Contents
What is popcorn lung
Popcorn lung is the laymen term for bronchiolitis obliterans. Bronchiolitis obliterans is an inflammatory obstruction of the lung’s tiniest airways, called bronchioles 1. The bronchioles become damaged and inflamed by chemical particles, inhalation of gases (e.g., anhydrous ammonia) or respiratory infections, particularly after organ transplants, leading to extensive scarring that blocks the airways. There are 2 major forms of bronchiolitis obliterans, obliterative bronchiolitis and constrictive bronchiolitis. Popcorn lung is sometimes referred to as constrictive bronchiolitis, a similar condition in which the small airways become constricted in diameter because of inflammation and scarring. The constrictive form is more common and may or may not be associated with other forms of diffuse lung injury. Recently, cases of bronchiolitis obliterans have been reported in workers exposed to the chemical diacetyl during the manufacture of butter-flavored microwave popcorn 2 and coffee processing facility producing both unflavored and flavored coffee 3. So-called popcorn workers’ lung may occur in workers exposed to other flavorings and in some consumers exposed to this chemical 4. When bronchiolitis obliterans occurs after lung transplantation or hematopoietic stem cell transplantation it is called bronchiolitis obliterans syndrome 5.
Bronchiolitis obliterans is a rare disease with characteristic features of fibrosis of terminal and distal bronchioles and spirometry showing airflow obstruction. Bronchiolitis obliterans usually leads to progressive decline in lung function and has variable outcomes.
Is popcorn lung real?
Yes. Popcorn lung is sometimes referred to as constrictive bronchiolitis, a similar condition in which the small airways become constricted in diameter because of inflammation and scarring. Recently, cases of bronchiolitis obliterans have been reported in workers exposed to the chemical diacetyl during the manufacture of butter-flavored microwave popcorn. So-called popcorn workers’ lung may occur in workers exposed to other flavorings and in some consumers exposed to this chemical 6.
How long does it take to get popcorn lung?
From small sample case reports, most workers who worked at the microwave popcorn packaging plant developed gradual onset of symptoms between 5 months and 5 years after starting work at the plant 7.
Is there a cure for popcorn lung disease?
Popcorn lung has no cure and is progressive. Most patients need some type of medical therapy to relieve the symptoms.
Is popcorn lung fatal?
The overall outlook for most patients is guarded and the quality of life is poor. Most patients do die prematurely from respiratory failure 8.
What causes popcorn lung
Popcorn lung can be caused by breathing in irritant fumes, such as chlorine, ammonia, oxides of nitrogen or sulfur dioxide. Diacetyl and its substitute, 2,3-pentanedione, a chemical used to provide butter flavor in many foods 9 and commonly used in e-cigarette flavoring 10, has been shown to cause bronchiolitis obliterans in workers who manufacture it or mix it into foods, such as butter-flavored popcorn 5.
What chemical causes popcorn lung?
Diacetyl and its substitute, 2,3-pentanedione, are chemicals that are used extensively to add flavorings to electronic cigarettes, some microwave popcorns and other foods and liquids. Inhaling diacetyl, especially the heated chemical, has been linked to serious respiratory diseases including bronchiolitis obliterans which is irreversible 11. In addition, 2,3-pentanedione is chemically similar and has had similar effects in animal models. The first observation of obliterative bronchiolitis in a food production employee may have occurred in 1985 in a facility where diacetyl was listed among ingredients used in making flavorings for the baking industry 12.
When inhaled, diacetyl can cause a persistent dry cough, shortness of breath, wheezing, phlegm production, fatigue, drowsiness, headache, fever, aches and nausea. However, exposed workers have developed lung disease in the absence of these warning symptoms. Diacetyl vapors irritate the eyes, skin, nose and throat and may lead to fixed airway restriction or obstruction. Diacetyl is also known as butanedione, 2,3-butandedione and food flavorings containing diacetyl (FFCD).
