may be done on the following few days as well.
This scan can also help decide on treatment. NETs that show up on SRS scans will often stop growing if treated with octreotide.
Positron emission tomography (PET) scan
For a PET scan, you are injected with a slightly radioactive form of sugar, which collects mainly in cancer cells. A special camera is then used to create a picture of areas of radioactivity in the body.
This test is sometimes used to look for spread from exocrine pancreatic cancers, but because NETs grow slowly, they do not show up well on PET scans.
PET/CT scan: Special machines can do both a PET and CT scan at the same time. This lets the doctor compare areas of higher radioactivity on the PET scan with the more detailed appearance of that area on the CT scan. This test can help determine the stage (extent) of the cancer. It might be especially useful for spotting cancer that has spread beyond the pancreas and wouldn’t be treatable by surgery.
Angiography
This is an x-ray test that looks at blood vessels. A small amount of contrast dye is injected into an artery to outline the blood vessels, and then x-rays are taken.
An angiogram can show if blood flow in a particular area is blocked or compressed by a tumor. It can also show abnormal blood vessels (feeding the cancer) in the area. This test can be useful in finding out if a pancreatic cancer has grown through the walls of certain blood vessels. Mainly, it helps surgeons decide if the cancer can be removed completely without damaging vital blood vessels, and it can also help them plan the operation.
Angiography can also be used to look for pancreatic NETs that are too small to be seen on other imaging tests. These tumors cause the body to make more blood vessels to “feed” the tumor, which can often be seen on angiography.
X-ray angiography can be uncomfortable because the doctor has to put a small catheter into the artery leading to the pancreas. Usually the catheter is put into an artery in your inner thigh and threaded up to the pancreas. A local anesthetic is often used to numb the area before inserting the catheter. Once the catheter is in place, the dye is injected to outline all the vessels while the x-rays are being taken.
Angiography can also be done with a CT scanner (CT angiography) or an MRI scanner (MR angiography). These techniques are now used more often because they can give the same information without the need for a catheter in the artery. You might still need an IV line so that a contrast dye can be injected into the bloodstream during the imaging.
Blood tests
Several types of blood tests can be used to help diagnose pancreatic cancer or to help determine treatment options if it is found.
Blood tests for exocrine pancreatic cancers
Liver function tests: Jaundice (yellowing of the skin and eyes) is often one of the first signs of pancreatic cancer, but it can have many causes other than cancer. Doctors often get blood tests to assess liver function in people with jaundice to help determine its cause.
For example, blood tests that look at levels of different kinds of bilirubin (a chemical made by the liver) can help tell whether a patient’s jaundice is caused by disease in the liver itself or by a blockage of bile flow (from a gallstone, a tumor, or other disease).
Tumor markers: Tumor markers are substances that can sometimes be found in the blood when a person has cancer. Two tumor markers may be helpful in pancreatic cancer:
- CA 19-9
- Carcinoembryonic antigen (CEA), which is not used as often as CA 19-9
Neither of these tumor marker tests is accurate enough to tell for sure if someone has pancreatic cancer. Levels of these tumor markers are not high in all people with pancreatic cancer, and some people who don’t have pancreatic cancer might have high levels of these markers for other reasons. Still, these tests can sometimes be helpful, along with other tests, in figuring out if someone has cancer.
In people already known to have pancreatic cancer and who have high CA19-9 or CEA levels, these levels can be measured over time to help tell how well treatment is working. If all of the cancer has been removed, these tests can also be done to look for the cancer coming back.
Other blood tests: Other tests can help evaluate a person’s general health (such as kidney and bone marrow function). These tests can help determine if they’ll be able to withstand the stress of a major operation.
Blood tests for pancreatic neuroendocrine tumors
Blood tests looking at the levels of certain pancreatic hormones can often help diagnose pancreatic neuroendocrine tumors (NETs). Tests might be done to check blood levels of:
- Hormones made by different types of NET cells, such as insulin, gastrin, glucagon, somatostatin, pancreatic polypeptide, and VIP (vasoactive intestinal peptide)
- Chromogranin A (CgA)
- Glucose and C-peptide (for insulinomas)
Carcinoid tumors: For carcinoids, a blood test may be done to look for serotonin, which is made by many of these tumors. The urine might also be tested for serotonin and for related chemicals such as 5-HIAA and 5-HTP.
