Contents
What is gangrene
Gangrene is a serious condition that refers to the decay and death of tissue resulting from an interruption in blood flow to a certain area of your body. Gangrene can affect any part of the body but typically starts in the toes, feet, fingers and hands.
Gangrene can occur as a result of an injury, infection or a long-term condition that affects blood circulation.
Symptoms of gangrene include:
- redness and swelling in the affected area
- either a loss of sensation or severe pain in the affected area
- sores or blisters in the affected area that bleed or produce a foul-smelling pus
You should see your doctor immediately if you’re worried you may have gangrene.
- The earlier treatment for gangrene begins, the more successful it’s likely to be. The main treatments include surgery to remove damaged tissue, known as debridement, and antibiotics to treat any underlying infection.
In some cases, surgery may be needed to restore blood flow to the affected area.
In more severe cases, it may be necessary to remove an entire body part such as a toe, foot, or lower leg. This is known as amputation.
If bacteria from gangrene pass into your bloodstream, you could go into septic shock. This is a life-threatening condition that occurs when an infection causes your blood pressure to drop to a dangerously low level.
Signs of septic shock include:
- a rapid but weak pulse
- dizziness when you stand up
- a change in your mental state, such as confusion or disorientation
- breathing difficulties
- vomiting
- diarrhea
- cold, clammy and pale skin
Dial your local emergency service number immediately to request an ambulance if you suspect that you or someone you know is in septic shock.
How do you get gangrene
Anyone can develop gangrene, particularly after a serious injury, but there are certain groups of people who are more at risk.
These include people with long-term conditions that can affect the blood vessels, such as:
- diabetes – a lifelong condition that causes a person’s blood sugar level to become too high
- atherosclerosis – where the arteries become clogged up with a fatty substance called plaque, narrowing them and restricting blood flow
- peripheral arterial disease – where a build-up of fatty deposits in the arteries restricts blood supply to leg muscles
- Raynaud’s phenomenon – where blood vessels in certain parts of the body, usually the fingers or toes, react abnormally to cold temperatures.
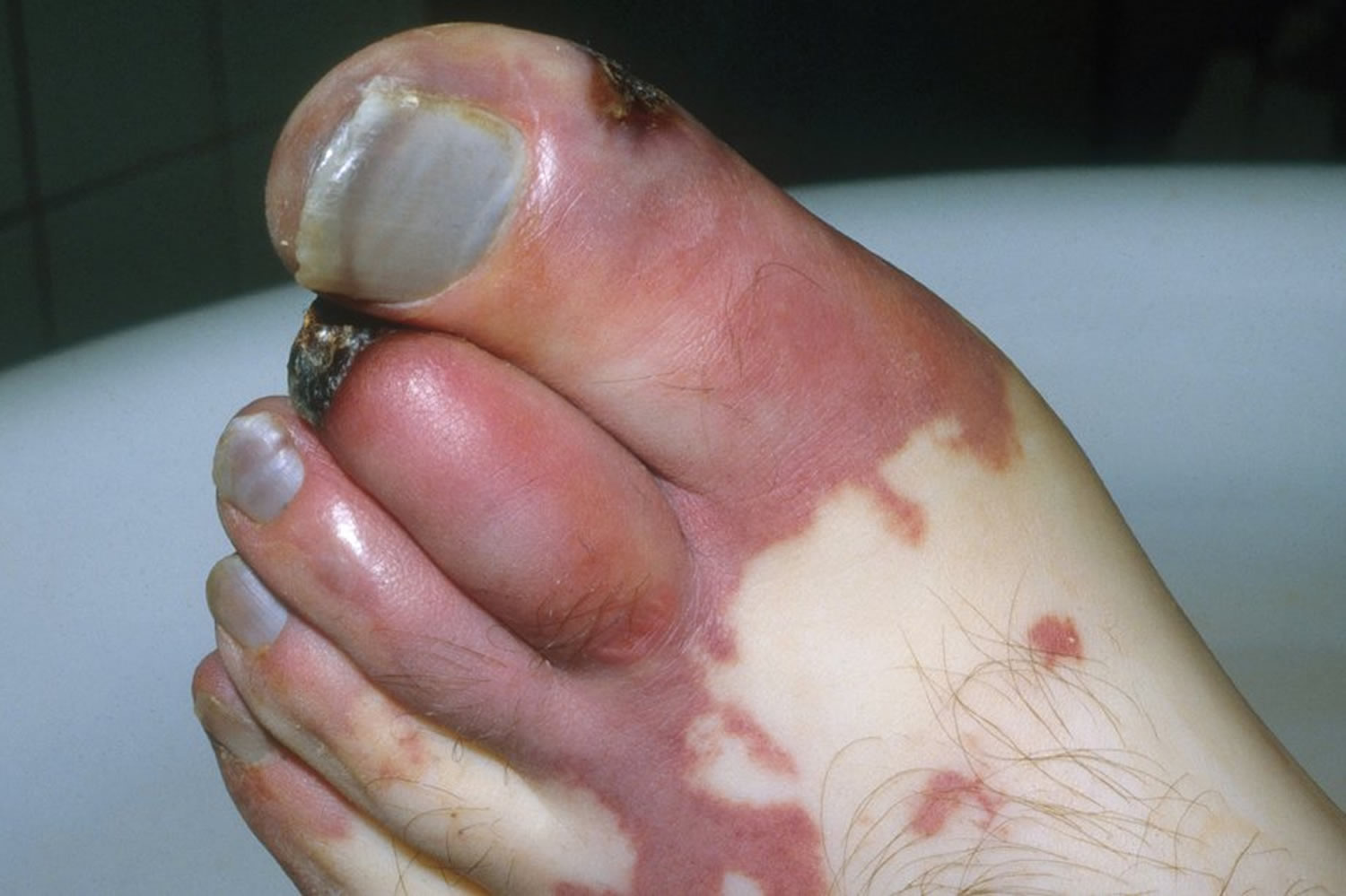
Figure 1. Gangrene toe (dry gangrene)
Types of gangrene
There are several different types of gangrene, each with a different cause. The main types are:
- Dry gangrene – where the blood flow to an area of the body becomes blocked
- Wet gangrene – caused by a combination of an injury and bacterial infection
- Gas gangrene – where an infection develops deep inside the body and the bacteria responsible begin releasing gas
- Necrotizing fasciitis – caused by a serious bacterial infection that spreads quickly through the deeper layers of skin and tissue
- Internal gangrene – where the blood flow to an internal organ, usually the intestines, gallbladder or appendix, becomes blocked
- Fournier’s gangrene: Fournier’s gangrene involves the genital organs. Men are more often affected, but women can develop this type of gangrene as well. Fournier’s gangrene usually arises due to an infection in the genital area or urinary tract and causes genital pain, tenderness, redness and swelling.
