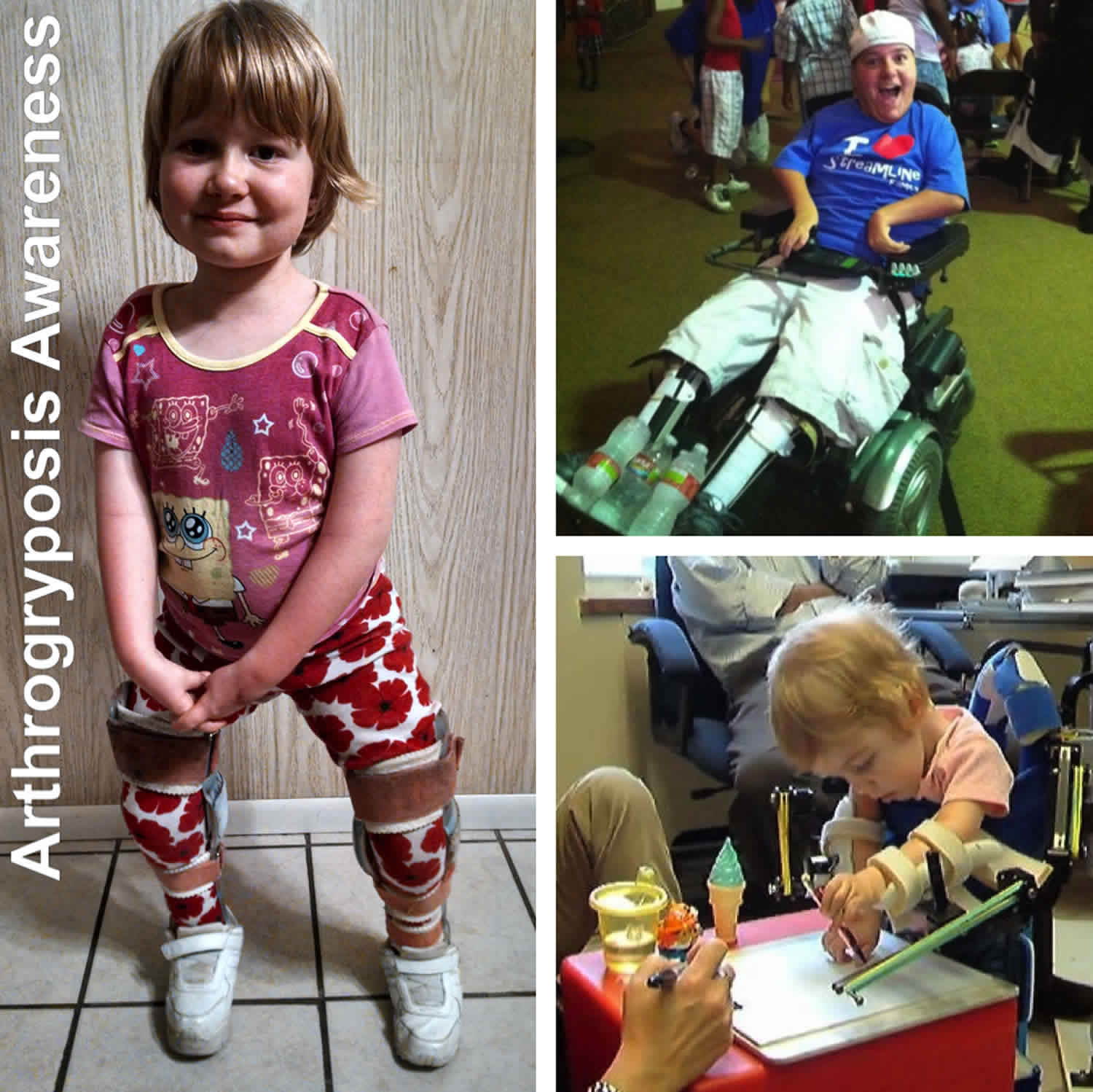
What is arthrogryposis
Arthrogryposis is a term used to describe a number of rare congenital (present at birth) conditions characterized by nonprogressive contractures, stiffness and loss of motion in more than one joint and abnormally developed muscles. A contracture is a condition in which a joint becomes permanently fixed in a bent (flexed) or straightened (extended) position, completely or partially restricting the movement of the affected joint. When congenital contractures occur only in one body area, it is not referred to as arthrogryposis but rather an isolated congenital contracture. The most common form of an isolated congenital contracture is clubfoot. When arthrogryposis affects two or more different areas of the body, it may be referred to as arthrogryposis multiplex congenita. The most common form of arthrogryposis multiplex congenita is Amyoplasia. Arthrogryposis and arthrogryposis multiplex congenita are sometimes used interchangeably.
