Contents
What are ovaries
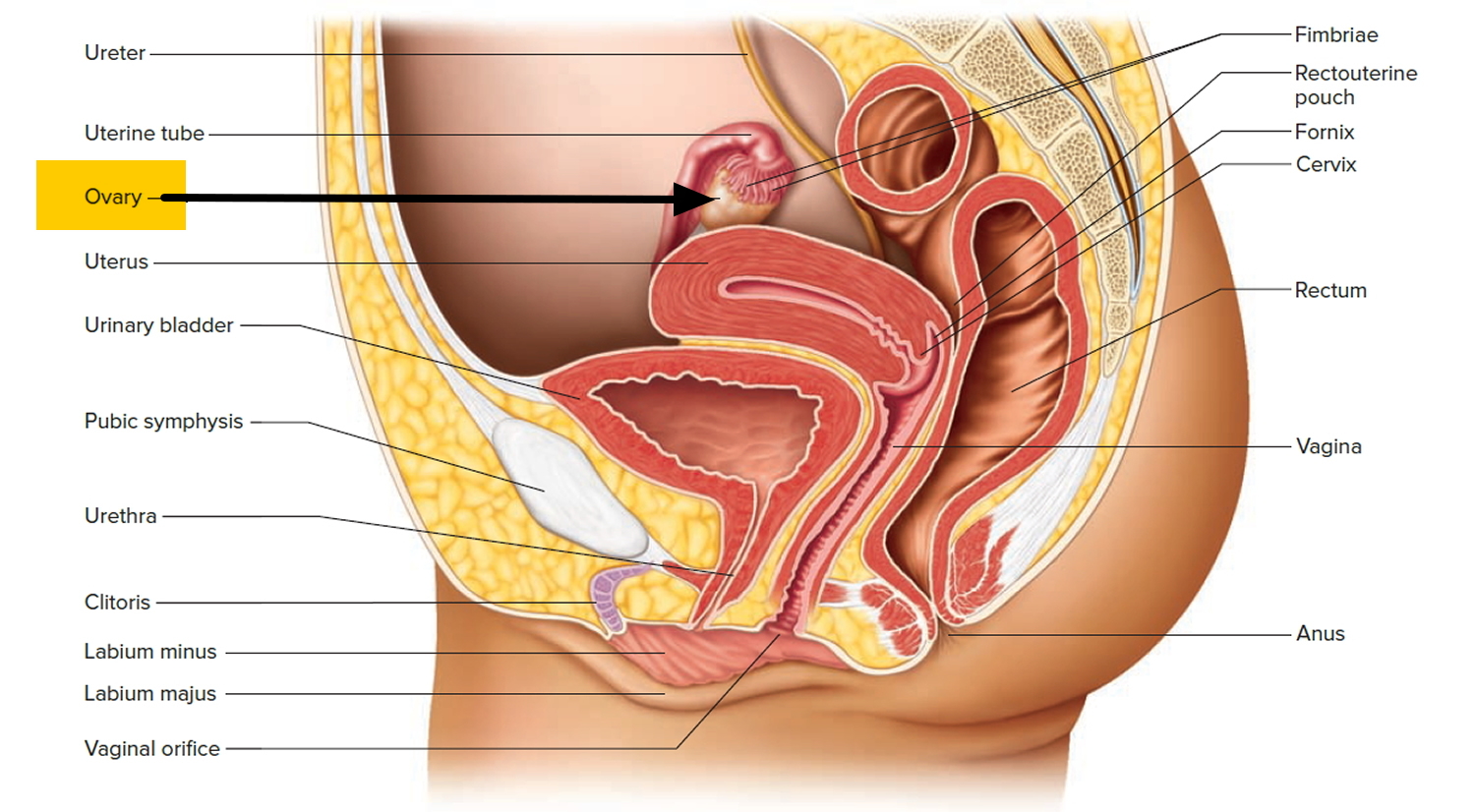
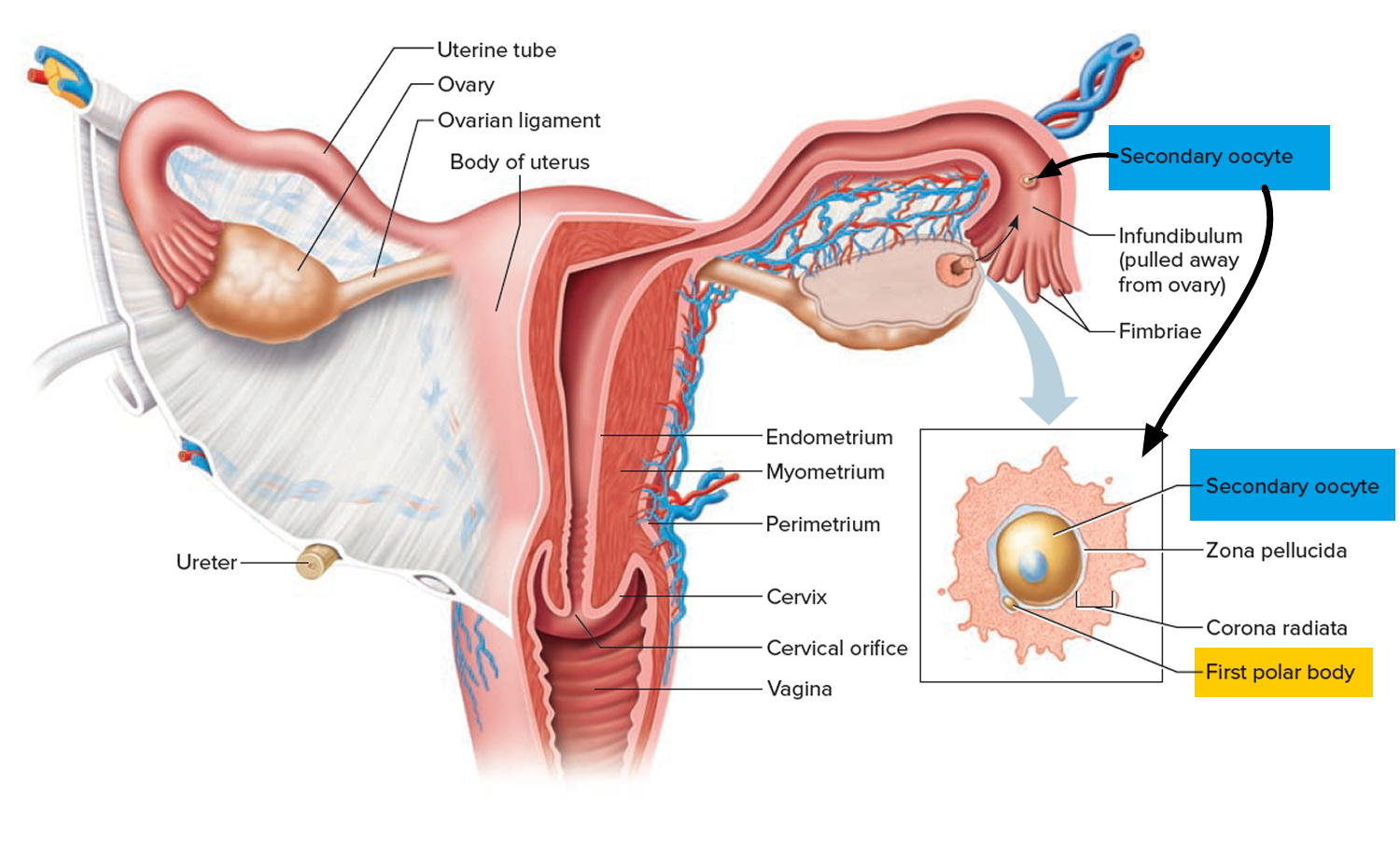
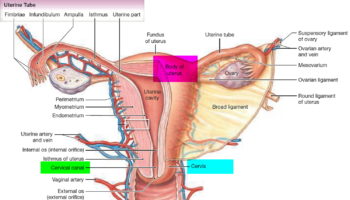
The ovaries are a pair of female reproductive glands in which the ova, or eggs, are formed. The two ovaries are solid, ovoid structures, each about 3.5 centimeters long, 2 centimeters wide, and 1 centimeter thick. The ovaries lie in shallow depressions in the lateral wall of the pelvic cavity one on each side of the uterus (see Figure 2).
Baby girls are born with all the egg cells in their ovaries that they will have in their lifetime 1. These egg cells lie in small pockets called follicles. Once puberty starts, different hormones ripen the first follicle so that it will release an egg cell (ovum). In addition to their role in producing ova, the ovaries also have the distinction of being an endocrine gland because they secrete hormones—primarily estrogen and progesterone—that are vital to normal reproductive development and fertility. Hormones are substances produced by the body that act as chemical transmitters. They regulate body functions like the menstrual cycle and body temperature. Hormones also trigger ovulation and promote the healthy development of female sex characteristics during puberty and to ensure fertility.
