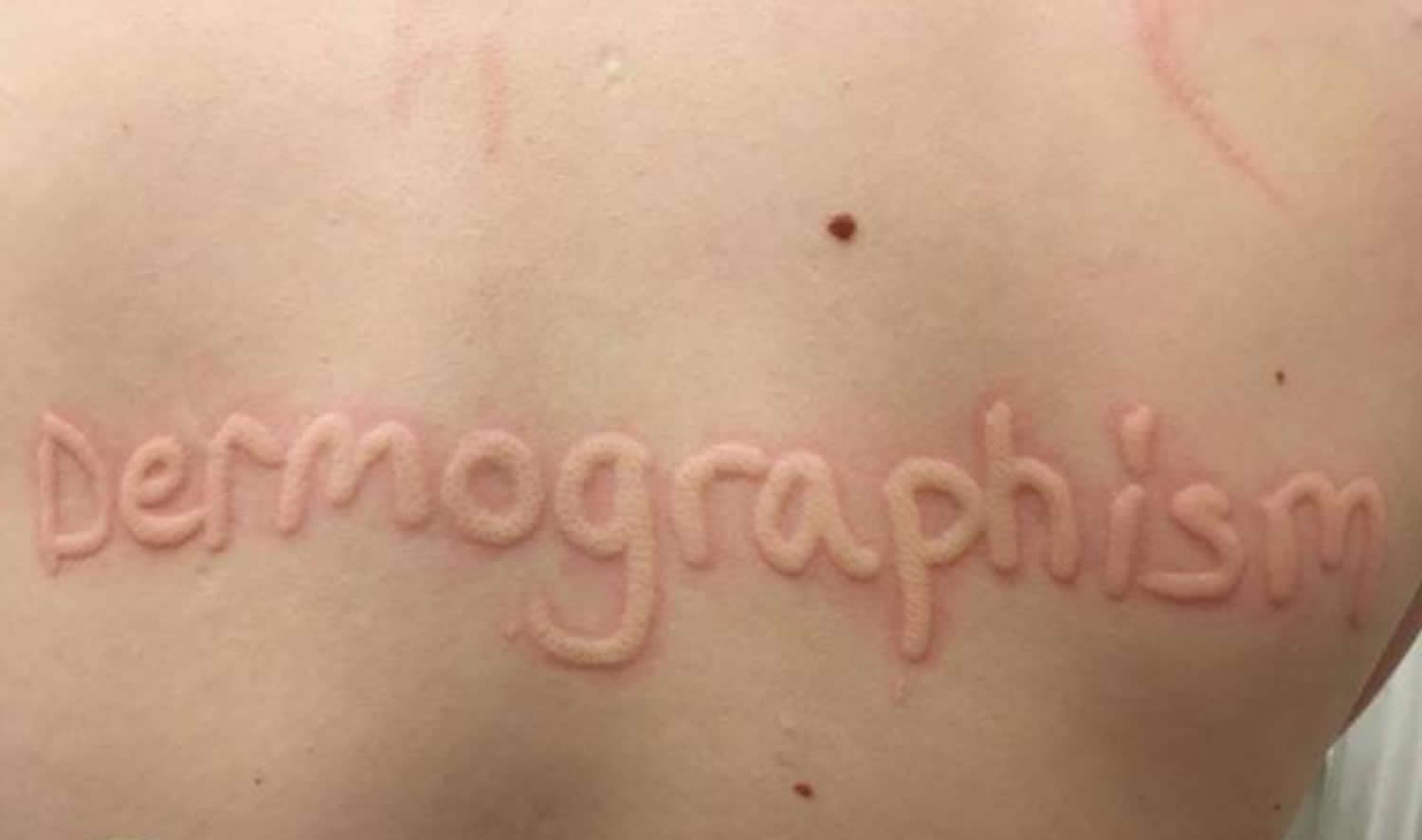Contents
What is dermatographic urticaria
The term dermographism (or dermatographism) literally means writing on the skin. When people who have dermatographic urticaria lightly scratch their skin, the scratches redden into a raised wheal similar to hives. These marks usually disappear within 30 minutes 1. Itching and whealing can affect all body surfaces, but the scalp and genitalia are less frequently involved.
Dermographism can be distressing but is not life threatening.
Histamine is the main chemical released by mast cells when the skin is stroked, but other chemical mediators may also be involved. Firm stroking of the skin releases produces an initial red line (capillary dilatation), followed by an axon-reflex flare with broadening erythema (arteriolar dilatation) and the formation of a linear wheal (transudation of fluid/edema).
Dermatographic urticaria is the most common of the physical urticarias and can occur with other forms of urticaria. An increased incidence has been reported during pregnancy (especially in the second half), at the onset of menopause, in atopic children, and in patients with Behçet disease 2.
Dermatographic urticaria can appear in persons of any age but is more common in young adults; the peak incidence is in the second and third decades. Whether a sexual variance in prevalence occurs is unclear. None has been consistently reported, though one study on dermatographic urticaria in children reported a female predominance 3. No racial variance in prevalence is known.