The word arthrogryposis (arthro, from Greek meaning joint, gryp meaning curved, posis meaning fixed) refers to curved joint(s) in a fixed position. Thus, arthrogryposis multiplex congenita means curved joints in many (multiplex) areas of the body, which are present at birth (congenita). Babies are born with arthrogryposis and it is usually permanent. But medical experts can help kids get the best range of motion their stiff joints will allow.
The joint stiffness that happens with arthrogryposis is called contracture. It means the joint can’t move the way it should. Joints may stay straight and not bend, or they may stay bent and a child can’t straighten them.
Some contractures are mild. Others can be severe. Children may have:
- trouble moving
- poor growth
- weak muscles
- very thin or bony-looking arms and legs
Some children have problems in most of their joints. They may have stiff shoulders, elbows, hands, hips, knees, and feet. Some kids have only a few stiff joints.
When a child has contracture in just one joint (such as clubfoot), it’s not usually arthrogryposis.
Arthrogryposis is a rare condition, though the exact frequency with which it occurs is unknown. Previous studies estimate that it affects one to three of every 10,000 babies.
Arthrogryposis is not thought to be a genetic or hereditary condition. The exact cause of arthrogryposis is unknown, but a number of different theories have been proposed:
- Some believe that arthrogryposis is caused by obstructions to intrauterine movement during pregnancy.
- Others believe that it may be a result of an early viral infection during a baby’s development.
- Others believe that arthrogryposis is the result of failure of the central nervous system and/or muscular system to develop appropriately.
Your child’s doctor may prescribe physical and occupational therapy to increase your child’s muscle strength and improve flexibility.
Splints can also increase your child’s range of motion. A removable splint works so that the joints can be moved and muscles exercised periodically. In some cases, merely wearing a splint at night may be sufficient.
Arthrogryposis multiplex congenita is a rare condition and it’s important to find an experienced doctor that will effectively treat you or your child. Whether you are atypical or have a diagnosis you will need treatment, support groups are an excellent place to connect with others who can lead you in the right direction. Arthrogryposis multiplex congenita support group (https://amcsupport.org/) can connect you with support groups, other parents and caregivers through social media, mini-meet ups, and the yearly arthrogryposis multiplex congenita conference. This will give you an enormous amount of moral support and also ideas for tools and adaptive equipment to help you or your child along.
Arthrogryposis causes
Experts don’t always know why children have arthrogryposis. It could be something that stops the muscles and joints from developing as they should. Sometimes it’s because of another condition, like a disease of the nerves or muscles. Or it might happen because a fetus doesn’t move much during pregnancy. This can affect the way the baby’s muscles and nerves develop.
With some babies, there’s a genetic reason for arthrogryposis. If doctors tell you that your child’s condition is genetic, ask if your family should see a genetic counselor.
Arthrogryposis symptoms
Each child with arthrogryposis experience symptoms differently, but here is a list of some common ones:
- The range of motion of the joints in your child’s arms and legs may be limited or fixed
- Your child’s shoulders may be rotated inward
- Your child may have abnormal extension of her elbows
- Your child may be able to flex her wrists and fingers abnormally
- Your child could have dislocated hips
- Your child may have clubfoot
Arthrogryposis diagnosis
When a baby is born with more than one contracture, doctors will check the baby’s nerves and muscles. They may order blood tests or imaging tests like X-rays.
