Contents
What is geographic tongue
Geographic tongue is characterized by irregularly shaped red, map-like smooth swollen patches on the surface of the tongue. A white border sometimes surrounds them. Geographic tongue also known as benign migratory glossitis or erythema migrans, because the appearance is constantly changing. Although geographic tongue is benign (harmless) it may persist for months or longer and often recurs. Although geographic tongue may look alarming, it doesn’t cause health problems and isn’t associated with infection or cancer.
Geographic tongue occurs affects 1 to 14 percent of the U.S. population and is of unknown etiology 1. It may occur in any race, age or sex. However, it appears more commonly in females than males and more frequently in adults 2.
Often there are no symptoms but burning or irritation of the tongue is common, particularly with hot or spicy foods, salt and even sweets. The discomfort may come and go over time and may worsen at certain times of a women’s menstrual cycle or during pregnancy.
Lesions are usually confined to the tongue but they sometimes arise elsewhere in the mouth or on the lips.
Although previous research pointed geographic tongue associations with diabetes, psoriasis, seborrheic dermatitis, and atopy, recent analysis of population data from U.S. patients does not support these findings 3. The prevalence is higher among white and black persons compared with Mexican Americans, and it has an association with fissured tongue and an inverse association with cigarette smoking 4.
With geographic tongue, the dorsal tongue develops areas of papillary atrophy that appear smooth and are surrounded by raised serpiginous borders. These regions of atrophy spontaneously resolve and migrate, giving the tongue a variegated appearance. The condition is benign and localized, generally requiring no treatment except reassurance. Some patients may have sensitivity to hot or spicy foods 5, 6. Topical steroid gels (e.g., triamcinolone dental paste [Oralone]) and antihistamine mouth rinses (e.g., diphenhydramine elixir [Banophen], 12.5 mg per 5 mL diluted in a 1:4 ratio with water) can reduce tongue sensitivity 7, 8, 9.
- Geographic tongue is a benign condition. It doesn’t pose a threat to your health, cause long-term complications or increase your risk of major health problems.
