Contents
What is tinea versicolor
Tinea versicolor also known as Pityriasis versicolor, is a common long-term (chronic) fungal infection of the skin. The fungus (Malassezia furfur, formerly known as Pityrosporum) interferes with the normal pigmentation of the skin, resulting in small, discolored patches. Tinea versicolor is a superficial infection of the stratum corneum by the lipophilic fungus known as Malassezia furfur. These patches may be lighter or darker in color than the surrounding skin and most commonly affect the trunk and shoulders. The most common predisposing factor is excessive sweating but others include application of oils and systemic steroids.
Tinea versicolor (pityriasis versicolor) is a skin reaction to overgrowth of normally occurring yeast organisms (Malassezia furfur) living on the skin. About 90% of healthy people have these yeast organisms growing on their skin but they grow in larger numbers with sweating and humidity and where the sebaceous (oil) glands in the skin are very active. Some people may have an inherited predisposition to overgrowth of these organisms. The yeast produces chemicals which may affect the normal pigment production in the skin.
Tinea versicolor is more common in warm humid environments and may be seasonal. Most people with tinea versicolor are concerned about the appearance of the rash. Sometimes it may cause minor symptoms such as scaling, itch or irritation. It can be much more widespread if there is a problem with your immune system.
Tinea versicolor occurs most frequently in teens and young adults. Sun exposure may make tinea versicolor more apparent.
Antifungal creams, lotions or shampoos can help treat tinea versicolor. But even after successful treatment, skin color may remain uneven for several weeks or months. Tinea versicolor often recurs, especially in warm, humid weather.
What does tinea versicolor look like?
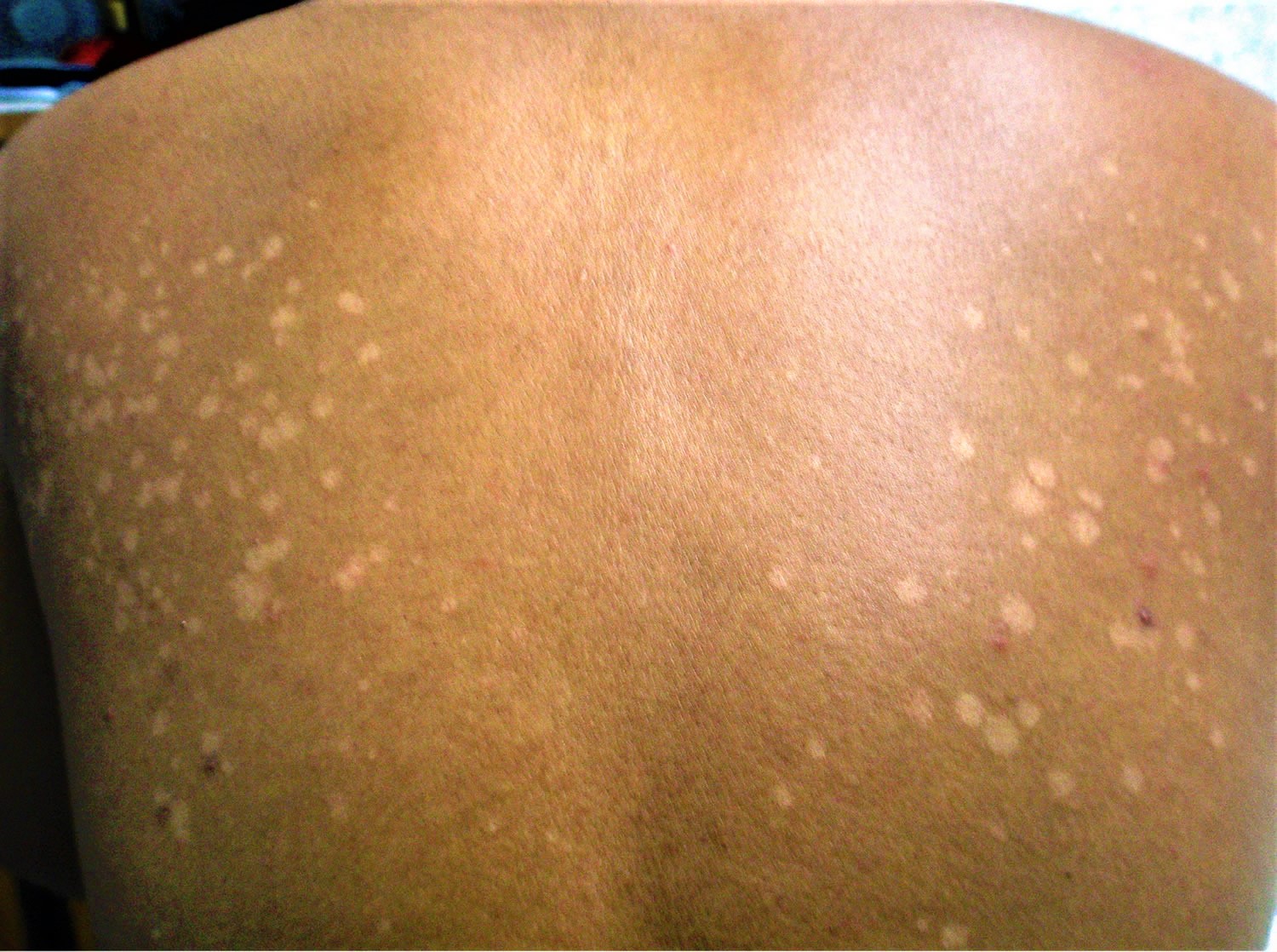
The typical appearance of the rash is of a discolored round or oval shaped eruption most commonly on the upper trunk region, sometimes extending