Other common tests to look for carcinoids include blood tests for chromogranin A (CgA), neuron-specific enolase (NSE), substance P, and gastrin.
Depending on where the tumor might be located and the patient’s symptoms, doctors might do other blood tests as well.
Biopsy
A person’s medical history, physical exam, and imaging test results may strongly suggest pancreatic cancer, but usually the only way to be sure is to remove a small sample of tumor and look at it under the microscope. This procedure is called a biopsy. Biopsies can be done in different ways.
Percutaneous (through the skin) biopsy: For this test, a doctor inserts a thin, hollow needle through the skin over the abdomen and into the pancreas to remove a small piece of a tumor. This is known as a fine needle aspiration (FNA). The doctor guides the needle into place using images from ultrasound or CT scans.
Endoscopic biopsy: Doctors can also biopsy a tumor during an endoscopy. The doctor passes an endoscope (a thin, flexible, tube with a small video camera on the end) down the throat and into the small intestine near the pancreas. At this point, the doctor can either use endoscopic ultrasound (EUS) to pass a needle into the tumor or endoscopic retrograde cholangiopancreatography (ERCP) to remove cells from the bile or pancreatic ducts. These tests are described in more detail above. You will be sedated (made sleepy) for these tests, but general anesthesia (being put into a deep sleep) is not usually needed. Major side effects from these types of biopsies are rare.
Surgical biopsy: Surgical biopsies are now done less often than in the past. They can be useful if the surgeon is concerned the cancer has spread beyond the pancreas and wants to look at (and possibly biopsy) other organs in the abdomen.
The most common way to do a surgical biopsy is to use laparoscopy (sometimes called keyhole surgery). You will be sedated or asleep for this procedure. The surgeon makes several small incisions (cuts) in the abdomen and inserts long, thin instruments. One of these has a small video camera on the end to let the surgeon see inside the abdomen. The surgeon can look at the pancreas and other organs for tumors and take biopsy samples of abnormal areas.
In the past, surgeons often used a laparotomy (a large incision through the skin into the wall of the abdomen) to examine internal organs and take biopsies. But this type of surgery requires a longer recovery and is now rarely used.
Some people might not need a biopsy
Rarely, the doctor might not do a biopsy on someone who has a tumor in the pancreas if imaging tests show the tumor is very likely to be cancer and if it looks like surgery can remove all of it. Instead, the doctor will proceed with surgery, at which time the tumor cells can be looked at to confirm the diagnosis. During surgery, if the doctor finds that the cancer has spread too far to be removed completely, only a sample of the cancer may be removed to confirm the diagnosis, and the rest of the planned operation will be stopped.
If treatment (such as chemotherapy or radiation) is planned before surgery, a biopsy is needed first to be sure of the diagnosis.
If your doctor confirms a diagnosis of pancreatic cancer, he or she tries to determine the extent (stage) of the cancer. Using information from staging tests, your doctor assigns your pancreatic cancer a stage, which helps determine what treatments are available to you.
Don’t hesitate to ask your doctor about his or her experience with diagnosing pancreatic cancer. If you have any doubts, get a second opinion.
Pancreatic cancer stages
After someone is diagnosed with pancreatic cancer, doctors will try to figure out if it has spread, and if so, how far. This process is called staging. The stage of a cancer describes how much cancer is in the body. It helps determine how serious the cancer is and how best to treat it. Doctors also use a cancer’s stage when talking about survival statistics.
The earliest stage pancreas cancers are stage 0 (carcinoma in situ), and then range from stages I (1) through IV (4). As a rule, the lower the number, the less the cancer has spread. A higher number, such as stage IV, means a more advanced cancer. Cancers with similar stages tend to have a similar outlook and are often treated in much the same way.
How is the stage determined?
The staging system used most often for pancreatic cancer is the American Joint Committee on Cancer (AJCC) TNM system, which is based on 3 key pieces of information:
- The extent of the tumor (T): How large is the tumor and has it grown outside the pancreas into nearby blood vessels?
- The spread to nearby lymph nodes (N): Has the cancer spread to nearby lymph nodes? If so, how many of the lymph nodes have cancer?
- The spread (metastasized) to distant sites (M): Has the cancer spread to distant lymph nodes or distant organs such as the liver, peritoneum (the lining of the abdominal cavity), lungs or bones?