Doctors sometimes know that a baby has arthrogryposis before birth. That’s because it can show up on a prenatal ultrasound.
Most of the time, doctors can diagnose arthrogryposis and plan treatment based on a physical exam and routine tests. Doctors may also need to do tests like these:
- nerve conduction studies and electromyography (EMG)
- muscle or nerve biopsy
Arthrogryposis treatment
Doctors and other medical experts work together as a team to treat arthrogryposis. To help kids get the best range of motion from stiff, tight joints, treatment might include:
- bracing and orthotics for joint support
- splints and casts to improve joint position and motion
- physical therapy and occupational therapy
- at-home exercises and stretching to increase strength and flexibility
- surgery to reposition bones or move tendons (the cords that connect muscles to the bones)
Your child’s doctor may recommend surgery to improve how she can position and move her limbs. These procedures may include muscle releases, tendon transfers or bone fusions to improve flexibility and correct deformities.
How can I help my child with arthrogryposis?
- Focus on the things your child can do.
- Encourage your child to try new things.
- Help your child be as active as possible.
- Give your child plenty of ways to learn and use all his or her abilities.
Arthrogryposis prognosis
Your child will most likely have persistent muscular and/or joint limitations due to his/her arthrogryposis. Unlike many other conditions, arthrogryposis is non-progressive and does not worsen as your child ages.
Therapy helps kids do the most they can as they grow. Your care team will give you exercises to do with your child at home. It takes time for a child’s abilities to improve. Be patient and offer your support to older kids. Parents play a big part in the treatment of arthrogryposis.
Many kids can do things on their own and grow up to be independent. Others need more help. Even when arthrogryposis limits physical abilities, kids usually can think and learn just as well as other kids do.
With physical therapy and other treatments, your child will likely have substantial improvement in his/her function. Most children go on to lead productive, independent lives as adults.
Arthrogryposis life expectancy
With physical therapy and other treatments, your child will likely have substantial improvement in his/her function. Most children go on to lead productive, independent lives as adults.
Arthrogryposis multiplex congenita
Arthrogryposis multiplex congenita refers to the development of multiple joint contractures affecting two or more areas of the body prior to birth. A contracture occurs when a joint becomes permanently fixed in a bent or straightened position, which can impact the function and range of motion of the joint and may lead to muscle atrophy. arthrogryposis multiplex congenita is not a specific diagnosis, but rather a physical symptom that can be associated with many different medical conditions. It is suspected that arthrogryposis multiplex congenita is related to decreased fetal movement during development which can have a variety of different causes, including environmental factors (i.e. maternal illness, limited space), single gene changes (autosomal dominant, autosomal recessive, X-linked), chromosomal abnormalities and various syndromes. Treatment varies based on the signs and symptoms found in each person, but may include physical therapy, removable splints, exercise, and/or surgery.
The number of males and females affected by arthrogryposis multiplex congenita is approximately equal. The condition has been reported in individuals of Asian, African and European descent. Isolated congenital contractures affect approximately 1 in 500 individuals in the general population. arthrogryposis multiplex congenita affects approximately 1 in 3,000 individuals. arthrogryposis multiplex congenita is present at birth (congenital).
The recognized definition of arthrogryposis multiplex congenita is a condition that causes congenital contractures of two or more body parts. It is important to remember that arthrogryposis multiplex congenita is not a diagnosis but is an umbrella term that covers over 300-400 different types of conditions and syndromes 1).
