Contents
What is a zoonotic disease
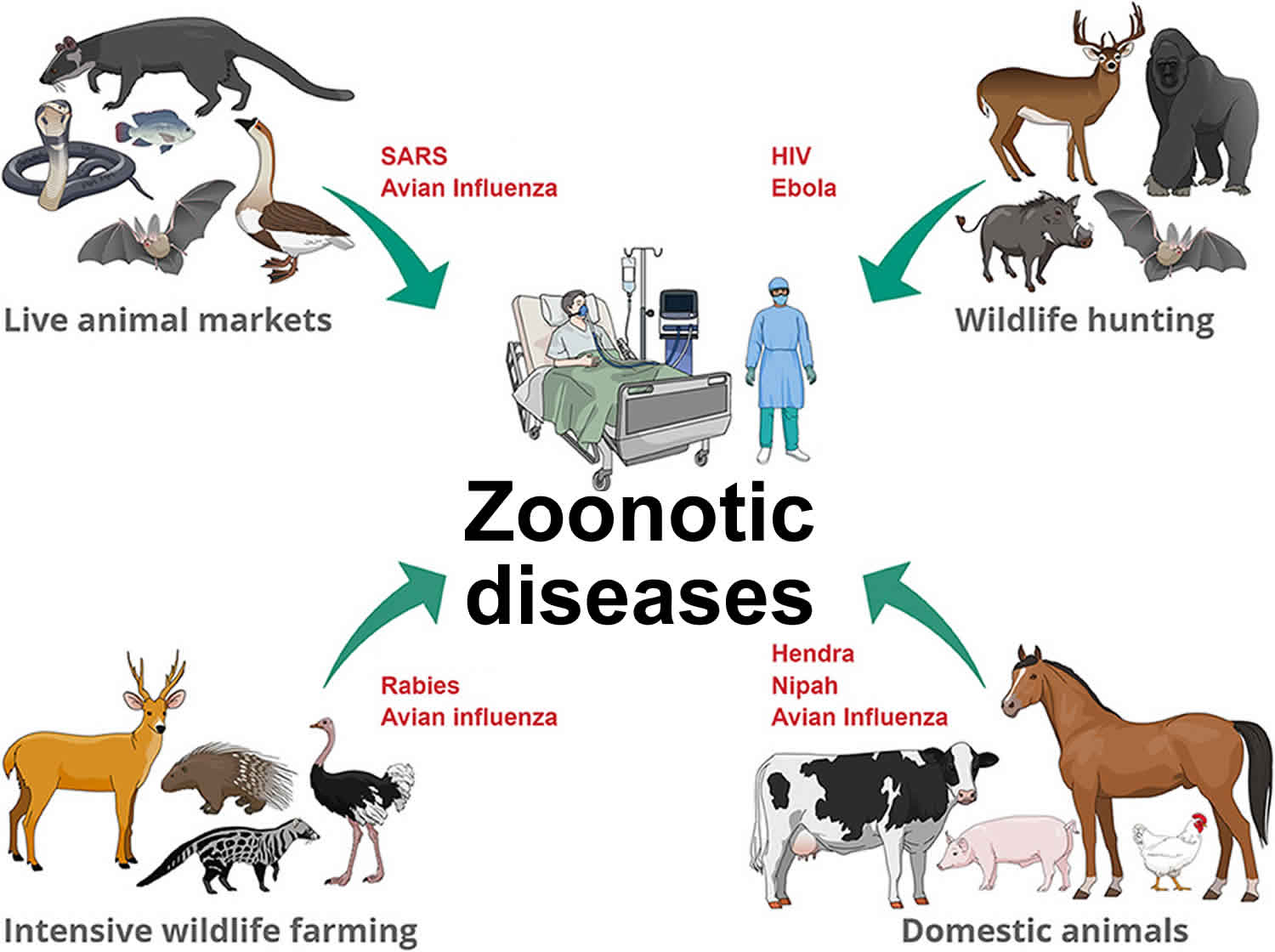
Zoonotic diseases also known as zoonoses, are caused by infections that spread between animals and people. Zoonotic means infectious diseases that are spread between animals and people. Every year, tens of thousands of Americans will get sick from zoonotic diseases spread between animals and people.
Animals provide many benefits to people. Many people interact with animals in their daily lives, both at home and away from home. Pets offer companionship and entertainment, with millions of households having one or more pets. You might come into close contact with animals at a county fair or petting zoo, or encounter wildlife while enjoying outdoor activities. Also, animals are an important food source and provide meat, dairy, and eggs.
However, some animals can carry harmful germs that can be shared with people and cause illness – these are known as zoonotic diseases or zoonoses. Zoonotic diseases are caused by harmful germs like viruses, bacterial, parasites, and fungi. These germs can cause many different types of illnesses in people and animals ranging from mild to serious illness and even death. Some animals can appear healthy even when they are carrying germs that can make people sick.
Zoonotic diseases are very common, both in the United States and around the world. Scientists estimate that more than 6 out of every 10 known infectious diseases in people are spread from animals, and 3 out of every 4 new or emerging infectious diseases in people are spread from animals. Every year, tens of thousands of Americans will get sick from harmful germs spread between animals and people.
How do zoonotic infections spread between animals and people?
Because of the close connection between people and animals, it’s important to be aware of the common ways people can get infected with germs that can cause zoonotic diseases. These can include:
- Direct contact: Coming into contact with the saliva, blood, urine, mucous, feces, or other body fluids of an infected animal. Examples include petting or touching animals, and bites or scratches.
- Indirect contact: Coming into contact with areas where animals live and roam, or objects or surfaces that have been contaminated with germs. Examples include aquarium tank water, pet habitats, chicken coops, plants, and soil, as well as pet food and water dishes.
- Vector-borne: Being bitten by a tick, or an insect like a mosquito or a flea.
- Foodborne: Each year, 1 in 6 Americans get sick from eating contaminated food. Eating or drinking something unsafe (such as unpasteurized milk, undercooked meat or eggs, or raw fruits and vegetables that are contaminated with feces from an infected animal).
Who is at a higher risk of serious illness from zoonotic diseases?
Anyone can become sick from a zoonotic disease, including healthy people. However, some people may be more at risk than others and should take steps to protect themselves or family members. These people are more likely than others to get really sick, and even die, from infection with certain diseases. These groups of people include:
- Children younger than 5
- Adults older than 65
- People with weakened immune systems
Zoonotic diseases prevention
People can come into contact with animals in many places. This includes at home and away from home, in places like petting zoos, fairs, schools, stores, and parks. Insects, like mosquitoes and fleas, and ticks bite people and animals day and night. Thankfully, there are things you can do to protect yourself and your family from zoonotic diseases.
- Keep hands clean. Washing your hands right after being around animals, even if you didn’t touch any animals, is one of the most important steps you can take to avoid getting sick and spreading germs to others.
- Always wash your hands after being around animals, even if you didn’t touch the animals.
- Many germs are spread by not washing hands with soap and clean, running water.
- If clean, running water is not accessible, use soap and available water.
- If soap and water are unavailable, use an alcohol-based hand sanitizer that contains at least 60% alcohol to clean hands. Because hand sanitizers do not eliminate all types of germs, it is important to wash your hands as soon as soap and water are available.