In 2012, National Institute for Occupational Safety and Health identified obliterative bronchiolitis in a group of workers that used artificial flavorings to produce and package flavored whole-bean and ground roasted coffee 13. It was determined that diacetyl in the artificial coffee flavorings was responsible for causing these new cases of disease 3. This led to a series of investigations at coffee roasting and packaging facilities. As part of these ongoing investigations, the National Institute for Occupational Safety and Health is evaluating diacetly, 2,3-pentanedione, and other chemicals that are naturally produced and released during the coffee roasting process 3. Grinding roasted coffee beans produces a greater surface area for off-gassing (sometimes called degassing) of these compounds.
In addition to diacetyl, here are other common and dangerous chemicals to avoid:
Acetaldehyde
Acetaldehyde is in cannabis and e-cigarette smoke. It irritates the skin, eyes, mucous membranes, throat and respiratory tract. It can also cause nausea, vomiting, headache, drowsiness, delirium and hallucinations in high concentrations. Other effects of acetaldehyde can include damage the mucous lining of the mouth, throat, stomach; skin irritation; kidney and liver damage; and cancer. Acetaldehyde is also known as acetic aldehyde, ethanal, ethyl aldehyde.
Formaldehyde
This colorless, flammable gas is used in building materials, household products, pressed-wood products, glues and adhesives, some fabrics, insulation materials, paper coatings, fungicides, germicides, disinfectants, and medical and scientific preservatives. Formaldehyde is a carcinogen. It has a strong odor and can irritate the eyes, nose, skin and throat, and causes coughing, wheezing and nausea. Formaldehyde is also known as methanal.
Nicotine
This chemical compound is a stimulant drug that is found in the nightshade family of plants including nicotiana rustica, cultivated tobacco and asclepias syriaca.
Nicotine is highly addictive and is associated with cardiovascular disease, birth defects, lung infections. Inhaling nicotine stimulates production of saliva and phlegm, increases heart rate and blood pressure, elevates serum cholesterol levels, promotes blood clot formation, and aids in plaque formation in the cardiovascular system.
Bronchiolitis obliterans also can result from respiratory infections, a connective tissue disorder such as rheumatoid arthritis, a medication reaction, and after a bone marrow, lung or heart-lung transplant. Also, the disease may be idiopathic (without a known cause).
Popcorn lung pathophysiology
In response to injury from inhalational toxins or autoimmune responses, there is inflammation of subepithelial structures and dysregulated repair, leading to fibroproliferation and abnormal regeneration of epithelium of the small airways. Histopathology classically demonstrates the involvement of terminal and respiratory bronchioles (distal small airways) but without significant changes in alveolar spaces and distal lung parenchyma. Hypertrophy of the smooth muscles of the bronchioles, peribronchiolar inflammatory infiltrates, accumulation of mucus in the bronchiolar lumen, and bronchiolar scarring can be noted in bronchiolitis obliterans 14. There is a concentric narrowing of the lumen of the bronchioles by the inflammatory fibrosis. There may even be complete occlusion of the lumen in some cases.
In lung transplantation, microvascular insufficiency and alloimmune responses to the transplanted lung may result in airway injury and development of bronchiolitis obliterans syndrome. Episodes of acute cellular rejection, HLA antibodies and gastroesophageal reflux disease with microaspiration have been shown to increase the risk of development of bronchiolitis obliterans syndrome after transplantation.
In bronchiolitis obliterans associated with paraneoplastic pemphigus, autoantibodies against desmoglein and plakin protein which are found both in cutaneous and respiratory epithelium have been implicated.
Popcorn lung symptoms
Popcorn lung (bronchiolitis obliterans) usually causes a dry cough and shortness of breath (dyspnea) that are persistent and progressive, especially on exertion, two to eight weeks after toxic fume exposure or a respiratory illness. Some may also have wheezing. Symptoms usually develop over weeks to months and are not episodic, unlike asthma. It may be several months or years until it presents itself after a transplant.
Fatigue and wheezing in the absence of a cold or asthma are other symptoms of popcorn lung disease.
Popcorn lung diagnosis
History may also elicit recent exposure to toxic fumes or gases, viral infections, symptoms of joint stiffness in cases of rheumatoid arthritis, prior lung or hematopoietic stem cell transplantation.
A physical exam may reveal decreased breath sounds and prolonged expiratory phase with or without wheeze. Rales may also be noted in some cases. Cases of bronchiolitis obliterans associated with Castleman’s disease may also have paraneoplastic pemphigus which may present with oral ulcers as well as lymphadenopathy.