A simple way to categorize arthrogryposis multiplex congenita issue is:
Amyoplasia
Amyoplasia (A = no, myo=muscle, plasia=growth) means no muscle growth and is the most common type of arthrogryposis multiplex congenita. It is estimated that one third of people born with arthrogryposis multiplex congenita will have Amyoplasia about 1 in 10,000 and it’s typically referred to as ‘Classical type arthrogryposis multiplex congenita.’ This is considered the non-genetic form of arthrogryposis multiplex congenita, meaning there has been no mutation in the genes to cause the condition to be present, and is not passed down from the parents. Amyoplasia appears to be sporadic and not recur in families.
Amyoplasia is a disorder characterized by multiple contractures of the joints. The shoulders may be internally rotated and drawn inward (adducted), the elbows are usually extended, and the wrists are usually flexed. In most affected individuals, the fingers are flexed and stiff. Although in most reports, the distal joints (i.e., those joints farthest away from the center of the body) are usually more severely affected, the shoulders and hips (which are proximal joints) often have significant contractures. Affected individuals usually have severe clubfoot. Some affected individuals may have dislocated hips. In some cases, a birthmark (a splotchy reddish birthmark also called a “Stork mark”) may be found at birth on the face. Individuals with Amyoplasia usually have normal intelligence, no significant craniofacial abnormalities, and no other serious abnormalities of internal organs (visceral abnormalities). However, about 10% of individuals with Amyoplasia have abdominal abnormalities such as gastroschisis (a condition in which a hole is present in the wall of the abdomen allowing the intestines to intrude out of the abdominal space) or intestinal atresia (blockage of the intestine). Another 10% have squashed or missing distal fingers or toes. Amyoplasia is common in one of monozygotic twins.
Common traits of people with Amyoplasia are 2):
- Affected in both arms and legs, and often the spine
- Internally rotated shoulders
- Extended elbows
- Flexed wrists
- Contractors of the fingers
- Lower limbs can be stuck in various positions
- Hips can have flexion/abduction/external rotational contractures (Buddha position or frog position)
- Dislocated hips (about 30%)
- Hip extension contractures (less common)
- Flexion contractures of the knees
- Extension contractures of the knees (less common)
- Club feet
- About 10% affected individuals may have squashed or missing fingers and toes. (less common)
- Scoliosis (20-30%)
- Splotchy red mark on the face (stork bite)
- About 10% of Amyoplasia cases individuals may have abdominal abnormalities such as gastroschisis. Gastroschisis is a condition in which a hole is present
- in the wall of the abdomen allowing the intestines to intrude out of the abdominal space. (less common)
- Normal or above average intelligence
Distal arthrogryposis
People with distal arthrogryposis are primarily affected in the hands and feet. Other areas and body functions can be affected depending on what type one has. There are currently 20+ different types of distal arthrogryposis all of which are linked back to genetic mutations. The best way to learn about you or your child’s specific type is to discuss it with health care providers and people in the arthrogryposis multiplex congenita community.
Distal arthrogryposis is characterized by multiple congenital contractures. Common symptoms include contractures of two or more areas of the body, less involvement of the proximal joints (those joints closest to the center of the body), and highly variable expressivity, which means that specific symptoms vary greatly even among individuals with the same disorder and even in the same family. At least 10 different forms of distal arthrogryposis have been identified including Freeman-Sheldon syndrome, Gordon syndrome, trismus-pseudocamptodactyly syndrome, multiple pterygium syndrome and Sheldon-Hall syndrome.
Here are a few of the more common types of distal arthrogryposis.
Type 1 Distal arthrogryposis
Type 1 is characterized by joint deformities that restrict movement in the hands and feet.
Common traits of distal type 1 distal arthrogryposis are:
- Facial sparing
- Multiple contractures in hands and feet
- Clenched hands
- Overlapping fingers
- A hand deformity in which all of the fingers are angled outward toward the little finger. This is called ulnar deviation
- Hips and knees can be affected but it is less common and usually mild
- Club feet
Type 2A (Freeman-Sheldon Syndrome)
Freeman-Sheldon Syndrome primarily affects the hands, feet and face. Distinctive facial features such as a small mouth, with purse lips give the appearance of a whistling face, hence also being called “Whistling Face Syndrome”.
