Contents
What is fibroadenoma
A fibroadenoma is a common benign (non-cancerous) solid breast lump made up of both glandular tissue and stromal (connective) tissue. Fibroadenomas have clear-cut borders and they tend to be round, smooth, firm or rubbery breast lump that move easily under the skin of the breast. The overlying skin is normal. Fibroadenomas can often feel like a marble within the breast, but they are not tender. Fibroadenomas are not fixed to the surrounding breast tissue and you can move them under the skin. When examined, they slip around under the palpating hand, hence the colloquial term a breast “mouse.” A fibroadenoma results from the excess proliferation of connective tissue and is not cancerous 1. A woman can have one or many fibroadenomas.
Fibroadenoma usually occurs in women between the ages of 10 and 40 years. It is the most common breast mass in the adolescent and young women in their 20s and 30s, but they can be found in women of any age 2. Fibroadenomas peak incidence is between 25 and 40 years. Incidence decreases after 40 years 3 and they tend to shrink after a woman goes through menopause..
The typical presentation is in a woman of reproductive age with a mobile palpable breast lump. Due to their hormonal sensitivity, the fibroadenoma commonly enlarges during pregnancy and involute at menopause. Hence, they rarely present after the age of 40 years.
Some fibroadenomas are too small to be felt, but some are several inches across or are only found on an imaging test (like a mammogram or ultrasound). A biopsy (taking out breast tissue to check it in the lab) is needed to know if a tumor is a fibroadenoma or some other problem.
Most fibroadenomas look the same all over when seen under a microscope and are called simple fibroadenomas. But some fibroadenomas have other changes, too, and are called complex fibroadenomas. Complex fibroadenomas tend to be bigger and tend to occur in older patients.
Women with simple fibroadenomas have a slightly increased risk of breast cancer – about 1½ times the risk of women with no breast changes. Complex fibroadenomas seem to increase the risk slightly more than simple fibroadenomas.
Treatment for fibroadenoma of breast might include monitoring to detect changes in size or feel, a biopsy to evaluate the lump or surgery to remove it.
Types of fibroadenomas
In addition to simple fibroadenomas, there are:
- Complex fibroadenomas. These can contain changes, such as an overgrowth of cells (hyperplasia) that can grow rapidly. A pathologist makes the diagnosis of a complex fibroadenoma after reviewing the tissue from a biopsy.
- Juvenile fibroadenomas. This is the most common type of breast lump found in girls and adolescents between the ages of 10 and 18. These fibroadenomas can grow large, but most shrink over time, and some disappear.
- Giant fibroadenomas. These can grow to larger than 2 inches (5 centimeters). They might need to be removed because they can press on or replace other breast tissue.
- Phyllodes tumor. Most phyllodes tumors are benign (not cancer), but about 1 out of 4 of these tumors are malignant (cancer). Doctors usually recommend that these be removed. Phyllodes tumors are most common in women in their 40s, but women of any age can have them. Women with Li-Fraumeni syndrome (a rare, inherited genetic condition) have an increased risk for phyllodes tumors.
In healthy women, normal breast tissue often feels lumpy.
