Contents
- What is broken ankle
- Ankle Anatomy
- Complications of a broken ankle
- Broken ankle cause
- Prevention of broken ankle or broken foot
- Broken ankle symptoms
- Broken ankle diagnosis
- Broken ankle treatment
- Broken ankle Recovery
- Broken ankle Pain Management
- Broken ankle Rehabilitation
- Broken ankle Weightbearing
- Broken ankle Supports
- Complications of Broken ankle
- Nonsurgical Treatment
- Surgical Treatment
- Broken ankle Outcomes
- Broken vs Sprained ankle
- Stress fracture ankle and foot
What is broken ankle
A broken ankle is also known as an ankle “fracture.” This means that one or more of the bones that make up the ankle joint are broken.
A fractured ankle can range from a simple break in one bone, which may not stop you from walking, to several fractures, which forces your ankle out of place and may require that you not put weight on it for a few months.
Simply put, the more bones that are broken, the more unstable the ankle becomes. There may be ligaments damaged as well. The ligaments of the ankle hold the ankle bones and joint in position.
Broken ankles affect people of all ages. During the past 30 to 40 years, doctors have noted an increase in the number and severity of broken ankles, due in part to an active, older population of “baby boomers.”
The seriousness of a broken ankle or broken foot varies. Fractures can range from tiny cracks in your bones to breaks that pierce your skin.
Treatment for a broken ankle or broken foot depends on the exact site and severity of the fracture. A severely broken ankle or broken foot may require surgery to implant plates, rods or screws into the broken bone to maintain proper position during healing.
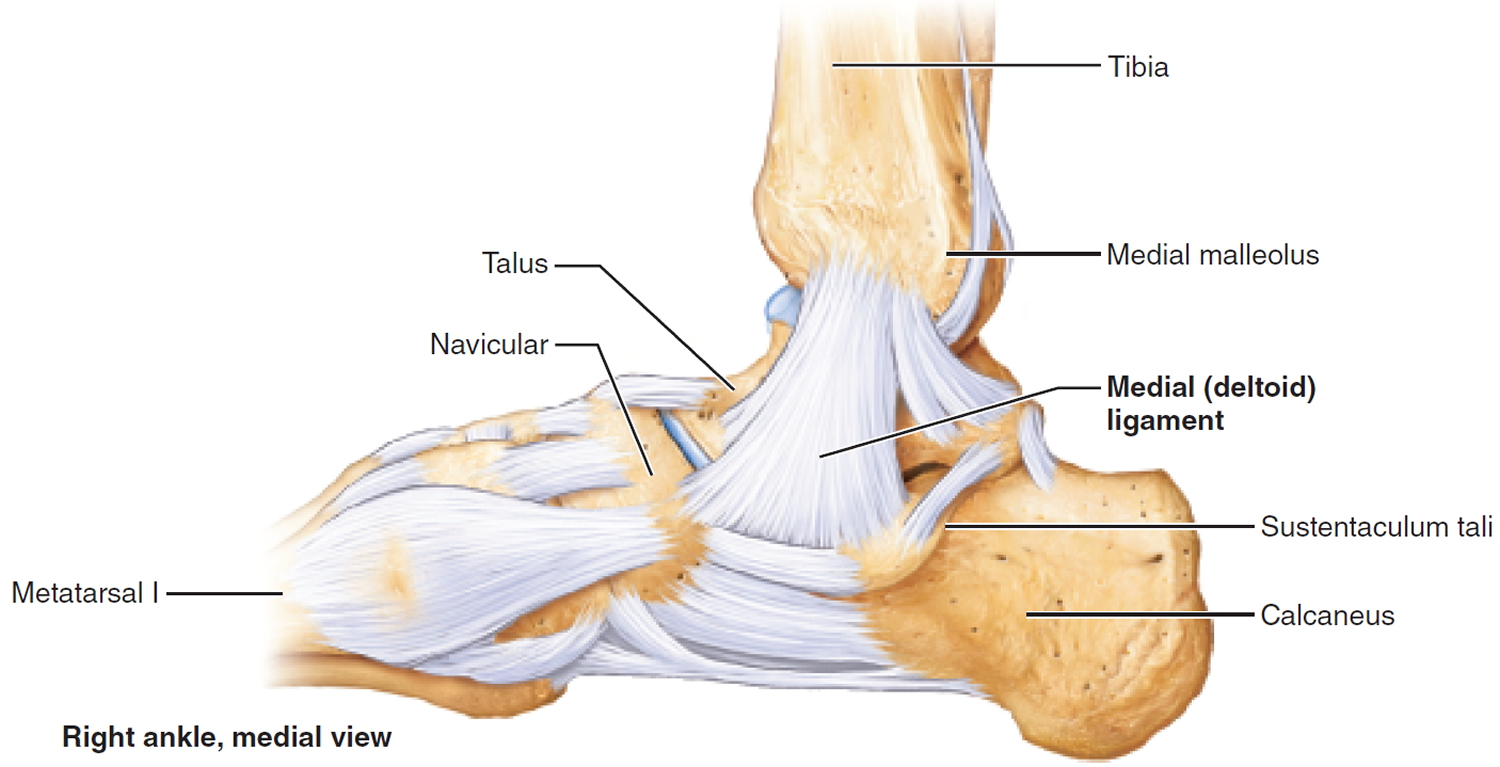
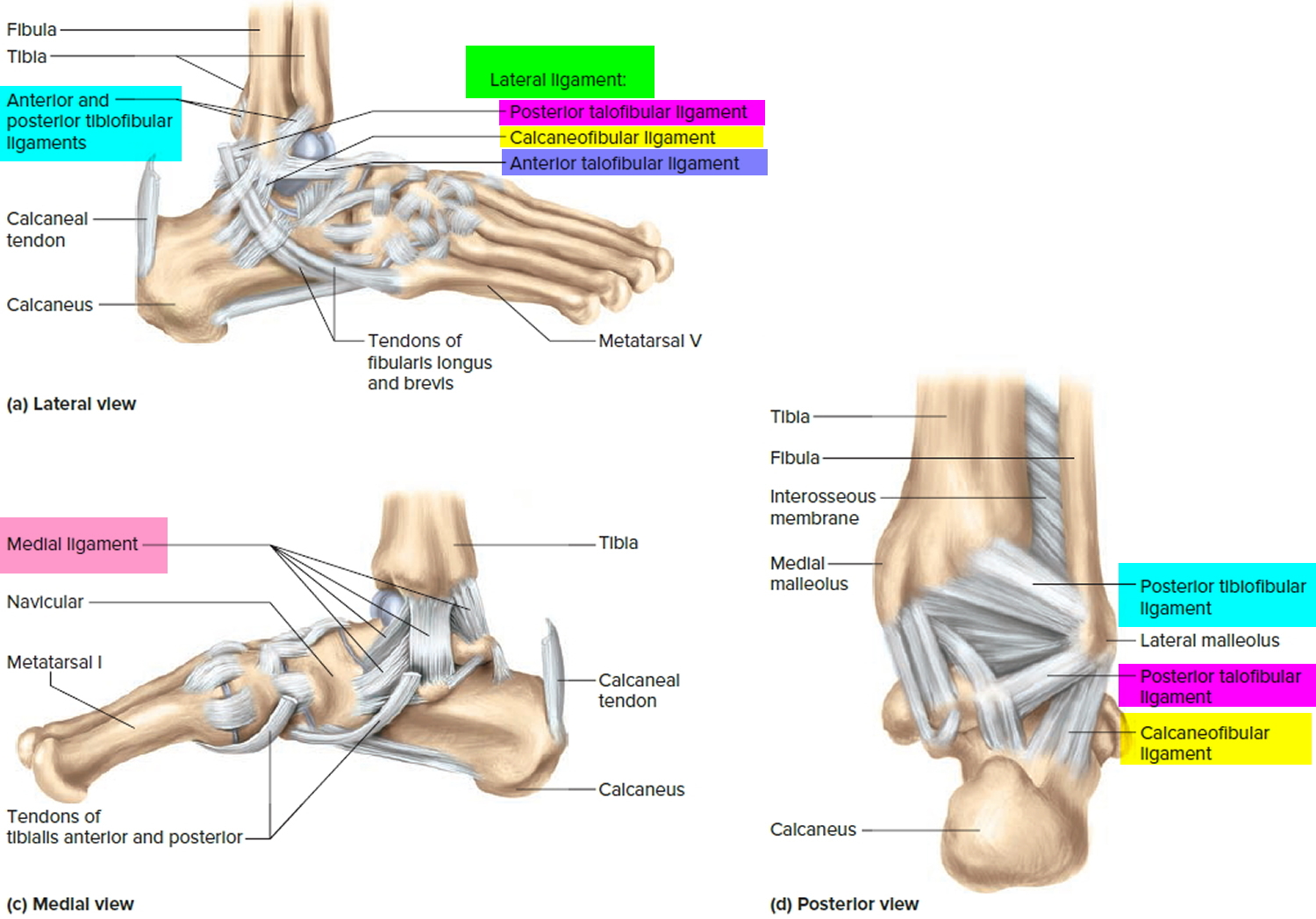
Ankle Anatomy
Three bones make up the ankle joint:
- Tibia – shinbone
- Fibula – smaller bone of the lower leg
- Talus – a small bone that sits between the heel bone (calcaneus) and the tibia and fibula
The tibia and fibula have specific parts that make up the ankle:
- Medial malleolus – inside part of the tibia
- Posterior malleolus – back part of the tibia
- Lateral malleolus – end of the fibula
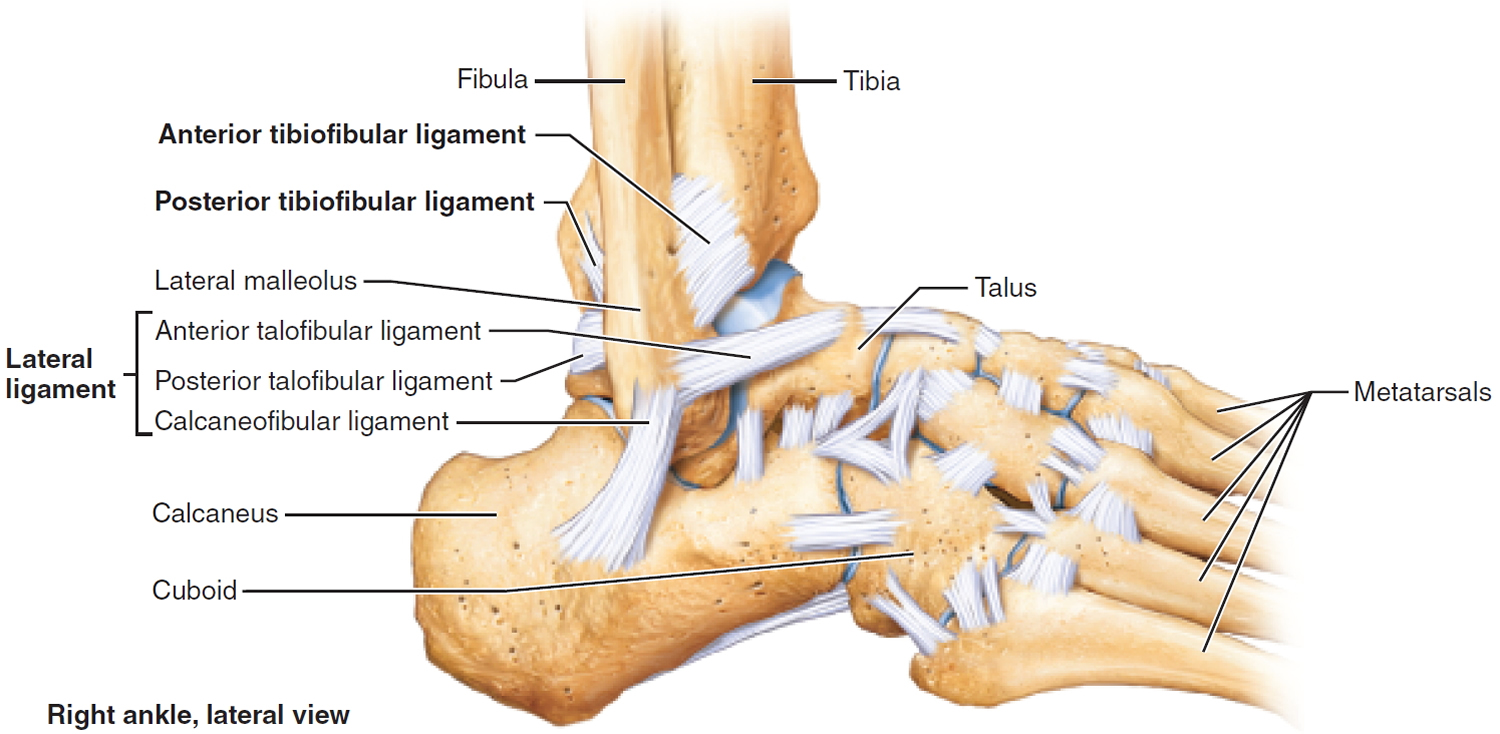
Figure 1. Ankle bones
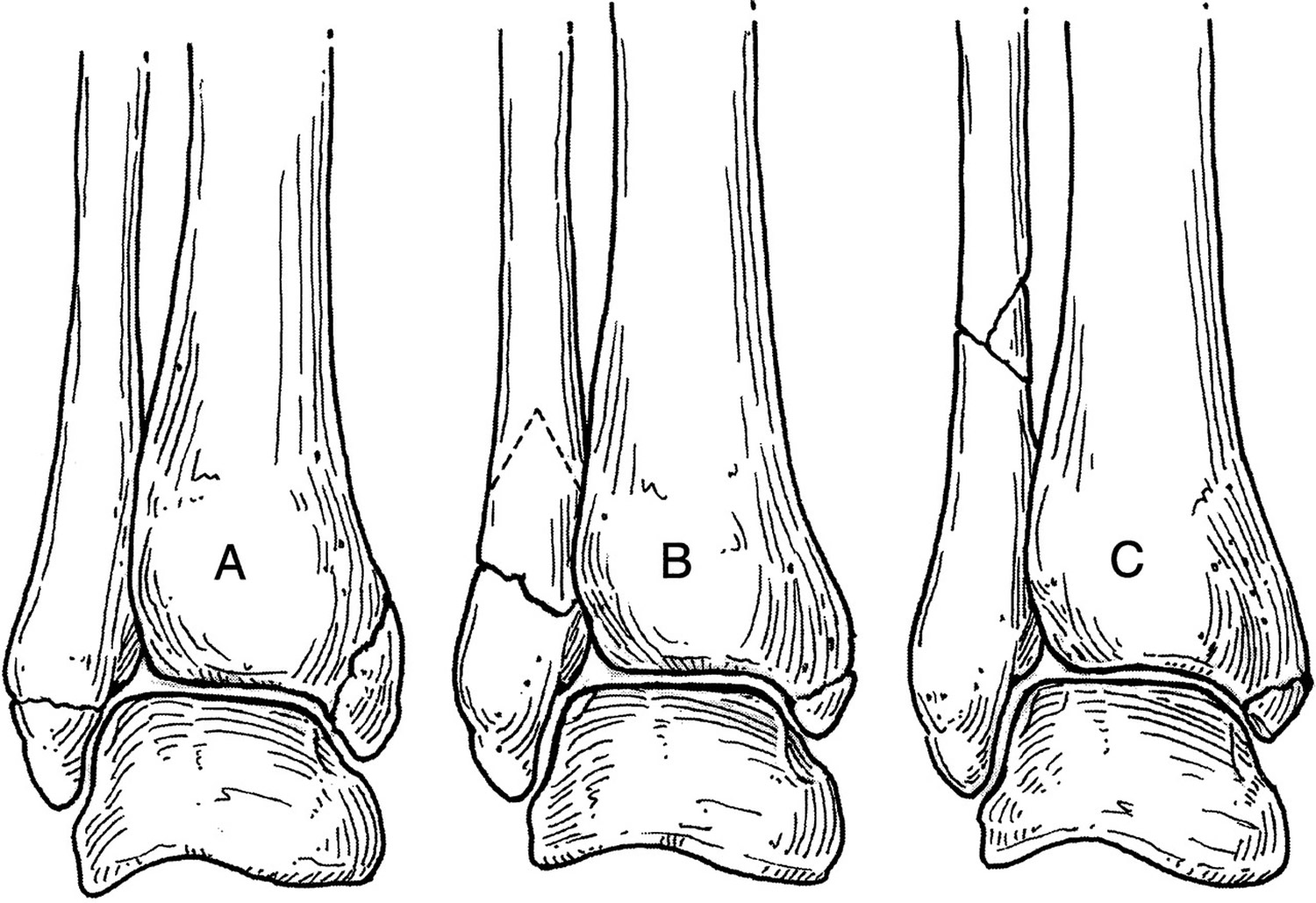
Doctors classify ankle fractures according to the area of bone that is broken. For example, a fracture at the end of the fibula is called a lateral malleolus fracture, or if both the tibia and fibula are broken, it is called a bimalleolar fracture.
Two joints are involved in ankle fractures:
- Ankle joint – where the tibia, fibula, and talus meet
- Syndesmosis joint – the joint between the tibia and fibula, which is held together by ligaments
Multiple ligaments help make the ankle joint stable.
Complications of a broken ankle
Complications of a broken ankle or broken foot are uncommon but may include:
- Arthritis. Fractures that extend into the joint can cause arthritis years later. If your ankle or foot starts to hurt long after a break, see your doctor for an evaluation.
- Bone infection (osteomyelitis). If you have an open fracture, meaning one end of the bone protrudes through the skin, your bone may be exposed to bacteria that cause infection.
- Compartment syndrome. This condition can rarely occur with ankle fractures. It causes pain, swelling and sometimes disability in affected muscles of the legs or arms.
- Nerve or blood vessel damage. Trauma to the foot or ankle can injure adjacent nerves and blood vessels, sometimes actually tearing them. Seek immediate attention if you notice any numbness or circulation problems. Lack of blood flow can cause a bone to die and collapse.
