Contents
What is a pustule
Pustule is smaller than 5–10 mm inflamed, pus-filled, blister-like sores (lesions) on the skin surface.
- Pus can indicate bacterial, fungal or viral infection
- Some pustules are sterile and are due to inflammatory skin disease
Pustules are common in acne and folliculitis (inflammation of the hair follicle). They may occur anywhere on the body, but are most commonly seen in these areas:
- Back
- Face
- Over the breastbone
- Shoulders
- Sweaty areas, such as the groin or armpit
Pustules may be a sign of an infection. They should be checked by a health care provider and may need to be tested (cultured) for bacteria or fungus.
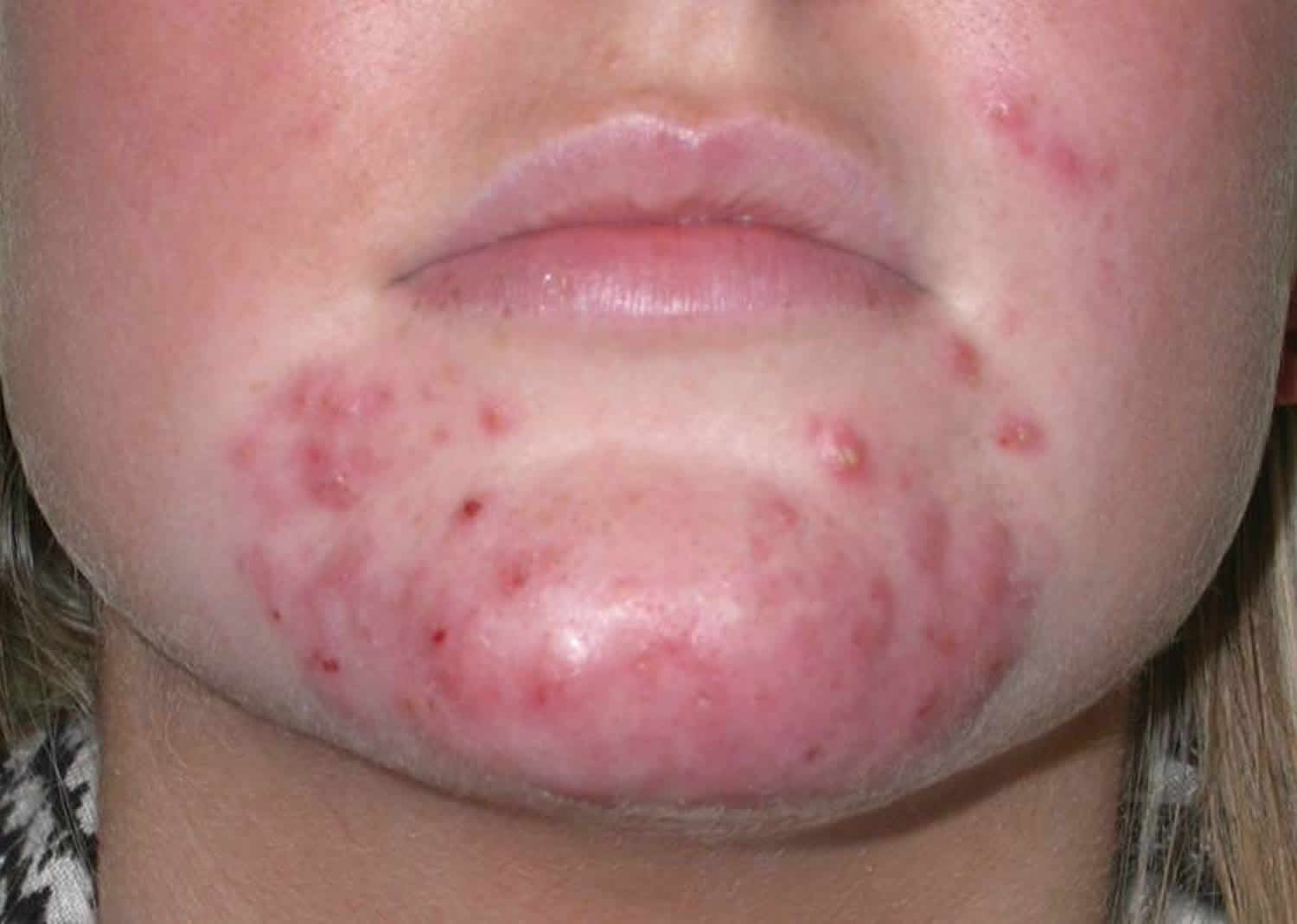
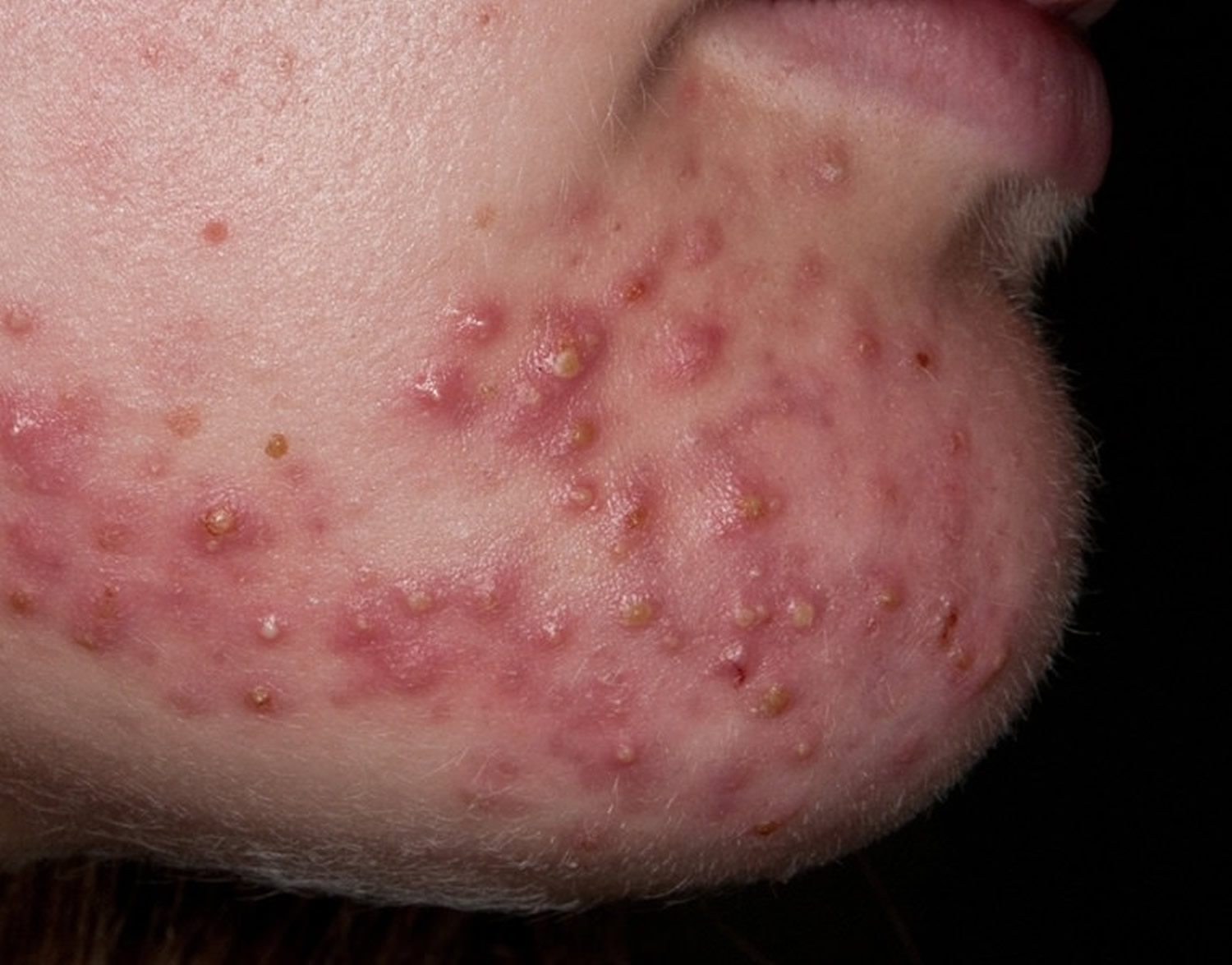
Figure 1. Pustule acne (pimples)
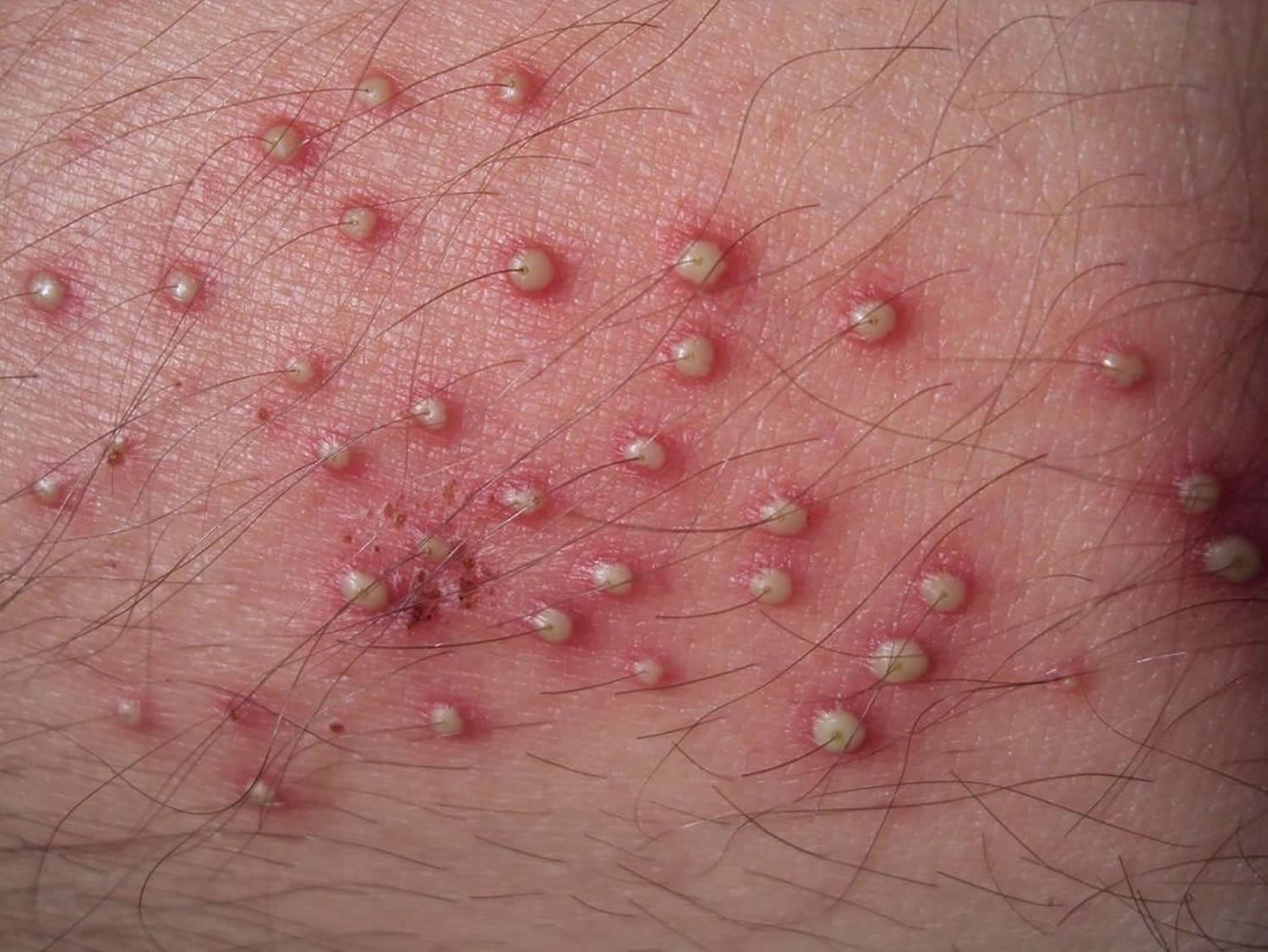
Figure 2. Folliculitis (inflamed hair follicles)
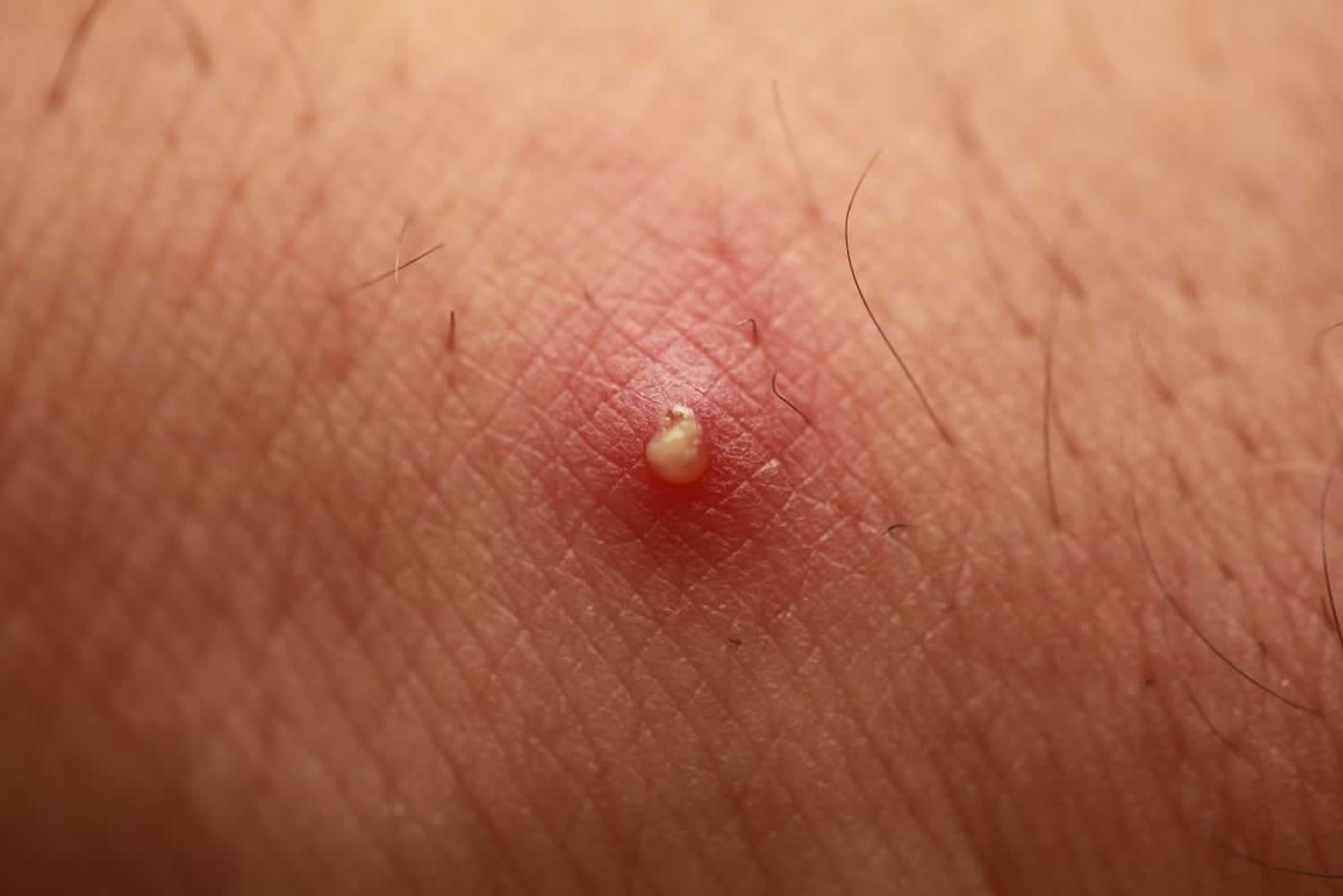
Figure 3. Boil (deeper, and more pronounced infection of the hair follicle)
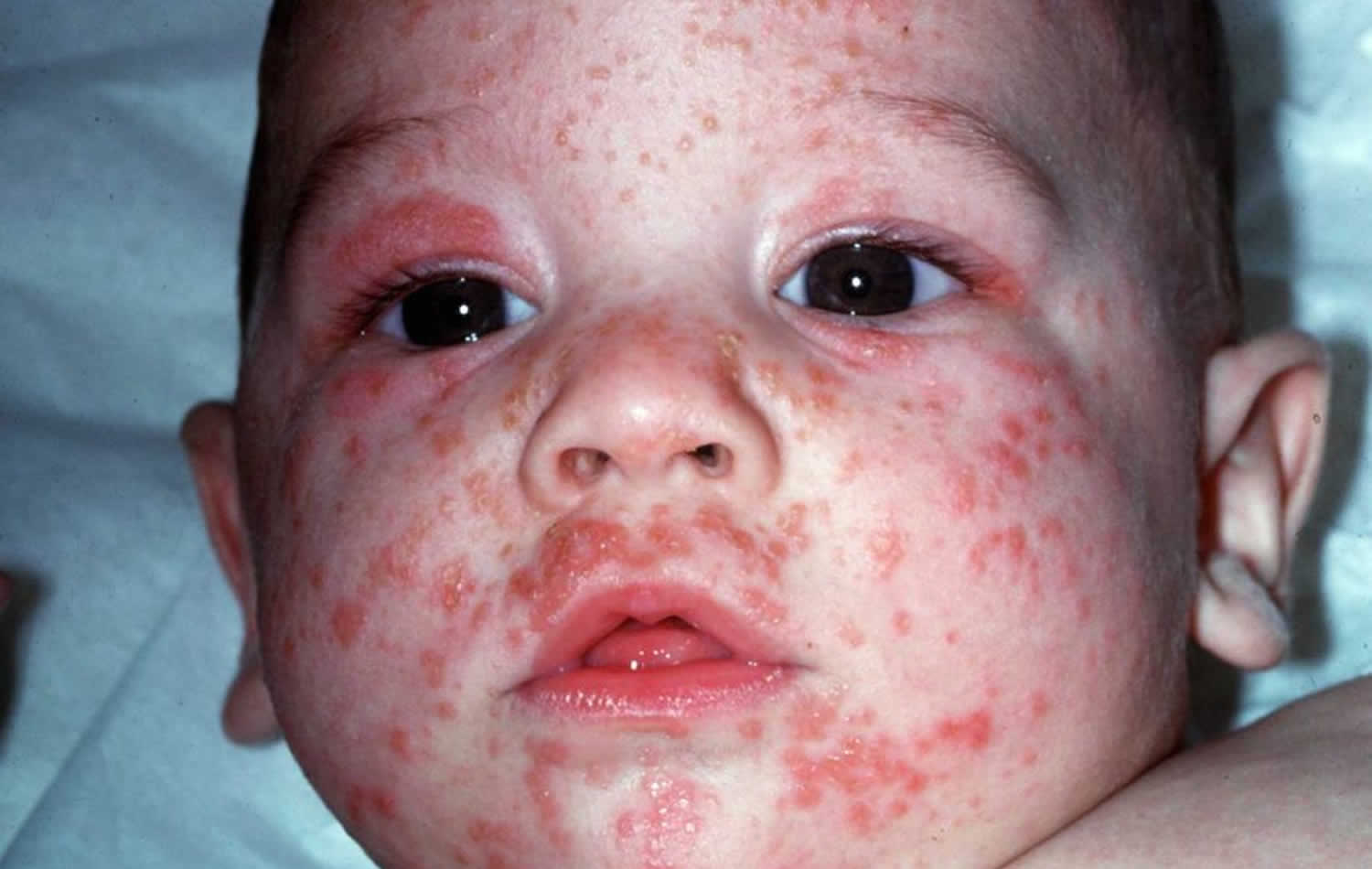
Figure 4. Scabies
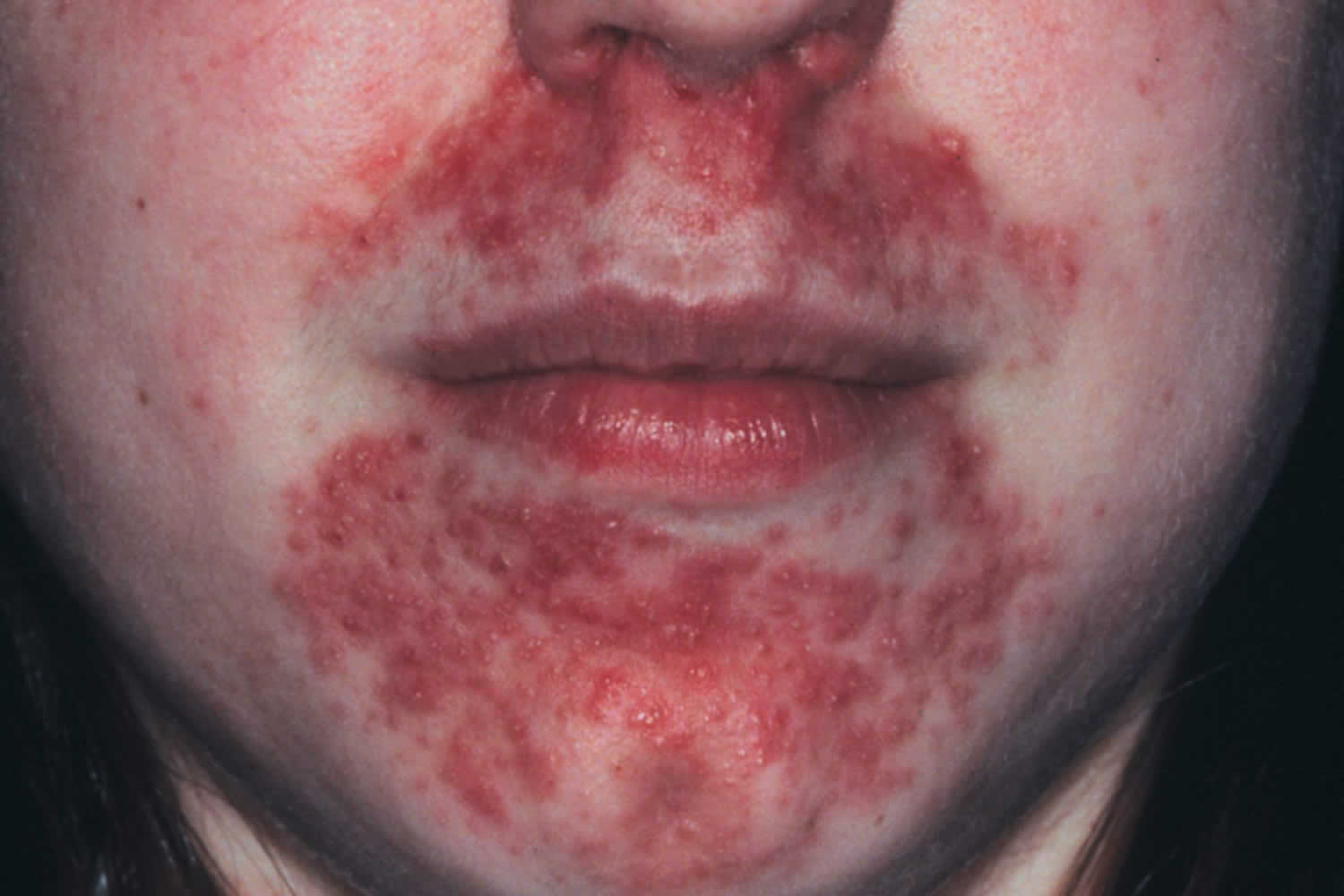
Figure 6. Peri-oral dermatitis
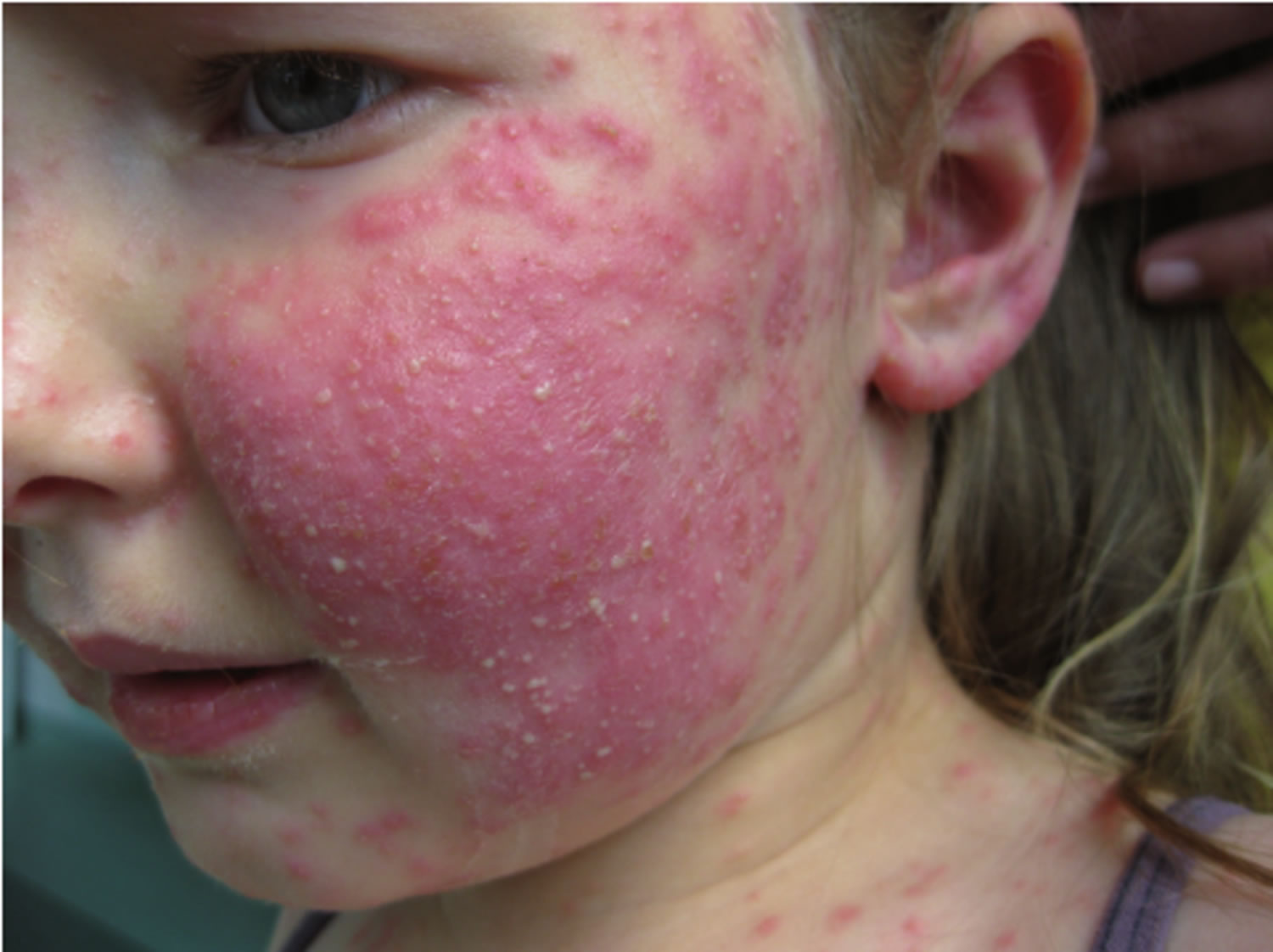
Figure 7. Inflammatory tinea
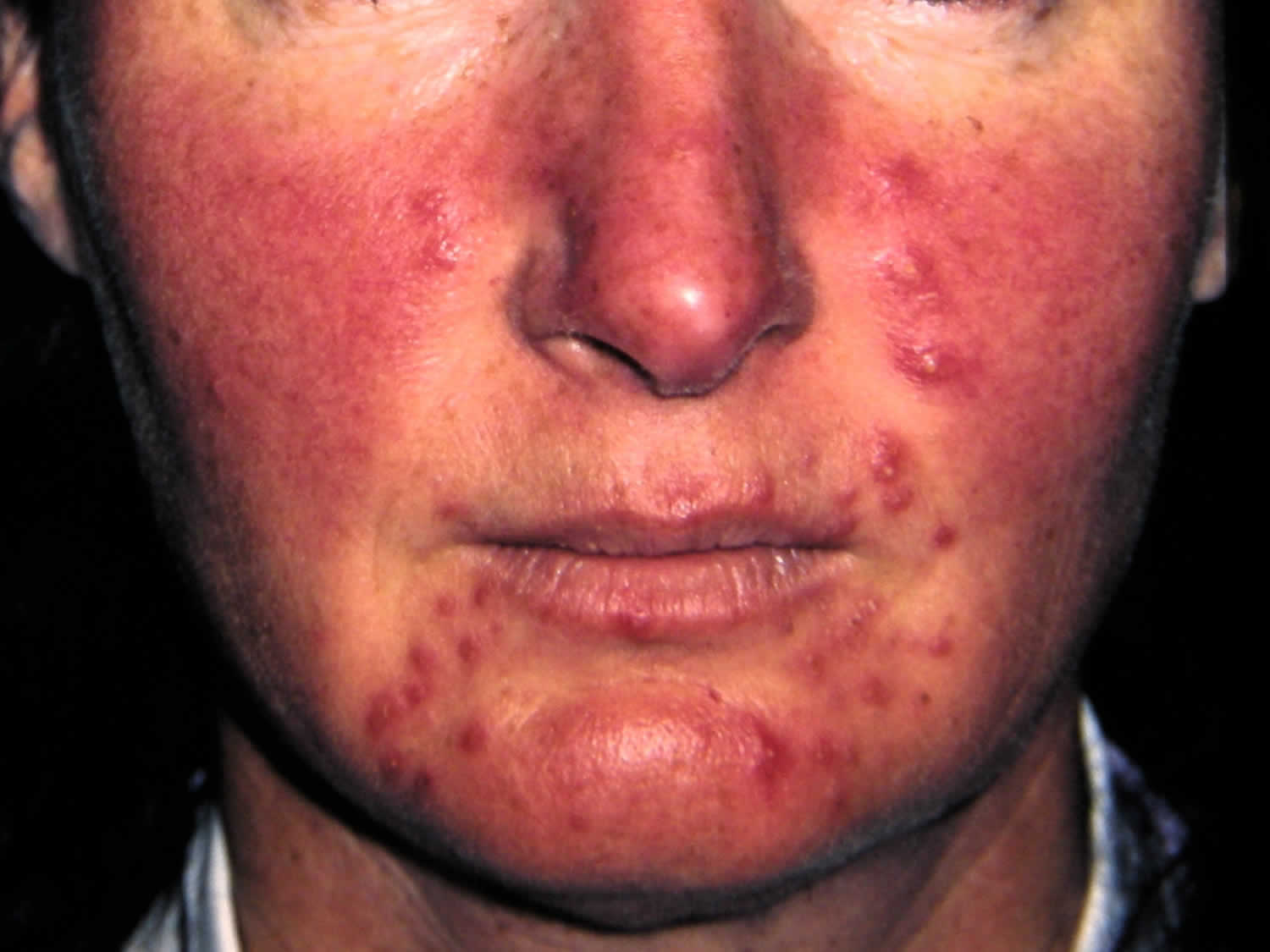
Figure 8. Rosacea
