Contents
What is diaper rash
Diaper rash also called nappy rash or napkin dermatitis are used to describe various skin conditions that affect the skin under a baby’s diaper. Diaper rash is most often a form of contact dermatitis.
Diaper rash is common and can happen no matter how careful you are about looking after your baby’s bottom. Almost all children who wear nappies get diaper rash at some stage. Up to a third of babies and toddlers in nappies have diaper rash at any one time. It doesn’t usually develop in newborns, but all babies can get diaper rash.
Diaper rash can be caused by:
- your baby’s skin being in contact with urine or poo (feces) for a long time. Urine and feces contain irritating substances that can penetrate broken skin and cause irritation and inflammation (redness)
- the diaper rubbing against your baby’s skin
- not cleaning the diaper area or changing the nappy often enough
- soap, detergent, bubble bath or synthetic cleaning agent, as is used in commercial ‘bubble bath’ products, dry out the skin and leave it open to cracks in the skin – which can then become a passage for infection.
- alcohol-based baby wipes
- your baby recently taking antibiotics
Irritated skin can quickly become infected with Candida, a fungal infection; this gives rise to small pustules (pimples) around the edge of the red area and requires a special cream from your chemist to clear it.
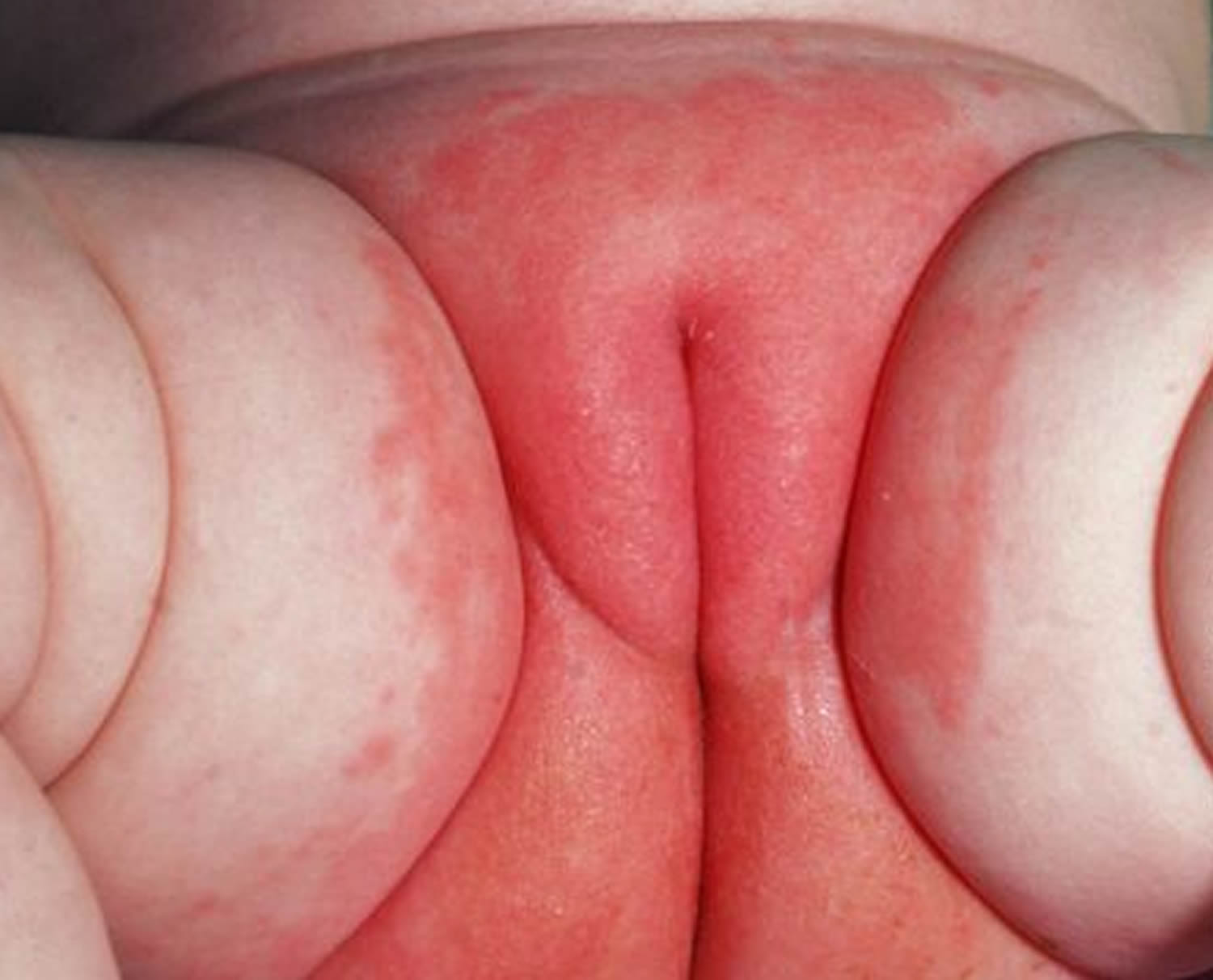
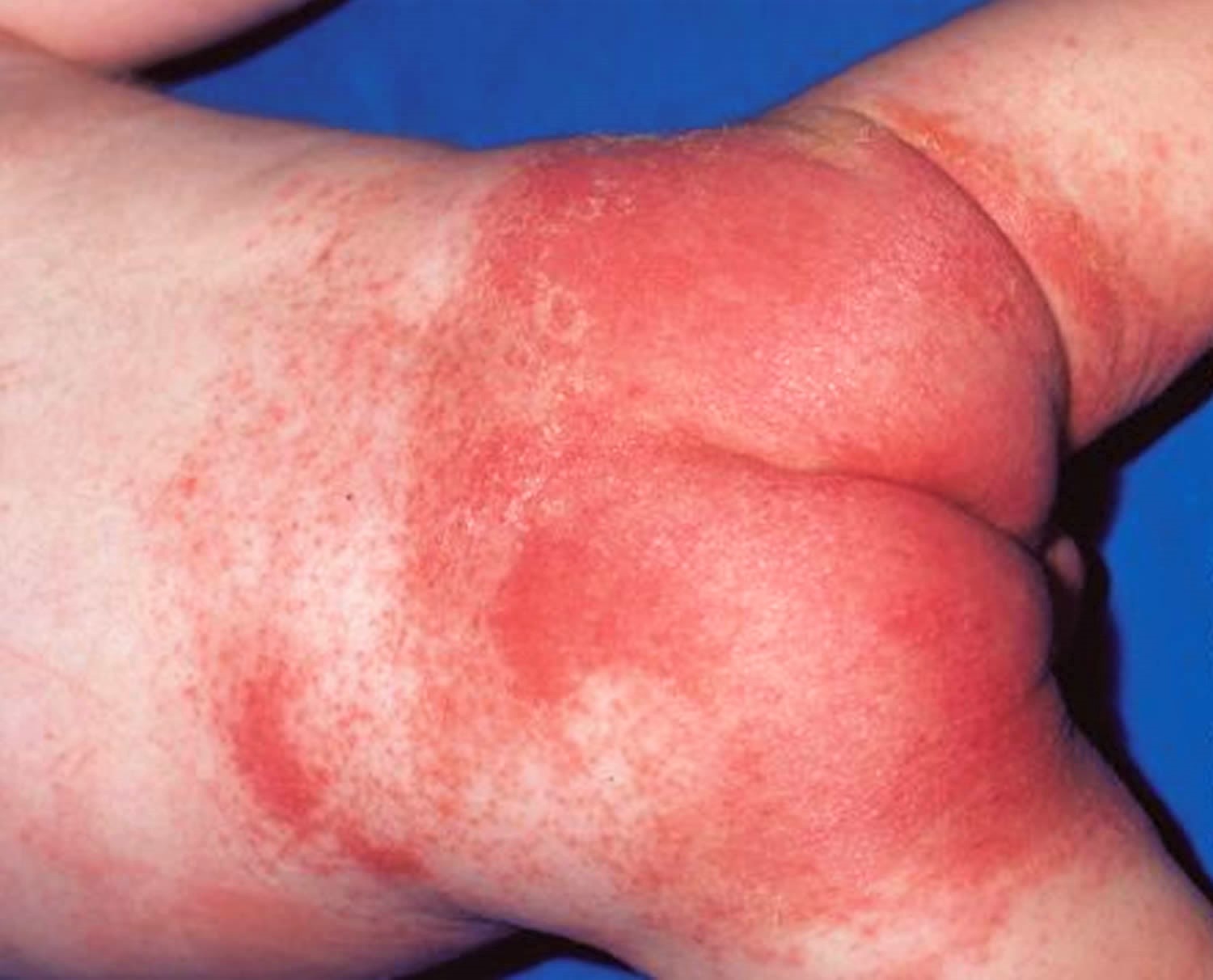
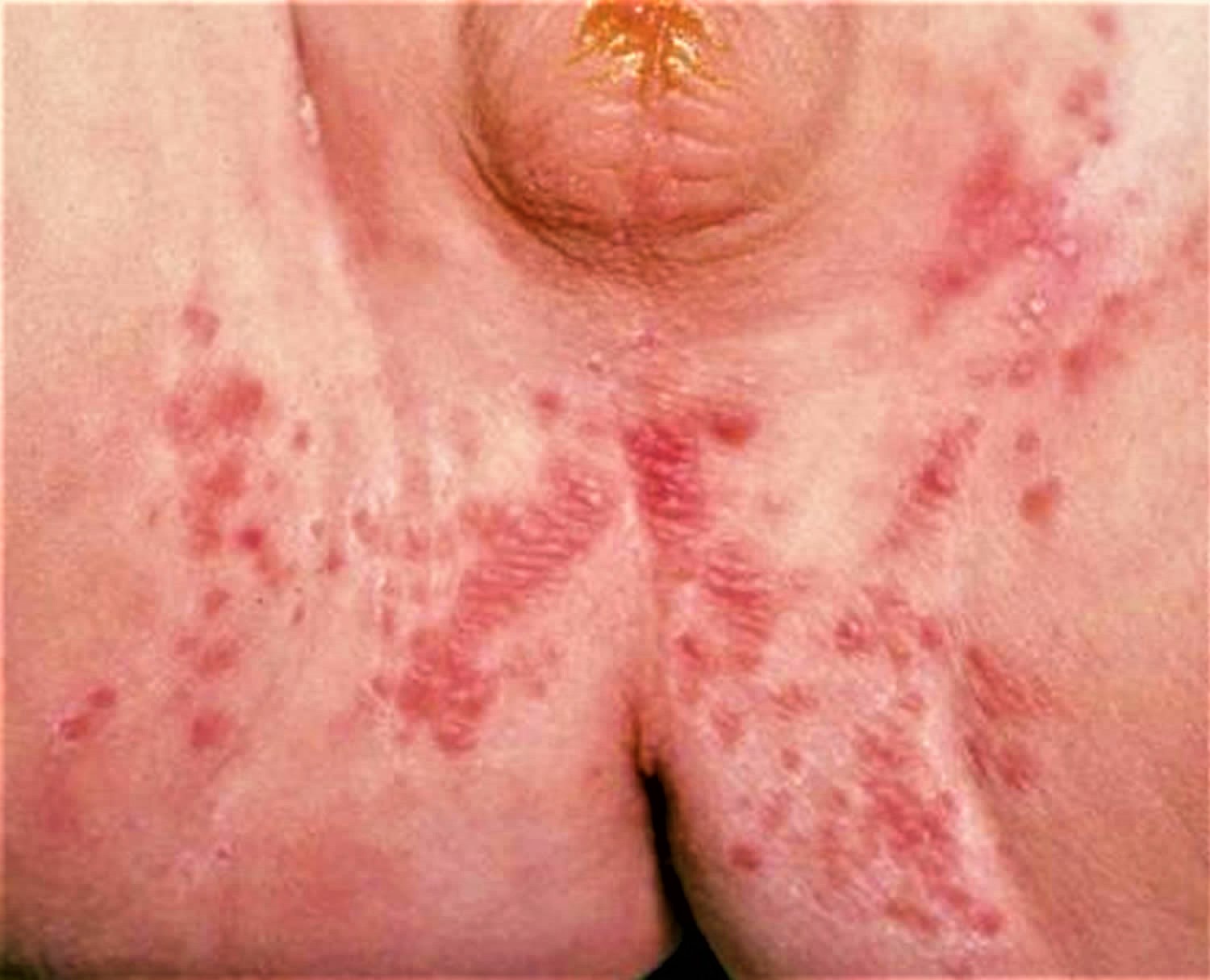
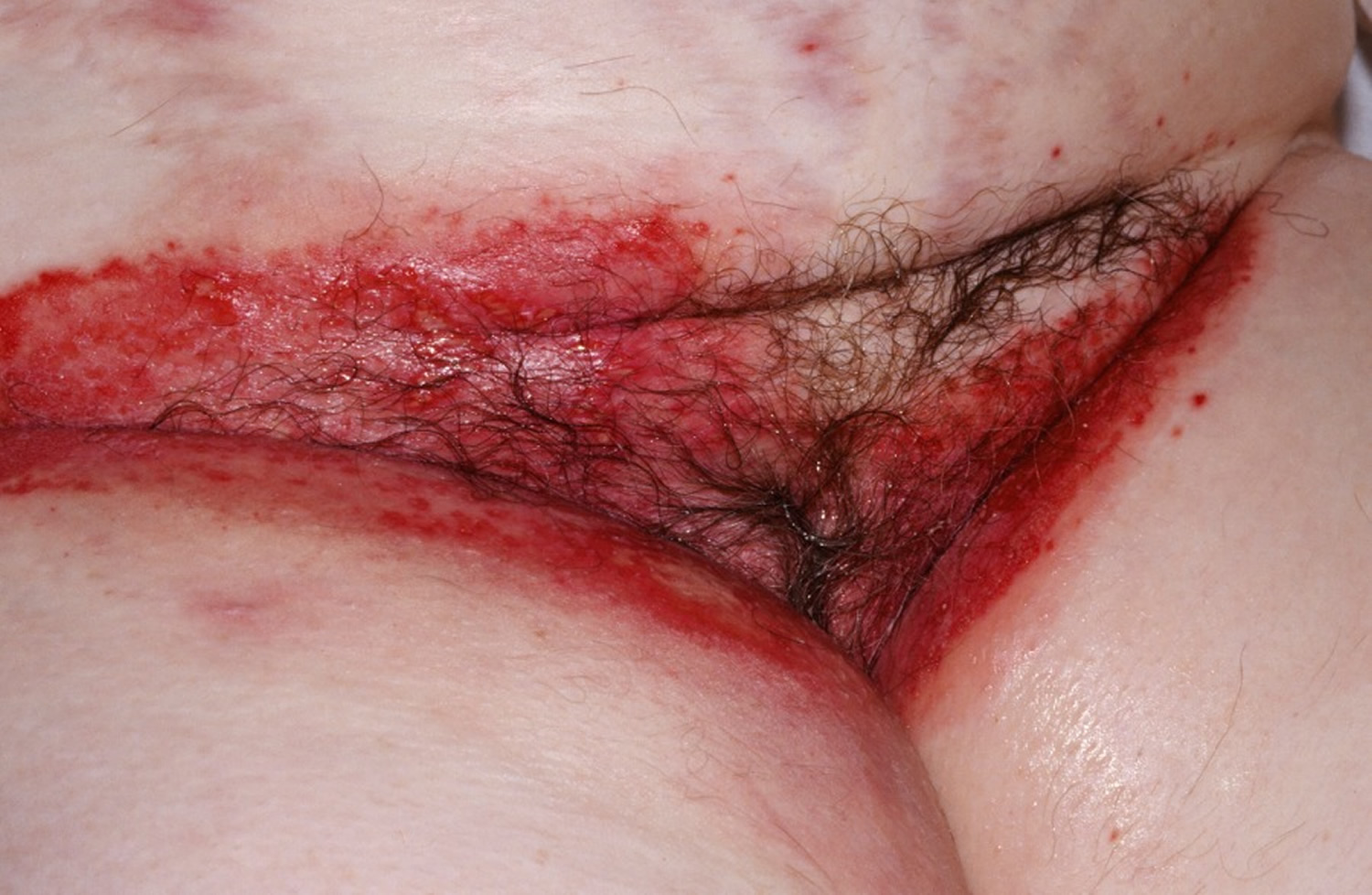
There may be red patches on your baby’s bottom, or the whole area may be red (see Figures 1 and 2). Their skin may look sore and feel hot to touch, and there may be spots, pimples or blisters.
Most babies with mild nappy rash don’t feel sore, but if the rash is severe your baby may feel uncomfortable and be distressed.
Diaper rash prevention
- Change diapers as soon as possible after they become wet or soiled
- Cleanse your baby with baby wipes or warm water and a cloth
- Give your baby some ‘diaper free’ time each day
- Avoid using plastic pants
- Wash and rinse all cloth diapers thoroughly
You should take your child to the doctor if:
- the rash hasn’t improved after three days, even when you use the treatment steps below
- blisters, crusts or pimples appear
- your child is upset and isn’t sleeping
- your child has an unexplained fever
- the rash is spreading
- the redness is severe
- the rash is in other places as well, such as your baby’s mouth, scalp, or the mother’s nipples
- the end of your son’s penis is red and swollen, or has a scab on it.
Figure 1. Baby diaper rash
Figure 2. Severe diaper rash
Diaper rash complications
It takes weeks for your baby’s skin to repair itself, so his/her skin will be more vulnerable to things that irritate it.
Secondary infections such as thrush (fungus or yeast) can happens. The warm, damp skin under your baby’s nappy provides an ideal place for Candida albicans fungi to grow. Diaper rash due to a Candida albicans fungal infection tends to be brighter red than simple diaper rash. These red areas have clearly defined borders. There may be small red or white pustules (satellite lesions) around the edge of the rash. The rash often spreads into the skin folds or onto the skin not covered by a nappy.
Candida albicans is a type of fungus normally found in the digestive (gastrointestinal) tract. If your baby is wearing a moist or blocked up (occluded) diaper, particularly one that is dirty (has fecal contamination), an inflammatory skin rash (dermatitis) may develop on the baby’s skin. Diarrhea increases the risk for developing candidal diaper dermatitis, and candida infection in the mouth (oral thrush) may also occur.
- Candidal diaper dermatitis most commonly appears in the genitals and diaper area, particularly the deep folds, and it consists of red elevated areas (papules) and flat, solid areas of skin (plaques) with sharp edges and skin flakes (scale) as well as surrounding “satellite” skin elevations containing pus (pustules).