Progesterone and estrogen are necessary to prepare the uterus for menstruation, and their release is triggered by the hypothalamus.
Once you reach puberty, the ovaries release a single egg each month (the ovaries typically alternate releasing an egg)—this is called ovulation. The hypothalamus sends a signal to the pituitary gland to release gonadotrophic substances (follicle stimulating hormone [FSH] and luteinizing hormone [LH]). These hormones are essential to normal reproductive function—including regulation of the menstrual cycle.
As the egg migrates down the fallopian tube, progesterone is released. It is secreted by a temporary gland formed within the ovary after ovulation called the corpus luteum. Progesterone prepares the body for pregnancy by causing the uterine lining to thicken. If a woman is not pregnant, the corpus luteum disappears.
If a woman is pregnant, the pregnancy will trigger high levels of estrogen and progesterone, which prevent further eggs from maturing. Progesterone is secreted to prevent uterine contractions that may disturb the growing embryo. The hormone also prepares the breasts for lactation.
Increased estrogen levels near the end of pregnancy alert the pituitary gland to release oxytocin, which causes uterine contractions. Before delivery, the ovaries release relaxin, which as the name suggests, loosens the pelvic ligaments in preparation for labor.
More hormones are released during pregnancy than at any other time of a woman’s life, but during menopause—which marks the end of fertility—estrogen levels fall fast. This can lead to a range of complications.
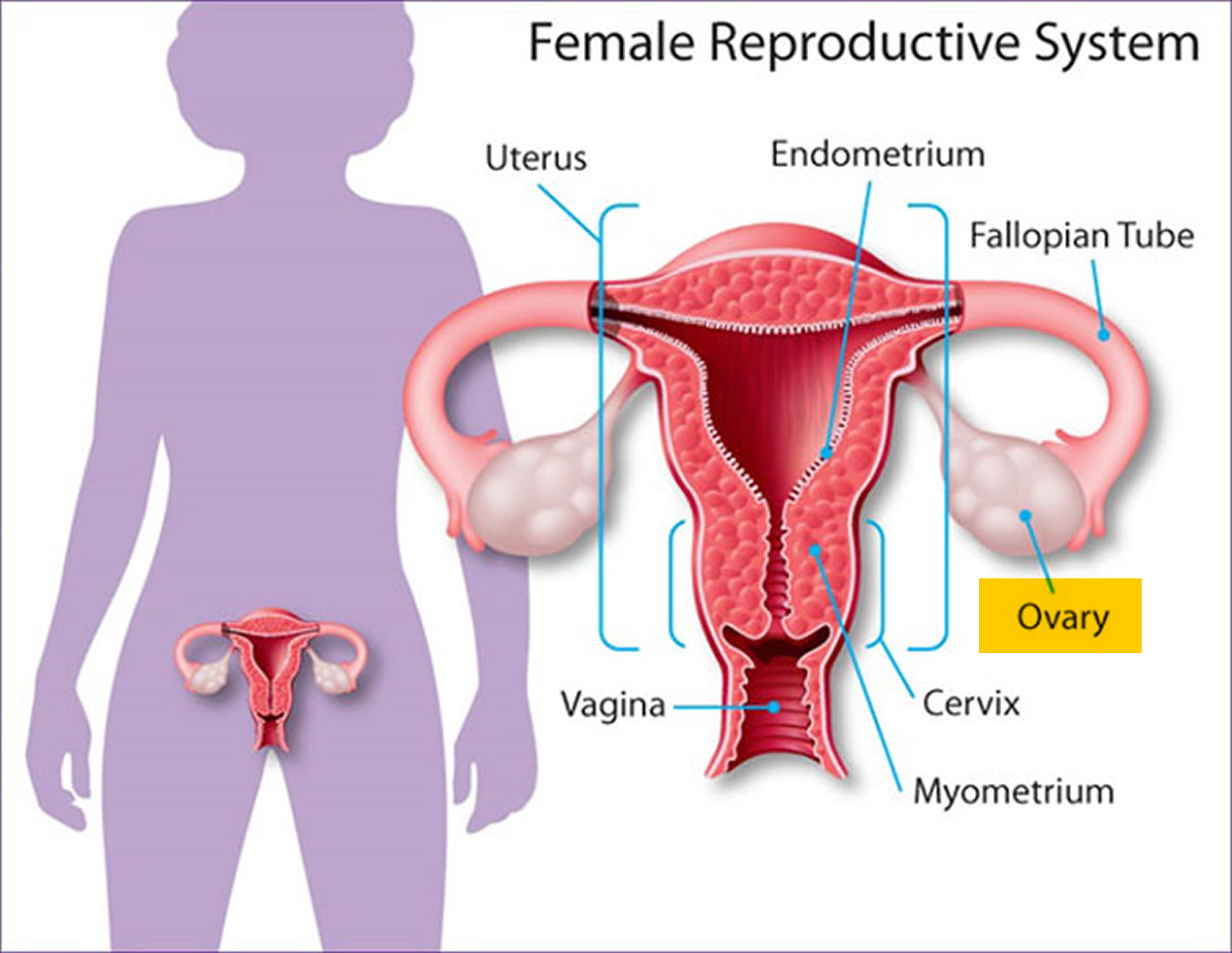
Figure 1. Female reproductive system
Figure 2. The ovaries lie in shallow depressions in the lateral wall of the pelvic cavity
Function of the ovaries
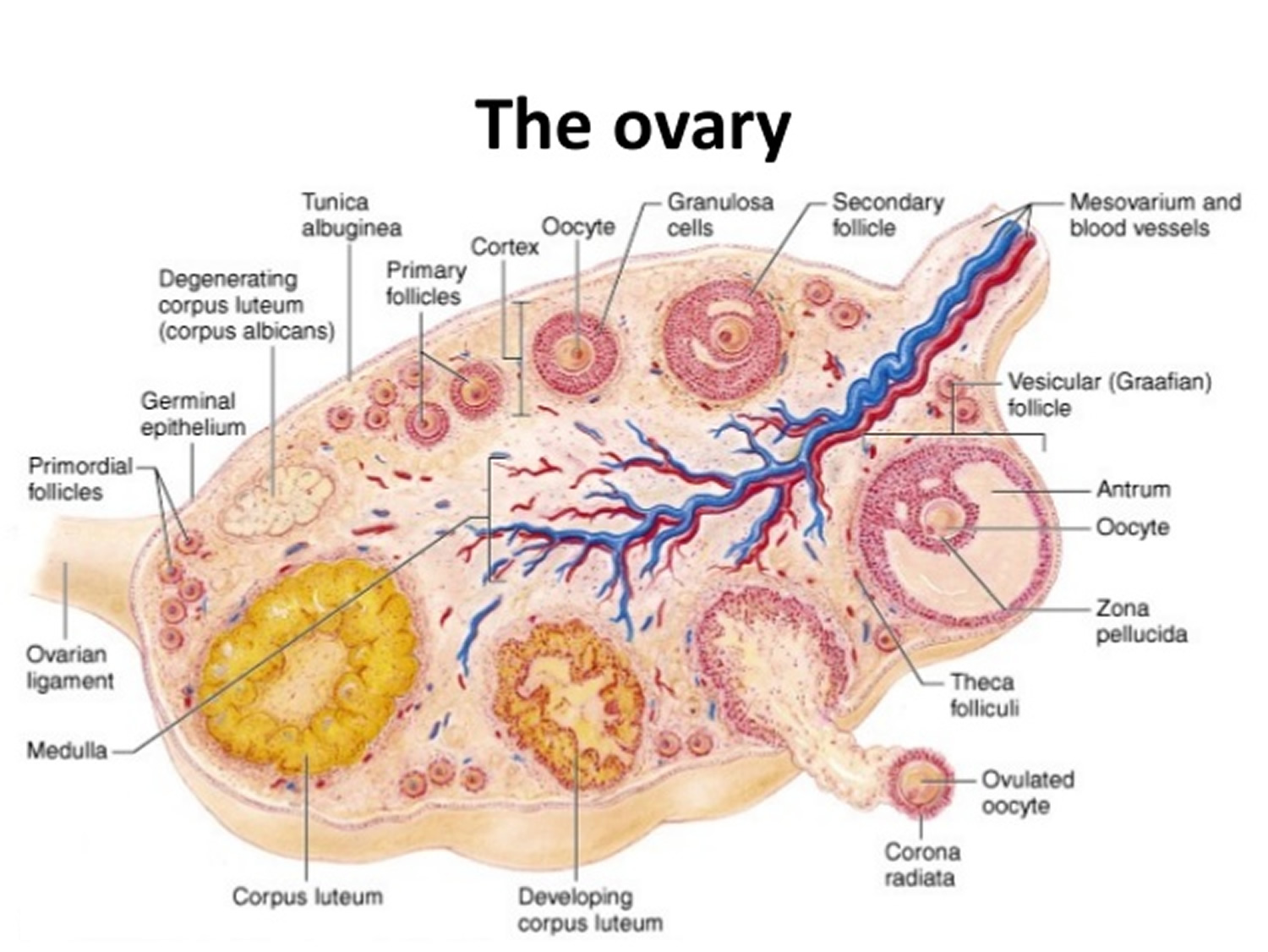
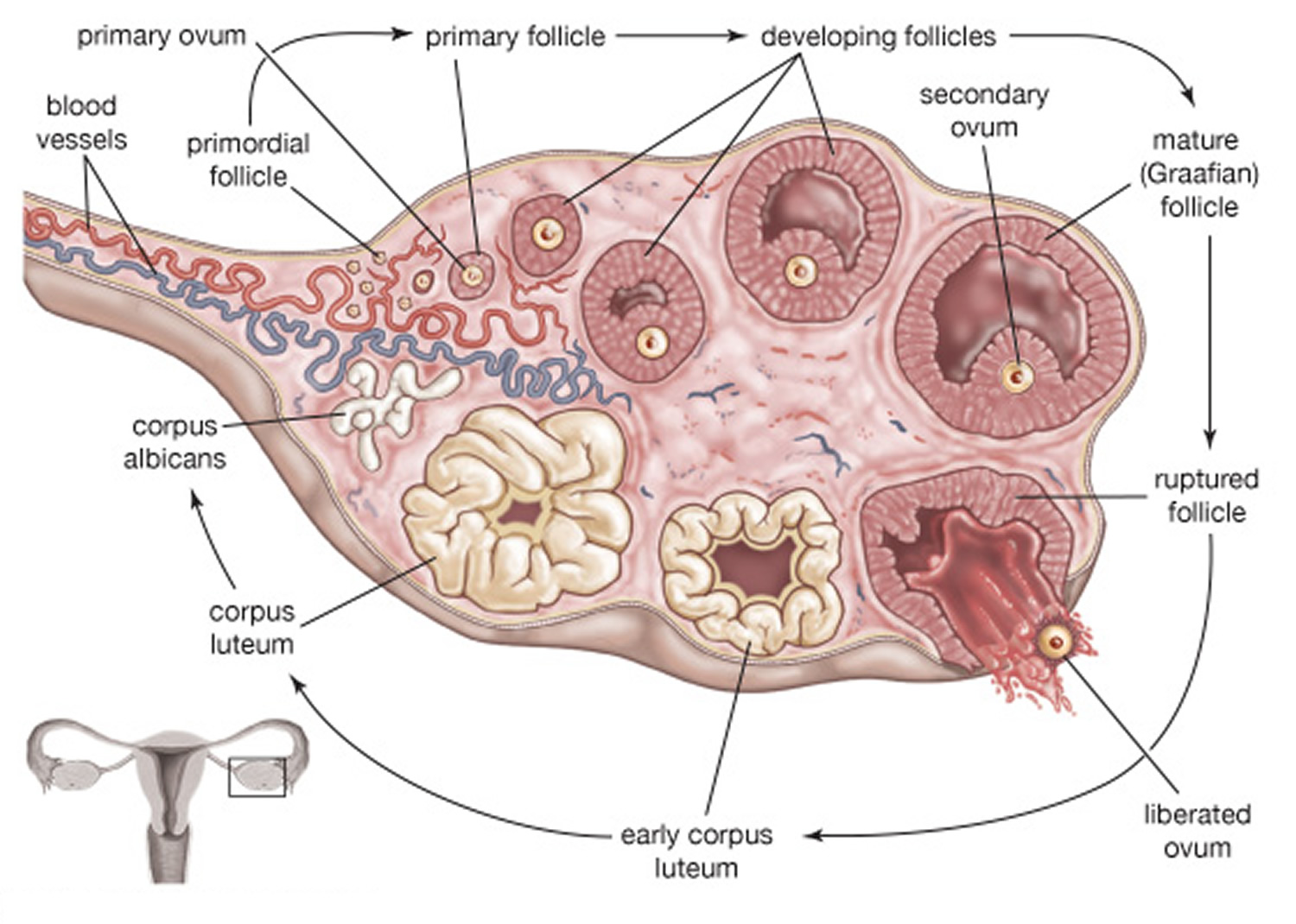
Ovarian tissues are divided into two indistinct regions—an inner medulla and an outer cortex. The ovarian medulla is mostly composed of loose connective tissue and contains many blood vessels, lymphatic vessels, and nerve fibers. The ovarian cortex consists of more compact tissue and has a granular appearance due to tiny masses of cells called ovarian follicles (see Figure 3). A layer of cuboidal epithelium covers the ovary’s free surface. Just beneath this epithelium is a layer of dense connective tissue.
Primordial Follicles
During prenatal development of a female, small groups of cells in the outer region of the ovarian cortex form several million primordial follicles. Each follicle consists of a single, large cell, called a primary oocyte, surrounded by epithelial cells called follicular cells.
Early in development, the primary oocytes begin to undergo meiosis, but the process soon halts and does not continue until the individual reaches puberty. Once the primordial follicles appear, no new ones form. Instead, the number of primary oocytes in the ovary steadily declines as many of the primary oocytes degenerate. Of the six to seven million primary oocytes that formed in the embryonic ovary, only a million or so remain at birth, and perhaps 300,000 are present at puberty. Of these, probably fewer than 300 to 400 oocytes will be released from the ovary during a female’s reproductive life.
Figure 3. Ovary anatomy
Oogenesis
Oogenesis is the process of oocyte formation. Beginning at puberty, some primary oocytes are stimulated to continue meiosis. Like sperm cells, the resulting cells have one-half as many chromosomes (23 chromosomes) in their nuclei as their parent cells.
