Contents
- What is cardiomyopathy
- Human Heart
- Cardiomyopathy types
- Cardiomyopathy prognosis
- Cardiomyopathy causes
- Risk Factors for developing cardiomyopathy
- Complications of cardiomyopathy
- Cardiomyopathy prevention
- Cardiomyopathy signs and symptoms
- Cardiomyopathy diagnosis
- Cardiomyopathy treatment
What is cardiomyopathy
Cardiomyopathy is a heart disease in which your heart muscle is damaged and becomes weak so it can’t pump blood as well as it should. The name cardiomyopathy literally means: CARDIO – heart, MYO – muscle, PATHY – disease. In cardiomyopathy, the heart muscle becomes enlarged, thick, or rigid. In rare cases, the muscle tissue in the heart is replaced with scar tissue. Most people with cardiomyopathy are only mildly affected and can lead fairly normal lives.
However, as cardiomyopathy worsens, the heart becomes weaker. It’s less able to pump blood through the body and maintain a normal electrical rhythm. This can lead to heart failure or irregular heartbeats called arrhythmias. In turn, heart failure can cause fluid to build up in the lungs, ankles, feet, legs, or abdomen.
The weakening of the heart also can cause other complications, such as heart valve problems.
There are different types of cardiomyopathy, which have different causes and affect different groups of people. The condition is usually managed with medication and living a healthy life.
Cardiomyopathy can be acquired or inherited. “Acquired” means you aren’t born with the disease, but you develop it due to another disease, condition, or factor. “Inherited” means your parents passed the gene for the disease on to you. Many times, the cause of cardiomyopathy isn’t known.
Cardiomyopathy can affect people of all ages. However, people in certain age groups are more likely to have certain types of cardiomyopathy.
According to the Pediatric Cardiomyopathy Registry, one in every 100,000 children in the U.S. under the age of 18 is diagnosed with cardiomyopathy. The majority of diagnosed children are under 12 months followed by children 12 to 18 years old.
If you have cardiomyopathy, it’s important to live a healthy life as far as possible. You can do this by:
- having a healthy diet
- not taking too much salt
- not drinking too much alcohol
- not no smoking
- exercising regularly.
However, some people will also need medicines, some will need surgery and some will need an implantable device to keep their heart going properly.
Human Heart
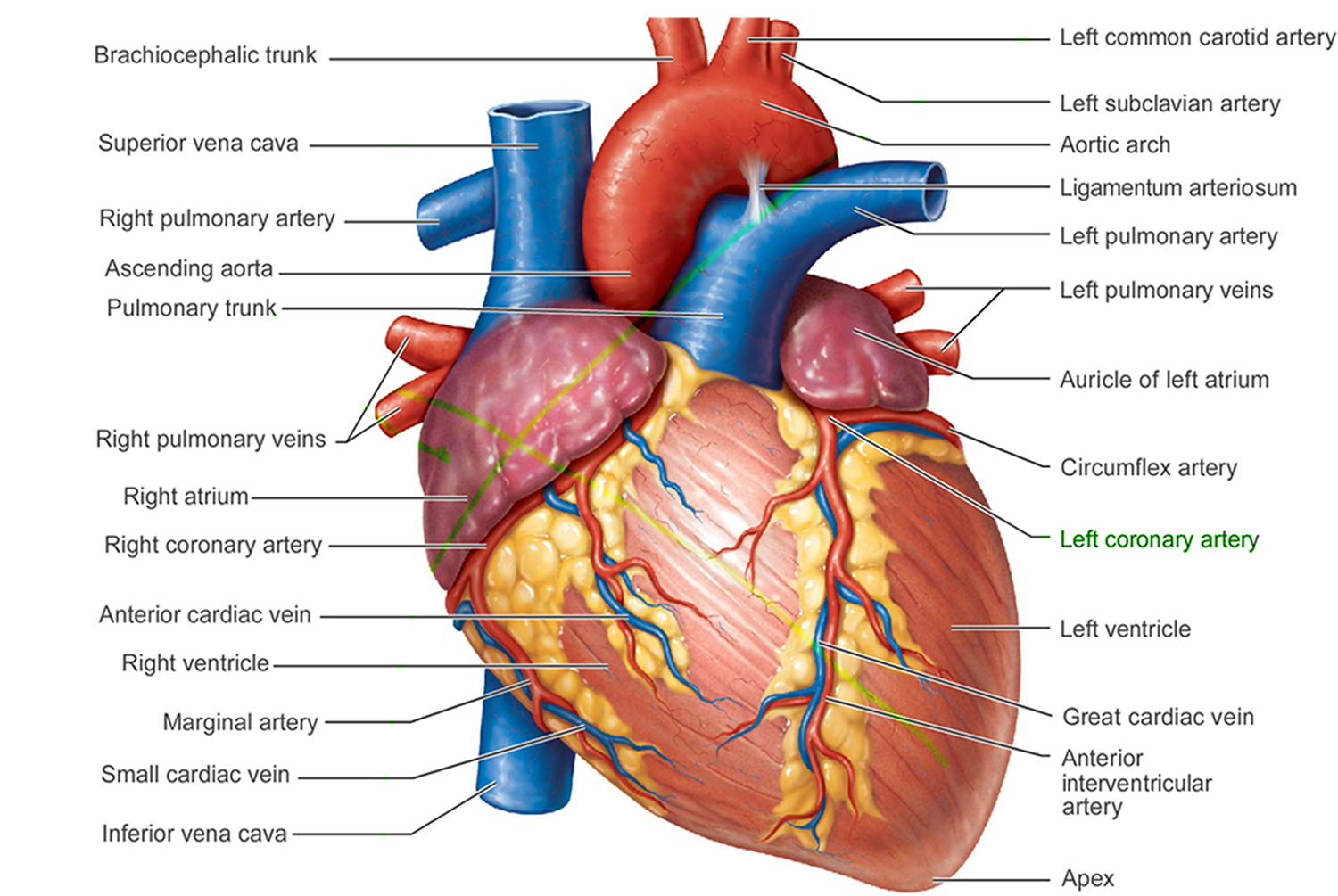
The heart is a specialized muscle that contracts regularly and continuously, pumping blood to the body and the lungs. It has four chambers – two at the top (the atria), and two at the bottom (the ventricles). See the Figures 1 to 3 below.
The heart is made up of three layers:
- the endocardium
- the myocardium
- the pericardium.
The endocardium is a thin layer on the inside of the heart, lining the chambers and valves. The myocardium is the thick, muscular layer of the heart that contracts and squeezes the blood out of the heart. It’s this layer that is affected by cardiomyopathy. The pericardium is a thin, double layer that forms a protective sac around the outside of the heart. It contains a small amount of fluid – called pericardial fluid – which acts as a lubricant when the heart is contracting.
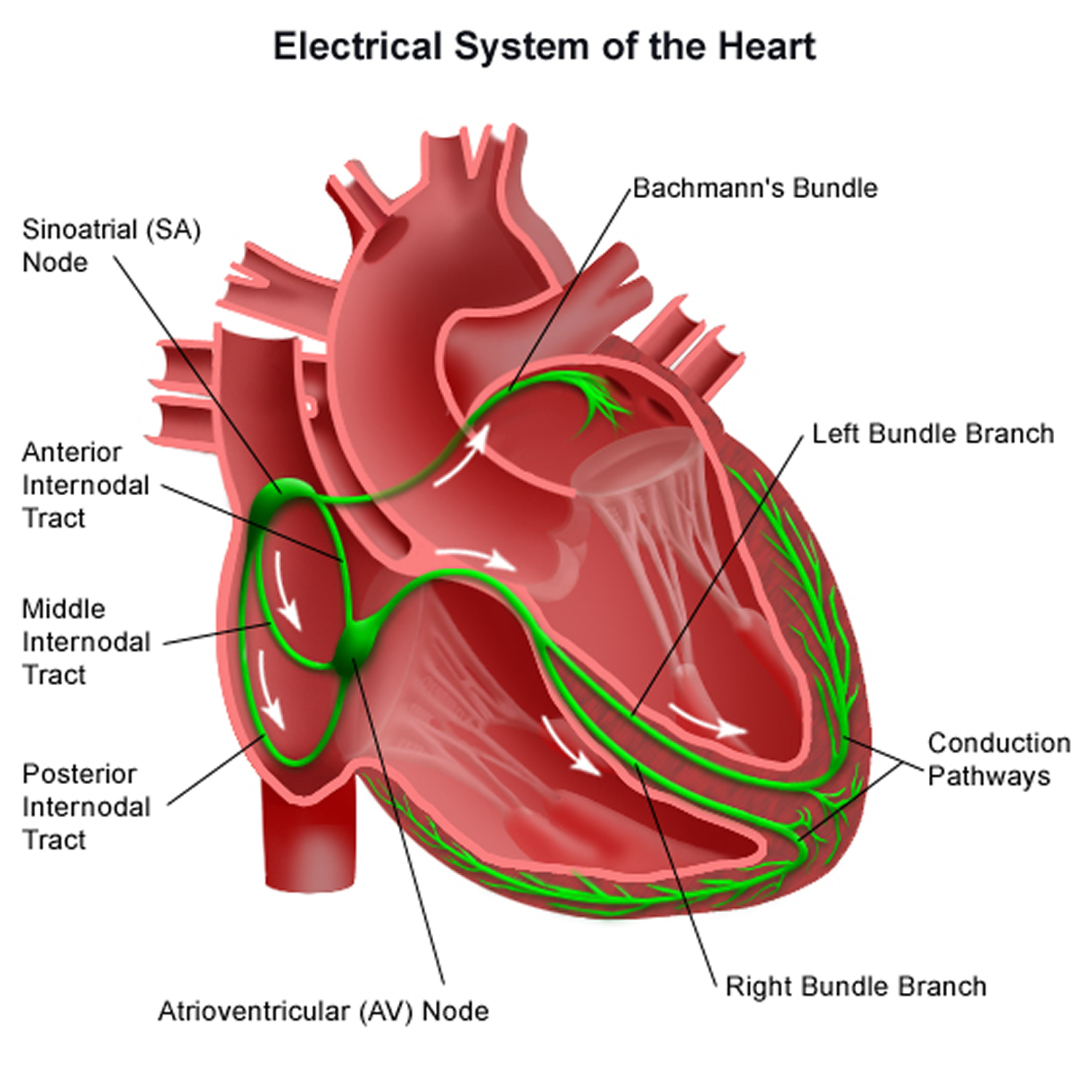
The pumping action of the heart is caused by a flow of electricity through the heart that repeats itself in a cycle. This is normally triggered by the heart’s natural pacemaker, the SA node (sino-atrial node), which is in the right atrium (see Figure 4 below). The SA node sends out regular electrical impulses, which make the atria contract and pump blood into the ventricles. The electrical impulse then passes to the ventricles through a form of ‘junction box’ called the AV node (atrio-ventricular node). This causes the ventricles to contract and pump blood out of the heart. The blood from the right ventricle goes through the pulmonary artery to the lungs, and the blood from the left ventricle goes through the aorta and then around the body.