The system described below is the most recent American Joint Committee on Cancer system, effective January 2018. It is used to stage most pancreatic cancers except for well-differentiated pancreatic neuroendocrine tumors (NETs), which have their own staging system.
The staging system in the table uses the pathologic stage. It is determined by examining tissue removed during an operation. This is also known as the surgical stage. Sometimes, if the doctor’s physical exam, imaging, or other tests show the tumor is too large or has spread to nearby organs and cannot be removed by surgery right away or at all, radiation or chemotherapy might be given first. In this case, the cancer will have a clinical stage. It is based on the results of physical exam, biopsy, and imaging tests (see Tests for Pancreatic Cancer). The clinical stage can be used to help plan treatment. Sometimes, though, the cancer has spread further than the clinical stage estimates, and may not predict the patient’s outlook as accurately as a pathologic stage. For more information, see Cancer Staging.
Numbers or letters after T, N, and M provide more details about each of these factors. Higher numbers mean the cancer is more advanced. Once a person’s T, N, and M categories have been determined, this information is combined in a process called stage grouping to assign an overall stage.
Cancer staging can be complex. If you have any questions about your stage, please ask your doctor to explain it to you in a way you understand. (Additional information of the TNM system also follows the stage table below.)
Table 1. Stages of pancreatic cancer
| AJCC Stage | Stage grouping | Stage description* |
| 0 | Tis N0 M0 | The cancer is confined to the top layers of pancreatic duct cells and has not invaded deeper tissues. It has not spread outside of the pancreas. These tumors are sometimes referred to as carcinoma in situ (Tis). It has not spread to nearby lymph nodes (N0) or to distant sites (M0). |
| IA | T1 N0 M0 | The cancer is confined to the pancreas and is no bigger than 2 cm (0.8 inch) across (T1). It has not spread to nearby lymph nodes (N0) or to distant sites (M0). |
| IB | T2 N0 M0 | The cancer is confined to the pancreas and is larger than 2 cm (0.8 inch) but no more than 4cm (1.6 inches) across (T2). It has not spread to nearby lymph nodes (N0) or to distant sites (M0). |
| IIA | T3 N0 M0 | The cancer is confined to the pancreas and is bigger than 4 cm (1.6 inches) across (T3). It has not spread to nearby lymph nodes (N0) or to distant sites (M0). |
| IIB
| T1 N1 M0 | The cancer is confined to the pancreas and is no bigger than 2 cm (0.8 inch) across (T1) AND it has spread to no more than 3 nearby lymph nodes (N1). It has not spread to distant sites (M0). |
| T2 N1 M0 | The cancer is confined to the pancreas and is larger than 2 cm (0.8 inch) but no more than 4cm (1.6 inches) across (T2) AND it has spread to no more than 3 nearby lymph nodes (N1). It has not spread to distant sites (M0). | |
| T3 N1 M0 | The cancer is confined to the pancreas and is bigger than 4 cm (1.6 inches) across (T3) AND it has spread to no more than 3 nearby lymph nodes (N1). It has not spread to distant sites (M0). | |
| III | T1 N2 M0 | The cancer is confined to the pancreas and is no bigger than 2 cm (0.8 inch) across (T1) AND it has spread to 4 or more nearby lymph nodes (N2). It has not spread to distant sites (M0). |
| OR | ||
| T2 N2 M0 | The cancer is confined to the pancreas and is larger than 2 cm (0.8 inch) but no more than 4cm (1.6 inches) across (T2) AND it has spread to 4 or more nearby lymph nodes (N2). It has not spread to distant sites (M0). | |
| OR | ||
| T3 N2 M0 | The cancer is confined to the pancreas and is bigger than 4 cm (1.6 inches) across (T3) AND it has spread to 4 or more nearby lymph nodes (N2). It has not spread to distant sites (M0). | |
| OR | ||
| T4 Any N M0 | The cancer is growing outside the pancreas and into nearby major blood vessels (T4). The cancer may or may not have spread to nearby lymph nodes (Any N). It has not spread to distant sites (M0). | |
| IV | Any T Any N M1 | The cancer has spread to distant sites such as the liver, peritoneum (the lining of the abdominal cavity), lungs or bones (M1). It can be any size (Any T) and might or might not have spread to nearby lymph nodes (Any N). |
* The following additional categories are not listed on the table above:
- TX: Main tumor cannot be assessed due to lack of information.