- Progressive bacterial synergistic gangrene (Meleney’s gangrene). This rare type of gangrene typically occurs after an operation, with painful skin lesions developing one to two weeks after surgery.
Generally, people who have dry gangrene have the best chance of a full recovery because dry gangrene doesn’t involve a bacterial infection and spreads more slowly than do the other types of gangrene. However, when gangrene caused by an infection is recognized and treated quickly, the odds of recovery are good.
Necrotizing fasciitis
Necrotizing fasciitis is a rare but serious bacterial infection that affects the tissue beneath the skin, and surrounding muscles and organs (fascia). Necrotizing fasciitis is a medical emergency that requires immediate treatment.
It’s sometimes called the “flesh-eating disease”, although the bacteria that cause it don’t “eat” flesh – they release toxins that damage nearby tissue.
Necrotizing fasciitis can start from a relatively minor injury, such as a small cut, but gets worse very quickly and can be life threatening if it’s not recognised and treated early on.
Causes of necrotizing fasciitis
Necrotizing fasciitis can be caused by several different types of bacteria.
The bacteria that cause the infection live in the gut, in the throat, or on the skin of some people, where they don’t usually cause any serious problems.
But in rare cases, they can cause necrotizing fasciitis if they get into deep tissue – either through the bloodstream, or an injury or wound, such as:
- cuts and scratches
- insect bites
- puncture wounds caused by injecting drugs
- surgical wounds
Necrotizing fasciitis typically occurs when bacteria already on the skin or in the body get into deep tissue. The infection can also be spread from person to person, but this is very rare.
Anyone can get necrotizing fasciitis – including young and otherwise healthy people – but it tends to affect older people and those in poor general health.
Preventing necrotizing fasciitis
There’s no vaccine for necrotizing fasciitis and it’s not always possible to prevent it.
The following measures may help to reduce your risk:
- treat wounds quickly – after stopping any bleeding, clean wounds with running water and pat them dry with a clean towel
- keep wounds clean and dry – after a wound has been cleaned, cover it with a sterile dressing (such as a plaster); change the dressing if it gets wet or dirty
- wash your hands regularly with soap and warm water – alcohol-based hand gels can also help, but washing with soap and water is generally best
If you’re in close contact with someone who has necrotizing fasciitis, you may be given a course of antibiotics to reduce your risk of infection.
Symptoms of necrotizing fasciitis
The symptoms of necrotising fasciitis develop quickly over hours or days. They may not be obvious at first and can be similar to less serious conditions such as flu, gastroenteritis or cellulitis.
Early symptoms can include:
- a small but painful cut or scratch on the skin
- intense pain that’s out of proportion to any damage to the skin
- a high temperature (fever) and other flu-like symptoms
After a few hours to days, you may develop:
- swelling and redness in the painful area – the swelling will usually feel firm to the touch
- diarrhea and vomiting
- dark blotches on the skin that turn into fluid-filled blisters
If left untreated, the infection can spread through the body quickly and cause symptoms such as dizziness, weakness and confusion.
Treatments for necrotizing fasciitis
Necrotizing fasciitis needs to be treated in hospital.