Some patients with severe dermatographic urticaria may carry an autoantibody to some unknown cutaneous protein.
Occasionally dermatographic urticaria is triggered by an allergy to some external agent such as penicillin, scabies or a worm infestation. Most people with dermatographic urticaria do not have an allergy.
Figure 1. Dermatographic urticaria

An exaggerated response to this constitutional whealing tendency is seen in approximately 2-5% of the population and is referred to as dermographism. In a minority of people, it is accompanied by itching (symptomatic dermographism).
The cause of dermatographic urticaria is unknown, but it can be triggered in some people by infections, emotional upset or medications such as penicillin.
Most people who have dermatographia don’t seek treatment. If your signs and symptoms are especially bothersome, your doctor may recommend allergy medications such as cetirizine (Zyrtec) or diphenhydramine (Benadryl).
Dermatographic urticaria symptoms
The onset of dermatographic urticaria is usually gradual, but in some the condition develops over a few days. In patients with symptomatic dermatographic urticaria, the skin eruption is associated with itching, which is often most severe at night.
Symptoms can be aggravated by heat (e.g, from a hot bath), minor pressure (e.g, from scratching, from friction with clothes, or from rubbing with towels), exercise, stress, and emotion.
Once a few weals develop, subsequent scratching readily starts others in the vicinity.
- The weals are usually on the surface but some deep extension may occur and giant weals develop.
- The weals die away rapidly and usually clear after half to one hour.
Signs and symptoms of dermatographic urticaria may include:
- Raised red lines
- Swelling
- Inflammation
- Hive-like welts
- Itching
The signs and symptoms may occur within a few minutes of your skin being rubbed or scratched and usually disappear within 30 minutes. Rarely, dermatographic urticaria develops more slowly and lasts several hours to several days.
The condition itself can last for months or years.
When to see a doctor
See your doctor if your signs and symptoms are particularly bothersome.
Dermatographic urticaria causes
The exact mechanism of dermatographic urticaria remains uncertain. It may be caused by an allergic response, yet no specific allergen has been identified.
Simple things can trigger symptoms of dermatographic urticaria. For example, rubbing from your clothes or bed sheets may irritate your skin. Sometimes, dermatographic urticaria is preceded by an infection, emotional upset or medications, such as penicillin.
Trauma may release an antigen that interacts with the membrane-bound immunoglobulin E (IgE) of mast cells, which release inflammatory mediators, particularly histamine, into the tissues. This process causes small blood vessels to leak, allowing fluid to accumulate in the skin. Other mediators that may be involved are leukotrienes, heparin, bradykinin, kallikrein, and peptides such as substance P.
Approximately 75% of patients with hypereosinophilic syndrome, which has multisystem involvement and high mortality, have dermatographic urticaria. Psychological factors and a history of stressful life events have been implicated as triggering factors in 30% of patients 4. However, a small prospective study showed no alteration in dermographic reaction after social stress provocation tests 5.
One case report describes symptomatic dermographism secondary to trauma from a coral reef 6. Symptomatic dermatographic urticaria may be a presenting feature of dermatomyositis 7.
Who gets dermatographic urticaria ?
Dermatographic urticaria can appear at any age but is most common in young adults.
- Dermatographic urticaria can occur with other types of urticaria (hives) including those due to cold or pressure.
- An association with thyroid disease has been noted, but is likely a reflection of an underlying tendency to autoimmune disease and does not appear to have a causative relationship.
People with dermatographic urticaria are usually otherwise healthy.
Prevention of dermatographic urticaria
To reduce discomfort and prevent the symptoms of dermatographia, try these tips:
- Avoid irritating your skin. Refrain from using harsh soaps on your skin. Don’t wear clothing made of itchy material, such as wool. Hot showers or baths may worsen the symptoms.
- Don’t scratch your skin. If you have dermatographia or other skin conditions that may cause frequent itching, try to avoid scratching your skin. Scratching will aggravate the condition.
- Keep your skin moisturized. Dry skin tends to make skin itchy. Keep your skin moisturized by using lotions and creams after bathing.
Diagnosis of dermatographic urticaria
Your doctor can diagnose dermatographic urticaria with a simple test. He or she will draw a tongue depressor across the skin of your arm or back to see if a red, swollen line or a welt (wheal) appears within a few minutes.
Dermatographic urticaria treatment
Symptoms of dermatographia usually go away on their own, and treatment for dermatographia generally isn’t necessary. Patients with simple dermatographic urticaria are asymptomatic and require no therapy. However, if the condition is severe or bothersome, your doctor may recommend antihistamine medications such as diphenhydramine (Benadryl), fexofenadine (Allegra) or cetirizine (Zyrtec).
Antihistamines usually give good relief from symptoms. Non-sedating options include:
- Cetirizine
- Loratidine
- Fexofenadine.
Antihistamines may need to be continued daily for at least several months; intermittent therapy is of less value.
Recognition of the problem, avoidance of precipitating physical stimuli, reduction of stress and anxiety are important factors in medical care. In addition, scratching because of dry skin can be reduced through good skin care and the use of emollients.