Broken ankle cause
- Twisting or rotating your ankle
- Rolling your ankle
- Tripping or falling. Tripping and falling can break bones in your ankles or feet, as can landing on your feet after jumping down from just a slight height.
- Impact during a car accident. The crushing injuries common in car accidents may cause breaks that require surgical repair.
- Impact from a heavy weight. Dropping something heavy on your foot is a common cause of fractures.
- Missteps. Sometimes just putting your foot down wrong can result in a broken bone. A toe can get broken from stubbing your toes on furniture. Twisting your ankle just right can cause a sprain or a broken bone.
- Overuse. Stress fractures are common in the weight-bearing bones of your ankles or feet. These tiny cracks are usually caused over time by repetitive force or overuse, such as running long distances. But they can also occur with normal use of a bone that’s been weakened by a condition such as osteoporosis or a stress fracture.
Risk factors for broken ankle
You may be at higher risk of a broken foot or ankle if you:
- Participate in high-impact sports. The stresses, direct blows and twisting injuries that occur in sports such as basketball, football, gymnastics, tennis and soccer are causes of foot and ankle fractures.
- Use improper technique or sports equipment. Faulty equipment, such as shoes that are too worn or not properly fitted, can contribute to stress fractures and falls. Improper training techniques, such as not warming up and stretching, also can cause foot and ankle injuries.
- Suddenly increase your activity level. Whether you’re a trained athlete or someone who’s just started exercising, suddenly boosting the frequency or duration of your exercise sessions can increase your risk of a stress fracture.
- Work in certain occupations. Certain work environments, such as a construction site, put you at risk of falling from a height or dropping something heavy on your foot.
- Keep your home cluttered or poorly lit. Walking around in a house with too much clutter or too little light may lead to falls and foot and ankle injuries.
- Have certain conditions. Having decreased bone density (osteoporosis) can put you at risk of injuries to your foot and ankle bones.
Prevention of broken ankle or broken foot
These basic sports and safety tips may help prevent a broken ankle or broken foot:
- Wear proper shoes. Use hiking shoes on rough terrain. Wear steel-toed boots in your work environment if necessary. Choose appropriate athletic shoes for your sport.
- Replace athletic shoes regularly. Discard sneakers as soon as the tread or heel wears out or if the shoes are wearing unevenly. If you’re a runner, replace your sneakers every 300 to 400 miles.
- Start slowly. That applies to a new fitness program and each individual workout.
- Cross-train. Alternating activities can prevent stress fractures. Rotate running with swimming or biking.
- Build bone strength. Calcium-rich foods, such as milk, yogurt and cheese, really can do your body good. Taking vitamin D supplements also can help.
- Use night lights. Many broken toes are the result of walking in the dark.
- Declutter your house. Keeping clutter off the floor can help you to avoid trips and falls.
- Strengthen your ankle muscles. If you are prone to twisting your ankle, ask your doctor for exercises to help strengthen the supporting muscles of your ankle.
Broken ankle symptoms
Because a severe ankle sprain can feel the same as a broken ankle, every ankle injury should be evaluated by a physician.
