Contents
What is Graves disease
Graves’ disease is an auto-immune condition where your body’s immune system produces antibodies against the thyroid TSH (thyroid stimulating hormone) receptor, leading to the thyroid becoming overactive or hyperthyroidism 1. In about three in every four cases, an overactive thyroid (thyrotoxicosis) is caused by a condition called Graves’ disease. Symptoms of Graves’ disease include racing heart, sweating, weight loss, irritability, fatigue and sleep loss.
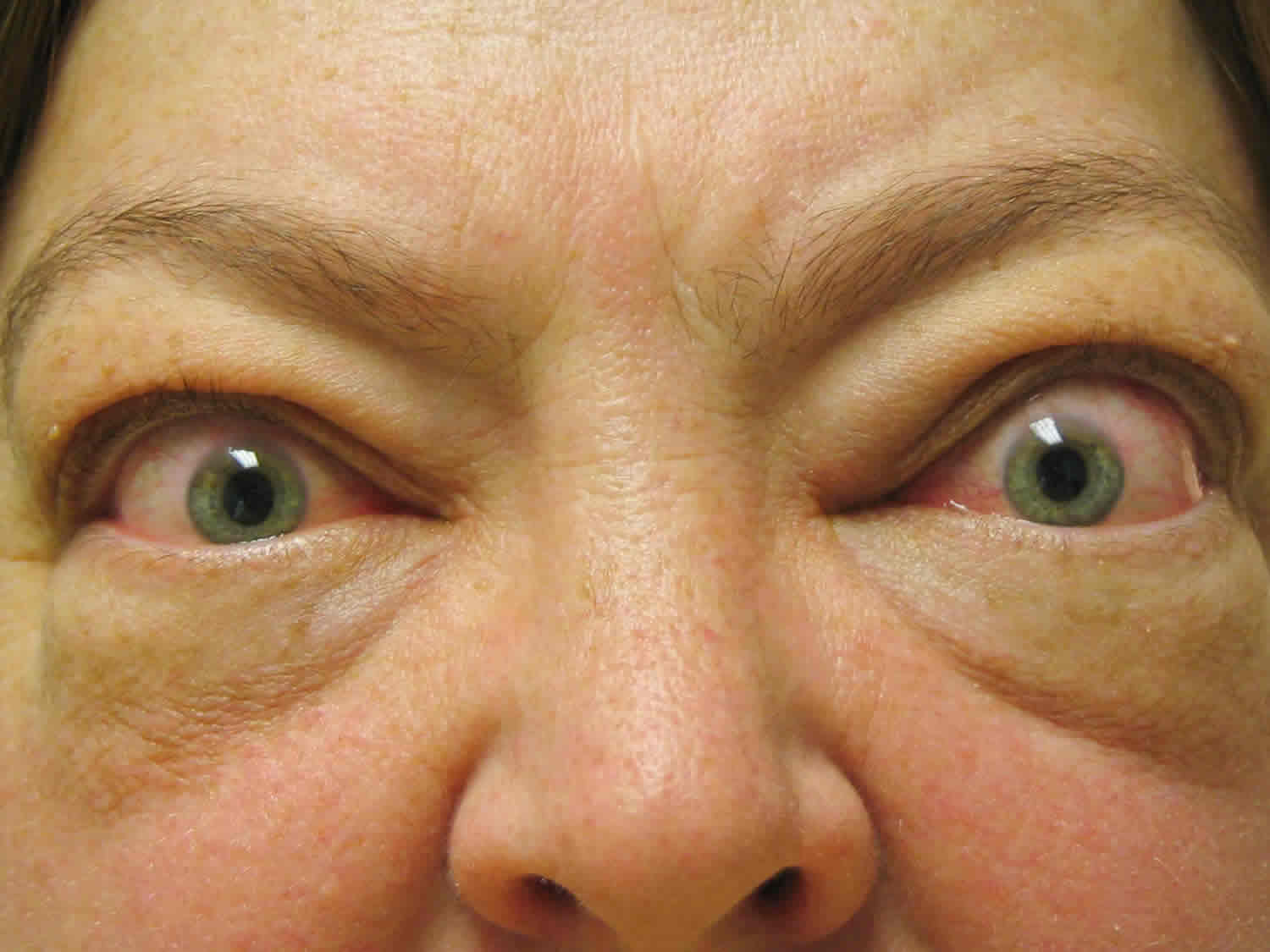
Graves’ disease causes the thyroid gland in the neck to produce too much thyroid hormone. People who have had Graves’ disease for long periods can develop bulging eyes or exophthalmos (see Figure 2 below). It is also possible to get a goiter, which is a swollen thyroid gland visible to others.