Make an appointment with your doctor if:
- You detect a new breast lump
- You notice other changes in your breasts
- A breast lump you’ve had checked before has grown or otherwise changed and appears to be separate from the surrounding breast tissue
- You’re worried about the breast lump
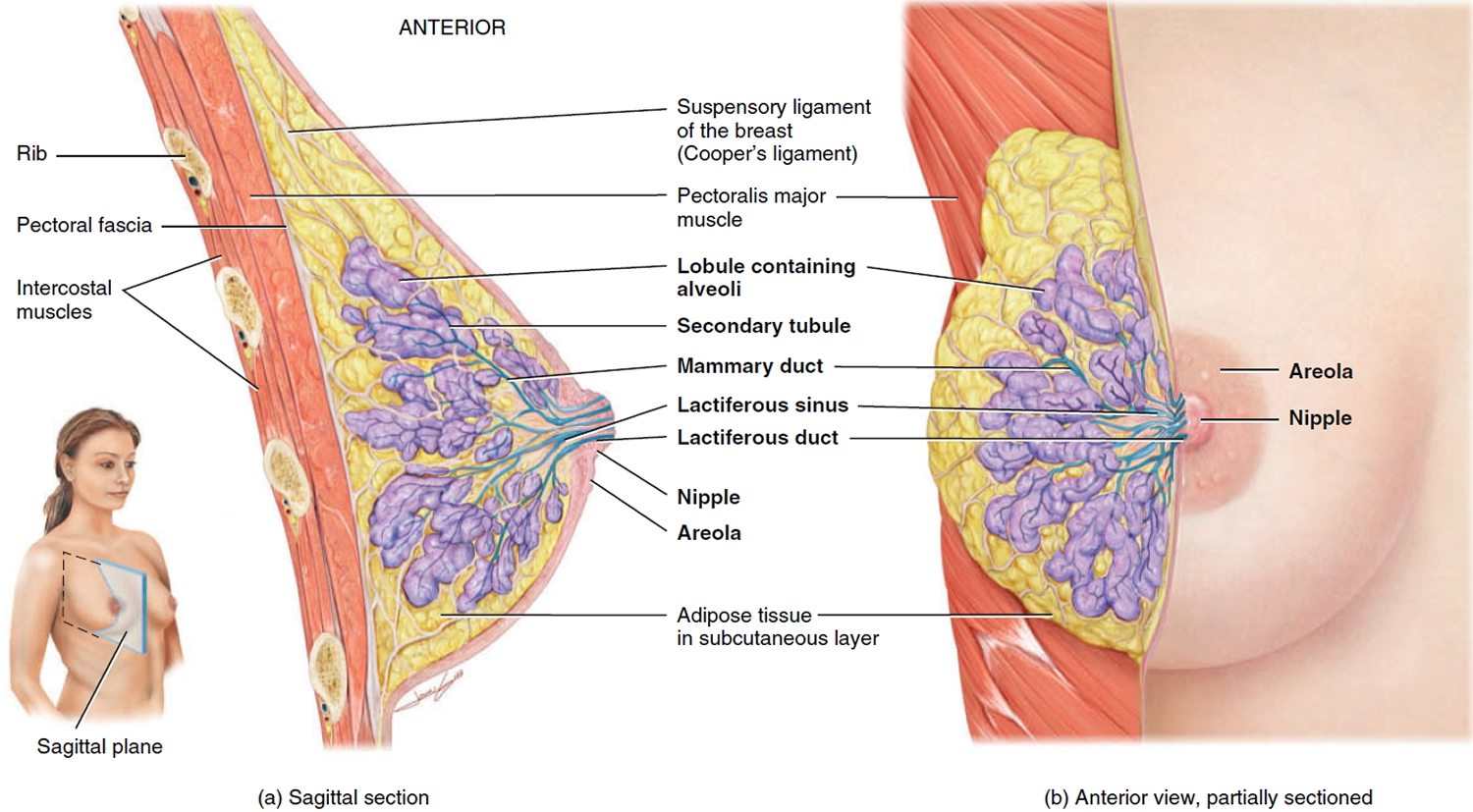
Figure 1. Normal breast (female)
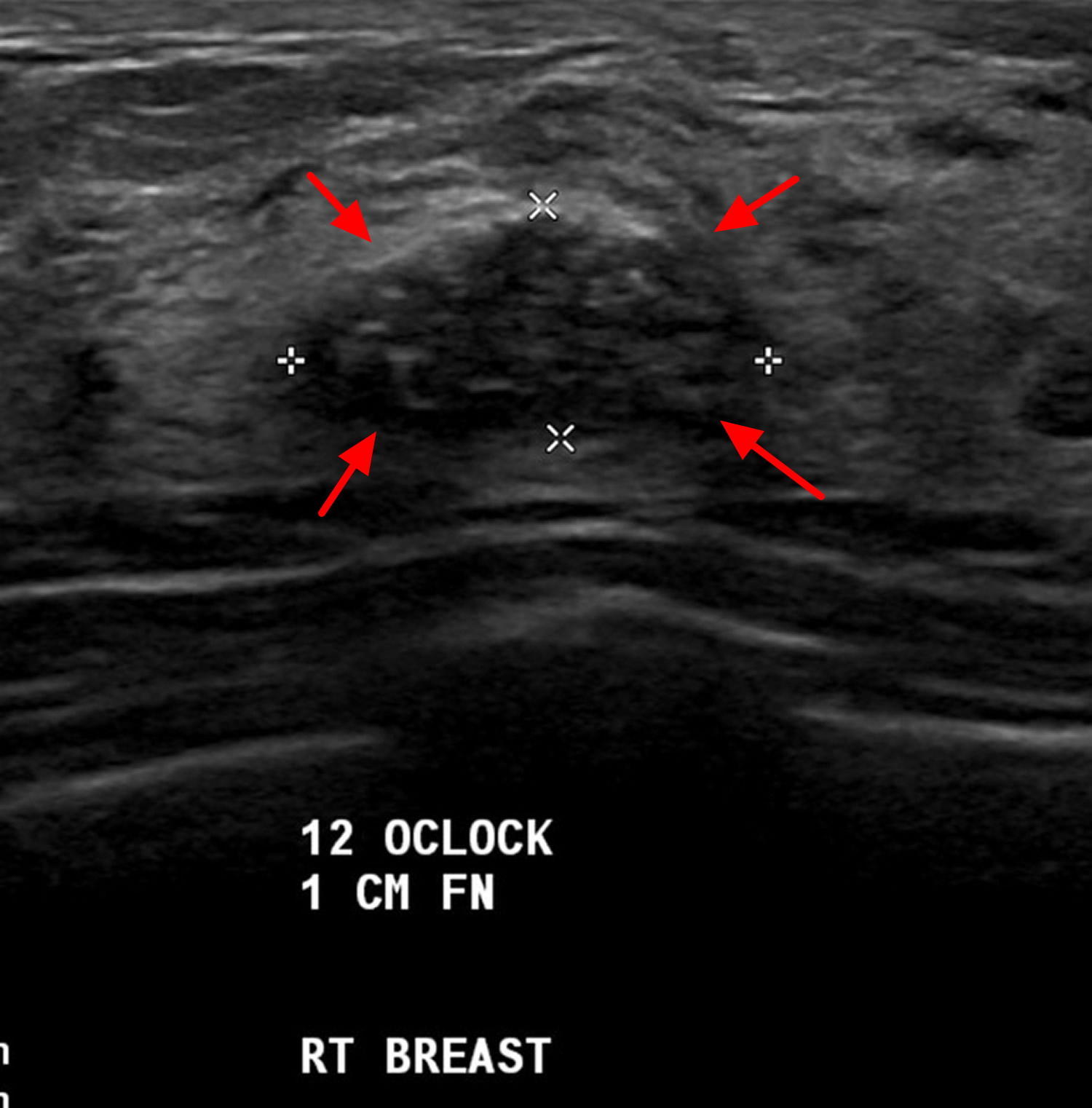