- Redness (erythema) may appear to be joined into one area (confluent).
- Breakdown (erosions) or loss of the upper layer of skin may be present.
- Alternatively, the lesions may be merging together (coalescing) small pink bumps with overlying scale, without any redness.
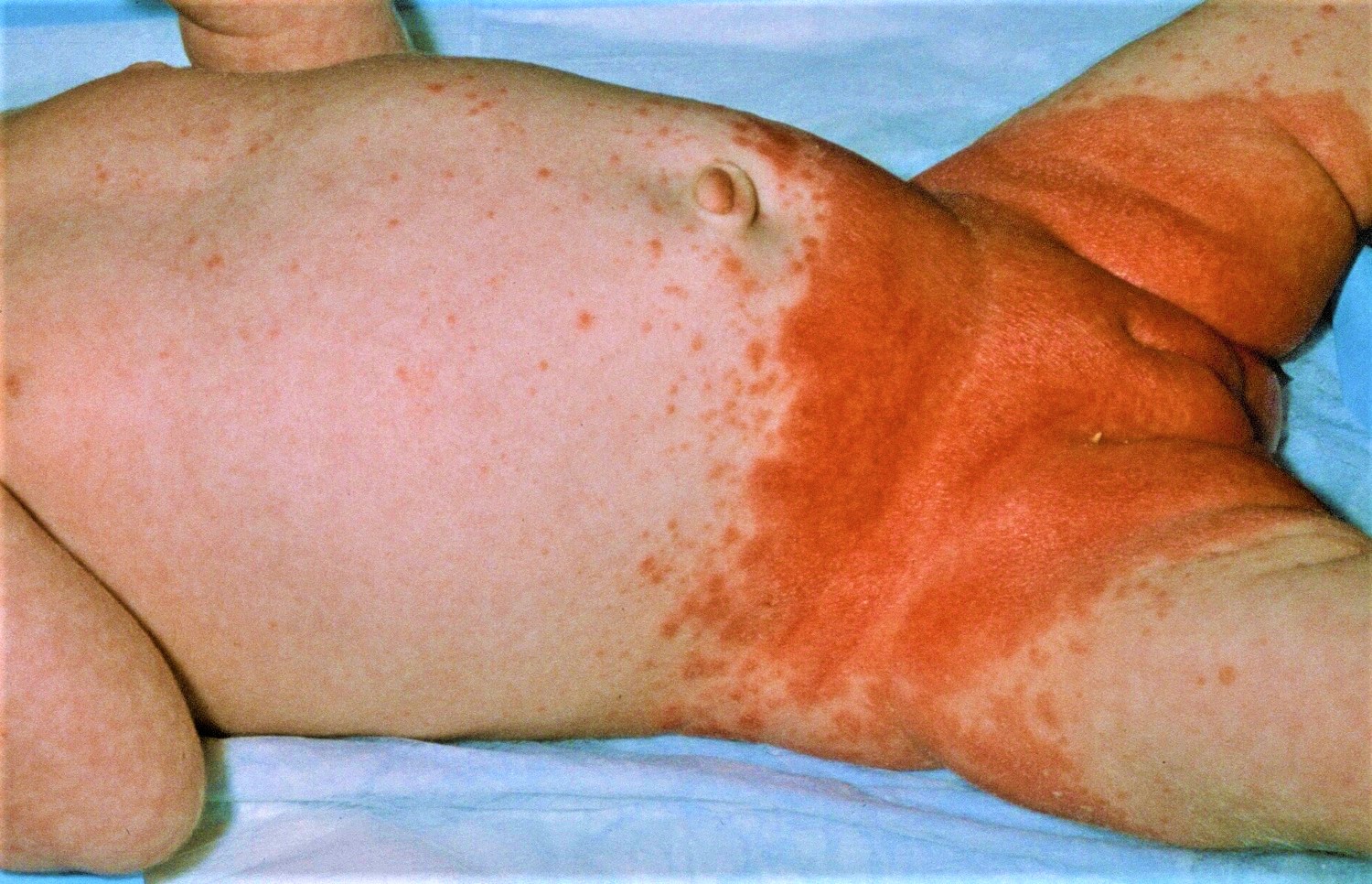
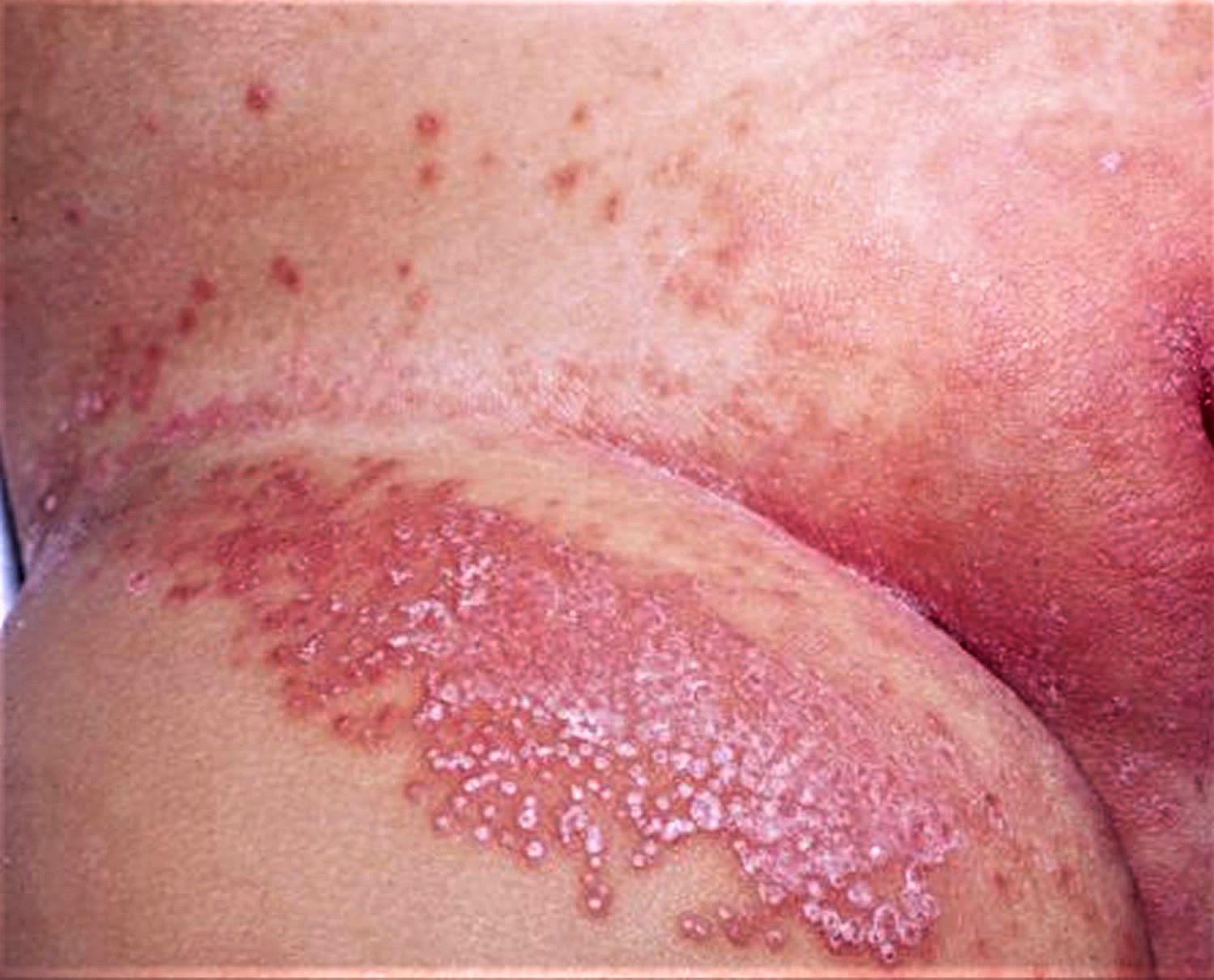
Your baby may also have a fungal infection in their mouth, called oral thrush. Their mouth will be sore and look red, and there may be white patches on their tongue or inside their cheeks. If your baby is breastfeeding, your nipples may also be affected by thrush (see Figures 3 and 4 below).
Treat thrush (diaper Candidiasis) with an antifungal cream prescribed by your doctor. Thrush can take longer to clear than regular diaper rash and often comes back. Treatment can take a long time, which can be frustrating.
Treatments your doctor may prescribe:
Topical antifungal therapies, applied twice a day:
- Nystatin cream
- Econazole cream
- Miconazole cream
- Clotrimazole cream
The doctor may also reassure you that once your baby is toilet trained, the diaper dermatitis will no longer develop.
Figure 3. Yeast infection diaper rash (Candida infection)
Figure 4. Yeast diaper rash
Figure 5. Adult diaper rash (Candida of the groin or thrush)
Diaper rash due to bacterial infection
Sometimes if a baby’s skin has been irritated and damaged by simple diaper rash it can become infected by bacteria. The skin can be red, warm and swollen and the baby may develop a fever. Parts of the skin may be broken and weeping, and a yellow crusting may be noticeable. This type of diaper rash needs to be treated by a doctor.
Diaper rash causes
Many things can combine to cause diaper rash in your child.
- The main cause is wearing a wet or dirty nappy for too long. Prolonged dampness, friction and ammonia substances released from baby’s urine can irritate your baby’s skin.
- A baby’s urine is sterile (there are no germs in urine), but there are germs on the baby’s skin, in feces and on clothing (including diapers). These germs make ammonia when wet with urine or feces. Ammonia can burn the skin.
- The nappy can rub on the skin (especially stiff cloth nappies).
- Plastic pants over the nappy prevent air flow around the nappy often make diaper rash worse, and they also hide a diaper which may be very wet or dirty, so the skin stays wet for a long time.
- Soaps and detergents left on cloth diapers after washing can also contribute to diaper rash.
Sometimes children also have other conditions such as eczema, psoriasis, thrush or impetigo, which might make diaper rash worse.
Diaper rash can be traced to a number of sources as well, including:
- Chafing or rubbing. Tightfitting diapers or clothing that rubs against the skin can lead to a rash.
