Contents
What is Churg Strauss syndrome
Churg-Strauss syndrome is one of the rarest disorder marked by predominantly small blood vessels inflammation or vasculitis. This inflammation can restrict blood flow to vital organs and tissues, sometimes permanently damaging them. Churg-Strauss syndrome, now also referred to by its medically more accurate term eosinophilic granulomatosis with polyangiitis or allergic granulomatous angiitis, is a systemic vasculitis 1. This disease was first described in 1951 by Dr. Jacob Churg and Dr. Lotte Strauss as a syndrome consisting of “asthma, eosinophilia [an excessive number of eosinophils in the blood], fever, and accompanying vasculitis of various organ systems”. Churg-Strauss syndrome (Eosinophilic Granulomatosis with Polyangiitis) shares many of the clinical and pathological features of polyarteritis nodosa (“PAN”, another type of vasculitis) and granulomatosis with polyangiitis. However, Drs. Churg and Strauss discovered that the presence of granulomas as well as the abundance of eosinophils distinguished this disease from polyarteritis nodosa (PAN) and granulomatosis with polyangiitis (Wegener’s Granulomatosis).
About 40% of people with Churg-Strauss syndrome test positive for antineutrophil cytoplasmic autoantibodies (ANCAs) in their blood. Because antineutrophil cytoplasmic auto-antibodies (ANCA) can be detected in the serum in up to 40% of the patients, Churg-Strauss syndrome is also considered one of the three ANCA-associated vasculitides, along with granulomatosis with polyangiitis (Wegener’s Granulomatosis) and microscopic polyangiitis. However, the clinical characteristics and outcomes of these 3 vasculitides differ noticeably.