Common symptoms for a broken ankle include:
- Immediate and severe pain
- Pain that increases with activity and decreases with rest
- Swelling
- Bruising
- Tender to touch
- Cannot put any weight on the injured foot
- Deformity (“out of place”), particularly if the ankle joint is dislocated as well.
Broken ankle diagnosis
Medical History and Physical Examination
After discussing your medical history, symptoms, and how the injury occurred, your doctor will do a careful examination of your ankle, foot, and lower leg.
During the physical exam, your doctor will check for points of tenderness in your foot and ankle. The precise location of your pain can help determine its cause.
He or she may move your foot into different positions, to check your range of motion. You may be asked to walk for a short distance so that your doctor can examine your gait.
Imaging Tests
If your doctor suspects an ankle fracture, he or she will order additional tests to provide more information about your injury.
X-rays. X-rays are the most common and widely available diagnostic imaging technique. X-rays can show if the bone is broken and whether there is displacement (the gap between broken bones). They can also show how many pieces of broken bone there are. X-rays may be taken of the leg, ankle, and foot to make sure nothing else is injured.
Stress test. Depending on the type of ankle fracture, the doctor may put pressure on the ankle and take a special x-ray, called a stress test. This x-ray is done to see if certain ankle fractures require surgery.
Computed tomography (CT) scan. This type of scan can create a cross-section image of the ankle and is sometimes done to further evaluate the ankle injury. It is especially useful when the fracture extends into the ankle joint.
Magnetic resonance imaging (MRI) scan. These tests provide high resolution images of both bones and soft tissues, like ligaments. For some ankle fractures, an MRI scan may be done to evaluate the ankle ligaments.
Broken ankle treatment
Treatments for a broken ankle or broken foot will vary, depending on which bone has been broken and the severity of the injury.
Medications
Your doctor may recommend an over-the-counter pain reliever, such as acetaminophen (Tylenol, others).
Therapy
After your bone has healed, you’ll probably need to loosen up stiff muscles and ligaments in your ankles and feet. A physical therapist can teach you exercises to improve your flexibility and strength.
Surgical and other procedures
Reduction. If you have a displaced fracture, meaning the two ends of the fracture are not aligned, your doctor may need to manipulate the pieces back into their proper positions — a process called reduction. Depending on the amount of pain and swelling you have, you may need a muscle relaxant, a sedative or even a general anesthetic before this procedure.
Immobilization. To heal, a broken bone must be immobilized so that its ends can knit back together. In most cases, this requires a cast.
Minor foot fractures may only need a removable brace, boot or shoe with a stiff sole. A fractured toe is usually taped to a neighboring toe, with a piece of gauze between them.
Surgery. In some cases, an orthopedic surgeon may need to use pins, plates or screws to maintain proper position of your bones during healing. These materials may be removed after the fracture has healed if they are prominent or painful.
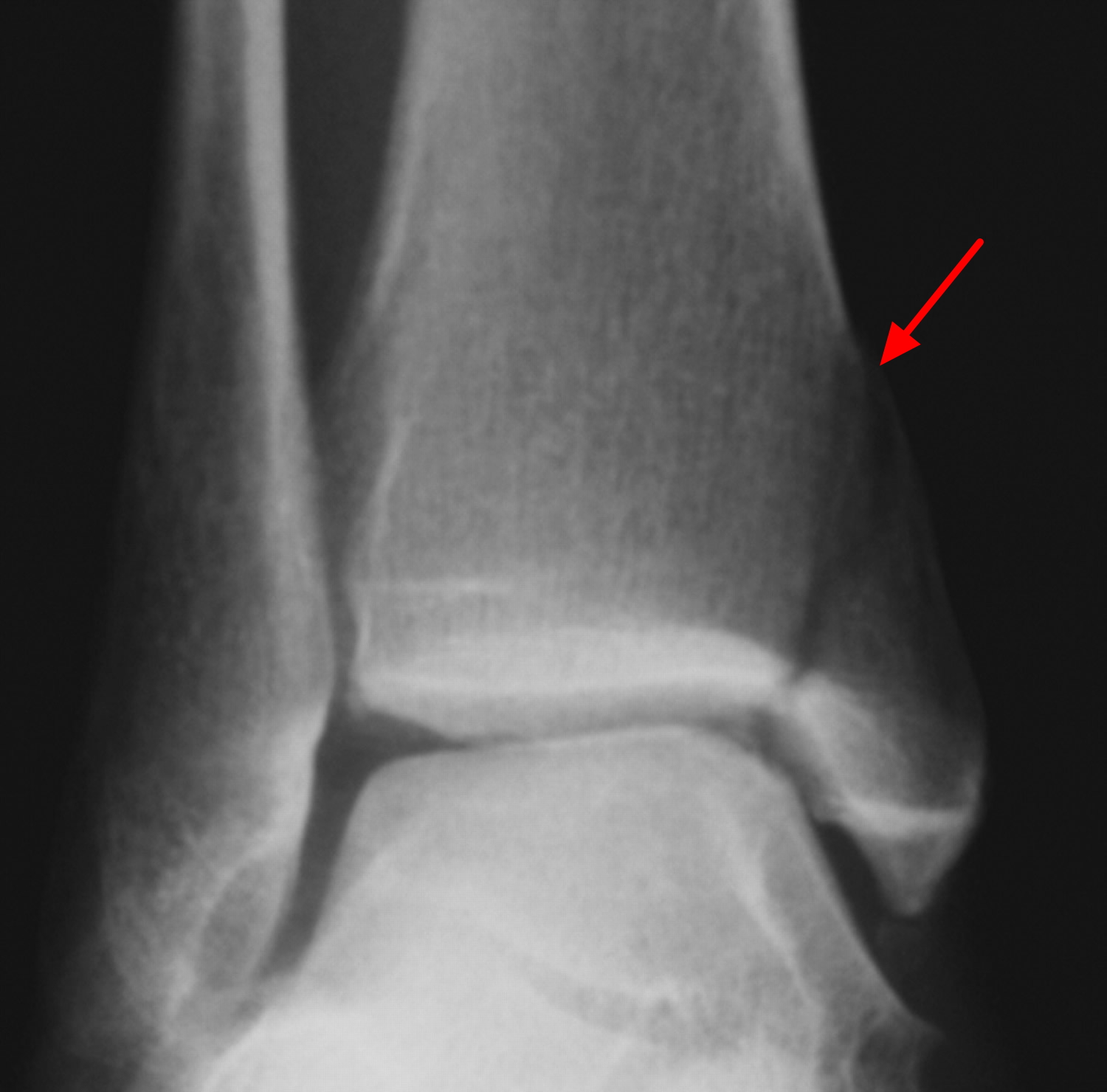
Lateral Malleolus Fracture
A lateral malleolus fracture is a fracture of the fibula.
There are different levels at which that the fibula can be fractured. The level of the fracture may direct the treatment.
Figure 2. Ankle fracture (broken ankle)
Nonsurgical Treatment
You may not require surgery if your ankle is stable, meaning the broken bone is not out of place or just barely out of place. A stress x-ray may be done to see if the ankle is stable. The type of treatment required may also be based on where the bone is broken.
Several different methods are used for protecting the fracture while it heals. ranging from a high-top tennis shoe to a short leg cast. Some physicians let patients put weight on their leg right away, while others have them wait for 6 weeks.
You will see your physician regularly to repeat your ankle x-rays to make sure the fragments of your fracture have not moved out of place during the healing process.
Surgical Treatment
If the fracture is out of place or your ankle is unstable, your fracture may be treated with surgery. During this type of procedure, the bone fragments are first repositioned (reduced) into their normal alignment. They are held together with special screws and metal plates attached to the outer surface of the bone. In some cases, a screw or rod inside the bone may be used to keep the bone fragments together while they heal.
Medial Malleolus Fracture
A medial malleolus fracture is a break in the tibia, at the inside of the lower leg. Fractures can occur at different levels of the medial malleolus.
Medial malleolar fractures often occur with a fracture of the fibula (lateral malleolus), a fracture of the back of the tibia (posterior malleolus), or with an injury to the ankle ligaments.
Figure 3. Medial malleolus fracture
Nonsurgical Treatment
If the fracture is not out of place or is a very low fracture with very small pieces, it can be treated without surgery.
A stress x-ray may be done to see if the fracture and ankle are stable.
The fracture may be treated with a short leg cast or a removable brace. Usually, you need to avoid putting weight on your leg for approximately 6 weeks.
You will need to see your physician regularly for repeat x-rays to make sure the fracture does not change in position.
Surgical Treatment
If the fracture is out of place or the ankle is unstable, surgery may be recommended.
In some cases, surgery may be considered even if the fracture is not out of place. This is done to reduce the risk of the fracture not healing (called a nonunion), and to allow you to start moving the ankle earlier.
A medial malleolus fracture can include impaction or indenting of the ankle joint. Impaction occurs when a force is so great it drives the end of one bone into another one. Repairing an impacted fracture may require bone grafting. This graft acts as a scaffolding for new bone to grow on, and may lower any later risk of developing arthritis.
