Contents
What is bradycardia
Bradycardia is a slower than normal heart rate, usually at a rate under 60 beats per minute (normal adult resting heart rate is between 60 to 100 beats per minute). If you have bradycardia, your heart beats fewer than 60 times a minute.
What’s too slow for you may depend on your age and physical condition.
- Physically active adults (and athletes) often have a resting heart rate slower than 60 beats per minute but it doesn’t cause problems and is normal for them.
- Your heart rate may fall below 60 beats per minute during deep sleep.
- Elderly people are more prone to problems with a slow heart rate.
There are two basic types of bradycardia:
- Sick sinus syndrome occurs when the sinus node (the heart’s own pacemaker) fails and does not reliably trigger heartbeats. This is very common in elderly persons, but may occur at any age.
- Heart block is a complete or partial interruption of the electrical impulses on their way to the ventricles and results in a slow, unreliable heartbeat. Heart block may be present at birth, may result from other types of heart disease (after a heart attack for example), or may be due to age-related wear and tear on the heart’s electrical system.
Bradycardia can be a serious problem if the heart doesn’t pump enough oxygen-rich blood to the body. For some people, however, bradycardia doesn’t cause symptoms or complications. Thresholds for different age, gender, and patient populations exist.
Symptoms of bradycardia
A heart rhythm that’s too slow can cause insufficient blood flow to the brain with symptoms such as:
- Fatigue or feeling tired or weak
- Dizziness or lightheadedness
- Confusion
- Fainting or near-fainting spells
- Some people may feel short of breathe
- Feeling like it’s hard to exercise
- In extreme cases, cardiac arrest may occur.