Pulmonary function testing is essential for diagnosis 5. Spirometry demonstrates airflow obstruction that does not reverse with inhaled bronchodilator challenge. Forced expiratory volume in one second (FEV1) will be reduced and the ratio of FEV1 to Forced vital capacity (FEV1/FVC) is also reduced. Hyperinflation may occur, and hence Total lung capacity (TLC) may be increased. Diffusion capacity (DLCO) is usually reduced 15. The degree of forced expiratory volume in one second (FEV1) decline from post-transplant value determines the stage of bronchiolitis obliterans syndrome in lung transplant.
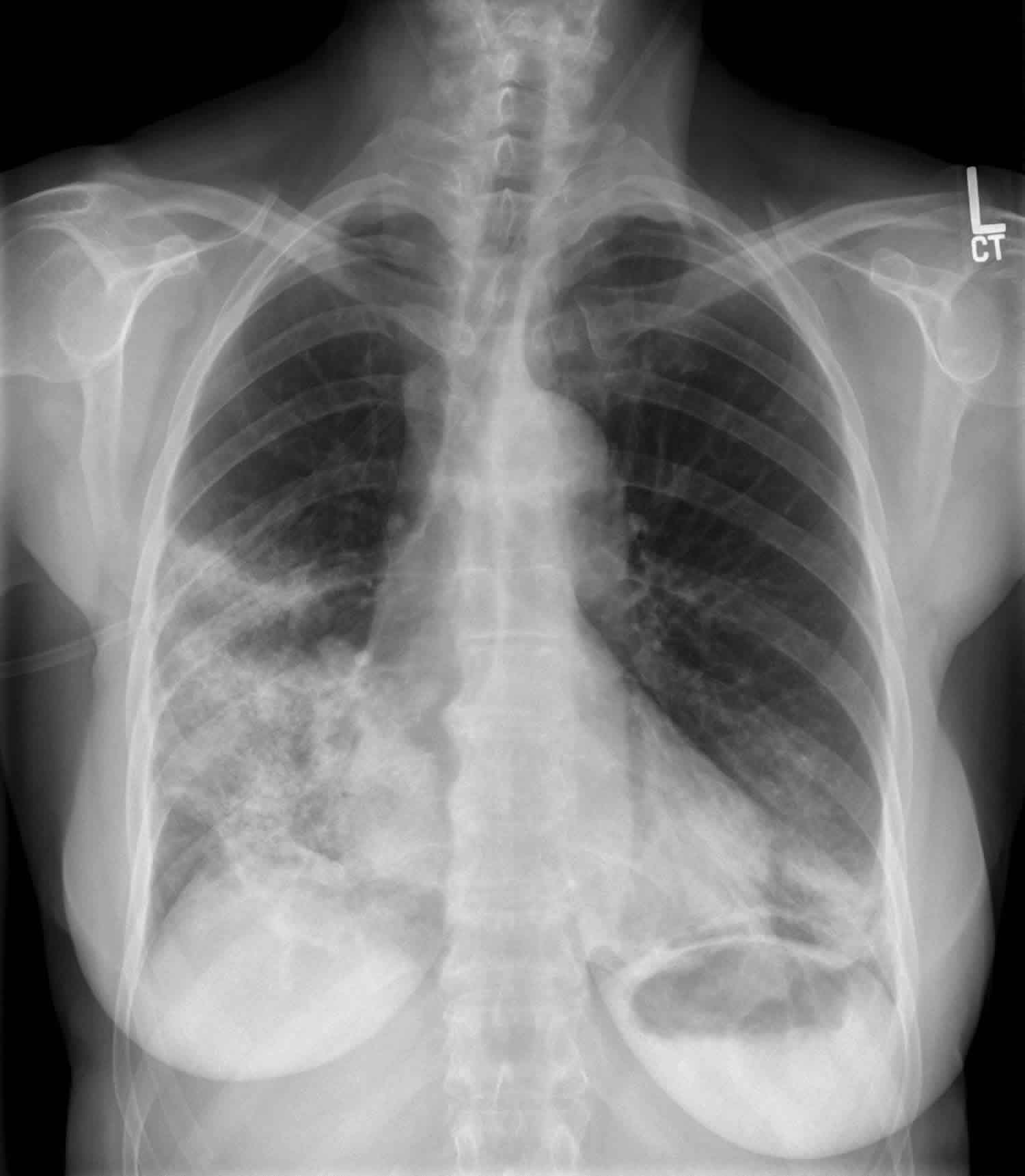
Chest radiographs may be normal in early disease or show signs of hyperinflation. Chest CT imaging may show bronchial wall thickening, patchy areas of hypo attenuation. If there are dynamic images with inspiratory and expiratory films, a mosaic pattern of perfusion may be noted due to air trapping from small airway disease.