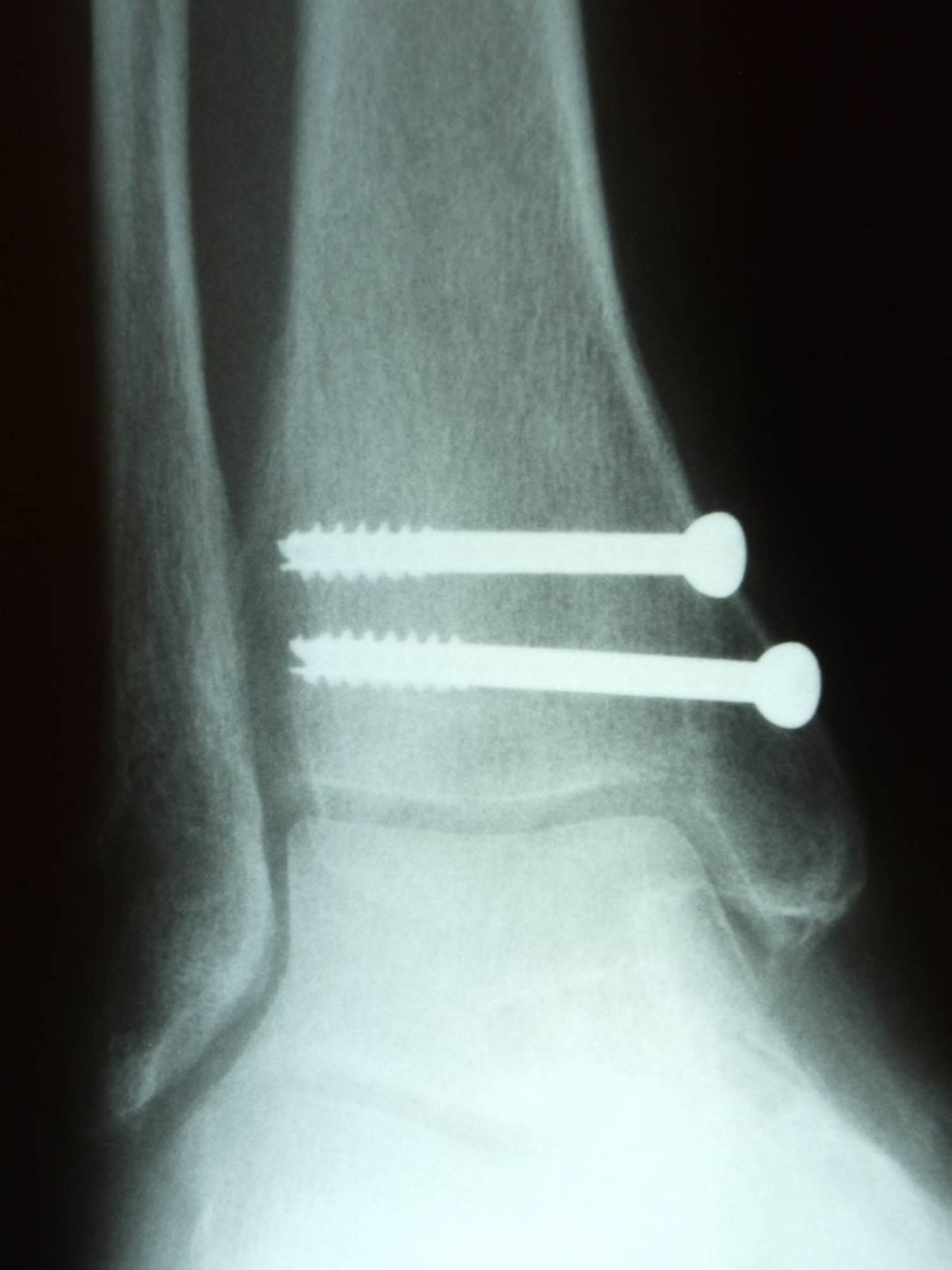
Depending on the fracture, the bone fragments may be fixed using screws, a plate and screws, or different wiring techniques.
Figure 4. Medial malleolus fracture – X-ray of a medial malleolus fracture. (Right) Surgical repair of a medial malleolus fracture with screws.
Posterior Malleolus Fracture
A posterior malleolus fracture is a fracture of the back of the tibia at the level of the ankle joint.
In most cases of posterior malleolus fracture, the lateral malleolus (fibula) is also broken. This is because it shares ligament attachments with the posterior malleolus. There can also be a fracture of the medial malleolus.
Depending on how large the broken piece is, the back of the ankle may be unstable. Some studies have shown that if the piece is bigger than 25% of the ankle joint, the ankle becomes unstable and should be treated with surgery.
It is important for a posterior malleolus fracture to be diagnosed and treated properly because of the risk for developing arthritis. The back of the tibia where the bone breaks is covered with cartilage. Cartilage is the smooth surface that lines a joint. If the broken piece of bone is larger than about 25% of your ankle, and is out of place more than a couple of millimeters, the cartilage surface will not heal properly and the surface of the joint will not be smooth. This uneven surface typically leads to increased and uneven pressure on the joint surface, which leads to cartilage damage and the development of arthritis.
Nonsurgical Treatment
If the fracture is not out place and the ankle is stable, it can be treated without surgery.
Treatment may be with a short leg cast or a removable brace. Patients are typically advised not to put any weight on the ankle for 6 weeks.
Surgical Treatment
If the fracture is out of place or if the ankle is unstable, surgery may be offered.
Different surgical options are available for treating posterior malleolar fractures. One option is to have screws placed from the front of the ankle to the back, or vice versa. Another option is to have a plate and screws placed along the back of the shin bone.
Bimalleolar Fractures or Bimalleolar Equivalent Fractures
“Bi” means two. “Bimalleolar” means that two of the three parts or malleoli of the ankle are broken. (Malleoli is plural for malleolus.)
In most cases of bimalleolar fracture, the lateral malleolus and the medial malleolus are broken and the ankle is not stable.
A “bimalleolar equivalent” fracture means that in addition to one of the malleoli being fractured, the ligaments on the inside (medial) side of the ankle are injured. Usually, this means that the fibula is broken along with injury to the medial ligaments, making the ankle unstable.
A stress test x-ray may be done to see whether the medial ligaments are injured.
Bimalleolar fractures or bimalleolar equivalent fractures are unstable fractures and can be associated with a dislocation.
Nonsurgical Treatment
These injuries are considered unstable and surgery is usually recommended.
Nonsurgical treatment might be considered if you have significant health problems, where the risk of surgery may be too great, or if you usually do not walk.
Immediate treatment typically includes a splint to immobilize the ankle until the swelling goes down. A short leg cast is then applied. Casts may be changed frequently as the swelling subsides in the ankle.
You will need to see your physician regularly to repeat your x-rays to make sure your ankle remains stable.
In most cases, Weight bearing is not be allowed for 6 weeks. After 6 weeks, the ankle may be protected by a removable brace as it continues to heal.
Surgical Treatment
Surgical treatment is often recommended because these fractures make the ankle unstable.
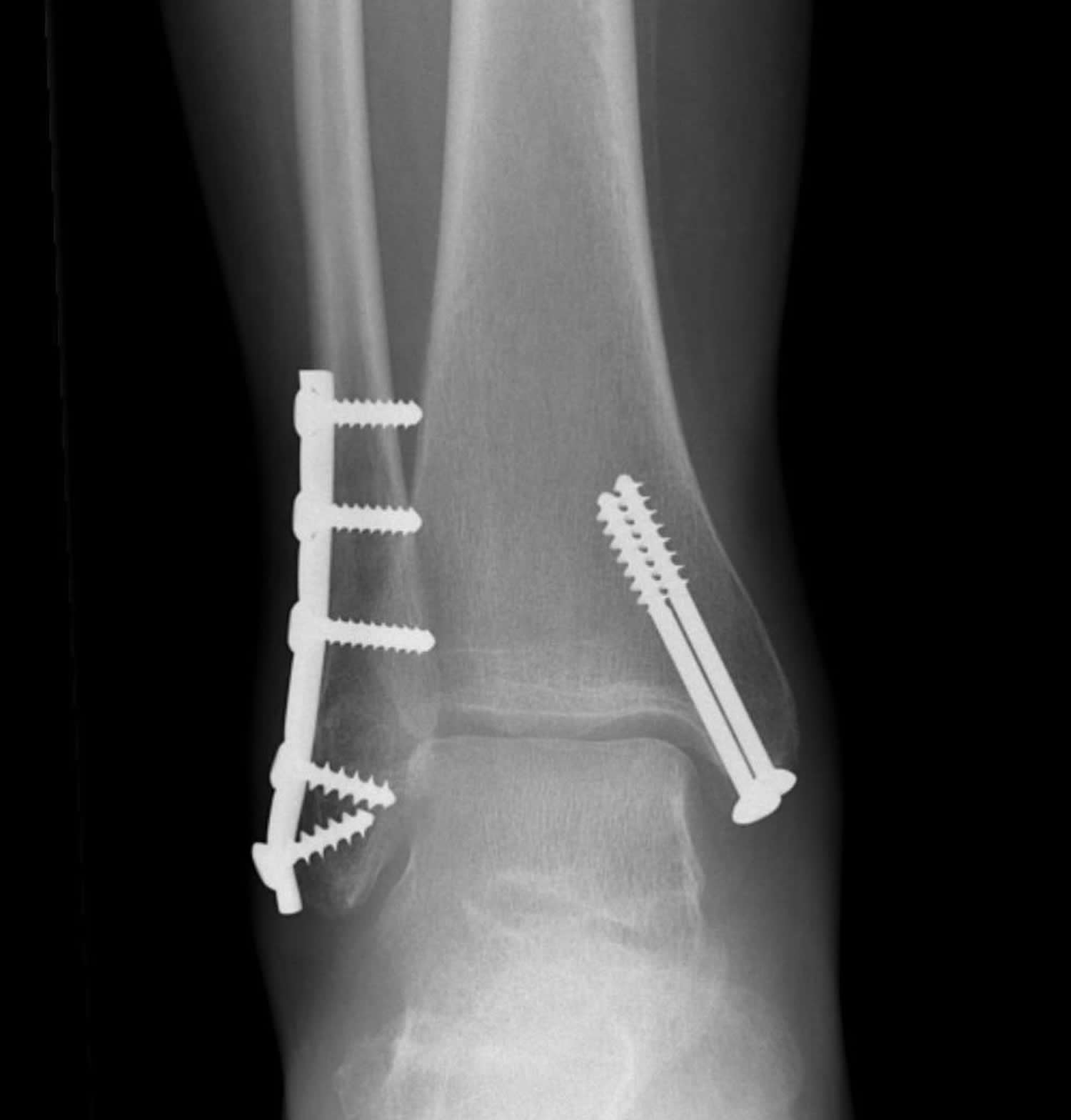
Lateral and medial malleolus fractures are treated with the same surgical techniques as written above for each fracture listed.
Figure 5. X-ray of bimalleolar ankle fracture. (Right) Surgical repair bimalleolar ankle fracture.
Trimalleolar Fractures
“Tri” means three. Trimalleolar fractures means that all three malleoli of the ankle are broken. These are unstable injuries and they can be associated with a dislocation.
Nonsurgical Treatment
These injuries are considered unstable and surgery is usually recommended.
As with bimalleolar ankle fractures, nonsurgical treatment might be considered if you have significant health problems, where the risk of surgery may be too great, or if you usually do not walk.
Nonsurgical treatment is similar to bimalleolar fractures, as described above.