- Irritation from a new product. Your baby’s skin may react to baby wipes, a new brand of disposable diapers, or a detergent, bleach or fabric softener used to launder cloth diapers. Other substances that can add to the problem include ingredients found in some baby lotions, powders and oils.
- Bacterial or yeast (fungal) infection. What begins as a simple skin infection may spread to the surrounding region. The area covered by a diaper — buttocks, thighs and genitals — is especially vulnerable because it’s warm and moist, making a perfect breeding ground for bacteria and yeast. These rashes can be found within the creases of the skin, and there may be red dots scattered around the creases.
- Introduction of new foods. As babies start to eat solid foods, the content of their stool changes. This increases the likelihood of diaper rash. Changes in your baby’s diet can also increase the frequency of stools, which can lead to diaper rash. If your baby is breast-fed, he or she may develop diaper rash in response to something the mother has eaten.
- Sensitive skin. Babies with skin conditions, such as atopic dermatitis or seborrheic dermatitis (eczema), may be more likely to develop diaper rash. However, the irritated skin of atopic dermatitis and eczema primarily affects areas other than the diaper area.
- Use of antibiotics. Antibiotics kill bacteria — the good kinds as well as the bad. When a baby takes antibiotics, bacteria that keep yeast growth in check may be depleted, resulting in diaper rash due to yeast infection. Antibiotic use also increases the risk of diarrhea. Breast-fed babies whose mothers take antibiotics are also at increased risk of diaper rash.
What triggers diaper rash?
- Many babies get diaper rash when they are unwell, particularly if they have diarrhea. Their skin seems to become more sensitive.
- Starting a new food seems to trigger the diaper rash for some babies.
- Having a wet or dirty diaper on for too long – change diapers regularly. ‘Too long’ is very variable – it depends, for example, on:
- the baby – some babies get diaper rash more easily than others
- the type of diaper – babies were more likely to get diaper rash when they wore cloth diapers with pilchers (waterproof nappy covers)
- whether or not there is feces there
- Chemicals in disposable diapers were a problem for some babies, but this seems to be much less of a problem now.
- An infection on the skin, such as thrush (Candida infection), can make the rash worse. Thrush normally lives in the gut and on skin without causing any problem, but when the skin is damaged thrush can make the damage worse.
How to change diapers or nappies
Choosing which diaper you will use for your baby will depend on what is important to you and your family. In the first few years of your child’s life, you’re going to be changing a lot of diapers – probably around 6000! There are a number of things to consider, such as cost, convenience and the environment.