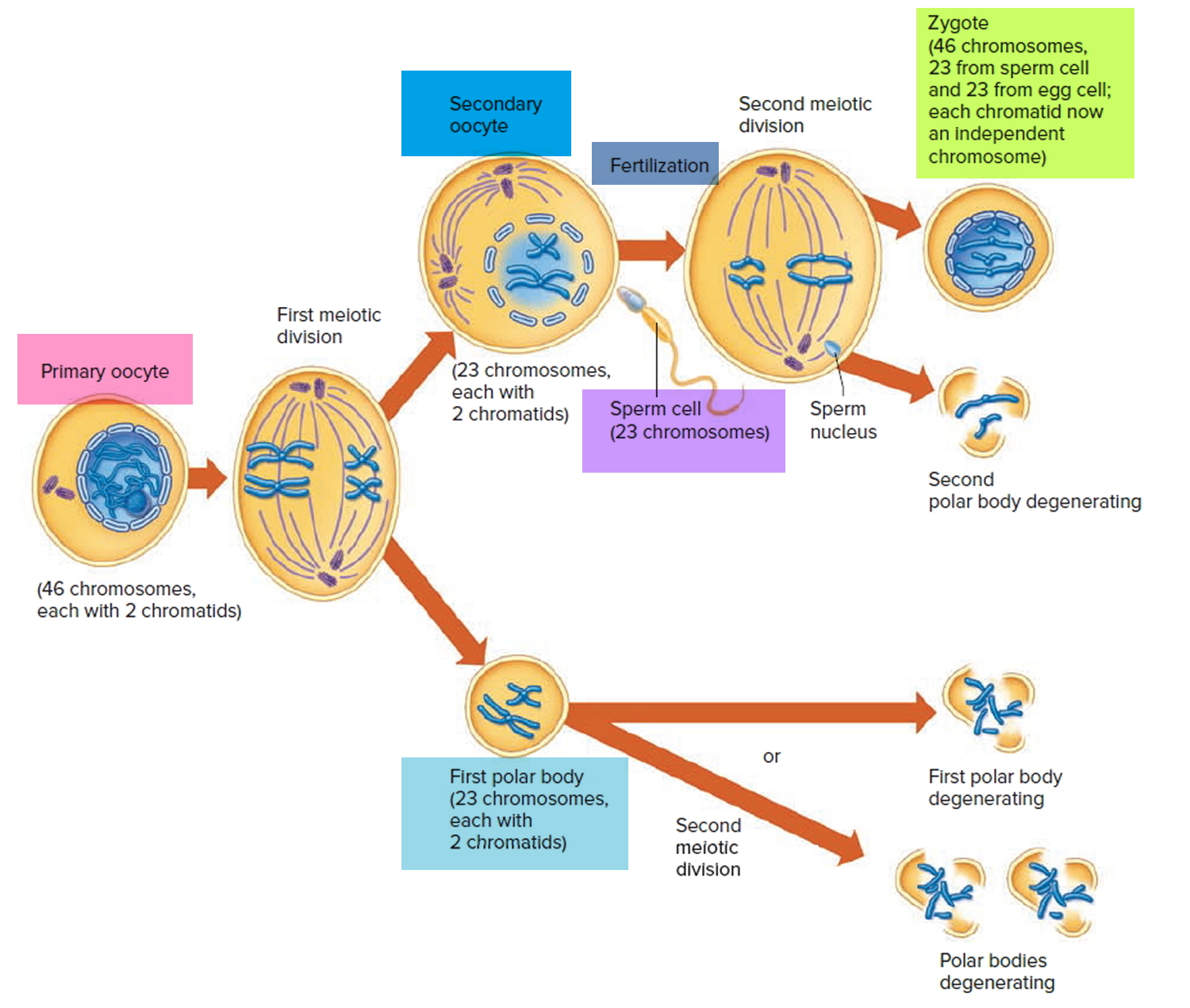
Unlike a primary spermatocyte, when a primary oocyte divides, the cytoplasm is distributed unequally. One of the resulting cells, called a secondary oocyte, is large, and the other, called the first polar body, is small. If fertilization occurs, the secondary oocyte undergoes the second meiotic division and divides unequally to produce a tiny second polar body and a large ovum. At the end of meiosis the chromosomes from the sperm combine with those of the ovum, and the ovum becomes a zygote.
The polar bodies have no further function and soon degenerate. Their role in reproduction allows for production of an oocyte that has not only just the haploid number of chromosomes but also the massive amounts of cytoplasm and the abundant organelles required to carry the zygote through the first few cell divisions.
Figure 4. Oogenesis
Note: During oogenesis, a secondary oocyte results from meiosis of a primary oocyte. If fertilized, the egg cell undergoes a second meiotic division. This division generates a second polar body and a zygote. The second meiotic division may not occur in the secondary oocyte if it is not fertilized.
Follicle Maturation
At puberty, the anterior pituitary gland secretes increased amounts of follicle-stimulating hormone (FSH), and the ovaries enlarge in response. Throughout a woman’s reproductive years, primordial follicles mature into primary follicles (Figure 4. Ovarian Follicle Maturation). Figure 4. Ovarian Follicle Maturation traces the maturation of a follicle in an ovary.
During early follicle maturation, the primary oocyte within the follicle enlarges, and surrounding follicular cells proliferate by mitosis. These follicular cells organize into layers, and eventually a cavity (antrum) appears in the cellular mass. The structure is now called an antral follicle. A clear follicular fluid fills the antrum (see Figure 3. Ovary anatomy).
In time, the antral follicle reaches a diameter of 10 millimeters or more and bulges outward on the ovary surface. The primary oocyte within the mature antral follicle is a large, spherical cell, surrounded by a layer of glycoprotein called the zona pellucida, with layers of follicular cells called the corona radiata (see Figure 3. Ovary anatomy). Processes from these follicular cells extend through the zona pellucida and supply nutrients to the primary oocyte.
Although as many as twenty primary follicles may begin maturing at any one time, one follicle usually outgrows the others. Typically, only the dominant follicle fully develops, and the other follicles degenerate. This entire process, from a primordial follicle to a dominant, fully developed antral follicle, takes almost 300 days. The process is ongoing in the ovaries, such that a new dominant antral follicle becomes ready for ovulation approximately every 28 days.
Figure 5. Ovarian Follicle Maturation
Ovulation
Just prior to ovulation, the primary oocyte in the mature antral follicle completes meiosis I, giving rise to a secondary oocyte (see Figure 4. Oogenesis) and a first polar body. A process called ovulation releases these cells from the mature antral follicle.
Release of luteinizing hormone (LH) from the anterior pituitary gland plays a role in triggering ovulation, during which the mature antral follicle swells and its wall weakens. Eventually the wall ruptures, and follicular fluid, accompanied by the secondary oocyte, is released from the ovary’s surface (see Figure 4. Oogenesis).
After ovulation, the secondary oocyte and one or two layers of follicular cells surrounding it are normally propelled to the opening of a nearby uterine tube (Figure 6. Ovulation). Compared to the overall size of the ovary, the mature antral follicle is so large that no matter where the secondary oocyte is released from the ovary, it will contact the branched extensions (fimbriae) of the associated uterine tube. If the secondary oocyte is not fertilized within hours, it degenerates.
