Contents
What is polypectomy
Polypectomy is the complete removal of the polyps or adenoma.
Colonoscopic polypectomy
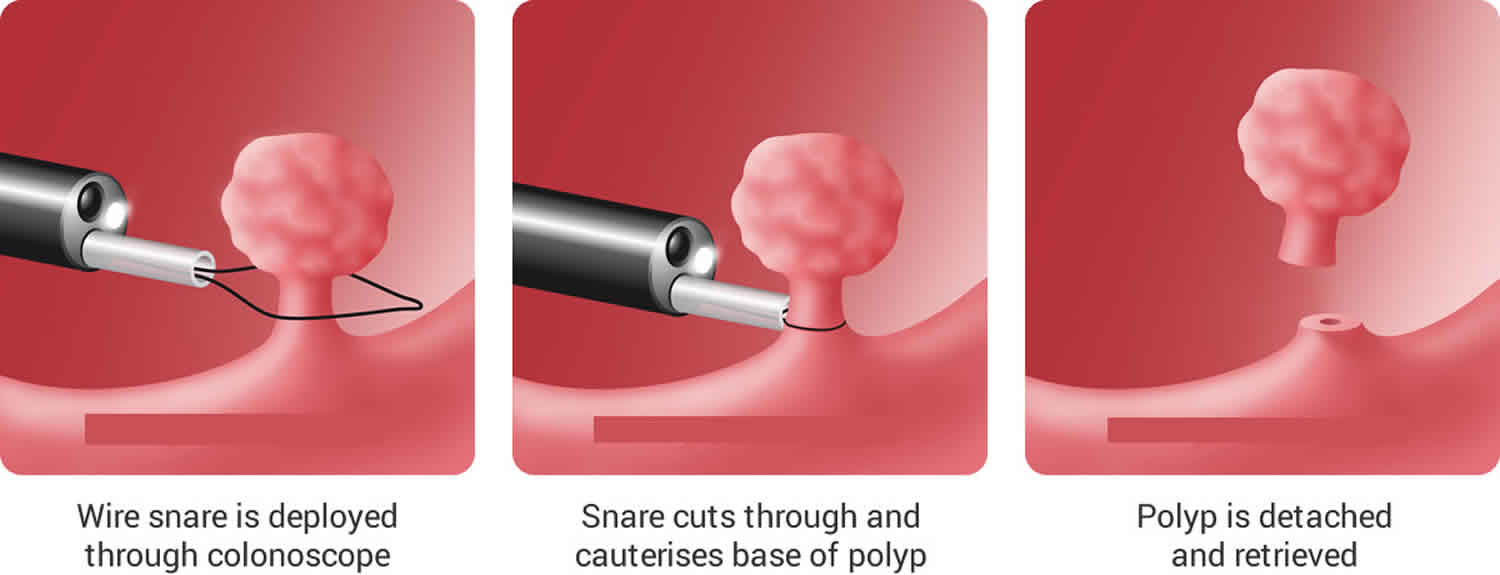
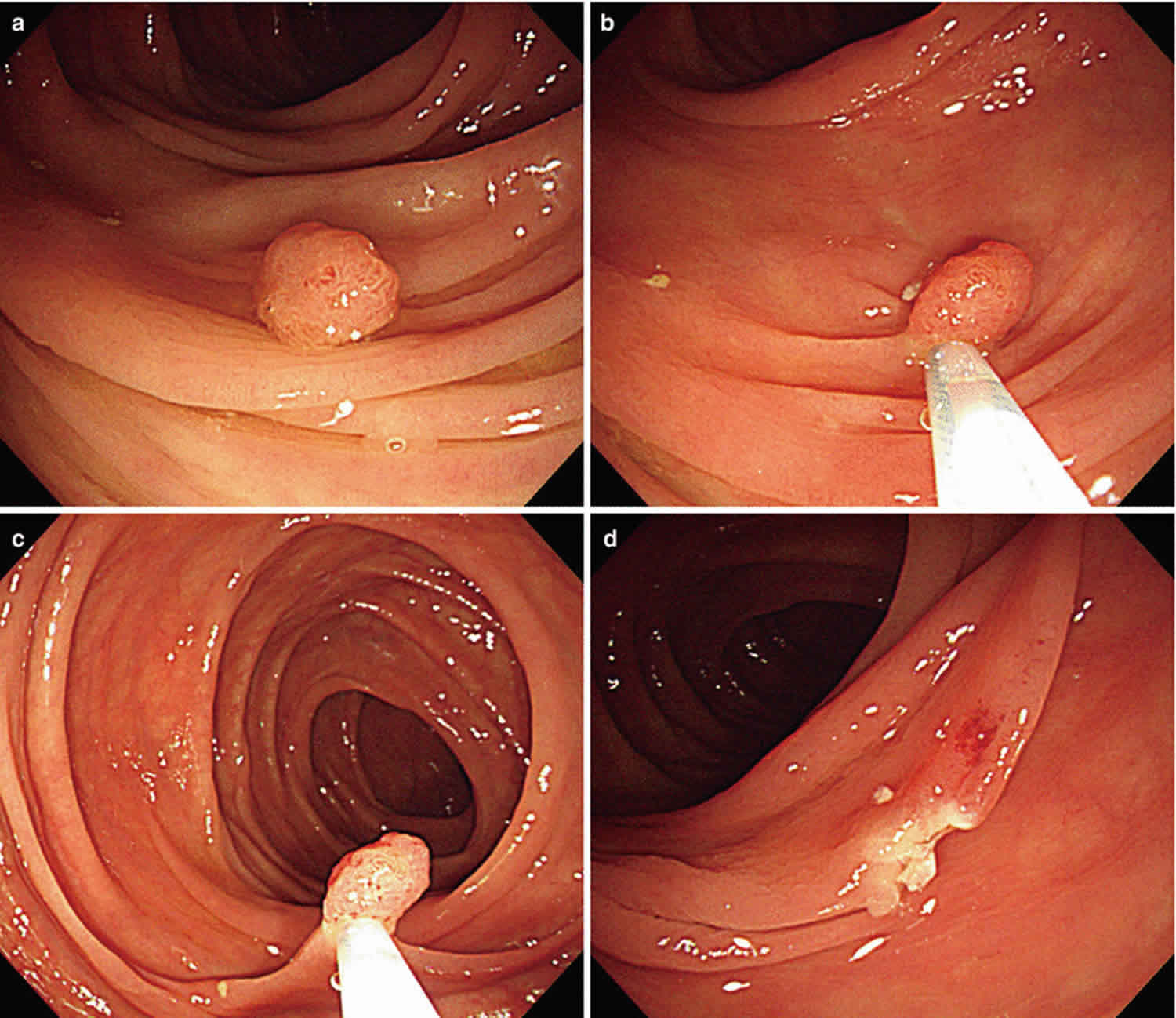
The colonoscopy involves passing a flexible tube called a colonoscope through your bottom and up into your bowel. The colonoscope has a wire attached to it with an electric current through it. This wire is used to either burn off (cauterise) or cut off (snare) the polyp. Both of these methods are painless.
After the polyp or polyps have been removed, they are sent to specialists in a laboratory, who will inform your consultant if:
- the polyp has been completely removed
- there is any risk of it regrowing
- there is any cancerous change in the polyp
If there is a cancerous change in the polyp, you may need further treatment (depending on the degree and extent of change). Your specialist will be able to advise you on this.
Figure 1. Colonoscopic polypectomy
Nasal polypectomy
Nasal polypectomy is a procedure performed to remove nose polyps, which are non-cancerous swellings or masses in the lining of the nose and paranasal sinuses. Large polyps or clusters of polyps can cause breathing difficulties, affect the patient’s sense of smell and can cause frequent infections and other problems.