to the neck or upper limbs. Occasionally, the rash may affect other areas of the body. The color of the eruption may appear lighter or darker than the surrounding normal skin, hence the name “versicolor”. The rash itself may be slightly raised with a fine scale.
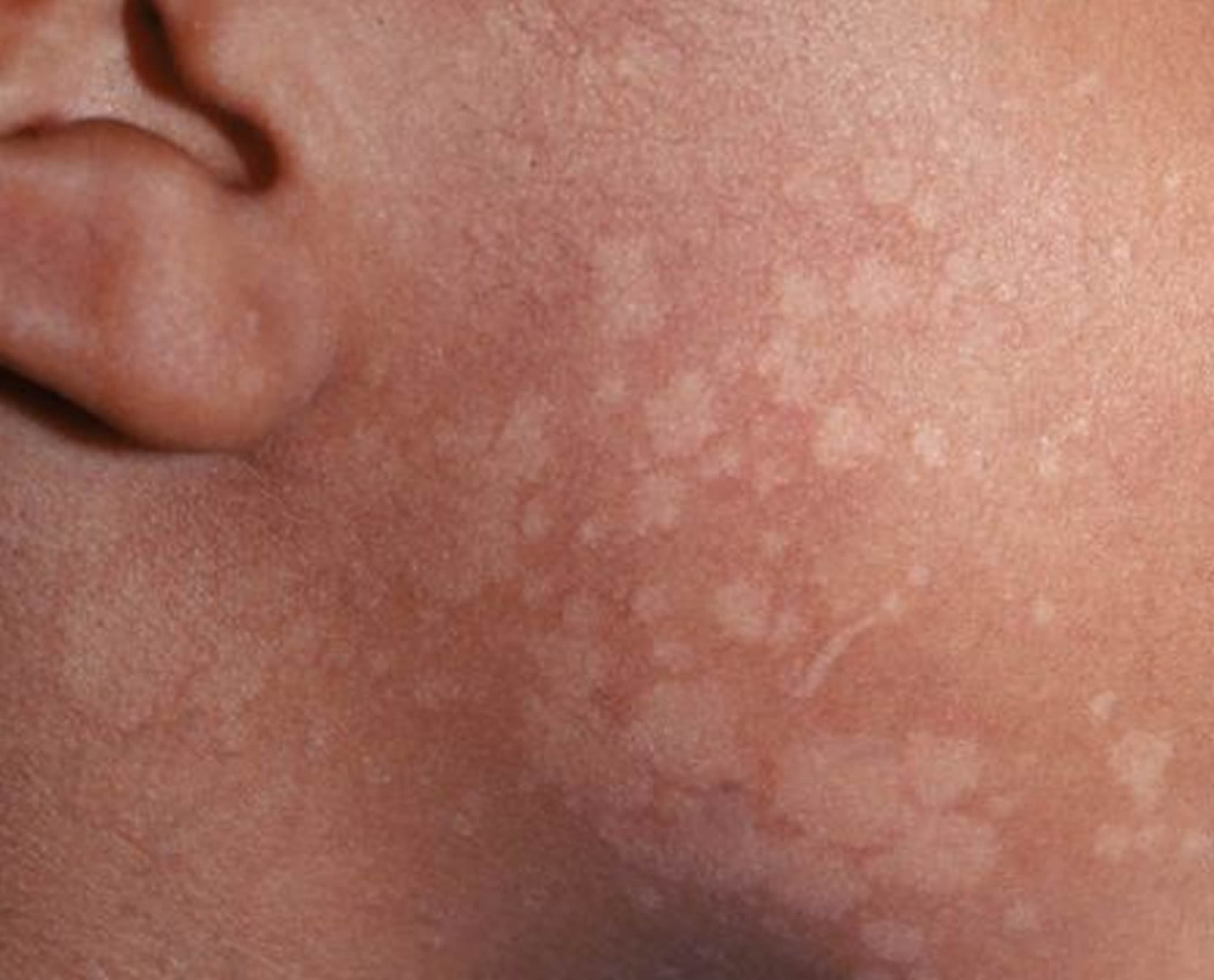
Figure 1. Tinea versicolor on face
Figure 2. Tinea versicolor upper back
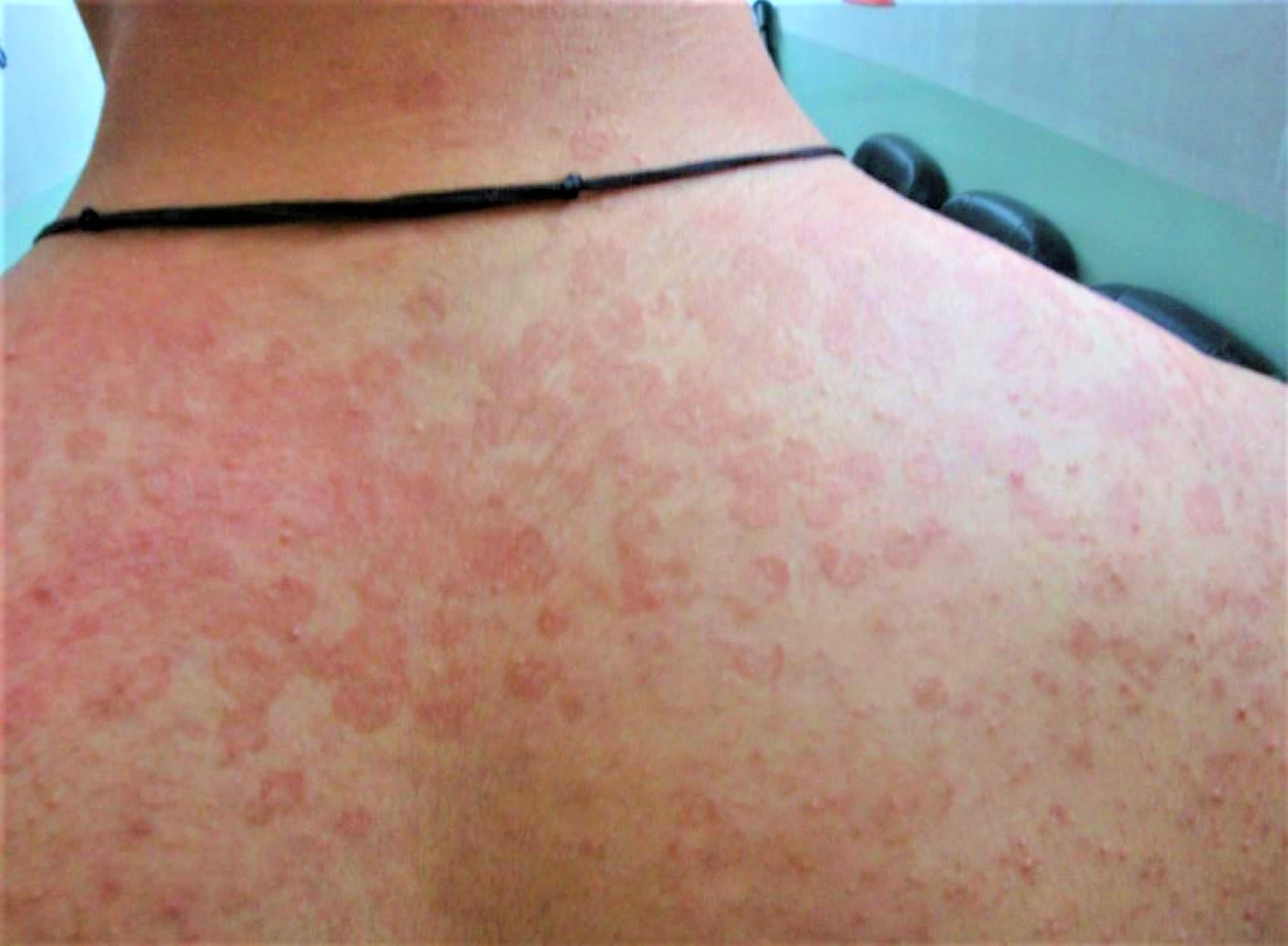
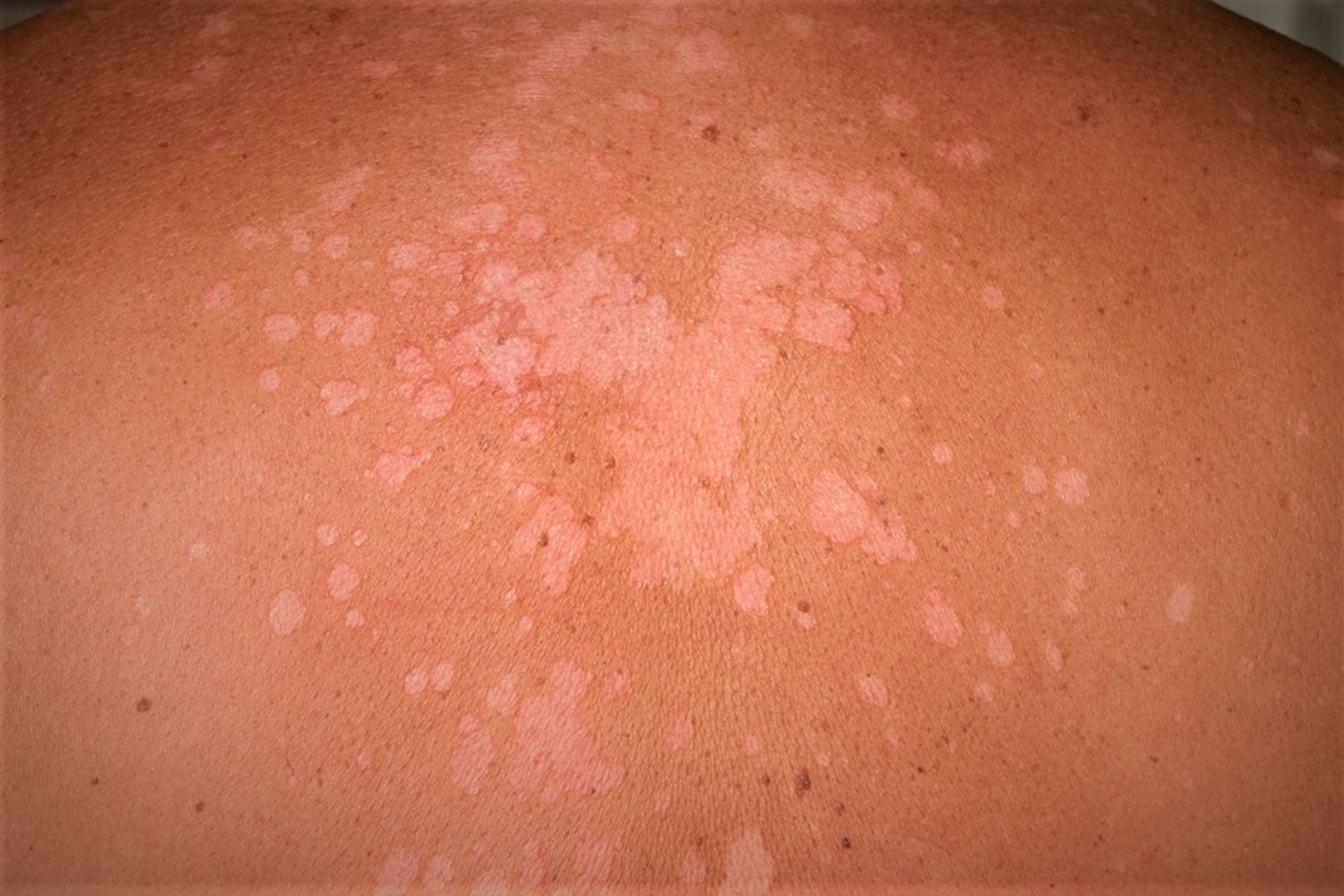
Figure 3. Tinea versicolor
Figure 4. Tinea versicolor
Is tinea versicolor contagious
Tinea versicolor, which is also called pityriasis versicolor, is not painful or contagious. But it can lead to emotional distress or self-consciousness.