Churg-Strauss syndrome is one of the rarest systemic vasculitis, with less than 2 people in a million population being diagnosed each year.
The main features of Churg-Strauss syndrome (eosinophilic granulomatosis with polyangiitis) are:
- Asthma
- Eosinophil infiltration in the lungs
- Eosinophils in the blood
- Small vessel vasculitis (inflamed blood vessels) and granulomas (mixed chronic inflammatory cells) on biopsy.
Main clinical characteristics of Churg-Strauss syndrome (eosinophilic granulomatosis with polyangiitis) include late-onset allergic rhinitis and asthma with increased blood eosinophil count (a type of white blood cells usually implicated in allergy and defense against certain parasitic infections) and vasculitis manifestations such as skin nodules or purpura (skin rash of punctuated red lesions) and mononeuritis multiplex (causing numbness or tingling or sudden loss of strength in the hands or feet). Cardiac involvement is also frequent and important to diagnose because it can be potentially severe and life-threatening. Other possible symptoms include fever, fatigue, muscle and joint pain, shortness of breath, rapid weight loss, and skin rash. Mechanisms of the disease are complex and not completely elucidated, but treatment is well standardized, and the majority of patients respond well to therapy. Long-term corticosteroid therapy is frequently needed because of persistent asthma, although some people with severe disease may need an immunosuppressant drug as well.
