Contents
What is vaginal discharge
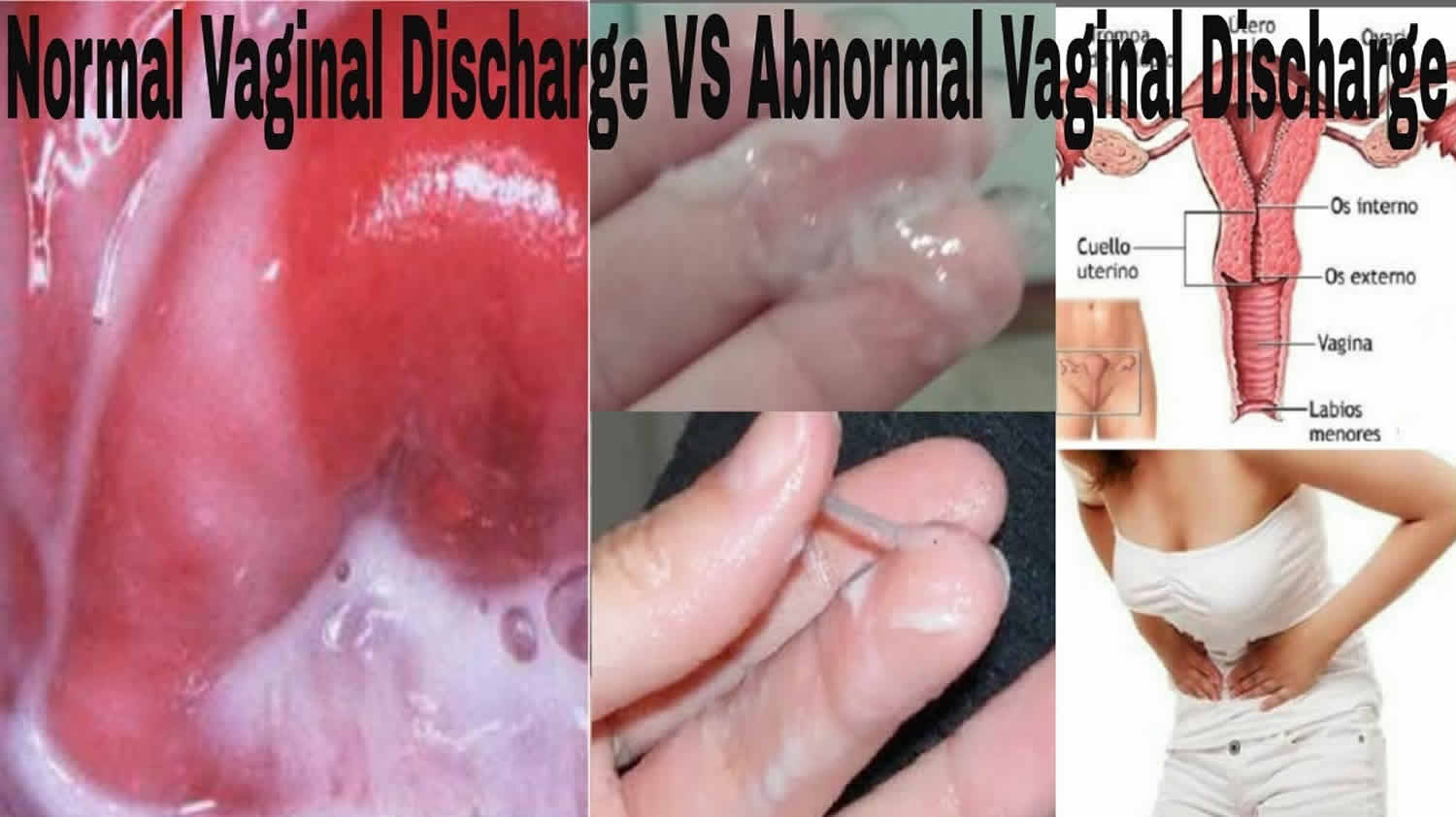
Vaginal discharge is normal – all women, whether they’re pregnant or not, have some vaginal discharge starting a year or two before puberty and ending after the menopause 1. Vaginal discharge is a combination of fluid or mucus, vaginal bacteria and dead cells continuously shed through your vagina that keeps your vagina clean and moist, and protects it from infection. This is because normal vaginal discharge is slightly acidic, which germs don’t like.
