Contents
- What is msg in food
- How is MSG made ?
- Is MSG safe to eat ?
- Does “glutamate” in a product mean it contains gluten ?
- What’s the difference between MSG and glutamate in food ?
- How can you know if there is MSG in your food ?
- Has there any adverse event reported to the FDA associated with MSG ?
- What is the Chinese restaurant syndrome ?
What is msg in food
Monosodium glutamate or “MSG” also known as sodium glutamate (Flavour enhancer E621), is the sodium salt of the common amino acid glutamic acid 1. Glutamic acid is one of the most abundant naturally occurring non-essential amino acids, naturally present in our bodies and in many foods and food additives 1. Monosodium glutamate is found naturally in tomatoes, cheese and other foods 1.
Other names for MSG:
- Sodium 2-aminopentanedioate
- Glutamic acid, monosodium salt, monohydrate
- L-Glutamic acid, monosodium salt, monohydrate
- L-Monosodium glutamate monohydrate
- Monosodium L-glutamate monohydrate
- MSG monohydrate
- Sodium glutamate monohydrate
- UNII-W81N5U6R6U
- Flavour enhancer E621
Figure 1. Monosodium glutamate chemical structure
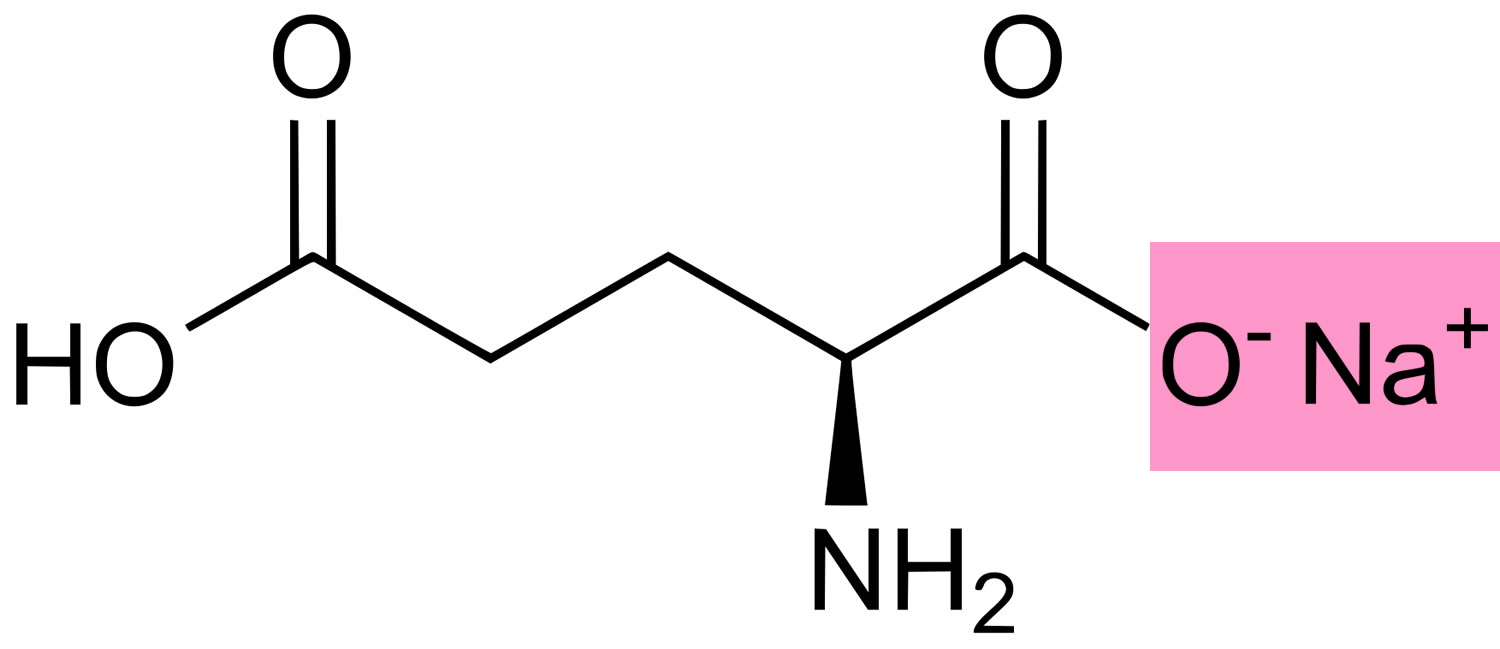
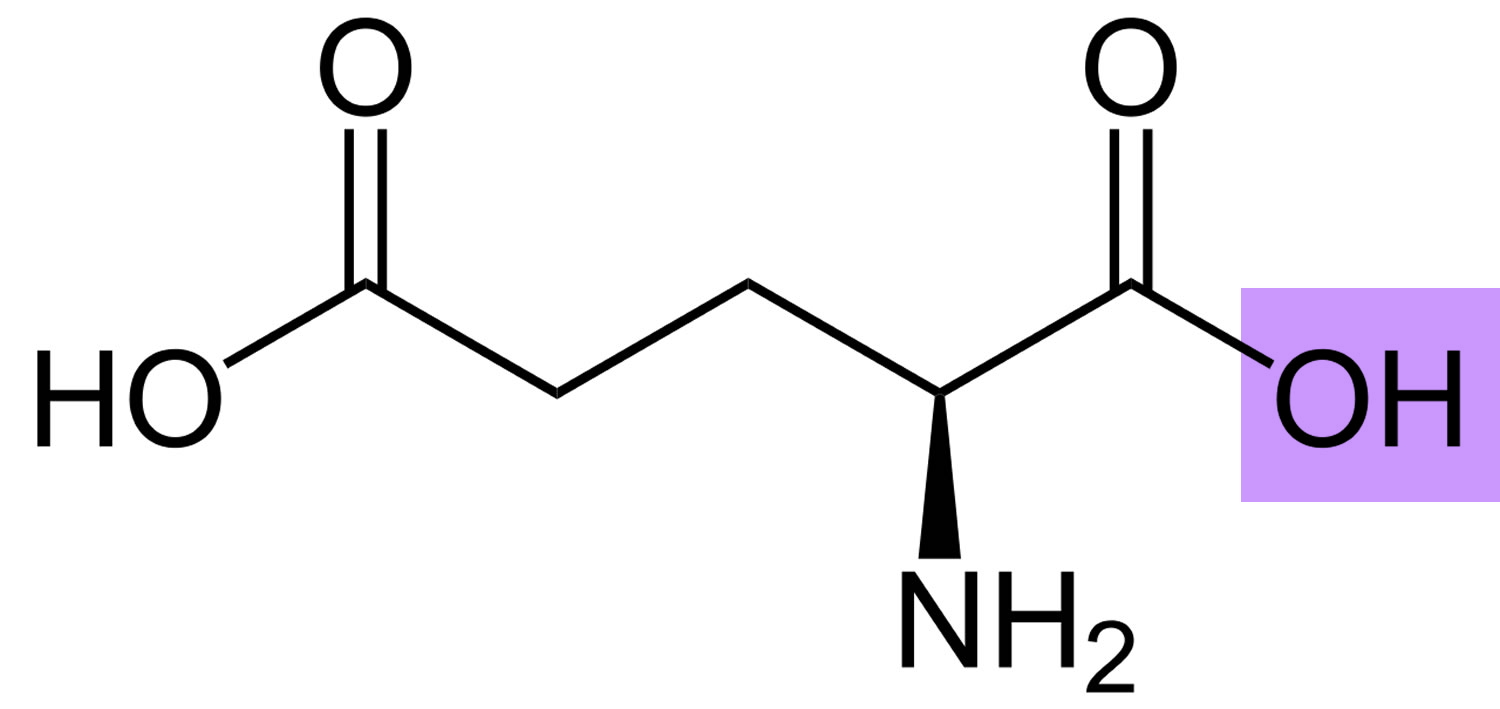
Figure 2. Glutamic acid chemical structure
How is MSG made ?
MSG (monosodium glutamate) occurs naturally in many foods, such as tomatoes and cheeses. People around the world have eaten glutamate-rich foods throughout history. For example, a historical dish in the Asian community is a glutamate-rich seaweed broth. In 1908, a Japanese professor named Kikunae Ikeda was able to extract glutamate from this broth and determined that glutamate provided the savory taste to the soup 1. Professor Ikeda then filed a patent to produce MSG (monosodium glutamate) and commercial production started the following year.