Figure 1. The anatomy of the heart
Figure 2. The anatomy of the heart chambers
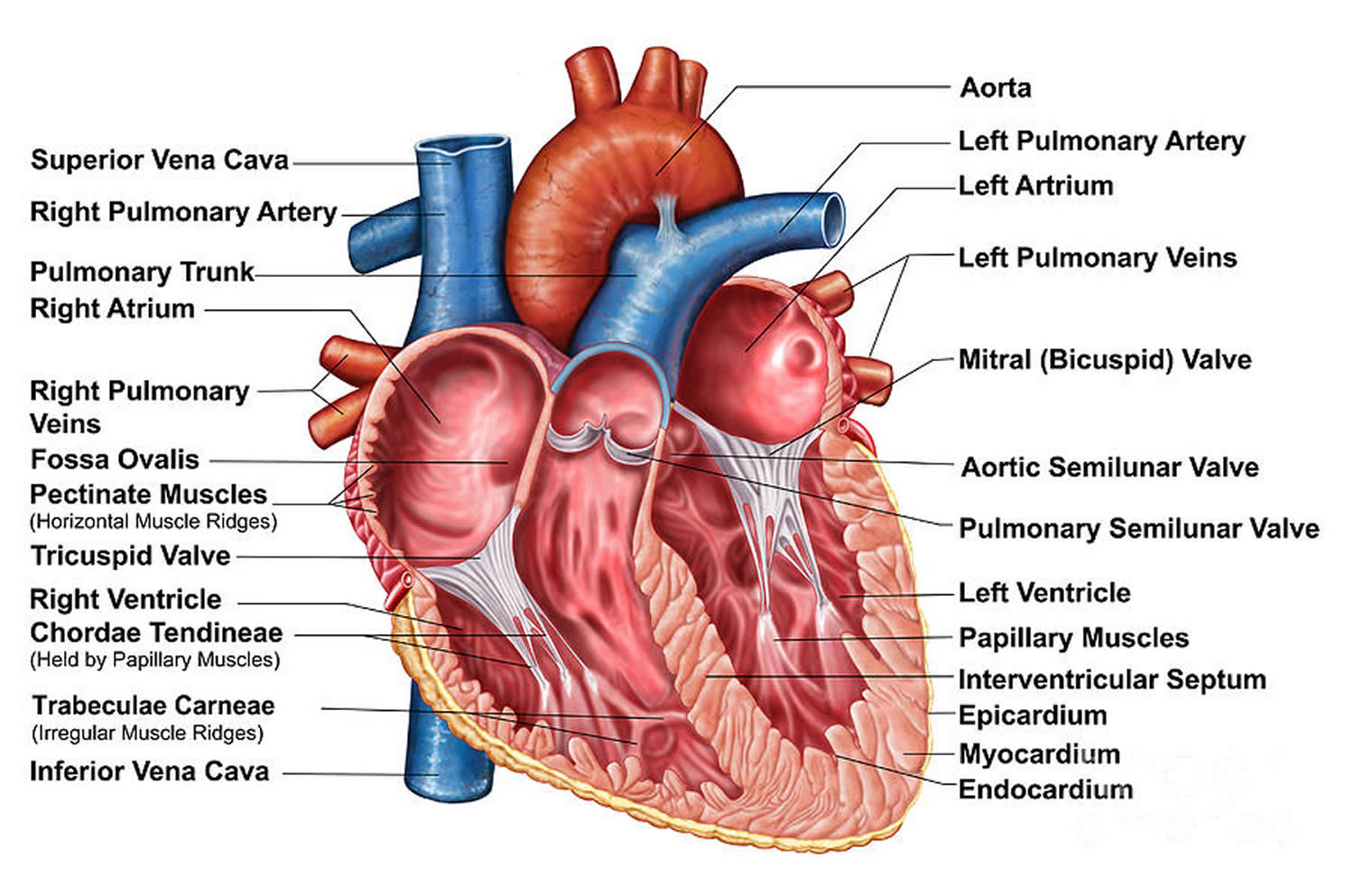 Figure 3. Normal heart blood flow
Figure 3. Normal heart blood flow
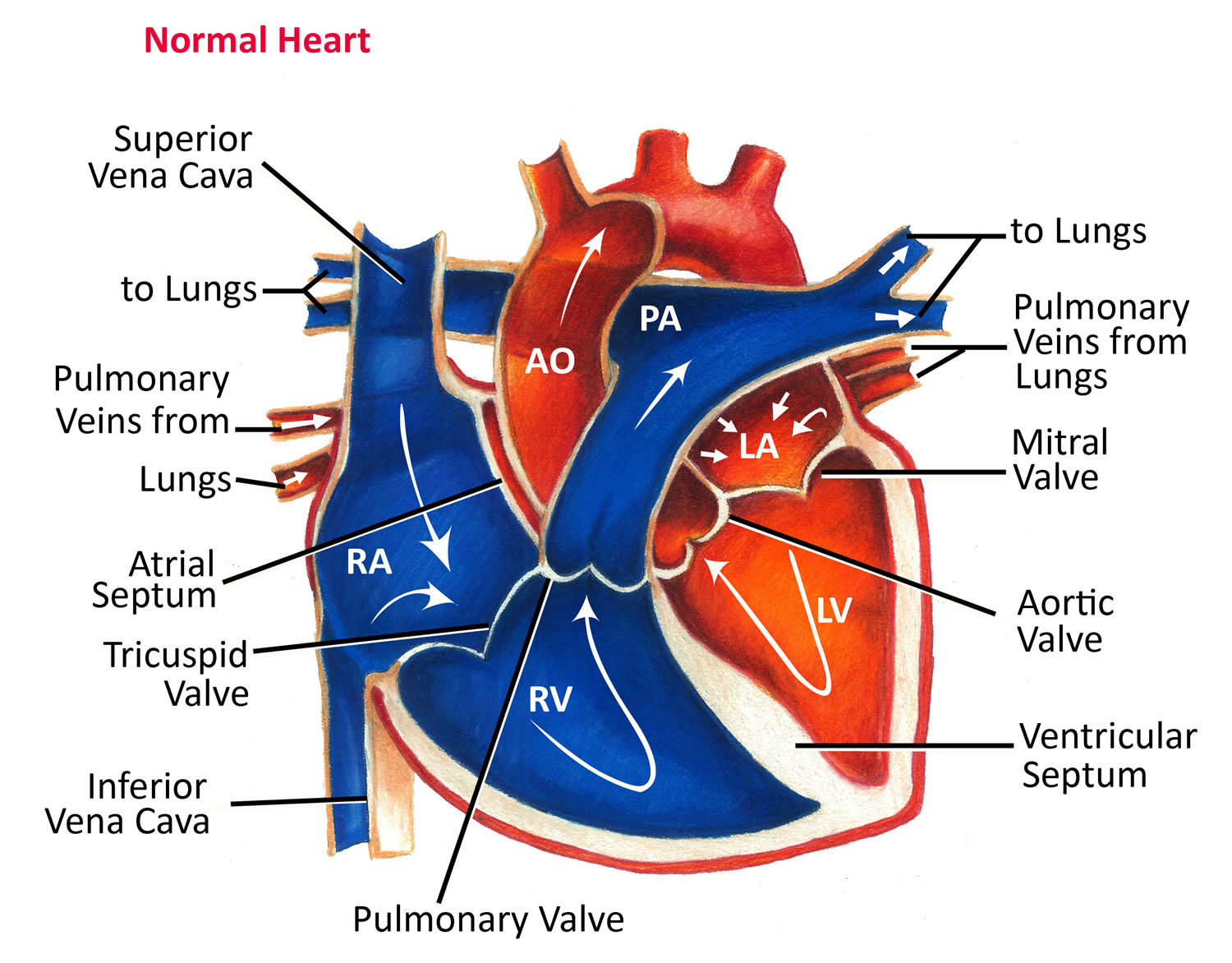 Figure 4. The heart’s electrical system
Figure 4. The heart’s electrical system
 Cardiomyopathy types
Cardiomyopathy types
- Dilated cardiomyopathy. In dilated cardiomyopathy or ‘enlarged’ heart, your heart muscle stretches and become thinner, so it hasn’t got the strength to beat properly. Dilated cardiomyopathy is the most common form of cardiomyopathy. The condition usually starts in the left ventricle and over time can affect the right ventricle. The weakened chambers of the heart don’t pump effectively, causing the heart muscle to work harder. Over time, the heart loses the ability to pump blood effectively. Dilated cardiomyopathy can lead to heart failure, heart valve disease, irregular heart rate, and blood clots in the heart.