- Geographic tongue is a minor — although sometimes uncomfortable — condition. Geographic tongue can sometimes cause tongue discomfort and increased sensitivity to certain substances, such as spices, spicy foods, salt and even sweets.
However, lesions on the tongue may indicate other more-serious conditions of the tongue or diseases affecting the body in general. If you have lesions on the tongue that don’t resolve within 10 days, see your doctor or dentist.
See your health provider if the symptoms last longer than 10 days. Seek medical help right away if:
- You have breathing problems.
- Your tongue is severely swollen.
- You have problems speaking, chewing, or swallowing.
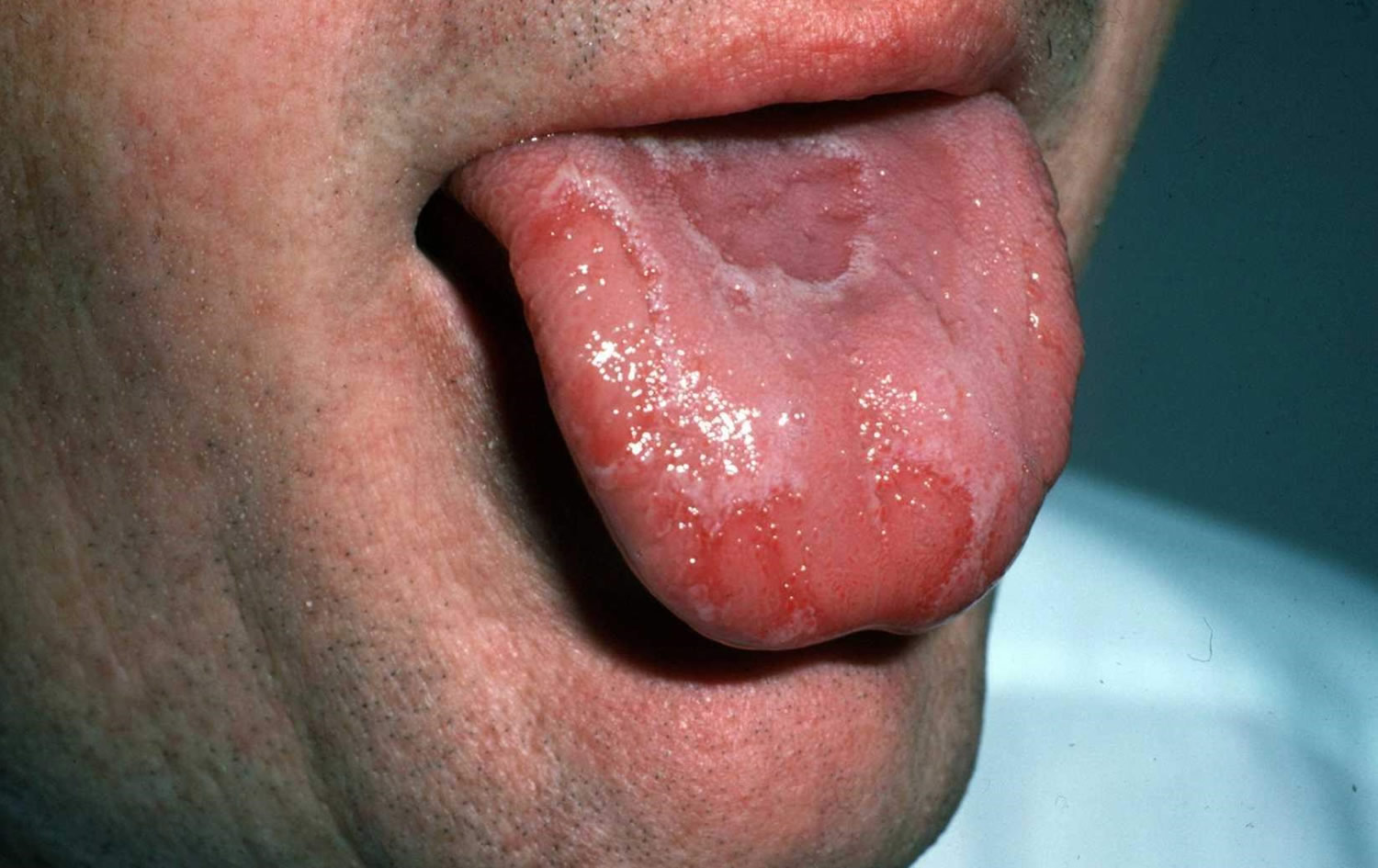
Figure 1. Geographic tongue
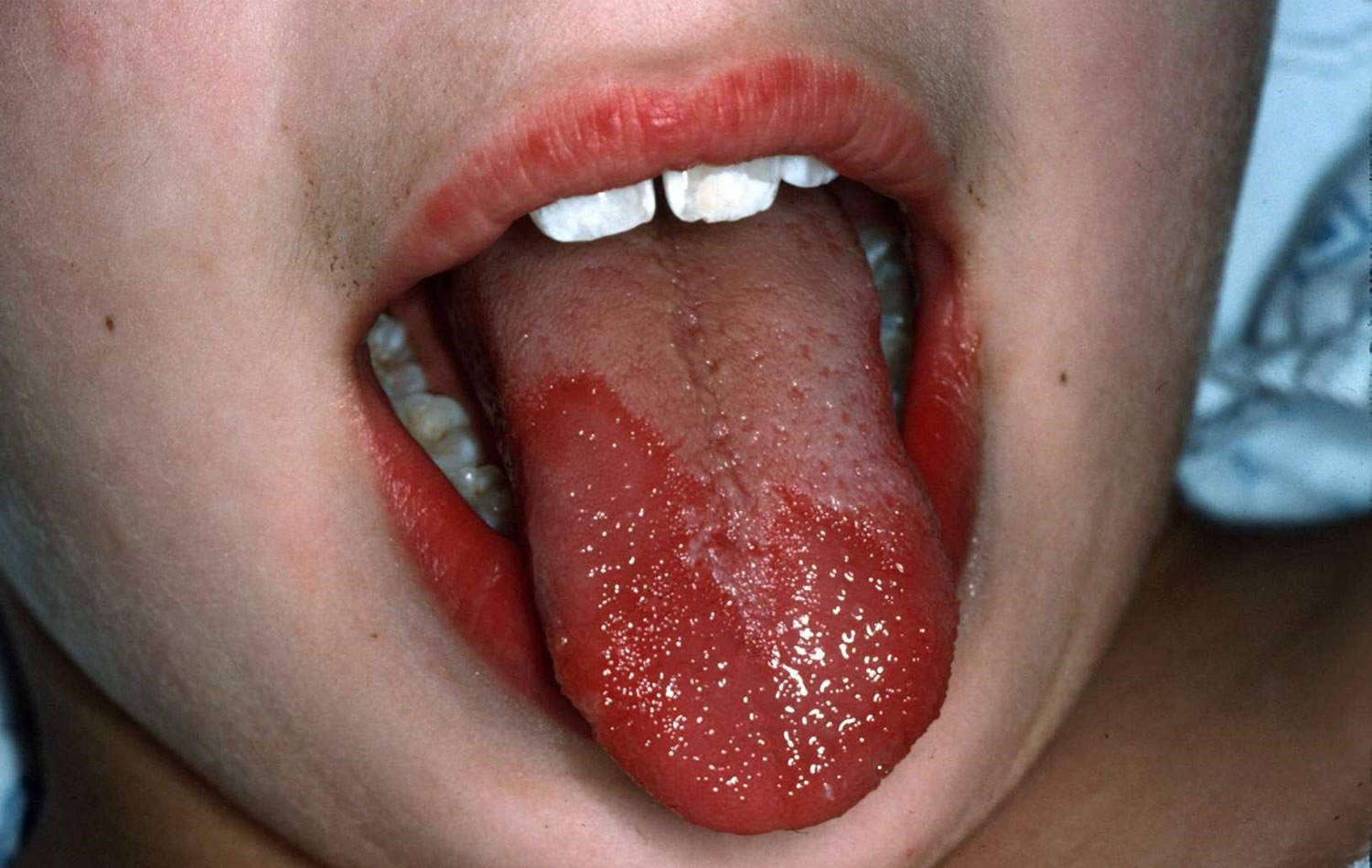
Figure 2. Geographic tongue
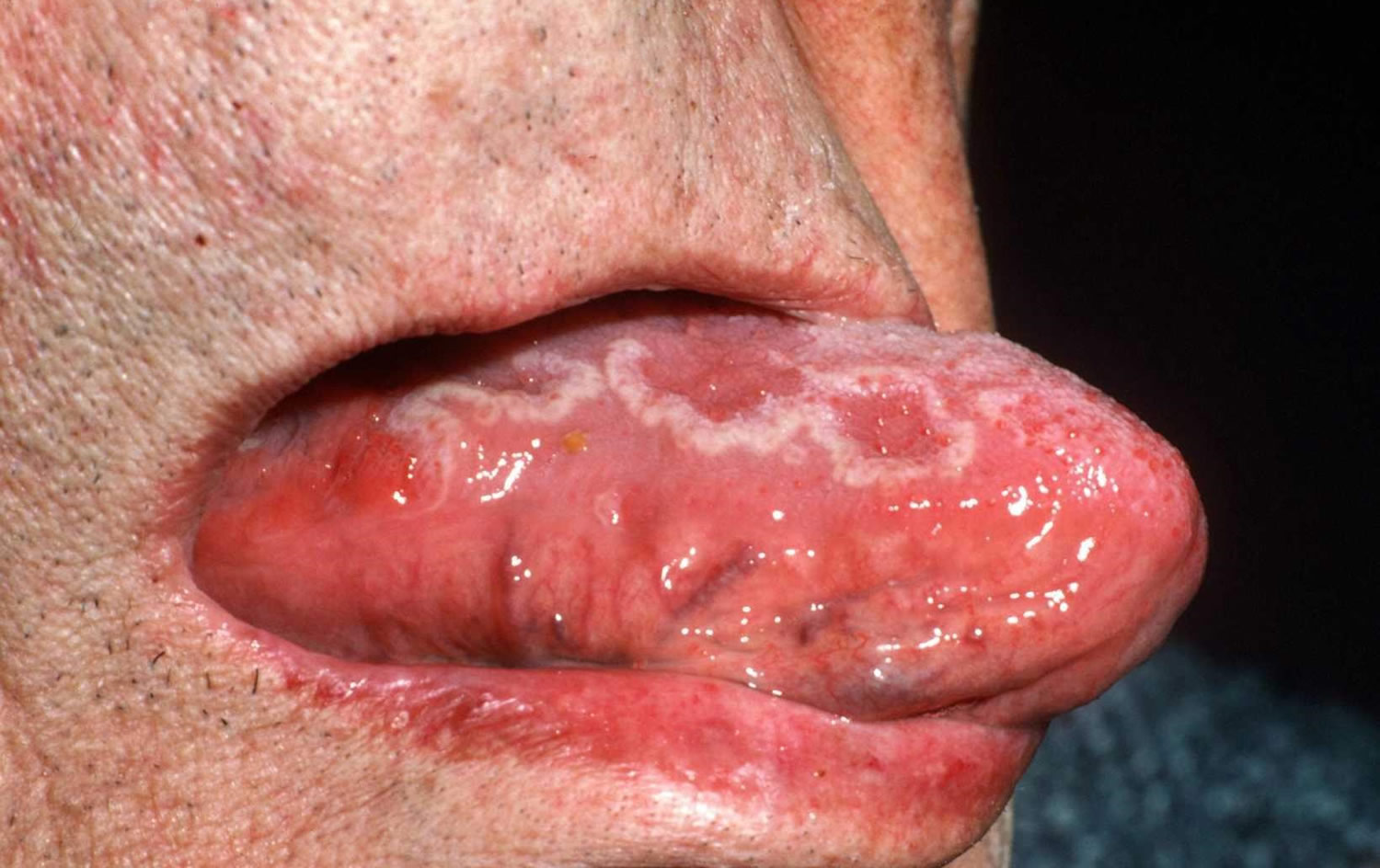
Figure 3. Geographic tongue
Geographic tongue symptoms
Signs and symptoms of geographic tongue may include:
- Smooth, red, irregularly shaped patches (lesions) on the top or side of your tongue
- Frequent changes in the location, size and shape of lesions
- Discomfort, pain or burning sensation in some cases, most often related to eating spicy or acidic foods
Many people with geographic tongue have no symptoms.