- T0: No evidence of a primary tumor.
- NX: Regional lymph nodes cannot be assessed due to lack of information.
Other prognostic factors
Although not formally part of the TNM system, other factors are also important in determining a person’s prognosis (outlook).
Tumor grade
The grade describes how closely the cancer looks like normal tissue under a microscope.
- Grade 1 (G1) means the cancer looks much like normal pancreas tissue.
- Grade 3 (G3) means the cancer looks very abnormal.
- Grade 2 (G2) falls somewhere in between.
Low-grade cancers (G1) tend to grow and spread more slowly than high-grade (G3) cancers. Most of the time, Grade 3 pancreas cancers tend to have a poor prognosis (outlook) compared to Grade 1 or 2 cancers.
Extent of resection
For patients who have surgery, another important factor is the extent of the resection — whether or not all of the tumor is removed:
- R0: All of the cancer is thought to have been removed. (There are no visible or microscopic signs suggesting that cancer was left behind.)
- R1: All visible tumor was removed, but lab tests of the removed tissue show that some small areas of cancer were probably left behind.
- R2: Some visible tumor could not be removed.
Resectable versus unresectable pancreatic cancer
The AJCC staging system gives a detailed summary of how far the cancer has spread. But for treatment purposes, doctors use a simpler staging system, which divides cancers into groups based on whether or not they can be removed (resected) with surgery:
- Resectable
- Borderline resectable
- Unresectable (either locally advanced or metastatic)
Resectable
If the cancer is only in the pancreas (or has spread just beyond it) and the surgeon believes the entire tumor can be removed, it is called resectable. (In general, this would include most stage IA, IB, and IIA cancers in the TNM system.)
It’s important to note that some cancers might appear to be resectable based on imaging tests, but once surgery is started it might become clear that not all of the cancer can be removed. If this happens, only some of the cancer may be removed to confirm the diagnosis (if a biopsy hasn’t been done already), and the rest of the planned operation will be stopped to help avoid the risk of major side effects.
Borderline resectable
This term is used to describe some cancers that might have just reached nearby blood vessels, but which the doctors feel might still be removed completely with surgery.
Unresectable
These cancers can’t be removed entirely by surgery.
Locally advanced: If the cancer has not yet spread to distant organs but it still can’t be removed completely with surgery, it is called locally advanced. Often the reason the cancer can’t be removed is because it has grown into or surrounded nearby major blood vessels. (This would include some stage III cancers in the TNM system.)
Surgery to try to remove these tumors would be very unlikely to be helpful and could still have major side effects. Some type of surgery might still be done, but it would be a less extensive operation with the goal of preventing or relieving symptoms or problems like a blocked bile duct or intestinal tract, instead of trying to cure the cancer.
Metastatic: If the cancer has spread to distant organs, it is called metastatic (Stage IV). These cancers can’t be removed completely. Surgery might still be done, but the goal would be to prevent or relieve symptoms, not to try to cure the cancer.
Tumor markers (CA 19-9)
Tumor markers are substances that can sometimes be found in the blood when a person has cancer. CA 19-9 is a tumor marker that may be helpful in pancreatic cancer. A drop in the CA 19-9 level after surgery (compared to the level before surgery) and low levels of CA 19-9 after pancreas surgery tend to predict a better prognosis (outlook).
Pancreatic Neuroendocrine Tumor Stages
After someone is diagnosed with a pancreatic neuroendocrine tumor (NET), doctors will try to figure out if it has spread, and if so, how far. This process is called staging. The stage of a cancer describes how much cancer is in the body. It helps determine how serious the cancer is and how best to treat it. Doctors also use a cancer’s stage when talking about survival statistics.
The stages of pancreatic NET range from I (1) through IV (4). As a rule, the lower the stage, the less the cancer has spread. A higher number, such as stage IV, means cancer has spread more. Although each person’s cancer experience is unique, cancers with similar stages tend to have a similar outlook and are often treated in much the same way.
How is the stage determined?
The staging system most often used for pancreatic NETs is the American Joint Committee on Cancer (AJCC) TNM system, which is based on 3 key pieces of information:
- The size and extent of the main tumor (T): How large is the tumor? Has it grown into nearby structures or organs?
- The spread to nearby lymph nodes (N): Has the cancer spread to nearby lymph nodes?