People around the age of 50 years are most affected. It is uncommon in people older than 65 years old and very rarely in childhood, but the disease can occur at any age. There is no sex preponderance and there is no strong evidence of a difference in occurrence of the disease around the globe, at least between European and North American countries, where Churg-Strauss syndrome (eosinophilic granulomatosis with polyangiitis) currently affects about 10 to 15 living patients in a million population.
Churg-Strauss syndrome is a serious disease that can be fatal. Untreated it is extremely dangerous and threatens the organs that are affected. With aggressive treatment and monitoring it can be controlled fairly well. Total inactivation of the disease (remission) is possible as well. Drug therapy can relieve symptoms of Churg-Strauss syndrome and send the disease into remission. But relapses are common.
Churg-Strauss syndrome pictures
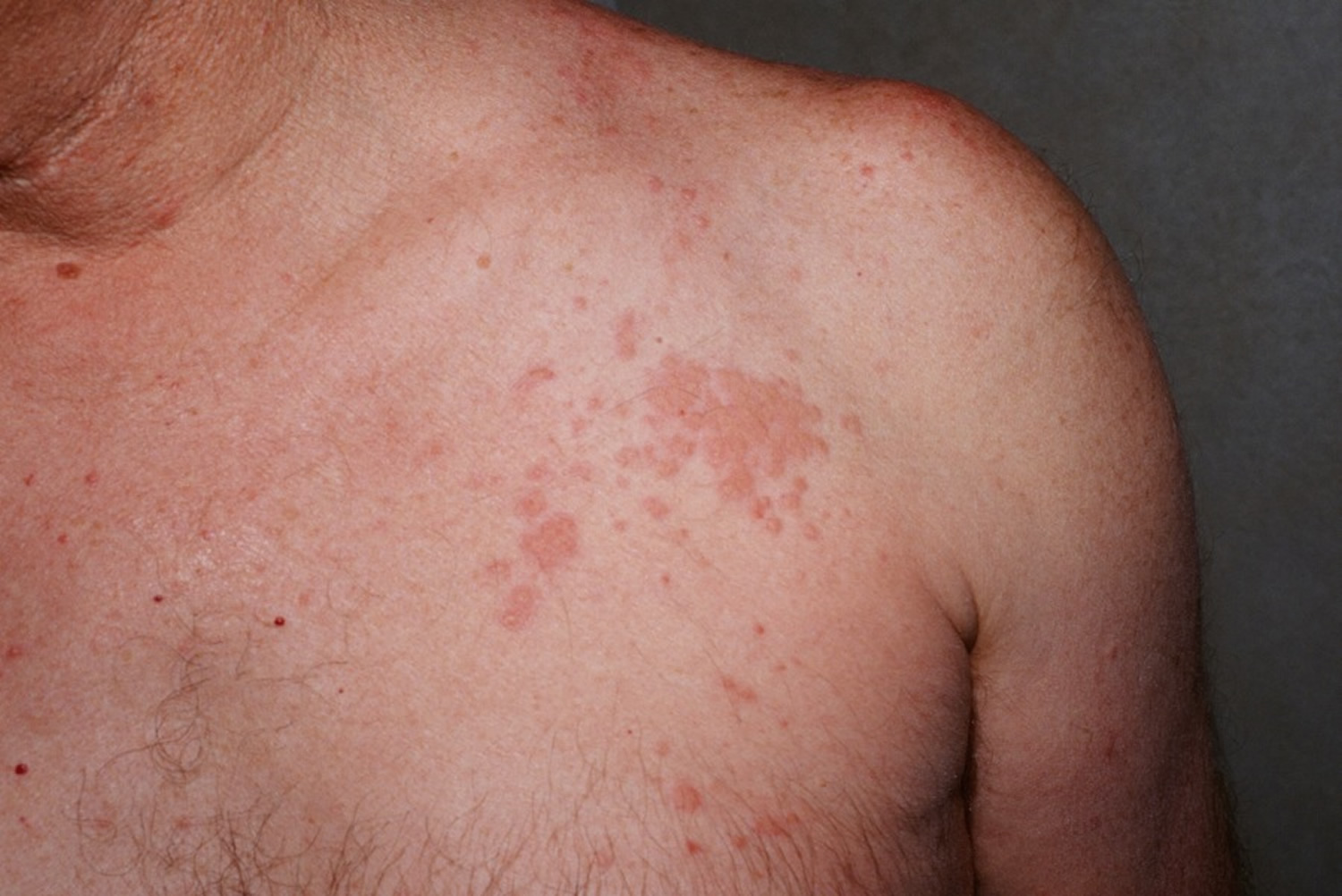
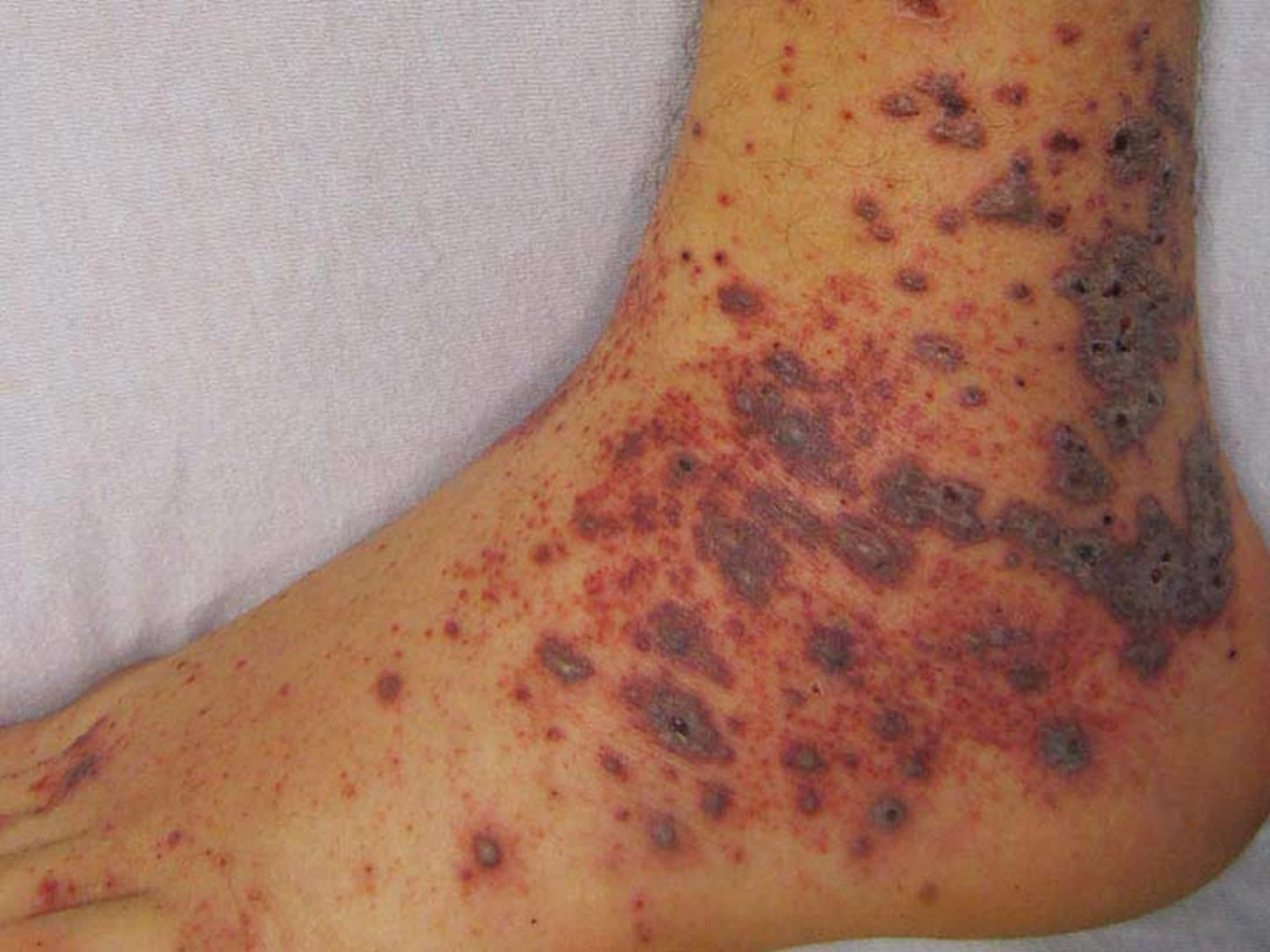
Figure 1. Churg-Strauss syndrome skin rash
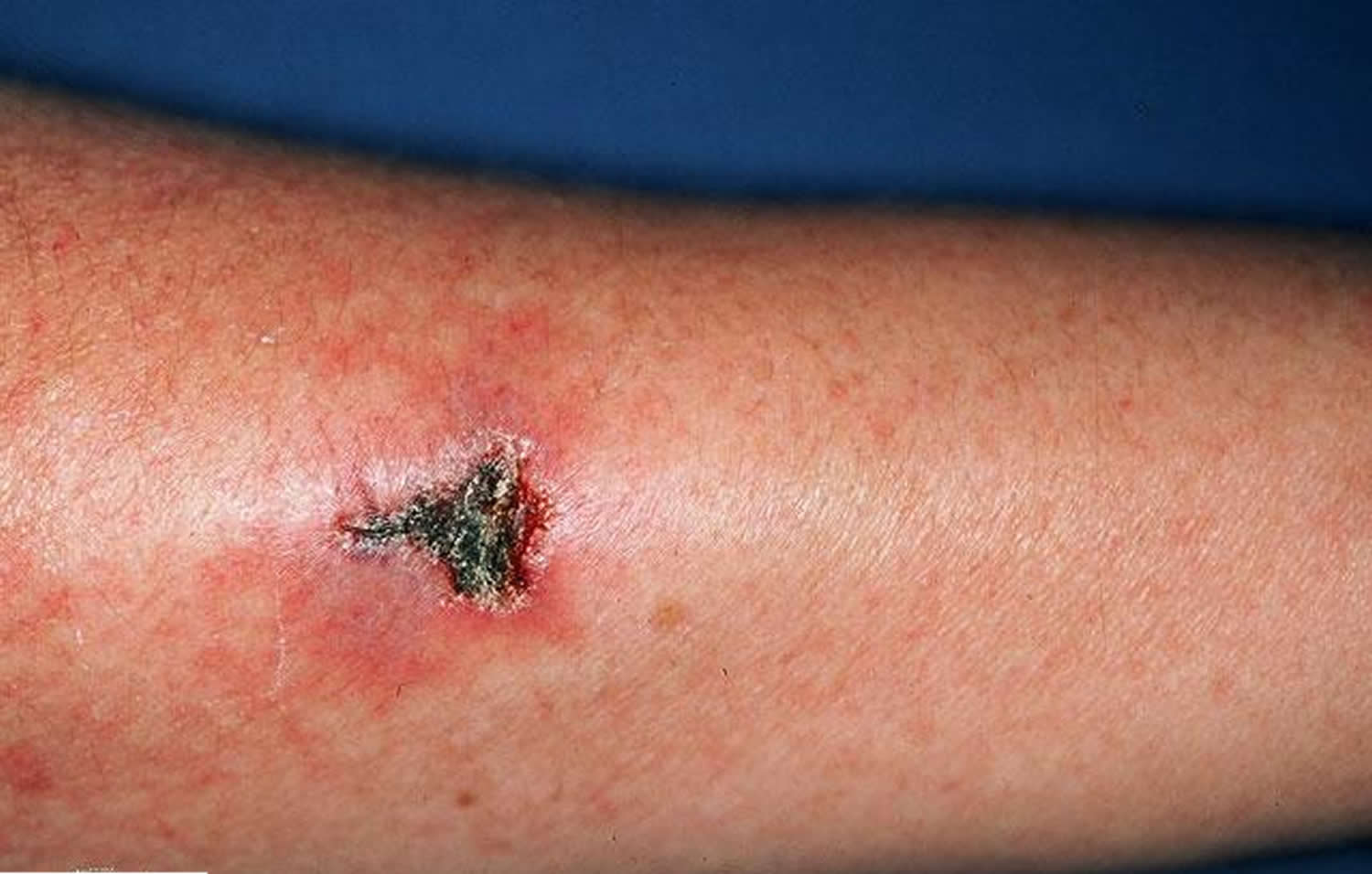
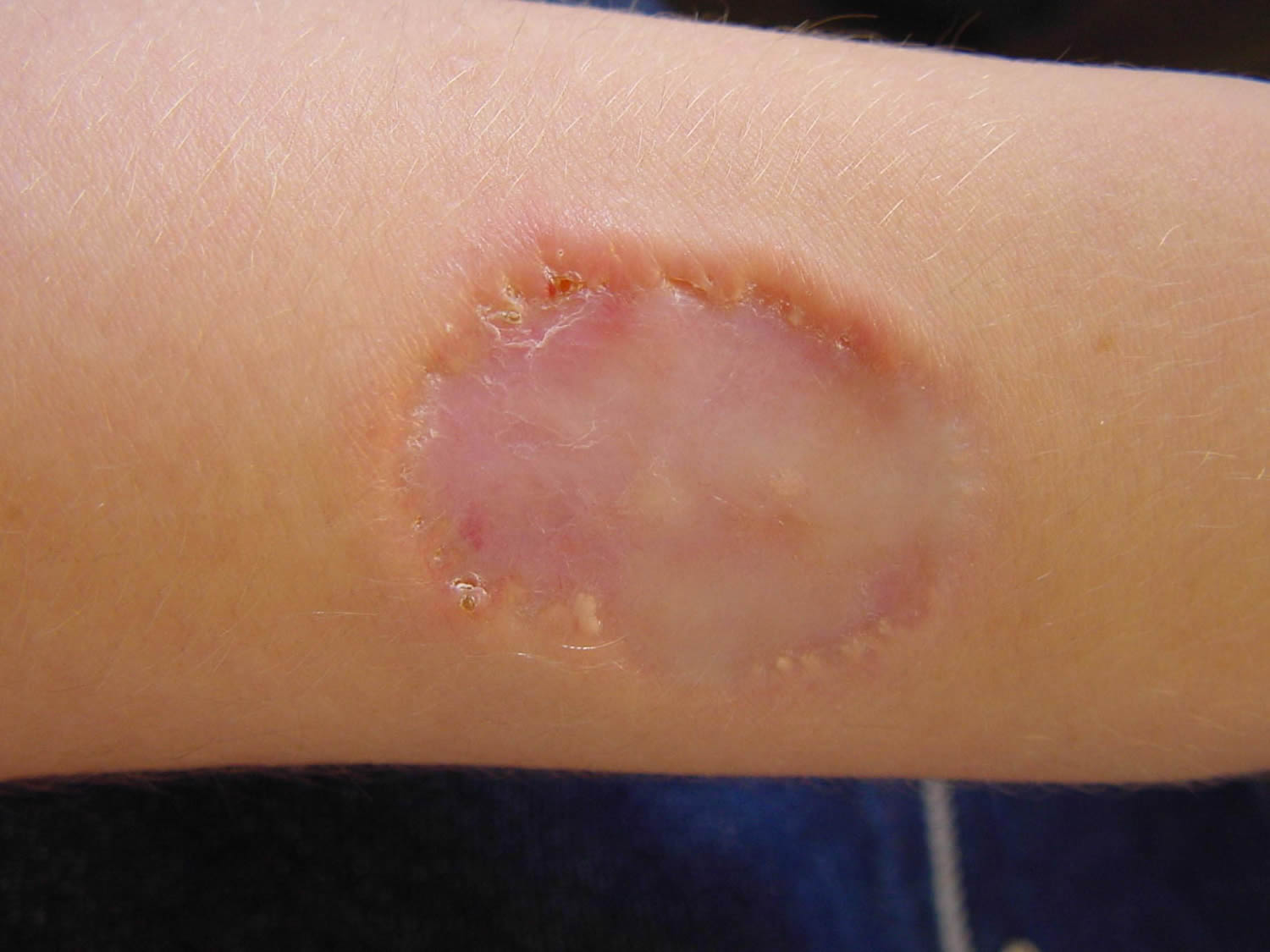
Figure 2. Churg-Strauss syndrome necrotic ulcer
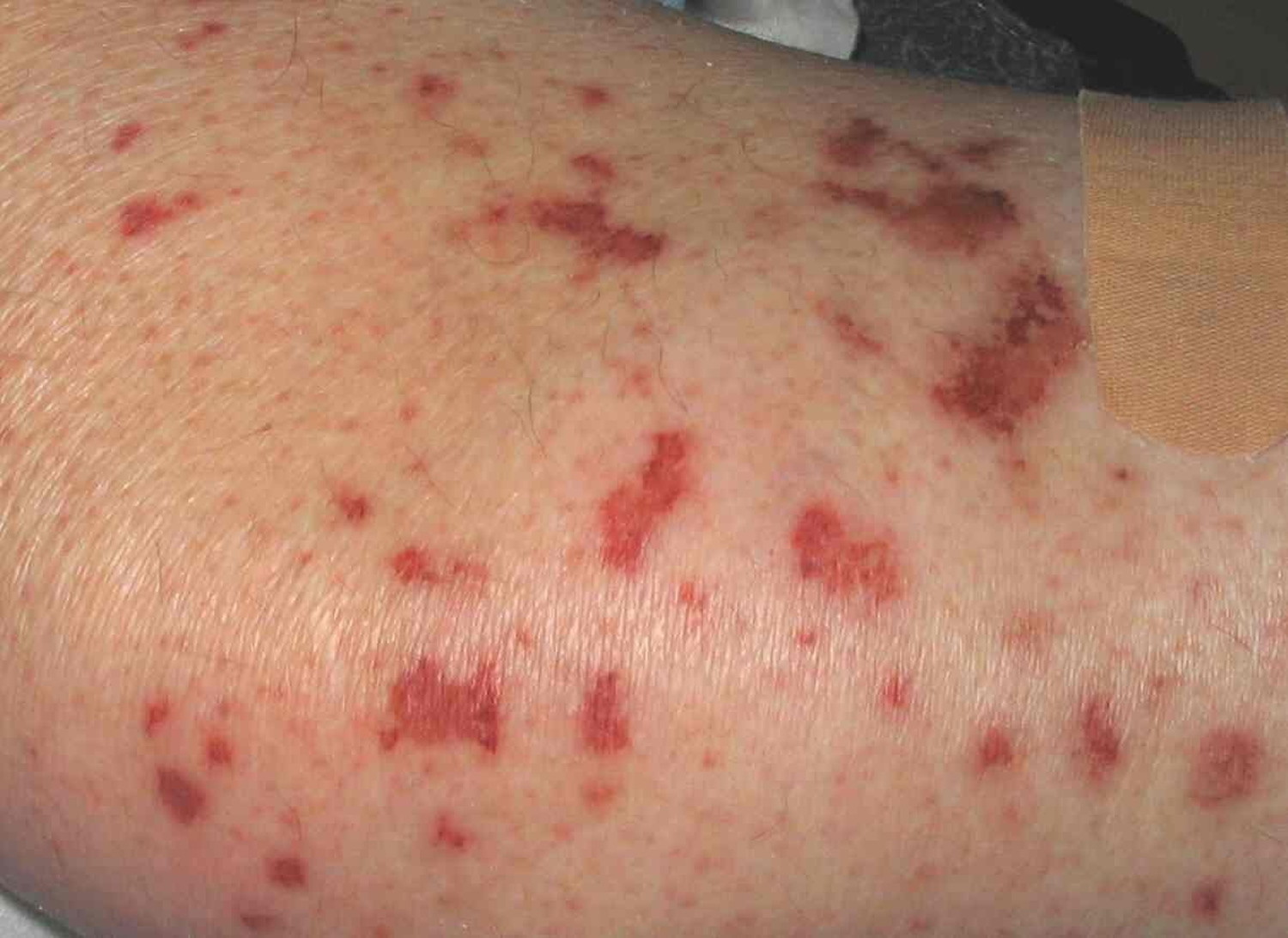
Figure 3. Churg-Strauss syndrome skin rash – eosinophilic phase
Figure 4. Churg Strauss syndrome – conjunctival granulomas on the bulbar conjunctiva
Figure 5. Churg-Strauss syndrome skin granuloma
Figure 6. Churg-Strauss syndrome skin vasculitis
Churg-Strauss syndrome stages