The main treatments are:
- surgery to remove infected tissue – this may be repeated several times to ensure all the infected tissue is removed, and occasionally it may be necessary to amputate affected limbs
- antibiotics – usually several different types are given directly into a vein
- supportive treatment – including treatment to control your blood pressure, fluid levels and organ functions
People with the condition will often need to be looked after in an intensive care unit and may need to stay in hospital for several weeks.
While in hospital, they may be isolated from other patients to reduce the risk of spreading the infection.
Outlook for necrotizing fasciitis
Necrotizing fasciitis can progress very quickly and lead to serious problems such as blood poisoning (sepsis) and organ failure.
Even with treatment, it’s estimated that 1 or 2 in every 5 cases are fatal.
People who survive the infection are sometimes left with long-term disability as a result of amputation or the removal of a lot of infected tissue.
They may need further surgery to improve the appearance of the affected area and may need ongoing rehabilitation support to help them adapt to their disability.
Fournier’s gangrene
Fournier’s gangrene is a type of necrotizing fasciitis or gangrene affecting the external genitalia and/or perineum. It commonly occurs in older men, but it can also occur in women and children. It is more likely to occur in diabetics, alcoholics, or those who are immune compromised. A 2009 epidemiological study found the incidence of Fournier’s gangrene to be 1.6 cases per 100,000 males, in the United States 1. Males 50 to 79 years old had the highest rate at 3.3 per 100,000. Out of 1,680 cases identified in the study 39 were women 1.
About 1 per 62,500 males are affected a year. Males are affected about 40 times more often than females. It was first described by Baurienne in 1764 and is named after a French venereologist, Jean Alfred Fournier, following five cases he presented in clinical lectures in 1883.
Initial symptoms of Fournier’s gangrene include swelling or sudden pain in the scrotum, fever, pallor and generalized weakness 2. More marked cases are characterized by a foul odor and purulent discharge from the infected tissue. Crepitus has been reported. It begins as a subcutaneous infection. However, soon necrotic patches appear in the overlying skin which later develop into necrosis 2.
Most cases of Fournier’s gangrene are infected by both aerobic and anaerobic bacteria 3. Resulting mortality increases in individuals lacking access not only to pragmatic resources such as sanitation and medical care, but to psychosocial resources as well.
A 2006 Turkish study reported 46% of those diagnosed with Fourniers had elevated blood sugars 4. There have been additional findings that seemingly link Fourniers with immunosuppression and alcoholism. One study reported approximately one third of those diagnosed with Fournier had alcoholism with resulting diabetes and malnutrition, while another 10% had been medical immunosuppressed either via chemotherapy, steroids, or malignancy 5.
Fournier’s gangrene is usually diagnosed clinically, but laboratory tests and imaging studies are used to confirm diagnosis, determine severity and predict outcomes. X-rays and ultrasounds may show the presence of gas below the surface of the skin. A CT scan can be useful in determining the site of origin and extent of spread.
Fournier’s gangrene prognosis
While recent case series (n=9-80) studies have found a mortality rate of 20-40%, a large (n=1641) 2009 study reported a mortality rate of 7.5% 1.
Fournier’s gangrene treatment
Fournier’s gangrene is a urological emergency requiring intravenous antibiotics and debridement (surgical removal) of necrotic (dead) tissue. In addition to surgery and antibiotics, hyperbaric oxygen therapy may be useful and acts to inhibit the growth of and kill the anaerobic bacteria 6.
Dry gangrene
Dry gangrene is characterized by dry and shriveled skin ranging in color from brown to purplish blue or black. Dry gangrene may develop slowly. It occurs most commonly in people who have arterial blood vessel disease, such as atherosclerosis, or in people who have diabetes.
Wet gangrene
Gangrene is referred to as “wet” if there’s a bacterial infection in the affected tissue. Swelling, blistering and a wet appearance are common features of wet gangrene.
It may develop after a severe burn, frostbite or injury. It often occurs in people with diabetes who unknowingly injure a toe or foot. Wet gangrene needs to be treated immediately because it spreads quickly and can be fatal.
Gas gangrene
Gas gangrene typically affects deep muscle tissue. If you have gas gangrene, the surface of your skin may initially appear normal.
As the condition progresses, your skin may become pale and then evolve to a gray or purplish red color. A bubbly appearance to your skin may become apparent, and the affected skin may make a crackling sound when you press on it because of the gas within the tissue.
Gas gangrene is most commonly caused by infection with the bacterium Clostridium perfringens, which develops in an injury or surgical wound that’s depleted of blood supply. The bacterial infection produces toxins that release gas — hence the name “gas” gangrene — and cause tissue death. Like wet gangrene, gas gangrene can be life-threatening.
Internal gangrene
Gangrene that affects one or more of your organs, such as your intestines, gallbladder or appendix, is called internal gangrene. This type of gangrene occurs when blood flow to an internal organ is blocked — for example, when your intestines bulge through a weakened area of muscle in your abdomen (hernia) and become twisted.
Internal gangrene may cause fever and severe pain. Left untreated, internal gangrene can be fatal.
Gangrene complications
Gangrene can lead to scarring or the need for reconstructive surgery. Sometimes, the amount of tissue death is so extensive that a body part, such as your foot, may need to be removed (amputated).
