Contents
What is acanthosis nigricans
Acanthosis nigricans is not a skin condition in itself, but can be a sign of an underlying health problem or disease. These underlying conditions aren’t usually serious, although occasionally acanthosis nigricans can be sign of cancer. And people who have acanthosis nigricans are much more likely to develop type 2 diabetes. Acanthosis nigricans is characterized by darkening (hyperpigmentation) and thickening (hyperkeratosis) of the skin, occurring mainly in the folds of the skin in the armpit (axilla), groin and back of the neck. The skin patches will be dry and rough, feeling similar to velvet. They may also be itchy.
If you have acanthosis nigricans, you’ll have thickened, brownish-grey or black patches of skin. The darkened and thickened patches usually develop slowly over time. Acanthosis nigricans patches that grow and spread quickly are more likely to be associated with cancer. In these cases, the mouth, tongue, throat, nose and windpipe may also be affected.
You may also have lots of tiny finger-like growths from the patches. This is known as papillomatosis. There may also be skin tags around the affected area. These are small flesh-colored or pigmented growths that hang off the skin and look a bit like warts.
These acanthosis nigricans patches may occur anywhere, but are usually seen around the neck, in the armpit, around the groin and sometimes in other skin folds. Occasionally, the skin over the joints of the fingers and toes may be affected, as well as the lips, palms of the hands and soles of the feet.
There are two important types of acanthosis: benign acanthosis nigricans and malignant acanthosis nigricans. Although classically described as a sign of internal malignancy, this is very rare. Benign types, sometimes described as ‘pseudoacanthosis nigricans’ are much more common.
Acanthosis nigricans can affect individuals of any age and of any ethnic background. Acanthosis nigricans can develop in children and in teenagers, though it is more common in adults. Acanthosis nigricans is also more common in people with darker skin. Males and females are affected equally.
Acanthosis nigricans more commonly develops in:
- Overweight or obese people
- People with diabetes or other glandular (endocrine) problems
- People taking certain medications (for example, oral contraceptives, niacinamide, or corticosteroids)
- People who have had kidney transplants
Seven types of acanthosis nigricans have been described:
- Obesity associated acanthosis nigricans:
- Most common type of acanthosis nigricans
- May occur at any age but more common in adulthood
- Obesity often caused by insulin resistance
- Syndromic acanthosis nigricans: defined as acanthosis nigricans that is associated with a syndrome, e.g. hyperinsulinaemia, Cushing syndrome, polycystic ovary syndrome (PCOS), total lipodystrophy, Crouzon syndrome, Down syndrome
- Benign acanthosis nigricans:
- Also referred to as acral acanthotic anomaly
- Thick velvety lesion most prominent over the upper surface of hands and feet in patients who are in otherwise good health
- Most common in dark-skinned people, especially those of African American descent
- Drug-induced acanthosis nigricans: Uncommon, but acanthosis nigricans may be induced by several medications, including nicotinic acid, insulin, systemic corticosteroids and hormone treatments.
- Hereditary benign acanthosis nigricans:
- Acanthosis nigricans inherited as an autosomal dominant trait
- Lesions may manifest at any age, infancy, childhood or adulthood
- Malignant acanthosis nigricans:
- Acanthosis nigricans associated with internal malignancy, e.g., digestive system, liver, kidney, bladder, or lymphoma
- Most common underlying cancer is tumour of the gut (90%) especially stomach cancer
- In 25-50% of cases, lesions are present in the mouth on the tongue and lips
- Mixed-type acanthosis nigricans: Patients with one type of acanthosis nigricans whom also develop new lesions of a different cause, e.g. overweight patient with obesity-associated acanthosis nigricans who then develops malignant acanthosis nigricans.
Benign acanthosis nigricans may be associated with obesity, polycystic ovary syndrome (PCOS), diabetes mellitus, adrenal insufficiency and other insulin-resistant conditions. Acanthosis nigricans may also occur secondary to the use of drugs such as nicotinic acid, insulin, systemic corticosteroids and diethylstilbestrol, and, less commonly, with oral contraceptives, fusidic acid and methyltestosterone. Discontinuation of the drug leads to improvement or even disappearance of the acanthosis nigricans lesions. Acanthosis nigricans maligna (malignant acanthosis nigricans) is a well-known paraneoplastic dermatosis that was first described in 1890 1. There is extensive mucocutaneous involvement and rapid progression in association with systemic cancer, usually a gastric adenocarcinoma. Rigel and Jacobs 2 reported the association of malignant acanthosis nigricans with cancers of the ovary, endometrium, cervix, breast, testicle, lung, kidney, pancreas, liver, esophagus, prostate, thyroid and pharynx, among others. The underlying malignancies tend to be very aggressive. Mean survival following diagnosis has been reported to range from 8.7 to 11.9 months.