Graves’ disease is characterized by hyperthyroidism and one or more of the following:
- goiter,
- exophthalmos (protrusion of the eyeballs), and
- pretibial myxoedema (swelling on the shin above the lateral bone of the ankle).
The cause of Graves’ disease is unknown, but it mostly affects young or middle-aged women and it often runs in families. Graves’ Disease is the most common cause of hyperthyroidism, affecting 2-5% of females at some time, with a female:male ratio of 7:1. The disease has a peak incidence between the ages of 20 and 40 years of age.
Smoking can also increase your risk of getting it 2. Treatments involve reducing the activity of the gland with medicines, and sometimes surgery.
The thyroid gland
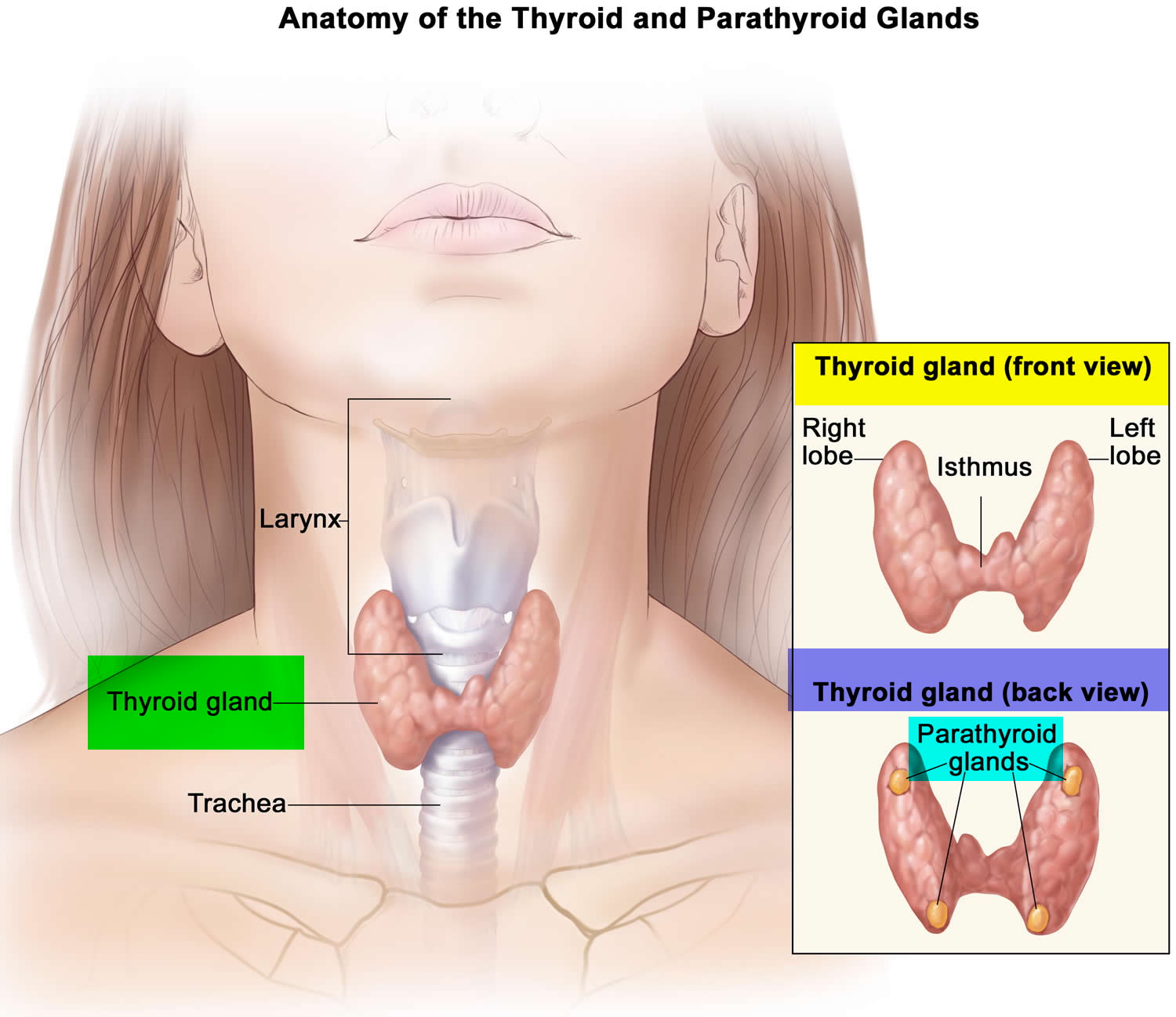
Your thyroid is a butterfly-shaped gland, located just inferior to the larynx, or voice box at the base of your neck (Figure 2). It’s right and left lateral lobes lie on either side of the trachea, or windpipe. Connecting the lobes is a mass of tissue called the isthmus, that lies in front of the windpipe. Microscopic sacs called thyroid follicles comprise most of the thyroid gland. The walls of each of these thyroid follicles is made up by two types of cells, follicular cells and parafollicular (or C) cells. The follicular cells produce the thyroid hormones, called thyroxine, or T4, and T3. Thyroid hormones that control many activities in your body, including how fast your heart beats and how fast you burn calories (your metabolism). Regulation of metabolism is critical in controlling mood, weight and mental and physical energy levels. Parafollicular cells produce the hormone calcitonin, which helps to regulate the levels of calcium in the body.
In a person with Graves’ disease, the immune system makes antibodies that cause the thyroid to make more thyroid hormone than the body needs. Graves’ disease most often leads to hyperthyroidism. Hyperthyroidism causes your metabolism to speed up.
Figure 1. Thyroid gland location
Is Graves disease curable?
Graves disease is a chronic illness without a true cure.
Graves disease is chronic with a fluctuating course, many patients show a pattern of alternating relapse and remission; perhaps only 40% of patients have a single episode. Many patients eventually become hypothyroid. The disease may remit spontaneously.