- Restrictive cardiomyopathy. In restrictive cardiomyopathy or ‘stiff heart’, your heart becomes rigid and can’t relax enough to beat properly, but the walls of the heart do not thicken. As a result, the ventricles do not relax and don’t fill with the normal blood volume. As the disease progresses, the ventricles do not pump as well and the heart muscle weakens. Over time, restrictive cardiomyopathy can lead to heart failure and problems with the heart valves.
- Hypertrophic cardiomyopathy. In hypertrophic cardiomyopathy or ‘thickened muscle’, your heart muscle enlarges and the walls of the heart thicken – leaving too little room for blood in the heart. In hypertrophic cardiomyopathy there is a 50% chance of the condition passing from a parent to a child. Upon diagnosis, screening of close relatives is always recommended. There is no way of predicting how severe the condition may be in an affected individual. For this reason children in the family should be screened at regular intervals.
- Arrhythmogenic right ventricular cardiomyopathy. Arrhythmogenic right ventricular dysplasia is a rare type of cardiomyopathy that occurs when the muscle tissue in the right ventricle is replaced with fatty or fibrous tissue. This can lead to disruptions in the heart’s electrical signals and causes arrhythmias. Arrhythmogenic right ventricular dysplasia usually affects teens or young adults and can cause sudden cardiac arrest in young athletes.
- Other types of cardiomyopathy are grouped into this category and can include:
- Left ventricular noncompaction happens when the left ventricle has trabeculations, projections of muscle inside the ventricle.
- Takotsubo cardiomyopathy, or broken heart syndrome, happens when extreme stress leads to heart muscle failure. Though rare, this condition is more common in post-menopausal women.
Dilated cardiomyopathy
In dilated cardiomyopathy the muscle walls of the heart have become stretched (dilated) and thin, so the heart can’t contract (squeeze) properly to pump blood around the body. This can lead to fluid building up in the lungs, ankles, abdomen and other organs of the body and a feeling of being breathless. This collection of symptoms is known as heart failure.
In most cases dilated cardiomyopathy develops slowly, so the heart can be quite severely affected before someone is diagnosed. In some cases, there may also be mitral regurgitation. This is when some of your blood flows in the wrong direction through the mitral valve, from the left ventricle to the left atrium.
It is estimated that 750,000 people in the United States have dilated cardiomyopathy; roughly half of these cases are familial.
How serious is dilated cardiomyopathy?
If you have dilated cardiomyopathy, the left ventricle of your heart becomes dilated (stretched or ‘baggy’). As a result, the heart muscle becomes weak, thin or floppy and is unable to pump blood around the body efficiently.
If you have dilated cardiomyopathy, you’re at greater risk of heart failure, where the heart fails to pump enough blood around the body at the right pressure.
Heart failure typically causes shortness of breath, extreme tiredness and ankle swelling.
There’s also a risk of heart valve problems, an irregular heartbeat and blood clots. You’ll need to have regular appointments with your doctor so the disease can be monitored.
Dilated cardiomyopathy causes
Dilated cardiomyopathy can affect both children and adults. In most cases, the exact reason for dilated cardiomyopathy is unknown and the condition is called ‘idiopathic dilated cardiomyopathy’. Idiopathic means that there is no known cause.
Inherited dilated cardiomyopathy is caused by a change or mutation in one or more genes. If you have dilated cardiomyopathy, there is a 50 per cent chance that your child will inherit the condition.
Genetics
Research has shown that dilated cardiomyopathy can be linked to an individual’s genetic make-up 1. Scientists have identified some gene mutations that are known to affect the development of heart muscle, and that may cause dilated cardiomyopathy. However, there are many other gene mutations that may also cause the condition. This makes genetic testing of individuals to find out if they have the condition more difficult.
Mutations in more than 30 genes have been found to cause familial dilated cardiomyopathy 2. These genes provide instructions for making proteins that are found in cardiac muscle cells called cardiomyocytes.
Many of these proteins play important roles in the contraction of the cardiac muscle through their association with cell structures called sarcomeres. Sarcomeres are the basic units of muscle contraction; they are made of proteins that generate the mechanical force needed for muscles to contract. Many other proteins associated with familial dilated cardiomyopathy make up the structural framework (the cytoskeleton) of cardiomyocytes. The remaining proteins play various roles within cardiomyocytes to ensure their proper functioning.
Mutations in one gene, TTN, account for approximately 20 percent of cases of familial dilated cardiomyopathy 2. The TTN gene provides instructions for making a protein called titin, which is found in the sarcomeres of many types of muscle cells, including cardiomyocytes. Titin provides structure, flexibility, and stability to sarcomeres. Titin also plays a role in chemical signaling and in assembling new sarcomeres. The TTN gene mutations that cause familial dilated cardiomyopathy result in the production of an abnormally short titin protein. It is unclear how the altered protein causes familial dilated cardiomyopathy, but it is likely that it impairs sarcomere function and disrupts chemical signaling.
It is unclear how mutations in the other genes cause familial dilated cardiomyopathy. It is likely that the changes impair cardiomyocyte function and reduce the ability of these cells to contract, weakening and thinning cardiac muscle.
People with familial dilated cardiomyopathy often do not have an identified mutation in any of the known associated genes. The cause of the condition in these individuals is unknown.
Familial dilated cardiomyopathy is described as nonsyndromic or isolated because it typically affects only the heart. However, dilated cardiomyopathy can also occur as part of syndromes that affect other organs and tissues in the body. These forms of the condition are described as syndromic and are caused by mutations in other genes.
Familial dilated cardiomyopathy has different inheritance patterns depending on the gene involved.
In 80 to 90 percent of cases, familial dilated cardiomyopathy is inherited in an autosomal dominant pattern, which means one copy of the altered gene in each cell is sufficient to cause the disorder. In most cases, an affected person inherits the mutation from one affected parent. However, some people who inherit the altered gene never develop features of familial dilated cardiomyopathy. (This situation is known as reduced penetrance.) Other cases result from new mutations in the gene and occur in people with no history of the disorder in their family.
In rare instances, this condition is inherited in an autosomal recessive pattern, which means both copies of the gene in each cell have mutations. The parents of an individual with an autosomal recessive condition each carry one copy of the mutated gene, but they typically do not show signs and symptoms of the condition.
In other rare cases, this condition is inherited in an X-linked pattern. In these cases, the gene associated with this condition is located on the X chromosome, which is one of the two sex chromosomes. In females (who have two X chromosomes), a mutation in one of the two copies of the gene in each cell increases the risk of developing heart disease, but females with such a mutation may not develop familial dilated cardiomyopathy. In males (who have only one X chromosome), a mutation in the only copy of the gene in each cell causes familial dilated cardiomyopathy. A characteristic of X-linked inheritance is that fathers cannot pass X-linked traits to their sons.
Additionally, there are many nongenetic causes of dilated cardiomyopathy, including viral infection and chronic alcohol abuse.
The heart muscle can also become stretched if you have an unhealthy lifestyle or an underlying medical condition, or both.
The following can all play a role in the development of dilated cardiomyopathy:
- uncontrolled high blood pressure
- an unhealthy lifestyle – such as a lack of vitamins and minerals in the diet, heavy alcohol drinking and recreational drug use
- a viral infection that causes inflammation of the heart muscle
- a heart valve problem
- auto-immune disease, a disease of the body tissues or vessels – such as Wegener’s granulomatosis, sarcoidosis, amyloidosis, lupus, polyarteritis nodosa, vasculitis or muscular dystrophy
- inheriting a mutated (changed) gene that makes you more vulnerable to the disease.
- pregnancy – cardiomyopathy can sometimes develop as a complication of pregnancy
In some people with dilated cardiomyopathy there may be more than one reason to explain their condition. For example, some people may carry a gene mutation that makes them more vulnerable to viral infections in the heart.
Viral infections
We’re all exposed to many viruses every day. Normally, your body’s immune system is very efficient at dealing with these viruses. However, sometimes a virus can affect the heart muscle of an apparently well person, even though the person has no other symptoms of having a virus. This is known as viral myocarditis.
Viral myocarditis is commonly caused by a number of different viruses. It is thought that dilated cardiomyopathy may occur when your heart muscle is badly damaged by the initial infection. Or it may be that the virus triggers your body’s own defence system (the immune system) which then attacks and damages your heart muscle.
Auto-immune disease
Your body’s immune system is responsible for defending your body against infection – for example, against viruses and bacteria. Sometimes your immune system breaks down and starts to attack your body’s own tissues. This is called auto-immune disease. Some people who are diagnosed with dilated cardiomyopathy appear to have this condition.
Exposure to toxins or certain medicines
In very rare cases, exposure to certain chemicals can cause dilated cardiomyopathy. In these cases, scientists don’t know if the person developed the condition because they already had a genetic tendency to develop it, or whether the toxins caused the cardiomyopathy.