- Know the simple things you can do to stay safe around your pets.
- Prevent bites from mosquitoes, ticks, and fleas.
- Learn more about ways to handle food safely—whether it’s for yourself or your family, your pet, or other animals.
- Be aware of zoonotic diseases both at home, away from home (such as at petting zoos or other animal exhibits), in child care settings or schools and when you travel.
- Avoid bites and scratches from animals.
Common zoonotic diseases in human
Cat-scratch disease
Cat-scratch disease is an infection with bartonella bacteria that is believed to be transmitted by cat scratches, cat bites, or flea bites.
Cat-scratch disease causes
Cat-scratch disease is caused by the bacteria Bartonella henselae. The disease is spread through contact with an infected cat (a bite or scratch) or exposure to cat fleas. It also can be spread through contact with cat saliva on broken skin or mucosal surfaces like those in the nose, mouth, and eyes.
Cat-scratch disease prevention
To prevent cat-scratch disease:
- Wash your hands thoroughly with soap and water after playing with your cat. Especially wash any bites or scratches.
- Play gently with cats so they don’t scratch and bite.
- Don’t allow a cat to lick your skin, eyes, mouth, or open wounds or scratches.
- Use flea control measures to lower the risk your cat develops the disease.
- Don’t touch feral cats.
Cat-scratch disease symptoms
A person who has had contact with an infected cat may show common symptoms, including:
- Bump (papule) or blister (pustule) at site of injury (usually the first sign)
- Fatigue
- Fever (in some people)
- Headache
- Lymph node swelling (lymphadenopathy) near the site of the scratch or bite
- Overall discomfort (malaise)
Less common symptoms may include:
- Loss of appetite
- Sore throat
- Weight loss
Cat-scratch disease possible complications
People whose immune systems are weakened may develop complications such as:
- Encephalopathy (loss of brain function)
- Neuroretinitis (inflammation of the retina and optic nerve of the eye)
- Osteomyelitis (bone infection)
- Parinaud syndrome (red, irritated, and painful eye)
Cat-scratch disease diagnosis
If you have swollen lymph nodes and a scratch or bite from a cat, your health care provider may suspect cat-scratch disease.
A physical examination may also reveal an enlarged spleen.
Sometimes, an infected lymph node may form a tunnel (fistula) through the skin and drain (leak fluid).
This disease is often not found because it is hard to diagnose. The Bartonella henselae immunofluorescence assay (IFA) blood test is an accurate way to detect the infection caused by these bacteria. The results of this test must be considered along with other information from your medical history, lab tests, or biopsy.
A lymph node biopsy may also be done to look for other causes of swollen glands.
Cat-scratch disease treatment
Generally, cat-scratch disease is not serious. Medical treatment may not be needed. In some cases, treatment with antibiotics such as azithromycin can be helpful. Other antibiotics may be used, including clarithromycin, rifampin, trimethoprim-sulfamethoxazole, or ciprofloxacin.
In people with HIV/AIDS and others, who have a weakened immune system, cat-scratch disease is more serious. Treatment with antibiotics is recommended.
Cat-scratch disease prognosis
People who have a healthy immune system should recover fully without treatment. In people with a weakened immune system, treatment with antibiotics usually leads to recovery.
Brucellosis
Brucellosis is an infectious disease that occurs from contact with animals carrying brucella bacteria.
Brucellosis causes
Brucella can infect cattle, goats, camels, dogs, and pigs. The bacteria can spread to humans if you come in contact with infected meat or the placenta of infected animals, or if you eat or drink unpasteurized milk or cheese.
Brucellosis is rare in the United States. About 100 to 200 cases occur each year. Most cases are caused by the Brucellosis melitensis bacteria.
People working in jobs where they often come in contact with animals or meat — such as slaughterhouse workers, farmers, and veterinarians — are at higher risk.
Brucellosis prevention
Drinking and eating only pasteurized dairy products, such as milk and cheeses, is the most important way to reduce the risk for brucellosis. People who handle meat should wear protective eyewear and clothing, and protect skin breaks from infection.
Detecting infected animals controls the infection at its source. Vaccination is available for cattle, but not humans.
Brucellosis symptoms
Acute brucellosis may begin with mild flu-like symptoms, or symptoms such as:
- Abdominal pain
- Back pain
- Chills
- Excessive sweating
- Fatigue
- Fever
- Headache
- Joint and muscle pain
- Loss of appetite
- Swollen glands
- Weakness
- Weight loss
High fever spikes often occur every afternoon. The name undulant fever is often used to describe this disease because the fever rises and falls in waves.
The illness may be chronic and last for years.
Brucellosis possible complications
Health problems that may result from brucellosis include:
- Bone and joint sores (lesions)
- Encephalitis (swelling, or inflammation, of the brain)
- Infective endocarditis (inflammation of the inside lining of the heart chambers and heart valves)
- Meningitis (infection of the membranes covering the brain and spinal cord)
Brucellosis diagnosis
Your doctor will examine you and ask about your symptoms. You’ll also be asked if you’ve been in contact with animals or possibly eaten dairy products that were not pasteurized.
Tests that may be done include:
- Blood test for brucellosis
- Blood culture
- Bone marrow culture
- Urine culture
- CSF (spinal fluid) culture
- Biopsy and culture of specimen from affected organ
Brucellosis treatment
Antibiotics, such as doxycycline, streptomycin, gentamicin, and rifampin, are used to treat the infection and prevent it from coming back. Often, you need to take the drugs for 6 weeks. If there are complications from brucellosis, you will likely need to take the drugs for a longer period.
Brucellosis prognosis
Symptoms may come and go for years. Also, the illness can come back after a long period of not having symptoms.
Tick Paralysis
Tick paralysis is a loss of muscle function that results from a tick bite.
Tick paralysis causes
Hard-bodied and soft-bodied female ticks are believed to make a poison that can cause paralysis in children. Ticks attach to the skin to feed on blood. The poison enters the bloodstream during this feeding process.
The paralysis is ascending. That means it starts in the lower body and moves up.
Tick paralysis prevention
Use insect repellents and protective clothing when in tick-infested areas. Tuck pant legs into socks. Carefully check the skin and hair after being outside and remove any ticks you find.
If you find a tick on your child, write the information down and keep it for several months. Many tick-borne diseases do not show symptoms right away, and you may forget the incident by the time your child becomes sick with a tick-borne disease.
Tick paralysis symptoms
Children with tick paralysis develop an unsteady gait followed several days later by weakness in the lower legs. This weakness gradually moves up to involve the upper limbs.
Paralysis may cause breathing difficulties, which may require the use of a breathing machine.
The child may also have mild, flu-like symptoms (muscle aches, tiredness).
Tick paralysis possible complications
Breathing difficulties can cause respiratory failure. When this happens, the body’s organs do not have enough oxygen to work well.
Tick paralysis diagnosis
People can be exposed to ticks in many ways. For example, they may have gone on a camping trip, live in a tick-infested area, or have dogs or other animals that can pick up ticks. Often, the tick is found only after thoroughly searching a person’s hair.