Treatment of bradycardia depends on the underlying medical cause:
- Treatment is not usually needed except with prolonged or repeated symptoms
- Can usually be corrected with an artificial pacemaker to speed up the heart rhythm as needed. An implanted pacemaker can correct bradycardia and help your heart maintain an appropriate rate.
- Some medications can cause a slow heartbeat, in this case, medication may be adjusted.
If you have a heart rate under 60, and you’re aren’t exceptionally fit, it’s important to see your doctor. It might help to make a note of the times you notice your heart is slow, and how you’re feeling at the time.
A number of conditions can cause signs and symptoms of bradycardia. It’s important to get a prompt, accurate diagnosis and appropriate care. See your doctor if you or your child has symptoms of bradycardia.
If you faint, have difficulty breathing or have chest pain lasting more than a few minutes, get emergency care or call your local emergency number. Seek emergency care for anyone with these symptoms.
What is sinus bradycardia
Sinus bradycardia is a sinus rhythm with a heart rate that is lower than normal. A resting heart rate slower than 60 beats a minute is normal for some people, particularly healthy young adults and trained athletes. For them, bradycardia isn’t considered a health problem.
People who have a sinus bradycardia because they are physically fit won’t need any treatment.
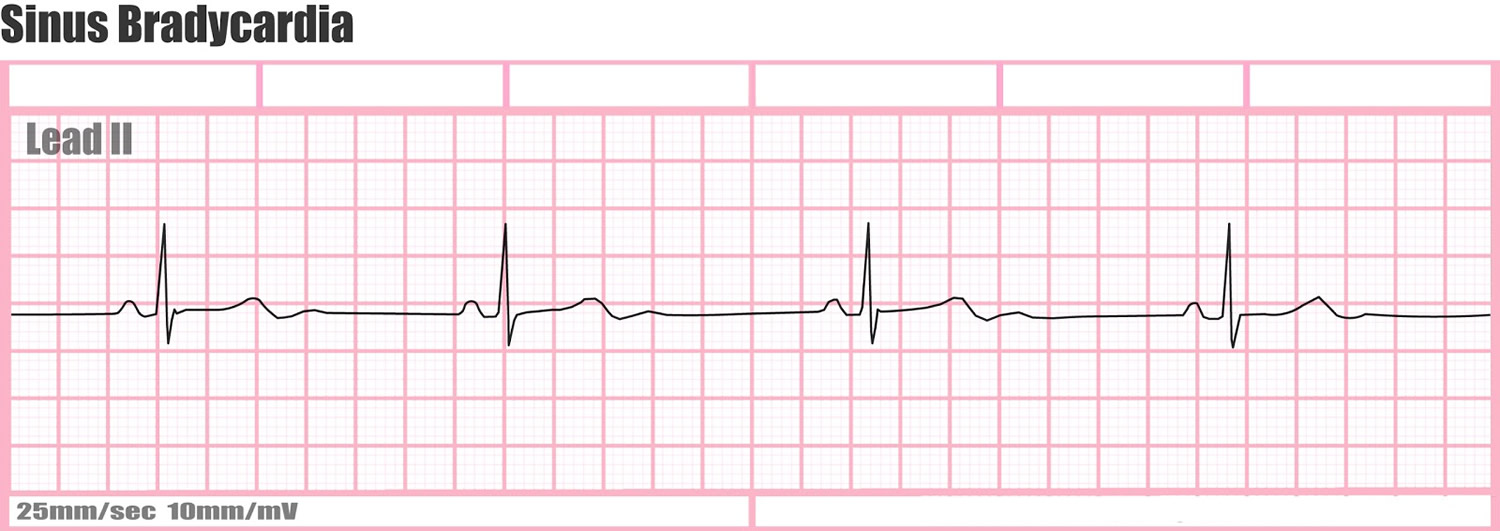
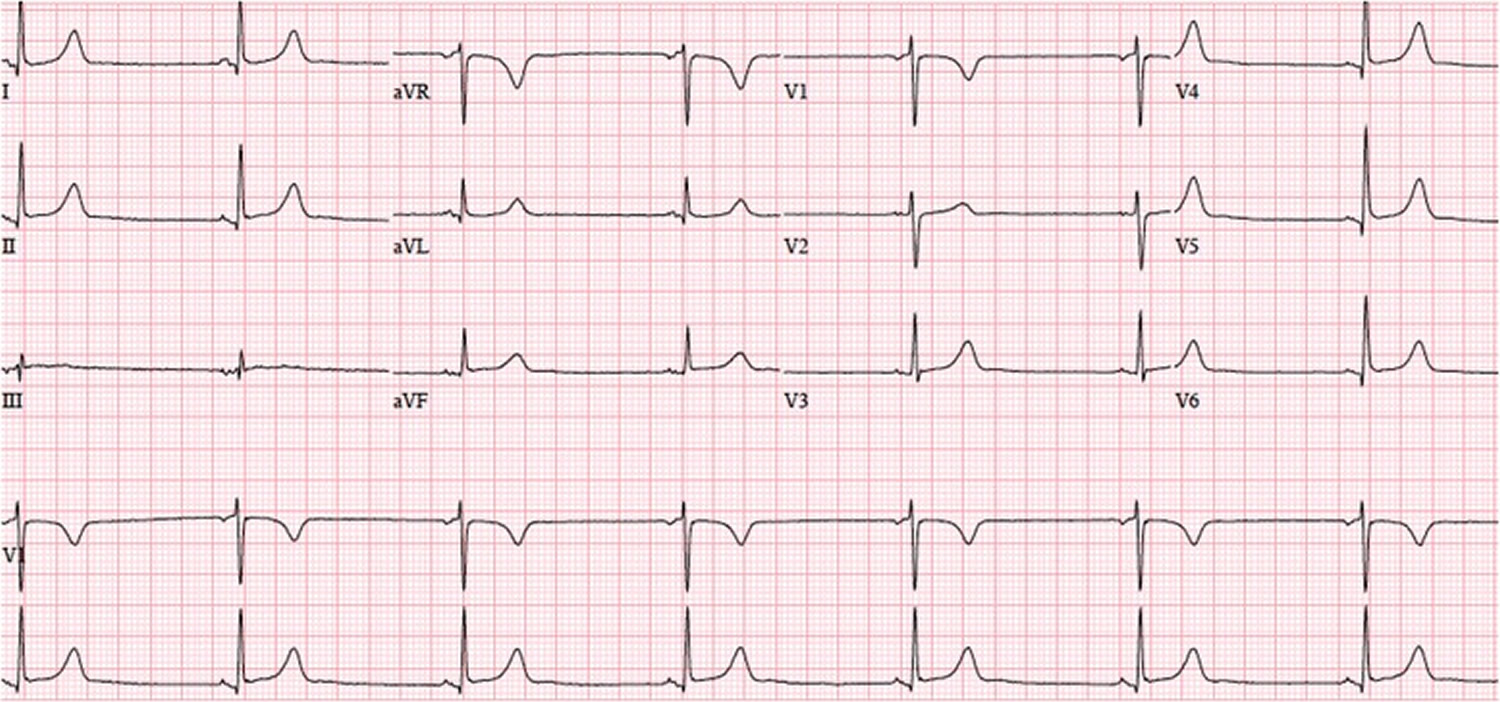
Sinus bradycardia ECG characteristics:
- Rate: Less than 60 beats per minute.
- Rhythm: Regular.
- P waves: Upright, consistent, and normal in morphology and duration.
- P-R Interval: Between 0.12 and 0.20 seconds in duration.
- QRS Complex: Less than 0.12 seconds in width, and consistent in morphology.