Gangrene that is infected with bacteria can spread quickly to other organs and may be fatal if left untreated.
What causes gangrene
Gangrene can develop when the supply of blood to one or more areas of your body is interrupted.
This can occur as the result of an injury, an infection, or an underlying condition that affects your circulation.
People most at risk of gangrene are those with an underlying health condition that can affect the blood vessels and arteries (particularly if it’s poorly managed), and those with a weakened immune system.
Conditions affecting the blood vessels
Conditions that can affect the blood vessels and increase your risk of developing gangrene include:
- diabetes – a lifelong condition that causes a person’s blood sugar level to become too high, which can damage nerves and blood vessels (see below)
- atherosclerosis – where arteries narrow and become clogged with a fatty substance known as plaque
- peripheral arterial disease – where a build-up of fatty deposits in the arteries restricts blood supply to leg muscles
- Raynaud’s phenomenon – where blood vessels in certain parts of the body, usually the fingers or toes, react abnormally to cold temperatures
As blood vessels are naturally narrow, any damage or extra narrowing has the potential to block blood flow to a part of the body and cause gangrene.
Diabetes
People with diabetes have an increased risk of developing gangrene. This is because the high blood sugar levels associated with the condition can damage your nerves, particularly those in your feet, which can make it easy to injure yourself without realising.
High blood sugar can also damage your blood vessels, restricting the blood supply to your feet. Less blood means your feet will also receive fewer infection-fighting cells, so wounds will take longer to heal and are more likely to become infected. It’s therefore important that you take extra care of your feet if you have diabetes.
Injuries and surgery
You’re also at an increased risk of developing gangrene if you experience a traumatic injury or serious damage to your skin and tissues, such as:
- a serious injury – for example, during a car accident
- a burn
- frostbite
These injuries can cause a sudden loss of blood to an area of your body, and any open wounds can become infected with bacteria.
Gangrene can also occur as a result of an infection that develops during surgery. However, with advances in surgical techniques and infection control, the chances of gangrene developing during surgery are small nowadays.
Weak immune system
If your immune system is seriously weakened, minor infections can become more serious and can lead to gangrene. A weak immune system can be caused by:
- chemotherapy or radiotherapy
- HIV
- diabetes
- long-term alcohol misuse
- injecting drugs, such as heroin
- malnutrition
- being over 60 years of age (the older you are, the less efficient your immune system is)
- obesity
- kidney failure
However, for reasons that are unclear, gangrene can sometimes occur in young and otherwise healthy people.
Risk factors for developing gangrene
Several factors increase your risk of developing gangrene. These include:
- Diabetes. If you have diabetes, your body doesn’t produce enough of the hormone insulin (which helps your cells take up blood sugar) or is resistant to the effects of insulin. High blood sugar levels can eventually damage blood vessels, decreasing or interrupting blood flow to a part of your body.
- Blood vessel disease. Hardened and narrowed arteries (atherosclerosis) and blood clots also can block blood flow to an area of your body.
- Severe injury or surgery. Any process that causes trauma to your skin and underlying tissue, including an injury or frostbite, increases your risk of developing gangrene, especially if you have an underlying condition that affects blood flow to the injured area.
- Smoking. People who smoke have a higher risk of gangrene.
- Obesity. Obesity often accompanies diabetes and vascular disease, but the stress of extra weight alone can also compress arteries, leading to reduced blood flow and increasing your risk of infection and poor wound healing.
- Immunosuppression. If you have an infection with the human immunodeficiency virus (HIV) or if you’re undergoing chemotherapy or radiation therapy, your body’s ability to fight off an infection is impaired.
- Medications or drugs that are injected. In rare instances, certain medications and illegal drugs that are injected have been shown to cause infection with bacteria that cause gangrene.
Gangrene prevention
There are a number of things you can do to help lower your risk of developing gangrene.
Many cases of gangrene can be prevented.
If you have a condition that increases your risk of getting gangrene, such as diabetes, it’s important you have regular check-ups to assess the state of your feet. Report any problems to your doctor as soon as possible.
Stopping smoking if you smoke and adopting a healthy lifestyle, with a low-fat diet and regular exercise, can also improve your circulation and reduce your risk of developing gangrene.
Foot care
If you have diabetes or another long-term condition that can cause atherosclerosis (hardening or thickening of the arteries), it’s important you take extra care of your feet.
If you have diabetes, you should have your feet checked at least once a year. However, you may need more frequent check-ups if you have additional risk factors, such as peripheral neuropathy (numbness in the hands and feet), or a history of foot ulcers.
The advice listed below can help prevent a diabetic foot ulcer developing:
- Check your feet daily for problems such as numbness, discoloration, breaks in the skin, pain or swelling. Report problems to your doctor immediately.
- Avoid walking barefoot outside and wearing shoes without socks.
- Don’t use chemical preparations for corns and calluses or ingrown toenails. Instead, contact a podiatrist (a healthcare professional who specializes in foot care).