Finding a tick embedded in the skin and having the above symptoms confirms the diagnosis. No other testing is required.
Tick paralysis treatment
Removing the tick removes the source of the poison. Recovery is rapid after the tick is removed.
Tick paralysis prognosis
Full recovery is expected following the removal of the tick.
Lyme disease
Lyme disease is a bacterial infection that is spread by ticks. It was first recognized in 1975. Large numbers of children around the town of Lyme, Connecticut, were being diagnosed with juvenile rheumatoid arthritis. Researchers investigated and found that tick bites were causing the illnesses.
Lyme disease is carried by black-legged ticks (sometimes called deer ticks). These ticks are typically about the size of a sesame seed. They live only in certain areas of the country:
- Northeast and mid-Atlantic (northeast Virginia to Maine)
- North central states (mostly Wisconsin and Minnesota)
- West Coast (mostly northern California)
Lyme disease can be found in other parts of the United States. But it is rare to get it outside of where the black-legged tick lives. The disease is also found in Europe, Asia, and Australia.
Lyme disease causes
People get Lyme disease when they are bitten by an infected tick. Ticks live in areas with a lot of plant life, such as wooded areas or fields. They sit near the top of grassy plants and low bushes. They wait there for people or animals to brush up against them. Ticks can crawl on your clothes or body for up to several hours or more before attaching to the skin.
Ticks can attach to any part of your body. They are usually found in hard-to-see areas, including the armpits, groin, or scalp. An infected tick needs to be attached to your skin for 36 to 48 hours before it passes the bacteria on to you.
People who spend time in outdoor areas where ticks are common are at higher risk of getting tick-borne diseases.
Lyme disease prevention
The best way to prevent Lyme disease is to avoid being bitten by ticks. When you are outdoors, follow these guidelines:
- Avoid areas that are wooded, brushy, or have tall grass.
- Walk in the center of trails.
- Use an insect repellent with at least 20% DEET. It can be put on clothing or sparingly on the skin. Don’t apply it to the face or hands of children.
- Treat clothing, tents, or other gear with repellents containing 0.5% permethrin.
- Wear light-colored clothing. This makes it easier to see and remove ticks from your clothes.
- Wear a long-sleeved shirt and long pants. Tuck your pant legs into your socks or boots for added protection.
After you get home, check everything and everyone for ticks.
- Bathe or shower as soon as you can to wash off any ticks that have not attached to you.
- Check your entire body for ticks. Use a mirror for places you can’t see. Check your children and your pets. Common tick locations include the back of the knees, groin area, underarms, ears, scalp, and the back of the neck.
- Check any gear you used, including coats, backpacks, or tents.
- Tumble dry clothes or blankets on high heat in the dryer for 10 to 15 minutes. This should kill any ticks. If clothes are dirty, wash them in hot water and dry on high heat for 60 minutes.
What to do if you find a tick on your skin?
Don’t panic. Use fine-tipped tweezers to grasp the tick as close to the skin’s surface as possible. Pull up with steady, even pressure. Be careful not to squeeze or twist the tick body. Sometimes parts of the tick remain in the skin. You can leave them alone or carefully remove them the same way you would a splinter. Do not use heat (such as a lit match), petroleum jelly, or other methods to try to make the tick “back out” on its own. These methods are not effective.
Wash the area where the tick was attached thoroughly with soap and water. Keep an eye on the area for a few weeks and note any changes. Call your doctor if you develop a rash around the area where the tick was attached. Be sure to tell your doctor that you were bitten by a tick and when it happened.
Lyme disease symptoms
The symptoms of Lyme disease can depend on what stage the disease is in.
Early symptoms (3 to 30 days after tick bite)
- fever
- chills
- headache
- fatigue
- joint and muscle aches
- rash.
The rash is a telltale sign of Lyme disease. It usually starts at the site of the tick bite. It expands gradually over a few days. It can reach up to 12 inches across or more. The center may fade, creating a “bull’s eye” or target appearance. The rash may feel warm to the touch.
Some people with Lyme disease do not get the bull’s-eye rash. They may have many red spots instead. Others don’t get a rash at all. Around 75% of people with Lyme disease get a rash.
Later symptoms (days to months after tick bite)
If Lyme disease isn’t treated, it can spread to other parts of the body. Late-stage symptoms include:
- headaches
- neck stiffness
- arthritis (painful, swollen joints)
- additional rashes
- facial palsy (face muscles droop)
- irregular or slow heartbeat
- numbness in arms or legs
- inflammation of the brain and spinal cord
- changes in mood or sleep habits
- short-term memory problems.
It is normal to have a small bump or red spot where a tick bit you. This does not mean you have Lyme disease. It usually goes away in a day or two.
Lyme disease diagnosis
It can be difficult to diagnose Lyme disease. The ticks that carry it are very small and the bites don’t hurt. Many patients don’t remember being bitten. In addition, most of the symptoms are common with other illnesses.
If you find a tick in your skin, use tweezers to remove it immediately. Then wait a few days to see if you develop any symptoms. If you do, call your family doctor. Your doctor will ask you about your symptoms. He or she will look at the bite and check for a rash. They may order a blood test. But those aren’t always necessary to make the diagnosis. They can often give false results, especially in early-stage Lyme disease.
People who have joint swelling or nervous system problems may need to have special tests. Your doctor may need to take some fluid from the swollen joint or the spine to check for clues to your condition.
If you have been sick for 4 weeks or more, call your doctor. He or she can give you a blood test at this stage. It will tell you if you have Lyme disease.
Lyme disease treatment
Lyme disease is treated with antibiotics. In most cases, people bitten by a tick are only given antibiotics if they are sick or have a rash. If you are bitten by a tick but don’t get sick or get a rash, you don’t need antibiotics.
Early-stage Lyme disease responds very well to treatment. In most cases, taking an antibiotic for 2 to 4 weeks kills the bacteria and clears up the infection. Your doctor will tell you how long to take the antibiotic. It’s important to take all the medicine your doctor prescribes. This will prevent the spread of Lyme disease to your joints, nervous system, or heart. If you have problems with the medicine, do not quit taking it. Call your doctor and talk to him or her about your side effects.
Late-stage Lyme disease is also treated with antibiotics. It may be necessary to give the antibiotics intravenously (through an IV) at this stage. Medicine that reduces swelling and pain can ease arthritis associated with late-stage Lyme disease. If necessary, excess fluid can be drained from any affected joints.
Living with Lyme disease
Most people treated in the early stages of Lyme disease make a quick and complete recovery. Some may experience symptoms for a few weeks after treatment. If you were treated for Lyme disease but you still don’t feel well, call your family doctor. He or she can make sure there isn’t something else wrong. They can help you find ways to ease your symptoms. Some patients have found relief with treatments typically used for chronic fatigue syndrome or fibromyalgia.
Other things you can do to help manage Lyme disease include:
- Educate yourself. There is a lot of inaccurate information to be sorted through, especially on the internet. Ask your doctor if you have questions.
- Track your symptoms. Keep a diary of your sleep patterns, eating habits, exercise routines, and how you’re feeling. You or your doctor may be able to make connections between them.
- Take care of yourself. Eat a healthy diet. Exercise as regularly as you can. Get plenty of rest.