There are several types of nappies that are available, some reusable, others disposable.
It isn’t clear whether cloth or disposable nappies are better at preventing diaper rash. The most important thing is to change a wet or dirty diaper straight away. Many parents prefer to use disposable diapers for a bad case of diaper rash, then go back to cloth diapers once baby’s skin has healed.
Reusable diapers
- Cloth squares – these are folded and fastened with pins or clips, and work best with a good-quality waterproof cover or pilcher. They fit snugly and are made of fabric that absorbs liquid, usually cotton (terry, flannelette), and also hemp, bamboo or a blend. Detergent makes some cloth nappies go hard over time, so using a wool mix is better.
- All-in-ones – these have a waterproof layer on the outside or near the outside layer. They’re as easy to use as disposables, but a lot cheaper. They don’t need extensive soaking or bleaching and can be fastened with velcro, clips or press studs.
- Pocket diapers – these have a water-resistant outer fitted shell, with a layer sewn to the shell along three sides and open at one end. Absorbent inserts are placed between the shell and the layer to absorb the liquid. The absorbency level can be adjusted with inserts made of different materials.
If you think you want to use cloth diapers for your baby, you’ll need around 20-24 diapers to start with, depending on your washing and drying routine, climate and season.
Washing cloth diapers
If you use cloth diapers, careful washing can help prevent diaper rash. Washing methods vary and many routines work well. They key is to clean, disinfect and remove soap residue. Here’s one effective method:
- Pre-soak heavily soiled cloth diapers in cold water.
- Wash diapers in hot water with a mild detergent and bleach. Bleach kills germs. You could also add vinegar to the wash cycle to eliminate odors and rinse out soap residue.
- Double rinse the diapers in cold water to remove traces of chemicals and soap.
- Skip fabric softener and dryer sheets because they can contain fragrances that may irritate your baby’s skin.
Disposable diapers
- Disposables – generally consist of a plastic outer layer, a layer of super-absorbent chemicals, and an inner liner. They come in different packet sizes and are made for a range of ages.
- Biodegradable disposables – these use a non-chemical absorption method. When you throw them away, they break down completely in landfill over time. They’re made from a variety of materials, such as bamboo, fabrics and paper pulp. These diapers are better for the environment, but are often more expensive than non-biodegradable disposables.
If you think you want to use disposable diapers, it’s a good idea to try a few different brands to see which one best suits your baby and budget.
You’ll need up to 12 diapers a day for a newborn and 6-8 a day for a toddler.
Cost and convenience
When weighing up the pros and cons of disposable vs reusable diapers, you might want to think about some of the following questions:
- What about financial costs? Cloth diapers are generally cheaper, but you might switch between types over the time your baby is in diapers, so it’s worth taking a look at the costs. You can do your own breakdown of the cost differences between reusable and disposable diapers – work out how many disposable diapers are in the packet and how many diapers you use every day. This will show you how much you’re spending on disposable diapers.
- Will you want to wash diapers rather than throw them away? For example, you might consider the time spent washing versus the smell of soiled diapers in your bin.
- What about when you’re out and about? Will you find reusables or disposable diapers more convenient? Does this matter to you?
- What type of diaper will perform the best? Is one type likely to result in less leakage or fewer daily changes? For example, reusable diapers will need to be changed more frequently than highly absorbent disposable diapers.
- What are the environmental costs? Are environmentally friendly options important to you?
Nappy hygiene
Put as much of the contents as you can down the toilet. If you’re using nappies with disposable liners the liner can be flushed away but it’s best to only flush liners that are soiled with poo. Don’t flush the nappy as it can block the toilet.
Disposable nappies can be rolled up and resealed, using the tabs. Put them in a plastic bag kept only for nappies, then tie it up and put it in an outside bin. Washable cloth nappies can be machine washed at 60°C (140 °F) or you could use a local nappy laundry service.
To avoid infection, wash your hands after changing a nappy and before doing anything else.
Safety tips
- If you are soaking nappies in a bucket, remember that even small amounts of water can be a drowning hazard for babies and young children.
- Never leave hot or boiling liquids unattended or within reach of children.
- Keep chemicals and chemical solutions out of reach of children.
Genital hygiene for babies
It’s important to keep your baby’s genitals clean. This will help prevent infections and keep your baby healthy.
To clean your baby’s genitals, you can use warm water and a cotton ball. You don’t need to use soap. If you do use soap, choose a mild one with a built-in moisturizer and use only a small amount. Always make sure to wash all the soap off your baby’s genitals.
You can clean your baby’s genitals when changing his/her nappy and at bath times.
Avoid using talcum powder anywhere on your baby, including around baby’s genitals. Talcum powder has fine particles that your baby can breathe in.
Cleaning your son’s penis
- If your baby boy is circumcised
If your son is circumcised, gently wash your baby’s penis and scrotum with warm water and a cotton ball. Lightly pat your baby’s penis and scrotum dry with a soft towel.
To prevent your baby’s penis from sticking to the nappy, it’s a good idea to moisten the front of the diaper with petroleum jelly, pawpaw cream or something similar.
- If your baby boy is uncircumcised
If your son is uncircumcised, you need to clean only the outside of the foreskin. You can clean inside the foreskin when it easily pulls back on its own. This usually happens when your boy is 2-3 years old, but sometimes it might not happen until puberty.
It’s normal for a milky white substance (called smegma) to gather under the foreskin. This is just made of dead skin cells and natural secretions.
Cleaning your daughter’s labia
Diaper creams, sweat and other substances can collect in and around the labia.
To clean your baby girl’s labia, wet a cotton ball, hold your baby’s legs apart and wipe between the labia with the cotton ball. Start at the front and gently wipe backwards. Lightly pat your baby’s genital area dry with a soft towel.
Don’t use vaginal deodorants or douches. They can upset the natural chemical balance of your baby’s vagina and increase the risk of infection.
You might notice a discharge that looks a bit like egg white. This is perfectly normal, and you don’t need to clean it away. If you’re unsure about any other discharge, see your doctor or child health nurse.
It’s common for newborn baby girls to have bloody vaginal discharge in the first few weeks. This is a normal response to mum’s hormones, so there’s no need to be alarmed. But if this discharge doesn’t go away, you should see your doctor or child and family health nurse.