- Wash your feet daily with warm water. Afterwards, make sure you dry your feet thoroughly, particularly between the toes.
- Keep your feet clean and free from infection.
- Wear shoes that fit properly and don’t squeeze or rub. Ill-fitting shoes can cause corns and callouses, ulcers and nail problems.
- Cut or file your toenails regularly.
- Get corns or hard skin treated by a podiatrist.
If you have a history of foot ulcers, wearing specially designed therapeutic or orthopedic shoes can help prevent further ulcers developing. Your podiatrist may be able to provide you with specially made-to-measure footwear, or they may be able to recommend a stockist.
Quit Smoking
Smoking can cause your arteries to become blocked, resulting in a loss of blood supply to your arms or legs. This is known as peripheral arterial disease (PAD).
If you decide to stop smoking, your doctor will be able to refer you to a stop smoking service, your doctor should be able to prescribe medical treatment to help with any withdrawal symptoms you may experience.
Stop smoking treatments
If you want to stop smoking, several different treatments are available from shops, pharmacies and on prescription to help you beat your addiction and reduce withdrawal symptoms.
The main options are:
- Nicotine replacement therapy e.g. skin patches, chewing gum, inhalators (which look like plastic cigarettes), tablets, oral strips and lozenges, nasal and mouth spray
- Varenicline. Varenicline reduces cravings for nicotine like nicotine replacement therapy, but it also blocks the rewarding and reinforcing effects of smoking. It’s taken as one to two tablets a day. You should start taking it a week or two before you try to quit. A course of treatment usually lasts around 12 weeks, but it can be continued for longer if necessary. Evidence suggests it’s the most effective medication for helping people stop smoking. Varenicline is only available on prescription, so you’ll usually need to see your doctor to get it.
- Bupropion. Bupropion is a medication originally used to treat depression, but it has since been found to help people quit smoking. It’s taken as one to two tablets a day. You should start taking it a week or two before you try to quit. Bupropion is only available on prescription, so you’ll usually need to see your doctor to get it.
- E-cigarettes
The best treatment for you will depend on your personal preference, your age, whether you’re pregnant or breastfeeding and any medical conditions you have. Speak to your doctor for stop smoking advice.
Healthy Diet
Eating an unhealthy diet high in fat will make any existing atherosclerosis worse and increase your risk of developing gangrene.
Continuing to eat high-fat foods will cause more fatty plaques to build-up in your arteries. This is because fatty foods contain cholesterol.
There are two types of fat – saturated and unsaturated. Avoid foods that contain saturated fats because they increase levels of “bad cholesterol” in your blood.
Foods high in saturated fat include:
- meat pies
- sausages and fatty cuts of meat
- butter
- ghee (a type of butter often used in Indian cooking)
- lard
- cream
- hard cheese
- cakes and biscuits
- food containing coconut or palm oil
Alcohol
Drinking excessive amounts of alcohol will cause your blood pressure to rise, and also raise the level of cholesterol in your blood.
Recommended daily limits of alcohol consumption are:
- 3-4 units for men
- 2-3 units for women
A unit of alcohol is equal to about half a pint of normal strength lager, half a standard glass of wine, or a pub measure (25ml) of spirits.
Exercise
A healthy, well-balanced diet and regular exercise will keep your blood pressure and cholesterol levels at a healthy level, helping prevent your blood vessels becoming damaged.
Unless advised otherwise by your doctor, you should be aiming for at least 150 minutes (two-and-a-half hours) of moderately intense physical exercise a week.
Moderate intensity physical activity is any activity that increases your heart and breathing rate. It may make you sweat but you’ll still be able to hold a normal conversation. Examples include:
- fast walking
- cycling on level ground or with few hills
- swimming
- tennis
You should choose physical activities you enjoy because you’re more likely to continue doing them.
It’s probably unrealistic to meet these exercise targets immediately if you haven’t exercised much in the past. Aim to start gradually and build up the amount of exercise you do over time.
Watch out when the temperature drops
Frostbitten skin can lead to gangrene because frostbite reduces blood circulation in an affected area. If you notice that any area of your skin has become pale, hard, cold and numb after prolonged exposure to cold temperatures, call your doctor.
Gangrene symptoms
The symptoms of gangrene vary depending on the underlying cause. It can affect any part of the body, but typically starts in the toes, feet, fingers or hands.