- Find support. It can be hard to not feel well and not know why. Some people may think your symptoms aren’t real. Talk to friends and family. If they can’t offer support, talk with a counselor who can help you.
Campylobacter infection
Campylobacter infection is caused by Campylobacter bacteria, a common foodborne illness (“food poisoning”), which is is one of the main causes of diarrhea and foodborne illness. You usually get it from eating contaminated food, especially raw or undercooked poultry. You can also get it from drinking contaminated water or raw milk, or handling infected animal feces (poop). More than 2 million people get a Campylobacter infection each year, with babies younger than 1 year old, teens, and young adults most commonly affected.
Campylobacter bacteria can infect the gastrointestinal tract and cause diarrhea, fever, and cramps.
Good hand-washing and food safety habits will help prevent Campylobacter infections (or campylobacteriosis), which usually clear up on their own but sometimes are treated with antibiotics.
Some infected people don’t have any symptoms. If you do have symptoms, they start two to five days after you are infected. They usually last about one week, and can include
- Diarrhea (which could be bloody)
- Cramping
- Abdominal pain
- Fever
- Fatigue
- Nausea and vomiting
Health care providers use stool tests to make a diagnosis. Most people get better without treatment. You should drink extra fluids for as long as the diarrhea lasts. People who have a severe infection or a weakened immune system may need to take antibiotics. In rare cases, the infection can cause reactive arthritis or Guillain-Barre syndrome.
To prevent Campylobacter infection, cook poultry thoroughly. Use a separate cutting board and utensils for meats. Make sure to clean them carefully with soap and hot water after you use them.
Campylobacter infection causes
Campylobacter bacteria live in the intestines of many wild and domestic animals. They can pass to humans when animal feces (poop) contaminate food, meats (especially chicken), water (streams or rivers near where animals graze), and unpasteurized (raw) milk.
Once inside the human digestive system, Campylobacter infect and attack the lining of the small and large intestines. The bacteria also can affect other parts of the body. In some cases — particularly in very young kids and those with chronic illnesses or a weak immune system — they can get into the bloodstream (this is called bacteremia).
Campylobacteriosis can spread from person to person when someone comes into contact with fecal matter (poop) from an infected person (especially a child in diapers). Household pets can carry and spread the bacteria to people.
Campylobacter infection prevention
To avoid Campylobacter infection, use drinking water that has been tested and approved for purity (especially in developing countries) and buy only pasteurized milk and juices. While hiking and camping, don’t drink water from streams or from sources that pass through land where animals graze.
Wash your hands well before you prepare foods and after touching raw meats, especially poultry. Kill any bacteria in meats and eggs by cooking them thoroughly and eating while still warm. Refrigerate leftovers promptly. Wash cutting boards, countertops, and utensils with soap and hot water after contact with raw meat. Clean produce — especially leafy greens — before serving.
When caring for a family member who has diarrhea, wash your hands well and often, especially before touching other people and before eating or preparing food. Clean and disinfect toilets after the person with diarrhea uses them. Also, if a pet dog or cat has diarrhea, wash your hands often and check with your veterinarian about treatment.
Campylobacter infection symptoms
Symptoms usually start 1 to 7 days after someone ingests the bacteria. The main symptoms are:
- fever
- abdominal cramps
- mild to severe diarrhea
The diarrhea is watery at first, but later may contain blood and mucus. Sometimes, the abdominal pain seems worse than the diarrhea. When this happens, the infection may be mistaken for appendicitis or a problem with the pancreas.
Campylobacter infection possible complications
Diarrhea can lead to dehydration, so kids with an infection should be watched closely. Signs of dehydration include thirst, irritability, restlessness, dizziness or drowsiness, sunken eyes, a dry or sticky mouth, dry skin, peeing less than usual, and in infants a dry diaper for more than 4–6 hours.
In a few cases, campylobacteriosis can lead to reactive arthritis (a type of joint inflammation) or, rarely, Guillain-Barré syndrome (an uncommon autoimmune disorder).
Campylobacter infection diagnosis
Doctors may send a stool sample to the lab to be tested for Campylobacter bacteria. They might order other lab tests, especially if there’s blood in the stool. If needed, a blood test can confirm bacteremia.
Campylobacter infection treatment
Most kids with Campylobacter infection will recover without needing medicine. Sometimes, doctors prescribe antibiotics, especially for very young children or when symptoms are severe or lasting. Kids should take the antibiotics on schedule for as long as the doctor directed to make sure the infection is gone. Do not use nonprescription medicines for diarrhea without a doctor’s OK.
After seeing a doctor, most kids with Campylobacter infections can recover at home, especially if they aren’t dehydrated. They should drink plenty of fluids for as long as the diarrhea lasts and be watched for signs of dehydration.
Kids with mild diarrhea and no dehydration should continue to eat normally and drink lots of fluids. Fruit juices and soft drinks can make diarrhea worse, though, and should be avoided. If your child is dehydrated, your doctor may recommend using an oral rehydration solution. Breastfed babies who get campylobacteriosis should continue to be breastfed throughout the illness.
Diarrhea usually stops within 2 to 5 days. Full recovery usually takes about 1 week. Sometimes, diarrhea can last longer or stop and then come back.
Rabies
Rabies is a deadly animal disease caused by a rabies virus that is almost always fatal following the onset of clinical symptoms. Rabies can happen in wild animals, including raccoons, skunks, bats and foxes, or in dogs, cats or farm animals. People get it from the bite of an infected animal. In up to 99% of cases, domestic dogs are responsible for rabies virus transmission to humans. Yet, rabies can affect both domestic and wild animals. Rabies is spread to people through bites or scratches, usually via saliva.
Rabies is present on all continents, except Antarctica, with over 95% of human deaths occurring in the Asia and Africa regions.
In people, symptoms of rabies include fever, headache and fatigue, then confusion, hallucinations and paralysis. Once the symptoms begin, the disease is usually fatal. A series of shots can prevent rabies in people exposed to the virus. You need to get them right away. If an animal bites you, wash the wound well; then get medical care.
To help prevent rabies
- Vaccinate your pet. Rabies vaccines are available for dogs, cats and farm animals
- Don’t let pets roam
- Don’t approach stray animals. Animals with rabies might be aggressive and vicious, or tired and weak
Rabies causes
Rabies is caused by the rabies virus. Infected animals have the virus in their saliva. The virus enters the body through broken skin or the eyes, nose, or mouth, and travels through nerves to the brain. People are usually infected following a deep bite or scratch from an animal with rabies, and transmission to humans by rabid dogs accounts for 99% of cases. Africa and Asia have the highest rabies burden in humans and account for 95% of rabies deaths, worldwide.
Bites from a wild infected animal cause most U.S. rabies cases. Raccoons are the most common carriers, but bats are most likely to infect people. Skunks and foxes also can be infected, and a few cases have been reported in wolves, coyotes, bobcats, and ferrets. Small rodents such as hamsters, squirrels, chipmunks, mice, and rabbits are rarely infected. Widespread animal vaccination has made transmission from dogs to people rare in the U.S. In the rest of the world, exposure to rabid dogs is the most common cause of transmission to humans.