Diaper rash prevention
The best way to deal with diaper rash is to try to prevent your baby getting it in the first place.
The simple steps below will help prevent diaper rash as well as help you to clear it up.
- Always keep your child’s diaper area clean and dry. Change your child’s diaper frequently and give his/her bottom air as often as you can.
- Protective barrier creams like Vaseline, Dermeze or zinc and castor oil or or zinc and cod liver oil can help keep your child’s skin in good condition. Note: these creams stain clothes and diapers. Many people use disposable diapers to avoid stains.
- If you are using cloth diapers, change them often and wash using soap powders which are labelled for sensitive skin. Drying them in a tumble dryer, if you have one, may make them softer than drying in the sun.
- Avoid using plastic pants whenever possible.
- Give your baby’s bottom more time without a diaper. When possible, let your baby go without a diaper. Exposing skin to air is a natural and gentle way to let it dry. To avoid messy accidents, try laying your baby on a large towel and engage in some playtime while he or she is bare-bottomed.
- Consider using ointment regularly. If your baby gets rashes often, apply a barrier ointment during each diaper change to prevent skin irritation. Petroleum jelly and zinc oxide are the time-proven ingredients in many diaper ointments.
- After changing diapers, wash your hands well. Hand-washing can prevent the spread of bacteria or yeast to other parts of your baby’s body, to you or to other children.
If your baby’s diaper is dirty, use the diaper to clean off most of the feces from your baby’s bottom. Then use the cotton wool and warm water (or baby lotion or sorbolene or baby wipes – alcohol free and made for baby’s sensitive skin) to remove the rest and get your baby really clean.
Girls should be cleaned from front to back to avoid getting germs into the vagina. Boys should be cleaned around the testicles (balls) and penis, but there’s no need to pull back the foreskin. It’s just as important to clean carefully when you’re changing a wet nappy.
- Powders are NOT necessary. Talc powder and other powders may be breathed in by a baby, and this may cause some health problems.
- The yeast that causes thrush feeds on cornstarch powder (corn flour), so this powder should NOT be used either.
If you’re using cloth diapers, put in a diaper liner then fasten the diaper around your baby. Adjust it to fit snugly round the waist and legs. If you’re using disposable nappies, take care not to get water or cream on the sticky tabs as they won’t stick if you do.
Diaper rash symptoms
The skin on your child’s bottom will look red and sore. Sometimes diaper rash might go up onto your child’s tummy or spread up towards your baby’s back. Some areas of skin might be raised or swollen, and there might be breaks in the skin. These breaks are called ulcers.
The skin folds aren’t usually affected because urine doesn’t get into them.
The diaper rash can cause discomfort and pain, which can make your baby irritable.
Diaper rash is characterized by the following:
- Skin signs. Diaper rash is marked by red, tender-looking skin in the diaper region — buttocks, thighs and genitals.
- Changes in your baby’s disposition. You may notice your baby seems more uncomfortable than usual, especially during diaper changes. A baby with a diaper rash often fusses or cries when the diaper area is washed or touched.
Diaper rash treatment
Simple measures are often the best. diaper rash will usually get better or go away within a few days of taking the following steps.
Change your baby’s diapers frequently
Frequent diaper changes keep the diaper area dry and give your child’s skin a chance to heal. Check your child every hour or so to see if his/her diaper is wet or soiled. Change wet or soiled diapers straight away.
Let your baby’s bottom ‘air’
Give your baby’s bottom some air for as long as possible every day. You can leave baby lying on an open nappy or a towel (naked from the waist down) even while she’s sleeping. You can also try fastening her diaper loosely, to allow air to circulate freely.
Clean your baby’s skin
Use lukewarm water and a mild soap to wash your baby’s skin. Rinse the skin thoroughly and gently pat him dry with a towel. Use running water to clean your baby where possible.
If you’re using disposable wipes, make sure they don’t contain alcohol or other irritants, which will sting and irritate the raw areas on your baby’s skin. Also, some babies might be allergic to the preservatives in disposable wipes.
Use an appropriate protective cream after each diaper change
Apply a simple cheap barrier cream – for example, zinc and castor oil, Vaseline or Dermeze – thickly with every change. You can get these creams from a supermarket or your chemist without a prescription.
Talcum-based powders aren’t recommended for diaper rash, because accidentally breathing in a puff of talcum powder can cause breathing difficulties in babies.
Rinse cloth diapers thoroughly after they’re washed
This gets rid of soap residue in your baby’s nappy. Bleach is most effective for killing bacteria, but make sure to rinse the nappies well in fresh water after using bleach-based detergents. Ensure the nappies are quite dry before using them again.
Avoid plastic overpants if you’re using cloth nappies.
Diaper rash cream
For severe diaper rash or nappy rash that won’t go away with simple measures, your doctor might recommend using cortisone creams or ointments (hydrocortisone 1%). Creams containing steroid medication should be used only after you’ve talked to your doctor. Always follow the instructions on the packet when putting these creams on your baby.
Your doctor might also prescribe particular creams or ointments if your baby has a secondary infection with bacteria or thrush.
Diaper rashes usually require several days to improve, and the rash may come back repeatedly. If the rash persists despite prescription treatment, your doctor may recommend that your baby see a specialist in skin conditions (dermatologist).
Home remedies for diaper rash
If your baby gets diaper rash, you can usually treat their skin yourself:
If the rash isn’t upsetting your baby, at each nappy change apply a thin layer of a barrier cream to protect their skin. Ask your health visitor or pharmacist to recommend one.
Follow this advice to help look after your baby’s skin.
- Change wet or dirty diapers as soon as possible.
- Clean the whole diaper area gently but thoroughly, wiping from front to back. Use water or fragrance-free and alcohol-free baby wipes.
- Bath your baby daily – but avoid bathing them more than twice a day as that may dry out their skin.
- Dry your baby gently after washing them – avoid vigorous rubbing.
- Lie your baby on a towel and leave their nappy off for as long and as often as you can to let fresh air get to their skin.
- DON’T use soap, bubble bath, or lotions.
- DON’T use talcum powder as it contains ingredients that could irritate your baby’s skin.