Normal physiological causes of sinus bradycardia
Sinus bradycardia is considered a normal finding in the following circumstances:
- Healthy young adults
- Well trained athletes due to highly efficient left ventricle capable of generating sufficient cardiac output at low heart rates.
- During vagal maneuvers (valsalva maneuver, carotid sinus stimulation)
- During sleep.
Abnormal (pathological) causes of sinus bradycardia
There are numerous pathological conditions that cause sinus bradycardia. The most important causes as follows:
- During a vasovagal syncope
- Myocardial ischemia/myocardial infarction (heart attack) – particularly myocardial ischemia/myocardial infarction involving the inferior wall of the left ventricle. This type of bradycardia is due to diminished automaticity (pacemaker function) in the sinoatrial (SA) node or conduction defects (e.g. second degree atrioventricular heart block)
- Sinus node dysfunction
- Side effects of drugs notably beta blockers, digitalis, verapamil, diltiazem, clonidine and amiodarone
- Increased intracranial pressure
- Hypothyroidism (under active thyroid gland)
- Hyperkalemia (high blood potassium levels)
- Hypothermia
Figure 1. Sinus bradycardia ECG (~42 beats per minute)
Electrical circuitry of the heart
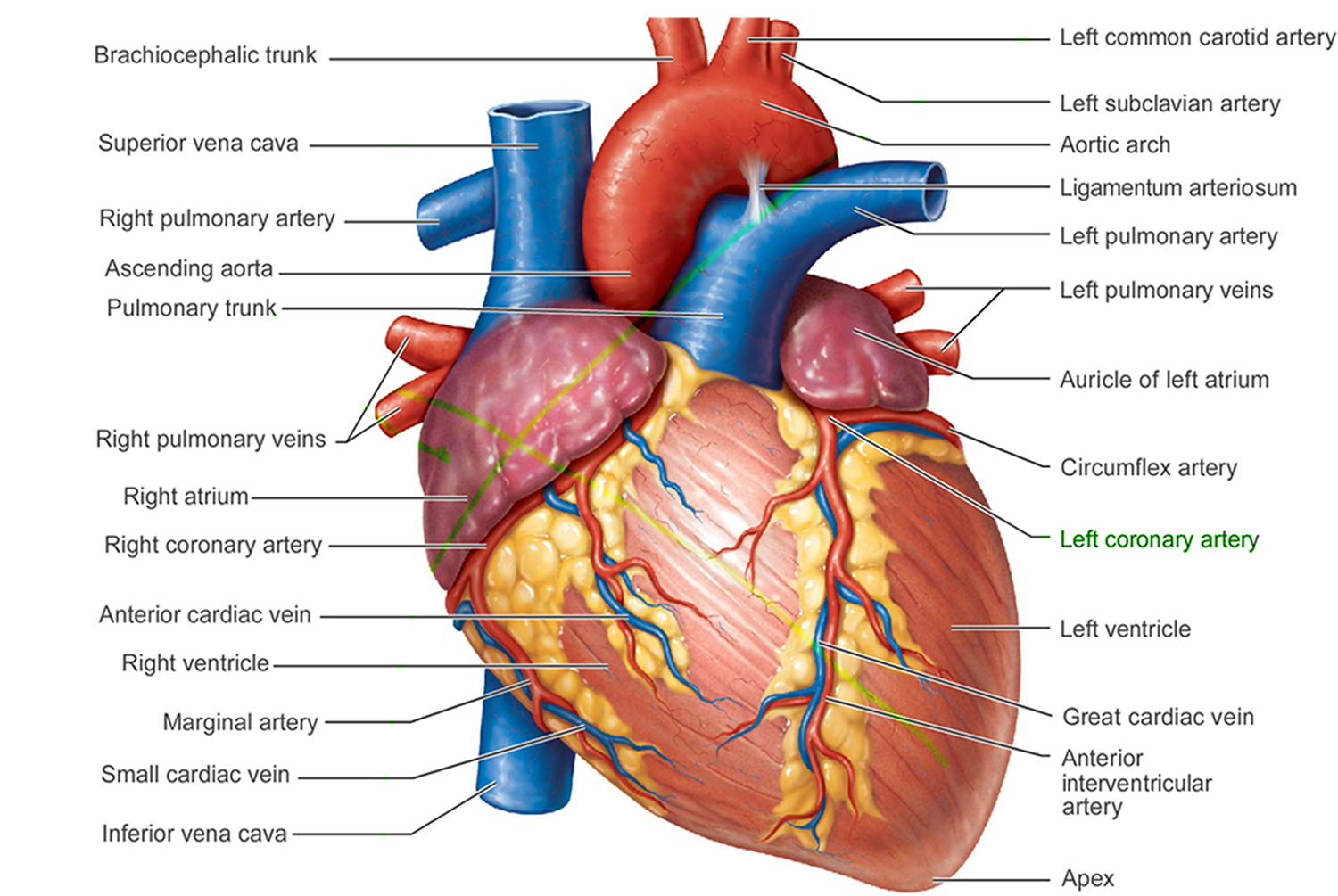
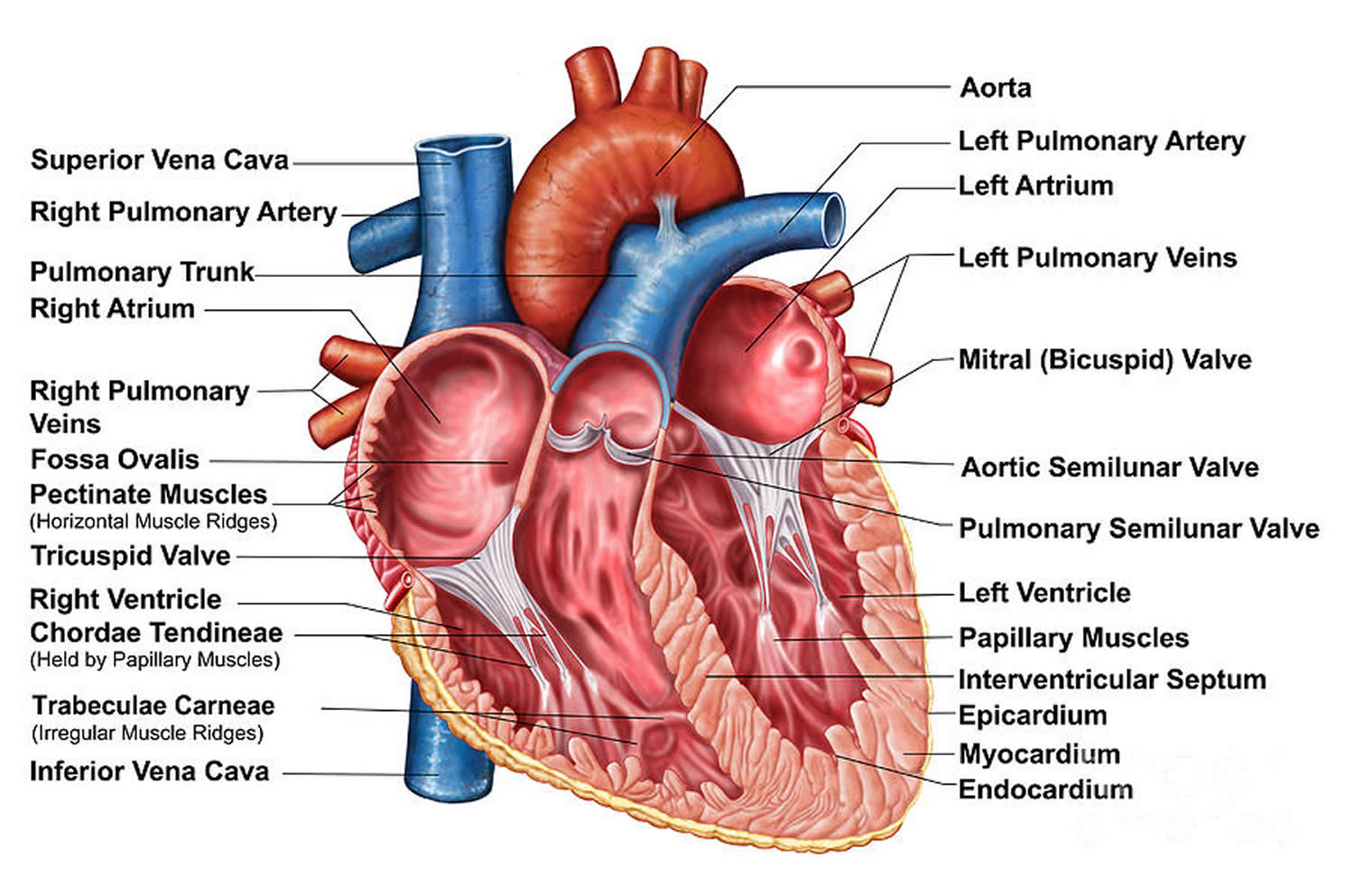
Your heart comprises four chambers — two upper (atria) and two lower (ventricles). A natural pacemaker (the sinus node), situated in the right atrium, normally controls your heart rhythm by producing electrical impulses that initiate each heartbeat.
