Contents
What is cervicitis
Cervicitis is swelling and inflammation of the cervix (the lower end of the uterus) (see Figures 1 and 2). Cervicitis is very common. It affects more than one half of all women at some point during their adult life. Cervicitis is most often caused by an infection that is caught during sexual activity. Sexually transmitted infections (STIs) that can cause cervicitis. The Centers for Disease Control and Prevention (CDC) estimates that over 19 million new sexually transmitted infections (STIs) occur annually, almost half of them among persons aged 15-24 years 1.
Possible symptoms of cervicitis include bleeding between menstrual periods, pain with intercourse or during a cervical exam, and abnormal vaginal discharge. However, it’s also possible to have cervicitis and not experience any signs or symptoms.
Often, cervicitis results from a sexually transmitted infection, such as chlamydia or gonorrhea. Cervicitis can develop from noninfectious causes, too. Successful treatment of cervicitis involves treating the underlying cause of the inflammation. Chlamydia, is the most frequently reported infectious disease in the US, with the majority of cases occurring in individuals aged 25 years or younger 2. The reported incidence of chlamydial infections has steadily increased over the past 2 decades, with 1.3 million cases reported in 2010. Although this increased incidence may reflect changes in screening efforts, many cases are not reported or are undiagnosed. More than 50% of sexually active young women are not screened annually, despite CDC recommendations 1.Gonorrhea is the second most commonly reported infectious disease in the United States, with more than 300,000 cases reported in 2010 1. Annually, approximately 700,000 new gonococcal infections occur 3. Much like chlamydia, gonorrhea is believed to be underreported. In a