Normal vaginal discharge helps keep your vaginal tissues healthy, provide lubrication and protect against infection and irritation. The amount, color and consistency of normal vaginal discharge varies — from whitish and sticky to clear and watery — depending on the stage of your reproductive (menstrual) cycle. Vaginal discharge usually gets heavier just before your period.
Abnormal vaginal discharge — for instance, fluid with an unusual odor or appearance or discharge that occurs along with itching or pain — may be a sign that something’s wrong.
Check if your vaginal discharge is normal.
Vaginal discharge usually isn’t anything to worry about if it:
- doesn’t have a strong or unpleasant smell
- is clear or white
- is thick and sticky
- is slippery and wet
You can get vaginal discharge at any age.
The amount of vaginal discharge varies. You usually get heavier vaginal discharge during pregnancy, if you’re sexually active or if you’re using birth control. It’s often slippery and wet for a few days between your periods (when you ovulate).
You can’t prevent vaginal discharge
Panty liners can help with heavy or excessive discharge or if you’re worried about any smell.
- To help prevent irritation, soreness or dryness:
- DO
- wash gently
- use water and an emollient, such as E45 cream, or plain soap
- DON’T
- use perfumed soaps or gels
- use deodorants or scented hygiene wipes
- douche
- DO
Most causes of abnormal vaginal discharge — such as yeast infection, bacterial vaginosis or menopause symptoms — are relatively harmless, but they can be uncomfortable.
For self-care at home:
- Try an over-the-counter antifungal cream for a suspected yeast infection.
- Use a cold compress, such as a washcloth or ice pack, to relieve itching, swelling or discomfort of the vulva.
- Have your partner use a condom for a week after beginning treatment, or wait a week before having sex.
- See your doctor if your symptoms don’t go away after a week or so.
Abnormal vaginal discharge can also be a symptom of certain sexually transmitted infections (STIs). Since these can spread to involve the uterus, ovaries and fallopian tubes, and can be passed on to sexual partners, detection and treatment of sexually transmitted infections (STIs) is important.
Rarely, a brownish or blood-tinged vaginal discharge could be a sign of cervical cancer.
Possible causes of abnormal vaginal discharge include:
- Causes related to infection or inflammation
- Cervicitis (an inflammation of the cervix)
- Chlamydia trachomatis
- Gonorrhea
- Forgotten (retained) tampon
- Pelvic inflammatory disease (PID) — infection of the female reproductive organs
- Sexually transmitted diseases (STDs)
- Trichomoniasis
- Vaginitis (bacterial vaginosis)
- Yeast infection (vaginal)
- Other causes
- Certain hygiene practices, such as douching or using scented sprays or soaps
- Cervical cancer
- Vaginal atrophy (genitourinary syndrome of menopause)
- Pregnancy
- Rectovaginal fistula (an abnormal opening between the rectum and vagina that allows feces to leak into the vagina)
- Vaginal cancer
- Vaginal fistula
Only rarely is vaginal discharge a sign of cancer.
When vaginal discharge can be a sign of an infection.
If your vaginal discharge changes – for example, in smell, color or texture – it might be a sign of an infection.
| Discharge | Possible cause |
|---|---|
| Smells fishy | bacterial vaginosis |
| Thick and white, like cottage cheese | thrush |
| Green, yellow or frothy | trichomoniasis |
| With pelvic pain or bleeding | chlamydia or gonorrhoea |
| With blisters or sores | genital herpes |
See a doctor or go to a sexual health clinic if:
- Your discharge changes color, smell or texture:
- Greenish, yellowish, thick or cheesy vaginal discharge
- Strong vaginal odor
- Redness, itching, burning or irritation of your vagina or the area of skin that surrounds the vagina and urethra (vulva)
- Bleeding or spotting unrelated to your period
- You produce more discharge than usual
- You feel itchy or sore
- You bleed between periods or after sex
- You get pain when peeing
- You get pain in the area between your tummy and thighs (pelvic pain)
What’s normal vaginal discharge?