Tinea versicolor is caused by a type of yeast called Malassezia furfur. This yeast is found on the skin of more than 90% of adults, where it normally lives without causing any problems. But tinea versicolor can develop if this yeast starts to multiply more than usual. It’s not clear exactly why this happens in some people and not in others.
Tinea versicolor outlook (prognosis)
Tinea versicolor is easy to treat. Changes in skin color may last for months. The condition may come back during warm weather.
Several factors can increase your risk of developing tinea versicolor, including:
- living or staying in a warm, moist environment, in the summer
- sweating excessively (hyperhidrosis)
- having naturally oily skin
- being a teenager or in your early 20s
Tinea versicolor isn’t related to poor hygiene. The condition can’t be spread from person to person because most people already have the Malassezia yeast on their skin.
Tinea versicolor causes
The Malassezia furfur fungus that causes tinea versicolor can be found on healthy skin. It only starts causing problems when the fungus overgrows. A number of factors may trigger this growth, including:
- Hot, humid weather
- Oily skin
- Hormonal changes
- Weakened immune system
Tinea versicolor prevention
To help prevent tinea versicolor from returning, your doctor can prescribe a skin or oral treatment that you use once or twice a month. You may need to use these just during warm and humid months. Preventive treatments include:
- Selenium sulfide (Selsun) 2.5 percent lotion or shampoo
- Ketoconazole (Ketoconazole, Nizoral, others) cream, gel, shampoo
- Itraconazole (Onmel, Sporanox) tablets, capsules or oral solution
- Fluconazole (Diflucan) tablets or oral solution.
Tinea versicolor symptoms
The main symptom is patches of discolored skin that:
- Have sharp borders (edges) and fine scales
- Tinea versicolor skin spots may be lighter (or darker) than your surrounding skin. The color of the spots can be white, pink, salmon, red, tan, or brown.
- Are often dark reddish to tan in color
- Are found on the back, underarms, upper arms, chest, and neck (can appear anywhere on the body).
- Do not darken in the sun so may appear lighter than the surrounding healthy skin. The yeast prevents the skin from tanning.
- Grow together, forming patches of lighter (or darker) skin.
- Grow slowly.
- Disappear when the temperature drops and return in the spring or summer when the air turns warm and humid.
Sometimes the spots are so faint that people do not realize they have tinea versicolor. If tinea versicolor causes light spots on the skin, it can be mistaken for vitiligo. Vitiligo is a skin disease that causes the skin to lose its natural color.
But there are many ways to tell the difference:
- Vitiligo often develops symmetrically (on both sides of your body at the same time), whereas tinea versicolor may not.
- Skin affected by vitiligo usually has a normal texture, whereas areas affected by tinea versicolor are usually slightly scaly or flaky.
- Vitiligo is more common around the mouth, eyes, fingers, wrists, armpits and groin, whereas tinea versicolor tends to develop on the chest, tummy, back and upper arms.
African Americans may have a loss of skin color or an increase in skin color.
Other symptoms include:
- Increased sweating
- Cause the affected skin to itch.
Tinea versicolor diagnosis
The diagnosis of tinea versicolor (pityriasis versicolor) is based on a clinical examination and the typical appearance of the eruption. Your doctor can diagnose tinea versicolor by looking at it. The affected skin may show yellowish fluorescence under long wave ultraviolet light (Wood’s lamp) examination. If there’s any doubt, he or she may take skin scrapings from the infected area and view them under a microscope. In rare cases, a skin biopsy taken under local anesthetic may be required for examination under a microscope.
Tinea versicolor treatment
Treatment may be required if the rash is causing concern. Treatment is directed towards reducing the number of yeast organisms living in the skin of the affected areas, using an anti-fungal preparation applied directly to the skin.
Tinea versicolor treatment over the counter
Examples include imidazole lotions or creams (such as ketoconazole, clotrimazole, econazole, miconazole) and anti-dandruff shampoos (such as ketoconazole, zinc pyrithione, selenium sulphide, ciclopirox olamine). With regard to topical therapy, ketaconazole is the most studied and seemingly the most effective. Topical antifungal, e.g., clotrimazole cream daily twice daily for 10 days is an alternative.
For smaller areas, one of the imidazole creams or lotions may be suitable and may be applied once or twice daily for 1 to 4 weeks.