None of the management options for this disorder actually remove the underlying immunologic disorder. Therefore, the prognosis of the disorder is very much dependent upon the form of therapy chosen.
Graves disease causes
Graves’ disease is an autoimmune disease. Autoimmune diseases are where the immune system attacks certain tissues of the body, and in Graves Disease that causes overactivity of the thyroid gland. It is caused by the body’s production of antibodies against the thyroid TSH (thyroid stimulating hormone) receptor, which results in continuous stimulation of the thyroid gland to synthesize and secrete excess quantities of the thyroid hormones, T4 and T3. Normally, thyroid function is regulated by a hormone released by a tiny gland at the base of the brain (pituitary gland). The antibody associated with Graves’ disease — thyrotropin receptor antibody (TRAb) — acts like the regulatory pituitary hormone. That means that TRAb overrides the normal regulation of the thyroid, causing an overproduction of thyroid hormones (hyperthyroidism).
There is also a genetic component to the disease, with its development being linked to the presence of certain genes in individuals. Graves’ Disease (and Hashimoto’s thyroiditis) is sometimes associated with other autoimmune disorders, including insulin dependent diabetes mellitus, pernicious anemia, collagen diseases, and rheumatoid arthritis.
Cause of Graves’ eye disease
This condition results from a buildup of certain carbohydrates in the muscles and tissues behind the eyes — the cause of which also isn’t known. It appears that the same antibody that can cause thyroid dysfunction may also have an “attraction” to tissues surrounding the eyes.
Graves’ ophthalmopathy often appears at the same time as hyperthyroidism or several months later. But signs and symptoms of ophthalmopathy may appear years before or after the onset of hyperthyroidism. Graves’ ophthalmopathy can also occur even if there’s no hyperthyroidism.
Who gets Graves’ disease?
Graves’ disease is more common in women than in men. Women are most often affected between the ages of 30 and 60.
Some women are more likely to develop Graves’ disease than other women. Your risk is higher if you 1:
- Have a family history. Graves’ disease may run in families. Researchers are working to find the gene or genes involved.
- Have another autoimmune disease, such as rheumatoid arthritis, type 1 diabetes, pernicious anemia, or lupus.