Features of acanthosis nigricans
- Thickened brown velvety textured patches of skin that may occur in any location but most commonly appear in the folds of the skin in the armpit, groin and back of the neck.
- Papillomatosis (multiple finger-like growths) is common on cutaneous and mucosal surfaces.
- Skin tags often found in and around affected areas.
- Pruritus (itching) may be present, particularly in acanthosis nigricans associated with malignancy (paraneoplastic pruritus).
- Acanthosis nigricans lesions may also appear on the mucous membranes of the oral cavity, nasal and laryngeal mucosa and oesophagus.
- Lesions involving the mucosa, palms and soles tends to be more extensive and more severe in malignant acanthosis nigricans.
- Patients with malignant acanthosis nigricans tend to be middle-aged, not obese and lesions develop abruptly.
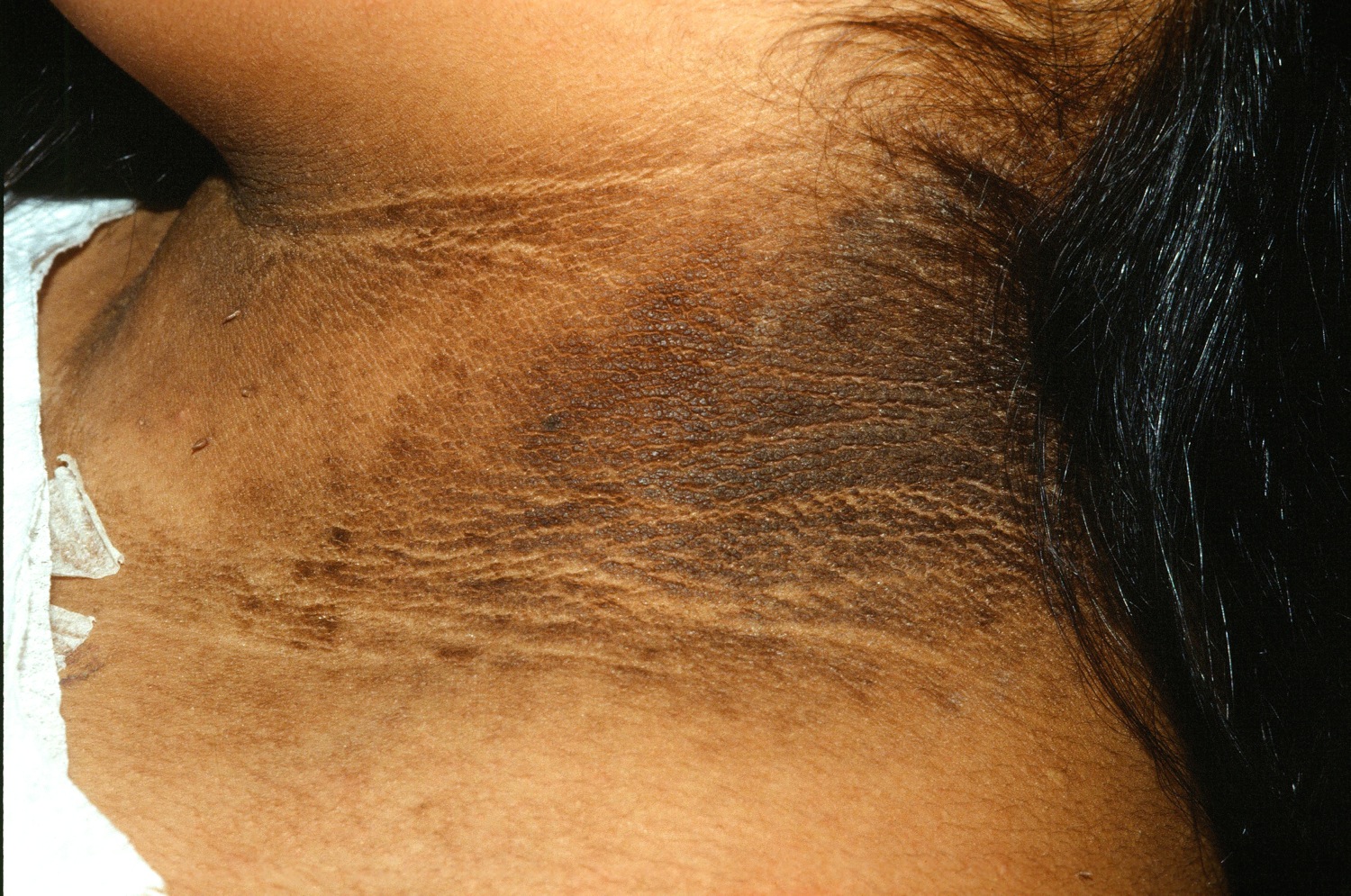
Figure 1. Acanthosis nigricans neck
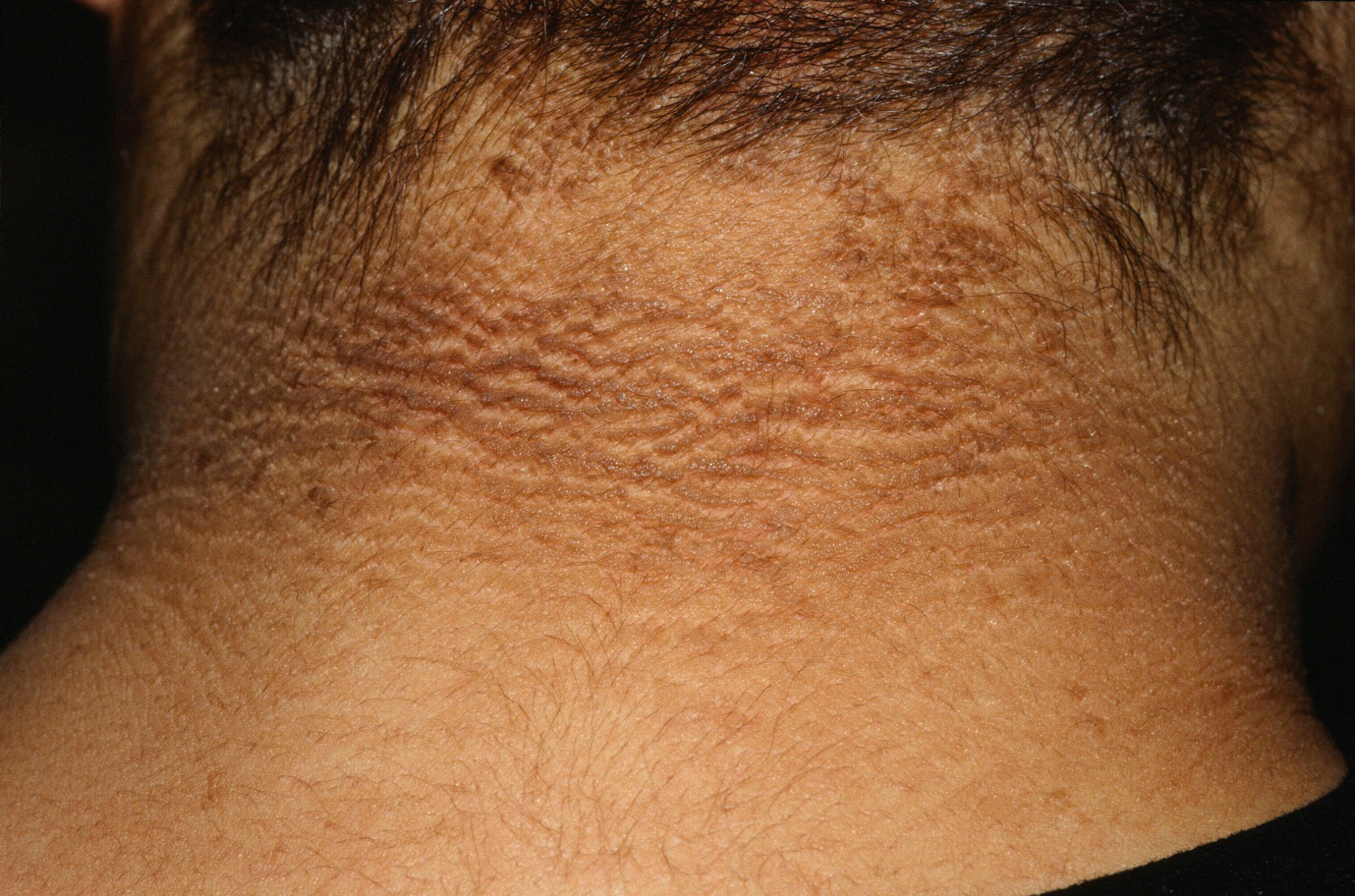
Figure 2. Acanthosis nigricans neck