General symptoms of gangrene include:
- initial redness and swelling
- either a loss of sensation or severe pain in the affected area
- sores or blisters that bleed or release a dirty-looking or foul-smelling discharge (if the gangrene is caused by an infection)
- the skin becoming cold and pale
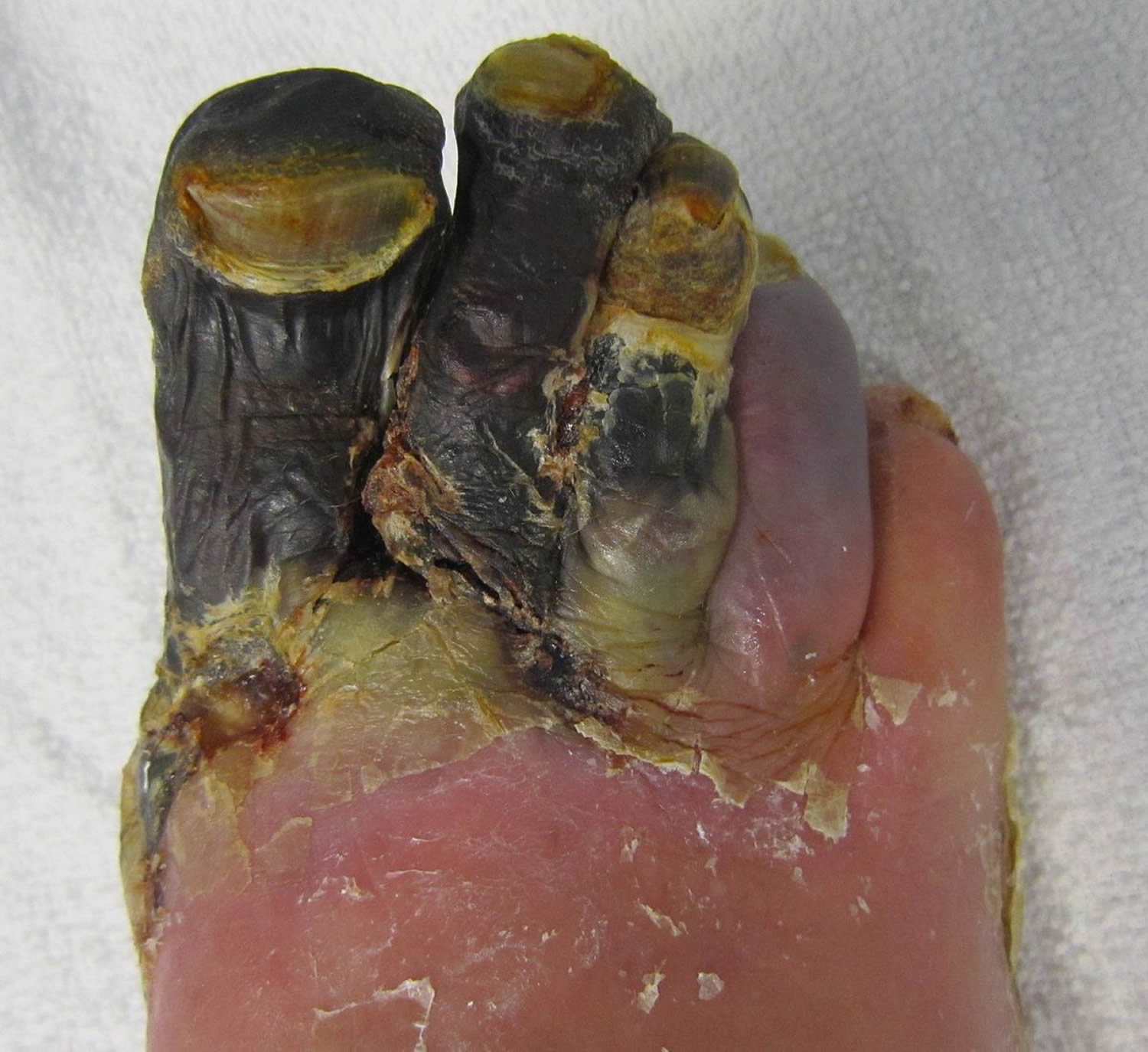
Figure 2. Gangrene foot
In some cases, the affected limb may feel heavy and pressing the skin may produce a crackling sound. These symptoms are caused by a build-up of gas under the skin.