- Are under stress. Severe emotional stress or trauma may trigger Graves’ disease.
- Recently had a baby. Pregnancy affects the thyroid gland. The risk of developing Graves’ disease is seven times higher in the year after giving birth. This suggests that pregnancy might trigger or reveal Graves’ disease in some women.
- Have a history of infection. Infection may play a role in the development of Graves’ disease. Researchers have found a link between Graves’ disease and infection with the virus that causes mononucleosis (“mono”; Epstein-Barr virus) 3.
- Smoke. Smoking raises your risk for Graves’ disease. It is also a leading risk factor for the eye problem seen in Graves’ disease, called Graves’ ophthalmopathy 2.
Risk factors for Graves disease
Although anyone can develop Graves’ disease, a number of factors can increase the risk of disease. These risk factors include the following:
- Family history. Because a family history of Graves’ disease is a known risk factor, there is likely a gene or genes that can make a person more susceptible to the disorder.
- Gender. Women are much more likely to develop Graves’ disease than are men.
- Age. Graves’ disease usually develops in people younger than 40.
- Other autoimmune disorders. People with other disorders of the immune system, such as type 1 diabetes or rheumatoid arthritis, have an increased risk.
- Emotional or physical stress. Stressful life events or illness may act as a trigger for the onset of Graves’ disease among people who are genetically susceptible.
- Pregnancy. Pregnancy or recent childbirth may increase the risk of the disorder, particularly among women who are genetically susceptible.
- Smoking. Cigarette smoking, which can affect the immune system, increases the risk of Graves’ disease. Smokers who have Graves’ disease are also at increased risk of developing Graves’ ophthalmopathy.
Graves disease complications
Complications of Graves’ disease can include:
- Pregnancy issues. Possible complications of Graves’ disease during pregnancy include miscarriage, preterm birth, fetal thyroid dysfunction, poor fetal growth, maternal heart failure and preeclampsia. Preeclampsia is a maternal condition that results in high blood pressure and other serious signs and symptoms.
- Heart disorders. If left untreated, Graves’ disease can lead to heart rhythm disorders, changes in the structure and function of the heart muscles, and the inability of the heart to pump enough blood to the body (congestive heart failure).
- Thyroid storm. A rare, but life-threatening complication of Graves’ disease is thyroid storm, also known as accelerated hyperthyroidism or thyrotoxic crisis. It’s more likely when severe hyperthyroidism is untreated or treated inadequately. The sudden and drastic increase in thyroid hormones can produce a number of effects, including fever, profuse sweating, vomiting, diarrhea, delirium, severe weakness, seizures, markedly irregular heartbeat (arrhythmia), yellow skin and eyes (jaundice), severe low blood pressure, and coma. Thyroid storm requires immediate emergency care.
- Brittle bones. Untreated hyperthyroidism also can lead to weak, brittle bones (osteoporosis). The strength of your bones depends, in part, on the amount of calcium and other minerals they contain. Too much thyroid hormone interferes with your body’s ability to incorporate calcium into your bones.
Graves disease symptoms
Many of the symptoms of Graves’ disease are the same as those of other causes of hyperthyroidism. Other signs are found only in Graves’ disease 4.
Symptoms of Graves’ disease include:
- Bulging eyes (only in Graves’ disease) 4
- Thickening and reddening of the skin, especially on the shins and upper feet (only in Graves’ disease) 4
- Anxiety, irritability or nervousness
- Tiredness or muscle weakness
- Heat sensitivity and an increase in perspiration or warm, moist skin
- Trouble sleeping
- A fine tremor of your hands or fingers
- Rapid and irregular heartbeat (palpitations)
- Diarrhea or frequent bowel movements
- Weight loss without dieting
- Goiter, which is an enlarged thyroid that can cause the neck to look swollen
- Change in menstrual cycles
- Erectile dysfunction or reduced libido
- Fatigue
- Thick, red skin usually on the shins or tops of the feet (Graves’ dermopathy)
The symptoms of Graves’ disease can start slowly or very suddenly. Some people do not have any symptoms.
How does Graves’ disease affect women?
Women are more likely to get Graves’ disease than men. Graves’ disease also affects women differently than men. In addition to causing heart problems and osteoporosis, Graves’ disease in women can cause:
- Problems with your menstrual period. Your thyroid hormone can affect your menstrual cycle. Too much thyroid hormone can cause irregular menstrual periods and make your periods lighter than normal.