Churg-Strauss syndrome (eosinophilic granulomatosis with polyangiitis) has been divided into 3 distinct phases, which may or may not be sequential. Symptoms depend upon the phase and organs involved.
Churg-Strauss Syndrome has traditionally been classified as occurring in three phases 2:
- The prodromal phase can start from months up to years before the other phases and can last for a long time. Churg-Strauss Syndrome is characterized by upper respiratory symptoms, asthma and general symptoms, such as arthralgia, myalgia, malaise, fever and weight loss. Allergic rhinitis may also occur 2. Asthma is a chronic inflammatory airway disease that is characterized by a specific inflammatory cell response resulting in a swollen, oedematous, hyper-reactive airway. It is the main manifestation during the prodromal phase of the disease. It is present in 96–100% of Churg-Strauss syndrome (eosinophilic granulomatosis with polyangiitis) patients 3. Asthma symptoms generally precede the onset of the systemic disease by several years and generally become corticodependent 4. Other upper respiratory symptoms are present in a majority of patients (47–93%). These symptoms include allergic rhinitis, nasal polyps, recurrent or chronic sinusitis 3. In this case report of a 38 year old man 5, the patient had an asthma diagnosis since childhood, but with a recent worsening of the symptoms, cough and dyspnea, which was followed by upper airway symptoms, hemoptoic sputum and constitutional symptoms, representing the prodromal phase of Churg-Strauss Syndrome. CT imaging of the paranasal sinus confirmed chronic sinusitis, which evolved into the frontal and ethmoidal sinuses in this patient’s case.