Typical vaginal discharge does not have an offensive smell and does not cause any irritation. It’s quite likely that you won’t even know you have any discharge until you see some in your underwear.
It is usually clear or creamy in color. Sometimes there may be a slight yellow tint to it.
Discharge also increases during pregnancy and when you’re sexually aroused.
Vaginal discharge and your menstrual cycle
Vaginal discharge changes throughout your menstrual cycle. Everyone will experience different amounts of discharge.
In the first week after your period a discharge is not usually present; although if some is visible will probably be quite thick.
In the middle of your cycle discharge is normally thin and clear around this time. It may look slightly yellow or brownish if it has been in your underwear for a length of time.
Vaginal discharge during pregnancy
Almost all women have more vaginal discharge in pregnancy 1. This is quite normal and happens for a few reasons. During pregnancy the cervix (neck of the womb) and vaginal walls get softer and discharge increases to help prevent any infections traveling up from the vagina to the womb.
Towards the end of pregnancy, the amount of vaginal discharge increases and can be confused with urine.
In the last week or so of pregnancy, your discharge may contain streaks of thick mucus and some blood. This is called a ‘show’ and happens when the mucus that has been present in your cervix during pregnancy comes away. It’s a sign that the body is starting to prepare for birth, and you may have a few small ‘shows’ in the days before you go into labor.
Increased vaginal discharge is a normal part of pregnancy, but it’s important to keep an eye on it and tell your doctor or midwife if it changes in any way.
When to see your midwife or doctor
- Tell your midwife or doctor if:
- the vaginal discharge is colored especially if it is blood colored
- the vaginal discharge smells strange
- you feel itchy or sore.
Healthy vaginal discharge should be clear and white and should not smell unpleasant. If the vaginal discharge is colored or smells strange, or if you feel itchy or sore, you may have a vaginal infection. If you suspect a bleed (blood) from the vagina see medical advice urgently.
The most common infection is thrush, which your doctor can treat easily. You should not use some thrush medicines in pregnancy.
Always talk to your doctor, pharmacist or midwife if you think you have thrush. You can help prevent thrush by wearing loose cotton underwear, and some women find it helps to avoid perfumed soap or perfumed bath products.
You should also tell your midwife or doctor if your vaginal discharge increases a lot in later pregnancy.
If you have any vaginal bleeding in pregnancy, you should contact your midwife or doctor, as it can sometimes be a sign of a more serious problem such as a miscarriage or a problem with the placenta.
Vaginal discharge after menopause
The vagina tends to lose its moisture after the menopause. This is caused by the lower oestrogen levels. You will still produce small amounts of discharge after menopause though.
However, if you are experiencing yellow-white discharge, it is possible you have an infection. Infection after menopause is common, as the vagina doesn’t produce so much anti-bacterial mucus.
If you are concerned about your vaginal discharge please consult your doctor.
What’s not normal vaginal discharge?
Changes that may signal a problem include an increase in the amount of discharge, a change in the color or smell of the discharge, and irritation, itchiness or burning in or around your vagina. This is called vaginitis. A discharge that’s stained with blood when you’re not having your period could also be a sign of a problem. If you have any of these signs, you should talk to your doctor.
Unusual vaginal discharge is often a sign of infection or inflammation, such as thrush or vaginosis. The signs of an abnormal vaginal discharge are:
- if it’s thick and white, like cottage cheese
- if it smells fishy
- if it’s greenish and smells very bad
- if it’s pink or brown
- if it’s irritating or causes your vaginal area to itch
- if you notice any genital sores or ulcers as well
- if you start having pain in your abdomen or sex becomes painful
- if you have had unprotected sex with someone who may have a sexually transmitted infection (STI).