- Problems getting pregnant. Irregular menstrual cycles can make it harder for women with Graves’ disease to get pregnant. About half of women with Graves’ disease have problems getting pregnant 5.
- Problems during pregnancy. Graves’ disease can cause problems for you during pregnancy and for your unborn baby’s development.
- Problems after pregnancy. Graves’ disease often gets better during the last three months of pregnancy, but it may get worse after delivery 6.
What eye problems are caused by Graves’ disease?
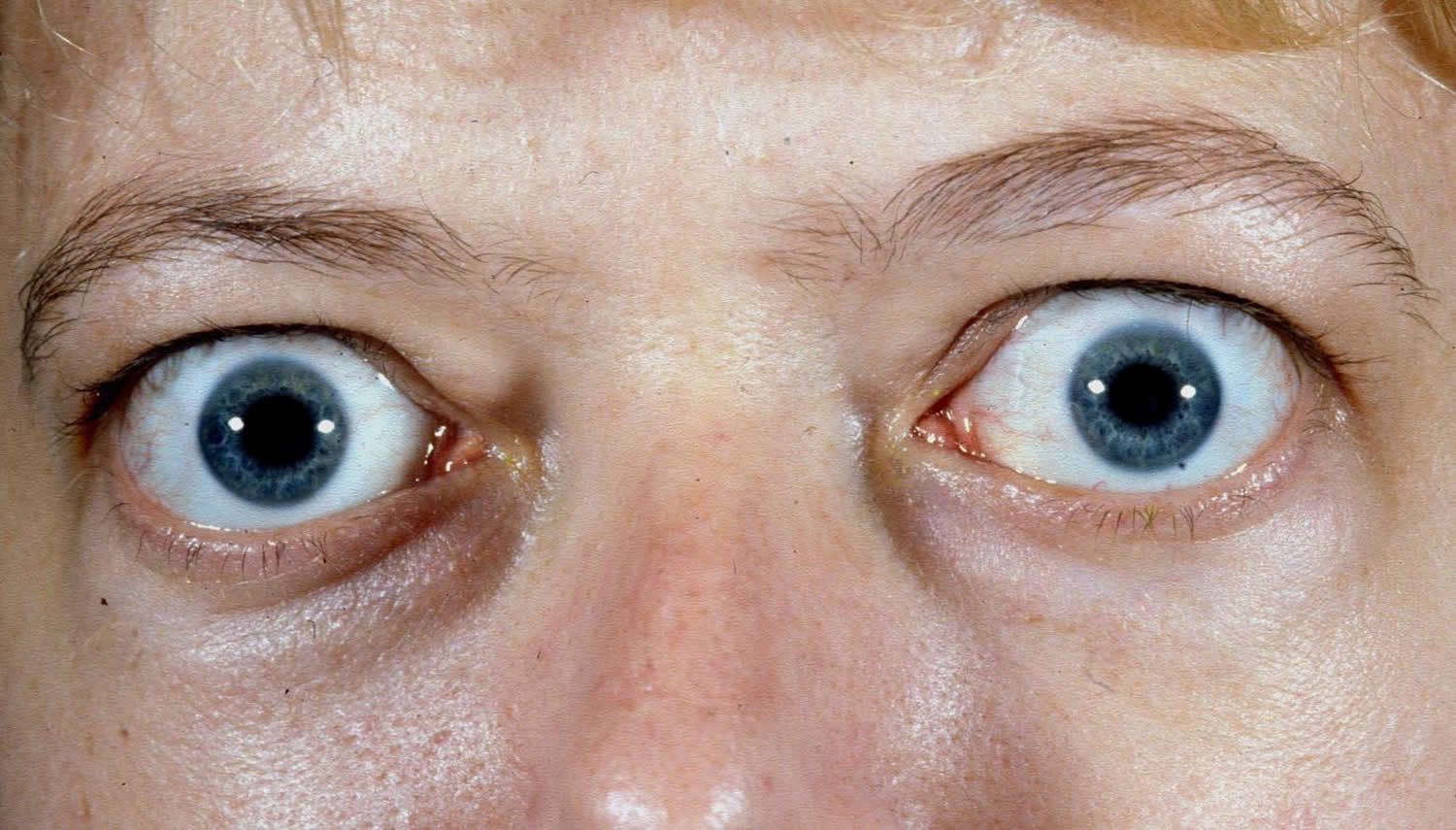
Graves’ disease can lead to an eye problem called Graves’ ophthalmopathy (Figure 2). It affects up to half of people with Graves’ disease 7. The main symptoms of Graves’ ophthalmopathy are eyes that seem to bulge out of their eye sockets, problems seeing, and irritated eyes.