- The spread (metastasis) to distant sites (M): Has the cancer spread to distant organs? (The most common site of spread is the liver.)
Numbers or letters after T, N, and M provide more details about each of these factors. Higher numbers mean the cancer is more advanced. Once a person’s T, N, and M categories have been determined, this information is combined in a process called stage grouping to assign an overall stage.
The system described below is the most recent version of the AJCC system, effective as of January 2018. It is used to stage well-differentiated pancreatic NETs, but not high-grade pancreatic NETs (known as neuroendocrine carcinomas) or other types of pancreatic cancer, which have their own staging system.
Pancreatic NETs are typically given a clinical stage based on the results of a physical exam, biopsy, and imaging tests (as described in Tests for Pancreatic Cancer). If surgery is done, the pathologic stage (also called the surgical stage) is determined by examining tissue removed during the operation.
Staging for pancreatic NETs can be complex. If you have any questions about the stage of your cancer or what it means, please ask your doctor to explain it to you in a way you understand.
Table 2. Stages of pancreatic neuroendocrine tumors
| AJCC Stage | Stage grouping | Stage description* |
| I | T1 N0 M0 | The tumor is less than 2 centimeters (cm) across and is still just in the pancreas (T1). The cancer has not spread to nearby lymph nodes (N0) or to distant parts of the body (M0). |
|
II | T2 N0 M0 | The tumor is at least 2 cm across but no more than 4 cm across, and it is still just in the pancreas (T2). The cancer has not spread to nearby lymph nodes (N0) or to distant parts of the body (M0). |
| OR | ||
| T3 N0 M0 | The tumor is more than 4 cm across and is still just in the pancreas, OR the tumor has grown into the duodenum (the first part of the small intestine) or the common bile duct (T3). The cancer has not spread to nearby lymph nodes (N0) or to distant parts of the body (M0). | |
|
III | T4 N0 M0 | The tumor has grown into nearby organs (such as the stomach, spleen, colon, or adrenal gland) or it has grown into nearby large blood vessels (T4). The cancer has not spread to nearby lymph nodes (N0) or to distant parts of the body (M0). |
| OR | ||
| Any T N1 M0 | The tumor can be any size and might or might not have grown outside of the pancreas (any T). It has spread to nearby lymph nodes (N1), but not to distant parts of the body (M0). | |
| IV | Any T Any N M1 | The tumor can be any size and might or might not have grown outside of the pancreas (any T). It might or might not have spread to nearby lymph nodes (any N). The cancer has spread to distant parts of the body (M1). |
* The following additional categories are not listed in the table above:
- TX: The main tumor cannot be assessed due to lack of information.
- T0: There is no evidence of a main tumor.
- NX: Nearby lymph nodes cannot be assessed due to lack of information.
Other prognostic factors
Although not formally part of the TNM system, other factors can also be important in determining a person’s prognosis (outlook).
Tumor grade
The grade describes how quickly the cancer is likely to grow and spread. For pancreatic NETs, an important part of grading is measuring how many of the cells are in the process of dividing into new cells. This is determined by:
- The mitotic count, which is the number of cells seen under a microscope that are in the process of splitting into two new cells (mitosis).
- The Ki-67 index, which is a measure of the portion of cells that are almost ready to start splitting.
Based on these tests, NETs are divided into 2 main groups:
- Well-differentiated NETs (which include low-grade [G1] and intermediate-grade [G2] tumors) have 20 or fewer mitoses and a Ki-67 index of 20% or lower.
- Poorly differentiated tumors (high-grade [G3] tumors) have more than 20 mitoses or a Ki-67 index of more than 20%. These are also called neuroendocrine carcinomas (NECs), and they often grow and spread quickly.
Tumor functionality
The outlook for pancreatic NETs can be affected by whether the tumor is functioning (making hormones) or non-functioning. For functioning tumors, the type of hormone can also be important. For example, insulinomas (NETs that make insulin) tend to have a lower risk of spreading than other types of NETs.
Pancreatic cancer treatment
Treatment for pancreatic cancer depends on the stage and location of the cancer as well as on your overall health and personal preferences. For most people, the first goal of pancreatic cancer treatment is to eliminate the cancer, when possible. When that isn’t an option, the focus may be on improving your quality of life and preventing the cancer from growing or causing more harm.