Figure 2. Fibroadenoma ultrasound (circumscribed ovoid solid nodule that is hypoechogenic and has some small echogenic foci)
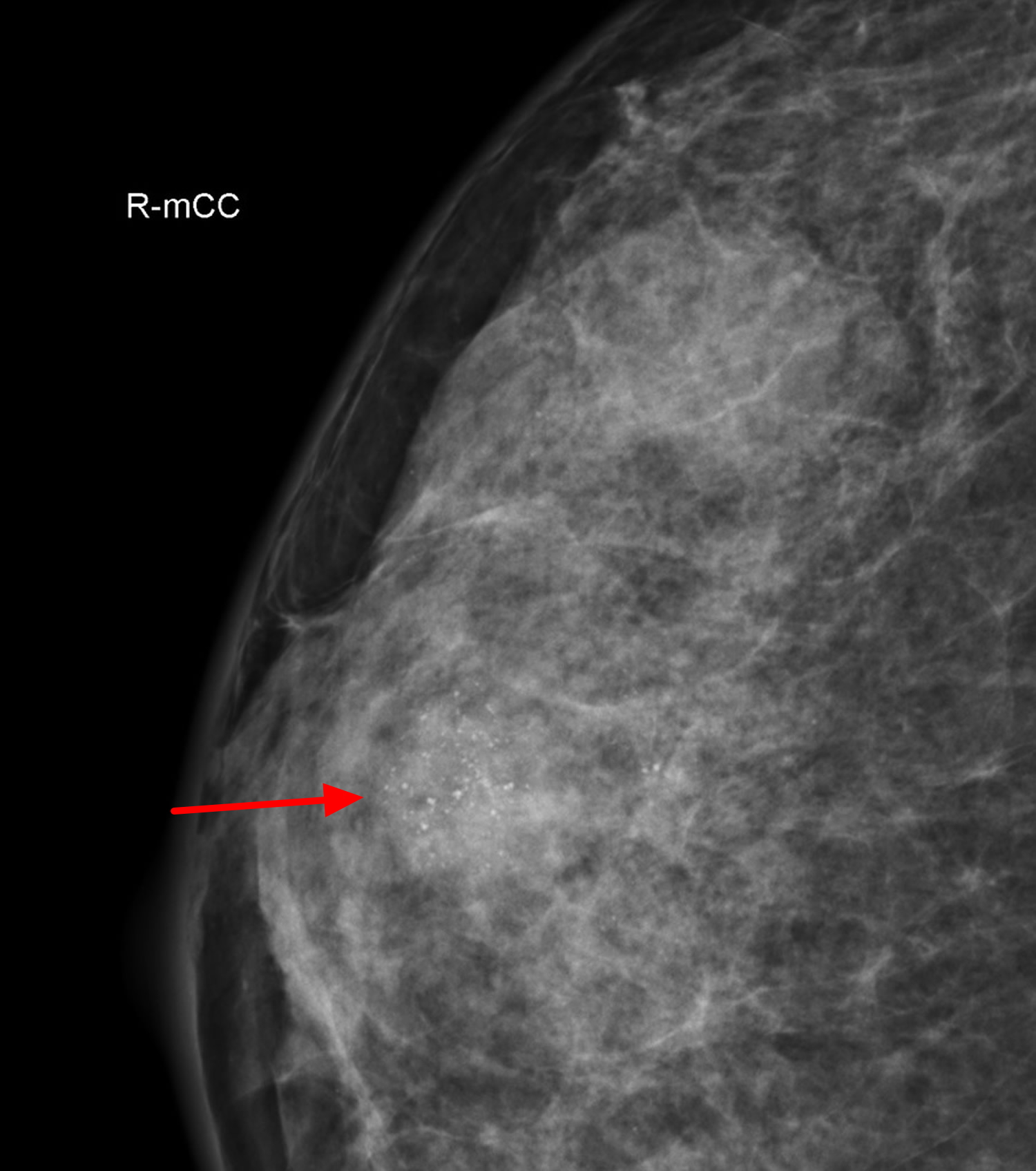
Figure 3. Fibroadenoma mammogram (craniocaudal = top to bottom view of the same fibroadenoma shown in ultrasound scan Figure 1)
Fibroadenoma causes
The cause of fibroadenomas is unknown, but they might be related to reproductive hormones. Fibroadenomas occur more often during your reproductive years, can become bigger during pregnancy or with use of hormone therapy, and might shrink after menopause, when hormone levels decrease.
Fibroadenoma symptoms
Fibroadenomas are solid breast lumps that usually are:
- Round with distinct, smooth borders
- Easily moved
- Firm or rubbery
- Painless
You can have one or many fibroadenomas in one or both breasts.