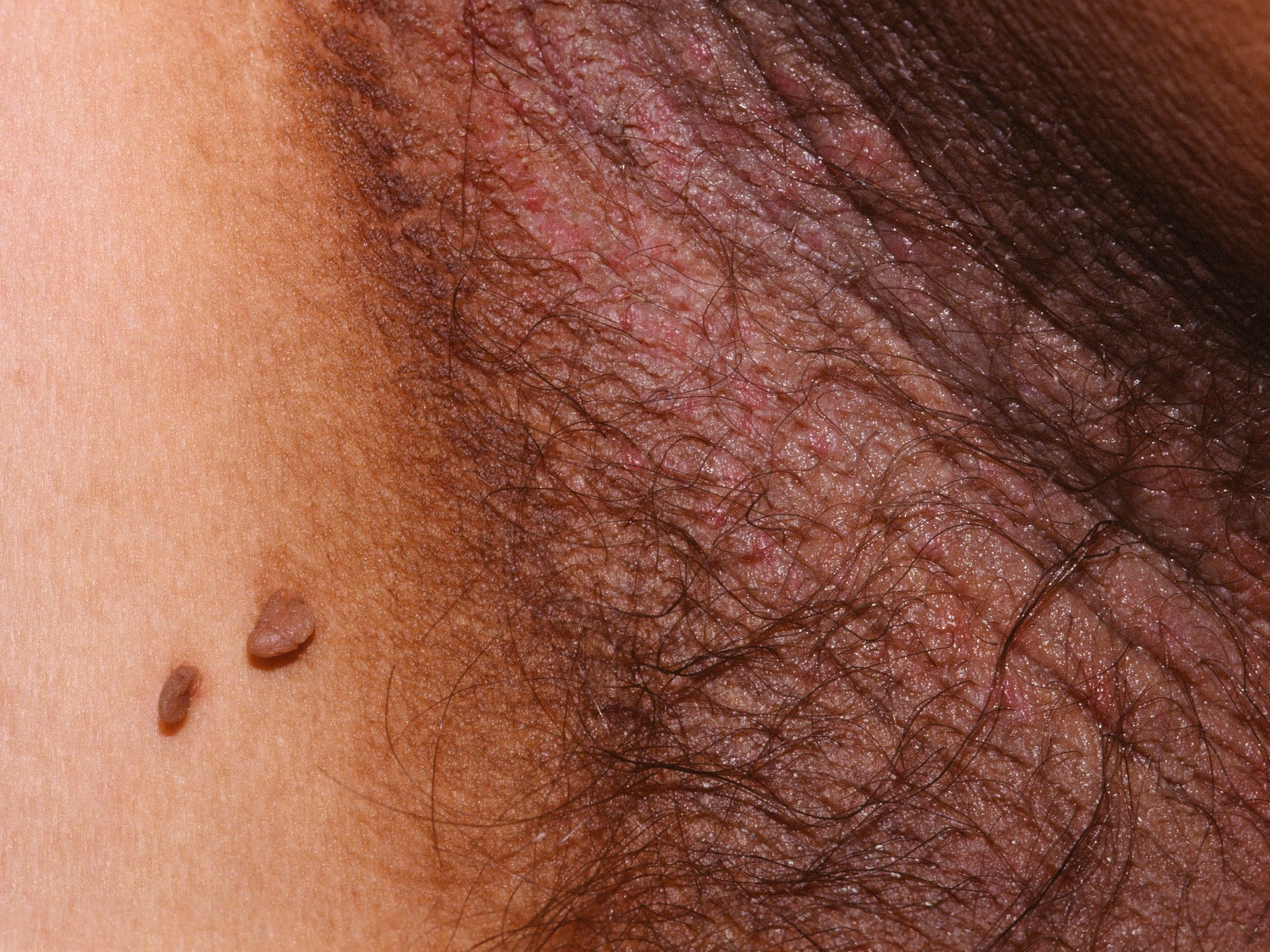
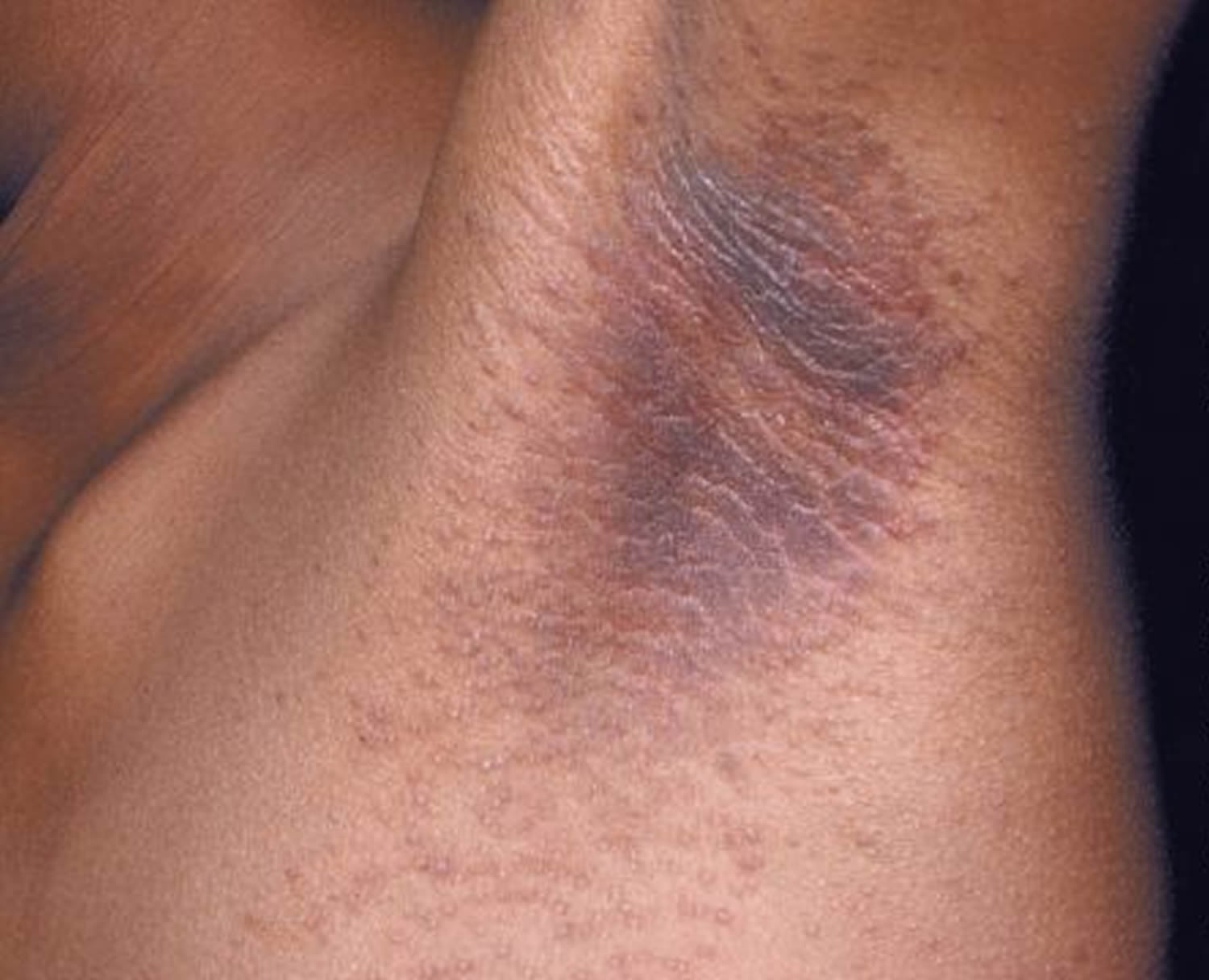
Figure 3. Acanthosis nigricans armpit
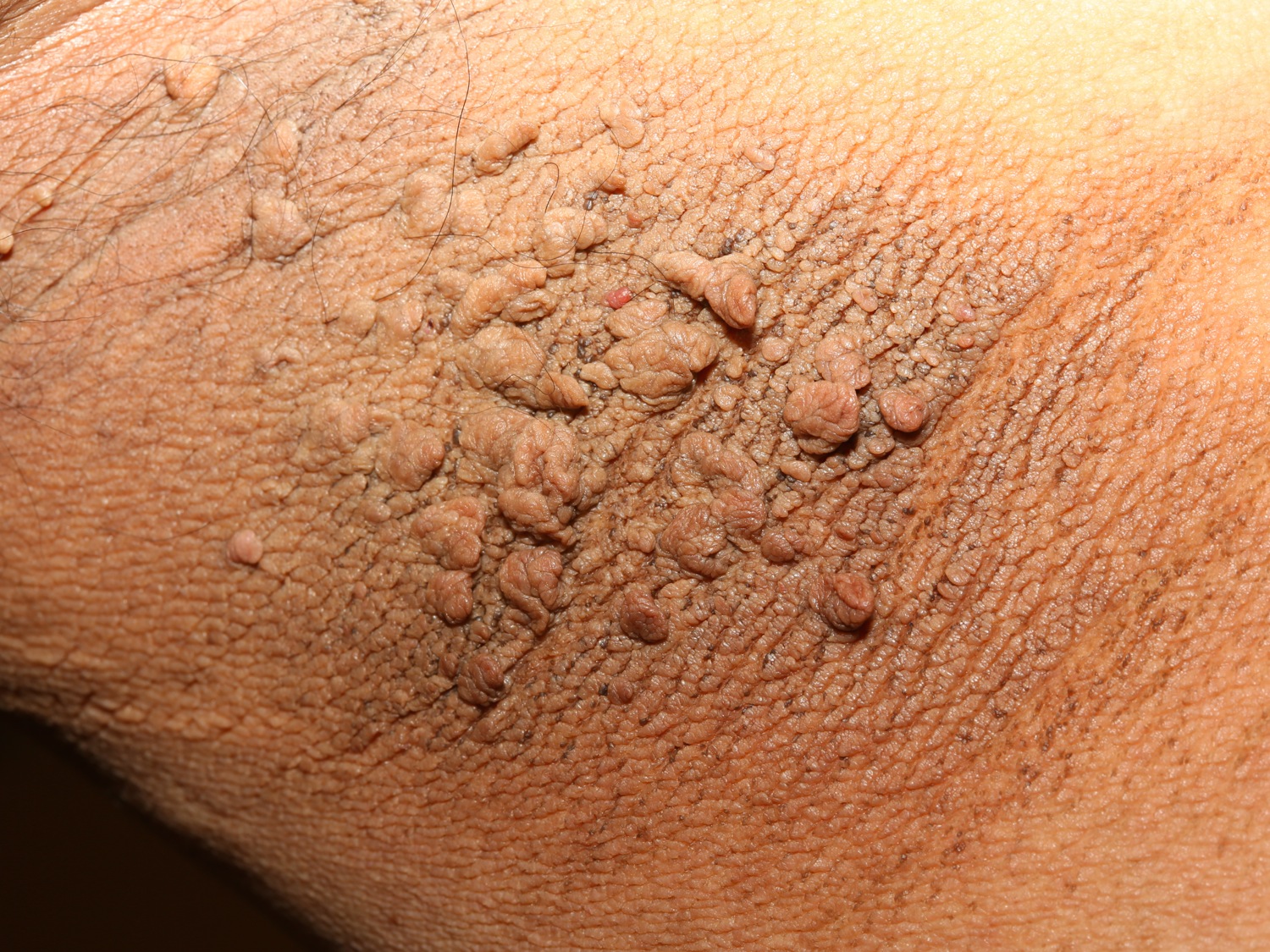
Figure 4. Acanthosis nigricans armpit
Malignant acanthosis nigricans
Malignant acanthosis nigricans is a paraneoplastic condition in which acanthosis nigricans is precipitated by an internal cancer.
The typical velvety thickening of the skin occurs. In contrast to the classic (and much more common) acanthosis nigricans, malignant acanthosis nigricans is often more severe and affects skin in unusual places. In 277 cases reviewed in one study, the condition was associated with gastric carcinomas in 55.5% and other intra-abdominal carcinomas in 17.7%. Tripe palms is a variant where velvety thickening is seen on the palms. Verrucous or velvety thickening of the lips may occur 3.
The exact incidence of malignant acanthosis nigricans has never been established; however, it was reported in 2 out of 12,000 patients with cancer over a 10-year period 4. There is extensive mucocutaneous involvement and rapid progression in association with systemic neoplasia, usually a gastric adenocarcinoma. Rigel and Jacobs 4 reported the association of malignant acanthosis nigricans with carcinomas of the ovary, endometrium, cervix, breast, testicle, lung, kidney, pancreas, liver, esophagus, prostate, thyroid and pharynx, among others. The underlying malignancies tend to be very aggressive. Mean survival following diagnosis has been reported to range from 8.7 to 11.9 months.