Transmission can also occur when infectious material – usually saliva – comes into direct contact with human mucosa or fresh skin wounds. Human-to-human transmission through bites is theoretically possible but has never been confirmed.
Contraction of rabies through inhalation of virus-containing aerosols or through transplantation of infected organs is rare. Contracting rabies through consumption of raw meat or animal-derived tissue has never been confirmed in humans.
Rabies prevention
To reduce the chances of rabies exposure:
- Vaccinate your pets.
- Report stray animals to your local health authorities or animal-control officer.
- Remind kids not to touch or feed stray cats or dogs wandering in the neighborhood or elsewhere.
- Teach kids to stay away from wild animals such as bats, raccoons, skunks, and foxes.
If your child has been bitten by an animal, especially if it was an unknown dog or wild animal:
- Wash the bite area well with soap and water and cover the bite with a clean bandage.
- Call your doctor right away and go to the nearest emergency department. Anyone with a possible rabies infection must be treated in a hospital.
- Call local animal-control authorities to help find the animal. It may need to be caught and watched for signs of rabies.
- If you know the owner of the animal that bit your child, get all the information you can, including its vaccination status and the owner’s name and address.
- Notify your local health department, especially if the animal wasn’t vaccinated.
Extensive wound washing
- This involves first-aid of the wound that includes immediate and thorough flushing and washing of the wound for a minimum of 15 minutes with soap and water, detergent, povidone iodine or other substances that kill the rabies virus.
Also call your doctor if:
- Your child was exposed to an animal that might have rabies, but is too young to describe the contact with the animal.
- Your child was exposed to bats, even if there is no bite.
- You plan to travel abroad and may come into contact with wild animals. This is even more important if you’re going to an area with limited access to health care.
Eliminating rabies in dogs
Rabies is a vaccine-preventable disease. Vaccinating dogs is the most cost-effective strategy for preventing rabies in people. Dog vaccination reduces deaths attributable to rabies and the need for post-exposure prophylaxis as a part of dog bite patient care.
Awareness on rabies and preventing dog bites
Education on dog behaviour and bite prevention for both children and adults is an essential extension of a rabies vaccination programme and can decrease both the incidence of human rabies and the financial burden of treating dog bites. Increasing awareness of rabies prevention and control in communities includes education and information on responsible pet ownership, how to prevent dog bites, and immediate care measures after a bite. Engagement and ownership of the programme at the community level increases reach and uptake of key messages.
Preventive immunization in people
Human rabies vaccines exist for pre-exposure immunization. These are recommended for people in certain high-risk occupations such as laboratory workers handling live rabies and rabies-related (lyssavirus) viruses; and people (such as animal disease control staff and wildlife rangers) whose professional or personal activities might bring them into direct contact with bats, carnivores, or other mammals that may be infected.
Pre-exposure immunization is also recommended for travellers to rabies-affected, remote areas who plan to spend a lot of time outdoors involved in activities such as caving or mountain-climbing. Expatriates and long-term travellers to areas with a high rabies exposure risk should be immunized if local access to rabies biologics is limited. Finally, immunization should also be considered for children living in, or visiting, remote, high-risk areas. As they play with animals, they may receive more severe bites, or may not report bites.
Post-exposure prophylaxis (PEP)
Post-exposure prophylaxis (PEP) is the immediate treatment of a bite victim after rabies exposure. This prevents virus entry into the central nervous system, which results in imminent death. Post-exposure prophylaxis consists of:
- extensive washing and local treatment of the wound as soon as possible after exposure;
- a course of potent and effective rabies vaccine that meets WHO (World Health Organization) standards; and
- the administration of rabies immunoglobulin (RIG), if indicated.
Effective treatment soon after exposure to rabies can prevent the onset of symptoms and death.
Is rabies contagious?
Rabies is not contagious from person to person. The virus most often spreads through bites from an infected animal. But it can also spread if the animal’s saliva (spit) gets directly into a person’s eyes, nose, mouth, or an open wound (such as a scratch or a scrape).
Rabies symptoms
The incubation period for rabies is typically 2–3 months but may vary from 1 week to 1 year, dependent upon factors such as the location of virus entry and viral load. Initial symptoms of rabies include a fever with pain and unusual or unexplained tingling, pricking, or burning sensation (paraesthesia) at the wound site. As the virus spreads to the central nervous system, progressive and fatal inflammation of the brain and spinal cord develops.
There are two forms of the disease:
- People with furious rabies exhibit signs of hyperactivity, excitable behaviour, hydrophobia (fear of water) and sometimes aerophobia (fear of drafts or of fresh air). Death occurs after a few days due to cardio-respiratory arrest.
- Paralytic rabies accounts for about 20% of the total number of human cases. This form of rabies runs a less dramatic and usually longer course than the furious form. Muscles gradually become paralyzed, starting at the site of the bite or scratch. A coma slowly develops, and eventually death occurs. The paralytic form of rabies is often misdiagnosed, contributing to the under-reporting of the disease.
Rabies diagnosis
There’s no way to know right away if a wild animal has rabies. When a person is bitten by or exposed to an animal that might be sick, doctors don’t wait for a diagnosis — they treat right away. Lab tests can check for infection, but the results come later in the disease, when it would be too late to treat.
A biting animal that’s caught can be tested to see the virus is in its brain, but it must be euthanized (put to sleep) first. If it’s a healthy pet, such as a dog, cat, or ferret, experts recommend watching the animal for 10 days to see if it gets sick. If it’s a rabbit, rodent, or other small animal that doesn’t usually spread rabies, a doctor can check with the local health department to decide what to do.
Rabies treatment
If rabies symptoms start, there is no effective treatment. This is why doctors focus on prevention and try to stop the disease right after a person is exposed.
Anyone who thinks they may have been exposed to the rabies virus must get medical care right away.
Doctors give two shots as soon possible:
- Rabies immune globulin: This provides protection right away while the vaccine starts working.
- Rabies vaccine: This is given as a series of four doses, on days 0, 3, 7, and 14 (day 0 is the day of the first dose). People with a weakened immune system get an extra dose on day 28.
Ringworm
Ringworm is a type of fungal skin infection. Fungi (the plural of fungus) are microscopic plant-like organisms that thrive in damp, warm environments. They’re usually not dangerous, but sometimes can cause disease. When they infect the skin, they cause mild but annoying rashes. Fungal skin infections are also known as tinea infections.
When fungus grows in the area of the groin, upper thighs, and buttocks, it is called jock itch. When it grows on the feet, it is called athlete’s foot.
But when fungus grows anywhere else on the body, it’s known as ringworm. Its medical name is tinea capitis when it’s on the scalp, and tinea corporis when it’s on the rest of the body. On the nails it is known as onychomycosis.
Ringworm causes
Ringworm is caused by fungi that normally live on the skin, hair, and nails called dermatophytes. When the environment they live in gets warm and moist, they grow out of control and start to cause symptoms.
Is ringworm contagious?
Yes. Ringworm can spread:
- from one person to another by skin-to-skin contact, especially in warm, damp environments
- to other areas of the body if a person touches the affected area and then touches other body parts, such as the hands
- from animals to people
How do people get ringworm?