Some anti-cancer medicines, such as anthracyclines, can cause dilated cardiomyopathy. These medicines are a very effective treatment for cancer, but they are toxic and can have harmful effects on your heart muscle, which can lead to dilated cardiomyopathy. The risk of this happening is usually related to the total dose of anthracyclines received.
If you’ve had treatment with anthracyclines, you should be seen by a cardiologist (heart specialist) at least once a year. If you know that you have a heart condition and that you will need treatment for cancer, you should discuss this with your cardiologist before you start the treatment.
In some cases, alcohol can be the cause of dilated cardiomyopathy. Over time, regularly drinking too much alcohol can weaken your heart by damaging your heart muscle. It can take years for dilated cardiomyopathy to develop and so the effects on your heart may not be seen immediately.
Pregnancy
In developed countries, up to one in every 2000 women may develop dilated cardiomyopathy during pregnancy. It can occur from mid to late pregnancy or soon after delivery and is known as peripartum cardiomyopathy. It’s possible that, in these circumstances, some women may have already had dilated cardiomyopathy but it had not been diagnosed.
For most women, the dilated heart returns to normal within six to eight weeks of the delivery, provided they get the appropriate treatment. However, it’s possible that the condition could develop again in subsequent pregnancies.
If you’ve had peripartum cardiomyopathy and have not fully recovered from it, your doctor may advise you not to have any more children.
Women who have dilated cardiomyopathy or peripartum cardiomyopathy should seek specialist advice before planning another baby or if they find themselves unexpectedly pregnant. This is particularly important if you’re receiving medication for your cardiomyopathy, as this can affect the baby.
Dilated cardiomyopathy symptoms
Most people who are affected by dilated cardiomyopathy remain well. Some people have a few symptoms and others may develop problems which need more complex treatment.
In most cases dilated cardiomyopathy develops slowly, so some people can have quite severe symptoms before they are diagnosed.
The symptoms of dilated cardiomyopathy are similar to those of heart failure. Heart failure is a term used to describe a group of symptoms caused when your heart muscle becomes less efficient at pumping blood around your body.
The symptoms of heart failure include:
- Shortness of breath
- Swelling of the ankles, feet, lower back and abdomen
- Excessive tiredness
- Palpitations. This is the sensation of your own heart beating and can feel like extra or skipped beats. In some cases, palpitations may start suddenly and feel very fast, and may be accompanied by sweating or light-headedness.
Not everyone who has dilated cardiomyopathy goes on to develop all the symptoms of heart failure. The symptoms usually come on slowly, but sometimes they can come on suddenly. Once the condition has been diagnosed, in most cases dilated cardiomyopathy symptoms can be controlled with medication or other treatments.
Dilated cardiomyopathy complications
Some people with dilated cardiomyopathy can develop a number of other conditions, which include:
- Arrhythmias
- Blood clots
- Angina
- Heart murmurs
Arrhythmias
Arrhythmias are a common complication in people with dilated cardiomyopathy.
When your heart muscle becomes dilated, it stretches the cells in the heart muscle and can cause scars to develop. These abnormalities can interfere with the way that the electrical impulses pass through your heart muscle and can lead to slow, fast or erratic abnormal heart rhythms known as arrhythmias.
Arrhythmias can cause a fall in blood pressure and lead to episodes of dizziness or cause blackouts. They can sometimes slow the flow of blood through your heart and lead to an increased risk of having a stroke. If this is the case, your cardiologist will prescribe anticoagulants for you to reduce that risk.
Some arrhythmias need to be corrected by delivering a controlled electric shock. This procedure is known as a cardioversion.
In atrial fibrillation – an abnormal heart rhythm – the heart electrical impulses are sent from different places (apart from the heart’s natural pacemaker [the SA node]) in the atria in a disorganised way. This makes your heart beat uncontrollably and often very fast. It can lead to feelings of palpitations or fluttering in your chest. The condition can usually be controlled with medication.
Ventricular tachycardias are arrhythmias that affect the ventricles, the lower pumping chambers of your heart. Electrical signals in the ventricles become disorganised and take over the heartbeat independently from the SA node. This leads to a rapid heartbeat. Ventricular tachycardias can be controlled with medication, but they can sometimes lead to more life-threatening arrhythmias and the risk of sudden death.
Ventricular ectopics usually occur as single extra beats, originating in the ventricles. They should be investigated to rule out a serious arrhythmia, but they normally don’t need any further treatment. They can be found in healthy people too.
Heart block can occur in a small number of people with dilated cardiomyopathy. This is when the electrical impulse travels down to the ventricles slowly, or may even be completely blocked. This affects the way that your heart contracts, and often causes your heart to beat too slowly.
Blood clots
People with dilated cardiomyopathy have an increased risk of blood clots forming in the heart, because the blood flows through the heart more slowly than normal. The formation of clots increases the risk of having a stroke. Some people with dilated cardiomyopathy will be prescribed anticoagulants to reduce this risk.
Angina
Angina is usually caused by a narrowing of the coronary arteries, the blood vessels that supply blood to your heart muscle, and causes symptoms such as chest pain. If a coronary artery becomes completely blocked, it can cause a heart attack. However, in people with dilated cardiomyopathy, angina is usually caused by the high pressure on the dilated wall of the left ventricle. This pressure reduces the supply of blood to your heart muscle, causing chest tightness or pain. Treatment for this is usually medication to reduce the pressure and widen the arteries.
Heart murmurs
Heart murmurs are extra or unusual sounds from your heart that can be heard through a stethoscope. In people with dilated cardiomyopathy it is usually caused by a structural problem in the heart valves such as a leaking heart valves. If your doctor hears a heart murmur, they may send you for an echocardiogram to check the structure of your heart.
Is there a risk of sudden death in people with dilated cardiomyopathy?
Dilated cardiomyopathy is a common condition, and the majority of affected people remain well and have few or no symptoms. Research has shown that, with proper treatment and follow-up, most people with dilated cardiomyopathy live a normal life. However, because there is a very small risk of developing a life-threatening arrhythmia, a small proportion of people with dilated cardiomyopathy are at risk of sudden death.
Some arrhythmias can cause your heart to beat too fast and chaotically, eventually causing your heart to stop beating. This is a cardiac arrest and can lead to sudden death. This is different to a heart attack, which happens when one of the coronary arteries that supply your heart with blood becomes blocked and the heart muscle which it supplies may be starved of oxygen.
Dilated cardiomyopathy treatment
At present there is no cure for dilated cardiomyopathy. However, treatment with medicines helps to control symptoms and reduce your risk of the condition getting worse or of getting new symptoms. Some people may need to have a pacemaker or an ICD (implantable cardioverter defibrillator) fitted. In some very rare cases, a heart transplant may be considered.
Hypertrophic cardiomyopathy
Hypertrophic cardiomyopathy is an inherited disease of your heart muscle, where the muscle wall of your heart becomes thickened. Hypertrophic cardiomyopathy is caused by a change or mutation in one or more genes and is passed on through families. Each child of someone with hypertrophic cardiomyopathy has a 50 per cent chance of inheriting the condition. Most often diagnosed during infancy or adolescence, hypertrophic cardiomyopathy is the second most common form of heart muscle disease and comprises about 35–40% of cardiomyopathies in children.
Hypertrophic cardiomyopathy is very common and can affect people of any age. Hypertrophic cardiomyopathy affects men and women equally.
About 1 in 500 of the US population has hypertrophic cardiomyopathy, although most people who have hypertrophic cardiomyopathy have few, if any, symptoms. Hypertrophic cardiomyopathy affects up to 500,000 people in the United States. with children under age 12 accounting for less than 10% of all cases. According to the Pediatric Cardiomyopathy Registry, Hypertrophic cardiomyopathy occurs at a rate of five per 1 million children.
If you have hypertrophic cardiomyopathy, the muscular wall of your heart – the myocardium – becomes thickened without an obvious cause, making the heart muscle stiff. Usually the ventricles, the lower chambers of the heart, and septum (the wall that separates the left and right side of the heart) thicken. The thickened areas create narrowing or blockages in the ventricles, making it harder for the heart to pump blood. Hypertrophic cardiomyopathy also can cause stiffness of the ventricles, changes in the mitral valve, and cellular changes in the heart tissue.
This thickening makes it harder for your heart to pump blood out of your heart and around your body.
How thick your muscle is and how much of your muscle is affected, varies from one person to another. The left ventricle (one of your heart’s four chambers) is almost always affected, and in some people the muscle of the right ventricle also thickens.
How serious is hypertrophic cardiomyopathy?
Most people with hypertrophic cardiomyopathy will be able to live a full, normal life. Some people don’t even have symptoms and don’t need treatment.
But that doesn’t mean the condition can’t be serious. Hypertrophic cardiomyopathy is the most common cause of sudden unexpected death in childhood and in young athletes.
The main heart chambers can become stiff, leading to back pressure on the smaller collecting chambers. This can sometimes worsen the symptoms of heart failure and lead to abnormal heart rhythms (atrial fibrillation).
Blood flow from the heart may become reduced or restricted (known as obstructive hypertrophic cardiomyopathy).
Also, the mitral heart valve can become leaky (mitral regurgitation), causing blood to leak backwards.
These heart changes can cause dizziness, chest pain, shortness of breath and temporary loss of consciousness.
You’ll also be at greater risk of developing endocarditis (a heart infection).
If you have severe hypertrophic cardiomyopathy, you’ll need to see your doctor regularly so your condition can be monitored.
Your doctor will advise about the level and amount of exercise you can do and sensible lifestyle changes to make.
Hypertrophic cardiomyopathy prognosis (outlook)
Research has shown that, with proper treatment and follow-up, most people with hypertrophic cardiomyopathy live a normal life.