Acanthosis nigricans causes
Acanthosis nigricans sometimes occurs in people who are otherwise in good health, particularly dark-skinned people of African descent.
However, in most cases acanthosis nigricans is a sign of an underlying problem or condition such as obesity, diabetes or abnormal hormone levels. The cause for acanthosis nigricans is still not clearly defined but it appears to be related to insulin resistance.
Acanthosis nigricans has been associated with various benign and malignant conditions. Some of the main causes of acanthosis nigricans are outlined below.
Obesity
Acanthosis nigricans is usually the result of obesity. This is known as obesity-associated acanthosis nigricans.
It occurs because obesity can cause insulin resistance (when the body is unable to properly use the hormone insulin), which may lead to high levels of insulin in the blood, affecting the skin cells.
Insulin resistance can also cause type 2 diabetes, so acanthosis nigricans can be an early sign that you have diabetes or are at risk of developing the condition.
Syndromes and hormone problems
Acanthosis nigricans is sometimes associated with an underlying syndrome or hormone problem, such as:
- Polycystic ovary syndrome (PCOS)– a condition that affects how a woman’s ovaries work, which can cause excessive body hair, irregular periods, infertility, acne and weight gain
- Cushing’s syndrome – symptoms such as weight gain, bruising and stretch marks caused by very high levels of the hormone cortisol in the body
- Acromegaly – where the body produces too much growth hormone, leading to the excess growth of body tissues over time
- Underactive thyroid (hypothyroidism) – where your thyroid gland does not produce enough hormones, causing symptoms such as tiredness and weight gain
This type of acanthosis nigricans is known as syndromic acanthosis nigricans.
Medication
Acanthosis nigricans is sometimes triggered by medicines, including insulin, corticosteroids, and hormone treatments such as human growth hormone or the contraceptive pill.
This is known as drug-induced or medication-associated acanthosis nigricans.
Genes
In rare cases, acanthosis nigricans can be caused by a faulty gene inherited directly from your parents. This is known as familial or benign genetic acanthosis nigricans.
This type is usually passed on in an autosomal dominant pattern, which means it can be passed on if only one of your parents carries the faulty gene.
Cancer
If the dark skin patches come on suddenly and spread quickly, it may be a sign you have cancer (usually stomach cancer). This is known as malignant acanthosis nigricans.
This is a rare condition that tends to affect middle-aged or elderly people, regardless of their weight or ethnic background.
The patches are more severe and the mouth, tongue and lips may also be affected. The skin may also become irritated and itchy.
Risk factors for acanthosis nigricans
Acanthosis nigricans risk factors include:
- Obesity. The heavier you are, the higher your risk of acanthosis nigricans.
- Race. Studies show that in the United States, acanthosis nigricans is more common among Native Americans.
- Family history. Some types of acanthosis nigricans appear to be hereditary.
Acanthosis nigricans outlook (prognosis)
Most cases of acanthosis nigricans are harmless and not a sign of anything serious. The skin patches often fade with time as the underlying condition is treated.
If you have inherited acanthosis nigricans from your parents, your patches may gradually get bigger before staying the same or eventually fading on their own.
Only in cases where there is underlying cancer is the situation very serious. If the tumor is successfully treated, the condition may disappear, but unfortunately the types of cancer that cause acanthosis nigricans tend to spread quickly and a cure is often not possible.
Acanthosis nigricans signs and symptoms
The lesions of acanthosis nigricans appear as “velvety” thickenings of the outer skin, and they can range in color from gray to brown to black. Darker-skinned people tend to have darker lesions.
The most common locations for acanthosis nigricans include:
- Sides and back of the neck
- Armpits
- Groin
Less commonly, acanthosis nigricans can affect the:
- Face
- Inner thighs
- Elbows
- Knees
- Belly button (navel)
Rarely, acanthosis nigricans can occur in the:
- Nipples
- Eyelids
- Lips
- Inside of the mouth
- Anus
Acanthosis nigricans diagnosis
Acanthosis nigricans is typically detected during a skin exam. Rarely, a small skin sample is removed (biopsied) for examination in a lab. If the cause of acanthosis nigricans is unclear, your doctor may recommend blood tests, X-rays or other tests to look for possible underlying causes.