Besides spreading from person to person, ringworm can come from pets or other animals (usually cats, dogs, or rodents). It thrives in warm, moist environments such as public showers, locker rooms, or pool areas and can spread when people are in close physical contact. That’s why it’s common in people who play contact sports such as wrestling. It can also be passed on objects like combs, brushes, hats, towels, or clothing.
Minor skin injuries (such as scratches), too much exposure to heat and humidity, and some health conditions (such as diabetes, obesity, or immune system problems) can make a person more likely to develop it.
Ringworm prevention
Ringworm can often be prevented. To avoid it, kids and teens should:
- Keep their skin clean and dry, by washing daily and drying completely, particularly after showering, swimming, and sweaty activities.
- Use clean towels and avoid sharing clothing, towels, combs, brushes, and hats.
- Wash sports gear and uniforms as often as possible and don’t share them.
- Avoid tight-fitting clothing.
- Change clothing every day.
- Wash hands well with soap and water after playing with pets.
- Treat any other fungal infections, such as athlete’s foot.
Ringworm signs and symptoms
Ringworm on the skin starts as a red, scaly patch or bump. Over time, it may look like one or more rings with raised, bumpy, scaly borders (the center is often clear). This ring pattern gave ringworm its name, but not every infected person has it. The skin may flake, peel, or crack, and it can itch, sting, burn, or feel uncomfortable.
Ringworm on the scalp may start as a small sore that looks like a pimple before becoming patchy, flaky, or scaly. These flakes may look like dandruff. It can make some hair fall out or break into stubble, leaving a bald spot. It also can make the scalp swollen, tender, and red.
Sometimes, it causes a pus-filled mass known as a kerion, which can be confused with impetigo or cellulitis (bacterial infections). When the scalp is infected, it can cause swollen lymph nodes at the back of the head or neck.
Ringworm on the nails may affect one or more nails on the hands or feet. The nails may become thick, white or yellowish, and brittle.
Ringworm diagnosis
A doctor can often diagnose ringworm just by looking at it and asking questions about the symptoms and the child’s lifestyle. Sometimes the doctor will scrape off a small sample of the flaky infected skin to look at under a microscope or to test in a laboratory.
Ringworm treatment
Using over-the-counter (OTC) antifungal creams, sprays, or powders may solve a mild infection. More serious infections may need prescription medicine, either topical (put on skin) or in pill/syrup form.
Ringworm on the nails or scalp usually is treated with medicine taken by mouth for 1 to 3 months. An antifungal shampoo prescribed by the doctor can help prevent the spread to other people.
Your child should use the medicine as long as is recommended, even if the rash seems to be getting better. If not, the infection can come back and spread to other parts of the body.
To help heal the skin, it’s important to keep the affected area clean and dry. Your child should:
- Wash and then dry the area with a clean towel. (A separate clean towel should be used for the rest of the body.)
- Apply the antifungal cream, powder, or spray as directed on the label.
- Change clothing every day.
- Treat any other fungal infections, such as athlete’s foot.
How long does ringworm last?
Most mild cases of ringworm usually clear up in 2 to 4 weeks. But treatment might be needed for up to 3 months if the infection is more serious, or affects the nails or the scalp.
Rocky Mountain spotted fever
Rocky Mountain spotted fever is a disease caused by a type of bacteria carried by ticks.
Rocky Mountain spotted fever causes
Rocky Mountain spotted fever is caused by the bacteria Rickettsia rickettsii (R. Rickettsii), which is carried by ticks. The bacteria spread to humans through a tick bite.
In the western United States, the bacteria are carried by the wood tick, and in the eastern US, they are carried by the dog tick. Other ticks spread the infection in the southern US and in Central and South America.
Contrary to the name “Rocky Mountain,” most recent cases have been reported in the eastern United States, including North and South Carolina, Virginia, Georgia, Tennessee, and Oklahoma. Most cases occur in the spring and summer and are found in children.
Risk factors include recent hiking or exposure to ticks in an area where the disease is known to occur. The bacteria are unlikely to be transmitted to a person by a tick that has been attached for less than 20 hours. Only about 1 in 1,000 wood and dog ticks carry the bacteria. Bacteria can also infect people who crush ticks they have removed from pets with their bare fingers.
Rocky Mountain spotted fever prevention
Rocky Mountain spotted fever can be prevented by avoiding tick-infested areas, like woods and tall grasses, brush, shrubs, and low tree branches, and by taking precautions when spending time outdoors.
When you’re outdoors, wear light-colored clothing that makes ticks more visible and, if it’s practical, long-sleeved shirts and long pants. Use an insect repellant that fends off ticks, being careful to follow the label instructions. Be sure to use a repellent that contains 10% to 30% concentration of DEET (look for N,N-diethyl-meta-toluamide).
Not all ticks carry the Rocky Mountain spotted fever bacteria, but it’s wise to remove any immediately. The longer a tick stays attached to the skin, the greater the chance of infection. It usually takes several hours for a tick to transmit the bacteria that cause Rocky Mountain spotted fever once it has become attached to the skin.
To remove a dog tick, use tweezers to grasp it by the head (not just the body) as close to the skin as possible. Pull steadily until the tick dislodges. Without touching the tick, preserve it in a jar or plastic bag until you can show it to your doctor. Disinfect the bite area with alcohol, wash your hands, and call your doctor.
Since pets also can bring ticks into your home, check their skin and fur for ticks whenever they have been playing in tick-infested areas. Follow your veterinarian’s advice about collars and other products that can be used to keep your pet tick-free.
If you have any concerns, talk with your doctor.
Rocky Mountain spotted fever symptoms
Symptoms usually develop about 2 to 14 days after the tick bite. They may include:
- Chills and fever
- Confusion
- Headache
- Muscle pain
- Rash — usually starts a few days after the fever; first appears on wrists and ankles as spots that are 1 to 5 mm in diameter, then spreads to most of the body.
- Some infected people don’t get a rash.
Other symptoms that may occur with this disease:
- Diarrhea
- Light sensitivity
- Hallucinations
- Loss of appetite
- Nausea and vomiting
- Abdominal pain
- Thirst
Rocky Mountain spotted fever possible complications
Untreated, the infection may lead to health problems such as:
- Brain damage
- Clotting problems
- Heart failure
- Kidney failure
- Lung failure
- Meningitis
- Pneumonitis (lung inflammation)
- Shock
Rocky Mountain spotted fever diagnosis
Your health care provider will perform a physical examination and ask about the symptoms.
Tests that may be done include:
- Antibody titer by complement fixation or immunofluorescence
- Complete blood count (CBC)
- Kidney function tests
- Partial thromboplastin time (PTT)
- Prothrombin time (PT)
- Skin biopsy taken from the rash to check for R. rickettsii
- Urinalysis to check for blood or protein in the urine
Rocky Mountain spotted fever treatment
Treatment involves carefully removing the tick from the skin. To get rid of the infection, antibiotics such as doxycycline or tetracycline need to be taken. Pregnant women are usually prescribed chloramphenicol.
Rocky Mountain spotted fever prognosis
Treatment usually cures the infection. About 3% of people who get this disease will die.