- The eosinophilic phase is characterized by peripheral eosinophilia and organ involvement, including lung, cardiac and gastrointestinal involvement. Eosinophilia is one of the hallmarks of the development of this syndrome into ANCA-associated vasculitis. It can be found in peripheral, sputum, bronchoalveolar lavage and tissue eosinophilia. Eosinophilia has been associated with several diseases that affect the small and large airways, as with many other lung diseases. Indeed, marked eosinophilia observed during the course of lung disease is not a common event, and thus, when it occurs, it generally indicates a specific diagnosis 6. A peripheral blood eosinophilia >10% is one of the clinical criteria for Churg-Strauss Syndrome diagnosis. Migratory infiltrates in lung imaging is another hallmark of Churg-Strauss Syndrome and one of the diagnostic criteria of the American College of Rheumatology. Chest CT scanning is a more sensitive method for evaluating the infiltrates 2. Extravascular eosinophil can be evaluated by performing a tissue biopsy. Histopathological analysis of the lungs has revealed that Churg-Strauss Syndrome can present with an eosinophil-rich granulomatous inflammation of the airways in addition to small- and medium-vessel vasculitis 7. Churg-Strauss Syndrome was originally described as a pathological triad consisting of eosinophilic infiltration, necrotizing vasculitis and extravascular granuloma formation. The early phase of the disease is characterized by extravascular tissue infiltration by eosinophils of any organ. In the vasculitis phase, signs of inflammation are observed in small to medium vessel walls. Vasculitis is characterized by fibrinoid necrosis and eosinophilic vessel wall inflammation 2. ANCA-positive patients more frequently exhibit vasculitis in histological specimens 7.
- The vasculitic phase presents with constitutional symptoms, such as fatigue, fever and weight loss. Paradoxically, an apparent improvement of asthma symptoms can also occur. Peripheral neuropathy can occur as multiplex mononeuritis or sensorimotor peripheral neuropathy. Renal manifestations can range from isolated urinary abnormalities to rapidly progressive glomerulonephritis. The most common presentation is pauci-immune focal and segmental necrotizing glomerulonephritis, with or without crescents, which usually involve less than 50% of the glomeruli 2. Skin lesions are also a prominent feature of the vasculitic phase and occur most commonly as palpable purpura and nodules 2. Neurologic involvement is observed in up to 60–70% of patients 8. Patients may present with multiplex mononeuritis or a mixed sensorial and motor peripheral neuropathy. The central nervous system is involved in 25% of cases with neurological involvement 2.
Churg-Strauss syndrome life expectancy
As compared with initial descriptions of Churg-Strauss syndrome (eosinophilic granulomatosis with polyangiitis) showing poor survival, patient outcomes have dramatically improved over the past 2 decades, although there is still no cure. Before the use of steroids, 50% of untreated patients die within 3 months of the onset of vasculitis. Treatment of eosinophilic granulomatosis with polyangiitis with systemic steroids has improved the survival of patients. At 1 and 5 years post-diagnosis, survival rates now exceed 90% and 85%, respectively 9, 10. Besides advances in the therapeutic management of Churg-Strauss syndrome, better awareness and recognition of this rare condition have clearly contributed to improved survival.
However, vasculitis relapse occur in up to 35% of the patients. Asthma, which is not considered to be directly due to the vasculitis, persists in more than 70% of patients even when the vasculitis is not active. Thus, patients may require continuing low doses of prednisone and/or inhaled corticosteroids for several months or years.
At least half of deaths in Churg-Strauss syndrome (eosinophilic granulomatosis with polyangiitis) are due to heart involvement.
Churg-Strauss syndrome prognosis
Prognostic criteria predicting survival in Churg-Strauss syndrome (eosinophilic granulomatosis with polyangiitis)
|
|
|
|
|
Cardiac involvement is the major cause of death and poor prognosis in Churg-Strauss Syndrome, occurring in as many as 27–47% of Churg-Strauss Syndrome cases 11. Clinical manifestations include congestive heart failure, myocarditis, pericarditis, valvular heart abnormalities myocardial ischemia and arrhythmia 11. It is more commonly found in ANCA-negative patients and directly correlates with blood eosinophilia 11.
Churg-Strauss Syndrome complications
Churg-Strauss syndrome can affect many organs, including your lungs, skin, gastrointestinal system, kidneys, muscles, joints and heart. Without treatment, the disease may be fatal. Complications depend on the organs involved and may include:
- Peripheral nerve damage. Peripheral nerves extend throughout your body, connecting your organs, glands, muscles, and skin with your spinal cord and brain. Churg-Strauss syndrome can damage the nerves in your hands and feet (peripheral neuropathy), leading to numbness, burning and loss of function.
- Skin scarring. The inflammation may cause sores to develop that can leave scars.
- Heart disease. Heart-related complications of Churg-Strauss syndrome include inflammation of the membrane surrounding your heart (pericarditis), inflammation of the muscular layer of your heart wall (myocarditis), heart attack and heart failure.
- Kidney (renal) damage. If Churg-Strauss syndrome affects your kidneys, you may develop glomerulonephritis. This is a kidney disease that hampers your kidneys’ filtering ability, leading to a buildup of waste products in your bloodstream (uremia). Kidney failure is uncommon.
Cardiac involvement represents the main potential and initial complication of Churg-Strauss Syndrome, along with treatment-induced adverse events, especially infections. In the long term, congestive heart failure and other cardiovascular complications due to long-term treatments or cardiac vasculitis involvement, can also occur. Comprehensive and long term follow-up is necessary.