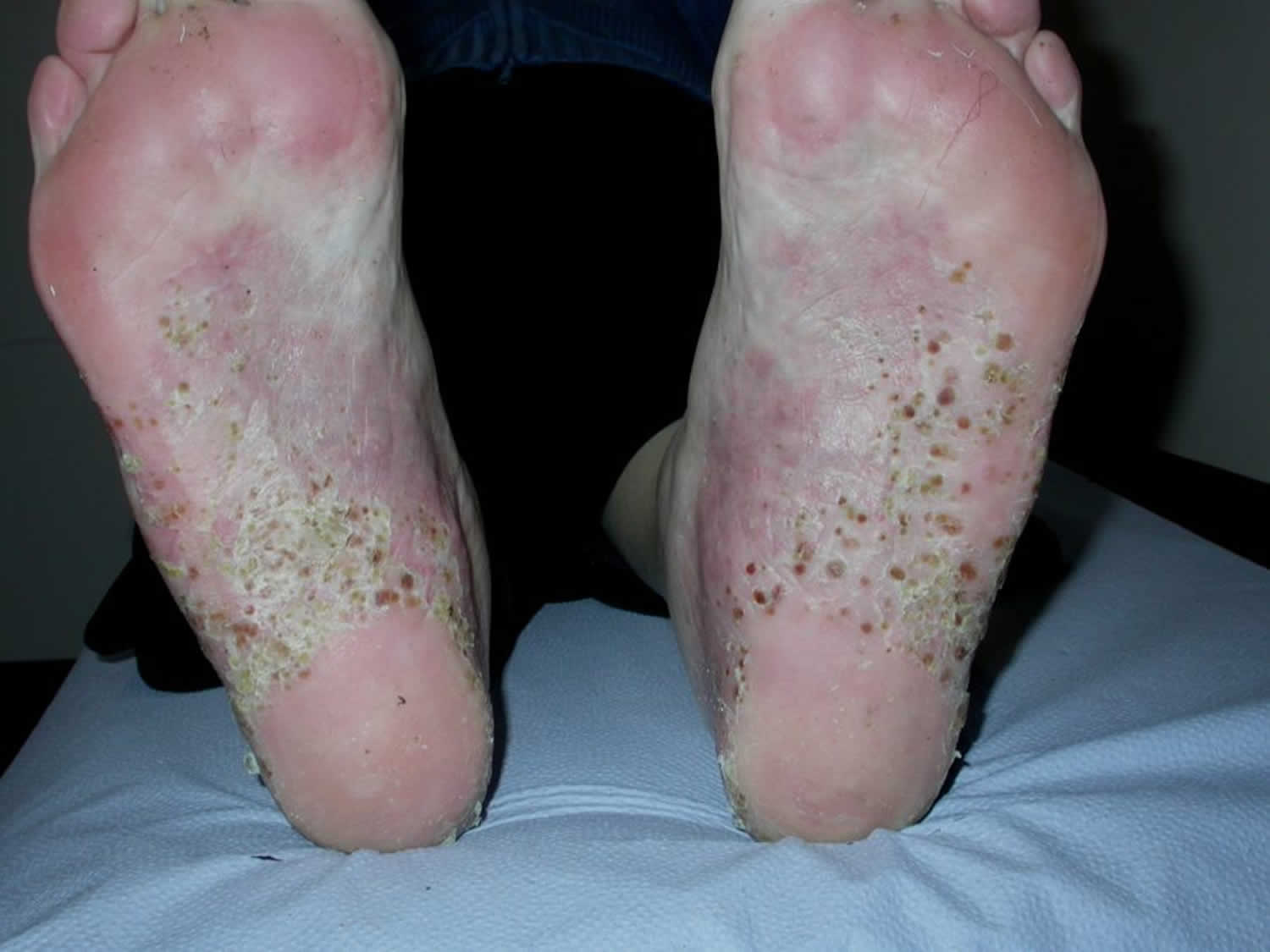
Figure 9. Palmoplantar pustulosis
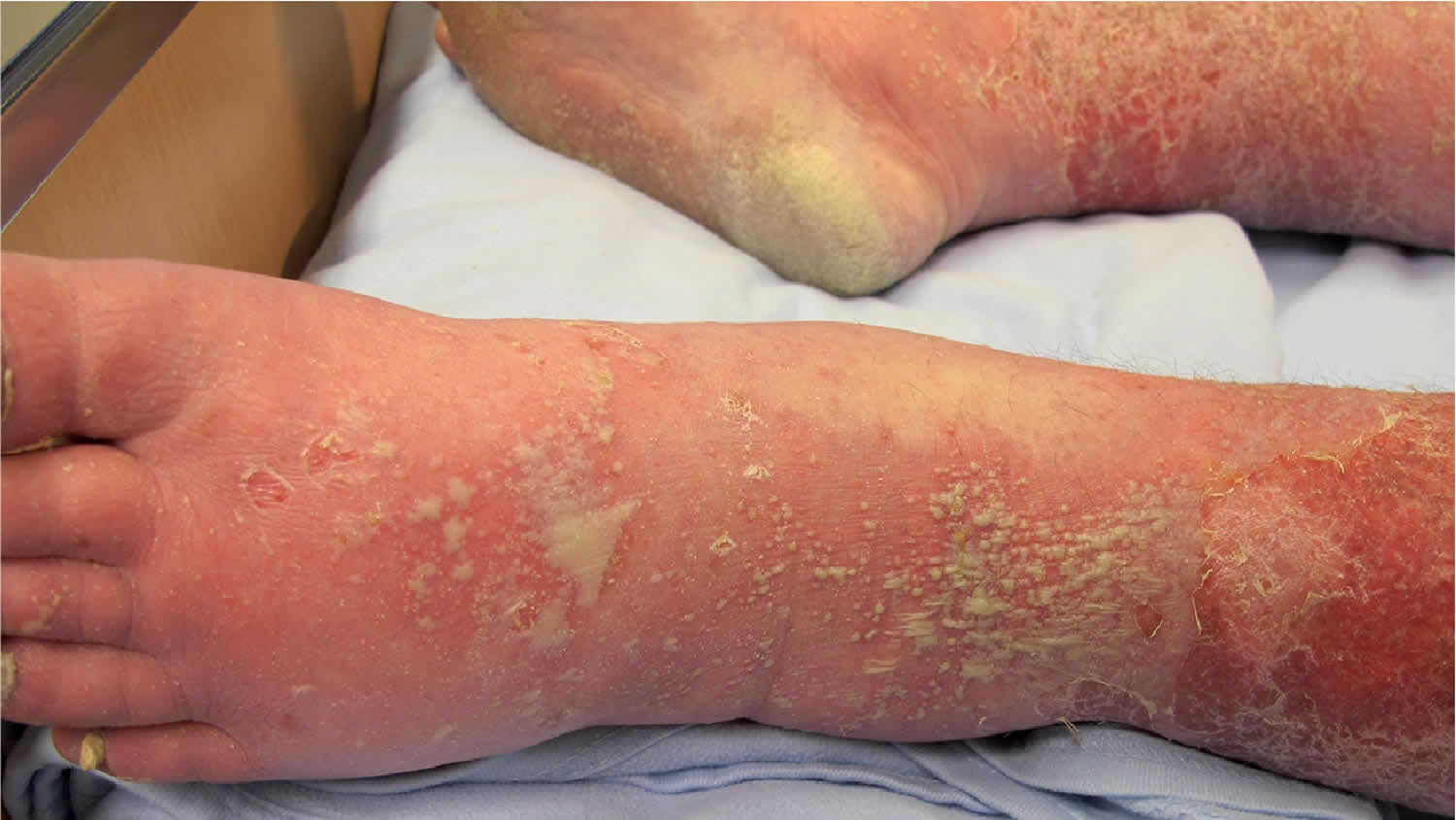
Figure 10. Pustular psoriasis
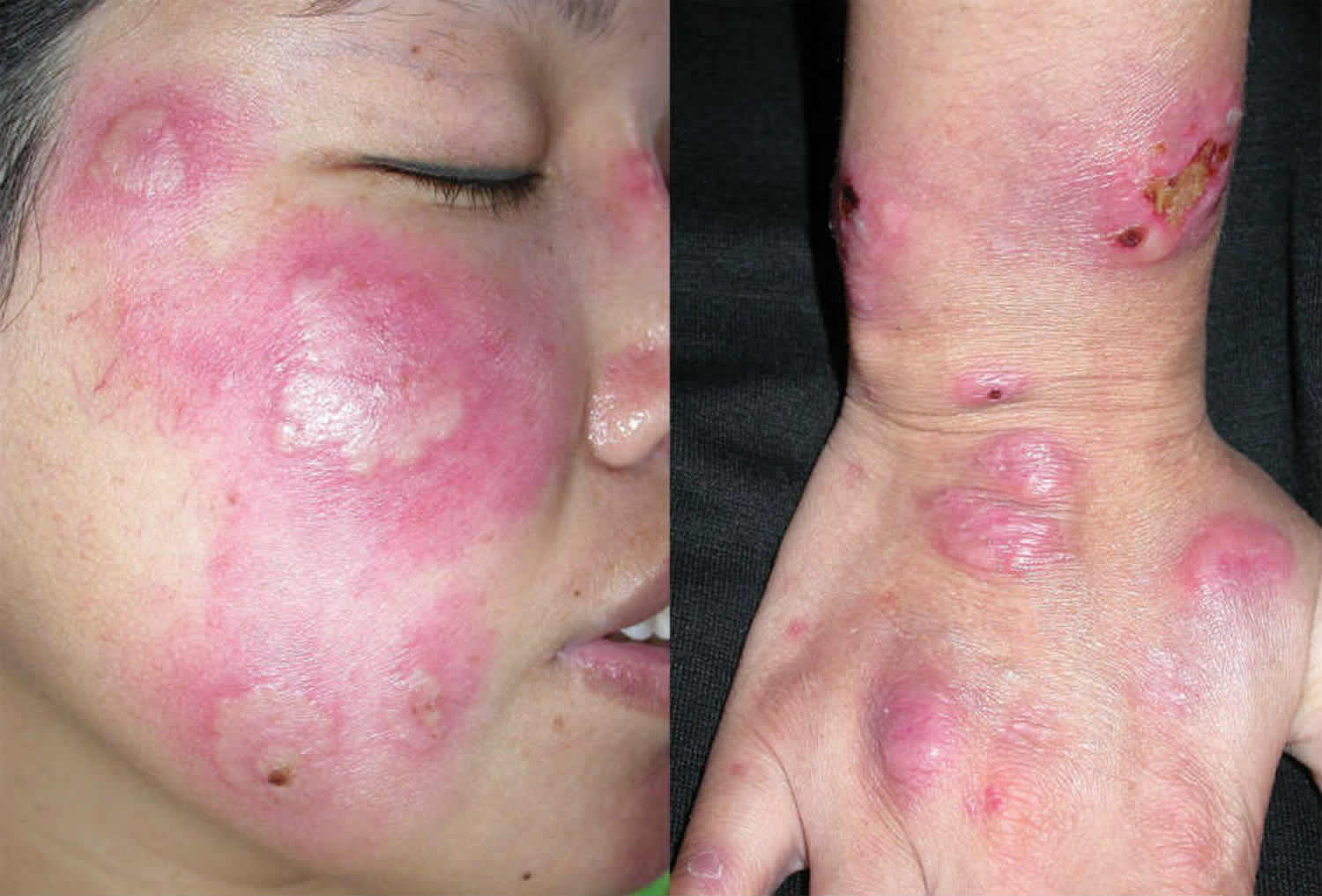
Figure 11. Sweet’s syndrome
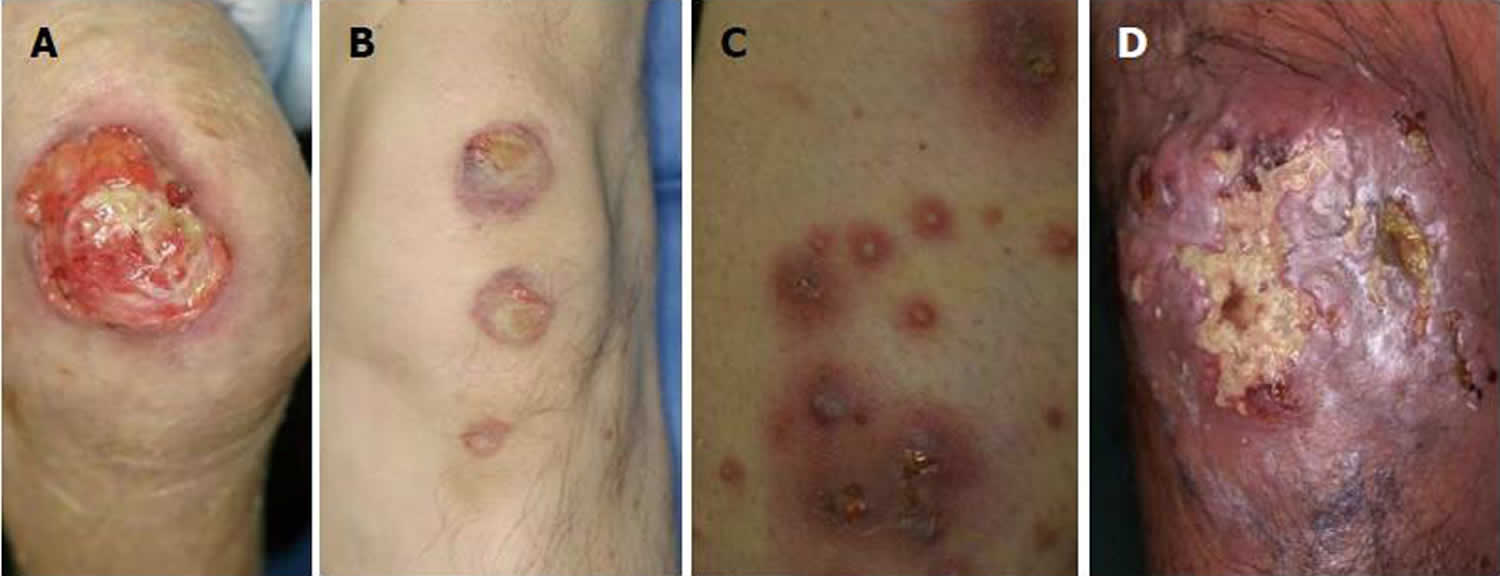
Figure 12. Pyoderma gangrenosum [(A) ulcerative type, (B) bullous type, (C) pustular type, (D) vegetative type]
Pustule causes
Causes of pustular skin conditions:
- Acute mainly pustular generalized eruptions
- Acute mainly pustular localized eruptions
- Chronic mainly pustular eruptions
Common causes of pustular skin conditions:
- Acne vulgaris (common acne) (any of – comedones, papules, pustules, nodules, scars)
- Rosacea (any of – papules, pustules, erythema, nodules. Comedones absent)
- Peri-oral and peri-ocular dermatitis (mainly around mouth, but occasionally around eyes / small monomorphic papules and pustules / nasolabial erythema quite common)
- Folliculitis / pseudofolliculitis (can itch / any hair-baring site / multiple small papules and pustules on an erythematous base that are pierced by a central hair)
- Inflammatory cases of tinea (can itch / often asymmetrical / erythema, often with a leading scaly edge, pustules)