Surgical Treatment
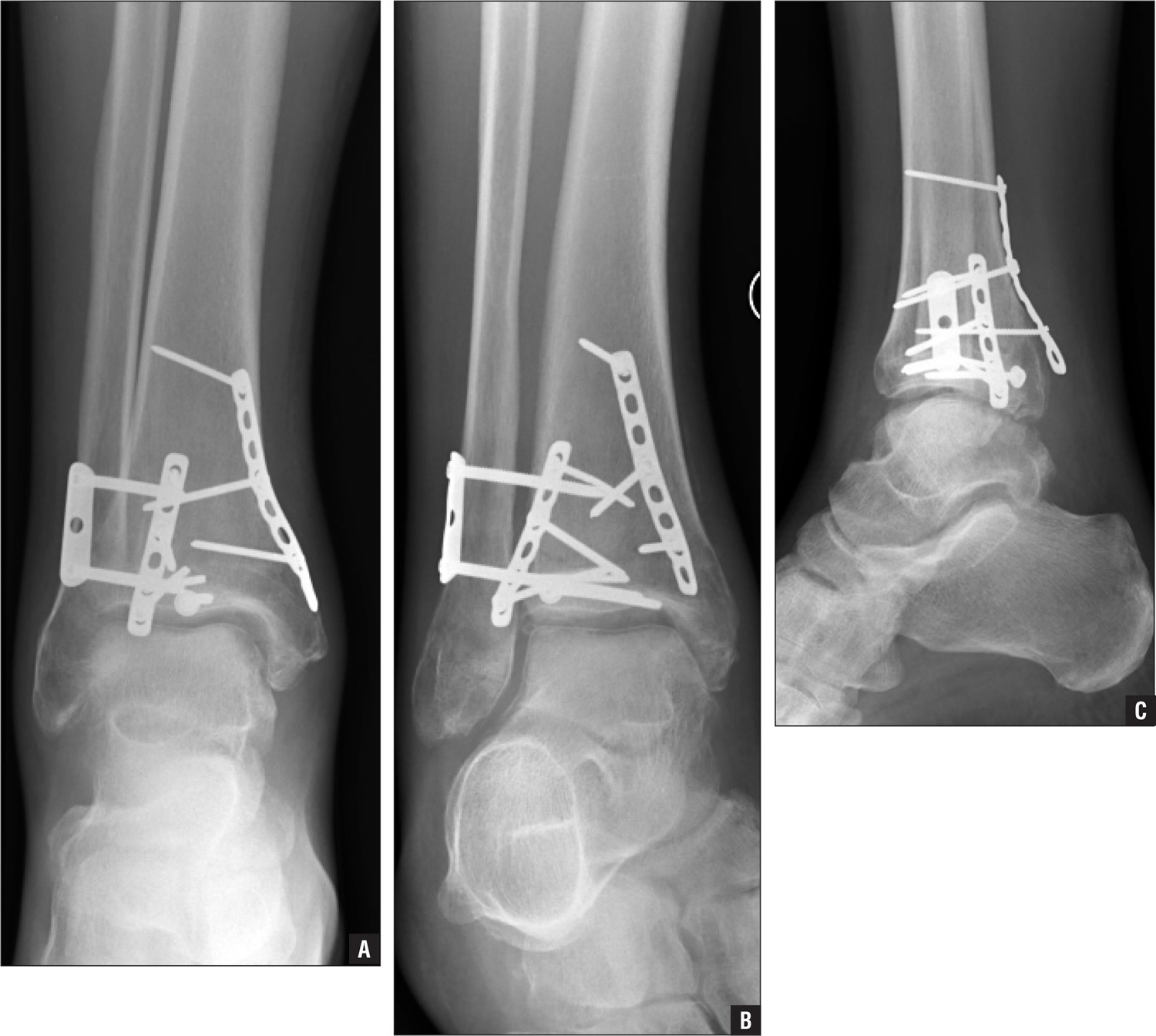
Each fracture can be treated with the same surgical techniques as written above for each individual fracture.
Figure 6. X-ray of trimalleolar ankle fracture. (Right) Surgical repair.
Syndesmotic Injury
The syndesmosis joint is located between the tibia and fibula, and is held together by ligaments. A syndesmotic injury may be just to the ligament — this is also known as high ankle sprain. Depending on how unstable the ankle is, these injuries can be treated without surgery. However, these sprains take longer to heal than the normal ankle sprain.
In many cases, a syndesmotic injury includes both a ligament sprain and one or more fractures. These are unstable injuries and they do very poorly without surgical treatment.
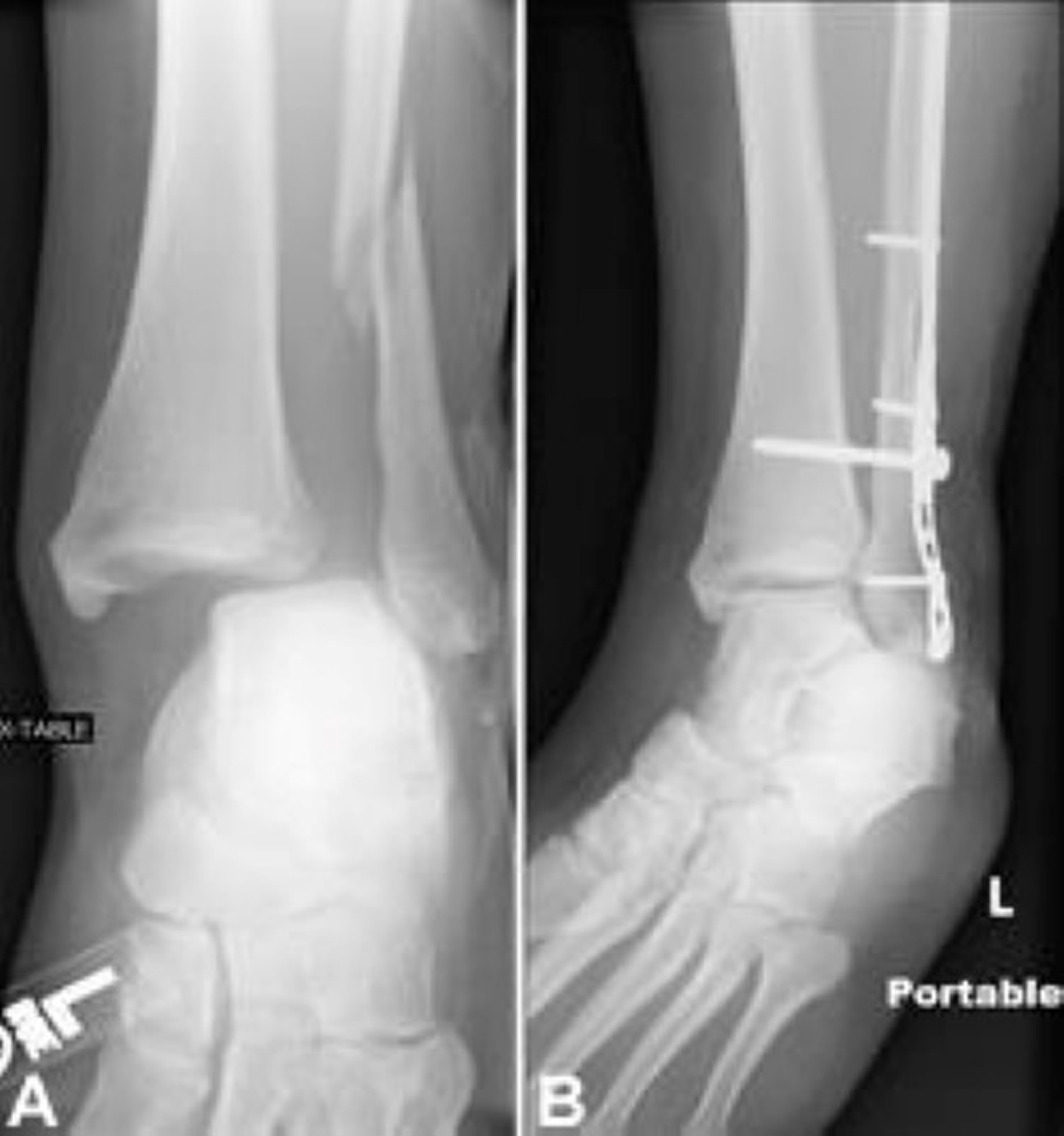
Your physician may do a stress test x-ray to see whether the syndesmosis is injured.
Figure 7. X-ray of syndesmotic injury with lateral malleolus fracture. Note the space between the tibia and fibula. (Right) Surgical repair.
Broken ankle Recovery
Because there is such a wide range of injuries, there is also a wide range of how people heal after their injury. It takes at least 6 weeks for the broken bones to heal. It may take longer for the involved ligaments and tendons to heal.
As mentioned above, your doctor will most likely monitor the bone healing with repeated x-rays. This is typically done more often during the first 6 weeks if surgery is not chosen.
Broken ankle Pain Management
Pain after an injury or surgery is a natural part of the healing process. Your doctor and nurses will work to reduce your pain, which can help you recover faster.
Medications are often prescribed for short-term pain relief after surgery or an injury. Many types of medicines are available to help manage pain, including opioids, non-steroidal anti-inflammatory drugs (NSAIDs), and local anesthetics. Your doctor may use a combination of these medications to improve pain relief, as well as minimize the need for opioids.
Be aware that although opioids help relieve pain after surgery or an injury, they are a narcotic and can be addictive. It is important to use opioids only as directed by your doctor. As soon as your pain begins to improve, stop taking opioids. Talk to your doctor if your pain has not begun to improve within a few days of your treatment.
Broken ankle Rehabilitation
Rehabilitation is very important regardless of how an ankle fracture is treated.
When your physician allows you to start moving your ankle, physical therapy and home exercise programs are very important. Doing your exercises regularly is key.
Eventually, you will also start doing strengthening exercises. It may take several months for the muscles around your ankle to get strong enough for you to walk without a limp and to return to your regular activities.
Again, exercises only make a difference if you actually do them.
Broken ankle Weightbearing
Your specific fracture determines when you can start putting weight on your ankle. Your physician will allow you to start putting weight on your ankle when he or she feels your injury is stable enough to do so.
It is very important to not put weight on your ankle until your physician says you can. If you put weight on the injured ankle too early, the fracture fragments may move or your surgery may fail and you may have to start over.
Broken ankle Supports
It is very common to have several different kinds of things to wear on the injured ankle, depending on the injury.
Initially, most ankle fractures are placed in a splint to protect your ankle and allow for the swelling to go down. After that, you may be put into a cast or removable brace.
Even after the fracture has healed, your physician may recommend wearing an ankle brace for several months while you are doing sporting activities.
Complications of Broken ankle
People who smoke, have diabetes, or are elderly are at a higher risk for complications after surgery, including problems with wound healing. This is because it may take longer for their bones to heal.
Nonsurgical Treatment
Without surgery, there is a risk that the fracture will move out of place before it heals. This is why it is important to follow up with your physician as scheduled.
If the fracture fragments do move out of place and the bones heal in that position, it is called a “malunion.” Treatment for this is determined by how far out of place the bones are and how the stability of the ankle joint is affected.
If a malunion does occur or if your ankle becomes unstable after it heals, this can eventually lead to arthritis in your ankle.