You should also be on the lookout for symptoms of yeast infections, bacterial vaginosis and trichomoniasis, 3 infections that can cause changes in your vaginal discharge.
Signs of yeast infections
- White, cottage cheese-like discharge
- Swelling and pain around the vulva
- Intense itching
- Painful sexual intercourse
What is a yeast infection?
Small amounts of yeast fungus are often found in a healthy vagina. But if too much grows, it can cause a yeast infection. Yeast infections usually aren’t caught from a sex partner. You may be more likely to get a yeast infection if you are using antibiotics, are pregnant, have diabetes, or stay hot and sweaty for long periods. Some women get frequent yeast infections for no obvious reason.
Signs of bacterial vaginosis
- A white, gray or yellowish vaginal discharge
- A fishy odor that is strongest after sex or after washing with soap
- Itching or burning
- Slight redness and swelling of the vagina or vulva
What is bacterial vaginosis?
Bacterial vaginosis is usually caused by Gardnerella vaginalis bacteria. Why some women get this infection isn’t clear. It’s probably not caught from a sex partner.
Signs of trichomoniasis
- A watery, yellowish or greenish bubbly discharge
- An unpleasant odor
- Pain and itching when urinating
- Most apparent after your period
What is trichomoniasis?
Trichomoniasis is caused by an organism called Trichomonas vaginalis. You can be infected but have no signs for a long time. Trichomoniasis is usually caught by having sex without a condom with someone who is infected.
What sexually transmitted infections present with vaginal discharge?
Chlamydia trachomatis, Neisseria gonorrhoeae, and Trichomonas vaginalis can present with vaginal discharge but may also be asymptomatic. These infections are associated with an increased risk of HIV transmission, especially in the developing world 2. Rates of sexually transmitted diseases (STDs) are rising in the United States 3 and elsewhere, but this observation may be confounded by increased awareness, increased testing, and, importantly, new laboratory techniques 4. Basic epidemiological data about these infections—such as point prevalence, lifetime incidence rate, complication rate, and natural clearance—are scarce for the general population.
Sexually transmitted diseases (STDs) are passed from one person to another through intimate physical contact – such as heavy petting – and from sexual activity including vaginal, oral, and anal sex 3. Sexually transmitted diseases (STDs) are very common. In fact, the Centers for Disease Control and Prevention (CDC) estimates 20 million new infections occur every year in the United States. STDs can mostly be prevented by not having sex. If you do have sex, you can lower your risk by using condoms and being in a sexual relationship with a partner who does not have an STD. Sexually transmitted diseases (STDs) do not always cause symptoms, so it is possible to have an infection and not know it. That is why it is important to get tested if you are having sex. If you are diagnosed with an STD, know that all can be treated with medicine and some can be cured entirely.
There are dozens of STDs. Some sexually transmitted diseases (STDs), such as syphilis, gonorrhea, and chlamydia, are spread mainly by sexual contact. Other diseases, including Zika and Ebola, can be spread sexually but are more often spread through ways other than sex.
Chlamydia is the most common sexually transmitted infection caused by a Chlamydia trachomatis bacterium (an obligate intracellular bacterium) in the US 5. In 2017, a total of 1,708,569 chlamydial infections were reported to CDC in 50 states and the District of Columbia 6. This case count corresponds to a rate of 528.8 cases per 100,000 population. Since many persons with chlamydial infection may have minimal or no symptoms, the actual number of annual infections is significantly higher than the reported cases 7. Based on National Health and Nutrition Examination Surveys (NHANES), chlamydia prevalence in the U.S. is estimated to be 1.5% 8. Chlamydia prevalence is highest among adolescents and young adults, as well as among racial and ethnic minorities. Chlamydia can cause a purulent vaginal discharge, but it is asymptomatic in 80% of women 9. It was thought that 10-40% of untreated chlamydial infections will result in pelvic inflammatory disease 9. Clearly this has implications for information given to patients and screening programmes.