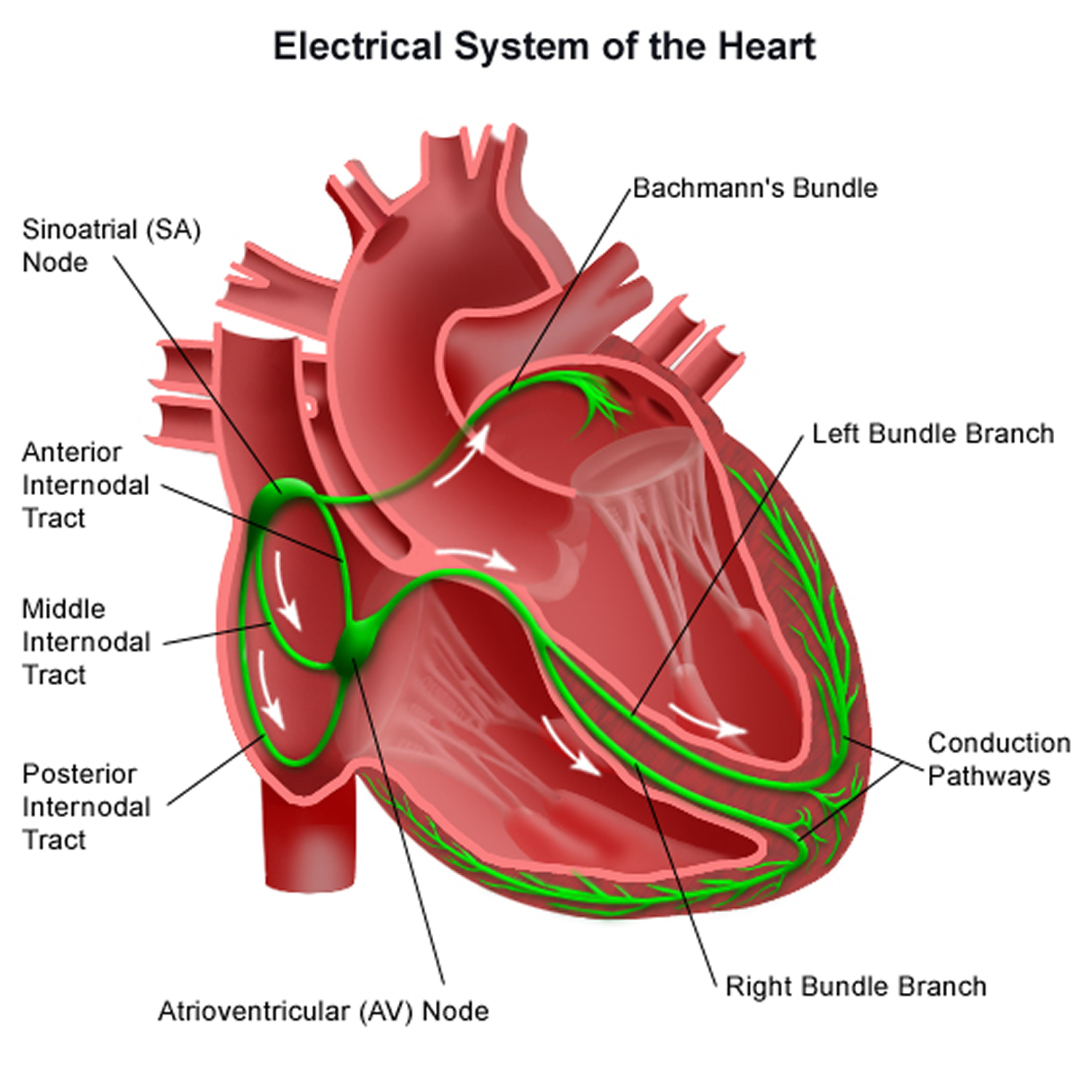
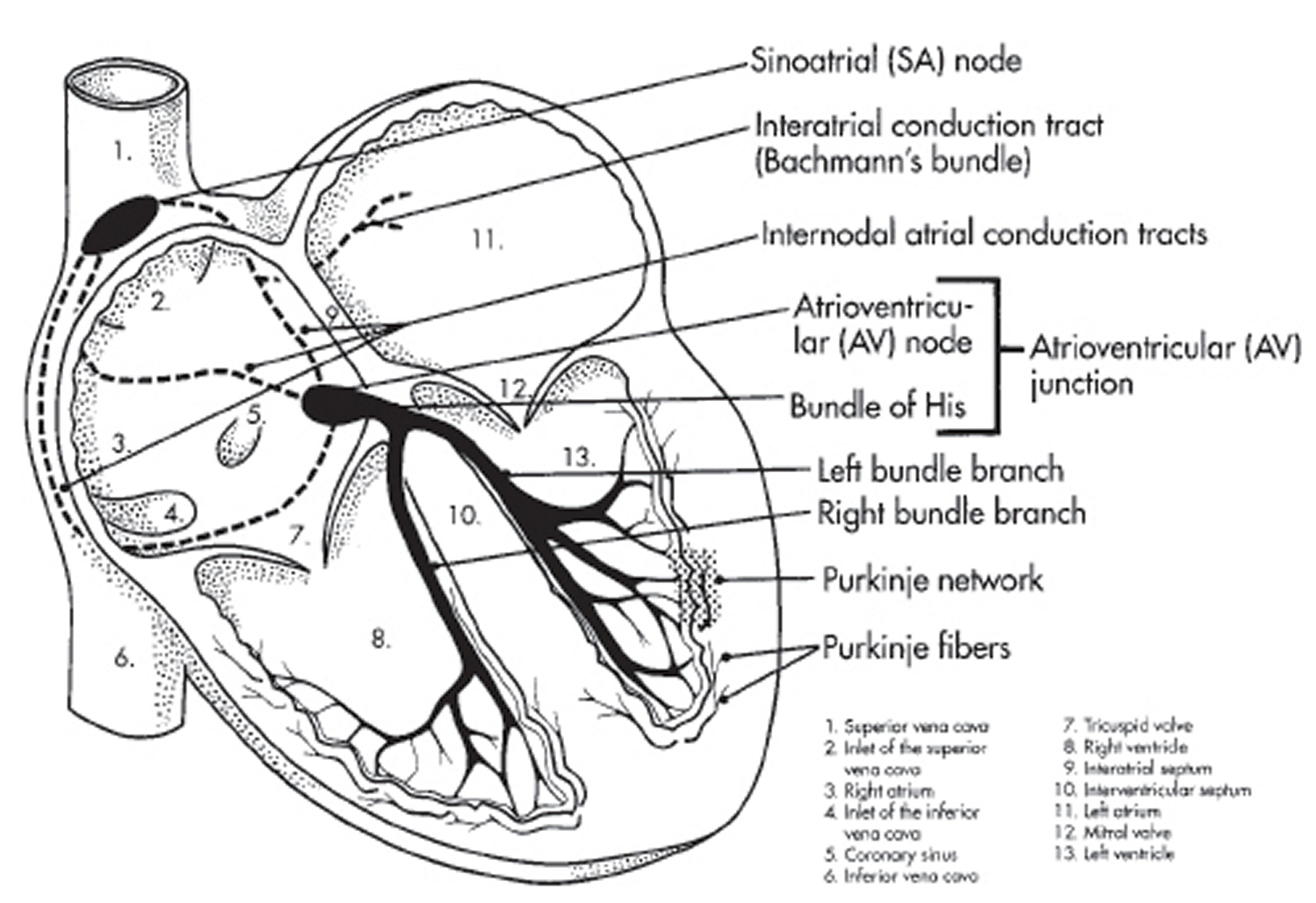
These electrical impulses travel across the atria, causing them to contract and pump blood into the ventricles. Then these impulses arrive at a cluster of cells called the atrioventricular (AV) node.
The AV node transmits the signal to a collection of cells called the bundle of His. These cells transmit the signal down a left branch serving the left ventricle and a right branch serving the right ventricle, which causes the ventricles to contract and pump blood — the right ventricle sending oxygen-poor blood to the lungs and the left ventricle sending oxygen-rich blood to the body.
Bradycardia occurs when electrical signals slow down or are blocked.
Figure 2. The anatomy of the heart
Figure 4. The heart’s electrical system
 Junctional bradycardia
Junctional bradycardia
Junctional bradycardia involves cardiac rhythms that arise from the atrioventricular (AV) junction at a heart rate of less than 60 beats/min 1. In patients with retrograde atrioventricular nodal conduction, a retrograde P wave can be accompanied with junctional bradycardia. The event occurs as enhanced automaticity or as an escape rhythm during significant bradycardia with rates slower than the intrinsic junctional pacemaker 2. Junctional bradycardia can appear in patients with sick sinus syndrome or those with significant bradycardia that allows the atrioventricular nodal region to determine the heart rate 3. As most of these patients are asymptomatic, there are no specific guidelines for evaluation and treatment. However, since there is no physiologic atrial contraction in junctional bradycardia, Junctional bradycardia may be a potential cause of cardioembolic source 4.
This study 1, junctional bradycardia was found to be potentially associated with the occurrence of a composite of thromboembolic events. Junctional bradycardia without a retrograde P wave was also shown to be a significant risk factor for both the occurrence of stroke and the composite of thromboembolic events. However, the main pathogenic mechanism for thromboembolic events is not well understood 1. Additionally, in the same study, left atrial volume index (LAVI) was significantly larger in the junctional bradycardia group (45 ml/m2 vs. 28 ml/m2) than in the control group. Thus, in the junctional bradycardia group, large left atrial volume index could be associated with loss of atrial kick, which might contribute to increased preload of the left atrium 1.