Common traits of Freeman-Sheldon Syndrome are:
- Prominent forehead and brow ridges
- Widely spaced eyes
- Deep set eyes
- Outside corner of the eyes that point downward
- Narrowing of the eye openings
- Droopy eye lids
- Eyes that do not look in the same direction
- Sunken appearance of the middle of the face
- Short nose and a long area between the nose and the mouth
- Deep folds in the skin between the nose and lips
- Full cheeks
- Small mouth with pursed lips
- Chin dimple shaped like an H or a V
- Small tongue and jaw and a high arch in the roof of the mouth
- Difficulty swallowing
- Multiple contractors in hands and feet
- A hand deformity in which all of the fingers are angled outward toward the little finger. This is called ulnar deviation.
- Club feet
- Spine that curves to the side (scoliosis)
- Failure to gain weight and grow at expected weight
- Respiratory complications
- Speech problems
- Hearing loss
- Malignant hyperthermia is a condition where people have negative reactions to certain drugs used during general anesthesia. If it is of concern you can speak to your doctor about avoiding the use of succinylcholine during general anesthesia.
Type 2B (Sheldon-Hall Syndrome)
Sheldon-Hall Syndrome is similar to Freeman Sheldon Syndrome in that both have joint contractures of various areas of the body. However there are enough differences between the two that they are considered separate conditions.
Common traits of Sheldon-Hall Syndrome are:
- Triangular shaped face
- Outside corner of the eyes that point downward
- Deep folds in the skin between the nose and lips
- Attached ear lobes
- Small mouth with pursed lips
- High arched roof of the mouth
- Extra folds of skin on the neck
- Permanently bent fingers and toes
- Overlapping fingers
- A hand deformity in which all of the fingers are angled outward toward the little finger. This is called ulnar deviation.
- Club feet
- Vertical talus deformity
Type 9 (Beals Syndrome)
Beals syndrome is also known as congenital contractural archnodactyly and has many of the same features as Marfan Syndrome. While Beals and Marfan share similar features they are also very distinct in the way they affect a person so it is important to obtain a accurate diagnosis so appropriate treatment can be given.
Common traits of Beals syndrome are:
- Abnormally shaped ears resulting in a crumpled appearance
- Unusually small jaw and or high arched palate
- Abnormal short neck
- Rounded upper back
- Chest sinks in or sticks out
- Long narrow body type with long limbs
- Abnormally long slender fingers and toes
- Joints being stuck in a permanent flexed position
- Contractors in elbows and hands
- Contractures in feet
- Club feet
- Contractures affecting the hips, knees and ankles
- Curved spine (scoliosis)
- Backward or lateral curved spine
- Reduced bone mass
- Underdeveloped muscles
- Cardiovascular complications. It is recommended that those with Beals Syndrome have their heart monitored yearly as a precaution because on occasion heart issues like aortic enlargement or mitral valve regurgitation can occur.
Everything else
This category is one of the most complex due to the fact that there are over 250 different diagnosis. Anything that is not Distal or Amyoplasia arthrogryposis multiplex congenita goes into everything else category.
These include,but not limited too:
- Pterygium syndromes
- Lethal conditions
- Atypical arthrogryposis multiplex congenita
Pterygium syndromes
Pterygium syndrome is a congenital condition where webbing of the skin occurs around the joints causing a lack of muscle movement which then causes muscle weakness and joint contractures. Escobar syndrome and Lethal multiple pterygium syndrome are a few pterygium syndromes that are connected to arthrogryposis multiplex congenita. Escobar type multiple pterygium syndrome (Escobar syndrome). There are different types of pterygium syndromes, Escobar being one of the more common types.