If the area is infected, you may also have other signs related to the underlying infection, such as:
- a high temperature (fever)
- loss of appetite
- rapid heartbeat and breathing
- dizziness
- shivering
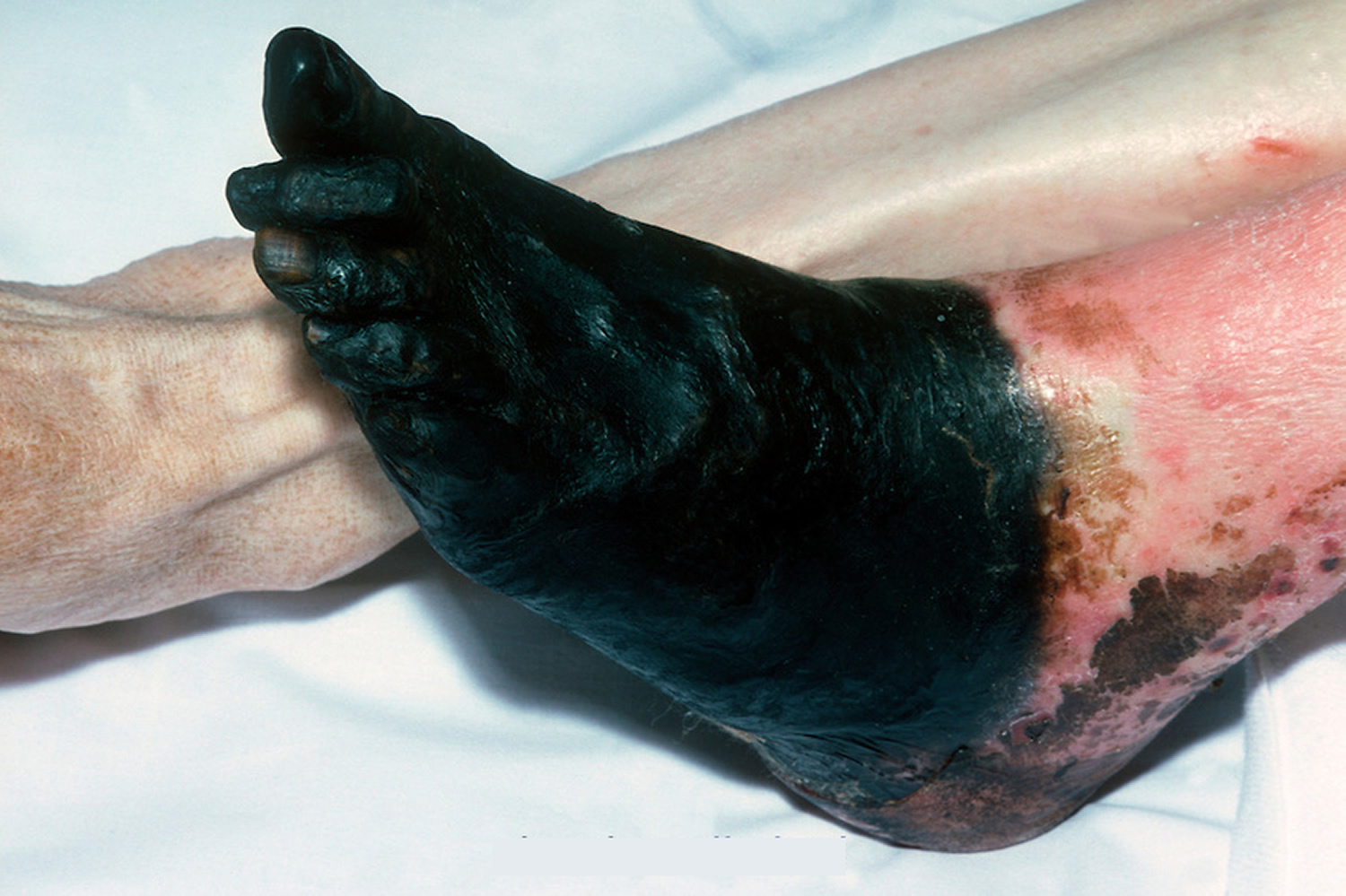
Without treatment the affected tissue will start to die. When this happens, the area changes color from red to brown to purple or black, before shriveling up and falling away from the surrounding healthy tissue.
Figure 3. Gangrene foot
Gangrene diagnosis
A diagnosis of gangrene is based on a combination of physical examination, medical history and tests.
Your doctor will want to find out whether you have any long-term health conditions, or if you’ve recently experienced any injuries that could have caused the condition.
They’ll also examine the affected area to check for any obvious signs of gangrene, such as a foul odor or discoloration of the skin.
A number of tests and investigations can be carried out to confirm the diagnosis of gangrene. These include:
- blood tests to check for an infection.
- fluid or tissue culture – where a small tissue or fluid sample from the affected area is tested to find out which bacteria are responsible for the condition and determine the most effective antibiotic to treat it with
- blood cultures – where a sample of blood is taken and put into special culture bottles and placed in a warm environment (incubated) to encourage the growth of bacteria so they can be examined further
- imaging tests – a range of imaging tests, such as X-rays, magnetic resonance imaging (MRI) scans or computerised tomography (CT) scans can be used to confirm the presence and spread of gangrene; these tests can also be used to study blood vessels so any blockages can be identified
- surgery – a surgical examination under anaesthetic may be necessary to confirm a diagnosis of gangrene deeper inside the body
As gangrene is a potentially serious condition, treatment is usually started before the results of any tests become available.
Gangrene treatment
Treatment for gangrene involves removing the affected tissue, preventing infection or treating any existing infection, and treating the problem that led to gangrene developing.
For example, if gangrene is caused by a poor blood supply, surgery may be used to repair damaged blood vessels. If gangrene is caused by an infection, strong antibiotics may be used as well as surgery.
Removing dead tissue
Surgery to cut out the dead tissue, known as debridement, is often necessary to prevent the gangrene from spreading and to allow the surrounding healthy tissue to heal.
Larval debridement therapy (biosurgery)
In some cases, it may be possible to use larval debridement therapy, also known as biosurgery, instead of conventional surgery to remove the dead tissue.
Certain types of fly larvae are ideal for this because they feed on dead and infected tissue but leave healthy tissue alone. They also help fight infection by releasing substances that kill bacteria and stimulate the healing process.
Maggots used for larval therapy are specially bred in a laboratory using eggs that have been treated to remove bacteria. The maggots are placed on the wound and covered with gauze, under a firm dressing, which keeps them on the wound (and out of sight). After a few days, the dressing is cut away and the maggots are removed.