Graves’ ophthalmopathy happens when cells from your body’s immune (defense) system attack the tissues around your eyes. The result is inflammation and swelling in the eye socket, causing the eyeball to bulge out. If left untreated, damage to the nerves in the eyes can also lead to blindness.
Smoking (including secondhand smoke) is the leading risk factor for Graves’ ophthalmopathy. Quitting smoking lowers your risk for developing Graves’ ophthalmopathy 2. If you already have Graves’ ophthalmopathy, quitting smoking can help your treatment work better.
In Graves’ ophthalmopathy, inflammation and other immune system events affect muscles and other tissues around your eyes. The resulting signs and symptoms may include:
- Bulging eyes (exophthalmos)
- Gritty sensation in the eyes
- Pressure or pain in the eyes
- Puffy or retracted eyelids
- Reddened or inflamed eyes
- Light sensitivity
- Double vision
- Vision loss
Graves’ ophthalmopathy is treated with eye drops and eyeglasses, radiation therapy, or eye surgery. Your treatment will depend on how serious your eye problems are 4.
Figure 2. Graves disease eyes (exophthalmos)
Graves disease diagnosis
To diagnose Graves’ disease, your doctor will do a physical exam and may do some tests. Tests that can help you find out if you have Graves’ disease include:
- Thyroid function tests. These tests check your blood for levels of the main thyroid hormone (T4) and thyroid-stimulating hormone (TSH). A high level of T4 plus a low level of TSH is a sign of an overactive thyroid gland. Sometimes, routine screening of thyroid function shows mild overactive thyroid in a person without symptoms. When this happens, your doctor may suggest treatment or watchful waiting to see if levels return to normal.
- Radioactive iodine uptake (RAIU) test. This test tells how much iodine the thyroid gland is using. The thyroid gland uses iodine to make thyroid hormone. Higher levels of iodine suggest Graves’ disease. The RAIU test can also help rule out other possible causes of an overactive thyroid gland.
- Antibody tests. These blood tests look for antibodies that suggest Graves’ disease.
- Ultrasound. Ultrasound uses high-frequency sound waves to produce images of structures inside the body. Ultrasound can show if the thyroid gland is enlarged, and is most useful in people who can’t undergo radioactive iodine uptake, such as pregnant women.
- Imaging tests. If the diagnosis of Graves’ ophthalmopathy isn’t clear from a clinical assessment, your doctor may order an imaging test, such as CT scan, a specialized X-ray technology that produces thin cross-sectional images. Magnetic resonance imaging (MRI), which uses magnetic fields and radio waves to create either cross-sectional or 3-D images, also may be used.
Your doctor will also need to perform the following investigations, most of which are possible from a simple blood test. Investigations include a full blood count, liver function tests, urea and electrolytes, and creatinine levels.
Graves disease treatment
Treatment consists of three possibilities: radioiodine, antithyroid drugs and surgery. 1) Radioactive iodine. Iodine-131 in an empirical dose accumulates in the thyroid and destroys the gland by local radiation, taking several months to be fully effective. 2) Antithyroid drugs. These include methimazole, carbimazole and propylthiouracil. These drugs inhibit the formation of thyroid hormones. 3) Subtotal thyroidectomy. Thyroidectomy can be performed only in patients who have previously been rendered euthyroid.
Radioactive iodine therapy
Radioactive iodine (RAI) is a type of iodine that damages the thyroid gland by giving it radiation. With this therapy, you take radioactive iodine, or radioiodine, by mouth. Because the thyroid needs iodine to produce hormones, the radioiodine goes into the thyroid cells and the radioactivity destroys the overactive thyroid cells over time. This causes your thyroid gland to shrink, and symptoms lessen gradually, usually over several weeks to several months.