- Scabies (papules and pustules on the palms and soles are characteristic of scabies in infancy)
Uncommon causes of pustular skin conditions:
- Palms and soles
- Palmoplantar pustulosis (soles, palms / numerous yellow pustules and brown macules)
- Reactive arthritis (spondyloarthritis and ocular inflammation following a genitourinary or gastrointestinal infection / cutaneous features – palmoplantar pustulosis especially affecting the tips of the digits, and psoriasiform hyperkeratosis)
- Acropustulosis of infancy (infants and young children under the age of three years / palms and soles / crops of small itchy bullae progress into pustules / self-limiting)
- Neutrophilic dermatoses of the (dorsal) hands (pustular or ulcerative plaques and nodules on the dorsal hands. Lesions tend to be blue-grey)
- Others
- Generalized pustular psoriasis (widespread pustules on a background of red, tender skin / patient unwell)
- Sweet’s syndrome syn. acute febrile neutrophilic dermatosis (more common in middle-aged women / most commonly affects arms, face and neck but can be more widespread / tender papules, pustules, plaques, and occasionally nodules – lesions can be studded with pustules / fever common)
- Subcorneal pustular dermatosis (lesions arise as numerous small, sterile pustules. Characteristically the pus accumulates in the lower half of the pustule / pustules easily rupture and tend to coalesce forming annular or serpiginous patterns with a scaly edge)
- Pyoderma gangrenosum – pustular variant (linked to inflammatory bowel disease / predominantly the extensor surfaces of the limbs but other sites can be affected / discrete painful pustular lesions with a surrounding erythematous halo)
- Neutrophilic dermatoses – others
Acute mainly pustular generalized eruptions
Generalized pustular psoriasis
- Febrile illness
- Annular plaques studded with pustules
Acute generalized exanthematous pustulosis
- Febrile illness
- Drug eruption
- Diffuse superficial pustules
Acute mainly pustular localized eruptions
Impetigo
- Rapidly enlarging plaque
- Swab Staphylococcus aureus +/- Streptococcus pyogenes
Furunculosis/boil
- Based on hair follicle
- May lead to abscess formation
- Usually caused by Staphylococcus aureus
Folliculitis
- Itchy or painful follicular pustules
- Various types
Dermatophyte infection
- Kerion: abscess formation
- Due to zoophilic fungus, e.g. Microsporum canis
Thrush
- Intertrigo, oral mucosa
- Superficial pustules that dry out easily
- Usually caused by Candida albicans