Figure 6. Ovulation
Female Sex Hormones
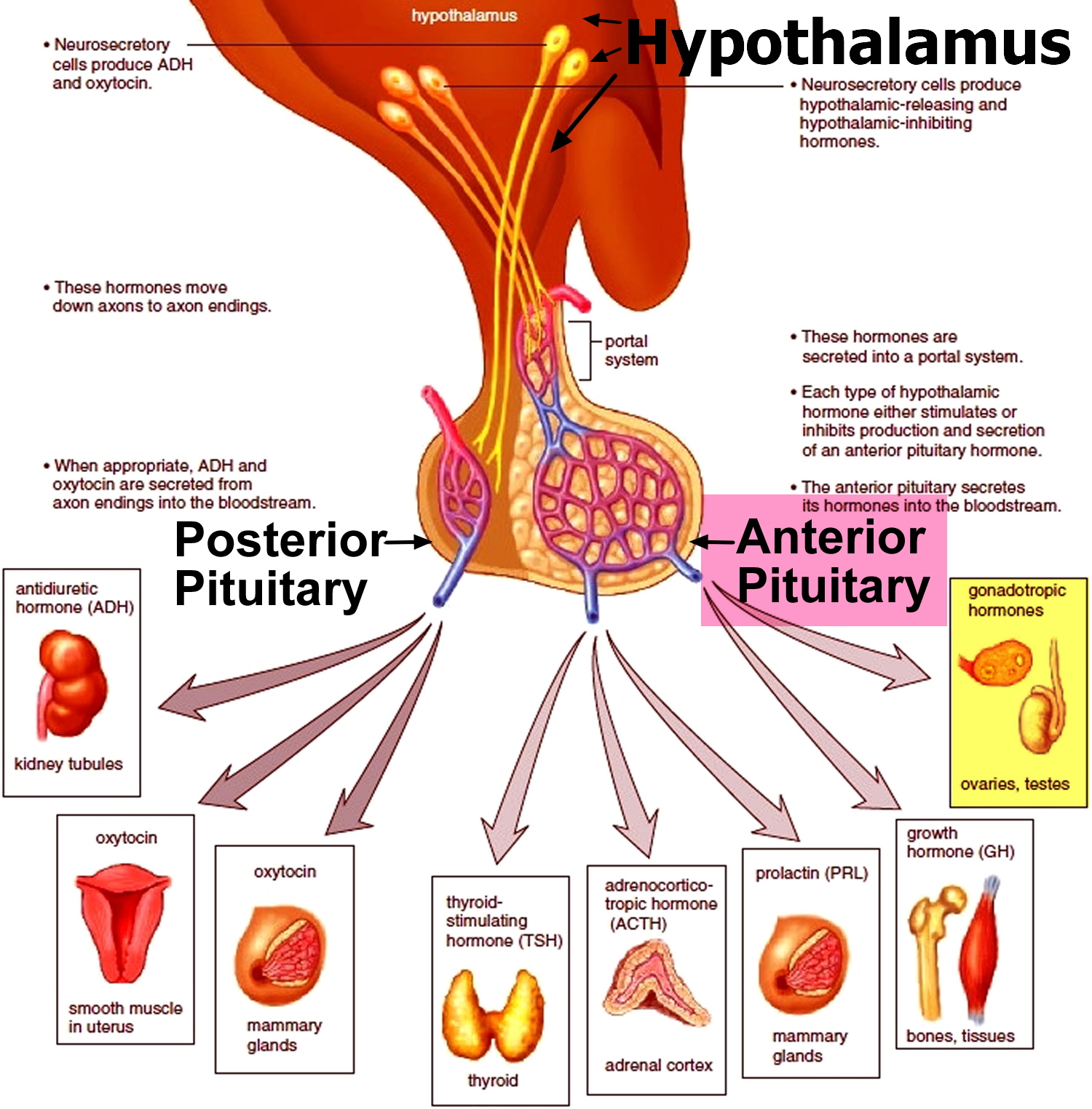
The female body is reproductively immature until about ten years of age. Then, the hypothalamus begins to secrete increasing amounts of Gonadotropin-releasing hormone (GnRH), which, in turn, stimulates the anterior pituitary to release the gonadotropins follicle-stimulating hormone (FSH) and luteinizing hormone (LH). These hormones play primary roles in controlling female sex cell maturation and in producing female sex hormones (Figure 7. Pituirary gland hormones).
The ovaries produce and release two groups of sex hormones—progesterone and estrogen 2. There are actually three major estrogens, known as estradiol, estrone, and estriol. Estradiol is the most abundant of the estrogens. These substances work together to promote the healthy development of female sex characteristics during puberty and to ensure fertility.
Several other tissues, including the adrenal cortices, and the placenta (during pregnancy), secrete female sex hormones —estrogens and progesterone, also.
However, the ovaries are the primary source of estrogens (in a nonpregnant female). At puberty, under the influence of the anterior pituitary, the ovaries secrete increasing amounts of estrogens. Estrogens stimulate enlargement of reproductive organs, including the vagina, uterus, uterine tubes, ovaries, and external reproductive structures.
Estrogen (estradiol, specifically) is instrumental in breast development, fat distribution in the hips, legs, and breasts, and the development of reproductive organs 2.
To a lesser extent, the ovaries release the hormone relaxin prior to giving birth. Another minor hormone is inhibin, which is important for signaling to the pituitary to inhibit follicle-stimulating hormone (FSH) secretion.