When patients with junctional bradycardia have co-morbidities that are known risk factors for embolic events, preventive strategies, such as anticoagulant administration or pacemaker implantation, might be considered. However, a randomized controlled study with a large population is also needed to confirm these findings.
Bradycardia causes
What causes bradycardia
Bradycardia can be caused by:
- Heart tissue damage related to aging
- Problems with the sinoatrial (SA) node, sometimes called the heart’s natural pacemaker
- Problems in the conduction pathways of the heart (electrical impulses are not conducted from the atria to the ventricles)
- Damage to heart tissues from heart disease or heart attack (myocardial infarction or MI)
- Heart disorder present at birth (congenital heart defect)
- Infection of heart tissue (myocarditis)
- A complication of heart surgery
- Underactive thyroid gland (hypothyroidism)
- Imbalance of chemicals in the blood, such as potassium or calcium
- Repeated disruption of breathing during sleep (obstructive sleep apnea)
- Inflammatory disease, such as rheumatic fever or lupus
- Medications, including some drugs for other heart rhythm disorders, high blood pressure and psychosis
Sinus node problems
Bradycardia often starts in the sinoatrial (SA) node. A slow heart rate might occur because the sinus node:
- Discharges electrical impulses slower than is normal
- Pauses or fails to discharge at a regular rate
- Discharges an electrical impulse that’s blocked before causing the atria to contract
In some people, the sinus node problems result in alternating slow and fast heart rates (bradycardia-tachycardia syndrome).
Heart block (atrioventricular block)
Bradycardia can also occur because electrical signals transmitted through the atria aren’t transmitted to the ventricles (heart block, or atrioventricular block).
Heart blocks are classified based on the degree to which signals from the atria reach your heart’s main pumping chambers (ventricles).
- First-degree heart block. In the mildest form, all electrical signals from the atria reach the ventricles, but the signal is slowed. First-degree heart block rarely causes symptoms and usually needs no treatment if there’s no other abnormality in electrical signal conduction.
- Second-degree heart block. Not all electrical signals reach the ventricles. Some beats are “dropped,” resulting in a slower and sometimes irregular rhythm.
- Third-degree (complete) heart block. None of the electrical impulses from the atria reaches the ventricles. When this happens, a natural pacemaker takes over, but this results in slow and sometimes unreliable electrical impulses to control the beat of the ventricles.
Risk factors for bradycardia
Age
A key risk factor for bradycardia is age. Heart problems, which are often associated with bradycardia, are more common in older adults.
Risk factors related to heart disease
Bradycardia is often associated with damage to heart tissue from some type of heart disease.
Therefore, factors that increase your risk of heart disease can also increase the risk of bradycardia. Lifestyle changes or medical treatment might decrease the risk of heart disease associated with the following factors:
- High blood pressure
- Smoking
- Heavy alcohol use
- Recreational drug use
- Psychological stress or anxiety
Bradycardia prevention
The most effective way to prevent bradycardia is to reduce your risk of developing heart disease. If you already have heart disease, monitor it and follow your treatment plan to lower your risk of bradycardia.
Prevent heart disease
Treat or eliminate risk factors that may lead to heart disease. Take the following steps:
- Exercise and eat a healthy diet. Live a heart-healthy lifestyle by exercising regularly and eating a healthy, low-fat, low-salt, low-sugar diet that’s rich in fruits, vegetables and whole grains.
- Maintain a healthy weight. Being overweight increases your risk of developing heart disease.
- Keep blood pressure and cholesterol under control. Make lifestyle changes and take medications as prescribed to correct high blood pressure (hypertension) or high cholesterol.
- Don’t smoke. If you smoke and can’t quit on your own, talk to your doctor about strategies or programs to help you break a smoking habit.
- If you drink, do so in moderation. For healthy adults, that means up to one drink a day for women of all ages and men older than age 65, and up to two drinks a day for men age 65 and younger. Ask your doctor if your condition means you should avoid alcohol. If you can’t control your alcohol use, talk to your doctor about a program to quit drinking and manage other behaviors related to alcohol abuse.
- Don’t use recreational drugs. Talk to your doctor about an appropriate program for you if you need help ending recreational drug use.
- Manage stress. Avoid unnecessary stress and learn coping techniques to handle normal stress in a healthy way.
- Go to scheduled checkups. Have regular physical exams and report signs or symptoms to your doctor.
Monitor and treat existing heart disease
If you already have heart disease, there are steps you can take to lower your risk of developing bradycardia or another heart rhythm disorder:
- Follow the plan. Be sure you understand your treatment plan, and take all medications as prescribed.