Churg-Strauss syndrome cause
The cause of Churg-Strauss syndrome is unknown but the presence of asthma, eosinophilia and raised immunoglobulin E levels suggest an allergic process and autoimmune process. This means that the antibodies in the body is targeting and destroying the body’s own tissue. Most patient have asthma, often with an allergic component as well as nasal polyps. In few cases, exposure to some environmental inhaled allergens, vaccinations, desensitization or drugs (like leukotriene receptor antagonists used for treating asthma), penicillin, penicillamine, iodides and mesalazine have been incriminated as potential triggers or precipitating factors for Churg-Strauss syndrome onset or flares in some patients.
Some people have developed Churg-Strauss syndrome after using an asthma and allergy medication called montelukast or after switching from low-dose oral systemic steroids to inhaled steroid medications. But no clear connection between Churg-Strauss syndrome and any medication has been proved.
Because of the possible connection between montelukast and Churg-Strauss syndrome, your doctor may take you off this medication to see if your signs and symptoms improve.
Risk factors for Churg-Strauss syndrome
Possible risk factors for Churg-Strauss syndrome include:
- Age. On average, people with Churg-Strauss syndrome are diagnosed between 30 and 50 years of age.
- History of asthma or nasal problems. Most people diagnosed with Churg-Strauss syndrome have a history of nasal allergies, chronic sinusitis or asthma, which is often severe or hard to control.
Churg-Strauss syndrome symptoms
Churg-Strauss syndrome (eosinophilic granulomatosis with polyangiitis) predominantly affects the small-sized arteries in the body. The symptoms depend on which organs are affected and to which extent. Thus, symptoms vary from one person to another and not all symptoms are present in everyone at the time of diagnosis or during the course of the disease. However, almost all patients have asthma and/or nasal sinus polyps and blood eosinophilia. Of note, eosinophilia is relatively frequent in patients with common allergic asthma even when a patient does not have Churg-Strauss syndrome.
Other features of Churg-Strauss syndrome can include:
- Fever
- Fatigue
- Rapid and sudden weight loss
- Muscle and joint pain
- Skin rash (purpura, subcutaneous nodules or recurrent and diffuse hives)
- Numbness or tingling of the hands or feet
- Sudden loss of strength in the hands or feet
- Chest pain or palpitations (unpleasant awareness of your own heartbeat, which can be irregular)
- Increasing shortness of breath or coughing (not improving with conventional anti-asthma drugs)
- Venous thrombotic events (phlebitis or pulmonary embolism)
- Abdominal pain
- Presence of blood in the stools
Churg-Strauss syndrome (eosinophilic granulomatosis with polyangiitis) has been divided into 3 distinct phases, which may or may not be sequential.
Symptoms depend upon the phase and organs involved.
Prodromal phase (Allergic stage)
Respiratory symptoms dominate, especially asthma.
- Asthma. The primary sign of Churg-Strauss syndrome, asthma develops on average three to nine years before other signs and symptoms appear. In people with Churg-Strauss syndrome who already have asthma, symptoms usually become worse and may require steroids for control. Other people develop what is known as late-onset asthma. Developing asthma, even later in life, doesn’t necessarily mean that you have Churg-Strauss syndrome.
- Allergic rhinitis (hay fever) may also occur. This affects the mucous membranes of your nose, causing a runny nose, sneezing and itching.
- Sinus pain and inflammation (sinusitis). You may experience facial pain and develop nasal polyps, which are soft, noncancerous (benign) growths that develop as a result of chronic inflammation.
Second phase (Eosinophilic phase)
- Peripheral blood eosinophilia
- Eosinophilic tissue infiltration in the lungs and/or intestine
- Weight loss, fever, sweats, abdominal pain and diarrhea may occur
An eosinophil is a type of white blood cell that helps your immune system fight certain infections. Normally, eosinophils make up only a small percentage of white blood cells. In people with Churg-Strauss syndrome, abnormally high numbers of these cells (hypereosinophilia) are found in the blood or tissues, where they can cause serious damage.
Signs and symptoms of hypereosinophilia depend on which part of your body is affected. Your lungs and digestive tract — including your stomach and esophagus — are involved most often.
Signs and symptoms of the hypereosinophilia phase may include:
- Fever
- Loss of appetite and weight loss
- Night sweats
- Joint pain
- Asthma
- Fatigue
- Cough
- Abdominal pain and gastrointestinal bleeding
Vasculitic phase
- May involve any organ: the heart is most frequently involved but the lung, kidney, lymph nodes and muscle can also be affected
- Symptoms may include bloody diarrhea, blood in the urine, joint aches, inflammation of the heart, convulsions, coma and damage to skin nerves
- Asthma may lessen as the disease progresses
- Skin involvement occurs in more than two thirds of patients:
- Blisters, bleeding areas and nodules (lumps), often with central black dimple due to tissue breakdown (necrosis).
- Affects backs of arms or fronts of legs, especially elbows and knees. Scalp or trunk may be involved.
- Crops of new lesions may appear over months.
Depending on which organs are affected, you may experience:
- Weakness, fatigue or a general feeling of being unwell
- Unintended weight loss
- Swollen lymph nodes
- Rash or skin sores
- Joint aches and swelling
- Severe pain, numbness and tingling in your hands and feet (peripheral neuropathy)
- Severe abdominal pain
- Diarrhea, nausea and vomiting
- Shortness of breath (dyspnea) from asthma or congestive heart failure
- Cough
- Chest pain
- Irregular heartbeat
- Blood in your urine (hematuria)
Churg-Strauss syndrome diagnosis
Churg-Strauss Syndrome is a rare disease with an incidence of about 1 to 2 per million people and a prevalence of about 10 to 15 per million 12. Hence, most physicians will not likely see more than a couple of Churg-Strauss Syndrome cases during their career.
Churg-Strauss Syndrome is a challenging disease to diagnose and consequently, many patients are diagnosed in the later stages of the disease after permanent organ damage, and tragically, even death occur.
The American College of Rheumatology 6 criteria
The disease is generally considered to be present if a person has four of the six criteria, but your doctor may feel confident diagnosing Churg-Strauss syndrome even if you meet only two or three of the criteria, which include:
- Asthma. Most people diagnosed with Churg-Strauss syndrome have chronic, often severe asthma.
- Higher than normal count of a type of white blood cells called eosinophils (eosinophilia). Eosinophils normally make up 1 to 3 percent of white blood cells. A count higher than 10 percent is considered abnormally high and a strong indicator of Churg-Strauss syndrome.