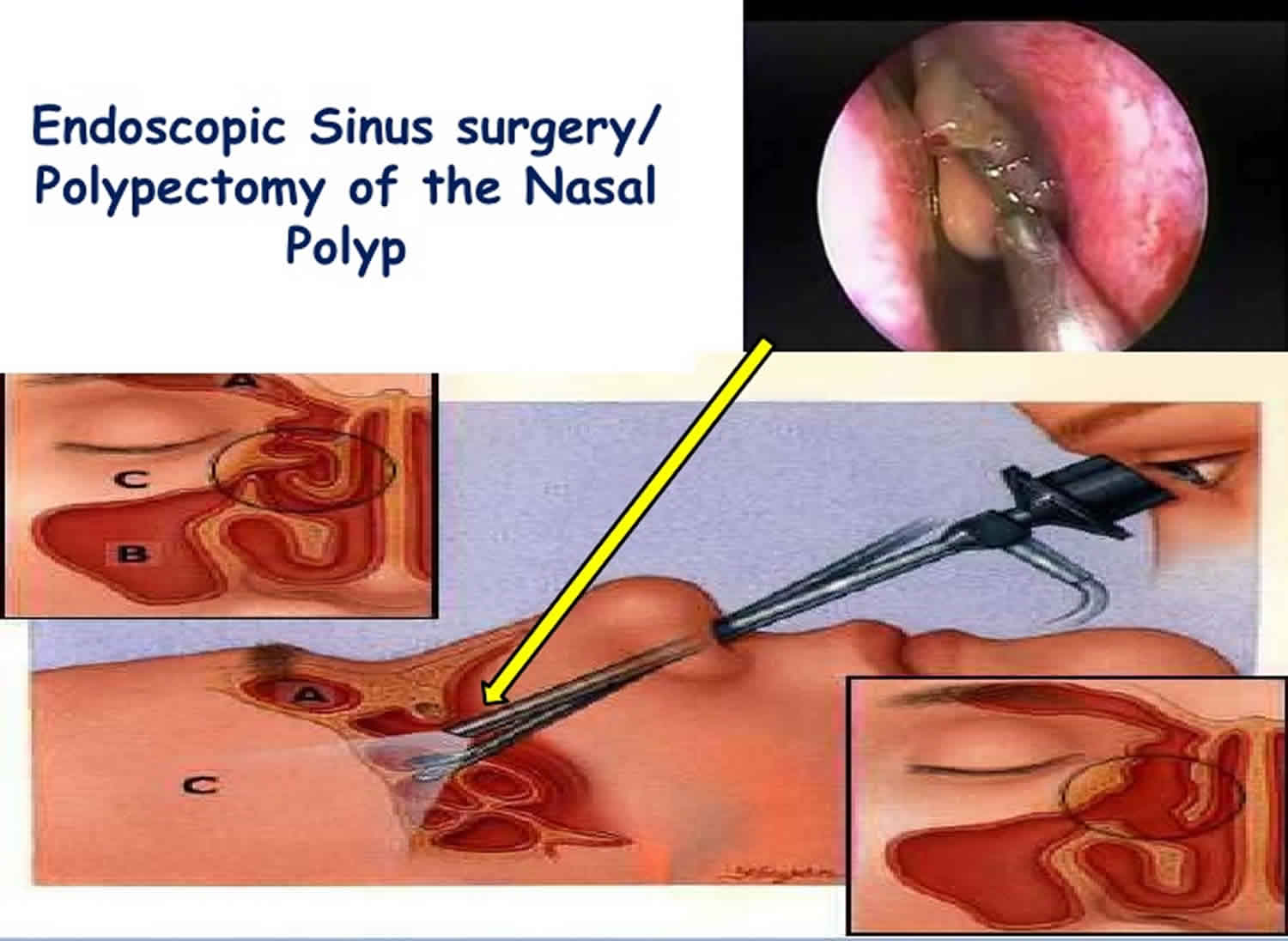
A nasal polypectomy is done general anesthesia and it is often done in association with endoscopic sinus surgery. The procedure involves the introduction of telescopes into the nose. A variety of specialty instruments are used to remove polyps in nose cavities and open the drainpipes from the sinuses leading back into the nose.
Nasal polypectomy operation takes approximately an hour and is performed under a general anesthetic in hospital. Nine out of ten people wake up without any wadding or packing in the nose, while one in ten people need some sort of absorbable packing left in the nose overnight.
It involves one night of hospitalization and usually one week of reduced physical activity to aid the healing process.
People who have had a nasal polypectomy are reviewed at three months, six months and then annually for life to ensure that the polyps do not recur or, if they do, facilitate early treatment for optimal results.