Geographic tongue can continue for days, months or years. The problem often resolves on its own but may appear again at a later time.
What causes geographic tongue
The cause of geographic tongue is unknown, and there’s no way to prevent the condition. There may be a link between geographic tongue and psoriasis and between geographic tongue and lichen planus. But more research is needed to better understand possible connections.
The following factors have been linked with geographic tongue:
- It occurs more commonly in patients with psoriasis, especially pustular psoriasis
- There are also associations with diabetes, anemia, atopy (asthma and/or eczema) and stress
- In some patients particular foods seem to be a trigger, especially cheese
- Clustering within a family suggests genetic involvement
- Variation with the menstrual cycle suggests hormonal factors.
Risk factors for geographic tongue
Studies of factors that may be associated with an increased risk of geographic tongue have produced mixed results. Factors that are likely associated with an increased risk include:
- Family history. Some people with geographic tongue have a family history of the disorder, so inherited genetic factors may increase risk.
- Fissured tongue. People with geographic tongue often have another disorder called fissured tongue, which has the appearance of deep grooves (fissures) on the surface of the tongue.
Geographic tongue diagnosis
Your physician or dentist can usually make a diagnosis of geographic tongue based on an examination of your tongue and your signs and symptoms.
During the exam, your physician or dentist may:
- Use a lighted instrument to check your tongue and mouth
- Ask you to move your tongue around in various positions
- Gently touch (palpate) your tongue to check for tenderness or unusual changes in the tongue’s texture or consistency
- Check for signs of infection, such as fever or swollen lymph nodes in the neck
Geographic tongue treatment
No treatment necessary, because geographic tongue is a benign (harmless) condition that usually resolves itself without causing any problems for the patient so most people do not require treatment. There is no known cure. If there are associated medical conditions, treatment of these may improve the appearance of the tongue.
Discomfort may be treated with a mouth gargle or rinse containing antiseptic and anesthetic agents. Topical steroid gels (e.g., triamcinolone dental paste [Oralone]) and antihistamine mouth rinses (e.g., diphenhydramine elixir [Banophen], 12.5 mg per 5 mL diluted in a 1:4 ratio with water) can reduce tongue sensitivity 7, 8, 9.
- Shulman JD, Beach MM, Rivera-Hidalgo F. The prevalence of oral mucosal lesions in U.S. adults: data from the Third National Health and Nutrition Examination Survey, 1988–1994. J Am Dent Assoc. 2004;135(9):1279–1286.[↩]
- Common Tongue Conditions in Primary Care. Am Fam Physician. 2010 Mar 1;81(5):627-634. https://www.aafp.org/afp/2010/0301/p627.html[↩]
- Byrd JA, Bruce AJ, Rogers RS III. Glossitis and other tongue disorders. Dermatol Clin. 2003;21(1):123–134.[↩]
- Shulman JD, Carpenter WM. Prevalence and risk factors associated with geographic tongue among US adults. Oral Dis. 2006;12(4):381–386.[↩]
- Assimakopoulos D, Patrikakos G, Fotika C, Elisaf M. Benign migratory glossitis or geographic tongue: an enigmatic oral lesion. Am J Med. 2002;113(9):751–755.[↩]
- Jainkittivong A, Langlais RP. Geographic tongue: clinical characteristics of 188 cases. J Contemp Dent Pract. 2005;6(1):123–135.[↩]
- Gonsalves WC, Chi AC, Neville BW. Common oral lesions: Part I. Superficial mucosal lesions. Am Fam Physician. 2007;75(4):501–507.[↩][↩]
- Assimakopoulos D, Patrikakos G, Fotika C, Elisaf M. Benign migratory glossitis or geographic tongue: an enigmatic oral lesion. Am J Med. 2002;113(9):751–755.[↩][↩]
- Sigal MJ, Mock D. Symptomatic benign migratory glossitis: report of two cases and literature review. Pediatr Dent. 1992;14(6):392–396.[↩][↩]