Surgical Treatment
General surgical risks include:
- Infection
- Bleeding
- Pain
- Blood clots in your leg
- Damage to blood vessels, tendons, or nerves
Risks from the surgical treatment of ankle fractures include:
- Difficulty with bone healing
- Arthritis
- Pain from the plates and screws that are used to fix fracture. Some patients choose to have them removed several months after their fracture heals
Broken ankle Outcomes
Although most people return to normal daily activities, except for sports, within 3 to 4 months, studies have shown that people can still be recovering up to 2 years after their ankle fractures. It may take several months for you to stop limping while you walk, and before you can return to sports at your previous competitive level. Most people return to driving within 9 to 12 weeks from the time they were injured.
Broken vs Sprained ankle
An ankle sprain occurs when the strong ligaments that support the ankle stretch beyond their limits and tear. Ligaments are connective tissues that connect bones to other bones and tightly bind bones together and resist stress. The ligaments in the ankle help to keep the bones in proper position and stabilize the joint.
Most sprained ankles occur in the lateral ligaments on the outside of the ankle. Sprains can range from tiny tears in the fibers that make up the ligament to complete tears through the tissue.
If there is a complete tear of the ligaments, the ankle may become unstable after the initial injury phase passes. Over time, this instability can result in damage to the bones and cartilage of the ankle joint.
Ankle sprains are common injuries that occur among people of all ages. They range from mild to severe, depending upon how much damage there is to the ligaments.
Most sprains are minor injuries that heal with home treatments like rest and applying ice. However, if your ankle is very swollen and painful to walk on — or if you are having trouble putting weight on your ankle at all, be sure to see your doctor.
Without proper treatment and rehabilitation, a more severe sprain can weaken your ankle—making it more likely that you will injure it again. Repeated ankle sprains can lead to long-term problems, including chronic ankle pain, arthritis, and ongoing instability.
Grades of Ankle Sprains
After the examination, your doctor will determine the grade of your sprain to help develop a treatment plan. Sprains are graded based on how much damage has occurred to the ligaments.
Grade 1 Sprain (Mild)
- Slight stretching and microscopic tearing of the ligament fibers
- Mild tenderness and swelling around the ankle
Grade 2 Sprain (Moderate)
- Partial tearing of the ligament
- Moderate tenderness and swelling around the ankle
- If the doctor moves the ankle in certain ways, there is an abnormal looseness of the ankle joint
Grade 3 Sprain (Severe)
- Complete tear of the ligament
- Significant tenderness and swelling around the ankle
- If the doctor pulls or pushes on the ankle joint in certain movements, substantial instability occurs
Figure 8. Ankle joint ligaments
Cause of sprained ankle
Your foot can twist unexpectedly during many different activities, such as:
- Walking or exercising on an uneven surface
- Falling down
- Participating in sports that require cutting actions or rolling and twisting of the foot—such as trail running, basketball, tennis, football, and soccer
- During sports activities, someone else may step on your foot while you are running, causing your foot to twist or roll to the side.
Prevention of ankle sprains
The best way to prevent ankle sprains is to maintain good muscle strength, balance, and flexibility. The following precautions will help prevent sprains:
- Warm up thoroughly before exercise and physical activity
- Pay careful attention when walking, running, or working on an uneven surface
- Wear shoes that are made for your activity
- Slow down or stop activities when you feel pain or fatigue
Symptoms of sprained ankle
A sprained ankle is painful. Other symptoms may include:
- Swelling
- Bruising
- Tenderness to touch
- Instability of the ankle—this may occur when there has been complete tearing of the ligament or a complete dislocation of the ankle joint.
If there is severe tearing of the ligaments, you might also hear or feel a “pop” when the sprain occurs. Symptoms of a severe sprain are similar to those of a broken bone and require prompt medical evaluation.
Imaging Tests
- X-rays. X-rays provide images of dense structures, such as bone. Your doctor may order x-rays to rule out a broken bone in your ankle or foot. A broken bone can cause similar symptoms of pain and swelling.
- Stress x-rays. In addition to plain x-rays, your doctor may also order stress x-rays. These scans are taken while the ankle is being pushed in different directions. Stress x-rays help to show whether the ankle is moving abnormally because of injured ligaments.
- Magnetic resonance imaging (MRI) scan. Your doctor may order an MRI if he or she suspects a very severe injury to the ligaments, damage to the cartilage or bone of the joint surface, a small bone chip, or another problem. The MRI may not be ordered until after the period of swelling and bruising resolves.
- Ultrasound. This imaging scan allows your doctor to observe the ligament directly while he or she moves your ankle. This helps your doctor to determine how much stability the ligament provides.
Sprained ankle treatment
Almost all ankle sprains can be treated without surgery. Even a complete ligament tear can heal without surgical repair if it is immobilized appropriately.
A three-phase program guides treatment for all ankle sprains—from mild to severe:
- Phase 1 includes resting, protecting the ankle and reducing the swelling.
- Phase 2 includes restoring range of motion, strength and flexibility.
- Phase 3 includes maintenance exercises and the gradual return to activities that do not require turning or twisting the ankle. This will be followed later by being able to do activities that require sharp, sudden turns (cutting activities)—such as tennis, basketball, or football.
This three-phase treatment program may take just 2 weeks to complete for minor sprains, or up to 6 to 12 weeks for more severe injuries.
Home Treatments
For milder sprains, your doctor may recommend simple home treatment.
The RICE protocol. Follow the RICE protocol as soon as possible after your injury:
- Rest your ankle by not walking on it.
- Ice should be immediately applied to keep the swelling down. It can be used for 20 to 30 minutes, three or four times daily. Do not apply ice directly to your skin.
- Compression dressings, bandages or ace-wraps will immobilize and support your injured ankle.
- Elevate your ankle above the level of your heart as often as possible during the first 48 hours.
Medication. Nonsteroidal anti-inflammatory drugs (NSAIDs) such as ibuprofen and naproxen can help control pain and swelling. Because they improve function by both reducing swelling and controlling pain, they are a better option for mild sprains than narcotic pain medicines.
Nonsurgical Treatment
Some sprains will require treatment in addition to the RICE protocol and medications.
Crutches. In most cases, swelling and pain will last from 2 to 3 days. Walking may be difficult during this time and your doctor may recommend that you use crutches as needed.
Immobilization. During the early phase of healing, it is important to support your ankle and protect it from sudden movements. For a Grade 2 sprain, a removable plastic device such as a cast-boot or air stirrup-type brace can provide support. Grade 3 sprains may require a short leg cast or cast-brace for 2 to 3 weeks.
Your doctor may encourage you to put some weight on your ankle while it is protected. This can help with healing.
Physical therapy. Rehabilitation exercises are used to prevent stiffness, increase ankle strength, and prevent chronic ankle problems.
- Early motion. To prevent stiffness, your doctor or physical therapist will provide you with exercises that involve range-of-motion or controlled movements of your ankle without resistance.
- Strengthening exercises. Once you can bear weight without increased pain or swelling, exercises to strengthen the muscles and tendons in the front and back of your leg and foot will be added to your treatment plan. Water exercises may be used if land-based strengthening exercises, such as toe-raising, are too painful. Exercises with resistance are added as tolerated.
- Proprioception (balance) training. Poor balance often leads to repeat sprains and ankle instability. A good example of a balance exercise is standing on the affected foot with the opposite foot raised and eyes closed. Balance boards are often used in this stage of rehabilitation.
- Endurance and agility exercises. Once you are pain-free, other exercises may be added, such as agility drills. Running in progressively smaller figures-of-8 is excellent for agility and calf and ankle strength. The goal is to increase strength and range of motion as balance improves over time.
Surgical Treatment
Surgical treatment for ankle sprains is rare. Surgery is reserved for injuries that fail to respond to nonsurgical treatment, and for patients who experience persistent ankle instability after months of rehabilitation and nonsurgical treatment.
Surgical options may include:
- Arthroscopy. During arthroscopy, your doctor uses a small camera, called an arthroscope, to look inside your ankle joint. Miniature instruments are used to remove any loose fragments of bone or cartilage, or parts of the ligament that may be caught in the joint.
Reconstruction. Your doctor may be able to repair the torn ligament with stitches or sutures. In some cases, he or she will reconstruct the damaged ligament by replacing it with a tissue graft obtained from other ligaments and/or tendons found in the foot and around the ankle. - Immobilization. There is typically a period of immobilization following surgery for an ankle sprain. Your doctor may apply a cast or protective boot to protect the repaired or reconstructed ligament. Be sure to follow your doctor’s instructions about how long to wear the protective device; if you remove it too soon, a simple misstep can re-tear the fixed ligament.
- Rehabilitation. Rehabilitation after surgery involves time and attention to restore strength and range of motion so you can return to pre-injury function. The length of time you can expect to spend recovering depends upon the extent of injury and the amount of surgery that was done. Rehabilitation may take from weeks to months.
Outcomes
Outcomes for ankle sprains are generally quite good. With proper treatment, most patients are able to resume their day-to-day activities after a period of time.
Most importantly, successful outcomes are dependent upon patient commitment to rehabilitation exercises. Incomplete rehabilitation is the most common cause of chronic ankle instability after a sprain. If a patient stops doing the strengthening exercises, the injured ligament(s) will weaken and put the patient at risk for continued ankle sprains.
Chronic Ankle Sprains
Once you have sprained your ankle, you may continue to sprain it if the ligaments do not have time to completely heal. It can be hard for patients to tell if a sprain has healed because even an ankle with a chronic tear can be highly functional because overlying tendons help with stability and motion.
If pain continues for more than 4 to 6 weeks, you may have a chronic ankle sprain. Activities that tend to make an already sprained ankle worse include stepping on uneven surfaces and participating in sports that require cutting actions or rolling and twisting of the foot.
Abnormal proprioception—a common complication of ankle sprains—can also lead to repeat sprains. There may be imbalance and muscle weakness that causes a reinjury. If you sprain your ankle over and over again, a chronic situation may persist with instability, a sense of the ankle giving way, and chronic pain. This can also happen if you return to work, sports, or other activities before your ankle heals and is rehabilitated.
Stress fracture ankle and foot
A stress fracture is a small crack in a bone, or severe bruising within a bone. Most stress fractures are caused by overuse and repetitive activity, and are common in runners and athletes who participate in running sports, such as soccer and basketball. Stress fractures occur over time when repetitive forces result in microscopic damage to the bone.
The repetitive force that causes a stress fracture is not great enough to cause an acute fracture — such as a broken ankle caused by a fall. Overuse stress fractures occur when an athletic movement is repeated so often, weight-bearing bones and supporting muscles do not have enough time to heal between exercise sessions.