It is very important to differentiate acanthosis nigricans related to malignancy from that related to benign conditions. Tumors in malignant acanthosis nigricans are usually very aggressive and spread quickly. Death often occurs soon after. If malignant acanthosis nigricans is suspected in a patient without known cancer, it is extremely important to perform a thorough workup for underlying malignancy and identify a hidden tumor. If the tumor can be successfully treated, the condition may resolve.
Other causes of acanthosis nigricans may be identified by screening for insulin resistance and diabetes mellitus.
Acanthosis nigricans treatment
How to get rid of acanthosis nigricans
Treatment for acanthosis nigricans aims to correct the underlying cause of your symptoms. This will usually cure the acanthosis nigricans or significantly improve the appearance of your skin.
- Correct hyperinsulinemia through diet, exercise and medication
- Lose weight with obesity-associated acanthosis nigricans
- Excise or treat underlying tumor
- Stop offending medicines in drug-induced acanthosis nigricans
In hereditary acanthosis nigricans, lesions tend to enlarge gradually before stabilizing and/or regressing on their own.
There is no specific treatment for acanthosis nigricans. Treatments considered are used primarily to improve cosmetic appearance and include topical retinoids, dermabrasion and laser therapy.
Final outcome of acanthosis nigricans varies depending on the cause of acanthosis nigricans. Benign conditions either on their own or through lifestyle changes and/or treatment have good outcomes. However, the prognosis for patients with malignant acanthosis nigricans is often poor. The associated cancer is often advanced and the average survival of these patients is approximately 2 years.
Acanthosis nigricans cure
- losing weight, exercise and making changes to your diet and taking medication to reduce the level of insulin in your blood. Some reports have documented complete clearing of acanthosis nigricans with weight loss and metformin over several years 5.
- taking medication to correct your hormone levels – read about treating Cushing’s syndrome, treating polycystic ovary syndrome and treating an underactive thyroid
- switching to a different medication if it’s triggering your symptoms
- surgery, chemotherapy, or radiotherapy for cancer
There’s no specific treatment to get rid of the patches, but a dermatologist (skin specialist) may be able to recommend treatments such as creams or tablets that may help improve the look of your skin.
Acanthosis nigricans treatment cream
Once the medical condition has been diagnosed and treatment has been started, the doctor may recommend a topical cream or lotion containing:
- Prescription-strength alpha- or beta-hydroxy acids (glycolic acid, lactic acid, salicylic acid)
- Prescription-strength urea
- A retinoid such as tretinoin, tazarotene, or adapalene
With regard to skin cream, some dermatologists suggest combination use of a keratolytic and a retinoid, e.g., ammonium lactate 12% or 20% urea cream every morning and tretinoin or tazarotene every night.
For more severe, stubborn acanthosis nigricans, oral treatments may include:
- Fish oils taken as diet supplements
- Isotretinoin (a very strong medication with many potential side effects, often used in the treatment of severe, scarring acne)
Other procedures, not usually covered by insurance, include:
- Dermabrasion (a mechanical process of controlled, surgical scraping of the skin)
- Laser treatments (which make the skin thinner by destroying the uppermost layers)
Home remedies
Because most people who develop acanthosis nigricans are overweight, their skin lesions can improve dramatically and even go away when they lose weight. Other medical conditions that cause these lesions should be treated as well.
Other treatments are:
- Lose weight, changing diet and exercise habits
- Apply over-the-counter preparations containing alpha-hydroxy acids such as glycolic acid or lactic acid
- Apply over-the-counter lotions containing the beta-hydroxy acid salicylic acid
- Apply over-the-counter creams containing urea
- Apply over-the-counter cortisone cream (if the areas are itchy)
- Unna PG, editor. International atlas of rare skin diseases. Part 4. London: HK Lewis and Co; 1890.[↩]
- Rigel DS, Jacobs MI. Malignant acantosis nigricans: a review. J Dermatol Surg Oncol. 1980;6:923-7.[↩]
- An. Bras. Dermatol. vol.86 no.3 Rio de Janeiro May/June 2011. http://www.scielo.br/scielo.php?pid=S0365-05962011000300025&script=sci_arttext&tlng=en[↩]
- Ortega-Loayza AG, Ramos W, Gutierrez EL, Chavez de Paz P, Bobbio L, Galarza C. Cutaneous manifestations of internal malignancies in a tertiary health care hospital of a developing country. An Bras Dermatol. 2010;85:736-42.[↩]
- PD 1017;34;e281[↩]