For larger areas, one of the above anti-dandruff shampoos may be used as a body wash. The shampoo is applied to the whole affected area (after wetting the skin) and left on for 10 minutes before washing off. This is to allow time for the active ingredient to penetrate into the skin and hair follicles to reduce the number of yeast organisms. The treatment is performed daily for 2 to 4 weeks and subsequent maintenance therapy once or twice a week may be required to prevent recurrence. The effectiveness is generally improved with a longer course of treatment and a higher concentration of the active ingredient. If skin irritation occurs, treatment should be stopped and medical advice obtained.
Tinea versicolor home remedies
For a mild case of tinea versicolor, you can apply an over-the-counter antifungal lotion, cream, ointment or shampoo. Most fungal infections respond well to these topical agents, which include:
- Clotrimazole (Lotrimin AF) cream or lotion
- Miconazole (Micaderm) cream
- Selenium sulfide (Selsun Blue) 1 percent lotion
- Terbinafine (Lamisil AT) cream or gel
- Zinc pyrithione soap
When using creams, ointments or lotions, wash and dry the affected area. Then apply a thin layer of the product once or twice a day for at least two weeks. If you’re using shampoo, rinse it off after waiting five to 10 minutes. If you don’t see an improvement after four weeks, see your doctor. You may need a stronger medication.
It also helps to protect your skin from the sun and artificial sources of UV light. Usually, the skin tone evens out eventually.
Some people need stronger medicine, so they see a doctor. Whether you decide to self-treat or see a doctor, these tips can help you get better results:
- Stop using skin care products that are oily. Use products that are oil-free. The label may also read “non-comedogenic.”
- Wear loose clothes. Nothing should feel tight.
- Protect your skin from the sun. A tan makes tinea versicolor easier to see.
- Do not use a tanning bed or sun lamp. Again, a tan makes tinea versicolor easier to see.
How to protect your skin from the sun
To get the best results, you need to protect your skin from the sun. To do this, you should apply sunscreen every day. Be sure to apply the sunscreen 20 minutes before you go outside. And apply it to all skin that will not be covered by clothing. Make sure to use a sunscreen that offers:
- UVA and UVB protection (label may say broad-spectrum).
- Sun Protection Factor (SPF) of 30+ or higher.
- Non-greasy formula (label may read “oil-free” or “non-comedogenic”).
Prescription-strength medication
If tinea versicolor is severe or doesn’t respond to over-the-counter antifungal medicine, you may need a prescription-strength medication. Some of these medications are topical preparations that you rub on your skin. Others are drugs that you swallow. Examples include:
- Ciclopirox (Loprox, Penlac) cream, gel or shampoo
- Fluconazole (Diflucan) tablets or oral solution. Fluconazole 300 mg once and repeat in one week.
- Itraconazole (Onmel, Sporanox) tablets, capsules or oral solution. Itraconazole 200 mg/day for 5-7 days.
- Pramiconazole 200 mg/day for 2 days.
- Ketoconazole (Ketoconazole, Nizoral, others) cream, gel or shampoo. Ketoconazole 2% shampoo, lather scalp and trunk for 10 minutes daily for 7 days.
- Selenium sulfide (Selsun) 2.5 percent lotion or shampoo
Oral anti-fungal treatment may be considered in unusually severe or resistant cases but there is a risk of side effects and drug interactions occurring with these oral medications. Your doctor will discuss these issues.
Side effects of these tablets are uncommon, although some people experience problems such as rashes, feeling sick and abdominal (tummy) pain while taking them.
With regard to oral anti fungal agents, itraconazole and fluconazole seem equally effective for the treatment of tinea versicolor. For simplicity, fluconazole 300 mg orally once and repeat in one week is recommended.
The discoloration of the skin may take several weeks, or even months to return to normal, even after successful treatment.
Also, the infection may return in hot, humid weather. In persistent cases, you may need to take a medication once or twice a month to prevent the infection from recurring.
Tinea versicolor recurrences
It’s common for tinea versicolor to come back after treatment, particularly during the summer or during holidays to warm and humid countries.
But you can reduce this likelihood by regularly using the antifungal shampoos mentioned above.
For example, continuing to use the shampoo once every 2 to 4 weeks after the initial treatment, or once a day for a few days before going on holiday, can help prevent tinea versicolor recurring.
As these shampoos are available to buy from pharmacies, you don’t need to see your doctor for a prescription if you run out.
If you develop tinea versicolor again after treatment, you can try treating it yourself with antifungal shampoo, or see your doctor for advice and alternative treatments.
If you have frequent and severe episodes of tinea versicolor, your doctor may consider prescribing antifungal tablets to take a few times a month to prevent the condition recurring.