Treatment may include surgery, radiation, chemotherapy or a combination of these. When pancreatic cancer is advanced and these treatments aren’t likely to offer a benefit, your doctor will offer symptom relief (palliative care) that makes you as comfortable as possible.
Pancreatic cancer surgery
The type of surgery you need depends on where the cancer is in your pancreas.
To find out if it might be possible to remove the cancer, your surgeon will look at:
- the size of the tumor
- where it is in the pancreas
- whether the cancer has grown into the tissues around the pancreas
- whether the cancer is in any of the lymph nodes around the pancreas
- whether the cancer has grown into the major blood vessels in or around the pancreas
- whether the cancer has spread to any other parts of the body
Operations used in people with pancreatic cancer include:
- Surgery for tumors in the pancreatic head. If your cancer is located in the head of the pancreas, you may consider an operation called a Whipple procedure (pancreaticoduodenectomy). The Whipple procedure is technically difficult operation to remove the head of the pancreas, the first part of the small intestine (duodenum), the gallbladder and part of the bile duct. In some situations, part of the stomach and nearby lymph nodes may be removed as well. Your surgeon reconnects the remaining parts of your pancreas, stomach and intestines to allow you to digest food.
- Surgery for tumors in the pancreatic body and tail. Surgery to remove the left side (body and tail) of the pancreas is called distal pancreatectomy. Your surgeon may also remove your spleen.
- Surgery to remove the entire pancreas. In some people, the entire pancreas may need to be removed. This is called total pancreatectomy. You can live relatively normally without a pancreas but do need lifelong insulin and enzyme replacement.
- Surgery for tumors affecting nearby blood vessels. Many people with advanced pancreatic cancer are not considered eligible for the Whipple procedure or other pancreatic surgeries if their tumors involve nearby blood vessels. At a very few medical centers in the United States, highly specialized and experienced surgeons will safely perform these operations with removal and reconstruction of parts of blood vessels in select patients.
Each of these surgeries carries the risk of bleeding and infection. After surgery some people experience nausea and vomiting if the stomach has difficulty emptying (delayed gastric emptying). Expect a long recovery after any of these procedures. You’ll spend several days in the hospital and then recover for several weeks at home.
Extensive research shows pancreatic cancer surgery tends to cause fewer complications when done by highly experienced surgeons at centers that do many of these operations. Don’t hesitate to ask about your surgeon’s and hospital’s experience with pancreatic cancer surgery. If you have any doubts, get a second opinion.
Chemotherapy
Chemotherapy uses drugs to help kill cancer cells. These drugs can be injected into a vein or taken orally. You may receive one chemotherapy drug or a combination of them.
Many different chemo drugs can be used to treat pancreatic cancer, including:
- Gemcitabine (Gemzar)
- 5-fluorouracil (5-FU)
- Irinotecan (Camptosar)
- Oxaliplatin (Eloxatin)
- Albumin-bound paclitaxel (Abraxane)
- Capecitabine (Xeloda)
- Cisplatin
- Paclitaxel (Taxol)
- Docetaxel (Taxotere)
- Irinotecan liposome (Onivyde)
In people who are healthy enough, 2 or more drugs are usually given together. For people who are not healthy enough for combined treatments, a single drug (usually gemcitabine, 5-FU, or capecitabine) can be used.
There are different types of chemotherapy, most people have one of the following:
- gemcitabine with capecitabine
- gemcitabine with nab paclitaxel
- gemcitabine on its own
- FOLIFIRINOX
Doctors give chemo in cycles, with each period of treatment followed by a rest period to allow the body time to recover. Each chemo cycle typically lasts for a few weeks.
Chemotherapy can also be combined with radiation therapy (chemoradiation). Chemoradiation is typically used to treat cancer that has spread beyond the pancreas, but only to nearby organs and not to distant regions of the body. At specialized medical centers, this combination may be used before surgery to help shrink the tumor. Sometimes it is used after surgery to reduce the risk that pancreatic cancer may recur.
In people with advanced pancreatic cancer, chemotherapy is often used to control cancer growth and prolong survival.
Targeted therapy for pancreatic cancer
As researchers have learned more about the changes in pancreatic cancer cells that help them grow, they have developed newer drugs to specifically target these changes. These targeted drugs work differently from standard chemo drugs. Sometimes they work when standard chemo drugs don’t, and they often have different (and less severe) side effects.