Bone is in a constant state of turnover—a process called remodeling. New bone develops and replaces older bone. If an athlete’s activity is too great, the breakdown of older bone occurs rapidly — it outpaces the body’s ability to repair and replace it. As a result, the bone weakens and becomes vulnerable to stress fractures.
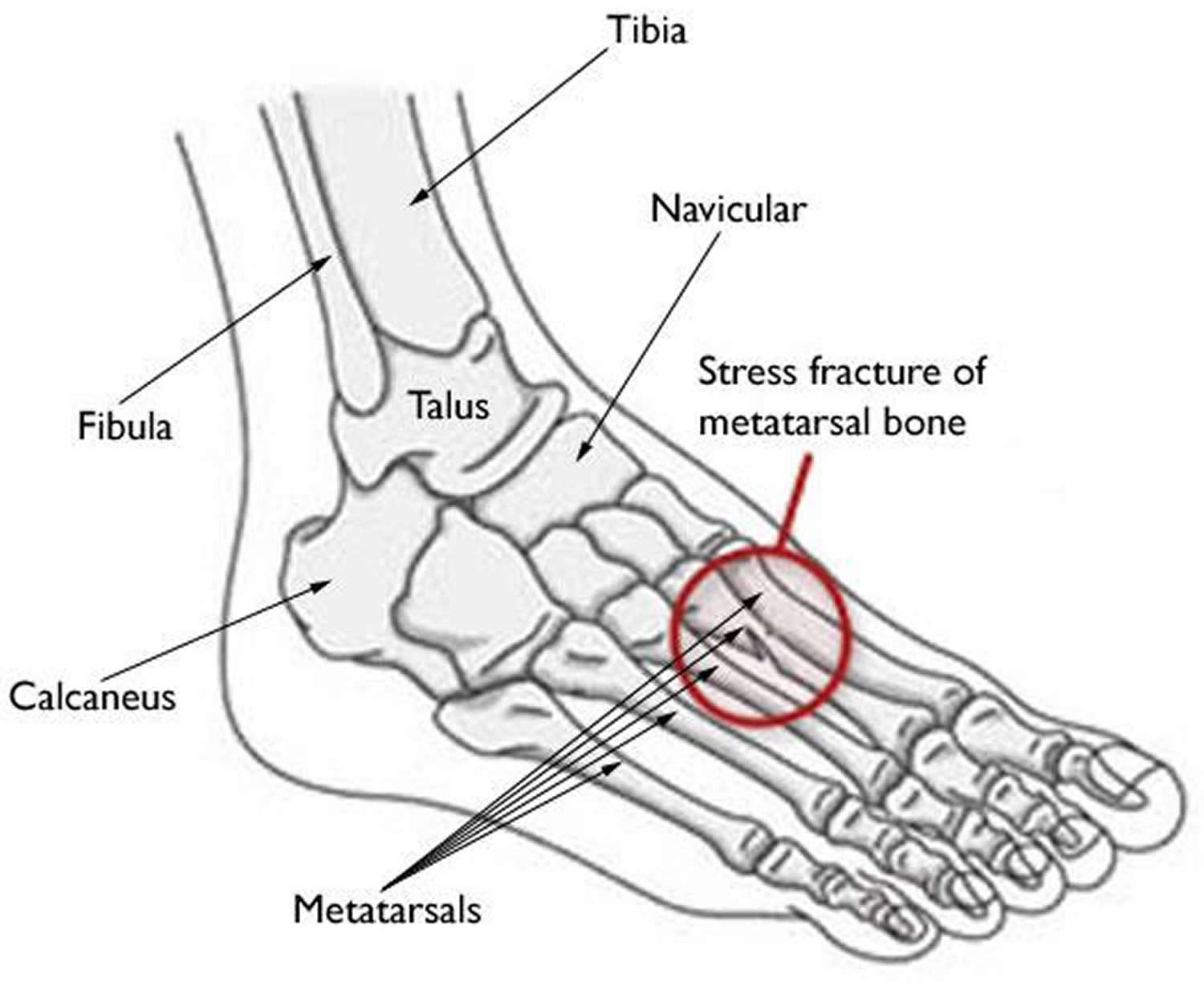
- Stress fractures occur most often in the second and third metatarsals in the foot, which are thinner (and often longer) than the adjacent first metatarsal. This is the area of greatest impact on your foot as you push off when you walk or run.
- Stress fractures are also common in the calcaneus (heel); fibula (the outer bone of the lower leg and ankle); talus (a small bone in the ankle joint); and the navicular (a bone on the top of the midfoot).
See your doctor as soon as possible if you think that you have a stress fracture in your foot or ankle. Ignoring the pain can have serious consequences. The bone may break completely.
Until your appointment with the doctor, follow the RICE protocol. RICE stands for rest, ice, compression, and elevation.
- Rest. Avoid activities that put weight on your foot. If you have to bear weight for any reason, make sure you are wearing a very supportive shoe. A thick-soled cork sandal is better than a thin slipper.
- Ice. Apply ice immediately after the injury to keep the swelling down. Use cold packs for 20 minutes at a time, several times a day. Do not apply ice directly on your skin.
- Compression. To prevent additional swelling, lightly wrap the area in a soft bandage.
- Elevation. As often as possible, rest with your foot raised up higher than your heart.
In addition, nonsteroidal anti-inflammatory drugs, or NSAIDs, such as ibuprofen or naproxen can help relieve pain and reduce swelling.
Figure 9. Stress fracture foot – the most common sites for stress fractures in the foot are the metatarsal bones.
Stress fractures usually occur when people change their activities — such as by trying a new exercise, suddenly increasing the intensity of their workouts, or changing the workout surface (jogging on a treadmill vs. jogging outdoors). In addition, if osteoporosis or other disease has weakened the bones, just doing everyday activities may result in a stress fracture.
The weight-bearing bones of the foot and lower leg are especially vulnerable to stress fractures because of the repetitive forces they must absorb during activities like walking, running, and jumping.
Refraining from high impact activities for an adequate period of time is key to recovering from a stress fracture in the foot or ankle. Returning to activity too quickly can not only delay the healing process but also increase the risk for a complete fracture. Should a complete fracture occur, it will take far longer to recover and return to activities.
Ankle and Foot Stress Fracture Cause
The most common cause of stress fractures is a sudden increase in physical activity. This increase can be in the frequency of activity—such as exercising more days per week. It can also be in the duration or intensity of activity—such as running longer distances.
Even for the nonathlete, a sudden increase in activity can cause a stress fracture. For example, if you walk infrequently on a day-to-day basis but end up walking excessively (or on uneven surfaces) while on a vacation, you might experience a stress fracture. A new style of shoes can lessen your foot’s ability to absorb repetitive forces and result in a stress fracture.
Bone Insufficiency
Conditions that decrease bone strength and density, such as osteoporosis, and certain long-term medications can make you more likely to experience a stress fracture-even when you are performing normal everyday activities. For example, stress fractures are more common in the winter months, when Vitamin D is lower in the body.
Studies show that female athletes are more prone to stress fractures than male athletes. This may be due, in part, to decreased bone density from a condition that doctors call the “female athlete triad.” When a girl or young woman goes to extremes in dieting or exercise, three interrelated illnesses may develop: eating disorders, menstrual dysfunction, and premature osteoporosis. As a female athlete’s bone mass decreases, her chances for getting a stress fracture increase.
Poor Conditioning
Doing too much too soon is a common cause of stress fracture. This is often the case with individuals who are just beginning an exercise program-but it occurs in experienced athletes, as well. For example, runners who train less over the winter months may be anxious to pick up right where they left off at the end of the previous season. Instead of starting off slowly, they resume running at their previous mileage. This situation in which athletes not only increase activity levels, but push through any discomfort and do not give their bodies the opportunity to recover, can lead to stress fractures.
Improper Technique
Anything that alters the mechanics of how your foot absorbs impact as it strikes the ground may increase your risk for a stress fracture. For example, if you have a blister, bunion, or tendonitis, it can affect how you put weight on your foot when you walk or run, and may require an area of bone to handle more weight and pressure than usual.
Change in Surface
A change in training or playing surface, such as a tennis player going from a grass court to a hard court, or a runner moving from a treadmill to an outdoor track, can increase the risk for stress fracture.
Improper Equipment
Wearing worn or flimsy shoes that have lost their shock-absorbing ability may contribute to stress fractures.
Ankle and foot stress fracture prevention
The following guidelines can help you prevent stress fractures in the future:
- Eat a healthy diet. A balanced diet rich in calcium and Vitamin D will help build bone strength.
- Use proper equipment. Old or worn running shoes may lose their ability to absorb shock and can lead to injury. In general, athletic shoes should have a softer insole, and a stiffer outer sole.
- Start new activity slowly. Gradually increase your time, speed, and distance. In most cases, a 10 percent increase per week is appropriate.
- Cross train. Vary your activities to help avoid over stressing one area of your body. For example, alternate a high-impact sport like running with lower-impact sports like swimming or cycling.
- Add strength training to your workout. One of the best ways to prevent early muscle fatigue and the loss of bone density that comes with aging is to incorporate strength training. Strength-training exercises use resistance methods like free weights, resistance bands, or your own body weight to build muscles and strength.
- Stop your activity if pain or swelling returns. Rest for a few days. If the pain continues, see your doctor.
Symptoms of ankle and foot stress fracture
The most common symptom of a stress fracture in the foot or ankle is pain. The pain usually develops gradually and worsens during weight-bearing activity. Other symptoms may include:
- Pain that diminishes during rest
- Pain that occurs and intensifies during normal, daily activities
- Swelling on the top of the foot or on the outside of the ankle
- Tenderness to touch at the site of the fracture
- Possible bruising
Ankle and Foot Stress fracture diagnosis
Physical Examination
Your doctor will discuss your medical history and general health. He or she will ask about your work, your activities, your diet, and what medications you are taking.It is important that your doctor is aware of your risk factors for stress fracture. If you have had a stress fracture before, your doctor may order a full medical work-up with laboratory tests to check for nutritional deficiencies such as low calcium or Vitamin D.
After discussing your symptoms and health history, your doctor will examine your foot and ankle. During the examination, he or she will look for areas of tenderness and apply gentle pressure directly to the injured bone. Often, the key to diagnosing a stress fracture is the patient’s report of pain in response to this pressure. Pain from a stress fracture is typically limited to the area directly over the injured bone and is not generalized over the whole foot.
Imaging Tests
Your doctor may order imaging tests to help confirm the diagnosis.