Toxocariasis
Toxocariasis is an infection transmitted from animals to humans (zoonosis) caused by the parasitic roundworms commonly found in the intestine of dogs (Toxocara canis) and cats (Toxocara cati). When common parasites of dogs and cats infect humans, the illness is called toxocariasis (or visceral larva migrans). Dogs and cats that are infected with Toxocara can shed Toxocara eggs in their feces. You or your children can become infected by accidentally swallowing dirt that has been contaminated with dog or cat feces that contain infectious Toxocara eggs. Although it is rare, people can also become infected from eating undercooked meat containing Toxocara larvae. Toxocariasis usually affects kids under age 10. Especially at risk are those who like to put things in their mouths, or kids whose families have pet dogs or cats.
Toxocariasis causes
Toxocariasis is an infection caused by the larvae of parasitic worms — Toxocara canis and Toxocara cati — that usually live in the intestines of dogs and cats. Eggs from the worms pass into the feces of dogs and cats and can contaminate pet areas around the home where kids play. The eggs can be swallowed by children, especially those who like to put things in their mouths and don’t often wash their hands.
After entering the body, the eggs hatch into larvae that penetrate through walls of the digestive tract and may migrate to a child’s liver, lungs, eyes, and elsewhere.
Toxocariasis usually happens in young children ages 2 to 7, but can happen at any age. It can’t be spread from person to person.
Toxocariasis prevention
To help prevent kids from being exposed to toxocariasis:
- keep them away from areas where dogs or cats play
- teach your kids to wash their hands often, especially after playing with a pet dog or cat (wash a toddler’s hands yourself)
- discourage toddlers from putting dirty hands in their mouth
- keep pets away from the sandbox and cover the sandbox when it’s not being used
- take household pets to the veterinarian to be dewormed, especially puppies younger than 6 months old
- make sure your kids don’t accidentally eat dirt or soil
Toxocariasis signs and symptoms
Many people who are infected with Toxocara do not have symptoms and do not ever get sick. Some people may get sick from the infection, and may develop:
- Ocular toxocariasis: Ocular toxocariasis occurs when Toxocara larvae migrate to the eye. Symptoms and signs of ocular toxocariasis include vision loss, eye inflammation or damage to the retina. Typically, only one eye is affected.
- Visceral toxocariasis: Visceral toxocariasis occurs when Toxocara larvae migrate to various body organs, such as the liver or central nervous system. Symptoms of visceral toxocariasis include fever, fatigue, coughing, wheezing, or abdominal pain.
Many kids won’t have symptoms, but if they do, they can include fever, cough or wheezing, abdominal pain, enlarged liver or spleen, poor appetite, a rash that sometimes looks like hives, and enlarged lymph nodes (“swollen glands”).
Toxocariasis also may affect the eyes, causing decreased vision, swelling around the eyes, or a cross-eyed appearance. Untreated toxocariasis can cause damage to the retina (the part at the back of the eye that senses light).
Most cases go undiagnosed and do not cause problems. Some toxocariasis cases are diagnosed during a routine eye exam or an X-ray study done for some other reason.
Toxocariasis diagnosis
A doctor can usually diagnose a case of toxocariasis by physical exam and blood tests. Doctors may not prescribe any medication to treat a child with mild symptoms. Severe toxocariasis involving the lungs, eye, or other important organs may be treated with antiparasitic drugs to kill the larvae. For severe toxocariasis, doctors sometimes also prescribe steroids or might refer a person to a specialist (like an ophthalmologist if the eye is involved).
Toxocariasis treatment
A child with severe toxocariasis should be given antiparasitic medicine as prescribed by your doctor. Treatment of ocular toxocariasis is more difficult and usually consists of measures to prevent progressive damage to the eye. Prevent reinfection by deworming your pets and keeping kids away from areas where pets defecate (poop). Remind your kids to wash their hands often during the day, especially after playing with pets.
Toxoplasmosis
Toxoplasmosis is an infection caused by a tiny parasite called Toxoplasma gondii, that can live inside the cells of humans and animals, especially cats and farm animals and be spread through its feces. It also can live in dirt and on some food you eat.
If you have been pregnant, you may already know it’s important to avoid toxoplasmosis, which people can develop by cleaning the litter box of an infected cat or eating undercooked meat or other contaminated foods.
The Centers for Disease Control and Prevention (CDC) estimates that about 60 million people in the United States could have toxoplasmosis, but most won’t have symptoms because their immune systems are strong.
Toxoplasmosis causes
People get toxoplasmosis when they come into contact with the parasite. This can happen in several ways.
You can get it through food if you:
- Eat raw or undercooked meat, especially pork, lamb, or wild game.
- Touch something, such as a cutting board or dish, that has been in contact with raw or undercooked meat and then touch your mouth, eyes, or face.
- Eat unwashed raw fruits and vegetables.
- Drink water with the parasite in it.
Cats can carry the parasite, especially if they hunt animals or eat raw meat. You can expose yourself to the parasite through your cat’s feces, either in its litter or in dirt that has cat droppings in it. You also can get it from touching anything that has been in contact with cat droppings.
People who have an organ transplant or a blood transfusion can get toxoplasmosis if the organ or blood is infected. This is very rare.
How toxoplasmosis spreads
People can catch toxoplasmosis from:
- touching or coming into contact with infected cat feces (poop). A cat can become infected from eating infected rodents, birds, or other small animals.
- eating raw or undercooked meat (especially lamb, pork, and venison) from animals that were infected
- eating raw, unwashed fruits or vegetables that have touched manure
- being born with it (a woman who gets toxoplasmosis while pregnant may pass the parasite to her unborn child through the bloodstream)
- accidentally ingesting (swallowing) the eggs of the parasite, which can get on the hands after handling soil without gloves or handling uncooked, unwashed foods
- drinking contaminated water
Although infection doesn’t normally spread from person to person except through pregnancy, in rare instances toxoplasmosis can contaminate blood transfusions and organs donated for transplantation.
Toxoplasmosis prevention
There are many things you can do to protect yourself and prevent toxoplasmosis.
- Wear gloves when you work outside. Cover children’s sandboxes when not in use. Cats often use gardens and sandboxes as litter boxes.
- Wash your hands after being outside, especially before you eat or prepare food.
- Wash your hands after touching cats, soil, or raw meat.
- Wash or peel all fruits and vegetables before eating them.
- Avoid touching your eyes, mouth, or face when preparing food.
- Use hot soapy water to clean items that have been in contact with raw meat.
- Clean the counter after preparing food.
- Cook meat and poultry until it is no longer pink in the center or until the juices run clear.
- Avoid eating undercooked meat and unwashed fruits and vegetables.
- Avoid drinking untreated water. This is more common in underdeveloped countries. Avoid drinking unpasteurized (raw) goat’s milk or eating raw eggs.
- Control flies and cockroaches as much as possible. They can spread contaminated soil or cat feces onto food.
If you are at risk, you should take extra precautions.
- Keep your cat indoors so that it does not pick up the parasite.
- Feed your cat only dry or canned cat food. Like humans, cats can become infected by eating raw or undercooked meat.
- Avoid touching outdoor or stray cats.