Fibroadenoma diagnosis
During a clinical breast exam, your doctor will check both breasts for lumps and other problems. Some fibroadenomas are too small to feel, so they can only be discovered in imaging tests.
If you have a lump that can be felt (palpable), your doctor might recommend certain tests or procedures, depending on your age and the characteristics of the lump.
Tests to evaluate the breast lump
- Diagnostic mammography. Mammography uses X-rays to produce an image (mammogram) of suspicious areas in your breast tissue. A fibroadenoma might appear on a mammogram as a breast mass with smooth, round edges, distinct from surrounding breast tissue.
- Breast ultrasound. This technology uses sound waves to produce pictures of the inside of the breast. Your doctor might recommend a breast ultrasound in addition to a mammogram to evaluate a breast lump if you have dense breast tissue. For women younger than 30 who have a breast lump, the doctor likely will order a breast ultrasound first to evaluate the lump. If a mammogram indicates that you have a breast lump or other abnormality, a breast ultrasound might be used to further assess the lump. A breast ultrasound can help your doctor determine whether a breast lump is solid or filled with fluid. A solid mass is more likely a fibroadenoma; a fluid-filled mass is more likely a cyst.
Procedures to evaluate the breast lump
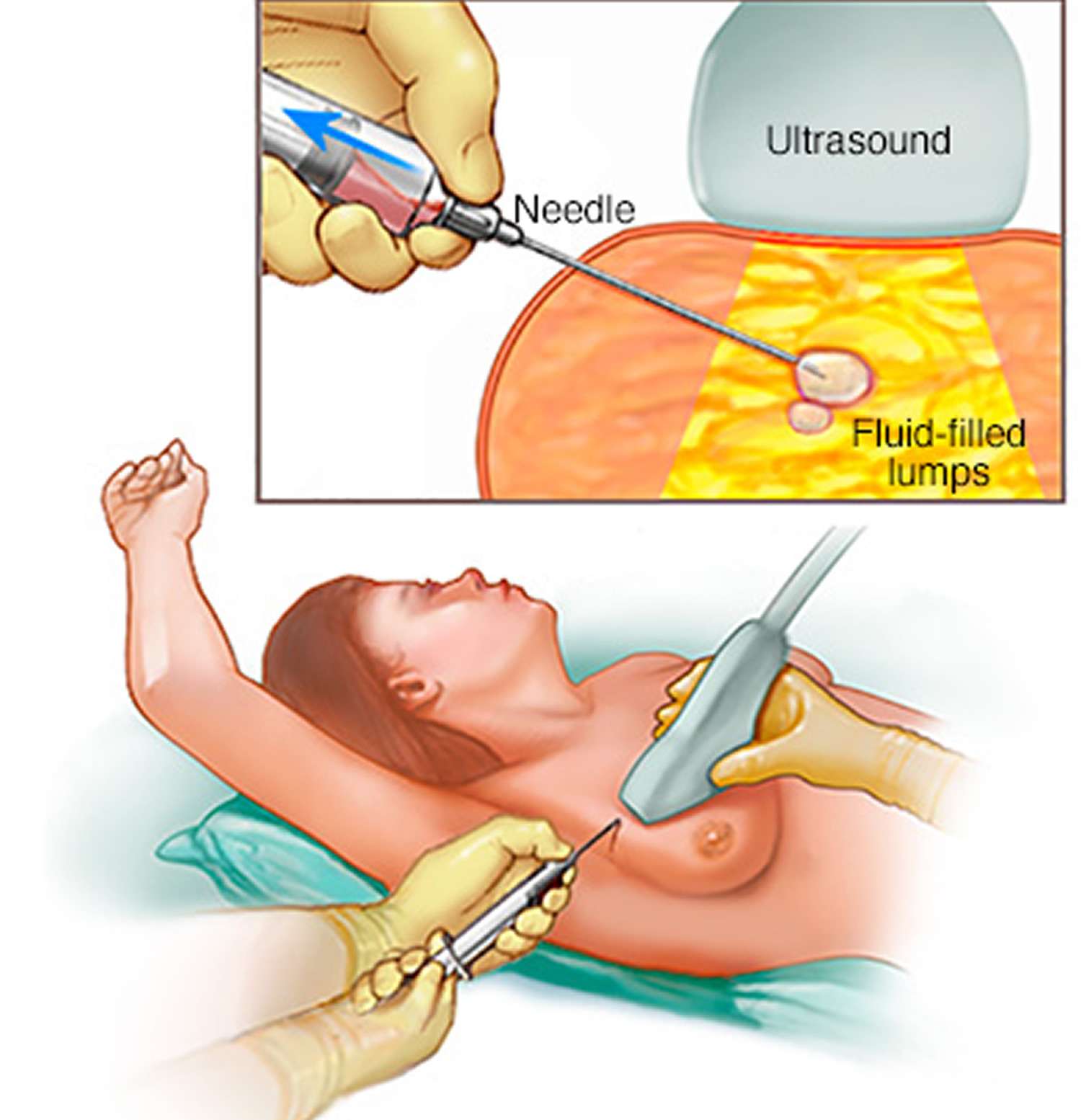
- Fine-needle aspiration. Through a thin needle inserted into your breast, your doctor attempts to withdraw the contents of the breast lump. If fluid comes out, the lump is likely a cyst.
- Core needle biopsy. A radiologist with guidance from an ultrasound usually performs this procedure. The doctor uses a needle to collect tissue samples from the lump, which go to a lab for analysis.
Figure 4. Fine-needle aspiration
Fibroadenoma treatment
Many doctors recommend removing fibroadenomas, especially if they keep growing or change the shape of the breast, to make sure that cancer is not causing the changes.