This cures the overactive thyroid gland, but it can lead to underactive thyroid gland. If this happens, you will need to take thyroid hormone for the rest of your life.
Radioiodine therapy may increase your risk of new or worsened symptoms of Graves’ ophthalmopathy. This side effect is usually mild and temporary, but the therapy may not be recommended if you already have moderate to severe eye problems.
Other side effects may include tenderness in the neck and a temporary increase in thyroid hormones. Radioiodine therapy isn’t used for treating pregnant women or women who are breast-feeding.
Graves disease medication
The Food and Drug Administration has approved two medicines for Graves’ disease: methimazole and propylthiouracil. These medicines keep the thyroid gland from making too much thyroid hormone. They are often given to patients before thyroid surgery or radioiodine therapy. Because the risk of liver disease is more common with propylthiouracil, methimazole is considered the first choice when doctors prescribe medication. However you cannot take methimazole in the early stages of pregnancy, because it may hurt your developing baby.
When these two drugs are used alone, a relapse of hyperthyroidism may occur at a later time. Taking the drug for longer than a year, however, may result in better long-term results. Anti-thyroid drugs may also be used before or after radioiodine therapy as a supplemental treatment.
Side effects of both drugs include rash, joint pain, liver failure or a decrease in disease-fighting white blood cells. Methimazole isn’t used to treat pregnant women in the first trimester because of the slight risk of birth defects. Therefore, propylthiouracil is the preferred anti-thyroid drug during the first trimester for pregnant women. After the first trimester, methimazole use is generally resumed and propylthiouracil is no longer prescribed.
Beta blockers
Your doctor may also suggest you take a medicine called a beta blocker. Beta blockers don’t inhibit the production of thyroid hormones, but they do block the effects of excess thyroid hormone on your body. They slow down your heart rate and reduce symptoms such as shaking and nervousness. Beta blockers work quickly and can help you feel better while you wait for additional treatment to start working.
Beta blockers may provide fairly rapid relief of irregular heartbeats, tremors, anxiety or irritability, heat intolerance, sweating, diarrhea, and muscle weakness.
Beta blockers include:
- Propranolol (Inderal)
- Atenolol (Tenormin)
- Metoprolol (Lopressor, Toprol-XL)
- Nadolol (Corgard)
Beta blockers aren’t often prescribed for people with asthma, because the drugs may trigger an asthma attack. These drugs may also complicate management of diabetes.
All medicines have risks. You should talk to your doctor about the benefits and risks of all medicines.
Surgery
Surgery to remove all or part of your thyroid (thyroidectomy or subtotal thyroidectomy) also is an option for the treatment of Graves’ disease. As with radioactive iodine, surgery cures overactive thyroid but can lead to underactive thyroid. You will need to take thyroid hormone to replace the needed thyroid hormone that your body can no longer make.
Risks of this surgery include potential damage to the nerve that controls your vocal cords and the tiny glands located adjacent to your thyroid gland (parathyroid glands). Your parathyroid glands produce a hormone that controls the level of calcium in your blood. Complications are rare under the care of a surgeon experienced in thyroid surgery.
Treating Graves’ Eye Disease
Mild symptoms of Graves’ ophthalmopathy may be managed by using over-the-counter artificial tears during the day and lubricating gels at night. If your symptoms are more severe, your doctor may recommend:
- Corticosteroids. Treatment with prescription corticosteroids, such as prednisone, may diminish swelling behind your eyeballs. Side effects may include fluid retention, weight gain, elevated blood sugar levels, increased blood pressure and mood swings.
- Prisms. You may have double vision either because of Graves’ disease or as a side effect of surgery for Graves’ disease. Though they don’t work for everyone, prisms in your glasses may correct your double vision.
- Orbital decompression surgery. In this surgery, your doctor removes the bone between your eye socket (orbit) and your sinuses — the air spaces next to the orbit. This gives your eyes room to move back to their original position. This treatment is usually used if pressure on the optic nerve threatens the loss of vision. Possible complications include double vision.
- Orbital radiotherapy. Orbital radiotherapy was once a common treatment for Graves’ ophthalmopathy, but the benefits of the procedure aren’t clear. Orbital radiotherapy uses targeted X-rays over the course of several days to destroy some of the tissue behind your eyes. Your doctor may recommend orbital radiotherapy if your eye problems are worsening and prescription corticosteroids alone aren’t effective or well-tolerated.