Erlotinib (Tarceva) is a drug that targets a protein on cancer cells called EGFR, which normally helps the cells grow. In people with advanced pancreatic cancer, this drug can be given along with the chemo drug gemcitabine. Some people may benefit more from this combination than others. Common side effects of erlotinib include an acne-like rash on the face and neck, diarrhea, loss of appetite, and feeling tired.
Radiation therapy
Radiation therapy uses high-energy beams, such as those made from X-rays and protons, to destroy cancer cells. You may receive radiation treatments before or after cancer surgery, often in combination with chemotherapy. Or your doctor may recommend a combination of radiation and chemotherapy treatments when your cancer can’t be treated surgically.
Radiation therapy usually comes from a machine that moves around you, directing radiation to specific points on your body (external beam radiation). In specialized medical centers, radiation therapy may be delivered during surgery (intraoperative radiation).
Radiation therapy traditionally uses X-rays to treat cancer. Some medical centers offer proton beam radiation therapy, which may be a treatment option for some people with advanced pancreatic cancer.
Clinical trials
Clinical trials are studies to test new treatments, such as systemic therapy, and new approaches to surgery or radiation therapy. If the treatment being studied proves to be safer and more effective than are current treatments, it can become the new standard of care.
Clinical trials for pancreatic cancer might give you a chance to try new targeted therapy, chemotherapy drugs, immunotherapy treatments or vaccines.
Clinical trials can’t guarantee a cure, and they might have serious or unexpected side effects. On the other hand, cancer clinical trials are closely monitored to ensure they’re conducted as safely as possible. And they offer access to treatments that wouldn’t otherwise be available to you.
Talk to your doctor about what clinical trials might be appropriate for you.
Pancreatic cancer diet
Having cancer of the pancreas will affect your eating and drinking habits, whatever your stage of cancer or treatment. Many people with pancreatic cancer lose weight. The pancreas is not only close to the stomach and bowel, it produces insulin and enzymes which help to digest food.
If you’ve had all or part of your pancreas removed, you may need to take insulin or tablets to regulate your blood sugar. You may also need to take enzyme supplements when you eat to help your digestion.
Blood sugar
If you are on insulin or tablets to regulate your blood sugar, your doctor will ask you to check your urine for sugar. Too much sugar in the urine indicates that the sugar balance of your body is not yet right.
If you are on insulin, you will probably also have to test your blood sugar levels. You will have to prick your finger and squeeze a drop of blood onto a test strip. This will show how much sugar is in your blood. You will then know how much insulin to take.
It takes time to get used to doing these tests. You will be shown how to do it before you leave hospital.
You may also have a nurse to visit you at home to help you and answer your questions.
Enzyme supplements
Digestive enzymes help your body to break down and absorb fats and proteins. Without enough enzymes, you may have diarrhoea or your poo (stools) may float, look pale and smell offensive. This is due to the undigested fat in the stool.
It might be difficult to put on weight as you are unable to absorb the nutrients from your food. If your pancreas is not working properly due to the cancer or you’ve had all or part of your pancreas removed, you may need to take enzyme supplements to reduce these effects.
Types of enzyme supplements
There are several different types of enzyme supplement. Creon is the most commonly used. The dose depends on:
- how well the remaining part of your pancreas is working
- your diet
You might need to take more enzymes if you are about to eat a large or fatty meal.
How to take them
You swallow the enzyme capsules whole, immediately before your meal. If you find it difficult to swallow capsules, you can open them and mix the granules in soft acidic foods that are at room temperature and easy to swallow. This can include apple sauce or mashed banana.
You must not chew or crush the granules. Have a drink of water afterwards to make sure none of the granules stay in your mouth as they can irritate the lining and cause mouth ulcers.
Your dietician will give you a diet plan to suit you and advise you on taking the supplements. It can take a bit of time to get the right dose of enzymes for you.
Snacks and small meals
You may find it easier to have lots of small meals through the day, rather than sticking to the traditional three meals a day.
It is a good idea to have plenty of nutritious snacks to hand that you can have whenever you feel like eating. If you can manage it, it’s best to choose full fat versions of yoghurts and puddings, so that you get the most calories.
You could try:
- yoghurts or fromage frais
- other soft puddings such as trifle or chocolate mousse
- dried fruit
- stewed or fresh fruit (bananas are high in calories)
- nuts
- cheese
- instant soups (make up with milk to boost calories)
- cereal
- milky drinks
- flapjacks
Some of these ideas may not suit your digestion but they might be worth a try. If in doubt, check with your dietitian.