Pharmacologic therapy
H1 antihistamines are the drugs of choice. In some patients, a combination of 2 or more antihistamines may be required. Sedating antihistamines such as hydroxyzine can be helpful. Regular treatment may have to be continued for several months. In a self-reported questionnaire of patients taking H1 antihistamines,18 (23%) of 79 were completely free from symptoms, 39 (49%) of 79 had a marked improvement, and only 3 (4%) of 79) reported no effect 8. The addition of H2-receptor antagonists appears to result in little symptomatic benefit, although some studies have shown a further small reduction in the whealing response 9. Physical urticarias are usually unresponsive to systemic corticosteroids.
Omalizumab, a recombinant humanized monoclonal antibody against immunoglobulin E (IgE), has been successfully used in patients with physical urticaria, including symptomatic dermographism. It is administered subcutaneously at an initial dosage of 150 mg/mo, but the dosage can be increased to 300 mg/mo. Some patients have reported complete symptom resolution within days after the first injection 10. Omalizumab was successfully used in a woman with 3 subtypes of chronic urticaria, including symptomatic dermographism 11. Treatment was continued throughout the patient’s pregnancy without any complications or obvious adverse effects, although the frequency of injections had to be increased to every 15 days.
Reinitiation of omalizumab treatment after relapse of disease appears to result in rapid and complete symptom control again after the first injection within the first 4 weeks, and no relevant adverse effects have been reported 12.
Light therapy
Narrowband ultraviolet (UV)-B phototherapy and oral psoralen plus UV-A light therapy have both been used as treatments for symptomatic dermographism. Subjective relief of pruritus and whealing and objective reduction of wheals have been reported 13. However, the improvement is short-lived, and most patients relapse within 2-3 months of completing phototherapy.
Prognosis of dermatographic urticaria
Simple dermatographic urticaria is the most common variant, and patients with this form are asymptomatic. However, other forms are associated with pruritus, and this can significantly affect quality of life. Most people with dermatographic urticaria are otherwise healthy. An association with thyroid disease has been described in some patients but remains controversial.
The natural history of symptomatic dermatographic urticaria is unpredictable. It may last for months or years, or be present intermittently. In many patients, the condition gradually improves and clears after several years. Of the chronic urticarias, symptomatic dermatographic urticaria appears to have the best prognosis in terms of clearance after 5 years (36%) and 10 years (51%) 14.
- Dermatographia. Mayo Clinic. https://www.mayoclinic.org/diseases-conditions/dermatographia/basics/definition/con-20025360[↩]
- Dermographism and atopy in patients with Behçet’s disease. J Investig Allergol Clin Immunol. 2000; 10(6):368-71.[↩]
- Prevalence of dermographism in children. J Investig Allergol Clin Immunol. 2000; 10(3):166-9.[↩]
- Evaluation of patients with symptomatic dermographism. J Eur Acad Dermatol Venereol. 2006; 20(1):58-62.[↩]
- Urticarial dermographism: clinical features and response to psychosocial stress. Acta Derm Venereol. 2007; 87(6):493-8.[↩]
- Dermographism secondary to trauma from a coral reef. J Eur Acad Dermatol Venereol. 2006; 20(10):1337-8.[↩]
- Dermatomyositis presenting with symptomatic dermographism and raised troponin T: a case report. J Med Case Rep. 2009; 3:7319.[↩]
- Schoepke N, Mlynek A, Weller K, Church MK, Maurer M. Symptomatic dermographism: an inadequately described disease. J Eur Acad Dermatol Venereol. 2015 Apr. 29(4):708-12.[↩]
- Sharpe GR, Shuster S. In dermographic urticaria H2 receptor antagonists have a small but therapeutically irrelevant additional effect compared with H1 antagonists alone. Br J Dermatol. 1993 Nov. 129(5):575-9.[↩]
- Metz M, Altrichter S, Ardelean E, at al. Anti-Immunoglobulin E Treatment of Patients with Recalcitrant Physical Urticaria. Int Arch Allergy Immunol. 2011. 154:177-180.[↩]
- Vieira Dos Santos R, Locks Bidese B, Rabello de Souza J, Maurer M. Effects of Omalizumab in a patient with three types of chronic urticaria. Br J Dermatol. 2013 Sep 14.[↩]
- Metz M, Ohanyan T, Chruch MK, Maurer M. Retreatment with omalizumab results in rapid remission in chronic spontaneous and inducible urticaria. JAMA Dermatol. 2014 Mar. 150(3):288-90.[↩]
- Borzova E, Rutherford A, Konstantinou GN, Leslie KS, Grattan CE. Narrowband ultraviolet B phototherapy is beneficial in antihistamine-resistant symptomatic dermographism: A pilot study. J Am Acad Dermatol. Sept 2008. 59:752-7.[↩]
- The natural history of chronic urticaria and angioedema in patients visiting a tertiary referral centre. Br J Dermatol. 2002; 146(1):110-3.[↩]