Today, instead of extracting and crystallizing MSG (monosodium glutamate) from seaweed broth, MSG (monosodium glutamate) is produced by the fermentation of starch, sugar beets, sugar cane or molasses 1. This fermentation process is similar to that used to make yogurt, vinegar and wine.
Is MSG safe to eat ?
The U.S. Food and Drug Administration (FDA) considers the addition of MSG (monosodium glutamate) to foods to be “generally recognized as safe” (GRAS) 1. Although many people identify themselves as sensitive to MSG (monosodium glutamate), in studies with such individuals given MSG (monosodium glutamate) or a placebo, scientists have not been able to consistently trigger reactions.
Does “glutamate” in a product mean it contains gluten ?
No—glutamate or glutamic acid have nothing to do with gluten 1. A person with Celiac disease may react to the wheat that may be present in soy sauce, but not to the MSG (monosodium glutamate) in the product.
What’s the difference between MSG and glutamate in food ?
The glutamate in MSG (monosodium glutamate) is chemically indistinguishable from glutamate present in food proteins 1. Our bodies ultimately metabolize both sources of glutamate in the same way. An average adult consumes approximately 13 grams of glutamate each day from the protein in food, while intake of added MSG (monosodium glutamate) is estimates at around 0.55 grams per day.
How can you know if there is MSG in your food ?
The FDA requires that foods containing added MSG (monosodium glutamate) list it in the ingredient panel on the packaging as monosodium glutamate. However, MSG (monosodium glutamate) occurs naturally in ingredients such as hydrolyzed vegetable protein, autolyzed yeast, hydrolyzed yeast, yeast extract, soy extracts, and protein isolate, as well as in tomatoes and cheeses 1. While the FDA requires that these products be listed on the ingredient panel, the agency does not require the label to also specify that they naturally contain MSG. However, foods with any ingredient that naturally contains MSG cannot claim “No MSG” or “No added MSG” on their packaging. MSG also cannot be listed as “spices and flavoring.”
Has there any adverse event reported to the FDA associated with MSG ?
Over the years, the FDA has received reports of symptoms such as headache and nausea after eating foods containing MSG (monosodium glutamate) 1. However, the FDA were never able to confirm that the MSG caused the reported effects 1.
These adverse event reports helped trigger the FDA to ask the independent scientific group Federation of American Societies for Experimental Biology to examine the safety of MSG in the 1990s. FASEB’s report 2 concluded that MSG is safe.
The FASEB report identified some short-term, transient, and generally mild symptoms, such as 2:
- headache 3,
- numbness,
- flushing,
- tingling,
- palpitations, and
- drowsiness that may occur in some sensitive individuals who consume 3 grams or more of MSG without food.
In a double-blind placebo-controlled, randomized study involving subjects who self-identified as being MSG-sensitive 4:757–762. https://www.ncbi.nlm.nih.gov/pubmed/9215242)). A positive response to challenge was defined as the reproduction of > of 2 of the specific symptoms in a subject ascertained on prechallenge interview. Sixty-one subjects entered the study. On initial challenge with 5 g MSG, 18 (29.5%) responded to neither MSG nor placebo, 6 (9.8%) to both, 15 (24.6%) to placebo, and 22 (36.1%) to MSG. Rechallenge with placebo and increasing dose of MSG from 1.25 g, 2.5 g and 5 gm MSG, revealed an apparent threshold dose for reactivity of 2.5 gm MSG. Headache, muscle tightness, numbness/tingling, general weakness and flushing occurred more frequently after MSG than placebo ingestion.
However, a typical serving of a food with added MSG contains less than 0.5 grams of MSG. Consuming more than 3 grams of MSG without food at one time is unlikely 1.
What is the Chinese restaurant syndrome ?
Chinese restaurant syndrome is a set of symptoms that some people have after eating Chinese food 5.