Try to think of quick ways of having the things you like to eat. If possible, get someone to prepare your favourite foods in advance and freeze them in small portions. A microwave makes defrosting and heating easier and quicker.
Managing diarrhea
If you have diarrhea after pancreatic surgery, it is probably related to difficulty digesting fat. Avoid very high fibre foods (such as cereal and dried fruit) for a time as these may make things worse. Tell your doctor, nurse or dietitian.
You may need some medicines to control your symptoms. If you’re taking enzyme supplements, your dietitian may need to alter the dose. They can also suggest some changes to your diet that may help.
Nutritional supplements
If you are finding it hard to eat, there are plenty of nutritional supplements available on prescription. Some are powders you sprinkle on your food and some are drinks that are complete meals in themselves.
Sipping a supplement between meals throughout the day can really boost your calorie intake. Again, ask your doctor or dietitian.
Supportive (palliative) care
Palliative care is specialized medical care that focuses on providing relief from pain and other symptoms of a serious illness. Palliative care specialists work with you, your family and your other doctors to provide an extra layer of support that complements your ongoing care. Palliative care can be used while undergoing aggressive treatments, such as surgery, chemotherapy and radiation therapy.
When palliative care is used along with other appropriate treatments — even soon after the diagnosis — people with cancer may feel better and live longer.
Palliative care is provided by teams of doctors, nurses and other specially trained professionals. These teams aim to improve the quality of life for people with cancer and their families. Palliative care is not the same as hospice care or end-of-life care.
Treatments to help you cope with distress
People with cancer frequently experience distress. Some research suggests distress is more common in people with pancreatic cancer than it is in people with other types of cancer.
If you’re distressed, you may have difficulty sleeping and find yourself constantly thinking about your cancer. You may feel angry or sad.
Discuss your feelings with your doctor. Specialists can help you sort through your feelings and help you devise strategies for coping. In some cases, medications may help.
Integrative medicine and alternative therapies may also help you cope with distress. Examples include:
- Art therapy
- Exercise
- Meditation
- Music therapy
- Relaxation exercises
- Spirituality
Talk with your doctor if you’re interested in these treatment options.
Coping and support
Learning you have a life-threatening illness can be devastating. Some of the following suggestions may help:
- Learn what you need to know about your cancer. Learn enough about your cancer to help you make decisions about your care. Ask your doctor about the details of your cancer and your treatment options. Ask about trusted sources of further information. If you’re doing your own research, good places to start include the National Cancer Institute and the Pancreatic Cancer Action Network.
- Assemble a support system. Ask your friends and family to form a support network for you. They may feel helpless and uncertain after your diagnosis. Helping you with simple tasks might give them comfort. And you might find relief in not having to worry about certain tasks. Think of things you want help with, such as meal preparation or getting to appointments.
- Find someone to talk with. Although friends and family can be your best allies, in some cases they have difficulty coping with the shock of your diagnosis. In these cases, talking with a counselor, medical social worker, or a pastoral or religious counselor can be helpful. Ask your doctor for a referral.
- Connect with other cancer survivors. You may find comfort in talking with other cancer survivors. Contact your local chapter of the American Cancer Society to find cancer support groups in your area. The Pancreatic Cancer Action Network can connect you with a pancreatic cancer survivor who can provide support by phone or email.
- Consider hospice. Hospice care provides comfort and support to terminally ill people and their loved ones. It allows family and friends — with the aid of nurses, social workers and trained volunteers — to care for and comfort a loved one at home or in a hospice residence. Hospice care also provides emotional, social and spiritual support for people who are ill and those closest to them.
- Pancreatic Cancer Survival Rates, by Stage. https://www.cancer.org/cancer/pancreatic-cancer/detection-diagnosis-staging/survival-rates.html[↩]
- Cancer Stat Facts: Pancreatic Cancer. https://seer.cancer.gov/statfacts/html/pancreas.html[↩][↩]
- Pancreatic Cancer Stages. https://www.cancer.org/cancer/pancreatic-cancer/detection-diagnosis-staging/staging.html[↩]
- Pancreatic Neuroendocrine Tumor Stages. https://www.cancer.org/cancer/pancreatic-cancer/detection-diagnosis-staging/net-staging.html[↩]