study of 1469 emergency department patients diagnosed with cervicitis, Burnett et al 4 found that 1.8% and 9.3% of patients with cervicitis were also positive for gonorrhea or chlamydia, respectively. Of a separate group of 343 patients with pelvic inflammatory disease (PID), 4.4% and 10% were positive for gonorrhea or chlamydia, respectively 4.
The annual rates of infection by herpes simplex virus (HSV) is difficult to estimate, because the vast majority of initial infections are asymptomatic or unrecognized. In addition, HSV infections are not required to be reported in the US 1. The prevalence of HSV type 2 is about 16% (primarily among black women: 48%) 5.
See your doctor if you have:
- Persistent, unusual vaginal discharge
- Nonmenstrual vaginal bleeding
- Pain during intercourse
What is a cervix
The cervix is part of the lower end of the uterus. The lumen (internal cavity) of the uterus communicates with the vagina by way of a narrow passage through the cervix called the cervical canal.
The cervix has two different parts and is covered with two different types of cells.
- The part of the cervix closest to the body of the uterus is called the endocervix and is covered with glandular cells.
- The part next to the vagina is the exocervix (or ectocervix) and is covered in squamous cells.
These two cell types meet at a place called the transformation zone. The exact location of the transformation zone changes as you get older and if you give birth.
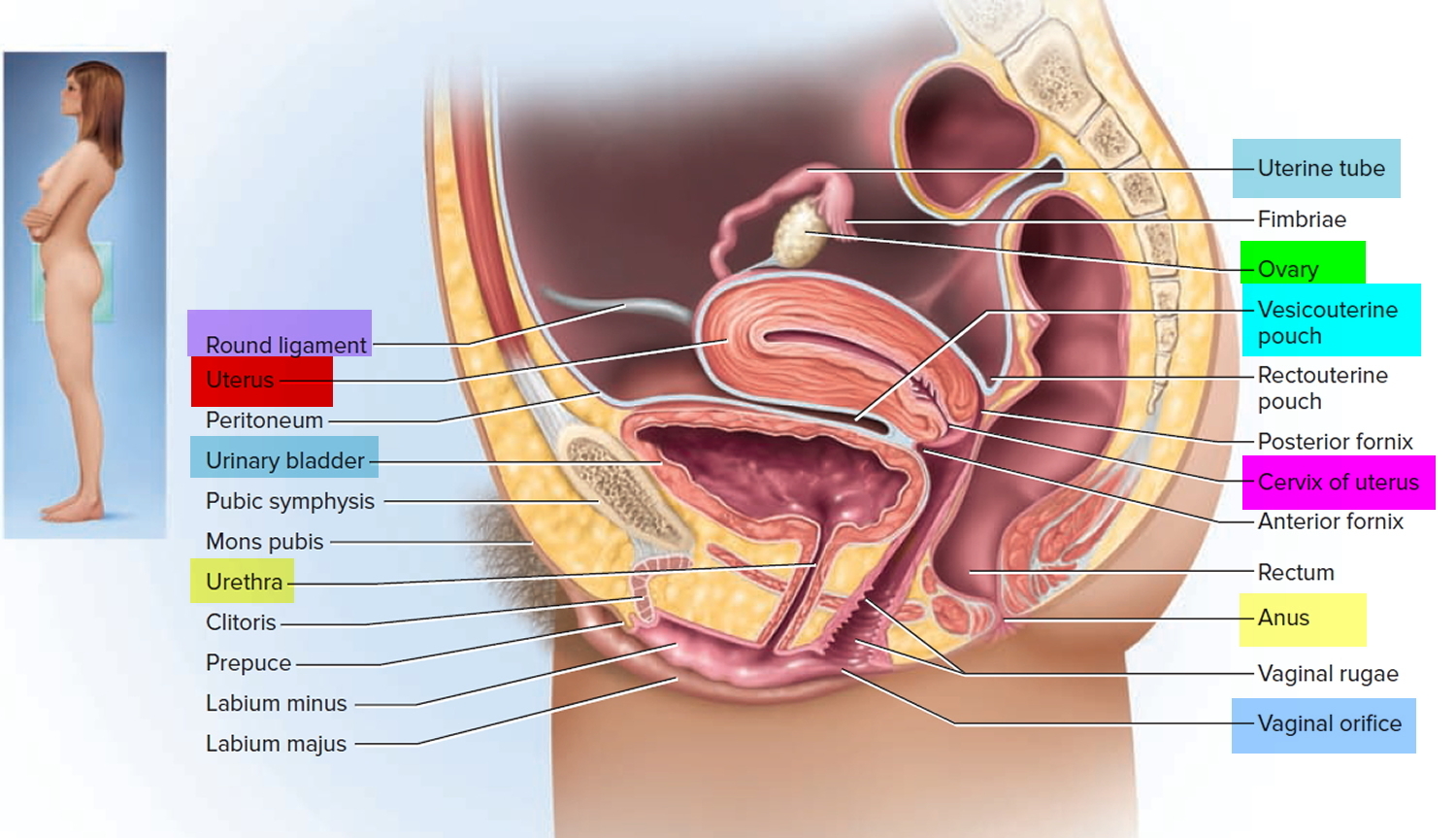
Figure 1. Cervix position
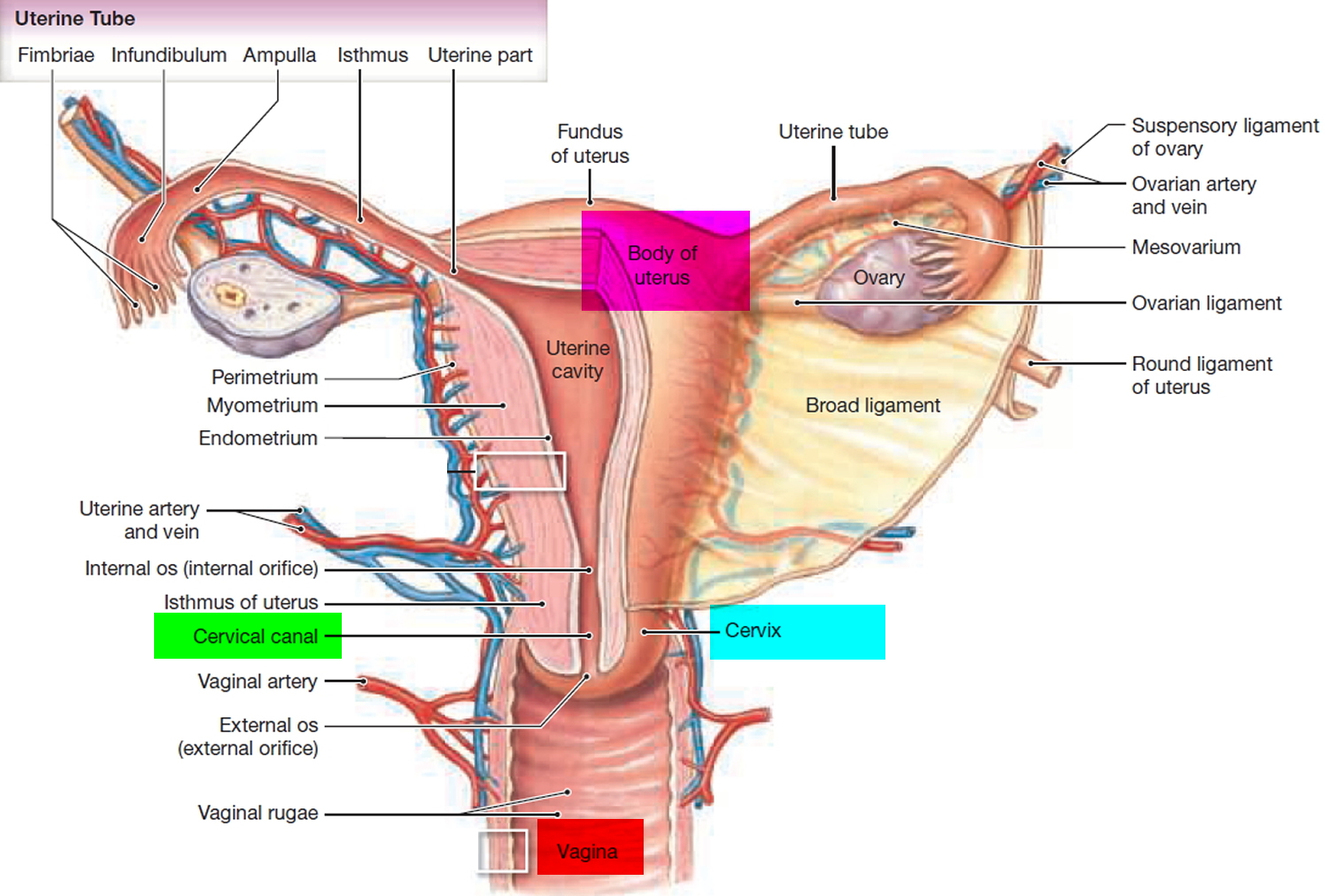
Figure 2. Cervix location
Acute cervicitis
Acute cervicitis is usually caused by an sexually transmitted infection. Cervicitis has classically been associated with Chlamydia trachomatis or Neisseria gonorrhoeae infection 6, but can also accompany Trichomonas vaginalis, Mycoplasma genitalium, and herpes simplex virus infection 7.