- Report changes immediately. If your symptoms change or worsen or you develop new symptoms, tell your doctor immediately.
Bradycardia complications
Prolonged untreated bradycardia possible complications can include:
- Frequent fainting spells or syncope (loss of consciousness; fainting)
- Inability of the heart to pump enough blood (heart failure)
- Angina pectoris (chest pain)
- Low blood pressure or hypotension
- High blood pressure or hypertension
- Sudden cardiac arrest or sudden death
Bradycardia symptoms
If you have bradycardia, your brain and other organs might not get enough oxygen, possibly causing these symptoms:
- Near-fainting (pre-syncope) or fainting (syncope)
- Dizziness or lightheadedness
- Fatigue
- Shortness of breath
- Chest pains
- Confusion or memory problems
- Easily tiring during physical activity
Bradycardia diagnosis
To diagnose your condition, your doctor will review your symptoms and your medical and family medical history and do a physical examination.
Your doctor will also order tests to measure your heart rate, establish a link between a slow heart rate and your symptoms, and identify conditions that might be causing bradycardia.
Electrocardiogram (ECG or EKG)
An electrocardiogram, also called an ECG or EKG, is a primary tool for evaluating bradycardia. Using small sensors (electrodes) attached to your chest and arms, it records electrical signals as they travel through your heart.
Because an ECG can’t record bradycardia unless it happens during the test, your doctor might have you use a portable ECG device at home. These devices include:
- Holter monitor. Carried in your pocket or worn on a belt or shoulder strap, this device records your heart’s activity for 24 to 48 hours. Your doctor will likely ask you to keep a diary during the same 24 hours. You’ll describe any symptoms you experience and record the time they occur.
- Event recorder. This device monitors your heart activity over a few weeks. You push a button to activate it when you feel symptoms so that it records your heart’s activity during that time.
Your doctor might use an ECG monitor while performing other tests to understand the impact of bradycardia. These tests include:
- Tilt table test. This test helps your doctor better understand how your bradycardia contributes to fainting spells. You lie flat on a special table, and then the table is tilted as if you were standing up to see if the change in position causes you to faint.
- Exercise test. Your doctor might monitor your heart rate while you walk on a treadmill or ride a stationary bike to see whether your heart rate increases appropriately in response to physical activity.
Laboratory and other tests
Your doctor will order blood tests to screen for conditions that might be contributing to bradycardia, such as an infection, hypothyroidism or an electrolyte imbalance.
If sleep apnea is suspected of contributing to bradycardia, you might undergo tests to monitor your sleep.
Bradycardia treatment
Treatment for bradycardia depends on the type of electrical conduction problem, the severity of symptoms and the cause of your slow heart rate. If you have no symptoms, treatment might not be necessary.
Treating underlying disorders
If a disorder such as hypothyroidism or obstructive sleep apnea is causing bradycardia, treatment of the disorder might correct bradycardia.
Change in medications
A number of medications, including some to treat other heart conditions, can cause bradycardia.
Your doctor will check what medications you’re taking and possibly recommend alternatives. Changing drugs or lowering dosages might correct problems with a slow heart rate.
When other treatments aren’t possible and symptoms require treatment, a pacemaker is necessary.
Implantable Cardiac Pacemaker
This battery-operated device about the size of a cellphone is implanted under your collarbone. Wires from the device are threaded through veins and into your heart. Electrodes at the end of the wires are attached to heart tissues. The pacemaker monitors your heart rate and generates electrical impulses as necessary to maintain an appropriate rate.
A wireless pacemaker has been approved by the FDA. The leadless system holds promise for people who need pacing in only one ventricle, but more study is needed.
- Kim GS, Uhm J-S, Kim T-H, et al. Junctional bradycardia is a potential risk factor of stroke. BMC Neurology. 2016;16:113. doi:10.1186/s12883-016-0645-9. https://www.ncbi.nlm.nih.gov/pmc/articles/PMC4959053/[↩][↩][↩][↩]
- Josephson M. Clinical Cardiac Electrophysiology. 4th ed. Philadelphia: Lippincott Williams and Wilkins; 2008.[↩]
- Libby P, Bonow R, Mann D, Zipes. Specific arrhythmias: diagnosis and treatment. In: A Textbook of Cardiovascular Medicine. 8th ed. Philadelphia: Saunders; 2007. p. 640–5.[↩]
- Fairfax AJ, Lambert CD, Leatham A. Systemic embolism in chronic sinoatrial disorder. N Engl J Med. 1976;295:190–192. doi: 10.1056/NEJM197607222950403. https://www.ncbi.nlm.nih.gov/pubmed/1272348[↩]