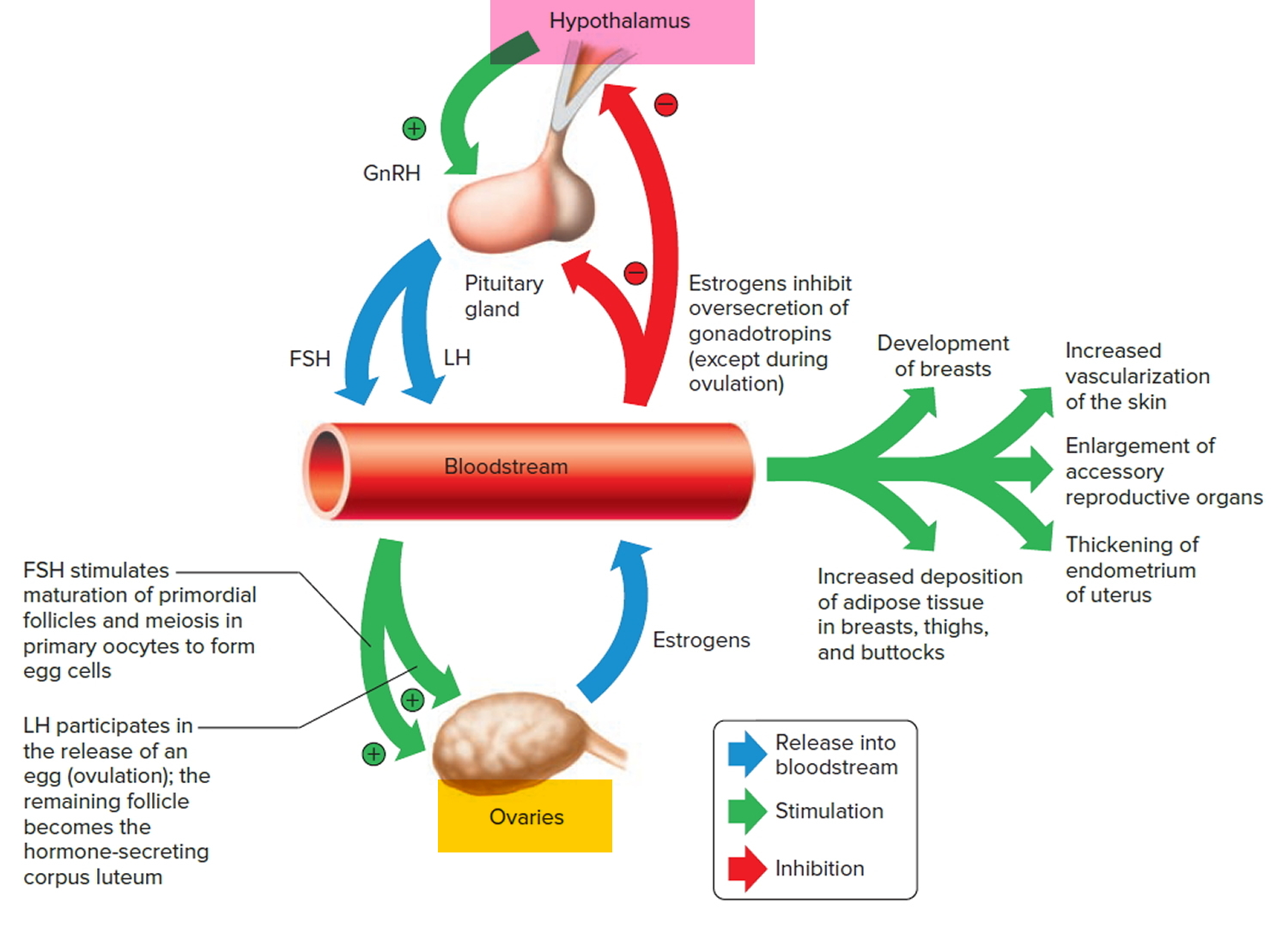
Figure 7. The Hypothalamus controlling the anterior lobe of the pituitary and the ovaries
Note: Note: The hypothalamus controls the production of an egg cell, ovulation of the egg cell, and development of the female secondary sex characteristics. Negative feedback among the hypothalamus, the anterior lobe of the pituitary, and the ovaries helps control the concentration of estrogens in the female body.
Estrogens also develop and maintain the female secondary sex characteristics, which include (Figure 8. Pituirary gland hormones):
- Development of the breasts and the ductile system of the mammary glands in the breasts.
- Increased deposition of adipose tissue in thesubcutaneous layer generally and in the breasts, thighs and buttocks particularly.
- Increased vascularization of the skin.
The ovaries are also the primary source of progesterone (in a nonpregnant female). This hormone promotes changes in the uterus during the female menstrual cycle, affects the mammary glands, and helps regulate the secretion of gonadotropins from the anterior pituitary gland.
[Androgens (male sex hormone) secreted by the adrenal gland cortices produce certain other changes in females at puberty. For example, increased hair growth in the pubic and axillary regions. Conversely, development of the female skeletal configuration, which includes narrow shoulders and broad hips, is a response to a low androgen concentration.]Figure 8. Pituitary gland hormones under the influence of the hypothalamus controlling the ovaries production of egg cell, ovulation and development of the female secondary sex characteristics
Menstrual Cycle
The menstrual cycle is characterized by regular, recurring changes in the endometrium, which culminate in menstrual bleeding (menses). Such cycles usually begin around age thirteen and continue into the early fifties, then cease.
A female’s first menstrual cycle, called menarche, occurs after the ovaries and other organs of the reproductive control system mature and begin responding
to certain hormones. Then, the hypothalamic secretion of gonadotropin-releasing hormone (GnRH) stimulates the anterior pituitary to release threshold levels of follicle-stimulating hormone (FSH) and luteinizing hormone (LH). Follicle-stimulating hormone (FSH) stimulates the final maturation of an ovarian follicle. The follicular cells produce increasing amounts of estrogens and some progesterone. Luteinizing hormone (LH) stimulates certain ovarian cells to secrete precursor molecules (such as testosterone), also used to produce estrogens.
In a young female, estrogens stimulate the development of secondary sex characteristics. Estrogens secreted during subsequent menstrual cycles continue the development and maintenance of these characteristics.