Medical studies have shown larval debridement therapy can achieve more effective results than surgical debridement. However, because of the nature of this type of treatment, many people are reluctant to try it.
Amputation
In severe cases of gangrene, where a whole body part, such as a finger, toe, or limb, is affected and debridement is unlikely to help, amputation may be considered.
Amputation can prevent gangrene spreading to other parts of the body and can be used to remove a severely damaged limb so an artificial (prosthetic) limb can be fitted.
Unless immediate emergency treatment is needed, a decision to amputate will only be made after a full discussion between you and the health professionals treating you.
Treating infection
Gangrene that’s caused by an infection can usually be treated with antibiotics, which can be given as tablets or injections.
Injections are usually necessary if you need surgery or you have a severe infection. Injecting antibiotics directly into a vein allows larger doses to be given and means that they’re more likely to reach the affected area.
To counter the effects of infection and accelerate the healing process, you’ll also need fluids and nutrients into a vein (intravenous fluids) and you may need blood transfusions.
Restoring blood flow
In some cases, surgery may be carried out to restore the blood flow to the affected area. The main techniques used to achieve this are:
- bypass surgery – where the surgeon redirects the flow of blood and bypasses the blockage by connecting (grafting) one of your veins to a healthy part of an artery
- angioplasty – where a tiny balloon is placed into a narrow or blocked artery and is inflated to open up the vessel; a small metal tube, known as a stent, may also be inserted into the artery to help keep it open
Research suggests that both techniques are equally effective in restoring blood flow and preventing the need for amputation in the short-term. An angioplasty has the advantage of having a faster recovery time than bypass surgery, although it may not be as effective in the long-term as bypass surgery.
Hyperbaric oxygen therapy
Hyperbaric oxygen therapy is an alternative treatment for some types of gangrene.
During hyperbaric oxygen therapy, you sit or lie down in a specially designed chamber filled with pressurized air. A plastic hood that provides pure oxygen for you to inhale is placed over your head.
The chamber is pressurized with pure oxygen, and the pressure inside the chamber will slowly rise to about 2.5 times normal atmospheric pressure. Hyperbaric oxygen therapy for gas gangrene generally lasts about 90 minutes. You may need two to three treatments daily.
This treatment results in high levels of oxygen being dispersed into your bloodstream and reaching the affected areas (even those with a poor blood supply), which speeds up healing. Blood rich in oxygen slows the growth of bacteria that thrive in the absence of oxygen and helps infected wounds heal more easily.
For gangrene caused by a bacterial infection, the oxygen can also stop some types of bacteria (particularly the type responsible for gas gangrene) producing the toxins that allow the infection to spread, preventing further tissue damage.
Hyperbaric oxygen therapy has proved effective in treating gangrene caused by infected diabetic foot ulcers, reducing the risk of amputation.
However, evidence relating to the effectiveness of hyperbaric oxygen therapy in treating other types of gangrene is limited and further research is required. Hyperbaric oxygen therapy also isn’t currently widely available in the US.
Reconstructive surgery
Reconstructive surgery using a skin graft may be used to cover the area of skin damaged by gangrene.
During a skin graft, the surgeon will remove healthy skin from another part of your body (usually a part that would be covered by clothing), and reconnect it over the damaged area.
- Sorensen MD, Krieger JN, Rivara FP, et al. Fournier’s Gangrene: Population Based Epidemiology and Outcomes. The Journal of urology. 2009;181(5):2120-2126. doi:10.1016/j.juro.2009.01.034. https://www.ncbi.nlm.nih.gov/pmc/articles/PMC3042351/[↩][↩][↩]
- Mallikarjuna MN, Vijayakumar A, Patil VS, Shivswamy BS. Fournier’s Gangrene: Current Practices. ISRN Surgery. 2012;2012:942437. doi:10.5402/2012/942437. https://www.ncbi.nlm.nih.gov/pmc/articles/PMC3518952/[↩][↩]
- Thwaini A, Khan A, Malik A, et al. Fournier’s gangrene and its emergency management. Postgraduate Medical Journal. 2006;82(970):516-519. doi:10.1136/pgmj.2005.042069. https://www.ncbi.nlm.nih.gov/pmc/articles/PMC2585703/[↩]
- Fournier’s gangrene: risk factors and strategies for management. World J Surg. 2006 Sep;30(9):1750-4. https://www.ncbi.nlm.nih.gov/pubmed/16927060[↩]
- Fournier’s gangrene: report of thirty-three cases and a review of the literature. Int J Urol. 2006 Jul;13(7):960-7. https://www.ncbi.nlm.nih.gov/pubmed/16882063[↩]
- Zamboni, WA; Riseman, JA; Kucan, JO (1990). “Management of Fournier’s gangrene and the role of hyperbaric oxygen”. J. Hyperbaric Med. 5 (3): 177–86 http://archive.rubicon-foundation.org/xmlui/bitstream/handle/123456789/4431/JHM_V5N3_4.pdf[↩]