Chronic cervicitis
Chronic cervicitis is an extremely common condition in adult females, at least at the microscopic level. Chronic cervicitis importance lies in the fact that it may lead to endometritis, salpingitis, pelvic inflammatory disease, chorioamnionitis, and other complications during pregnancy, and it may also play a role in initiation or promotion of cervical neoplasia 8.
Viral infections in the cervix result in two types of tissue responses. The first one being degeneration and death; in the second, cells are stimulated into mitotic activity, which sometimes leads to overt neoplasia 9.
Mucopurulent cervicitis
Mucopurulent cervicitis is a clinical syndrome characterized by mucopurulent discharge from the cervix and other signs of inflammation such as easily induced cervical bleeding (bleeding that occurs with gentle passage of a cervical swab) 10. In some clinics, the presence of ≥ 30 white blood cells per oil immersion field on cervical Gram’s stain is also used 11. Mucopurulent cervicitis is associated with sexually transmitted infections (e.g., Gonorrhea and Chlamydia) in the majority of cervicitis cases and with a smaller percentage the causes were unknown 12, 13.
Cervicitis causes
Cervicitis is most often caused by an infection that is caught during sexual activity.
Sexually transmitted infections (STIs) that can cause cervicitis include:
- Chlamydia
- Gonorrhea
- Herpes virus (genital herpes)
- Human papilloma virus (genital warts)
- Trichomoniasis
Other things that can cause cervicitis include:
- A device inserted into the pelvic area such as a cervical cap, diaphragm, or pessary
- Allergy to spermicides used for birth control
- Allergy to latex in condoms
- Exposure to a chemical
Cervicitis is very common. It affects more than one half of all women at some point during their adult life.