Bronchoscopy can be performed if other causes of airflow obstruction are suspected like endobronchial tumor or sarcoid, but may be unrevealing in bronchiolitis obliterans. A lung biopsy is usually not necessary for diagnosis in the setting of classic symptoms, air trapping on imaging, airflow obstruction on spirometry in the setting of organ transplantation or toxic inhalational injury. If required for diagnosis, surgical lung biopsy is preferred over transbronchial biopsy since it involves distal bronchioles and not parenchyma. In cases following lung transplantation, a biopsy is not required for the diagnosis of bronchiolitis obliterans syndrome but may be required to exclude other causes of deterioration lung function like infection or acute rejection. Spirometry showing obstructive pattern is necessary for diagnosis.
Imaging tests (such as high resolution chest CT scan) and pulmonary function tests can help detect bronchiolitis obliterans.
Popcorn lung treatment
Popcorn lung disease is irreversible. Treatment, however, can help to stabilize or at least slow its progression. For that reason, it is important to recognize popcorn lung early because intervention in the late stages of popcorn lung disease may prove ineffective.
Treatment usually involves medication therapy, primarily the use of corticosteroids. In some cases, immunosuppressive therapies, which decrease the body’s immune response, and lung transplants are used to treat the disease. Immunosuppression with corticosteroids and cytotoxic agents like cyclophosphamide have been used for bronchiolitis obliterans related to rheumatoid arthritis, but have not been beneficial for bronchiolitis obliterans from toxic inhalation or post infectious etiology. In these patients, symptomatic treatment should be provided with cough suppressants, inhaled bronchodilators, and oxygen supplementation if needed.
In the case of toxic exposures, immediate removal from the irritating environment and offending agents is crucial to slowing progression of popcorn lung disease.
If left untreated, bronchiolitis obliterans can be fatal. It is the primary cause of death following a lung or heart-lung transplant.
Treatment of bronchiolitis obliterans syndrome after lung transplant involves augmenting immunosuppression since it is thought to be a form of chronic rejection. Hence, increasing or addition of immunosuppressive agents like tacrolimus, cyclosporine, mycophenolate mofetil, and prednisone has been used to treat bronchiolitis obliterans syndrome after transplant. Azithromycin has also been shown to decrease the incidence of bronchiolitis obliterans syndrome and improvement in lung function. The combination of inhaled fluticasone, oral montelukast and azithromycin triple therapy has also shown to decrease decline in lung function in bronchiolitis obliterans syndrome post-hematopoietic stem cell transplantation. In addition to these therapies, controlling gastro esophageal reflux is also recommended to decrease bronchiolitis obliterans syndrome. In cases where bronchiolitis obliterans syndrome is progressive and severe, then retransplantation of a lung may be indicated 16. Extracorporeal photopheresis has also been successfully used to slow the decline in lung function from bronchiolitis obliterans syndrome.
Popcorn lung prognosis
Prognosis of patients with bronchiolitis obliterans is poor, and some may have a rapid decline in lung function. The clinical course of bronchiolitis obliterans syndrome related to lung or hematopoietic stem cell transplant is variable with some patients being asymptomatic or stable after diagnosis and some patients with the slow and steady decline and others with an episodic drop in FEV1. If bronchiolitis obliterans syndrome develops with two years of lung transplantation, it is seen as predictive of worse outcome.
Retransplant is an option but most patients are frail and not fit for surgery. Patients managed with corticosteroids and cytotoxic drugs also develop a whole host of adverse drug reactions.