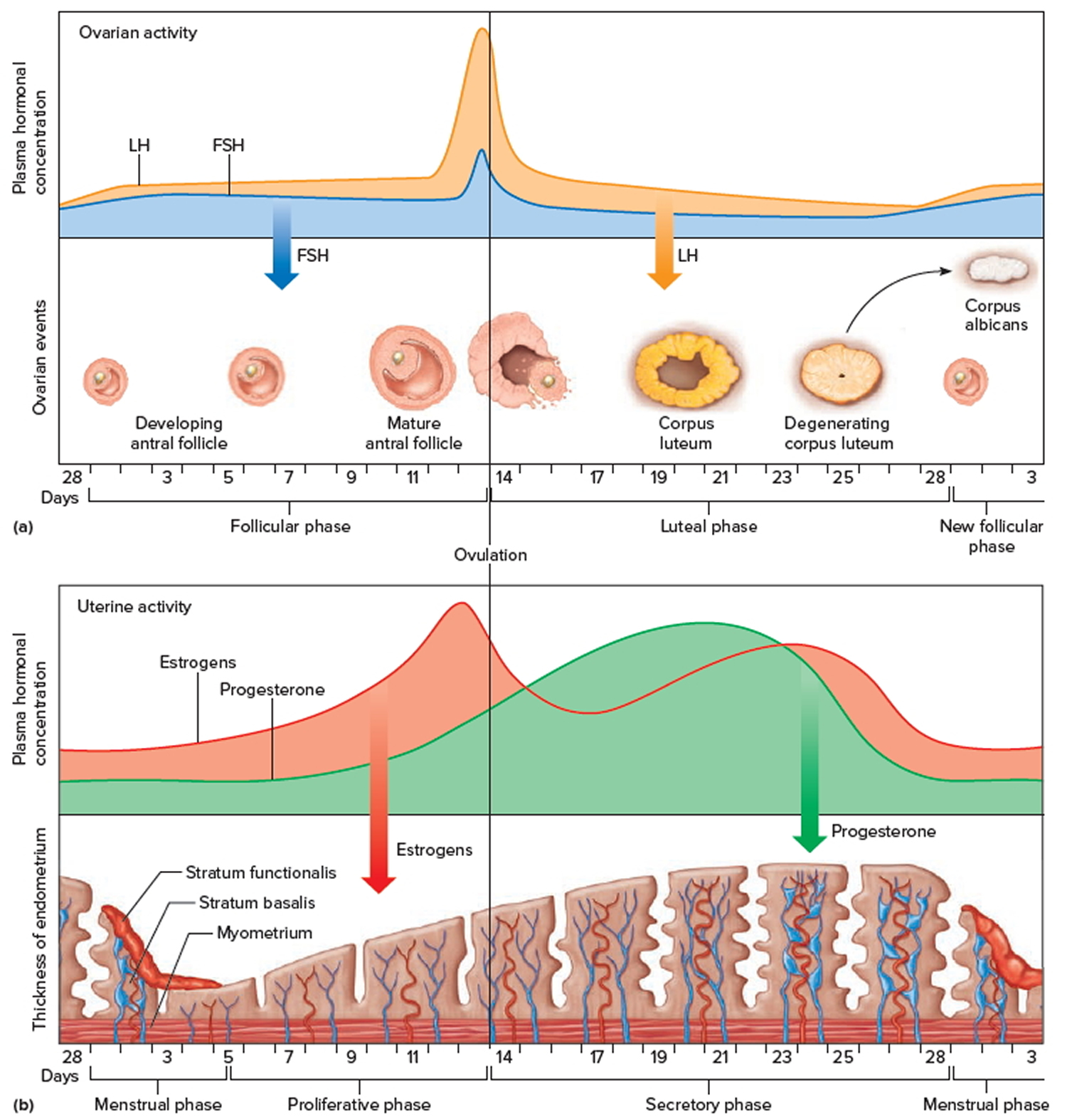
Figure 9. Ovarian activity during the Menstrual cycle
Note: Major events in the female menstrual cycle. (a) Plasma hormonal concentrations of follicle-stimulating hormone (FSH) and luteinizing hormone (LH) affect follicle maturation in the ovaries. (b) Plasma hormonal concentrations of estrogen and progesterone influence changes in the uterine lining.
Increasing concentration of estrogens during the first week or so of a menstrual cycle changes the uterine lining, thickening the glandular endometrium (proliferative phase). Meanwhile, the follicle fully matures, and by around the fourteenth day of the cycle, the antral follicle appears on the ovary surface as a blisterlike bulge. Within the follicle, the follicular cells, which surround and connect the secondary oocyte to the inner wall, loosen. Follicular fluid accumulates.
While the follicle matures, it secretes estrogens that inhibit the release of luteinizing hormone (LH) from the anterior pituitary gland but allow luteinizing hormone (LH) to be stored in the gland. Estrogens also make anterior pituitary cells more sensitive to the action of gonadotropin-releasing hormone (GnRH), which is released from the hypothalamus in rhythmic pulses about ninety minutes apart.
Near the fourteenth day of follicular development, the anterior pituitary cells finally respond to the pulses of GnRH and release the stored LH. The resulting surge in LH concentration lasts about thirty-six hours. In response to the LH, the primary oocyte completes meiosis I. The LH also acts with FSH inducing complex interactions with prostaglandins, progesterone, plasmin, and proteolytic enzymes, leading to the weakening and rupturing of the bulging follicular wall. This event sends the secondary oocyte and follicular fluid out of the ovary (ovulation).
Following ovulation, the space containing the follicular fluid fills with blood, which soon clots. Under the influence of LH, the remnants of the follicle within the ovary form a temporary glandular structure in the ovary called a corpus luteum (“yellow body”).
Follicular cells secrete some progesterone during the first part of the menstrual cycle. During the second half of the cycle, cells of the corpus luteum secrete abundant progesterone and estrogens. Consequently, as a corpus luteum forms, the blood progesterone concentration sharply increases.
Progesterone causes the endometrium to become more vascular and glandular. It also stimulates the uterine glands to secrete more glycogen and lipids (secretory phase). The endometrial tissues fill with fluids containing nutrients and electrolytes, which provide a favorable environment for an embryo to develop.
High levels of estrogens and progesterone inhibit the anterior pituitary gland’s release of LH and FSH. Consequently, no other follicles are stimulated to complete development when the corpus luteum is active. However, if the secondary oocyte released at ovulation is not fertilized, the corpus luteum begins to degenerate (regress) on about the twenty-fourth day of the cycle. Eventually, connective tissue replaces it. The remnant of such a corpus luteum is called a corpus albicans, and is eventually absorbed.
When the corpus luteum ceases to function, concentrations of estrogens and progesterone rapidly decline, and in response, blood vessels in the endometrium constrict. This reduces the supply of oxygen and nutrients to the thickened endometrium (stratum functionalis and stratum basalis), and these lining tissues soon disintegrate and slough off. At the same time, blood leaves damaged capillaries, creating a flow of blood and cellular debris that passes through the vagina as the menstrual flow (menses). This flow usually begins about the twenty-eighth day of the cycle and continues for three to five days, while the concentrations of estrogens are relatively low. The beginning of the menstrual flow marks the end of a menstrual cycle and the beginning of the next cycle as a new developing antral follicle becomes available.
Low blood concentrations of estrogens and progesterone at the beginning of the menstrual cycle mean that the hypothalamus and anterior pituitary gland are no longer inhibited. Consequently, FSH and LH concentrations soon increase, stimulating a new antral follicle to mature. As this follicle secretes estrogens, the uterine lining undergoes repair, and the endometrium begins to thicken again.
Menopause
After puberty, menstrual cycles continue at regular intervals into the late forties or early fifties, when the ovaries start to produce less estrogen and progesterone. This results in the menstrual cycles becoming less predictable. Then, within a few months or years, the cycles cease. This period in life is called menopause or female climacteric.