Graves’ ophthalmopathy doesn’t always improve with treatment for Graves’ disease. Symptoms of Graves’ ophthalmopathy may even get worse for three to six months. After that, the signs and symptoms of Graves’ ophthalmopathy usually stabilize for a year or so and then begin to get better, often on their own.
Lifestyle and home remedies
If you have Graves’ disease, make your mental and physical well-being a priority:
- Eating well and exercising can enhance the improvement in some symptoms while being treated and help you feel better in general. For example, because your thyroid controls your metabolism, you may have a tendency to gain weight when the hyperthyroidism is corrected. Brittle bones also can occur with Graves’ disease, and weight-bearing exercises can help maintain bone density.
- Easing stress as much as you can may be helpful, as stress may trigger or worsen Graves’ disease. Listening to music, taking a warm bath or walking can help relax you and put you in a better frame of mind. Partner with your doctor to construct a plan that incorporates good nutrition, exercise and relaxation into your daily routine.
For Graves’ ophthalmopathy
These steps may make your eyes feel better if you have Graves’ ophthalmopathy:
- Apply cool compresses to your eyes. The added moisture may soothe your eyes.
- Wear sunglasses. When your eyes protrude, they’re more vulnerable to ultraviolet rays and more sensitive to bright light. Wearing sunglasses that wrap around the sides of your head will also lessen the irritation of your eyes from the wind.
- Use lubricating eyedrops. Eyedrops may relieve the dry, scratchy sensation on the surface of your eyes. A paraffin-based gel, such as Lacri-Lube, can be applied at night.
- Elevate the head of your bed. Keeping your head higher than the rest of your body lessens fluid accumulation in the head and may relieve the pressure on your eyes.
- Don’t smoke. Smoking worsens Graves’ ophthalmopathy.
For Graves’ dermopathy
If the disease affects your skin (Graves’ dermopathy), use over-the-counter creams or ointments containing hydrocortisone to relieve swelling and reddening. In addition, using compression wraps on your legs may help.
- Girgis, C.M., Champion, B.L., Wall, J.R., (2011). Current Concepts in Graves’ Disease. Therapeutic Advances in Endocrinology and Metabolism; 2(3): 135–144. https://www.ncbi.nlm.nih.gov/pmc/articles/PMC3474632/[↩][↩]
- Stan, M.N., Bahn, R.S. (2010). Risk factors for development or deterioration of Graves’ ophthalmopathy. Thyroid; 20(7): 777–783. https://www.ncbi.nlm.nih.gov/pmc/articles/PMC3357079/[↩][↩][↩]
- Janegova, A., Janega, P., Rychly, B., Kuracinova, K., Babal, P. (2015). The role of Epstein-Barr virus infection in the development of autoimmune thyroid diseases. Endokrynologia Polska; 66(2): 132–136. https://www.ncbi.nlm.nih.gov/pubmed/25931043[↩]
- Tanda, M.L., Piantanida, E., Liparulo, L., Veronesi, G., Lai, A., Sassi, L., … Bartalena, L. (2013). Prevalence and natural history of Graves’ orbitopathy in a large series of patients with newly diagnosed Graves’ hyperthyroidism seen at a single center. Journal of Clinical Endocrinology & Metabolism; 98(4): 1443–1449. https://www.ncbi.nlm.nih.gov/pubmed/23408569[↩][↩][↩][↩]
- Quintono-Moro, A., Zantut-Wittmann, D., Tambascia, M., da Costa Machado, H., Fernandes, A. (2014). High prevalence of infertility among women with Graves’ disease and Hashimoto’s thyroiditis. (link is external) International Journal of Endocrinology. doi:10.1155/2014/982705. https://www.hindawi.com/journals/ije/2014/982705/cta/[↩]
- American Thyroid Association. https://www.thyroid.org/thyroid-disease-pregnancy/[↩]
- Quintono-Moro, A., Zantut-Wittmann, D., Tambascia, M., da Costa Machado, H., Fernandes, A. (2014). High prevalence of infertility among women with Graves’ disease and Hashimoto’s thyroiditis. International Journal of Endocrinology. doi:10.1155/2014/982705. https://www.hindawi.com/journals/ije/2014/982705/cta/[↩]