- Damage to one or more nerve groups (mononeuropathy or polyneuropathy). Most people with Churg-Strauss syndrome have a type of nerve damage called peripheral neuropathy, which causes numbness or pain in your hands and feet.
- Migratory spots or lesions on a chest X-ray (pulmonary infiltrates). These lesions typically move from one place to another or come and go. On chest X-rays, the lesions mimic pneumonia.
- Sinus problems. A history of acute or chronic sinusitis is common in people with Churg-Strauss syndrome.
- White blood cells present outside your blood vessels (extravascular eosinophils). Your doctor may order a tissue biopsy of either your skin or a removed nasal polyp. A biopsy of a person with Churg-Strauss syndrome may show the presence of eosinophils outside of a blood vessel.
The most frequent clinical settings that should alert physicians (and patients) to the possibility of Churg-Strauss Syndrome are relatively easy to identify and remember.
- Asthma, especially late-onset asthma (i.e., starting in adulthood), that gradually worsens and becomes refractory to usual antiasthma drugs, with increased eosinophilia on white blood cell count. In most of these cases, allergic asthma or allergic bronchopulmonary aspergillosis is diagnosed, but early stages of Churg-Strauss Syndrome can present in this way.
- Recurrent bronchitides and/or “pneumoniae” in a patient with background asthma, especially late-onset asthma, with increased eosinophilia on white blood cell count. In most of these cases, “simple” infection, allergic bronchopulmonary aspergillosis or eosinophilic pneumonia is diagnosed, but early stages of Churg-Strauss Syndrome can present in this way.
- Worsening, lingering and/or recurrent sino-nasal polyposis and/or sinusitis, especially if associated with (late-onset) asthma, with increased eosinophilia on white blood cell count. These manifestations are not sufficient for a diagnosis of Churg-Strauss Syndrome because of no vasculitis, but early stages of Churg-Strauss Syndrome can present in this way.
- Recurrent skin rash (any type) or hives with increased eosinophilia on white blood cell count. In most of these cases, simple allergy or chronic urticaria is diagnosed, but early 4 stages of Churg-Strauss Syndrome can present in this way and many different types of skin lesions can occur in Churg-Strauss Syndrome.
- In a patient with asthma and/or sino-nasal polyposis, any symptoms of systemic vasculitis, including skin purpuric rash, numbness, tingling or weakness in hands or feet (mononeuritis multiplex), scleritis (or episcleritis), or renal disease (microscopic hematuria being the first manifestation of glomerulonephritis). Other possible and/or more severe manifestations, such as coronary arteritis or gut perforations due to inflammation and occlusion of the small vessels of the bowels, are rare features of Churg-Strauss Syndrome that are more easily considered related to vasculitis (Churg-Strauss Syndrome or another type of vasculitis).
- In a patient with asthma and/or sino-nasal polyposis, any new or worsening general or constitutional symptoms, including fever, joint pain, diffuse muscle pain, major involuntary weight loss, chest pain, palpitations or abdominal pain. These symptoms are not specific but may be the first signs of a vasculitis, including Churg-Strauss Syndrome.
There is no specific blood test for Churg-Strauss Syndrome. Investigations usually include:
- Complete blood count
- Rheumatoid factor (RhF), antinuclear antibody (ANA), antineutrophil antibodies (ANCA)
- Kidney, liver and muscle function tests, as indicated by symptoms and signs
- Imaging studies may include X-rays of the lungs and sinuses, and electrocardiogram (ECG).
- Skin biopsy and/or kidney biopsy may demonstrate the diagnostic combination of tissue eosinophilia, leukocytoclastic vasculitis and granulomas.
In such cases, it is wise to check the blood cell count, including eosinophil count; check some inflammatory signs such as level of C-reactive protein (CRP) and/or erythrocyte sedimentation rate (ESR); and perhaps order an ANCA screening test as well as other investigations according to the clinical presentation (e.g., chest X-ray or CT with respiratory symptoms; CT scan of sinuses with ear nose, and throat manifestations; electromyography of peripheral nerve conduction with numbness; electrocardiography and cardiac imaging). Biopsies of skin lesions are easy to perform but may show non-specific leucocytoclastic vasculitis. The sensitivity of sinus biopsy is low (<50%). Other biopsies, such as peripheral nerve or lung lesion, may be considered depending on the clinical presentation and after review of all obtained results, which may be sufficient to consider the diagnosis of Churg-Strauss Syndrome highly probable for starting the appropriate treatment.
Churg-Strauss syndrome treatment
Patients without severe vasculitis manifestations (that is, if there is no vasculitis-related cerebral, cardiac, renal or gastrointestinal involvement) can initially be treated with corticosteroids alone. Systemic corticosteroids are the first-line therapy with more than 90% of such patients achieving remission, but one-third may experience relapses and thus require the addition of another drug. Mild disease may initially be treated with oral corticosteroids, but most authors suggest beginning therapy for extensive disease with intravenous (IV) corticosteroids. They are usually prescribed long-term.
The patient’s response to corticosteroids is often dramatic. Within 1-2 weeks eosinophilia, the ESR and muscle enzyme levels may normalize. Corticosteroids can then be tapered, and remission is normally sustained. Low-dose prednisone may be continued for residual asthma or other symptoms.
Patients with severe manifestations are generally treated with a combination of corticosteroids and an immunosuppressant drug, such as cyclophosphamide, methotrexate or azathioprine, depending on the clinical situation. Frequently a combination of corticosteroids and cyclophosphamide are used for the first three to six months, and thereafter the cyclophosphamide is switched to methotrexate or azathioprine for maintenance for several additional months.
If vasculitic symptoms are uncontrolled or if large doses of steroids are required, cyclophosphamide may be used. This appears to improve outcome in severe disease and may reduce the chance of relapse.
Immune globulin. Given as a monthly infusion, immune globulin is generally given to people who haven’t responded to other treatments. The most common side effects are flu-like symptoms that usually last just a day or so. Immune globulin has two major drawbacks: It’s very expensive, and it doesn’t work for everyone.