Common traits of Escobar syndrome are:
Webbing of the skin that affects:
- Skin on the neck
- Fingers
- Forearms
- Inner thighs
- Backs of knees
Other features:
- Droopy eye lids
- Outside corners of the eyes point downward
- Skin folds covering the inner corner of the eyes
- Low set ears
- Small jaw
- Arms and legs that cannot fully extend
- Scoliosis
- Respiratory distress at birth due to underdeveloped lungs
- Males can have undescended testes
Lethal multiple pterygium syndrome is tragically individuals with this form of multiple pterygium syndrome typically do not make it past the 2nd or 3rd trimester of pregnancy.
Common traits of Lethal multiple pterygium syndrome are:
- Abnormally small head
- An opening in the roof of the mouth which is called cleft palet
- Fluid filled sac typically found on the back of the neck
- Excessive fluid in the body
- Severe multiple contractors
- Underdevelopment of the heart, lungs, or brain
- Twisting of the intestines
- Kidney abnormalities
- A hole in the muscle that separates the abdomen from the chest cavity
Lethal multiple pterygium syndrome also falls under the Lethal conditions subgroup in the Everything else category.
Lethal conditions
Tragically it is estimated that 1/3 of babies born with arthrogryposis multiplex congenita will either be still born or die during their first year of life. There are several forms of arthrogryposis multiplex congenita that can be deadly. As mentioned above Lethal Multiple pterygium syndrome is one. Another is cerebro-oculo-facio-skeletal syndrome (COFS) as well as restrictive dermopathy. People with cerebro-oculo-facio-skeletal syndrome (COFS) will progressively deteriorate and sadly many times will not survive past 7 years old.
Common traits of cerebro-oculo-facio-skeletal syndrome (COFS) can be:
- Extremely small head
- Abnormally small eyes
- Clouding of the eyes lens (cataract)
- Horizontally narrow opening between the eye lids
- Unusually prominent nose
- Abnormally large ears
- Upper lip over lapping lower lip
- Abnormally long groove in upper lip
- Unusually small jaw
- Elbows with flexion contractures
- One line in the palm of the hand formed by the fusion of two lines
- Hip deformities
- Knees with flexion contractures
- Congenital vertical talus deformity (rocker bottom)
- Grove over the length of the soles of the feet
- Osteoporosis
- Lack of muscle tone
- Feeding difficulties
- Vulnerability to respiratory infections
- Failure to thrive
- Developmental retardation
Restrictive dermopathy – Restrictive dermopathy is a lethal genetic skin condition that is connected to arthrogryposis multiplex congenita. Unfortunately most born with Restrictive dermopathy will not make it past the first week of life.
Common traits of Restrictive dermopathy are:
- delayed and stunted prenatal growth
- reduced fetal movements
- excessive amount of amniotic fluid
- premature rupture of the membranes
- thin tight skin
- translucent skin
- skin with damage at body parts that bend
- facial dysmorphism
- joint ankylosis (stiffness or fixation of joints and/or union of separate bones to
- form a single bone)
- death with in the first week of life
Atypical arthrogryposis multiplex congenita
Atypical arthrogryposis multiplex congenita is a term used to describe individuals with a unknown type of arthrogryposis multiplex congenita. arthrogryposis multiplex congenita is rare and highly complex and it can take years for certain people to receive the diagnosis that caused arthrogryposis multiplex congenita, and some may never receive a diagnosis at all. This can be a very long and frustrating journey for many families seeking answers about their loved ones with arthrogryposis multiplex congenita. Arthrogryposis multiplex congenita is a rare condition and it’s important to find an experienced doctor that will effectively treat you or your child. Whether you are atypical or have a diagnosis you will need treatment, support groups are an excellent place to connect with others who can lead you in the right direction. Arthrogryposis multiplex congenita support group (https://amcsupport.org/) can connect you with support groups, other parents and caregivers through social media, mini-meet ups, and the yearly arthrogryposis multiplex congenita conference. This will give you an enormous amount of moral support and also ideas for tools and adaptive equipment to help you or your child along.