Sometimes these fibroadenoma tumors stop growing or even shrink on their own, without any treatment. In this case, as long as the doctors are sure the masses are fibroadenomas and not breast cancer, they may be left in place and watched to be sure they don’t grow. This approach is useful for women with many fibroadenomas that are not growing. In such cases, removing them might mean removing a lot of nearby normal breast tissue, causing scarring that would change the shape and texture of the breast. This could also make future mammograms harder to read.
- It’s important for women who have fibroadenomas to have regular breast exams or imaging tests to make sure the fibroadenomas are not growing.
Sometimes one or more new fibroadenomas can grow after one is removed. This means that another fibroadenoma has formed – it does not mean that the old one has come back.
Fibroadenoma surgery
Your doctor might recommend surgery to remove the fibroadenoma if one of your tests — the clinical breast exam, an imaging test or a biopsy — is abnormal or if the fibroadenoma is extremely large, gets bigger or causes symptoms.
Procedures to remove a fibroadenoma include:
- Lumpectomy or excisional biopsy. In this procedure, a surgeon removes breast tissue and sends it to a lab to check for cancer.
- Cryoablation. Your doctor inserts a thin, wand-like device (cryoprobe) through your skin to the fibroadenoma. A gas is used to freeze and destroy the tissue.
After a fibroadenoma is removed, it’s possible for one or more new fibroadenomas to develop. New breast lumps need to be assessed with a mammogram, ultrasound and possibly biopsy — to determine if the lump is a fibroadenoma or might become cancerous.
- Weissleder R, Wittenberg J, Harisinghani MMGH et-al. Primer of Diagnostic Imaging. Mosby. (2011) ISBN:0323065384.[↩]
- Chung EM, Cube R, Hall GJ et-al. From the archives of the AFIP: breast masses in children and adolescents: radiologic-pathologic correlation. Radiographics. 29 (3): 907-31. doi:10.1148/rg.293095010 https://pubs.rsna.org/doi/10.1148/rg.293095010[↩]
- Pope TL. Aunt Minnie’s Atlas and Imaging-Specific Diagnosis. Lippincott Williams & Wilkins. (2003) ISBN:0781741602.[↩]