Other medications reported to be useful in Churg-Strauss Syndrome include:
- Methotrexate
- Tumour necrosis factor (TNF) blockers, such as infliximab and etanercept
- Recombinant interferon (IFN)-alpha
- Rituximab
These medications have only been studied in small trials, and their long-term safety and efficacy is still unknown. They may be suggested for those who haven’t responded to other treatments.
Antibiotic prophylaxis with sulfamethoxazole-trimethoprim may be advised because intense immunosuppression increases the risk of infection.
Monitoring the disease
Patients require close and prolonged follow-up with their doctors with periodic monitoring of the disease activity which is done based on symptoms and laboratory evaluations. In addition to monitoring for disease relapses, patients also need to be monitored for problems related to asthma, organ damage due to vasculitis, cardiovascular status and treatment related side effects.
Blood eosinophil count and parameters of inflammation (sedimentation rate or C reactive protein) are among the tests ordered on a regular basis to monitor disease activity. However, these test results should be interpreted cautiously because they can be altered in several other conditions (allergies, infections etc).
Lifestyle and home remedies
Long-term treatment with prednisone can cause a number of side effects. You can minimize these problems by taking the following steps:
- Protect your bones. Ask your doctor how much vitamin D and calcium you need in your diet, and discuss whether you need to take any supplements.
- Exercise. Exercise can help you maintain a healthy weight, which is important when you’re taking corticosteroid medications that can cause weight gain.
- Strength training and weight-bearing exercises such as walking and jogging also help improve bone health.
- Stop smoking. This is one of the most significant things you can do for your overall health. By itself, smoking causes serious health problems. It also makes problems you already have worse and can increase the side effects of medications you’re taking.
- Adopt a healthy diet. Steroids can cause high blood sugar levels and, eventually, type 2 diabetes. It helps to include in your diet foods that help keep blood sugar stable, such as fruits, vegetables and whole grains.
Keep doctor appointments. During therapy for Churg-Strauss syndrome, your doctor will monitor you closely for side effects. This will likely include regular bone scans, eye exams, and tests for blood pressure, blood sugar and cholesterol levels. If caught in time, it’s possible to reverse many of the side effects resulting from steroid use.
He or she will also look for signs of Churg-Strauss syndrome affecting new organs (relapse).
Coping and support
Churg-Strauss syndrome is a serious disease. Even when it’s in remission, you may worry about the possibility of recurrence or about long-term damage to your heart, lungs and nerves. Here are some suggestions for coping with the disease:
- Educate yourself about Churg-Strauss syndrome. The more you know, the better prepared you may be to deal with complications or recurrences. Besides talking to your doctor, you may want to talk to a counselor or medical social worker. Or you may find it helpful to talk to other people with Churg-Strauss syndrome.
- Maintain a support system. Family and friends can help tremendously. But sometimes you may find it especially helpful to talk with others who with Churg-Strauss syndrome. Your doctor or a medical social worker may be able to put you in touch with a support group.
- What is Eosinophilic Granulomatosis with Polyangiitis (Churg-Strauss Syndrome). http://www.cssassociation.org/what-is-churg-strauss-syndrome.html[↩]
- Greco A., Rizzo M.I., De Virgilio A., Gallo A., Fusconi M., Ruoppolo G. Churg-Strauss syndrom. Autoimmun. Rev. 2015 Apr;14(4):341–348. https://www.ncbi.nlm.nih.gov/pubmed/25500434[↩][↩][↩][↩][↩][↩][↩]
- Baldini C., Talarico R., Della Rossa A., Bombardieri R. Clinical manifestations and treatment of Churg–Strauss syndrome. Rheum. Dis. Clin. North Am. 2010 Aug;36(3):527–543. https://www.ncbi.nlm.nih.gov/pubmed/20688248[↩][↩]
- Abril A., Calamia K.T., Cohen M.D. The Churg Strauss syndrome (allergic granulomatous angiitis): review and update. Semin. Arthritis Rheum. 2003 Oct;33(2):106–114. https://www.ncbi.nlm.nih.gov/pubmed/14625818[↩]
- Santos YAP, Silva BRA, Lira PNZBA, et al. Eosinophilic granulomatosis with polyangiitis (formerly known as Churg-Strauss syndrome) as a differential diagnosis of hypereosinophilic syndromes. Respiratory Medicine Case Reports. 2017;21:1-6. doi:10.1016/j.rmcr.2017.03.006. https://www.ncbi.nlm.nih.gov/pmc/articles/PMC5352719/[↩]
- Woolnough K., Wardlaw A. Eosinophilia in pulmonary disorders. Immunol. Allergy Clin. N. Am. 2015 Aug;35(3):477492. https://www.ncbi.nlm.nih.gov/pubmed/26209896[↩]
- Sharma A., Dogra S., Sharma K. Granulomatous vasculitis. Dermatol. Clin. 2015 Jul;33(3):475–487. https://www.ncbi.nlm.nih.gov/pubmed/26143427[↩][↩]
- Woolnough K., Wardlaw A. Eosinophilia in pulmonary disorders. Immunol. Allergy Clin. N. Am. 2015 Aug;35(3):477492.https://www.ncbi.nlm.nih.gov/pubmed/26209896[↩]
- Comarmond, C., et al., Eosinophilic granulomatosis with polyangiitis (Churg-Strauss): clinical characteristics and long-term followup of the 383 patients enrolled in the French Vasculitis Study Group cohort. Arthritis Rheum, 2013. 65(1): p. 270-81.[↩]
- Moosig, F., et al., A vasculitis centre based management strategy leads to improved outcome in eosinophilic granulomatosis and polyangiitis (Churg-Strauss, EGPA): monocentric experiences in 150 patients. Ann Rheum Dis, 2013. 72(6): p. 1011-7.[↩]
- Mahra A., Moosig F., Neumann T., Szczeklik W., Taillé C., Vaglio A. Eosinophilic granulomatosis with polyangiitis (Churg-Strauss): evolutions in classification, etiopathogenesis, assessment and management. Curr. Opin. Rheumatol. 2014 Jan;26(1):16–23. https://www.ncbi.nlm.nih.gov/pubmed/24257370[↩][↩][↩]
- Vaglio, A., C. Buzio, and J. Zwerina, Eosinophilic granulomatosis with polyangiitis (Churg-Strauss): state of the art. Allergy, 2013. 68(3): p. 261-73.[↩]