- Keeping diaper area clean and dry. The best way to keep your baby’s diaper area clean and dry is by changing diapers immediately after they are wet or soiled. Until the rash is better, this may mean getting up during the night to change the diaper.After you’ve gently cleaned and dried the skin, apply a cream, paste or ointment. Certain products, such as zinc oxide and petroleum jelly, work well to protect the skin from moisture. Don’t try to scrub off this protective layer completely at the next diaper change, as that could hurt the skin more. If you do want to remove it, try using mineral oil on a cotton ball.
- Increasing airflow. To aid the healing of diaper rash, do what you can to increase air exposure to the diaper region. These tips may help:
- Air out your baby’s skin by letting him or her go without a diaper and ointment for short periods of time, perhaps three times a day for 10 minutes each time, such as during naps.
- Avoid airtight plastic pants and diaper covers.
- Use diapers that are larger than usual until the rash goes away.
Diaper rash usually clears up after about three days if you follow these hygiene tips.
If the rash is causing your baby discomfort, your doctor may prescribe a diaper rash cream to treat it. You should apply the prescribed cream first and wait a few minutes before you apply the barrier cream.
- Applying ointment, paste, cream or lotion. Various diaper rash medications are available without a prescription. Talk to your doctor or pharmacist for specific recommendations. Some popular over-the-counter products include A + D, Balmex, Desitin, Triple Paste and Lotrimin (for yeast infections). Zinc oxide is the active ingredient in many diaper rash products. They are usually applied to the rash throughout the day to soothe and protect your baby’s skin. It doesn’t take much – a thin covering will do. The product can be applied over medicated creams, such as an antifungal or a steroid, when necessary. You could also apply petroleum jelly on top, which helps keep the diaper from sticking to the cream.Ointments, pastes or creams may be less irritating than lotions. But ointments and pastes create a barrier over the skin and don’t allow it to receive air. Creams dry on the skin and allow air through. Talk with your doctor about what type of product would be better for your child’s rash.As a general rule, stick with products designed for babies. Avoid items containing baking soda, boric acid, camphor, phenol, benzocaine, diphenhydramine, or salicylates. These ingredients can be toxic for babies.
Other rashes in the nappy area
If the rash doesn’t go away or your baby develops a persistent bright red, moist rash with white or red pimples that spreads into the folds of their skin, they may have an infection.
Ask your pharmacist or doctor for advice. The pharmacist may advise a cream to use.
If the rash is severe, take your baby to the doctor who may prescribe cream or medicine. Follow your doctor’s instructions on whether and when to apply barrier cream as well as the prescribed cream.
It’s normal for babies to develop skin rashes, but it’s important to know the difference between a minor irritation and a condition that requires attention.
Pain relief
Nappy rash is painful.
- Most babies with diaper rash will be more irritable than usual and may sleep poorly. They often need more attention, holding and comforting.
- Pain relief using paracetamol or acetaminophen can help. Make sure the dose is the right one for your baby (check the label on the bottle).
- Covering damaged skin using a barrier cream gently and often can be soothing. You could talk with your local pharmacist (chemist) to help choose one.
Diaper rash medications
More severe nappy rash may need short-term treatment with a mild steroid cream to settle the irritation. This medicine should be used on babies only when recommended by a doctor. Steroid creams and fungal treatments are often used together.
Medicines recommended or prescribed by doctors and dermatologists (skin doctors) for short-term treatment of nappy rash include combinations of:
- Hydrocortisone 1% ointment (e.g. DermAid cream/DermAid Soft Cream)+
- Methylprednisolone aceponate 0.1% ointment (e.g. Advantan Cream, Advantan Fatty Ointment)+ – for more severe nappy rash, not for very young babies
- Triamcinolone acetonide 0.02% ointment (e.g. Aristocort, Tricortone)+
- Nystatin cream (e.g. Mycostatin Topical)*
- Clotrimazole cream (e.g. Canesten Clotrimazole)*
- Clotrimazole plus hydrocortisone 1% cream (e.g. Hydrozole)*+
- Miconazole plus zinc oxide (e.g. Resolve Nappy Rash)*.
Note: + = corticosteroid; * = antifungal; *+= corticosteroid plus antifungal
Your doctor will explain when and how long to use each medicine.
If your baby has a bacterial skin infection, your doctor may prescribe an antibiotic cream such as mupirocin (e.g. Bactroban), or oral antibiotics (tablets).
Antifungal preparations
e.g. clotrimazole (Canesten range) econazole (Pevaryl range), miconazole (Daktarin, Resolve Balm), miconazole + zinc oxide (Daktozin, Resolve Nappy Rash Ointment)
- Antifungal creams should be used for one to two weeks after the rash has cleared to make sure the infection has been fully treated; check product information
- Antifungal creams can be used with barrier creams to protect the skin; apply the antifungal cream first, then the barrier cream
- Daktozin contains an antifungal agent and zinc oxide, which provides a barrier on the skin and helps soothe and heal nappy rash
Antifungal + hydrocortisone combinations
e.g. Canesten Plus Clotrimazole and Hydrocortisone Cream, Resolve Plus 0.5, Resolve Plus 1.0
- these products are useful if the skin is particularly inflamed and red, or if the baby also has eczema or seborrheic dermatitis; they should not be used in babies except on medical advice.
Alternative medicine
The following alternative treatments have worked for some people:
- Witch hazel (winter bloom), a flowering plant. A study showed that applying an ointment made with witch hazel to diaper rash helped. The study included 309 children.
- Human breast milk. Results are mixed on whether human breast milk applied to diaper rash is better than other treatments. One study showed that applying breast milk to diaper rash is an effective and safe treatment. Infants with diaper rash were treated with either 1 percent hydrocortisone ointment or breast milk. The study included 141 infants. Treatment with breast milk was as effective as the ointment alone.Another study compared human breast milk with a cream made from zinc oxide and cod liver oil. Newborns with diaper rash were treated with the cream or the breast milk. The study included 63 newborns. Treatment with the cream was more effective.
- Calendula and aloe vera. A study comparing aloe vera and calendula in the treatment of diaper rash in children found each to be an effective treatment of diaper rash.
- Shampoo clay (bentonite). A study showed that shampoo clay was effective in healing diaper rash and that it worked faster than calendula. The study included 60 infants.
- Other substances. Other natural remedies have been tried, including evening primrose and a mixture of honey, olive oil, and beeswax. Further study is needed to prove their effectiveness for treating diaper rash. Some of these substances may promote bacterial growth.