The overall outlook for most patients is guarded and the quality of life is poor. Most patients do die prematurely from respiratory failure 8.
- Chambers DC. Bronchiolitis obliterans syndrome ‘endotypes’ in haematopoietic stem cell transplantation. Respirology. 2019 Feb 07[↩]
- Clinical bronchiolitis obliterans in workers at a microwave-popcorn plant. N Engl J Med. 2002 Aug 1;347(5):330-8. DOI: 10.1056/NEJMoa020300[↩]
- Duling MG, LeBouf RF, Cox-Ganser JM, Kreiss K, Martin SB Jr, Bailey RL. Environmental characterization of a coffee processing workplace with obliterative bronchiolitis in former workers. J Occup Environ Hyg. 2016;13(10):770–781. doi:10.1080/15459624.2016.1177649 https://www.ncbi.nlm.nih.gov/pmc/articles/PMC5836548[↩][↩][↩]
- National Institute for Occupational Safety and Health (NIOSH) Draft Criteria for a Recommended Standard: Occupational Exposure to Diacetyl and 2,3-Pentanedione. https://www.cdc.gov/niosh/docket/archive/pdfs/NIOSH-245/0245-081211-draftdocument.pdf[↩]
- Krishna R, Oliver TI. Bronchiolitis Obliterans (Obliterative Bronchiolitis, Constrictive Bronchiolitis) [Updated 2019 Mar 13]. In: StatPearls [Internet]. Treasure Island (FL): StatPearls Publishing; 2019 Jan-. Available from: https://www.ncbi.nlm.nih.gov/books/NBK441865[↩][↩][↩]
- Bronchiolitis Obliterans. https://www.nationaljewish.org/conditions/bronchiolitis-obliterans[↩]
- Akpinar-Elci M, Kanwal R, Kreiss K [2002]. Bronchiolitis obliterans syndrome in popcorn plant workers. Am J Respir Crit Care Med 165:A 526[↩]
- Bondeelle L, Bergeron A. Managing pulmonary complications in allogeneic hematopoietic stem cell transplantation. Expert Rev Respir Med. 2018 Dec 07[↩][↩]
- Pierce JS, Abelmann A, Finley BL. Comment on “Flavoring Chemicals in E-Cigarettes: Diacetyl, 2,3-Pentanedione, and Acetoin in a Sample of 51 Products, Including Fruit-, Candy-, and Cocktail-Flavored E-Cigarettes”. Environ Health Perspect. 2016;124(6):A100–A101. doi:10.1289/ehp.1611350 https://www.ncbi.nlm.nih.gov/pmc/articles/PMC4892932[↩]
- Allen JG, Flanigan SS, LeBlanc M, et al. Flavoring Chemicals in E-Cigarettes: Diacetyl, 2,3-Pentanedione, and Acetoin in a Sample of 51 Products, Including Fruit-, Candy-, and Cocktail-Flavored E-Cigarettes. Environ Health Perspect. 2015;124(6):733–739. doi:10.1289/ehp.1510185 https://www.ncbi.nlm.nih.gov/pmc/articles/PMC4892929[↩]
- FLAVORINGS-RELATED LUNG DISEASE. https://www.cdc.gov/niosh/topics/flavorings/[↩]
- Health Hazard Evaluation Report. https://www.cdc.gov/niosh/hhe/reports/pdfs/1985-0171-1710.pdf[↩]
- Obliterative bronchiolitis in workers in a coffee-processing facility – Texas, 2008-2012. Centers for Disease Control and Prevention (CDC). MMWR Morb Mortal Wkly Rep. 2013 Apr 26; 62(16):305-7.[↩]
- Colom AJ, Teper AM. Post-infectious bronchiolitis obliterans. Pediatr. Pulmonol. 2019 Feb;54(2):212-219.[↩]
- Kavaliunaite E, Aurora P. Diagnosing and managing bronchiolitis obliterans in children. Expert Rev Respir Med. 2019 Feb 23;:1-8[↩]
- Williams KM. How I treat bronchiolitis obliterans syndrome after hematopoietic stem cell transplantation. Blood. 2017 Jan 26;129(4):448-455[↩]