Arthrogryposis multiplex congenita causes
The cause of arthrogryposis multiplex congenita depends on the specific type. For many types, the cause is not fully understood. Arthrogryposis or arthrogryposis multiplex congenita is not a specific diagnosis, but a physical finding that can be associated with numerous disorders and conditions. arthrogryposis multiplex congenita is thought to be related to decreased movement in utero, which can have multiple causes. Neurologic and muscle problems may well be the most common causes of decreased fetal movement, but connective tissue disorders, maternal illness, and limited space are also common causes. Some cases of arthrogryposis multiplex congenita occur as part of rare genetic disorders that are inherited. Some cases of arthrogryposis multiplex congenita are related to multiple factors including genetic and environmental ones (multifactorial inheritance).
arthrogryposis multiplex congenita may occur as part of certain single-gene disorders that can be inherited as autosomal recessive, autosomal dominant or X-linked traits. arthrogryposis multiplex congenita may also occur as part of chromosomal disorders (e.g., Trisomy 18, many microdeletions and microduplications). arthrogryposis multiplex congenita can also occur as part of certain connective tissue disorders. In addition, some cases of arthrogryposis multiplex congenita may occur due to abnormalities or disorders associated with improper developmental of the central nervous system or the peripheral nervous system or as part of intrinsic muscle disorders. These disorders may be genetic or may occur due to environmental factors.
The primary underlying mechanism that causes congenital contractures is believed to be decreased fetal movement during development. The joints begin to develop in a fetus around five or six weeks into pregnancy. Motion is essential for the proper development of fetal joints. A lack of fetal movement allows for excess connective tissue to form around the joints, which can result in the joint becoming fixed and/or limiting the movement of a joint. In theory, any factor that diminishes or restricts fetal movement can cause congenital contractures. Such factors would include fetal crowding (in which there is not enough room for the fetus to move around) such as when there are multiple births or uterine structural abnormalities. Restricted fetal movement can also occur secondary to maternal disorders including viral infections, drug use, trauma or other maternal illness. Low levels of amniotic fluid around the fetus (oligohydramnios) have also been linked to decreased fetal movement.
Amyoplasia, the most common form of arthrogryposis multiplex congenita, occurs randomly (sporadically). The distal arthrogryposes, another common form of arthrogryposis multiplex congenita, are usually inherited as autosomal dominant traits. Genetic diseases are determined by the combination of genes for a particular trait that are on the chromosomes received from the father and the mother. Dominant genetic disorders occur when only a single copy of an abnormal gene is necessary for the appearance of the disease. The abnormal gene can be inherited from either parent, or can be the result of a new mutation (gene change) only in the affected individual. The risk of passing the abnormal gene from affected parent to offspring is 50 percent for each pregnancy regardless of the sex of the resulting child.
Central and peripheral nervous system disorders that are associated with arthrogryposis multiplex congenita include a condition in which the brain and spinal cord do not close before birth (meningomyelocele), the spinal muscular atrophies, and disorders in which there is incomplete development of certain portions of the brain (e.g., anencephaly, hydranencephaly or holoprosencephaly). Most of these disorders develop due to multiple factors including genetic and environmental ones (multifactorial inheritance).
Less often, arthrogryposis multiplex congenita may be associated with certain muscle disorders including the muscular dystrophies, certain mitochondrial disorders and a variety of genetic muscle disorders that are present at birth (congenital myopathies). Such disorders are usually inherited.
Abnormalities affecting the development of connective tissue can cause arthrogryposis multiplex congenita as well. Connective tissue is the material between the cells of the body that gives tissues form and strength. The abnormal development of connective tissue in the joints can restrict fetal movements, potentially causing multiple contractures. A lack of joint development or the abnormal fusion of bones (synostosis) that are normally separate have also been associated with multiple congenital contractures. Several disorders, which are associated with abnormalities of connective tissue development, have been associated with multiple congenital contractures including diastrophic dysplasia, metatropic dwarfism, popliteal pterygium syndrome and Larsen syndrome.