Alternative Names
- Hot dog headache;
- Glutamate-induced asthma;
- MSG (monosodium glutamate) syndrome
A food additive called monosodium glutamate (MSG) has been blamed for the condition. However, this has not been proven to be the cause 5. A study 6 involving 71 volunteers fed 1.5 g, 3.0 g and 3.15 g of MSG over breakfast for 5 straight days found no adverse reactions or side effects compared to placebo. That study led to the conclusion that ‘Chinese Restaurant Syndrome’ is an anecdote applied to a variety of postprandial illnesses; rigorous and realistic scientific evidence linking the syndrome to MSG could not be found 6.
Causes of Chinese restaurant syndrome
Reports of serious reactions to Chinese food first appeared in 1968. At that time, MSG was thought to be the cause of these symptoms. There have been many studies since then that have failed to show a connection between MSG and the symptoms some people describe.
For this reason, MSG continues to be used in some meals. However, it is possible that some people are particularly sensitive to food additives. MSG is chemically similar to one of the brain’s most important chemicals, glutamate.
Symptoms of Chinese restaurant syndrome
Symptoms include 7:
- Chest pain
- Flushing
- Headache
- Numbness or burning in or around the mouth
- Sense of facial pressure or swelling
- Sweating
Exams and Tests for Chinese restaurant syndrome
Chinese restaurant syndrome is most often diagnosed based on the symptoms. The health care provider may ask the following questions as well:
- Have you eaten Chinese food within the past 2 hours?
- Have you eaten any other food that may contain monosodium glutamate within the past 2 hours?
The following signs may also be used to aid in diagnosis:
- Abnormal heart rhythm observed on an electrocardiogram
- Decreased air entry into the lungs
- Rapid heart rate
Treatment of Chinese restaurant syndrome
Treatment depends on the symptoms. Most mild symptoms, such as headache or flushing, need no treatment.
Life-threatening symptoms require immediate medical attention. They may be similar to other severe allergic reactions and include 8:
- Chest pain
- Heart palpitations
- Shortness of breath
- Swelling of the throat
Outlook (Prognosis) for Chinese restaurant syndrome
Most people recover from mild cases of Chinese restaurant syndrome without treatment and have no lasting problems.
People who have had life-threatening reactions need to be extra careful about what they eat. They should also always carry medicines prescribed by their provider for emergency treatment.
- Questions and Answers on Monosodium glutamate (MSG). U.S. Food and Drug Administration. https://www.fda.gov/food/ingredientspackaginglabeling/foodadditivesingredients/ucm328728.htm[↩][↩][↩][↩][↩][↩][↩][↩][↩][↩][↩][↩]
- Federation of American Societies for Experimental Biology. Analysis of Adverse Reactions To Monosodium Glutamate (MSG). https://www.faseb.org/Portals/2/PDFs/LSRO_Legacy_Reports/1995_Executive%20Summary%20From%20the%20Report_Analysis%20of%20Adverse%20Reactions%20to%20Monosodium%20Glutamate%20MSG%20Report.pdf[↩][↩]
- MSG and hydrolyzed vegetable protein induced headache: review and case studies. Scopp AL. Headache. 1991 Feb; 31(2):107-10. https://www.ncbi.nlm.nih.gov/pubmed/2030071/[↩]
- Yang WH, Drouin MA, Herbert M, Mao Y, Karsh J. The monosodium glutamate symptom complex: assessment in a double-blind, placebo-controlled, randomized study. J Allergy Clin Immunol. 1997;99((6 Pt 1[↩]
- Chinese restaurant syndrome. Medline Plus. https://medlineplus.gov/ency/article/001126.htm[↩][↩]
- Monosodium L-glutamate: a double-blind study and review. Food Chem Toxicol. 1993 Dec;31(12):1019-35. https://www.ncbi.nlm.nih.gov/pubmed/8282275[↩][↩]
- Aronson JK. Monosodium glutamate. In: Aronson JK, ed. Meyler’s Side Effects of Drugs. 16th ed. Philadelphia, PA: Elsevier; 2016:1103-1104.[↩]
- Bush RK, Taylor SL. Reactions to food and drug additives. In: Adkinson NF, Bochner BS, Burks AW, et al, eds. Middleton’s Allergy: Principles and Practice. 8th ed. Philadelphia, PA: Elsevier Saunders; 2014:chap 82.[↩]