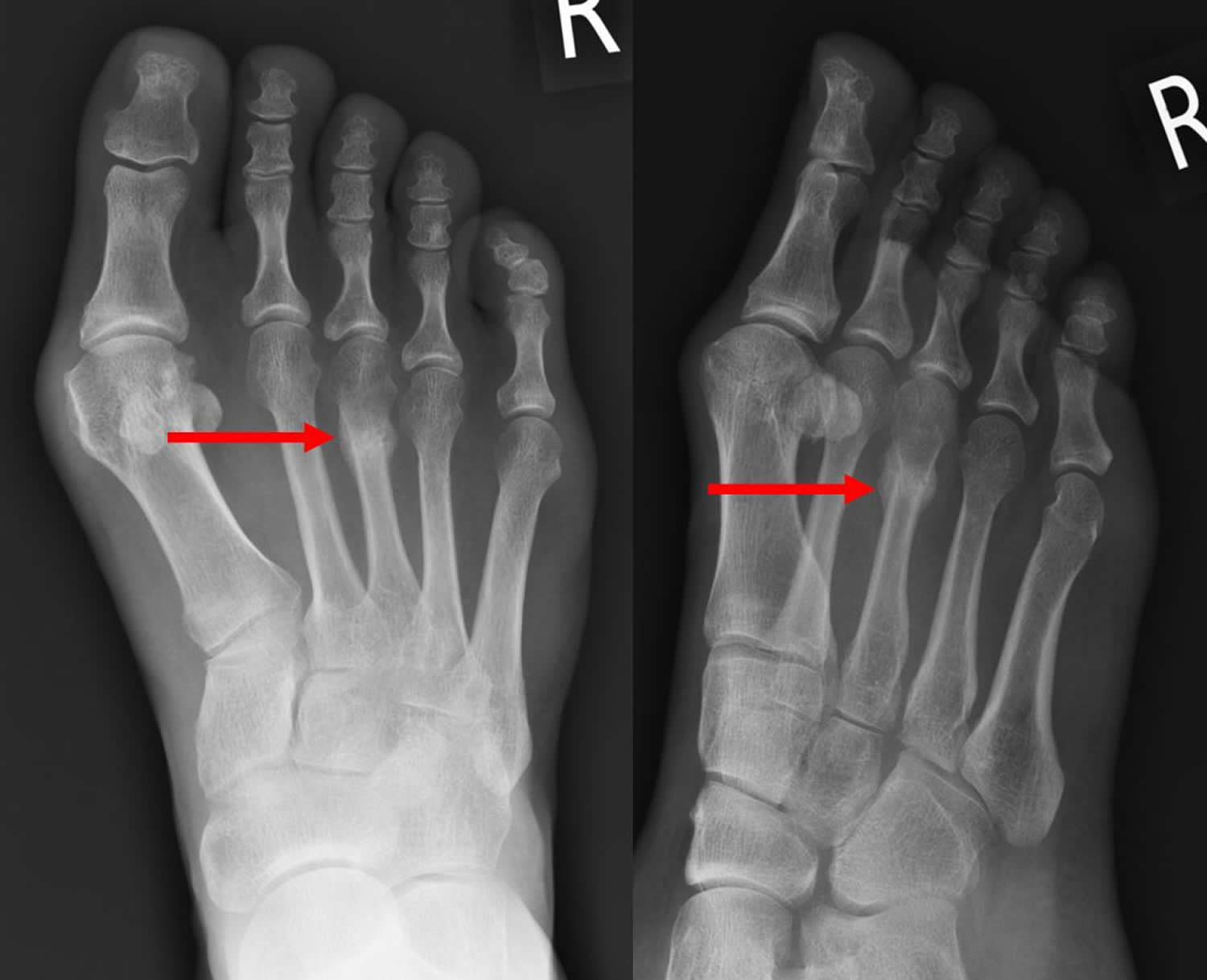
X-rays. X-rays provide images of dense structures, such as bone. Since a stress fracture starts as a tiny crack, it is often difficult to see on a first x-ray. The fracture may not be visible until several weeks later when it has actually started to heal. After a few weeks, a type of healing bone called callus may appear around the fracture site. In many cases, this is the point at which the fracture line actually becomes visible in the bone.
Figure 10. Stress fracture foot – x-ray showing callus formation at the site of the stress fracture (3rd metatarsal).
Other imaging studies. If your doctor suspects a stress fracture but cannot see it on an x-ray, he or she may recommend a bone scan or a magnetic resonance imaging (MRI) scan. Although a bone scan is less specific than an MRI in showing the actual location of the stress fracture, both of these types of studies are more sensitive than x-rays and can detect stress fractures earlier.
Ankle and foot stress fracture treatment
The goal of treatment is to relieve pain and allow the fracture to heal so that you are able to return to your activities. Following your doctor’s treatment plan will help you return to activities faster and prevent further damage to the bone.
Treatment will vary depending on the location of the stress fracture and its severity. The majority of stress fractures are treated nonsurgically.
Nonsurgical Treatment
In addition to the RICE protocol and anti-inflammatory medication, your doctor may recommend that you use crutches to keep weight off your foot until the pain subsides. Other recommendations for nonsurgical treatment may include:
- Modified activities. It typically takes from 6 to 8 weeks for a stress fracture to heal. During that time, switch to activities that place less stress on your foot and leg. Swimming and cycling are good alternative activities. However, you should not resume any type of physical activity that involves your injured foot or ankle-even if it is low impact-without your doctor’s recommendation.
- Protective footwear. To reduce stress on your foot and leg, your doctor may recommend wearing protective footwear. This may be a stiff-soled shoe, a wooden-soled sandal, or a removable short-leg fracture brace shoe.
- Casting. Stress fractures in the fifth metatarsal bone (on the outer side of the foot) or in the navicular or talus bones take longer to heal. Your doctor may apply a cast to your foot to keep your bones in a fixed position and to remove the stress on your involved leg.
Surgical Treatment
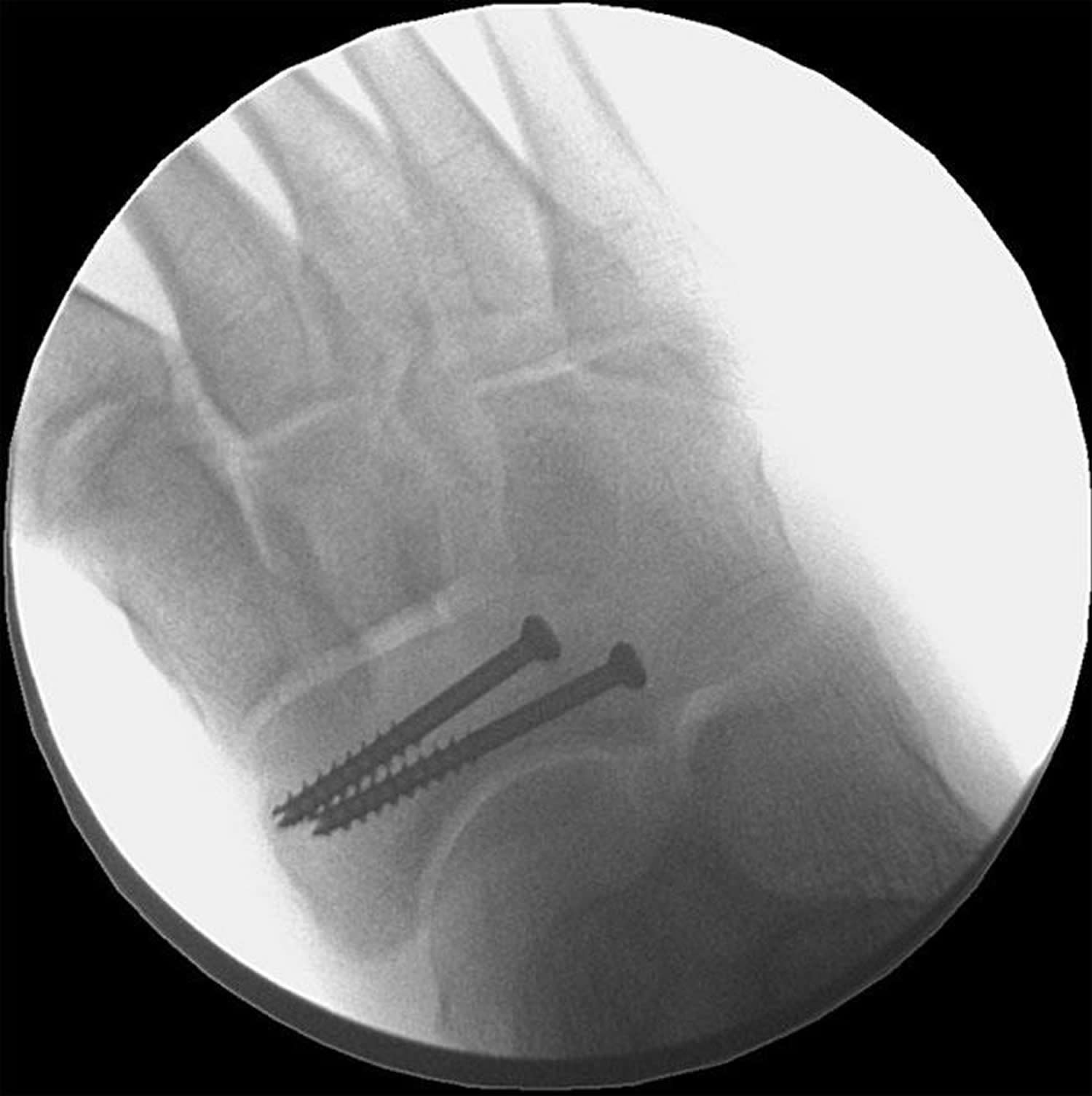
Some stress fractures require surgery to heal properly. In most cases, this involves supporting the bones by inserting a type of fastener. This is called internal fixation. Pins, screws, and/or plates are most often used to hold the small bones of the foot and ankle together during the healing process.
Figure 11. X-ray of the mid-foot shows screws placed in the navicular bone to keep the fracture in a fixed position during healing
Ankle and foot stress fracture recovery
In most cases, it takes from 6 to 8 weeks for a stress fracture to heal. More serious stress fractures can take longer. Although it can be hard to be sidelined with an injury, returning to activity too soon can put you at risk for larger, harder-to-heal stress fractures and an even longer down time. Reinjury could lead to chronic problems and the stress fracture might never heal properly.
Once your pain has subsided, your doctor may confirm that the stress fracture has healed by taking x-rays. A computed tomography (CT) scan can also be useful in determining healing, especially in bones where the fracture line was initially hard to see.
Once the stress fracture has healed and you are pain free, your doctor will allow a gradual return to activity. During the early phase of rehabilitation, your doctor may recommend alternating days of activity with days of rest. This gives your bone the time to grow and withstand the new demands being placed upon it. As your fitness level improves, slowly increase the frequency, duration, and intensity of your exercise.