Risk factors for cervicitis
You’re at greater risk of cervicitis if you:
- High-risk sexual behavior
- History of sexually transmitted infections
- Many sexual partners
- Sex (intercourse) at an early age
- Sexual partners who have engaged in high-risk sexual behavior or have had an sexually transmitted infection
Bacteria (such as staphylococcus and streptococcus) and too much growth of normal bacteria in the vagina (bacterial vaginosis) can also cause cervicitis.
Cervicitis possible complications
Your cervix acts as a barrier to keep bacteria and viruses from entering your uterus. When the cervix is infected, there’s an increased risk that the infection will travel into your uterus. Complications from untreated infectious cervicitis depend on the pathogen.
Cervicitis that’s caused by gonorrhea or chlamydia can spread to the uterine lining and the fallopian tubes, resulting in pelvic inflammatory disease (PID), an infection of the female reproductive organs that can cause fertility problems, chronic pelvic pain and ectopic pregnancy if left untreated. Other morbidity may include spontaneous abortion, premature rupture of membranes, and preterm delivery if infection is present during pregnancy.
Cervicitis can also increase the risk of a woman getting HIV from an infected sexual partner.
Certain subtypes of HPV are linked with the development of cervical cancer. Untreated active HSV infections in the perinatal and neonatal period can cause mental retardation, blindness, low birth weight, stillbirth, meningitis, and death.
Cervicitis prevention
Things you can do to reduce your risk of developing cervicitis include:
- Avoid irritants such as douches and deodorant tampons.
- Make sure that any foreign objects you insert into your vagina (such as tampons) are properly placed. Be sure to follow instructions on how long to leave it inside, how often to change it, or how often to clean it.
- Make sure your partner is free of any sexually transmitted infection. You and your partner should not have sex with any other people.
- Use a condom every time you have sex to lower your risk of getting an sexually transmitted infection. Condoms are available for both men and women, but are most commonly worn by the man. A condom must be used properly every time. Condoms are very effective against the spread of STIs, such as gonorrhea and chlamydia, which can lead to cervicitis.
Cervicitis symptoms
There may be no signs and symptoms and you may only learn you have the condition after a pelvic exam performed by your doctor for another reason. Women who may be at risk for chlamydia, gonorrhea, and Trichomonas vaginalis infections should be tested for this infection, even if they do not have symptoms.
If you do have signs and symptoms, they may include:
- Abnormal vaginal bleeding that occurs after intercourse, after menopause, or between periods
- Unusual vaginal discharge that does not go away: discharge may be gray, white or yellow in color
- Painful sexual intercourse
- Pain in the vagina
- Pressure or heaviness in the pelvis
- Frequent, painful urination.
Cervicitis diagnosis
To diagnose cervicitis, your doctor will likely perform a physical exam that includes:
- A pelvic exam. During this exam, your doctor checks your pelvic organs for areas of swelling and tenderness. He or she may also place a speculum in your vagina to view the upper, lower and side walls of the vagina and the cervix.
- A specimen collection. In a process similar to a Pap test, your doctor uses a small cotton swab or a brush to gently remove a sample of cervical and vaginal fluid. Your doctor sends the sample to a lab to test for infections. Lab tests may also be performed on a urine sample.
A pelvic exam is done to look for:
- Discharge from the cervix
- Redness of the cervix
- Swelling (inflammation) of the walls of the vagina
Tests that may be done include:
- Inspection of the discharge under a microscope (may show candidiasis, trichomoniasis, or bacterial vaginosis)
- Pap test
- Tests for gonorrhea or chlamydia
Rarely, colposcopy and biopsy of the cervix is necessary.
Cervicitis treatment
Most of the time, simple cervicitis caused by an allergic reaction to products such as spermicide or feminine hygiene products usually heals with treatment if the cause is found and there is a treatment for that cause.
If you have cervicitis caused by a sexually transmitted infection (STI), both you and your partner will need treatment, often with an antibiotic medication. Antibiotics are prescribed for STIs such as gonorrhea, chlamydia or bacterial infections, including bacterial vaginosis.