Neisseria gonorrhoeae may present with a purulent vaginal discharge but is asymptomatic in up to 50% of women 10. The true prevalence and epidemiology in the general community is not known 11. Gonorrhoea may be complicated by pelvic inflammatory disease.
Trichomonas vaginalis can cause an offensive yellow vaginal discharge, which is often profuse and frothy, along with associated symptoms of vulval itch and soreness, dysuria, and superficial dyspareunia, but many patients are asymptomatic 12. This infection is associated with preterm delivery 13. The true prevalence and epidemiology in the general community is not known.
The presence of one sexually transmitted infection makes the presence of other infections more likely, but this depends on the population studied 10. For example, in a recent large community screened population in the Netherlands, only 0.2% of woman diagnosed with Chlamydia had concurrent gonorrhoea 14. In contrast, up to 40% of women diagnosed with gonorrhoea have a coexisting chlamydial infection 15. Women who have one sexually transmitted infection are likely to have another, including HIV and syphilis, but the role of routine screening for these infections is not established in the literature 10.
- Vaginal discharge during pregnancy. https://www.pregnancybirthbaby.org.au/vaginal-discharge-during-pregnancy[↩][↩]
- WHO. Sexually transmitted and other reproductive tract infections. 1 Sexually transmitted diseases. 2 HIV infections. 3 Genital diseases, female. 4 Genital diseases, male. 5 Infection. 6 Pregnancy complications, infectious. 7 Rape. 8 Practice guidelines. 9 Developing countries. Geneva: WHO, 2005[↩]
- Sexually Transmitted Diseases (STDs). https://www.cdc.gov/std/[↩][↩]
- Burckhardt F, Warner P, Young H. What is the impact of change in diagnostic test method on surveillance data trends in Chlamydia trachomatis infection? Sex Transm Infect 2006;82:24-30.[↩]
- Chlamydia. https://www.cdc.gov/std/chlamydia/stats.htm[↩]
- Sexually Transmitted Disease Surveillance 2017. https://www.cdc.gov/std/stats17/chlamydia.htm[↩]
- Chlamydial Infections. https://www.cdc.gov/std/tg2015/chlamydia.htm[↩]
- Chlamydia trachomatis trends in the United States among persons 14 to 39 years of age, 1999-2008. https://www.ncbi.nlm.nih.gov/pubmed/22249296[↩]
- Horner PJ, Boag F. National guideline for the management of genital tract infection with Chlamydia trachomatis. Clinical Effectiveness group. British Association for Sexual Health and HIV. 2006[↩][↩]
- Spence D, Melville C. Vaginal discharge. BMJ : British Medical Journal. 2007;335(7630):1147-1151. doi:10.1136/bmj.39378.633287.80. https://www.ncbi.nlm.nih.gov/pmc/articles/PMC2099568/[↩][↩][↩]
- Bignell C. National guideline on the diagnosis and treatment of gonorrhoea in adults. Clinical Effectiveness group. British Association for Sexual Health and HIV. 2005. https://www.bashh.org/[↩]
- Sherrard J. National guideline on the management of Trichomonas vaginalis. Clinical Effectiveness group. British Association for Sexual Health and HIV. 2007. https://www.bashh.org/[↩]
- FFPRHC and BASHH Guidance. The management of women of reproductive age attending non-genitourinary medicine settings complaining of vaginal discharge. J Fam Plann Reprod Health Care 2006;32:33-42.[↩]
- Van Bergen JE, Spaargaren J, Gotz HM, Veldhuijzen IK, Bindels PJ, Coenen TJ, et al. Should asymptomatic persons be tested during population-based Chlamydia screening also for gonorrhoea or only if chlamydial infection is found? BMC Infect Dis 2006;6:42 https://www.ncbi.nlm.nih.gov/pmc/articles/PMC1450285/[↩]
- Bignell C. National guideline on the diagnosis and treatment of gonorrhoea in adults. Clinical Effectiveness group. British Association for Sexual Health and HIV. 2005 https://www.bashh.org[↩]