However, because there is a very small risk of getting a life-threatening abnormal heart rhythm, a small number of people with hypertrophic cardiomyopathy are at risk of sudden cardiac death. It’s important to discuss this risk with your doctor, who may offer medication or advise that you need to have an implantable cardioverter defibrillator (ICD) fitted if you are at an increased risk.
You may have to make some small changes to your lifestyle, such as avoiding competitive sports, but you should be able to continue to work and drive a car, for example.
However, you will not be able to drive a commercial passenger vehicle and you may have to reconsider manual jobs which involve strenuous activity.
Hypertrophic cardiomyopathy symptoms
Common symptoms include:
- Shortness of breath
- Chest pain
- Palpitations
- Light headedness and fainting
You may find that you never have any serious problems related to your condition, and with treatment, your symptoms should be controlled. However some people may find that their symptoms worsen or become harder to control in later life.
The area of heart muscle that is affected by hypertrophic cardiomyopathy and the amount of stiffening that occurs will determine how the symptoms affect you.
For some people, a number of other conditions can develop as a result of having hypertrophic cardiomyopathy. These may include abnormal heart rhythms, or arrythmias, including heart block and endocarditis.
Hypertrophic cardiomyopathy diagnosis
The most common tests for hypertrophic cardiomyopathy are:
- ECG – this records the electrical activity of your heart.
- Echocardiogram – this shows the pumping action of your heart.
- Exercise test – in this test, an ECG is recorded while you’re on a treadmill or an exercise bike, to see how your heart works when it’s more active.
- MRI scan – creates detailed images of your internal organs, such as your heart.
Genetic testing for hypertrophic cardiomyopathy
Hypertrophic cardiomyopathy is an inherited heart condition, which means that it’s passed on through families. If your doctor thinks that you have hypertrophic cardiomyopathy, you may be offered a genetic test to identify a faulty gene that may be causing your condition.
If you’re found to have a faulty gene, your specialist may ask for your help in identifying close relatives – such as parents, siblings or children – who may have also inherited this gene.
Being tested as soon as possible means that your treatment can start as quickly as possible, which will reduce your risk of developing life-threatening abnormal heart rhythms.
Hypertrophic cardiomyopathy treatment
At present there is no cure for hypertrophic cardiomyopathy, but treatments are available to help control your symptoms and prevent complications. Your treatment will depend on how your heart is affected and what symptoms you have.
You may need:
- Medicines – to help control your blood pressure, abnormal heart rhythms or other symptoms you may have
- A Pacemaker – to control your heart rate
- An implantable cardioverter defibrillator (ICD) – if you are at risk of having a life threatening abnormal heart rhythm.
Restrictive cardiomyopathy
Restrictive cardiomyopathy is rare and mostly affects older adults. The walls of the main heart chambers become stiffened and rigid and can’t relax properly after contracting. This means the heart can’t fill up properly with blood.
In restrictive cardiomyopathy, the muscle cells in the heart become replaced with abnormal tissue (such as scar tissue). This causes the muscle walls of the ventricles (the lower chambers of the heart) to become stiff, which restricts the movement of the heart. The pumping action of the heart is not usually affected, and the heart can contract to pump blood around the body. However, it is the filling function of the heart, where the heart muscle relaxes and the ventricles fill with blood, that is affected.
The stiffened muscle of the ventricles does not relax properly which means that the ventricles can’t fill with blood. This poor filling function means that the ventricles receive less blood than normal, and so blood flow around the body and the heart is reduced. Also, blood gets ‘backed up’ as it cannot enter the heart as normal, which causes a build-up of pressure. This can cause the atria (top chambers of the heart) to enlarge.
This results in reduced blood flow from the heart and can lead to symptoms of heart failure, such as breathlessness, tiredness and ankle swelling, as well as heart rhythm problems.
In many cases the cause of restrictive cardiomyopathy is unknown, although sometimes it can be inherited.
Restrictive cardiomyopathy is relatively rare compared to other types of cardiomyopathy. It is most often diagnosed in children (rather than adults) at 5 – 6 years of age, although it can develop at any age.
Restrictive cardiomyopathy causes
Although the cause of restrictive cardiomyopathy is often unknown, it can be genetic and run in families. It can also develop due to other conditions such as:
- scar tissue in the heart;
- amyloidosis – a condition where there is too much of an abnormal protein (called amyloid) in the body, and when it builds up in the heart muscle it can cause restrictive cardiomyopathy;
- hemochromatosis – a condition where too much iron from the diet is absorbed and it builds up in the organs, including the heart; and
- following some treatments for cancer, such as radiation therapy.
Restrictive cardiomyopathy symptoms
Some people have no symptoms of restrictive cardiomyopathy, or very mild symptoms. But over time, the restricted function of the heart can lead to heart failure (where the heart fails to pump enough blood, at the right pressure, to meet the body’s needs). This can cause symptoms, which develop as the heart’s function reduces. Symptoms can include the following:
- tiredness due to reduced blood flow and oxygen levels;
- shortness of breath due to fluid around the lungs (which might be when exercising, but can develop and happen even when resting);
- swelling in the abdomen and ankles due to oedema (a build up of fluid caused by reduced blood flow through the heart);
- arrhythmias (abnormal heart rhythms, where the heart beats too fast, too slow or erratically) caused by disrupted electrical signals in the heart;
- palpitations (feeling your heart beating or like it is ‘fluttering’), caused by arrhythmias;
- chest pain (which may be caused by reduced blood flow from the heart);
- a cough;
- loss of appetite;
- weight gain; and
- fainting (due to reduced oxygen and blood flow to the brain).
In some people, how the electrical messages are transmitted through the heart can become slowed or blocked. This is called ‘heart block’, and can cause symptoms such as breathlessness, dizziness and palpitations.
Restrictive cardiomyopathy diagnosis
As symptoms can be subtle to start with, diagnosis may be difficult. A diagnosis might involve some or all of the following tests.
- Medical history – to look at symptoms and whether other family members have this condition (as it can be genetic).
- Physical exam – to see what physical symptoms, if any, are happening.
- ECG (electrocardiogram) – to look at the conduction of electrical impulses through the heart and see if arrhythmias are happening.
- Echo (echocardiogram) and MRI (magnetic resonance imaging) scan – types of scan that show the structure of the heart. They can also show how the heart is working and the flow of blood through the heart.
Additional tests are not always needed, but might include the following:
- Cardiac catheterisation – this involves a thin plastic tube (a catheter) being inserted through the blood vessels into the heart. This allows tests to be done such as measuring the pressure within the heart’s chambers, and using ultrasound or x-rays to show the structure and function of the heart.
- Myocardial biopsy – this is rarely done, but might help to identify the cause of the someone’s restrictive cardiomyopathy. It involves surgically removing a small piece of heart muscle, which is then examined. This is more likely to be done in adults than in children.
- A bone scan might be suggested if the restrictive cardiomyopathy could be caused by amyloidosis.
There may be other tests suggested, depending on what the doctors think could be the cause of the restrictive cardiomyopathy. If this is the case, they will talk to about what the other tests are, and what they are used for.
Restrictive cardiomyopathy treatment
Although restrictive cardiomyopathy cannot be cured, treatment aims to reduce and control symptoms, particularly those of heart failure. Some treatments may not be suitable, depending on the underlying cause of the restrictive cardiomyopathy. Treatment may involve any of the following.
Medication
- ACE inhibitors (angiotensin-converting enzyme inhibitors) – relax the smooth muscle around the blood vessels to reduce the workload on the heart, and
- duce the volume of the blood, making it easier for the heart to work.
- Anti-arrhythmic medication – reduces abnormal heart rhythms.
- Anticoagulants (blood thinners) – may be used in people with arrhythmias to reduce the risk of blood clots forming, which could lead to a stroke.
- Beta-blockers – reduce the rate and force of the heart’s contraction, by reducing stimulation of adrenalin (which would normally make the heart beat faster).
- Calcium channel blockers – reduce the force at which the heart contracts. This can help to reduce blood pressure, chest pain and arrhythmias.
- Diuretics (water tablets) – reduce the build-up of fluid on the lungs or the ankles by encouraging the kidneys to get rid of water as urine.
- Vasodilators – relax and widen the blood vessels, helping blood to flow more easily.
Other treatments
- Life-style changes – such as a healthy diet, low salt intake, exercise, and avoiding alcohol, caffeine and smoking, may all help symptoms of heart failure.
- Diet – some children with restrictive cardiomyopathy have difficulties gaining weight, which can affect their growth. They might need a special high-calorie diet to help them to gain weight.
- Pacemaker – may be recommended for people who have heart block due to restrictive cardiomyopathy (which makes the heart rate slow down). Pacemakers take over the electrical signalling of the heart to keep a normal heart rhythm.
- Left ventricular assist devices (LVADs) – these artificial pumps are used to help the heart to pump blood around the body. They are used for severe heart failure, and often for people while they are waiting for a transplant.
- Heart transplant – in some cases, people with restrictive cardiomyopathy require a heart transplant, if their heart function is very poor.
- Treatment for other conditions – if the restrictive cardiomyopathy is caused by another underlying condition, this might be treated separately.
Arrhythmogenic right ventricular cardiomyopathy
Arrhythmogenic right ventricular cardiomyopathy is an uncommon inherited condition, which means that it’s passed on through families. It is caused by a change or mutation in one or more genes. The chances of inheriting arrhythmogenic right ventricular cardiomyopathy vary, and you might inherit the mutation but not develop the condition.