Miliaria
- Sweat rash
Chronic mainly pustular eruptions
Acne
- Face, neck, upper trunk
- Comedones + inflammatory lesions
Acneform eruptions
- Rosacea
- Periorificial dermatitis
- Chronic folliculitis
Scabies
- Irregular pustules on hands and feet
- Burrows between fingers, volar wrists
- Papules axillae, groin
- Generalized itchy rash
Dermatophyte infection
- Irregular annular plaque with peripheral scale
- Pustules on feet due to Trichophyton interdigitale
Localized pustulosis
- Hands, feet
- Sterile tender, itchy, pustules
Erosive pustular dermatosis
- Sun damaged scalp
- Often, underlying squamous cell carcinoma
- Greenish pus
- Culture Staphylococcus aureus
Pustule treatment
Pustule acne treatment
The type of acne is important. For example there are some variants such as sandpaper acne and macrocomedonal acne that respond poorly to conventional treatment
The primary aim of acne treatment is to prevent or minimize scarring, once scarred the skin will never return to normal, accordingly:
- Patients with severe acne e.g., nodular scarring acne should be referred immediately
- Papular-pustular acne can also scar, as such patients starting to scar who do not respond to the treatments referred to in steps 2 and 3 (below) should also be referred
- Ideally patients with scarring should be referred as semi-urgent and seen within six weeks
For patients with mild-moderate acne:
- Topical preparations containing benzoyl peroxide and/or topical retinoids are an essential part of the treatment. It is important to explain to the patient that such treatments will dry the skin and cause local irritation, in order to reduce adverse effects patients may wish to start using the treatments two to three evenings (or nights) a week and gradually increase the frequency and duration of applications
- There are increasing levels of Propionibacterium acnes resistance to antibiotics, especially erythromycin, the use of which should be restricted
It is important to have a way of monitoring response to treatment. This could be done as follows:
- Serial photography is perhaps the best method
- Using standardized grading methods
Treatment ladder
Step 1: Treatment of comedonal acne (figures 6 and 7 above)
- First line – a topical retinoid
- A topical retinoid is needed as this reduces comedonal activity
- Choices include adapalene (Differin ®), adapalene combined with benzoyl peroxide 2.5% (Epiduo ®), or isotretinoin (eg Isotrex ®)
- Although topical retinoids should be avoided in pregnancy they are safe to use in all other patients including sexually active women
- Second line – azelaic acid
Step 2: Treatment of mild to moderate pustular acne or papular acne
- Use a fixed dose combination treatment, ideally containing benzoyl peroxide (BPO), which reduces bacterial resistance, with either a topical retinoid or topical antibiotic:
- First line – Epiduo gel (adapalene + benzoyl peroxide)
- Second line – Duac ® gel (clindamycin + benzoyl peroxide)
- Other options:
- Treclin ® gel (clindamycin and tretinoin)
- Erythromycin combinations – Aknemycin ® Plus solution, Isotrexin ® gel
- As in step one above, it is important to explain to the patient that both benzoyl peroxide and topical retinoids will dry the skin and cause local irritation, in order to reduce adverse effects patients may wish to start two to three evenings (or nights a week) and gradually increase the frequency and duration of applications
Step 3: not responding to the above and/or more widely distributed
- Combine systemic antibiotics with an appropriate topical agent, preferably benzoyl peroxide to reduce bacterial resistance. If patients cannot tolerate benzoyl peroxide use a topical retinoid.