Figure 2. Nasal polypectomy
Hysteroscopic polypectomy
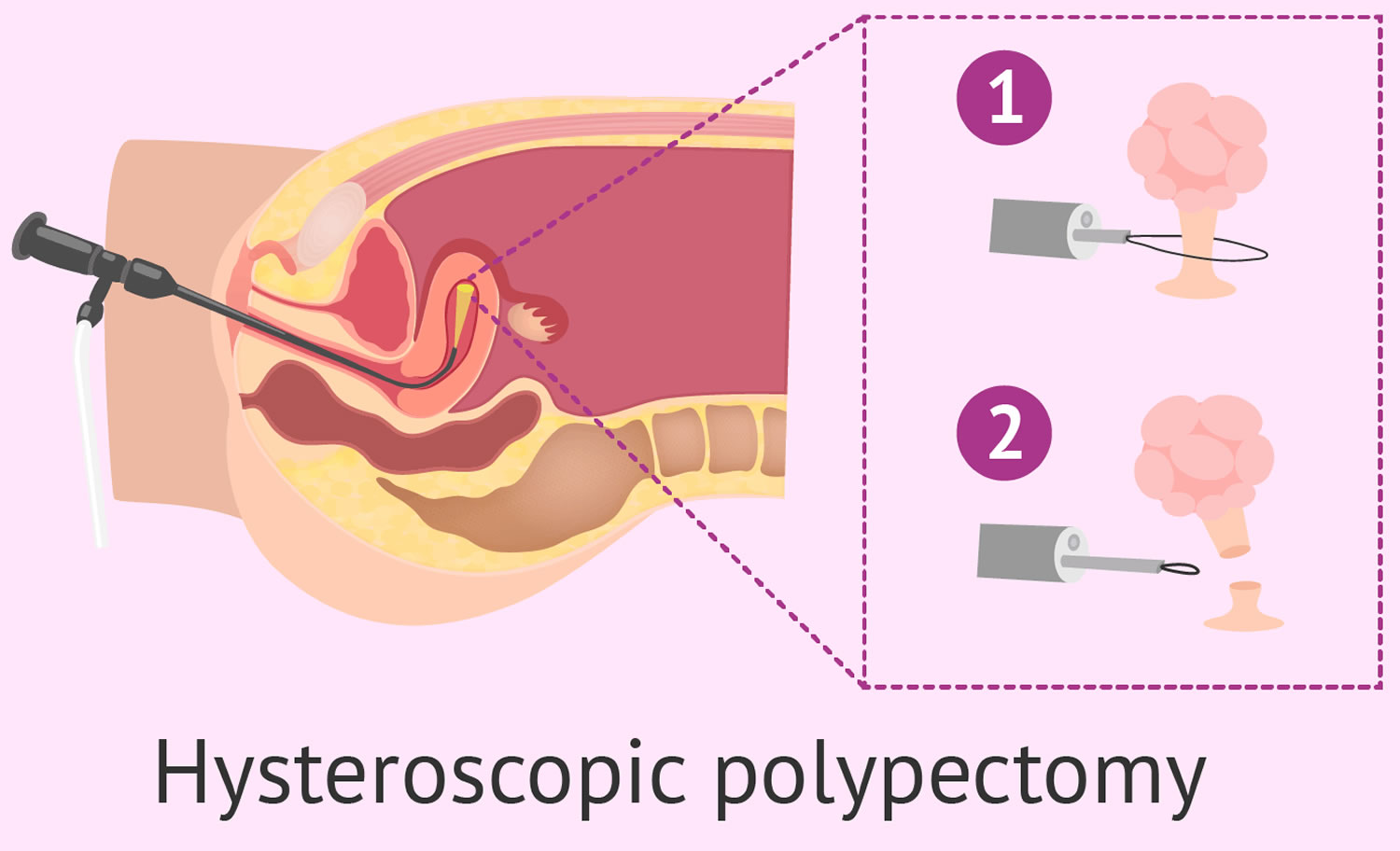
A hysteroscopic polypectomy is a procedure your gynecologist may perform if you have abnormal bleeding patterns that may or may not be accompanied by infertility issues as well. A hysteroscopy is the process of looking into your uterus with a telescopic instrument called a hysteroscope. A hysteroscope is a thin tube with a light on the end that can expand. Surgical instruments can be passed through a hysteroscope. Polypectomy is the removal of the uterine polyps. Hysteroscopic polypectomy procedure generally takes from 5 minutes to 1 hour to perform, depending on what you’re having done.
Endometrial polyps are one of the most common causes of abnormal vaginal bleeding in both premenopausal and postmenopausal women. The likelihood of developing endometrial polyps appears to increase with age. Risk factors for developing endometrial polyps include Tamoxifen (used to treat breast cancer), hormone replacement therapy, hypertension and obesity.