Arrhythmogenic right ventricular cardiomyopathy can affect teenagers or young adults and has been the reason for some sudden unexplained deaths in young athletes.
In arrhythmogenic right ventricular cardiomyopathy, the proteins that normally hold the heart muscle cells together are abnormal. The muscle cells become detached and fatty deposits build up in an attempt to repair the damage. Muscle cells can die and the dead muscle tissue is replaced with fatty and fibrous tissue. The condition is usually progressive, which means that it will get worse over time.
The walls of the main heart chambers become thin and stretched, and can’t pump blood around the body properly.
Arrhythmogenic right ventricular cardiomyopathy usually affects the right side of your heart but it can affect both sides. The changes to the heart muscle mean the walls of the ventricle – one of four chambers in your heart – become thin and stretched. This means your heart doesn’t pump blood around your body properly.
Arrhythmogenic right ventricular cardiomyopathy can also cause abnormal heart rhythms, because your heart’s normal electrical impulses are disrupted as they pass through areas of damaged and scarred muscle cells. It usually takes many years for this to happen so most people are not diagnosed until later in life.
People with arrhythmogenic right ventricular cardiomyopathy typically have heart rhythm problems. Reduced blood flow from the heart can also lead to symptoms of heart failure.
There’s increasing evidence that prolonged, strenuous exercise worsens the symptoms of arrhythmogenic right ventricular cardiomyopathy. It’s important that people with or at risk of arrhythmogenic right ventricular cardiomyopathy have a careful discussion about this with their cardiologist.
Arrhythmogenic right ventricular cardiomyopathy symptoms
Arrhythmogenic right ventricular cardiomyopathy has four phases. Not everyone will develop all of the phases or be affected in the same way. Many people with the condition never develop any serious problems.
1. Concealed phase
There are small changes in the right ventricle.
2. Overt phase
There are noticeable structural changes to your heart muscle. These changes affect the pumping action of the heart and cause abnormal heart rhythms.
3. Weakening of the right ventricle
Your right ventricle becomes stretched and its pumping action becomes weaker.
4. Weakening of the left ventricle
Your left ventricle is also affected. The pumping action of both your ventricles becomes weaker.
If you have arrhythmogenic right ventricular cardiomyopathy, you may have one or more of the following symptoms:
- Palpitations
- Light-headedness
- Fainting
- Breathlessness
- Abnormal heart rhythms
- Swollen ankles or legs
- Swelling in the abdomen
- Risk of sudden death on exertion
Arrhythmogenic right ventricular cardiomyopathy diagnosis
It can be difficult to diagnose arrhythmogenic right ventricular cardiomyopathy, because the changes to the heart muscle are often very minor or build up in a ‘patchy’ pattern. Many of the changes and symptoms could also be caused by a number of other conditions, making diagnosis even more difficult.
Your doctor may suspect that you have arrhythmogenic right ventricular cardiomyopathy because of your symptoms, or because of the results of a chest x-ray. Or you may be going for tests because someone else in your family has been diagnosed with the condition.
The most common tests for this cardiomyopathy are an ECG, which records the electrical activity of your heart, and an echocardiogram, which shows the pumping action of your heart.
Your doctor may also arrange for you to have an exercise test, signal averaged electrocardiogram or MRI scan.
Arrhythmogenic right ventricular cardiomyopathy treatment
There are three aims for treatment:
- To identify those at risk of sudden cardiac death
- To prevent or control arrhythmias (abnormal heart rhythms)
- To improve the pumping action of the heart muscle
Arrhythmogenic right ventricular cardiomyopathy is not curable, but most of the symptoms caused by the condition can be controlled using medicines. You may also undergo treatments such as cardioversion or catheter ablation. Your treatment may stay the same for many years, or may change more frequently. It’s different for everyone.
Arrhythmogenic right ventricular cardiomyopathy prognosis
Research has shown that with proper treatment and follow-up, most people with arrhythmogenic right ventricular cardiomyopathy are able to control their symptoms and live a normal life.
Most people with arrhythmogenic right ventricular cardiomyopathy are at low risk of sudden cardiac death. However, there are certain times – known as ‘hot phases’ – when the disease becomes more active and this increases the risk of sudden cardiac death. Unexplained dizzy spells, sustained palpitations, or blackouts can be signs of a hot phase.
If you experience any of these symptoms, you should see your doctor immediately. Hot phases may come and go, but they could be a sign that the disease is progressing. This is why regular monitoring and follow-up with your doctor are important. If you are at high risk of sudden cardiac death, your doctor may advise that you have an implantable cardioverter defibrillator (ICD) fitted.
You may have to make some changes to manage your symptoms, but you should be able to drive a car and continue to work for example. However, you will not be able to drive a commercial passenger vehicle and there may be some restrictions on your employment depending on your type of work.
Cardiomyopathy prognosis
Cardiomyopathy life expectancy depends on the causes, types and severity of the cardiomyopathy. Cardiomyopathy may have no signs or symptoms and need no treatment. But other cases of cardiomyopathy, the disease develops quickly with severe symptoms, and serious complications occur.
In children with dilated cardiomyopathy, approximately 35% recover completely, 35% stabilize and the remaining may progressively worsen. Children with dilated cardiomyopathy are more prone to congestive heart failure and have a higher rate of heart transplantation compared with other forms of cardiomyopathy. However, improved medical therapy may eventually change this scenario. Current average five-year survival rates for children with dilated cardiomyopathy are 40–50%. If the cause of dilated cardiomyopathy is myocarditis, children are more likely to improve and have a better outcome than children with other causes of dilated cardiomyopathy.
Dilated cardiomyopathy
This has a poor prognosis. Fifty percent of patients die within 2 years; 25% of patients survive longer than 5 years. The two most common causes of death are progressive cardiac failure and arrhythmia.
Hypertrophic cardiomyopathy
The overall annual mortality from sudden death is 3-5% in adults and at least 6% in children and young adults. However, severity of disease and prognosis varies widely according to the genetic features involved. Certain genes are associated with a worse prognosis.
Restrictive cardiomyopathy
The worst prognosis is in patients with cardiac amyloidosis, in whom disease may recur after transplantation. Overall this disease has a poor diagnosis with many patients dying within a year of the diagnosis.
Arrhythmogenic right ventricular cardiomyopathy
This condition often leads to heart failure and sudden cardiac death as people are often unaware they have this condition as it is asymptomatic.
Cardiomyopathy causes
Cardiomyopathy can be acquired or inherited. “Acquired” means you aren’t born with the disease, but you develop it due to another disease, condition, or factor.
“Inherited” means your parents passed the gene for the disease on to you. Researchers continue to look for the genetic links to cardiomyopathy and to explore how these links cause or contribute to the various types of the disease.
Many times, the cause of cardiomyopathy isn’t known. This often is the case when the disease occurs in children.
Cardiomyopathy is sometimes also called either primary or secondary. In primary cardiomyopathy, the cause is not known, while in secondary cardiomyopathy, tests are able to show the cause.
The main causes of cardiomyopathy are:
- Heavy alcohol consumption
- A heart attack or coronary heart disease
- Family history of cardiomyopathy
- Viral infections. Most viral infections don’t cause heart problems, but occasionally a viral infection can affect the heart, causing cardiomyopathy.
- Hereditary factors. Some types of cardiomyopathy are inherited and affect several members of the same family.
- Coronary heart disease. As well as causing heart attacks, narrowing of the coronary arteries can cause cardiomyopathy.
- Uncontrolled high blood pressure.
- Certain chronic conditions, including diabetes and thyroid disease.
- Sometimes cardiomyopathy can develop during pregnancy.
- Connective tissue diseases such as rheumatoid arthritis, can be associated with cardiomyopathy.
- Conditions such as haemochromatosis, sarcoidosis and amyloidosis can damage the heart muscle.
- Drug use, including cocaine, amphetamines and anabolic steroids, can increase your risk of cardiomyopathy.
- Nutritional deficiencies. Lack of essential nutrients, such as thiamine, can lead to cardiomyopathy.
- Side effects from some cancer treatments (such as certain chemotherapy drugs and radiation therapy) can also cause some types of cardiomyopathy.
Hypertrophic Cardiomyopathy
Hypertrophic cardiomyopathy usually is inherited. About 50% of cases are familial (i.e. inherited). The type of inheritance is called autosomal dominant which means the abnormal gene only needs to be passed from one parent for offspring to get the disorder. The genes involved are associated with the heart’s contractile mechanism so that when they are abnormal the muscle becomes thick and overactive. It’s caused by a mutation or change in some of the genes in heart muscle proteins. Hypertrophic cardiomyopathy also can develop over time because of high blood pressure, aging, or other diseases, such as diabetes, thyroid disease, Friedrich’s ataxia and Noonan’s syndrome. Sometimes the cause of the disease isn’t known.
Dilated Cardiomyopathy
The cause of dilated cardiomyopathy often isn’t known. About one-third of the people who have dilated cardiomyopathy inherit it from their parents.
Certain diseases, conditions, and substances also can cause the disease, such as:
- Alcohol, especially if you also have a poor diet
- Certain toxins, such as poisons and heavy metals, including the chemotherapy drug doxorubicin
- Complications during the last months of pregnancy
- Coronary heart disease, heart attack, high blood pressure, diabetes, thyroid disease, viral hepatitis, and HIV
- Illegal drugs, such as cocaine and amphetamines, and some medicines used to treat cancer
- Other diseases: Haemochromatosis, sarcoidosis, systemic lupus erythematosus (SLE), systemic sclerosis and muscular dystrophy have all been associated with dilated cardiomyopathy.