Your doctor may also recommend repeat testing for cervicitis caused by gonorrhea or chlamydia.
- To avoid passing a bacterial infection along to your partner, wait to have sexual intercourse until you’re finished with the treatment recommended by your doctor.
Antibiotics are used to treat chlamydia or gonorrhea. Drugs called antivirals may be used to treat herpes infections. However, there is no cure for herpes. Herpes is a chronic condition that may be passed to your sexual partner at any time.
Hormonal therapy (with estrogen or progesterone) may be used in women who have reached menopause.
When these treatments have not worked or when cervicitis has been present for a long time, treatment may include:
- Cryosurgery (freezing)
- A small probe with an electric current running through it is used to burn or destroy the tissue
- Laser therapy.
- Centers for Disease Control and Prevention. STD trends in the United States: 2010 national data for gonorrhea, chlamydia, and syphilis. https://www.cdc.gov/std/stats10/trends.htm[↩][↩][↩][↩]
- Centers for Disease Control and Prevention. Sexually transmitted diseases treatment guidelines, 2010: chlamydial infections. https://www.cdc.gov/std/treatment/2010/chlamydial-infections.htm[↩]
- Centers for Disease Control and Prevention. Sexually transmitted diseases treatment guidelines, 2010: gonococcal infections. https://www.cdc.gov/std/treatment/2010/gonococcal-infections.htm[↩]
- Burnett AM, Anderson CP, Zwank MD. Laboratory-confirmed gonorrhea and/or chlamydia rates in clinically diagnosed pelvic inflammatory disease and cervicitis. Am J Emerg Med. 2012 Sep. 30(7):1114-7.[↩][↩]
- Centers for Disease Control and Prevention. Seroprevalence of herpes simplex virus type 2 among persons aged 14-49 years–United States, 2005-2008. MMWR Morb Mortal Wkly Rep. 2010 Apr 23. 59(15):456-9.[↩]
- Brunham RC, Paavonen J, Stevens CE, et al. Mucopurulent cervicitis–the ignored counterpart in women of urethritis in men. N Engl J Med. 1984;311(1):1–6. https://www.ncbi.nlm.nih.gov/pubmed/6427611[↩]
- Manhart LE, Critchlow CW, Holmes KK, et al. Mucopurulent cervicitis and Mycoplasma genitalium. J Infect Dis. 2003;187(4):650–7. https://www.ncbi.nlm.nih.gov/pubmed/12599082[↩]
- Rosai Juan. Rosai and Ackerman’s Surgical Pathology. 10th ed. St.Louis: Mosby; 2011. p. 1439. Chapter 19, Female reproductive system.[↩]
- Fox Harold, Wells Michael. Haines and Taylor Obstetrical and Gynaecological pathology. 5th ed. Edinburgh: Churchill Livingstone; 2003. p. 255. Chapter 6, Non-neoplastic conditions of the cervix.[↩]
- Taylor SN, Lensing S, Schwebke J, et al. Prevalence and Treatment Outcome of Cervicitis of Unknown Etiology. Sexually transmitted diseases. 2013;40(5):10.1097/OLQ.0b013e31828bfcb1. doi:10.1097/OLQ.0b013e31828bfcb1. https://www.ncbi.nlm.nih.gov/pmc/articles/PMC3868214/[↩]
- Marrazzo JM, Handsfield HH, Whittington WLH. Predicting chlamydial and gonococcal cervical infection: implications for management of cervicitis. Obstet Gynecol. 2002;100:579–584. https://www.ncbi.nlm.nih.gov/pubmed/12220782[↩]
- Paavonen J, Critchlow CW, DeRouen T, et al. Etiology of cervical inflammation. Am J Obstet Gynecol. 1986;154:556–564. https://www.ncbi.nlm.nih.gov/pubmed/3485379[↩]
- Paavonen J. Chlamydia trachomatis: a major cause of mucopurulent cervicitis and pelvic inflammatory disease in women. Curr Probl Dermatol. 1996;24:110–22. https://www.ncbi.nlm.nih.gov/pubmed/8743261[↩]