In many cases of arthrogryposis multiplex congenita, the exact underlying cause of the contractures cannot be identified.
Arthrogryposis multiplex congenita signs and symptoms
The symptoms of arthrogryposis multiplex congenita are present at birth (congenital). However, specific symptoms and physical findings can differ greatly in range and severity from one person to another. In most cases, affected infants have contractures of various joints. The joints of the legs and arms are usually affected, the legs are affected more often than the arms. The joints of the shoulders, elbows, knees, wrists, ankles, fingers, toes, and/or hips are also commonly affected. In addition, the jaws and back may also be affected in individuals with arthrogryposis multiplex congenita. In most cases, arthrogryposis multiplex congenita occurs randomly, for no apparent reason (sporadic). More than 400 different conditions can cause isolated or multiple contractures and the causes, genetics, specific symptoms, and severity of these disorders vary dramatically. Over 350 genes have been identified as responsible for different types of arthrogryposis.
The most common universal symptom of arthrogryposis multiplex congenita is limited or absent movement around small and large joints (contractures). The contractures are present at birth (congenital). The muscles of the affected limbs may be underdeveloped (hypoplastic), resulting in a tube-shaped limb with a soft, doughy feeling. Soft tissue webbing may develop over the affected joints.
In addition to joint abnormalities, other findings occur with greater frequency in individuals with arthrogryposis multiplex congenita. These include abnormally slender and fragile long bones of the arms and legs and cleft palate, a condition in which the roof of the mouth fails to fuse together leaving a groove across the top of the mouth. In males, the testes may fail to descend into the scrotum (cryptorchidism). Intelligence may or may not be affected. Approximately one-third of individuals with arthrogryposis multiplex congenita may have structural or functional abnormalities of the central nervous system.
Additional symptoms associated with arthrogryposis multiplex congenita are related to the underlying disorder that causes the condition in each individual. The specific symptoms and their severity can vary dramatically based upon the underlying cause. Two of the most common forms of arthrogryposis multiplex congenita are Amyoplasia and a group of genetic disorders called the Distal Arthrogryposes.
Arthrogryposis multiplex congenita diagnosis
A diagnosis of arthrogryposis multiplex congenita is made based upon identification of characteristic symptoms (e.g., multiple congenital contractures), a detailed patient history, and a thorough clinical evaluation. Certain tests may be necessary to determine the underlying cause of arthrogryposis multiplex congenita including nerve conduction, electromyography and muscle biopsy, which can help diagnose neuropathic or myopathic disorders. A nerve conduction study measures how rapidly nerves carry an electrical impulse. An electromyography is a test that records electrical activity in skeletal voluntary muscles at rest and during muscle contraction. A biopsy is a procedure in which a small amount of affected tissue (e.g., muscle) is removed and studied under a microscopic to detect characteristic changes or findings that can aid in obtaining a diagnosis. Imaging studies of the central nervous system (CNS) and comparative genomic hybridization array, microarray, and exome studies are also useful studies in making diagnoses.
Arthrogryposis multiplex congenita treatment
The treatment of arthrogryposis multiplex congenita is directed toward the specific findings that are apparent in each individual. Standard physical therapy, which can improve joint motion and avoid muscle atrophy in the newborn period is beneficial. Gentle joint manipulation and stretching exercises may also be beneficial. Removable splints for the knees and feet that permit regular muscle movement and exercise are also recommended.
In some cases, surgery may be necessary to achieve better positioning and increase the range of motion in certain joints, especially the ankles, knees, hips, elbows, or wrists. In rare cases, tendon transfers have been performed to improve muscle function. Tendons are the tissue by which muscle is attached to bone.
Genetic counseling may be of benefit for affected individuals and their families. Other treatment is symptomatic and supportive.
References [ + ]