- Infections, especially viral infections that inflame the heart muscle (myocarditis), from coxsackie virus B and others.
Restrictive Cardiomyopathy
Certain diseases, conditions, and factors can cause restrictive cardiomyopathy, including:
- Amyloidosis: A disease in which abnormal proteins build up in the body’s organs, including the heart
- Connective tissue disorders
- Hemochromatosis: A disease in which too much iron builds up in the body. The extra iron is toxic to the body and can damage the organs, including the heart.
- Sarcoidosis: A disease that causes inflammation and can affect various organs in the body. Researchers believe that an abnormal immune response may cause sarcoidosis. This abnormal response causes tiny lumps of cells to form in the body’s organs, including the heart.
- Some cancer treatments, such as radiation and chemotherapy
- Endomyocardial fibrosis (a disease occurring mainly in Africa and tropical areas);
- Loeffler’s endocarditis (a disease causing fibrosis and thickening of cardiac muscle).
Arrhythmogenic Right Ventricular Dysplasia
Researchers think that arrhythmogenic right ventricular dysplasia is an inherited disease.
Risk Factors for developing cardiomyopathy
People of all ages and races can have cardiomyopathy. However, certain types of the disease are more common in certain groups.
Dilated cardiomyopathy is more common in African Americans than Whites. This type of the disease also is more common in men than women.
Teens and young adults are more likely than older people to have arrhythmogenic right ventricular dysplasia, although it’s rare in both groups.
Major Risk Factors
Certain diseases, conditions, or factors can raise your risk for cardiomyopathy. Major risk factors include:
- A family history of cardiomyopathy, heart failure, or sudden cardiac arrest
- A disease or condition that can lead to cardiomyopathy, such as coronary heart disease, heart attack, or a viral infection that inflames the heart muscle
- Diabetes or other metabolic diseases, or severe obesity
- Diseases that can damage the heart, such as hemochromatosis, sarcoidosis, or amyloidosis
- Long-term alcoholism
- Long-term high blood pressure
Some people who have cardiomyopathy never have signs or symptoms. Thus, it’s important to identify people who may be at high risk for the disease. This can help prevent future problems, such as serious arrhythmias (irregular heartbeats) or sudden cardiac arrest.
Complications of cardiomyopathy
There are several serious complications associated with cardiomyopathy. Some types of cardiomyopathy are more likely to cause complications than others.
Heart failure
Heart failure is a common complication and can happen with all types of cardiomyopathy. Heart failure does not mean a sudden giving up of your heart, but is when your heart is not pumping blood around your body as well as it should. It can lead to symptoms such as swollen legs and ankles, as well as feeling short of breath when lying down.
Arrhythmias and sudden death
Arrhythmias are an abnormal heart rhythm. Some types of arrhythmias are life-threatening, and can result in sudden death. Hypertrophic cardiomyopathy can cause sudden cardiac arrest, often in young people.
Problems with heart valves
Having an enlarged heart can affect some of the heart valves, making them leaky. This allows blood to flow in the wrong direction and increases work for the heart.
Blood clots
In some types of cardiomyopathy, especially dilated cardiomyopathy, blood flows more slowly than usual through the heart. Slow blood flow increases the chances of blood clots forming in the heart chambers. If a blood clot breaks free and circulates in the bloodstream (called an embolus), it can be life-threatening if it travels to the brain or a coronary artery and lodges there.
Cardiomyopathy prevention
You can’t prevent inherited types of cardiomyopathy. If you have several family members who have cardiomyopathy, you may want to ask your doctor about being tested for an inherited form of cardiomyopathy. Finding out that you have inherited cardiomyopathy before you develop symptoms can be lifesaving, especially if you have a type of cardiomyopathy that can cause sudden cardiac arrest. You can adjust your activities and receive treatments to avoid complications. Examples include coronary heart disease, high blood pressure, and heart attack.
There are some types of cardiomyopathy that can be avoided, such as those that are caused by excessive alcohol or drug use. Healthy lifestyle choices are important to keep your heart healthy.
Your doctor may advise you to make heart-healthy lifestyle changes, such as:
- Avoiding the use of alcohol and illegal drugs
- Getting enough sleep and rest
- Heart-healthy eating
- Physical activity
- Quitting smoking
- Managing stress
Your cardiomyopathy may be due to an underlying disease or condition. If you treat that condition early enough, you may be able to prevent cardiomyopathy complications. For example, to control high blood pressure, high blood cholesterol, and diabetes:
- Follow your doctor’s advice about lifestyle changes.
- Get regular checkups with your doctor.
- Take all of your medicines as your doctor prescribes.
Cardiomyopathy signs and symptoms
Some people who have cardiomyopathy never have signs or symptoms. Others don’t have signs or symptoms in the early stages of the disease.
As cardiomyopathy worsens and the heart weakens, signs and symptoms of heart failure usually occur. These signs and symptoms include:
- Shortness of breath or trouble breathing, especially with physical exertion
- Fatigue (tiredness)
- Swelling in the ankles, feet, legs, abdomen, and veins in the neck
Other signs and symptoms may include dizziness; light-headedness; fainting during physical activity; arrhythmias (irregular heartbeats); chest pain, especially after physical exertion or heavy meals; and heart murmurs. (Heart murmurs are extra or unusual sounds heard during a heartbeat.)
Palpitations
This is the sensation of your own heart beating and can feel like extra or skipped beats. In some cases, palpitations may start suddenly and feel very fast, and may be accompanied by sweating or light-headedness.
You may feel that your heart is beating too quickly (tachycardia) or too slowly (bradycardia). You may describe it as a feeling of fluttering, missed beats or ‘thumps’ in your chest or stomach area. Some people describe it as a thudding in their ears.
Children with cardiomyopathy may become breathless or have chest pain when exercising or be unable to keep up with their friends while playing. They may also have:
- a cough;
- abdominal pain;
- nausea; or
- reduced appetite.
In babies, signs of cardiomyopathy may include:
- fast or heavy breathing during feeding;
- feeding that takes a long time;
- sweating during feeding; and
- poor weight gain.
Cardiomyopathy diagnosis
Your doctor will diagnose cardiomyopathy based on your medical and family histories, a physical exam, and the results from tests and procedures.
Specialists Involved
Often, a cardiologist or pediatric cardiologist diagnoses and treats cardiomyopathy. A cardiologist specializes in diagnosing and treating heart diseases. A pediatric cardiologist is a cardiologist who treats children.
Medical and Family Histories
Your doctor will want to learn about your medical history. He or she will want to know what signs and symptoms you have and how long you’ve had them.
Your doctor also will want to know whether anyone in your family has had cardiomyopathy, heart failure, or sudden cardiac arrest.
Physical Exam
Your doctor will use a stethoscope to listen to your heart and lungs for sounds that may suggest cardiomyopathy. These sounds may even suggest a certain type of the disease.
For example, the loudness, timing, and location of a heart murmur may suggest obstructive hypertrophic cardiomyopathy. A “crackling” sound in the lungs may be a sign of heart failure. Heart failure often develops in the later stages of cardiomyopathy.
Physical signs also help your doctor diagnose cardiomyopathy. Swelling of the ankles, feet, legs, abdomen, or veins in your neck suggests fluid buildup, a sign of heart failure.
Your doctor may notice signs and symptoms of cardiomyopathy during a routine exam. For example, he or she may hear a heart murmur, or you may have abnormal test results.
Diagnostic Tests
Your doctor may recommend one or more of the following tests to diagnose cardiomyopathy.
Blood Tests
During a blood test, a small amount of blood is taken from your body. It’s often drawn from a vein in your arm using a needle. The procedure usually is quick and easy, although it may cause some short-term discomfort.
Blood tests give your doctor information about your heart and help rule out other conditions.
Chest X Ray
A chest x ray takes pictures of the organs and structures inside your chest, such as your heart, lungs, and blood vessels. This test can show whether your heart is enlarged. A chest x ray also can show whether fluid is building up in your lungs.
EKG (Electrocardiogram)
An EKG is a simple test that records the heart’s electrical activity. The test shows how fast the heart is beating and its rhythm (steady or irregular). An EKG also records the strength and timing of electrical signals as they pass through each part of the heart.
This test is used to detect and study many heart problems, such as heart attacks, arrhythmias (irregular heartbeats), and heart failure. EKG results also can suggest other disorders that affect heart function.
A standard EKG only records the heartbeat for a few seconds. It won’t detect problems that don’t happen during the test.
To diagnose heart problems that come and go, your doctor may have you wear a portable EKG monitor. The two most common types of portable EKGs are Holter and event monitors.
Holter and Event Monitors
Holter and event monitors are small, portable devices. They record your heart’s electrical activity while you do your normal daily activities. A Holter monitor records the heart’s electrical activity for a full 24- or 48-hour period.
An event monitor records your heart’s electrical activity only at certain times while you’re wearing it. For many event monitors, you push a button to start the monitor when you feel symptoms. Other event monitors start automatically when they sense abnormal heart rhythms.
Echocardiography
Echocardiography (echo) is a test that uses sound waves to create a moving picture of your heart. The picture shows how well your heart is working and its size and shape.
There are several types of echo, including stress echo. This test is done as part of a stress test (see below). Stress echo can show whether you have decreased blood flow to your heart, a sign of coronary heart disease.
Another type of echo is transesophageal echo (TEE). Transesophageal echo (TEE) provides a view of the back of the heart.
For this test, a sound wave wand is put on the end of a special tube. The tube is gently passed down your throat and into your esophagus (the passage leading from your mouth to your stomach). Because this passage is right behind the heart, transesophageal echo (TEE) can create detailed pictures of the heart’s structures.