Endometrial polyps are occasionally found in women who are not experiencing any symptoms at all. They may show up on a pelvic ultrasound examination or even as an incidental finding on a CT scan of the pelvis done for entirely different issues such as hip pain.
The precise diagnosis of an endometrial polyp can only be made by removing it and having it examined by a pathologist. Occasionally a polyp resembles a uterine fibroid — they can easily be confused with one another on ultrasound and hysteroscopy.
The risks and side effects associated with hysteroscopy are similar to other gynecological procedures:
- Introducing an infection
- Causing heavy bleeding
- Accidentally damaging your bladder, bowels, cervix or uterus
- Scarring of the endomtrium (the lining of your uterus)
- Creating unexpected problems from the gas or liquid used to expand your uterus
Furthermore, you should not have a hysteroscopy done if you’re pregnant or suffering from:
- A cervix that’s inflamed
- An unusual discharge from your vagina
- Pelvic inflammatory disease
- A bladder that’s bloated
Figure 3. Hysteroscopic polypectomy
Does hysteroscopic polypectomy hurt?
No. Doctors generally use intravenous sedation so that the procedure is virtually painless.
Hysteroscopy polypectomy recovery
You rarely need to do anything special after a hysteroscopy since it’s so minimally invasive. You will likely be observed for an hour following a hysteroscopic polypectomy procedure but should plan on spending 2 hours there from the moment you arrive. You’ll wish to rest most of the day after the procedure. If you’ve having a simple hysteroscopic polypectomy with no other procedure you will experience some cramping and some bright red bleeding for about 4-5 days. This will be followed by a brown discharge for another week until it stops entirely. If your gynecologist used gas, you may feel some bloating after hysteroscopy, but it’s not serious. You may feel manageable pain in your abdomen or shoulder from the gas. You can take a mild pain reliever (except aspirin and ibuprofen, which can increase bleeding) as needed.
You may be asked to take 24 to 48 hours off from work depending on your own individual circumstances.
Your gynecologist may advise you not to douche or have sexual intercourse for two weeks after your hysteroscopy, but you can return immediately to all your other normal daily activities without limitations. You can even eat your normal diet right after your procedure. Just remember that you may be a little gassy.
Can endometrial polyps come back?
The short answer is yes. In about 10-15% of cases they recur. For this reason doctors occasionally suggest removal of the entire lining—which is where polyps originate from. This is only offered under very specific circumstances. For women who still wish to retain their ability to have children this is never offered as an option.
Cervical polypectomy
Cervical polypectomy is the removal of cervical polyps or visible endocervical polyps; it is generally a simple, painless office procedure. Cervical polyps are usually benign (non-cancerous) pedunculated growths of the cervix that are often asymptomatic but can cause bleeding. Because they are occasionally malignant, small polyps are best removed during a gynecologic examination and sent to the pathology laboratory for diagnosis.
Cervical polyps can range from a few millimeters to a few centimeters in diameter. Cervical polyps are often picked up during routine health screenings or Pap smears. They may also be found during a gynecological ultrasound, where the polyp is seen as an “echogenic” bright spot. Cervical polyps are common in women, regardless of age.
There are two types of cervical polyps that may occur:
- Ectocervical polyps. Develop on the outer surface layer of the cervix.
- Endocervical polyps. Develop from cervical glands within the cervical canal, and mostly seen attached to a thick stalk.
While most cervical polyps do not display any symptoms, they may occasionally cause abnormal bleeding during your menstrual cycle.
Other symptoms you may experience include:
- Heavy periods
- Bleeding after sexual intercourse
- Bleeding after menopause
- Foul-smelling vaginal discharge
Depending on the type of cervical polyp and its location, there are two options to remove it:
- In the doctor’s office. Your doctor can remove cervical polyps that are small and located outside of the cervix. Your doctor will grasp the polyp with a pair of forceps, and remove it with a gentle twisting motion.
- Surgical removal. Larger cervical polyps, or those located deep within the cervix, may need to be removed via a polypectomy or a dilation and curettage. These procedures are performed in an operating theatre, usually under general anaesthesia to reduce the amount of pain felt.
Your doctor will send the removed cervical polyp for further testing and assessment.
While cervical polyps do not grow back after being removed, women with prior cervical polyps are at higher risk of growing more polyps. Regular screening and Pap smears will help detect any polyps early.