- Have someone else take care of your cat or change your cat’s litter box while you are pregnant. If you have to change the cat litter yourself, wear gloves while you do it. When you finish, wash your hands well with soap and warm water. Clean the litter box daily. Disinfect it with boiling water for 5 minutes.
Toxoplasmosis signs and symptoms
Toxoplasmosis is passed from animals to humans, sometimes without causing any symptoms.
Most people do not show signs of toxoplasmosis. This is because their immune systems attack the parasite and prevent illness. You may have flu-like symptoms, such as:
- fatigue
- headache
- body aches
- fever
- swollen lymph nodes (glands in your neck).
People who have a weak immune system may have worse symptoms. These can include:
- confusion
- blurry vision
- trouble with balance and coordination
- seizures
- lung problems.
You may have a weak immune system if you:
- Have human immunodeficiency virus (HIV). This can lead to acquired immunodeficiency syndrome (AIDS).
- Have cancer.
- Have had an organ transplant.
Congenital Toxoplasmosis
When a pregnant woman (even one with no symptoms) catches toxoplasmosis during pregnancy and it’s not treated, there’s a chance that she could pass the infection to her developing fetus. Babies infected during their mother’s first trimester tend to have the most severe symptoms.
A woman who got toxoplasmosis before getting pregnant usually won’t pass the infection to the baby — this is because she (and, therefore, her baby) will have built up immunity to the infection. Toxoplasmosis can be reactivated, meaning it can come back, in a pregnant woman who’s had a previous toxoplasma infection and has a weakened immune system. Generally, it’s probably a good idea to wait to try to get pregnant until at least 6 months after a toxoplasmosis infection.
Up to 90% of children born with congenital toxoplasmosis have no symptoms early in infancy, but a large percentage will show signs of infection months to years later. Premature newborns and very small newborns show clear signs of infection at birth or shortly after.
Signs and symptoms, if they happen, can include:
- fever
- swollen glands (lymph nodes)
- jaundice (yellowed skin and eyes caused by high levels of the liver chemical bilirubin)
- an unusually large or small head
- rash
- bruises or bleeding under the skin
- anemia
- an enlarged liver or spleen
Some babies with congenital toxoplasmosis have brain and nervous system problems that cause:
- seizures
- limp muscle tone
- feeding problems
- hearing loss
- intellectual disability (mental retardation)
They’re also at high risk for eye damage involving the retina (the light-sensitive lining at the back of the eye that’s responsible for sight), resulting in severe vision problems.
If a child is born with congenital toxoplasmosis and isn’t treated during infancy, there’s almost always some sign of the infection (often eye damage) by early childhood to adolescence.
Toxoplasmosis diagnosis
Routine screening for toxoplasmosis is not recommended. Contact you doctor if you have symptoms or are at risk. Doctors can diagnose toxoplasmosis through laboratory tests that check for microscopic parasites in the blood, spinal fluid, amniotic fluid, placenta, lymph nodes, bone marrow, or other body tissues.
More often, doctors order blood tests to measure the level of antibodies (substances that are part of the body’s defensive immune reaction) produced to fight the parasites.
Genetic tests can identify the DNA-containing genes of toxoplasmosis parasites once they’ve invaded the body. These tests are especially useful for checking the amniotic fluid for evidence of congenital toxoplasmosis in a fetus. Obstetricians may use ultrasounds to help diagnose congenital toxoplasmosis. But these tests aren’t 100% accurate and can lead to false-positive results, meaning there may not actually be an infection.
For babies, doctors ask the mother about things like exposure to household cats or contaminated food or water sources. Tests that might be done for these babies include eye, ear, and nervous system examinations, spinal fluid analysis, and imaging of the head to look for changes in the brain.
Talk to your doctor if you are pregnant or planning to become pregnant, or if you have a weak immune system. These people are at an increased risk.
Toxoplasmosis treatment
Unless someone has a weakened immune system or is pregnant, there’s often no need to treat a toxoplasmosis infection — symptoms (such as swollen glands) usually go away on their own in a few weeks or months. However, kids should always be checked by a doctor because swollen glands can be a sign of other illnesses.
If a pregnant woman gets infected, her doctor and an infectious disease specialist work together to create a treatment plan. Research has shown that treating the mother can help make the infant’s disease less severe, but it won’t necessarily prevent the infant from getting toxoplasmosis.
Children born with congenital toxoplasmosis are treated with different combinations of anti-toxoplasmosis medications, usually for 1 year after birth. A specialist will decide which medicines to use and for how long.
In healthy older kids who develop serious toxoplasmosis infections, treatment usually lasts 4 to 6 weeks (or for at least 2 weeks after symptoms are gone). Kids with weakened immune systems often need to be hospitalized when they develop toxoplasmosis, and those with AIDS may need to take anti-toxoplasmosis medication for life.
Living with toxoplasmosis
Women who get toxoplasmosis while pregnant are at risk of passing it to their unborn babies. In most cases, infected babies are born healthy but may have future health issues. These include damage to the eyes and brain.
Women who were infected at least 6 to 9 months before pregnancy should have immunity. This means the infection will not be active during pregnancy, and the risk of passing it to your baby is low.
There is no benefit to testing your cat’s droppings for toxoplasmosis. Once cats are infected, they only spread the parasite in their droppings for the first few weeks.
Birds
Pet birds, even if they are kept in a cage, may transmit these diseases:
- Cryptococcosis: a fungal disease contracted when someone inhales organisms found in bird droppings, especially from pigeons, that can cause pneumonia. People with weakened immune systems from illnesses such as HIV or cancer are at increased risk of contracting this disease and developing serious complications, such as meningitis.
- Psittacosis: also known as parrot fever, a bacterial illness that can happen from contact with infected bird feces or with the dust that builds up in birdcages. Symptoms include coughing, high fever, and headache. It is treated with antibiotics.
Reptiles and Amphibians
Reptiles (including lizards, snakes, and turtles) and amphibians (including frogs, toads, and salamanders) put kids at risk for:
- Salmonellosis: Reptiles and amphibians shed Salmonella in their feces. Touching the reptile’s skin, cage, and other contaminated surfaces can lead to infection. Salmonellosis causes symptoms such as abdominal pain, diarrhea, vomiting, and fever. Young children are at risk for more serious illness, including dehydration, meningitis, and sepsis (blood infection).
Other Animals
Handling and caring for rodents — including hamsters and gerbils — as well as fish can place kids at risk for:
- Lymphocytic choriomeningitis virus (LCMV): People can get lymphocytic choriomeningitis virus by inhaling particles that come from urine, feces, or saliva from infected rodents, such as mice and hamsters. Lymphocytic choriomeningitis virus infection can cause flu-like symptoms — fever, tiredness, headaches, muscle aches, nausea, and vomiting — and may even lead to meningitis (an inflammation of the membrane that surrounds the brain and spinal cord) and encephalitis (an inflammation of the brain). As with most viruses, there is no specific treatment, but some patients might need to be hospitalized. Like toxoplasmosis, lymphocytic choriomeningitis may be passed from an infected pregnant woman to her fetus.
- Mycobacterium marinum: This infection may happen in people exposed to contaminated water in aquariums or pools. Although mycobacterium marinum infections are generally mild and limited to the skin, they can be more severe in people with HIV or weakened immune systems.