Before transesophageal echo (TEE), you’re given medicine to help you relax, and your throat is sprayed with numbing medicine.
Stress Test
Some heart problems are easier to diagnose when your heart is working hard and beating fast. During stress testing, you exercise (or are given medicine if you’re unable to exercise) to make your heart work hard and beat fast while heart tests are done.
These tests may include nuclear heart scanning, echo, and positron emission tomography (PET) scanning of the heart.
Diagnostic Procedures
You may have one or more medical procedures to confirm a diagnosis or to prepare for surgery (if surgery is planned). These procedures may include cardiac catheterization, coronary angiography, or myocardial biopsy.
Cardiac Catheterization
This procedure checks the pressure and blood flow in your heart’s chambers. The procedure also allows your doctor to collect blood samples and look at your heart’s arteries using x-ray imaging.
During cardiac catheterization, a long, thin, flexible tube called a catheter is put into a blood vessel in your arm, groin (upper thigh), or neck and threaded to your heart. This allows your doctor to study the inside of your arteries for blockages.
Coronary Angiography
This procedure often is done with cardiac catheterization. During the procedure, dye that can be seen on an x ray is injected into your coronary arteries. The dye lets your doctor study blood flow through your heart and blood vessels.
Dye also may be injected into your heart chambers. This allows your doctor to study the pumping function of your heart.
Myocardial Biopsy
For this procedure, your doctor removes a piece of your heart muscle. This can be done during cardiac catheterization. The heart muscle is studied under a microscope to see whether changes in cells have occurred. These changes may suggest cardiomyopathy.
Myocardial biopsy is useful for diagnosing some types of cardiomyopathy.
Genetic Testing
Some types of cardiomyopathy run in families. Thus, your doctor may suggest genetic testing to look for the disease in your parents, brothers and sisters, or other family members.
Genetic testing can show how the disease runs in families. It also can find out the chances of parents passing the genes for the disease on to their children.
Genetic testing also may be useful if your doctor thinks you have cardiomyopathy, but you don’t yet have signs or symptoms. If the test shows you have the disease, your doctor can start treatment early, when it may work best.
Cardiomyopathy treatment
Cardiomyopathy cannot usually be completely reversed or ‘cured’. However, it can be helped or controlled by treatments which, depending on symptoms, may include medications, pacemakers, implantable defibrillators and, in a small number of cases, surgery. In its most advanced stages, cardiomyopathy may be treated by heart transplantation with good long-term results.
It is important to note that although the condition does vary in severity, the majority of those diagnosed will be able to lead a relatively normal life.
People who have cardiomyopathy but no signs or symptoms may not need treatment. Sometimes, dilated cardiomyopathy that comes on suddenly may go away on its own. For other people who have cardiomyopathy, treatment is needed. Treatment depends on the type of cardiomyopathy you have, the severity of your symptoms and complications, and your age and overall health.
Treatments may include:
- Heart-healthy lifestyle changes
- Medicines
- Nonsurgical procedure
- Surgery and implanted devices
The main goals of treating cardiomyopathy include:
- Controlling signs and symptoms so that you can live as normally as possible
- Managing any conditions that cause or contribute to the disease
- Reducing complications and the risk of sudden cardiac arrest
- Stopping the disease from getting worse
Heart-Healthy Lifestyle Changes
Your doctor may suggest lifestyle changes to manage a condition that’s causing your cardiomyopathy including:
- Heart-healthy eating
- Aiming for a healthy weight
- Managing stress
- Physical activity
- Quitting smoking
Medicines
Many medicines are used to treat cardiomyopathy. Your doctor may prescribe medicines to:
- Balance electrolytes in your body. Electrolytes are minerals that help maintain fluid levels and acid-base balance in the body. They also help muscle and nerve tissues work properly. Abnormal electrolyte levels may be a sign of dehydration (lack of fluid in your body), heart failure, high blood pressure, or other disorders. Aldosterone blockers are an example of a medicine used to balance electrolytes.
- Keep your heart beating with a normal rhythm. These medicines, called antiarrhythmics, help prevent arrhythmias.
- Lower your blood pressure. ACE inhibitors, angiotensin II receptor blockers, beta blockers, and calcium channel blockers are examples of medicines that lower blood pressure.
- Prevent blood clots from forming. Anticoagulants, or blood thinners, are an example of a medicine that prevents blood clots. Blood thinners often are used to prevent blood clots from forming in people who have dilated cardiomyopathy.
- Reduce inflammation. Corticosteroids are an example of a medicine used to reduce inflammation.
- Remove excess sodium from your body. Diuretics, or water pills, are an example of medicines that help remove excess sodium from the body, which reduces the amount of fluid in your blood.
- Slow your heart rate. Beta blockers, calcium channel blockers, and digoxin are examples of medicines that slow the heart rate. Beta blockers and calcium channel blockers also are used to lower blood pressure.
Take all medicines regularly, as your doctor prescribes. Don’t change the amount of your medicine or skip a dose unless your doctor tells you to.
Nonsurgical Procedure
Doctors may use a nonsurgical procedure called alcohol septal ablation to treat cardiomyopathy. During this procedure, the doctor injects ethanol (a type of alcohol) through a tube into the small artery that supplies blood to the thickened area of heart muscle. The alcohol kills cells, and the thickened tissue shrinks to a more normal size. This procedure allows blood to flow freely through the ventricle, which improves symptoms.
Surgery and Implanted Devices
Doctors use several types of surgery to treat cardiomyopathy, including septal myectomy, surgically implanted devices, and heart transplant.
Septal Myectomy
Septal myectomy is open-heart surgery and is used to treat people who have hypertrophic cardiomyopathy and severe symptoms. This surgery generally is used for younger patients and for people whose medicines aren’t working well.
A surgeon removes part of the thickened septum that’s bulging into the left ventricle. This improves blood flow through the heart and out to the body. The removed tissue doesn’t grow back. If needed, the surgeon also can repair or replace the mitral valve at the same time. Septal myectomy often is successful and allows you to return to a normal life with no symptoms.
Surgically Implanted Devices
Surgeons can place several types of devices in the heart to improve function and symptoms, including:
- Cardiac resynchronization therapy (CRT) device. A cardiac resynchronization therapy device coordinates contractions between the heart’s left and right ventricles.
- Implantable cardioverter defibrillator (ICD). An implantable cardioverter defibrillator helps control life-threatening arrhythmias that may lead to sudden cardiac arrest. This small device is implanted in the chest or abdomen and connected to the heart with wires. If an implantable cardioverter defibrillator senses a dangerous change in heart rhythm, it will send an electric shock to the heart to restore a normal heartbeat.
- Left ventricular assist device (LVAD). This device helps the heart pump blood to the body. An left ventricular assist device can be used as a long-term therapy or as a short-term treatment for people who are waiting for a heart transplant.
- Pacemaker. This small device is placed under the skin of your chest or abdomen to help control arrhythmias. The device uses electrical pulses to prompt the heart to beat at a normal rate.
Heart Transplant
For this surgery, a surgeon replaces a person’s diseased heart with a healthy heart from a deceased donor. A heart transplant is a last resort treatment for people who have end-stage heart failure. “End-stage” means the condition has become so severe that all treatments, other than heart transplant, have failed.
Living With Cardiomyopathy
Some people who have cardiomyopathy—especially those who have hypertrophic cardiomyopathy—may live a healthy life with few problems or symptoms. Others may have serious symptoms and complications.
If you have cardiomyopathy, you can take steps to take care of your heart. Lifestyle changes and ongoing care can help you manage the disease.
Lifestyle Changes
A healthy diet and physical activity are part of a heart healthy lifestyle. Your doctor can help you decide what kind of eating plan is right for you. Talk with your doctor about the amounts and types of fluids that are safe and healthy for you. Too much fluid can worsen certain heart conditions.
Your doctor also may suggest a diet that’s low in sodium (salt) and fat.
Talk with your doctor about the amount and type of physical activity that’s right for you. People who have hypertrophic cardiomyopathy shouldn’t do vigorous activity. However, moderate activity, such as walking, often is a good idea.
Your doctor also may suggest other lifestyle changes, such as:
- Quitting smoking
- Losing excess weight
- Avoiding the use of alcohol and illegal drugs
- Getting enough sleep and rest
- Reducing stress
Physical Activity
Children with dilated cardiomyopathy are not allowed to play competitive sports because of the possibility of a sudden collapse or increased heart failure. A competitive sport is an organized team activity for which training is required. A child with dilated cardiomyopathy and no heart failure symptoms can be allowed to perform recreational athletic activities, also known as low-dynamic or low-static sports, in a non-competitive situation. In milder cases, the child may even participate in gym class after careful discussions between the child, teacher, and parents to ensure that the level of activity does not cause overexertion (breathlessness, chest pain, excessive sweating). Specific activity recommendations should be individualized by the treating cardiologist.
Ongoing Care
If you have cardiomyopathy, it’s important to get ongoing care. Call your doctor if you notice new or worsening symptoms, such as swelling in your ankles, feet, legs, abdomen, or veins in the neck. These symptoms may be a sign that the disease is getting worse.
You also should:
- Take all of your medicines as your doctor prescribes.
- Make all of the lifestyle changes that your doctor suggests.
- Make sure you go to all of your medical checkups.
- Follow your treatment plan for any underlying conditions, such as diabetes and high blood pressure.
Cardiomyopathy often runs in families. Your doctor may suggest that your parents, brothers and sisters, and children get checked to see whether they have the disease.