- Antibiotic choice:
- Tetracyclines
- Lymecycline 408 mg once daily (Tetralysal ®) is a good first line antibiotic as compliance is good (it can be taken with food) and bacterial resistance is less than with first generation tetracyclines
- Review the patient in six weeks, if the response is poor then change to doxycycline 100 mg od (can take with food). Doxycycline can occasionally cause a photosensitive eruption
- Minocycline is rarely used due to the increased risk of hepatotoxicity and lupus-like conditions
- Macrolides
- Should generally be avoided due to high levels of P.acnes resistance
- They are first line in pregnancy and in children under the age of 12 years (in both groups tetracyclines are contraindicated)
- The dose of erythromycin is 500 mg twice daily, or, clarithromycin 250 mg twice daily – smaller doses are required in patients aged under 12 years
- Trimethoprim
- Again there are concerns of bacterial resistance, so this treatment may best be reserved for young children who do not tolerate macrolides
- Tetracyclines
- Duration of treatment
- The evidence suggests that there is little additional benefit in using antibiotics for more than three months, and in addition, prolonged use increases the resistance of P.acnes
- It is therefore recommended that antibiotics should be stopped after three months, however, the patient should remain on their topical agent
- The antibiotic course could be repeated in the future if needed
- If the patient does not respond to two types of antibiotics, especially if they are starting to scar, the patient should be referred for consideration of Isotretinoin
Step 4: Treatment of moderate-severe acne in a woman
- If no contraindications consider adding in Dianette ® to the topical / systemic treatments referred to above
- Dianette may be of particular value in patients with significant endocrinopathies such as polycystic ovarian syndrome (PCOS)
Acne in pigmented skin
- Acne is no more common or severe in pigmented skin, but post-inflammatory hyperpigmentation can be significant and often persists for months to years. As such, early and more aggressive treatment is advocated, including early referral for consideration of isotretinoin
- Secondary acne can be a result of cultural practices – hair oil can induce pomade acne on the forehead and skin lightening products containing topical steroids can cause a steroid-induced acne
- Topical retinoids, benzoyl peroxide and azelaic acid play an important role in the treatment of the comedonal aspects of acne. If used daily they often cause dryness and irritation, which in pigmented skin can lead to further hyperpigmentation. Accordingly these treatments should initially be used for shorter periods of time (eg in an evening and washed off before bed) and perhaps less frequently (eg every 2nd or 3rd day), if tolerated the duration and/or frequency of treatment can be increased – if used in this way then as well as treating the comedones they may help treat hyperpigmentation rather than aggravate it
Acne in pregnancy
The following are usually regarded as being safe, should the physician and patient feel it necessary, to prescribe during pregnancy:
- Benzoyl peroxide preparations
- 2% topical erythromycin
- If the acne is troublesome and not responding to topical treatments consider oral erythromycin, 500 mg twice daily
Step 5: Referral to Secondary Care
Who to refer
- Severe acne – refer early
- Moderate acne only partially responding to treatment and starting to scar and/or causing significant hyperpigmentation (more common in patients with brown or black skin)
- Patients with associated and severe psychological symptoms, regardless of the physical signs
Treatment options once referred:
- Oral isotretinoin (see below)
- High dose oral antibiotics such as lymecycline 408 mg twice daily or trimethoprim 300 mg twice daily
- Dianette ® with additional cyproterone acetate (50-100 mg/10 days)
- Short courses of oral corticosteroids may be required
Prescribing isotretinoin in the community
Because isotretinoin can be so harmful to a developing baby, both women and men must register with the iPLEDGE program before they can take it. iPLEDGE is sponsored by the company that makes isotretinoin. iPLEDGE is approved by the Food and Drug Administration (FDA), the government agency that checks the safety of medicine and food in this country.
Both men and women who take isotretinoin must agree to follow strict iPLEDGE rules to help prevent pregnant women and women who may become pregnant from having contact with isotretinoin. Only doctors and pharmacists who are registered in the program may prescribe and give isotretinoin to patients.
If you’re taking isotretionoin, you must agree to use two different forms of effective birth control. Your provider can help you choose two effective forms of birth control that work together. You also must take regular pregnancy tests and agree not to get pregnant:
- For at least 4 weeks before you start using the medicine
- While taking the medicine
- For at least 4 weeks after you stop using the medicine
Men who take isotretinoin can have it in their semen (fluid that contains sperm). Experts don’t know if semen with isotretinoin can lead to birth defects. Talk to your provider if your partner takes isotretinoin and you’re planning to get pregnant.
Management of scarring
Up to 50% of scars (especially smaller scars) may improve naturally over 6-12 months. Treatment of established scars is difficult and while some patients will benefit from treatment others will not. Patients should only be referred to dermatologists / plastic surgeons familiar with treating scars. Funding will vary depending on local commissioning arrangements.
Atrophic scars
- The development of ablative lasers combined with appropriate surgical techniques has led to a significant improvement in the way that certain atrophic scars can be treated
- Punch excision of small atrophic scars which can be very helpful prior to resurfacing
- For deep scars – scar revision may help
- Other options include intradermal injections of collagen or compounds, which stimulate collagen synthesis
Hypertrophic / keloid scars
- Silicone gels applied to scars can be prescribed by general practitioners
- Local steroids for a trial period of two to three months. Look closely for side-effects such as skin thinning and telangiectasia. Treatments can be administered as topically ie a potent or super-potent steroid cream or ointment carefully applied, Haelan ® tape (fludroxycortide) or by using intradermal triamcinolone given as an injection
- Pulsed dye laser, which can reduce the redness of scars and flatten them. This procedure is only possible through specialised hospital departments.